Prevalence of Cardiovascular Risk Factors Among Adults in the European Union: A Systematic Review with Meta-Analysis
Abstract
1. Introduction
2. Materials and Methods
2.1. Protocol
2.2. Eligibility Criteria
2.3. Information Sources
2.4. Search Strategy
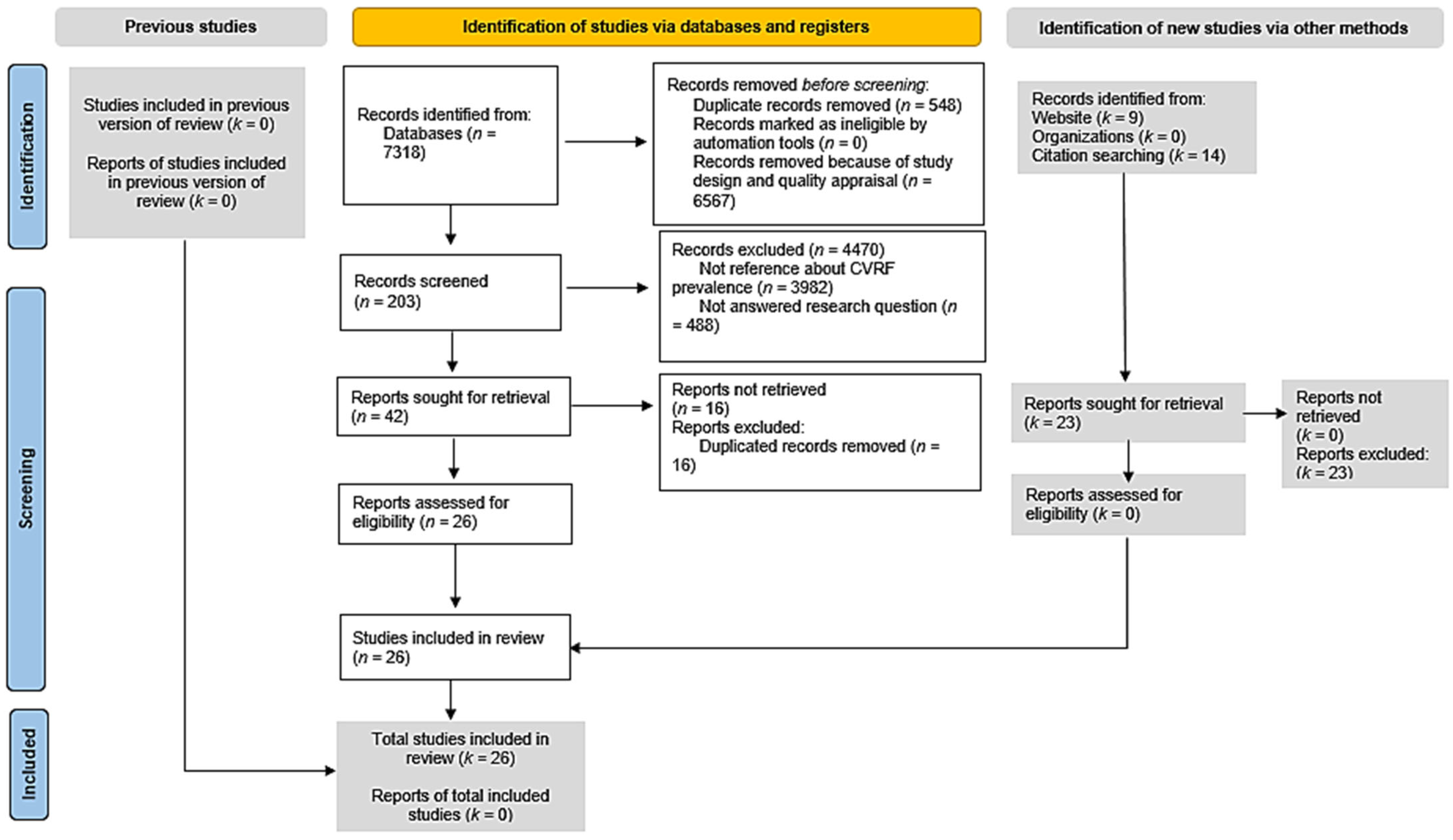
2.5. Selection of Studies
2.6. Data Collection
2.7. Data Aggregation
2.8. Risk of Bias
2.9. Synthesis Methods
2.10. Reporting the Risk of Bias
2.11. Assessment of Certainty
2.12. Data Analysis
3. Results
3.1. Review of Main Results
3.2. Individual Study Results and Characteristics
3.2.1. EUROASPIRE V
3.2.2. Belgium
3.2.3. Croatia
3.2.4. Cyprus
3.2.5. Czech Republic
3.2.6. Estonia
3.2.7. France
3.2.8. Germany
3.2.9. Greece
3.2.10. Hungary
3.2.11. Ireland
3.2.12. Italy
3.2.13. Lithuania
3.2.14. Luxembourg
3.2.15. The Netherlands
3.2.16. Poland
3.2.17. Portugal
3.2.18. Romania
3.2.19. Spain
3.2.20. Sweden
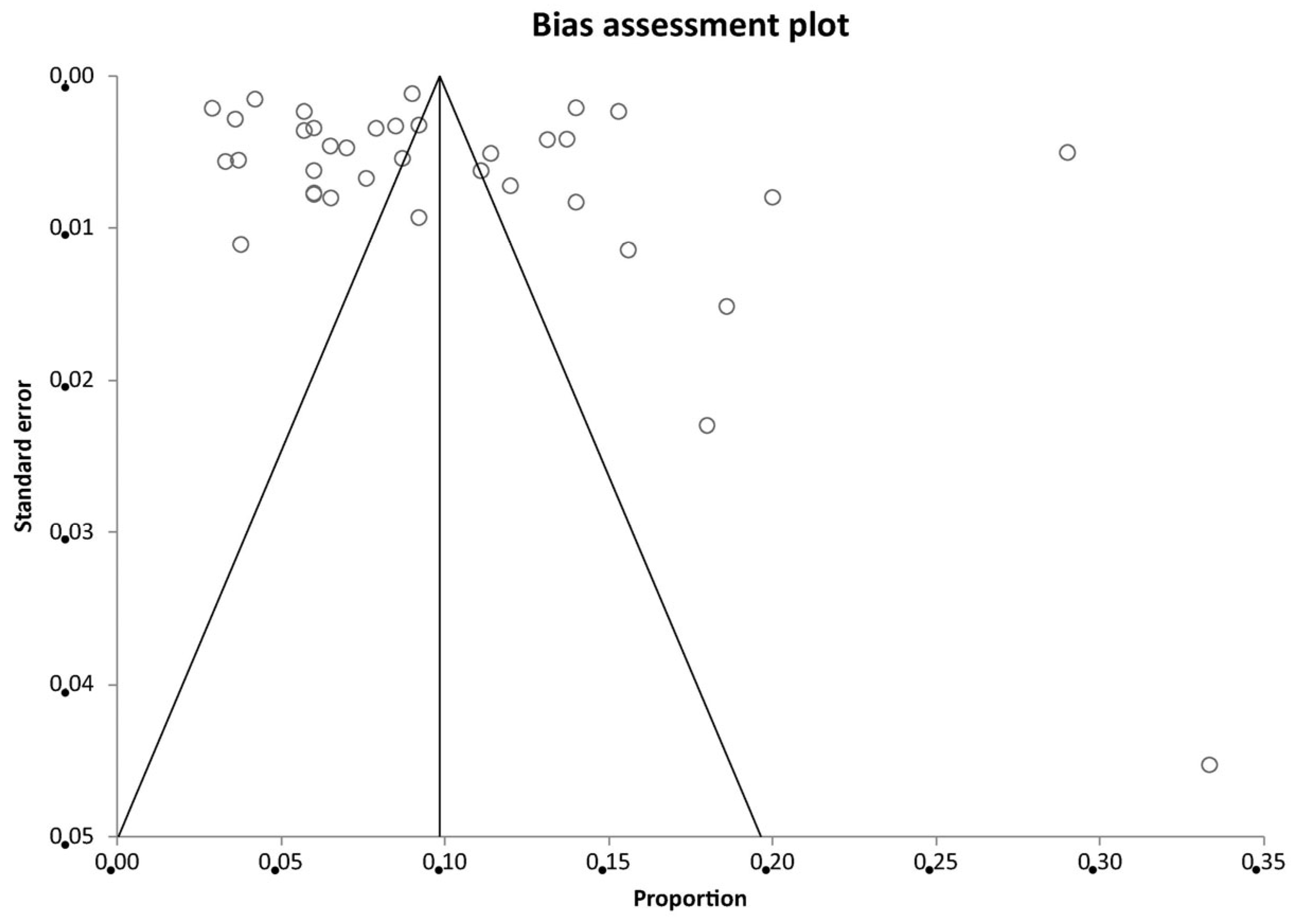
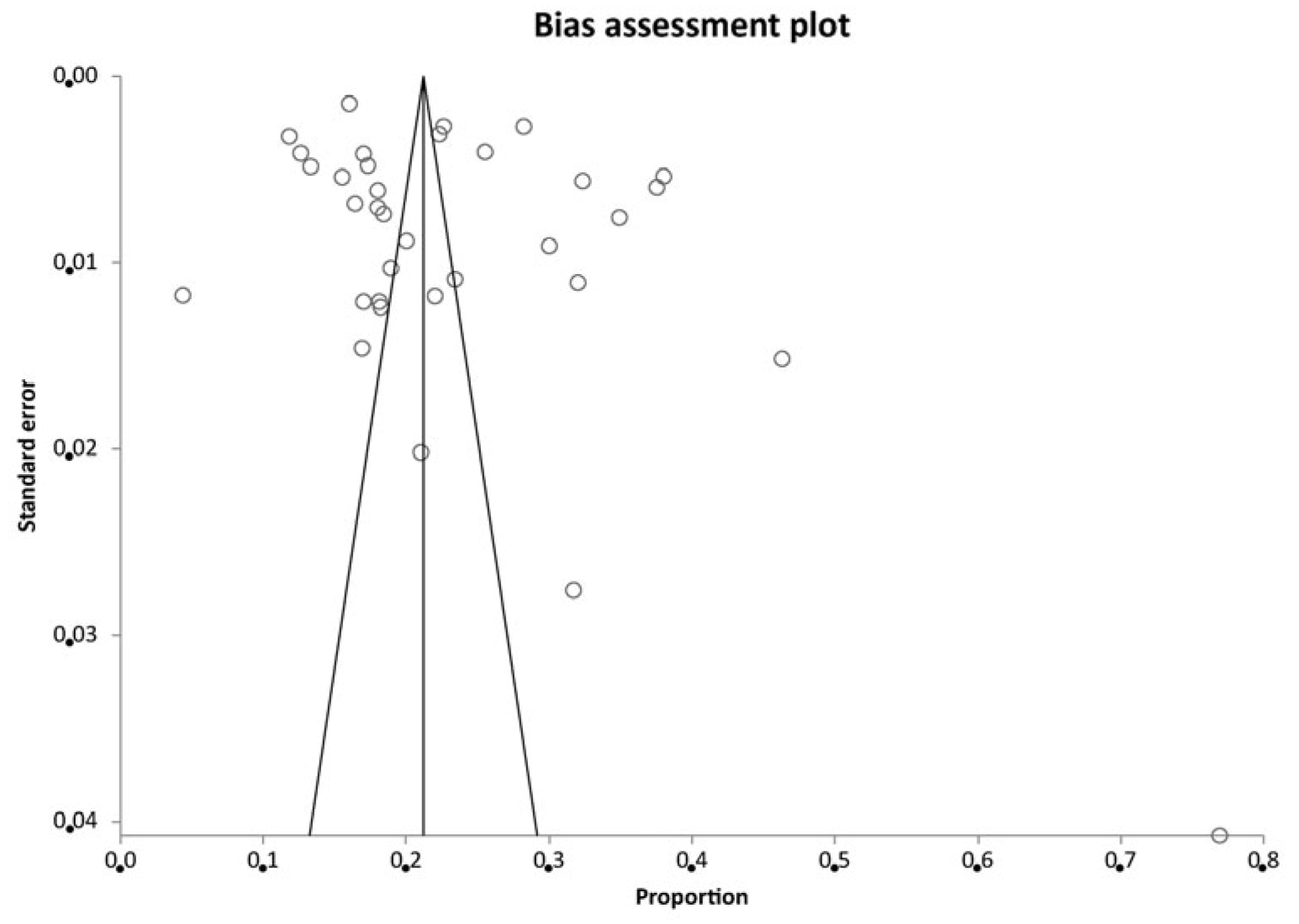
3.3. Risk of Bias
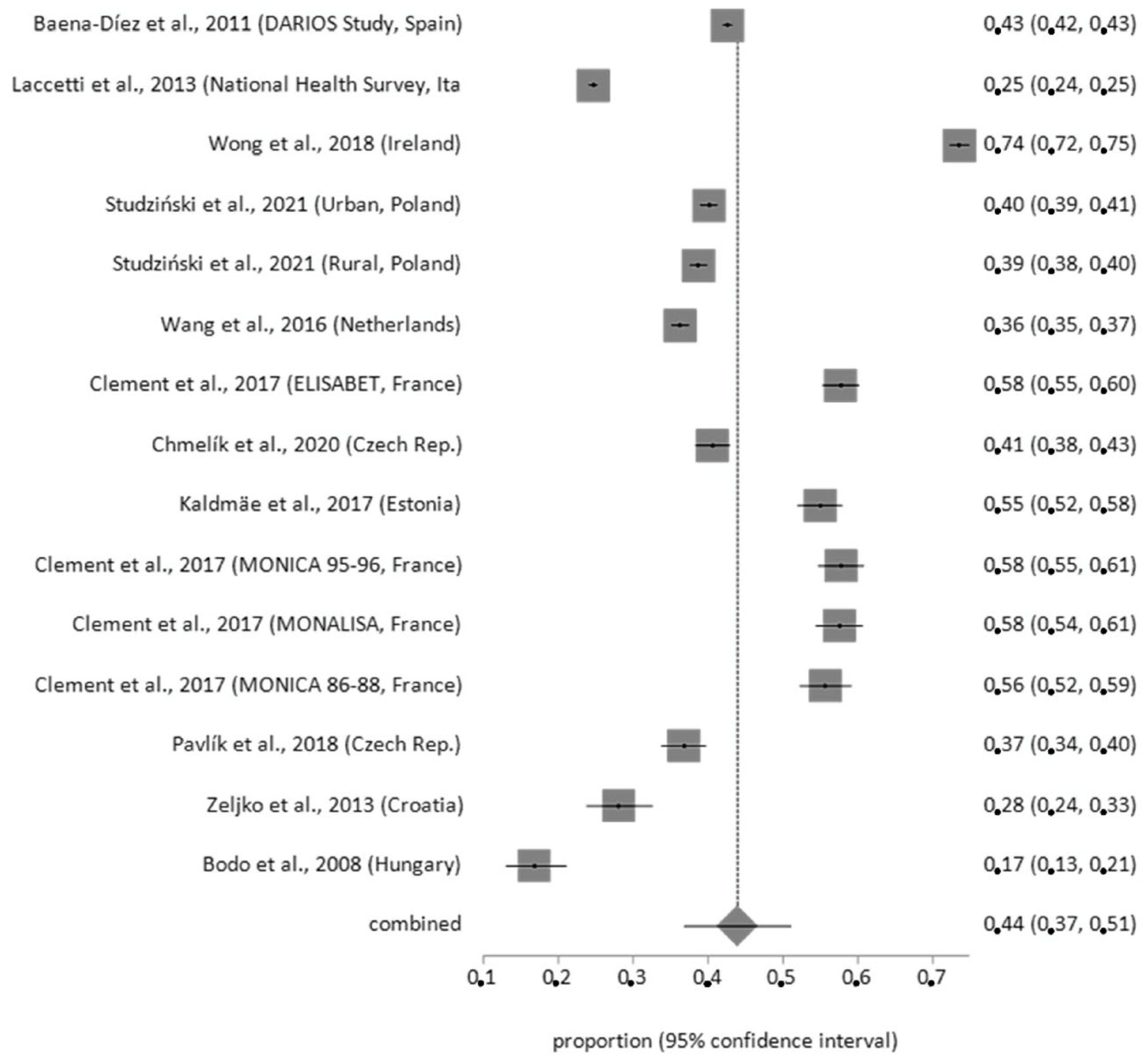
3.4. Synthesis of Results and Meta-Analysis
4. Discussion
4.1. Interpretation of Studies
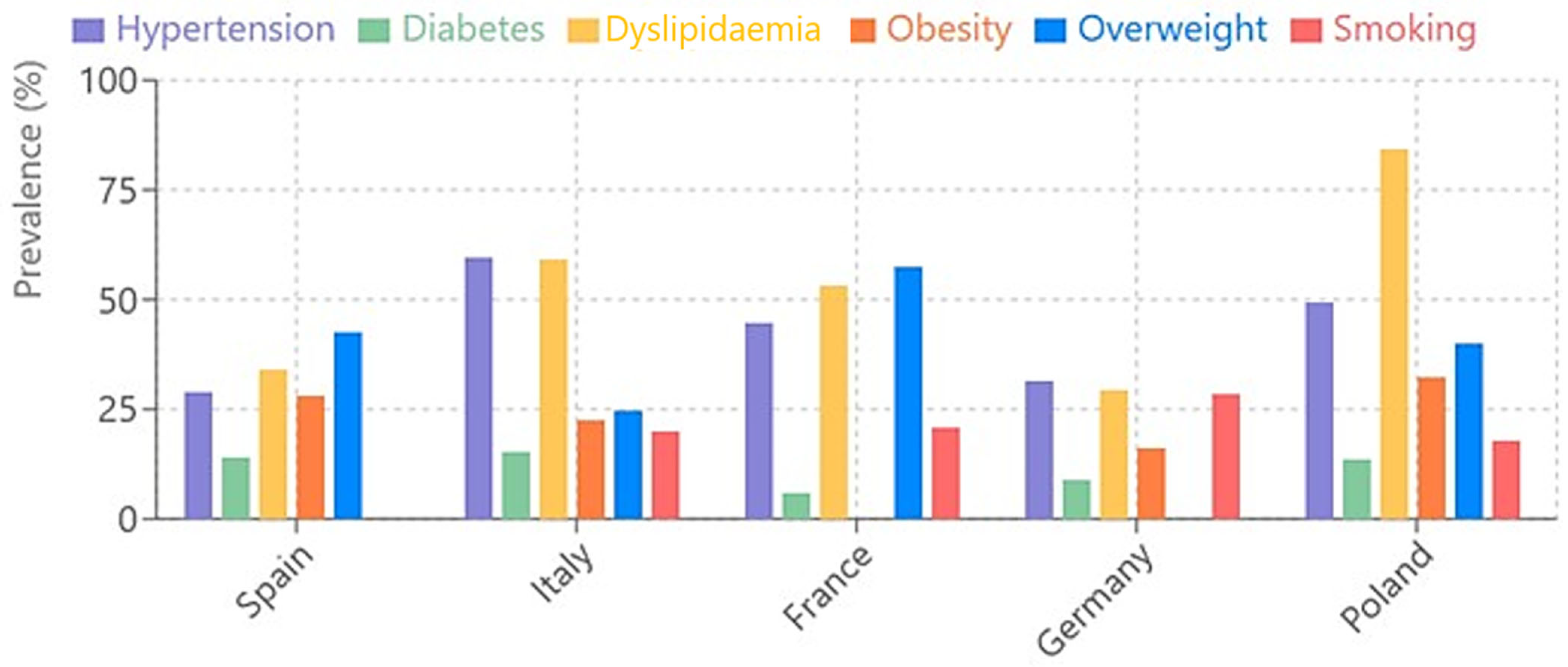
- It can be seen that Poland has the highest prevalence of dyslipidaemia (84.22%), which is significantly higher than in the other countries.
- Italy has the highest prevalence of hypertension (59.6%), followed by Poland (49.54%) and France (44.8%).
- France has the lowest value for diabetes (6%), while Italy has the highest value (15.3%).
- Overweight is particularly high in France (57.5%) and Spain (42.6%).
- Obesity varies considerably, being highest in Poland (32.34%) and lowest in Germany (16%).
4.2. Insights to Inform Public Health Policies and Strategies
4.3. Limitations
5. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Conflicts of Interest
Abbreviations
| CVRF | Cardiovascular Risk Factor |
| CVD | Cardiovascular Disease |
| HBP | High Blood Pressure |
| DM/DM2 | Diabetes Mellitus/Type 2 Diabetes Mellitus |
| MS | Metabolic Syndrome |
| Hcol | Hypercholesterolemia |
| Htri | Hypertriglyceridemia |
| SCORE | Systematic Coronary Risk Evaluation |
| REGICOR | Registre Gironí del Cor |
| LE | Level of Evidence |
| DR | Degree of Recommendation |
| SING/SIGN | Scottish Intercollegiate Guidelines Network |
| CASPe | Critical Appraisal Skills Programme español |
| IDF | International Diabetes Federation |
| AHA | American Heart Association |
| NCEP | National Cholesterol Education Program |
| EU | European Union |
| PRISMA | Preferred Reporting Items for Systematic Reviews and Meta-Analyses |
| CoCoPop | Condition, Context, Population |
| VHL | Virtual Health Library |
| LILACS | Latin American and Caribbean Health Sciences Literature |
| Redalyc | Red de Revistas Científicas de Acceso Abierto Diamante |
Appendix A. Supplementary Tables
| Database | Date | Search Equations | Total Articles | Selected Articles (Titles And Abstracts) | Selected Articles (After Full Reading) | Selected Articles (After Removing Duplicates) |
|---|---|---|---|---|---|---|
| Pubmed | 18 June 2024 | Cardiovascular risk factors AND prevalence AND Europe | 621 | 54 | 3 | 1 |
| Virtual Health Library | 18 June 2024 | Cardiovascular risk factors AND prevalence AND Europe | 130 | 12 | 2 | 0 |
| LILACS | 26 March 2025 | Cardiovascular risk factors AND prevalence AND Europe | 2 | 0 | 0 | 0 |
| Dialnet | 26 March 2025 | Cardiovascular risk factors AND prevalence AND Europe | 1 | 0 | 0 | 0 |
| Scielo | 26 March 2025 | Cardiovascular risk factors AND prevalence AND Europe | 6 | 0 | 0 | 0 |
| Redalyc | 26 March 2025 | Cardiovascular risk factors AND prevalence AND Europe | 2418 | 23 | 23 | 0 |
| Pubmed | 18 June 2024 | Cardiovascular risk factors AND prevalence AND Germany | 550 | 32 | 1 | 1 |
| Pubmed | 18 June 2024 | Cardiovascular risk factors AND prevalence AND Belgium | 161 | 28 | 1 | 1 |
| Pubmed | 18 June 2024 | Cardiovascular risk factors AND prevalence AND Croatia | 241 | 14 | 4 | 1 |
| Pubmed | 18 June 2024 | Cardiovascular risk factors AND prevalence AND Denmark | 238 | 0 | 0 | 0 |
| Pubmed | 18 June 2024 | Cardiovascular risk factors AND prevalence AND Ireland | 108 | 1 | 1 | 1 |
| Pubmed | 18 June 2024 | Cardiovascular risk factors AND prevalence AND Latvia | 9 | 0 | 0 | 0 |
| Pubmed | 18 June 2024 | Cardiovascular risk factors AND prevalence AND Luxembourg | 19 | 1 | 1 | 1 |
| Pubmed | 18 June 2024 | Cardiovascular risk factors AND prevalence AND Netherlands | 524 | 1 | 1 | 1 |
| Pubmed | 18 June 2024 | Cardiovascular risk factors AND prevalence AND Sweden | 359 | 27 | 1 | 1 |
| Pubmed | 18 June 2024 | Cardiovascular risk factors AND prevalence AND Italy | 635 | 5 | 5 | 2 |
| Pubmed | 18 June 2024 | Cardiovascular risk factors AND prevalence AND Bulgaria | 21 | 0 | 0 | 0 |
| Pubmed | 18 June 2024 | Cardiovascular risk factors AND prevalence AND Slovakia | 26 | 3 | 0 | 0 |
| Pubmed | 18 June 2024 | Cardiovascular risk factors AND prevalence AND Estonia | 22 | 1 | 1 | 1 |
| Pubmed | 18 June 2024 | Cardiovascular risk factors AND prevalence AND Greece | 7 | 4 | 4 | 1 |
| Pubmed | 18 June 2024 | Cardiovascular risk factors AND prevalence AND Malta | 6 | 0 | 0 | 0 |
| Pubmed | 18 June 2024 | Cardiovascular risk factors AND prevalence AND Poland | 178 | 3 | 2 | 2 |
| Pubmed | 18 June 2024 | Cardiovascular risk factors AND prevalence AND Czech Republic | 59 | 2 | 2 | 2 |
| Pubmed | 18 June 2024 | Cardiovascular risk factors AND prevalence AND Austria | 130 | 0 | 0 | 0 |
| Pubmed | 18 June 2024 | Cardiovascular risk factors AND prevalence AND Cyprus | 27 | 2 | 2 | 1 |
| Pubmed | 18 June 2024 | Cardiovascular risk factors AND prevalence AND Slovenia | 32 | 1 | 0 | 0 |
| Pubmed | 18 June 2024 | Cardiovascular risk factors AND prevalence AND Finland | 143 | 0 | 0 | 0 |
| Pubmed | 18 June 2024 | Cardiovascular risk factors AND prevalence AND Hungary | 39 | 2 | 2 | 1 |
| Pubmed | 18 June 2024 | Cardiovascular risk factors AND prevalence AND Lithuania | 12 | 1 | 1 | 1 |
| Pubmed | 18 June 2024 | Cardiovascular risk factors AND prevalence AND Portugal | 77 | 2 | 2 | 1 |
| Pubmed | 18 June 2024 | Cardiovascular risk factors AND prevalence AND Romania | 69 | 2 | 1 | 1 |
| Pubmed | 18 June 2024 | Cardiovascular risk factors AND prevalence AND Spain | 233 | 4 | 4 | 4 |
| Pubmed | 18 June 2024 | Cardiovascular risk factors AND prevalence AND France | 215 | 1 | 1 | 1 |
| Total | 7318 | 218 | 55 | 26 | ||
Appendix B. Supplementary Figures



References
- Sacramento-Pacheco, J.; Duarte-Clíments, G.; Gómez-Salgado, J.; Romero-Martín, M.; Sánchez-Gómez, M.B. Cardiovascular risk assessment tools: A scoping review. Aust. Crit. Care 2019, 32, 540–559. [Google Scholar] [CrossRef]
- Michas, G.; Karvelas, G.; Trikas, A. Cardiovascular disease in Greece; the latest evidence on risk factors. Hell. J. Cardiol. 2019, 60, 271–275. [Google Scholar] [CrossRef]
- Cayuela, L.; Gómez-Enjuto, S.; Olivares-Martínez, B.; Rodríguez-Domínguez, S.; Cayuela, A. ¿Se está desacelerando el ritmo de disminución de la mortalidad cardiovascular en España? Rev. Esp. Cardiol. 2021, 74, 750–756. [Google Scholar] [CrossRef]
- Diederichs, C.; Neuhauser, H.; Kroll, L.E.; Lange, C.; Mensink, G.; Dornquast, C.; Heidemann, C.; Scheidt-Nave, C.; Busch, M. Regionale Unterschiede in der Prävalenz von kardiovaskulären Risikofaktoren bei Männern und Frauen in Deutschland. Bundesgesundheitsblatt—Gesundheitsforschung—Gesundheitsschutz 2017, 60, 151–162. [Google Scholar] [CrossRef]
- Dev, R.; Adams, A.M.; Raparelli, V.; Norris, C.M.; Pilote, L.; GOING-FWD Investigators. Sex and Gender Determinants of Vascular Disease in the Global Context. Can. J. Cardiol. 2022, 38, 1799–1811. [Google Scholar] [CrossRef]
- Al-Shakarchi, N.J.; Evans, H.; Luchenski, S.A.; Story, A.; Banerjee, A. Cardiovascular disease in homeless versus housed individuals: A systematic review of observational and interventional studies. Heart 2020, 106, 1483–1488. [Google Scholar] [CrossRef]
- Kennedy, O.; Su, F.; Pears, R.; Walmsley, E.; Roderick, P. Evaluating the effectiveness of the NHS Health Check programme in South England: A quasi-randomised controlled trial. BMJ Open 2019, 9, e029420. [Google Scholar] [CrossRef] [PubMed]
- Ruan, Y.; Guo, Y.; Zheng, Y.; Huang, Z.; Sun, S.; Kowal, P.; Shi, Y.; Wu, F. Cardiovascular disease (CVD) and associated risk factors among older adults in six low-and middle-income countries: Results from SAGE Wave 1. BMC Public Health 2018, 18, 778. [Google Scholar] [CrossRef] [PubMed]
- Kotseva, K.; De Backer, G.; De Bacquer, D.; Rydén, L.; Hoes, A.; Grobbee, D.; Maggioni, A.; Marques-Vidal, P.; Jennings, C.; Abreu, A.; et al. Lifestyle and impact on cardiovascular risk factor control in coronary patients across 27 countries: Results from the European Society of Cardiology ESC-EORP EUROASPIRE V registry. Eur. J. Prev. Cardiol. 2019, 26, 824–835. [Google Scholar] [CrossRef] [PubMed]
- Eurostat Statistics Explained. Estadísticas Sobre Causa de Muerte. [Updated 20 September 2018]. Available online: https://ec.europa.eu/eurostat/statistics-explained/index.php?title=Archive:Estad%C3%ADsticas_sobre_causas_de_muerte&oldid=404953 (accessed on 24 July 2023).
- European Hearth Network. Estadísticas Europeas de Enfermedades Cardiovasculares. 2017. Available online: https://ehnheart.org/library/cvd-statistics/european-cardiovascular-disease-statistics-2017/ (accessed on 24 July 2023).
- Lobos-Bejarano, J.M.; Brotons-Cuixart, C. Factores de riesgo cardiovascular y atención primaria: Evaluación e intervención. Aten. Primaria 2011, 43, 668–677. [Google Scholar] [CrossRef] [PubMed]
- Bergum, H.; Sandven, I.; Abdelnoor, M.; Anderssen, S.A.; Grimsmo, J.; Rivrud, D.E.; Myhr, N.E.; Vold, M.B.; Stenbakken, C.; Lidfors, B.; et al. Randomized trial of cardiovascular prevention in Norway combining an in-hospital lifestyle course with primary care follow-up: The Hjerteløftet study. Eur. J. Prev. Cardiol. 2022, 29, 2252–2263. [Google Scholar] [CrossRef]
- Ford, G. Prevalence vs Incidence: What Is the Difference. Cochrane Blog [Sede Web]. [Updated 6 November 2020]. Available online: https://s4be.cochrane.org/blog/2020/11/06/prevalence-vs-incidence-what-is-the-difference/ (accessed on 17 June 2024).
- Page, M.J.; McKenzie, J.E.; Bossuyt, P.M.; Boutron, I.; Hoffmann, T.C.; Mulrow, C.D.; Shamseer, L.; Tetzlaff, J.M.; Akl, E.A.; Brennan, S.E.; et al. The PRISMA 2020 statement: An updated guideline for reporting systematic reviews. BMJ 2021, 372, n71. [Google Scholar] [CrossRef]
- Linares-Espinós, E.; Hernández, V.; Domínguez-Escrig, J.L.; Fernández-Pello, S.; Hevia, V.; Mayor, J.; Padilla-Fernández, B.; Ribal, M.J. Methodology of a systematic review. Actas. Urol. Esp. 2018, 42, 499–506. [Google Scholar] [CrossRef]
- Munn, Z.; Stern, C.; Aromataris, E.; Lockwood, C.; Jordán, Z. ¿Qué tipo de revisión sistemática debo realizar? Una tipología propuesta y orientación para revisores sistemáticos en las ciencias médicas y de la salud. Método BMC Med. Res. 2018, 18, 5. [Google Scholar]
- van den Akker, O.R.; Peters, G.Y.; Bakker, C.J.; Carlsson, R.; Coles, N.A.; Corker, K.S.; Feldman, G.; Moreau, D.; Nordström, T.; Pickering, J.S.; et al. Increasing the transparency of systematic reviews: Presenting a generalized registration form. Syst. Rev. 2023, 12, 170. [Google Scholar] [CrossRef]
- Servicio Público de Empleo Estatal (SEPE), Ministerio de Trabajo y Economía Social, Gobierno de España. Países de la Unión Europea y del Espacio Económico Europeo. Available online: https://www.sepe.es/HomeSepe/Personas/distributiva-prestaciones/paises-ue.html#:~:text=Pa%C3%ADses%20de%20la%20Uni%C3%B3n%20Europea%20(UE)%3A%20Alemania%2C%20B%C3%A9lgica%2C,%2C%20Lituania%2C%20Portugal%20y%20Ruman%C3%ADaç (accessed on 28 June 2023).
- Unión Europea. Perfiles de los Países. Available online: https://european-union.europa.eu/principles-countries-history/country-profiles_es?page=0 (accessed on 28 June 2023).
- Cabello, J.B. Chapter 11. Critical Appraisal of Reviews of Clinical Evidence. In Critical Appraisal Skills Programme Español (CASPe). Lectura Crítica de la Evidencia Clínica, 2nd ed.; Elsevier: Barcelona, Spain, 2021; pp. 122–134. [Google Scholar]
- Cabello, J.B. Chapter 7. Critical Appraisal of Prognostic Studies: Cohort Studies. In Critical Appraisal Skills Programme Español (CASPe). Lectura Crítica de la Evidencia Clínica, 2nd ed.; Elsevier: Barcelona, Spain, 2021; pp. 67–77. [Google Scholar]
- Berra, S.; Elorza-Ricart, J.M.; Estrada, M.D.; Sánchez, E. Aroot for the critical appraisal of epidemiological cross-sectional studies. Gac. Sanit. 2008, 22, 492–497. [Google Scholar] [CrossRef] [PubMed]
- Sekhon, M.; de Thurah, A.; Fragoulis, G.E.; Schoones, J.; Stamm, T.A.; Vliet Vlieland, T.P.M.; Esbensen, B.A.; Lempp, H.; Bearne, L.; Kouloumas, M.; et al. Synthesis of guidance available for assessing methodological quality and grading of evidence from qualitative research to inform clinical recommendations: A systematic literature review. RMD Open 2024, 10, e004032. [Google Scholar] [CrossRef]
- Streel, S.; Donneau, A.F.; Hoge, A.; Majerus, S.; Kolh, P.; Chapelle, J.P.; Albert, A.; Guillaume, M. Socioeconomic Impact on the Prevalence of Cardiovascular Risk Factors in Wallonia, Belgium: A Population-Based Study. BioMed Res. Int. 2015, 2015, 580849. [Google Scholar] [CrossRef] [PubMed]
- Zeljko, H.M.; Skarić-Jurić, T.; Narančić, N.S.; Barešić, A.; Tomas, Z.; Petranović, M.Z.; Miličić, J.; Salihović, M.P.; Janićijević, B. Age trends in prevalence of cardiovascular risk factors in Roma minority population of Croatia. Econ. Hum. Biol. 2013, 11, 326–336. [Google Scholar] [CrossRef] [PubMed]
- Panagiotakos, D.B.; Kinlaw, M.; Papaerakleous, N.; Papoutsou, S.; Toutouzas, P.; Polychronopoulos, E. Depressive symptomatology and the prevalence of cardiovascular risk factors among older men and women from Cyprus; the MEDIS (Mediterranean Islands Elderly) epidemiological study. J. Clin. Nurs. 2008, 17, 688–695. [Google Scholar] [CrossRef]
- Pavlík, V.; Fajfrová, J.; Šafka, V.; Pravdová, L.; Urban, M.; Krutišová, P.; Tuček, M. Prevalence of risk factors in cardiovascular diseases in selected population of the Czech Republic. Cent. Eur. J. Public Health 2018, 26, 118–123. [Google Scholar] [CrossRef]
- Chmelík, Z.; Vaclová, M.; Lánská, V.; Laštůvka, J.; Vrablík, M. Analysis of incidence and prevalence of cardiovascular risk factors and evaluation of their control in epidemiological survey in the Czech Republic. Cent. Eur. J. Public Health 2020, 28, 114–119. [Google Scholar] [CrossRef]
- Kaldmäe, M.; Zemtsovskaja, G.; Abina, J.; Land, T.; Viigimaa, M. Prevalence of cardiovascular disease risk factors in Tallinn, Estonia. Medicina 2017, 53, 268–276. [Google Scholar] [CrossRef]
- Clement, G.; Giovannelli, J.; Cottel, D.; Montaye, M.; Ciuchete, A.; Dallongeville, J.; Amouyel, P.; Dauchet, L. Changes over time in the prevalence and treatment of cardiovascular risk factors, and contributions to time trends in coronary mortality over 25 years in the Lille urban area (northern France). Arch. Cardiovasc. Dis. 2017, 110, 689–699. [Google Scholar] [CrossRef]
- Bodo, M.; Thróczy, G.; Pánczél, G.; Sipos, K. Prevalence of stroke/cardiovascular risk factors in rural Hungary—A cross—Sectional descriptive study. Ideggyogy. Sz. 2008, 61, 87–96. [Google Scholar]
- Wong, T.Y.; Massa, M.S.; O’Halloran, A.M.; Kenny, R.A.; Clarke, R. Cardiovascular risk factors and frailty in a cross-sectional study of older people: Implications for prevention. Age Ageing 2018, 47, 714–720. [Google Scholar] [CrossRef]
- Tocci, G.; Ferrucci, A.; Passerini, J.; Averna, M.; Bellotti, P.; Bruno, G.; Cosentino, F.; Crepaldi, G.; Giannattasio, C.; Modena, M.G.; et al. Prevalence of ‘borderline’ values of cardiovascular risk factors in the clinical practice of general medicine in Italy: Results of the BORDERLINE study. High Blood Press. Cardiovasc. Prev. 2011, 18, 43–51. [Google Scholar] [CrossRef]
- Laccetti, R.; Pota, A.; Stranges, S.; Falconi, C.; Memoli, B.; Bardaro, L.; Guida, B. Evidence on the prevalence and geographic distribution of major cardiovascular risk factors in Italy. Public Health Nutr. 2013, 16, 305–315. [Google Scholar] [CrossRef] [PubMed]
- Burokienė, N.; Domarkienė, I.; Ambrozaitytė, L.; Uktverytė, I.; Meškienė, R.; Karčiauskaitė, D.; Kasiulevičius, V.; Šapoka, V.; Kučinskas, V.; Kučinskienė, Z.A. Classical rather than genetic risk factors account for high cardiovascular disease prevalence in Lithuania: A cross-sectional population study. Adv. Med. Sci. 2017, 62, 121–128. [Google Scholar] [CrossRef] [PubMed]
- Alkerwi, A.; Sauvageot, N.; El Bahi, I.; Delagardelle, C.; Beissel, J.; Noppe, S.; Roderick, P.J.; Mindell, J.S.; Stranges, S. Prevalence and related risk factors of chronic kidney disease among adults in Luxembourg: Evidence from the observation of cardiovascular risk factors (ORISCAV-LUX) study. BMC Nephrol. 2017, 18, 358. [Google Scholar] [CrossRef] [PubMed]
- Wang, X.; Bots, M.L.; Yang, F.; Sun, J.; He, S.; Hoes, A.W.; Niu, J.; Vaartjes, I. A comparison of the prevalence and clustering of major cardiovascular risk factors in the Netherlands and China. Eur. J. Prev. Cardiol. 2016, 23, 1766–1773. [Google Scholar] [CrossRef]
- Trzeciak, B.G.; Gutknecht, P.; Molisz, A.; Nowicka-Sauer, K.; Buczkowski, K.; Siebert, J. Porównanie czynników ryzyka chorób sercowo-naczyniowych w województwach północnej i południowej części Polski. Fam. Med. Prim. Care Rev. 2013, 15, 198–199. [Google Scholar]
- Studziński, K.; Tomasik, T.; Windak, A.; Banach, M.; Wójtowicz, E.; Mastej, M.; Tomaszewski, M.; Mikhailidis, D.P.; Toth, P.P.; Catapano, A.; et al. The Differences in the Prevalence of Cardiovascular Disease, Its Risk Factors, and Achievement of Therapeutic Goals among Urban and Rural Primary Care Patients in Poland: Results from the LIPIDOGRAM 2015 Study. J. Clin. Med. 2021, 10, 5656. [Google Scholar] [CrossRef]
- Alves, L.; Azevedo, A.; Barros, H.; Vollenweider, P.; Waeber, G.; Marques-Vidal, P. Prevalence and management of cardiovascular risk factors in Portuguese living in Portugal and Portuguese who migrated to Switzerland. BMC Public Health 2015, 15, 307. [Google Scholar] [CrossRef] [PubMed][Green Version]
- Rus, M.; Crisan, S.; Andronie-Cioara, F.L.; Indries, M.; Marian, P.; Pobirci, O.L.; Ardelean, A.I. Prevalence and Risk Factors of Metabolic Syndrome: A Prospective Study on Cardiovascular Health. Medicina 2023, 59, 1711. [Google Scholar] [CrossRef]
- Baena-Díez, J.M.; Félix-Redondo, F.J.; Grau-Magaña, M.; Cabrera de León, A.; Sanz, H.; Leal, M.; Elosua, R.; Rodríguez-Pérez, M.C.; Guembe, M.J.; Torán, P.; et al. Tratamiento y control de los factores de riesgo según el riesgo coronario en la población española del estudio DARIOS. Rev. Esp. Cariol. 2011, 64, 766–773. [Google Scholar] [CrossRef]
- Félix-Redondo, F.J.; Grau, M.; Baena-Díez, J.M.; Dégano, I.R.; de León, A.C.; Guembe, M.J.; Alzamora, M.T.; Vega-Alonso, T.; Robles, N.R.; Ortiz, H.; et al. Prevalence of obesity and associated cardiovascular risk: The DARIOS study. BMC Public Health 2013, 13, 542. [Google Scholar] [CrossRef] [PubMed]
- Fernández-Bergés, D.; Cabrera de León, A.; Sanz, H.; Elosua, R.; Guembe, M.J.; Alzamora, M.; Vega-Alonso, T.; Félix-Redondo, F.J.; Ortiz-Marrón, H.; Rigo, F.; et al. Síndrome metabólico en España: Prevalencia y riesgo coronario asociado a la definición armonizada y a la propuesta por la OMS. Estudio DARIOS. Rev. Esp. Cardiol. 2012, 65, 241–248. [Google Scholar] [CrossRef]
- Sacramento-Pacheco, J.; Sánchez-Gómez, M.B.; Gómez-Salgado, J.; Novo-Muñoz, M.M.; Duarte-Clíments, G. Prevalence of Cardiovascular Risk Factors in Spain: A Systematic Review. J. Clin. Med. 2023, 12, 6944. [Google Scholar] [CrossRef]
- Welin, L.; Adlerberth, A.; Caidahl, K.; Eriksson, H.; Hansson, P.O.; Johansson, S.; Rosengren, A.; Svärdsudd, K.; Welin, C.; Wilhelmsen, L. Prevalence of cardiovascular risk factors and the metabolic syndrome in middle-aged men and women in Gothenburg, Sweden. BMC Public Health 2008, 8, 403. [Google Scholar] [CrossRef] [PubMed]
- Salari, A.; Mahdavi-Roshan, M.; Hasandokht, T.; Gholipour, M.; Soltanipour, S.; Nagshbandi, M.; Javadzadeh, A. Nutritional intake, depressive symptoms and vitamin D status in hypertensive patients in the north of Iran: A case-control study. Hipertens. Riesgo Vasc. 2017, 34, 65–71. [Google Scholar] [CrossRef] [PubMed]
- Collazos-Perdomo, D.; Ramirez-Ramos, C.F.; Torres de Galvis, M.Y.; Correas-Orozco, L.; Ramirez-Mendez, D.; Castilla Agudelo, G.A.; Martinez Cano, C.A.; Gallego, C.; Saldarriaga, C. Association between major depression and arterial hypertension in a Colombian population. Hipertens. Riesgo Vasc. 2020, 37, 162–168. [Google Scholar] [CrossRef] [PubMed]
| Reference | Type of Study | Critical Reading | Synthesis of the Evidence 3 LE/DR |
|---|---|---|---|
| Cardiovascular disease in Greece; the latest evidence on risk factors [2] | Systematic review | 8/10 2 | LE: 2++ DR: B |
| Regionale Unterschiede in der Prävalenz von kardiovaskulären Risikofaktoren bei Männern und Frauen in Deutschland [4] | Cross-sectional study | High quality 1 | LE: 2++ DR: B |
| Lifestyle and impact on cardiovascular risk factor control in coronary patients across 27 countries: Results from the European Society of Cardiology ESC-EORP EUROASPIRE V registry [9] | Cross-sectional study | High quality 1 p < 0.001–0.0001 | LE: 2++ DR: B |
| Impact on the Prevalence of Cardiovascular Risk Factors in Wallonia, Belgium: A Population-Based Study [25] | Cross-sectional study | High quality 1 p < 0.0001–0.46 | LE: 2++ DR: B |
| Age trends in prevalence of cardiovascular risk factors in Roma minority population of Croatia [26] | Cross-sectional study | High quality 1 p < 0.001–0.98 | LE: 2++ DR: B |
| Depressive symptomatology and the prevalence of cardiovascular risk factors among older men and women from Cyprus; the MEDIS (Mediterranean Islands Elderly) epidemiological study [27] | Cross-sectional study | High quality 1 p < 0.001–0.98 | LE: 2++ DR: B |
| Prevalence of risk factors in cardiovascular diseases in selected population of the Czech Republic [28] | Cross-sectional study | High quality 1 p < 0.001 | LE: 2++ DR: B |
| Analysis of incidence and prevalence of cardiovascular risk factors and evaluation of their control in epidemiological survey in the Czech Republic [29] | Cross-sectional study | High quality 1 | LE: 2++ DR: B |
| Prevalence of cardiovascular disease risk factors in Tallinn, Estonia [30] | Cross-sectional study | High quality 1 p < 0.001–1 | LE: 2++ DR: B |
| Changes over time in the prevalence and treatment of cardiovascular risk factors, and contributions to time trends in coronary mortality over 25 years in the Lille urban area (northern France) [31] | Cross-sectional study | High quality 1 p < 0.0001–0.95 | LE: 2++ DR: B |
| Prevalence of stroke/cardiovascular risk factors in rural Hungary—A cross—sectional descriptive study [32] | Cross-sectional study | High quality 1 p < 0.0001–0.038 | LE: 2++ DR: B |
| Cardiovascular risk factors and frailty in a cross-sectional study of older people: implications for prevention [33] | Cross-sectional study | High quality 1 p < 0.001 | LE: 2++ DR: B |
| Prevalence of ‘borderline’ values of cardiovascular risk factors in the clinical practice of general medicine in Italy: results of the BORDERLINE study [34] | Cross-sectional study | High quality 1 p < 0.05 | LE: 2++ DR: B |
| Evidence on the prevalence and geographic distribution of major cardiovascular risk factors in Italy [35] | Cross-sectional study | High quality 1 p < 0.001–0.488 | LE: 2++ DR: B |
| Classical rather than genetic risk factors account for high cardiovascular disease prevalence in Lithuania: A cross-sectional population study [36] | Cross-sectional study | High quality 1 p < 0.001–1 | LE: 2++ DR: B |
| Prevalence and related risk factors of chronic kidney disease among adults in Luxembourg: evidence from the observation of cardiovascular risk factors (ORISCAV-LUX) study [37] | Cross-sectional study | High quality 1 p < 0.001–0.01 | LE: 2++ DR: B |
| A comparison of the prevalence and clustering of major cardiovascular risk factors in the Netherlands and China [38] | Cross-sectional study | High quality 1 p < 0.05 | LE: 2++ DR: B |
| Porównanie czynników ryzyka chorób sercowo-naczyniowych w województwach północnej i południowej części Polski [39] | Cross-sectional study | High quality 1 p < 0.001–0.1 | LE: 2++ DR: B |
| The Differences in the Prevalence of Cardiovascular Disease, Its Risk Factors, and Achievement of Therapeutic Goals among Urban and Rural Primary Care Patients in Poland: Results from the LIPIDOGRAM 2015 Study [40] | Cross-sectional study | High quality 1 p < 0.01–0.92 | LE: 2++ DR: B |
| Prevalence and management of cardiovascular risk factors in Portuguese living in Portugal and Portuguese who migrated to Switzerland [41] | Cross-sectional study | High quality 1 p < 0.001–0.99 | LE: 2++ DR: B |
| Prevalence and Risk Factors of Metabolic Syndrome: A Prospective Study on Cardiovascular Health [42] | Cross-sectional study | High quality 1 p < 0.0009–0.71 | LE: 2++ DR: B |
| Tratamiento y control de los factores de riesgo según el riesgo coronario en la población española del estudio DARIOS [43] | Pooled analysis of 11 population-based studies (Cross-sectional study) | High quality 1 p < 0.01–0.024 | LE: 2++ DR: B |
| Prevalence of obesity and associated cardiovascular risk: the DARIOS study [44] | Pooled analysis of 11 population-based studies (Cross-sectional study) | High quality 1 p < 0.00–0.05 | LE: 2++ DR: B |
| Síndrome metabólico en España: prevalencia y riesgo coronario asociado a la definición armonizada y a la propuesta por la OMS. Estudio DARIOS [45] | Pooled analysis of 11 population-based studies (Cross-sectional study) | High quality 1 p < 0.001 | LE: 2++ DR: B |
| Prevalence of Cardiovascular Risk Factors in Spain: A Systematic Review [46] | Systematic review | 10/10 2 | LE: 2++ DR: B |
| Prevalence of cardiovascular risk factors and the metabolic syndrome in middle-aged men and women in Gothenburg, Sweden [47] | Cross-sectional study | High quality 1 p < 0.001 | LE: 2++ DR: B |
| Country | N 1 | Age Range | Male Sex (%) | Female Sex (%) | |
|---|---|---|---|---|---|
| EUROASPIRE | 8261 | 18–80 | 74.3 | 25.7 | |
| Belgium | 1017 | 20–69 | 49.9 | 50.1 | |
| Croatia | 19,070 2 430 3 | 18–65 2 18–84 3 | 35.12 3 | 64.88 3 | |
| Cyprus | 300 | >65 | 45.34 | 54.66 | |
| Czech Republic | 1051 4 1812 5 | >40 in males 5 >50 in females 5 | 45.86 4 53.03 5 | 54.14 4 46.97 5 | |
| Estonia | 1111 | 20–65 | 46 | 54 | |
| France | 860 6 1021 7 1021 8 1636 9 | 40–64 6–9 | 52.7 6 49 7 50.4 8 47.3 9 | 47.3 6 51 7 49.6 8 52.7 9 | |
| Germany | 62,606 | 18–99 in males 18–100 in females | 48.9 | 50.9 | |
| Greece | EPIC STUDY | 26,913 | 25–86 | ||
| NAOUSSA | 1937 | 15–73 | |||
| MEDICAL EXPRESS | 2805 | 20–94 | |||
| ATTICA | 3042 | 18–89 | |||
| HYPERTENSHELL | 11,540 | >17 | |||
| National Epidemiological Survey | 17,887 | 20–70 | |||
| A Nutrition & Health Survey | 5003 | 18–74 | |||
| ATTICA 1 | 2101 | >22 | |||
| Hellas Health I | 1005 | >18 | |||
| Panagiotakos et al. [27] | 10,141 | 18–95 | |||
| Hellas Health II | 1490 | >18 | |||
| Nationwide survey | 3007 | >18 | |||
| Hellenic Statistical Authority health survey for 2009 | 6325 | >15 | |||
| ATTICA 2 | 2583 | >17 | |||
| Hellas Health IV | 1008 | >18 | |||
| HYDRIA | 4011 | >18 | |||
| GAST Study | 4359 | >15 | |||
| HNNHS | 4574 | No age range is specified | |||
| SARONIKOS | 2636 | 20–65 | |||
| Hellenic Statistical Authority health survey for 2014 | 8223 | >15 | |||
| Hellas Health V | 1001 | >15 | |||
| Hungary | 546 | 14–83 | |||
| Ireland | 4330 | 55–67 | 44.5 | 55.5 | |
| Italy | 692 10 24,213 11 | >18 11 | 54.5 10 52 11 | 45.5 10 48 11 | |
| Lithuania | 435 | 40–60 | 49.7 | 50.3 | |
| Luxembourg | 1270 1331 12 | 18–69 | 48.7 | 51.3 | |
| Netherlands | 6542 | >18 | 44.8 | 55.2 | |
| Poland | 7376 13 | 40–65 13 | |||
| 13,724 14 | No age range is specified 14 | 36.7 14 | 63.3 14 | ||
| Portugal | 1550 | 35–65 | 37.3 | 62.7 | |
| Romania | 117 | 30–79 | 45.3 | 54.7 | |
| Spain | 27,903 15 28,887 16 24,670 17 | 35–74 15–17 | 46 15 46.5 16 | 54 15 53.5 16 | |
| Sweden | 1927 | Males born in 1953 and 1943 and females born in 1953 | 30.9 18 34.5 19 | 34.6 18 | |
| Country | N | High Blood Pressure (%) | Diabetes Mellitus (%) | Dyslipidaemia (%) | Sedentary Lifestyle (%) | Metabolic Syndrome (%) | Overweight (%) | Obesity (%) | Smoking Habit (%) | Hypercholesterolemia (%) | Hypertriglyceridemia (%) | Alcohol Use (%) | Fruit and Vegetables Intake (%) 12 | Population Group | |
|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|
| EUROASPIRE | 8261 | 42 | 29 | 42 | 38/59 1 | 19 | --- | --- | --- | --- | Total | ||||
| 42 | 28.3 | 39.3 | 34.8/51.9 1 | 20.9 | --- | --- | --- | --- | Males | ||||||
| 42.4 | 33.4 | 48.6 | 45.9/77.8 1 | 12.9 | --- | --- | --- | --- | Females | ||||||
| Belgium | 1017 | 31.2 | 6.52 | 65.7 | 52.2 | --- | --- | --- | 25 | --- | --- | --- | --- | Total | |
| --- | --- | --- | --- | --- | --- | --- | --- | --- | --- | --- | --- | Males | |||
| --- | --- | --- | --- | --- | --- | --- | --- | --- | --- | --- | --- | Females | |||
| Croatia (Croatian sample) | 19,070 | --- | --- | --- | --- | --- | --- | --- | --- | --- | --- | --- | --- | Total | |
| 40.7 | --- | --- | --- | --- | 42 | 19.8 | 34.1 | 72 | 49.2 | --- | --- | Males | |||
| 33.1 | --- | --- | --- | --- | 30.8 | 17.8 | 26.6 | 67.5 | 26.1 | --- | --- | Females | |||
| Croatia (Roma sample) | 430 | 26.3 | --- | --- | --- | --- | 28.1 | 21 | 70.2 | 67.7 | 43 | --- | --- | Total | |
| 26 | --- | --- | --- | --- | 33.6 | 18.1 | 71.5 | 64.4 | 45.6 | --- | --- | Males | |||
| 26.4 | --- | --- | --- | --- | 25.2 | 22.6 | 69.4 | 69.5 | 41.6 | --- | --- | Females | |||
| Cyprus | 300 | 59.7 | 18 | --- | 62.3 | --- | --- | 31.7 | 7 | 49.3 | --- | 9 | --- | Total | |
| 60 | 18 | --- | 49 | --- | --- | 24 | 14 | 36 | --- | 15 | --- | Males | |||
| 59 | 18 | --- | 73 | --- | --- | 38 | 1 | 55 | --- | 4 | --- | Females | |||
| Czech Rep. [28] | 1051 | --- | 15.6 | --- | --- | --- | 36.8 | 18.1 | --- | 50.8 | 20 | --- | --- | Total | |
| --- | 18.9 | --- | --- | --- | 48.8 | 20.3 | --- | 52.9 | 24.9 | --- | --- | Males | |||
| --- | 12.8 | --- | --- | --- | 26.7 | 16.3 | --- | 49 | 15.8 | --- | --- | Females | |||
| Czech Rep. [29] | 1812 | 50.6 | 14 | --- | --- | --- | 40.6 | 32 | 29.4 | --- | --- | --- | --- | Total | |
| 51 | 14 | --- | --- | --- | 49 | 32 | 36 | --- | --- | --- | --- | Males | |||
| 50 | 14 | ---- | --- | --- | 31 | 32 | 22 | --- | --- | --- | --- | Females | |||
| Estonia | 1111 | 31.1 | 3.3 | --- | --- | 22.9 | 55 | 46.3 1 | 27.8 | 62.3 | 23.5 | --- | --- | Total | |
| 36.8 | 4 | --- | --- | 29.1 | 66.2 | 48.5 1 | 36.1 | 63.8 | 30.9 | --- | --- | Males | |||
| 26.1 | 2.7 | --- | --- | 17.5 | 48.3 | 44.5 1 | 20.5 | 60.9 | 17 | --- | --- | Females | |||
| France MONICA 86–88 | 860 | 63.8 | --- | 66.6 | --- | --- | 55 2 | --- | 31.2 | --- | --- | --- | --- | Total | |
| 70.5 | --- | 71.1 | --- | --- | 59.6 2 | --- | 44.1 | --- | --- | --- | --- | Males | |||
| 56.6 | --- | 60.9 | --- | --- | 49.8 2 | --- | 16.7 | --- | --- | --- | --- | Females | |||
| France MONICA 95–96 | 1021 | 45.8 | 9.2 | 57.2 | --- | --- | 57.7 2 | --- | 24.2 | --- | --- | --- | --- | Total | |
| 49.5 | 9.5 | 66.2 | --- | --- | 62.5 2 | --- | 33.1 | --- | --- | --- | --- | Males | |||
| 42.4 | 8.9 | 48.5 | --- | --- | 53 2 | --- | 15.5 | --- | --- | --- | --- | Females | |||
| France MONALISA | 1021 | 44.8 | 6 | 53 | --- | --- | 57.5 2 | --- | 20.4 | --- | --- | --- | --- | Total | |
| 48 | 7.8 | 60.8 | --- | --- | 64.5 2 | --- | 22.4 | --- | --- | --- | --- | Males | |||
| 45 | 4.1 | 45 | --- | --- | 50.4 2 | --- | 18.4 | --- | --- | --- | --- | Females | |||
| France ELISABET | 1636 | 38.2 | 7.6 | 49.9 | --- | --- | 57 2 | --- | 20.8 | --- | --- | --- | --- | Total | |
| 42.5 | 10.1 | 58.3 | --- | --- | 65.1 2 | --- | 24.7 | --- | --- | --- | --- | Males | |||
| 34.3 | 5.4 | 42.2 | --- | --- | 49.8 2 | --- | 17.3 | --- | --- | --- | --- | Females | |||
| Germany 3 | 62,606 | 31.7 | 9 | 29.4 | 35.3 | --- | --- | 16 | 28.3 | --- | --- | 26.7 | 19.8 | Total | |
| 32.5 | 8.7 | 31 | 35.4 | --- | --- | 16.3 | 32.6 | --- | --- | 32.8 | 32.6 | Males | |||
| 31.1 | 9.2 | 28.2 | 35.3 | --- | --- | 15.7 | 24.9 | --- | --- | 21.7 | 24.9 | Females | |||
| Greece 4 | EPIC Study | 26,913 | 44.4 | --- | --- | --- | --- | --- | --- | --- | --- | --- | --- | --- | Total |
| NAOUSSA | 1937 | 30.5 | --- | --- | --- | --- | --- | --- | --- | --- | --- | --- | --- | Total | |
| MEDICAL EXPRESS | 2805 | 20.1 | 8.7 | --- | --- | --- | --- | 18.4 | --- | --- | --- | --- | --- | Total | |
| ATTICA | 3042 | 30 | 7 | --- | --- | --- | --- | 18 | 43 | 39 | --- | --- | --- | Total | |
| HYPERTENSHELL | 11,540 | 31.1 | --- | --- | --- | --- | --- | 25.5 | --- | --- | --- | --- | --- | Total | |
| National Epidemiological Survey | 17,887 | 8.6 | 4.2 | --- | --- | --- | --- | 22.3 | --- | 13.3 | --- | --- | --- | Total | |
| A Nutrition & Health Survey | 5003 | 15.6 | 6 | --- | --- | --- | --- | 13.3 | 41.5 | 19.2 | --- | --- | --- | Total | |
| ATTICA 1 | 2101 | 40 | 12 | --- | --- | --- | --- | 20 | 38 | 54 | --- | --- | --- | Total | |
| Hellas Health I | 4005 | --- | --- | --- | --- | --- | --- | 18 | 43.1 | --- | --- | --- | --- | Total | |
| Panagiotakos et al. [27] | 10,141 | 14.9 | 5.7 | --- | --- | --- | --- | 11.8 | 37.1 | 10.6 | --- | --- | --- | Total | |
| Hellas Health II | 1490 | --- | --- | --- | --- | --- | --- | 18.9 | 42.6 | --- | --- | --- | --- | Total | |
| Nationwide survey | 3007 | 17.7 | 6.5 | --- | --- | --- | --- | 16.4 | 36.1 | 14 | --- | --- | --- | Total | |
| Hellenic Statistical Authority health survey for 2009 | 6325 | 20.2 | 7.9 | --- | --- | --- | --- | 17.3 | 37.9 | 15 | --- | --- | --- | Total | |
| ATTICA 2 | 2583 | 52 | 20 | --- | --- | --- | --- | 30 | 33 | 62 | --- | --- | --- | Total | |
| Hellas Health IV | 1008 | --- | --- | --- | --- | --- | --- | 18.2 | 38.1 | --- | --- | --- | --- | Total | |
| HYDRIA | 4011 | 41.7 | 11.4 | --- | --- | --- | --- | 34.9 | 35.7 | 13.4 | --- | --- | --- | Total | |
| GAST Study | 4359 | --- | --- | --- | --- | --- | --- | 38.2 | --- | --- | --- | --- | Total | ||
| HNNHS | 4574 | 13.3 | 3.6 | --- | --- | --- | --- | 15.5 | 33.8 | 16.7 | --- | --- | --- | Total | |
| SARONIKOS | 2636 | 27.2 | 11.1 | --- | --- | --- | --- | 38.9 | 23.8 | --- | --- | --- | Total | ||
| Hellenic Statistical Authority health survey for 2014 | 8223 | 20.9 | 9.2 | --- | --- | --- | --- | 17 | 32.6 | 15.4 | --- | --- | --- | Total | |
| Hellas Health V | 1001 | 15 | 6 | --- | --- | --- | --- | 17 | 37 | 12 | --- | --- | --- | Total | |
| Hungary | --- | --- | --- | --- | --- | --- | --- | --- | --- | --- | --- | --- | Total | ||
| 23 | 4.6 | --- | --- | --- | 60 | --- | 39 | 26.9 | 36.5 | 12.7 | --- | Males | |||
| 32.7 | 4.4 | --- | --- | --- | 66.5 | --- | 22 | 30.5 | 12.2 | 0.84 | --- | Females | |||
| Ireland | 4330 | 83.2 | 5.7 | --- | 54.4 | --- | 73.5 2 | --- | 17.1 | 57.8 | --- | --- | --- | Total | |
| --- | --- | --- | --- | --- | --- | --- | --- | --- | --- | --- | --- | Males | |||
| --- | --- | --- | --- | --- | --- | --- | --- | --- | --- | --- | --- | Females | |||
| Italy (BORDERLINE study) | 692 | 59.4 | 18.6 | --- | --- | --- | --- | 16.9 | 24.4 | 43.8 | --- | --- | --- | Total | |
| 66.7 | 22.8 | --- | --- | --- | --- | 16.5 | 30.8 | 46 | --- | --- | --- | Males | |||
| 55.1 | 15.1 | --- | --- | --- | --- | 17.2 | 19.1 | 41.9 | --- | --- | --- | Females | |||
| Italy (National Survey) | 24,213 | 59.6 | 15.3 | 59 | --- | --- | 24.7 | 22.6/56.7 1 | 19.8 | 29.6 | 45.5 | --- | --- | Total | |
| 70 | 19 | 60.3 | --- | --- | 56.7 | 26.1/57 1 | 25.2 | 26.8 | 52 | --- | --- | Males | |||
| 48.3 | 11.2 | 55.7 | --- | --- | 31.6 | 18.9/56.4 1 | 14 | 32.7 | 48.1 | --- | --- | Females | |||
| Lithuania | 435 | 72.7 | --- | --- | 32.9 | --- | --- | --- | 21 | --- | --- | 84 | --- | Total | |
| --- | --- | --- | --- | --- | --- | --- | --- | --- | --- | --- | --- | Males | |||
| --- | --- | --- | --- | --- | --- | --- | --- | --- | --- | --- | --- | Females | |||
| Luxembourg | 1270 (1331 for diabetes) | 35.7 | 3.7 | --- | --- | --- | --- | 22 | 22 | --- | 85.7 | --- | Total | ||
| --- | --- | --- | --- | --- | --- | --- | --- | --- | --- | --- | --- | Males | |||
| --- | --- | --- | --- | --- | --- | --- | --- | --- | --- | --- | --- | Females | |||
| Netherlands | 6542 | 22 | 2.9 | --- | --- | --- | 36.3 | 12.6 | 23 | 48.4 | --- | 19 | --- | Total | |
| 29.9 | 3.6 | --- | --- | --- | 44.3 | 11.4 | 25.7 | 50.4 | --- | 28.3 | --- | Males | |||
| 15.6 | 2.3 | --- | --- | --- | 29.8 | 13.6 | 20.9 | 46.8 | --- | 11.6 | --- | Females | |||
| Poland 5 | 7376 | 37 | 8.5 | --- | --- | --- | --- | --- | 29 | 64.7 | --- | --- | --- | Total | |
| 33.8 | 10 | --- | --- | --- | --- | --- | 29.5 | 61.2 | --- | --- | --- | Norte | |||
| 42.1 | 6.2 | --- | --- | --- | --- | --- | 28.1 | 70.2 | --- | --- | --- | Sur | |||
| Poland 6 | 6696 | 49.37 | 13.13 | 85.22 | --- | --- | 38.75 | 37.53/46.40 1 | 15.77 | --- | --- | --- | --- | Total rural | |
| 7028 | 49.54 | 13.72 | 84.22 | --- | --- | 40.15 | 32.34/43.18 1 | 17.74 | --- | --- | --- | --- | Total urban | ||
| 4195 | 47.44 | 11.61 | 82.5 | --- | --- | 36.42 | 35.69/56.16 1 | 13.13 | --- | --- | --- | --- | Rural females | ||
| 4495 | 47.88 | 11.88 | 82.27 | --- | --- | 36.11 | 30.37/50.99 1 | 16.64 | --- | --- | --- | --- | Urban females | ||
| 2501 | 52.62 | 15.67 | 89.76 | --- | --- | 42.66 | 40.62/30.03 1 | 20.19 | --- | --- | --- | --- | Rural males | ||
| 2533 | 52.61 | 16.98 | 87.68 | --- | --- | 47.34 | 35.85/29.33 1 | 19.70 | --- | --- | --- | --- | Urban males | ||
| Portugal | 1550 | 39.6 | 6 | --- | --- | --- | --- | 23.4/30.6 1 | 25.5 | 72.2 | --- | --- | --- | Total | |
| --- | --- | --- | --- | --- | --- | --- | --- | --- | --- | --- | Males | ||||
| --- | --- | --- | --- | --- | --- | --- | --- | --- | --- | --- | Females | ||||
| Spain | 27,903 | 29 | 14 | 34 | --- | 31.7 7 | 42.6 8 | 28.28 | --- | --- | --- | --- | --- | Total | |
| --- | --- | --- | --- | 32 7 | 50.7 8 | 28 8 | --- | --- | --- | --- | --- | Males | |||
| --- | --- | --- | --- | 29 7 | 35.6 8 | 28.3 8 | --- | --- | --- | --- | --- | Females | |||
| Romania | 117 | 70.08 | 33.33 | --- | --- | 68.37 | --- | 76.92 | --- | --- | 61.53 | --- | --- | At the start | |
| 41.02 | 24.7 | --- | 61.52 | 59 | --- | 52.1 | 54.45 | --- | 34.18 | 37.6 | 36.76 | At 6 months | |||
| 43.58 | 25.6 | --- | --- | 63.2 | --- | 54.7 | --- | --- | 35.8 | --- | --- | At 12 months | |||
| Sweden | 46.2 | 4 | --- | 17.7 | 16.1 9 22.6 10 26 11 | 63.4 | 15.3 | 21.5 | 32.4 | 38.2 | --- | --- | Males n = 53 | ||
| 36 | 2 | --- | 13.8 | 10.5 9 12.6 10 15.8 11 | 45.9 | 15.1 | 26.1 | 22.6 | 17.3 | --- | --- | Females n = 53 | |||
| 66.7 | 6.4 | --- | 11.6 | 19.9 9 26.1 10 35 11 | 71.6 | 16.6 | 15.1 | 26 | 22.4 | --- | --- | Males n = 43 | |||
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2025 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Sacramento-Pacheco, J.; Sánchez-Gómez, M.B.; Duarte-Clíments, G.; Gómez-Salgado, J.; Novo-Muñoz, M.M. Prevalence of Cardiovascular Risk Factors Among Adults in the European Union: A Systematic Review with Meta-Analysis. J. Clin. Med. 2025, 14, 5752. https://doi.org/10.3390/jcm14165752
Sacramento-Pacheco J, Sánchez-Gómez MB, Duarte-Clíments G, Gómez-Salgado J, Novo-Muñoz MM. Prevalence of Cardiovascular Risk Factors Among Adults in the European Union: A Systematic Review with Meta-Analysis. Journal of Clinical Medicine. 2025; 14(16):5752. https://doi.org/10.3390/jcm14165752
Chicago/Turabian StyleSacramento-Pacheco, Jennifer, María Begoña Sánchez-Gómez, Gonzalo Duarte-Clíments, Juan Gómez-Salgado, and María Mercedes Novo-Muñoz. 2025. "Prevalence of Cardiovascular Risk Factors Among Adults in the European Union: A Systematic Review with Meta-Analysis" Journal of Clinical Medicine 14, no. 16: 5752. https://doi.org/10.3390/jcm14165752
APA StyleSacramento-Pacheco, J., Sánchez-Gómez, M. B., Duarte-Clíments, G., Gómez-Salgado, J., & Novo-Muñoz, M. M. (2025). Prevalence of Cardiovascular Risk Factors Among Adults in the European Union: A Systematic Review with Meta-Analysis. Journal of Clinical Medicine, 14(16), 5752. https://doi.org/10.3390/jcm14165752