Non-Surgical Approaches to the Management of Lumbar Disc Herniation Associated with Radiculopathy: A Narrative Review
Abstract
1. Introduction
2. Pathophysiology of Disc Herniation
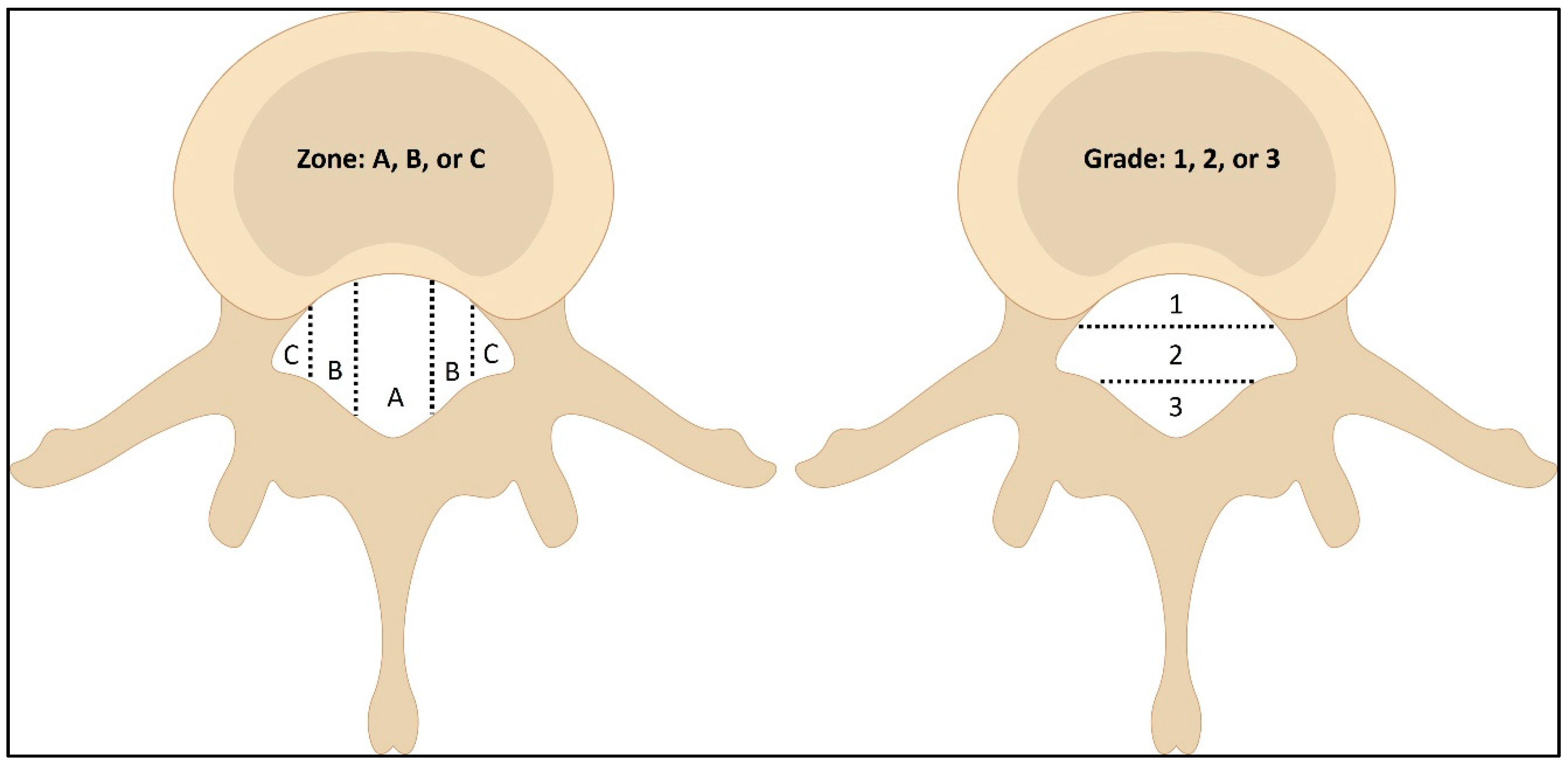
3. Classification of Lumbar Disc Herniation
4. Conservative Treatment Approaches
4.1. Patient Education and Self-Management
4.2. Electrodiagnosis-Based Management
4.3. Mechanical Diagnosis and Therapy
4.4. Mobilization and Manipulation Techniques
4.5. Exercise Therapy
4.6. Traction-Distraction and Flexion
Extension Traction or Lordosis Enhancing
4.7. Neural Mobilization
4.8. Laser and Ultrasound
4.9. Electrotherapy
4.10. Dry Needling
4.11. Epidural Injection
5. Discussion
6. Evidence-Based Practice
Gaps in Knowledge
7. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Conflicts of Interest
List of Abbreviations
| LBP | Low-back pain |
| CLBP | Chronic low-back pain |
| NP | Nucleus pulposus |
| AF | Annulus fibrosus |
| LDHR | Lumbar disc herniation associated with radiculopathy |
| LDH | Lumbar disc herniation |
| MMP | Matrix metalloproteinase expression |
| ECM | Extracellular matrix |
| DSE | Direction-sensitive exercise |
| USP | Undesired spinal posture |
| OSP | Optimum spinal posture |
| MDT | Mechanical diagnosis and therapy |
| NSD | Non-surgical spinal decompression |
| LET | Lumbar extension traction |
| US | Ultrasound |
| TENS | Transcutaneous electrical nerve stimulation |
| IF | Interferential |
| CTPI | Combination of pulsed ultrasound and interferential current |
References
- Ozturk, B.; Gunduz, O.H.; Ozoran, K.; Bostanoglu, S. Effect of continuous lumbar traction on the size of herniated disc material in lumbar disc herniation. Rheumatol. Int. 2006, 26, 622–626. [Google Scholar] [CrossRef]
- Satpute, K.; Hall, T.; Bisen, R.; Lokhande, P. The Effect of Spinal Mobilization with Leg Movement in Patients with Lumbar Radiculopathy—A Double-Blind Randomized Controlled Trial. Arch. Phys. Med. Rehabil. 2019, 100, 828–836. [Google Scholar] [CrossRef]
- Schoenfeld, A.J.; Laughlin, M.; Bader, J.O.; Bono, C.M. Characterization of the Incidence and Risk Factors for the Development of Lumbar Radiculopathy. J. Spinal Disord. Tech. 2012, 25, 163–167. [Google Scholar] [CrossRef]
- Waxenbaum, J.A.; Reddy, V.; Futterman, B. Anatomy, Back, Intervertebral Discs. In StatPearls; StatPearls Publishing: Treasure Island, FL, USA, 2023. [Google Scholar]
- Schoenfeld, A.J.; Weiner, B.K. Treatment of lumbar disc herniation: Evidence-based practice. Int. J. Gen. Med. 2010, 3, 209–214. [Google Scholar]
- Tamarkin, R.G.; Isaacson, A.C. Electrodiagnostic Evaluation of Lumbosacral Radiculopathy. In StatPearls; StatPearls Publishing: Treasure Island, FL, USA, 2023. [Google Scholar]
- Fritz, J.M.; Thackeray, A.; Childs, J.D.; Brennan, G.P. A randomized clinical trial of the effectiveness of mechanical traction for sub-groups of patients with low back pain: Study methods and rationale. BMC Musculoskelet. Disord. 2010, 11, 81. [Google Scholar] [CrossRef]
- Eichen, P.M.; Achilles, N.; Konig, V.; Mosges, R.; Hellmich, M.; Himpe, B.; Kirchner, R. Nucleoplasty, a minimally invasive procedure for disc decompression: A systematic review and meta-analysis of published clinical studies. Pain Physician 2014, 17, E149–E173. [Google Scholar]
- Hahne, A.J.; Ford, J.J.; McMeeken, J.M. Conservative management of lumbar disc herniation with associated radiculopathy: A systematic review. Spine 2010, 35, E488–E504. [Google Scholar] [CrossRef]
- Alentado, V.J.; Lubelski, D.; Steinmetz, M.P.; Benzel, E.C.; Mroz, T.E. Optimal Duration of Conservative Management Prior to Surgery for Cervical and Lumbar Radiculopathy: A Literature Review. Glob. Spine J. 2014, 4, 279–286. [Google Scholar] [CrossRef]
- Kreiner, D.S.; Hwang, S.W.; Easa, J.E.; Resnick, D.K.; Baisden, J.L.; Bess, S.; Cho, C.H.; DePalma, M.J.; Dougherty, P.; Fernand, R.; et al. An evidence-based clinical guideline for the diagnosis and treatment of lumbar disc herniation with radiculopathy. Spine J. 2014, 14, 180–191. [Google Scholar] [CrossRef]
- Berry, J.A.; Elia, C.; Saini, H.S.; Miulli, D.E. A Review of Lumbar Radiculopathy, Diagnosis, and Treatment. Cureus 2019, 11, e5934. [Google Scholar] [CrossRef]
- Singh, V.; Malik, M.; Kaur, J.; Kulandaivelan, S.; Punia, S. A systematic review and meta-analysis on the efficacy of physiotherapy intervention in management of lumbar prolapsed intervertebral disc. Int. J. Health Sci. 2021, 15, 49. [Google Scholar]
- De Cicco, F.L.; Camino Willhuber, G.O. Nucleus Pulposus Herniation. In StatPearls; StatPearls Publishing: Treasure Island, FL, USA, 2023. [Google Scholar]
- Al Qaraghli, M.I.; De Jesus, O. Lumbar Disc Herniation. In StatPearls; StatPearls Publishing: Treasure Island, FL, USA, 2023. [Google Scholar]
- Martin, M.D.; Boxell, C.M.; Malone, D.G. Pathophysiology of lumbar disc degeneration: A review of the literature. Neurosurg. Focus 2002, 13, E1. [Google Scholar] [CrossRef]
- Martins, D.E.; de Medeiros, V.P.; Wajchenberg, M.; Paredes-Gamero, E.J.; Lima, M.; Reginato, R.D.; Nader, H.B.; Puertas, E.B.; Faloppa, F. Changes in human intervertebral disc biochemical composition and bony end plates between middle and old age. PLoS ONE 2018, 13, e0203932. [Google Scholar] [CrossRef]
- Żak, M.; Pezowicz, C. Effect of overload on changes in mechanical and structural properties of the annulus fibrosus of the intervertebral disc. Biomech. Model. Mechanobiol. 2021, 20, 2259–2267. [Google Scholar] [CrossRef]
- Zhou, M.; Theologis, A.A.; O’connell, G.D. Understanding the etiopathogenesis of lumbar intervertebral disc herniation: From clinical evidence to basic scientific research. JOR Spine 2023, 7, e1289. [Google Scholar] [CrossRef]
- Chadha, M.; Srivastava, A.; Kumar, V.; Tandon, A. Disc Degeneration in Lumbar Spine of Asymptomatic Young Adults: A Descriptive Cross-Sectional Study. Indian J. Orthop. 2022, 56, 1083–1089. [Google Scholar] [CrossRef]
- Ye, F.; Lyu, F.; Wang, H.; Zheng, Z. The involvement of immune system in intervertebral disc herniation and degeneration. JOR Spine 2022, 5, e1196. [Google Scholar] [CrossRef]
- Fujii, K.; Yamazaki, M.; Kang, J.D.; Risbud, M.V.; Cho, S.K.; A Qureshi, S.; Hecht, A.C.; Iatridis, J.C. Discogenic Back Pain: Literature Review of Definition, Diagnosis, and Treatment. JBMR Plus 2019, 3, e10180. [Google Scholar] [CrossRef]
- Hornung, A.L.; Baker, J.D.; Mallow, G.M.; Sayari, A.J.; Albert, H.B.; Tkachev, A.; An, H.S.; Samartzis, D. Resorption of Lumbar Disk Herniation. JBJS Rev. 2023, 11, e22.00148. [Google Scholar] [CrossRef]
- Mysliwiec, L.W.; Cholewicki, J.; Winkelpleck, M.D.; Eis, G.P. MSU Classification for herniated lumbar discs on MRI: Toward developing objective criteria for surgical selection. Eur. Spine J. 2010, 19, 1087–1093. [Google Scholar] [CrossRef]
- Gugliotta, M.; da Costa, B.R.; Dabis, E.; Theiler, R.; Jüni, P.; Reichenbach, S.; Landolt, H.; Hasler, P. Surgical versus conservative treatment for lumbar disc herniation: A prospective cohort study. BMJ Open 2016, 6, e012938. [Google Scholar] [CrossRef]
- Akca, N.K.; Aydin, G.; Gumus, K. Effect of body mechanics brief education in the clinical setting on pain patients with lumbar disc hernia: A randomized controlled trial. Int. J. Caring Sci. 2017, 10, 1498–1506. [Google Scholar]
- Sabbahi, M.A.; Ovak-Bittar, F. Electrodiagnosis-based management of patients with radiculopathy: The concept and application involving a patient with a large lumbosacral disc herniation. Clin. Neurophysiol. Pract. 2018, 3, 141–147. [Google Scholar] [CrossRef]
- Sabbahi, M.; Ovak-Bittar, F.; Abdilahi, A. Low back pain: Manipulate and mobilize in the right direction based on EMG studies. Physiotherapy 2015, 101, e1311–e1312. [Google Scholar] [CrossRef][Green Version]
- McKenzie, R.A. The Lumbar Spine: Mechanical Diagnosis and Therapy; Orthopedic Physical Therapy Products: Minneapolis, MN, USA, 2003. [Google Scholar]
- Rabin, A.; Shmushkevich, Y.; Kalichman, L. Initial pain and disability characteristics can assist the prediction of the centralization phenomenon on initial assessment of patients with low back pain. J. Man. Manip. Ther. 2019, 27, 66–72. [Google Scholar] [CrossRef]
- Browder, D.A.; Childs, J.D.; Cleland, J.A.; Fritz, J.M. Effectiveness of an Extension-Oriented Treatment Approach in a Subgroup of Subjects with Low Back Pain: A Randomized Clinical Trial. Phys. Ther. 2007, 87, 1608–1618. [Google Scholar] [CrossRef]
- Halliday, M.H.; Pappas, E.; Hancock, M.J.; Clare, H.A.; Pinto, R.Z.; Robertson, G.; Ferreira, P.H. A Randomized Controlled Trial Comparing the McKenzie Method to Motor Control Exercises in People with Chronic Low Back Pain and a Directional Preference. J. Orthop. Sports Phys. Ther. 2016, 46, 514–522. [Google Scholar] [CrossRef]
- Petersen, T.; Larsen, K.; Nordsteen, J.; Olsen, S.; Fournier, G.; Jacobsen, S. The McKenzie method compared with manipulation when used adjunctive to information and advice in low back pain patients presenting with centralization or peripheralization: A randomized controlled trial. LWW 2011, 36, 1999–2010. [Google Scholar] [CrossRef]
- Zafereo, J.; Wang-Price, S.; Roddey, T.; Brizzolara, K. Regional manual therapy and motor control exercise for chronic low back pain: A randomized clinical trial. J. Man. Manip. Ther. 2018, 26, 193–202. [Google Scholar] [CrossRef]
- Bello, B.; Danazumi, M.S.; Kaka, B. Comparative Effectiveness of 2 Manual Therapy Techniques in the Management of Lumbar Radiculopathy: A Randomized Clinical Trial. J. Chiropr. Med. 2019, 18, 253–260. [Google Scholar] [CrossRef]
- Danazumi, M.S.; Bello, B.; Yakasai, A.M.; Kaka, B. Two manual therapy techniques for management of lumbar radiculopathy: A randomized clinical trial. J. Am. Osteopat. Assoc. 2021, 121, 391–400. [Google Scholar] [CrossRef]
- Lizis, P.; Wiater, S.; Kobza, W. Manual Therapy vs. Kinesiotherapy for People with Lumbar Discopathy: A Pilot Randomized Trial. Rehabil. Sci. 2017, 2, 6–11. [Google Scholar] [CrossRef]
- Huber, J.; Lisiński, P.; Samborski, W.; Wytrążek, M. The effect of early isometric exercises on clinical and neurophysiological parameters in patients with sciatica: An interventional randomized single-blinded study. Isokinet. Exerc. Sci. 2011, 19, 207–214. [Google Scholar] [CrossRef]
- Kennedy, D.J.; Noh, M.Y. The Role of Core Stabilization in Lumbosacral Radiculopathy. Phys. Med. Rehabil. Clin. N. Am. 2011, 22, 91–103. [Google Scholar] [CrossRef] [PubMed]
- Jeong, D.-K.; Choi, H.-H.; Kang, J.-I. Effect of lumbar stabilization exercise on disc herniation index, sacral angle, and functional improvement in patients with lumbar disc herniation. J. Phys. Ther. Sci. 2017, 29, 2121–2125. [Google Scholar] [CrossRef] [PubMed]
- Ye, C.; Ren, J.; Zhang, J.; Wang, C.; Liu, Z.; Li, F.; Sun, T. Comparison of lumbar spine stabilization exercise versus general exercise in young male patients with lumbar disc herniation after 1 year of follow-up. Int. J. Clin. Exp. Med. 2015, 8, 9869–9875. [Google Scholar] [PubMed]
- Gaowgzeh, R.A.M.; Chevidikunnan, M.F.; BinMulayh, E.A.; Khan, F. Effect of spinal decompression therapy and core stabilization exercises in management of lumbar disc prolapse: A single blind randomized controlled trial. J. Back Musculoskelet. Rehabil. 2020, 33, 225–231. [Google Scholar] [CrossRef] [PubMed]
- Kang, J.-I.; Jeong, D.-K.; Choi, H. Effect of spinal decompression on the lumbar muscle activity and disk height in patients with herniated intervertebral disk. J. Phys. Ther. Sci. 2016, 28, 3125–3130. [Google Scholar] [CrossRef] [PubMed]
- Demirel, A.; Yorubulut, M.; Ergun, N. Regression of lumbar disc herniation by physiotherapy. Does non-surgical spinal decompression therapy make a difference? Double-blind randomized controlled trial. J. Back Musculoskelet. Rehabil. 2017, 30, 1015–1022. [Google Scholar] [CrossRef] [PubMed]
- E Ljunggren, A.; Weber, H.; Larsen, S. Autotraction versus manual traction in patients with prolapsed lumbar intervertebral discs. Scand. J. Rehabil. Med. 1984, 16, 117–124. [Google Scholar] [CrossRef]
- Chou, R.; Côté, P.; Randhawa, K.; Torres, P.; Yu, H.; Nordin, M.; Hurwitz, E.L.; Haldeman, S.; Cedraschi, C. The Global Spine Care Initiative: Applying evidence-based guidelines on the non-invasive management of back and neck pain to low- and middle-income communities. Eur. Spine J. 2018, 27, 851–860. [Google Scholar] [CrossRef] [PubMed]
- WHO Guideline for Non-Surgical Management of Chronic Primary Low Back Pain in Adults in Primary and Community Care Settings. 2023. Available online: https://www.who.int/publications/i/item/9789240081789 (accessed on 28 January 2024).
- Cheng, Y.-H.; Hsu, C.-Y.; Lin, Y.-N. The effect of mechanical traction on low back pain in patients with herniated intervertebral disks: A systemic review and meta-analysis. Clin. Rehabil. 2020, 34, 13–22. [Google Scholar] [CrossRef]
- Vanti, C.; Panizzolo, A.; Turone, L.; A Guccione, A.; Violante, F.S.; Pillastrini, P.; Bertozzi, L. Effectiveness of Mechanical Traction for Lumbar Radiculopathy: A Systematic Review and Meta-Analysis. Phys. Ther. 2021, 101, pzaa231. [Google Scholar] [CrossRef] [PubMed]
- Wang, W.; Long, F.; Wu, X.; Li, S.; Lin, J. Clinical Efficacy of Mechanical Traction as Physical Therapy for Lumbar Disc Herniation: A Meta-Analysis. Comput. Math. Methods Med. 2022, 2022, 5670303. [Google Scholar] [CrossRef] [PubMed]
- Vanti, C.; Saccardo, K.; Panizzolo, A.; Turone, L.; Guccione, A.A.; Pillastrini, P. The effects of the addition of mechanical traction to physical therapy on low back pain? A systematic review with meta-analysis. Acta Orthop. Traumatol. Turc. 2023, 57, 3–16. [Google Scholar] [CrossRef] [PubMed]
- Amjad, F.; Mohseni-Bandpei, M.A.; Gilani, S.A.; Ahmad, A.; Hanif, A. Effects of non-surgical decompression therapy in addition to routine physical therapy on pain, range of motion, endurance, functional disability and quality of life versus routine physical therapy alone in patients with lumbar radiculopathy; a randomized controlled trial. BMC Musculoskelet. Disord. 2022, 23, 255. [Google Scholar] [CrossRef]
- A Harte, A.; Baxter, G.D.; Gracey, J.H. The effectiveness of motorised lumbar traction in the management of LBP with lumbo sacral nerve root involvement: A feasibility study. BMC Musculoskelet. Disord. 2007, 8, 118. [Google Scholar] [CrossRef]
- Kang, J.; Hyong, I. Changes in Electromyographic Activity of Lumbar Paraspinal Muscles According to Type of Inverted-Spinal-Traction. Wirel. Pers. Commun. 2017, 93, 35–45. [Google Scholar] [CrossRef]
- Filiz, M.B.; Kiliç, Z.; Uçkun, A.; Çakir, T.; Doğan, Ş.K.; Toraman, N.F. Mechanical traction for lumbar radicular pain: Supine or prone? A randomized controlled trial. Am. J. Phys. Med. Rehabil. 2018, 97, 433–439. [Google Scholar] [CrossRef]
- Khan, R.R.; Riaz, S.; Rashid, S.; Sulman, M. Effectiveness of mechanical traction in supine versus prone lying position for lumbosacral radiculopathy. Pak. J. Med. Sci. 2021, 37, 1451–1455. [Google Scholar] [CrossRef]
- Tadano, S.; Tanabe, H.; Arai, S.; Fujino, K.; Doi, T.; Akai, M. Lumbar mechanical traction: A biomechanical assessment of change at the lumbar spine. BMC Musculoskelet. Disord. 2019, 20, 155. [Google Scholar] [CrossRef]
- Chun, S.-W.; Lim, C.-Y.; Kim, K.; Hwang, J.; Chung, S.G. The relationships between low back pain and lumbar lordosis: A systematic review and meta-analysis. Spine J. 2017, 17, 1180–1191. [Google Scholar] [CrossRef]
- Cardoso, L.; Khadka, N.; Dmochowski, J.P.; Meneses, E.; Lee, K.; Kim, S.; Jin, Y.; Bikson, M. Computational modeling of posteroanterior lumbar traction by an automated massage bed: Predicting intervertebral disc stresses and deformation. Front. Rehabil. Sci. 2022, 3, 931274. [Google Scholar] [CrossRef]
- Lee, C.-H.; Heo, S.J.; Park, S.H. The Real Time Geometric Effect of a Lordotic Curve-Controlled Spinal Traction Device: A Randomized Cross Over Study. Healthcare 2021, 9, 125. [Google Scholar] [CrossRef]
- Oakley, P.A.; Ehsani, N.N.; Moustafa, I.M.; Harrison, D.E. Restoring lumbar lordosis: A systematic review of controlled trials utilizing Chiropractic Bio Physics® (CBP®) non-surgical approach to increasing lumbar lordosis in the treatment of low back disorders. J. Phys. Ther. Sci. 2020, 32, 601–610. [Google Scholar] [CrossRef] [PubMed]
- Moustafa, I.M.; A Diab, A. Extension traction treatment for patients with discogenic lumbosacral radiculopathy: A randomized controlled trial. Clin. Rehabil. 2013, 27, 51–62. [Google Scholar] [CrossRef] [PubMed]
- Lee, C.-H.; Heo, S.J.; Park, S.H.; Jeong, H.S.; Kim, S.-Y. Functional Changes in Patients and Morphological Changes in the Lumbar Intervertebral Disc after Applying Lordotic Curve-Controlled Traction: A Double-Blind Randomized Controlled Study. Medicina 2019, 56, 4. [Google Scholar] [CrossRef] [PubMed]
- Paulk, G.P.; Harrison, D.E. Management of a Chronic Lumbar Disk Herniation with Chiropractic Biophysics Methods after Failed Chiropractic Manipulative Intervention. J. Manip. Physiol. Ther. 2004, 27, 579. [Google Scholar] [CrossRef] [PubMed]
- Oakley, P.A.; Harrison, D.E. Lumbar extension traction alleviates symptoms and facilitates healing of disc herniation/sequestration in 6-weeks, following failed treatment from three previous chiropractors: A CBP® case report with an 8 year follow-up. J. Phys. Ther. Sci. 2017, 29, 2051–2057. [Google Scholar] [CrossRef] [PubMed][Green Version]
- Yoon, Y.-S.; Lee, J.-H.; Lee, M.; Kim, K.-E.; Jang, H.-Y.; Lee, K.-J.; Bajgai, J.; Kim, C.-S.; Cho, I.-Y. Mechanical Changes of the Lumbar Intervertebral Space and Lordotic Angle Caused by Posterior-to-Anterior Traction Using a Spinal Thermal Massage Device in Healthy People. Healthcare 2021, 9, 900. [Google Scholar] [CrossRef] [PubMed]
- Peacock, M.; Douglas, S.; Nair, P. Neural mobilization in low back and radicular pain: A systematic review. J. Man. Manip. Ther. 2023, 31, 4–12. [Google Scholar] [CrossRef]
- Plaza-Manzano, G.; Cancela-Cilleruelo, I.; Fernández-de-Las-Peñas, C.; Cleland, J.A.; Arias-Buría, J.L.; Thoomes-de-Graaf, M.; Ortega-Santiago, R. Effects of adding a neurodynamic mobilization to motor control training in patients with lumbar radiculopathy due to disc herniation: A randomized clinical trial. Am. J. Phys. Med. Rehabil. 2020, 99, 124–132. [Google Scholar] [CrossRef]
- Ahmed, I.; Bandpei, M.A.M.; Gilani, S.A.; Ahmad, A.; Zaidi, F. Effectiveness of Low-Level Laser Therapy in Patients with Discogenic Lumbar Radiculopathy: A Double-Blind Randomized Controlled Trial. J. Healthc. Eng. 2022, 2022, 6437523. [Google Scholar] [CrossRef] [PubMed]
- Boyraz, I.; Yildiz, A.; Koc, B.; Sarman, H. Comparison of High-Intensity Laser Therapy and Ultrasound Treatment in the Patients with Lumbar Discopathy. BioMed Res. Int. 2015, 2015, 304328. [Google Scholar] [CrossRef] [PubMed]
- Unlu, Z.; Tascı, S.; Tarhan, S.; Pabuscu, Y.; Islak, S. Comparison of 3 Physical Therapy Modalities For Acute Pain in Lumbar Disc Herniation Measured by Clinical Evaluation and Magnetic Resonance Imaging. J. Manip. Physiol. Ther. 2008, 31, 191–198. [Google Scholar] [CrossRef]
- Ariel, E.; Levkovitz, Y.; Goor-Aryeh, I.; Motti, R. The effects of TENS, interferential stimulation, and combined interferential stimulation and pulsed ultrasound on patients with disc herniation-induced radicular pain. J. Back Musculoskelet. Rehabil. 2022, 35, 363–371. [Google Scholar] [CrossRef]
- Karimi, A.; Mahmoudzadeh, A.; Rezaeian, Z.S.; Dommerholt, J. The effect of dry needling on the radiating pain in subjects with discogenic low-back pain: A randomized control trial. J. Res. Med. Sci. 2016, 21, 86. [Google Scholar] [CrossRef]
- Dernek, B.; Adiyeke, L.; Duymus, T.M.; Gokcedag, A.; Kesiktas, F.N.; Aksoy, C. Efficacy of Trigger Point Injections in Patients with Lumbar Disc Hernia without Indication for Surgery. Asian Spine J. 2018, 12, 232–237. [Google Scholar] [CrossRef]
- Hosseini, L.; Shariat, A.; Ghaffari, M.S.; Honarpishe, R.; Cleland, J.A. The effect of exercise therapy, dry needling, and nonfunctional electrical stimulation on radicular pain: A case report. J. Exerc. Rehabil. 2018, 14, 864–869. [Google Scholar] [CrossRef] [PubMed]
- Manchikanti, L.; Buenaventura, R.M.; Manchikanti, K.N.; Ruan, X.; Gupta, S.; Smith, H.S.; Christo, P.J.; Ward, S. Effectiveness of Therapeutic Lumbar Transforaminal Epidural Steroid Injections in Managing Lumbar Spinal Pain. Pain Physician 2012, 15, E199–E245. [Google Scholar] [CrossRef]
- George, S.Z.; Fritz, J.M.; Silfies, S.P.; Schneider, M.J.; Beneciuk, J.M.; Lentz, T.A.; Gilliam, J.R.; Hendren, S.; Norman, K.S. Interventions for the management of acute and chronic low back pain: Revision 2021: Clinical practice guidelines linked to the international classification of functioning, disability and health from the academy of orthopaedic physical therapy of the American Physical Therapy Association. J. Orthop. Sports Phys. Ther. 2021, 51, CPG1–CPG60. [Google Scholar] [PubMed]
- Kreiner, D.S.; Matz, P.; Bono, C.M.; Cho, C.H.; Easa, J.E.; Ghiselli, G.; Ghogawala, Z.; Reitman, C.A.; Resnick, D.K.; Watters, W.C.; et al. Guideline summary review: An evidence-based clinical guideline for the diagnosis and treatment of low back pain. Spine J. 2020, 20, 998–1024. [Google Scholar] [CrossRef] [PubMed]
- Vialle, L.R.; Vialle, E.N.; Henao, J.E.; Giraldo, G. Lumbar disc herniation. Rev. Bras. Ortop. (Engl. Ed.) 2010, 45, 17–22. [Google Scholar] [CrossRef]
- Kuligowski, T.; Skrzek, A.; Cieślik, B. Manual Therapy in Cervical and Lumbar Radiculopathy: A Systematic Review of the Literature. Int. J. Environ. Res. Public Health 2021, 18, 6176. [Google Scholar] [CrossRef]
| Intervention | Description | Level of Evidence |
|---|---|---|
| Patient Education and Self-Management | A comprehensive area of healthcare that focuses on providing information and support to patients, empowering them to make informed decisions about their health and well-being. The patient education domain encompasses various elements to enhance patients’ understanding of their medical conditions, treatment options, and self-care strategies. | Level B (II) |
| Electro-Diagnosis-Based Management | A method for determining the proper spine posture during manipulation that can help decompress the nerve root. | Level D |
| McKenzie Method | A method of classification based on variations in symptoms associated with low-back pain (and/or lower extremity in response to repeated direction-specific movements of the lumbar spine). The findings are employed to categorize patients into different syndromes (derangement, dysfunction, or postural), directing the choice of treatment approach. | Level B (II) |
| Mobilization and Manipulation | Mobilization is a manual therapy technique that involves passive movement applied to a joint or soft tissue to restore or enhance range of motion. Manipulation, also known as high-velocity, low-amplitude thrust (HVLA), is a manual therapy technique involving a quick, controlled force applied to a joint beyond its passive range of motion. Both are used to address musculoskeletal issues, improve joint mobility and reduce pain. | Level B (II) |
| Exercise Therapy | Exercise therapy is a crucial component of the management and rehabilitation of disc herniation. The primary goals of exercise therapy for disc herniation include improving flexibility, strength, posture, and overall function, while also addressing pain and preventing future issues. | Level B (II) |
| Traction | A treatment involving the application of manual or mechanical forces with the aim of stretching and separating the spine; or, in the case of LET, the goal is restoring the natural lumbar lordosis. | Level B (I) Short term; Level C Long term |
| Neural Mobilization | A therapeutic intervention involving systematic and controlled movements of neural tissues, including nerves, to alleviate neural tension, improve nerve glide, and optimize neurophysiological function. | Level B (II) |
| Laser and Ultrasound | Therapeutic modalities used in physiotherapy. | Level D |
| Electrotherapy | Electrotherapy modalities entail introducing physical energy into a biological system, leading to specific physiological changes utilized for therapeutic advantages. | Level D |
| Dry Needling | A technique that utilizes thin, solid needles to penetrate the skin and stimulate underlying myofascial trigger points, providing relief from muscle tension and pain, and promoting muscle function. | Level C (III) |
| Epidural Injection | Epidural injection for nerve block is a common medical procedure used to alleviate pain and inflammation associated with conditions such as disc herniation. This intervention involves the injection of medication into the epidural space, which is the space surrounding the spinal cord and nerve roots. | Level B (II) |
| I | High-quality diagnostic studies, prospective study, randomized–controlled trial, or systematic review and/or meta-analysis. |
| II | Lesser-quality diagnostic studies, prospective studies, randomized–controlled trial, or systematic review (weak diagnostic criteria, less than 80% follow up, no blinding). |
| III | Case–control studies or retrospective studies. |
| IV | Case series. |
| V | Expert opinion. |
| Grades of Recommendation | Strength of Evidence |
|---|---|
| A (Strong Evidence) | The suggestion is backed by a majority of level I and/or level II studies, with a requirement for at least one level I study. |
| B (Moderate Evidence) | The recommendation is substantiated by either a well-executed randomized–controlled trial of high quality or a majority of exclusively level II studies. This encompasses studies with brief follow-up periods (e.g., 3 months or less) and smaller sample sizes (e.g., fewer than 100 participants). |
| C (Weak Evidence) | The recommendation is backed by only one level II study. |
| D (Conflicting or No Evidence) | Level I and/or level II studies either contradict in their conclusions or offer no evidence of benefit. |
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2024 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
El Melhat, A.M.; Youssef, A.S.A.; Zebdawi, M.R.; Hafez, M.A.; Khalil, L.H.; Harrison, D.E. Non-Surgical Approaches to the Management of Lumbar Disc Herniation Associated with Radiculopathy: A Narrative Review. J. Clin. Med. 2024, 13, 974. https://doi.org/10.3390/jcm13040974
El Melhat AM, Youssef ASA, Zebdawi MR, Hafez MA, Khalil LH, Harrison DE. Non-Surgical Approaches to the Management of Lumbar Disc Herniation Associated with Radiculopathy: A Narrative Review. Journal of Clinical Medicine. 2024; 13(4):974. https://doi.org/10.3390/jcm13040974
Chicago/Turabian StyleEl Melhat, Ahmed M., Ahmed S. A. Youssef, Moustafa R. Zebdawi, Maya A. Hafez, Lamia H. Khalil, and Deed E. Harrison. 2024. "Non-Surgical Approaches to the Management of Lumbar Disc Herniation Associated with Radiculopathy: A Narrative Review" Journal of Clinical Medicine 13, no. 4: 974. https://doi.org/10.3390/jcm13040974
APA StyleEl Melhat, A. M., Youssef, A. S. A., Zebdawi, M. R., Hafez, M. A., Khalil, L. H., & Harrison, D. E. (2024). Non-Surgical Approaches to the Management of Lumbar Disc Herniation Associated with Radiculopathy: A Narrative Review. Journal of Clinical Medicine, 13(4), 974. https://doi.org/10.3390/jcm13040974







