The Burden and Psychological Distress of Family Caregivers of Individuals with Autism Spectrum Disorder: A Gender Approach
Abstract
1. Introduction
2. Materials and Methods
2.1. Participants, Design, and Procedure
2.2. Measures
2.2.1. Sociodemographic Variable and Objective Burden
2.2.2. Burden
2.2.3. Psychological Distress
2.3. Statistical Analysis
3. Results
3.1. Gender Differences in Sociodemographic Variables, Hours per Day Caring, Perceived Burden, and Psychological Distress
3.2. Correlation Analysis between Caregivers’ Ages, Hours per Day Caring, Perceived Burden, and Psychological Distress for Men and Women Separately
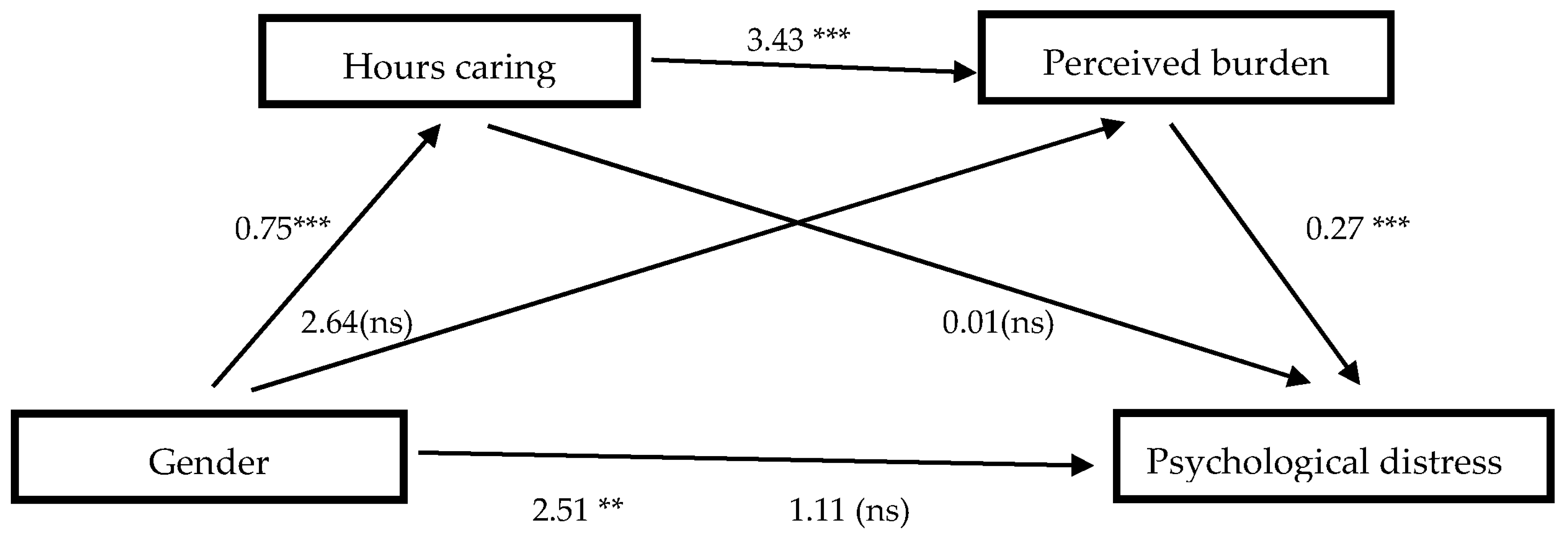
3.3. Multiple Serial Mediation
4. Discussion
5. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Acknowledgments
Conflicts of Interest
References
- APA, American Psychiatric Association. Diagnostic and Statistical Manual of Mental Disorders, 5th ed.; American Psychiatric Association: Arlington, VA, USA, 2013. [Google Scholar]
- Okoye, C.; Obialo-Ibeawuchi, C.M.; Obajeun, O.A.; Sarwar, S.; Tawfik, C.; Waleed, M.S.; Wasim, A.U.; Mohamoud, I.; Afolayan, A.Y.; Mbaezue, R.N. Early diagnosis of autism spectrum disorder: A review and analysis of the risks and benefits. Cureus 2023, 15, e43226. [Google Scholar] [CrossRef] [PubMed]
- Elsabbagh, M.; Divan, G.; Koh, Y.J.; Kim, Y.S.; Kauchali, S.; Marcín, C.; Montiel-Nava, C.; Patel, V.; Paula, C.S.; Wang, C.; et al. Global prevalence of autism and other pervasive developmental disorders. Autism Res. 2012, 5, 160–179. [Google Scholar] [CrossRef]
- Tsai, L.Y. Impact of DSM-5 on epidemiology of autism spectrum disorder. Res. Autism Spectr. Disord. 2014, 8, 1454–1470. [Google Scholar] [CrossRef]
- Chiarotti, F.; Venerosi, A. Epidemiology of autism spectrum disorders: A review of worldwide prevalence estimates since 2014. Brain Sci. 2020, 10, 274. [Google Scholar] [CrossRef]
- Zeidan, J.; Fombonne, E.; Scorah, J.; Ibrahim, A.; Durkin, M.S.; Saxena, S.; Yusuf, A.; Shih, A.; Elsabbagh, M. Global prevalence of autism: A systematic review update. Autism Res. 2022, 15, 778–790. [Google Scholar] [CrossRef] [PubMed]
- World Health Organization. Autism. Available online: https://www.who.int/news-room/fact-sheets/detail/autism-spectrum-disorders (accessed on 22 March 2024).
- Loomes, R.; Hull, L.; Mandy, W.P. What is the male-to-female ratio in autism spectrum disorder? A systematic review and meta-analysis. J. Am. Acad. Child Adolesc. Psychiatry 2017, 56, 466–474. [Google Scholar] [CrossRef]
- Hiller, R.M.; Young, R.L.; Weber, N. Sex differences in pre-diagnosis concerns for children later diagnosed with autism spectrum disorder. Autism 2016, 20, 75–84. [Google Scholar] [CrossRef] [PubMed]
- Khachadourian, V.; Mahjani, B.; Sandin, S.; Kolevzon, A.; Buxbaum, J.D.; Reichenberg, A.; Janecka, M. Comorbidities in autism spectrum disorder and their etiologies. Transl. Psychiatry 2023, 13, 71. [Google Scholar] [CrossRef]
- Lord, C.; Elsabbagh, M.; Baird, G.; Veenstra-Vanderweele, J. Autism spectrum disorder. Lancet 2018, 392, 508–520. [Google Scholar] [CrossRef]
- Appah, J.; Senoo-Dogbey, V.E.; Armah, D.; Wuaku, D.A.; Ohene, L.A. A qualitative enquiry into the challenging roles of caregivers caring for children with Autism Spectrum Disorders in Ghana. J. Pediatr. Nurs. 2024, 76, 23–29. [Google Scholar] [CrossRef]
- Snow, M.; Donnelly, J. Factors mediating dysphoric moods and help seeking behaviour among Australian parents of children with autism. J. Autism Dev. Disord. 2016, 46, 1941–1952. [Google Scholar] [CrossRef]
- Eisenhower, A.S.; Baker, B.L.; Blacher, J. Preschool children with intellectual disability: Syndrome specificity, behaviour problems, and maternal well-being. J. Intellect. Disabil. Res. 2005, 49, 657–671. [Google Scholar] [CrossRef]
- ten Hoopen, L.W.; de Nijs, P.F.A.; Duvekot, J.; Greaves-Lord, K.; Hillegers, M.H.J.; Brouwer, W.B.F.; Hakkaart-van Roijen, L. Children with an autism spectrum disorder and their caregivers: Capturing health-related and care-related quality of life. J. Autism Dev. Disord. 2020, 50, 263–277. [Google Scholar] [CrossRef]
- Buhse, M. Assessment of caregiver burden in families of persons with multiple sclerosis. J. Neurosci. Nurs. 2008, 40, 25–31. [Google Scholar] [CrossRef]
- Stuart, M.; McGrew, J.H. Caregiver burden after receiving a diagnosis of an autism spectrum disorder. Res. Autism Spectr. Disord. 2009, 3, 86–97. [Google Scholar] [CrossRef]
- Yıldız, M.; Demir, Y.; Kırcalı, A.; İncedere, A. Caregiver burden in schizophrenia and autism spectrum disorders: A comparative study. Psychiatry Investig. 2021, 18, 1180–1187. [Google Scholar] [CrossRef]
- Zarit, S.H.; Zarit, J.M. The Memory and Behavior Problems Checklist and the Burden Interview; Technical Report; Pennsylvania State University: State College, PA, USA, 1987. [Google Scholar]
- Pandey, S.; Sharma, C. Perceived burden in caregivers of children with autism spectrum disorder. J. Nepal Health Res. Counc. 2018, 16, 184–189. [Google Scholar] [CrossRef]
- Al-Qahtani, F.S. Experienced burden by caregivers of autistic children. Med. J. Cairo Univ. 2018, 86, 1523–1528. [Google Scholar] [CrossRef][Green Version]
- Baykal, S.; Karakurt, M.N.; Çakır, M.; Karabekiroğlu, K. An examination of the relations between symptom distributions in children diagnosed with autism and caregiver burden, anxiety and depression levels. Community Ment. Health J. 2019, 55, 311–317. [Google Scholar] [CrossRef]
- Pruitt, M.M.; Rhoden, M.; Ekas, N.V. Relationship between the broad autism phenotype, social relationships and mental health for mothers of children with autism spectrum disorder. Autism 2018, 22, 171–180. [Google Scholar] [CrossRef]
- Ingersoll, B.; Hambrick, D. The relationship between the broader autism phenotype, child severity, and stress and depression in parents of children with autism spectrum disorders. Res. Autism Spectr. Disord. 2011, 5, 337–344. [Google Scholar] [CrossRef]
- Yamada, A.; Suzuki, M.; Kato, M.; Suzuki, M.; Tanaka, S.; Shindo, T.; Taketani, K.; Akechi, T.; Furukawa, T.A. Emotional distress and its correlates among parents of children with pervasive developmental disorders. Psychiatry Clin. Neuros. 2007, 61, 651–657. [Google Scholar] [CrossRef]
- Salomone, E.; Leadbitter, K.; Aldred, C.; Barrett, B.; Byford, S.; Charman, T.; Howlin, P.; Green, J.; Le Couteur, A.; McConachie, H.; et al. The association between child and family characteristics and the mental health and wellbeing of caregivers of children with autism in mid-childhood. J. Autism Dev. Disord. 2018, 48, 1189–1198. [Google Scholar] [CrossRef]
- Yorke, I.; White, P.; Weston, A.; Rafla, M.; Charman, T.; Simonoff, E. The association between emotional and behavioral problems in children with autism spectrum disorder and psychological distress in their parents: A systematic review and meta-analysis. J. Autism Dev. Disord. 2018, 48, 3393–3415. [Google Scholar] [CrossRef]
- Quintero, N.; McIntyre, L.L. Sibling adjustment and maternal well-being: An examination of families with and without a child with an autism spectrum disorder. Focus Autism Other Dev. Disabil. 2010, 25, 37–46. [Google Scholar] [CrossRef]
- Padden, C.; James, J. Stress among parents of children with and without autism spectrum disorder: A comparison involving physiological indicators and parent self-reports. J. Dev. Phys. Disabil. 2017, 9, 567–586. [Google Scholar] [CrossRef]
- Scherer, N.; Verhey, I.; Kuper, H. Depression and anxiety in parents of children with intellectual and developmental disabilities: A systematic review and meta-analysis. PLoS ONE 2019, 14, e0219888. [Google Scholar] [CrossRef]
- Ang, K.Q.P.; Loh, P.R. Mental health and coping in parents of children with autism spectrum disorder (ASD) in Singapore: An examination of gender role in caring. J. Autism Dev. Disord. 2019, 49, 2129–2145. [Google Scholar] [CrossRef]
- Johnson, N.; Frenn, M.; Feetham, S.; Simpson, P. Autism spectrum disorder: Parenting stress, family functioning and health-related quality of life. Fam. Syst. Health 2011, 29, 232–252. [Google Scholar] [CrossRef]
- Green, C.C.; Smith, J.; Bent, C.A.; Chetcuti, L.; Sulek, R.; Uljarević, M.; Hudry, K. Differential predictors of well-being versus mental health among parents of pre-schoolers with autism. Autism 2021, 25, 1125–1136. [Google Scholar] [CrossRef]
- Landon, J.; Shepherd, D.; Goedeke, S. Predictors of satisfaction with life in parents of children with autism spectrum disorder. J. Autism Dev. Disord. 2018, 48, 1640–1650. [Google Scholar] [CrossRef]
- Martin, F.; Clyne, W.; Pearce, G.; Turner, A. Self-management support intervention for parents of children with developmental disorders: The role of gratitude and hope. J. Child. Fam. Stud. 2019, 28, 980–992. [Google Scholar] [CrossRef]
- Vats, T.; Sinha, A.K.; Priti Arun, P. Gender differences in caregiving: An exploration among families of individuals with autism spectrum disorder. Front. Anthropol. 2023, 12, 19–31. [Google Scholar]
- Swinkels, J.; Tilburg, T.V.; Verbakel, E.; Broese van Groenou, M. Explaining the gender gap in the caregiving burden of partner caregivers. J. Gerontol. B Psychol. Sci. Soc. Sci. 2019, 74, 309–317. [Google Scholar] [CrossRef]
- Williams, L.A.; Giddings, L.S.; Bellamy, G.; Gott, M. A Canadian qualitative study exploring the diversity of the experience of family caregivers of older adults with multiple chronic conditions using a social location perspective. Int. J. Equity Health 2016, 15, 40. [Google Scholar] [CrossRef]
- Jones, L.; Totsika, V.; Hastings, R.P.; Petalas, M.A. Gender differences when parenting children with autism spectrum disorders: A multilevel modeling approach. J. Autism Dev. Disord. 2013, 43, 2090–2098. [Google Scholar] [CrossRef]
- van Niekerk, K.; Stancheva, V.; Smith, C. Caregiver burden among caregivers of children with autism spectrum disorder. AJP-S. Afr. J. Psychiatry 2023, 29, 2079. [Google Scholar] [CrossRef]
- Smith, L.E.; Seltzer, M.M.; Tager-Flusberg, H.; Greenberg, J.S.; Carter, A.S. A comparative analysis of well-being and coping among mothers of toddlers and mothers of adolescents with ASD. J. Autism Dev. Disord. 2008, 38, 876–889. [Google Scholar] [CrossRef]
- Mathias, K.; Kermode, M.; San Sebastian, M.; Davar, B.; Goicolea, I. An asymmetric burden: Experiences of men and women as caregivers of people with psychosocial disabilities in rural North India. Transcult. Psychiatry 2019, 56, 76–102. [Google Scholar] [CrossRef]
- Caputo, J.; Pavalko, E.K.; Hardy, M.A. The long-term effects of caregiving on women’s health and mortality. J. Marriage Fam. 2016, 78, 1382–1398. [Google Scholar] [CrossRef]
- Pinquart, M.; Sörensen, S. Gender differences in caregiver stressors, social resources, and health: An updated meta-anal-ysis. J. Gerontol. B Psychol. Sci. Soc. Sci. 2006, 61, 33–45. [Google Scholar] [CrossRef]
- McDonnell, E.; Ryan, A.A. The experience of sons caring for a parent with dementia. Dementia 2014, 13, 788–802. [Google Scholar] [CrossRef]
- Penning, M.J.; Wu, Z. Caregiver stress and mental health: Impact of caregiving relationship and gender. Gerontologist 2016, 56, 1102–1113. [Google Scholar] [CrossRef]
- Revenson, T.A.; Konstadina, G.; Aleksandra, L.; Morrison, V.; Panagopoulou, E.; Vilchinsky, N.; Hagedoorn, M. Gender and Caregiving: The Costs of Caregiving for Women. In Caregiving in the Illness Context; Revenson, T.A., Griva, K., Luszczynska, A., Morrison, V., Panagopoulou, E., Vilchinsky, N., Eds.; Palgrave Pivot: London, UK, 2016. [Google Scholar]
- Mulud, Z.A.; McCarthy, G. Caregiver burden among caregivers of individuals with severe mental illness: Testing the moderation and mediation models of resilience. Arch. Psychiatry Nurs. 2017, 31, 24–30. [Google Scholar] [CrossRef]
- Goldberg, D.P.; Gater, R.; Sartorius, N.; Ustun, T.B.; Piccinelli, M.; Gureje, O. The validity of two versions of the GHQ in the WHO study of mental illness in general health care. Psychol. Med. 1997, 27, 191–197. [Google Scholar] [CrossRef]
- Lundin, A.; Åhs, J.; Åsbring, N.; Kosidou, K.; Dal, H.; Tinghög, P.; Saboonchi, F.; Dalman, C. Discriminant validity of the 12-item version of the general health questionnaire in a Swedish case-control study. Nord. J. Psychiatry 2016, 71, 171–179. [Google Scholar] [CrossRef]
- Hayes, A.F. Introduction to Mediation, Moderation, and Conditional Process Analysis: A Regression-Based Approach, 3rd ed.; The Guilford Press: New York, NY, USA, 2018. [Google Scholar]
- INE. Instituto Nacional de Estadística Encuesta de Discapacidad, Autonomía Personal y Situaciones de Dependencia (EDAD 2020). Survey on Disability, Personal Autonomy and Dependency Situations. Spanish Government. 2022. Available online: https://www.ine.es/dyngs/INEbase/es/operacion.htm?c=Estadistica_C&cid=1254736176782&menu=resultados&idp=1254735573175#!tabs-1254736195764 (accessed on 28 February 2024).
- Lazarus, R.S.; Folkman, S. Stress, Appraisal and Coping; Springer Publishing Company: New York, NY, USA, 1984. [Google Scholar]
- Pearlin, L.I. The careers of caregivers. Gerontologist 1992, 32, 647. [Google Scholar] [CrossRef]
| Men | Women | χ2 Value | |||
|---|---|---|---|---|---|
| Variables | N | % | N | % | (p) |
| Education level | 0.25 (0.882) | ||||
| Primary | 8 | 14.8 | 25 | 12.7 | |
| Secondary | 20 | 37.1 | 70 | 35.7 | |
| University | 26 | 48.1 | 16 | 51.6 | |
| Marital status | 0.11 (0.746) | ||||
| Single/separated/widow | 6 | 11.1 | 25 | 12.8 | |
| Married/with partner | 48 | 85.9 | 171 | 87.2 | |
| Hours/day caring | 26.66 (<0.001) | ||||
| <5 h | 6 | 11.1 | 10 | 5.1 | |
| 5–10 h | 28 | 51.9 | 43 | 21.9 | |
| 11–15 h | 11 | 20.4 | 46 | 23.5 | |
| >15 h | 9 | 16.7 | 97 | 49.5 | |
| Relation with the ASD relative | 2.21 (0.531) | ||||
| Parents | 53 | 98.1 | 187 | 95.4 | |
| Other | 1 | 1.9 | 9 | 4.5 | |
| Care recipient’s age | 2.25 (0.522) | ||||
| <3 years | 0 | 0.0 | 4 | 2.0 | |
| 3–12 years | 42 | 77.8 | 157 | 80.1 | |
| 13–17 years | 6 | 11.1 | 22 | 11.2 | |
| 18–31 years | 6 | 11.1 | 13 | 6.6 | |
| N | M | SD | t | d | ||
|---|---|---|---|---|---|---|
| Perceived Burden | Men | 54 | 50.48 | 15.72 | ||
| Women | 196 | 55.68 | 13.64 | −2.40 * | −0.35 | |
| Psychological Distress | Men | 54 | 12.37 | 6.40 | ||
| Women | 196 | 14.88 | 5.95 | −2.70 ** | −0.40 |
| 1 | 2 | 3 | 4 | |
|---|---|---|---|---|
| 1. Caregivers’ ages | --- | −0.09 | 0.05 | 0.02 |
| 2. Hours/day caring + | 0.02 | --- | 0.15 * | 0.03 |
| 3. Perceived burden | 0.15 | 0.42 ** | --- | 0.59 *** |
| 4. Psychological distress | 0.16 | 0.51 *** | 0.71 *** | --- |
| Bootstrapping 95% Confidence Interval | ||||
|---|---|---|---|---|
| Effects | Point Estimate | SE | Lower | Upper |
| 1. Gender–hours/day caring–psychological distress | 0.01 | 0.26 | −0.52 | 0.49 |
| 2. Gender–hours/day caring–perceived burden–psychological distress | 0.70 | 0.61 | −0.45 | 1.94 |
| 3. Gender–perceived burden–psychological distress | 0.68 | 0.20 | 0.31 | 1.10 |
| Contrasts | ||||
| Model 1 versus Model 2 | −0.70 | 0.72 | −2.17 | 0.67 |
| Model 1 versus Model 3 | −0.68 | 0.32 | −1.35 | −0.11 |
| Model 2 versus Model 3 | 0.02 | 0.66 | −1.22 | 1.35 |
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2024 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Herrero, R.; Díaz, A.; Zueco, J. The Burden and Psychological Distress of Family Caregivers of Individuals with Autism Spectrum Disorder: A Gender Approach. J. Clin. Med. 2024, 13, 2861. https://doi.org/10.3390/jcm13102861
Herrero R, Díaz A, Zueco J. The Burden and Psychological Distress of Family Caregivers of Individuals with Autism Spectrum Disorder: A Gender Approach. Journal of Clinical Medicine. 2024; 13(10):2861. https://doi.org/10.3390/jcm13102861
Chicago/Turabian StyleHerrero, Raquel, Amelia Díaz, and Jesús Zueco. 2024. "The Burden and Psychological Distress of Family Caregivers of Individuals with Autism Spectrum Disorder: A Gender Approach" Journal of Clinical Medicine 13, no. 10: 2861. https://doi.org/10.3390/jcm13102861
APA StyleHerrero, R., Díaz, A., & Zueco, J. (2024). The Burden and Psychological Distress of Family Caregivers of Individuals with Autism Spectrum Disorder: A Gender Approach. Journal of Clinical Medicine, 13(10), 2861. https://doi.org/10.3390/jcm13102861






