Developing a Robotic Surgical Platform Is Beneficial to the Implementation of the ERAS Program for Colorectal Surgery: An Outcome and Learning Curve Analysis
Abstract
1. Introduction
2. Materials and Method
3. Results
3.1. Patients’ Demographics and Tumor Characteristics
3.2. Compliance of ERAS Program
3.3. Perioperative Data and Clinical Outcome Analysis
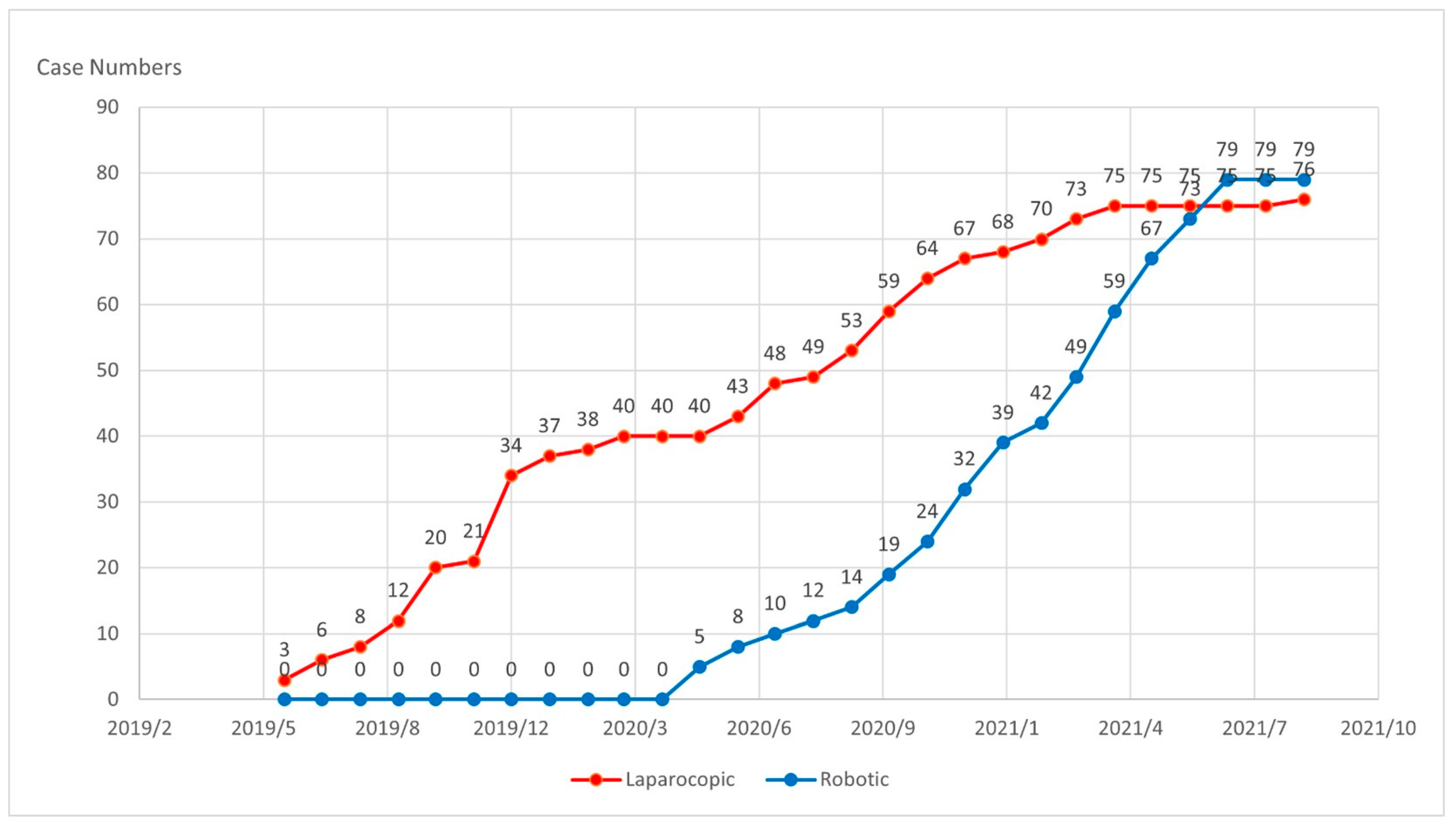
3.4. Comparison of Laparoscopic Surgery and Robotic Surgery
4. Discussion
5. Conclusions
Supplementary Materials
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Conflicts of Interest
References
- Gustafsson, U.O.; Scott, M.J.; Hubner, M.; Nygren, J.; Demartines, N.; Francis, N.; Ljungqvist, O. Guidelines for perioperative care in elective colorectal surgery: Enhanced Recovery After Surgery (ERAS®) Society recommendations: 2018. World J. Surg. 2019, 43, 659–695. [Google Scholar] [CrossRef] [PubMed]
- Melnyk, M.; Casey, R.G.; Black, P.; Koupparis, A.J. Enhanced recovery after surgery (ERAS) protocols: Time to change practice? Can. Urol. Assoc. J. 2011, 5, 342. [Google Scholar] [CrossRef] [PubMed]
- Kehlet, H. ERAS Implementation-Time to Move Forward. Ann Surg. 2018, 267, 998–999. [Google Scholar] [CrossRef] [PubMed]
- Kehlet, H. Fast-track colorectal surgery. Lancet 2008, 371, 791–793. [Google Scholar] [CrossRef] [PubMed]
- Toh, J.; Collins, G.P.; Pathma-Nathan, N.; El-Khoury, T.; Engel, A.; Smith, S.; Richardson, A.; Ctercteko, G. Attitudes towards Enhanced Recovery after Surgery (ERAS) interventions in colorectal surgery: A nationwide survey of Australia and New Zealand colorectal surgeons. Langenbeck’s Arch. Surg. 2022, 407, 1637–1646. [Google Scholar] [CrossRef] [PubMed]
- Khan, N.; Abboudi, H.; Khan, M.S.; Dasgupta, P.; Ahmed, K. Measuring the surgical ‘learning curve’: Methods, variables and competency. BJU Int. 2014, 113, 504–508. [Google Scholar] [CrossRef] [PubMed]
- Lohsiriwat, V. Learning curve of enhanced recovery after surgery program in open colorectal surgery. World J. Gastrointest. Surg. 2019, 11, 169–178. [Google Scholar] [CrossRef] [PubMed]
- Pędziwiatr, M.; Kisialeuski, M.; Wierdak, M.; Stanek, M.; Natkaniec, M.; Matłok, M.; Major, P.; Małczak, P.; Budzyński, A. Early implementation of Enhanced Recovery after Surgery (ERAS®) protocol-Compliance improves outcomes: A prospective cohort study. Int. J. Surg. 2015, 21, 75–81. [Google Scholar] [CrossRef] [PubMed]
- Jiménez-Rodríguez, R.M.; Rubio-Dorado-Manzanares, M.; Díaz-Pavón, J.M.; Reyes-Díaz, M.L.; Vazquez-Monchul, J.M.; Garcia-Cabrera, A.M.; Padillo, J.; De la Portilla, F. Learning curve in robotic rectal cancer surgery: Current state of affairs. Int. J. Color. Dis. 2016, 31, 1807–1815. [Google Scholar] [CrossRef] [PubMed]
- Pisarska, M.; Pędziwiatr, M.; Małczak, P.; Major, P.; Ochenduszko, S.; Zub-Pokrowiecka, A.; Kulawik, J.; Budzyński, A. Do we really need the full compliance with ERAS protocol in laparoscopic colorectal surgery? A prospective cohort study. Int. J. Surg. 2016, 36 Pt A, 377–382. [Google Scholar] [CrossRef]
- Ripollés-Melchor, J.; Ramírez-Rodríguez, J.M.; Casans-Francés, R.; Aldecoa, C.; Abad-Motos, A.; Logroño-Egea, M.; García-Erce, J.A.; Camps-Cervantes, Á.; Ferrando-Ortolá, C.; Suarez de la Rica, A.; et al. Association between Use of Enhanced Recovery After Surgery Protocol and Postoperative Complications in Colorectal Surgery: The Postoperative Outcomes Within Enhanced Recovery After Surgery Protocol (POWER) Study. JAMA Surg. 2019, 154, 725–736. [Google Scholar] [CrossRef] [PubMed]
- Wei, I.H.; Pappou, E.P.; Smith, J.J.; Widmar, M.; Nash, G.M.; Weiser, M.R.; Paty, P.B.; Guillem, J.G.; Afonso, A.; Garcia-Aguilar, J. Monitoring an Ongoing Enhanced Recovery After Surgery (ERAS) Program: Adherence Improves Clinical Outcomes in a Comparison of Three Thousand Colorectal Cases. Clin. Surg. 2020, 5, 2909. [Google Scholar] [PubMed]
- Milone, M.; Elmore, U.; Manigrasso, M.; Ortenzi, M.; Botteri, E.; Arezzo, A.; Silecchia, G.; Guerrieri, M.; De Palma, G.D.; Agresta, F.; et al. ERas and COLorectal endoscopic surgery: An Italian society for endoscopic surgery and new technologies (SICE) national report. Surg. Endosc. 2022, 36, 7619–7627. [Google Scholar] [CrossRef] [PubMed]
- Lee, S.H.; Kim, D.H.; Lim, S.W. Robotic versus laparoscopic intersphincteric resection for low rectal cancer: A systematic review and meta-analysis. Int. J. Color. Disease 2018, 33, 1741–1753. [Google Scholar] [CrossRef] [PubMed]
- Kim, N.K.; Kim, Y.W.; Cho, M.S. Total mesorectal excision for rectal cancer with emphasis on pelvic autonomic nerve preservation: Expert technical tips for robotic surgery. Surg. Oncol. 2015, 24, 172–180. [Google Scholar] [CrossRef] [PubMed]
- Liu, G.; Zhang, S.; Zhang, Y.; Fu, X.; Liu, X. Robotic Surgery in Rectal Cancer: Potential, Challenges, and Opportunities. Curr. Treat. Options Oncol. 2022, 23, 961–979. [Google Scholar] [CrossRef] [PubMed]
| Preadmission |
|
| |
| |
| |
| Preoperative |
|
| |
| |
| |
| Intraoperative |
|
| |
| |
| Postoperative |
|
| |
| |
| |
| |
| |
|
| Parameters | Overall | Group 1 | Group 2 | Group 3 | Group 4 | Group 5 | p Value |
|---|---|---|---|---|---|---|---|
| Number of patients, n | 155 | 31 | 31 | 31 | 31 | 31 | |
| Males, n (%) | 85 (54.8%) | 22 (71%) | 17 (54.8%) | 17 (54.8%) | 16 (51.6%) | 13 (41.9%) | 0.242 P |
| Mean age, years ± SD | 61.3 ± 14.2 | 61.4 ± 13.6 | 64.4 ± 16.0 | 63.8 ± 13.4 | 60.4 ± 12.8 | 56.4 ± 14.3 | 0.176 A |
| BMI, kg/m2 ± SD | 24.9 ± 4.2 | 25.3 ± 4.0 | 24.4 ± 5.1 | 25.3 ± 3.6 | 24.4 ± 3.2 | 24.9 ± 4.9 | 0.577 K |
| ASA ≤ 2, n (%) | 117 (75.5%) | 26 (83.9%) | 23 (74.2%) | 24 (77.4%) | 23 (74.2%) | 21 (67.7%) | 0.681 P |
| Cigarette use, n (%) | 35 (22.6%) | 12 (38.7%) | 5 (16.1%) | 6 (19.4%) | 7 (22.6%) | 5 (16.1%) | 0.180 P |
| Any comorbidity, n (%) | 94 (60.6%) | 19 (61.3%) | 19 (61.3%) | 22 (71.0%) | 18 (58.1%) | 16 (51.6%) | 0.637 P |
| Hypertension, n (%) | 70 (45.2%) | 13 (41.9%) | 15 (48.4%) | 16 (51.6%) | 14 (45.2%) | 12 (38.7%) | 0.861 P |
| Diabetes, n (%) | 39 (25.2%) | 7 (22.6%) | 5 (16.1%) | 9 (29.0%) | 9 (29.0%) | 9 (29.0%) | 0.700 P |
| Cardiovascular, n (%) | 15 (9.7%) | 1 (3.2%) | 4 (12.9%) | 6 (19.4%) | 1 (3.2%) | 3 (9.7%) | 0.156 P |
| Multiple primary cancers, n (%) | 7 (4.5%) | 3 (9.7%) | 1 (3.2%) | 1 (3.2%) | 1 (3.2%) | 1 (3.2%) | 0.664 P |
| Median preop hemoglobin, gm/dl (IQR) | 13.1 (11.8–14.5) | 13.4 (11.9–14.8) | 13.5 (11.5–14.9) | 13.1 (11.9–13.8) | 13.5 (12.0–14.5) | 13.0 (11.6–14.1) | 0.290 A |
| Previous abdominopelvic surgery, n (%) | 32 (20.6%) | 5 (16.1%) | 6 (19.4%) | 8 (25.8%) | 6 (19.4%) | 7 (22.6%) | 0.906 P |
| Neoadjuvant CCRT, n (%) | 22 (14.2%) | 6 (19.4%) | 2 (6.5%) | 2 (6.5%) | 8 (25.8%) | 4 (12.9%) | 0.125 P |
| Parameters | Overall (n = 155) | Group 1 (n = 31) | Group 2 (n = 31) | Group 3 (n = 31) | Group4 (n = 31) | Group 5 (n = 31) | p Value |
|---|---|---|---|---|---|---|---|
| Tumor location | 0.313 P | ||||||
| Right-sided colon, n (%) | 29 (18.7%) | 5 (16.1%) | 8 (25.8%) | 9 (29.0%) | 2 (6.5%) | 5 (16.1%) | |
| Left-sided colon, n (%) | 65 (41.9%) | 14 (45.2%) | 14 (45.2%) | 11 (35.5%) | 16 (51.6%) | 10 (32.3%) | |
| Rectum, n (%) | 61 (39.4%) | 12 (38.7%) | 9 (29.0%) | 11 (35.5%) | 13 (41.9%) | 16 (51.6%) | |
| Malignant tumor, n (%) | 136 (87.7%) | 28 (90.3%) | 25 (80.6%) | 27 (87.1%) | 29 (93.5%) | 27 (87.1%) | 0.620 P |
| T4 lesion | 16 (10.3%) | 1 (3.2%) | 4 (12.9%) | 4 (12.9%) | 3 (9.7%) | 4 (12.9%) | 0.668 P |
| Stage | 0.462 P | ||||||
| * Stage 0 | 10 (6.5%) | 3 (9.7%) | 1 (3.2%) | 2 (6.5%) | 2 (6.5%) | 2 (6.5%) | |
| Stage I | 26 (16.8%) | 6 (19.4%) | 1 (3.2%) | 5 (16.1%) | 5 (16.1%) | 9 (29.0%) | |
| Stage II | 33 (21.3%) | 9 (29.0%) | 7 (22.6%) | 8 (25.8%) | 3 (9.7%) | 6 (19.4%) | |
| Stage III | 49 (31.6%) | 5 (16.1%) | 13 (41.9%) | 10 (32.3%) | 12 (38.7%) | 9 (29.0%) | |
| Stage IV | 9 (5.8%) | 3 (9.7%) | 2 (6.5%) | 1 (3.2%) | 2 (6.5%) | 1 (3.2%) | |
| Median length of safe margin, cm (IQR) | 2.4 (1.5–4.0) | 2.3 (1.9–4.1) | 4.0 (1.8–4.5) | 2.2 (1.0–4.0) | 2.8 (2.0–3.5) | 2.0 (1.0–3.0) | 0.173 K |
| No residual tumor after neoadjuvant therapy | 28 (18.1%) | 5 (16.1%) | 7 (22.6%) | 5 (16.1%) | 7 (22.6%) | 4 (12.9%) | 0.814 P |
| Parameters | Overall (n = 155) | Group 1 (n = 31) | Group 2 (n = 31) | Group 3 (n = 31) | Group4 (n = 31) | Group 5 (n = 31) | p Value |
|---|---|---|---|---|---|---|---|
| Total ERAS protocol, % (Median, range) | 83.3% (50.0–94.4) | 72.2% (50.0–88.9) | 83.3% (66.7–94.4) | 83.3% (72.2–88.9) | 83.3% (72.2–94.4) | 83.3% (72.2–94.4) | <0.001 K |
| Preadmission items | 100% (50.0–100) | 75.0% (75.0–100) | 100% (50.0–100) | 100% (50.0–100) | 100% (50.0–100) | 100% (50.0–100) | 0.486 K |
| Preoperative items | 100% (75.0–100) | 100% (75.0–100) | 100% (75.0–100) | 100% (75.0–100) | 100% (75.0–100) | 100% (75.0–100) | 0.161 K |
| Intraoperative items | 100% (33.3–100) | 66.7% (33.3–100) | 66.7% (33.3–100) | 100% (66.7–100) | 100% (66.7–100) | 100% (66.7–100) | <0.001 K |
| Postoperative items | 71.4% (14.3–100) | 57.1% (14.3–85.7) | 71.4% (28.6–100) | 71.4% (28.6–100) | 71.4% (42.9–100) | 71.4% (42.9–100) | <0.001 K |
| Parameters | Overall (n = 155) | Group 1 (n = 31) | Group 2 (n = 31) | Group 3 (n = 31) | Group 4 (n = 31) | Group 5 (n = 31) | p Value |
|---|---|---|---|---|---|---|---|
| Robotic method, n (%) | 79 (51%) | 0 | 13 (42%) | 15 (48.4%) | 23 (74.2%) | 28 (90.3%) | <0.001 P |
| Operative time, minutes | 0.088 K | ||||||
| Mean (SD) | 250.3 (83.3) | 229.3 (92.6) | 242.7 (96.0) | 258.1 (75.3) | 262.7 (87.0) | 258.9 (61.5) | |
| Median (IQR) | 235 (195–297.5) | 220 (182.5–232.5) | 225 (169–285) | 250 (210–310) | 242 (195.5–315.5) | 255 (207–282.5) | |
| Minimal blood loss, n (%) | 129 (83.2%) | 22 (71%) | 25 (80.6%) | 28 (90.3%) | 25 (80.6%) | 29 (93.5%) | 0.130 P |
| Stoma construction, n (%) | 29 (18.7%) | 5 (16.1%) | 2 (6.5%) | 5 (16.1%) | 11 (35.5%) | 6 (19.4%) | 0.059 P |
| Drainage tube placement, n (%) | 73 (47.1%) | 29 (93.5%) | 28 (90.3%) | 5 (16.1%) | 5 (16.1%) | 6 (19.4%) | <0.001 P |
| Visual analog scale ≤ 3, n (%) | 127 (81.9%) | 25 (80.6%) | 24 (77.4%) | 23 (74.2%) | 29 (93.5%) | 26 (83.9%) | 0.329 P |
| First oral intake within 24 h, n (%) | 137 (88.4%) | 26 (83.9%) | 21 (67.7%) | 30 (96.8%) | 30 (96.8%) | 30 (96.8%) | 0.001 P |
| Mean time to first stool *, day ± SD | 2.5 ± 1.8 | 3.9 ± 1.8 | 2.8 ± 2.0 | 2.1 ± 1.2 | 2.0 ± 2.0 | 1.6 ± 1.0 | <0.001 K |
| Mean IV amount, ml (SD) | |||||||
| POD-0 | 1573.4 (810.3) | 1145.4 (555.6) | 1822.9 (738.4) | 1658.1 (929.6) | 1511.3 (707.1) | 1729.3 (928.7) | 0.005 K |
| POD-1 | 1478.5 (728.3) | 1533.4 (822.1) | 1811.8 (1013.4) | 1277.6 (638.6) | 1312.3 (390.6) | 1457.2 (520.3) | 0.230 K |
| POD-2 | 927.3 (904.8) | 1198.1 (905.2) | 1448.4 (1104.0) | 551.6 (680.1) | 782.1 (852.5) | 656.5 (613.0) | 0.001 K |
| POD-3 | 644.3 (945.9) | 1034.6 (935.7) | 1461.7 (1045.5) | 304.0 (640.4) | 275.8 (738.6) | 145.5 (551.0) | <0.001 K |
| Mean urine amount, ml (SD) | |||||||
| POD-1 | 1771.5 (884.6) | 1714.8 (794.9) | 2029.2 (1065.1) | 1410.8 (764.1) | 1662.7 (739.0) | 2046.6 (912.7) | 0.029 K |
| POD-2 | 2019.9 (902.0) | 2253.8 (1069.7) | 2109.6 (958.7) | 1621.0 (593.9) | 2010.7 (852.3) | 2115.4 (902.4) | 0.139 K |
| POD-3 | 2039.5 (879.6) | 2178.6 (916.9) | 2104.1 (894.5) | 1837.9 (672.4) | 1978.7 (711.4) | 2139.7 (1232.0) | 0.663 K |
| ** Optimal recovery, n (%) | 85 (54.8%) | 4 (12.9%) | 11 (35.5%) | 21 (67.7%) | 24 (77.4%) | 25 (80.6%) | <0.001 P |
| $ Any complications, n (%) | 24 (15.5%) | 9 (29.0%) | 7 (22.6%) | 4 (12.9%) | 1 (3.2%) | 3 (9.7%) | 0.078 P |
| Major (grade 3–5) | 8 (5.2%) | 5 (16.1%) | 2 (6.5%) | 1 (3.2%) | 0 | 0 | |
| Minor (grade 1–2) | 16 (10.3%) | 4 (12.9%) | 5 (16.1%) | 3 (9.7%) | 1 (3.2%) | 3 (9.7%) | |
| Postoperative LOS | |||||||
| Day, median (Q1–Q3) | 5 (4–7) | 8 (6–9) | 7 (5–10) | 5 (4–6) | 4 (4–5) | 4 (4–5) | <0.001 K |
| More than 5 days, n (%) | 67 (43.2%) | 26 (83.9%) | 20 (64.5%) | 9 (29%) | 7 (22.6%) | 5 (16.1%) | <0.001 P |
| Readmission within 30 days, n (%) | 7 (4.5%) | 3 (9.7%) | 2 (6.5%) | 1 (3.2%) | 0 | 1 (3.2%) | 0.421 P |
| Parameters | Overall (N = 155) | Laparoscopic (N = 76) | Robotic (N = 79) | p Value |
|---|---|---|---|---|
| Total ERAS protocol, % (Median, range) | 88.9 (55.6–100.0) | 83.3 (55.6–94.4) | 88.9 (72.2–100.0) | <0.001 m |
| Preadmission items | 100.0 (50.0–100.0) | 87.5 (50.00–100.0) | 100.0 (50.0–100.0) | 0.14 m |
| Preoperative items | 100.0 (75.0–100.0) | 100.0 (75.00–100.0) | 100.0 (75.0–100.0) | 0.100 m |
| Intraoperative items | 100.0 (33.3–100.0) | 66.7 (33.33–100.0) | 100.0 (33.3–100.0) | <0.001 m |
| Postoperative items | 85.7 (28.8–100.0) | 71.4 (28.8–100.0) | 85.7 (42.9–100.0) | <0.001 m |
| Postoperative LOS | ||||
| Day, median (Q1–Q3) | 5 (4–7) | 6 (5–9) | 4.1 (3.8–5.0) | 0.016 m |
| More than 5 days, n (%) | 67 (43.2%) | 48 (63.1%) | 19 (24%) | <0.001 y |
| LOS ≤ 5d | |||
|---|---|---|---|
| Factors | OR | 95% CI | p Value |
| Robotic surgery | 5.029 | 1.321 to 19.412 | 0.018 |
| Quintile group sequence | 1.270 | 0.779 to 2.070 | 0.337 |
| Compliance of total ERAS protocol | 0.995 | 0.918 to 1.079 | 0.910 |
| Male | 0.758 | 0.256 to 2.244 | 0.617 |
| Age | 0.996 | 0.958 to 1.036 | 0.849 |
| BMI | 1.087 | 0.961 to 1.229 | 0.184 |
| ASA ≤ 2 | 4.560 | 1.262 to 16.382 | 0.020 |
| Any comorbidity | 0.816 | 0.288 to 2.311 | 0.702 |
| Pre-op hemoglobin | 1.198 | 0.930 to 1.542 | 0.163 |
| Previous abdominopelvic surgery | 0.803 | 0.265 to 2.435 | 0.698 |
| Multiple primary cancers | 0.430 | 0.036 to 5.185 | 0.507 |
| Neoadjuvant CCRT | 0.336 | 0.045 to 2.485 | 0.285 |
| Cigarette use | 1.773 | 0.458 to 6.862 | 0.407 |
| Malignant disease | 0.870 | 0.218 to 3.471 | 0.843 |
| T4 lesions | 1.205 | 0.243 to 5.981 | 0.819 |
| Minimal blood loss | 0.688 | 0.171 to 2.772 | 0.599 |
| Stoma construction | 1.721 | 0.261 to 11.356 | 0.573 |
| Drainage tube placement | 0.143 | 0.042 to 0.490 | 0.002 |
| Operative time | 0.989 | 0.980 to 0.998 | 0.019 |
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2023 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Hung, C.-Y.; Lin, C.-Y.; Chen, M.-C.; Chiu, T.-Y.; Chiang, T.-W.; Chiang, F.-F. Developing a Robotic Surgical Platform Is Beneficial to the Implementation of the ERAS Program for Colorectal Surgery: An Outcome and Learning Curve Analysis. J. Clin. Med. 2023, 12, 2661. https://doi.org/10.3390/jcm12072661
Hung C-Y, Lin C-Y, Chen M-C, Chiu T-Y, Chiang T-W, Chiang F-F. Developing a Robotic Surgical Platform Is Beneficial to the Implementation of the ERAS Program for Colorectal Surgery: An Outcome and Learning Curve Analysis. Journal of Clinical Medicine. 2023; 12(7):2661. https://doi.org/10.3390/jcm12072661
Chicago/Turabian StyleHung, Chun-Yen, Chun-Yu Lin, Ming-Cheng Chen, Teng-Yi Chiu, Tzu-Wei Chiang, and Feng-Fan Chiang. 2023. "Developing a Robotic Surgical Platform Is Beneficial to the Implementation of the ERAS Program for Colorectal Surgery: An Outcome and Learning Curve Analysis" Journal of Clinical Medicine 12, no. 7: 2661. https://doi.org/10.3390/jcm12072661
APA StyleHung, C.-Y., Lin, C.-Y., Chen, M.-C., Chiu, T.-Y., Chiang, T.-W., & Chiang, F.-F. (2023). Developing a Robotic Surgical Platform Is Beneficial to the Implementation of the ERAS Program for Colorectal Surgery: An Outcome and Learning Curve Analysis. Journal of Clinical Medicine, 12(7), 2661. https://doi.org/10.3390/jcm12072661






