Exercise Stress Echocardiography in Athletes: Applications, Methodology, and Challenges
Abstract
:1. Introduction
2. Indications for ESE in Athletes
2.1. Exercise-Induced Ischemia
2.2. Athlete’s Heart Grey Zone
2.3. Hypertrophic Cardiomyopathy
2.4. Valvular Heart Disease
2.5. Lung Screening
3. Methodology of ESE
4. Emerging Techniques and Innovations in ESE
5. Limitations of ESE in Athletes
6. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Conflicts of Interest
References
- Palermi, S.; Serio, A.; Vecchiato, M.; Sirico, F.; Gambardella, F.; Ricci, F.; Iodice, F.; Radmilovic, J.; Russo, V.; D’Andrea, A. Potential Role of an Athlete-Focused Echocardiogram in Sports Eligibility. World J. Cardiol. 2021, 13, 271–297. [Google Scholar] [CrossRef]
- Palermi, S.; Cavarretta, E.; Ascenzi, F.D.; Castelletti, S.; Ricci, F.; Vecchiato, M.; Serio, A.; Cavigli, L.; Bossone, E.; Limongelli, G.; et al. Athlete’ s Heart: A Cardiovascular Step-By-Step Multimodality Approach. Rev. Cardiovasc. 2023, 24, 151. [Google Scholar] [CrossRef]
- D’Andrea, A.; Sperlongano, S.; Russo, V.; D’Ascenzi, F.; Benfari, G.; Renon, F.; Palermi, S.; Ilardi, F.; Giallauria, F.; Limongelli, G.; et al. The Role of Multimodality Imaging in Athlete’s Heart Diagnosis: Current Status and Future Directions. J. Clin. Med. 2021, 10, 5126. [Google Scholar] [CrossRef]
- Baggish, A.L.; Battle, R.W.; Beaver, T.A.; Border, W.L.; Douglas, P.S.; Kramer, C.M.; Martinez, M.W.; Mercandetti, J.H.; Phelan, D.; Singh, T.K.; et al. Recommendations on the Use of Multimodality Cardiovascular Imaging in Young Adult Competitive Athletes: A Report from the American Society of Echocardiography in Collaboration with the Society of Cardiovascular Computed Tomography and the Society for Cardiovascular Magnetic Resonance. J. Am. Soc. Echocardiogr. 2020, 33, 523–549. [Google Scholar]
- Donati, F.; Guicciardi, C.; Lodi, E.; Fernando, F.; Palermi, S.; Modena, M.G.; Biffi, A. Echocardiography in the Preparticipation Screening: An Old Topic Revisited. J. Cardiovasc. Med. 2023, 24, 297–301. [Google Scholar] [CrossRef]
- De Innocentiis, C.; Ricci, F.; Khanji, M.Y.; Aung, N.; Tana, C.; Verrengia, E.; Petersen, S.E.; Gallina, S. Athlete’s Heart: Diagnostic Challenges and Future Perspectives. Sports Med. 2018, 48, 2463–2477. [Google Scholar] [CrossRef] [PubMed]
- Cotrim, C.A.; Café, H.; João, I.; Cotrim, N.; Guardado, J.; Cordeiro, P.; Cotrim, H.; Baquero, L. Exercise Stress Echocardiography: Where Are We Now? World J. Cardiol. 2022, 14, 64–82. [Google Scholar] [CrossRef]
- Picano, E.; Pellikka, P.A. Stress Echo Applications beyond Coronary Artery Disease. Eur. Heart J. 2014, 35, 1033–1040. [Google Scholar] [CrossRef] [PubMed]
- Cotrim, C.; João, I.; Fazendas, P.; Almeida, A.R.; Lopes, L.; Stuart, B.; Cruz, I.; Caldeira, D.; Loureiro, M.J.; Morgado, G.; et al. Clinical Applications of Exercise Stress Echocardiography in the Treadmill with Upright Evaluation during and after Exercise. Cardiovasc. Ultrasound 2013, 11, 26. [Google Scholar] [CrossRef] [PubMed]
- Palermi, S.; Sirico, F.; Fernando, F.; Gregori, G.; Belviso, I.; Ricci, F.; D’Ascenzi, F.; Cavarretta, E.; De Luca, M.; Negro, F.; et al. Limited Diagnostic Value of Questionnaire-Based Pre-Participation Screening Algorithms: A “Risk-Exposed” Approach to Sports Activity. J. Basic. Clin. Physiol. Pharmacol. 2022, 33, 655–663. [Google Scholar] [CrossRef]
- Galderisi, M.; Cardim, N.; D’Andrea, A.; Bruder, O.; Cosyns, B.; Davin, L.; Donal, E.; Edvardsen, T.; Freitas, A.; Habib, G.; et al. The Multi-Modality Cardiac Imaging Approach to the Athlete’s Heart: An Expert Consensus of the European Association of Cardiovascular Imaging. Eur. Heart J. Cardiovasc. Imaging 2015, 16, 353. [Google Scholar] [CrossRef] [PubMed]
- Pelliccia, A.; Sharma, S.; Gati, S.; Bäck, M.; Börjesson, M.; Caselli, S.; Collet, J.P.; Corrado, D.; Drezner, J.A.; Halle, M.; et al. 2020 ESC Guidelines on Sports Cardiology and Exercise in Patients with Cardiovascular Disease. Eur. Heart J. 2021, 42, 17–96. [Google Scholar] [CrossRef] [PubMed]
- Pelliccia, A.; Caselli, S.; Sharma, S.; Basso, C.; Bax, J.J.; Corrado, D.; D’Andrea, A.; D’Ascenzi, F.; Di Paolo, F.M.; Edvardsen, T.; et al. European Association of Preventive Cardiology (EAPC) and European Association of Cardiovascular Imaging (EACVI) Joint Position Statement: Recommendations for the Indication and Interpretation of Cardiovascular Imaging in the Evaluation of the Athlete’s heart. Eur. Heart J. 2018, 39, 1949–1969. [Google Scholar] [CrossRef] [PubMed]
- D’Andrea, A.; Severino, S.; Caso, P.; Liccardo, B.; Forni, A.; Fusco, A.; Lo Piccolo, R.; Scherillo, M.; Mininni, N.; Calabrò, R. Prognostic Value of Supine Bicycle Exercise Stress Echocardiography in Patients with Known or Suspected Coronary Artery Disease. Eur. J. Echocardiogr. 2005, 6, 271–279. [Google Scholar] [CrossRef] [PubMed]
- Claessen, G.; La Gerche, A.; Voigt, J.-U.; Dymarkowski, S.; Schnell, F.; Petit, T.; Willems, R.; Claus, P.; Delcroix, M.; Heidbuchel, H. Accuracy of Echocardiography to Evaluate Pulmonary Vascular and RV Function During Exercise. JACC Cardiovasc. Imaging 2016, 9, 532–543. [Google Scholar] [CrossRef] [PubMed]
- Abernethy, W.B.; Choo, J.K.; Hutter, A.M.J. Echocardiographic Characteristics of Professional Football Players. J. Am. Coll. Cardiol. 2003, 41, 280–284. [Google Scholar] [CrossRef]
- Qasem, M.; Utomi, V.; George, K.; Somauroo, J.; Zaidi, A.; Forsythe, L.; Bhattacharrya, S.; Lloyd, G.; Rana, B.; Ring, L.; et al. A Meta-Analysis for the Echocardiographic Assessment of Right Ventricular Structure and Function in ARVC: A Study by the Research and Audit Committee of the British Society of Echocardiography. Echo Res. Pract. 2016, 3, 95. [Google Scholar] [CrossRef]
- Champion, S. Stress Echocardiography: A Major Tool for Determining Arrhythmogenic Right Ventricular Dysplasia/Cardiomyopathy. J. Am. Soc. Echocardiogr. 2017, 30, 1042–1043. [Google Scholar] [CrossRef]
- Adler, Y.; Fisman, E.Z.; Koren-Morag, N.; Tanne, D.; Shemesh, J.; Lasry, E.; Tenenbaum, A. Left Ventricular Diastolic Function in Trained Male Weight Lifters at Rest and during Isometric Exercise. Am. J. Cardiol. 2008, 102, 97–101. [Google Scholar] [CrossRef]
- Millar, L.M.; Fanton, Z.; Finocchiaro, G.; Sanchez-Fernandez, G.; Dhutia, H.; Malhotra, A.; Merghani, A.; Papadakis, M.; Behr, E.R.; Bunce, N.; et al. Differentiation between Athlete’s Heart and Dilated Cardiomyopathy in Athletic Individuals. Heart 2020, 106, 1059–1065. [Google Scholar] [CrossRef]
- Plehn, G.; Vormbrock, J.; Perings, S.; Plehn, A.; Meissner, A.; Butz, T.; Trappe, H.J. Comparison of Right Ventricular Functional Response to Exercise in Hypertrophic versus Idiopathic Dilated Cardiomyopathy. Am. J. Cardiol. 2010, 105, 116–121. [Google Scholar] [CrossRef]
- D’Andrea, A.; Cocchia, R.; Riegler, L.; Scarafile, R.; Salerno, G.; Gravino, R.; Golia, E.; Pezzullo, E.; Citro, R.; Limongelli, G.; et al. Left Ventricular Myocardial Velocities and Deformation Indexes in Top-Level Athletes. J. Am. Soc. Echocardiogr. 2010, 23, 1281–1288. [Google Scholar] [CrossRef]
- Studer Bruengger, A.A.; Kaufmann, B.A.; Buser, M.; Hoffmann, M.; Bader, F.; Bernheim, A.M. Diastolic Stress Echocardiography in the Young: A Study in Nonathletic and Endurance-Trained Healthy Subjects. J. Am. Soc. Echocardiogr. 2014, 27, 1053–1059. [Google Scholar] [CrossRef] [PubMed]
- Mirea, O.; Corîci, O.M.; Istrătoaie, O.; Donoiu, I.; Iancău, M.; Militaru, C. Left and Right Ventricular Morphology and Function in Athletes with Elevated Pulmonary Systolic Arterial Pressure. Echocardiography 2018, 35, 769–776. [Google Scholar] [CrossRef]
- Gargani, L.; Pugliese, N.R.; De Biase, N.; Mazzola, M.; Agoston, G.; Arcopinto, M.; Argiento, P.; Armstrong, W.F.; Bandera, F.; Cademartiri, F.; et al. Exercise Stress Echocardiography of the Right Ventricle and Pulmonary Circulation. J. Am. Coll. Cardiol. 2023, 82, 1973–1985. [Google Scholar] [CrossRef] [PubMed]
- El Assaad, I.; Gauvreau, K.; Rizwan, R.; Margossian, R.; Colan, S.; Chen, M.H. Value of Exercise Stress Echocardiography in Children with Hypertrophic Cardiomyopathy. J. Am. Soc. Echocardiogr. 2020, 33, 888–894.e2. [Google Scholar] [CrossRef] [PubMed]
- Rowin, E.J.; Maron, B.J.; Olivotto, I.; Maron, M.S. Role of Exercise Testing in Hypertrophic Cardiomyopathy. JACC Cardiovasc. Imaging 2017, 10, 1374–1386. [Google Scholar] [CrossRef]
- Lancellotti, P.; Pellikka, P.A.; Budts, W.; Chaudhry, F.A.; Donal, E.; Dulgheru, R.; Edvardsen, T.; Garbi, M.; Ha, J.-W.; Kane, G.C.; et al. The Clinical Use of Stress Echocardiography in Non-Ischaemic Heart Disease: Recommendations from the European Association of Cardiovascular Imaging and the American Society of Echocardiography. Eur. Heart J. Cardiovasc. Imaging 2016, 17, 1191–1229. [Google Scholar] [CrossRef]
- Gaitonde, M.; Jones, S.; McCracken, C.; Ferguson, M.E.; Michelfelder, E.; Sachdeva, R.; Border, W. Evaluation of Left Ventricular Outflow Gradients During Staged Exercise Stress Echocardiography Helps Differentiate Pediatric Patients with Hypertrophic Cardiomyopathy from Athletes and Normal Subjects. Pediatr. Exerc. Sci. 2021, 33, 196–202. [Google Scholar] [CrossRef]
- Mert, K.U.; Radi, F.; Sadati, A.; Mert, G.Ö.; Dural, M. Evaluation of Increase in Intraventricular Gradient and Dynamic Obstruction during Exercise Stress Test in Competitive Runners. Turk. Kardiyol. Dern. Ars. 2017, 45, 715–722. [Google Scholar] [CrossRef]
- Segreti, A.; Celeski, M.; Monticelli, L.M.; Perillo, A.; Crispino, S.P.; Di Gioia, G.; Cammalleri, V.; Fossati, C.; Mega, S.; Papalia, R.; et al. Mitral and Tricuspid Valve Disease in Athletes. J. Clin. Med. 2023, 12, 3562. [Google Scholar] [CrossRef] [PubMed]
- Pratali, L.; Cavana, M.; Sicari, R.; Picano, E. Frequent Subclinical High-Altitude Pulmonary Edema Detected by Chest Sonography as Ultrasound Lung Comets in Recreational Climbers. Crit. Care Med. 2010, 38, 1818–1823. [Google Scholar] [CrossRef] [PubMed]
- Frassi, F.; Pingitore, A.; Cialoni, D.; Picano, E. Chest Sonography Detects Lung Water Accumulation in Healthy Elite Apnea Divers. J. Am. Soc. Echocardiogr. 2008, 21, 1150–1155. [Google Scholar] [CrossRef] [PubMed]
- D’Andrea, A.; Radmilovic, J.; Russo, V.; Sperlongano, S.; Carbone, A.; Di Maio, M.; Ilardi, F.; Riegler, L.; D’Alto, M.; Giallauria, F.; et al. Biventricular Dysfunction and Lung Congestion in Athletes on Anabolic Androgenic Steroids: A Speckle Tracking and Stress Lung Echocardiography Analysis. Eur. J. Prev. Cardiol. 2022, 28, 1928–1938. [Google Scholar] [CrossRef]
- Gonzalez, J.A.; Beller, G.A. Choosing Exercise or Pharmacologic Stress Imaging, or Exercise ECG Testing Alone: How to Decide. J. Nucl. Cardiol. 2017, 24, 555–557. [Google Scholar] [CrossRef] [PubMed]
- Moir, S.; Marwick, T.H. Combination of Contrast with Stress Echocardiography: A Practical Guide to Methods and Interpretation. Cardiovasc. Ultrasound 2004, 2, 15. [Google Scholar] [CrossRef] [PubMed]
- Sicari, R.; Nihoyannopoulos, P.; Evangelista, A.; Kasprzak, J.; Lancellotti, P.; Poldermans, D.; Voigt, J.-U.; Zamorano, J.L. Stress Echocardiography Expert Consensus Statement-Executive Summary: European Association of Echocardiography (EAE) (a Registered Branch of the ESC). Eur. Heart J. 2009, 30, 278–289. [Google Scholar] [CrossRef]
- Rigo, F. Coronary Flow Reserve in Stress-Echo Lab. From Pathophysiologic Toy to Diagnostic Tool. Cardiovasc. Ultrasound 2005, 3, 8. [Google Scholar] [CrossRef]
- D’Andrea, A.; Cante, L.; Palermi, S.; Carbone, A.; Ilardi, F.; Sabatella, F.; Crescibene, F.; Di Maio, M.; Giallauria, F.; Messalli, G.; et al. COVID-19 Myocarditis: Prognostic Role of Bedside Speckle-Tracking Echocardiography and Association with Total Scar Burden. Int. J. Environ. Res. Public Health 2022, 19, 5898. [Google Scholar] [CrossRef]
- D’Andrea, A.; Carbone, A.; Radmilovic, J.; Russo, V.; Fabiani, D.; Di Maio, M.; Ilardi, F.; Giallauria, F.; Caputo, A.; Cirillo, T.; et al. Myocardial Work Efficiency in Physiologic Left Ventricular Hypertrophy of Power Athletes. J. Cardiovasc. Echogr. 2022, 32, 154–159. [Google Scholar] [CrossRef]
- Santoro, A.; Alvino, F.; Antonelli, G.; Caputo, M.; Padeletti, M.; Lisi, M.; Mondillo, S. Endurance and Strength Athlete’s Heart: Analysis of Myocardial Deformation by Speckle Tracking Echocardiography. J. Cardiovasc. Ultrasound 2014, 22, 196–204. [Google Scholar] [CrossRef]
- Gruca, M.M.; Cheema, B.; Garg, G.; Ryan, J.; Thomas, J.D.; Rigolin, V.H.; Zielinski, A.R.; Puthumana, J.J. Strain Echocardiography to Describe Left Ventricular Function Pre- and Postexercise in Elite Basketball Athletes: A Feasibility Study. Echocardiography 2021, 38, 1165–1172. [Google Scholar] [CrossRef] [PubMed]
- Boe, E.; Russell, K.; Eek, C.; Eriksen, M.; Remme, E.W.; Smiseth, O.A.; Skulstad, H. Non-Invasive Myocardial Work Index Identifies Acute Coronary Occlusion in Patients with Non-ST-Segment Elevation-Acute Coronary Syndrome. Eur. Heart J. Cardiovasc. Imaging 2015, 16, 1247–1255. [Google Scholar] [CrossRef] [PubMed]
- Marwick, T.H. Measurement of Strain and Strain Rate by Echocardiography: Ready for Prime Time? J. Am. Coll. Cardiol. 2006, 47, 1313–1327. [Google Scholar] [CrossRef]
- D’Andrea, A.; Radmilovic, J.; Carbone, A.; Mandoli, G.E.; Santoro, C.; Evola, V.; Bandera, F.; D’Ascenzi, F.; Bossone, E.; Galderisi, M.; et al. Speckle Tracking Evaluation in Endurance Athletes: The “Optimal” Myocardial Work. Int. J. Cardiovasc. Imaging 2020, 36, 1679–1688. [Google Scholar] [CrossRef] [PubMed]
- Ilardi, F.; D’Andrea, A.; D’Ascenzi, F.; Bandera, F.; Benfari, G.; Esposito, R.; Malagoli, A.; Mandoli, G.E.; Santoro, C.; Russo, V.; et al. Myocardial Work by Echocardiography: Principles and Applications in Clinical Practice. J. Clin. Med. 2021, 10, 4521. [Google Scholar] [CrossRef] [PubMed]
- von Scheidt, F.; Kiesler, V.; Kaestner, M.; Bride, P.; Krämer, J.; Apitz, C. Left Ventricular Strain and Strain Rate during Submaximal Semisupine Bicycle Exercise Stress Echocardiography in Healthy Adolescents and Young Adults: Systematic Protocol and Reference Values. J. Am. Soc. Echocardiogr. 2020, 33, 848–857.e1. [Google Scholar] [CrossRef]
- Stefani, L.; Toncelli, L.; Di Tante, V.; Vono, M.C.R.; Cappelli, B.; Pedrizzetti, G.; Galanti, G. Supernormal Functional Reserve of Apical Segments in Elite Soccer Players: An Ultrasound Speckle Tracking Handgrip Stress Study. Cardiovasc. Ultrasound 2008, 6, 14. [Google Scholar] [CrossRef]
- Refoyo, E.; Troya, J.; de la Fuente, A.; Beltrán, A.; Celada, O.L.; Díaz-González, L.; Pedrero-Tomé, R.; García-Yébenes, M.; Villalón, J.M. Myocardial Work Index in Professional Football Players: A Novel Method for Assessment of Cardiac Adaptation. J. Clin. Med. 2023, 12, 3059. [Google Scholar] [CrossRef]
- Schnell, F.; Matelot, D.; Daudin, M.; Kervio, G.; Mabo, P.; Carré, F.; Donal, E. Mechanical Dispersion by Strain Echocardiography: A Novel Tool to Diagnose Hypertrophic Cardiomyopathy in Athletes. J. Am. Soc. Echocardiogr. 2017, 30, 251–261. [Google Scholar] [CrossRef]
- Santoro, C.; Sorrentino, R.; Esposito, R.; Lembo, M.; Capone, V.; Rozza, F.; Romano, M.; Trimarco, B.; Galderisi, M. Cardiopulmonary Exercise Testing and Echocardiographic Exam: An Useful Interaction. Cardiovasc. Ultrasound 2019, 17, 29. [Google Scholar] [CrossRef] [PubMed]
- Barry, T.; Farina, J.M.; Chao, C.-J.; Ayoub, C.; Jeong, J.; Patel, B.N.; Banerjee, I.; Arsanjani, R. The Role of Artificial Intelligence in Echocardiography. J. Imaging 2023, 9, 50. [Google Scholar] [CrossRef] [PubMed]
- PubMed. Artificially Intelligent Interpretation of Stress Echocardiography: The Future Is Now. Available online: https://pubmed.ncbi.nlm.nih.gov/35512949/ (accessed on 24 September 2023).
- Upton, R.; Mumith, A.; Beqiri, A.; Parker, A.; Hawkes, W.; Gao, S.; Porumb, M.; Sarwar, R.; Marques, P.; Markham, D.; et al. Automated Echocardiographic Detection of Severe Coronary Artery Disease Using Artificial Intelligence. JACC Cardiovasc. Imaging 2022, 15, 715–727. [Google Scholar] [CrossRef] [PubMed]
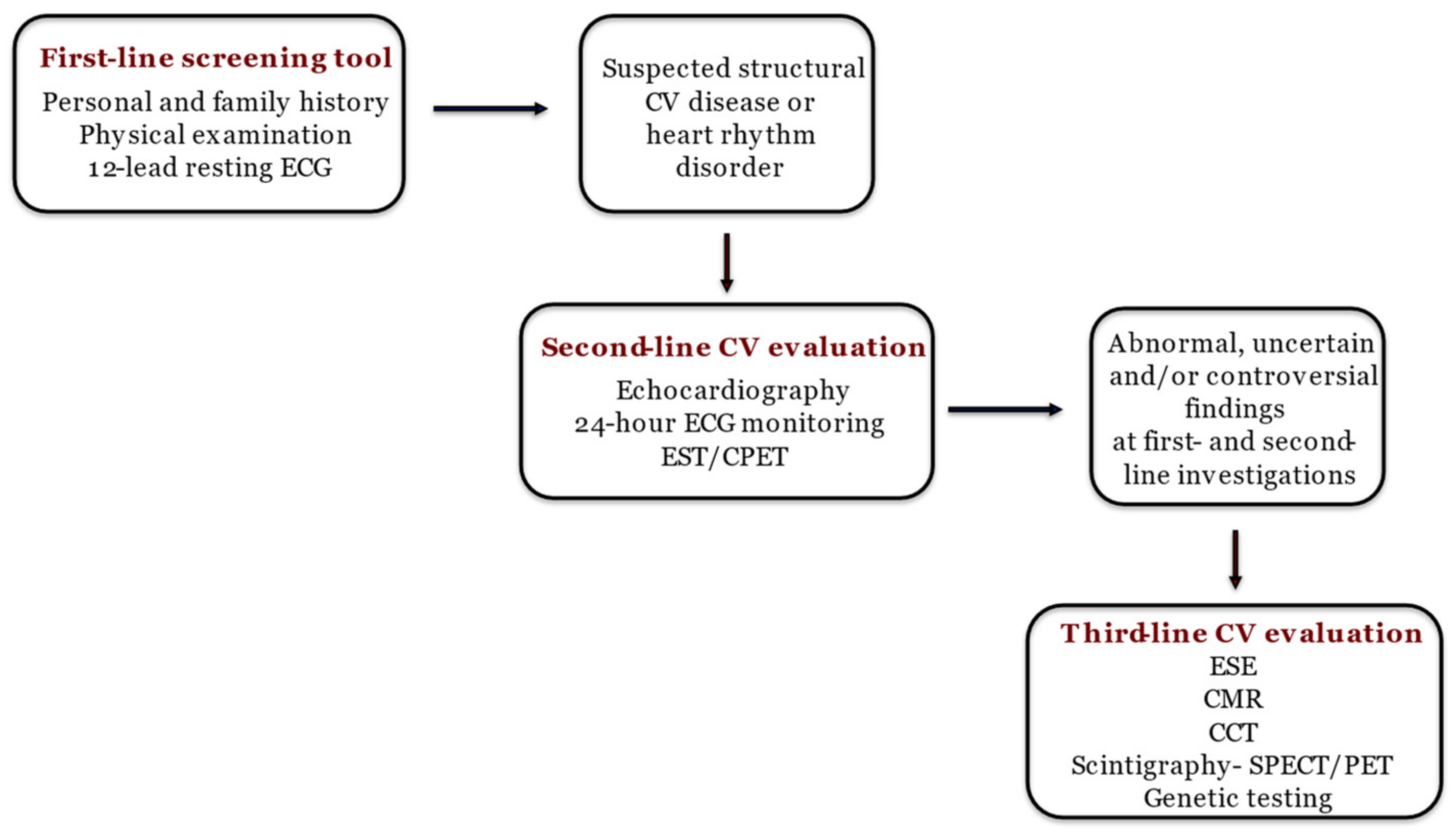


| Detection of exercise-induced ischemia |
| Differential diagnosis in grey zones: LV wall thickening, LV/RV dilatation, LV hypertrabeculation |
| Diagnosis and prognosis of HCM |
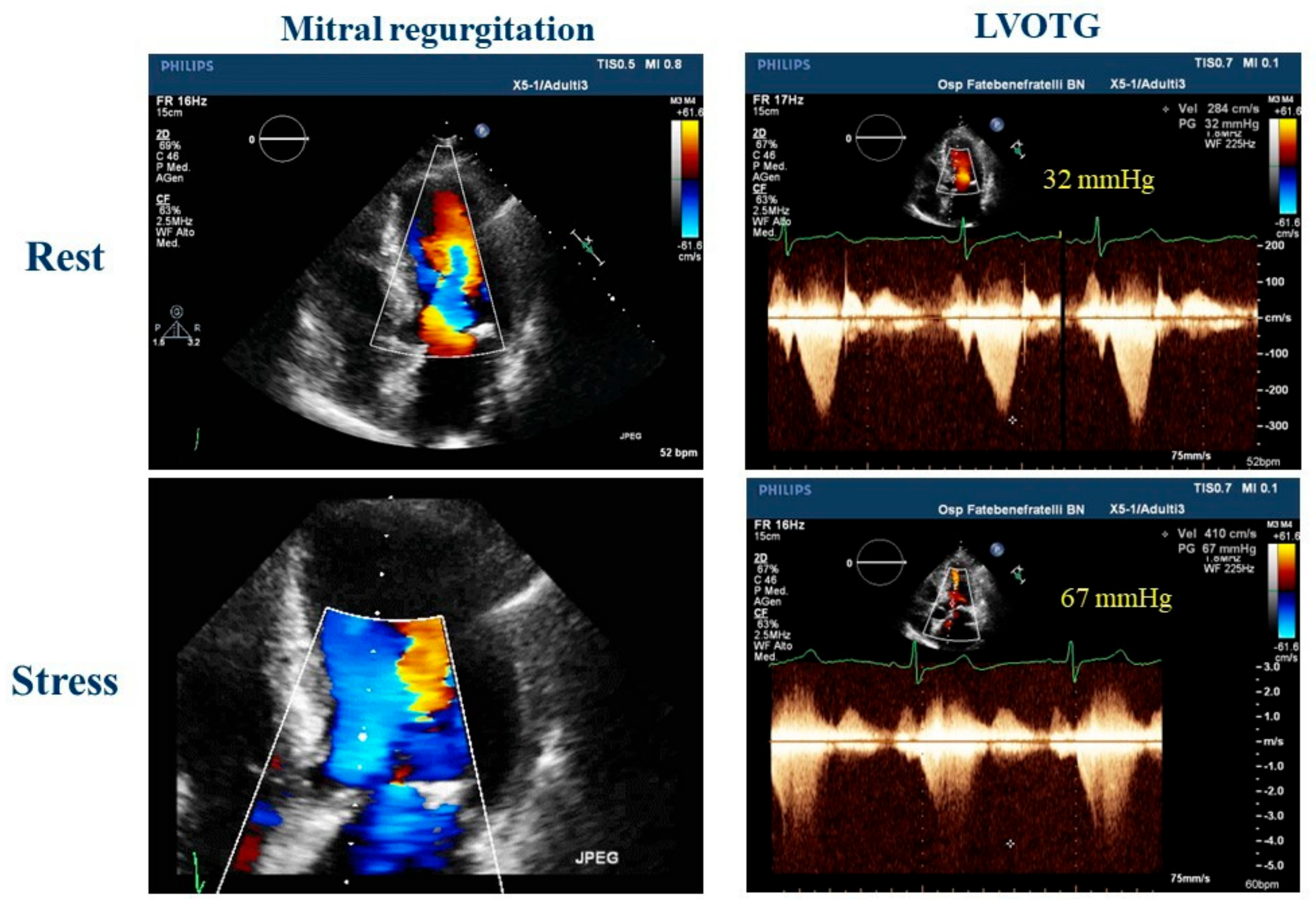
| Diagnosis and prognosis of heart valve diseases |
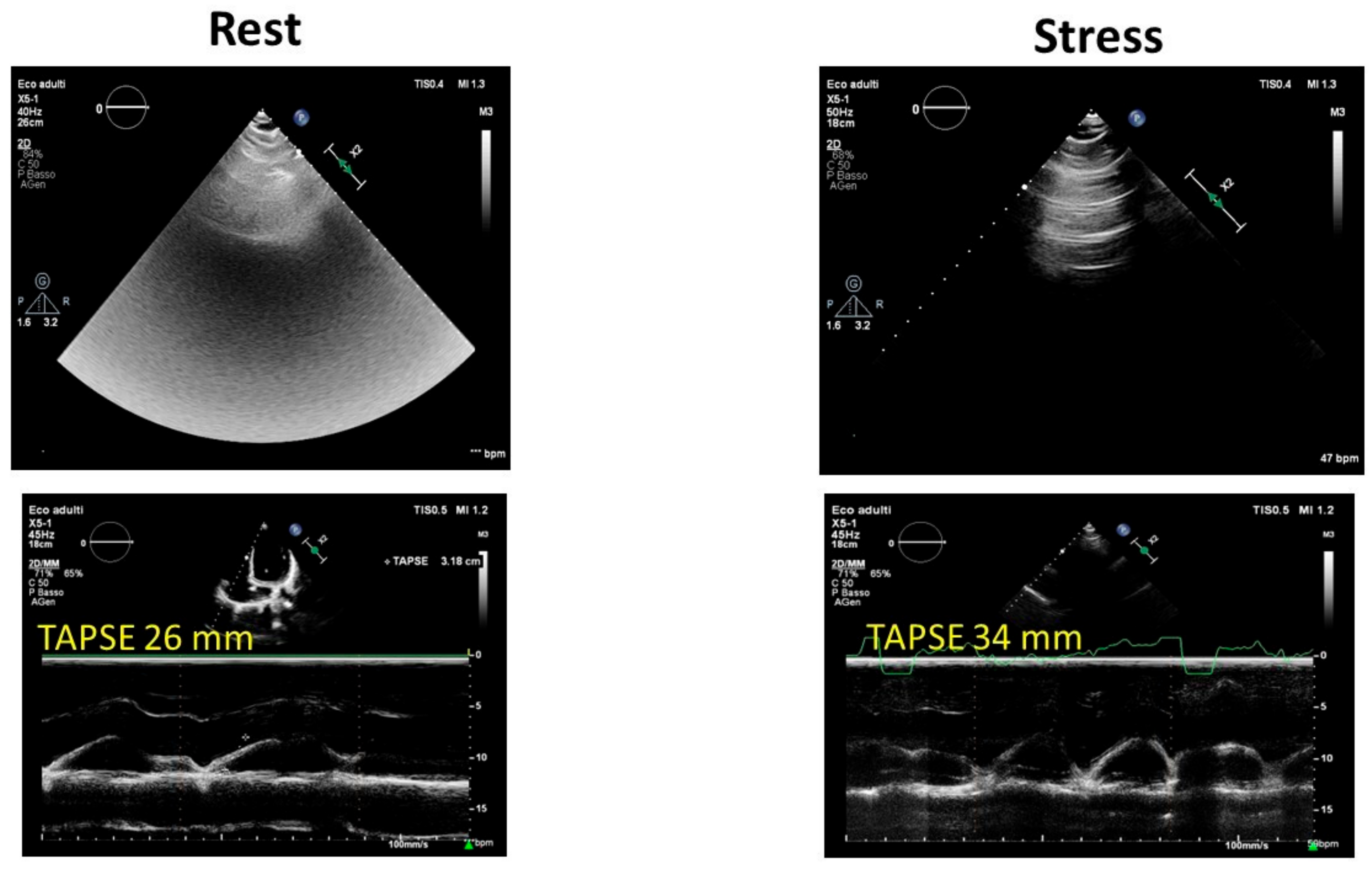
| Lung B line screening |
| Pros | Cons | |
|---|---|---|
| ESE |
|
|
| CCT |
|
|
| Nuclear imaging |
|
|
| Parameters during Effort | Findings Suggestive of Normal Heart | Finding Suggestive of CV Pathologies |
|---|---|---|
| Contractile reserve | Significant improvement | Absent or subnormal improvement |
| Dynamic obstruction | No dynamic intraventricular obstruction | LVOTO or mid-cavity obstruction |
| Diastolic function | Normal/supranormal diastolic function indexes | Diastolic dysfunction |
| Heart valve diseases | Absent | Dynamic/functional new onset/worsening valve diseases |
| Ischemia | Absent | Inducible ischemia |
| Lung echocardiography | Normal | Pulmonary congestion |
| MVP | MR | MS | TR/TS | |
|---|---|---|---|---|
| ESE parameters to be evaluated | Evaluation of sPAP increase during exercise | Evaluation of hemodynamic consequences and arrhythmias during exercise | Symptoms, sPAP, and MV dynamic gradient evaluation during exercise | Symptoms, sPAP, and TV dynamic gradient evaluation during exercise |
| Indications | Query | Parameters to Be Acquired | Levels of Image Acquisition | Possible Results | Report |
|---|---|---|---|---|---|
| HCM |
|
|
|
|
|
| DCM |
|
|
|
|
|
| Primary mitral regurgitation |
|
|
|
|
|
| Aortic regurgitation |
|
|
|
|
|
| Symptomatic athlete |
|
|
|
|
|
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2023 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Palermi, S.; Sperlongano, S.; Mandoli, G.E.; Pastore, M.C.; Lisi, M.; Benfari, G.; Ilardi, F.; Malagoli, A.; Russo, V.; Ciampi, Q.; et al. Exercise Stress Echocardiography in Athletes: Applications, Methodology, and Challenges. J. Clin. Med. 2023, 12, 7678. https://doi.org/10.3390/jcm12247678
Palermi S, Sperlongano S, Mandoli GE, Pastore MC, Lisi M, Benfari G, Ilardi F, Malagoli A, Russo V, Ciampi Q, et al. Exercise Stress Echocardiography in Athletes: Applications, Methodology, and Challenges. Journal of Clinical Medicine. 2023; 12(24):7678. https://doi.org/10.3390/jcm12247678
Chicago/Turabian StylePalermi, Stefano, Simona Sperlongano, Giulia Elena Mandoli, Maria Concetta Pastore, Matteo Lisi, Giovanni Benfari, Federica Ilardi, Alessandro Malagoli, Vincenzo Russo, Quirino Ciampi, and et al. 2023. "Exercise Stress Echocardiography in Athletes: Applications, Methodology, and Challenges" Journal of Clinical Medicine 12, no. 24: 7678. https://doi.org/10.3390/jcm12247678
APA StylePalermi, S., Sperlongano, S., Mandoli, G. E., Pastore, M. C., Lisi, M., Benfari, G., Ilardi, F., Malagoli, A., Russo, V., Ciampi, Q., Cameli, M., & D’Andrea, A., on behalf of the Echocardiography Working Group of the Italian Society of Cardiology (SIC). (2023). Exercise Stress Echocardiography in Athletes: Applications, Methodology, and Challenges. Journal of Clinical Medicine, 12(24), 7678. https://doi.org/10.3390/jcm12247678













