Prognostic Value of a New Tool (the 3D/3D+) for Predicting 30-Day Mortality in Emergency Department Patients Aged 75 Years and Older
Abstract
:1. Introduction
2. Materials and Methods
3. Results
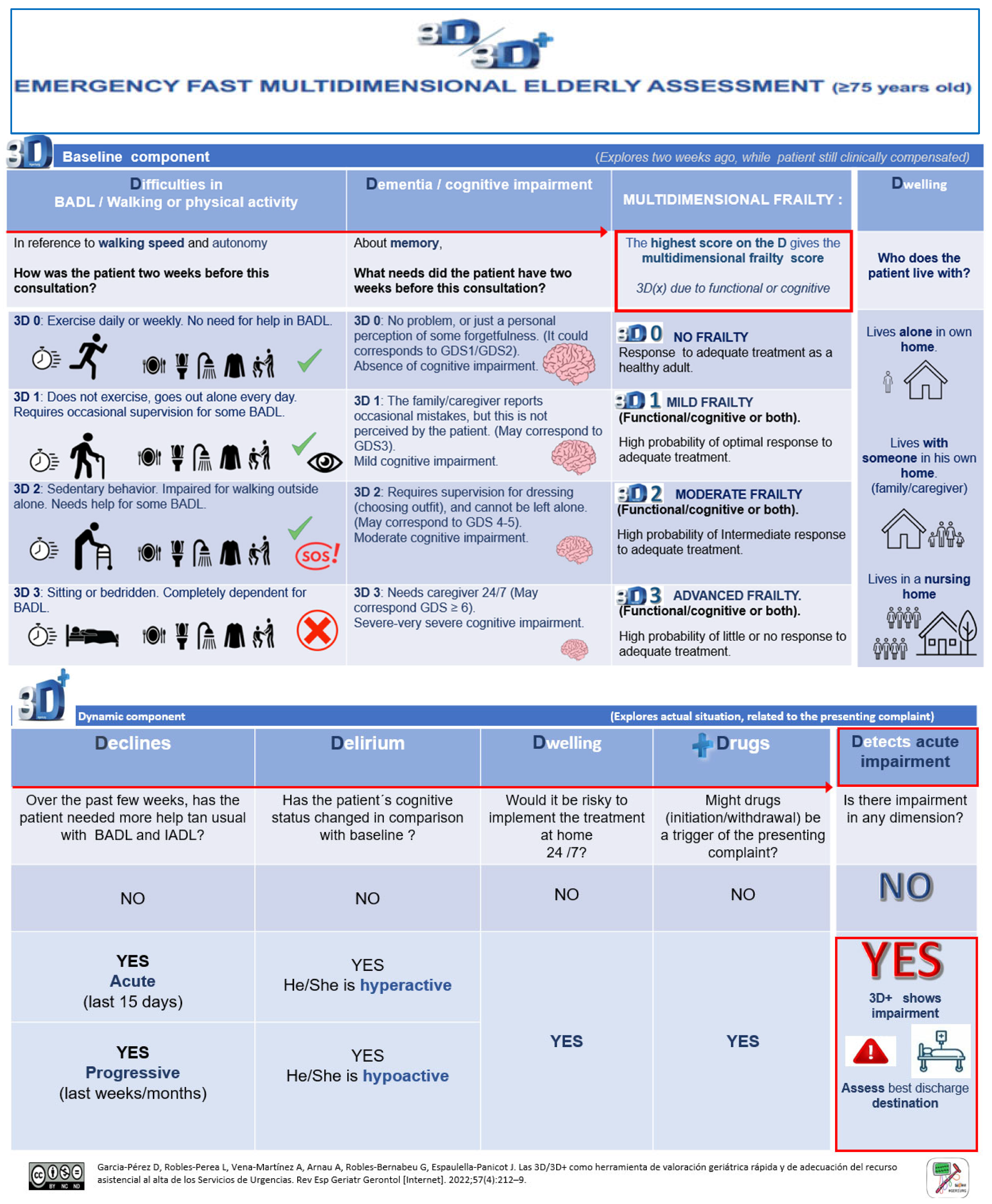
3.1. The 3D/3D+ Tool
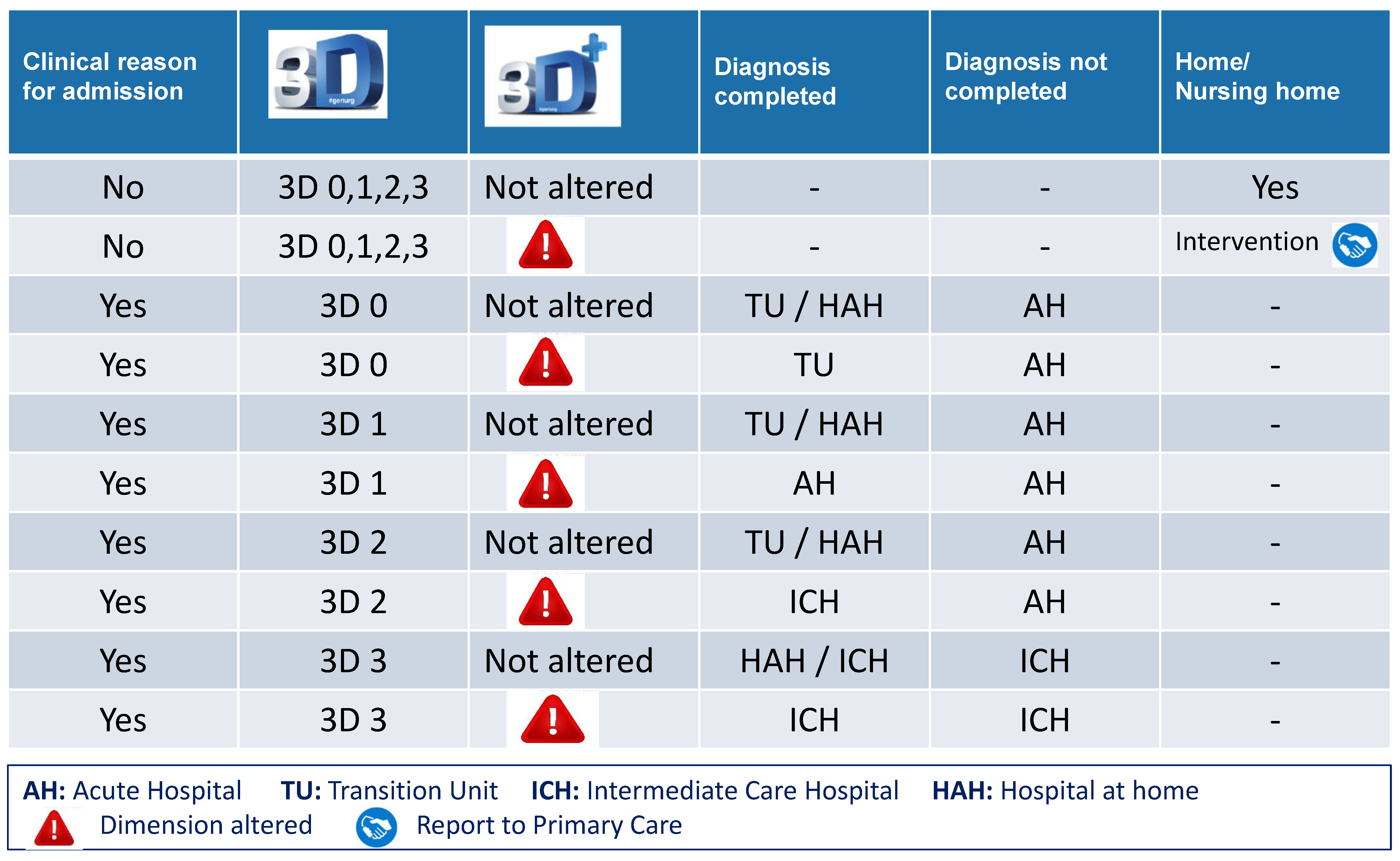
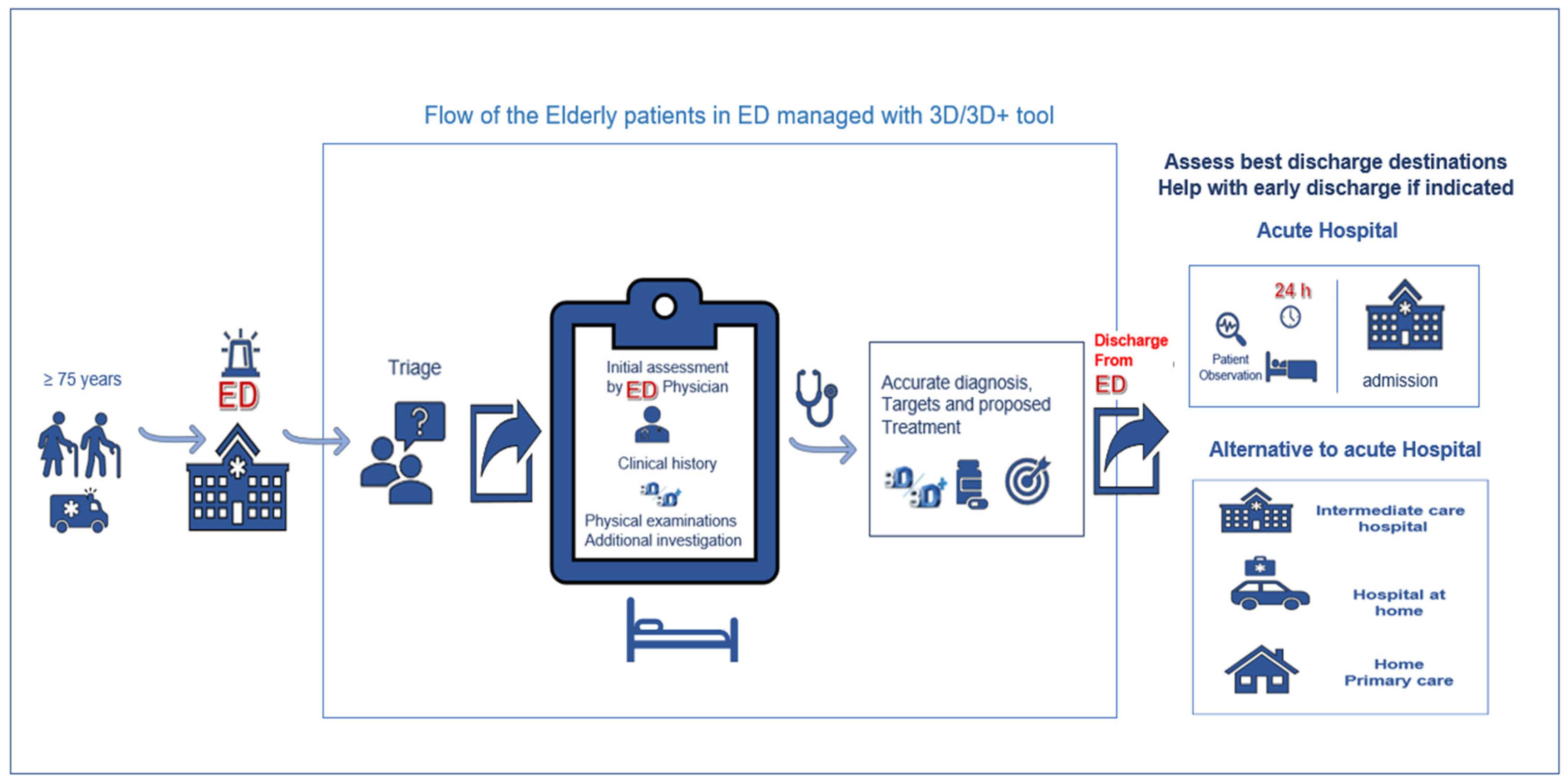
3.2. Destination upon Discharge from the ED and Its Suitability
3.3. Prognostic Accuracy of 3D/3D+ for Predicting Adverse Outcomes
4. Discussion
Supplementary Materials
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Acknowledgments
Conflicts of Interest
References
- Aminzadeh, F.; Dalziel, W.B. Older adults in the emergency department: A systematic review of patterns of use, adverse outcomes, and effectiveness of interventions. Ann. Emerg. Med. 2002, 39, 238–247. [Google Scholar] [CrossRef] [PubMed]
- Terrell, K.M.; Hustey, F.M.; Hwang, U.; Gerson, L.W.; Wenger, N.S.; Miller, D.K. Quality indicators for geriatric Emergency care. Acad. Emerg. Med. 2009, 16, 441–449. [Google Scholar] [CrossRef]
- Puig-Campmany, M.; Ris-Romeu, J. Frail older patients in the emergency department: Main challenges. Emergencias 2022, 34, 415–417. [Google Scholar] [PubMed]
- Martín-Sánchez, F.J.; Fernández-Alonso, C.; Merino, C. El paciente geriátrico en urgencias. In Anales del Sistema Sanitario de Navarra; Gobierno de Navarra, Departamento de Salud: Pamplona, Spain, 2010; Volume 33, pp. 163–172. [Google Scholar]
- Fried, L.P.; Tangen, C.M.; Walston, J.; Newman, A.B.; Hirsch, C.; Gottdiener, J.; Seeman, T.; Tracy, R.; Kop, W.J.; Burke, G.; et al. Frailty in older adults: Evidence for a phenotype. J. Gerontol. A Biol. Sci. Med. Sci. 2001, 56, 146–156. Available online: http://www.ncbi.nlm.nih.gov/pubmed/11253156 (accessed on 1 February 2023). [CrossRef] [PubMed]
- Morley, J.E.; Vellas, B.; van Kan, G.A.; Anker, S.D.; Bauer, J.M.; Bernabei, R.; Cesari, M.; Chumlea, W.C.; Doehner, W.; Evans, J.; et al. Frailty consensus: A call to action. J. Am. Med. Dir. Assoc. 2013, 14, 392–397. Available online: http://www.ncbi.nlm.nih.gov/pubmed/23764209 (accessed on 1 February 2023). [CrossRef] [PubMed]
- Rodríguez-Mañas, L.; Féart, C.; Mann, G.; Viña, J.; Chatterji, S.; Chodzko-Zajko, W.; Gonzalez-Colaço Harmand, M.; Bergman, H.; Carcaillon, L.; Nicholson, C.; et al. Searching for an operational definition of frailty: A Delphi method based consensus statement. The frailty operative definition-consensus conference project. J. Gerontol. A Biol. Sci. Med. Sci. 2013, 68, 62–67. [Google Scholar] [CrossRef]
- Pulok, M.H.; Theou, O.; van der Valk, A.M.; Rockwood, K. The role of illness acuity on the association between frailty and morality in emergency department patients referred to internal medicine. Age Ageing 2020, 49, 1071–1079. [Google Scholar] [CrossRef]
- American College of Emergency Physicians; American Geriatrics Society; Emergency Nurses Association; Society for Academic Emergency Medicine; Geriatric Emergency Department Guidelines Task Force. Geriatric emergency department guidelines. Ann. Emerg. Med. 2014, 63, 7–25. [Google Scholar] [CrossRef]
- Ellis, G.; Gardner, M.; Tsiachristas, A.; Langhorne, P.; Burke, O.; Harwood, R.H.; Conroy, S.P.; Kircher, T.; Somme, D.; Saltvedt, I.; et al. Comprehensive geriatric assessment for older adults admitted to hospital. Cochrane Database Syst. Rev. 2017, 9, CD006211. [Google Scholar] [CrossRef]
- Pilotto, A.; Gallina, P.; Fontana, A.; Sancarlo, D.; Bazzano, S.; Copetti, M.; Maggi, S.; Paroni, G.; Marcato, F.; Pellegrini, F.; et al. Development and validation of a multidimensional prognostic index for mortality based on a standardized Multidimensional Assessment Schedule (MPI-SVaMA) in community-dwelling older subjects. J. Am. Med. Dir. Assoc. 2013, 14, 287–292. [Google Scholar] [CrossRef]
- McCusker, J.; Bellavance, F.; Cardin, S.; Trepanier, S.; Verdon, J.; Ardman, O. Detection of older people at increased risk of adverse health outcomes after an emergency visit: The ISAR screening tool. J. Am. Geriatr. Soc. 1999, 47, 1229–1237. [Google Scholar] [CrossRef] [PubMed]
- Rockwood, K.; Song, X.; MacKnight, C.; Bergman, H.; Hogan, D.B.; McDowell, I.; Mitnitski, A. A global clinical measure of fitness and frailty in elderly people. CMAJ 2005, 173, 489–495. [Google Scholar] [CrossRef] [PubMed]
- Serina, P.; Lo, A.X.; Kocherginsky, M.; Gray, E.; Lindquist, L.A.; Post, L.A.; Heinemann, A.W.; Cruz, D.; Dresden, S.M. The clinical frailty scale and health services use for older adults in the emergency department. J. Am. Geriatr. Soc. 2021, 69, 837–839. [Google Scholar] [CrossRef] [PubMed]
- Martín- Sánchez, F.J.; Fernández Alonso, C.; Gil Gregorio, P. Puntos claves en la asistencia al anciano frágil en Urgencias. Med. Clin. 2013, 140, 24–29. [Google Scholar] [CrossRef] [PubMed]
- Church, S.; Rogers, E.; Rockwood, K.; Theou, O. A scoping review of the Clinical Frailty Scale. BMC Geriatr. 2020, 20, 393. [Google Scholar] [CrossRef]
- Garcia-Pérez, D.; Robles-Perea, L.; Vena-Martínez, A.; Arnau, A.; Robles-Bernabeu, G.; Espaulella-Panicot, J. Las 3D/3D+ como herramienta de valoración geriátrica rápida y de adecuación del recurso asistencial al alta de los Servicios de Urgencias. Rev. Esp. Geriatr. Gerontol. 2022, 57, 212–219. [Google Scholar] [CrossRef]
- Rivero-Santana, A.; del Pino-Sedeño, T.; Ramallo-Fariña, Y.; Vergara, I.; Serrano-Aguilar, P. Valor de los instrumentos ISAR y TRST para predecir resultados adversos en población general geriátrica asistida en los servicios de urgencias: Metaanálisis. Emergencias 2017, 29, 49–60. [Google Scholar]
- Bases Conceptuals i Model d’atenció per a les Persones Fràgils, Amb Cronicitat Complexa (PCC) o Avançada (MACA). (Consultado 04-03-2022). Departament de Salut. Generalitat de Catalunya. Available online: https://salutweb.gencat.cat/ca/ambits_actuacio/linies_dactuacio/estrategies_salut/cronicitat/documentacio-pla-de-salut-2016-2020/ (accessed on 1 February 2023).
- Lasmarías, C.; Aradilla-Herrero, A.; Esquinas, C.; Santaeugènia, S.; Cegri, F.; Limón, E.; Subirana-Casacuberta, M. Primary care professionals’ self-efficacy surrounding advance care planning and its link to sociodemographics, background and perceptions: A cross-sectional study. Int. J. Environ. Res. Public Health 2021, 18, 9034. [Google Scholar] [CrossRef]
- Wylie, C.M. Measuring end results of rehabilitation of patients with stroke. Public Health Rep. 1967, 82, 893–898. [Google Scholar] [CrossRef]
- Gresham, G.E.; Philips, T.F.; Labi, M.L.C. ADL status in stroke: Relative merits of three standard indexes. Arch. Phys. Med. Rehabil. 1980, 61, 355–358. [Google Scholar]
- Pfeiffer, E. A short portable mental status questionnaire for the assessment of organic brain deficit in elderly patients. J. Am. Geriatr. Soc. 1975, 23, 433–441. [Google Scholar] [CrossRef] [PubMed]
- Sánchez Bermejo, R.; Cortés Fadrique, C.; Rincón Fraile, B.; Fernández Centeno, E.; Peña Cueva, S.; de las Heras Castro, E.M. El triaje en urgencias en los hospitales españoles. Emergencias 2013, 25, 66–70. [Google Scholar]
- Harris, P.A.; Taylor, R.; Thielke, R.; Payne, J.; Gonzalez, N.; Conde, J.G. Research electronic data capture (REDCap) a metadata-driven methodology and workflow process for providing translational research informatics support. J. Biomed. Inform. 2009, 42, 377–381. [Google Scholar] [CrossRef] [PubMed]
- COVID-19 Rapid Guideline: Critical Care in Adults; National Institute for Health and Care Excellence (NICE): London, UK, 2021.
- Rockwood, K.; Theou, O. Using the clinical frailty scale in allocating scarce health care resources. Can. Geriatr. J. 2020, 23, 210–215. [Google Scholar] [CrossRef] [PubMed]
- Hubbard, R.E.; Peel, N.M.; Samanta, M.; Gray, L.C.; Mitnitski, A.; Rockwood, K. Frailty status at admission to hospital predicts multiple adverse outcomes. Age Ageing 2017, 46, 801–806. [Google Scholar] [CrossRef] [PubMed]
- Evans, S.J.; Sayers, M.; Mitnitski, A.; Rockwood, K. The risk of adverse outcomes in hospitalized older patients in relation to a frailty index based on a comprehensive geriatric assessment. Age Ageing 2014, 43, 127–132. [Google Scholar] [CrossRef]
- Elliott, A.; Phelps, K.; Regen, E.; Conroy, S.P. Identifying frailty in the emergency department-feasibility study. Age Ageing 2017, 46, 840–845. [Google Scholar] [CrossRef]
- Elliott, A.; Hull, L.; Conroy, S.P. Frailty identification in the emergency department-a systematic review focussing on feasibility. Age Ageing 2017, 46, 509–513. [Google Scholar] [CrossRef]
- Fehlmann, C.A.; Nickel, C.H.; Cino, E.; Al-Najjar, Z.; Langlois, N.; Eagles, D. Frailty assessment in emergency medicine using the Clinical Frailty Scale: A scoping review. Intern. Emerg. Med. 2022, 17, 2407–2418. [Google Scholar] [CrossRef]
- Elliott, A.; Taub, N.; Banerjee, J.; Aijaz, F.; Jones, W.; Teece, L.; van Oppen, J.; Conroy, S. Does the Clinical Frailty Scale at Triage Predict Outcomes from Emergency Care for Older People? Ann. Emerg. Med. 2021, 77, 620–627. [Google Scholar] [CrossRef]
- Nissen, S.K.; Rueegg, M.; Carpenter, C.R.; Kaeppeli, T.; Busch, J.M.; Fournaise, A.; Nickel, C.H. Prognosis for older people at presentation to emergency department based on frailty and aggregated vital signs. J. Am. Geriatr. Soc. 2023, 71, 1250–1258. [Google Scholar] [CrossRef] [PubMed]
- Rueegg, M.; Nissen, S.K.; Brabrand, M.; Kaeppeli, T.; Dreher, T.; Carpenter, C.R.; Bingisser, R.; Nickel, C.H. The clinical frailty scale predicts 1-year mortality in emergency department patients aged 65 years and older. Acad. Emerg. Med. 2022, 29, 572–580. [Google Scholar] [CrossRef] [PubMed]
- Carpenter, C.R.; Shelton, E.; Fowler, S.; Suffoletto, B.; Platts-Mills, T.F.; Rothman, R.E.; Hogan, T.M. Risk factors and screening instrument to predict adverse outcome for undifferentiated older emergency department patients: A systematic review and meta-analysis. Acad. Emerg. Med. 2015, 22, 1–21. [Google Scholar] [CrossRef]
- Francis, J.; Kapoor, W.N. Prognosis after hospital discharge of older medical patients with delirium. J. Am. Geriatr. Soc. 1992, 40, 601–606. [Google Scholar] [CrossRef]
- Marcantonio, E.R. Delirium in hospitalized older adults. N. Engl. J. Med. 2017, 15, 1456–1466. [Google Scholar] [CrossRef] [PubMed]
- Rockwood, K.; Cosway, S.; Carver, D.; Jarrett, P.; Stadnyk, K.; FisK, J. The risk of dementia and death after delirium. Age Ageing 1999, 28, 551–556. [Google Scholar] [CrossRef]
- McCusker, M.J.; Cole, M.; Abrahamowicz, M.; Primeau, F.; Belzile, E. Delirium predicts 12-month mortality. Arch. Intern. Med. 2002, 162, 457–463. [Google Scholar] [CrossRef]
- Leslie, D.L.; Zhang, Y.; Holford, T.R.; Bogardus, S.T.; Leo-Summers, L.S.; Inouye, S.K. Premature death associated with delirium at 1-year follow-up. Arch. Intern. Med. 2005, 165, 1657–1662. [Google Scholar] [CrossRef]
- Cano-Escalera, G.; Graña, M.; Irazusta, J.; Labayen, I.; Besga, A. Survival of frail elderly with delirium. Int. J. Environ. Res. Public Health 2022, 19, 2247. [Google Scholar] [CrossRef]
- Umegaki, H.; Nagae, M.; Komiya, H.; Watanabe, K.; Yamada, Y.; Sakai, T. Association between changes in frailty during hospitalization in older adults and 3-month mortality after discharge. Eur. Geriatr. Med. 2022, 13, 1403–1406. [Google Scholar] [CrossRef]
- Amblàs-Novellas, J.; Torné, A.; Oller, R.; Martori, J.C.; Espaulella, J.; Romero-Ortuno, R. Transitions between degrees of multidimensional frailty among older people admitted to intermediate care: A multicentre prospective study. BMC Geriatr. 2022, 22, 722. [Google Scholar] [CrossRef] [PubMed]
- Megalla, M.; Avula, R.; Manners, C.; Chinnery, P.; Perrella, L.; Finefrock, D. Using the 4M Model to Screen Geriatric Patients in the Emergency Department. J. Geriatr. Emerg. Med. 2021, 2, 9. [Google Scholar] [CrossRef]
- Mate, K.; Fulmer, T.; Pelton, L.; Berman, A.; Bonner, A.; Huang, W.; Zhang, J. Evidence for the 4Ms: Interactions and outcomes across the care continuum. J. Aging Health 2021, 33, 469–481. [Google Scholar] [CrossRef]
- Puig Campmany, M.; Ris Romeu, J.; Blázquez Andión, M.; Benito Vales, S. Development of a comprehensive, multidisciplinary program of care for frailty in an emergency department. Eur. Geriatr. Med. 2019, 10, 37–46. [Google Scholar] [CrossRef] [PubMed]
| Total | Women | Men | p-Value | |
|---|---|---|---|---|
| N = 278 | n = 166 | n = 112 | ||
| Age [median (p25–p75)] | 86.0 [83.0–90.0] | 87.0 [83.0–91.8] | 85.0 [81.8–89.0] | 0.021 |
| Gender (female) | 166 (59.7) | NA | ||
| Time frame | 0.523 | |||
| 07:01–14:00 | 120 (43.2) | 71 (42.8) | 49 (43.8) | |
| 14:01–22:00 | 106 (38.1) | 67 (40.4) | 39 (34.8) | |
| 22:01–07:00 | 52 (18.7) | 28 (16.9) | 24 (21.4) | |
| Triage level | 0.222 | |||
| II | 47 (16.9) | 24 (14.5) | 23 (20.5) | |
| III | 175 (62.9) | 104 (62.7) | 71 (63.4) | |
| IV | 56 (20.1) | 38 (22.9) | 18 (16.1) | |
| Prior medical care at home (Yes) | 119 (42.8) | 76 (45.8) | 43 (38.4) | 0.222 |
| Arrival at ED by ambulance (Yes) | 223 (80.2) | 141 (84.9) | 82 (73.2) | 0.016 |
| PCC (Yes) | 186 (66.9) | 117 (70.5) | 69 (61.6) | 0.123 |
| MACA (Yes) | 36 (12.9) | 18 (10.8) | 18 (16.1) | 0.203 |
| Readmission (≥2 or more times/last year) | 107 (38.9) | 62 (37.6) | 45 (40.9) | 0.579 |
| Reason for consultation | ||||
| Dyspnea | 140 (50.4) | 78 (47.0) | 62 (55.4) | 0.171 |
| General malaise | 40 (14.4) | 30 (18.1) | 10 (8.93) | 0.033 |
| Anemia | 6 (2.16) | 4 (2.41) | 2 (1.79) | 0.726 |
| Fever | 34 (12.2) | 20 (12.0) | 14 (12.5) | 0.910 |
| Chest pain | 9 (3.24) | 5 (3.01) | 4 (3.57) | 0.796 |
| Abdominal pain | 20 (7.19) | 16 (9.64) | 4 (3.57) | 0.055 |
| Locomotor pain | 1 (0.36) | 1 (0.60) | 0 (0.00) | 0.410 |
| Falls | 23 (8.27) | 15 (9.04) | 8 (7.14) | 0.574 |
| Neurological symptoms | 38 (13.7) | 22 (13.3) | 16 (14.3) | 0.806 |
| Others | 16 (5.76) | 7 (4.22) | 9 (8.04) | 0.180 |
| Barthel Index 1 | 0.041 | |||
| Independent (90–100) | 60 (23.9) | 27 (18.1) | 33 (32.3) | |
| Mild dependency (61–89) | 51 (20.3) | 29 (19.5) | 22 (21.6) | |
| Moderate dependency (45–60) | 63 (25.1) | 41 (27.5) | 22 (21.6) | |
| Severe dependency (<45) | 77 (30.7) | 52 (34.9) | 25 (24.5) | |
| Pfeiffer Questionnaire 2 | 0.094 | |||
| No cognitive impairment | 128 (52.9) | 67 (47.2) | 61 (61.0) | |
| Mild cognitive impairment | 67 (27.7) | 43 (30.3) | 24 (24.0) | |
| Moderate cognitive impairment | 10 (4.1) | 5 (3.5) | 5 (5.0) | |
| Severe cognitive impairment | 37 (15.3) | 27 (19.0) | 10 (10.0) | |
| Rockwood Clinical Frailty Scale | 0.008 | |||
| Fit (CFS 1) | 3 (1.08) | 0 (0.00) | 3 (2.68) | |
| Well (CFS 2) | 15 (5.40) | 4 (2.41) | 11 (9.82) | |
| Managing well (CFS 3) | 28 (10.1) | 13 (7.83) | 15 (13.4) | |
| Vulnerable (CFS 4) | 44 (15.8) | 26 (15.7) | 18 (16.1) | |
| Slightly frail (CFS 5) | 32 (11.5) | 18 (10.8) | 14 (12.5) | |
| Moderately frail (CFS 6) | 56 (20.1) | 38 (22.9) | 18 (16.1) | |
| Severely frail (CFS 7) | 66 (23.7) | 47 (28.3) | 19 (17.0) | |
| Very severely frail (CFS 8) | 30 (10.8) | 19 (11.4) | 11 (9.82) | |
| Terminally ill (CFS 9) | 4 (1.4) | 1 (0.60) | 3 (2.68) | |
| ISAR scale | ||||
| ≥2 | 253 (91.0) | 157 (94.6) | 96 (85.7) | 0.011 |
| ≥3 | 209 (75.2) | 137 (82.5) | 72 (64.3) | <0.001 |
| ≥4 | 141 (50.7) | 92 (55.4) | 49 (43.8) | 0.056 |
| Diagnosis at ED discharge | 0.524 | |||
| Cardiac respiratory failure | 32 (11.5) | 21 (12.7) | 11 (9.82) | |
| Lung respiratory failure | 65 (23.4) | 36 (21.7) | 29 (25.9) | |
| Mixed respiratory failure | 12 (4.3) | 7 (4.22) | 5 (4.46) | |
| Lung infection | 36 (12.9) | 18 (10.8) | 18 (16.1) | |
| Abdominal infection | 8 (2.9) | 7 (4.22) | 1 (0.89) | |
| Urinary infection | 26 (9.4) | 18 (10.8) | 8 (7.14) | |
| Skin infection | 2 (0.7) | 1 (0.60) | 1 (0.89) | |
| Fractures | 3 (1.1) | 3 (1.81) | 0 (0.00) | |
| Stroke | 12 (4.3) | 7 (4.22) | 5 (4.46) | |
| Others | 82 (29.5) | 48 (28.9) | 34 (30.4) | |
| The patient or family prioritizes treatment at home (Yes) | 121 (43.5) | 73 (44.0) | 48 (42.9) | 0.854 |
| Total N = 278 | Women n = 166 | Men n = 112 | p-Value | |
|---|---|---|---|---|
| 3D Baseline component | ||||
| Difficulties with BADL, walking, or physical activity | <0.001 | |||
| No (D0) | 52 (18.7) | 18 (10.8) | 34 (30.4) | |
| Mild (D1) | 53 (19.1) | 28 (16.9) | 25 (22.3) | |
| Moderate (D2) | 96 (34.5) | 66 (39.8) | 30 (26.8) | |
| Severe (D3) | 77 (27.7) | 54 (32.5) | 23 (20.5) | |
| Dementia/Cognitive impairment | 0.142 | |||
| No (D0) | 139 (50.0) | 75 (45.2) | 64 (57.1) | |
| Mild (D1) | 55 (19.8) | 33 (19.9) | 22 (19.6) | |
| Moderate (D2) | 47 (16.9) | 34 (20.5) | 13 (11.6) | |
| Severe (D3) | 37 (13.3) | 24 (14.5) | 13 (11.6) | |
| Dwelling | 0.030 | |||
| Lives in own home alone | 30 (10.8) | 18 (10.8) | 12 (10.7) | |
| Lives in own home with family or caregiver | 178 (64.0) | 97 (58.4) | 81 (72.3) | |
| Nursing home | 70 (25.2) | 51 (30.7) | 19 (17.0) | |
| 3D Baseline component | <0.001 | |||
| No frailty (3D 0) | 47 (16.9) | 16 (9.6) | 31 (27.7) | |
| Mild frailty (3D 1) | 52 (18.7) | 28 (16.9) | 24 (21.4) | |
| Moderate frailty (3D 2) | 94 (33.8) | 65 (39.2) | 29 (25.9) | |
| Advanced frailty (3D 3) | 85 (30.6) | 57 (34.3) | 28 (25.0) | |
| 3D+ Dynamic component | ||||
| Decline in BADL-IADL | 0.530 | |||
| No | 116 (41.7) | 65 (39.2) | 51 (45.5) | |
| Yes, acute | 104 (37.4) | 66 (39.8) | 38 (33.9) | |
| Yes, progressive | 58 (20.9) | 35 (21.1) | 23 (20.5) | |
| Delirium | 0.130 | |||
| No | 212 (76.3) | 122 (73.5) | 90 (80.4) | |
| Yes, hyperactive | 17 (6.1) | 14 (8.4) | 3 (2.7) | |
| Yes, hypoactive | 49 (17.6) | 30 (18.1) | 19 (17.0) | |
| Dwelling | 0.572 | |||
| Is 24 h treatment at home feasible? (No) | 55 (19.8) | 31 (18.7) | 24 (21.4) | |
| Drugs | 0.090 | |||
| Might drugs (start/withdrawal) be a trigger of the presenting complaint? | 39 (14.0) | 29 (17.5) | 10 (8.93) | |
| 3D+ Dynamic component (impact of acute illness) | 0.187 | |||
| Impairment | 167 (60.1) | 105 (63.3) | 62 (55.4) | |
| No impairment | 111 (39.9) | 61 (36.7) | 50 (44.6) | |
| 3D+ (Delirium) | 3D+ (Delirium and Functional Decline) | ||||||
|---|---|---|---|---|---|---|---|
| N = 278 | No Alteration n = 212 | Alteration n = 66 | p-Value | No Alteration n = 220 | Alteration n = 58 | p-Value | |
| 72 h ED returns | 5 (1.8) | 4 (1.9) | 1 (1.5) | 0.843 | 4 (1.8) | 1 (1.7) | 0.962 |
| 72 h hospital readmission | 3 (1.1) | 3 (1.4) | 0 (0) | 0.331 | 3 (1.6) | 0 (0) | 0.371 |
| 30-day ED returns | 50 (18.0) | 42 (19.8) | 8 (12.1) | 0.155 | 43 (19.6) | 7 (12.1) | 0.187 |
| 30-day hospital readmission | 28 (10.1) | 23 (10.9) | 5 (7.6) | 0.440 | 23 (10.5) | 5 (8.6) | 0.680 |
| 30-day mortality | 54 (19.4) | 21 (9.9) | 33 (50.0) | <0.001 | 23 (10.5) | 31 (53.5) | <0.001 |
| 30-day any adverse outcome | 100 (36.0) | 60 (28.3) | 40 (60.6) | <0.001 | 63 (28.6) | 37 (63.8) | <0.001 |
| 6-month mortality | 86 (30.9) | 45 (21.2) | 41 (62.1) | <0.001 | 49 (22.2) | 37 (63.8) | <0.001 |
| 12-month mortality | 107 (38.5) | 64 (30.2) | 43 (65.2) | <0.001 | 69 (31.4) | 38 (65.5) | <0.001 |
| Sensitivity (95% CI) | Specificity (95% CI) | PPV (95% CI) | NPV (95% CI) | |
|---|---|---|---|---|
| 30-day mortality | ||||
| 3D+ (delirium) | 0.61 (0.55–0.67) | 0.85 (0.81–0.89) | 0.50 (0.44–0.56) | 0.90 (0.87–0.94) |
| 3D+ (delirium and functional decline) | 0.57 (0.52–0.63) | 0.88 (0.84–0.92) | 0.53 (0.48–0.59) | 0.90 (0.86–0.93) |
| CFS (≥5) | 0.81 (0.69–0.91) | 0.36 (0.29–0.42) | 0.23 (0.18–0.30) | 0.89 (0.81–0.95) |
| CFS (≥7) | 0.54 (0.40–0.67) | 0.68 (0.62–0.74) | 0.29 (0.20–0.39) | 0.86 (0.80–0.91) |
| ISAR (≥2) | 0.94 (0.85–0.99) | 0.10 (0.06–0.14) | 0.20 (0.15–0.26) | 0.88 (0.69–0.97) |
| ISAR (≥3) | 0.83 (0.71–0.92) | 0.27 (0.21–0.33) | 0.22 (0.16–0.28) | 0.87 (0.77–0.94) |
| 72 h ED returns | ||||
| 3D+ (delirium) | 0.20 (0.15–0.25) | 0.76 (0.71–0.81) | 0.02 (0.00–0.03) | 0.98 (0.97–1.00) |
| 3D+ (delirium and functional decline) | 0.20 (0.15–0.25) | 0.79 (0.74–0.84) | 0.02 (0.00–0.04) | 0.98 (0.97–1.00) |
| CFS (≥5) | 1.00 (0.48–1.00) | 0.33 (0.27–0.39) | 0.03 (0.01–0.06) | 1.00 (0.96–1.00) |
| CFS (≥7) | 0.80 (0.28–0.99) | 0.65 (0.59–0.70) | 0.04 (0.01–0.10) | 0.99 (0.97–1.00) |
| ISAR (≥2) | 1.00 (0.48–1.00) | 0.09 (0.06–0.13) | 0.02 (0.01–0.05) | 1.00 (0.86–1.00) |
| ISAR (≥3) | 1.00 (0.48–1.00) | 0.25 (0.20–0.31) | 0.02 (0.01–0.05) | 1.00 (0.95–1.00) |
| 30-day ED returns | ||||
| 3D+ (delirium) | 0.16 (0.12–0.20) | 0.75 (0.69–0.80) | 0.12 (0.08–0.16) | 0.80 (0.76–0.85) |
| 3D+ (delirium and functional decline) | 0.14 (0.10–0.18) | 0.78 (0.73–0.83) | 0.12 (0.08–0.16) | 0.80 (0.76–0.85) |
| CFS (≥5) | 0.66 (0.51–0.79) | 0.32 (0.26–0.38) | 0.18 (0.12–0.24) | 0.81 (0.71–0.89) |
| CFS (≥7) | 0.28 (0.16–0.42) | 0.62 (0.56–0.69) | 0.14 (0.08–0.22) | 0.80 (0.73–0.85) |
| ISAR (≥2) | 0.88 (0.76–0.95) | 0.08 (0.05–0.13) | 0.17 (0.13–0.23) | 0.76 (0.55–0.91) |
| ISAR (≥3) | 0.70 (0.55–0.82) | 0.24 (0.18–0.30) | 0.17 (0.12–0.23) | 0.78 (0.67–0.87) |
| 30-day any adverse outcome | ||||
| 3D+ (delirium) | 0.40 (0.34–0.46) | 0.85 (0.81–0.90) | 0.61 (0.55–0.66) | 0.72 (0.66–0.77) |
| 3D+ (delirium and functional decline) | 0.37 (0.31–0.43) | 0.88 (0.84–0.92) | 0.64 (0.58–0.69) | 0.71 (0.66–0.77) |
| CFS (≥5) | 0.74 (0.64–0.82) | 0.36 (0.29–0.43) | 0.39 (0.32–0.47) | 0.71 (0.61–0.80) |
| CFS (≥7) | 0.41 (0.31–0.51) | 0.67 (0.59–0.74) | 0.41 (0.31–0.51) | 0.67 (0.59–0.74) |
| ISAR (≥2) | 0.92 (0.85–0.96) | 0.10 (0.06–0.15) | 0.36 (0.30–0.43) | 0.68 (0.46–0.85) |
| ISAR (≥3) | 0.78 (0.69–0.86) | 0.26 (0.20–0.34) | 0.37 (0.31–0.44) | 0.68 (0.56–0.79) |
| 6-month mortality | ||||
| 3D+ (delirium) | 0.48 (0.42–0.54) | 0.87 (0.83–0.91) | 0.62 (0.56–0.68) | 0.79 (0.74–0.84) |
| 3D+ (delirium and functional decline) | 0.43 (0.37–0.49) | 0.89 (0.85–0.93) | 0.64 (0.58–0.69) | 0.78 (0.73–0.83) |
| CFS (≥5) | 0.81 (0.72–0.89) | 0.39 (0.32–0.46) | 0.37 (0.30–0.45) | 0.82 (0.73–0.89) |
| CFS (≥7) | 0.52 (0.41–0.63) | 0.71 (0.64–0.78) | 0.45 (0.35–0.55) | 0.77 (0.70–0.83) |
| ISAR (≥2) | 0.95 (0.89–0.99) | 0.11 (0.07–0.16) | 0.32 (0.27–0.39) | 0.84 (0.64–0.95) |
| ISAR (≥3) | 0.83 (0.73–0.90) | 0.28 (0.22–0.35) | 0.34 (0.28–0.41) | 0.78 (0.67–0.87) |
| 12-month mortality | ||||
| 3D+ (delirium) | 0.40 (0.34–0.46) | 0.87 (0.83–0.91) | 0.65 (0.60–0.71) | 0.70 (0.64–0.75) |
| 3D+ (delirium and functional decline) | 0.36 (0.30–0.41) | 0.88 (0.85–0.92) | 0.66 (0.60–0.71) | 0.69 (0.63–0.74) |
| CFS (≥5) | 0.80 (0.72–0.87) | 0.40 (0.33–0.48) | 0.46 (0.38–0.53) | 0.77 (0.67–0.85) |
| CFS (≥7) | 0.51 (0.42–0.61) | 0.74 (0.66–0.80) | 0.55 (0.45–0.65) | 0.71 (0.64–0.77) |
| ISAR (≥2) | 0.93 (0.86–0.97) | 0.10 (0.06–0.15) | 0.39 (0.33–0.45) | 0.68 (0.46–0.85) |
| ISAR (≥3) | 0.79 (0.71–0.87) | 0.27 (0.21–0.35) | 0.41 (0.34–0.48) | 0.68 (0.56–0.79) |
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2023 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Garcia-Pérez, D.; Vena-Martínez, A.; Robles-Perea, L.; Roselló-Padullés, T.; Espaulella-Panicot, J.; Arnau, A. Prognostic Value of a New Tool (the 3D/3D+) for Predicting 30-Day Mortality in Emergency Department Patients Aged 75 Years and Older. J. Clin. Med. 2023, 12, 6469. https://doi.org/10.3390/jcm12206469
Garcia-Pérez D, Vena-Martínez A, Robles-Perea L, Roselló-Padullés T, Espaulella-Panicot J, Arnau A. Prognostic Value of a New Tool (the 3D/3D+) for Predicting 30-Day Mortality in Emergency Department Patients Aged 75 Years and Older. Journal of Clinical Medicine. 2023; 12(20):6469. https://doi.org/10.3390/jcm12206469
Chicago/Turabian StyleGarcia-Pérez, Dolors, Anabelén Vena-Martínez, Laura Robles-Perea, Teresa Roselló-Padullés, Joan Espaulella-Panicot, and Anna Arnau. 2023. "Prognostic Value of a New Tool (the 3D/3D+) for Predicting 30-Day Mortality in Emergency Department Patients Aged 75 Years and Older" Journal of Clinical Medicine 12, no. 20: 6469. https://doi.org/10.3390/jcm12206469
APA StyleGarcia-Pérez, D., Vena-Martínez, A., Robles-Perea, L., Roselló-Padullés, T., Espaulella-Panicot, J., & Arnau, A. (2023). Prognostic Value of a New Tool (the 3D/3D+) for Predicting 30-Day Mortality in Emergency Department Patients Aged 75 Years and Older. Journal of Clinical Medicine, 12(20), 6469. https://doi.org/10.3390/jcm12206469







