Mitral Valve Repair in Advanced Age Groups: Does Cardiac Age Differ from Chronological Age?
Abstract
1. Introduction
2. Patients and Methods
2.1. Ethical Statement
2.2. Study Design and Data Collection
2.3. Statistical Analysis
3. Result
3.1. Baseline
3.2. Cardiac Parameters
3.3. Surgical Procedure
3.4. Postoperative Morbidity and Mortality
4. Healthy vs. Unhealthy Heart and Its Influence on Mortality and Outcome
5. Preoperative Condition and Postoperative Outcome in Different Life Decades
6. Discussion
7. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Conflicts of Interest
References
- Roger, V.L.; Go, A.S.; Lloyd-Jones, D.M.; Adams, R.J.; Berry, J.D.; Brown, T.M.; Carnethon, M.R.; Dai, S.; de Simone, G.; Ford, E.S.; et al. Executive Summary: Heart Disease and Stroke Statistics—2011 Update: A Report from the American Heart Association. Circulation 2011, 123, 459–463. [Google Scholar] [CrossRef] [PubMed]
- Tsao, C.W.; Aday, A.W.; Almarzooq, Z.I.; Alonso, A.; Beaton, A.Z.; Bittencourt, M.S.; Boehme, A.K.; Buxton, A.E.; Carson, A.P.; Commodore-Mensah, Y.; et al. Heart Disease and Stroke Statistics—2022 Update: A Report From the American Heart Association. Circulation 2022, 145, e153–e639. [Google Scholar] [CrossRef] [PubMed]
- Donato, A.J.; Machin, D.R.; Lesniewski, L.A. Mechanisms of Dysfunction in the Aging Vasculature and Role in Age-Related Disease. Circ. Res. 2018, 123, 825–848. [Google Scholar] [CrossRef] [PubMed]
- Dai, D.-F.; Chen, T.; Johnson, S.; Szeto, H.; Rabinovitch, P.S. Cardiac Aging: From Molecular Mechanisms to Significance in Human Health and Disease. Antioxid. Redox Signal. 2012, 16, 1492–1526. [Google Scholar] [CrossRef]
- Lazzeroni, D.; Villatore, A.; Souryal, G.; Pili, G.; Peretto, G. The Aging Heart: A Molecular and Clinical Challenge. Int. J. Mol. Sci. 2022, 23, 16033. [Google Scholar] [CrossRef]
- Ren, J.; Zhang, Y. Targeting Autophagy in Aging and Aging-Related Cardiovascular Diseases. Trends Pharmacol. Sci. 2018, 39, 1064–1076. [Google Scholar] [CrossRef]
- Yan, M.; Sun, S.; Xu, K.; Huang, X.; Dou, L.; Pang, J.; Tang, W.; Shen, T.; Li, J. Cardiac Aging: From Basic Research to Therapeutics. Oxidative Med. Cell. Longev. 2021, 2021, 9570325. [Google Scholar] [CrossRef]
- Wessells, R.J.; Bodmer, R. Cardiac aging. Semin. Cell Dev. Biol. 2007, 18, 111–116. [Google Scholar] [CrossRef]
- Beckmann, A.; Meyer, R.; Lewandowski, J.; Markewitz, A.; Blaßfeld, D.; Böning, A. German Heart Surgery Report 2021: The Annual Updated Registry of the German Society for Thoracic and Cardiovascular Surgery. Thorac. Cardiovasc. Surg. 2022, 70, 362–376. [Google Scholar] [CrossRef]
- Available online: https://www.dgthg.de/sites/default/files/Grafiken-DGTHG-Leistungsstatistik%202021_free-access_pdf (accessed on 29 March 2023).
- Goyal, P.; Kwak, M.J.; Al Malouf, C.; Kumar, M.; Rohant, N.; Damluji, A.A.; Denfeld, Q.E.; Bircher, K.K.; Krishnaswami, A.; Alexander, K.P.; et al. Geriatric Cardiology: Coming of Age. JACC Adv. 2022, 1, 100070. [Google Scholar] [CrossRef]
- Lakatta, E.G.; Levy, D. Arterial and Cardiac Aging: Major Shareholders in Cardiovascular Disease Enterprises: Part II: The aging heart in health: Links to heart disease. Circulation 2003, 107, 346–354. [Google Scholar] [CrossRef] [PubMed]
- Xu, B.; Daimon, M. Cardiac aging phenomenon and its clinical features by echocardiography. J. Echocardiogr. 2016, 14, 139–145. [Google Scholar] [CrossRef] [PubMed]
- Pietri, P.; Stefanadis, C. Cardiovascular Aging and Longevity: JACC State-of-the-Art Review. J. Am. Coll. Cardiol. 2021, 77, 189–204. [Google Scholar] [CrossRef]
- Gorter, T.M.; van Veldhuisen, D.J.; Bauersachs, J.; Borlaug, B.A.; Celutkiene, J.; Coats, A.J.; Crespo-Leiro, M.G.; Guazzi, M.; Harjola, V.-P.; Heymans, S.; et al. Right heart dysfunction and failure in heart failure with preserved ejection fraction: Mechanisms and management. Position statement on behalf of the Heart Failure Association of the European Society of Cardiology. Eur. J. Heart Fail. 2018, 20, 16–37. [Google Scholar] [CrossRef] [PubMed]
- Zornoff, L.A.; Skali, H.; Pfeffer, M.A.; Sutton, M.S.J.; Rouleau, J.L.; Lamas, G.A.; Plappert, T.; Rouleau, J.R.; Moyé, L.A.; Lewis, S.J.; et al. Right ventricular dysfunction and risk of heart failure and mortality after myocardial infarction. J. Am. Coll. Cardiol. 2002, 39, 1450–1455. [Google Scholar] [CrossRef] [PubMed]
- AlJaroudi, W.; Alraies, M.C.; Halley, C.; Rodriguez, L.; Grimm, R.A.; Thomas, J.D.; Jaber, W.A. Impact of Progression of Diastolic Dysfunction on Mortality in Patients With Normal Ejection Fraction. Circulation 2012, 125, 782–788. [Google Scholar] [CrossRef]
- Halley, C.M.; Houghtaling, P.L.; Khalil, M.K.; Thomas, J.D.; Jaber, W.A. Mortality Rate in Patients With Diastolic Dysfunction and Normal Systolic Function. Arch. Intern. Med. 2011, 171, 1082–1087. [Google Scholar] [CrossRef] [PubMed]
- Playford, D.; Strange, G.; Celermajer, D.S.; Evans, G.; Scalia, G.M.; Stewart, S.; Prior, D.; The NEDA Investigators. Diastolic dysfunction and mortality in 436 360 men and women: The National Echo Database Australia (NEDA). Eur. Heart J. Cardiovasc. Imaging 2021, 22, 505–515. [Google Scholar] [CrossRef] [PubMed]
- R Core Team. R: A Language and Environment for Statistical Computing; R Foundation for Statistical Computing: Vienna, Austria, 2020; Available online: https://www.R-project.org/ (accessed on 11 April 2022).
- Ho, D.; Imai, K.; King, G.; Stuart, E.A. MatchIt: Nonparametric Preprocessing for Parametric Causal Inference. J. Stat. Softw. 2011, 42, 1–28. [Google Scholar] [CrossRef]
- Therneau, T.M.; Grambsch, P.M. Modeling Survival Data: Extending the Cox Model; Springer: Berlin/Heidelberg, Germany, 2000; ISBN 0387987843. [Google Scholar]
- Ostovar, R.; Schröter, F.; Kühnel, R.-U.; Hartrumpf, M.; Albes, J.M. What Exactly Makes Age a Risk Factor for an Unfavorable Outcome after Mitral Valve Surgery? J. Clin. Med. 2022, 11, 6907. [Google Scholar] [CrossRef]
- Steenman, M.; Lande, G. Cardiac aging and heart disease in humans. Biophys. Rev. 2017, 9, 131–137. [Google Scholar] [CrossRef] [PubMed]
- Roh, J.; Rhee, J.; Chaudhari, V.; Rosenzweig, A. The Role of Exercise in Cardiac Aging: From Physiology to Molecular Mechanisms. Circ. Res. 2016, 118, 279–295. [Google Scholar] [CrossRef] [PubMed]
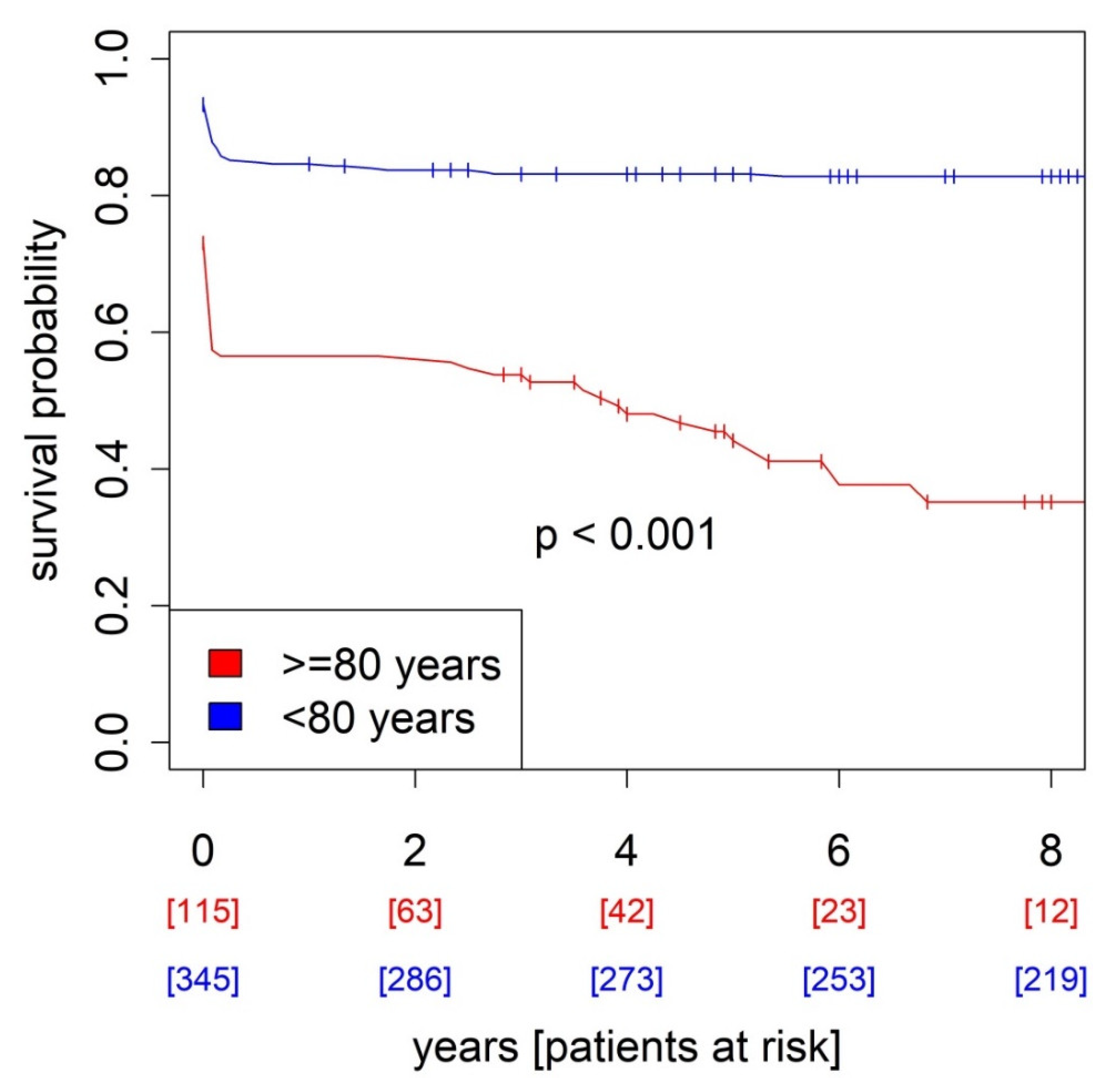
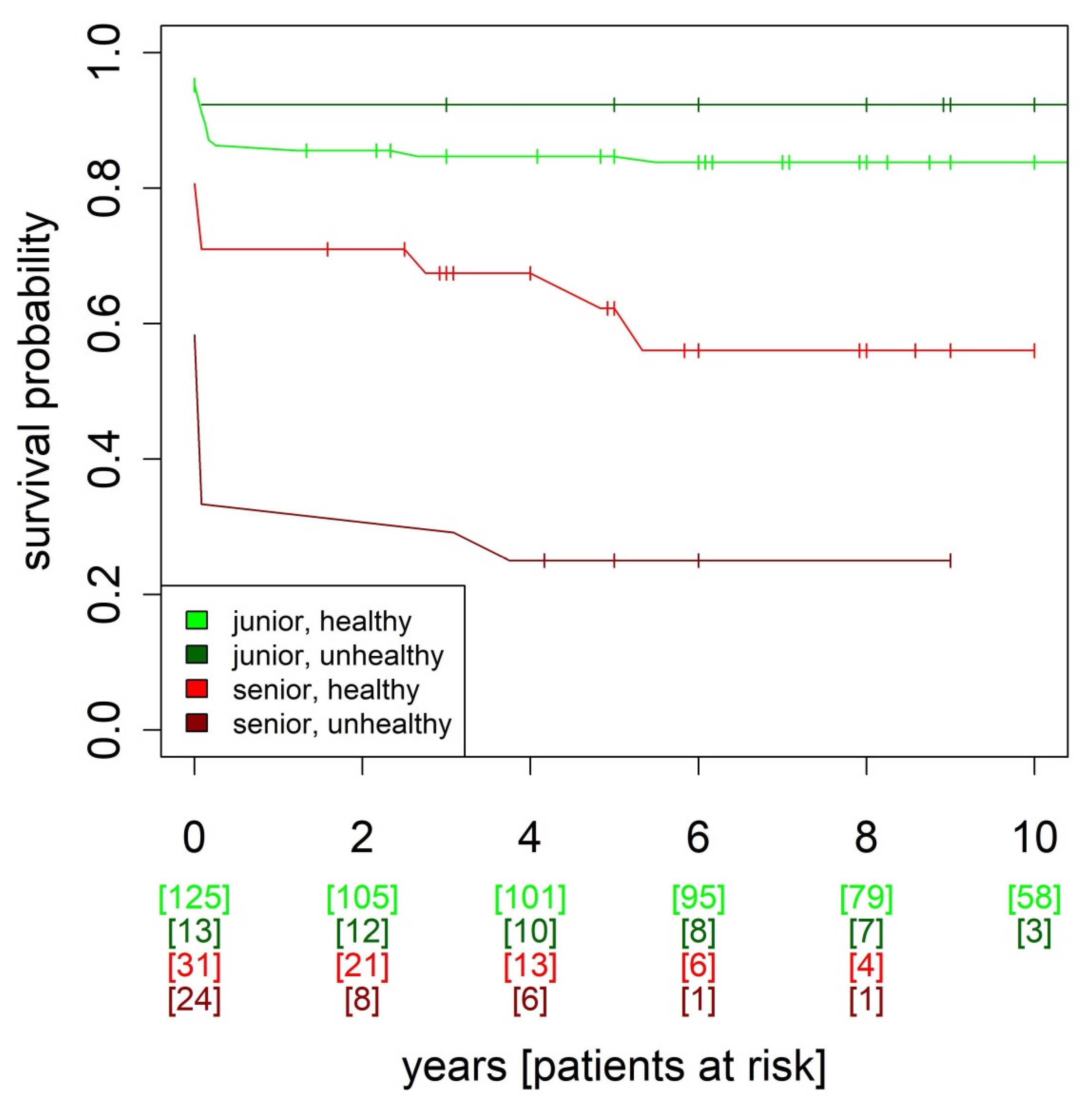

| Senior (n = 115) | Junior (n = 345) | p | |
|---|---|---|---|
| Gender (male) | 58.26% (67) | 56.81% (196) | 0.87 |
| Isolated MVR | 56.52% (65) | 57.68% (199) | 0.913 |
| Redo-Surgery | 13.08% (15) | 10.72% (37) | 0.61 |
| COPD | 12.17% (14) | 11.88% (41) | 1 |
| PAD | 6.96% (8) | 5.8% (20) | 0.822 |
| Cardiomyopathy | 5.22% (6) | 2.61% (9) | 0.289 |
| Liver cirrhosis | 0% (0) | 0% (0) | 1 |
| Hypertension | 86.09% (99) | 87.25% (301) | 0.873 |
| Renal failure | 37.39% (43) | 35.94% (124) | 0.916 |
| Stg. I | 17.39% (20) | 14.2% (49) | 0.497 |
| Stg. II | 1.74% (2) | 4.93% (17) | 0.18 |
| Stg. III | 15.65% (18) | 13.04% (45) | 0.584 |
| Stg. IV | 1.74% (2) | 1.45% (5) | 1 |
| Stg. V | 0.87% (1) | 2.32% (8) | 0.461 |
| No RF | 62.61% (72) | 64.06% (221) | 0.867 |
| Senior | Junior | p | |
|---|---|---|---|
| TAPSE (mm) | 16.59 ± 5.5 | 21.18 ± 5.7 | <0.001 |
| LVEF (mm) | 52 ± 12.9 | 54.09 ± 12.7 | 0.109 |
| LVESD (mm) | 39.31 ± 11.1 | 33.38 ± 8.3 | <0.001 |
| LVEDD (mm) | 54.37 ± 9.4 | 50.83 ± 9.1 | <0.001 |
| LAD (mm) | 48.72 ± 7.2 | 45.65 ± 8.3 | <0.001 |
| Diastolic dysfunction | 56.52% | 8.41% | <0.001 |
| Grade I | 27.83% | 6.67% | |
| Grade II | 21.74% | 0.87% | |
| Grade III | 6.95% | 0.87% | |
| NT-proBNP (pg/mL) | 10,079 ± 11,666 | 2727 ± 6263 | <0.001 |
| Senior (n = 115) | Junior (n = 345) | p-Value | |
|---|---|---|---|
| Surgical data | |||
| CPB time (min) | 170.7 ± 63.8 | 179.8 ± 67.2 | 0.234 |
| Cross clamp time (min) | 105.8 ± 44.1 | 115.5 ± 45.2 | 0.068 |
| Concomitant AVR or TVR | 56.52% | 57.67% | 0.913 |
| Postoperative complications | |||
| Respiratory insufficiency | 28.9% | 11.5% | <0.001 |
| Pneumonia | 14% | 5.3% | 0.004 |
| Pleural effusion | 29.8% | 17.7% | 0.008 |
| CIP/CIM | 7% | 0.6% | <0.001 |
| Low cardiac output | 11.4% | 3.2% | 0.002 |
| SIRS | 29% | 9.7% | <0.001 |
| Kidney failure | 40.7% | 19.1% | <0.001 |
| Dialysis necessity | 26.6% | 16.1% | 0.02 |
| Stroke | 6.3% | 3.3% | 0.256 |
| Pericardial tamponade | 4.4% | 2.6% | 0.534 |
| Delirium | 20.5% | 18.3% | 0.708 |
|
Junior, Cardiac Healthy |
Junior, Cardiac Unhealthy |
Senior, Cardiac Healthy |
Senior, Cardiac Unhealthy | p | ||
|---|---|---|---|---|---|---|
| LVEF | 61.62 ± 5.1 | 31.69 ± 9.2 | 61.52 ± 4.65 | 34.33 ± 7.98 | <0.001 | |
| TAPSE | 23.58 ± 4.04 | 11.77 ± 3.96 | 23.1 ± 3.76 | 12 ± 1.89 | <0.001 | |
| Diastolic dysfunction | 2.4% | 38.46% | 25.81% | 91.67% | <0.001 | |
| Postoperative outcome | ||||||
| In-Hospital Mortality | 11.38% | 7.69% | 29.03% | 66.67% | <0.001 | |
| SIRS | 6.61% | 15.38% | 22.58% | 50% | <0.001 | |
| CIP/CIM | 0% | 0% | 6.45% | 8.33% | 0.014 | |
| Acute kidney failure | 13.93% | 23.08% | 32.26% | 54.17% | <0.001 | |
| Atrial fibrillation | 7.32% | 0% | 29.03% | 41.67% | <0.001 | |
| Respiratory insufficiency | 8.33% | 30.77% | 29.03% | 25% | 0.002 | |
| p -value after posthoc analysis | ||||||
|
Ju healthy vs. Ju unhealthy |
Ju healthy vs. Se healthy |
Ju healthy vs. Se unhealthy |
Ju unhealthy vs. Se healthy |
Ju unhealthy vs. Se unhealthy |
Se healthy vs. Se. unhealthy | |
| In-Hospital Mortality | 1 | 0.087 | <0.001 | 0.503 | 0.01 | 0.049 |
| SIRS | 1 | 0.101 | <0.001 | 1 | 0.266 | 0.266 |
| CIP/CIM | - | 0.215 | 0.126 | 1 | 1 | 1 |
| Acute kidney failure | 1 | 0.168 | <0.001 | 1 | 0.561 | 0.561 |
| Atrial fibrillation | 0.979 | 0.011 | <0.001 | 0.231 | 0.078 | 0.979 |
| Respiratory insufficiency | 0.213 | 0.031 | 0.213 | 1 | 1 | 1 |
|
<60 Years (n = 65) |
60–69 Years (n = 83) | 70–79 Years (n = 197) |
≥80 Years (n = 115) | p | |
|---|---|---|---|---|---|
| Risk profile | |||||
| BMI (kg/cm2) | 28.68 ± 6.46 | 28 ± 4.8 | 27.73 ± 5.37 | 26.29 ± 4.15 | 0.002 |
| EuroSCORE II (%) | 10.31 ± 17.23 | 11.95 ± 13.81 | 18.7 ± 18.01 | 26.53 ± 21.88 | <0.001 |
| Kidney failure | 21.54% | 26.51% | 44.67% | 37.39% | 0.004 |
| Concomitant surgery | 43.08% | 55.42% | 63.45% | 56.52% | 0.063 |
| NT-proBNP (pg/mL) | 1998 ± 2927 | 3008 ± 7022 | 2799 ± 6566 | 10079 ± 11,666 | <0.001 |
| Echocardiographic data | |||||
| LVESD (mm) | 35.2 ± 8.91 | 34.73 ± 7.88 | 32.22 ± 8.1 | 39.31 ± 11.12 | 0.057 |
| LVEDD (mm) | 52.37 ± 10.25 | 54.04± 8.59 | 48.97 ± 8.5 | 54.37 ± 9.39 | 0.563 |
| LAD (mm) | 42.46 ± 7.14 | 47.57 ± 7.69 | 45.89 ± 8.57 | 48.72 ± 7.18 | <0.001 |
| LVEF (%) | 53.11 ± 12.77 | 54.83 ± 13.49 | 54.1 ± 12.3 | 52 ± 12.93 | 0.362 |
| TAPSE (mm) | <0.001 | ||||
| Diastolic dysfunction | 6.15% | 9.64% | 8.63% | 57.39% | <0.001 |
| Postoperative outcome | |||||
| In-Hospital Mortality | 9.23 | 6.02% | 18.56% | 41.47% | <0.001 |
| SIRS | 6.15% | 7.41% | 11.79% | 28.95% | <0.001 |
| Low output syndrome | 3.08% | 2.47% | 3.59% | 11.4% | 0.009 |
| Pleural effusion | 10.94% | 18.52% | 19.49% | 29.82% | 0.003 |
| CIP/CIM | 0% | 1.23% | 0.51% | 7.02% | 0.003 |
| Acute kidney failure | 12.5% | 9.88% | 25.13% | 40.71% | <0.001 |
| Atrial fibrillation | 16.92% | 7.41% | 9.28% | 21.93% | 0.164 |
| Pneumonia | 1.54% | 2.47% | 7.69% | 14.04% | <0.001 |
| Respiratory insufficiency | 7.81% | 12.35% | 12.31% | 28.95% | <0.001 |
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2023 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Ostovar, R.; Schröter, F.; Hartrumpf, M.; Kuehnel, R.-U.; Bruch, D.; Motazedian, F.; Albes, J.M. Mitral Valve Repair in Advanced Age Groups: Does Cardiac Age Differ from Chronological Age? J. Clin. Med. 2023, 12, 3790. https://doi.org/10.3390/jcm12113790
Ostovar R, Schröter F, Hartrumpf M, Kuehnel R-U, Bruch D, Motazedian F, Albes JM. Mitral Valve Repair in Advanced Age Groups: Does Cardiac Age Differ from Chronological Age? Journal of Clinical Medicine. 2023; 12(11):3790. https://doi.org/10.3390/jcm12113790
Chicago/Turabian StyleOstovar, Roya, Filip Schröter, Martin Hartrumpf, Ralf-Uwe Kuehnel, Dunja Bruch, Farnoosh Motazedian, and Johannes Maximilian Albes. 2023. "Mitral Valve Repair in Advanced Age Groups: Does Cardiac Age Differ from Chronological Age?" Journal of Clinical Medicine 12, no. 11: 3790. https://doi.org/10.3390/jcm12113790
APA StyleOstovar, R., Schröter, F., Hartrumpf, M., Kuehnel, R.-U., Bruch, D., Motazedian, F., & Albes, J. M. (2023). Mitral Valve Repair in Advanced Age Groups: Does Cardiac Age Differ from Chronological Age? Journal of Clinical Medicine, 12(11), 3790. https://doi.org/10.3390/jcm12113790







