Intracranial Haemorrhage in Haemophilia Patients Is Still an Open Issue: The Final Results of the Italian EMO.REC Registry
Abstract
:1. Background
2. Aim
3. Patients and Methods
3.1. Patients
3.2. Methods
3.3. Statistical Analysis
4. Results
Prophylaxis
5. Discussion
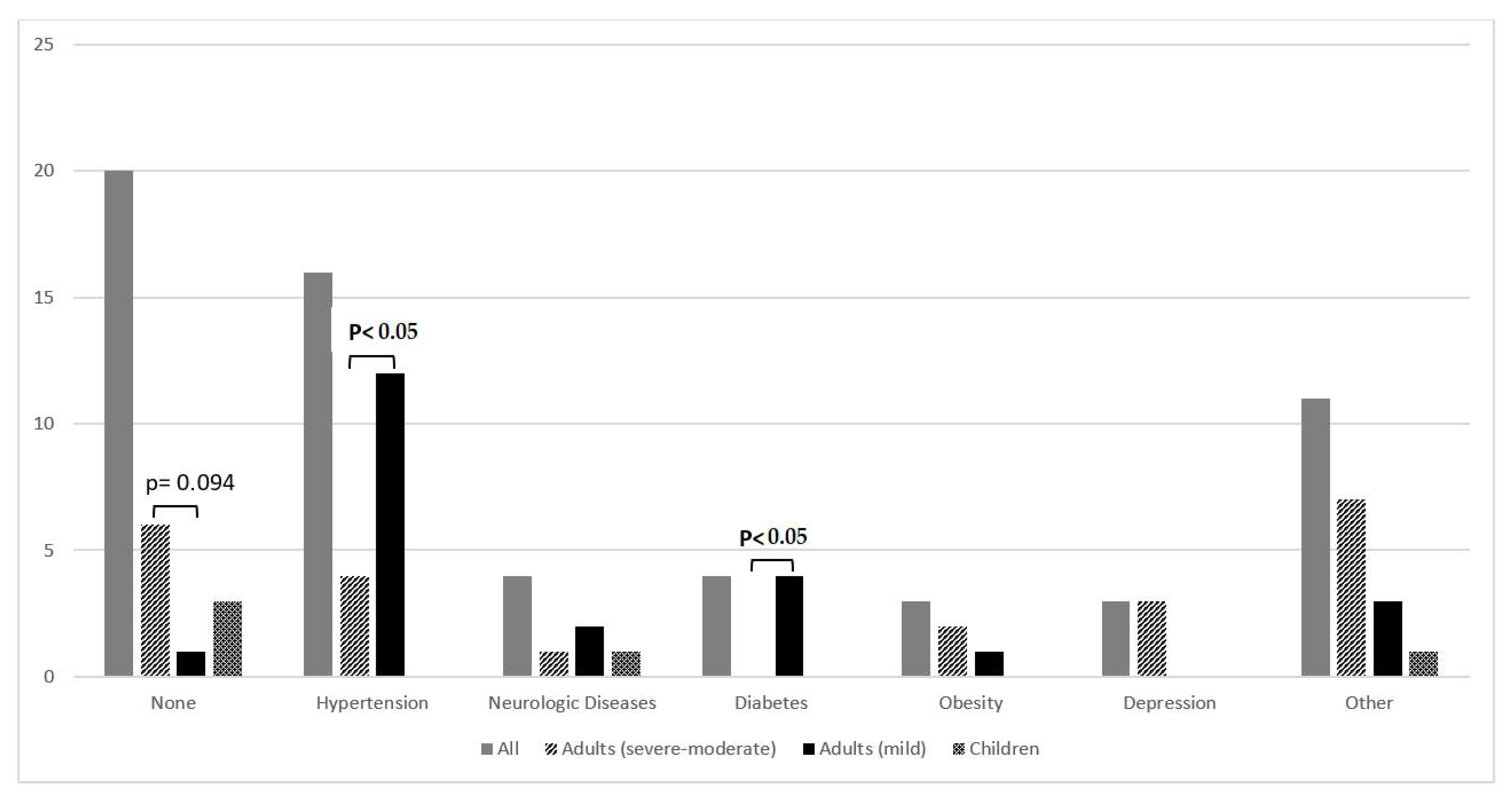
- Start prophylaxis (and carefully monitor adequate adherence) in all patients affected by severe hemophilia but also in those with mild forms in whom risk factors (hypertension in particular) are effectively controlled.
- Check the risk factors and treat the comorbidities of the patient during follow-up examination.
- In newborns with severe forms, start a prophylaxis treatment as soon as possible.
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Conflicts of Interest
References
- Zwagemaker, A.F.; Gouw, S.C.; Jansen, J.S.; Vuong, C.; Coppens, M.; Hu, Q.; Feng, X.; Kim, S.K.; van der Bom, J.G.; Fijnvandraat, K. Incidence and mortality rates of intracranial hemorrahge in hemophilia: A systematic review and meta-analysis. Blood 2021, 138, 2853–2873. [Google Scholar] [CrossRef] [PubMed]
- Stieltjes, N.; Calvez, T.; DeMiguel, V.; Torchet, M.F.; Briquel, M.E.; Fressinaud, E.; Claeyssens, S.; Coatmelec, B.; Chambost, H.; The French ICH Study Group. Intracranial haemorrhage in French haemophilia patients (1991–2001): Clinical presentation, management and prognosis factors for death. Haemophilia 2005, 11, 452–458. [Google Scholar] [CrossRef] [PubMed]
- Zanon, E.; Iorio, A.; Rocino, A.; Artoni, A.; Santoro, R.; Tagliaferri, A.; Coppola, A.; Castaman, G.; Mannucci, P.M.; Italian Association of Hemophilia Centers. Intracranial haemorrhage in the Italian population of haemophilia patients with and without inhibitors. Haemophilia 2012, 18, 39–445. [Google Scholar] [CrossRef] [PubMed]
- Ljung, R.C. Intracranial haemorrhage in haemophilia A and B. Br. J. Haematol. 2008, 140, 378–384. [Google Scholar] [CrossRef] [PubMed]
- Zanon, E.; Pasca, S. Intracranial haemorrhage in children and adults with haemophilia A and B: A literature review of the last 20 years. Blood Transfus. 2019, 17, 378–384. [Google Scholar]
- Chalmers, E.A.; Alamelu, J.; Collins, P.W.; Mathias, M.; Payne, J.; Richards, M.; Tunstall, O.; Williams, M.; Palmer, B.; Mumford, A.; et al. Intracranial haemorrhage in children with inherited bleeding disorders in the UK 2003–2015: A national cohort study. Haemophilia 2018, 24, 641–647. [Google Scholar] [CrossRef]
- Davies, J.; Kadir, R.A. Mode of delivery and cranial bleeding in newborns with haemophilia: A systematic review and meta-analysis of the literature. Haemophilia 2016, 22, 32–38. [Google Scholar] [CrossRef]
- Nazir, H.F.; Al Lawati, T.; Beshlawi, I.; AlSharidah, S.; Elshinawy, M.; Alkasim, F.; Khanani, M.F.; Tarawa, A.; Al Subhi, T.; Alrawas, A.; et al. Mode of delivery and risk of intracranial haemorrhage in newborns with severe haemophilia A: A multicentre study in Gulf region. Haemophilia 2016, 22, e134–e138. [Google Scholar] [CrossRef]
- Witmer, C.; Presley, R.; Kulkarni, R.; Soucie, J.M.; Manno, C.S.; Raffini, L. Associations between intracranial haemorrhage and prescribed prophylaxis in a large cohort of haemophilia patients in the United States. Br. J. Haematol. 2011, 152, 211–216. [Google Scholar] [CrossRef]
- Andersson, N.G.; Auerswald, G.; Barnes, C.; Carcao, M.; Dunn, A.; Fijnvandraat, K.; Hoffmann, M.; Kavakli, K.; Kenet, G.; Kobelt, R.; et al. Intracranial haemorrhage in children and adolescents with severe haemophilia A or B—the impact of prophylactic treatment. Br. J. Haematol. 2017, 179, 298–307. [Google Scholar] [CrossRef]
- Loomans, J.I.; Eckhardt, C.L.; Reitter-Pfoertner, S.E.; Holmström, M.; Van Gorkom, B.L.; Leebeek, F.W.; Santoro, C.; Haya, S.; Meijer, K.; Nijziel, M.R.; et al. Mortality caused by intracranial bleeding in non-severe hemophilia A patients. J. Thromb. Haemost. 2017, 15, 1115–1122. [Google Scholar] [CrossRef] [PubMed]
- Nuss, R.; Soucie, J.M.; Evatt, B. Hemophilia Surveillance System Project Investigators Changes in the occurrence of and risk factors for hemophilia-associated intracranial hemorrhage. Am. J. Hematol. 2001, 68, 37–42. [Google Scholar] [CrossRef] [PubMed]
- Berger, K.; Schopohl, D.; Lowe, G.; Holme, P.A.; Tait, R.; Combescure, C.; Rauchensteiner, S.; Klamroth, R. How to compare cardiovascular disease and risk factors in elderly patients with hemophilia with the general population. Haemophilia 2016, 22, e406–e416. [Google Scholar] [CrossRef] [PubMed]
- White, G.C., II; Rosendaal, F.; Aledort, L.M.; Lusher, J.M.; Rothschild, C.; Ingerslev, J. Factor VIII and Factor IX Subcommittee Definitions in hemophilia. Recommendation of the scientific subcommittee on factor VIII and factor IX of the scientific and standardization committee of the International Society on Thrombosis and Haemostasis. Thromb. Haemost. 2001, 85, 560. [Google Scholar]
- Haque, Q.; Abuduaini, Y.; Li, H.; Wen, J.; Wu, X.; Feng, X. Intracranial hemorrhage in children with inherited bbleeding disorders: A single center study in China. J. Pediatric Hematol. Oncol. 2019, 41, 207–209. [Google Scholar] [CrossRef]
- Hassan, S.; Monahan, R.C.; Mauser-Bunschoten, E.P.; van Vulpen, L.F.D.; Eikenboom, J.; Beckers, E.A.M.; Hooimeijer, L.; Paula, F.Y.; Nieuwenhuizen, L.; Coppens, M.; et al. Mortality, life expectancy, and causes of death of person with hemophilia in the Netherlands 2001–2018. J. Thromb. Haemost. 2020, 19, 645–653. [Google Scholar] [CrossRef]
- Nilsson, O.G.; Lindgren, A.; Ståhl, N.; Brandt, L.; Säveland, H. Incidence of intracerebral and subarachnoid haemorrhage in souther Sweden. J. Neurol. Neurosurg. Psychiatry 2000, 69, 601–607. [Google Scholar] [CrossRef] [Green Version]
- Kulkarni, R.; Presley, R.J.; Lusher, J.M.; Shapiro, A.D.; Gill, J.C.; Manco-Johnson, M.; Koerper, M.A.; Abshire, T.C.; DiMichele, D.; Hoots, W.K.; et al. Complications of haemophilia in babies (first two years of life): A report from the Center for Disease Control and Prevention Universal Data collection System. Haemophilia 2017, 23, 207–214. [Google Scholar] [CrossRef]
- Bladen, M.; Main, E.; Khair, K.; Hubert, N.; Koutoumanou, E.; Liesner, R. The incidence, risk and functional outcomes of intracranial haemorrhage in children with inherited bleeding disorders at one haemophilia center. Haemophilia 2016, 22, 556–563. [Google Scholar] [CrossRef]
- Lövdahl, S.; Henriksson, K.M.; Baghaei, F.; Holmström, M.; Berntorp, E.; Astermark, J. Hypertension and cardiovascular disease in Swedish person with haemophilia-A longitudinal registry study. Thromb. Res. 2019, 181, 106–111. [Google Scholar] [CrossRef]
- Srivastava, A.; Santagostino, E.; Dougall, A.; Kitchen, S.; Sutherland, M.; Pipe, S.W.; Carcao, M.; Mahlangu, J.; Ragni, M.V.; Windyga, J.; et al. WFH Guidelines for the Management of Hemophilia, 3rd edition. Haemophilia 2020, 26, 1–158. [Google Scholar] [CrossRef] [PubMed]
| All n (%) | Adults n (%) | Children n (%) | |
|---|---|---|---|
| Number of total patients | 46 (100.0) | 31 (100.0) | 15 (100.0) |
| Type of haemophilia: | |||
| A | 39 (84.8) | 26 (83.9) | 13 (86.7) |
| B | 7 (15.2) | 5 (16.1) | 2 (13.3) |
| Degree of haemophilia: | |||
| Mild | 14 (30.4) | 14 (45.2) | |
| Moderate | 4 (8.7) | 4 (12.9) | |
| Severe | 28 (60.9) | 13 (41.9) | 15 (100.0) |
| Family history: | |||
| Family | 19 (41.3) | 14 (45.2) | 5 (33.4) |
| Sporadic | 27 (58.7) | 17 (54.8) | 10 (66.6) |
| Inhibitor: | |||
| Yes | 5 (10.9) | 2 (6.5) | 3 (20.0) |
| No | 41 (89.1) | 29 (95.5) | 12 (80.0) |
| Viral Infections: | |||
| None | 22 (47.8) | 7 (22.6) | 15 (100.0) |
| HCV | 23 (50.0) | 23 (74.2) | |
| HIV | 3 (6.5) | 3 (9.7) | |
| HBV | 2 (4.3) | 2 (6.5) | |
| Other | 1 (2.2) | 1 (3.2) | |
| Trauma: | |||
| No | 32 (69.6) | 25 (80.6) | 7 (46.7) |
| Yes | 12 (26.1) | 6 (19.4) | 6 (40.0) |
| Peri-Partum | 2 (4.3) | 2 (13.3) | |
| Smoke: | |||
| Yes | 10 (32.3) | 10 (32.3) | NA |
| No | 17 (58.8) | 17 (58.8) | NA |
| Not reported | 4 (12.9) | 4 (12.9) | NA |
| Alcohol intake: | |||
| No | 11 (35.5) | 11 (35.5) | NA |
| Usually | 13 (41.9) | 13 (41.9) | NA |
| Rarely | 3 (9.7) | 3 (9.7) | NA |
| Not reported | 4 (12.9) | 4 (12.9 | NA |
| * Symptoms at diagnosis: | |||
| None | 13 (28.2) | 11 (35.5) | 2 (13.3) |
| Headache | 12 (26.0) | 9 (29.0) | 3 (20.0) |
| Epilepsy | 4 (8.7) | 1 (3.2) | 3 (20.0) |
| Motor dysfunction | 4 (8.7) | 3 (9.7) | 1 (6.7) |
| Syncope | 1 (2.2) | 1 (3.2) | |
| Asthenia | 5 (10.9) | 4 (12.9) | 1 (6.7) |
| Drowsiness | 7 (15.2) | 4 (12.9) | 3 (20.0) |
| Coma | 7 (15.2) | 5 (16.1) | 5 (33.4) |
| Vomiting | 2 (4.3) | 1 (3.2) | 1 (6.7) |
| Other | 3 (6.5) | 3 (9.7) | |
| * Site of ICH: | |||
| Intraparenchymal | 21 (45.7) | 16 (51.6) | 5 (33.4) |
| Subdural | 8 (17.4) | 4 (12.9) | 4 (26.7) |
| Subarachnoid | 9 (19.6) | 6 (19.4) | 3 (20.0) |
| Intraventricular | 2 (4.3) | 2 (13.3) | |
| Not specified | 11 (23.9) | 8 (25.8) | 3 (20.0) |
| Sequelae: | |||
| All | 13 (28.2) | 8 (25.8) | 5 (33.4) |
| Neurological | 5 (10.9) | 2 (6.5) | 3 (20.0) |
| Recurrences | 2 (4.3) | 1 (3.2) | 1 (6.7) |
| Deaths | 14 (30.4) | 13 (41.9) | 1 (6.7) |
| ICH n (%) | Years at Risk | Rate (×1000/Person Years) | 95% CI | |
|---|---|---|---|---|
| Whole population | 46 (100.0) | 127,923.5 | 0.360 | 0.269–0.480 |
| 0–2 years | 12 (26.1) | 6139.0 | 1.955 | 1.110–3.442 |
| 3–16 years | 4 (8.7) | 46,754.0 | 0.086 | 0.032–0.228 |
| 17–40 years | 7 (15.2) | 95,018.5 | 0.074 | 0.035–0.155 |
| 41–59 years | 12 (26.1) | 85,585.0 | 0.140 | 0.080–0.247 |
| ≥60 years | 11 (23.9) | 42,348.9 | 0.260 | 0.144–0.469 |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2022 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Zanon, E.; Pasca, S.; Demartis, F.; Tagliaferri, A.; Santoro, C.; Cantori, I.; Molinari, A.C.; Biasoli, C.; Coppola, A.; Luciani, M.; et al. Intracranial Haemorrhage in Haemophilia Patients Is Still an Open Issue: The Final Results of the Italian EMO.REC Registry. J. Clin. Med. 2022, 11, 1969. https://doi.org/10.3390/jcm11071969
Zanon E, Pasca S, Demartis F, Tagliaferri A, Santoro C, Cantori I, Molinari AC, Biasoli C, Coppola A, Luciani M, et al. Intracranial Haemorrhage in Haemophilia Patients Is Still an Open Issue: The Final Results of the Italian EMO.REC Registry. Journal of Clinical Medicine. 2022; 11(7):1969. https://doi.org/10.3390/jcm11071969
Chicago/Turabian StyleZanon, Ezio, Samantha Pasca, Francesco Demartis, Annarita Tagliaferri, Cristina Santoro, Isabella Cantori, Angelo Claudio Molinari, Chiara Biasoli, Antonio Coppola, Matteo Luciani, and et al. 2022. "Intracranial Haemorrhage in Haemophilia Patients Is Still an Open Issue: The Final Results of the Italian EMO.REC Registry" Journal of Clinical Medicine 11, no. 7: 1969. https://doi.org/10.3390/jcm11071969
APA StyleZanon, E., Pasca, S., Demartis, F., Tagliaferri, A., Santoro, C., Cantori, I., Molinari, A. C., Biasoli, C., Coppola, A., Luciani, M., Sottilotta, G., Ricca, I., Pollio, B., Borchiellini, A., Tosetto, A., Peyvandi, F., Frigo, A. C., & Simioni, P. (2022). Intracranial Haemorrhage in Haemophilia Patients Is Still an Open Issue: The Final Results of the Italian EMO.REC Registry. Journal of Clinical Medicine, 11(7), 1969. https://doi.org/10.3390/jcm11071969








