COVID-19-Associated Encephalopathy—Case Series and Clinical Considerations
Abstract
:1. Introduction
2. Clinical Cases
2.1. Patient 1
2.2. Patient 2
2.3. Patient 3
3. Discussion
4. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Acknowledgments
Conflicts of Interest
Abbreviations
References
- Prabhakar, H.; Mahajan, C.; Kapoor, I. COVID-19 and Neuroinvasion. Anesth. Analg. 2020, 131, e91–e92. [Google Scholar] [CrossRef]
- Machhi, J.; Herskovitz, J.; Senan, A.M.; Dutta, D.; Nath, B.; Oleynikov, M.D.; Blomberg, W.R.; Meigs, D.D.; Hasan, M.; Patel, M.; et al. The Natural History, Pathobiology, and Clinical Manifestations of SARS-CoV-2 Infections. J. Neuroimmune Pharmacol. 2020, 15, 359–386. [Google Scholar] [CrossRef]
- Marshall, M. COVID and the brain: Researchers zero in on how damage occurs. Nature 2021, 595, 484–485. [Google Scholar] [CrossRef]
- ACE2 Cell Biology, Regulation, and Physiological Functions|Elsevier Enhanced Reader. Available online: https://reader.elsevier.com/reader/sd/pii/B9780128013649000250?token=EBFA81B22EA489EAFF1D5C3B83263F6060E65499A574EDF137163D6D3DF0719EA3B9B72F992F27F26723B0024BBA38A7&originRegion=eu-west-1&originCreation=20211001175004 (accessed on 1 October 2021).
- Murça, T.M.; Moraes, P.L.; Capuruço, C.A.; Santos, S.H.; Melo, M.B.; Santos, R.A.; Shenoy, V.; Katovich, M.J.; Raizada, M.K.; Ferreira, A.J. Oral administration of an angiotensin-converting enzyme 2 activator ameliorates diabetes-induced cardiac dysfunction. Regul. Pept. 2012, 177, 107–115. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Nuzzo, D.; Picone, P. Potential neurological effects of severe COVID-19 infection. Neurosci. Res. 2020, 158, 1–5. [Google Scholar] [CrossRef] [PubMed]
- Verma, K.; Amitabh; Prasad, D.N.; Kumar, B.; Kohli, E. Brain and COVID-19 Crosstalk: Pathophysiological and Psychological Manifestations. ACS Chem. Neurosci. 2020, 11, 3194–3203. [Google Scholar] [CrossRef]
- Kanwar, D.; Baig, A.M.; Wasay, M. Neurological manifestations of COVID-19. J. Pak. Med Assoc. 2020, 3, S101–S103. [Google Scholar] [CrossRef]
- Correia, A.O.; Feitosa, P.W.G.; Moreira, J.L.D.S.; Nogueira, S.; Átila, R.; Fonseca, R.B.; Nobre, M.E.P. Neurological manifestations of COVID-19 and other coronaviruses: A systematic review. Neurol. Psychiatry Brain Res. 2020, 37, 27–32. [Google Scholar] [CrossRef]
- Berger, J.R. COVID-19 and the nervous system. J. Neurovirol. 2020, 26, 143–148. [Google Scholar] [CrossRef]
- Meppiel, E.; Peiffer-Smadja, N.; Maury, A.; Bekri, I.; Delorme, C.; Desestret, V.; Gorza, L.; Hautecloque-Raysz, G.; Landre, S.; Lannuzel, A.; et al. Neurologic manifestations associated with COVID-19: A multicentre registry. Clin. Microbiol. Infect. 2021, 27, 458–466. [Google Scholar] [CrossRef] [PubMed]
- Brouwer, M.C.; Ascione, T.; Pagliano, P. Neurologic aspects of covid-19: A concise review. Infez. Med. 2020, 28, 42–45. [Google Scholar]
- Ellul, M.A.; Benjamin, L.; Singh, B.; Lant, S.; Michael, B.D.; Easton, A.; Kneen, R.; Defres, S.; Sejvar, J.; Solomon, T. Neurological associations of COVID-19. Lancet Neurol. 2020, 19, 767–783. [Google Scholar] [CrossRef]
- Maury, A.; Lyoubi, A.; Peiffer-Smadja, N.; de Broucker, T.; Meppiel, E. Neurological manifestations associated with SARS-CoV-2 and other coronaviruses: A narrative review for clinicians. Rev. Neurol. 2021, 177, 51–64. [Google Scholar] [CrossRef]
- Ziemele, D.; Ķauķe, G.; Skrējāne, K.; Jaunozoliņa, L.; Karelis, G. A fatal case of COVID-19-associated acute necrotizing encephalopathy. Eur. J. Neurol. 2021, 28, 3870–3872. [Google Scholar] [CrossRef] [PubMed]
- Nalbantoglu, M.; Mestanzade, T.; Altunrende, B.; Orken, D.N. COVID-19 associated severe encephalopathy. Eur. J. Neurol. 2021, 93, 689. [Google Scholar] [CrossRef]
- Ciolac, D.; Crivorucica, I.; Zota, E.; Gorincioi, N.; Efremova, D.; Manea, D.; Crivorucica, V.; Ciocanu, M.; Groppa, S.A. Extensive cerebellar involvement and cognitive impairment in COVID-19-associated acute necrotizing encephalopathy. Ther. Adv. Neurol. Disord. 2021, 14, 1756286420985175. [Google Scholar] [CrossRef]
- Cuthbert, S.C.; Goodheart, G.J., Jr. On the reliability and validity of manual muscle testing: A literature review. Chiropr. Osteopat. 2007, 15, 4. [Google Scholar] [CrossRef] [Green Version]
- Fig. 11.5, [Fazekas Scale for White Matter].—Diseases of the Brain, Head and Neck, Spine 2020–2023—NCBI Bookshelf. Available online: https://www.ncbi.nlm.nih.gov/books/NBK554327/figure/ch11.Fig5/?report=objectonly (accessed on 6 January 2022).
- COVID-19: Neurologic Complications and Management of Neurologic Conditions—UpToDate. Available online: https://www.uptodate.com/contents/covid-19-neurologic-complications-and-management-of-neurologic-conditions#H431248232 (accessed on 6 January 2022).
- Bernard-Valnet, R.; Perriot, S.; Canales, M.; Pizzarotti, B.; Caranzano, L.; Castro-Jiménez, M.; Epiney, J.-B.; Vijiala, S.; Salvioni-Chiabotti, P.; Anichini, A.; et al. Encephalopathies Associated With Severe COVID-19 Present Neurovascular Unit Alterations Without Evidence for Strong Neuroinflammation. Neurol.-Neuroimmunol. Neuroinflammation 2021, 8, e1029. [Google Scholar] [CrossRef]
- Yan, R.; Zhang, Y.; Li, Y.; Xia, L.; Guo, Y.; Zhou, Q. Structural basis for the recognition of SARS-CoV-2 by full-length human ACE2. Science 2020, 367, 1444–1448. [Google Scholar] [CrossRef] [Green Version]
- Yalcin, H.C.; Sukumaran, V.; Al-Ruweidi, M.K.A.A.; Shurbaji, S. Do Changes in ACE-2 Expression Affect SARS-CoV-2 Virulence and Related Complications: A Closer Look into Membrane-Bound and Soluble Forms. Int. J. Mol. Sci. 2021, 22, 6703. [Google Scholar] [CrossRef]
- Alenina, N.; Bader, M. ACE2 in Brain Physiology and Pathophysiology: Evidence from Transgenic Animal Models. Neurochem. Res. 2019, 44, 1323–1329. [Google Scholar] [CrossRef]
- Hernández, V.S.; Zetter, M.A.; Guerra, E.C.; Hernández-Araiza, I.; Karuzin, N.; Hernández-Pérez, O.R.; Eiden, L.E.; Zhang, L. ACE2 expression in rat brain: Implications for COVID-19 associated neurological manifestations. Exp. Neurol. 2021, 345, 113837. [Google Scholar] [CrossRef] [PubMed]
- Yachou, Y.; El Idrissi, A.; Belapasov, V.; Benali, S.A. Neuroinvasion, neurotropic, and neuroinflammatory events of SARS-CoV-2: Understanding the neurological manifestations in COVID-19 patients. Neurol. Sci. 2020, 41, 2657–2669. [Google Scholar] [CrossRef]
- Morgello, S. Coronaviruses and the central nervous system. J. Neurovirol. 2020, 26, 459–473. [Google Scholar] [CrossRef]
- Valeri, A.; Chiricosta, L.; Calcaterra, V.; Biasin, M.; Cappelletti, G.; Carelli, S.; Zuccotti, G.V.; Bramanti, P.; Pelizzo, G.; Mazzon, E.; et al. Transcriptomic analysis of hcn-2 cells suggests connection among oxidative stress, senescence, and neuron death after sars-cov-2 infection. Cells 2021, 10, 2189. [Google Scholar] [CrossRef] [PubMed]
- Johansson, A.; Mohamed, M.S.; Moulin, T.C.; Schiöth, H.B. Neurological manifestations of COVID-19: A comprehensive literature review and discussion of mechanisms. J. Neuroimmunol. 2021, 358, 577658. [Google Scholar] [CrossRef] [PubMed]
- Ramani, A.; Müller, L.; Ostermann, P.N.; Gabriel, E.; Abida-Islam, P.; Müller-Schiffmann, A.; Mariappan, A.; Goureau, O.; Gruell, H.; Walker, A.; et al. SARS -CoV-2 targets neurons of 3D human brain organoids. EMBO J. 2020, 39, e106230. [Google Scholar] [CrossRef]
- Panciani, P.P.; Saraceno, G.; Zanin, L.; Renisi, G.; Signorini, L.; Battaglia, L.; Fontanella, M. SARS-CoV-2: “Three-steps” infection model and CSF diagnostic implication. Brain Behav. Immun. 2020, 87, 128–129. [Google Scholar] [CrossRef]
- Franke, C.; Ferse, C.; Kreye, J.; Reincke, S.M.; Sanchez-Sendin, E.; Rocco, A.; Steinbrenner, M.; Angermair, S.; Treskatsch, S.; Zickler, D.; et al. High frequency of cerebrospinal fluid autoantibodies in COVID-19 patients with neurological symptoms. Brain Behav. Immun. 2021, 93, 415–419. [Google Scholar] [CrossRef]
- Ehrenfeld, M.; Tincani, A.; Andreoli, L.; Cattalini, M.; Greenbaum, A.; Kanduc, D.; Alijotas-Reig, J.; Zinserling, V.; Semenova, N.; Amital, H.; et al. Covid-19 and autoimmunity. Autoimmun. Rev. 2020, 19, 102597. [Google Scholar] [CrossRef]
- Parsons, T.; Banks, S.; Bae, C.; Gelber, J.; Alahmadi, H.; Tichauer, M. COVID-19-associated acute disseminated encephalomyelitis (ADEM). J. Neurol. 2020, 267, 2799–2802. [Google Scholar] [CrossRef] [PubMed]
- Guilmot, A.; Slootjes, S.M.; Sellimi, A.; Bronchain, M.; Hanseeuw, B.; Belkhir, L.; Yombi, J.C.; De Greef, J.; Pothen, L.; Yildiz, H.; et al. Immune-mediated neurological syndromes in SARS-CoV-2-infected patients. J. Neurol. 2021, 268, 751–757. [Google Scholar] [CrossRef] [PubMed]
- Mulder, J.; Lindqvist, I.; Rasmusson, A.J.; Husén, E.; Rönnelid, J.; Kumlien, E.; Rostami, E.; Virhammar, J.; Cunningham, J.L. Indirect immunofluorescence for detecting anti-neuronal autoimmunity in CSF after COVID-19—Possibilities and pitfalls. Brain Behav. Immun. 2021, 94, 473–474. [Google Scholar] [CrossRef] [PubMed]
- Miller, E.H.; Namale, V.S.; Kim, C.; Dugue, R.; Waldrop, G.; Ciryam, P.; Chong, A.M.; Zucker, J.; Miller, E.C.; Bain, J.M.; et al. Cerebrospinal Analysis in Patients With COVID-19. Open Forum Infect. Dis. 2020, 7, ofaa501. [Google Scholar] [CrossRef]
- Edén, A.; Simrén, J.; Price, R.W.; Zetterberg, H.; Gisslén, M. Neurochemical biomarkers to study CNS effects of COVID-19: A narrative review and synthesis. J. Neurochem. 2021, 159, 61–77. [Google Scholar] [CrossRef]
- Lewis, A.; Frontera, J.; Placantonakis, D.G.; Galetta, S.; Balcer, L.; Melmed, K.R. Cerebrospinal Fluid from COVID-19 Patients with Olfactory/Gustatory Dysfunction: A Review. Clin. Neurol. Neurosurg. 2021, 207, 106760. [Google Scholar] [CrossRef]
- Neumann, B.; Schmidbauer, M.L.; Dimitriadis, K.; Otto, S.; Knier, B.; Niesen, W.-D.; Hosp, J.A.; Günther, A.; Lindemann, S.; Nagy, G.; et al. Cerebrospinal fluid findings in COVID-19 patients with neurological symptoms. J. Neurol. Sci. 2020, 418, 117090. [Google Scholar] [CrossRef]
- Moghimi, M.; Moghtader, A.; Jozpanahi, M.; Khodadadi, K.; Jafarzade, M.; Abbaspour, Z. Correlation between CSF biomarkers and COVID-19 meningoencephalitis: A case series. Respir. Med. Case Rep. 2021, 32, 101335. [Google Scholar] [CrossRef]
- Edén, A.; Kanberg, N.; Gostner, J.; Fuchs, D.; Hagberg, L.; Andersson, L.-M.; Lindh, M.; Price, R.W.; Zetterberg, H.; Gisslén, M. CSF biomarkers in patients with COVID-19 and neurological symptoms. Neurology 2021, 96, e294–e300. [Google Scholar] [CrossRef]
- Wang, M.; Li, T.; Qiao, F.; Wang, L.; Li, C.; Gong, Y. Coronavirus disease 2019 associated with aggressive neurological and mental abnormalities confirmed based on cerebrospinal fluid antibodies. Medicine 2020, 99, e21428. [Google Scholar] [CrossRef]
- Ladopoulos, T.; Zand, R.; Shahjouei, S.; Chang, J.J.; Motte, J.; James, J.C.; Katsanos, A.H.; Kerro, A.; Farahmand, G.; Far, A.V.; et al. COVID-19: Neuroimaging Features of a Pandemic. J. Neuroimaging 2021, 31, 228–243. [Google Scholar] [CrossRef]
- Kandemirli, S.G.; Dogan, L.; Sarikaya, Z.T.; Kara, S.; Akinci, C.; Kaya, D.; Kaya, Y.; Yildirim, D.; Tuzuner, F.; Yildirim, M.S.; et al. Brain MRI Findings in Patients in the Intensive Care Unit with COVID-19 Infection. Radiology 2020, 297, E232–E235. [Google Scholar] [CrossRef] [PubMed]
- Hernández-Fernández, F.; Sandoval Valencia, H.; Barbella-Aponte, R.A.; Collado-Jiménez, R.; Ayo-Martín, Ó.; Barrena, C.; Molina-Nuevo, J.D.; García-García, J.; Lozano-Setién, E.; Alcahut-Rodriguez, C.; et al. Cerebrovascular disease in patients with COVID-19: Neuroimaging, histological and clinical description. Brain A J. Neurol. 2020, 143, 3089–3103. [Google Scholar] [CrossRef] [PubMed]
- Gulko, E.; Oleksk, M.; Gomes, W.; Ali, S.; Mehta, H.; Overby, P.; Al-Mufti, F.; Rozenshtein, A. MRI Brain Findings in 126 Patients with COVID-19: Initial Observations from a Descriptive Literature Review. Am. J. Neuroradiol. 2020, 41, 2199–2203. [Google Scholar] [CrossRef] [PubMed]
- Katal, S.; Balakrishnan, S.; Gholamrezanezhad, A. Neuroimaging and neurologic findings in COVID-19 and other coronavirus infections: A systematic review in 116 patients. J. Neuroradiol. 2021, 48, 43–50. [Google Scholar] [CrossRef] [PubMed]
- Fotuhi, M.; Mian, A.; Meysami, S.; Raji, C.A. Neurobiology of COVID-19. J. Alzheimer’s Dis. 2020, 76, 3–19. [Google Scholar] [CrossRef] [PubMed]
- Kremer, S.; Lersy, F.; Anheim, M.; Merdji, H.; Schenck, M.; Oesterlé, H.; Bolognini, F.; Messie, J.; Khalil, A.; Gaudemer, A.; et al. Neurologic and neuroimaging findings in patients with COVID-19. Neurology 2020, 95, e1868–e1882. [Google Scholar] [CrossRef] [PubMed]
- Picod, A.; Dinkelacker, V.; Savatovsky, J.; Trouiller, P.; Guéguen, A.; Engrand, N. SARS-CoV-2-associated encephalitis: Arguments for a post-infectious mechanism. Crit. Care 2020, 24, 658. [Google Scholar] [CrossRef]
- Lv, P.; Peng, F.; Zhang, Y.; Li, N.; Sun, L.; Wang, Y.; Hou, P.; Huang, T.; Wang, X.; Zhang, L. COVID-19-associated meningoencephalitis: A care report and literature review. Exp. Ther. Med. 2021, 21, 362. [Google Scholar] [CrossRef] [PubMed]
- Freire-Álvarez, E.; Guillén, L.; Lambert, K.; Baidez, A.; García-Quesada, M.; Andreo, M.; Alom, J.; Masiá, M.; Gutiérrez, F. COVID-19-associated encephalitis successfully treated with combination therapy. Clin. Infect. Pract. 2020, 7, 100053. [Google Scholar] [CrossRef]
- Efe, I.E.; Aydin, O.U.; Alabulut, A.; Çelik, Ö.; Aydin, K. COVID-19−Associated Encephalitis Mimicking Glial Tumor. World Neurosurg. 2020, 140, 46–48. [Google Scholar] [CrossRef] [PubMed]
- Mullaguri, N.; Sivakumar, S.; Battineni, A.; Anand, S.; Vanderwerf, J. COVID-19 Related Acute Hemorrhagic Necrotizing Encephalitis: A Report of Two Cases and Literature Review. Cureus 2021, 13, e14236. [Google Scholar] [CrossRef] [PubMed]
- Moriguchi, T.; Harii, N.; Goto, J.; Harada, D.; Sugawara, H.; Takamino, J.; Ueno, M.; Sakata, H.; Kondo, K.; Myose, N.; et al. A first case of meningitis/encephalitis associated with SARS-Coronavirus-2. Int. J. Infect. Dis. 2020, 94, 55–58. [Google Scholar] [CrossRef] [PubMed]
- Fukushima, E.F.A.; Nasser, A.; Bhargava, A.; Moudgil, S. Post-infectious focal encephalitis due to COVID-19. Germs 2021, 11, 111–115. [Google Scholar] [CrossRef] [PubMed]
- Garg, R.K.; Paliwal, V.K.; Gupta, A. Encephalopathy in patients with COVID-19: A review. J. Med. Virol. 2021, 93, 206–222. [Google Scholar] [CrossRef]
- Umapathi, T.; Quek, W.M.J.; Yen, J.M.; Khin, H.S.W.; Mah, Y.Y.; Chan, C.Y.J.; Ling, L.M.; Yu, W.-Y. Encephalopathy in COVID-19 patients; viral, parainfectious, or both? eNeurologicalSci 2020, 21, 100275. [Google Scholar] [CrossRef] [PubMed]
- Abildúa, M.A.; Atienza, S.; Monteiro, G.C.; Aguirre, M.E.; Aguayo, L.I.; Álvarez, E.F.; García-Azorín, D.; Montesinos, I.G.-O.; Lezama, L.L.; Pérez, M.N.; et al. Encefalopatías y encefalitis durante la infección aguda por SARS-CoV2. Registro de la Sociedad Española de Neurología SEN COVID-19. Neurología 2021, 36, 127–134. [Google Scholar] [CrossRef]
- Lazraq, M.; Benhamza, S.; Saadaoui, S.; Hayar, S.; Louardi, M.; Moujahid, H.; Bensaid, A.; Miloudi, Y.; El Harrar, N. Encephalopathy and COVID-19: A case report. Pan Afr. Med. J. 2021, 38, 139. [Google Scholar] [CrossRef] [PubMed]
- Vandervorst, F.; Guldolf, K.; Peeters, I.; Vanderhasselt, T.; Michiels, K.; Berends, K.J.; Van Laethem, J.; Pipeleers, L.; Vincken, S.; Seynaeve, L.; et al. Encephalitis associated with the SARS-CoV-2 virus: A case report. Interdiscip. Neurosurg. 2020, 22, 100821. [Google Scholar] [CrossRef]
- Kihira, S.; Delman, B.; Belani, P.; Stein, L.; Aggarwal, A.; Rigney, B.; Schefflein, J.; Doshi, A.; Pawha, P. Imaging Features of Acute Encephalopathy in Patients with COVID-19: A Case Series. Am. J. Neuroradiol. 2020, 41, 1804–1808. [Google Scholar] [CrossRef]
- Krett, J.D.; Jewett, G.A.; Elton-Lacasse, C.; Fonseca, K.; Hahn, C.; Au, S.; Koch, M.W. Hemorrhagic encephalopathy associated with COVID-19. J. Neuroimmunol. 2020, 346, 577326. [Google Scholar] [CrossRef] [PubMed]

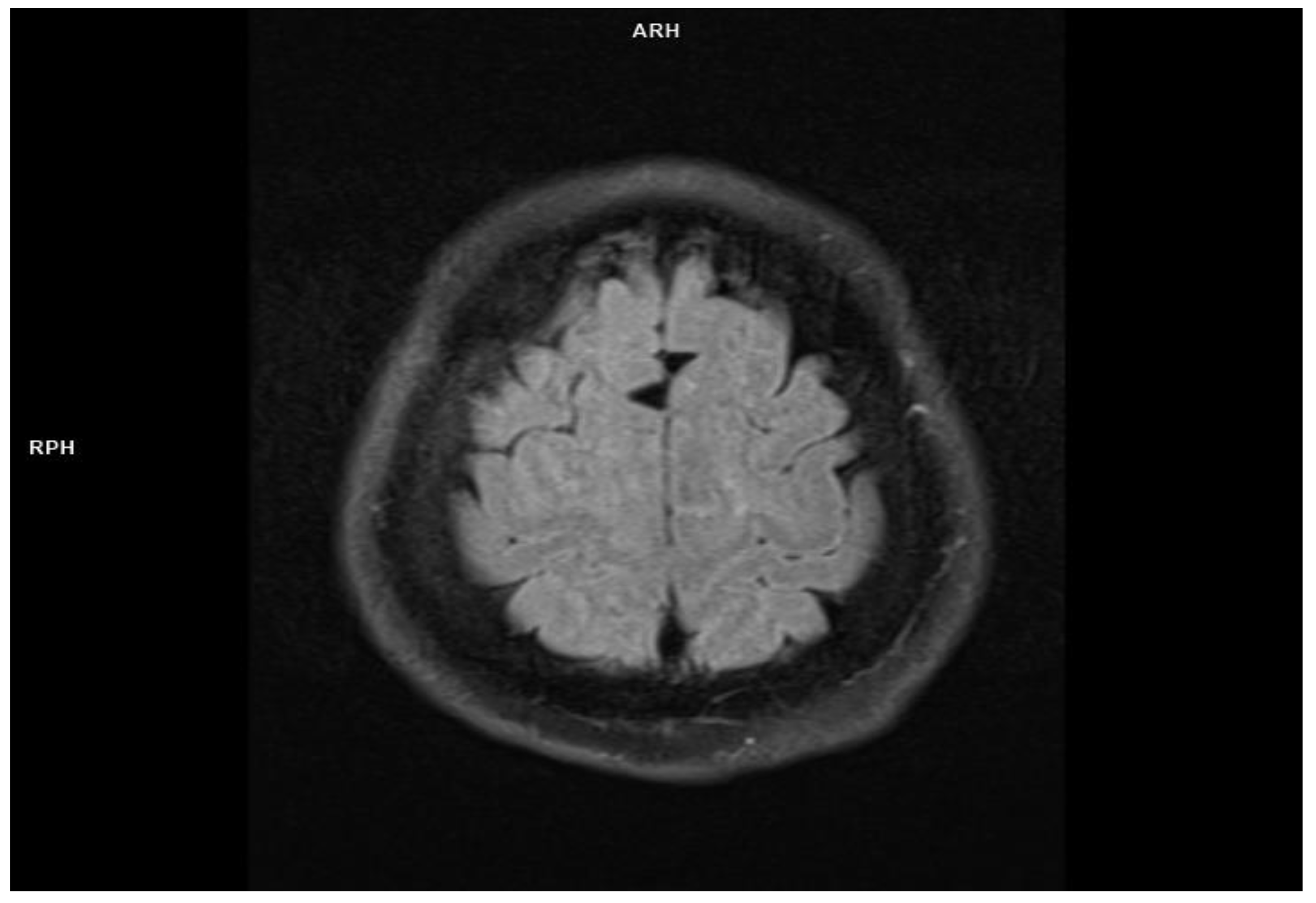
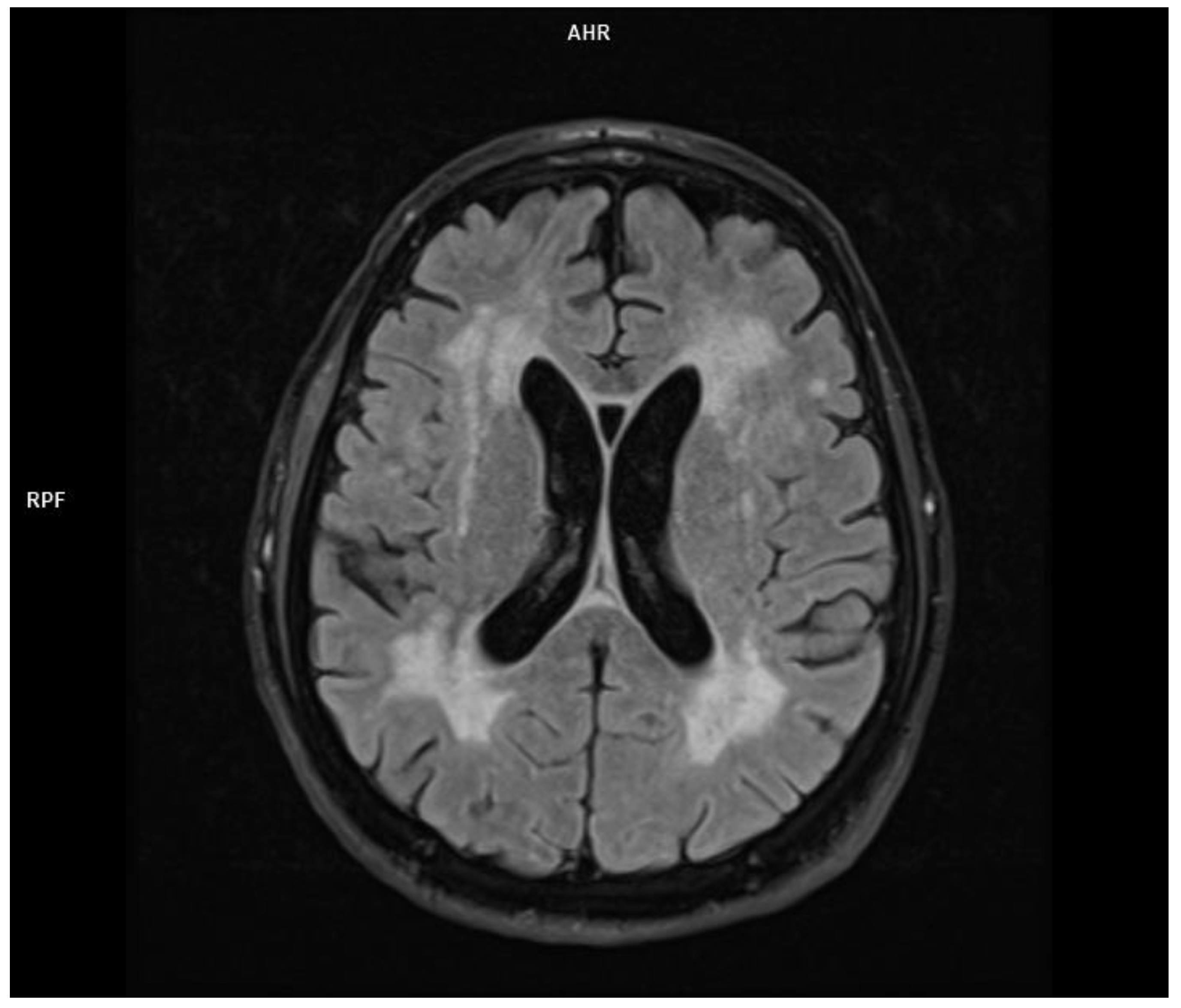
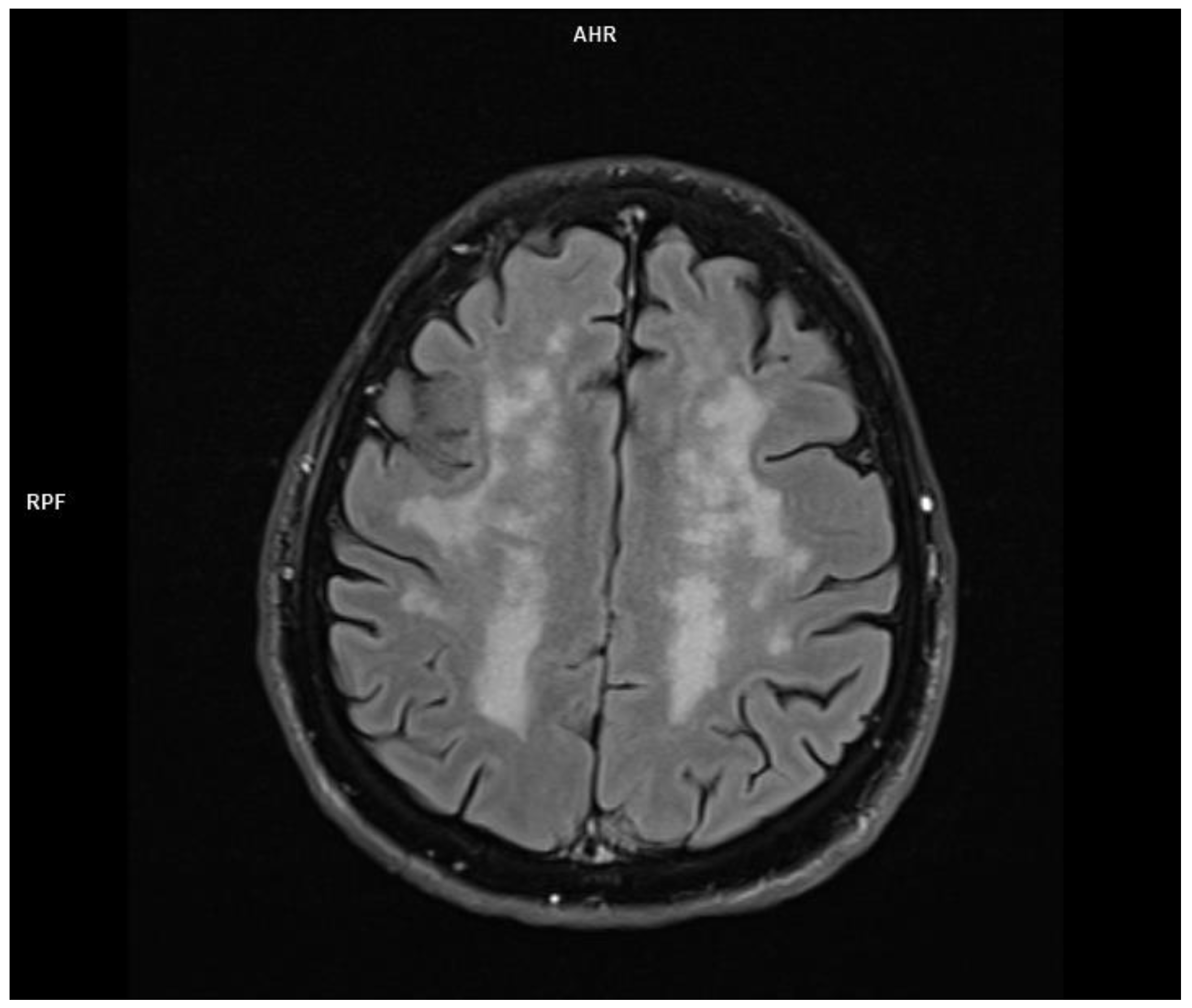

| Mild | headache |
| dizziness | |
| anosmia | |
| Moderate | psychomotor deceleration and memory impairment (including “brain fog”) |
| ataxia | |
| speech disorders | |
| neuralgia and neuropathic pain | |
| Severe | muscular paresis and paralysis |
| epileptic seizures | |
| coma |
| Parameters | LP 1 | LP 2 | LP 3 | LP 4 | |
|---|---|---|---|---|---|
| Patient 1 | Glucose: | 79 | 77 | 47 | X |
| Cl−: | 127.9 | 121.7 | 119.6 | X | |
| Protein: | 66.5 | 75.1 | 72.3 | X | |
| WBC: | 2 | 1 | 1 | X | |
| Macrophages: | 0 | 0 | 1 | X | |
| Patient 2 | Glucose: | 123 | X | X | X |
| Cl−: | 135.8 | X | X | X | |
| Protein: | 72.1 | X | X | X | |
| WBC: | 7 | X | X | X | |
| Macrophages: | 0 | X | X | X | |
| Patient 3 | Glucose: | 76 | 93 | 85 | 78 |
| Cl−: | 127.9 | 137.1 | 127.1 | 121.8 | |
| Protein: | 24.7 | 39.9 | 38.2 | 22.7 | |
| WBC: | 2 | 4 | 5 | 2 | |
| Macrophages: | 0 | 0 | 0 | 0 |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2022 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Udzik, J.; Jakubowski, P.; Niekrasz, M.; Barczyszyn, A.; Parczewski, M. COVID-19-Associated Encephalopathy—Case Series and Clinical Considerations. J. Clin. Med. 2022, 11, 981. https://doi.org/10.3390/jcm11040981
Udzik J, Jakubowski P, Niekrasz M, Barczyszyn A, Parczewski M. COVID-19-Associated Encephalopathy—Case Series and Clinical Considerations. Journal of Clinical Medicine. 2022; 11(4):981. https://doi.org/10.3390/jcm11040981
Chicago/Turabian StyleUdzik, Jakub, Paweł Jakubowski, Małgorzata Niekrasz, Adrian Barczyszyn, and Miłosz Parczewski. 2022. "COVID-19-Associated Encephalopathy—Case Series and Clinical Considerations" Journal of Clinical Medicine 11, no. 4: 981. https://doi.org/10.3390/jcm11040981
APA StyleUdzik, J., Jakubowski, P., Niekrasz, M., Barczyszyn, A., & Parczewski, M. (2022). COVID-19-Associated Encephalopathy—Case Series and Clinical Considerations. Journal of Clinical Medicine, 11(4), 981. https://doi.org/10.3390/jcm11040981






