Contrast-Enhanced Ultrasound in the Differentiation between the Most Common Benign Parotid Gland Tumors: A Systematic Review and Meta-Analysis
Abstract
1. Introduction
2. Materials and Methods
2.1. Study Guidance
2.2. Search Strategy and Criteria
2.3. Eligibility Criteria
2.4. Data Extraction
2.5. Quality Assessment
2.6. Evaluation of Qualitative CEUS-Derived Data
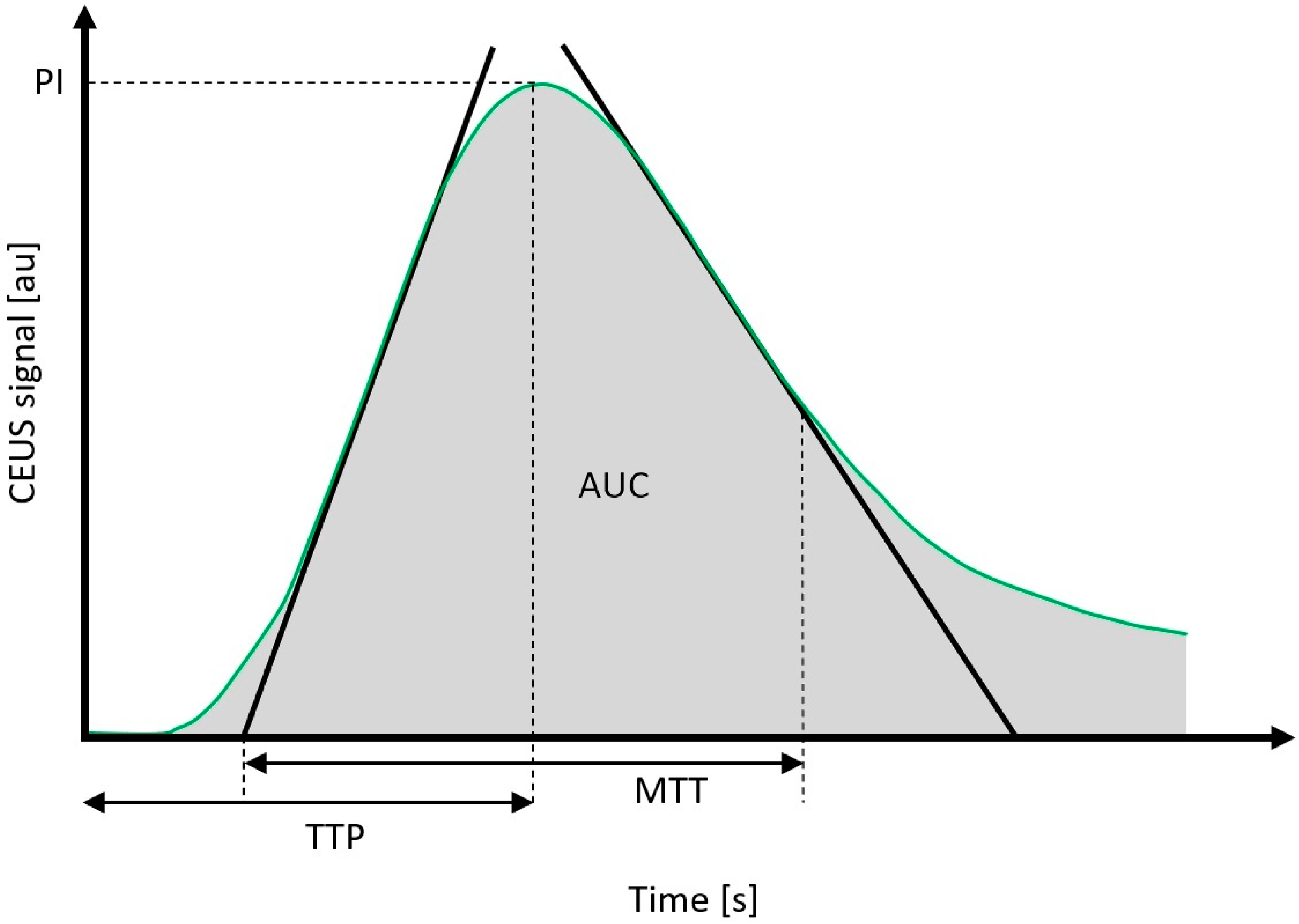
2.7. Evaluation of Quantitative CEUS-Derived Data
2.8. Statistical Analysis
3. Results
3.1. Study Selection
3.2. Study Characteristics
3.3. Study Heterogeneity
3.4. Study Quality
3.5. Qualitative CEUS-Derived Data
3.6. Quantitative CEUS-Derived Data
4. Discussion
4.1. Qualitative CEUS-Derived Data
4.2. Quantitative CEUS-Derived Data
4.3. Limitations
5. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Conflicts of Interest
References
- Dostalova, L.; Kalfert, D.; Jechova, A.; Koucky, V.; Novak, S.; Kuchar, M.; Zabrodsky, M.; Novakova Kodetova, D.; Ludvikova, M.; Kholova, I.; et al. The Role of Fine-Needle Aspiration Biopsy (FNAB) in the Diagnostic Management of Parotid Gland Masses with Emphasis on Potential Pitfalls. Eur. Arch. Otorhinolaryngol. 2020, 277, 1763–1769. [Google Scholar] [CrossRef] [PubMed]
- Zhan, K.Y.; Khaja, S.F.; Flack, A.B.; Day, T.A. Benign Parotid Tumors. Otolaryngol. Clin. N. Am. 2016, 49, 327–342. [Google Scholar] [CrossRef]
- Thielker, J.; Grosheva, M.; Ihrler, S.; Wittig, A.; Guntinas-Lichius, O. Contemporary Management of Benign and Malignant Parotid Tumors. Front. Surg. 2018, 5, 39. [Google Scholar] [CrossRef] [PubMed]
- Podlesák, T.; Dolecková, V.; Sibl, O. Malignancy of a Cystadenolymphoma of the Parotid Gland. Eur. Arch. Otorhinolaryngol. 1992, 249, 233–235. [Google Scholar] [CrossRef]
- Zajkowski, P.; Jakubowski, W.; Białek, E.J.; Wysocki, M.; Osmólski, A.; Serafin-Król, M. Pleomorphic Adenoma and Adenolymphoma in Ultrasonography. Eur. J. Ultrasound 2000, 12, 23–29. [Google Scholar] [CrossRef] [PubMed]
- Teymoortash, A.; Krasnewicz, Y.; Werner, J.A. Clinical Features of Cystadenolymphoma (Warthin’s Tumor) of the Parotid Gland: A Retrospective Comparative Study of 96 Cases. Oral Oncol. 2006, 42, 569–573. [Google Scholar] [CrossRef]
- Yan, M.; Xu, D.; Chen, L.; Zhou, L. Comparative Study of Qualitative and Quantitative Analyses of Contrast-Enhanced Ultrasound and the Diagnostic Value of B-Mode and Color Doppler for Common Benign Tumors in the Parotid Gland. Front. Oncol. 2021, 11, 669542. [Google Scholar] [CrossRef] [PubMed]
- Quer, M.; Hernandez-Prera, J.C.; Silver, C.E.; Casasayas, M.; Simo, R.; Vander Poorten, V.; Guntinas-Lichius, O.; Bradley, P.J.; Tong-Ng, W.; Rodrigo, J.P.; et al. Current Trends and Controversies in the Management of Warthin Tumor of the Parotid Gland. Diagnostics 2021, 11, 1467. [Google Scholar] [CrossRef] [PubMed]
- Steinhart, H.; Zenk, J.; Sprang, K.; Bozzato, A.; Iro, H. Contrast-Enhanced Color Doppler Sonography of Parotid Gland Tumors. Eur. Arch. Otorhinolaryngol. 2003, 260, 344–348. [Google Scholar] [CrossRef]
- Bhatia, K.S.S.; Cho, C.C.M.; Tong, C.S.L.; Lee, Y.Y.P.; Yuen, E.H.Y.; Ahuja, A.T. Shear Wave Elastography of Focal Salivary Gland Lesions: Preliminary Experience in a Routine Head and Neck US Clinic. Eur. Radiol. 2012, 22, 957–965. [Google Scholar] [CrossRef]
- Wang, J.; Jiang, L. Application Value of Shear Wave Elastography in Salivary Gland Tumors. Oral Radiol. 2021, 37, 653–657. [Google Scholar] [CrossRef]
- Stoia, S.; Băciuț, G.; Lenghel, M.; Badea, R.; Băciuț, M.; Bran, S.; Cristian, D. Ultrasonography Techniques in the Preoperative Diagnosis of Parotid Gland Tumors - an Updated Review of the Literature. Med. Ultrason. 2021, 23, 194–202. [Google Scholar] [CrossRef] [PubMed]
- Li, C.; Zhang, C.; Li, N.; Li, J. Compression Real-Time Elastography for Evaluation of Salivary Gland Lesions: A Meta-Analysis. J. Ultrasound Med. 2016, 35, 999–1007. [Google Scholar] [CrossRef] [PubMed]
- Bhatia, K.S.S.; Dai, Y.-L. Routine and Advanced Ultrasound of Major Salivary Glands. Neuroimaging Clin. N. Am. 2018, 28, 273–293. [Google Scholar] [CrossRef] [PubMed]
- Baohong, W.; Jing, Z.; Zanxia, Z.; Kun, F.; Liang, L.; Eryuan, G.; Yong, Z.; Fei, H.; Jingliang, C.; Jinxia, Z. T2 Mapping and Readout Segmentation of Long Variable Echo-Train Diffusion-Weighted Imaging for the Differentiation of Parotid Gland Tumors. Eur. J. Radiol. 2022, 151, 110265. [Google Scholar] [CrossRef] [PubMed]
- Wu, Q.; Zhu, L.-N.; Jiang, J.-S.; Bu, S.-S.; Xu, X.-Q.; Wu, F.-Y. Characterization of Parotid Gland Tumors Using T2 Mapping Imaging: Initial Findings. Acta Radiol. 2020, 61, 629–635. [Google Scholar] [CrossRef] [PubMed]
- Karaman, C.Z.; Tanyeri, A.; Özgür, R.; Öztürk, V.S. Parotid Gland Tumors: Comparison of Conventional and Diffusion-Weighted MRI Findings with Histopathological Results. Dentomaxillofac. Radiol. 2021, 50, 20200391. [Google Scholar] [CrossRef]
- Salgarelli, A.C.; Capparè, P.; Bellini, P.; Collini, M. Usefulness of Fine-Needle Aspiration in Parotid Diagnostics. Oral Maxillofac. Surg. 2009, 13, 185–190. [Google Scholar] [CrossRef]
- Howlett, D.C. Diagnosing a Parotid Lump: Fine Needle Aspiration Cytology or Core Biopsy? Br. J. Radiol. 2006, 79, 295–297. [Google Scholar] [CrossRef]
- Marotti, J.; Heger, S.; Tinschert, J.; Tortamano, P.; Chuembou, F.; Radermacher, K.; Wolfart, S. Recent Advances of Ultrasound Imaging in Dentistry—A Review of the Literature. Oral Surg. Oral Med. Oral Pathol. Oral Radiol. 2013, 115, 819–832. [Google Scholar] [CrossRef]
- Quaia, E. Microbubble Ultrasound Contrast Agents: An Update. Eur. Radiol. 2007, 17, 1995–2008. [Google Scholar] [CrossRef] [PubMed]
- Greis, C. Ultrasound Contrast Agents as Markers of Vascularity and Microcirculation. Clin. Hemorheol. Microcirc. 2009, 43, 1–9. [Google Scholar] [CrossRef] [PubMed]
- Sultan, S.R.; AlKharaiji, M.; Rajab, S.H. Diagnosis of Parotid Gland Tumours with Contrast-Enhanced Ultrasound: A Systematic Review and Meta-Analysis. Med. Ultrason. 2022, 24, 211–218. [Google Scholar] [CrossRef]
- Page, M.J.; McKenzie, J.E.; Bossuyt, P.M.; Boutron, I.; Hoffmann, T.C.; Mulrow, C.D.; Shamseer, L.; Tetzlaff, J.M.; Akl, E.A.; Brennan, S.E.; et al. The PRISMA 2020 Statement: An Updated Guideline for Reporting Systematic Reviews. BMJ 2021, 327, n71. [Google Scholar] [CrossRef] [PubMed]
- Rogalska, M.; Antkowiak, L.; Kasperczuk, A.; Scierski, W. Contrast-Enhanced Ultrasound in the Differentiation between the Most Common Benign Parotid Gland Tumors: A Systematic Review and Meta-Analysis; INPLASY—International Platform of Registered Systematic Review and Meta-Analysis Protocols: Middletown, DE, USA, 2022. [Google Scholar]
- Whiting, P.F.; Rutjes, A.W.S.; Westwood, M.E.; Mallett, S.; Deeks, J.J.; Reitsma, J.B.; Leeflang, M.M.G.; Sterne, J.A.C.; Bossuyt, P.M.M.; QUADAS-2 Group. QUADAS-2: A Revised Tool for the Quality Assessment of Diagnostic Accuracy Studies. Ann. Intern. Med. 2011, 155, 529–536. [Google Scholar] [CrossRef] [PubMed]
- Badea, A.F.; Bran, S.; Tamas-Szora, A.; Floareş, A.; Badea, R.; Baciut, G. Solid Parotid Tumors: An Individual and Integrative Analysis of Various Ultrasonographic Criteria. A Prospective and Observational Study. Med. Ultrason. 2013, 15, 289–298. [Google Scholar] [CrossRef] [PubMed]
- Fischer, T.; Paschen, C.F.; Slowinski, T.; Alkhameri, A.; Berl, J.C.; Klingebiel, R.; Thomas, A. Differentiation of Parotid Gland Tumors with Contrast-Enhanced Ultrasound. Rofo 2010, 182, 155–162. [Google Scholar] [CrossRef]
- Jiang, L.-P. Characteristics of Pleomorphic Adenomas, Adenolymphomas, and Malignant Tumors of the Salivary Glands on Color Doppler Ultrasonography and Contrast Enhanced Ultrasonography. Eur. Rev. Med. Pharmacol. Sci. 2020, 24, 11509–11517. [Google Scholar] [CrossRef]
- Knopf, A.; Mansour, N.; Chaker, A.; Bas, M.; Stock, K. Multimodal Ultrasonographic Characterisation of Parotid Gland Lesions—A Pilot Study. Eur. J. Radiol. 2012, 81, 3300–3305. [Google Scholar] [CrossRef]
- Wei, X.; Li, Y.; Zhang, S.; Li, X.; Wang, H.; Yong, X.; Wang, X.; Li, X.; Gao, M. Evaluation of Microvascularization in Focal Salivary Gland Lesions by Contrast-Enhanced Ultrasonography (CEUS) and Color Doppler Sonography. Clin. Hemorheol. Microcirc. 2013, 54, 259–271. [Google Scholar] [CrossRef]
- Welkoborsky, H.J.; Albers, M.; Küstermeyer, J. Perfusion Analysis of Benign Parotid Gland Tumors by Contrast-Enhanced Ultrasonography (CEUS). Eur. Arch. Otorhinolaryngol. 2022, 279, 4137–4146. [Google Scholar] [CrossRef] [PubMed]
- Bozzato, A.; Zenk, J.; Greess, H.; Hornung, J.; Gottwald, F.; Rabe, C.; Iro, H. Potential of Ultrasound Diagnosis for Parotid Tumors: Analysis of Qualitative and Quantitative Parameters. Otolaryngol. Head Neck Surg. 2007, 137, 642–646. [Google Scholar] [CrossRef] [PubMed]
- Wang, Y.; Nie, F.; Wang, P. Clinical Diagnostic Application of Contrast-Enhanced Ultrasound in Focal Lesions of the Salivary Glands. J. Ultrasound Med. 2022, 41, 2535–2546. [Google Scholar] [CrossRef] [PubMed]
- Guo, J.-M.; Chen, Q.; Wu, H.; Feng, L.-T.; Chen, J.; Chao, W.-B. Differential Diagnosis between Acinic Cell Carcinoma and Pleomorphic Adenoma Using the Quantitative Parameters of Contrast-Enhanced Ultrasound. Eur. Rev. Med. Pharmacol. Sci. 2021, 25, 1936–1943. [Google Scholar] [CrossRef] [PubMed]
- Klotz, L.V.; Gürkov, R.; Eichhorn, M.E.; Siedek, V.; Krause, E.; Jauch, K.-W.; Reiser, M.F.; Clevert, D.-A. Perfusion Characteristics of Parotid Gland Tumors Evaluated by Contrast-Enhanced Ultrasound. Eur. J. Radiol. 2013, 82, 2227–2232. [Google Scholar] [CrossRef]
- Klotz, L.V.; Ingrisch, M.; Eichhorn, M.E.; Niemoeller, O.; Siedek, V.; Gürkov, R.; Clevert, D.-A. Monitoring Parotid Gland Tumors with a New Perfusion Software for Contrast-Enhanced Ultrasound. Clin. Hemorheol. Microcirc. 2014, 58, 261–269. [Google Scholar] [CrossRef] [PubMed]
- Mansour, N.; Bas, M.; Stock, K.F.; Strassen, U.; Hofauer, B.; Knopf, A. Multimodal Ultrasonographic Pathway of Parotid Gland Lesions. Ultraschall. Med. 2017, 38, 166–173. [Google Scholar] [CrossRef]
- Saito, D.; Shiga, K.; Katagiri, K.; Oikawa, S.-I.; Ikeda, A.; Tsuchida, K.; Miyaguchi, J.; Kusaka, T.; Kuroda, H.; Takahashi, F. Contrast-Enhanced Ultrasonography for the Differential Diagnosis of Pleomorphic Adenomas and Warthin Tumors in Salivary Glands. Laryngoscope Investig. Otolaryngol. 2021, 6, 425–431. [Google Scholar] [CrossRef]
- Guiban, O.; Rubini, A.; Fresilli, D.; Lucarelli, G.T.; Ralli, M.; Cassoni, A.; Bezzi, M.; Radzina, M.; Greco, A.; De Vincentiis, M.; et al. Preoperative Multiparametric Ultrasound and Fine Needle Aspiration Cytology Evaluation of Parotid Gland Tumors: Which Is the Best Technique? Med. Ultrason. 2021, 23, 402–409. [Google Scholar] [CrossRef]
- Cantisani, V.; Bertolotto, M.; Weskott, H.P.; Romanini, L.; Grazhdani, H.; Passamonti, M.; Drudi, F.M.; Malpassini, F.; Isidori, A.; Meloni, F.M.; et al. Growing Indications for CEUS: The Kidney, Testis, Lymph Nodes, Thyroid, Prostate, and Small Bowel. Eur. J. Radiol. 2015, 84, 1675–1684. [Google Scholar] [CrossRef]
- David, E.; Cantisani, V.; De Vincentiis, M.; Sidhu, P.S.; Greco, A.; Tombolini, M.; Drudi, F.M.; Messineo, D.; Gigli, S.; Rubini, A.; et al. Contrast-Enhanced Ultrasound in the Evaluation of Parotid Gland Lesions: An Update of the Literature. Ultrasound 2016, 24, 104–110. [Google Scholar] [CrossRef] [PubMed]
- Sučić, M.; Ljubić, N.; Perković, L.; Ivanović, D.; Pažanin, L.; Sučić Radovanović, T.; Župnić-Krmek, D.; Knežević, F. Cytopathology and Diagnostics of Warthin’s Tumour. Cytopathology 2020, 31, 193–207. [Google Scholar] [CrossRef] [PubMed]


| First Author (Year) | No. of Tumors (PAs/WTs) | Reference Standard | Contrast Agent | ROI | Time Considered for Analysis | Assessed Quantitative CEUS Parameters | Qualitative CEUS Findings |
|---|---|---|---|---|---|---|---|
| Badea (2013) [27] | 12 (12/0) | histopathology | SonoVue | whole tumor | 120 s | TTP | CEUS uptake pattern in PAs was variable due to the displacement of the tumor vessels towards periphery (homogenous, 4/12; inhomogeneous, 6/12). |
| Bozzato (2007) [33] | 81 (51/30) | histopathology | SonoVue | Area within the tumor decided by the user | 90 s | PI, TTP, WiT, WiV | PAs showed a presence of distal echo enhancement and a trend to higher marginal perfusion, whereas WTs presented a tendency towards higher blood supply and manifested a marked central perfusion trend. |
| Fischer (2010) [28] | 18 (9/9) | histopathology | SonoVue | Vascularized area within the tumor | 60 s | AUC, TTP | Contrast enhancement differed between PAs and WTs. In the PA group: an increase in echogenicity mainly in the tumor periphery; no enhancement of the center in 7/9 PAs; central non-enhancing areas corresponding to pseudocysts and necrosis. In the WT group: small nodular peripheral defects and fairly homogeneous central enhancement in 5/9 WTs; well-demarcated small cystic areas; central enhancement was absent in only 2/9 cases |
| Guiban (2021) [40] | 44 (16/28) | histopathology | SonoVue | Area within the tumor decided by the user, and adjacent parotid tissue | 120 s | NA | NA |
| Guo (2021) [35] | 98 (98/0) | histopathology | SonoVue | Highly perfused area within the tumor | 120 s–180 s | TTP, Peak, RBV, RBF, ∆Simax, Simean | NA |
| Jiang (2020) [29] | 52 (28/24) | histopathology | SonoVue | Area within the tumor with avid enhancement, and surrounding parotid tissue | 90 s | TTP, PI, TPH | PAs were significantly more heterogeneous than WTs. Significantly more PAs showed rim enhancement compared to WTs. |
| Klotz (2013) [36] | 32 (17/15) | histopathology | SonoVue | At the centre of solid tumor tissue, and surrounding parotid tissue | 90 s (first 30 s) | AUC, MMT, TTP, ∆Simax | NA |
| Klotz (2014) [37] | 24 (13/11) | histopathology | SonoVue | Area within the tumor decided by the user | 90 s (first 30 s) | AUC, PI, RT, WiR, WiPI | NA |
| Knopf (2012) [30] | 16 (8/8) | histopathology | SonoVue | Area within the tumor decided by the user, normalized by surrounding parotid tissue | NA | nMTT, nTTP | CEUS visualized poor perfusion in PAs and apparent hyperperfusion in WTs. |
| Mansour (2017) [38] | 137 (64/73) | histopathology | SonoVue | Area within the tumor decided by the user, normalized by surrounding parotid tissue | NA | nMTT | NA |
| Saito (2021) [39] | 23 (10/13) | histopathology | Sonazoid | Area within the tumor decided by the user | 120 s | TTP, AUC, Grand | NA |
| Wang (2022) [34] | 58 (36/22) | histopathology | SonoVue | Area within the tumor with abundant blood flow, and surrounding parotid tissue | 90 s | NA | The differences between PAs and WTs were statistically significant in terms of enhancement degree, enhancement pattern, enhancement homogeneity, and wash-in pattern. Most PAs showed simultaneous or later wash-in, inhomogeneous hypo- or isoenhancement and centripetal enhancement pattern. Contrarily, most WTs displayed earlier wash-in, homogeneous hyperenhancement, and non-centripetal enhancement pattern. |
| Wei (2013) [31] | 132 (62/70) | histopathology | SonoVue | Area within the remarkable perfusion area of the tumor, and surrounding parotid tissue | 180 s | AUC, TTP, PI | All PAs showed heterogeneous enhancement, mainly corresponding to the CEUS type 2b, whereas all WTs displayed diffuse homogeneous enhancement (representing CEUS type 1). |
| Welkoborsky (2022) [32] | 67 (31/36) | histopathology | SonoVue | 8 standardized areas distributed throughout the entire tumor | NA | AUC, TTP, Peak | Perfusion pattern significantly differed between PAs and WTs. No visible perfusion was found in 42% of PA and in 11% of WT, a peripheral (centripetal) perfusion pattern in 19.5% and 22%, respectively, and a centrifugal perfusion pattern in 6.5% and 25%, respectively. |
| Yan (2021) [7] | 88 (54/34) | histopathology | SonoVue | Area within the solid tumor tissue, and surrounding parotid tissue | 120 s | AUC, MTT, RT, PI, TPH, TTP, RS | The majority of WTs showed high homogeneous enhancement with a “fast in” and “slow out” pattern. Contrarily, most PAs displayed low heterogenous enhancement and presented with an echo-free area, and a pattern of “slow in” and “fast out”. |
| Feature | PAs Mean (95% CI) | WTs Mean (95% CI) | p Value |
|---|---|---|---|
| Rise time (RT) [s] | 4.08 (2.56–5.60) | 4.36 (2.49–6.23) | 0.444 |
| Mean transit time (MTT) [s] | 36.75 (24.93–48.57) | 63.90 (40.00–87.80) | <0.001 |
| Normalized mean transit time (nMTT) [s] | 1.45 (1.31–1.59) | 0.62 (0.51–0.74) | 0.002 |
| Area under curve (AUC) | 66.26 (57.66–74.87) | 107.99 (46.28–169.71) | <0.001 |
| Time from peak to one half (TPH) [s] | 46.29 (31.44–61.14) | 57.30 (40.54–74.06) | 0.001 |
| Time to peak (TTP) [s] | 26.92 (22.46–31.39) | 16.92 (16.04–17.72) | 0.001 |
| Normalized time to peak (nTTP) [s] | 1.46 (1.17–1.75) | 0.74 (0.67–0.81) | <0.001 |
| Rising slope (of wash-in curve) (RS) [dB/s] | 2.42 (1.34–5.76) | 1.28 (0.84–1.72) | 0.052 |
| Wash-in-rate (WiR) | 3.26 (2.51–4.01) | 16.3 (13.23–18.83) | <0.001 |
| Wash-in-perfusion-index (WiPI) | 8.0 (6.87–9.13) | 44.6 (37.20–52.00) | <0.001 |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2022 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Rogalska, M.; Antkowiak, L.; Kasperczuk, A.; Scierski, W. Contrast-Enhanced Ultrasound in the Differentiation between the Most Common Benign Parotid Gland Tumors: A Systematic Review and Meta-Analysis. J. Clin. Med. 2022, 11, 7360. https://doi.org/10.3390/jcm11247360
Rogalska M, Antkowiak L, Kasperczuk A, Scierski W. Contrast-Enhanced Ultrasound in the Differentiation between the Most Common Benign Parotid Gland Tumors: A Systematic Review and Meta-Analysis. Journal of Clinical Medicine. 2022; 11(24):7360. https://doi.org/10.3390/jcm11247360
Chicago/Turabian StyleRogalska, Marta, Lukasz Antkowiak, Anna Kasperczuk, and Wojciech Scierski. 2022. "Contrast-Enhanced Ultrasound in the Differentiation between the Most Common Benign Parotid Gland Tumors: A Systematic Review and Meta-Analysis" Journal of Clinical Medicine 11, no. 24: 7360. https://doi.org/10.3390/jcm11247360
APA StyleRogalska, M., Antkowiak, L., Kasperczuk, A., & Scierski, W. (2022). Contrast-Enhanced Ultrasound in the Differentiation between the Most Common Benign Parotid Gland Tumors: A Systematic Review and Meta-Analysis. Journal of Clinical Medicine, 11(24), 7360. https://doi.org/10.3390/jcm11247360






