Adalimumab plus Conventional Therapy versus Conventional Therapy in Refractory Non-Infectious Scleritis
Abstract
1. Introduction
2. Materials and Methods
2.1. Patient Population
2.2. Treatment Protocols
2.3. Follow-Up
2.4. Clinical Endpoints
2.5. Statistical Analysis
3. Results
3.1. Baseline Characteristics
3.2. Outcome Measures
4. Discussion
5. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Conflicts of Interest
Appendix A
| Group | No. | Age at Onset | Sex | OD/OS/OU | Interval before Baseline, m | Site of Scleritis | Systemic Immune- Related Diseases | Follow-Up, m | Dates of Onset |
|---|---|---|---|---|---|---|---|---|---|
| CT | 1 | 46 | F | OD | 22 | anterior | 21 | Aug, 2020 | |
| 2 | 47 | F | OD | 24 | anterior | erythema nodosum | 9 | Dec, 2020 | |
| 3 | 58 | M | OS | 10 | anterior | 8 | Mar, 2021 | ||
| 4 | 39 | M | OD | 1 | anterior | leukoderma | 22 | Aug, 2020 | |
| 5 | 31 | F | OU | 24 | anterior | 7 | Jul, 2020 | ||
| 6 | 41 | M | OD | 8 | anterior | 15 | Jul, 2020 | ||
| 7 | 32 | F | OD | 5 | panscleritis | 17 | Sep, 2020 | ||
| 8 | 28 | F | OS | 4 | anterior | 11 | Sep, 2020 | ||
| 9 | 24 | F | OU | 24 | anterior | 7 | Mar, 2021 | ||
| ACT | 10 | 49 | M | OD | 2 | anterior | 12 | Jan, 2021 | |
| 11 | 15 | M | OU | 15 | posterior | 14 | Aug, 2020 | ||
| 12 | 39 | F | OD | 10 | anterior | 15 | Jun,2020 | ||
| 13 | 40 | F | OU | 9 | anterior | 12 | Jun, 2020 | ||
| 14 | 19 | M | OU | 10 | posterior | 19 | Jan, 2020 | ||
| 15 | 56 | F | OS | 2 | anterior | 12 | Oct, 2020 | ||
| 16 | 28 | F | OS | 3 | anterior | connective tissue disease | 7 | May, 2021 | |
| 17 | 15 | M | OS | 10 | panscleritis | 10 | Mar, 2021 | ||
| 18 | 20 | F | OD | 10 | panscleritis | 8 | Jan, 2021 |
| Clinical Features | Score Range | Score Definition |
|---|---|---|
| Tenderness * | 0–4 | 0–4 |
| Nodules | 0–1 | 0 for absent, 1 for present |
| Corneal involvement @ | 0/2/4 | 0 for absent, 2 for present, 4 for progressive |
| Anterior chamber cells | 0/1/2 | 0 for no cells, 1 for ≤20 cells/field, 2 for >20 cells/field |
| Vitreous cells | 0/1/2 | 0 for no vitreous haze, 1 for grade 1/2 haze, 2 for grade 3/4 haze |
| retinal detachment | 0/2 | 0 for absent, 2 for present |
| increased scleral thickness or T sign in B-mode ultrasound | 0/2 | 0 for absent, 2 for present |
| optic nerve swelling | 0/2 | 0 for absent, 2 for present |
References
- Okhravi, N.; Odufuwa, B.; McCluskey, P.; Lightman, S. Scleritis. Surv. Ophthalmol. 2005, 50, 351–363. [Google Scholar] [CrossRef] [PubMed]
- Majumder, P.D.; Agrawal, R.; McCluskey, P.; Biswas, J. Current Approach for the Diagnosis and Management of Noninfective Scleritis. Asia-Pacific J. Ophthalmol. 2020, 10, 212–223. [Google Scholar] [CrossRef] [PubMed]
- Watson, P.G.; Hayreh, S.S. Scleritis and episcleritis. Br. J. Ophthalmol. 1976, 60, 163–191. [Google Scholar] [CrossRef] [PubMed]
- de la Maza, M.S.; Molina, N.; Gonzalez-Gonzalez, L.A.; Doctor, P.P.; Tauber, J.; Foster, C.S. Clinical Characteristics of a Large Cohort of Patients with Scleritis and Episcleritis. Ophthalmology 2011, 119, 43–50. [Google Scholar] [CrossRef]
- Yang, P.; Ye, Z.; Tang, J.; Du, L.; Zhou, Q.; Qi, J.; Liang, L.; Wu, L.; Wang, C.; Xu, M.; et al. Clinical Features and Complications of Scleritis in Chinese Patients. Ocul. Immunol. Inflamm. 2016, 26, 387–396. [Google Scholar] [CrossRef]
- Vignesh, A.P.; Srinivasan, R. Ocular manifestations of rheumatoid arthritis and their correlation with anti-cyclic citrullinated peptide antibodies. Clin. Ophthalmol. 2015, 9, 393–397. [Google Scholar]
- Williamson, J. Incidence of eye disease in cases of connective tissue disease. Trans. Ophthalmol. Soc. UK 1974, 94, 742–752. [Google Scholar]
- Tanaka, R.; Kaburaki, T.; Ohtomo, K.; Takamoto, M.; Komae, K.; Numaga, J.; Fujino, Y.; Aihara, M. Clinical characteristics and ocular complications of patients with scleritis in Japanese. JPN J. Ophthalmol. 2018, 62, 517–524. [Google Scholar] [CrossRef]
- Wieringa, W.G.; Wieringa, J.E.; Loon, N.H.T.D.-V.; Los, L.I. Visual Outcome, Treatment Results, and Prognostic Factors in Patients with Scleritis. Ophthalmology 2013, 120, 379–386. [Google Scholar] [CrossRef]
- Wakefield, D.; Di Girolamo, N.; Thurau, S.; Wildner, G.; McCluskey, P. Scleritis: Immunopathogenesis and molecular basis for therapy. Prog. Retin. Eye Res. 2013, 35, 44–62. [Google Scholar] [CrossRef]
- Vergouwen, D.; Rothova, A.; Berge, J.T.; Verdijk, R.; van Laar, J.; Vingerling, J.; Schreurs, M. Current insights in the pathogenesis of scleritis. Exp. Eye Res. 2020, 197, 108078. [Google Scholar] [CrossRef] [PubMed]
- Sota, J.; Girolamo, M.-M.; Frediani, B.; Tosi, G.M.; Cantarini, L.; Fabiani, C. Biologic Therapies and Small Molecules for the Management of Non-Infectious Scleritis: A Narrative Review. Ophthalmol. Ther. 2021, 10, 777–813. [Google Scholar] [CrossRef]
- Fidelix, T.S.D.A.D.; Vieira, L.A.; De Freitas, D.; Trevisani, V.F.M. Biologic therapy for refractory scleritis: A new treatment perspective. Int. Ophthalmol. 2015, 35, 903–912. [Google Scholar] [CrossRef] [PubMed]
- Lacomba, M.S.; Martín, C.M.; Galera, J.M.G.; Vidal, M.A.G.; Estévez, E.C.; Chamond, R.R.; Omar, M.M. Aqueous Humor and Serum Tumor Necrosis Factor-α in Clinical Uveitis. Ophthalmic Res. 2001, 33, 251–255. [Google Scholar] [CrossRef] [PubMed]
- Hu, Y.; Huang, Z.; Yang, S.; Chen, X.; Su, W.; Liang, D. Effectiveness and Safety of Anti-Tumor Necrosis Factor-Alpha Agents Treatment in Behcets’ Disease-Associated Uveitis: A Systematic Review and Meta-Analysis. Front. Pharmacol. 2020, 11, 941. [Google Scholar] [CrossRef] [PubMed]
- Suzuki, Y.; Motoya, S.; Hanai, H.; Matsumoto, T.; Hibi, T.; Robinson, A.M.; Mostafa, N.M.; Chao, J.; Arora, V.; Camez, A.; et al. Efficacy and safety of adalimumab in Japanese patients with moderately to severely active ulcerative colitis. J. Gastroenterol. 2013, 49, 283–294. [Google Scholar] [CrossRef]
- Pelechas, E.; Voulgari, P.V.; Drosos, A.A. Preclinical discovery and development of adalimumab for the treatment of rheu-matoid arthritis. Expert Opin. Drug Discov. 2021, 16, 227–234. [Google Scholar] [CrossRef]
- Cimaz, R.; Maioli, G.; Calabrese, G. Current and emerging biologics for the treatment of juvenile idiopathic arthritis. Expert Opin. Biol. Ther. 2020, 20, 725–740. [Google Scholar] [CrossRef]
- Cholapranee, A.; Hazlewood, G.S.; Kaplan, G.G.; Peyrin-Biroulet, L.; Ananthakrishnan, A.N. Systematic review with me-ta-analysis: Comparative efficacy of biologics for induction and maintenance of mucosal healing in Crohn′s disease and ul-cerative colitis controlled trials. Aliment. Pharmacol. Ther. 2017, 45, 1291–1302. [Google Scholar] [CrossRef]
- Jaffe, G.J.; Dick, A.D.; Brézin, A.P.; Nguyen, Q.D.; Thorne, J.E.; Kestelyn, P.; Barisani-Asenbauer, T.; Franco, P.; Heiligenhaus, A.; Scales, D.; et al. Adalimumab in Patients with Active Noninfectious Uveitis. N. Engl. J. Med. 2016, 375, 932–943. [Google Scholar] [CrossRef]
- Lawuyi, L.E.; Gurbaxani, A. Refractory necrotizing scleritis successfully treated with adalimumab. J. Ophthalmic Inflamm. Infect. 2016, 6, 37. [Google Scholar] [CrossRef] [PubMed]
- Restrepo, J.P.; Molina, M.P. Successful treatment of severe nodular scleritis with adalimumab. Clin. Rheumatol. 2010, 29, 559–561. [Google Scholar] [CrossRef] [PubMed]
- González-López, J.J.; Lavric, A.; Majumder, P.D.; Bansal, N.; Biswas, J.; Pavesio, C.; Agrawal, R. Bilateral Posterior Scleritis: Analysis of 18 Cases from a Large Cohort of Posterior Scleritis. Ocul. Immunol. Inflamm. 2015, 24, 16–23. [Google Scholar] [CrossRef] [PubMed]
- McCluskey, P.; Wakefield, D. Prediction of response to treatment in patients with scleritis using a standardised scoring system. Aust. N. Z. J. Ophthalmol. 1991, 19, 211–215. [Google Scholar] [CrossRef]
- O′Neil, E.C.; Huang, J.; Suhler, E.B.; Dunn, J.P., Jr.; Perez, V.L.; Gritz, D.C.; McWilliams, K.; Peskin, E.; Ying, G.S.; Bunya, V.Y.; et al. Iontophoretic delivery of dexamethasone phosphate for non-infectious, non-necrotising anterior scleritis, dose-finding clinical trial. Br. J. Ophthalmol. 2018, 102, 1011–1013. [Google Scholar] [CrossRef]
- Schulze-Bonsel, K.; Feltgen, N.; Burau, H.; Hansen, L.; Bach, M. Visual acuities "hand motion" and "counting fingers" can be quantified with the freiburg visual acuity test. Investig. Ophthalmol. Vis. Sci. 2006, 47, 1236–1240. [Google Scholar] [CrossRef]
- Jabs, D.A.; Nussenblatt, R.B.; Rosenbaum, J.T. Standardization of Uveitis Nomenclature (SUN) Working Group. Standard-ization of uveitis nomenclature for reporting clinical data. Results of the First International Workshop. Am. J. Ophthalmol. 2005, 140, 509–516. [Google Scholar]
- Sims, J. Scleritis: Presentations, disease associations and management. Postgrad. Med. J. 2012, 88, 713–718. [Google Scholar] [CrossRef]
- Suhler, E.B.; Lowder, C.Y.; Goldstein, D.A.; Giles, T.; Lauer, A.K.; Kurz, P.A.; Pasadhika, S.; Lee, S.T.; de Saint Sardos, A.; Butler, N.J.; et al. Adalimumab therapy for refractory uveitis: Results of a multicentre, open-label, prospective trial. Br. J. Ophthalmol. 2013, 97, 481–486. [Google Scholar] [CrossRef]
- Borrás-Blasco, J.; Casterá, D.E.; Cortes, X.; Abad, F.J.; Rosique-Robles, J.D.; Mallench, L.G. Effectiveness of infliximab, ada-limumab and golimumab for non-infectious refractory uveitis in adults. Int. J. Clin. Pharmacol. Ther. 2015, 53, 377–390. [Google Scholar] [CrossRef]
- Díaz-Llopis, M.; Salom, D.; Garcia-De-Vicuña, C.; Cordero-Coma, M.; Ortega, G.; Ortego, N.; Suarez-De-Figueroa, M.; Rio-Pardo, M.J.; Fernandez-Cid, C.; Fonollosa, A.; et al. Treatment of Refractory Uveitis with Adalimumab: A Prospective Multicenter Study of 131 Patients. Ophthalmology 2012, 119, 1575–1581. [Google Scholar] [CrossRef] [PubMed]
- Markomichelakis, N.; Delicha, E.; Masselos, S.; Fragiadaki, K.; Kaklamanis, P.; Sfikakis, P.P. A single infliximab infusion vs corticosteroids for acute panuveitis attacks in Behçet′s disease: A comparative 4-week study. Rheumatology 2011, 50, 593–597. [Google Scholar] [CrossRef] [PubMed]
- Nguyen, Q.D.; Merrill, P.T.; Jaffe, G.J.; Dick, A.D.; Kurup, S.K.; Sheppard, J.; Schlaen, A.; Pavesio, C.; Cimino, L.; Van Calster, J.; et al. Adalimumab for prevention of uveitic flare in patients with inactive noninfectious uveitis controlled by cortico-steroids (VISUAL II): A multicentre, double-masked, randomised, placebo-controlled phase 3 trial. Lancet 2016, 388, 1183–1192. [Google Scholar] [CrossRef]
- Oray, M.; Abu Samra, K.; Ebrahimiadib, N.; Meese, H.; Foster, C.S. Long-term side effects of glucocorticoids. Expert Opin. Drug Saf. 2016, 15, 457–465. [Google Scholar] [CrossRef] [PubMed]
- Bitossi, A.; Bettiol, A.; Silvestri, E.; Di Scala, G.; Bacherini, D.; Lopalco, G.; Venerito, V.; Iannone, F.; Vitale, A.; Tosi, G.M.; et al. Adalimumab Accounts for Long-Term Control of Noninfectious Uveitis Also in the Absence of Concomitant DMARD Treatment: A Multicenter Retrospective Study. Mediat. Inflamm. 2019, 2019, 1–8. [Google Scholar] [CrossRef]
- Silvestri, E.; Bitossi, A.; Bettiol, A.; Emmi, G.; Urban, M.L.; Mattioli, I.; Di Scala, G.; Bacherini, D.; Lopalco, G.; Venerito, V.; et al. Adalimumab effectively controls both anterior and posterior noninfectious uveitis associated with systemic inflammatory diseases: Focus on Behçet’s syndrome. Inflammopharmacology 2020, 28, 711–718. [Google Scholar] [CrossRef]
- Riono, W.P.; Hidayat, A.A.; Rao, N.A. Scleritis: A clinicopathologic study of 55 cases. Ophthalmology 1999, 106, 1328–1333. [Google Scholar] [CrossRef]
- Silva, L.C.; Ortigosa, L.C.; Benard, G. Anti-TNF-α agents in the treatment of immune-mediated inflammatory diseases: Mechanisms of action and pitfalls. Immunotherapy 2010, 2, 817–833. [Google Scholar] [CrossRef]
- Zhou, L.; Yan, C.; Gieling, R.G.; Kida, Y.; Garner, W.; Li, W.; Han, Y.-P. Tumor necrosis factor-alpha induced expression of matrix metalloproteinase-9 through p21-activated Kinase-1. BMC Immunol. 2009, 10, 15. [Google Scholar] [CrossRef]
- Seo, K.Y.; Lee, H.K.; Kim, E.K.; Lee, J.H. Expression of Tumor Necrosis Factor Alpha and Matrix Metalloproteinase-9 in Surgically Induced Necrotizing Scleritis. Ophthalmic Res. 2006, 38, 66–70. [Google Scholar] [CrossRef]
- Di Girolamo, N.; Lloyd, A.; McCluskey, P.; Filipic, M.; Wakefield, D. Increased expression of matrix metalloproteinases in vivo in scleritis tissue and in vitro in cultured human scleral fibroblasts. Am. J. Pathol. 1997, 150, 653–666. [Google Scholar]
- Di Girolamo, N.; Visvanathan, K.; Lloyd, A.; Wakefield, D. Expression of TNF-alpha by human plasma cells in chronic in-flammation. J. Leukoc. Biol. 1997, 61, 667–678. [Google Scholar] [CrossRef] [PubMed]
- Sainz-De-La-Maza, M.; Molins, B.; Mesquida, M.; Llorenç, V.; Zarranz-Ventura, J.; Sala-Puigdollers, A.; Matas, J.; Adan, A.; Foster, C.S. Interleukin-22 serum levels are elevated in active scleritis. Acta Ophthalmol. 2016, 94, e395–e399. [Google Scholar] [CrossRef] [PubMed]
- Nishio, Y.; Taniguchi, H.; Takeda, A.; Hori, J. Immunopathological Analysis of a Mouse Model of Arthritis-Associated Scleritis and Implications for Molecular Targeted Therapy for Severe Scleritis. Int. J. Mol. Sci. 2021, 23, 341. [Google Scholar] [CrossRef] [PubMed]
- Gao, Y.; Du, L.; Li, F.; Ding, J.; Li, G.; Cao, Q.; Li, N.; Su, G.; Kijlstra, A.; Yang, P. The haplotypes of various TNF related genes associated with scleritis in Chinese Han. Hum. Genom. 2020, 14, 1–9. [Google Scholar] [CrossRef] [PubMed]
- Levy-Clarke, G.; Jabs, D.A.; Read, R.W.; Rosenbaum, J.T.; Vitale, A.; Van Gelder, R.N. Expert Panel Recommendations for the Use of Anti–Tumor Necrosis Factor Biologic Agents in Patients with Ocular Inflammatory Disorders. Ophthalmology 2014, 121, 785–796.e3. [Google Scholar] [CrossRef]
- Dobner, B.C.; Max, R.; Becker, M.D.; Heinz, C.; Veltrup, I.; Heiligenhaus, A.; Barisani-Asenbauer, T.; Mackensen, F. A three-centre experience with adalimumab for the treatment of non-infectious uveitis. Br. J. Ophthalmol. 2012, 97, 134–138. [Google Scholar] [CrossRef]
- Yang, S.; Huang, Z.; Liu, X.; Li, H.; Xie, L.; Chen, X.; Wen, F.; Liang, D.; Su, W. Comparative study of adalimumab versus conventional therapy in sight-threatening refractory Behçet’s uveitis with vasculitis. Int. Immunopharmacol. 2021, 93, 107430. [Google Scholar] [CrossRef]
- Yang, S.; Huang, Z.; Hu, Y.; Zhang, J.; Liu, X.; Li, H.; Xie, L.; Wen, F.; Liang, D.; Su, W. The Efficacy of Adalimumab as an Initial Treatment in Patients with Behçet’s Retinal Vasculitis. Front. Pharmacol. 2021, 12, 609148. [Google Scholar] [CrossRef]
- Yang, S.; Tao, T.; Huang, Z.; Liu, X.; Li, H.; Xie, L.; Wen, F.; Chi, W.; Su, W. Adalimumab in Vogt-Koyanagi-Harada Disease Refractory to Conventional Therapy. Front. Med. 2022, 8, 799427. [Google Scholar] [CrossRef]
- Yang, S.; Tao, T.; Li, Z.; Chen, B.; Huang, Z.; Liu, X.; Li, H.; Xie, L.; Feng, W.; Su, W. Systemic glucocorticoid-free therapy with adalimumab plus immunosuppressants versus conventional therapy in treatment-naïve Vogt-Koyanagi-Harada disease pa-tients. Ann. Transl. Med. 2022, 10, 699. [Google Scholar] [CrossRef] [PubMed]
- Bawazeer, A.M.; Raffa, L. Adalimumab in the treatment of recurrent idiopathic bilateral nodular scleritis. Oman J. Ophthalmol. 2011, 4, 139–141. [Google Scholar] [CrossRef]
- Akhtar, S.; Babar, S.; Lightman, S.; Mason, J.C. Adalimumab-induced remission of anterior scleritis: A very rare late mani-festation of Takayasu arteritis. Rheumatology 2015, 54, 2288–2290. [Google Scholar] [CrossRef][Green Version]
- Durrani, K.; Kempen, J.H.; Ying, G.-S.; Kacmaz, R.O.; Artornsombudh, P.; Rosenbaum, J.T.; Suhler, E.B.; Thorne, J.E.; Jabs, D.A.; Levy-Clarke, G.A.; et al. Adalimumab for Ocular Inflammation. Ocul. Immunol. Inflamm. 2016, 25, 405–412. [Google Scholar] [CrossRef]
- Huynh, N.; Cervantes-Castañeda, R.A.; Bhat, P.; Gallagher, M.J.; Foster, C.S. Biologic Response Modifier Therapy for Psoriatic Ocular Inflammatory Disease. Ocul. Immunol. Inflamm. 2008, 16, 89–93. [Google Scholar] [CrossRef] [PubMed]
- Sharma, S.M.; Damato, E.; Hinchcliffe, E.A.; Andrews, C.D.; Myint, K.; Lee, R.; Dick, A.D. Long-term efficacy and tolerability of TNFα inhibitors in the treatment of non-infectious ocular inflammation: An 8-year prospective surveillance study. Br. J. Ophthalmol. 2019, 105, 1256–1262. [Google Scholar] [CrossRef] [PubMed]
- Biswas, J.; Sadhu, S.; Majumder, P.D. Biological therapy in refractory cases of uveitis and scleritis: An analysis of 18 cases from a tertiary eye care center from South India. Indian J. Ophthalmol. 2020, 68, 1929–1933. [Google Scholar] [CrossRef]
- Ragam, A.; Kolomeyer, A.M.; Fang, C.; Xu, Y.; Chu, D.S. Treatment of Chronic, Noninfectious, Nonnecrotizing Scleritis with Tumor Necrosis Factor Alpha Inhibitors. Ocul. Immunol. Inflamm. 2013, 22, 469–477. [Google Scholar] [CrossRef]
- Suhler, E.B.; Lim, L.L.; Beardsley, R.M.; Giles, T.R.; Pasadhika, S.; Lee, S.T.; de Saint Sardos, A.; Butler, N.J.; Smith, J.R.; Rosenbaum, J.T. Rituximab therapy for refractory scleritis: Results of a phase I/II dose-ranging, randomized, clinical trial. Ophthalmology 2014, 121, 1885–1891. [Google Scholar] [CrossRef]
- Sen, H.N.; Sangave, A.A.; Goldstein, D.A.; Suhler, E.B.; Cunningham, D.; Vitale, S.; Nussenblatt, R.B. A Standardized Grading System for Scleritis. Ophthalmology 2011, 118, 768–771. [Google Scholar] [CrossRef]
- Fabiani, C.; Sota, J.; Sainz-De-La-Maza, M.; Pelegrín, L.; Emmi, G.; Lopalco, G.; Iannone, F.; Vannozzi, L.; Guerriero, S.; Frediani, B.; et al. Effectiveness of TNF-α blockade in the treatment of refractory non-infectious scleritis: A multicentre study. Clin. Exp. Rheumatol. 2020, 38, 1138–1144. [Google Scholar] [PubMed]
- Benson, W.E. Posterior scleritis. Surv. Ophthalmol. 1988, 32, 297–316. [Google Scholar] [CrossRef]
- Burmester, G.R.; Panaccione, R.; Gordon, K.B.; McIlraith, M.J.; Lacerda, A.P.M. Adalimumab: Long-term safety in 23 458 patients from global clinical trials in rheumatoid arthritis, juvenile idiopathic arthritis, ankylosing spondylitis, psoriatic arthritis, psoriasis and Crohn′s disease. Ann. Rheum. Dis. 2012, 72, 517–524. [Google Scholar] [CrossRef] [PubMed]
| Characteristic | CT | ACT | p-Value |
|---|---|---|---|
| Number of patients | 9 | 9 | |
| Number of eyes | 11 | 12 | |
| Male, n (%) | 3 (33.3%) | 4 (44.4%) | 1 |
| Age at onset, mean ± SD (years) | 38.44 ± 10.806 | 31.22 ± 15.328 | 0.265 |
| Interval before baseline, mean ± SD (months) | 13.56 ± 9.774 | 7.89 ± 4.512 | 0.142 |
| Site of scleritis, n (%) | 0.149 | ||
| Anterior scleritis | 8 | 5 | |
| Posterior scleritis | 0 | 2 | |
| Panscleritis | 1 | 2 | |
| Binocular, n (%) | 2(22.2%) | 3 (33.3%) | 1 |
| Sytemic immune-related diseases, n (%) | 2 (22.2%) | 1 (11.1%) | 1 |
| Follow-up duration, mean ± SD (months) | 13 ± 5.937 | 12.11 ± 3.655 | 0.708 |
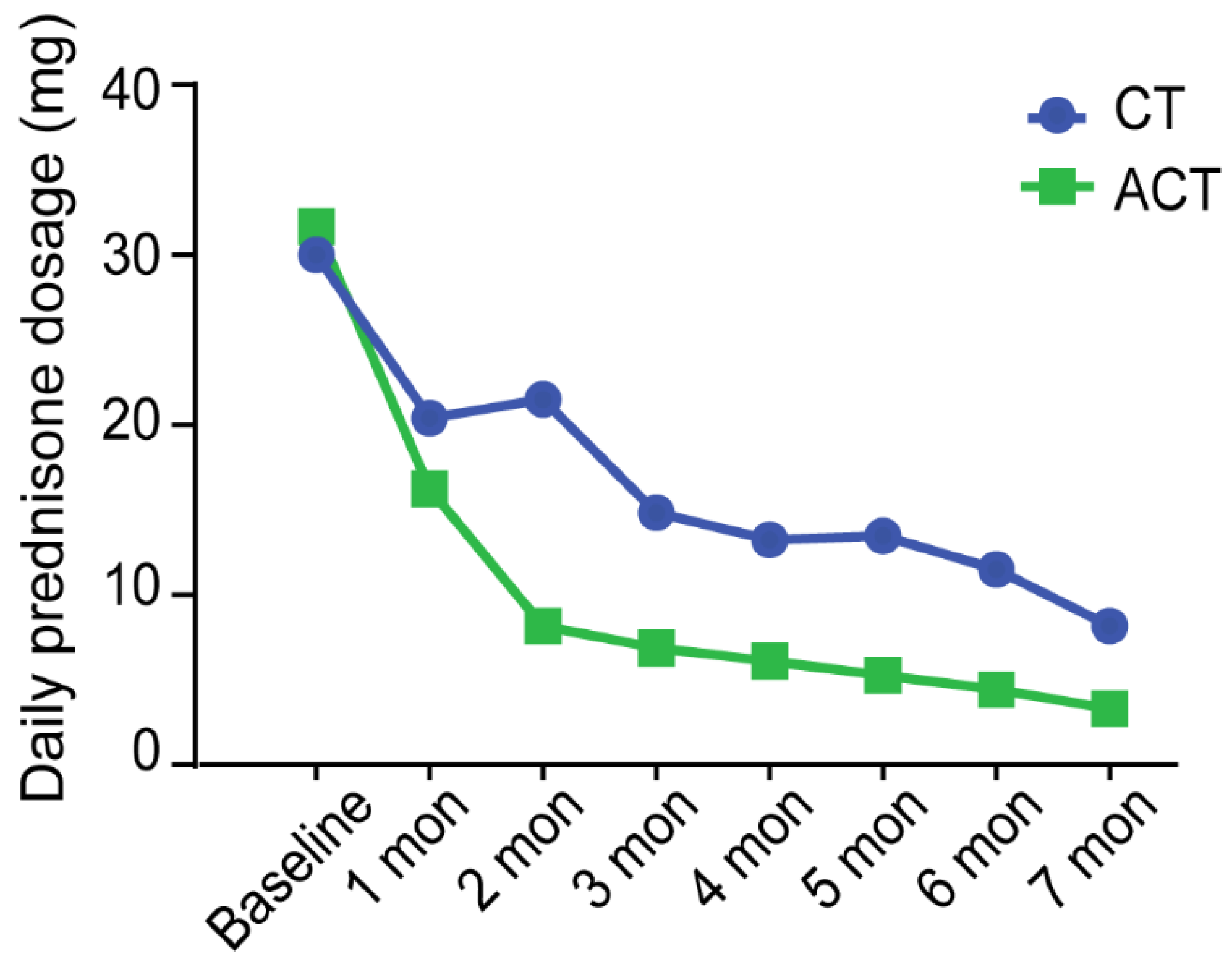
| Baseline oral GC dosage, mean ± SD (mg/day) | 30 ± 5.449 | 31.67 ± 24.206 | 0.845 |
| Baseline concomitant immunomodulators | 0.71 | ||
| MTX | 6 | 8 | |
| CsA | 5 | 8 | |
| MMF | 3 | 2 |
| Outcome Measures | CT | ACT | p-Value |
|---|---|---|---|
| Baseline McCluskey’s scores, mean ± SD | 8 ± 2.569 | 8.42 ± 2.392 | 0.691 |
| McCluskey’s scores at the last visit, median (IQR) | 2 (2,6) | 0 (0, 1.75) | 0.032 |
| Changes in McCluskey’s scores, mean ± SD | −4.364 ± 2.618 | −7.25 ± 2.734 | 0.017 |
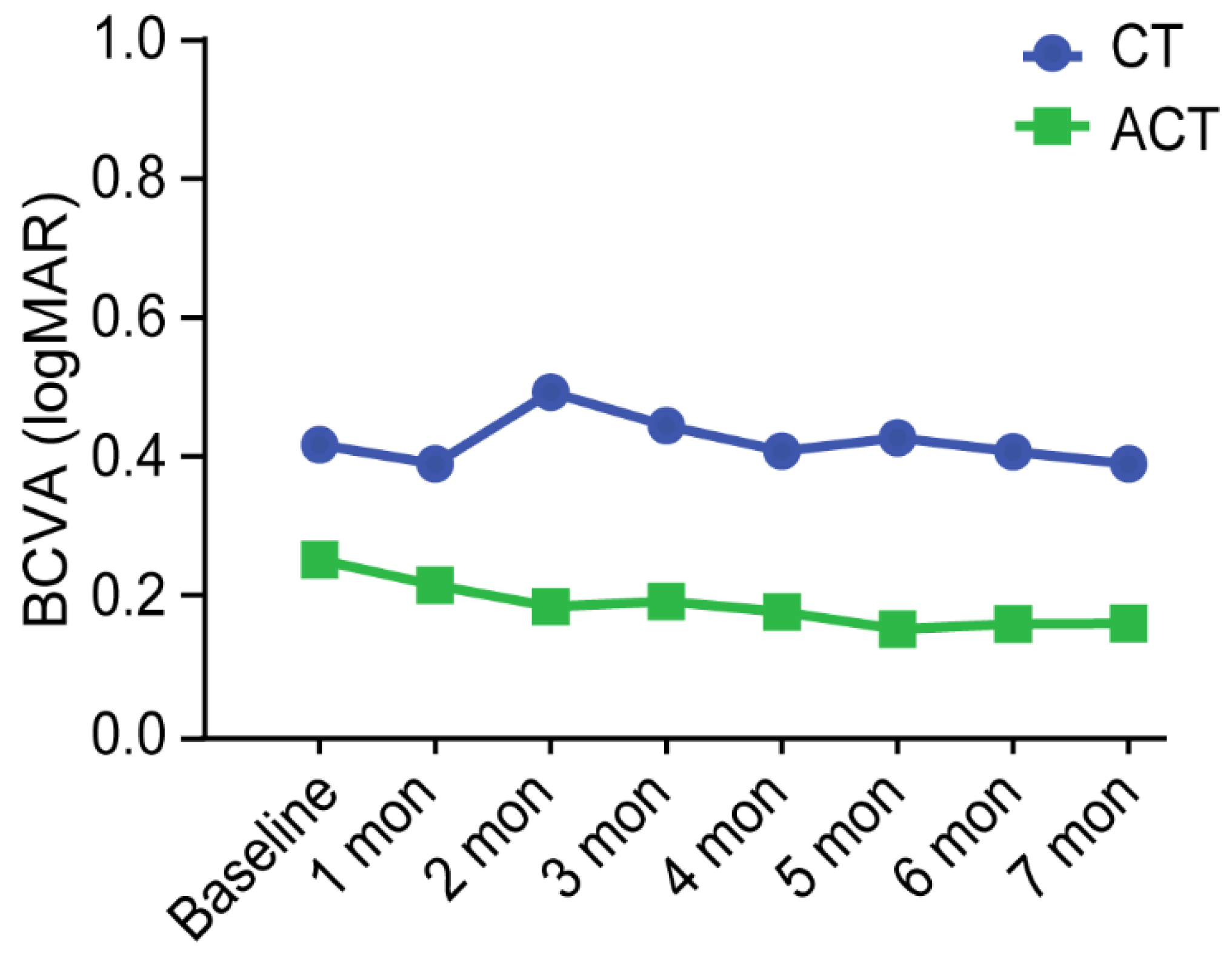
| logMAR BCVA, median (IQR) | 0.201 (0.097, 0.398) | 0.097 (0, 0.374) | 0.26 |
| logMAR BCVA at the last visit, median (IQR) | 0.201 (0.097, 0.699) | 0.048 (0, 0.301) | 0.134 |
| Changes in logMAR BCVA, median (IQR) | 0 (−0.201, 0.104) | −0.049 (−0.097, 0) | 0.651 |
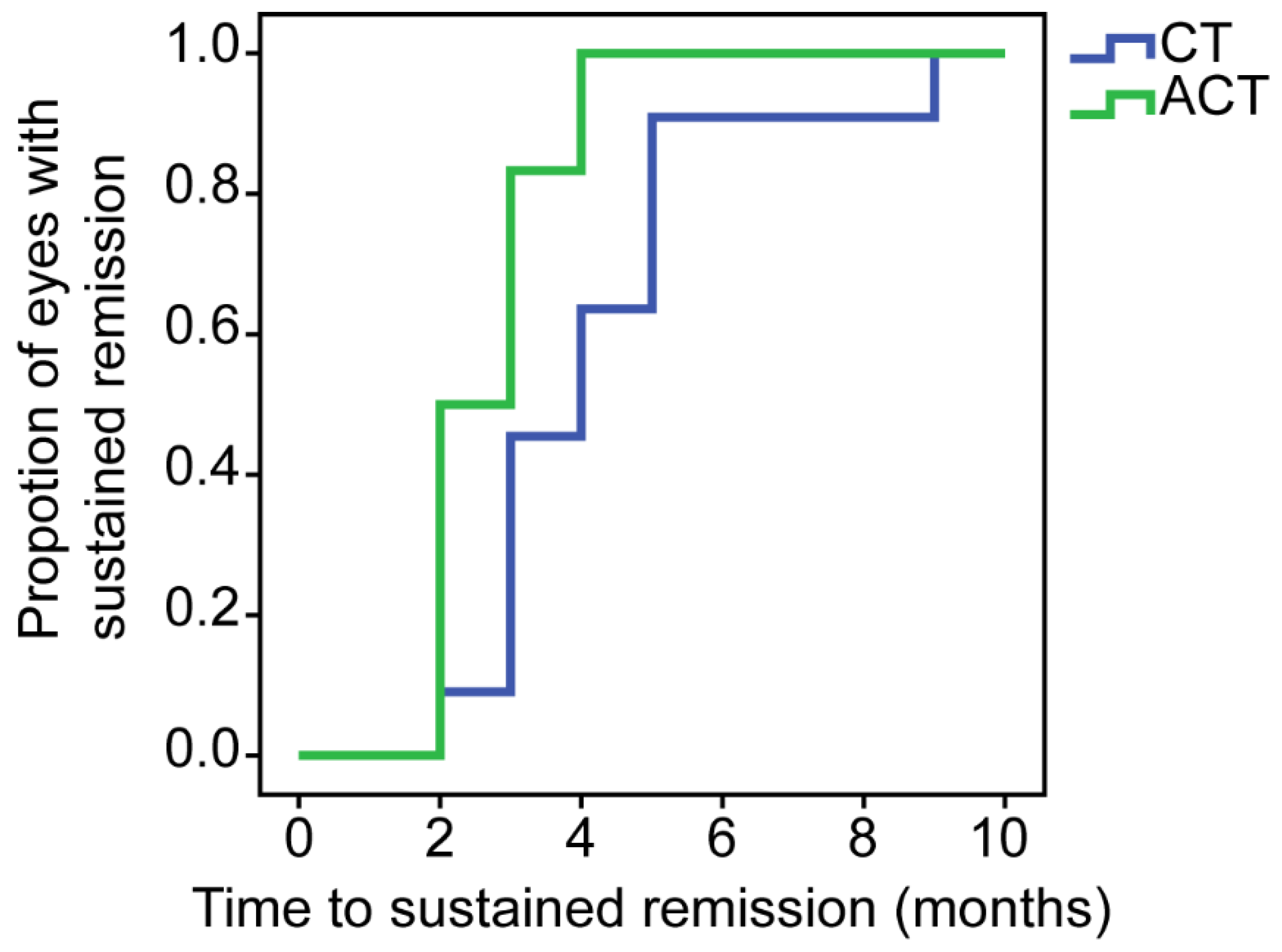
| Eyes with sustained remission, n (%) | 11 (100%) | 12 (100%) | |
| Time to achieve sustained remission, median (IQR), months | 4 (3, 5) | 2.5 (2, 3) | 0.016 |
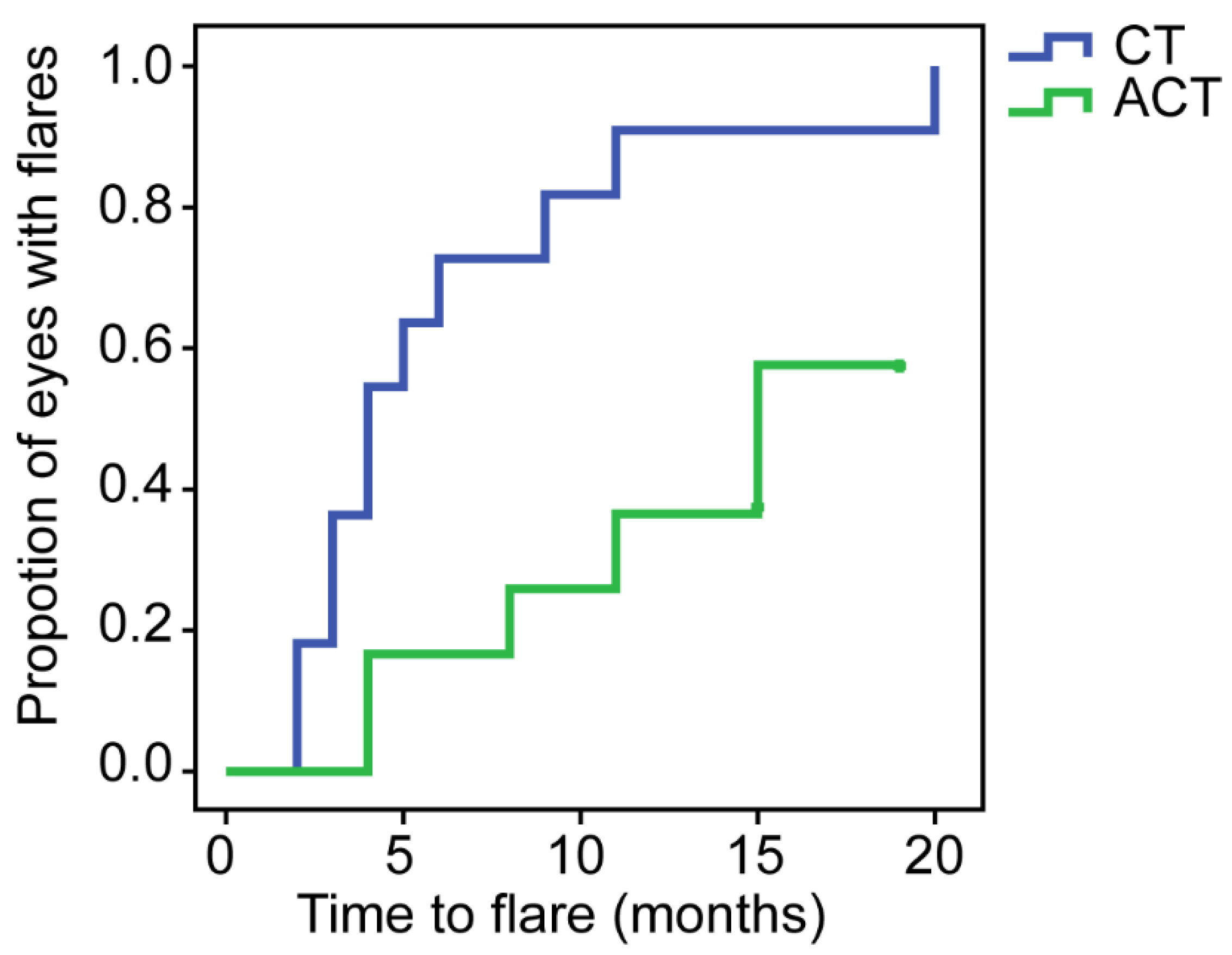
| Eyes with flares, n (%) | 11 (100%) | 5 (41.67%) | 0.005 |
| Time to first flare, median (IQR), months | 4 (3, 9) | 11.5 (7.25, 14.75) | 0.019 |
| Flare times per eye per month, median (IQR) | 0.125 (0.091, 0.143) | 0 (0, 0.083) | 0 |
| Flare times per eye, median (IQR) | 1 (1, 1) | 0 (0, 1) | 0.006 |
| Documented Adverse Events | CT | ACT |
|---|---|---|
| Any adverse event | 0 | 3 |
| Adverse event leading to death | 0 | 0 |
| Adverse event leading to discontinuation of study drug | 0 | 0 |
| Injection-site reactions | 0 | 1 |
| Malignancies | 0 | 0 |
| Opportunistic infections | 0 | 0 |
| Demyelinating disease | 0 | 0 |
| Lupus-like reaction | 0 | 0 |
| Erythema multiforme-like skin reactions | 0 | 1 |
| Joint pain | 0 | 1 |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2022 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Chen, B.; Yang, S.; Zhu, L.; Peng, X.; He, D.; Tao, T.; Su, W. Adalimumab plus Conventional Therapy versus Conventional Therapy in Refractory Non-Infectious Scleritis. J. Clin. Med. 2022, 11, 6686. https://doi.org/10.3390/jcm11226686
Chen B, Yang S, Zhu L, Peng X, He D, Tao T, Su W. Adalimumab plus Conventional Therapy versus Conventional Therapy in Refractory Non-Infectious Scleritis. Journal of Clinical Medicine. 2022; 11(22):6686. https://doi.org/10.3390/jcm11226686
Chicago/Turabian StyleChen, Binyao, Shizhao Yang, Lei Zhu, Xuening Peng, Daquan He, Tianyu Tao, and Wenru Su. 2022. "Adalimumab plus Conventional Therapy versus Conventional Therapy in Refractory Non-Infectious Scleritis" Journal of Clinical Medicine 11, no. 22: 6686. https://doi.org/10.3390/jcm11226686
APA StyleChen, B., Yang, S., Zhu, L., Peng, X., He, D., Tao, T., & Su, W. (2022). Adalimumab plus Conventional Therapy versus Conventional Therapy in Refractory Non-Infectious Scleritis. Journal of Clinical Medicine, 11(22), 6686. https://doi.org/10.3390/jcm11226686









