Pulmonary Embolism Presenting with Pulmonary Infarction: Update and Practical Review of Literature Data
Abstract
:1. Introduction
2. Epidemiology
3. Physiopathology
4. Possible Diagnostic Criteria
4.1. Signs and Symptoms of Pulmonary Infarction
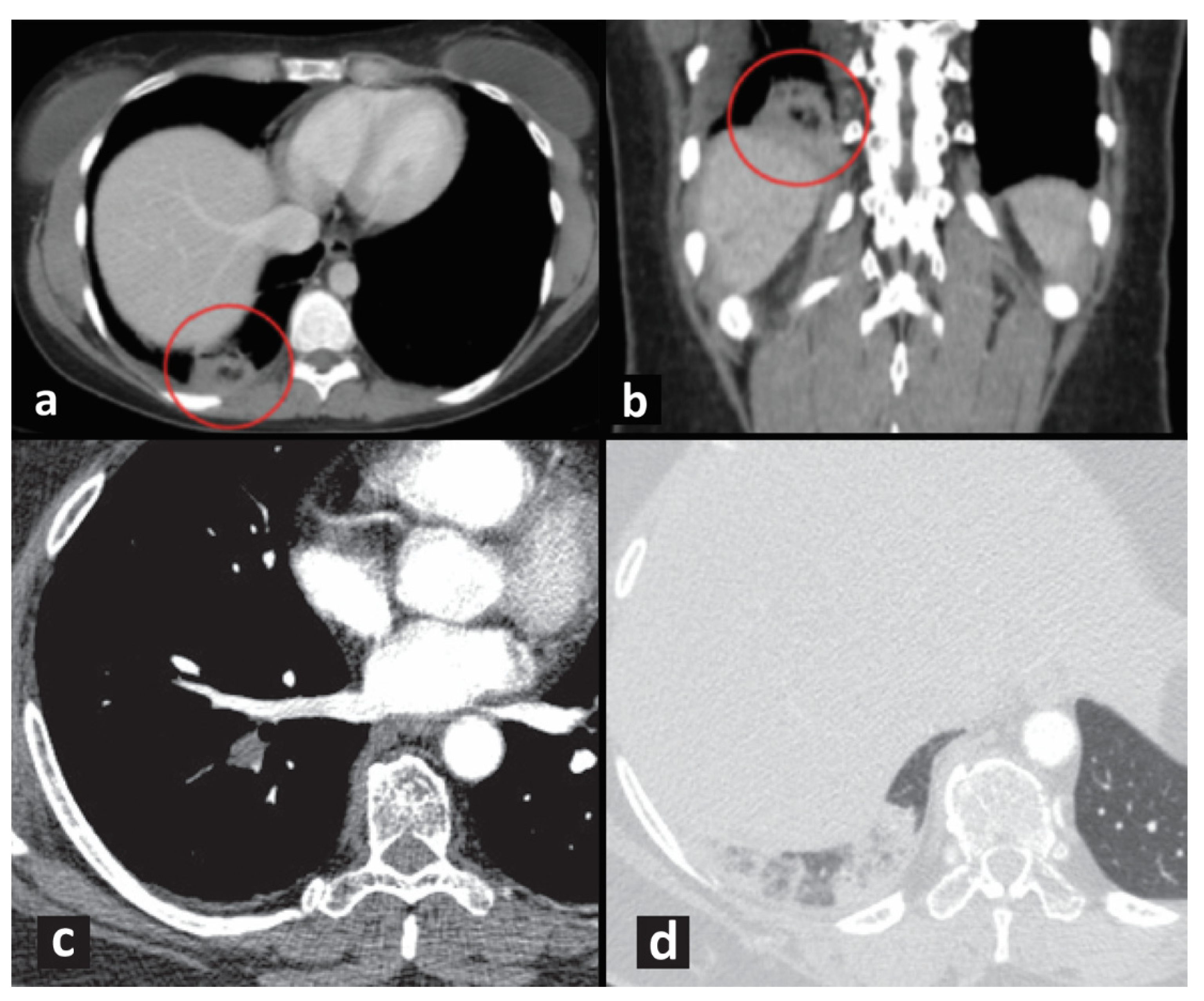
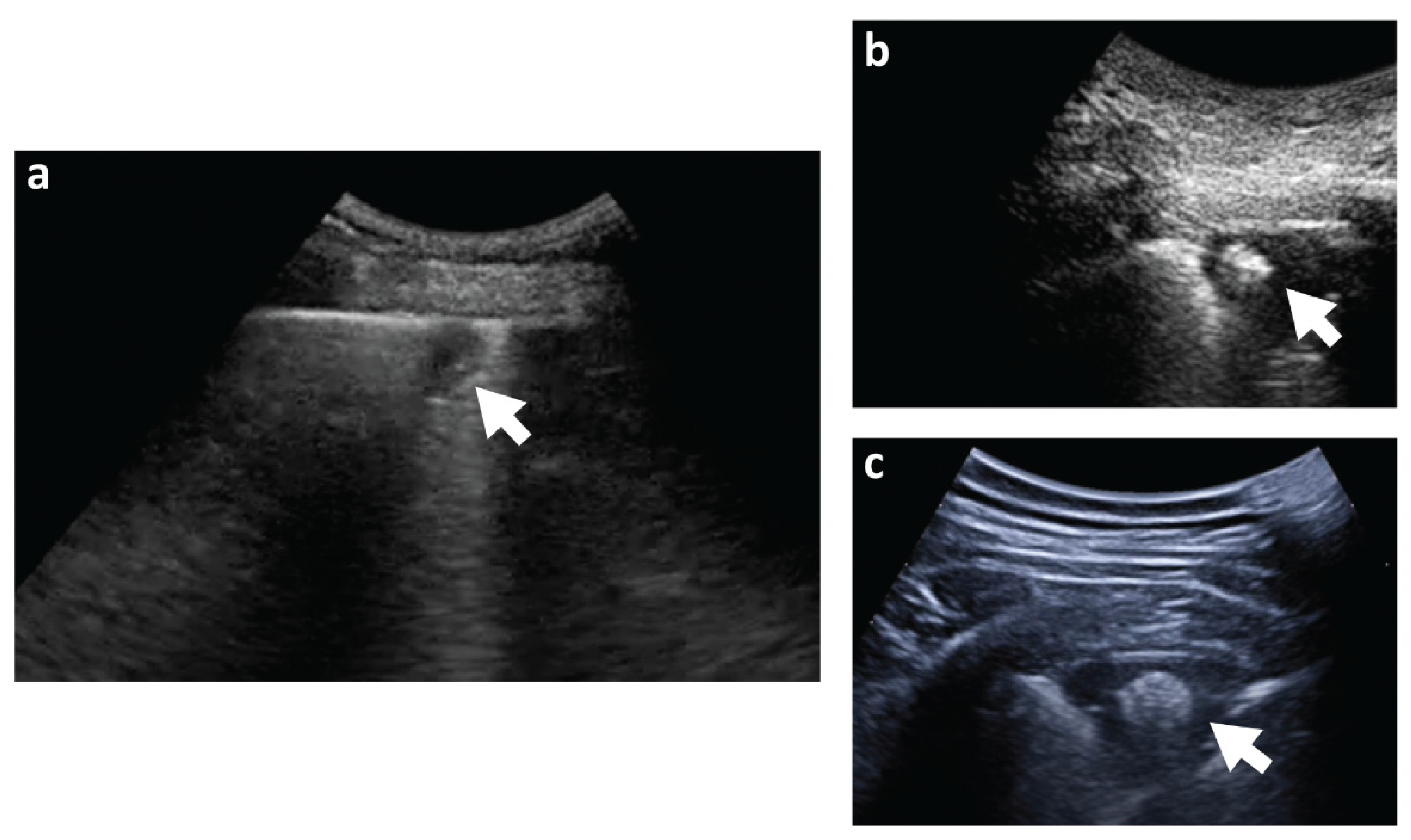
4.2. Imaging Techniques for the Diagnosis of Pulmonary Infarction
4.3. Molecular Diagnosis
5. Clinical Management and Prognostic Implication
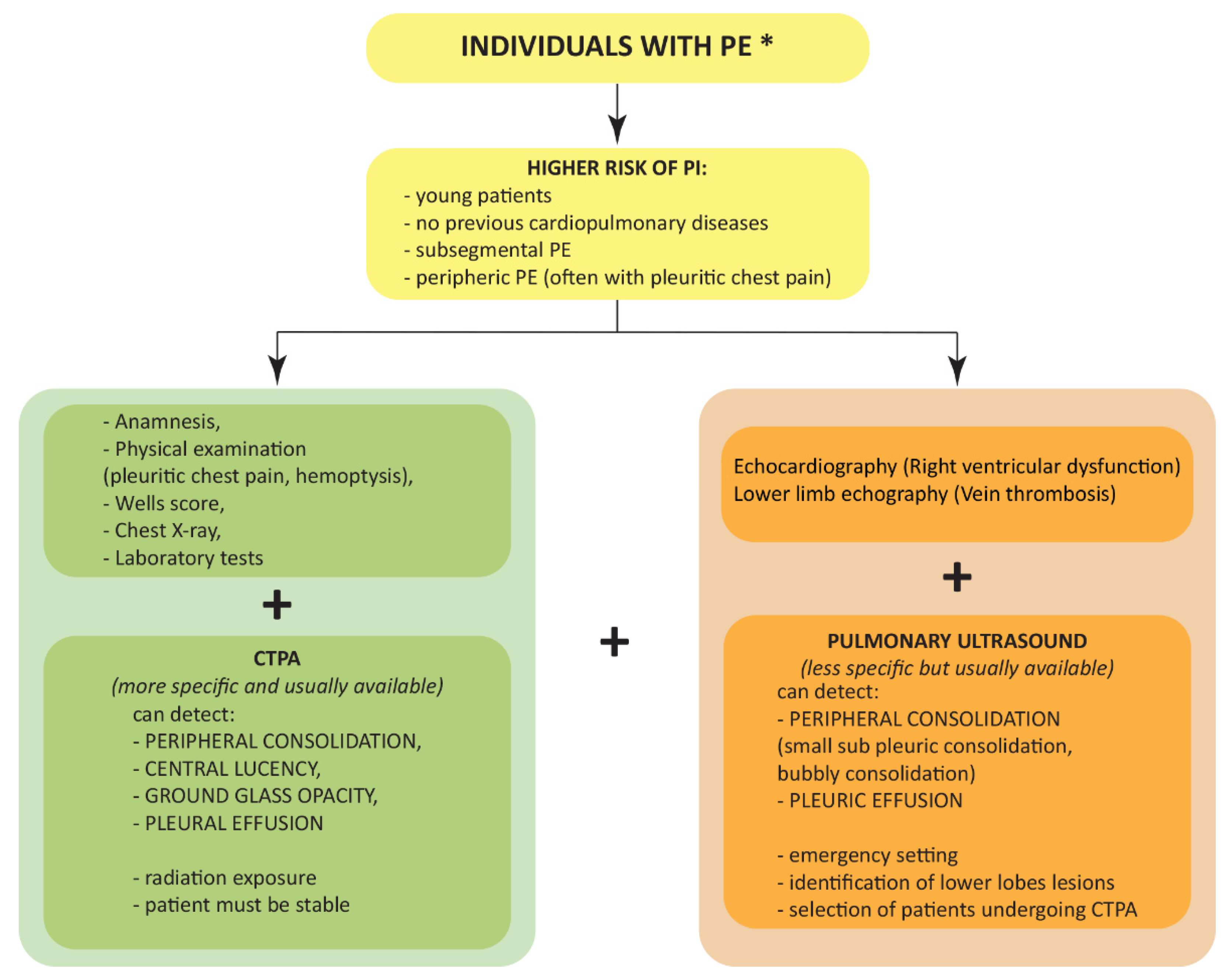
6. Pulmonary Infarction: What Are the Prospects for the Diagnostic Algorithm?
7. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Conflicts of Interest
References
- Kaptein, F.H.J.; Kroft, L.J.M.; Hammerschlag, G.; Ninaber, M.K.; Bauer, M.P.; Huisman, M.V.; Klok, F.A. Pulmonary infarction in acute pulmonary embolism. Thromb. Res. 2021, 202, 162–169. [Google Scholar] [CrossRef] [PubMed]
- Kirchner, J.; Obermann, A.; Stuckradt, S.; Tushaus, C.; Goltz, J.; Liermann, D.; Kickuth, R. Lung Infarction Following Pulmonary Embolism: A Comparative Study on Clinical Conditions and CT Findings to Identify Predisposing Factors. Rofo 2015, 187, 440–444. [Google Scholar] [CrossRef] [PubMed]
- Islam, M.; Filopei, J.; Frank, M.; Ramesh, N.; Verzosa, S.; Ehrlich, M.; Bondarsky, E.; Miller, A.; Steiger, D. Pulmonary infarction secondary to pulmonary embolism: An evolving paradigm. Respirology 2018, 23, 866–872. [Google Scholar] [CrossRef]
- Tapson, V.F. Pulmonary infarction: A disease of the (mostly) young. Respirology 2018, 23, 805–806. [Google Scholar] [CrossRef] [PubMed]
- Zanon, M.; Valentinuz, E.; Montanaro, M.; Radaelli, D.; Manfredi, A.; Bonuccelli, D.; Martelloni, M.; D’Errico, S. Is hospital autopsy auditing suitable for clinical risk management? Actualities and perspectives of auditing in the autopsy room following Italian Law 24/2017 on patient safety. Curr. Pharm. Biotechnol. 2020, 22, 1964–1970. [Google Scholar] [CrossRef]
- Parambil, J.G.; Savci, C.D.; Tazelaar, H.D.; Ryu, J.H. Causes and presenting features of pulmonary infarctions in 43 cases identified by surgical lung biopsy. Chest 2005, 127, 1178–1183. [Google Scholar] [CrossRef]
- Miniati, M.; Bottai, M.; Ciccotosto, C.; Roberto, L.; Monti, S. Predictors of Pulmonary Infarction. Medicine 2015, 94, e1488. [Google Scholar] [CrossRef] [PubMed]
- Chengsupanimit, T.; Sundaram, B.; Lau, W.B.; Keith, S.W.; Kane, G.C. Clinical characteristics of patients with pulmonary infarction—A retrospective review. Respir. Med. 2018, 139, 13–18. [Google Scholar] [CrossRef]
- Mordeglia, F.; Ríos, J.; Dutrey, D.; Bengolea, A. Anatomoclinical study of pulmonary embolism in patients with or without pulmonary infarction. Medicina 1965, 25, 360–368. [Google Scholar]
- Konstantinides, S.V.; Meyer, G.; Becattini, C.; Bueno, H.; Geersing, G.J.; Harjola, V.P.; Huisman, M.V.; Humbert, M.; Jennings, C.S.; Jimenez, D.; et al. 2019 ESC Guidelines for the diagnosis and management of acute pulmonary embolism developed in collaboration with the European Respiratory Society (ERS). Eur. Heart J. 2020, 41, 543–603. [Google Scholar] [CrossRef] [Green Version]
- Lee, J.S.; Moon, T.; Kim, T.H.; Kim, S.Y.; Choi, J.Y.; Lee, K.B.; Kwon, Y.J.; Song, S.H.; Kim, S.H.; Kim, H.O.; et al. Deep Vein Thrombosis in Patients with Pulmonary Embolism: Prevalance, Clinical Significance and Outcome. Vasc. Specialist Int. 2016, 32, 166–174. [Google Scholar] [CrossRef] [PubMed]
- Cao, Y.; Geng, C.; Li, Y.; Zhang, Y. In situ Pulmonary Artery Thrombosis: A Previously Overlooked Disease. Front Pharmacol. 2021, 12, 671589. [Google Scholar] [CrossRef] [PubMed]
- Kim, N.H.; Delcroix, M.; Jais, X.; Madani, M.M.; Matsubara, H.; Mayer, E.; Ogo, T.; Tapson, V.F.; Ghofrani, H.A.; Jenkins, D.P. Chronic thromboembolic pulmonary hypertension. Eur. Respir. J. 2019, 53, 1801915. [Google Scholar] [CrossRef]
- Tsao, M.S.; Schraufnagel, D.; Wang, N.S. Pathogenesis of pulmonary infarction. Am. J. Med. 1982, 72, 599–606. [Google Scholar] [CrossRef]
- Terry, P.B.; Buescher, P.C. Pulmonary Infarction: In the Beginning: The Natural History of Pulmonary Infarction. Chest 2017, 152, 1135–1139. [Google Scholar] [CrossRef]
- Emerling, A.; Cook, J. Pulmonary Infarction; StatPearls: Treasure Island, FL, USA, 2021. [Google Scholar]
- Tapson, V.F. Acute pulmonary embolism. N. Engl. J. Med. 2008, 358, 1037–1052. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Zhou, X.; Hou, G. A radiomics nomogram based on CT pulmonary angiographic data for predicting adverse outcomes in non-high-risk acute pulmonary embolism patients. Eur. Respir. J. 2018, 52, OA3596. [Google Scholar] [CrossRef]
- Gao, L.; Li, Y.; Zhai, Z.; Liang, T.; Zhang, Q.; Xie, S.; Chen, H. Radiomics study on pulmonary infarction mimicking community-acquired pneumonia. Clin. Respir. J. 2021, 15, 661–669. [Google Scholar] [CrossRef]
- Sin, D.; McLennan, G.; Rengier, F.; Haddadin, I.; Heresi, G.A.; Bartholomew, J.R.; Fink, M.A.; Thompson, D.; Partovi, S. Acute pulmonary embolism multimodality imaging prior to endovascular therapy. Int. J. Cardiovasc. Imaging 2021, 37, 343–358. [Google Scholar] [CrossRef]
- Farag, A.; Fielding, J.; Catanzano, T. Role of Dual-energy Computed Tomography in Diagnosis of Acute Pulmonary Emboli, a Review. Semin. Ultrasound CT MR 2022, 43, 333–343. [Google Scholar] [CrossRef]
- Palm, V.; Rengier, F.; Rajiah, P.; Heussel, C.P.; Partovi, S. Acute Pulmonary Embolism: Imaging Techniques, Findings, Endovascular Treatment and Differential Diagnoses. Rofo 2020, 192, 38–49. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Bray, T.J.P.; Mortensen, K.H.; Gopalan, D. Multimodality imaging of pulmonary infarction. Eur. J. Radiol. 2014, 83, 2240–2254. [Google Scholar] [CrossRef] [PubMed]
- Stefanidis, K.; Green, J.; Konstantelou, E.; Robbie, H. Flow artefact mimicking pulmonary embolism in pulmonary hypertension. BMJ Case Rep. 2020, 13, e234652. [Google Scholar] [CrossRef] [Green Version]
- Cano-Espinosa, C.; Cazorla, M.; González, G. Computer Aided Detection of Pulmonary Embolism Using Multi-Slice Multi-Axial Segmentation. Appl. Sci. 2020, 10, 2945. [Google Scholar] [CrossRef]
- Revel, M.P.; Triki, R.; Chatellier, G.; Couchon, S.; Haddad, N.; Hernigou, A.; Danel, C.; Frija, G. Is It possible to recognize pulmonary infarction on multisection CT images? Radiology 2007, 244, 875–882. [Google Scholar] [CrossRef] [PubMed]
- Dandamudi, S.; Palaparti, R.; Chowdary, P.; Kondru, P.; Palaparthi, S.; Koduru, G.; Ghanta, S.; Mannuva, B. “Bubbly lung consolidation”—A highly specific imaging marker for pulmonary infarction. J. Dr. NTR Univ. Health Sci. 2020, 9, 273–275. [Google Scholar] [CrossRef]
- Fosmire, S.T.; Gibson, G.N.; Copeland, J.C.; Maydew, M.S.; Eggers, C. Pulmonary Infarction: Right Upper Quadrant Pain as a Presenting Symptom with Review of Typical Computed Tomography Imaging Features. Mil. Med. 2018, 183, e779–e782. [Google Scholar] [CrossRef] [Green Version]
- Copetti, R.; Cominotto, F.; Meduri, S.; Orso, D. The “Survived Lung”: An Ultrasound Sign of “Bubbly Consolidation” Pulmonary Infarction. Ultrasound Med. Biol. 2020, 46, 2546–2550. [Google Scholar] [CrossRef]
- Raheja, R.; Brahmavar, M.; Joshi, D.; Raman, D. Application of Lung Ultrasound in Critical Care Setting: A Review. Cureus 2019, 11, e5233. [Google Scholar] [CrossRef] [Green Version]
- Squizzato, A.; Rancan, E.; Dentali, F.; Bonzini, M.; Guasti, L.; Steidl, L.; Mathis, G.; Ageno, W. Diagnostic accuracy of lung ultrasound for pulmonary embolism: A systematic review and meta-analysis. J. Thromb. Haemost. 2013, 11, 1269–1278. [Google Scholar] [CrossRef]
- Baz, A.A.; Hamdy, I.M.; Mohammed, A.S.; Assal, H.H. Diagnostic validity of thoracic ultrasound in the assessment of pulmonary embolism. Egypt. J. Radiol. Nucl. Med. 2019, 50, 5. [Google Scholar] [CrossRef] [Green Version]
- Kagima, J.; Stolbrink, M.; Masheti, S.; Mbaiyani, C.; Munubi, A.; Joekes, E.; Mortimer, K.; Rylance, J.; Morton, B. Diagnostic accuracy of combined thoracic and cardiac sonography for the diagnosis of pulmonary embolism: A systematic review and meta-analysis. PLoS ONE 2020, 15, e0235940. [Google Scholar] [CrossRef] [PubMed]
- Muhammed Abdelkader, A.A.; Zidan, M.; Eshmawey, H.; Gharraf, H. Study for evaluation of using transthoracic lung ultrasound in diagnosis of pulmonary embolism. Eur. Respir. J. 2021, 58, PA3546. [Google Scholar] [CrossRef]
- Nazerian, P.; Volpicelli, G.; Gigli, C.; Becattini, C.; Sferrazza Papa, G.F.; Grifoni, S.; Vanni, S.; Ultrasound Wells Study, G. Diagnostic Performance of Wells Score Combined with Point-of-care Lung and Venous Ultrasound in Suspected Pulmonary Embolism. Acad Emerg Med. 2017, 24, 270–280. [Google Scholar] [CrossRef] [Green Version]
- Mathis, G.; Blank, W.; Reissig, A.; Lechleitner, P.; Reuss, J.; Schuler, A.; Beckh, S. Thoracic ultrasound for diagnosing pulmonary embolism: A prospective multicenter study of 352 patients. Chest 2005, 128, 1531–1538. [Google Scholar] [CrossRef] [PubMed]
- Squizzato, A.; Galli, L.; Gerdes, V.E. Point-of-care ultrasound in the diagnosis of pulmonary embolism. Crit. Ultrasound J. 2015, 7, 7. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Trenker, C.; Dohse, M.; Ramaswamy, A.; Michel, C.; Gorg, C. Histological validation of pulmonary infarction detected with contrast-enhanced ultrasound in patients with negative computed tomography pulmonary angiogram: A case series. J. Clin. Ultrasound 2019, 47, 461–465. [Google Scholar] [CrossRef]
- Zotzmann, V.; Lang, C.N.; Wengenmayer, T.; Bemtgen, X.; Schmid, B.; Mueller-Peltzer, K.; Supady, A.; Bode, C.; Duerschmied, D.; Staudacher, D.L. Combining lung ultrasound and Wells score for diagnosing pulmonary embolism in critically ill COVID-19 patients. J. Thromb Thrombolysis 2021, 52, 76–84. [Google Scholar] [CrossRef]
- Chen, F.; Shen, Y.H.; Zhu, X.Q.; Zheng, J.; Wu, F.J. Comparison between CT and MRI in the assessment of pulmonary embolism: A meta-analysis. Medicine 2017, 96, e8935. [Google Scholar] [CrossRef]
- Herr, N.; Lombardo, P.; Jackowski, C.; Zech, W.D. Diagnosis of pulmonary infarction in post-mortem computed tomography and post-mortem magnetic resonance imaging-a technical note. Int. J. Legal. Med. 2020, 134, 1817–1821. [Google Scholar] [CrossRef]
- Kluge, A.; Mueller, C.; Strunk, J.; Lange, U.; Bachmann, G. Experience in 207 combined MRI examinations for acute pulmonary embolism and deep vein thrombosis. AJR Am. J. Roentgenol. 2006, 186, 1686–1696. [Google Scholar] [CrossRef] [PubMed]
- Janisset, L.; Castan, M.; Poenou, G.; Lachand, R.; Mismetti, P.; Viallon, A.; Bertoletti, L. Cardiac Biomarkers in Patients with Acute Pulmonary Embolism. Medicina 2022, 58, 541. [Google Scholar] [CrossRef] [PubMed]
- Lorenz, G.; Saeedan, M.B.; Bullen, J.; Klok, F.A.; Kroft, L.J.M.; Meijboom, L.J.; Heresi, G.A.; Sripariwuth, A.; Renapurkar, R.D. CT-Based Biomarkers for Prediction of Chronic Thromboembolic Pulmonary Hypertension After an Acute Pulmonary Embolic Event. AJR Am. J. Roentgenol. 2020, 215, 800–806. [Google Scholar] [CrossRef] [PubMed]
- Sun, H.J.; Wu, Z.Y.; Nie, X.W.; Bian, J.S. Role of Endothelial Dysfunction in Cardiovascular Diseases: The Link Between Inflammation and Hydrogen Sulfide. Front. Pharmacol. 2019, 10, 1568. [Google Scholar] [CrossRef] [Green Version]
- Yang, P.; Li, H.; Zhang, J.; Xu, X. Research progress on biomarkers of pulmonary embolism. Clin. Respir. J. 2021, 15, 1046–1055. [Google Scholar] [CrossRef] [PubMed]
- Reamy, B.V.; Williams, P.M.; Odom, M.R. Pleuritic Chest Pain: Sorting Through the Differential Diagnosis. Am. Fam. Physician 2017, 96, 306–312. [Google Scholar] [PubMed]
- Sonmez, M.; Aboussouan, L.S.; Farver, C.; Murthy, S.C.; Kaw, R. Pulmonary infarction due to pulmonary embolism. Cleve Clin. J. Med. 2018, 85, 848–852. [Google Scholar] [CrossRef] [Green Version]
- Sakuma, M.; Nakamura, M.; Takahashi, T.; Kitamukai, O.; Yazu, T.; Yamada, N.; Ota, M.; Kobayashi, T.; Nakano, T.; Ito, M.; et al. Pulmonary embolism is an important cause of death in young adults. Circ. J. 2007, 71, 1765–1770. [Google Scholar] [CrossRef] [Green Version]
- Felipe, S.; Umaña, S.; Marcela, L.; Gaviria, V.; Garcés Arias, A.; Fernando, A.; Rodriguez-Gutierrez, A.F.; Fernando, D.; Donato, L.; Patino, L.; et al. Infected pulmonary infarction. Case report. Case Rep. 2017, 3, 49–56. [Google Scholar] [CrossRef] [Green Version]
- Wong, D.D.; Ramaseshan, G.; Mendelson, R.M. Comparison of the Wells and Revised Geneva Scores for the diagnosis of pulmonary embolism: An Australian experience. Intern. Med. J. 2011, 41, 258–263. [Google Scholar] [CrossRef]
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2022 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Gagno, G.; Padoan, L.; D’Errico, S.; Baratella, E.; Radaelli, D.; Fluca, A.L.; Pierri, A.; Janjusevic, M.; Aleksova Noveska, E.; Cova, M.A.; et al. Pulmonary Embolism Presenting with Pulmonary Infarction: Update and Practical Review of Literature Data. J. Clin. Med. 2022, 11, 4916. https://doi.org/10.3390/jcm11164916
Gagno G, Padoan L, D’Errico S, Baratella E, Radaelli D, Fluca AL, Pierri A, Janjusevic M, Aleksova Noveska E, Cova MA, et al. Pulmonary Embolism Presenting with Pulmonary Infarction: Update and Practical Review of Literature Data. Journal of Clinical Medicine. 2022; 11(16):4916. https://doi.org/10.3390/jcm11164916
Chicago/Turabian StyleGagno, Giulia, Laura Padoan, Stefano D’Errico, Elisa Baratella, Davide Radaelli, Alessandra Lucia Fluca, Alessandro Pierri, Milijana Janjusevic, Elena Aleksova Noveska, Maria Assunta Cova, and et al. 2022. "Pulmonary Embolism Presenting with Pulmonary Infarction: Update and Practical Review of Literature Data" Journal of Clinical Medicine 11, no. 16: 4916. https://doi.org/10.3390/jcm11164916
APA StyleGagno, G., Padoan, L., D’Errico, S., Baratella, E., Radaelli, D., Fluca, A. L., Pierri, A., Janjusevic, M., Aleksova Noveska, E., Cova, M. A., Copetti, R., Cominotto, F., Sinagra, G., & Aleksova, A. (2022). Pulmonary Embolism Presenting with Pulmonary Infarction: Update and Practical Review of Literature Data. Journal of Clinical Medicine, 11(16), 4916. https://doi.org/10.3390/jcm11164916







