TMJ Position in Symmetric Dentofacial Deformity
Abstract
1. Introduction
2. Materials and Methods
2.1. Mandibular Plane (Angle)
2.2. Gonial Angle
2.3. Joint Space (Sagittal Measurements)
2.4. Joint Space (JS) Average
2.5. Coronal Analysis of the Condyle
2.6. Molar Class
3. Results
4. Discussion
5. Conclusions
Supplementary Materials
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Conflicts of Interest
References
- Lobo, F.; De Souza Tolentino, E.; Iwaki, L.C.V.; Walewski, L.A.; Takeshita, W.M.; Chicarelli, M. Imaginology tridimensional study of temporomandibular joint osseous components according to sagittal skeletal relationship, sex, and age. J. Craniofac. Surg. 2019, 30, 1462–1465. [Google Scholar] [CrossRef] [PubMed]
- Ahmad, M.; Hollender, L.; Anderson, Q.; Kartha, K.; Ohrbach, R.; Truelove, E.L.; John, M.T.; Schiffman, E.L. Research diagnostic criteria for temporomandibular disorders (RDC/TMD): Development of image analysis criteria and examiner reliability for image analysis. Oral Surg. Oral Med. Oral Pathol. Oral Radiol. Endodontol. 2009, 107, 844–860. [Google Scholar] [CrossRef] [PubMed]
- Nur, R.B.; Çakan, D.G.; Arun, T. Evaluation of facial hard and soft tissue asymmetry using cone-beam computed tomography. Am. J. Orthod. Dentofac. Orthop. 2016, 149, 225–237. [Google Scholar] [CrossRef]
- Rodrigues, D.B.; Castro, V. Condylar Hyperplasia of the Temporomandibular Joint. Types, Treatment, and Surgical Implications. Oral Maxillofac. Surg. Clin. N. Am. 2015, 27, 155–167. [Google Scholar] [CrossRef] [PubMed]
- Olate, S.; Cantín, M.; Alister, J.P.; Uribe, F.; Navarro, P.; Olate, G.; de Moraes, M. Relación entre el tamaño condilar y la asimetría facial transversal en individuos con Hiperplasia Condilar. Int. J. Morphol. 2013, 31, 937–941. [Google Scholar] [CrossRef]
- Almăşan, O.C.; Băciuţ, M.; Almăşan, H.A.; Bran, S.; Lascu, L.; Iancu, M.; Băciuţ, G. Skeletal pattern in subjects with temporomandibular joint disorders. Arch. Med. Sci. 2013, 9, 118–126. [Google Scholar] [CrossRef]
- Manfredini, D.; Perinetti, G.; Guarda-Nardini, L. Dental malocclusion is not related to temporomandibular joint clicking: A logistic regression analysis in a patient population. Angle Orthod. 2014, 84, 310–315. [Google Scholar] [CrossRef]
- Manfredini, D.; Perinetti, G.; Stellini, E.; di Leonardo, B.; Guarda-Nardini, L. Prevalence of static and dynamic dental malocclusion features in subgroups of temporomandibular disorder patients: Implications for the epidemiology of the TMD-occlusion association. Quintessence Int. 2015, 46, 341–349. [Google Scholar]
- Manfredini, D.; Segù, M.; Arveda, N.; Lombardo, L.; Siciliani, G.; Rossi, A.; Guarda-Nardini, L. Temporomandibular joint disorders in patients with different facial morphology. A systematic review of the literature. J. Oral Maxillofac. Surg. 2016, 74, 29–46. [Google Scholar] [CrossRef]
- Aboalnaga, A.A.; Amer, N.M.; Elnahas, M.O.; Fayed, M.M.; ElDakroury, A.E.; Labib, A.H.; Fahim, F.H. Malocclusion and Temporomandibular Disorders: Verification of the Controversy. J. Oral Facial Pain Headache 2019, 33, 440–450. [Google Scholar] [CrossRef]
- Amer, N.; Aboalnaga, A.; Fayed, M.; Labib, A. Transverse Malocclusion and Temporomandibular Disorders: Verification of the Controversy. J. Oral Facial Pain Headache 2019, 33, 355–361. [Google Scholar] [CrossRef] [PubMed]
- Fariña, R.; Olate, S.; Raposo, A.; Araya, I.; Alister, J.P.; Uribe, F. High condylectomy versus proportional condylectomy: Is secondary orthognathic surgery necessary? Int. J. Oral Maxillofac. Surg. 2016, 45, 72–77. [Google Scholar] [CrossRef] [PubMed]
- Muñoz, G.; Olate, S.; Cantín, M.; Vasquez, B.; del Sol, M.; Fariña, R. TMJ in facial class III deformity. Condyle/fossa relations. Int. J. Clin. Exp. Med. 2014, 7, 2735–2743. [Google Scholar]
- Vitral, R.W.; Telles, C.d.; Fraga, M.R.; de Oliveira, R.S.M.F.; Tanaka, O.M. Computed tomography evaluation of temporomandibular joint alterations in patients with class II division 1 subdivision malocclusions: Condyle-fossa relationship. Am. J. Orthod. Dentofac. Orthop. 2004, 126, 48–52. [Google Scholar] [CrossRef] [PubMed]
- Fraga, M.R.; Rodrigues, A.F.; Ribeiro, L.C.; Campos, M.J.d.; Vitral, R.W.F. Anteroposterior condylar position: A comparative study between subjects with normal occlusion and patients with Class I, Class II Division 1, and Class III malocclusions. Med. Sci. Monit. 2013, 19, 903–907. [Google Scholar]
- Muñoz, G.; Olate, S.; Cantín, M.; Vásquez, B.; del Sol, M. TMJ in facial class III deformity. Condylar morphology relations. Int. J. Clin. Exp. Med. 2014, 7, 3113–3117. [Google Scholar]
- Larheim, T.A.; Abrahamsson, A.K.; Kristensen, M.; Arvidsson, L.Z. Temporomandibular joint diagnostics using cone beam computed tomography. Dentomaxillofac. Radiol. 2014, 20, 0235. [Google Scholar]
- Yalcin, E.D.; Ararat, E. Cone-Beam Computed Tomography Study of Mandibular Condylar Morphology. J. Craniofacial Surg. 2019, 30, 2621–2624. [Google Scholar] [CrossRef]
- Saccucci, M.; Polimeni, A.; Festa, F.; Tecco, S. Do skeletal cephalometric characteristics correlate with condylar volume, surface and shape? A 3D analysis. Head Face Med. 2012, 8, 15. [Google Scholar] [CrossRef]
- Katsavrias, E.G. Morphology of the temporomandibular joint in subjects with Class II Division 2 malocclusions. Am. J. Orthod. Dentofac. Orthop. 2006, 129, 470–478. [Google Scholar] [CrossRef]
- Kikuchi, K.; Takeuchi, S.; Tanaka, E.; Shibaguchi, T.; Tanne, K. Association between condylar position, joint morphology and craniofacial morphology in orthodontic patients without temporomandibular joint disorders. J. Oral Rehabil. 2003, 30, 1070–1075. [Google Scholar] [CrossRef]
- Paknahad, M.; Shahidi, S.; Abbaszade, H. Correlation between condylar position and sagittal skeletal facial types. J. Orofac. Orthop. 2016, 77, 350–356. [Google Scholar] [CrossRef]
- Paknahad, M.; Shahidi, S. Association between condylar position and vertical skeletal craniofacial morphology: A cone beam computed tomography study. Int. Orthod. 2017, 15, 740–751. [Google Scholar] [CrossRef] [PubMed]
- Santander, P.; Quast, A.; Olbrisch, C.; Rose, M.; Moser, N.; Schliephake, H.; Meyer-Marcotty, P. Comprehensive 3D analysis of condylar morphology in adults with different skeletal patterns—A cross-sectional study. Head Face Med. 2020, 16, 33. [Google Scholar] [CrossRef] [PubMed]
- Goulart, D.R.; Muñoz, P.; Cantín, M.; López, M.G.; de Moraes, M.; Olate, S. Comparative Evaluation of Condylar Volume Between Patients With Unilateral Condylar Hyperplasia and Class III Dentofacial Deformity. J. Oral Maxillofac. Surg. 2017, 75, 180–188. [Google Scholar] [CrossRef] [PubMed][Green Version]
- Goulart, D.R.; Muñoz, P.; Olate, S.; de Moraes, M.; Fariña, R. No differences in morphological characteristics between hyperplastic condyle and class III condyle. Int. J. Oral Maxillofac. Surg. 2015, 44, 1281–1286. [Google Scholar] [CrossRef] [PubMed]
- Rodrigues, A.F.; Fraga, M.R.; Vitral, R.W.F. Computed tomography evaluation of the temporomandibular joint in Class I malocclusion patients: Condylar symmetry and condyle-fossa relationship. Am. J. Orthod. Dentofac. Orthop. 2009, 136, 192–198. [Google Scholar] [CrossRef]
- Merigue, L.F.; Conti, A.C.D.F.; Oltramari-Navarro, P.V.P.; Navarro, R.D.; de Almeida, M.R. Tomographic evaluation of the temporomandibular joint in malocclusion subjects: Condylar morphology and position. Braz. Oral Res. 2016, 30, 1–7. [Google Scholar] [CrossRef] [PubMed]
- Kahn, J.; Tallents, R.H.; Katzberg, R.W.; Ross, M.E.; Murphy, W.C. Prevalence of dental occlusal variables and intraarticular temporomandibular disorders: Molar relationship, lateral guidance, and nonworking side contacts. J. Prosthet. Dent. 1999, 82, 410–415. [Google Scholar] [CrossRef]
- Ebadian, B.; Abbasi, M.; Nazarifar, A. Frequency distribution of temporomandibular disorders according to occlusal factors: A cross-sectional study. Dent. Res. J. 2020, 17, 186–192. [Google Scholar]
- Owtad, P.; Park, J.H.; Shen, G.; Potres, Z.; Darendellier, M.A. The biology of TMJ growth modification: A review. J. Dent. Res. 2013, 92, 315–336. [Google Scholar] [CrossRef] [PubMed]
- Jung, H.D.; Kim, S.Y.; Park, H.S.; Jung, Y.S. Orthognathic surgery and temporomandibular joint symptoms. Maxillofac. Plast. Reconstr. Surg. 2015, 37, 14. [Google Scholar] [CrossRef] [PubMed]
- Iguchi, R.; Yoshizawa, K.; Moroi, A.; Tsutsui, T.; Hotta, A.; Hiraide, R.; Takayama, A.; Tsunoda, T.; Saito, Y.; Sato, M.; et al. Comparison of temporomandibular joint and ramus morphology between class II and class III cases before and after bi-maxillary osteotomy. J. Cranio-Maxillofac. Surg. 2017, 45, 2002–2009. [Google Scholar] [CrossRef] [PubMed]
- Nale, J.C. Orthognathic surgery and the temporomandibular joint patient. Oral Maxillofac. Surg. Clin. N. Am. 2014, 26, 551–564. [Google Scholar] [CrossRef]
- Dolwick, M.F.; Widmer, C.G. Orthognathic Surgery as a Treatment for Temporomandibular Disorders. Oral Maxillofac. Surg. Clin. N. Am. 2018, 30, 303–323. [Google Scholar] [CrossRef]
- Al-Moraissi, E.A.; Wolford, L.M.; Perez, D.; Laskin, D.M.; Ellis, E. Does Orthognathic Surgery Cause or Cure Temporomandibular Disorders? A Systematic Review and Meta-Analysis. J. Oral Maxillofac. Surg. 2017, 75, 1835–1847. [Google Scholar] [CrossRef]
- Möhlhenrich, S.C.; Winterhalder, P.; Ooms, M.; Heitzer, M.; Kilic, K.; Prescher, A.; Hölzle, F.; Danesh, G.; Modabber, A. Changes in the temporomandibular joint position depending on the sagittal osteotomy technique and extent of mandibular movement. Int. J. Oral Maxillofac. Surg. 2020, 50, 356–366. [Google Scholar] [CrossRef]

| Item | Measurement Strategy |
|---|---|
| Mandibular plane | Po-Or/Go-Ch (Normality: 25° ± 4) |
| Gonial angle | J-Go-Ch (Normality: 130° ± 7) |
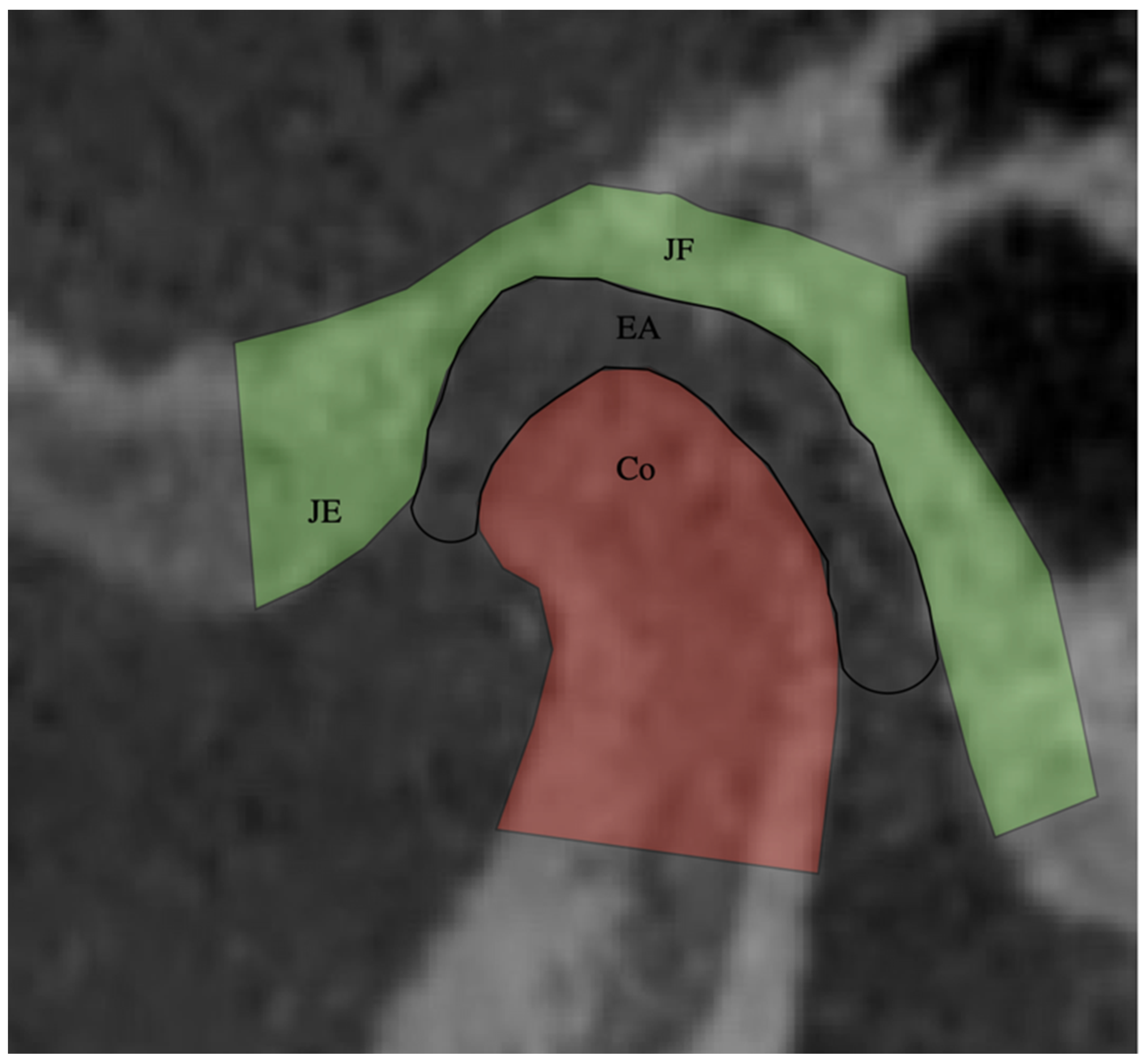
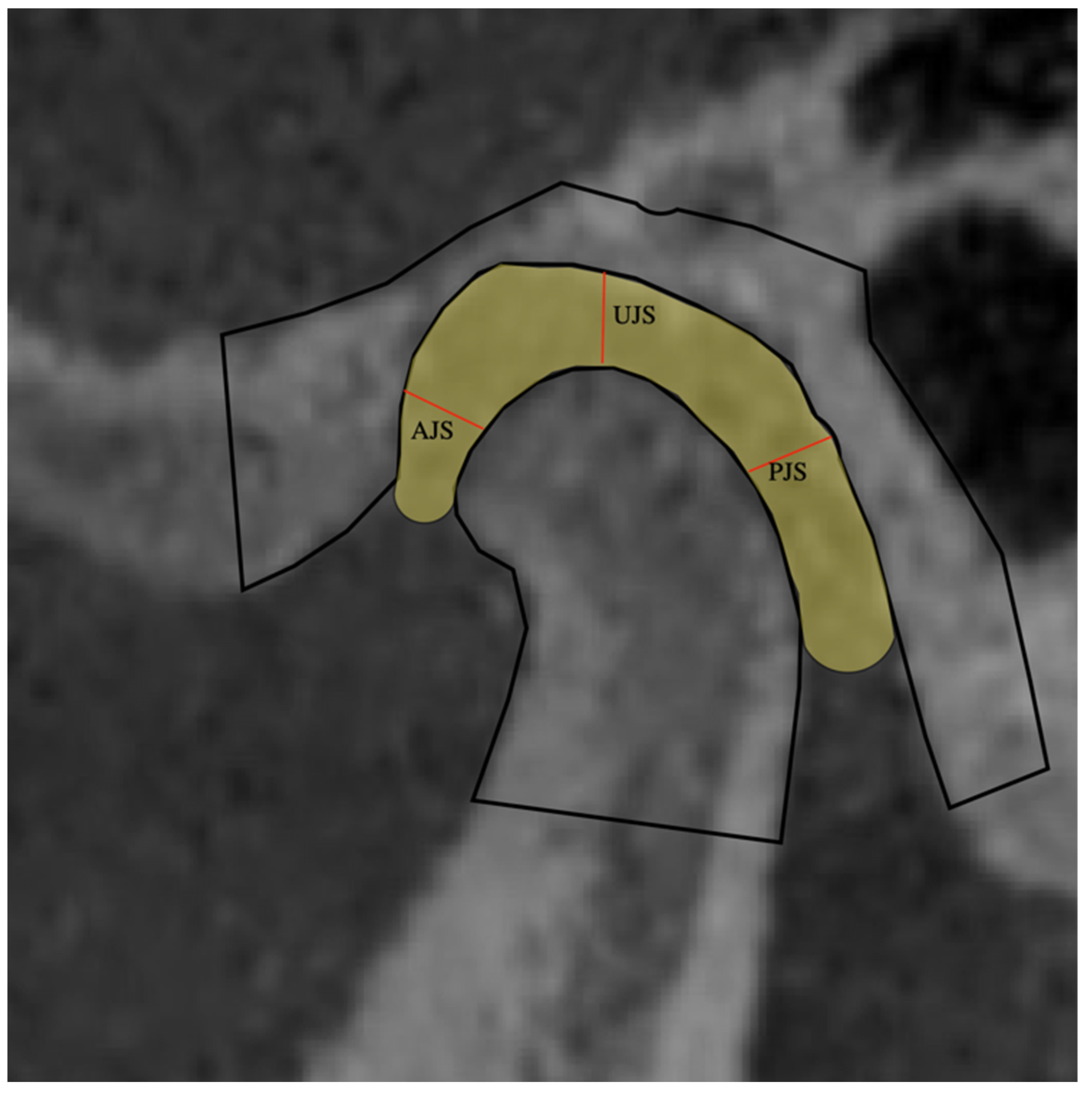
| Anterior Joint Space | Distance between the most anterior point of the condylar surface and the posterior wall of the articular tubercle. |
| Upper joint Space | Distance between the upper point of the condylar surface and the most upper point of the articular fossa. |
| Posterior Joint Space | Distance between the posterior point of the condylar surface and the posterior wall of the articular fossa. |
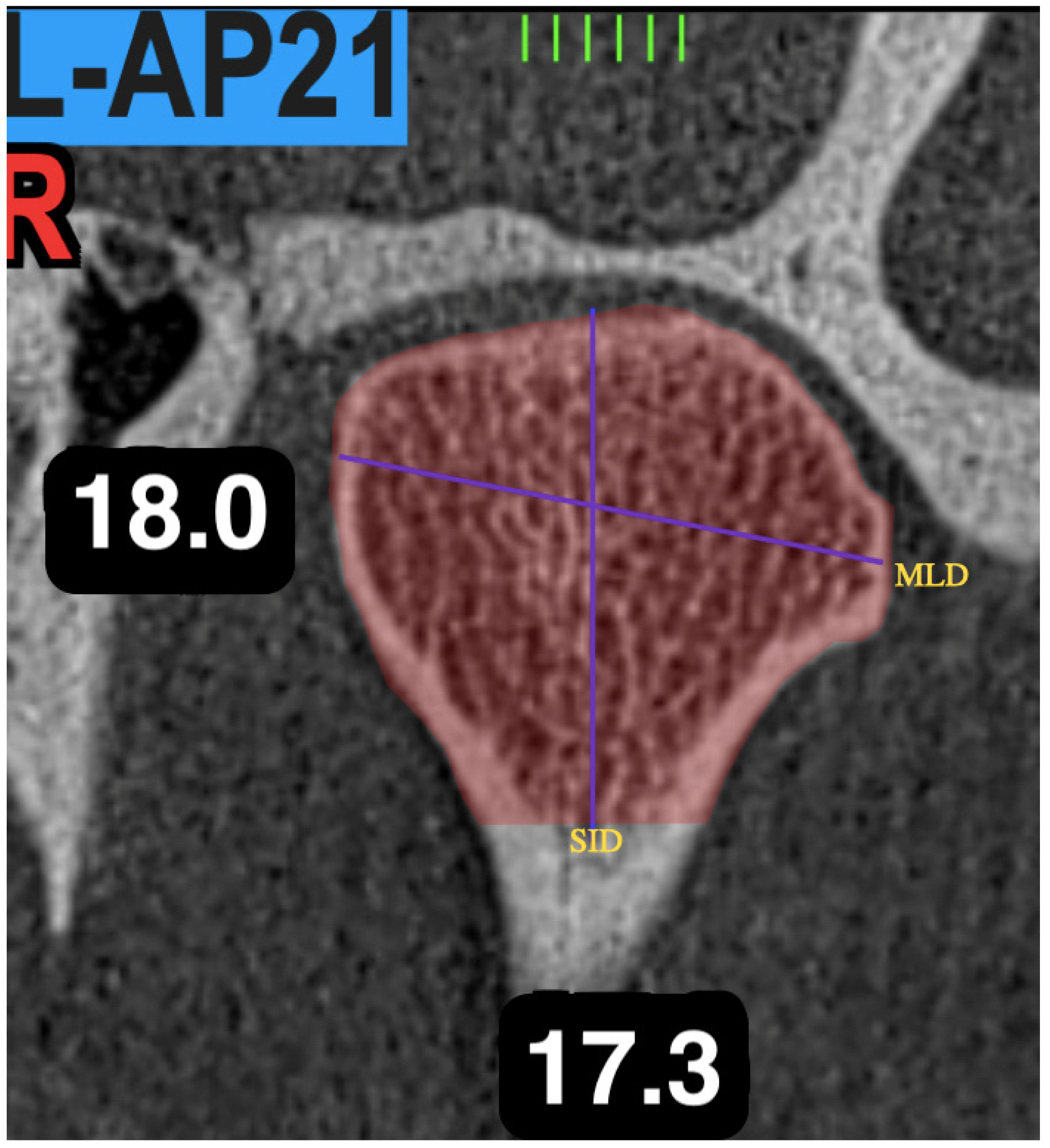
| Mediolateral Distance of the Condyle | Distance between the most medial and most lateral cortical point of the condyle. |
| Vertical Distance of the Condyle | Distance between the highest cortical point and the lowest point of the condylar head |
| Male (n: 36) | Female (n: 53) | ||||||||
|---|---|---|---|---|---|---|---|---|---|
| Right TMJ | Left TMJ | Right TMJ | Left TMJ | ||||||
| X | SD | X | SD | X | SD | X | SD | p Value | |
| AJS | 2.21 mm | 0.88 | 2.32 mm | 4.74 | 2.42 mm | 0.94 | 2.43 mm | 0.93 | 0.12 |
| UJS | 2.75 mm | 1.15 | 2.67 mm | 1.03 | 2.30 mm | 0.96 | 2.42 mm | 0.87 | 0.25 |
| PJS | 2.34 mm | 1.34 | 2.26 mm | 1.25 | 2.55 mm | 1.40 | 2.58 mm | 1.07 | 0.41 |
| MLD | 21.90 mm | 4.67 | 22.07 mm | 4.75 | 19.99 mm | 3.40 | 19.82 mm | 3.74 | 0.009 * |
| VD | 19.37 mm | 4.49 | 20.12 mm | 4.23 | 18.52 mm | 4.22 | 18.57 mm | 4.01 | 0.47 |
| Facial CII (n: 56) | Facial CIII (n: 33) | ||||||||
|---|---|---|---|---|---|---|---|---|---|
| Right TMJ | Left TMJ | Right TMJ | Left TMJ | ||||||
| X | DS | X | DS | X | DS | X | DS | p Value | |
| AJS | 2.34 mm | 0.86 | 2.49 mm | 0.82 | 2.33 mm | 1.03 | 2.43 mm | 1.05 | 0.32 |
| UJS | 2.53 mm | 1.14 | 2.61 mm | 0.98 | 2.35 mm | 0.89 | 2.37 mm | 0.86 | 0.42 |
| PJS | 2.73 mm | 1.48 | 2.58 mm | 1.26 | 1.97 mm | 1.02 | 2.22 mm | 0.90 | 0.12 |
| MLD | 19.43 mm | 3.90 | 19.66 mm | 4.41 | 23.03 mm | 3.24 | 22.55 mm | 3.48 | 0.0001 * |
| VD | 17.07 mm | 4.05 | 17.98 mm | 4.19 | 21.91 mm | 2.86 | 21.27 mm | 3.16 | 0.0001 * |
| CII (n: 56) | CIII (n: 33) | |||||
|---|---|---|---|---|---|---|
| n | % | n | % | p Value | ||
| Mandibular Plane | Low | 2 | 2.24 | 31 | 34.83 | |
| High | 43 | 43.87 | 12 | 13.48 | 0.04 * | |
| Condylar position | Centric | 12 | 12.24 | 6 | 6.12 | |
| Anterior | 27 | 27.55 | 8 | 8.16 | ||
| Posterior | 17 | 17.34 | 19 | 19.38 | 0.03 * | |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2022 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Ravelo, V.; Olate, G.; de Moraes, M.; Guevara, H.G.; Parra, M.; Olate, S. TMJ Position in Symmetric Dentofacial Deformity. J. Clin. Med. 2022, 11, 3631. https://doi.org/10.3390/jcm11133631
Ravelo V, Olate G, de Moraes M, Guevara HG, Parra M, Olate S. TMJ Position in Symmetric Dentofacial Deformity. Journal of Clinical Medicine. 2022; 11(13):3631. https://doi.org/10.3390/jcm11133631
Chicago/Turabian StyleRavelo, Victor, Gabriela Olate, Marcio de Moraes, Henry Garcia Guevara, Marcelo Parra, and Sergio Olate. 2022. "TMJ Position in Symmetric Dentofacial Deformity" Journal of Clinical Medicine 11, no. 13: 3631. https://doi.org/10.3390/jcm11133631
APA StyleRavelo, V., Olate, G., de Moraes, M., Guevara, H. G., Parra, M., & Olate, S. (2022). TMJ Position in Symmetric Dentofacial Deformity. Journal of Clinical Medicine, 11(13), 3631. https://doi.org/10.3390/jcm11133631







