History of Heart Failure in Patients Hospitalized Due to COVID-19: Relevant Factor of In-Hospital Complications and All-Cause Mortality up to Six Months
Abstract
:1. Introduction
2. Materials and Methods
2.1. Study Population
- (a)
- (b)
- Non-HF group: Patients without previous diagnosis of HF.
2.2. End-Points of the Study and Clinical Follow-Up
- (a)
- in-hospital mortality,
- (b)
- duration of hospitalization,
- (c)
- admission to intensive care unit (ICU),
- (d)
- the incidence of complications during hospitalization: shock, myocardial infarc-tion (diagnosed according to Fourth Universal Definition of Myocardial Infarction [27]), thromboembolic disease, stroke, acute HF,
- (e)
- all-cause mortality at six months.
2.3. Study Procedures
2.4. Statistical Analysis
3. Results
3.1. Characteristic of Study Population and Difference between Patients with a History of HF and without HF
3.2. The Association of HF History with In-Hospital Course and Applied Treatment and Procedures during Hospitalization
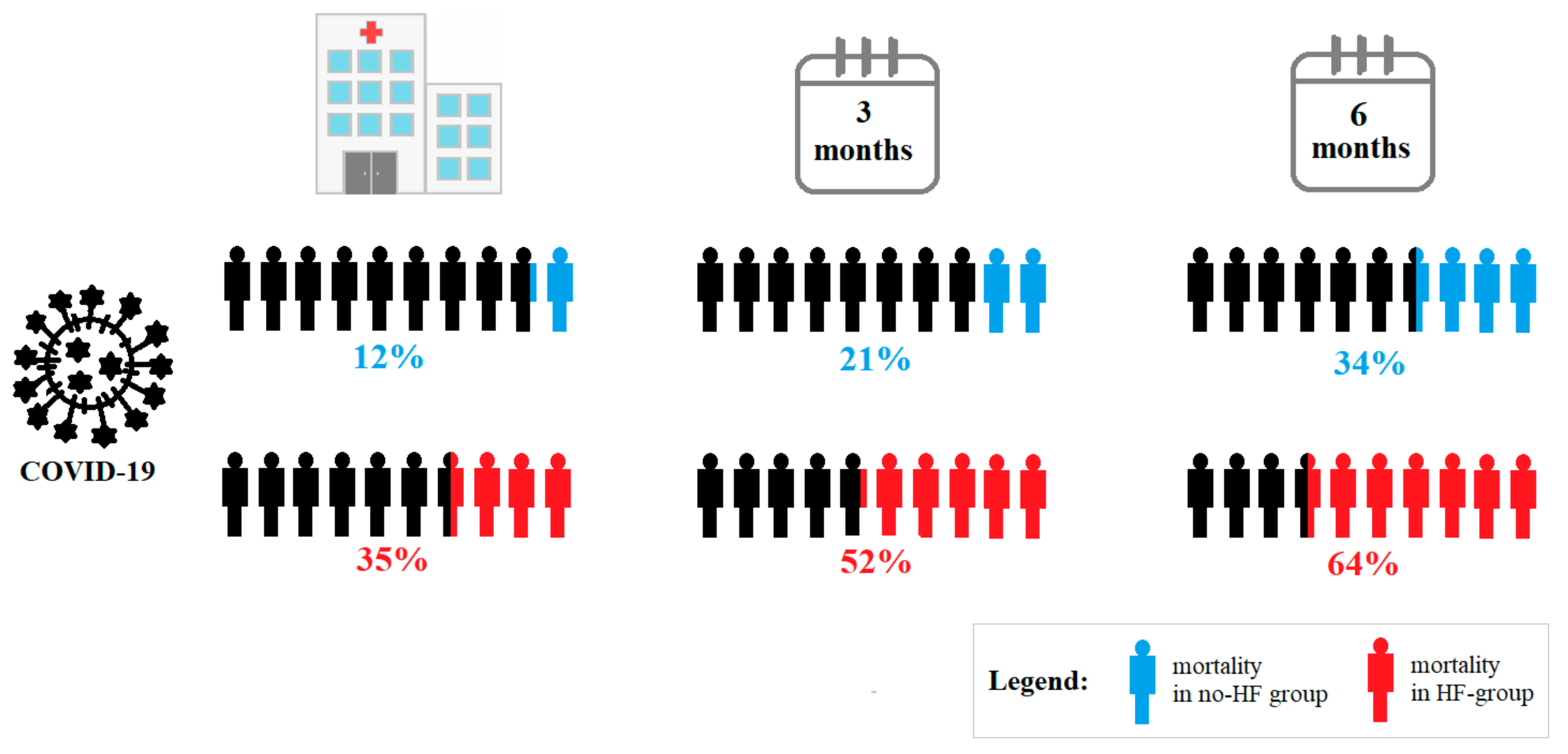
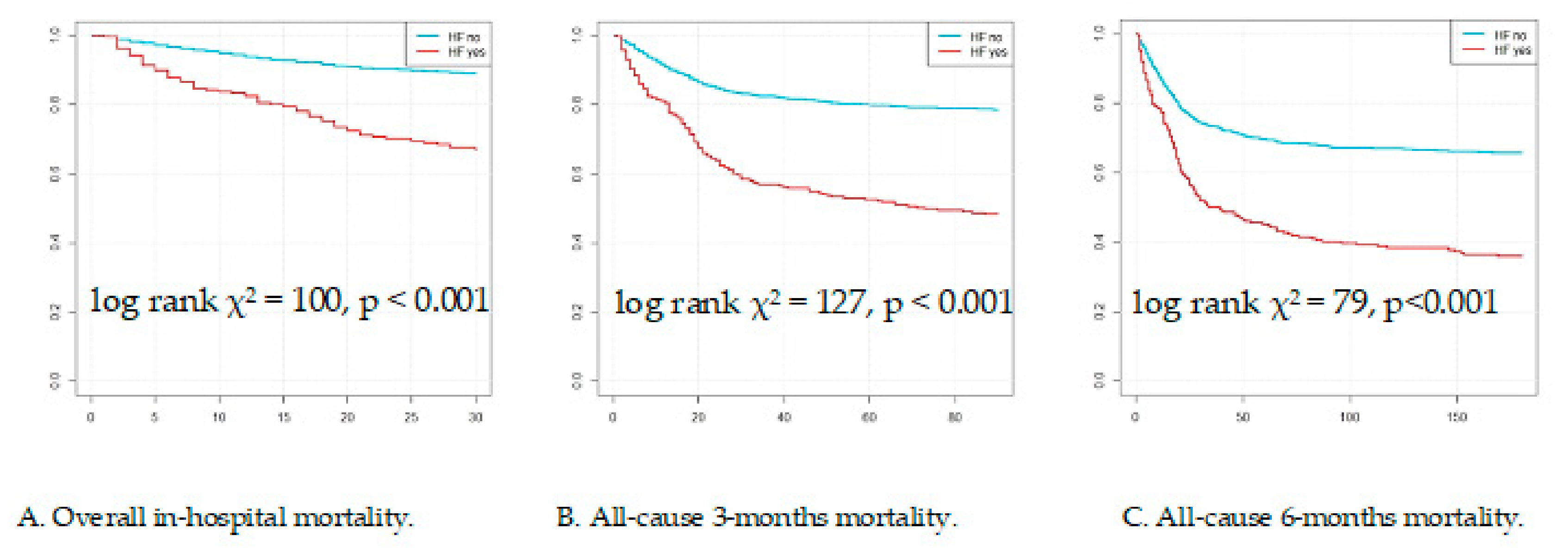
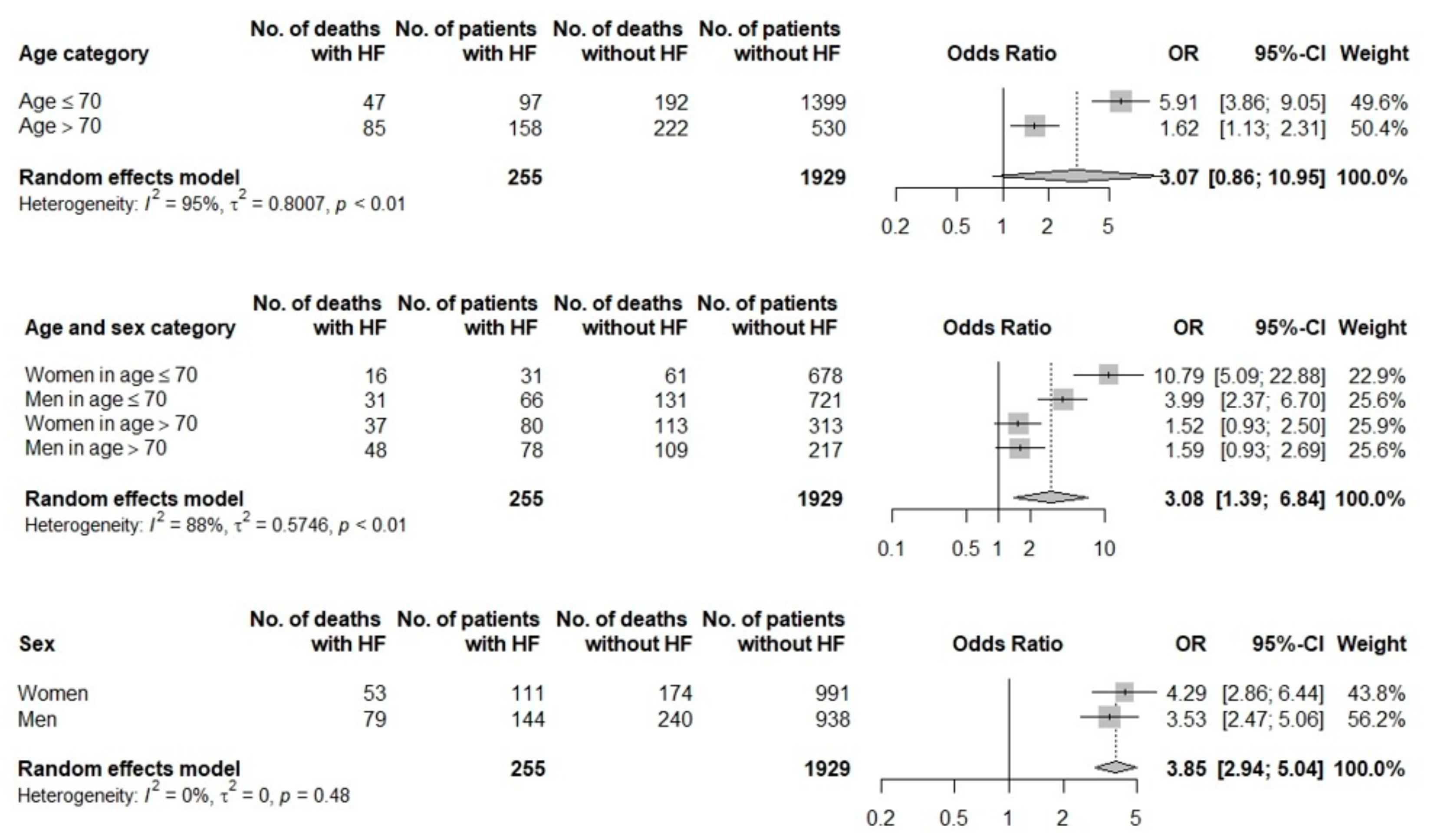
3.3. Outcome
4. Discussion
Limitations
5. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Conflicts of Interest
References
- GBD 2016 Disease and Injury Incidence and Prevalence Collaborators. Global, regional, and national incidence, prevalence, and years lived with disability for 328 diseases and injuries for 195 countries, 1990–2016: A systematic analysis for the Global Burden of Disease Study 2016. Lancet 2017, 390, 1211–1259. [Google Scholar] [CrossRef] [Green Version]
- Groenewegen, A.; Rutten, F.H.; Mosterd, A.; Hoes, A.W. Epidemiology of heart failure. Eur. J. Heart Fail. 2020, 22, 1342–1356. [Google Scholar] [CrossRef]
- Benjamin, E.J.; Virani, S.S.; Callaway, C.W.; Chamberlain, A.M.; Chang, A.R.; Cheng, S.; Chiuve, S.E.; Cushman, M.; Delling, F.N.; Deo, R.; et al. Heart Disease and Stroke Statistics—2018 Update: A Report from the American Heart Association. Circulation 2018, 137, e67–e492. [Google Scholar] [CrossRef]
- Nessler, J.; Siniarski, A.; Leszek, P.; Gumprecht, J.; Drożdż, J.; Kaźmierczak, J.; Witkowski, A.; Gackowski, A.; Jankowska, E.A.; Kukulski, T.; et al. Expert opinion of the Heart Failure Working Group of the Polish Cardiac Society on the use of dapagliflozin in the treatment of heart failure with reduced ejection fraction. Kardiol. Pol. 2021, 79, 363–370. [Google Scholar] [CrossRef]
- Taylor, C.J.; Ordóñez-Mena, J.M.; Roalfe, A.K.; Lay-Flurrie, S.; Jones, N.; Marshall, T.; Hobbs, F.D.R. Trends in survival after a diagnosis of heart failure in the United Kingdom 2000–2017: Population based cohort study. BMJ 2019, 364, l223. [Google Scholar] [CrossRef] [Green Version]
- Sierpiński, R.; Sokolska, J.M.; Suchocki, T.; Koń, B.; Urbański, F.; Kruk, M.; Sokolski, M.; Ponikowski, P.; Jankowska, E.A. 10 year trends in hospitalization rates due to heart failure and related in-hospital mortality in Poland (2010–2019). ESC Heart Fail. 2020, 7, 3365–3373. [Google Scholar] [CrossRef]
- World Health Organization. COVID-19 Explorer. Available online: https://worldhealthorg.shinyapps.io/covid/ (accessed on 21 October 2021).
- Jin, Y.; Yang, H.; Ji, W.; Wu, W.; Chen, S.; Zhang, W.; Duan, G. Virology, Epidemiology, Pathogenesis, and Control of COVID-19. Viruses 2020, 12, 372. [Google Scholar] [CrossRef] [Green Version]
- Roth, G.A.; Emmons-Bell, S.; Alger, H.M.; Bradley, S.M.; Das, S.R.; de Lemos, J.A.; Gakidou, E.; Elkind, M.S.V.; Hay, S.; Hall, J.L.; et al. Trends in Patient Characteristics and COVID-19 In-Hospital Mortality in the United States during the COVID-19 Pandemic. JAMA Netw. Open 2021, 4, e218828. [Google Scholar] [CrossRef]
- Gray, W.K.; Navaratnam, A.V.; Day, J.; Babu, P.; Mackinnon, S.; Adelaja, I.; Bartlett-Pestell, S.; Moulton, C.; Mann, C.; Batchelor, A.; et al. Variability in COVID-19 in-hospital mortality rates between national health service trusts and regions in England: A national observational study for the Getting It Right First Time Programme. EClinicalMedicine 2021, 35, 100859. [Google Scholar] [CrossRef]
- Günster, C.; Busse, R.; Spoden, M.; Rombey, T.; Schillinger, G.; Hoffmann, W.; Weber-Carstens, S.; Schuppert, A.; Karagiannidis, C. 6-month mortality and readmissions of hospitalized COVID-19 patients: A nationwide cohort study of 8679 patients in Germany. PLoS ONE 2021, 16, e0255427. [Google Scholar] [CrossRef]
- Streeck, H.; Schulte, B.; Kümmerer, B.M.; Richter, E.; Höller, T.; Fuhrmann, C.; Bartok, E.; Dolscheid-Pommerich, R.; Berger, M.; Wessendorf, L.; et al. Infection fatality rate of SARS-CoV2 in a super-spreading event in Germany. Nat. Commun. 2020, 11, 5829. [Google Scholar] [CrossRef]
- Yang, X.; Yu, Y.; Xu, J.; Shu, H.; Xia, J.; Liu, H.; Wu, Y.; Zhang, L.; Yu, Z.; Fang, M.; et al. Clinical course and outcomes of critically ill patients with SARS-CoV-2 pneumonia in Wuhan, China: A single-centered, retrospective, observational study. Lancet Respir. Med. 2020, 8, 475–481. [Google Scholar] [CrossRef] [Green Version]
- Gao, Y.-D.; Ding, M.; Dong, X.; Zhang, J.-J.; Azkur, A.K.; Azkur, D.; Gan, H.; Sun, Y.-L.; Fu, W.; Li, W.; et al. Risk factors for severe and critically ill COVID-19 patients: A review. Allergy 2021, 76, 428–455. [Google Scholar] [CrossRef]
- Centers for Disease Control and Prevention. Provisional COVID-19 Death Counts by Sex, Age, and State. Available online: https://data.cdc.gov/NCHS/Provisional-COVID-19-Death-Counts-by-Sex-Age-and-S/9bhg-hcku (accessed on 21 October 2021).
- Pollard, C.A.; Morran, M.P.; Nestor-Kalinoski, A.L. The COVID-19 pandemic: A global health crisis. Physiol. Genom. 2020, 52, 549–557. [Google Scholar] [CrossRef]
- Jin, J.M.; Bai, P.; He, W.; Wu, F.; Liu, X.F.; Han, D.M.; Liu, S.; Yang, J.K. Gender Differences in Patients with COVID-19: Focus on Severity and Mortality. Front. Public Health 2020, 8, 152. [Google Scholar] [CrossRef]
- Bader, F.; Manla, Y.; Atallah, B.; Starling, R.C. Heart failure and COVID-19. Heart Fail. Rev. 2020, 26, 1–10. [Google Scholar] [CrossRef]
- Sokolski, M.; Sokolska, J.M.; Zymliński, R.; Biegus, J.; Banasiak, W.; Reczuch, K.; Ponikowski, P. Cardiac emergencies during the coronavirus disease 2019 pandemic in the light of the current evidence. Kardiol. Pol. 2020, 78, 818–824. [Google Scholar] [CrossRef]
- Zhou, F.; Yu, T.; Du, R.; Fan, G.; Liu, Y.; Liu, Z.; Xiang, J.; Wang, Y.; Song, B.; Gu, X.; et al. Clinical course and risk factors for mortality of adult inpatients with COVID-19 in Wuhan, China: A retrospective cohort study. Lancet 2020, 395, 1054–1062. [Google Scholar] [CrossRef]
- Kubica, J.; Ostrowska, M.; Stolarek, W.; Kasprzak, M.; Grzelakowska, K.; Kryś, J.; Kubica, A.; Adamski, P.; Podhajski, P.; Navarese, E.P.; et al. Impact of COVID-19 pandemic on acute heart failure admissions and mortality: A multicentre study (COV-HF-SIRIO 6 study). ESC Heart Fail 2021. advance online publication. [Google Scholar] [CrossRef]
- Severino, P.; D’Amato, A.; Saglietto, A.; D’Ascenzo, F.; Marini, C.; Schiavone, M.; Ghionzoli, N.; Pirrotta, F.; Troiano, F.; Cannillo, M.; et al. Reduction in heart failure hospitalization rate during coronavirus disease 19 pandemic outbreak. ESC Heart Fail. 2020, 7, 4182–4188. [Google Scholar] [CrossRef]
- Sokolski, M.; Gajewski, P.; Zymliński, R.; Biegus, J.; Berg, J.M.T.; Bor, W.; Braunschweig, F.; Caldeira, D.; Cuculi, F.; D’Elia, E.; et al. Impact of Coronavirus Disease 2019 (COVID-19) Outbreak on Acute Admissions at the Emergency and Cardiology Departments Across Europe. Am. J. Med. 2020, 134, 482–489. [Google Scholar] [CrossRef]
- Sokolski, M.; Trenson, S.; Sokolska, J.M.; D’Amario, D.; Meyer, P.; Poku, N.K.; Biering-Sørensen, T.; Lassen, M.C.H.; Skaarup, K.G.; Barge-Caballero, E.; et al. Heart failure in COVID-19: The multicentre, multinational PCHF-COVICAV registry. ESC Heart Fail. 2021. [Google Scholar] [CrossRef]
- Ponikowski, P.; Voors, A.A.; Anker, S.D.; Bueno, H.; Cleland, J.G.F.; Coats, A.J.S.; Falk, V.; González-Juanatey, J.R.; Harjola, V.-P.; Jankowska, E.A.; et al. 2016 ESC Guidelines for the diagnosis and treatment of acute and chronic heart failure: The Task Force for the diagnosis and treatment of acute and chronic heart failure of the European Society of Cardiology (ESC)Developed with the special contribution of the Heart Failure Association (HFA) of the ESC. Eur. Heart J. 2016, 37, 2129–2200. [Google Scholar] [CrossRef]
- McDonagh, T.A.; Metra, M.; Adamo, M.; Gardner, R.S.; Baumbach, A.; Böhm, M.; Burri, H.; Butler, J.; Čelutkienė, J.; Chioncel, O.; et al. 2021 ESC Guidelines for the diagnosis and treatment of acute and chronic heart failure. Eur. Heart J. 2021, 42, 3599–3726. [Google Scholar] [CrossRef]
- Thygesen, K.; Alpert, J.S.; Jaffe, A.S.; Chaitman, B.R.; Bax, J.J.; Morrow, D.A.; White, H.D. Fourth Universal Definition of Myocardial Infarction (2018). J. Am. Coll. Cardiol. 2018, 72, 2231–2264. [Google Scholar] [CrossRef]
- Rivera-Caravaca, J.M.; Núñez-Gil, I.J.; Vivas, D.; Viana-Llamas, M.C.; Uribarri, A.; Becerra-Muñoz, V.M.; Trabattoni, D.; Rozas, I.F.; Feltes, G.; López-Pais, J.; et al. Clinical profile and prognosis in patients on oral anticoagulation before admission for COVID-19. Eur. J. Clin. Investig. 2020, 51, e13436. [Google Scholar] [CrossRef]
- Tremblay, D.; Van Gerwen, M.; Alsen, M.; Thibaud, S.; Kessler, A.J.; Venugopal, S.; Makki, I.; Qin, Q.; Dharmapuri, S.; Jun, T.; et al. Impact of anticoagulation prior to COVID-19 infection: A propensity score-matched cohort study. Blood 2020, 136, 144–147. [Google Scholar] [CrossRef]
- Kornej, J.; Börschel, C.S.; Benjamin, E.J.; Schnabel, R.B. Epidemiology of Atrial Fibrillation in the 21st Century. Circ. Res. 2020, 127, 4–20. [Google Scholar] [CrossRef]
- Bavishi, A.; Patel, R.B. Addressing Comorbidities in Heart Failure. Heart Fail. Clin. 2020, 16, 441–456. [Google Scholar] [CrossRef]
- Tomasoni, D.; Italia, L.; Adamo, M.; Inciardi, R.M.; Lombardi, C.M.; Solomon, S.D.; Metra, M. COVID-19 and heart failure: From infection to inflammation and angiotensin II stimulation. Searching for evidence from a new disease. Eur. J. Heart Fail. 2020, 22, 957–966. [Google Scholar] [CrossRef]
- Wu, C.; Chen, X.; Cai, Y.; Xia, J.; Zhou, X.; Xu, S.; Huang, H.; Zhang, L.; Zhou, X.; Du, C.; et al. Risk Factors Associated with Acute Respiratory Distress Syndrome and Death in Patients with Coronavirus Disease 2019 Pneumonia in Wuhan, China. JAMA Intern. Med. 2020, 180, 934–943. [Google Scholar] [CrossRef] [Green Version]
- Sama, I.; Ravera, A.; Santema, B.T.; Van Goor, H.; Ter Maaten, J.M.; Cleland, J.G.F.; Rienstra, M.; Friedrich, A.W.; Samani, N.J.; Ng, L.L.; et al. Circulating plasma concentrations of angiotensin-converting enzyme 2 in men and women with heart failure and effects of renin–angiotensin–aldosterone inhibitors. Eur. Heart J. 2020, 41, 1810–1817. [Google Scholar] [CrossRef]
- Varga, Z.; Flammer, A.J.; Steiger, P.; Haberecker, M.; Andermatt, R.; Zinkernagel, A.S.; Mehra, M.R.; Schuepbach, R.A.; Ruschitzka, F.; Moch, H. Endothelial cell infection and endotheliitis in COVID-19. Lancet 2020, 395, 1417–1418. [Google Scholar] [CrossRef]
- Schiavone, M.; Gasperetti, A.; Mancone, M.; Kaplan, A.V.; Gobbi, C.; Mascioli, G.; Busana, M.; Saguner, A.M.; Mitacchione, G.; Giacomelli, A.; et al. Redefining the Prognostic Value of High-Sensitivity Troponin in COVID-19 Patients: The Importance of Concomitant Coronary Artery Disease. J. Clin. Med. 2020, 9, 3263. [Google Scholar] [CrossRef] [PubMed]
- Peterson, E.; Lo, K.B.; DeJoy, R.; Salacup, G.; Pelayo, J.; Bhargav, R.; Gul, F.; Albano, J.; Azmaiparashvili, Z.; Amanullah, A.; et al. The relationship between coronary artery disease and clinical outcomes in COVID-19. Coron. Artery Dis. 2020, 32, 367–371. [Google Scholar] [CrossRef]
- Schiavone, M.; Gobbi, C.; Biondi-Zoccai, G.; D’Ascenzo, F.; Palazzuoli, A.; Gasperetti, A.; Mitacchione, G.; Viecca, M.; Galli, M.; Fedele, F.; et al. Acute Coronary Syndromes and Covid-19: Exploring the Uncertainties. J. Clin. Med. 2020, 9, 1683. [Google Scholar] [CrossRef]
- Barman, H.A.; Atici, A.; Sahin, I.; Alici, G.; Tekin, E.A.; Baycan, F.; Ozturk, F.; Oflar, E.; Tugrul, S.; Yavuz, M.B.; et al. Prognostic significance of cardiac injury in COVID-19 patients with and without coronary artery disease. Coron. Artery Dis. 2020, 32, 359–366. [Google Scholar] [CrossRef]
- Sokolski, M.; Zymlinski, R.; Biegus, J.; Siwołowski, P.; Nawrocka-Millward, S.; Todd, J.; Yerramilli, M.R.; Estis, J.; A Jankowska, E.; Banasiak, W.; et al. Urinary levels of novel kidney biomarkers and risk of true worsening renal function and mortality in patients with acute heart failure. Eur. J. Heart Fail. 2017, 19, 760–767. [Google Scholar] [CrossRef] [Green Version]
- Alvarez-Garcia, J.; Lee, S.; Gupta, A.; Cagliostro, M.; Joshi, A.A.; Rivas-Lasarte, M.; Contreras, J.; Mitter, S.S.; LaRocca, G.; Tlachi, P.; et al. Prognostic Impact of Prior Heart Failure in Patients Hospitalized with COVID-19. J. Am. Coll. Cardiol. 2020, 76, 2334–2348. [Google Scholar] [CrossRef]
- Rey, J.R.; Caro-Codón, J.; Rosillo, S.O.; Iniesta, Á.M.; Castrejón-Castrejón, S.; Marco-Clement, I.; Martín-Polo, L.; Merino-Argos, C.; Rodríguez-Sotelo, L.; García-Veas, J.M.; et al. Heart failure in COVID-19 patients: Prevalence, incidence and prognostic implications. Eur. J. Heart. Fail. 2020, 22, 2205–2215. [Google Scholar] [CrossRef]
- Rumery, K.; Seo, A.; Jiang, L.; Choudhary, G.; Shah, N.R.; Rudolph, J.L.; Wu, W.; Erqou, S. Outcomes of coronavirus disease-2019 among veterans with pre-existing diagnosis of heart failure. ESC Heart Fail. 2021, 8, 2338–2344. [Google Scholar] [CrossRef] [PubMed]
- Anyu, A.T.; Badawy, L.; Cannata, A.; Bromage, D.I.; Rind, I.A.; Albarjas, M.; Piper, S.; Shah, A.M.; McDonagh, T.A. Long-term outcomes after heart failure hospitalization during the COVID-19 pandemic: A multisite report from heart failure referral centers in London. ESC Heart Fail. 2021. [Google Scholar] [CrossRef]
| Variables, Units | HF Group n = 255 | Non-HF Group n = 1929 | p | Available Data, n (%) |
|---|---|---|---|---|
| Demographics | ||||
| Age, years | 75 ± 12 | 58 ± 19 | <0.001 | 2184 (100) |
| Age ≥ 70 years, n (%) | 169 (66) | 571 (30) | <0.001 | 2184 (100) |
| Male gender, n (%) | 144 (57) | 938 (49) | 0.022 | 2184 (100) |
| Body mass index, kg/m2 | 28 ± 6 | 28 ± 5 | 0.950 | 554 (25) |
| Co-Morbidities | ||||
| Hypertension, n (%) | 215 (84) | 807 (42) | <0.001 | 2184 (100) |
| Diabetes mellitus, n (%) | 122 (48) | 394 (20) | <0.001 | 2182 (100) |
| Atrial fibrillation/flutter, n (%) | 134 (53) | 156 (8) | <0.001 | 2184 (100) |
| Previous coronary revascularization, n (%) | 93 (37) | 61 (3) | <0.001 | 2184 (100) |
| Previous myocardial infarction, n (%) | 92 (36) | 99 (5) | <0.001 | 2184 (100) |
| Significant valvular heart disease or previous valve heart surgery, n (%) | 64 (25) | 32 (2) | <0.001 | 2184 (100) |
| Peripheral artery disease, n (%) | 43 (17) | 57 (3) | <0.001 | 2184 (100) |
| Previous stroke/transient ischemic attack, n (%) | 53 (21) | 111 (6) | <0.001 | 2184 (100) |
| Chronic kidney disease or/and hemodialysis, n (%) | 92 (36) | 139 (7) | <0.001 | 2184 (100) |
| Asthma, n (%) | 10 (4) | 75 (4) | 0.979 | 2184 (100) |
| Chronic obstructive pulmonary disease, n (%) | 29 (11) | 46 (2) | <0.001 | 2184 (100) |
| Cigarette smoking (previous or current), n (%) | 55 (22) | 138 (7) | <0.001 | 2180 (100) |
| Sleep apnea syndrome, n (%) | 7 (3) | 9 (1) | <0.001 | 2184 (100) |
| Chronic liver disease, n (%) | 15 (6) | 59 (3) | 0.031 | 2183 (100) |
| Thyroid disease, n (%) | 33 (13)/7 (3) | 175 (9)/14 (1) | 0.001 | 2184 (100) |
| Dementia, n (%) | 50 (20) | 82 (4.3) | <0.001 | 2184 (100) |
| Malignancy, n (%) | 29 (11) | 156 (8) | 0.099 | 2184 (100) |
| Transplant recipients, n (%) | 7 (3) | 26 (1) | 0.148 | 2184 (100) |
| Treatment Applied before Hospitalization | ||||
| Angiotensin-converting enzyme inhibitors, n (%) | 104 (41) | 248 (13) | <0.001 | 2184 (100) |
| Angiotensin receptor blockers, n (%) | 24 (9) | 120 (6) | 0.073 | 2184 (100) |
| Mineralocorticoid receptor antagonists, n (%) | 56 (22) | 44 (2) | <0.001 | 2184 (100) |
| β-blockers, n (%) | 153 (60) | 380 (20) | <0.001 | 2184 (100) |
| Ivabradine, n (%) | 1 (0.4) | 2 (0.1) | 0.788 | 2184 (100) |
| Digitalis glycoside, n (%) | 10 (4) | 9 (1) | <0.001 | 2184 (100) |
| Calcium blockers (nondihydropyridine), n (%) | 11 (4) | 27 (1) | 0.002 | 2184 (100) |
| Calcium blockers (dihydropyridine), n (%) | 65 (26) | 196 (10) | <0.001 | 2184 (100) |
| α-adrenergic blockers, n (%) | 39 (15) | 79 (4) | <0.001 | 2184 (100) |
| Thiazide or thiazidelike diuretics, n (%) | 28 (11) | 122 (6) | 0.009 | 2184 (100) |
| Loop diuretics, n (%) | 100 (39) | 85 (4) | <0.001 | 2184 (100) |
| Statins, n (%) | 123 (48) | 227 (12) | <0.001 | 2184 (100) |
| Acetylsalicylic acid, n (%) | 76 (30) | 182 (9) | <0.001 | 2184 (100) |
| Second antiplatelet drug, n (%) | 20 (8) | 19 (1) | <0.001 | 2184 (100) |
| Low-molecular-weight heparin, n (%) | 28 (11) | 113 (6) | 0.003 | 2184 (100) |
| Vitamin K antagonists, n (%) | 22 (9) | 25 (1) | <0.001 | 2184 (100) |
| Direct oral anticoagulants, n (%) | 55 (22) | 52 (3) | <0.001 | 2184 (100) |
| Insulin, n (%) | 39 (15) | 92 (5) | <0.001 | 2184 (100) |
| Metformin, n (%) | 52 (20) | 170 (9) | <0.001 | 2184 (100) |
| Sodium–glucose cotransporter-2 inhibitors, n (%) | 11 (4) | 16 (1) | <0.001 | 2184 (100) |
| Oral antidiabetics other than mentioned above, n (%) | 30 (12) | 59 (3) | <0.001 | 2184 (100) |
| Oral corticosteroid, n (%) | 9 (4) | 83 (4) | 0.680 | 2184 (100) |
| Immunosuppression other than corticosteroid, n (%) | 8 (3) | 65 (3) | 0.993 | 2184 (100) |
| Home oxygen therapy or ventilation n (%) | 4 (1.6) | 4 (0.2) | 0.005 | 2184 (100) |
| Hemodialysis, n (%) | 21 (8) | 37 (2) | <0.001 | 2184 (100) |
| Variables, Units | HF Group n = 255 | Non-HF Group n = 1929 | p | Available Data, n (%) |
|---|---|---|---|---|
| Patient-Reported Symptoms | ||||
| Cough, n (%) | 67 (26) | 581 (30) | 0.234 | 2184 (100) |
| Dyspnea, n (%) | 144 (57) | 777 (40) | <0.001 | 2184 (100) |
| Chest pain, n (%) | 29 (11) | 134 (7) | 0.016 | 2184 (100) |
| Hemoptysis, n (%) | 4 (2) | 11 (1) | 0.158 | 2184 (100) |
| Smell dysfunction, n (%) | 4 (2) | 72 (4) | 0.112 | 2184 (100) |
| Taste dysfunction, n (%) | 5 (2) | 61 (3) | 0.391 | 2184 (100) |
| Abdominal pain, n (%) | 16 (6) | 131 (7) | 0.860 | 2184 (100) |
| Diarrhea, n (%) | 16 (6) | 111 (6) | 0.848 | 2184 (100) |
| Vomiting, n (%) | 11 (4) | 87 (4) | 0.887 | 2184 (100) |
| Measured Vital Signs | ||||
| Body temperature, °C | 36.9 ± 0.9 | 37.0 ± 0.9 | 0.182 | 1186 (54) |
| Heart rate, beats/minute | 85 ± 19 | 86 ± 16 | 0.364 | 1672 (77) |
| Systolic blood pressure, mmHg | 133 ± 26 | 132 ± 22 | 0.494 | 1169 (76) |
| SpO2 on room air, % | 90 ± 10 | 92 ± 8 | 0.001 | 1263 (58) |
| SpO2 on oxygen supplementation, % | 94 ± 6 | 95 ± 6 | 0.420 | 824 (38) |
| Abnormalities Detected during Physical Examination | ||||
| Wheezing, n (%) | 59 (23) | 160 (8) | <0.001 | 2184 (100) |
| Pulmonary congestion, n (%) | 85 (33) | 282 (15) | <0.001 | 2184 (100) |
| Peripheral oedema, n (%) | 58 (23) | 131 (7) | <0.001 | 2184 (100) |
| Variables, Units | HF Group n = 255 | Non-HF Group n = 1929 | p | Available Data,n (%) |
|---|---|---|---|---|
| Morphology | ||||
| Leukocytes, 103/µL | 7.7 (5.8–10.6) | 7.3 (5.3–10.3) | 0.040 | 2050 (94) |
| Lymphocytes, 103/µL | 0.9 (0.6–1.4) | 1.0 (0.7–1.4) | 0.007 | 1296 (59) |
| Neutrophils, 103/µL | 5.7 (3.8–9.1) | 5.5 (3.4–8.2) | 0.058 | 1299 (59) |
| Hemoglobin, g/dL | 12.0 ± 2.4 | 13.1 ± 2.2 | <0.001 | 2050 (94) |
| Electrolytes, Inflammatory | ||||
| Sodium, mmol/L | 138 ± 6 | 138 ± 5 | 0.958 | 2032 (93) |
| Potassium, mmol/L | 4.3 ± 0.8 | 4.1 ± 0.6 | <0.001 | 2039 (93) |
| CRP, mg/L | 46 (13–102) | 49 (13–117) | 0.686 | 2020 (92) |
| Procalcitonin, ng/mL | 0.15 (0.06–0.57) | 0.08 (0.04–0.26) | <0.001 | 1475 (68) |
| IL-6, pg/mL | 28 (11–59) | 16 (6–44) | 0.002 | 702 (32) |
| Ferritin, ng/mL | 557 (197–1212) | 602 (297–1150) | 0.309 | 969 (44) |
| Biochemistry | ||||
| Urea, mg/dL | 64 (44–101) | 36 (25–57) | <0.001 | 1859 (85) |
| eGFR, ml/min/1.73 m2 | 53 ± 31 | 78 ± 34 | <0.001 | 1958 (90) |
| Albumin, g/L | 3.0 ± 0.6 | 3.1 ± 0.6 | 0.132 | 665 (30) |
| Uric acid, mg/dL | 6.7 (5.4–9.2) | 5.2 (3.9–6.7) | <0.001 | 623 (29) |
| Bilirubin, mg/dL | 0.7 (0.5–1.1) | 0.6 (0.5–0.8) | <0.001 | 1408 (64) |
| GGTP, U/L | 43 (24–97) | 43 (24–86) | 0.916 | 1352 (62) |
| Cardiac Biomarkers | ||||
| NT-proBNP, pg/mL | 6496 (2255–15,881) | 551 (160–2441) | <0.001 | 379 (17) |
| Troponin I, ng/L | 55 (23–157) | 11 (4–36) | <0.001 | 1174 (64) |
| Variables, Units | HF Group n = 255 | Non-HF Group n = 1929 | p | Available Data, n (%) |
|---|---|---|---|---|
| In-hospital Course | ||||
| Duration of hospitalization, days | 13 (4–21) | 9 (2–15) | <0.001 | 2184 (100) |
| Admission at intensive care unit, n (%) | 33 (13) | 181 (9) | 0.092 | 2184 (100) |
| Shock, n (%) | 38 (15) | 150 (8) | <0.001 | 2184 (100) |
| Myocardial infarction, n (%) | 10 (4) | 16 (1) | <0.001 | 2184 (100) |
| Thromboembolic disease, n (%) | 10 (4) | 59 (3) | 0.459 | 2184 (100) |
| Stroke, n (%) | 7 (3) | 37 (2) | 0.377 | 2184 (100) |
| Acute HF, n (%) | 53 (21) | 23 (1) | <0.001 | 2184 (100) |
| Applied Treatment and Procedures | ||||
| Passive oxygen therapy, n (%) | 109 (43) | 654 (34) | 0.006 | 2181 (100) |
| Non-invasive ventilation, n (%) | 37 (15) | 136 (7) | <0.001 | 2181 (100) |
| Mechanical ventilation, n (%) | 33 (13) | 182 (9) | 0.098 | 2184 (100) |
| Duration of mechanical ventilation, days | 8 (2–15) | 9 (4–17) | 0.176 | 197 (9) |
| Therapy with catecholamines, n (%) | 45 (18) | 173 (9) | <0.001 | 2184 (100) |
| Therapy with loop diuretics, n (%) | 104 (41) | 229 (12) | <0.001 | 2184 (100) |
| Extracorporeal membrane oxygenation, n (%) | 1 (0.4) | 22 (1.1) | 0.439 | 2184 (100) |
| Coronary angiography, n (%) | 12 (5) | 18 (1) | <0.001 | 2184 (100) |
| Coronary revascularization, n (%) | 11 (4) | 20 (1) | 0.001 | 2184 (100) |
| Hemodialysis, n (%) | 17 (7) | 55 (3) | 0.003 | 2184 (100) |
| Amiodarone, n (%) | 17 (7) | 39 (2) | <0.001 | 2184 (100) |
| Nitroglycerine (i.v.), n (%) | 7 (3) | 12 (1) | 0.002 | 2184 (100) |
| Low-molecular-weight heparin, n (%) | 160 (63) | 1105 (57) | 0.111 | 2184 (100) |
| Unfractionated heparin, n (%) | 12 (5) | 110 (6) | 0.613 | 2184 (100) |
| Direct oral anticoagulants, n (%) | 29 (11) | 6 (3) | <0.001 | 2184 (100) |
| Vitamin K antagonists, n (%), n (%) | 5 (2) | 15 (1) | 0.130 | 2184 (100) |
| Acetylsalicylic acid, n (%) | 81 (32) | 285 (15) | <0.001 | 2184 (100) |
| Thrombolytic therapy, n (%) | 1 (0.4) | 13 (0.7) | 0.911 | 2184 (100) |
| Systemic corticosteroid, n (%) | 129 (51) | 967 (50) | 0.943 | 2184 (100) |
| Convalescent plasma, n (%) | 33 (13) | 206 (11) | 0.327 | 2184 (100) |
| Hydroxychloroquine/chloroquine, n (%) | 0 (0) | 9 (1) | 0.567 | 2184 (100) |
| Tocilizumab, n (%) | 1 (0.4) | 24 (1.2) | 0.374 | 2184 (100) |
| Remdesivir, n (%) | 38 (15) | 305 (16) | 0.777 | 2184 (100) |
| Antibiotic, n (%) | 168 (66) | 1073 (56) | 0.002 | 2184 (100) |
| Prone positioning, n (%) | 22 (9) | 182 (9) | 0.761 | 2184 (100) |
| Variables, Units | Univariable Models | Multivariable Model | |
|---|---|---|---|
| OR (95% CI) | OR (95% CI) | p | |
| Age, per 5 years | 1.39 (1.27–1.51) | 1.23 (1.11–1.36) | <0.001 |
| Arterial hypertension, yes/no | 3.82 (2.24–6.54) | - | - |
| Diabetes mellitus, yes/no | 2.73 (1.72–4.34) | - | - |
| History of heart failure, yes/no | 21.74 (13.05–36.23) | 11.42 (6.49–20.10) | <0.001 |
| History of myocardial infarction, yes/no | 6.12 (3.71–10.10) | 1.67 (0.95–2.94) | 0.074 |
| Atrial fibrillation/flutter, yes/no | 5.52 (3.45–8.86) | - | - |
| Valvular heart disease, yes/no | 5.58 (3.00–10.38) | - | - |
| Peripheral artery disease, yes/no | 3.84 (1.96–7.53) | - | - |
| Chronic kidney disease, yes/no | 4.53 (2.75–7.46) | - | - |
| Variables | Units | Univariable Model | |
|---|---|---|---|
| HR (95% CI) | p | ||
| Age | 5 years | 1.31 (1.27–1.35) | <0.001 |
| History of heart failure | yes/no | 2.95 (2.42–3.59) | <0.001 |
| Gender | Male | 1.53 (1.29–1.82) | <0.001 |
| Diabetes mellitus | yes/no | 1.89 (1.57–2.26) | <0.001 |
| Arterial hypertension | yes/no | 2.16 (1.82–2.58) | <0.001 |
| Chronic obstructive pulmonary disease | yes/no | 2.59 (1.87–3.59) | <0.001 |
| Previous stroke/transient ischemic attack | yes/no | 1.80 (1.39–2.33) | <0.001 |
| Chronic kidney disease | yes/no | 2.43 (1.97–3.00) | <0.001 |
| Malignancy | yes/no | 2.42 (1.93–3.03) | <0.001 |
| C-reactive protein | Ln 1 mg/L | 1.49 (1.39–1.60) | <0.001 |
| Hemoglobin | 1 g/dL | 0.87 (0.84–0.90) | <0.001 |
| Variables | Units | Multivariable Models | |||
|---|---|---|---|---|---|
| HR (95% CI) | Wald’s Statistics | p | Chi2 (p) | ||
| Age | 5 years | 1.29 (1.25–1.33) | 269 | <0.001 | 416 (<0.001) |
| History of heart failure | yes/no | 1.54 (1.25–1.88) | 17 | < 0.001 | |
| Gender | Male | 1.53 (1.29–1.82) | 20 | <0.001 | 114 (<0.001) |
| History of heart failure | yes/no | 2.86 (2.35–3.48) | 109 | < 0.001 | |
| Age | 5 years | 1.32 (1.28–1.37) | 283 | < 0.001 | 462 (<0.001) |
| Gender | Male | 1.82 (1.53–2.17) | 45 | < 0.001 | |
| History of heart failure | yes/no | 1.48 (1.21–1.81) | 14 | < 0.001 | |
| Age | 5 years | 1.32 (1.27–1.36) | 250 | < 0.001 | 504 (<0.001) |
| Gender | Male | 1.71 (1.43–2.04) | 36 | < 0.001 | |
| Diabetes mellitus | yes/no | 1.20 (0.99–1.44) | 3.6 | 0.059 | |
| Arterial hypertension | yes/no | 0.91 (0.75–1.11) | 0.9 | 0.346 | |
| COPD | yes/no | 1.40 (1.00–1.96) | 3.9 | 0.049 | |
| Previous stroke/TIA | yes/no | 0.93 (0.71–1.21) | 0.3 | 0.579 | |
| Chronic kidney disease | yes/no | 1.40 (1.11–1.75) | 8.1 | 0.004 | |
| Malignancy | yes/no | 1.87 (1.49–2.35) | 29 | <0.001 | |
| History of heart failure | yes/no | 1.31 (1.05–1.63) | 5.78 | 0.016 | |
| Age | 5 years | 1.30 (1.26–1.35) | 204 | <0.001 | 571 (<0.001) |
| Gender | Male | 1.59 (1.33–1.91) | 26 | <0.001 | |
| Diabetes mellitus | yes/no | 1.12 (0.92–1.35) | 1.3 | 0.252 | |
| Arterial hypertension | yes/no | 0.93 (0.76–1.12) | 0.6 | 0.433 | |
| COPD | yes/no | 1.38 (0.98–1.93) | 3.4 | 0.065 | |
| Previous stroke/TIA | yes/no | 0.98 (0.74–1.29) | 0.03 | 0.87 | |
| Chronic kidney disease | yes/no | 1.30 (1.03–1.65) | 4.7 | 0.03 | |
| Malignancy | yes/no | 1.86 (1.47–2.35) | 27 | <0.001 | |
| CRP | Ln 1 mg/L | 1.42 (1.32–1.52) | 93 | <0.001 | |
| Hemoglobin | 1 g/dL | 0.94 (0.91–0.98) | 9.2 | 0.002 | |
| History of heart failure | yes/no | 1.35 (1.08–1.69) | 7 | 0.008 | |
| Variables, Units | HFrEF | HFmrEF | HFpEF | p |
|---|---|---|---|---|
| In-hospital mortality, n (%) | 18 (44) | 8 (42) | 14 (20) | 0.016 |
| 3-month mortality, n (%) | 26 (63) | 13 (68) | 19 (27) | <0.001 |
| 6-month mortality, n (%) | 26 (74) | 13 (76) | 25 (42) | 0.002 |
| Variables, Units | Intensive Care Unit Stay | Without Intensive Care Unit Stay | p |
|---|---|---|---|
| In-hospital mortality, n (%) | 118 (55) | 208 (11) | <0.001 |
| 3-month mortality, n (%) | 132 (62) | 414 (21) | <0.001 |
| 6-month mortality, n (%) | 134 (71) | 444 (34) | <0.001 |
| Variables, Units | HF Group | Non-HF Group | p |
|---|---|---|---|
| In-hospital mortality, n (%) | 25 (76) | 93 (51) | 0.009 |
| 3-month mortality, n (%) | 27 (82) | 105 (58) | 0.010 |
| 6-month mortality, n (%) | 27 (87) | 17 (68) | 0.033 |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2022 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Sokolski, M.; Reszka, K.; Suchocki, T.; Adamik, B.; Doroszko, A.; Drobnik, J.; Gorka-Dynysiewicz, J.; Jedrzejczyk, M.; Kaliszewski, K.; Kilis-Pstrusinska, K.; et al. History of Heart Failure in Patients Hospitalized Due to COVID-19: Relevant Factor of In-Hospital Complications and All-Cause Mortality up to Six Months. J. Clin. Med. 2022, 11, 241. https://doi.org/10.3390/jcm11010241
Sokolski M, Reszka K, Suchocki T, Adamik B, Doroszko A, Drobnik J, Gorka-Dynysiewicz J, Jedrzejczyk M, Kaliszewski K, Kilis-Pstrusinska K, et al. History of Heart Failure in Patients Hospitalized Due to COVID-19: Relevant Factor of In-Hospital Complications and All-Cause Mortality up to Six Months. Journal of Clinical Medicine. 2022; 11(1):241. https://doi.org/10.3390/jcm11010241
Chicago/Turabian StyleSokolski, Mateusz, Konrad Reszka, Tomasz Suchocki, Barbara Adamik, Adrian Doroszko, Jarosław Drobnik, Joanna Gorka-Dynysiewicz, Maria Jedrzejczyk, Krzysztof Kaliszewski, Katarzyna Kilis-Pstrusinska, and et al. 2022. "History of Heart Failure in Patients Hospitalized Due to COVID-19: Relevant Factor of In-Hospital Complications and All-Cause Mortality up to Six Months" Journal of Clinical Medicine 11, no. 1: 241. https://doi.org/10.3390/jcm11010241
APA StyleSokolski, M., Reszka, K., Suchocki, T., Adamik, B., Doroszko, A., Drobnik, J., Gorka-Dynysiewicz, J., Jedrzejczyk, M., Kaliszewski, K., Kilis-Pstrusinska, K., Konopska, B., Kopec, A., Larysz, A., Lis, W., Matera-Witkiewicz, A., Pawlik-Sobecka, L., Rosiek-Biegus, M., Sokolska, J. M., Sokolowski, J., ... Jankowska, E. A. (2022). History of Heart Failure in Patients Hospitalized Due to COVID-19: Relevant Factor of In-Hospital Complications and All-Cause Mortality up to Six Months. Journal of Clinical Medicine, 11(1), 241. https://doi.org/10.3390/jcm11010241








