Periodontal Disease Is Associated with Increased Vulnerability of Coronary Atheromatous Plaques in Patients Undergoing Coronary Computed Tomography Angiography—Results from the Atherodent Study
Abstract
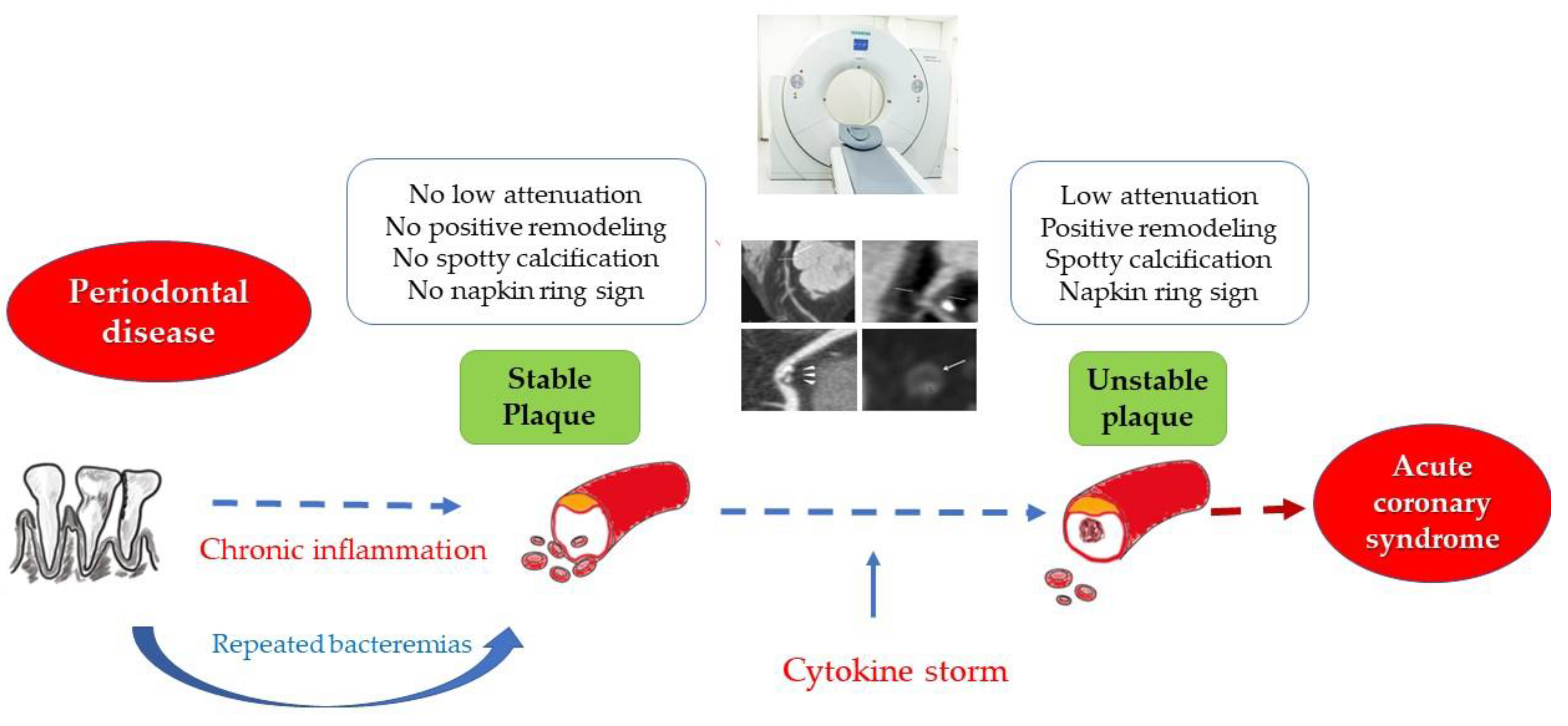
1. Introduction
2. Materials and Methods
2.1. Study Population
2.2. CCTA and Image Processing
2.3. Assessment of the Total Coronary Artery Calcium Score
2.4. Plaque Morphology
2.5. Dental Examination
2.6. Intima–Media Thickness Assessment
2.7. Study Groups
2.8. Statistical Analysis
2.9. Ethical Consideration
3. Results
3.1. Basic Characteristics of the Study Population
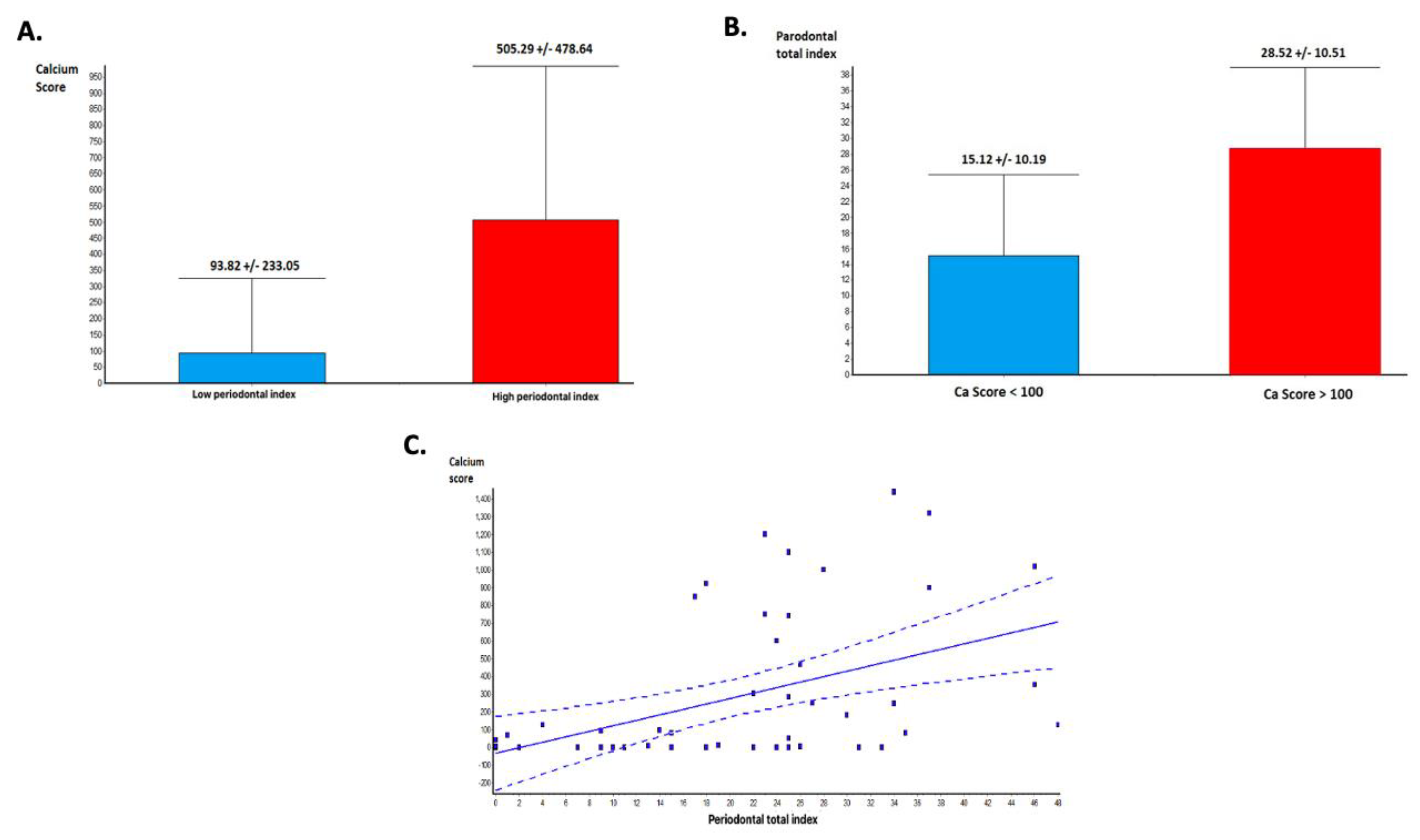
3.2. Periodontal Status and Total Coronary Calcium Score
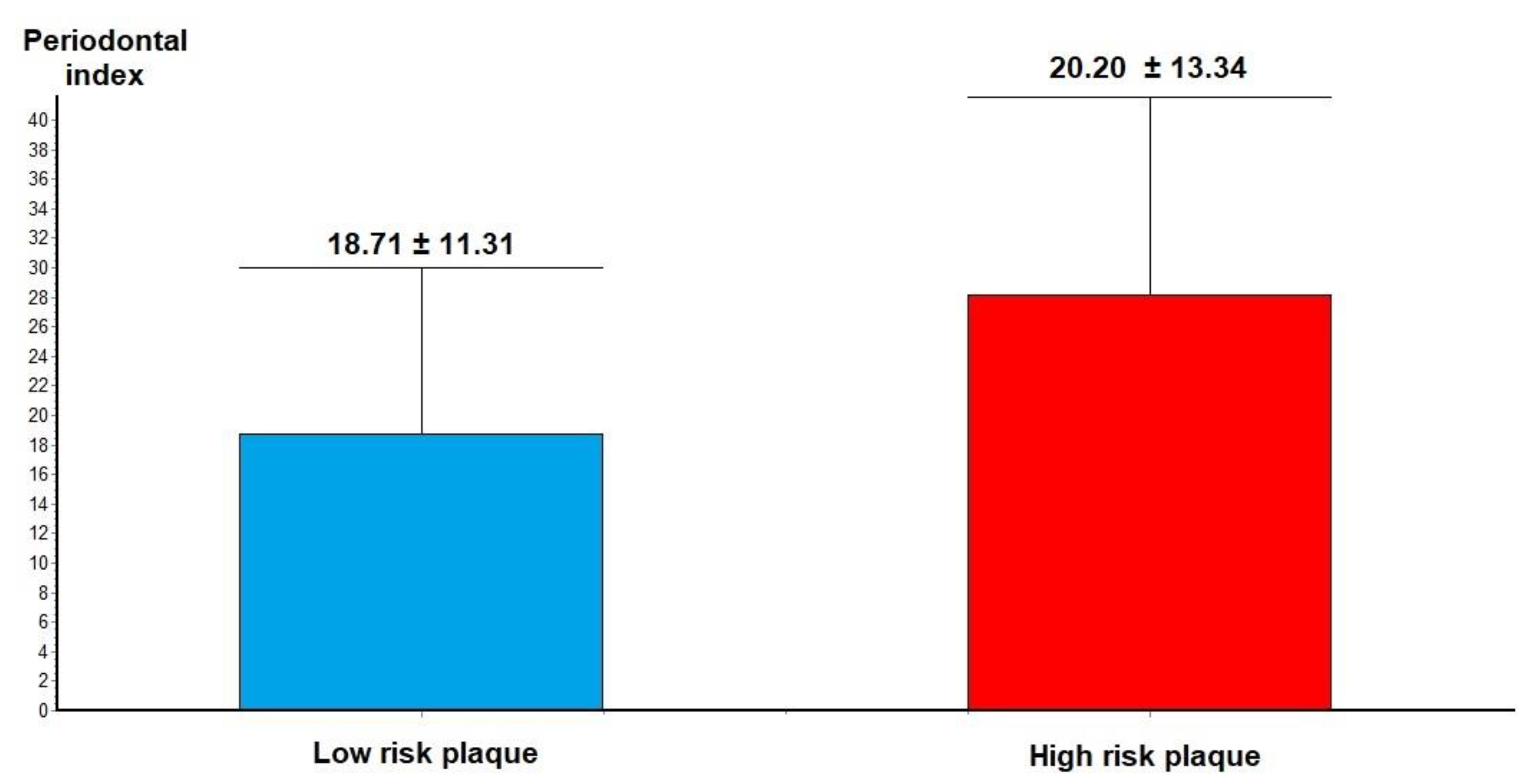
3.3. Periodontal Status and Plaque Vulnerability
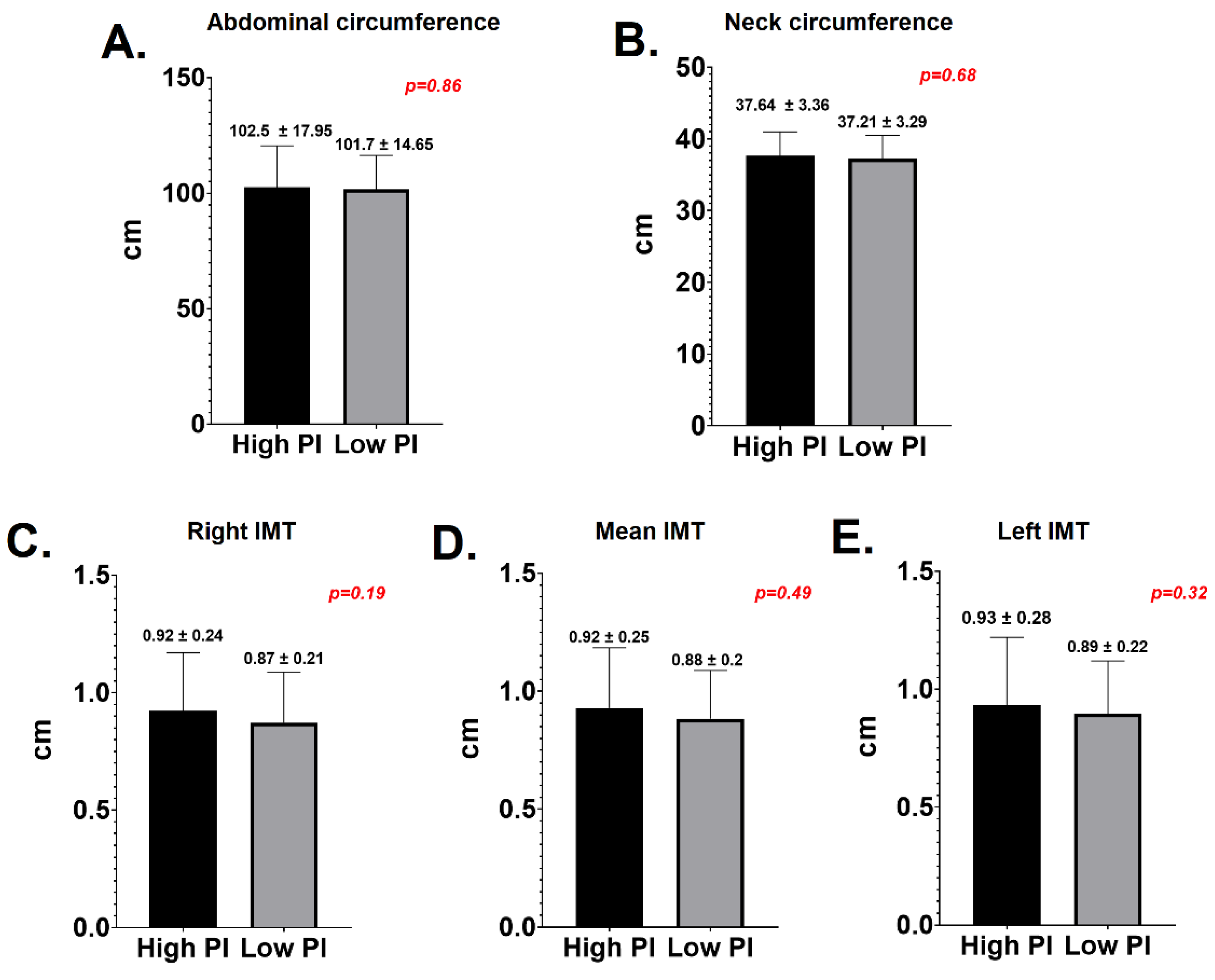
3.4. Periodontal Status and Subclinical Atherosclerosis
4. Discussion
Study Limitation
5. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Conflicts of Interest
References
- Beck, J.D.; Philips, K.; Moss, K.; Sen, S.; Morelli, T.; Preisser, J.; Pankow, J. Periodontal Disease Classifications and Incident Coronary Heart Disease in the Atherosclerosis Risk in Communities Study. J. Periodontol. 2020, 91, 1409–1418. [Google Scholar] [CrossRef] [PubMed]
- Gode, S.; Sarp, T.Z.; Saribas, S.; Ergin, S.; Kasnak, G.; Dinc, H.O.; Caliskan, R.; Akkus, S.; Tokman, H.B.; Kocak, B.T.; et al. The prevalence of periodontal pathogenic bacteria in atherosclerotic cardiovascular disease. Clin. Lab. 2020, 66, 893–900. [Google Scholar] [CrossRef]
- Diaz, C.M.; Bullon, B.; Ruiz-Salmeron, R.; Fernandez-Riejos, P.; Fernandez-Palacin, A.; Bttino, M.; Cordero, M.D.; Quiles, J.L.; Varela-Lopez, A.; Bullon, P. Molecular inflammation and oxidative stress are shared mechanism involved in both myocardial infarction and periodontitis. J. Periodont. Res. 2020, 55, 519–528. [Google Scholar] [CrossRef]
- Byon, M.J.; Kim, S.Y.; Kim, J.S.; Kim, H.N.; Kim, J.B. Association of periodontitis with atherosclerotic cardiovascular disease: A nationwide population-based retrospective matched cohort study. Int. J. Environ. Res. Public Health 2020, 17, 7261. [Google Scholar] [CrossRef]
- Zhang, T.Y.; Zhao, O.; Liu, Z.S.; Zhang, C.Y.; Yang, J.; Meng, K. Relationship between monocyte/lymphocyte ratio and non-culprit plaque vulnerability in patients with acute coronary syndrome: An optical coherence tomography study. Medicine 2020, 99, e21562. [Google Scholar] [CrossRef]
- Benedek, T. The link between Periodontal Disease, Inflammation and Atherosclerosis–An interdisciplinary approach. J. Interdiscip. Med. 2017, 2, 11–16. [Google Scholar] [CrossRef][Green Version]
- Arabi, G.; Zeller, T.; Seedorf, H.; Reissmann, D.R.; Heydecke, G.; Schaefer, A.S.; Seedorf, U. Genetic susceptibility contributing to periodontal and cardiovascular disease. J. Dent. Res. 2017, 96, 610–617. [Google Scholar] [CrossRef] [PubMed]
- Lijestrand, J.M.; Paju, S.; Pietiäinen, M.; Buhlin, K.; Persson, G.R.; Nieminen, M.S.; Sinisalo, J.; Mäntylä, P.; Pussinen, P.J. Immunologic burden links periodontitis to acute coronary syndrome. Atherosclerosis 2018, 268, 177–184. [Google Scholar] [CrossRef]
- Beukers, N.G.F.M.; van der Heijden, G.J.M.G.; van Wijk, A.J.; Loss, B.G. Periodontitis is an independent risk indicator for atherosclerotic cardiovascular disease among 60174 participants in a large dental school in the Netherlands. J. Epidemiol. Community Health 2017, 71, 37–42. [Google Scholar] [CrossRef]
- Benedek, T.; Rodean, I.; Ratiu, M.; Rat, N.; Yero Eremie, L.; Biriș, C.; Lazăr, L.; Păcurar, M.; Benedek, I. Periodontal disease, inflammation and atherosclerotic progression in patients with acute coronary syndromes – the ATHERODENT study. J. Cardiovasc. Emerg. 2018, 4, 17–23. [Google Scholar] [CrossRef]
- Mitra, N.; Hodas, R.; Szabo, E.; Parajko, Z.; Benedek, T.; Benedek, I. Impact of coronary plaque vulnerability on acute cardiovascular events – Design of a CT-based 2-year Follow-up Study. J. Interdiscip. Med. 2019, 4, 64–71. [Google Scholar] [CrossRef]
- Bom, M.J.; van der Heijden, D.J.; Kehdi, E.; van der Heyden, J.; Meuwissen, M.; Knaapen, P.; Timmer, S.A.J.; van Royen, N. Early detection and treatment of the vulnerable coronary plaque: Can we prevent acute coronary syndromes? Circ. Cardiovasc. Imaging 2017, 10, 1–21. [Google Scholar] [CrossRef] [PubMed]
- Carrizales-Sepulveda, E.F.; Ordaz-Farias, A.; Vera-Pineda, R.; Flores-Ramirez, R. Periodontal disease, systemic inflammation and the risk of cardiovascular disease. Hear Lung. Circ. 2018, 27, 1327–1334. [Google Scholar] [CrossRef]
- Greenland, P.; Blaha, M.J.; Budoff, M.J.; Erbel, R.; Watson, K. Coronary calcium score and cardiovascular risk. J. Am. Coll. Cardiol. 2018, 72, 434–447. [Google Scholar] [CrossRef]
- Azour, L.; Kadoch, M.A.; Ward, T.J.; Eber, C.D.; Jacobi, A.H. Estimation of cardiovascular risk on routine chest CT: Ordinal coronary artery calcium scoring as an accurate predictor of Agaston score ranges. J. Cardiovasc. Comput. Tomog. 2017, 11, 8–15. [Google Scholar] [CrossRef]
- Licu, R.-A.; Blându, E.; Opincariu, D.; Benedek, T. Vulnerable plaques producing an acute coronary syndrome exhibit a different CT phenotype than those that remain silent. J. Cardiovasc. Emerg. 2020, 6, 26–34. [Google Scholar] [CrossRef]
- Collet, J.P.; Thiele, H.; Barbato, E.; Barthélémy, O.; Bauersachs, J.; Bhatt, D.L.; Dendale, P.; Dorobantu, M.; Edvardsen, T.; Folliguet, T.; et al. 2020 ESC guidelines for the management of acute coronary syndromes in patients presenting without persistent ST-segment elevation. Eur. Heart J. 2020, 1–79. [Google Scholar]
- Cho, I.; Al’Aref, S.J.; Berger, A.; Hartaigh, B.; Gransar, H.; Valenti, V.; Lin, F.Y.; Achenbach, S.; Berman, D.S.; Budoff, M.J.; et al. Prognostic value of coronary computed tomographic angiography findings in asymptomatic individuals: A 6-year follow-up from the prospective multicentre international CONFIRM study. Eur. Heart J. 2018, 39, 934–941. [Google Scholar] [CrossRef]
- Sun, Z.; Xu, L. Coronary CT angiography in the quantitative assessment of coronary plaques. Biomed. Res. Int. 2014, 2014, 346380. [Google Scholar] [CrossRef]
- Augusta, M.; Rebelo, B.; De Queiroz, A.C. Gingival Indices: State of Art, Gingival Diseases-Their Aetiology, Prevention and Treatment; InTech: London, UK, 2011; pp. 41–54. [Google Scholar]
- Newman, M.G.; Takei, H.H.; Klokkevold, P.R. Carranza’s Clinical Periodontology; Carranza, F.A., Ed.; Saunders Elsevier: St. Louis, MO, USA, 2012; Internet resource. [Google Scholar]
- Dhingra, K.; Laxman, V. Indices for measuring periodontitis: A literature review. Int. Dent. J. 2011, 61, 76–84. [Google Scholar] [CrossRef]
- Dogan, S.; Duivenvoorden, R.; Grobbee, D.E.; Kastelein, J.J.; Shear, C.L.; Evans, G.W.; Visseren, F.L.; Bots, M.L. Ultrasound protocols to measure carotid intima-media thickness in trials; comparison of reproducibility, rate of progression, and effect of intervention in subjects with familial hypercholesterolemia and subjects with mixed dyslipidemia. Ann. Med. 2010, 42, 447–464. [Google Scholar] [CrossRef] [PubMed]
- Stein, J.H.; Korcarz, C.E.; Hurst, R.T.; Lonn, E.; Kendall, C.B.; Mohler, E.R.; Najjar, S.S.; Rembold, C.M.; Post, W.S. Use of carotid ultrasound to identify subclinical vascular disease and evaluate cardiovascular disease risk: A consensus statement from the American Society of Echocardiography Carotid Intima-Media Thickness Task Force. Endorsed by the Society for Vascular Medicine. J. Am. Soc. Echocardiogr. 2007, 21, 189–193. [Google Scholar]
- Priyamvara, A.; Dey, A.K.; Bandyopadhyay, D.; Katikineni, V.; Zaghlol, R.; Basyal, B.; Barssoum, K.; Amarin, R.; Bhatt, D.L.; Lavie, C.J. Periodontal inflammation and the risk of Cardiovascular Disease. Curr. Atheroscler Rep. 2020, 22, 2–6. [Google Scholar] [CrossRef]
- Bourgeois, D.; Inquimbert, C.; Ottolenghi, L.; Carrouel, F. Periodontal pathogens as risk factors of cardiovascular disease, diabetes, rheumatoid arthritis, cancer, and chronic obstructive pulmonary disease–is there cause for consideration? Microorganisms 2019, 7, 424. [Google Scholar] [CrossRef] [PubMed]
- DeStefano, F.; Anda, R.F.; Kahn, H.S.; Williamson, D.F.; Russell, C.M. Dental disease and risk of coronary heart disease and mortality. Br. Med. J. 1993, 306, 688–691. [Google Scholar] [CrossRef]
- Van der Biyl, P. Periodontal and cardiovascular diseases. Actual Probl. Dent. 2014, 10, 4–9. [Google Scholar] [CrossRef][Green Version]
- Singer, R.H.; Stoutenberg, M.; Feaster, D.J.; Cai, J.; Hlaing, W.W.M.; Metsch, L.R.; Salazar, C.R.; Beaver, S.M.; Finlayson, T.L.; Talavera, G.; et al. The association of periodontal disease and cardiovascular disease risk: Results from the Hispanic Community Health Study/Study of Latinos. J. Periodontol. 2018, 89, 840–857. [Google Scholar] [CrossRef]
- Pires, J.R.; dos Santos, I.P.; de Camargo, L.F.; Zuza, E.P.; de Toledo, B.E.C.; Monteiro, S.C.M. Framingham cardiovascular risk in patients with obesity and periodontitis. J. Indian Soc. Periodontol. 2014, 18, 14–18. [Google Scholar] [CrossRef]
- Dwivedi, A.; Al’Aref, S.J.; Lin, F.Y.; Min, J.K. Evaluation of atherosclerotic plaque in non-invasive coronary imaging. Korean Circ. J. 2018, 48, 124–133. [Google Scholar] [CrossRef] [PubMed]
- Donders, H.C.M.; IJzerman, L.M.; Soffner, M.; van ‘t Hof, A.W.J.; Loss, B.G.; de Lange, J. Elevated coronary artery calcium scores are associated with tooth loss. PLoS ONE 2020, 15, e0243232. [Google Scholar] [CrossRef] [PubMed]
- De Boer, S.P.M.; Cheng, J.M.; Range, H.; Garcia-Garcia, H.M.; Heo, J.H.; Akkerhuis, K.M.; Meilhac, O.; Cosler, G.; Pussinen, P.J.; van Genus, R.-J.; et al. Antibodies to periodontal pathogens are associated with coronary plaque remodeling but not with vulnerability or burden. Atherosclerosis 2014, 237, 84–91. [Google Scholar] [CrossRef] [PubMed]
- World Health Organization. Time to deliver: Report of the WHO Independent High-level Commission on Noncommunicable Diseases; Licence: CC BY-NC-SA 3.0 IGO; 2018; pp. 1–44. Available online: https://www.who.int/ncds/management/time-to-deliver/en/ (accessed on 1 February 2021).
- Bobetsis, Y.A.; Kotsikoris, I.; Liapis, C.D.; Liasis, N.; Kakisis, J.; Kourlaba, G.; Lazari, P.; Antonopoulos, C.N.; Deliargyris, E.N.; Madianos, P.N. Association between periodontal disease and vulnerable plaque morphology in patients undergoing carotid endarterectomy. IJC Hear Vasc. 2020, 30, 100601. [Google Scholar] [CrossRef] [PubMed]
- Wojtkowska, A.; Zapolski, T.; Wysokinska-Miszczuk, J.; Wysokinski, A.P. The inflammation link between periodontal disease and coronary atherosclerosis in patients with acute coronary syndromes: Case-control study. BMC Oral Health 2021, 21, 5. [Google Scholar] [CrossRef] [PubMed]
- Gustafsson, N.; Ahlqvist, J.; Näslund, U.; Buhlin, K.; Gustafsson, A.; Kjellström, B.; Klinge, B.; Levring Jäghagen, E. Associations among periodontitis, calcified carotid artery atheromas and risk of myocardial infarction. J. Dent. Res. 2020, 99, 60–68. [Google Scholar] [CrossRef]
- Nitya, K.N.; Doshi, D.; Kulkarni, S.; Reddy, M.P.; Srilatha, A.; Satyanarayana, D. Assessment of periodontal status based on carotid artery intima media thickness. Oral Health Prev. Dent. 2020, 18, 511–519. [Google Scholar]
- Pussinen, P.J.; Paju, S.; Koponen, J.; Vilkari, J.S.A.; Taittonen, L.; Laitinen, T.; Burgner, D.P.; Kähönen, M.; Hutri-Kähönen, N.; Raitakari, O.T.; et al. Association of childhood oral infections with cardiovascular risk factors and subclinical atherosclerosis in adulthood. JAMA Netw. Open 2019, 2, e192523. [Google Scholar] [CrossRef]
- Bell, S.; Gibson, J.T.; Harshfield, E.L.; Markus, H.S. Is periodontitis a risk factor for ischaemic stroke, coronary artery disease and subclinical atherosclerosis? A Mendelian randomization study. Atherosclerosis 2020, 313, 111–117. [Google Scholar] [CrossRef]
- Karraeren, C.; Uraz, A.; Gursoy, C.; Bal, A.B. Association between body mass index and waist circumference with periodontal health state. Ann. Med. Res. 2019, 26, 1531–1540. [Google Scholar] [CrossRef]
- Saxlin, T.; Ylostalo, P.; Suominen-Taipale, L.; Aromaa, A.; Knuuttila, M. Overweight and obesity wakly predict the development of periodontal infection. J. Clin. Periodontol. 2010, 37, 1059–1067. [Google Scholar] [CrossRef] [PubMed]
- Kahn, S.; Barrington, G.; Bettiol, S.; Barnett, T.; Crocombe, L. Is overweight/obesity a risk factor for periodontitis in young adults and adolscents?: A systematic review. Obes. Rev. 2018, 19, 852–883. [Google Scholar] [CrossRef] [PubMed]
- Abdalla-Aslan, R.; Findler, M.; Levin, L.; Zini, A.; Shay, B.; Twig, G.; Almoznino, G. Where periodontitis meets metabolic syndrome – the role of common health-related risk factors. J. Oral Reh. 2019, 46, 647–656. [Google Scholar] [CrossRef] [PubMed]
| Periodontal Indices | 0 | 1 | 2 | 3 | 4 |
|---|---|---|---|---|---|
| GI | Normal, healthy gum | Mild inflammation | Moderate inflammation | Advanced inflammation | - |
| PqI | No plaque | Plaque < 1/3 of the tooth surface | Plaque between 1/3–2/3 of the tooth surface | Plaque > 2/3 of the tooth surface | - |
| CI | No calculus | Calculus < 1/3 of the tooth surface | Calculus between 1/3–2/3 of the tooth surface | Calculus > 2/3 of the tooth surface | - |
| FI | The furcation probe cannot enter the furcation area | The probe is able to partially enter the furcation, extending less than 1/3 of the width of the tooth | The probe extends more than ½ of the width of the tooth but does not pass completely through the furcation | The probe passes completely through the furcation | - |
| PBI (Muehlemann index) | No bleeding | Bleeding isolated visible one point | Multiple bleeding points | Red line in the margin | Heavy bleeding or profuse |
| Tooth mobility | No apparent mobility | Horizontal, bucco–oral movement < 1 mm | Horizontal, bucco–oral movement >1 mm | Horizontal, bucco-oral movement >1 mm, also in the axial direction | - |
| CAL | No attachment loss | Mild, between 1 and 2 mm | Moderates between 3 and 4 mm | Severe, >5 mm | - |
| PPD | Distance between 1 and 3 mm | Distance between 3 and 5 mm | Distance between 5 and 7 mm | Distance > 7 mm | - |
| Variables | Group 1—LPI | Group 2—HPI | p VALU | ||
|---|---|---|---|---|---|
| Mean age (y) | |||||
| 50.27 | 54.65 | 0.2 | |||
| Mean Weight (kg) | 87.5 | 85.04 | 0.6 | ||
| Mean height (cm) | |||||
| 173.90 | 169.5 | 0.1 | |||
| Mean BMI (kg/m2) | 28.75 | 29.49 | 0.6 | ||
| Gender distribution N (%) | Male | Female | Male | Female | 0.008 |
| 17 (65.38%) | 9 (34.61%) | 20 (76.92%) | 6 (23.08%) | ||
| Residency N (%) | Urban | Rural | Urban | Rural | 0.6 |
| 15 (57.69%) | 11 (42.31%) | 16 (61.53%) | 9 (38.47%) | ||
| Smoker status N (%) | Smoker | Non-smoker | Smoker | Non-smoker | 0.2 |
| 6 (23.07%) | 20 (76.93%) | 8 (30.76%) | 16 (69.24%) | ||
| Periodontal Indices | Low-Risk Plaque | High-Risk Plaque | p Value |
|---|---|---|---|
| GI | 3.5 +/− 2.21 | 5 +/− 2.66 | 0.07 |
| PqI | 5.14 +/− 4.02 | 7.5 +/− 3.97 | 0.1 |
| CI | 2.74 +/− 2.14 | 2.6 +/− 1.83 | 0.7 |
| FI | 0.21 +/− 0.56 | 0.4 +/− 1.26 | 0.4 |
| PBI | 2.048 +/− 1.96 | 4.5 +/− 3.064 | 0.002 |
| Mobility | 2.83 +/− 2.56 | 3.2 +/− 2.57 | 0.6 |
| CAL | 1.66 +/− 1.8 | 3.6 +/− 2.91 | 0.009 |
| PPD | 0.83 +/− 1.2 | 1.4 +/− 1.35 | 0.2 |
| Low-Risk Plaque | High-Risk Plaque | p Value | |
| Plaque volume | 143.88 +/− 217.08 | 320.89 +/− 329.27 | 0.01 |
| Calcified volume | 109.08 +/− 157.46 | 270 +/− 297.41 | 0.01 |
| Noncalcified plaque volume | 34.85 +/− 89.77 | 55.02 +/− 65.75 | 0.003 |
| Lipid-rich plaque volume | 15.77 +/− 53.37 | 10.29 +/− 11.87 | 0.05 |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2021 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Rodean, I.-P.; Lazăr, L.; Halațiu, V.-B.; Biriș, C.; Benedek, I.; Benedek, T. Periodontal Disease Is Associated with Increased Vulnerability of Coronary Atheromatous Plaques in Patients Undergoing Coronary Computed Tomography Angiography—Results from the Atherodent Study. J. Clin. Med. 2021, 10, 1290. https://doi.org/10.3390/jcm10061290
Rodean I-P, Lazăr L, Halațiu V-B, Biriș C, Benedek I, Benedek T. Periodontal Disease Is Associated with Increased Vulnerability of Coronary Atheromatous Plaques in Patients Undergoing Coronary Computed Tomography Angiography—Results from the Atherodent Study. Journal of Clinical Medicine. 2021; 10(6):1290. https://doi.org/10.3390/jcm10061290
Chicago/Turabian StyleRodean, Ioana-Patricia, Luminița Lazăr, Vasile-Bogdan Halațiu, Carmen Biriș, Imre Benedek, and Theodora Benedek. 2021. "Periodontal Disease Is Associated with Increased Vulnerability of Coronary Atheromatous Plaques in Patients Undergoing Coronary Computed Tomography Angiography—Results from the Atherodent Study" Journal of Clinical Medicine 10, no. 6: 1290. https://doi.org/10.3390/jcm10061290
APA StyleRodean, I.-P., Lazăr, L., Halațiu, V.-B., Biriș, C., Benedek, I., & Benedek, T. (2021). Periodontal Disease Is Associated with Increased Vulnerability of Coronary Atheromatous Plaques in Patients Undergoing Coronary Computed Tomography Angiography—Results from the Atherodent Study. Journal of Clinical Medicine, 10(6), 1290. https://doi.org/10.3390/jcm10061290







