Non-Criteria Manifestations of Juvenile Antiphospholipid Syndrome
Abstract
1. Introduction
2. Primary and Secondary Antiphospholipid Syndrome in Children
3. Thrombogenic Mechanisms in Antiphospholipid Syndrome
4. Classification Criteria for Antiphospholipid Syndrome
5. Non-Criteria Manifestations in Antiphospholipid Syndrome
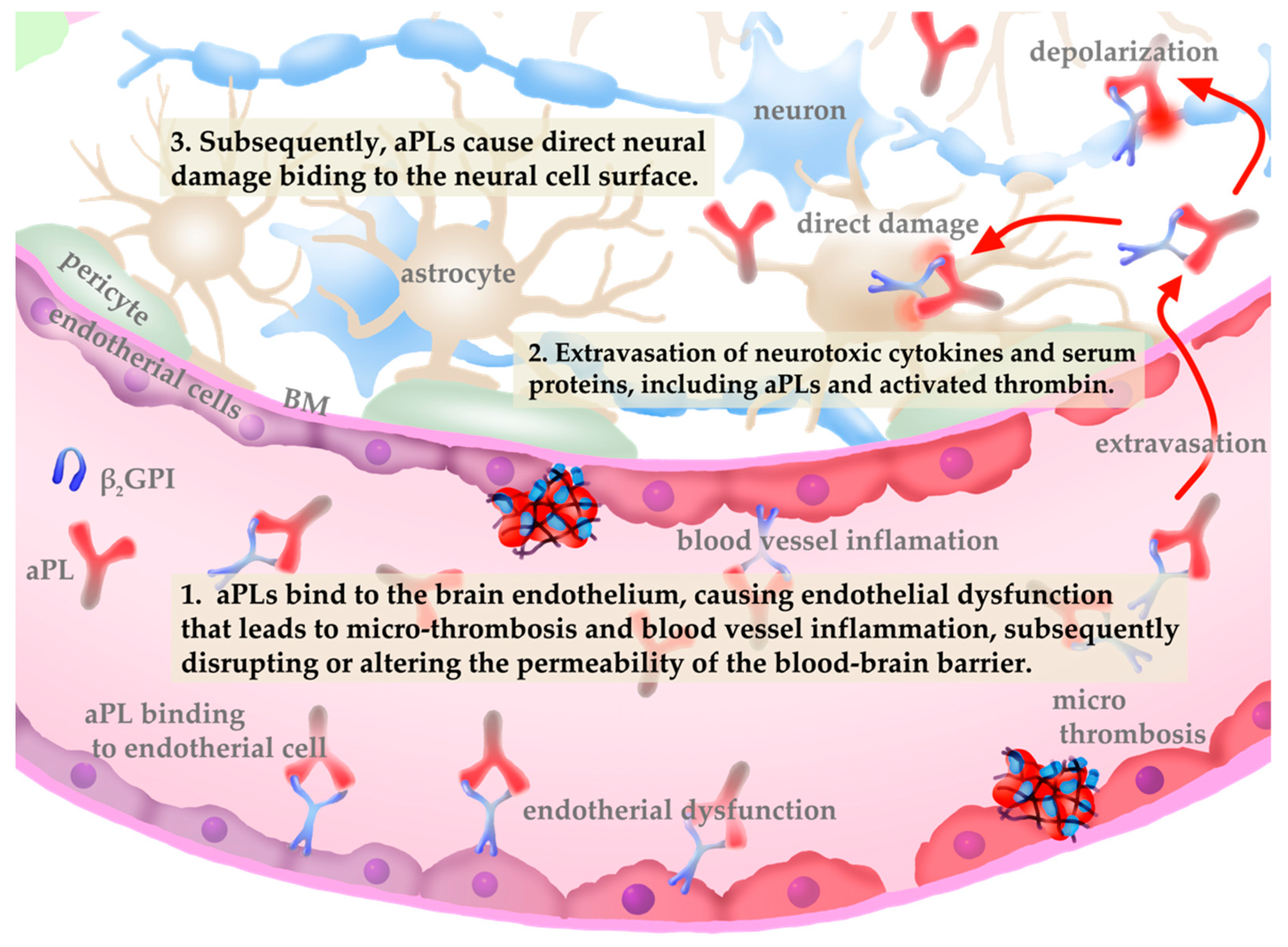
5.1. Non-Criteria Neurological Manifestations in Antiphospholipid Syndrome
5.1.1. Migraine
5.1.2. Chorea
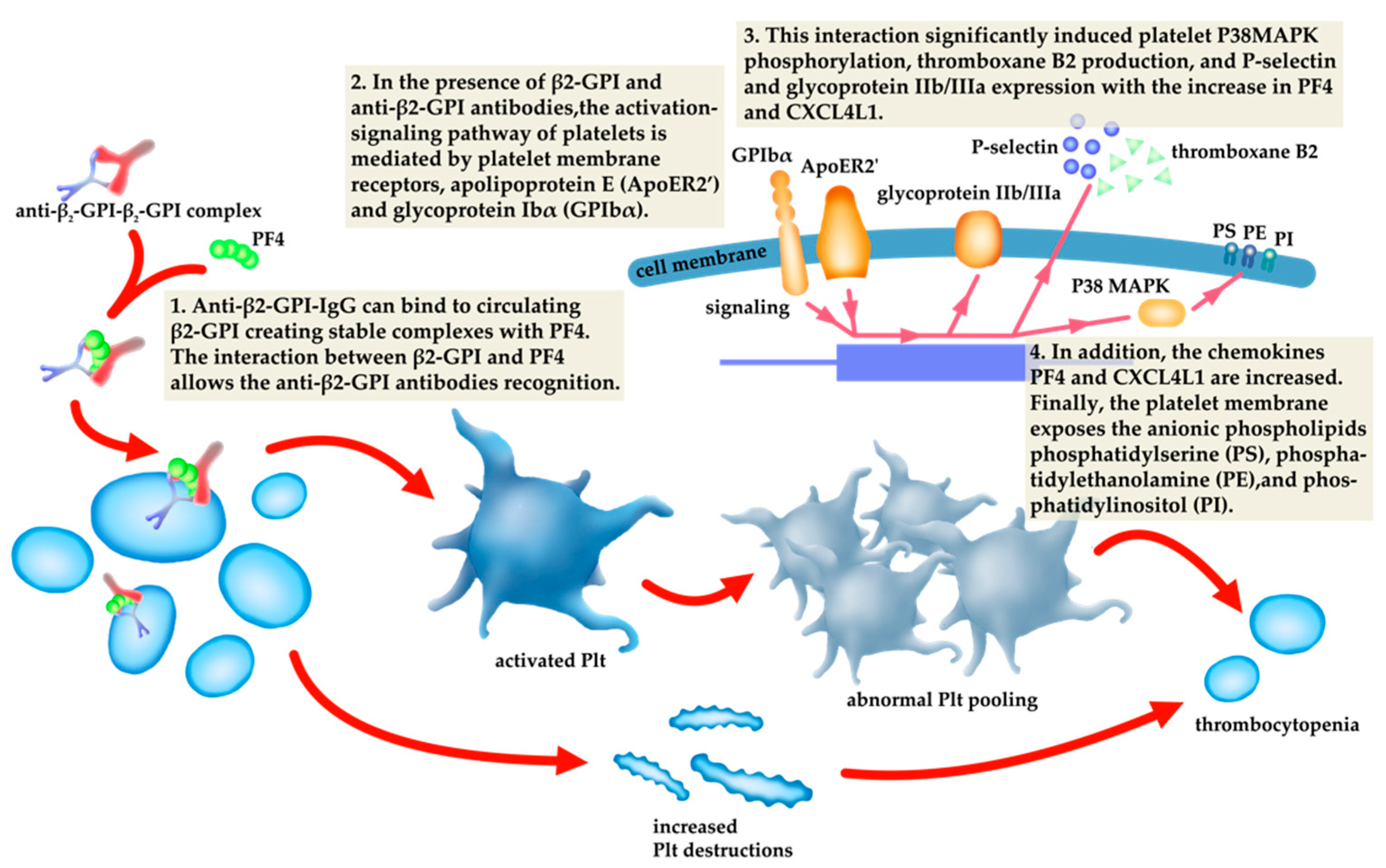
5.2. Non-Criteria Haematologic Manifestations of Antiphospholipid Syndrome
5.3. Non-Criteria Cardiovascular Manifestations in Antiphospholipid Syndrome
5.4. Non-Criteria Cutaneous Manifestations in Antiphospholipid Syndrome
5.5. Non-Criteria Renal Manifestations in Antiphospholipid Syndrome
6. Mechanisms Underlying Non-Criteria Manifestations Associated with aPLs and Potential Targeted Therapies
7. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Acknowledgments
Conflicts of Interest
References
- Lim, W. Antiphospholipid syndrome. Hematol. Am. Soc. Hematol. Educ. Program. 2013, 2013, 675–680. [Google Scholar] [CrossRef]
- Miyakis, S.; Lockshin, M.D.; Atsumi, T.; Branch, D.W.; Brey, R.L.; Cervera, R.; Derksen, R.H.W.M.; De Groot, P.G.; Koike, T.; Meroni, P.L.; et al. International consensus statement on an update of the classification criteria for definite antiphospholipid syndrome (APS). J. Thromb. Haemost. 2006, 4, 295–306. [Google Scholar] [CrossRef]
- Pengo, V.; Tripodi, A.; Reber, G.; Rand, J.H.; Ortel, T.L.; Galli, M.; De Groot, P.G. Update of the guidelines for lupus anticoagulant detection. J. Thromb. Haemost. 2009, 7, 1737–1740. [Google Scholar] [CrossRef]
- Hughes, G.R. Thrombosis, abortion, cerebral disease, and the lupus anticoagulant. BMJ 1983, 287, 1088–1089. [Google Scholar] [CrossRef]
- Giannakopoulos, B.; Krilis, S.A. The Pathogenesis of the Antiphospholipid Syndrome. N. Engl. J. Med. 2013, 368, 1033–1044. [Google Scholar] [CrossRef]
- Avčin, T.; Cimaz, R.; Silverman, E.D.; Cervera, R.; Gattorno, M.; Garay, S.; Berkun, Y.; Sztajnbok, F.R.; Silva, C.A.; Campos, L.M.; et al. Pediatric Antiphospholipid Syndrome: Clinical and Immunologic Features of 121 Patients in an International Registry. Pediatrics 2008, 122, e1100–e1107. [Google Scholar] [CrossRef] [PubMed]
- Petri, M. Epidemiology of the Antiphospholipid Antibody Syndrome. J. Autoimmun. 2000, 15, 145–151. [Google Scholar] [CrossRef]
- Cervera, R.; Serrano, R.; Pons-Estel, G.; Ceberio-Hualde, L.; Shoenfeld, Y.; De Ramón, E.; Buonaiuto, V.; Jacobsen, S.; Zeher, M.; Tarr, T.; et al. Morbidity and mortality in the antiphospholipid syndrome during a 10-year period: A multicentre prospective study of 1000 patients. Ann. Rheum. Dis. 2014, 74, 1011–1018. [Google Scholar] [CrossRef]
- Amengual, O.; Atsumi, T.; Khamashta, M.A. Tissue factor in antiphospholipid syndrome: Shifting the focus from coagulation to endothelium. Rheumatology 2003, 42, 1029–1031. [Google Scholar] [CrossRef] [PubMed]
- Vlachoyiannopoulos, P.G.; Routsias, J.G. A novel mechanism of thrombosis in antiphospholipid antibody syndrome. J. Autoimmun. 2010, 35, 248–255. [Google Scholar] [CrossRef]
- Sikara, M.P.; Routsias, J.G.; Samiotaki, M.; Panayotou, G.; Moutsopoulos, H.M.; Vlachoyiannopoulos, P.G. β2 Glycoprotein I (β2GPI) binds platelet factor 4 (PF4): Implications for the pathogenesis of antiphospholipid syndrome. Blood 2010, 115, 713–723. [Google Scholar] [CrossRef]
- Harper, B.E.; Willis, R.; Pierangeli, S.S. Pathophysiological mechanisms in antiphospholipid syndrome. Int. J. Clin. Rheumatol. 2011, 6, 157–171. [Google Scholar] [CrossRef] [PubMed]
- Manukyan, G.; Martirosyan, A.; Slavik, L.; Margaryan, S.; Ulehlova, J.; Mikulkova, Z.; Hlusi, A.; Papajik, T.; Kriegova, E. Anti-domain 1 β2 glycoprotein antibodies increase expression of tissue factor on monocytes and activate NK Cells and CD8+ cells in vitro. Autoimmun. Highlights 2020, 11, 5–9. [Google Scholar] [CrossRef]
- Oku, K.; Nakamura, H.; Kono, M.; Ohmura, K.; Kato, M.; Bohgaki, T.; Horita, T.; Yasuda, S.; Amengual, O.; Atsumi, T. Complement and thrombosis in the antiphospholipid syndrome. Autoimmun. Rev. 2016, 15, 1001–1004. [Google Scholar] [CrossRef]
- Kronbichler, A.; Frank, R.; Kirschfink, M.; Szilagyi, A. Efficacy of eculizumab in a patient with immunoadsorption-dependent catastrophic antiphospholipid syndrome: A case report. Medicine 2014. [Google Scholar] [CrossRef]
- Wig, S.; Chan, M.; Thachil, J.; Bruce, I.; Barnes, T. A case of relapsing and refractory catastrophic anti-phospholipid syndrome successfully managed with eculizumab, a complement 5 inhibitor. Rheumatology 2015, 55, 382–384. [Google Scholar] [CrossRef][Green Version]
- Lonze, B.E.; Zachary, A.A.; Magro, C.M.; Desai, N.M.; Orandi, B.J.; Dagher, N.N.; Singer, A.L.; Carter-Monroe, N.; Nazarian, S.M.; Segev, D.L.; et al. Eculizumab Prevents Recurrent Antiphospholipid Antibody Syndrome and Enables Successful Renal Transplantation. Am. J. Transp. 2014, 14, 459–465. [Google Scholar] [CrossRef] [PubMed]
- Aggarwal, R.; Ringold, S.; Khanna, D.; Neogi, T.; Johnson, S.R.; Miller, A.; Brunner, H.I.; Ogawa, R.; Felson, D.; Ogdie, A.; et al. Distinctions between diagnostic and classification criteria? Arthritis. Care Res. 2015, 67, 891–897. [Google Scholar] [CrossRef] [PubMed]
- Groot, N.; De Graeff, N.; Avcin, T.; Bader-Meunier, B.; Dolezalova, P.; Feldman, B.; Kenet, G.; Koné-Paut, I.; Lahdenne, P.; Marks, S.D.; et al. European evidence-based recommendations for diagnosis and treatment of paediatric antiphospholipid syndrome: The SHARE initiative. Ann. Rheum. Dis. 2017, 76, 1637–1641. [Google Scholar] [CrossRef]
- Avcin, T.; Cimaz, R.; Meroni, P. Letter to the Editor. Lupus 2001, 10, 897–898. [Google Scholar] [CrossRef]
- Avcin, T.; Cimaz, R.; Meroni, P.L. Recent advances in antiphospholipid antibodies and antiphospholipid syndromes in pediatric populations. Lupus 2002, 11, 4–10. [Google Scholar] [CrossRef] [PubMed]
- Cimaz, R.; Descloux, E. Pediatric Antiphospholipid Syndrome. Rheum. Dis. Clin. N. Am. 2006, 32, 553–573. [Google Scholar] [CrossRef] [PubMed]
- Ravelli, A.; Martini, A. Antiphospholipid Syndrome in Pediatrics. Rheum. Dis. Clin. N. Am. 2007, 33, 499–523. [Google Scholar] [CrossRef] [PubMed]
- Asherson, R.A. The catastrophic antiphospholipid syndrome. J. Rheumatol. 1992, 19, 508–512. [Google Scholar]
- Piette, J.C.; Cervera, R.; Levy, R.A.; Nasonov, E.L.; Triplett, D.A.; Shoenfeld, Y. The catastrophic antiphospholipid syn-drome--Asherson’s syndrome. Ann. Med. Intern. 2003, 154, 195–196. [Google Scholar]
- Campos, L.M.A.; Kiss, M.H.; A D’Amico, É.; Silva, C.A.A. Antiphospholipid antibodies and antiphospholipid syndrome in 57 children and adolescents with systemic lupus erythematosus. Lupus 2003, 12, 820–826. [Google Scholar] [CrossRef]
- Rozic, M.; Trampus-Bakija, A.; Rener-Primec, Z.; Kitanovski, L.; Kveder, T.; Avcin, T. PReS-FINAL-2349: Spectrum of thrombotic and non-thrombotic manifestations in 159 children with positive antiphospholipid antibodies. Pediatr. Rheumatol. 2013, 11, P339. [Google Scholar] [CrossRef]
- Ma, J.; Song, H.; Wei, M.; He, Y. Clinical characteristics and thrombosis outcomes of paediatric antiphospholipid syndrome: Analysis of 58 patients. Clin. Rheumatol. 2018, 37, 1295–1303. [Google Scholar] [CrossRef]
- DeVeber, G.; Andrew, M.; Adams, C.; Bjornson, B.; Booth, F.; Buckley, D.J.; Camfield, C.S.; David, M.; Humphreys, P.; Langevin, P.; et al. Cerebral Sinovenous Thrombosis in Children. N. Engl. J. Med. 2001, 345, 417–423. [Google Scholar] [CrossRef]
- Muscal, E.; Brey, R. Antiphospholipid syndrome and the brain in pediatric and adult patients. Lupus 2010, 19, 406–411. [Google Scholar] [CrossRef] [PubMed]
- Cervera, R.; Boffa, M.-C.; A Khamashta, M.; Hughes, G.R.V. The Euro-Phospholipid project: Epidemiology of the antiphospholipid syndrome in Europe. Lupus 2009, 18, 889–893. [Google Scholar] [CrossRef] [PubMed]
- Chapman, J.; Rand, J.H.; Brey, R.L.; Levine, S.R.; Blatt, I.; A Khamashta, M.; Shoenfeld, Y. Non-stroke neurological syndromes associated with antiphospholipid antibodies: Evaluation of clinical and experimental studies. Lupus 2003, 12, 514–517. [Google Scholar] [CrossRef] [PubMed]
- Muscal, E.; Brey, R.L. Neurologic manifestations of the antiphospholipid syndrome: Integrating molecular and clinical lessons. Curr. Rheumatol. Rep. 2008, 10, 67–73. [Google Scholar] [CrossRef]
- Ziporen, L.; Shoenfeld, Y.; Lévy, Y.; Korczyn, A.D. Neurological dysfunction and hyperactive behavior associated with antiphospholipid antibodies. A mouse model. J. Clin. Investig. 1997, 100, 613–619. [Google Scholar] [CrossRef]
- Caronti, B.; Pittoni, V.; Palladini, G.; Valesini, G. Anti-β2-glycoprotein I antibodies bind to central nervous system. J. Neurol. Sci. 1998, 156, 211–219. [Google Scholar] [CrossRef]
- Steens, S.C.A.; Bosma, G.P.T.H.; Steup-Beekman, G.M.; Le Cessie, S.; Huizinga, T.W.J.; A Van Buchem, M. Association between microscopic brain damage as indicated by magnetization transfer imaging and anticardiolipin antibodies in neuropsychiatric lupus. Arthritis Res. 2006, 8, R38. [Google Scholar] [CrossRef] [PubMed]
- Stojanovich, L.; Kontic, M.; Smiljanic, D.; Djokovic, A.; Stamenkovic, B.; Marisavljevic, D. Association between non-thrombotic neurological and cardiac manifestations in patients with antiphospholipid syndrome. Clin. Exp. Rheumatol. 2013, 31, 756–760. [Google Scholar]
- Islam, A.; Alam, F.; Wong, K.K. Comorbid association of antiphospholipid antibodies and migraine: A systematic review and meta-analysis. Autoimmun. Rev. 2017, 16, 512–522. [Google Scholar] [CrossRef] [PubMed]
- Noureldine, M.H.A.; Haydar, A.A.; Berjawi, A.; Elnawar, R.; Sweid, A.; Khamashta, M.A.; Hughes, G.R.V.; Uthman, I. Antiphospholipid syndrome (APS) revisited: Would migraine headaches be included in future classification criteria? Immunol. Res. 2016, 65, 230–241. [Google Scholar] [CrossRef] [PubMed]
- Dvilansky, A.; Rishpon, S.; Nathan, I.; Zolotow, Z.; Korczyn, A.D. Release of platelet 5-hydroxytryptamine by plasma taken from patients during and between migraine attacks. Pain 1976, 2, 315–318. [Google Scholar] [CrossRef]
- Gladman, D.D.; Urowits, M.B.; Tozman, E.C.; Glynn, M.F.X. Haemostatic Abnormalities in Systemic Lupus Erythematosus. QJM Int. J. Med. 1983, 52, 424–433. [Google Scholar] [CrossRef]
- Karpatkin, S.; Siskind, G.W. In Vitro detection of platelet antibody in patients with idiopathic thrombocytopenic purpura and systemic lupus erythematosus. Blood 1969, 33, 795–812. [Google Scholar] [CrossRef] [PubMed]
- Harris, E.N.; Gharavi, A.E.; Hegde, U.; Derue, G.; Morgan, S.H.; Englert, H.; Chan, J.K.H.; Asherson, R.A.; Hughes, G.R.V. Anticardiolipin antibodies in autoimmune thrombocytopenic purpura. Br. J. Haematol. 1985, 59, 231–234. [Google Scholar] [CrossRef]
- Hughes, G. Connective tissue disease and the skin. Clin. Exp. Dermatol. 1984, 9, 535–544. [Google Scholar] [CrossRef] [PubMed]
- Cervera, R.; Piette, J.-C.; Font, J.; Khamashta, M.A.; Shoenfeld, Y.; Camps, M.T.; Jacobsen, S.; Lakos, G.; Tincani, A.; Kontopoulou-Griva, I.; et al. Antiphospholipid syndrome: Clinical and immunologic manifestations and patterns of disease expression in a cohort of 1000 patients. Arthritis Rheum. 2002, 46, 1019–1027. [Google Scholar] [CrossRef] [PubMed]
- Peluso, S.; Antenora, A.; De Rosa, A.; Roca, A.; Maddaluno, G.; Morra, V.B.; De Michele, G. Antiphospholipid-Related Chorea. Front. Neurol. 2012, 3, 150. [Google Scholar] [CrossRef] [PubMed]
- Abbott, N.J.; Mendonça, L.L.F.; Dolman, D.E.M. The blood-brain barrier in systemic lupus erythematosus. Lupus 2003, 12, 908–915. [Google Scholar] [CrossRef]
- Soltesz, P.; Der, H.; Veres, K.; Laczik, R.; Sipka, S.; Szegedi, G.; Szodoray, P. Immunological features of primary anti-phospholipid syndrome in connection with endothelial dysfunction. Rheumatology 2008, 47, 1628–1634. [Google Scholar] [CrossRef] [PubMed]
- Daneman, R.; Prat, A. The Blood–Brain Barrier. Cold Spring Harb. Perspect. Biol. 2015, 7, a020412. [Google Scholar] [CrossRef]
- Katzav, A.; Shoenfeld, Y.; Chapman, J. The Pathogenesis of Neural Injury in Animal Models of the Antiphospholipid Syndrome. Clin. Rev. Allergy Immunol. 2009, 38, 196–200. [Google Scholar] [CrossRef]
- Caronti, B.; Calderaro, C.; Alessandri, C.; Conti, F.; Tinghino, R.; Pini, C.; Palladini, G.; Valesini, G. Serum Anti-β2-glycoprotein I Antibodies from Patients with Antiphospholipid Antibody Syndrome Bind Central Nervous System Cells. J. Autoimmun. 1998, 11, 425–429. [Google Scholar] [CrossRef] [PubMed]
- Gris, J.-C.; Nobile, B.; Bouvier, S. Neuropsychiatric presentations of antiphospholipid antibodies. Thromb. Res. 2015, 135, S56–S59. [Google Scholar] [CrossRef]
- Brenner, B.; Gris, J.-C. Antiphospholipid Antibodies: Neuropsychiatric Presentations. Semin. Thromb. Hemost. 2013, 39, 935–942. [Google Scholar] [CrossRef]
- Chapman, J.; Cohen-Armon, M.; Shoenfeld, Y.; Korczyn, A.D. Antiphospholipid antibodies permeabilize and depolarize brain synaptoneurosomes. Lupus 1999, 8, 127–133. [Google Scholar] [CrossRef]
- Cervera, R.; Asherson, R.A.; Font, J.; Tikly, M.; Pallarés, L.; Chamorro, A.; Ingelmo, M. Chorea in the Antiphospholipid Syndrome: Clinical, Radiologic, and Immunologic Characteristics of 50 Patients from Our Clinics and the Recent Literature. Medicine 1997, 76, 203–226. [Google Scholar] [CrossRef] [PubMed]
- Orzechowski, N.M.; Wolanskyj, A.P.; Ahlskog, J.E.; Kumar, N.; Moder, K.G. Antiphospholipid Antibody-Associated Chorea. J. Rheumatol. 2008, 35, 2165–2170. [Google Scholar] [CrossRef]
- Reiner, P.; Galanaud, D.; Leroux, G.; Vidailhet, M.; Haroche, J.; Huong, D.L.T.; Francès, C.; Papo, T.; De Gennes, C.; Musset, L.; et al. Long-term outcome of 32 patients with chorea and systemic lupus erythematosus or antiphospholipid antibodies. Mov. Disord. 2011, 26, 2422–2427. [Google Scholar] [CrossRef]
- Zamora-Ustaran, A.; Escarcega-Alarcón, R.O.; Garcia-Carrasco, M.; Faugier, E.; Mendieta-Zeron, S.; Mendoza-Pinto, C.; Montiel-Jarquin, A.; Muñoz-Guarneros, M.; Lopez-Colombo, A.; Cervera, R. Antiphospholipid syndrome in Mexican children. Isr. Med. Assoc. J. 2012, 14, 286–289. [Google Scholar]
- El-Bostany, E.A.; El-Ghoroury, E.A.; El-Ghafar, E.A. Anti-β2-glycoprotein I in childhood immune thrombocytopenic purpura. Blood Coagul. Fibrinolysis 2008, 19, 26–31. [Google Scholar] [CrossRef]
- Baroni, G.; Banzato, A.; Bison, E.; Denas, G.; Zoppellaro, G.; Pengo, V. The role of platelets in antiphospholipid syndrome. Platelets 2017, 28, 762–766. [Google Scholar] [CrossRef] [PubMed]
- Patsouras, M.D.; Sikara, M.P.; Grika, E.P.; Moutsopoulos, H.M.; Tzioufas, A.G.; Vlachoyiannopoulos, P.G. Elevated expression of platelet-derived chemokines in patients with antiphospholipid syndrome. J. Autoimmun. 2015, 65, 30–37. [Google Scholar] [CrossRef] [PubMed]
- Zhang, W.; Zha, C.; Lu, X.; Jia, R.; Gao, F.; Sun, Q.; Jin, M.; Liu, Y. Anti-β2GPI/β2GPI complexes induce platelet activation and promote thrombosis via p38MAPK: A pathway to targeted therapies. Front. Med. 2019, 13, 680–689. [Google Scholar] [CrossRef] [PubMed]
- Artim-Esen, B.; Diz-Küçükkaya, R.; Inanç, M. The Significance and Management of Thrombocytopenia in Antiphospholipid Syndrome. Curr. Rheumatol. Rep. 2015, 17, 1–10. [Google Scholar] [CrossRef]
- Langer, H.F.; Verschoor, A. Crosstalk between platelets and the complement system in immune protection and disease. Thromb. Haemost. 2013, 110, 910–919. [Google Scholar] [CrossRef] [PubMed]
- Amigo, M.-C. What do we know about the cardiac valve lesion in the antiphospholipid syndrome (APS)? Lupus 2014, 23, 1259–1261. [Google Scholar] [CrossRef] [PubMed]
- Clauss, S.; Manco-Johnson, M.; Quivers, E.; Takemoto, C.; Spevak, P. Primary Antiphospholipid Antibody Syndrome and Cardiac Involvement in a Child. Pediatr. Cardiol. 2003, 24, 292–294. [Google Scholar] [CrossRef]
- Zuily, S.; Huttin, O.; Mohamed, S.; Marie, P.-Y.; Selton-Suty, C.; Wahl, D. Valvular Heart Disease in Antiphospholipid Syndrome. Curr. Rheumatol. Rep. 2013, 15, 320. [Google Scholar] [CrossRef] [PubMed]
- Asherson, R.A.; Cervera, R.; Shepshelovich, D.; Shoenfeld, Y. Nonthrombotic manifestations of the antiphospholipid syn-drome: Away from thrombosis? J. Rheumatol. 2006, 33, 1038–1044. [Google Scholar] [PubMed]
- Sciascia, S.; Amigo, M.-C.; Roccatello, D.; Khamashta, M. Diagnosing antiphospholipid syndrome: ‘extra-criteria’ manifestations and technical advances. Nat. Rev. Rheumatol. 2017, 13, 548–560. [Google Scholar] [CrossRef]
- Turrent-Carriles, A.; Herrera-Félix, J.P.; Amigo, M.-C. Renal Involvement in Antiphospholipid Syndrome. Front. Immunol. 2018, 9, 1008. [Google Scholar] [CrossRef] [PubMed]
- Canaud, G.; Bienaimé, F.; Tabarin, F.; Bataillon, G.; Seilhean, D.; Noël, L.-H.; Dragon-Durey, M.-A.; Snanoudj, R.; Friedlander, G.; Halbwachs-Mecarelli, L.; et al. Inhibition of the mTORC Pathway in the Antiphospholipid Syndrome. N. Engl. J. Med. 2014, 371, 303–312. [Google Scholar] [CrossRef] [PubMed]
- Kello, N.; El Khoury, L.; Marder, G.; Furie, R.; Zapantis, E.; Horowitz, D.L. Secondary thrombotic microangiopathy in systemic lupus erythematosus and antiphospholipid syndrome, the role of complement and use of eculizumab: Case series and review of literature. Semin. Arthritis Rheum. 2019, 49, 74–83. [Google Scholar] [CrossRef]
- Alves, J.D.; Grima, B. Oxidative stress in systemic lupus erythematosus and antiphospholipid syndrome: A gateway to atherosclerosis. Curr. Rheumatol. Rep. 2003, 5, 383–390. [Google Scholar] [CrossRef]
- López-Pedrera, C.; Barbarroja, N.; Jimenez-Gomez, Y.; Collantes-Estevez, E.; Aguirre, M.A.; Cuadrado, M.J. Oxidative stress in the pathogenesis of atherothrombosis associated with anti-phospholipid syndrome and systemic lupus erythematosus: New therapeutic approaches. Rheumatolology 2016, 55, 2096–2108. [Google Scholar] [CrossRef] [PubMed]
| Neurologic | Ophtalmoogic | Hematologic | Dermatologic | Musculosceletal | Cardiac | Pulmonary | Renal | Endocrine |
|---|---|---|---|---|---|---|---|---|
| Chorea * | Amaurosis Fugax [26] | Thrombocytopenia * | Livedo reticularis * | Osteonecrosis [26] | Valvular disease * | Pulmonary Hypertension | Intrarenal vasculopathy; APS neprhopathy (APSN) * | Adrenal insufficiency |
| Migraine/Headache | Hemolytic anemia | Raynaud’s Phenomenon | Arthritis [28] | Intestinal pneumonitis [26] | Glomerular disease | |||
| Seisure/Epilepsy | Evans syndrome | Purpura fulminans | Hypertension | |||||
| Transverse myelitis | Leukopenia | Skin ulcers | ||||||
| Pseudotumor cerebri | Bleeding diathesis | Pseudocasculitis lesions | ||||||
| Mood disorder | Chronic urticaria | |||||||
| Cognitive impairment |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2021 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Miyamae, T.; Kawabe, T. Non-Criteria Manifestations of Juvenile Antiphospholipid Syndrome. J. Clin. Med. 2021, 10, 1240. https://doi.org/10.3390/jcm10061240
Miyamae T, Kawabe T. Non-Criteria Manifestations of Juvenile Antiphospholipid Syndrome. Journal of Clinical Medicine. 2021; 10(6):1240. https://doi.org/10.3390/jcm10061240
Chicago/Turabian StyleMiyamae, Takako, and Tomohiro Kawabe. 2021. "Non-Criteria Manifestations of Juvenile Antiphospholipid Syndrome" Journal of Clinical Medicine 10, no. 6: 1240. https://doi.org/10.3390/jcm10061240
APA StyleMiyamae, T., & Kawabe, T. (2021). Non-Criteria Manifestations of Juvenile Antiphospholipid Syndrome. Journal of Clinical Medicine, 10(6), 1240. https://doi.org/10.3390/jcm10061240






