Relationship between Clinical Symptoms and Magnetic Resonance Imaging in Temporomandibular Disorder (TMD) Patients Utilizing the Piper MRI Diagnostic System
Abstract
1. Introduction
2. Experimental Section
2.1. Inclusion/Exclusion Criteria and Clinical Protocol
- -
- -
- Facial pain noted at least 3 months prior to the visit
- -
- Full dental arches (previous normal dental treatment without implants)
- -
- Orthodontic treatment was ended at least one year ago
- -
- General good health
- -
- At least 18 years of age
- -
- Fluent in Norwegian or English.
- -
- The exclusion criteria were as follows:
- -
- Undergoing or completed orthodontic treatment in the last 12 months
- -
- Previous craniofacial surgery and/or noted injuries
- -
- The patient was not willing to undergo MRI or not suited for MRI
- -
- Cognitive impairment
- -
- Psychiatric limitations that may affect the participation in the study assessments
2.2. MRI Imaging and TMJ Classification
2.3. Statistical Analysis
3. Results
3.1. The Correlation of Piper Classification on the Symptoms Related to TMJ Functioning
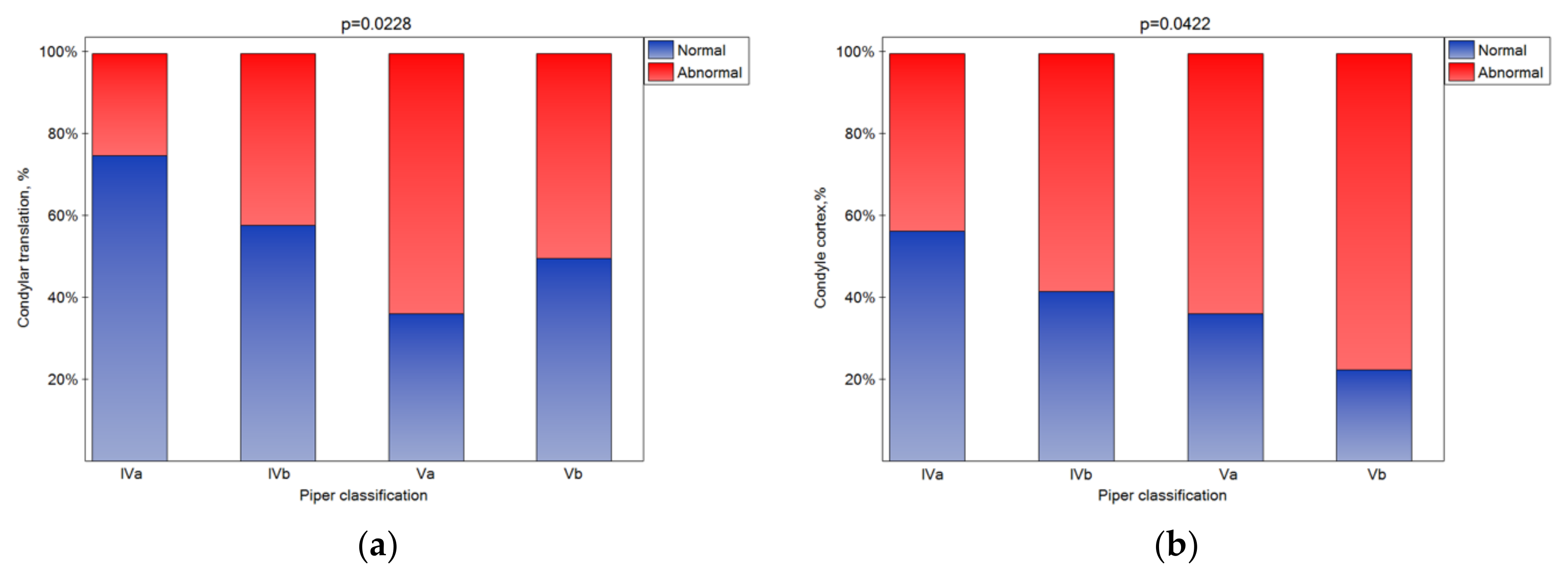
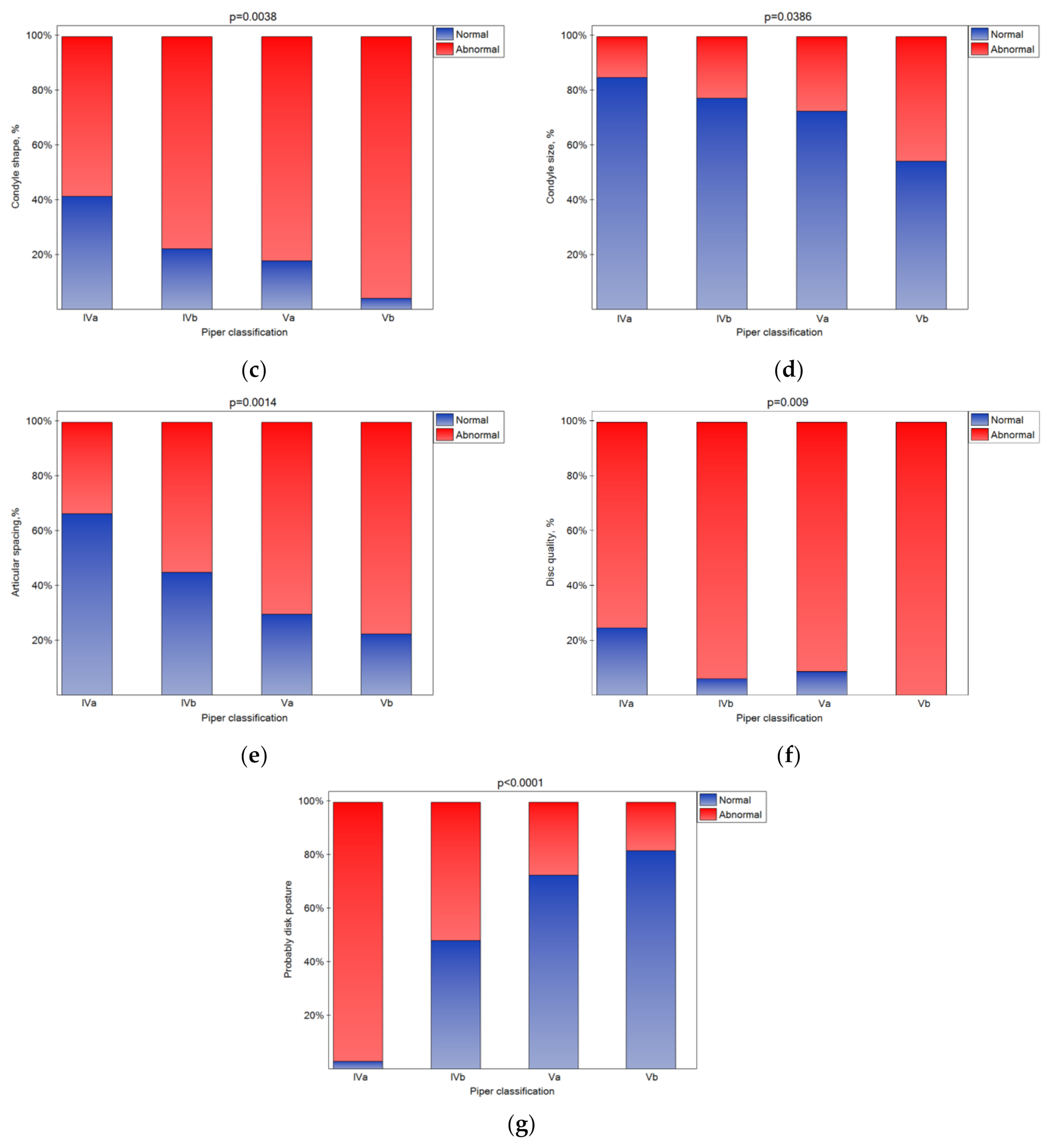
3.2. The Influence of the Piper Classification on Magnetic Resonance Imaging Results
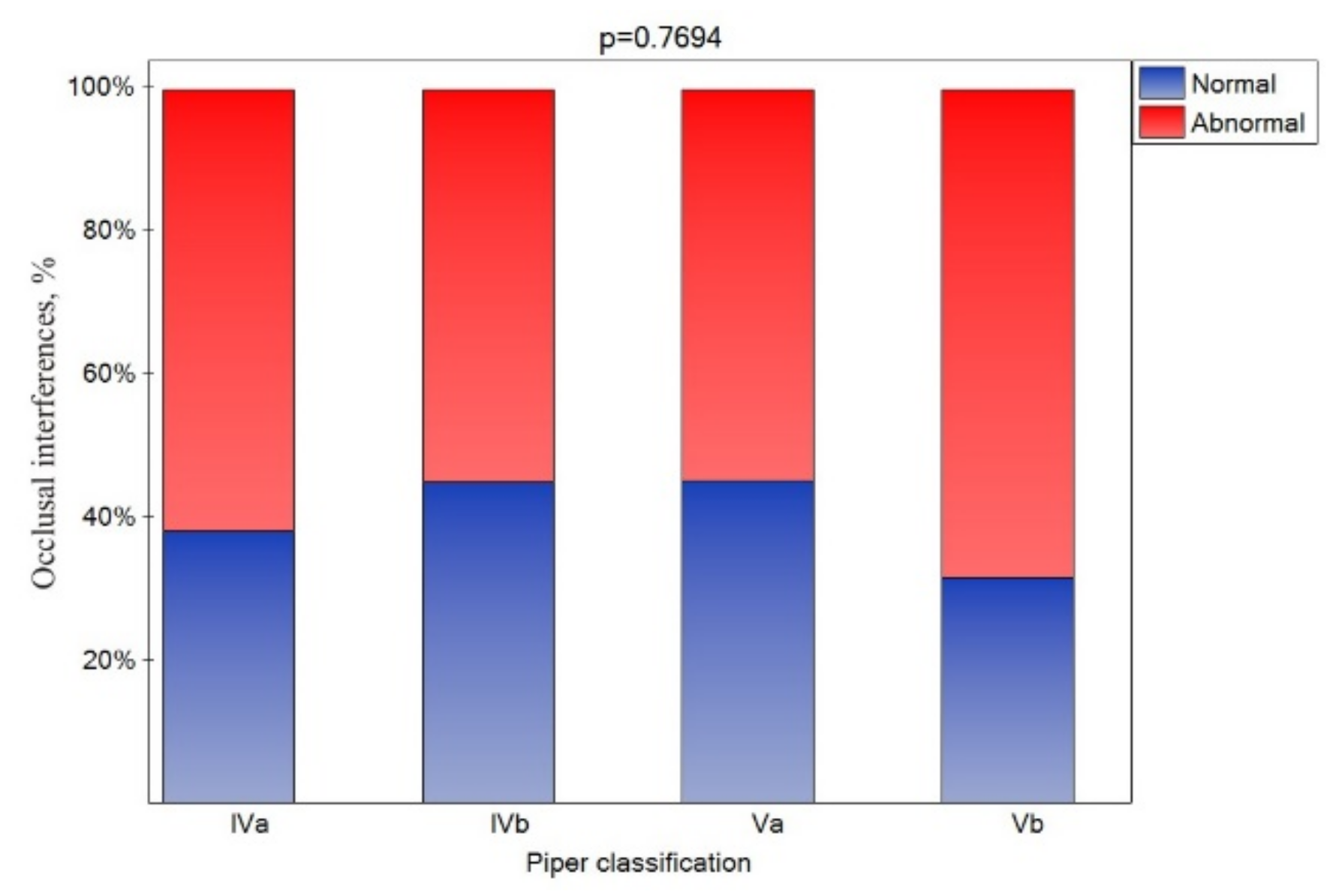
3.3. The Influence of the Piper Classification on Occlusal Interference
4. Discussion
4.1. MRI Accuracy
4.2. Clinical Symptoms and Imaging Findings
4.3. Occlusal Factors
4.4. Limitations
5. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Acknowledgments
Conflicts of Interest
References
- Upadhyaya, C.; Humagain, M. The Pattern of Tooth Loss Due to Dental Caries and Periodontal Disease among Patients Attending Dental Department (OPD), Dhulikhel Hospital, Kathmandu University Teaching Hospital (KUTH), Nepal. Kathmandu Univ. Med. J. 2009, 7, 59–62. [Google Scholar] [CrossRef]
- De Trize, D.M.; Calabria, M.P.; de Franzolin, S.O.B.; Cunha, C.O.; Marta, S.N. Is Quality of Life Affected by Temporomandibular Disorders? Einstein 2018, 16, eAO4339. [Google Scholar] [CrossRef]
- Maini, K.; Dua, A. Temporomandibular joint syndrome. In StatPearls; StatPearls Publishing: Treasure Island, FL, USA, 2020. [Google Scholar]
- Wieckiewicz, M.; Boening, K.; Wiland, P.; Shiau, Y.-Y.; Paradowska-Stolarz, A. Reported Concepts for the Treatment Modalities and Pain Management of Temporomandibular Disorders. J. Headache Pain 2015, 16, 106. [Google Scholar] [CrossRef]
- Durham, J.; Newton-John, T.R.O.; Zakrzewska, J.M. Temporomandibular Disorders. Br. Med. J. 2015, 350, h1154. [Google Scholar] [CrossRef]
- Thumati, P.; Manwani, R.; Mahantshetty, M. The Effect of Reduced Disclusion Time in the Treatment of Myofascial Pain Dysfunction Syndrome Using Immediate Complete Anterior Guidance Development Protocol Monitored by Digital Analysis of Occlusion. Cranio 2014, 32, 289–299. [Google Scholar] [CrossRef] [PubMed]
- Manfredini, D.; Guarda-Nardini, L.; Winocur, E.; Piccotti, F.; Ahlberg, J.; Lobbezoo, F. Research Diagnostic Criteria for Temporomandibular Disorders: A Systematic Review of Axis I Epidemiologic Findings. Oral Surg. Oral Med. Oral Pathol. Oral Radiol. Endod. 2011, 112, 453–462. [Google Scholar] [CrossRef]
- Liu, F.; Steinkeler, A. Epidemiology, Diagnosis, and Treatment of Temporomandibular Disorders. Dent. Clin. N. Am. 2013, 57, 465–479. [Google Scholar] [CrossRef] [PubMed]
- Lipton, J.A.; Ship, J.A.; Larach-Robinson, D. Estimated Prevalence and Distribution of Reported Orofacial Pain in the United States. J. Am. Dent. Assoc. 1993, 124, 115–121. [Google Scholar] [CrossRef] [PubMed]
- Sena, M.F.D.; Mesquita, K.S.F.D.; Santos, F.R.R.; Silva, F.W.G.; Serrano, K.V.D. Prevalence of Temporomandibular Dysfunction in Children and Adolescents. Rev. Paul Pediatr. 2013, 31, 538–545. [Google Scholar] [CrossRef] [PubMed]
- Greene, C.S. The Etiology of Temporomandibular Disorders: Implications for Treatment. J. Orofac. Pain 2001, 15, 93–105. [Google Scholar]
- Larheim, T.A.; Westesson, P.; Sano, T. Temporomandibular Joint Disk Displacement: Comparison in Asymptomatic Volunteers and Patients. Radiology 2001, 218, 428–432. [Google Scholar] [CrossRef] [PubMed]
- Espí-López, G.V.; Arnal-Gómez, A.; Cuerda del Pino, A.; Benavent-Corai, J.; Serra-Añó, P.; Inglés, M. Effect of Manual Therapy and Splint Therapy in People with Temporomandibular Disorders: A Preliminary Study. J. Clin. Med. 2020, 9, 2411. [Google Scholar] [CrossRef] [PubMed]
- Ebadian, B.; Abbasi, M.; Nazarifar, A.M. Frequency Distribution of Temporomandibular Disorders According to Occlusal Factors: A Cross-Sectional Study. Dent. Res. J. 2020, 17, 186–192. [Google Scholar]
- Van Grootel, R.J.; Buchner, R.; Wismeijer, D.; van der Glas, H.W. Towards an Optimal Therapy Strategy for Myogenous TMD, Physiotherapy Compared with Occlusal Splint Therapy in an RCT with Therapy-and-Patient-Specific Treatment Durations. BMC Musculoskelet. Disord. 2017, 18, 1–17. [Google Scholar] [CrossRef]
- Osiewicz, M.; Kojat, P.; Gut, M.; Kazibudzka, Z.; Pytko-Polończyk, J. Self-Perceived Dentists’ Knowledge of Temporomandibular Disorders in Krakow: A Pilot Study. Pain Res. Manag. 2020, 2020, 9531806. [Google Scholar] [CrossRef] [PubMed]
- López-Frías, F.-J.; Gil-Flores, J.; Bonilla-Represa, V.; Ábalos-Labruzzi, C.; Herrera-Martinez, M. Knowledge and Management of Temporomandibular Joint Disorders by General Dentists in Spain. J. Clin. Exp. Dent. 2019, 11, e680–e685. [Google Scholar] [CrossRef]
- Gnauck, M.; Magnusson, T.; Ekberg, E. Knowledge and Competence in Temporomandibular Disorders among Swedish General Dental Practitioners and Dental Hygienists. Acta Odontol. Scand. 2017, 75, 429–436. [Google Scholar] [CrossRef] [PubMed]
- Schiffman, E.; Ohrbach, R.; Truelove, E.; Look, J.; Anderson, G.; Goulet, J.-P.; List, T.; Svensson, P.; Gonzalez, Y.; Lobbezoo, F.; et al. Diagnostic Criteria for Temporomandibular Disorders (DC/TMD) for Clinical and Research Applications: Recommendations of the International RDC/TMD Consortium Network * and Orofacial Pain Special Interest Group †. J. Oralfac. Pain Headache 2014, 28, 6–27. [Google Scholar] [CrossRef]
- Kondrat, W.; Sierpińska, T.; Radke, J. Assessment of the Temporomandibular Joint Function in Young Adults without Complaints from the Masticatory System. Int. J. Med. Sci. 2018, 15, 161–169. [Google Scholar] [CrossRef]
- Huang, Z.; Lin, X.; Li, X. Characteristics of Temporomandibular Joint Vibrations in Anterior Disk Displacement with Reduction in Adults. Cranio 2011, 29, 276–283. [Google Scholar] [CrossRef]
- Emshoff, R.; Innerhofer, K.; Rudisch, A.; Bertram, S. Relationship between Temporomandibular Joint Pain and Magnetic Resonance Imaging Findings of Internal Derangement. Int. J. Oral Maxillofac. Surg. 2001, 30, 118–122. [Google Scholar] [CrossRef]
- Campos, P.S.F.; Macedo Sobrinho, J.B.; Crusoé-Rebello, I.M.R.; Pena, N.; Dantas, J.A.; Mariz, A.C.R.; Oliveira, C. Temporomandibular Joint Disc Adhesion without Mouth-Opening Limitation. J. Oral Maxillofac. Surg. 2008, 66, 551–554. [Google Scholar] [CrossRef][Green Version]
- Koh, K.-J.; List, T.; Petersson, A.; Rohlin, M. Relationship between Clinical and Magnetic Resonance Imaging Diagnoses and Findings in Degenerative and Inflammatory Temporomandibular Joint Diseases: A Systematic Literature Review. J. Orofac. Pain 2009, 23, 123–139. [Google Scholar] [PubMed]
- Lin, W.-C.; Lo, C.-P.; Chiang, I.-C.; Hsu, C.-C.; Hsu, W.-L.; Liu, D.-W.; Juan, Y.-H.; Liu, G.-C. The Use of Pseudo-Dynamic Magnetic Resonance Imaging for Evaluating the Relationship between Temporomandibular Joint Anterior Disc Displacement and Joint Pain. Int. J. Oral Maxillofac. Surg. 2012, 41, 1501–1504. [Google Scholar] [CrossRef]
- Sano, T.; Yamamoto, M.; Okano, T.; Gokan, T.; Westesson, P.-L. Common Abnormalities in Temporomandibular Joint Imaging. Curr. Probl. Diagn. Radiol. 2004, 33, 16–24. [Google Scholar] [CrossRef]
- Haley, D.P.; Schiffman, E.L.; Lindgren, B.R.; Anderson, Q.; Andreasen, K. The Relationship between Clinical and MRI Findings in Patients with Unilateral Temporomandibular Joint Pain. J. Am. Dent. Assoc. 2001, 132, 476–481. [Google Scholar] [CrossRef] [PubMed]
- Lopes, S.L.P.C.; Costa, A.L.F.; Cruz, A.D.; Li, L.M.; de Almeida, S.M. Clinical and MRI Investigation of Temporomandibular Joint in Major Depressed Patients. Dentomaxillofac. Radiol. 2012, 41, 316–322. [Google Scholar] [CrossRef] [PubMed]
- Vieira-Queiroz, I.; Gomes Torres, M.G.; de Oliveira-Santos, C.; Flores Campos, P.S.; Crusoé-Rebello, I.M. Biometric Parameters of the Temporomandibular Joint and Association with Disc Displacement and Pain: A Magnetic Resonance Imaging Study. Int. J. Oral Maxillofac. Surg. 2013, 42, 765–770. [Google Scholar] [CrossRef]
- Arayasantiparb, R.; Mitrirattanakul, S.; Kunasarapun, P.; Chutimataewin, H.; Netnoparat, P.; Sae-Heng, W. Association of Radiographic and Clinical Findings in Patients with Temporomandibular Joints Osseous Alteration. Clin. Oral Investig. 2020, 24, 221–227. [Google Scholar] [CrossRef]
- Palconet, G.; Ludlow, J.B.; Tyndall, D.A.; Lim, P.F. Correlating Cone Beam CT Results with Temporomandibular Joint Pain of Osteoarthritic Origin. Dentomaxillofac. Radiol. 2012, 41, 126–130. [Google Scholar] [CrossRef]
- Brooks, S.L.; Brand, J.W.; Gibbs, S.J.; Hollender, L.; Lurie, A.G.; Omnell, K.A.; Westesson, P.L.; White, S.C. Imaging of the Temporomandibular Joint: A Position Paper of the American Academy of Oral and Maxillofacial Radiology. Oral Surg. Oral Med. Oral Pathol. Oral Radiol. Endod. 1997, 83, 609–618. [Google Scholar] [CrossRef]
- Ohlmann, B.; Rammelsberg, P.; Henschel, V.; Kress, B.; Gabbert, O.; Schmitter, M. Prediction of TMJ Arthralgia According to Clinical Diagnosis and MRI Findings. Int. J. Prosthodont. 2006, 19, 333–338. [Google Scholar]
- Ronga, M.; Angeretti, G.; Ferraro, S.; de Falco, G.; Genovese, E.A.; Cherubino, P. Imaging of Articular Cartilage: Current Concepts. Joints 2014, 2, 137–140. [Google Scholar] [CrossRef] [PubMed]
- Dawson, P.E.; Cranham, J.C. The Complete Dentist Manual: The Essential Guide to Being a Complete Care Dentist, 1st ed.; Dawson Academy: St. Petersburg, FL, USA, 2017. [Google Scholar]
- McKee, J. TMJ Issues: Which Joint Classification System Should I Use? Spear Education. Available online: https://www.speareducation.com/2021/05/which-joint-classification-system-should-i-use (accessed on 3 October 2021).
- Piper, M. Temporomandibular joint imaging. In Handbook of Research on Clinical Applications of Computerized Occlusal Analysis in Dental Medicine; IGI Global: Hershey, PA, USA, 2020; pp. 582–697. ISBN 978-1-5225-9254-9. [Google Scholar]
- Limchaichana, N.; Nilsson, H.; Ekberg, E.C.; Nilner, M.; Petersson, A. Clinical Diagnoses and MRI Findings in Patients with TMD Pain. J. Oral Rehabil. 2007, 34, 237–245. [Google Scholar] [CrossRef] [PubMed]
- Larheim, T.A.; Hol, C.; Ottersen, M.K.; Mork-Knutsen, B.B.; Arvidsson, L.Z. The Role of Imaging in the Diagnosis of Temporomandibular Joint Pathology. Oral Maxillofac. Surg. Clin. N. Am. 2018, 30, 239–249. [Google Scholar] [CrossRef]
- Türp, J.C.; Schlenker, A.; Schröder, J.; Essig, M.; Schmitter, M. Disk Displacement, Eccentric Condylar Position, Osteoarthrosis—Misnomers for Variations of Normality? Results and Interpretations from an MRI Study in Two Age Cohorts. BMC Oral Health 2016, 16, 124. [Google Scholar] [CrossRef]
- Behzadi, F.; Mandell, J.C.; Smith, S.E.; Guenette, J.P. Temporomandibular Joint Imaging: Current Clinical Applications, Biochemical Comparison with the Intervertebral Disc and Knee Meniscus, and Opportunities for Advancement. Skelet. Radiol. 2020, 49, 1183–1193. [Google Scholar] [CrossRef]
- Dworkin, S.F.; LeResche, L. Research Diagnostic Criteria for Temporomandibular Disorders: Review, Criteria, Examinations and Specifications, Critique. J. Craniomandib. Disord. 1992, 6, 301–355. [Google Scholar]
- Serdar, C.C.; Cihan, M.; Yücel, D.; Serdar, M.A. Sample Size, Power and Effect Size Revisited: Simplified and Practical Approaches in Pre-Clinical, Clinical and Laboratory Studies. Biochem. Med. 2021, 31, 010502. [Google Scholar] [CrossRef]
- Manoliu, A.; Spinner, G.; Wyss, M.; Erni, S.; Ettlin, D.A.; Nanz, D.; Ulbrich, E.J.; Gallo, L.M.; Andreisek, G. Quantitative and Qualitative Comparison of MR Imaging of the Temporomandibular Joint at 1.5 and 3.0 T Using an Optimized High-Resolution Protocol. Dentomaxillofac. Radiol. 2016, 45, 20150240. [Google Scholar] [CrossRef]
- Stehling, C.; Vieth, V.; Bachmann, R.; Nassenstein, I.; Kugel, H.; Kooijman, H.; Heindel, W.; Fischbach, R. High-Resolution Magnetic Resonance Imaging of the Temporomandibular Joint: Image Quality at 1.5 and 3.0 Tesla in Volunteers. Investig. Radiol. 2007, 42, 428–434. [Google Scholar] [CrossRef]
- Schmid-Schwap, M.; Drahanowsky, W.; Bristela, M.; Kundi, M.; Piehslinger, E.; Robinson, S. Diagnosis of Temporomandibular Dysfunction Syndrome—Image Quality at 1.5 and 3.0 Tesla Magnetic Resonance Imaging. Eur. Radiol. 2009, 19, 1239–1245. [Google Scholar] [CrossRef] [PubMed]
- Eberhard, L.; Giannakopoulos, N.N.; Rohde, S.; Schmitter, M. Temporomandibular Joint (TMJ) Disc Position in Patients with TMJ Pain Assessed by Coronal MRI. Dentomaxillofac. Radiol. 2013, 42, 20120199. [Google Scholar] [CrossRef]
- Litko-Rola, M.; Szkutnik, J.; Różyło-Kalinowska, I. The Importance of Multisection Sagittal and Coronal Magnetic Resonance Imaging Evaluation in the Assessment of Temporomandibular Joint Disc Position. Clin. Oral Investig. 2021, 25, 159–168. [Google Scholar] [CrossRef]
- Manoliu, A.; Spinner, G.; Wyss, M.; Ettlin, D.A.; Nanz, D.; Kuhn, F.P.; Gallo, L.M.; Andreisek, G. Magnetic Resonance Imaging of the Temporomandibular Joint at 7.0 T Using High-Permittivity Dielectric Pads: A Feasibility Study. Investig. Radiol. 2015, 50, 843–849. [Google Scholar] [CrossRef]
- Kuhn, F.P.; Spinner, G.; del Grande, F.; Wyss, M.; Piccirelli, M.; Erni, S.; Pfister, P.; Ho, M.; Sah, B.-R.; Filli, L.; et al. MR Imaging of the Temporomandibular Joint: Comparison between Acquisitions at 7.0 T Using Dielectric Pads and 3.0 T. Dentomaxillofac. Radiol. 2017, 46, 20160280. [Google Scholar] [CrossRef]
- Nordmeyer-Massner, J.A.; Wyss, M.; Andreisek, G.; Pruessmann, K.P.; Hodler, J. In Vitro and in Vivo Comparison of Wrist MR Imaging at 3.0 and 7.0 Tesla Using a Gradient Echo Sequence and Identical Eight-Channel Coil Array Designs. J. Magn. Reson. Imaging 2011, 33, 661–667. [Google Scholar] [CrossRef] [PubMed]
- Dzingutė, A.; Pileičikienė, G.; Baltrušaitytė, A.; Skirbutis, G. Evaluation of the Relationship between the Occlusion Parameters and Symptoms of the Temporomandibular Joint Disorder. Acta Med. Litu. 2017, 24, 167–175. [Google Scholar] [CrossRef]
- Østensjø, V.; Moen, K.; Storesund, T.; Rosén, A. Prevalence of Painful Temporomandibular Disorders and Correlation to Lifestyle Factors among Adolescents in Norway. Pain Res. Manag. 2017, 2017, 2164825. [Google Scholar] [CrossRef]
- Correia, L.M.F.; Guimarães, A.S.; Teixeira, M.L.; Rodrigues, L.L.; Correia, L.M.F.; Guimarães, A.S.; Teixeira, M.L.; Rodrigues, L.L. Evaluation of Body Painful Areas in Patients with Muscular Temporomandibular Disorder: A Retrospective Study. Rev. Dor. 2015, 16, 249–253. [Google Scholar] [CrossRef]
- Marasa, F.K.; Ham, B.D. Case Reports Involving the Treatment of Children with Chronic Otitis Media with Effusion via Craniomandibular Methods. Cranio 1988, 6, 256–270. [Google Scholar] [CrossRef]
- Kitsoulis, P.; Marini, A.; Iliou, K.; Galani, V.; Zimpis, A.; Kanavaros, P.; Paraskevas, G. Signs and Symptoms of Temporomandibular Joint Disorders Related to the Degree of Mouth Opening and Hearing Loss. BMC Ear Nose Throat Disord. 2011, 11, 5. [Google Scholar] [CrossRef] [PubMed]
- Kaygusuz, I.; Karlidağ, T.; Keleş, E.; Yalçin, S.; Yildiz, M.; Alpay, H.C. Ear symptoms accompanying temporomandibular joint diseases. KBB J. Ear Nose Throat Disord. 2006, 16, 205–208. [Google Scholar]
- Kusdra, P.M.; Stechman-Neto, J.; de Leão, B.L.C.; Martins, P.F.A.; de Lacerda, A.B.M.; Zeigelboim, B.S. Relationship between Otological Symptoms and TMD. Int. Tinnitus J. 2018, 22, 30–34. [Google Scholar] [CrossRef]
- Peck, C.C.; Goulet, J.-P.; Lobbezoo, F.; Schiffman, E.L.; Alstergren, P.; Anderson, G.C.; de Leeuw, R.; Jensen, R.; Michelotti, A.; Ohrbach, R.; et al. Expanding the Taxonomy of the Diagnostic Criteria for Temporomandibular Disorders. J. Oral Rehabil. 2014, 41, 2–23. [Google Scholar] [CrossRef]
- Derwich, M.; Mitus-Kenig, M.; Pawlowska, E. Interdisciplinary Approach to the Temporomandibular Joint Osteoarthritis-Review of the Literature. Medicina 2020, 56, 225. [Google Scholar] [CrossRef] [PubMed]
- Cairns, B.E. Pathophysiology of TMD Pain—Basic Mechanisms and Their Implications for Pharmacotherapy. J. Oral Rehabil. 2010, 37, 391–410. [Google Scholar] [CrossRef] [PubMed]
- Eriksen, E.S.; Hellem, S.; Skartveit, L.; Brun, J.G.; Bøe, O.E.; Moen, K.; Geitung, J.T. Temporomandibular Joint Pain and Associated Magnetic Resonance Findings: A Retrospective Study with a Control Group. Acta Radiol. Open 2020, 9, 2058460120938738. [Google Scholar] [CrossRef]
- Chantaracherd, P.; John, M.T.; Hodges, J.S.; Schiffman, E.L. Temporomandibular Joint Disorders’ Impact on Pain, Function, and Disability. J. Dent. Res. 2015, 94, 79S–86S. [Google Scholar] [CrossRef]
- Güler, N.; Uçkan, S.; Imirzalioğlu, P.; Açikgözoğlu, S. Temporomandibular Joint Internal Derangement: Relationship between Joint Pain and MR Grading of Effusion and Total Protein Concentration in the Joint Fluid. Dentomaxillofac. Radiol. 2005, 34, 175–181. [Google Scholar] [CrossRef]
- Giudice, A.L.; Brewer, I.; Leonardi, R.; Roberts, N.; Bagnato, G. Pain Threshold and Temporomandibular Function in Systemic Sclerosis: Comparison with Psoriatic Arthritis. Clin. Rheumatol. 2018, 37, 1861–1867. [Google Scholar] [CrossRef]
- Jeon, K.J.; Lee, C.; Choi, Y.J.; Han, S.-S. Analysis of Three-Dimensional Imaging Findings and Clinical Symptoms in Patients with Temporomandibular Joint Disorders. Quant. Imaging Med. Surg. 2021, 11, 1921–1931. [Google Scholar] [CrossRef]
- Edwards, R.; Alsufyani, N.; Heo, G.; Flores-Mir, C. The Frequency and Nature of Incidental Findings in Large-Field Cone Beam Computed Tomography Scans of an Orthodontic Sample. Prog. Orthod. 2014, 15, 37. [Google Scholar] [CrossRef]
- Rohlin, M.; Westesson, P.L.; Eriksson, L. The Correlation of Temporomandibular Joint Sounds with Joint Morphology in Fifty-Five Autopsy Specimens. J. Oral Maxillofac. Surg. 1985, 43, 194–200. [Google Scholar] [CrossRef]
- Honda, K.; Natsumi, Y.; Urade, M. Correlation between MRI Evidence of Degenerative Condylar Surface Changes, Induction of Articular Disc Displacement and Pathological Joint Sounds in the Temporomandibular Joint. Gerodontology 2008, 25, 251–257. [Google Scholar] [CrossRef]
- Güler, N.; Yatmaz, P.I.; Ataoglu, H.; Emlik, D.; Uckan, S. Temporomandibular Internal Derangement: Correlation of MRI Findings with Clinical Symptoms of Pain and Joint Sounds in Patients with Bruxing Behaviour. Dentomaxillofac. Radiol. 2003, 32, 304–310. [Google Scholar] [CrossRef] [PubMed]
- Spruijt, R.J.; Wabeke, K.B. Psychological Factors Related to the Prevalence of Temporomandibular Joint Sounds. J. Oral Rehabil. 1995, 22, 803–808. [Google Scholar] [CrossRef] [PubMed]
- Suenaga, S.; Nagayama, K.; Nagasawa, T.; Indo, H.; Majima, H.J. The Usefulness of Diagnostic Imaging for the Assessment of Pain Symptoms in Temporomandibular Disorders. Jpn. Dent. Sci. Rev. 2016, 52, 93–106. [Google Scholar] [CrossRef] [PubMed]
- Paesani, D.; Salas, E.; Martinez, A.; Isberg, A. Prevalence of Temporomandibular Joint Disk Displacement in Infants and Young Children. Oral Surg. Oral Med. Oral Pathol. Oral Radiol. Endod. 1999, 87, 15–19. [Google Scholar] [CrossRef]
- Vogl, T.J.; Lauer, H.-C.; Lehnert, T.; Naguib, N.N.N.; Ottl, P.; Filmann, N.; Soekamto, H.; Nour-Eldin, N.-E.A. The Value of MRI in Patients with Temporomandibular Joint Dysfunction: Correlation of MRI and Clinical Findings. Eur. J. Radiol. 2016, 85, 714–719. [Google Scholar] [CrossRef]
- Su, N.; Poon, R.; Friedman, L.; Darling, M.; Grushka, M. TMJ Changes in Adolescent TMD Patients Seen on MRI in Clinical Setting. N. Y. State Dent. J. 2015, 81, 27–30. [Google Scholar] [PubMed]
- Whyte, A.M.; McNamara, D.; Rosenberg, I.; Whyte, A.W. Magnetic Resonance Imaging in the Evaluation of Temporomandibular Joint Disc Displacement—A Review of 144 Cases. Int. J. Oral Maxillofac. Surg. 2006, 35, 696–703. [Google Scholar] [CrossRef]
- Posthumus, M.; September, A.V.; Keegan, M.; O’Cuinneagain, D.; van der Merwe, W.; Schwellnus, M.P.; Collins, M. Genetic Risk Factors for Anterior Cruciate Ligament Ruptures: COL1A1 Gene Variant. Br. J. Sports Med. 2009, 43, 352–356. [Google Scholar] [CrossRef] [PubMed]
- Collins, M.; Posthumus, M.; Schwellnus, M.P. The COL1A1 Gene and Acute Soft Tissue Ruptures. Br. J. Sports Med. 2010, 44, 1063–1064. [Google Scholar] [CrossRef] [PubMed]
- Hocking, L.J.; Smith, B.H.; Jones, G.T.; Reid, D.M.; Strachan, D.P.; Macfarlane, G.J. Genetic Variation in the Beta2-Adrenergic Receptor but Not Catecholamine-O-Methyltransferase Predisposes to Chronic Pain: Results from the 1958 British Birth Cohort Study. Pain 2010, 149, 143–151. [Google Scholar] [CrossRef] [PubMed]
- Abdelnabi, M.H.; Swelem, A.A. Influence of Defective Complete Dentures Renewal on TMD; an MRI and Clinical Controlled Prospective Study. Gerodontology 2015, 32, 211–221. [Google Scholar] [CrossRef]
- Manfredini, D.; Perinetti, G.; Stellini, E.; di Leonardo, B.; Guarda-Nardini, L. Prevalence of Static and Dynamic Dental Malocclusion Features in Subgroups of Temporomandibular Disorder Patients: Implications for the Epidemiology of the TMD-Occlusion Association. Quintessence Int. 2015, 46, 341–349. [Google Scholar] [CrossRef] [PubMed]
- Gesch, D.; Bernhardt, O.; Kirbschus, A. Association of Malocclusion and Functional Occlusion with Temporomandibular Disorders (TMD) in Adults: A Systematic Review of Population-Based Studies. Quintessence Int. 2004, 35, 211–221. [Google Scholar]
- Wilkes, C.H. Internal Derangements of the Temporomandibular Joint. Pathological Variations. Arch. Otolaryngol. Head Neck Surg. 1989, 115, 469–477. [Google Scholar] [CrossRef]
- Goodlin, G.T.; Roos, T.R.; Roos, A.K.; Kim, S.K. The Dawning Age of Genetic Testing for Sports Injuries. Clin. J. Sport Med. 2015, 25, 1–5. [Google Scholar] [CrossRef] [PubMed]
- Gauer, R.L.; Semidey, M.J. Diagnosis and Treatment of Temporomandibular Disorders. Am. Fam. Physician 2015, 91, 378–386. [Google Scholar]
- Türp, J.C.; Schindler, H. The Dental Occlusion as a Suspected Cause for TMDs: Epidemiological and Etiological Considerations. J. Oral Rehabil. 2012, 39, 502–512. [Google Scholar] [CrossRef] [PubMed]
- Li, D.T.S.; Leung, Y.Y. Temporomandibular Disorders: Current Concepts and Controversies in Diagnosis and Management. Diagnostics 2021, 11, 459. [Google Scholar] [CrossRef]
- Stone, J.C.; Hannah, A.; Nagar, N. Dental Occlusion and Temporomandibular Disorders. Evid. Based Dent. 2017, 18, 86–87. [Google Scholar] [CrossRef] [PubMed]
- De Kanter, R.J.A.M.; Battistuzzi, P.G.F.C.M.; Truin, G.-J. Temporomandibular Disorders: “Occlusion” Matters! Pain Res. Manag. 2018, 2018, 8746858. [Google Scholar] [CrossRef] [PubMed]
- Stohler, C. Management of dental occlusion. In TMDs an Evidence-Based Approach to Diagnosis and Treatment; Quintessence: Chicago, IL, USA, 2006; pp. 403–411. ISBN 0-86715-447-0. [Google Scholar]
- Al-Ani, Z.; Davies, S.; Sloan, P.; Gray, R. Change in the Number of Occlusal Contacts Following Splint Therapy in Patients with a Temporomandibular Disorder (TMD). Eur. J. Prosthodont. Restor. Dent. 2008, 16, 98–103. [Google Scholar]
- Obrez, A.; Stohler, C.S. Jaw Muscle Pain and Its Effect on Gothic Arch Tracings. J. Prosthet. Dent. 1996, 75, 393–398. [Google Scholar] [CrossRef]
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2021 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Tegnander, T.; Chladek, G.; Hovland, A.; Żmudzki, J.; Wojtek, P. Relationship between Clinical Symptoms and Magnetic Resonance Imaging in Temporomandibular Disorder (TMD) Patients Utilizing the Piper MRI Diagnostic System. J. Clin. Med. 2021, 10, 4698. https://doi.org/10.3390/jcm10204698
Tegnander T, Chladek G, Hovland A, Żmudzki J, Wojtek P. Relationship between Clinical Symptoms and Magnetic Resonance Imaging in Temporomandibular Disorder (TMD) Patients Utilizing the Piper MRI Diagnostic System. Journal of Clinical Medicine. 2021; 10(20):4698. https://doi.org/10.3390/jcm10204698
Chicago/Turabian StyleTegnander, Tor, Grzegorz Chladek, Anders Hovland, Jarosław Żmudzki, and Piotr Wojtek. 2021. "Relationship between Clinical Symptoms and Magnetic Resonance Imaging in Temporomandibular Disorder (TMD) Patients Utilizing the Piper MRI Diagnostic System" Journal of Clinical Medicine 10, no. 20: 4698. https://doi.org/10.3390/jcm10204698
APA StyleTegnander, T., Chladek, G., Hovland, A., Żmudzki, J., & Wojtek, P. (2021). Relationship between Clinical Symptoms and Magnetic Resonance Imaging in Temporomandibular Disorder (TMD) Patients Utilizing the Piper MRI Diagnostic System. Journal of Clinical Medicine, 10(20), 4698. https://doi.org/10.3390/jcm10204698







