Risk Factors for Recurrence of Benign Paroxysmal Positional Vertigo. A Clinical Review
Abstract
:1. Introduction
2. Materials and Methods
2.1. Literature Search
2.2. Eligibility and Exclusion Criteria for Study Selection
- Retrospective or prospective studies on the recurrence of BPPV.
- BPPV diagnosis according to clinical practice guideline [9]
- Assessment of the demographics (sex, age) of recurrent BPPV patients and the potential risk factors of BPPV recurrence.
- Articles published in English.
- Systematic reviews, case reports, book chapters.
- Experimental studies.
- Studies not based on outcomes of canalith repositioning procedure (CRP).
- Studies with insufficient data for analysis.
- Diagnosis, treatment, or definition of recurrence of BPPV was not clear.
- Follow-up time less than 6 months or unstated.
2.3. Data Extraction
3. Results
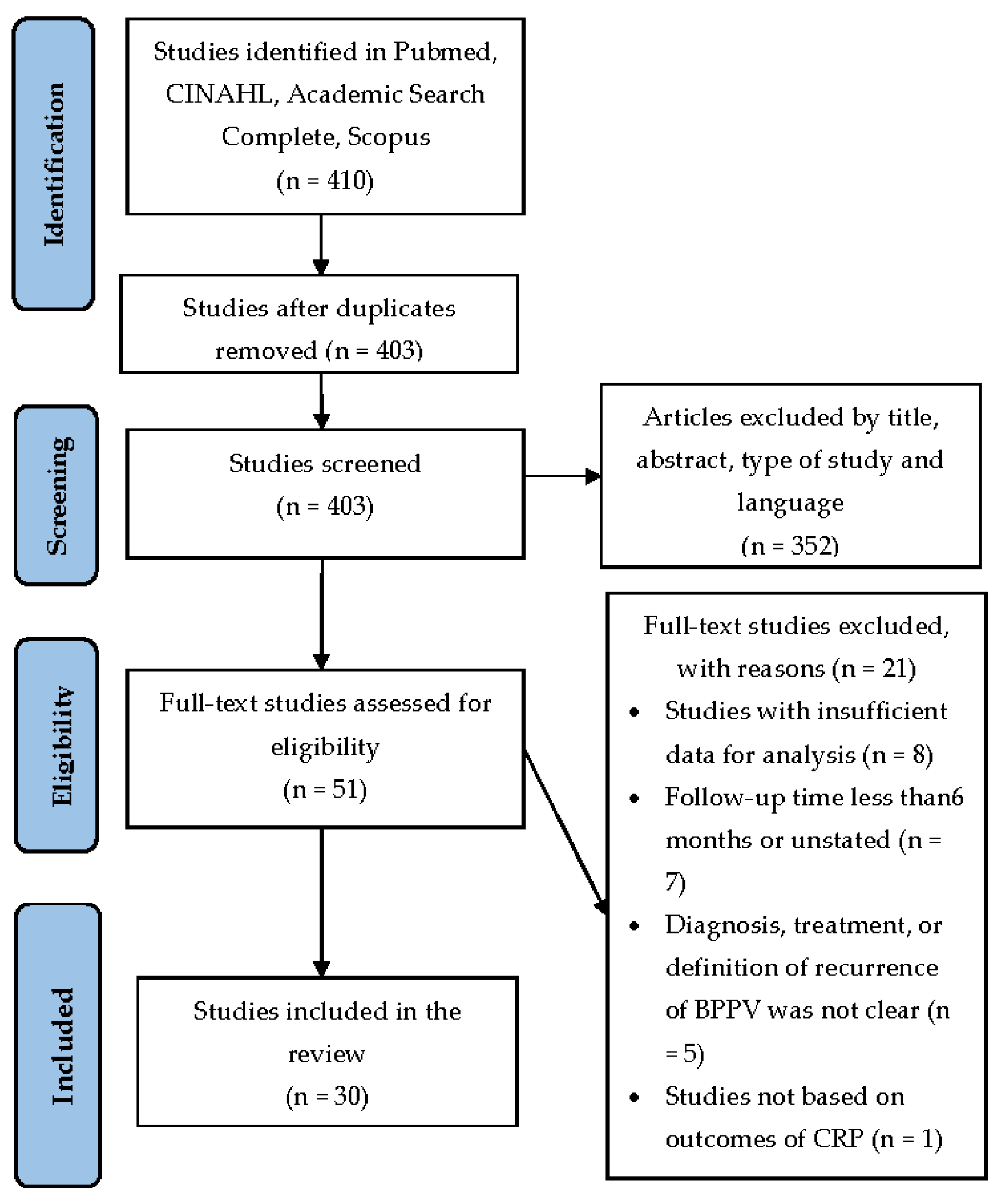
3.1. Study Selection
3.2. Findings
4. Discussion
4.1. Age
4.2. Gender
4.3. Meniere’s Disease
4.4. Trauma
4.5. Osteoporosis
4.6. Vitamin D
4.7. Diabetes Mellitus/Hyperinsulinism/Hyperglycemia
4.8. Vascular Comorbidities (Hypertension, Hyperlipidemia, Cardiovascular Disease)
4.9. Migraine
4.10. Bilateral/Multicanal BPPV
4.11. Cervical Osteoarthritis (Spondylosis)
4.12. Sleep Disorders
5. Limitations
6. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Conflicts of Interest
References
- De Stefano, A.; Dispenza, F.; Suarez, H.; Perez-Fernandez, N.; Manrique-Huarte, R.; Ban, J.H.; Kim, M.B.; Strupp, M.; Feil, K.; Oliveira, C.A.; et al. A Multicenter Observational Study on the Role of Comorbidities in the Recurrent Episodes of Benign Paroxysmal Positional Vertigo. Auris Nasus Larynx 2014, 41, 31–36. [Google Scholar] [CrossRef] [PubMed]
- Sreenivas, V.; Sima, N.H.; Philip, S. The Role of Comorbidities in Benign Paroxysmal Positional Vertigo. Ear Nose Throat J. 2021, 100, NP225–NP230. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Su, P.; Liu, Y.C.; Lin, H.C. Risk Factors for the Recurrence of Post-Semicircular Canal Benign Paroxysmal Positional Vertigo after Canalith Repositioning. J. Neurol. 2016, 263, 45–51. [Google Scholar] [CrossRef]
- Picciotti, P.M.; Lucidi, D.; De Corso, E.; Meucci, D.; Sergi, B.; Paludetti, G. Comorbidities and Recurrence of Benign Paroxysmal Positional Vertigo: Personal Experience. Int. J. Audiol. 2016, 55, 279–284. [Google Scholar] [CrossRef] [PubMed]
- Pérez, P.; Franco, V.; Cuesta, P.; Aldama, P.; Alvarez, M.J.; Méndez, J.C. Recurrence of Benign Paroxysmal Positional Vertigo. Otol. Neurotol. 2012, 33, 437–443. [Google Scholar] [CrossRef] [Green Version]
- Brandt, T.; Huppert, D.; Hecht, J.; Karch, C.; Strupp, M. Benign Paroxysmal Positioning Vertigo: A Long-Term Follow-up (6–17 Years) of 125 Patients. Acta Otolaryngol. 2006, 126, 160–163. [Google Scholar] [CrossRef] [PubMed]
- Kansu, L.; Avci, S.; Yilmaz, I.; Ozluoglu, L.N. Long-Term Follow-up of Patients with Posterior Canal Benign Paroxysmal Positional Vertigo. Acta Otolaryngol. 2010, 130, 1009–1012. [Google Scholar] [CrossRef] [PubMed]
- Kim, S.Y.; Han, S.H.; Kim, Y.H.; Park, M.H. Clinical Features of Recurrence and Osteoporotic Changes in Benign Paroxysmal Positional Vertigo. Auris Nasus Larynx 2017, 44, 156–161. [Google Scholar] [CrossRef] [PubMed]
- Bhattacharyya, N.; Gubbels, S.P.; Schwartz, S.R.; Edlow, J.A.; El-Kashlan, H.; Fife, T.; Holmberg, J.M.; Mahoney, K.; Hollingsworth, D.B.; Roberts, R.; et al. Clinical Practice Guideline: Benign Paroxysmal Positional Vertigo (Update). Otolaryngol.—Head Neck Surg. 2017, 156, S1–S47. [Google Scholar] [CrossRef] [PubMed]
- Del Rio, M.; Arriaga, M.A. Benign Positional Vertigo: Prognostic Factors. Otolaryngol.—Head Neck Surg. 2004, 130, 426–429. [Google Scholar] [CrossRef]
- Korres, S.; Balatsouras, D.G.; Ferekidis, E. Prognosis of Patients with Benign Paroxysmal Positional Vertigo Treated with Repositioning Manoeuvres. J. Laryngol. Otol. 2006, 120, 528–533. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Choi, S.J.; Lee, J.B.; Lim, H.J.; Park, H.Y.; Park, K.; In, S.M.; Oh, J.H.; Choung, Y.H. Clinical Features of Recurrent or Persistent Benign Paroxysmal Positional Vertigo. Otolaryngol.—Head Neck Surg. 2012, 147, 919–924. [Google Scholar] [CrossRef] [PubMed]
- Yamanaka, T.; Shirota, S.; Sawai, Y.; Murai, T.; Fujita, N.; Hosoi, H. Osteoporosis as a Risk Factor for the Recurrence of Benign Paroxysmal Positional Vertigo. Laryngoscope 2013, 123, 2813–2816. [Google Scholar] [CrossRef]
- Webster, G.; Sens, P.M.; Salmito, M.C.; Cavalcante, J.D.R.; dos Santos, P.R.B.; da Silva, A.L.M.; de Souza, É.C.F. Hyperinsulinemia and Hyperglycemia: Risk Factors for Recurrence of Benign Paroxysmal Positional Vertigo. Braz. J. Otorhinolaryngol. 2015, 81, 347–351. [Google Scholar] [CrossRef] [Green Version]
- Babac, S.; Djeric, D.; Petrovic-Lazic, M.; Arsovic, N.; Mikic, A. Why Do Treatment Failure and Recurrences of Benign Paroxysmal Positional Vertigo Occur? Otol. Neurotol. 2014, 35, 1105–1110. [Google Scholar] [CrossRef]
- Luryi, A.L.; Lawrence, J.; Bojrab, D.I.; LaRouere, M.; Babu, S.; Zappia, J.; Sargent, E.W.; Chan, E.; Naumann, I.; Hong, R.S.; et al. Recurrence in Benign Paroxysmal Positional Vertigo: A Large, Single-Institution Study. Otol. Neurotol. 2018, 39, 622–627. [Google Scholar] [CrossRef]
- Nunez, R.A.; Cass, S.P.; Furman, J.M. Short- and Long-Term Outcomes of Canalith Repositioning for Benign Paroxysmal Positional Vertigo. Otolaryngol. Neck Surg. 2000, 122, 647–653. [Google Scholar] [CrossRef]
- Zhu, C.T.; Zhao, X.Q.; Ju, Y.; Wang, Y.; Chen, M.M.; Cui, Y. Clinical Characteristics and Risk Factors for the Recurrence of Benign Paroxysmal Positional Vertigo. Front. Neurol. 2019, 10, 1190. [Google Scholar] [CrossRef]
- Messina, A.; Casani, A.P.; Manfrin, M.; Guidetti, G. Survey Italiana Sulla Vertigine Parossistica Posizionale. Acta Otorhinolaryngol. Ital. 2017, 37, 328–335. [Google Scholar] [CrossRef] [PubMed]
- Rhim, G. Il Serum Vitamin D and Recurrent Benign Paroxysmal Positional Vertigo. Laryngoscope Investig. Otolaryngol. 2016, 1, 150–153. [Google Scholar] [CrossRef] [PubMed]
- Balatsouras, D.G.; Ganelis, P.; Aspris, A.; Economou, N.C.; Moukos, A.; Koukoutsis, G. Benign Paroxysmal Positional Vertigo Associated with Meniere’s Disease: Epidemiological, Pathophysiologic, Clinical, and Therapeutic Aspects. Ann. Otol. Rhinol. Laryngol. 2012, 121, 682–688. [Google Scholar] [CrossRef]
- Talaat, H.S.; Abuhadied, G.; Talaat, A.S.; Abdelaal, M.S.S. Low Bone Mineral Density and Vitamin D Deficiency in Patients with Benign Positional Paroxysmal Vertigo. Eur. Arch. Oto-Rhino-Laryngol. 2015, 272, 2249–2253. [Google Scholar] [CrossRef]
- Yang, C.J.; Kim, Y.; Lee, H.S.; Park, H.J. Bone Mineral Density and Serum 25-Hydroxyvitamin D in Patients with Idiopathic Benign Paroxysmal Positional Vertigo. J. Vestib. Res. Equilib. Orientat. 2018, 27, 287–294. [Google Scholar] [CrossRef] [Green Version]
- Wei, W.; Sayyid, Z.N.; Ma, X.; Wang, T.; Dong, Y. Presence of Anxiety and Depression Symptoms Affects the First Time Treatment Efficacy and Recurrence of Benign Paroxysmal Positional Vertigo. Front. Neurol. 2018, 9, 178. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Faralli, M.; Ricci, G.; Molini, E.; Bressi, T.; Simoncelli, C.; Frenguelli, A.; Division, C.S. Paroxysmal Positional Vertigo: The Role of Age. Acta Otorhinolaryngol. Ital. 2006, 26, 25–31. [Google Scholar]
- Tan, J.; Deng, Y.; Zhang, T.; Wang, M. Clinical Characteristics and Treatment Outcomes for Benign Paroxysmal Positional Vertigo Comorbid with Hypertension. Acta Otolaryngol. 2017, 137, 482–484. [Google Scholar] [CrossRef]
- Prokopakis, E.; Vlastos, I.M.; Tsagournisakis, M.; Christodoulou, P.; Kawauchi, H.; Velegrakis, G. Canalith Repositioning Procedures among 965 Patients with Benign Paroxysmal Positional Vertigo. Audiol. Neurotol. 2013, 18, 83–88. [Google Scholar] [CrossRef] [PubMed]
- Rashad, U.M. Long-Term Follow up after Epley’s Manoeuvre in Patients with Benign Paroxysmal Positional Vertigo. J. Laryngol. Otol. 2009, 123, 69–74. [Google Scholar] [CrossRef] [PubMed]
- Hilton, D.B.; Luryi, A.L.; Bojrab, D.I.; Babu, S.C.; Hong, R.S.; Santiago Rivera, O.J.; Schutt, C.A. Comparison of Associated Comorbid Conditions in Patients with Benign Paroxysmal Positional Vertigo with or without Migraine History: A Large Single Institution Study. Am. J. Otolaryngol.—Head Neck Med. Surg. 2020, 41, 102650. [Google Scholar] [CrossRef]
- Ishiyama, A.; Jacobson, K.M.; Baloh, R.W. Migraine and Benign Positional Vertigo. Ann. Otol. Rhinol. Laryngol. 2000, 109, 377–380. [Google Scholar] [CrossRef] [PubMed]
- Gordon, C.R.; Levite, R.; Joffe, V.; Gadoth, N. Is Posttraumatic Benign Paroxysmal Positional Vertigo Different from the Idiopathic Form? Arch. Neurol. 2004, 61, 1590–1593. [Google Scholar] [CrossRef] [Green Version]
- Agrawal, Y.; Carey, J.P.; Della Santina, C.C.; Schubert, M.C.; Minor, L.B. Disorders of Balance and Vestibular Function in US Adults: Data from the National Health and Nutrition Examination Survey, 2001–2004. Arch. Intern. Med. 2009, 169, 938–944. [Google Scholar] [CrossRef] [PubMed]
- Li, S.; Wang, Z.; Liu, Y.; Cao, J.; Zheng, H.; Jing, Y.; Han, L.; Ma, X.; Xia, R.; Yu, L. Risk Factors for the Recurrence of Benign Paroxysmal Positional Vertigo: A Systematic Review and Meta-Analysis. Ear Nose Throat J. 2020, 0145561320943362. [Google Scholar] [CrossRef] [PubMed]
- Vibert, D.; Kompis, M.; Häusler, R. Benign Paroxysmal Positional Vertigo in Older Women May Be Related to Osteoporosis and Osteopenia. Ann. Otol. Rhinol. Laryngol. 2003, 112, 885–889. [Google Scholar] [CrossRef] [PubMed]
- Kutlubaev, M.A.; Xu, Y.; Hornibrook, J. Benign Paroxysmal Positional Vertigo in Meniere’s Disease: Systematic Review and Meta-Analysis of Frequency and Clinical Characteristics. J. Neurol. 2021, 268, 1608–1614. [Google Scholar] [CrossRef] [PubMed]
- Chen, J.; Zhang, S.; Cui, K.; Liu, C. Risk Factors for Benign Paroxysmal Positional Vertigo Recurrence: A Systematic Review and Meta-Analysis. J. Neurol. 2020, 1–11. [Google Scholar] [CrossRef]
- Lundberg, Y.W.; Zhao, X.; Yamoah, E.N. Assembly of the Otoconia Complex to the Macular Sensory Epithelium of the Vestibule. Brain Res. 2006, 1091, 47–57. [Google Scholar] [CrossRef]
- Ross, M.D. Calcium Ion Uptake and Exchange in Otoconia. Adv. Otorhinolaryngol. 1979, 25, 26–33. [Google Scholar]
- Preston, R.E.; Johnsson, L.G.; Hill, J.H.; Schacht, J. Incorporation of Radioactive Calcium into Otolithic Membranes and Middle Ear Ossicles of the Gerbil. Acta Otolaryngol. 1975, 80, 269–275. [Google Scholar] [CrossRef]
- Vibert, D.; Sans, A.; Kompis, M.; Travo, C.; Mühlbauer, R.C.; Tschudi, I.; Boukhaddaoui, H.; Häusler, R. Ultrastructural Changes in Otoconia of Osteoporotic Rats. Audiol. Neurotol. 2008, 13, 293–301. [Google Scholar] [CrossRef]
- Thalmann, R.; Ignatova, E.; Kachar, B.; Ornitz, D.M.; Thalmann, I. Development and Maintenance of Otoconia: Biochemical Considerations. Ann. N. Y. Acad. Sci. 2001, 942, 162–178. [Google Scholar] [CrossRef] [PubMed]
- Yamauchi, D.; Nakaya, K.; Raveendran, N.N.; Harbidge, D.G.; Singh, R.; Wangemann, P.; Marcus, D.C. Expression of Epithelial Calcium Transport System in Rat Cochlea and Vestibular Labyrinth. BMC Physiol. 2010, 10, 1. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Takemura, T.; Sakagami, M.; Nakase, T.; Kubo, T.; Kitamura, Y.; Nomura, S. Localization of Osteopontin in the Otoconial Organs of Adult Rats. Hear. Res. 1994, 79, 99–104. [Google Scholar] [CrossRef]
- Mikulec, A.A.; Kowalczyk, K.A.; Pfitzinger, M.E.; Harris, D.A.; Jackson, L.E. Negative Association between Treated Osteoporosis and Benign Paroxysmal Positional Vertigo in Women. J. Laryngol. Otol. 2010, 124, 374–376. [Google Scholar] [CrossRef]
- Parham, K.; Leonard, G.; Feinn, R.S.; Lafreniere, D.; Kenny, A.M. Prospective Clinical Investigation of the Relationship between Idiopathic Benign Paroxysmal Positional Vertigo and Bone Turnover: A Pilot Study. Laryngoscope 2013, 123, 2834–2839. [Google Scholar] [CrossRef] [PubMed]
- Jeong, S.H.; Kim, J.S.; Shin, J.W.; Kim, S.; Lee, H.; Lee, A.Y.; Kim, J.M.; Jo, H.; Song, J.; Ghim, Y. Decreased Serum Vitamin D in Idiopathic Benign Paroxysmal Positional Vertigo. J. Neurol. 2013, 260, 832–838. [Google Scholar] [CrossRef]
- Yamauchi, D.; Raveendran, N.N.; Pondugula, S.R.; Kampalli, S.B.; Sanneman, J.D.; Harbidge, D.G.; Marcus, D.C. Vitamin D Upregulates Expression of ECaC1 MRNA in Semicircular Canal. Biochem. Biophys. Res. Commun. 2005, 331, 1353–1357. [Google Scholar] [CrossRef] [PubMed]
- Talaat, H.S.; Kabel, A.M.H.; Khaliel, L.H.; Abuhadied, G.; El-Naga, H.A.E.R.A.; Talaat, A.S. Reduction of Recurrence Rate of Benign Paroxysmal Positional Vertigo by Treatment of Severe Vitamin D Deficiency. Auris Nasus Larynx 2016, 43, 237–241. [Google Scholar] [CrossRef]
- Angeli, R.D.; Lavinsky, L.; Dolganov, A. Alterations in Cochlear Function during Induced Acute Hyperinsulinemia in an Animal Model. Braz. J. Otorhinolaryngol. 2009, 75, 760–764. [Google Scholar] [CrossRef] [Green Version]
- Yoda, S.; Cureoglu, S.; Yildirim-Baylan, M.; Morita, N.; Fukushima, H.; Harada, T.; Paparella, M.M. Association between Type 1 Diabetes Mellitus and Deposits in the Semicircular Canals. Otolaryngol.—Head Neck Surg. 2011, 145, 458–462. [Google Scholar] [CrossRef] [PubMed]
- Paula Serra, A.; de Carvalho Lopes, K.; Dorigueto, R.S.; Freitas Ganança, F. Blood Glucose and Insulin Levels in Patients with Peripheral Vestibular Disease. Braz. J. Otorhinolaryngol. 2009, 75, 701–705. [Google Scholar] [CrossRef] [Green Version]
- D’Silva, L.J.; Staecker, H.; Lin, J.; Sykes, K.J.; Phadnis, M.A.; McMahon, T.M.; Connolly, D.; Sabus, C.H.; Whitney, S.L.; Kludinga, P.M. Retrospective Data Suggests That the Higher Prevalence of Benign Paroxysmal Positional Vertigo in Individuals with Type 2 Diabetes Is Mediated by Hypertension. J. Vestib. Res. Equilib. Orientat. 2016, 25, 233–239. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Liu, M.; Pereira, F.A.; Price, S.D.; Chu, M.J.; Shope, C.; Himes, D.; Eatock, R.A.; Brownell, W.E.; Lysakowski, A.; Tsai, M.J. Essential Role of BETA2/NeuroD1 in Development of the Vestibular and Auditory Systems. Genes Dev. 2000, 14, 2839–2854. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Von Brevern, M.; Radtke, A.; Lezius, F.; Feldmann, M.; Ziese, T.; Lempert, T.; Neuhauser, H. Epidemiology of Benign Paroxysmal Positional Vertigo: A Population Based Study. J. Neurol. Neurosurg. Psychiatry 2007, 78, 710–715. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Bruss, D.; Abouzari, M.; Sarna, B.; Goshtasbi, K.; Lee, A.; Birkenbeuel, J.; Djalilian, H.R. Migraine Features in Patients With Recurrent Benign Paroxysmal Positional Vertigo. Otol. Neurotol. 2021, 42, 461–465. [Google Scholar] [CrossRef] [PubMed]
- Vuković, V.; Plavec, D.; Galinović, I.; Lovrenčić-Huzjan, A.; Budišić, M.; Demarin, V. Prevalence of Vertigo, Dizziness, and Migrainous Vertigo in Patients with Migraine. Headache 2007, 47, 1427–1435. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Kuritzky, A.; Ziegler, D.K.; Hassanein, R. Vertigo, Motion Sickness and Migraine. Headache J. Head Face Pain 1981, 21, 227–231. [Google Scholar] [CrossRef]
- Güçlütürk, M.T.; Ünal, Z.N.; Ismi, O.; Çimen, M.B.Y.; Ünal, M. The Role of Oxidative Stress and Inflammatory Mediators in Benign Paroxysmal Positional Vertigo. J. Int. Adv. Otol. 2016, 12, 101–105. [Google Scholar] [CrossRef]
- Neri, M.; Frustaci, A.; Milic, M.; Valdiglesias, V.; Fini, M.; Bonassi, S.; Barbanti, P. A Meta-Analysis of Biomarkers Related to Oxidative Stress and Nitric Oxide Pathway in Migraine. Cephalalgia 2015, 35, 931–937. [Google Scholar] [CrossRef]
- Vass, Z.; Steyger, P.S.; Hordichok, A.J.; Trune, D.R.; Jancsó, G.; Nuttall, A.L. Capsaicin Stimulation of the Cochlea and Electric Stimulation of the Trigeminal Ganglion Mediate Vascular Permeability in Cochlear and Vertebro-Basilar Arteries: A Potential Cause of Inner Ear Dysfunction in Headache. Neuroscience 2001, 103, 189–201. [Google Scholar] [CrossRef]
- Ophoff, R.A.; Terwindt, G.M.; Vergouwe, M.N.; Van Eijk, R.; Oefner, P.J.; Hoffman, S.M.G.; Lamerdin, J.E.; Mohrenweiser, H.W.; Bulman, D.E.; Ferrari, M.; et al. Familial Hemiplegic Migraine and Episodic Ataxia Type-2 Are Caused by Mutations in the Ca2+ Channel Gene CACNL1A4. Cell 1996, 87, 543–552. [Google Scholar] [CrossRef] [Green Version]
- Lempert, T.; von Brevern, M. Vestibular Migraine. Neurol. Clin. 2019, 37, 695–706. [Google Scholar] [CrossRef] [PubMed]
- Argaet, E.C.; Bradshaw, A.P.; Welgampola, M.S. Benign Positional Vertigo, Its Diagnosis, Treatment and Mimics. Clin. Neurophysiol. Pract. 2019, 4, 97–111. [Google Scholar] [CrossRef]
- Kelly, J.C.; Groarke, P.J.; Butler, J.S.; Poynton, A.R.; O’Byrne, J.M. The Natural History and Clinical Syndromes of Degenerative Cervical Spondylosis. Adv. Orthop. 2012, 2012, 393642. [Google Scholar] [CrossRef] [Green Version]
- Bayrak, I.K.; Durmus, D.; Bayrak, A.O.; Diren, B.; Canturk, F. Effect of Cervical Spondylosis on Vertebral Arterial Flow and Its Association with Vertigo. Clin. Rheumatol. 2009, 28, 59–64. [Google Scholar] [CrossRef] [PubMed]
- Li, Y.; Peng, B. Pathogenesis, Diagnosis, and Treatment of Cervical Vertigo. Pain Physician 2015, 18, E583–E595. [Google Scholar]
- Martellucci, S.; Attanasio, G.; Ralli, M.; Marcelli, V.; de Vincentiis, M.; Greco, A.; Gallo, A. Does Cervical Range of Motion Affect the Outcomes of Canalith Repositioning Procedures for Posterior Canal Benign Positional Paroxysmal Vertigo? Am. J. Otolaryngol.—Head Neck Med. Surg. 2019, 40, 494–498. [Google Scholar] [CrossRef] [PubMed]
- Fernandez-Mendoza, J.; Vgontzas, A.N. Insomnia and Its Impact on Physical and Mental Health. Curr. Psychiatry Rep. 2013, 15, 418. [Google Scholar] [CrossRef] [Green Version]
- Shih, C.P.; Wang, C.H.; Chung, C.H.; Lin, H.C.; Chen, H.C.; Lee, J.C.; Chien, W.C. Increased Risk of Benign Paroxysmal Positional Vertigo in Patients with Non-Apnea Sleep Disorders: A Nationwide, Population-Based Cohort Study. J. Clin. Sleep Med. 2018, 14, 2021–2029. [Google Scholar] [CrossRef]
- Bronstein, A. (Ed.) Oxford Textbook of Vertigo and Imbalance; Oxford University Press: London, UK, 2013; ISBN 9780199608997. [Google Scholar]
- Eckhardt-Henn, A.; Dieterich, M. Psychiatric Disorders in Otoneurology Patients. Neurol. Clin. 2005, 23, 731–749. [Google Scholar] [CrossRef]
| Authors | Year | Study | Patients (M/F) | Mean Age | Location of BPPV | Follow up | Recurrence Rate | Time to Recurrence | Location of Recurrence | Risk Factors Assessed |
|---|---|---|---|---|---|---|---|---|---|---|
| Del Rio et al. [10] | 2004 | R | 104 (35/69) | 64.3 y | PSC | 6–15 mo | 22.6% (21/93) | 118 d | N/A | RF3 *:7/16 ** RF4:1/12 |
| Korres et al. [11] | 2006 | R | 143 (62/81) | 59.9 y | 3SC bilateral multicanal | 24 mo | 13.3 % (19/143) | N/A | PSC HSC bilateral 2-canals | RF1 *:19/124 RF2: 11/81 RF4: 1/4 RF12 *:5/8 |
| Kansu et al. [7] | 2010 | R | 118 (44/74) | 51.8 y | PSC | 53–78 mo | 33.1% (39/118) | 53.8% within 2 y 33.1% within 5 y | PSC bilateral | RF1: 39/79 RF2: 25/74 RF3 *: 3/8 RF4 *:12/25 RF11:5/16 RF12: 2/5 |
| Choi et al. [12] | 2012 | R | 120 (43/77) | 50.4 y | PSC HSC | 6–29 mo | 10% (12/120) | N/A | PSC HSC | RF3 *: 2/2 RF4*: 2/8 |
| Yamanaka et al. [13] | 2013 | R | 61 (0/61) | 63.7 y | N/A | 12 mo | 56% (9/16) | N/A | N/A | RF5 *: 9/16 |
| Webster et al. [14] | 2014 | P | 72 (N/A) | N/A | N/A | 41 mo | 36.1% (26/72) | N/A | N/A | RF7 * |
| De Stefano et al. [1] | 2013 | R | 1092 (407/685) | 72.9 y | 3SC multicanal | 6–24 mo | 50.5% (551/1092) | N/A | PSC (36.8%) | RF5: 1/ 13 RF7 *: 10/16 RF8 *: 100/163 RF13 *: 8/13 |
| Babac et al. [15] | 2014 | P | 400 (119/281) | 58.7 y | 3SC bilateral multicanal | 12 mo | 15.5% (62/400) | 48.4% within 3 mo | ipsilateral PSC (61.29%) contralateral PSC (30.65%) multicanal ipsilateral (1 case) | RF1(>50 y): 51/254 RF2: 48/281 RF4: 4/18 RF5: 12/65 RF11: 6/55 RF10: 36/224 RF12: 0/5 |
| Su et al. [3] | 2016 | R | 243 (47/19) | 57.5 y | PSC | 24 mo | 18.9% (46/243) | RF1(>65 y): 15/58 RF2 *: 42/196 RF4: 2/11 RF10: 20/80 RF14 *: 14/40 | ||
| Kim et al. [8] | 2017 | R | 198 (59/139) | 62.9 y | 3SC | ≥12 mo | 33.8% (67/198) | mean period of 11.6 mo | 16% in different SC | RF1: 67/131 RF2: 49/139 RF5: 7/14 RF7 *:14/17 RF8 *:27/32 |
| Luryi et al. [16] | 2018 | R | 1105 (315/790) | 64.8 y | 3SC bilateral | 602 d | 37% | 76% within 2 y | 28% in the same ear | RF1(>60 y):267/700 RF2 *: 319/790 RF3: 31/103 RF4: 27/82 RF7: 47/134 |
| Nunez et al. [17] | 2000 | P | 151 (44/107) | 63.0 y | PSC | 15.9 mo | 26.8% (37/138) | 15% per year 40% within 40 mo | PSC | RF4: 10/27 |
| Brandt et al. [6] | 2009 | R | 125 (49/76) | 55.1 y | PSC | 10.3 y | 50% | 80% within 1 y 94% within 5 y | RF1: 37/54* RF2 *: 44/76 RF4: 7/17 RF11: 8/15 | |
| Perez et al. [5] | 2012 | P | 69 (25/44) | 62.0 y | 3SC bilateral multicanal | 47 mo | 27% (19/69) | 50% within 6 mo | 7/19 contralateral ear 5/7 other canal 6/12 other canal | RF1: 19/69 RF2 RF4 *: 3/6 RF12 *: 8/17 |
| Zhu et al. [18] | 2019 | R | 1012 (316/696) | 54.6 y | PSC HSC multicanal | 12 mo | 33,7% (255/757) | 12 mo | RF1(>60 y): 91/315 RF2 *: 187/696 RF3 *: 16/24 RF7: 24/87 RF8 *: 89/276 RF9 *: 84/266 RF10: 77/258 RF11 *: 14/29 | |
| Messina et al. [19] | 2017 | R | 2682 (1008/1571) | 59.3 y | 3SC | ≥6 mo | 52.5% (1386/2638) | 1–5 episodes per year (84.3%) | 49.2% same canal | RF7 *: 261/413 RF8 *: 844/1401 RF9 *: 1401/1906 RF10 *: 82/265 |
| Sreenivas et al. [2] | 2019 | R | 71 (31/40) | 49.0 y | N/A | 6–12 mo | 22.5% (16/71) | RF1(>60 y) *: 5/11 RF6: 12/56 RF7 *: 5/8 RF8: 8/21 RF9: 10/33 | ||
| Rhim et al. [20] | 2016 | R | 232 (63/169) | 50.35 y | 3SC bilateral multicanal | 10.2 mo | 17.7% (41/232) | N/A | N/A | RF1:41/191 RF2: 31/169 RF6 *:41/191 RF12: 6/28 |
| Balatsouras [21] | 2012 | R | 262 (97/165) 233 iBPPV 29 mBPPV | 53.4 y | 3SC bilateral multicanal | 12 mo | 44.4% (iBPPV) 13.3% (mBPPV) | N/A | N/A | RF3 *: 12/27 |
| Talaat et al. [22] | 2014 | P | 80 (28/52) | 47.6 y | 3SC | ≥12 mo | 45% (36/80) | N/A | N/A | RF1: 36/44 RF2: 27/52 RF5 *: 22/48 RF6 *: 34/72 |
| Yang CJ et al. [23] | 2017 | R | 130 (30/100) | 54.9 y | 3SC | 12 mo | 48% (63/130) | N/A | N/A | RF1 *: 63/67 RF2: 50/100 RF5: 39/68 RF6: 63/67 |
| Wei et al. [24] | 2018 | R | 127 (46/81) | 53.9 y | 3SC | 6 mo | 14.17% | 6 mo | N/A | RF1(>60y) RF2 RF7 RF8 RF9 RF11 RF13 |
| Faralli et al. [25] | 2006 | R | 566 (204/362) | 56.8 y | 3SC | 6 mo | 13.7% (77/560) | N/A | N/A | RF1(>50 y): 64/396 RF10 *: 22/111 |
| Piccioti et al. [4] | 2016 | R | 475 (188/287) | 61.9 y | PSC HSC | 30 mo | 23.4% (139/475) | N/A | N/A | RF1 *: 139/475 RF2 *: 95/287 RF4: 13/42 RF7 * RF8 * RF9 * RF10 * |
| Tan et al. [26] | 2016 | R | 88 (33/55) 47 i-BPPV 41 h-BPPV | 53.44 y (h-BPPV) 51.64 y (i-BPPV) | 3SC | ≥12 mo | 12.7% (6/47, i-BPPV) 31.7% (13/41, h-BPPV) | N/A | N/A | RF8 *: 13/41 |
| Prokopakis et al. [27] | 2012 | P | 965 (481/484) | N/A | 3SC | 74 mo | 15.5% (139/895) | N/A | N/A | RF1(>70 y) * RF4* |
| Rashad et al. [28] | 2009 | P | 103 (45/58) | 48.2 y | PSC | 5 y | 65% (67/103) | 46.3 mo | N/A | RF1(≥40 y) *: 49/82 RF2: 34/58 |
| Hilton et al. [29] | 2020 | R | 1481 (389/1092) | 63.3 y | N/A | ≥6 mo | 33.8% (267/791) | N/A | N/A | RF11: 80/209 |
| Ishiyama et al. [30] | 2000 | R | 247 (93/154) | N/A | PSC | ≥6 mo | 68.4% (169/247) | N/A | N/A | RF11 *: 48/62 |
| Gordon et al. [31] | 2004 | R | 21 t- BPPV (10/11) 42 i-BPPV (10/32) | 56.3 y (t-BPPV) 61.1 y (i-BPPV) | PSC HSC bilateral | 6–42 mo | 57% (12/21, t-BPPV) 19% (8/42, i-BPPV) | N/A | N/A | RF4 *: 12/21 |
| N of Studies Assessed | N of Studies with Statistical Significance | Recurrence/ Non-Recurrence (Cases) | Recurrence (%) | |
|---|---|---|---|---|
| Advanced Age | 18 | 6 | 976/2069 | 32.05% |
| Female gender | 15 | 5 | 962/2037 | 32.08% |
| Meniere’s disease | 6 | 5 | 71/109 | 39.44% |
| Trauma | 12 | 4 | 94/176 | 34.81% |
| Osteopenia/Osteoporosis | 6 | 2 | 90/134 | 40.18% |
| Vitamin D deficiency | 4 | 2 | 150/236 | 38.86% |
| Diabetesmellitus/Hyperisulinism/Hypergl-ycemia | 9 | 6 | 361/314 | 53.48% |
| Hypertension | 8 | 6 | 1081/853 | 55.89% |
| Hyperlipidemia | 5 | 3 | 1495/710 | 67.80% |
| Cardiovascular disease | 6 | 3 | 237/701 | 25.27% |
| Migraine | 7 | 2 | 161/225 | 41.71% |
| Bilateral/multicanal BPPV | 5 | 2 | 21/42 | 33.33% |
| Cervical osteoarthrosis | 2 | 1 | 8/5 | 61.54% |
| Sleep disorders | 1 | 1 | 14/26 | 35.00% |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2021 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Sfakianaki, I.; Binos, P.; Karkos, P.; Dimas, G.G.; Psillas, G. Risk Factors for Recurrence of Benign Paroxysmal Positional Vertigo. A Clinical Review. J. Clin. Med. 2021, 10, 4372. https://doi.org/10.3390/jcm10194372
Sfakianaki I, Binos P, Karkos P, Dimas GG, Psillas G. Risk Factors for Recurrence of Benign Paroxysmal Positional Vertigo. A Clinical Review. Journal of Clinical Medicine. 2021; 10(19):4372. https://doi.org/10.3390/jcm10194372
Chicago/Turabian StyleSfakianaki, Ioanna, Paris Binos, Petros Karkos, Grigorios G. Dimas, and George Psillas. 2021. "Risk Factors for Recurrence of Benign Paroxysmal Positional Vertigo. A Clinical Review" Journal of Clinical Medicine 10, no. 19: 4372. https://doi.org/10.3390/jcm10194372
APA StyleSfakianaki, I., Binos, P., Karkos, P., Dimas, G. G., & Psillas, G. (2021). Risk Factors for Recurrence of Benign Paroxysmal Positional Vertigo. A Clinical Review. Journal of Clinical Medicine, 10(19), 4372. https://doi.org/10.3390/jcm10194372








