Use of Phentolamine Mesylate in Implant Surgery: Analysis of Adverse Effects and Haemodynamic Changes
Abstract
1. Introduction
2. Materials and Methods
2.1. Study Design and Patient Selection
2.2. Surgical Technique
2.3. Data Recording and Monitoring
2.4. Statistical Analysis
3. Results
4. Discussion
5. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Conflicts of Interest
References
- Yang, F.; Gao, Y.; Zhang, L.; Zheng, B.; Wang, L.; Sun, H.; Huang, D. Local anaesthesia for surgical extraction of mandibular third molars: A systematic review and network meta-analysis. Clin. Oral Investig. 2020, 24, 3781–3800. [Google Scholar] [CrossRef] [PubMed]
- Camps-Font, O.; Figueiredo, R.; Sánchez-Torres, A.; Clé-Ovejero, A.; Coulthard, P.; Gay-Escoda, C.; Valmaseda-Castellón, E. Which is the most suitable local anaesthetic when inferior nerve blocks are used for impacted mandibular third molar extraction? A network meta-analysis. Int. J. Oral Maxillofac. Surg. 2020, 49, 1497–1507. [Google Scholar] [CrossRef]
- Al-Shayyab, M.H.; Baqain, Z.H. Factors predictive of the onset and duration of action of local anesthesia in mandibular third-molar surgery: A prospective study. Eur. J. Oral Sci. 2018, 126, 110–117. [Google Scholar] [CrossRef] [PubMed]
- Boonsiriseth, K.; Chaimanakarn, S.; Chewpreecha, P.; Nonpassopon, N.; Khanijou, M.; Ping, B.; Wongsirichat, N. 4% lidocaine versus 4% articaine for inferior alveolar nerve block in impacted lower third molar surgery. J. Dent. Anesth. Pain Med. 2017, 17, 29–35. [Google Scholar] [CrossRef][Green Version]
- Nourbakhsh, N.; Shirani, F.; Babaei, M. Effect of phentolamine mesylate on duration of soft tissue local anesthesia in children. J. Res. Pharm. Pract. 2012, 1, 55–59. [Google Scholar] [CrossRef] [PubMed]
- Saunders, T.R.; Psaltis, G.; Weston, J.F.; Yanase, R.R.; Rogy, S.S.; Ghalie, R.G. In-practice evaluation of OraVerse for the reversal of soft-tissue anesthesia after dental procedures. Compend. Contin. Educ. Dent. 2011, 32, 58–62. [Google Scholar]
- Hersh, E.V.; Moore, P.A.; Papas, A.S.; Goodson, J.M.; Navalta, L.A.; Rogy, S.; Rutherford, B.; Yagiela, J.A. Reversal of soft-tissue local anesthesia with phentolamine mesylate in adolescents and adults. J. Am. Dent. Assoc. 2008, 139, 1080–1093. [Google Scholar] [CrossRef] [PubMed]
- Rutherford, B.; Zeller, J.R.; Thake, D. Local and systemic toxicity of intraoral submucosal injections of phentolamine mesylate (OraVerse). Anesth. Prog. 2009, 56, 123–127. [Google Scholar] [CrossRef] [PubMed]
- Hersh, E.V.; Lindemeyer, R.; Berg, J.H.; Casamassimo, P.S.; Chin, J.; Marberger, A.; Lin, B.P.; Hutcheson, M.C.; Moore, P.A. Phase four, randomized, double-blinded, controlled trial of phentolamine mesylate in two- to five-year-old dental patients. Pediatr. Dent. 2017, 39, 39–45. [Google Scholar]
- Laviola, M.; McGavin, S.K.; Freer, G.A.; Plancich, G.; Woodbury, S.C.; Marinkovich, S.; Morrison, R.; Reader, A.; Rutherford, R.B.; Yagiela, J.A. Randomized study of phentolamine mesylate for reversal of local anesthesia. J. Dent. Res. 2008, 87, 635–639. [Google Scholar] [CrossRef]
- Morrow, T. OraVerse helps you lose that numbing feeling. Manag. Care 2008, 17, 50–51. [Google Scholar]
- Moore, P.A.; Hersh, E.V.; Papas, A.S.; Goodson, J.M.; Yagiela, J.A.; Rutherford, B.; Rogy, S.; Navalta, L. Pharmacokinetics of lidocaine with epinephrine following local anesthesia reversal with phentolamine mesylate. Anesth. Prog. 2008, 55, 40–48. [Google Scholar] [CrossRef]
- Haghighat, A.; Davoudi, A.; Minaiyan, M.; Molai, M.; Afshar, A.; Basiri, K. Effect of a trial pharmaceutical solution on reversing sensations after using lidocain: An animal study. Anesth. Essays Res. 2015, 9, 79–82. [Google Scholar] [CrossRef]
- Prados-Frutos, J.C.; Rojo, R.; Gonzalez-Serrano, J.; Gonzalez-Serrano, C.; Sammartino, G.; Martinez-Gonzalez, J.M.; Sánchez-Moncescillo, A. Phentolamine mesylate to reverse oral soft-tissue local anesthesia: A systematic review and meta-analysis. J. Am. Dent. Assoc. 2015, 146, 751–759. [Google Scholar] [CrossRef]
- Fowler, S.; Nusstein, J.; Drum, M.; Reader, A.; Beck, M. Reversal of soft-tissue anesthesia in asymptomatic endodontic patients: A preliminary, prospective, randomized, single-blind study. J. Endod. 2011, 37, 1353–1358. [Google Scholar] [CrossRef]
- Elmore, S.; Nusstein, J.; Drum, M.; Reader, A.; Beck, M.; Fowler, S. Reversal of pulpal and soft tissue anesthesia by using phentolamine: A prospective randomized, single-blind study. J. Endod. 2013, 39, 429–434. [Google Scholar] [CrossRef] [PubMed]
- Michaud, P.L.; Flood, B.; Brillant, M.S. Reversing the effects of 2% lidocaine: A randomized controlled clinical trial. J. Dent. 2018, 72, 76–79. [Google Scholar] [CrossRef]
- Wynn, R.L. Phentolamine mesylate—An old medical drug becomes a new dental drug. Gen. Dent. 2009, 57, 200–202. [Google Scholar] [PubMed]
- Grover, H.S.; Gupta, A.; Saksena, N.; Saini, N. Phentolamine mesylate: It’s role as a reversal agent for unwarranted prolonged local analgesia. J. Indian Soc. Pedod. Prev. Dent. 2015, 33, 265–268. [Google Scholar] [CrossRef]
- Yagiela, J.A. What’s new with phentolamine mesylate: A reversal agent for local anaesthesia? SAAD Dig. 2011, 27, 3–7. [Google Scholar] [PubMed]
- Tavares, M.; Goodson, J.M.; Studen-Pavlovich, D.; Yagiela, J.A.; Navalta, L.A.; Rogy, S.; Rutherford, B.; Gordon, S.; Papas, A.S. Reversal of soft-tissue local anesthesia with phentolamine mesylate in pediatric patients. J. Am. Dent. Assoc. 2008, 139, 1095–1104. [Google Scholar] [CrossRef]
- Helmi, M.; AlDosari, M.; Tavares, M. Phentolamine Mesylate may be a safe and effective option to reduce discomfort and time to recovery after dental care with local anesthesia. J. Evid. Based. Dent. Pract. 2018, 18, 181–184. [Google Scholar] [CrossRef]
- Daubländer, M.; Liebaug, F.; Niedeggen, G.; Theobald, K.; Kürzinger, M.L. Effectiveness and safety of phentolamine mesylate in routine dental care. J. Am. Dent. Assoc. 2017, 148, 149–156. [Google Scholar] [CrossRef]
- Boynes, S.G.; Riley, A.E.; Milbee, S.; Bastin, M.R.; Price, M.E.; Ladson, A. Evaluating complications of local anesthesia administration and reversal with phentolamine mesylate in a portable pediatric dental clinic. Gen. Dent. 2013, 61, 70–76. [Google Scholar]
- Prasanna, J.S. OraVerse: Reverses numbness after dental procedures. J. Maxillofac. Oral Surg. 2012, 11, 212–219. [Google Scholar] [CrossRef] [PubMed][Green Version]
- Vinnakota, D.N.; Kamatham, R. Safety profile of phentolamine mesylate as reversal agent of pulpal and soft tissue dental anesthesia: A systematic review and meta-analysis. Quintessence Int. 2019, 50, 568–575. [Google Scholar] [CrossRef]
- Froum, S.J.; Froum, S.H.; Malamed, S.F. The use of phentolamine mesylate to evaluate mandibular nerve damage following implant placement. Compend. Contin. Educ. Dent. 2010, 31, 522–528. [Google Scholar]
- Hersh, E.V.; Lindemeyer, R.G. Phentolamine mesylate for accelerating recovery from lip and tongue anesthesia. Dent. Clin. N. Am. 2010, 54, 631–642. [Google Scholar] [CrossRef] [PubMed]
- Gago-García, A.; Barrilero-Martin, C.; Alobera-Gracia, M.A.; Del Canto-Pingarrón, M.; Seco-Calvo, J. Efficacy of phentolamine mesylate in reducing the duration of various local anesthetics. J. Dent. Anesth. Pain Med. 2021, 21, 49–59. [Google Scholar] [CrossRef]
- Michaud, P.L.; Nowe, E.; Smith Brillant, M. Reversing the effects of 0.5% bupivacaine using phentolamine mesylate: A preliminary randomized controlled clinical trial. J. Clin. Pharmacol. 2020, 60, 669–674. [Google Scholar] [CrossRef] [PubMed]
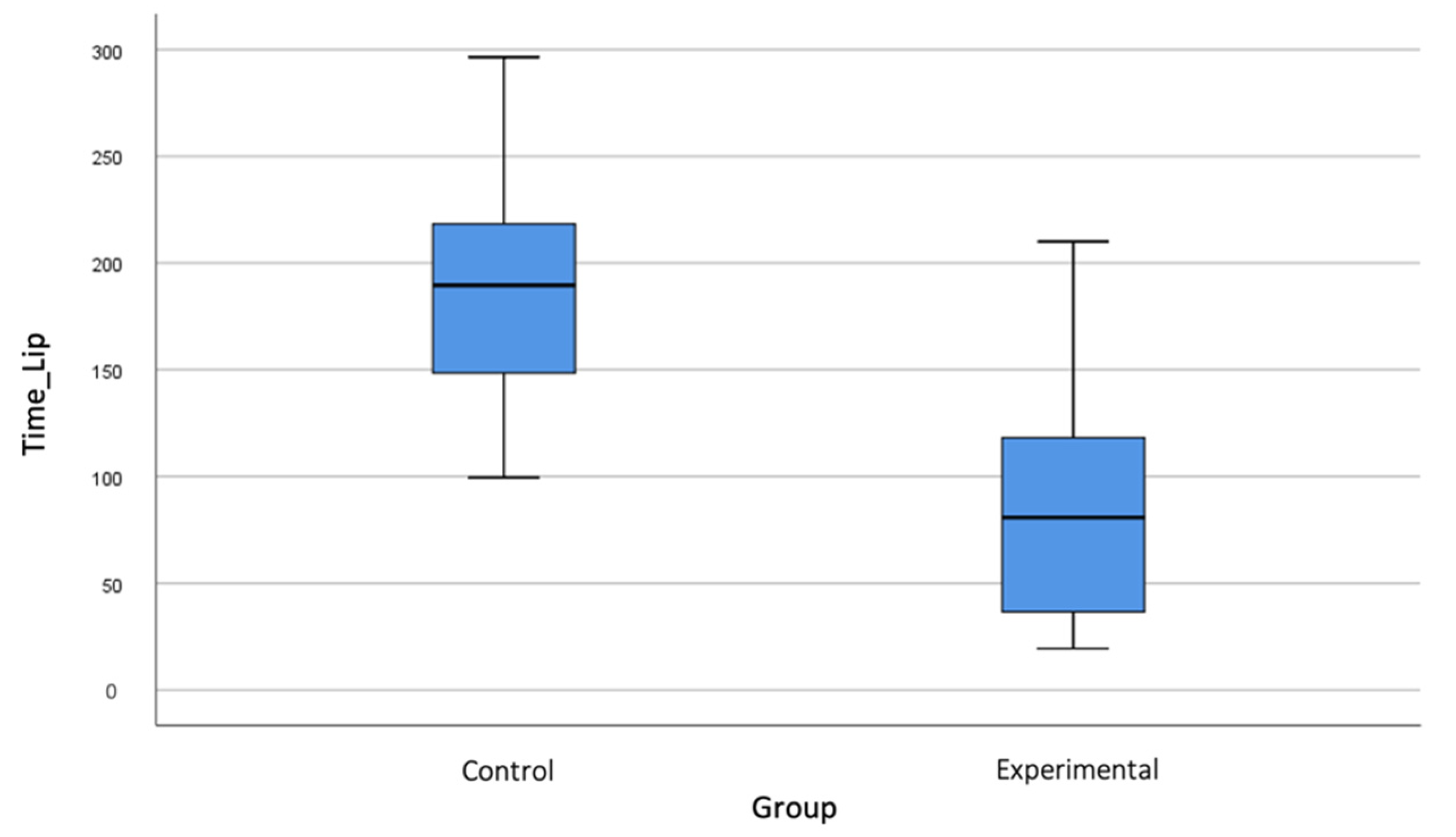

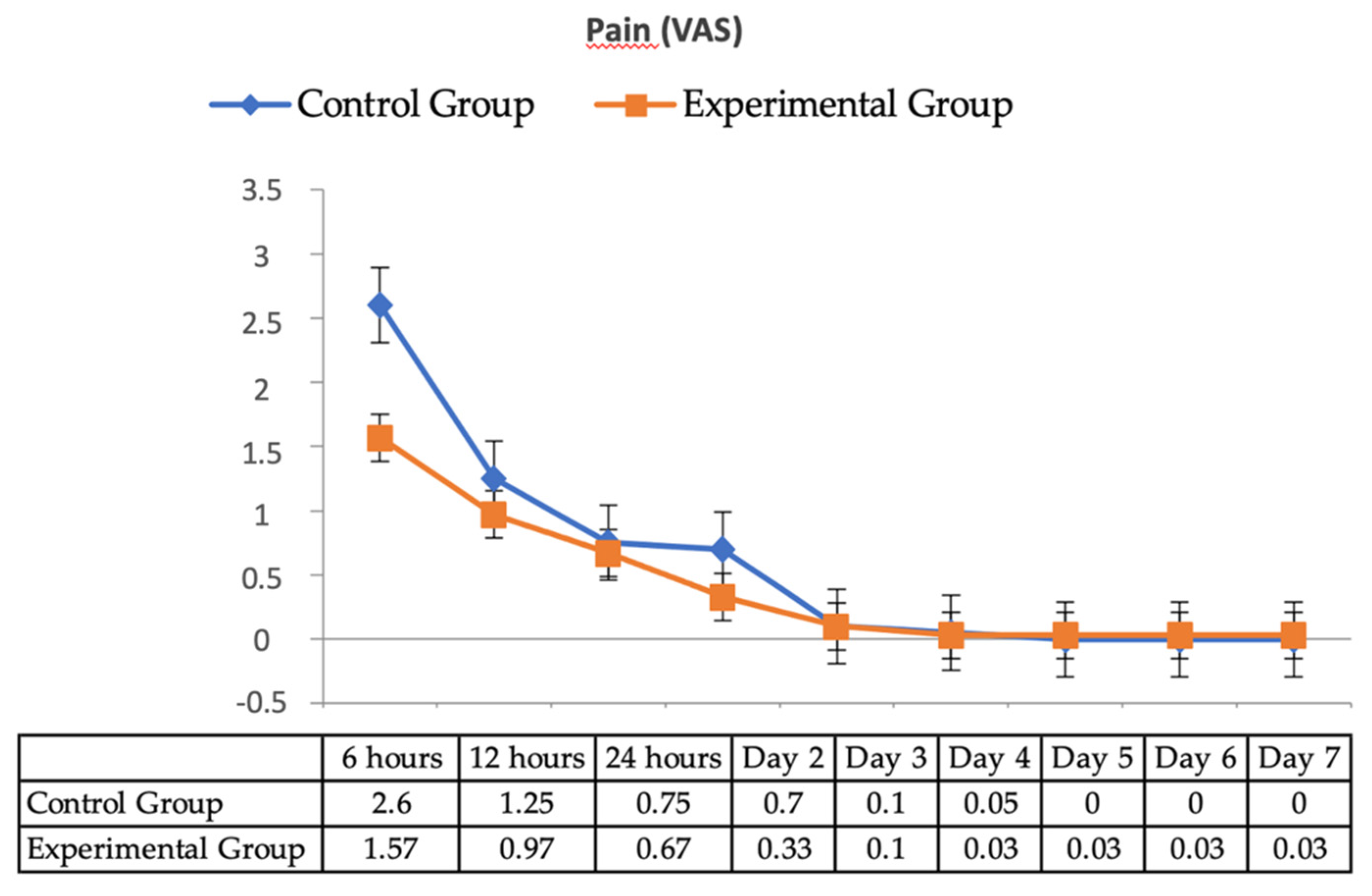
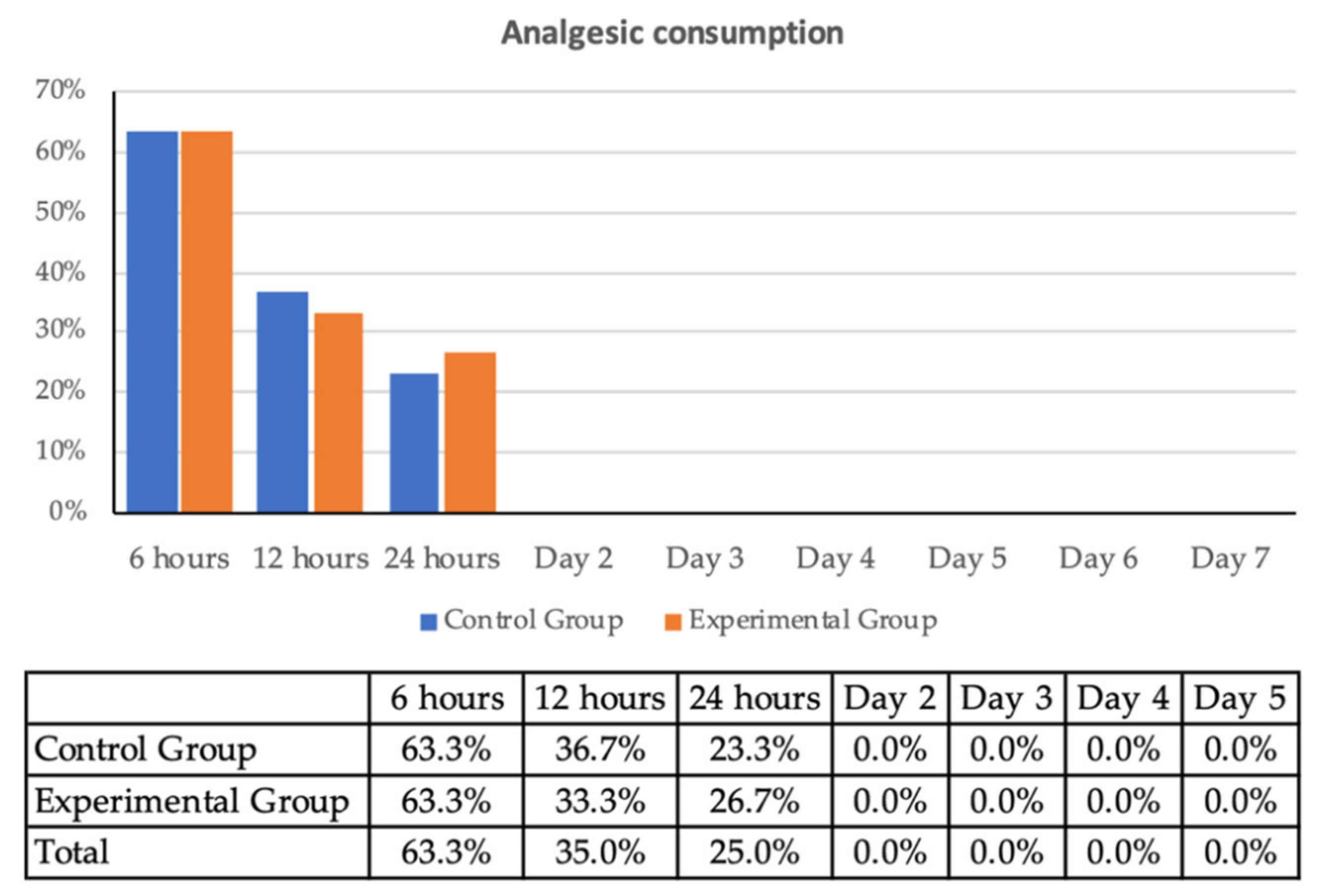
| Baseline Values | ||||||||
|---|---|---|---|---|---|---|---|---|
| SBP | p | DBP | p | HR | p | SaO2 | p | |
| CG | 128.37 | 0.041 * | 78.50 | 0.905 | 74.93 | 0.754 | 99% | 0.155 |
| EG | 121.40 | 78.27 | 75.73 | 98.99% | ||||
| Final Values | ||||||||
| SBP | p | DBP | p | HR | p | SaO2 | p | |
| CG | 128.40 | 0.341 | 80.87 | 0.550 | 72.33 | 0.373 | 99% | 0.155 |
| EG | 125.20 | 79.47 | 74.47 | 98.99% | ||||
| Questions | 0 | 1 | 2 | 3 | 4 | Average | p | ||
|---|---|---|---|---|---|---|---|---|---|
| 1 | Have you experienced speech impairment? | CG | 60% | 30% | 5% | 5% | 0.55 | 0.253 | |
| EG | 76.7% | 13.3% | 10% | 0.33 | |||||
| 2 | Have you had any difficulty eating? | CG | 20% | 60% | 10% | 10% | 1.10 | 0.01 * | |
| EG | 73.3% | 13.3% | 13.3% | 0.40 | |||||
| 3 | Have you bitten your tongue, lip or cheek during this time? | CG | 80% | 5% | 15% | 0.35 | 0.05 * | ||
| EG | 96.7% | 3.3% | 0.03 | ||||||
| 4 | Have you experienced more salivation than usual? | CG | 75% | 10% | 10% | 5% | 0.45 | 0.703 | |
| EG | 66.7% | 26.7% | 3.3% | 3.3% | 0.43 | ||||
| 5 | Have you felt unwell? (headache, nausea, etc.) | CG | 95% | 5% | 0.10 | 0.361 | |||
| EG | 86.7% | 10% | 3.3% | 0.23 | |||||
| 6 | Have you had difficulty communicating? | CG | 80% | 20% | 0.20 | 0.523 | |||
| EG | 73.3% | 20% | 6.7% | 0.33 | |||||
| 7 | Have you felt a temporary decrease in your quality of life? | CG | 55% | 40% | 5% | 0.60 | 0.084 | ||
| EG | 80% | 13.3% | 3.3% | 3.3% | 0.30 | ||||
| 8 | Have you had pain in the area where the anaesthetic solution was injected? | CG | 70% | 30% | 0.30 | 0.043 * | |||
| EG | 46.7% | 30% | 16.7% | 3.3% | 3.3% | 0.87 | |||
| 9 | Have you noticed palpitations or a dizzy feeling? (heart rate) | CG | 100% | 0.00 | 0.414 | ||||
| EG | 96.7% | 3.3% | 0.03 | ||||||
| 10 | Have you had a headache or neck pain? (blood pressure) | CG | 90% | 10% | 0.10 | 0.725 | |||
| EG | 86.7% | 13.3% | 0.13 | ||||||
| 11 | Have you had an itching, tingling or burning sensation in the area around the injection site? | CG | 75% | 25% | 0.25 | 0.191 | |||
| EG | 60% | 26% | 10% | 3.3% | 0.57 |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2021 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Vintanel-Moreno, C.; Martínez-González, J.M.; Martínez-Rodríguez, N.; Meniz-García, C.; Leco-Berrocal, I. Use of Phentolamine Mesylate in Implant Surgery: Analysis of Adverse Effects and Haemodynamic Changes. J. Clin. Med. 2021, 10, 3875. https://doi.org/10.3390/jcm10173875
Vintanel-Moreno C, Martínez-González JM, Martínez-Rodríguez N, Meniz-García C, Leco-Berrocal I. Use of Phentolamine Mesylate in Implant Surgery: Analysis of Adverse Effects and Haemodynamic Changes. Journal of Clinical Medicine. 2021; 10(17):3875. https://doi.org/10.3390/jcm10173875
Chicago/Turabian StyleVintanel-Moreno, Clara, José María Martínez-González, Natalia Martínez-Rodríguez, Cristina Meniz-García, and Isabel Leco-Berrocal. 2021. "Use of Phentolamine Mesylate in Implant Surgery: Analysis of Adverse Effects and Haemodynamic Changes" Journal of Clinical Medicine 10, no. 17: 3875. https://doi.org/10.3390/jcm10173875
APA StyleVintanel-Moreno, C., Martínez-González, J. M., Martínez-Rodríguez, N., Meniz-García, C., & Leco-Berrocal, I. (2021). Use of Phentolamine Mesylate in Implant Surgery: Analysis of Adverse Effects and Haemodynamic Changes. Journal of Clinical Medicine, 10(17), 3875. https://doi.org/10.3390/jcm10173875







