Immunotherapy and Vaccination in Surgically Resectable Non-Small Cell Lung Cancer (NSCLC)
Abstract
:1. Introduction
2. Current Immune Checkpoint Inhibitors in Advanced Non-Small Cell Lung Cancer (NSCLC)
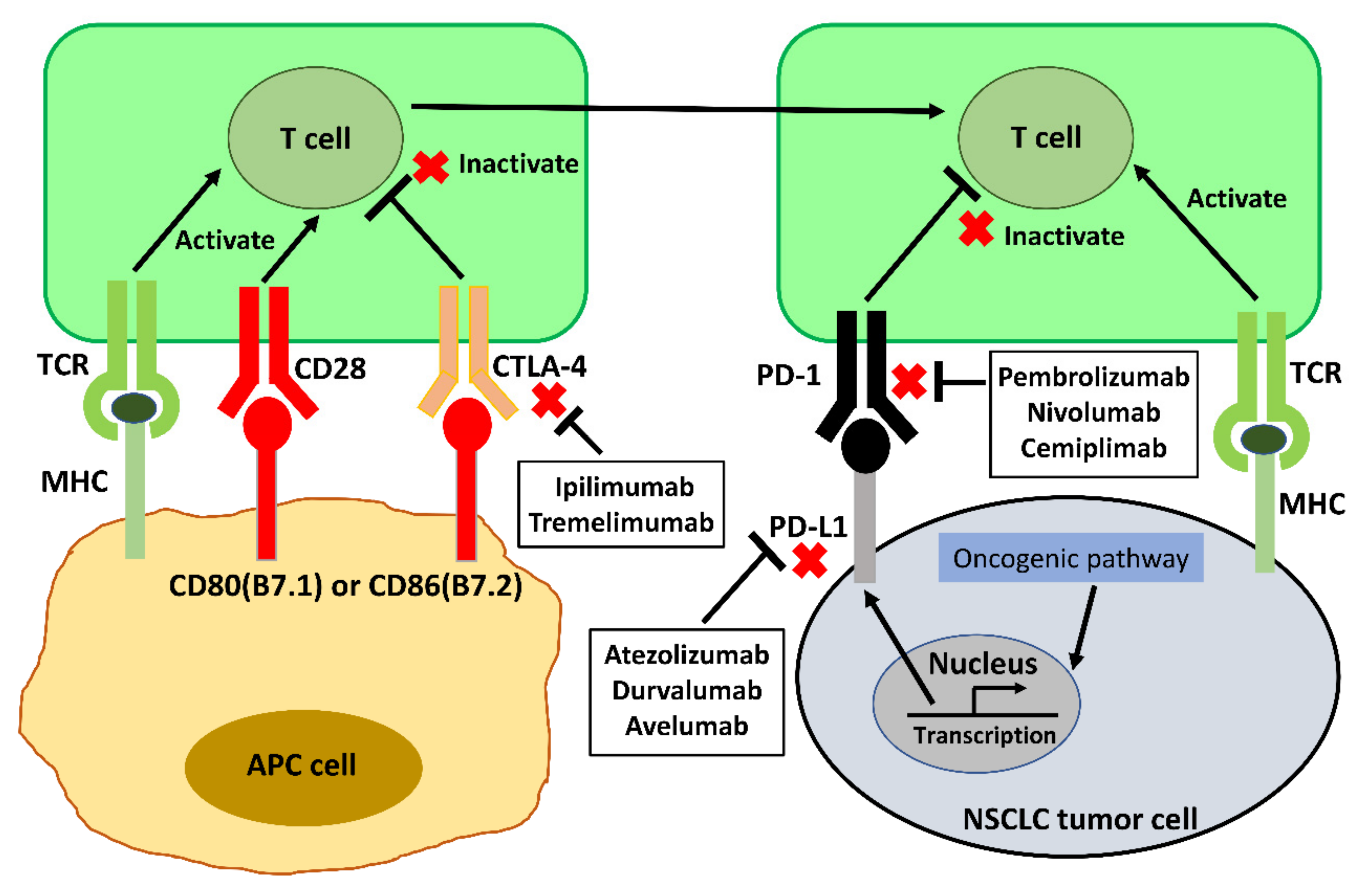
2.1. Anti-Programmed Cell Death Protein-1 (PD-1)/Programmed Death-Ligand 1 (PD-L1) Immune Checkpoint Antibodies in NSCLC
2.2. Anti-Cytotoxic T-Lymphocyte-Associated Protein 4 (CTLA-4) Antibodies
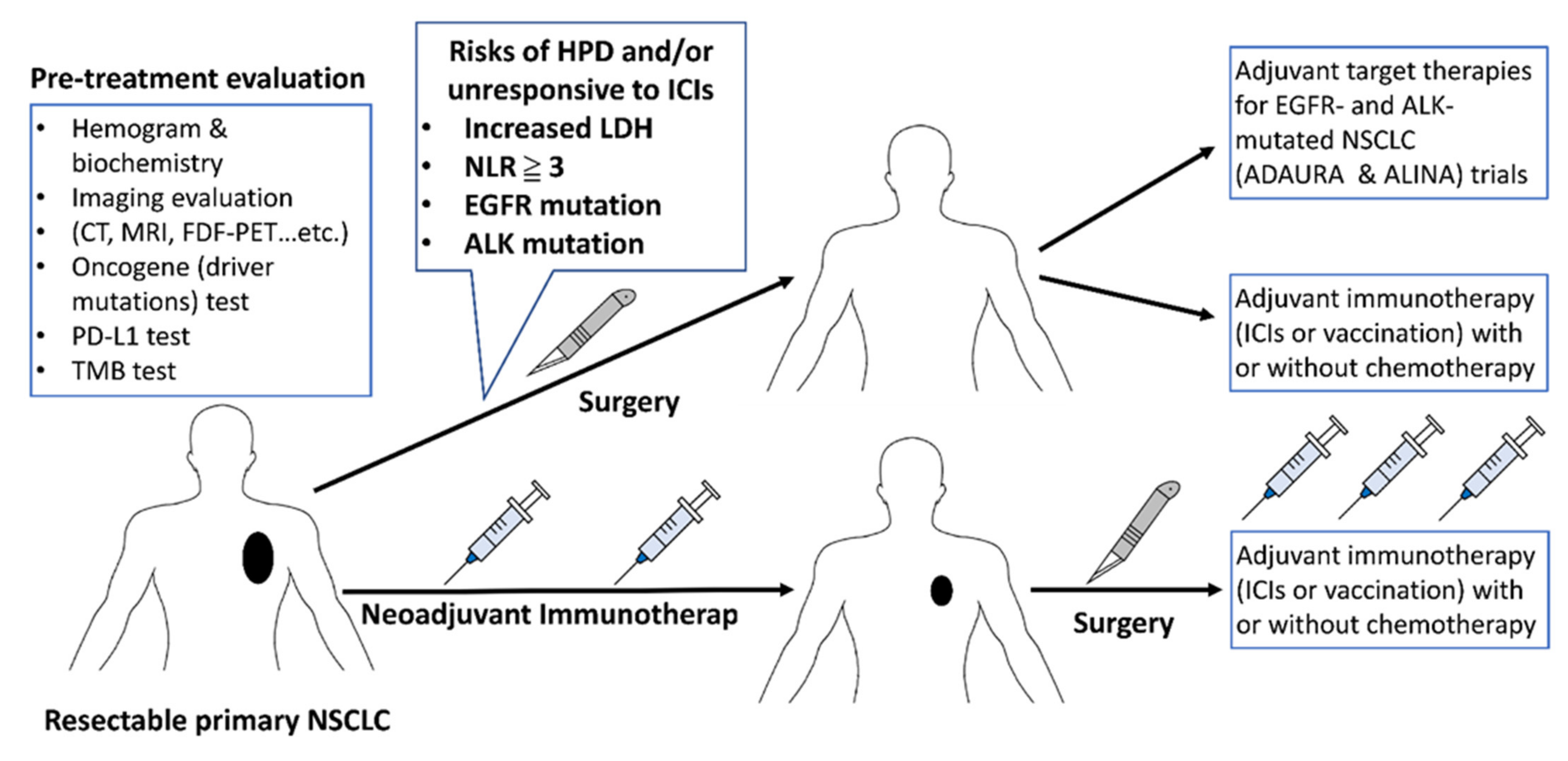
3. Neoadjuvant and Adjuvant Immunotherapy in Surgically Resectable NSCLC
3.1. Immune Checkpoints Inhibitors (ICIs) in Neoadjuvant Therapy
3.2. Immune Checkpoint Inhibitors (ICIs) in Post-Operation Adjuvant Therapy
3.3. Immune Checkpoint Inhibitors (ICIs) in Neoadjuvant Therapy or Adjuvant Therapy
4. Therapeutic Vaccination in NSCLC
4.1. Cancer Vaccines and Tumor Antigens
4.2. Interaction between Immune Cells and Tumor Microenvironment
4.3. Clinical Trials of Cancer Vaccines in NSCLC
4.4. Cancer Vaccination in Combination with Immunotherapies
5. Future Perspectives: The Challenges of Immunotherapy in Surgically Resectable NSCLC
5.1. Imaging Evaluation of Response before Surgery and Post-Operative Follow-Up
5.2. Predictive Biomarkers in Therapy
5.3. The Primary Endpoints: Pathological Response and Survival; Timing and Type of Surgery
6. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Conflicts of Interest
References
- McIntyre, A.; Ganti, A.K. Lung cancer-A global perspective. J. Surg. Oncol. 2017, 115, 550–554. [Google Scholar] [CrossRef]
- Cao, M.; Chen, W. Epidemiology of lung cancer in China. Thorac. Cancer 2018, 10, 3–7. [Google Scholar] [CrossRef]
- Gridelli, C.; Rossi, A.; Carbone, D.P.; Guarize, J.; Karachaliou, N.; Mok, T.; Petrella, F.; Spaggiari, L.; Rosell, R. Non-small-cell lung cancer. Nat. Rev. Dis. Prim. 2015, 1, 15009. [Google Scholar] [CrossRef] [PubMed]
- Chen, Z.; Fillmore, C.M.; Hammerman, P.S.; Kim, C.F.; Wong, K.-K. Non-small-cell lung cancers: A heterogeneous set of diseases. Nat. Rev. Cancer 2014, 14, 535–546. [Google Scholar] [CrossRef]
- Donington, J.S.; Kim, Y.T.; Tong, B.; Moreira, A.L.; Bessich, J.; Weiss, K.D.; Colson, Y.L.; Wigle, D.; Osarogiagbon, R.U.; Zweig, J.; et al. Progress in the Management of Early-Stage Non–Small Cell Lung Cancer in 2017. J. Thorac. Oncol. 2018, 13, 767–778. [Google Scholar] [CrossRef] [Green Version]
- Kris, M.G.; Gaspar, L.E.; Chaft, J.E.; Kennedy, E.B.; Azzoli, C.G.; Ellis, P.M.; Lin, S.H.; Pass, H.; Seth, R.; Shepherd, F.A.; et al. Adjuvant Systemic Therapy and Adjuvant Radiation Therapy for Stage I to IIIA Completely Resected Non–Small-Cell Lung Cancers: American Society of Clinical Oncology/Cancer Care Ontario Clinical Practice Guideline Update. J. Clin. Oncol. 2017, 35, 2960–2974. [Google Scholar] [CrossRef] [Green Version]
- Goldstraw, P.; Chansky, K.; Crowley, J.; Rami-Porta, R.; Asamura, H.; Eberhardt, W.E.; Nicholson, A.G.; Groome, P.; Mitchell, A.; Bolejack, V.; et al. The IASLC Lung Cancer Staging Project: Proposals for Revision of the TNM Stage Groupings in the Forthcoming (Eighth) Edition of the TNM Classification for Lung Cancer. J. Thorac. Oncol. 2016, 11, 39–51. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Wu, Y.-L.; Tsuboi, M.; He, J.; John, T.; Grohe, C.; Majem, M.; Goldman, J.W.; Laktionov, K.; Kim, S.-W.; Kato, T.; et al. Osimertinib in Resected EGFR-Mutated Non–Small-Cell Lung Cancer. N. Engl. J. Med. 2020, 383, 1711–1723. [Google Scholar] [CrossRef] [PubMed]
- Hsu, P.-C.; Jablons, D.M.; Yang, C.-T.; You, L. Epidermal Growth Factor Receptor (EGFR) Pathway, Yes-Associated Protein (YAP) and the Regulation of Programmed Death-Ligand 1 (PD-L1) in Non-Small Cell Lung Cancer (NSCLC). Int. J. Mol. Sci. 2019, 20, 3821. [Google Scholar] [CrossRef] [Green Version]
- Vaddepally, R.K.; Kharel, P.; Pandey, R.; Garje, R.; Chandra, A.B. Review of Indications of FDA-Approved Immune Check-point Inhibitors per NCCN Guidelines with the Level of Evidence. Cancers 2020, 12, 738. [Google Scholar] [CrossRef] [Green Version]
- Broderick, S.R. Adjuvant and Neoadjuvant Immunotherapy in Non-small Cell Lung Cancer. Thorac. Surg. Clin. 2020, 30, 215–220. [Google Scholar] [CrossRef]
- Iwai, Y.; Ishida, M.; Tanaka, Y.; Okazaki, T.; Honjo, T.; Minato, N. Involvement of PD-L1 on tumor cells in the escape from host immune system and tumor immunotherapy by PD-L1 blockade. Proc. Natl. Acad. Sci. USA 2002, 99, 12293–12297. [Google Scholar] [CrossRef] [Green Version]
- Okazaki, T.; Honjo, T. The PD-1–PD-L pathway in immunological tolerance. Trends Immunol. 2006, 27, 195–201. [Google Scholar] [CrossRef]
- Keir, M.E.; Butte, M.; Freeman, G.J.; Sharpe, A.H. PD-1 and Its Ligands in Tolerance and Immunity. Annu. Rev. Immunol. 2008, 26, 677–704. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Sun, C.; Mezzadra, R.; Schumacher, T.N. Regulation and Function of the PD-L1 Checkpoint. Immunity 2018, 48, 434–452. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Falcone, M.; Fousteri, G. Role of the PD-1/PD-L1 Dyad in the Maintenance of Pancreatic Immune Tolerance for Prevention of Type 1 Diabetes. Front. Endocrinol. 2020, 11, 567. [Google Scholar] [CrossRef] [PubMed]
- Pardoll, D.M. The blockade of immune checkpoints in cancer immunotherapy. Nat. Rev. Cancer 2012, 12, 252–264. [Google Scholar] [CrossRef] [Green Version]
- Postow, M.A.; Callahan, M.K.; Wolchok, J.D. Immune Checkpoint Blockade in Cancer Therapy. J. Clin. Oncol. 2015, 33, 1974–1982. [Google Scholar] [CrossRef] [Green Version]
- Iwai, Y.; Hamanishi, J.; Chamoto, K.; Honjo, T. Cancer immunotherapies targeting the PD-1 signaling pathway. J. Biomed. Sci. 2017, 24, 1–11. [Google Scholar] [CrossRef] [Green Version]
- Ogunleyea, F.; Blankenshipa, L.; Millisorb, V.; Anderson, J.; Jaiyesimi, I. Programmed cell death-1/Programmed cell death ligand-1(PD-1/PD-L1) inhibitors, heralding a new era of immunotherapy in the management of advanced Non-Small Cell Lung Cancer (NSCLC). Cancer Treat. Res. Commun. 2017, 12, 6–13. [Google Scholar] [CrossRef]
- Nasser, N.; Gorenberg, M.; Agbarya, A. First Line Immunotherapy for Non-Small Cell Lung Cancer. Pharmaceuticlas 2020, 13, 373. [Google Scholar] [CrossRef]
- Reck, M.; Rodríguez-Abreu, D.; Robinson, A.G.; Hui, R.; Csőszi, T.; Fülöp, A.; Gottfried, M.; Peled, N.; Tafreshi, A.; Cuffe, S.; et al. Pembrolizumab versus Chemotherapy for PD-L1–Positive Non–Small-Cell Lung Cancer. N. Engl. J. Med. 2016, 375, 1823–1833. [Google Scholar] [CrossRef] [Green Version]
- Mok, T.S.K.; Wu, Y.-L.; Kudaba, I.; Kowalski, D.M.; Cho, B.C.; Turna, H.Z.; Castro, G.; Srimuninnimit, V.; Laktionov, K.K.; Bondarenko, I.; et al. Pembrolizumab versus chemotherapy for previously untreated, PD-L1-expressing, locally advanced or metastatic non-small-cell lung cancer (KEYNOTE-042): A randomised, open-label, controlled, phase 3 trial. Lancet 2019, 393, 1819–1830. [Google Scholar] [CrossRef]
- Gandhi, L.; Rodríguez-Abreu, D.; Gadgeel, S.; Esteban, E.; Felip, E.; De Angelis, F.; Domine, M.; Clingan, P.; Hochmair, M.J.; Powell, S.F.; et al. Pembrolizumab plus Chemotherapy in Metastatic Non–Small-Cell Lung Cancer. N. Engl. J. Med. 2018, 378, 2078–2092. [Google Scholar] [CrossRef] [PubMed]
- Paz-Ares, L.; Luft, A.; Vicente, D.; Tafreshi, A.; Gümü¸s, M.; Mazières, J.; Hermes, B.; Çay ¸Senler, F.; Cs˝oszi, T.; Fülöp, A.; et al. Pembrolizumab plus Chemotherapy for Squamous Non-Small-Cell Lung Cancer. N. Engl. J. Med. 2018, 379, 2040–2051. [Google Scholar] [CrossRef]
- Hellmann, M.D.; Paz-Ares, L.; Caro, R.B.; Zurawski, B.; Kim, S.-W.; Costa, E.C.; Park, K.; Alexandru, A.; Lupinacci, L.; De la Mora, J.E.; et al. Nivolumab plus ipilimumab in advanced non–small-cell lung cancer. N. Engl. J. Med. 2019, 381, 2020–2031. [Google Scholar] [CrossRef] [PubMed]
- Paz-Ares, L.; Ciuleanu, T.-E.; Cobo, M.; Schenker, M.; Zurawski, B.; Menezes, J.; Richardet, E.; Bennouna, J.; Felip, E.; Juan-Vidal, O.; et al. First-line nivolumab plus ipilimumab combined with two cycles of chemotherapy in patients with non-small-cell lung cancer (CheckMate 9LA): An international, randomised, open-label, phase 3 trial. Lancet Oncol. 2021, 22, 198–211. [Google Scholar] [CrossRef]
- Sezer, A.; Kilickap, S.; Gümüş, M.; Bondarenko, I.; Özgüroğlu, M.; Gogishvili, M.; Turk, H.M.; Cicin, I.; Bentsion, D.; Gladkov, O.; et al. Cemiplimab monotherapy for first-line treatment of advanced non-small-cell lung cancer with PD-L1 of at least 50%: A multicentre, open-label, global, phase 3, randomised, controlled trial. Lancet 2021, 397, 592–604. [Google Scholar] [CrossRef]
- Socinski, M.A.; Jotte, R.M.; Cappuzzo, F.; Orlandi, F.; Stroyakovskiy, D.; Nogami, N.; Rodríguez-Abreu, D.; Moro-Sibilot, D.; Thomas, C.A.; Barlesi, F. Atezolizumab for First-Line Treatment of Metastatic Nonsquamous NSCLC. N. Engl. J. Med. 2018, 378, 2288–2301. [Google Scholar] [CrossRef]
- Reck, M.; Mok, T.; Nishio, M.; Jotte, R.M.; Cappuzzo, F.; Orlandi, F.; Stroyakovskiy, D.; Nogami, N.; Rodríguez-Abreu, D.; Moro-Sibilot, D.; et al. Atezolizumab plus bevacizumab and chemotherapy in non-small-cell lung cancer (IMpower150): Key subgroup analyses of patients with EGFR mutations or baseline liver metastases in a randomised, open-label phase 3 trial. Lancet Respir. Med. 2019, 7, 387–401. [Google Scholar] [CrossRef]
- West, H.; McCleod, M.; Hussein, M.; Morabito, A.; Rittmeyer, A.; Conter, H.J.; Kopp, H.-G.; Daniel, D.; McCune, S.; Mekhail, T.; et al. Atezolizumab in combination with carboplatin plus nab-paclitaxel chemotherapy compared with chemotherapy alone as first-line treatment for metastatic non-squamous non-small-cell lung cancer (IMpower130): A multicentre, randomised, open-label, phase 3 trial. Lancet Oncol. 2019, 20, 924–937. [Google Scholar] [CrossRef]
- Herbst, R.S.; Giaccone, G.; De Marinis, F.; Reinmuth, N.; Vergnenegre, A.; Barrios, C.H.; Morise, M.; Felip, E.; Andric, Z.; Geater, S.; et al. Atezolizumab for First-Line Treatment of PD-L1–Selected Patients with NSCLC. N. Engl. J. Med. 2020, 383, 1328–1339. [Google Scholar] [CrossRef]
- Antonia, S.J.; Villegas, A.; Daniel, D.; Vicente, D.; Murakami, S.; Hui, R.; Yokoi, T.; Chiappori, A.; Lee, K.H.; De Wit, M.; et al. Durvalumab after Chemoradiotherapy in Stage III Non–Small-Cell Lung Cancer. N. Engl. J. Med. 2017, 377, 1919–1929. [Google Scholar] [CrossRef] [Green Version]
- Faivre-Finn, C.; Vicente, D.; Kurata, T.; Planchard, D.; Paz-Ares, L.; Vansteenkiste, J.F.; Spigel, D.R.; Garassino, M.C.; Reck, M.; Senan, S.; et al. Four-Year Survival With Durvalumab After Chemoradiotherapy in Stage III NSCLC—an Update From the PACIFIC Trial. J. Thorac. Oncol. 2021, 16, 860–867. [Google Scholar] [CrossRef]
- Passiglia, F.; Bronte, G.; Bazan, V.; Natoli, C.; Rizzo, S.; Galvano, A.; Listì, A.; Cicero, G.; Rolfo, C.; Santini, D.; et al. PD-L1 expression as predictive biomarker in patients with NSCLC: A pooled analysis. Oncotarget 2016, 7, 19738–19747. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Zhang, H.; Dutta, P.; Liu, J.; Sabri, N.; Song, Y.; Li, W.; Li, J. Tumour cell-intrinsic CTLA4 regulates PD-L1 expression in non-small cell lung cancer. J. Cell. Mol. Med. 2018, 23, 535–542. [Google Scholar] [CrossRef] [Green Version]
- Inaba-Higashiyama, R.; Yoshida, T.; Jo, H.; Shirasawa, M.; Motoi, N.; Ohe, Y. Clinical outcomes of pembrolizumab therapy in advanced- NSCLC patients with poor performance status (≥3) and high PD-L1 expression (TPS ≥50%): A case series. Thorac. Cancer 2020, 11, 3618–3621. [Google Scholar] [CrossRef]
- Ferrara, M.G.; Di Noia, V.; D’Argento, E.; Vita, E.; Damiano, P.; Cannella, A.; Ribelli, M.; Pilotto, S.; Milella, M.; Tortora, G.; et al. Oncogene-Addicted Non-Small-Cell Lung Cancer: Treatment Opportunities and Future Perspectives. Cancers 2020, 12, 1196. [Google Scholar] [CrossRef]
- Metro, G.; Baglivo, S.; Moretti, R.; Bellezza, G.; Sidoni, A.; Roila, F. Is There a Role for Multiple Lines of Anti-HER2 Therapies Administered Beyond Progression in HER2-Mutated Non-Small Cell Lung Cancer? A Case Report and Literature Review. Oncol. Ther. 2020, 8, 341–350. [Google Scholar] [CrossRef]
- Hsu, P.-C.; Wang, C.-W.; Kuo, S.C.-H.; Lin, S.-M.; Lo, Y.-L.; Huang, A.C.-C.; Chiu, L.-C.; Yang, C.-T. The Co-Expression of Programmed Death-Ligand 1 (PD-L1) in Untreated EGFR-Mutated Metastatic Lung Adenocarcinoma. Biomedicines 2020, 8, 36. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Mazieres, J.; Drilon, A.; Lusque, A.; Mhanna, L.; Cortot, A.; Mezquita, L.; Thai, A.; Mascaux, C.; Couraud, S.; Veillon, R.; et al. Immune checkpoint inhibitors for patients with advanced lung cancer and oncogenic driver alterations: Results from the IMMUNOTARGET registry. Ann. Oncol. 2019, 30, 1321–1328. [Google Scholar] [CrossRef] [PubMed]
- Oya, Y.; Kuroda, H.; Nakada, T.; Takahashi, Y.; Sakakura, N.; Hida, T. Efficacy of Immune Checkpoint Inhibitor Monotherapy for Advanced Non-Small-Cell Lung Cancer with ALK Rearrangement. Int. J. Mol. Sci. 2020, 21, 2623. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Kartolo, A.; Feilotter, H.; Hopman, W.; Fung, A.S.; Robinson, A. A single institution study evaluating outcomes of PD-L1 high KRAS-mutant advanced non-small cell lung cancer (NSCLC) patients treated with first line immune checkpoint inhibitors. Cancer Treat. Res. Commun. 2021, 27, 100330. [Google Scholar] [CrossRef]
- Guisier, F.; Dubos-Arvis, C.; Viñas, F.; Doubre, H.; Ricordel, C.; Ropert, S.; Janicot, H.; Bernardi, M.; Fournel, P.; Lamy, R.; et al. Efficacy and Safety of Anti–PD-1 Immunotherapy in Patients with Advanced NSCLC With BRAF, HER2, or MET Mutations or RET Translocation: GFPC 01-2018. J. Thorac. Oncol. 2020, 15, 628–636. [Google Scholar] [CrossRef] [PubMed]
- Tanaka, I.; Morise, M.; Miyazawa, A.; Kodama, Y.; Tamiya, Y.; Gen, S.; Matsui, A.; Hase, T.; Hashimoto, N.; Sato, M.; et al. Potential Benefits of Bevacizumab Combined with Platinum-Based Chemotherapy in Advanced Non–Small-Cell Lung Cancer Patients With EGFR Mutation. Clin. Lung Cancer 2020, 21, 273–280. [Google Scholar] [CrossRef]
- Hsu, P.-C.; Huang, C.-Y.; Wang, C.-C.; Kuo, S.C.-H.; Chu, C.-H.; Tung, P.-H.; Huang, A.C.-C.; Wang, C.-L.; Chiu, L.-C.; Fang, Y.-F.; et al. The Combination of Afatinib and Bevacizumab in Untreated EGFR-Mutated Advanced Lung Adenocarcinoma: A Multicenter Observational Study. Pharmaceuticals 2020, 13, 331. [Google Scholar] [CrossRef]
- Barlesi, F.; Vansteenkiste, J.; Spigel, D.; Ishii, H.; Garassino, M.; de Marinis, F.; Özgüroğlu, M.; Szczesna, A.; Polychronis, A.; Uslu, R.; et al. Avelumab versus docetaxel in patients with platinum-treated advanced non-small-cell lung cancer (JAVELIN Lung 200): An open-label, randomised, phase 3 study. Lancet Oncol. 2018, 19, 1468–1479. [Google Scholar] [CrossRef]
- Verschraegen, C.F.; Jerusalem, G.; McClay, E.F.; Iannotti, N.; Redfern, C.H.; Bennouna, J.; Chen, F.L.; Kelly, K.; Mehnert, J.; Morris, J.C.; et al. Efficacy and safety of first-line avelumab in patients with advanced non-small cell lung cancer: Results from a phase Ib cohort of the JAVELIN Solid Tumor study. J. Immunother. Cancer 2020, 8, e001064. [Google Scholar] [CrossRef]
- Alegre, M.-L.; Frauwirth, K.A.; Thompson, C.B. T-cell regulation by CD28 and CTLA-4. Nat. Rev. Immunol. 2001, 1, 220–228. [Google Scholar] [CrossRef]
- Rudd, C.E.; Taylor, A.; Schneider, H. CD28 and CTLA-4 coreceptor expression and signal transduction. Immunol. Rev. 2009, 229, 12–26. [Google Scholar] [CrossRef] [Green Version]
- Verma, N.; Burns, O.S.; Walker, L.S.K.; Sansom, D.M. Immune deficiency and autoimmunity in patients with CTLA-4 (CD152) mutations. Clin. Exp. Immunol. 2017, 190, 1–7. [Google Scholar] [CrossRef] [Green Version]
- Yang, L.; Wang, G.; Xia, H. Molecular mechanism for impaired suppressive function of Tregs in autoimmune diseases: A summary of cell-intrinsic and cell-extrinsic factors. J. Cell. Mol. Med. 2020, 24, 11056–11063. [Google Scholar] [CrossRef]
- Chambers, C.A.; Kuhns, M.S.; Egen, J.G.; Allison, J.P. CTLA-4-mediated inhibition in regulation of T cell responses: Mechanisms and manipulation in tumor immunotherapy. Annu. Rev. Immunol. 2001, 19, 565–594. [Google Scholar] [CrossRef] [Green Version]
- Ribas, A.; Wolchok, J.D. Cancer immunotherapy using checkpoint blockade. Science 2018, 359, 1350–1355. [Google Scholar] [CrossRef] [Green Version]
- Leach, D.R.; Krummel, M.F.; Allison, J.P. Enhancement of Antitumor Immunity by CTLA-4 Blockade. Science 1996, 271, 1734–1736. [Google Scholar] [CrossRef] [Green Version]
- Hodi, F.S.; Mihm, M.C.; Soiffer, R.J.; Haluska, F.G.; Butler, M.; Seiden, M.V.; Davis, T.; Henry-Spires, R.; MacRae, S.; Willman, A.; et al. Biologic activity of cytotoxic T lymphocyte-associated antigen 4 antibody blockade in previously vaccinated metastatic melanoma and ovarian carcinoma patients. Proc. Natl. Acad. Sci. USA 2003, 100, 4712–4717. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Goldman, J.W.; Dowlati, A.; Antonia, S.J.; Nemunaitis, J.J.; Butler, M.O.; Segal, N.H.; Smith, P.A.; Weiss, J.; Zandberg, D.P.; Xiao, F.; et al. Preliminary efficacy of durvalumab plus tremelimumab in platinum-refractory/resistant ED-SCLC from arm A of the phase II BALTIC study. Ann. Oncol. 2018, 29, 596–602. [Google Scholar]
- Ribas, A. Clinical Development of the Anti–CTLA-4 Antibody Tremelimumab. Semin. Oncol. 2010, 37, 450–454. [Google Scholar] [CrossRef] [PubMed]
- Hodi, F.S.; O’Day, S.J.; McDermott, D.F.; Weber, R.W.; Sosman, J.A.; Haanen, J.B.; Gonzalez, R.; Robert, C.; Schadendorf, D.; Hassel, J.C.; et al. Improved Survival with Ipilimumab in Patients with Metastatic Melanoma. N. Engl. J. Med. 2010, 363, 711–723. [Google Scholar] [CrossRef] [PubMed]
- Robert, C.; Thomas, L.; Bondarenko, I.; O’Day, S.; Weber, J.; Garbe, C.; Lebbe, C.; Baurain, J.-F.; Testori, A.; Grob, J.-J.; et al. Ipilimumab plus Dacarbazine for Previously Untreated Metastatic Melanoma. N. Engl. J. Med. 2011, 364, 2517–2526. [Google Scholar] [CrossRef] [Green Version]
- Motzer, R.J.; Escudier, B.; McDermott, D.F.; George, S.; Hammers, H.J.; Srinivas, S.; Tykodi, S.S.; Sosman, J.A.; Procopio, G.; Plimack, E.R.; et al. Nivolumab versus Everolimus in Advanced Renal-Cell Carcinoma. N. Engl. J. Med. 2015, 373, 1803–1813. [Google Scholar] [CrossRef]
- Hammers, H.J.; Plimack, E.R.; Infante, J.R.; Rini, B.I.; McDermott, D.F.; Lewis, L.D.; Voss, M.H.; Sharma, P.; Pal, S.K.; Razak, A.R.A.; et al. Safety and Efficacy of Nivolumab in Combination with Ipilimumab in Metastatic Renal Cell Carcinoma: The CheckMate 016 Study. J. Clin. Oncol. 2017, 35, 3851–3858. [Google Scholar] [CrossRef] [Green Version]
- Overman, M.J.; McDermott, R.; Leach, J.L.; Lonardi, S.; Lenz, H.-J.; Morse, A.M.; Desai, J.; Hill, A.; Axelson, M.; Moss, A.R.; et al. Nivolumab in patients with metastatic DNA mismatch repair-deficient or microsatellite instability-high colorectal cancer (CheckMate 142): An open-label, multicentre, phase 2 study. Lancet Oncol. 2017, 18, 1182–1191. [Google Scholar] [CrossRef]
- Baas, P.; Scherpereel, A.; Nowak, A.K.; Fujimoto, N.; Peters, S.; Tsao, A.S.; Mansfield, A.S.; Popat, S.; Jahan, T.; Antonia, S.; et al. First-line nivolumab plus ipilimumab in unresectable malignant pleural mesothelioma (CheckMate 743): A multicentre, randomised, open-label, phase 3 trial. Lancet 2021, 397, 375–386. [Google Scholar] [CrossRef]
- Reck, M.; Luft, A.; Szczesna, A.; Havel, L.; Kim, S.W.; Akerley, W.; Pietanza, M.C.; Wu, Y.L.; Zielinski, C.; Thomas, M.; et al. Phase III Randomized Trial of Ipilimumab Plus Etoposide and Platinum Versus Placebo Plus Etoposide and Platinum in Extensive-Stage Small-Cell Lung Cancer. J. Clin. Oncol. 2016, 34, 3740–3748. [Google Scholar] [CrossRef] [PubMed]
- Calles, A.; Aguado, G.; Sandoval, C.; Álvarez, R. The role of immunotherapy in small cell lung cancer. Clin. Transl. Oncol. 2019, 21, 961–976. [Google Scholar] [CrossRef]
- Spigel, D.; Vicente, D.; Ciuleanu, T.; Gettinger, S.; Peters, S.; Horn, L.; Audigier-Valette, C.; Aranda, N.P.; Juan-Vidal, O.; Cheng, Y.; et al. Second-line nivolumab in relapsed small-cell lung cancer: CheckMate 331. Ann. Oncol. 2021, 32, 631–641. [Google Scholar] [CrossRef]
- Owonikoko, T.K.; Park, K.; Govindan, R.; Ready, N.; Reck, M.; Peters, S.; Dakhil, S.R.; Navarro, A.; Rodríguez-Cid, J.; Schenker, M.; et al. Nivolumab and Ipilimumab as Maintenance Therapy in Extensive-Disease Small-Cell Lung Cancer: CheckMate 451. J. Clin. Oncol. 2021, 39, 1349–1359. [Google Scholar] [CrossRef] [PubMed]
- Hellmann, M.D.; Rizvi, A.N.; Goldman, J.W.; Gettinger, S.N.; Borghaei, H.; Brahmer, J.R.; Ready, E.N.; Gerber, E.D.; Chow, L.Q.; Juergens, A.R.; et al. Nivolumab plus ipilimumab as first-line treatment for advanced non-small-cell lung cancer (CheckMate 012): Results of an open-label, phase 1, multicohort study. Lancet Oncol. 2017, 18, 31–41. [Google Scholar] [CrossRef] [Green Version]
- Hellmann, M.D.; Ciuleanu, T.-E.; Pluzanski, A.; Lee, J.S.; Otterson, G.A.; Audigier-Valette, C.; Minenza, E.; Linardou, H.; Burgers, S.; Salman, P.; et al. Nivolumab plus Ipilimumab in Lung Cancer with a High Tumor Mutational Burden. N. Engl. J. Med. 2018, 378, 2093–2104. [Google Scholar] [CrossRef]
- Gubens, M.A.; Sequist, L.V.; Stevenson, J.P.; Powell, S.F.; Villaruz, L.C.; Gadgeel, S.M.; Langer, C.J.; Patnaik, A.; Borghaei, H.; Jalal, S.I.; et al. Pembrolizumab in combination with ipilimumab as second-line or later therapy for advanced non–small-cell lung cancer: KEYNOTE-021 cohorts D and H. Lung Cancer 2019, 130, 59–66. [Google Scholar] [CrossRef] [Green Version]
- Goldman, J.W.; Dvorkin, M.; Chen, Y.; Reinmuth, N.; Hotta, K.; Trukhin, D.; Statsenko, G.; Hochmair, M.J.; Özgüroğlu, M.; Ji, J.H.; et al. CASPIAN investigators. Durvalumab, with or without tremelimumab, plus platinum-etoposide versus plati-num-etoposide alone in first-line treatment of extensive-stage small-cell lung cancer (CASPIAN): Updated results from a ran-domised, controlled, open-label, phase 3 trial. Lancet Oncol. 2021, 22, 51–65. [Google Scholar]
- Planchard, D.; Reinmuth, N.; Orlov, S.; Fischer, J.; Sugawara, S.; Mandziuk, S.; Marquez-Medina, D.; Novello, S.; Takeda, Y.; Soo, R.; et al. ARCTIC: Durvalumab with or without tremelimumab as third-line or later treatment of metastatic non-small-cell lung cancer. Ann. Oncol. 2020, 31, 609–618. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Rizvi, N.A.; Cho, B.C.; Reinmuth, N.; Lee, K.H.; Luft, A.; Ahn, M.J.; van den Heuvel, M.M.; Cobo, M.; Vicente, D.; Smolin, A.; et al. Durvalumab with or Without Tremelimumab vs Standard Chemotherapy in First-line Treatment of Metastatic Non-Small Cell Lung Cancer: The MYSTIC Phase 3 Randomized Clinical Trial. JAMA Oncol. 2020, 6, 661–674. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Suh, J.W.; Park, S.Y.; Lee, C.Y.; Lee, J.G.; Kim, D.J.; Paik, H.C.; Chung, K.Y. Feasibility and surgical outcomes of video-assisted thoracoscopic pulmonary resection in patients with advanced-stage lung cancer after neoadjuvant chemoradiotherapy. Thorac. Cancer 2019, 10, 1241–1247. [Google Scholar] [CrossRef] [PubMed]
- Hsu, P.C.; Chang, J.W.; Wang, C.C.; Wu, C.T.; Lin, Y.C.; Wang, C.L.; Lin, T.Y.; Li, S.H.; Wu, Y.C.; Kuo, S.C.; et al. Oral vi-norelbine plus cisplatin with concomitant radiotherapy as induction therapy for stage III non-small cell lung cancer: Results of a single-arm prospective cohort study. Thorac Cancer. 2019, 10, 1683–1691. [Google Scholar] [CrossRef]
- Cascone, T.; Hamdi, H.; Zhang, F.; Poteete, A.; Li, L.; Hudgens, C.W.; Williams, L.J.; Wu, Q.; Gudikote, J.; Peng, W.; et al. Abstract 1719: Superior efficacy of neoadjuvant compared to adjuvant immune checkpoint blockade in non-small cell lung cancer. Immunology 2018, 78, 1719. [Google Scholar] [CrossRef]
- Uprety, D.; Mandrekar, S.J.; Wigle, D.; Roden, A.C.; Adjei, A.A. Neoadjuvant Immunotherapy for NSCLC: Current Concepts and Future Approaches. J. Thorac. Oncol. 2020, 15, 1281–1297. [Google Scholar] [CrossRef]
- Forde, P.M.; Chaft, J.E.; Smith, K.N.; Anagnostou, V.; Cottrell, T.R.; Hellmann, M.D.; Zahurak, M.; Yang, S.C.; Jones, D.R.; Bro derick, S.; et al. Neoadjuvant PD-1 Blockade in Resectable Lung Cancer. N. Engl. J. Med. 2018, 378, 1976–1986. [Google Scholar] [CrossRef]
- Bersanelli, M.; Tiseo, M.; Banna, G.L. Nivolumab plus Ipilimumab in Non-Small-Cell Lung Cancer. N. Engl. J. Med. 2020, 382, 874–875. [Google Scholar]
- Reuss, E.J.; Anagnostou, V.; Cottrell, T.R.; Smith, K.N.; Verde, F.; Zahurak, M.; Lanis, M.; Murray, J.C.; Chan, H.Y.; McCarthy, C.; et al. Neoadjuvant nivolumab plus ipilimumab in resectable non-small cell lung cancer. J. Immunother. Cancer 2020, 8, e001282. [Google Scholar] [CrossRef] [PubMed]
- Jia, X.-H.; Xu, H.; Geng, L.-Y.; Jiao, M.; Wang, W.-J.; Jiang, L.-L.; Guo, H. Efficacy and safety of neoadjuvant immunotherapy in resectable nonsmall cell lung cancer: A meta-analysis. Lung Cancer 2020, 147, 143–153. [Google Scholar] [CrossRef] [PubMed]
- Cascone, T.; William, W.N., Jr.; Weissferdt, A.; Leung, C.H.; Lin, H.Y.; Pataer, A.; Godoy, M.C.B.; Carter, B.W.; Federico, L.; Reuben, A.; et al. Neoadjuvant nivolumab or nivolumab plus ipilimumab in operable non-small cell lung cancer: The phase 2 randomized NEOSTAR trial. Nat. Med. 2021, 27, 504–514. [Google Scholar] [CrossRef]
- Beatty, G.L.; Gladney, W.L. Immune Escape Mechanisms as a Guide for Cancer Immunotherapy. Clin. Cancer Res. 2015, 21, 687–692. [Google Scholar] [CrossRef] [Green Version]
- Gotwals, P.; Cameron, S.; Cipolletta, D.; Cremasco, V.; Crystal, A.; Hewes, B.; Mueller, B.; Quaratino, S.; Sabatos-Peyton, C.; Petruzzelli, S.C.A.C.B.H.S.Q.L.; et al. Prospects for combining targeted and conventional cancer therapy with immunotherapy. Nat. Rev. Cancer 2017, 17, 286–301. [Google Scholar] [CrossRef] [PubMed]
- Galon, J.; Bruni, D. Approaches to treat immune hot, altered and cold tumours with combination immunotherapies. Nat. Rev. Drug Discov. 2019, 18, 197–218. [Google Scholar] [CrossRef]
- Provencio, M.; Nadal, E.; Insa, A.; García-Campelo, M.R.; Casal-Rubio, J.; Dómine, M.; Majem, M.; Rodríguez-Abreu, D.; Martínez-Martí, A.; Carpeño, J.D.C.; et al. Neoadjuvant chemotherapy and nivolumab in resectable non-small-cell lung cancer (NADIM): An open-label, multicentre, single-arm, phase 2 trial. Lancet Oncol. 2020, 21, 1413–1422. [Google Scholar] [CrossRef]
- Shu, A.C.; Gainor, J.F.; Awad, M.M.; Chiuzan, C.; Grigg, C.M.; Pabani, A.; Garofano, R.F.; Stoopler, M.B.; Cheng, S.K.; White, A.; et al. Neoadjuvant atezolizumab and chemotherapy in patients with resectable non-small-cell lung cancer: An open-label, multicentre, single-arm, phase 2 trial. Lancet Oncol. 2020, 21, 786–795. [Google Scholar] [CrossRef]
- Kris, M.G.; Faivre-Finn, C.; Kordbacheh, T.; Chaft, J.; Luo, J.; Tsao, A.; Swisher, S. Making Checkpoint Inhibitors Part of Treat ment of Patients with Locally Advanced Lung Cancers: The Time Is Now. Am. Soc. Clin. Oncol. Educ. Book 2020, 40, 1–12. [Google Scholar]
- Hopstaken, J.S.; de Ruiter, J.C.; Damhuis, R.A.M.; de Langen, A.J.; van Diessen, J.N.A.; Klomp, H.M.; Klompenhouwer, E.G.; Hartemink, K.J. Stage I non-small cell lung cancer: Treatment modalities, Dutch daily practice and future perspectives. Cancer Treat. Res. Commun. 2021, 28, 100404. [Google Scholar] [CrossRef]
- Belluomini, L.; Fiorica, F.; Frassoldati, A. Immune Checkpoint Inhibitors and Radiotherapy in NSCLC Patients: Not Just a Fluke. Oncol. Ther. 2019, 7, 83–91. [Google Scholar] [CrossRef] [Green Version]
- Ngwa, W.; Irabor, O.C.; Schoenfeld, J.D.; Hesser, J.; Demaria, S.; Formenti, S.C. Using immunotherapy to boost the ab-scopal effect. Nat. Rev. Cancer 2018, 18, 313–322. [Google Scholar] [CrossRef] [PubMed]
- Besse, B.; Adam, J.; Cozic, N.; Chaput-Gras, N.; Planchard, D.; Mezquita, L.; Masip, J.R.; Lavaud, P.; Naltet, C.; Gazzah, A.; et al. 1215O—SC Neoadjuvant atezolizumab (A) for resectable non-small cell lung cancer (NSCLC): Results from the phase II PRINCEPS trial. Ann. Oncol. 2020, 31, 794–795. [Google Scholar] [CrossRef]
- Gao, S.; Li, N.; Gao, S.; Xue, Q.; Ying, J.; Wang, S.; Tao, X.; Zhao, J.; Mao, Y.; Wang, B.; et al. Neoadjuvant PD-1 inhibitor (Sintilimab) in NSCLC. J. Thorac. Oncol. 2020, 15, 816–826. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Eichhorn, F.; Klotz, L.V.; Bischoff, H.; Thomas, M.; Lasitschka, F.; Winter, H.; Hoffmann, H.; Eichhorn, M.E. Neoadjuvant anti-programmed Death-1 immunotherapy by Pembrolizumab in resectable nodal positive stage II/IIIa non-small-cell lung cancer (NSCLC): The NEOMUN trial. BMC Cancer 2019, 19, 413. [Google Scholar] [CrossRef] [PubMed]
- Wislez, M.; Mazieres, J.; Lavole, A.; Zalcman, G.; Carre, O.; Egenod, T.; Caliandro, R.; Gervais, R.; Jeannin, G.; Molinier, O.; et al. 1214O Neoadjuvant durvalumab in resectable non-small cell lung cancer (NSCLC): Preliminary results from a multicenter study (IFCT-1601 IONESCO). Ann. Oncol. 2020, 31, 794. [Google Scholar] [CrossRef]
- Hong, M.; Ahn, B.; Kim, H.; Lim, S.; Lee, S.; Park, S.; Lee, C.; Lee, J.; Kim, D.; Yoon, H.; et al. FP03.02 Interim Analysis of Neoadjuvant Chemoradiotherapy and Durvalumab for Potentially Resectable Stage III Non-Small Cell Lung Cancer (NSCLC). J. Thorac. Oncol. 2021, 16, 194–195. [Google Scholar] [CrossRef]
- Felip, E.; Brahmer, J.; Broderick, S.S.; Swanson, S.; Awad, M.; Mitsudomi, T.; Girard, N.; Kerr, K.; Spicer, J.; Cai, J.; et al. P2.16-03 CheckMate 816: A Phase 3 Trial of Neoadjuvant Nivolumab Plus Ipilimumab or Chemotherapy vs Chemotherapy in Early-Stage NSCLC. J. Thorac. Oncol. 2018, 13, 831–832, ISSN 1556-0864. [Google Scholar] [CrossRef] [Green Version]
- Peters, S.; Kim, A.; Solomon, B.; Gandara, D.; Dziadziuszko, R.; Brunelli, A.; Garassino, M.; Reck, M.; Wang, L.; To, I.; et al. IMpower030: Phase III study evaluating neoadjuvant treatment of resectable stage II-IIIB non-small cell lung cancer (NSCLC) with atezolizumab (atezo) + chemotherapy. Ann. Oncol. 2019, 30, 30. [Google Scholar] [CrossRef]
- Heymach, J.; Taube, J.; Mitsudomi, T.; Harpole, D.; Aperghis, M.; Trani, L.; Powell, M.; Dennis, P.; Reck, M. P1.18-02 The AEGEAN Phase 3 Trial of Neoadjuvant/Adjuvant Durvalumab in Patients with Resectable Stage II/III NSCLC. J. Thorac. Oncol. 2019, 14, 625–626. [Google Scholar] [CrossRef]
- Salazar, M.C.; Rosen, J.E.; Wang, Z.; Arnold, B.N.; Thomas, D.C.; Herbst, R.S.; Kim, A.W.; Detterbeck, F.C.; Blasberg, J.D.; Boffa, D.J. Association of Delayed Adjuvant Chemotherapy with Survival After Lung Cancer Surgery. JAMA Oncol. 2017, 3, 610–619. [Google Scholar] [CrossRef] [PubMed]
- Bai, R.; Li, L.; Chen, X.; Chen, N.; Song, W.; Cui, J. Neoadjuvant and Adjuvant Immunotherapy: Opening New Horizons for Patients with Early-Stage Non-small Cell Lung Cancer. Front. Oncol. 2020, 10, 575472. [Google Scholar] [CrossRef]
- Battiloro, C.; Della Gravara, L.; Rocco, D.; Gridelli, C. What pharmacotherapeutics should one use for early stage non-small cell lung cancer? Expert Opin. Pharmacother. 2018, 19, 1403–1406. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Pirker, R.; Filipits, M. Adjuvant Therapy in Patients with Completely Resected Non–small-cell Lung Cancer: Current Status and Perspectives. Clin. Lung Cancer 2019, 20, 1–6. [Google Scholar] [CrossRef]
- Gagliasso, M.; Migliaretti, G.; Ardissone, F. Assessing the prognostic impact of the International Association for the Study of Lung Cancer proposed definitions of complete, uncertain, and incomplete resection in non-small cell lung cancer surgery. Lung Cancer 2017, 111, 124–130. [Google Scholar] [CrossRef] [PubMed]
- Califano, R.; Karamouzis, M.; Banerjee, S.; de Azambuja, E.; Guarneri, V.; Hutka, M.; Jordan, K.; Kamposioras, K.; Martinelli, E.; Corral, J.; et al. Use of adjuvant chemotherapy (CT) and radiotherapy (RT) in incompletely resected (R1) early stage Non-Small Cell Lung Cancer (NSCLC): A European survey conducted by the European Society for Medical Oncology (ESMO) Young Oncologists Committee. Lung Cancer 2014, 85, 74–80. [Google Scholar] [CrossRef] [PubMed]
- Jou, J.; Harrington, K.J.; Zocca, M.-B.; Ehrnrooth, E.; Cohen, E.E. The Changing Landscape of Therapeutic Cancer Vaccines—Novel Platforms and Neoantigen Identification. Clin. Cancer Res. 2021, 27, 689–703. [Google Scholar] [CrossRef]
- Buonaguro, L.; Tagliamonte, M. Selecting Target Antigens for Cancer Vaccine Development. Vaccines 2020, 8, 615. [Google Scholar] [CrossRef]
- Cheever, M.A.; Higano, C.S. PROVENGE (Sipuleucel-T) in Prostate Cancer: The First FDA-Approved Therapeutic Cancer Vaccine. Clin. Cancer Res. 2011, 17, 3520–3526. [Google Scholar] [CrossRef] [Green Version]
- Andtbacka, R.H.; Kaufman, H.L.; Collichio, F.; Amatruda, T.; Senzer, N.; Chesney, J.; Delman, K.A.; Spitler, L.E.; Puzanov, I.; Agarwala, S.S.; et al. Talimogene Laherparepvec Improves Durable Response Rate in Patients with Advanced Melanoma. J. Clin. Oncol. 2015, 33, 2780–2788. [Google Scholar] [CrossRef]
- Finn, O.J. The dawn of vaccines for cancer prevention. Nat. Rev. Immunol. 2018, 18, 183–194. [Google Scholar] [CrossRef]
- Mougel, A.; Terme, M.; Tanchot, C. Therapeutic Cancer Vaccine and Combinations with Antiangiogenic Therapies and Im mune Checkpoint Blockade. Front. Immunol. 2019, 10, 467. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Baghban, R.; Roshangar, L.; Jahanban-Esfahlan, R.; Seidi, K.; Ebrahimi-Kalan, A.; Jaymand, M.; Kolahian, S.; Javaheri, T.; Zare, P. Tumor microenvironment complexity and therapeutic implications at a glance. Cell Commun. Signal. 2020, 18, 1–19. [Google Scholar] [CrossRef] [Green Version]
- De Looff, M.; De Jong, S.; Kruyt, F.A.E. Multiple Interactions Between Cancer Cells and the Tumor Microenvironment Modulate TRAIL Signaling: Implications for TRAIL Receptor Targeted Therapy. Front. Immunol. 2019, 10, 1530. [Google Scholar] [CrossRef] [Green Version]
- Labani-Motlagh, A.; Ashja-Mahdavi, M.; Loskog, A. The Tumor Microenvironment: A Milieu Hindering and Obstructing Antitumor Immune Responses. Front. Immunol. 2020, 11, 940. [Google Scholar] [CrossRef]
- Lorenzo-Luaces, P.; Sanchez, L.; Saavedra, D.; Crombet, T.; Van Der Elst, W.; Alonso, A.; Molenberghs, G.; Lage, A. Identifying predictive biomarkers of CIMAvaxEGF success in non–small cell lung cancer patients. BMC Cancer 2020, 20, 1–8. [Google Scholar] [CrossRef]
- Rodriguez, P.C.; Popa, X.; Martínez, O.; Mendoza, S.; Santiesteban, E.; Crespo, T.; Amador, R.M.; Fleytas, R.; Acosta, S.C.; Otero, Y.; et al. A Phase III Clinical Trial of the Epidermal Growth Factor Vaccine CIMAvax-EGF as Switch Maintenance Therapy in Advanced Non-Small Cell Lung Cancer Patients. Clin. Cancer Res. 2016, 22, 3782–3790. [Google Scholar] [CrossRef] [Green Version]
- Hirschowitz, E.A.; Mullins, A.; Prajapati, D.; Baeker, T.; Kloecker, G.; Foody, T.; Damron, K.; Love, C.; Yannelli, J.R. Pilot Study of 1650-G: A Simplified Cellular Vaccine for Lung Cancer. J. Thorac. Oncol. 2011, 6, 169–173. [Google Scholar] [CrossRef] [Green Version]
- Hirschowitz, E.A.; Foody, T.; Hidalgo, G.E.; Yannelli, J.R. Immunization of NSCLC patients with antigen-pulsed im-mature autologous dendritic cells. Lung Cancer 2007, 57, 365–372. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Vansteenkiste, J.; Zielinski, M.; Linder, A.; Dahabreh, J.; Gonzalez, E.E.; Malinowski, W.; Lopez-Brea, M.; Vanakesa, T.; Jassem, J.; Kalofonos, H.; et al. Adjuvant MAGE-A3 immunotherapy in resected non-small-cell lung cancer: Phase II ran-domized study results. J. Clin. Oncol. 2013, 31, 2396–2403. [Google Scholar] [CrossRef] [PubMed]
- Aurisicchio, L.; Fridman, A.; Mauro, D.; Sheloditna, R.; Chiappori, A.; Bagchi, A.; Ciliberto, G. Safety, tolerability and immunogenicity of V934/V935 hTERT vaccination in cancer patients with selected solid tumors: A phase I study. J. Transl. Med. 2020, 18, 1–8. [Google Scholar] [CrossRef] [Green Version]
- Zhao, J.; Chen, Y.; Ding, Z.-Y.; Liu, J.-Y. Safety and Efficacy of Therapeutic Cancer Vaccines Alone or in Combination with Immune Checkpoint Inhibitors in Cancer Treatment. Front. Pharmacol. 2019, 10, 1184. [Google Scholar] [CrossRef]
- Cuzzubbo, S.; Mangsbo, S.; Nagarajan, D.; Habra, K.; Pockley, A.G.; McArdle, S.E.B. Cancer Vaccines: Adjuvant Potency, Importance of Age, Lifestyle, and Treatments. Front. Immunol. 2021, 11, 615240. [Google Scholar] [CrossRef] [PubMed]
- Tran, T.; Blanc, C.; Granier, C.; Saldmann, A.; Tanchot, C.; Tartour, E. Therapeutic cancer vaccine: Building the future from lessons of the past. Semin. Immunopathol. 2019, 41, 69–85. [Google Scholar] [CrossRef] [PubMed]
- Carter, B.W.; Bhosale, P.R.; Yang, W.T. Immunotherapy and the role of imaging. Cancer 2018, 124, 2906–2922. [Google Scholar] [CrossRef] [PubMed]
- Nishino, M.; Hatabu, H.; Hodi, F.S. Imaging of Cancer Immunotherapy: Current Approaches and Future Directions. Radiology 2019, 290, 9–22. [Google Scholar] [CrossRef]
- Wei, H.; Jiang, H.; Song, B. Role of medical imaging for immune checkpoint blockade therapy: From response assessment to prognosis prediction. Cancer Med. 2019, 8, 5399–5413. [Google Scholar] [CrossRef] [PubMed]
- Indini, A.; Rijavec, E.; Grossi, F. Circulating Biomarkers of Response and Toxicity of Immunotherapy in Advanced Non-Small Cell Lung Cancer (NSCLC): A Comprehensive Review. Cancers 2021, 13, 1794. [Google Scholar] [CrossRef]
- You, W.; Shang, B.; Sun, J.; Liu, X.; Su, L.; Jiang, S. Mechanistic insight of predictive biomarkers for antitumor PD-1/PD-L1 blockade: A paradigm shift towards immunome evaluation (Review). Oncol. Rep. 2020, 44, 424–437. [Google Scholar] [CrossRef]
- Ahern, E.; Solomon, B.J.; Hui, R.; Pavlakis, N.; O’Byrne, K.; Hughes, B.G.M. Neoadjuvant immunotherapy for non-small cell lung cancer: Right drugs, right patient, right time? J. Immunother. Cancer 2021, 9, e002248. [Google Scholar] [CrossRef]
- Choi, Y.J.; Kim, T.; Kim, E.Y.; Lee, S.H.; Kwon, D.S.; Chang, Y.S. Prediction model for hyperprogressive disease in non-small cell lung cancer treated with immune checkpoint inhibitors. Thorac. Cancer 2020, 11, 2793–2803. [Google Scholar] [CrossRef]
- Kim, J.Y.; Lee, K.H.; Kang, J.; Borcoman, E.; Saada-Bouzid, E.; Kronbichler, A.; Hong, S.H.; de Rezende, L.F.M.; Ogino, S.; Keum, N.; et al. Hyperprogressive Disease during Anti-PD-1 (PDCD1)/PD-L1 (CD274) Therapy: A Systematic Review and Meta-Analysis. Cancers 2019, 11, 1699. [Google Scholar] [CrossRef]
- Chen, Y.; Hu, J.; Bu, F.; Zhang, H.; Fei, K.; Zhang, P. Clinical characteristics of hyperprogressive disease in NSCLC after treatment with immune checkpoint inhibitor: A systematic review and meta-analysis. BMC Cancer 2020, 20, 1–9. [Google Scholar] [CrossRef] [PubMed]
- Zhang, L.; Bai, L.; Liu, X.; Liu, Y.; Li, S.; Liu, J.; Zhang, S.; Yang, C.; Ren, X.; Cheng, Y. Factors related to rapid progression of non-small cell lung cancer in Chinese patients treated using single-agent immune checkpoint inhibitor treatment. Thorac. Cancer 2020, 11, 1170–1179. [Google Scholar] [CrossRef] [Green Version]
- Lin, C.-Y.; Wu, Y.-M.; Hsieh, M.-H.; Wang, C.-W.; Wu, C.-Y.; Chen, Y.-J.; Fang, Y.-F. Prognostic implication of EGFR gene mutations and histological classification in patients with resected stage I lung adenocarcinoma. PLoS ONE 2017, 12, e0186567. [Google Scholar] [CrossRef] [Green Version]
- Chang, W.-Y.; Wu, Y.-L.; Su, P.-L.; Yang, S.-C.; Lin, C.-C.; Su, W.-C. The impact of EGFR mutations on the incidence and survival of stages I to III NSCLC patients with subsequent brain metastasis. PLoS ONE 2018, 13, e0192161. [Google Scholar] [CrossRef] [PubMed]
- Aredo, J.V.; Mambetsariev, I.; Hellyer, J.A.; Amini, A.; Neal, J.W.; Padda, S.K.; McCoach, C.E.; Riess, J.W.; Cabebe, E.C.; Naidoo, J.; et al. Durvalumab for Stage III EGFR-Mutated NSCLC After Definitive Chemoradiotherapy. J. Thorac. Oncol. 2021, 16, 1030–1041. [Google Scholar] [CrossRef]
- Chan, H.T.; Chin, Y.M.; Low, S.-K. The Roles of Common Variation and Somatic Mutation in Cancer Pharmacogenomics. Oncol. Ther. 2019, 7, 1–32. [Google Scholar] [CrossRef] [PubMed]
- Wang, L.; Wang, W. Safety and efficacy of anaplastic lymphoma kinase tyrosine kinase inhibitors in non-small cell lung cancer (Review). Oncol. Rep. 2020, 45, 13–28. [Google Scholar] [CrossRef]
- Solomon, B.J.; Ahn, J.S.; Barlesi, F.; Dziadziuszko, R.; Nishio, M.; Shaw, A.T.; Bordogna, W.; Meyenberg, C.; Wu, Y.-L. ALINA: A phase III study of alectinib versus chemotherapy as adjuvant therapy in patients with stage IB–IIIA anaplastic lymphoma kinase-positive (ALK+) non-small cell lung cancer (NSCLC). J. Clin. Oncol. 2019, 37, 8569. [Google Scholar] [CrossRef]
- Blank, C.U.; Rozeman, E.A.; Fanchi, L.F.; Sikorska, K.; Van De Wiel, B.; Kvistborg, P.; Krijgsman, O.; Braber, M.V.D.; Philips, D.; Broeks, A.; et al. Neoadjuvant versus adjuvant ipilimumab plus nivolumab in macroscopic stage III melanoma. Nat. Med. 2018, 24, 1655–1661. [Google Scholar] [CrossRef] [PubMed]
- Albain, K.S.; Swann, R.S.; Rusch, V.W.; Turrisi, A.T.; Shepherd, A.F.; Smith, C.; Chen, Y.; Livingston, R.B.; Feins, R.H.; Gandara, D.R.; et al. Radiotherapy plus chemotherapy with or without surgical resection for stage III non-small-cell lung cancer: A phase III randomised controlled trial. Lancet 2009, 374, 379–386. [Google Scholar] [CrossRef] [Green Version]
- Schiavon, M.; Comacchio, G.M.; Mammana, M.; Faccioli, E.; Stocca, F.; Gregori, D.; Lorenzoni, G.; Zuin, A.; Nicotra, S.; Pasello, G.; et al. Lobectomy with artery reconstruction and pneumonectomy for NSCLC: A propensity score weighting study. Ann. Thorac. Surg. 2021. [Google Scholar] [CrossRef]
| Trial Name [Reference] | Histology | PD-L1 Expression | Arm 1 | Arm 2 | Median OS (Months) Arm 1 vs. Arm 2 (HR) |
|---|---|---|---|---|---|
| KEYNOTE-024 [22] | NSCLC | PD-L1 positive (≥50% expression) | Pembrolizumab | Platinum-based chemotherapy | 30.0 vs. 14.2 0.63 |
| KEYNOTE-042 23] | NSCLC | PD-L1 positive (≥1% expression) | Pembrolizumab | Platinum-based chemotherapy | 16.7 vs. 12.1 0.81 |
| KEYNOTE-189 [24] | Non-squamous | Any level | Pembrolizumab + pemetrexed + cisplatin/ carboplatin | Placebo + pemetrexed + cisplatin/ carboplatin | 22.0 vs. 10.7 0.56 |
| KEYNOTE-407 [25] | Squamous | Any level | Pembrolizumab + carboplatin + paclitaxel/nab–paclitaxel | Placebo + carboplatin + paclitaxel/nab–paclitaxel | 17.1 vs. 11.6 0.71 |
| CHECKMATE-227 [26] | NSCLC | Any level | Nivolumab + ipilimumab | Platinum-based chemotherapy + pemetrexed (non-squamous)/ gemcitabine (squamous) | PD-L1 ≥ 1% 17.1 vs. 14.9 0.79 PD-L1 negative 17.2 vs. 12.2 0.62 |
| CHECKMATE 9LA [27] | NSCLC | Any level | Nivolumab + ipilimumab + 2 cycles of platinum-based chemotherapy + pemetrexed (non-squamous)/ paclitaxel (squamous) | Platinum-based + pemetrexed (non-squamous) paclitaxel (squamous) | 15.6 vs. 10.9 0.66 |
| EMPOWER-Lung 1 [28] | NSCLC | PD-L1 positive (≥50% expression) | Cemiplimab | Platinum-based chemotherapy | NR vs. 14.2 0.57 |
| IMpower150 [29,30] | Non-squamous | Any level | Atezolizumab + bevacizumab + carboplatin + Paclitaxel | Bevacizumab+ carboplatin + Paclitaxel | 19.8 vs. 14.9 0.76 |
| IMpower130 [31] | Non-squamous | Any level | Atezolizumab + Carboplatin + nab-paclitaxel | Carboplatin + nab-paclitaxel | 18.6 vs. 13.9 0.79 |
| IMpower110 [32] | NSCLC | PD-L1 positive (≥1% expression) | Atezolizumab | Platinum-based chemotherapy | 20.2 vs. 13.1 0.59 |
| PACIFIC [33,34] | NSCLC | Any level | Durvalumab | Placebo | 47.5 vs. 29.1 0.71 |
| Trial [Reference] | Stage | Number of Patients Recruited | Drugs Used in Neoadjuvant Therapy | Primary Endpoint | MPR (%) |
|---|---|---|---|---|---|
| Forde et al. (NCT02259621) [79] | Stages I-IIIA | 21 | Nivolumab (monotherapy) | Safety and feasibility | 45 |
| NEOSTAR (NCT03158129) [83] | Stages IA-IIIA | 44 | Nivolumab or nivolumab + ipilimumab | MPR | 24 in nivolumab group 50 in nivolumab + ipilimumab group |
| NADIM (NCT03081689) [87] | Stages IIIA | 46 | Nivolumab + carboplatin + paclitaxel | 24-month PFS (77.1%) | 83 |
| Shu et al. (NCT02716038) [88] | Stages II-IIIA | 30 | Atezolizumab + carboplatin + nab-paclitaxel | MPR | 57 |
| LCMC3 (NCT02927301) [78,89] | Stages IB-IIIB | 82 | Atezolizumab (monotherapy) | MPR | 18 |
| Ready et al. (NCT02818920) [89] | Stages IB-IIIB | 25 | Pembrolizumab (monotherapy) | MPR | 28 |
| PRINCEPS (NCT02994576) [93] | Stages IA (>2 cm)-IIIA | 30 | Atezolizumab (monotherapy) | Toxicity | Not available |
| Gao et al. (ChiCTR-OIC-17013726) [94] | Stages IA-IIIB | 40 | Sintilimab (monotherapy) | MPR | 40.5 |
| Trial [Reference] | Phase | Stage | Number of Patients Recruited or Target Number | Drugs Used in the Trial | Primary Endpoint |
|---|---|---|---|---|---|
| NEOMUN (NCT03197467) [95] | II | Stages II-IIIA | 30 | Pembrolizumab (monotherapy) | Safety and feasibility |
| IFCT-1601 IONESCO (NCT03030131) [96] | II | Stages IB (>4 cm)-IIIA | 50 | Durvalumab (monotherapy) | Complete surgical resection (R0) |
| ACTS-30 (NCT03694236) [97] | Ib | Resectable Stage IIIA | 14 | Durvalumab + chemoradiotherapy | Safety and feasibility |
| KEYNOTE 617 (NCT03425643) [78] | III | Stages II-IIIB | 786 | Chemotherapy + pembrolizumab/placebo × 4 cycles → surgery → pembrolizumab/placebo × 13 cycles | Event-free survival (EFS) and OS |
| CheckMate 816 (NCT02998528) [98] | III | Stages IB-IIIA | 350 | Chemotherapy + nivolumab × 3 cycles vs. chemotherapy alone × 3 cycles → surgery | EFS and pathological complete response (pCR) |
| IMpower 030 (NCT03456063) [99] | III | Stages II-IIIB | 374 | Chemotherapy + atezolizumab/placebo × 4 cycles → surgery → pembrolizumab/placebo × 16 cycles | MPR, EFS |
| AEGEAN (NCT03800134) [100] | III | Stages IIA-IIIB | 300 | Chemotherapy + durvalumab/placebo × 3 cycles → surgery → durvalumab/placebo × 12 cycles | MPR |
| Trial | Stage | Estimated Enrollment | Treatment Procedure | Primary Endpoint |
|---|---|---|---|---|
| ANVIL (NCT02595944) | Stages IB-IIIA | 903 | Surgery +/− chemotherapy → nivolumab vs. observation | DFS, OS |
| PEARLS (NCT02504372) | Stages IB-IIIA | 1177 | Surgery +/− chemotherapy → pembrolizumab vs. placebo | DFS |
| IMpower010 (NCT02486718) | Stages IB-IIIA | 1280 | Surgery +/− chemotherapy → atezolizumab vs. best supportive care | DFS |
| BR31 (NCT02273375) | Stages IB-IIIA | 1360 | Surgery +/− chemotherapy → durvalumab vs. placebo | DFS |
| Vaccine | Aims and Design | Indications | Intervention or Results | Trial Phase and Status | Clinicaltrials.gov Identifier |
|---|---|---|---|---|---|
| CIMAvax-EGF | Prevention of lung cancer development or recurrence Human recombinant EGF coupled to a carrier protein, recombinant P64K | NSCLC, stage IB to IIIA | Recombinant Human EGF-rP64K/Montanide ISA 51 Vaccine I Loading phase: 0, 2, 4, and 6 weeks, and maintain phase: Q4W in the absence of disease progression or unacceptable toxicity | Early phase I, recruiting | NCT04298606 |
| 1650-G Vaccine | Allogeneic cellular vaccine | NSCLC, stages I and II after completion of initial definitive therapies | Administered intradermally in the thigh at week 0 and week 4 | Phase II, completed; 12 participants | NCT00654030 [96] |
| Tumor vaccine | Neoantigen tumor vaccine | Lung adenocarcinoma, stage IIIA, post radical operation | 5 injections for every 3 days and then 1 injection for every 3 months until recurrence or up to 2 years | Phases I and II, not yet recruiting | NCT03807102 |
| Autologous dendritic cell cancer vaccine | Autologous dendritic cell cancer vaccine | NSCLC, stages I to III | Injection under the skin in the front, upper thigh. Two vaccine injections total, given one month a part. | Phases II, completed, 32 participants | NCT00103116 [97] |
| MCU1 vaccine | MUC1 peptide-Poly-ICLC vaccine | Current and former smokers at high risk for lung cancer. | Subcutaneously at weeks 0, 2, and 10. | Phase II, recruiting | NCT03300817 |
| MUC1 (Mucin1) peptide vaccine | Vaccine + PolyICLC | NSCLC, stages IA to IIIB | Subcutaneously every 3 weeks × 3 | Phases I and II, recruiting | NCT01720836 |
| Autologous tumor cell vaccine | Autologous tumor Lysate-Pulsed Dendritic Cells vaccine | NSCLC, stages IB to IIIA | SubcutaneouslyTwice subcutaneously twice, 4 weeks apart | Phase I, completed | NCT00023985 |
| MIDRIXNEO | Autologous neoantigen-targeted dendritic cell vaccine | NSCLC, considered functionally operable and surgically resectable | Intravenous infusions of MIDRIXNEO-LUNG DCs every 2 weeks, using an intra-patient dose escalation scheme | Phases I and II, recruiting | NCT04078269 |
| DRibble vaccine | Cyclophosphamide with Dribble vaccine alone or with GM-CSF or Imiquimod for adjuvant treatment | NSCLC, stages IIIA or IIIB | Cyclophosphamide is administered as a single dose three days prior to vaccine therapy. | Phase II, completed | NCT01909752 |
| Peptide-pulsed DCs | Mutant p53 peptide-pulsed dendritic cell vaccine | NSCLC, stages IIIA or IIIB with p53 mutation | Four timesIV weekly for 5 weeks. | Phase II, completed | NCT00019929 |
| Monoclonal antibody 11D10/3H1 anti-idiotype vaccine | Combining vaccine therapy with radiation therapy | NSCLC, stages II or IIIA, completely removed in surgery | Intracutaneously once weekly for 3 weeks beginning 2–7 weeks (no later than 49 days) after surgery, and then subcutaneously once monthly for 2 years, regardless of disease progression | Phase II, completed | NCT00006470 |
| GSK 249553 vaccine | Recombinant MAGE-A3 protein combined with an immunostimulant | NSCLC, stages IB or II, complete surgical resection | Intramuscular injection; 5 doses at 3-week intervals and 8 doses at 3-month intervals | Phase II, completed | NCT00290355 [98] |
| GV 1001 | Telomerase peptide vaccine | NSCLC, stages IIIA and IIIB received concurrent chemoradiotherapy | Intradermal | Phase II, completed | NCT00509457 |
| DC vaccines | Tumor neoantigen primed dendritic cell vaccines | NSCLC has undergone a curative resection or ablation | Subcutaneous, at 2–3 week intervals for a total of 3–5 times | Phase I, recruiting | NCT04147078 |
| V934/935 | V934/V935 human telomerase reverse transcriptase (hTERT) vaccination | NSCLC stages I to III | Intramuscular | Phase I, completed | NCT00753415 [99] |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2021 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Chiu, L.-C.; Lin, S.-M.; Lo, Y.-L.; Kuo, S.C.-H.; Yang, C.-T.; Hsu, P.-C. Immunotherapy and Vaccination in Surgically Resectable Non-Small Cell Lung Cancer (NSCLC). Vaccines 2021, 9, 689. https://doi.org/10.3390/vaccines9070689
Chiu L-C, Lin S-M, Lo Y-L, Kuo SC-H, Yang C-T, Hsu P-C. Immunotherapy and Vaccination in Surgically Resectable Non-Small Cell Lung Cancer (NSCLC). Vaccines. 2021; 9(7):689. https://doi.org/10.3390/vaccines9070689
Chicago/Turabian StyleChiu, Li-Chung, Shu-Min Lin, Yu-Lun Lo, Scott Chih-Hsi Kuo, Cheng-Ta Yang, and Ping-Chih Hsu. 2021. "Immunotherapy and Vaccination in Surgically Resectable Non-Small Cell Lung Cancer (NSCLC)" Vaccines 9, no. 7: 689. https://doi.org/10.3390/vaccines9070689
APA StyleChiu, L.-C., Lin, S.-M., Lo, Y.-L., Kuo, S. C.-H., Yang, C.-T., & Hsu, P.-C. (2021). Immunotherapy and Vaccination in Surgically Resectable Non-Small Cell Lung Cancer (NSCLC). Vaccines, 9(7), 689. https://doi.org/10.3390/vaccines9070689







