Austria’s Digital Vaccination Registry: Stakeholder Views and Implications for Governance
Abstract
1. Introduction
2. Materials and Methods
3. Results
3.1. Background
3.1.1. What Are Vaccination Registries?
3.1.2. Context: eHealth & Electronic Health Records in Austria
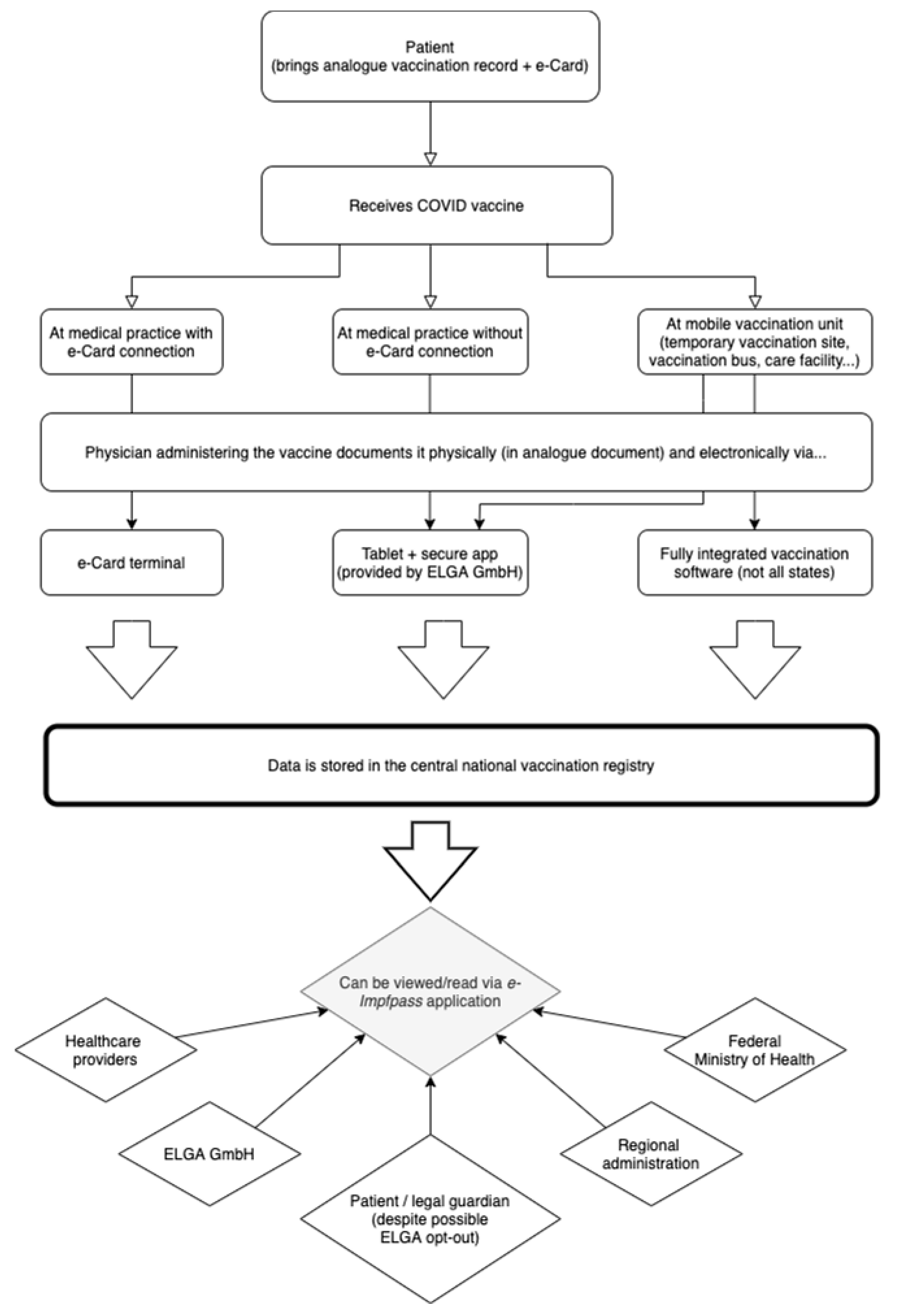
3.1.3. The Austrian e-Impfpass—Digital Vaccination Record: Features and Functions
“That only emerged now during COVID, that we can say, (…) it is mandatory that the vaccine is included in the vaccination registry. For the moment, this only applies to COVID. How it will continue, whether an Opt-Out will be possible in some other way (…) that was definitely a huge point of discussion, which of course accompanied the entire project, and where it came to delays again and again.”—ITV 1.
“And that is, yes and, and, building a national vaccination registry and to say: You can opt out from it, that makes absolutely no sense. But I have also already heard that people don’t want to be vaccinated because of it.”—ITV 6.
3.1.4. The Role of the COVID-19 Pandemic
“[…] and COVID of course, which changed the scope somewhat and added a little pressure, because it probably wouldn’t have called anyone to action whether children between 0 and 6 are included half a year earlier or later, but then, the political pressure was there accordingly and the goals were also pretty clear.”—ITV 6.
“[…] the demand would be in a pandemic to have a real-time vaccination ticker, so to speak, which segment of the population. That’s logical. That is the first thing you know when you start a vaccination campaign: I want to have daily updated numbers so that I can steer things. Also politically. The politicians demand this. And we didn’t have that then.”—ITV 2.
“The pressure is on: we are receiving COVID-vaccines and we will need to document these vaccinations. We have to document them for citizens in a fast way, that’s a matter of patient safety. Because you have two doses, so we have to document the immunization events, we have to document it easily and digitally and we already anticipated, the signals were already very clear during the summer, that the citizens will only be able to go back to their normal lives or do certain things in life only when they can, when we can show that they have been vaccinated.”—ITV 5.
3.2. Unpacking the Value of Data
3.2.1. Data and Data Quality as Political Capital
3.2.2. Administrative Efficiency as a Central Value
“At some point it became clear, if we introduce a national vaccination registry, if all these vaccination registries that have evolved regionally (…) they all primarily have an accounting purpose. And you will recognize again, also back during the pandemic, the accounting purpose. That means that the implementation of a digital registry is always, I’ll say, very simple and politically clear when it comes to money. If it’s just about the epidemiological aspects, the money doesn’t flow.”—ITV 2.
4. Discussion
Supplementary Materials
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Acknowledgments
Conflicts of Interest
References
- Madsen, A.K.; Flyverbom, M.; Hilbert, M.; Ruppert, E. Big Data: Issues for an International Political Sociology of Data Practices: Table 1. Int. Polit. Sociol. 2016, 10, 275–296. [Google Scholar] [CrossRef]
- Mayer-Schönberger, V. Big Data: A Revolution that Will Transform How We Live, Work and Think; Hodder & Stoughton: London, UK, 2013; ISBN 978-1-84854-790-2. [Google Scholar]
- Sadoughi, F.; Khodaveisi, T.; Ahmadi, H. The used theories for the adoption of electronic health record: A systematic literature review. Health Technol. 2019, 9, 383–400. [Google Scholar] [CrossRef]
- Taylor, L. The price of certainty: How the politics of pandemic data demand an ethics of care. Big Data Soc. 2020, 7, 205395172094253. [Google Scholar] [CrossRef]
- European Commission. eHealth Action Plan 2012–2020-Innovative Healthcare for the 21st Century; European Commission: Brussels, Belgium, 2012. [Google Scholar]
- Council of the European Union. Council Recommendation of 7 December 2018 on Strengthened Cooperation against Vaccine-Preventable Diseases; Council of the European Union: Brussels, Belgium, 2018. [Google Scholar]
- Fisher, A. From Diagnosing Under-immunization to Evaluating Health Care Systems. In Governance by Indicators; Oxford University Press: Oxford, UK, 2012; pp. 217–246. ISBN 978-0-19-965824-4. [Google Scholar]
- Pichelstorfer, A.; Paul, K.T. Unpacking the role of metrics in global vaccination governance. Int. Polit. Sociol. 2020, in press. [Google Scholar] [CrossRef]
- Felt, U.; Gugglberger, L.; Mager, A. Shaping the future e-patient. Sci. Technol. Stud. 2009, 22, 24–43. [Google Scholar] [CrossRef]
- Holmberg, C.; Bischof, C.; Bauer, S. Making Predictions: Computing Populations. Sci. Technol. Hum. Values 2013, 38, 398–420. [Google Scholar] [CrossRef]
- Porter, T.M. Trust in Numbers: The Pursuit of Objectivity in Science and Public Life; Princeton Univ. Press: Princeton, NJ, USA, 1995; ISBN 0-691-03776-0. [Google Scholar]
- Hoeyer, K. Data as promise: Reconfiguring Danish public health through personalized medicine. Soc. Stud. Sci. 2019, 49, 531–555. [Google Scholar] [CrossRef]
- Sadowski, J. When data is capital: Datafication, accumulation, and extraction. Big Data Soc. 2019, 6, 205395171882054. [Google Scholar] [CrossRef]
- Jahn, B.; Sroczynski, G.; Bicher, M.; Rippinger, C.; Mühlberger, N.; Santamaria, J.; Urach, C.; Schomaker, M.; Stojkov, I.; Schmid, D.; et al. Targeted COVID-19 Vaccination (TAV-COVID) Considering Limited Vaccination Capacities—An Agent-Based Modeling Evaluation. Vaccines 2021, 9, 434. [Google Scholar] [CrossRef]
- Paul, K.T.; Loer, K. Contemporary vaccination policy in the European Union: Tensions and dilemmas. J. Public Health Policy 2019, 40, 166–179. [Google Scholar] [CrossRef]
- van Lier, A.; Oomen, P.; de Hoogh, P.; Drijfhout, I.; Elsinghorst, B.; Kemmeren, J.; Conyn-van Spaendonck, M.; de Melker, H. Præventis, the immunisation register of the Netherlands: A tool to evaluate the National Immunisation Programme. Eurosurveillance 2012, 17, 20153. [Google Scholar] [CrossRef]
- Robbins, A.; Freeman, P. Optimal disease prevention using vaccination depends on a system. Public Health Rep. 1998, 113, 533–534. [Google Scholar]
- Guttmann, A.; Shulman, R.; Manuel, D. Improving accountability for children’s health: Immunization registries and public reporting of coverage in Canada. Paediatr. Child Health 2011, 16, 16–18. [Google Scholar] [CrossRef][Green Version]
- Gunter, T.D.; Terry, N.P. The Emergence of National Electronic Health Record Architectures in the United States and Australia: Models, Costs, and Questions. J. Med. Internet Res. 2005, 7, e3. [Google Scholar] [CrossRef]
- Dorda, W.; Duftschmid, G.; Gerhold, L.; Gall, W.; Gambal, J. Introducing the electronic health record in Austria. Stud. Health Technol. Inform. 2005, 116, 119–124. [Google Scholar]
- Hoerbst, A.; Kohl, C.D.; Knaup, P.; Ammenwerth, E. Attitudes and behaviors related to the introduction of electronic health records among Austrian and German citizens. Int. J. Med. Inf. 2010, 79, 81–89. [Google Scholar] [CrossRef]
- Herbek, S.; Eisl, H.A.; Hurch, M.; Schator, A.; Sabutsch, S.; Rauchegger, G.; Kollmann, A.; Philippi, T.; Dragon, P.; Seitz, E.; et al. The Electronic Health Record in Austria: A strong network between health care and patients. Eur. Surg. 2012, 44, 155–163. [Google Scholar] [CrossRef]
- Kollmann, A.; Hameed, A.S.; Sabutsch, S.W. Die Entwicklung der e-Medikation als ELGA-Anwendung in Österreich. GMS Med. Inform. Biom. Und Epidemiol. 2017, 13, 1–14. [Google Scholar] [CrossRef]
- Ammenwerth, E.; Duftschmid, G.; Gall, W.; Hackl, W.O.; Hoerbst, A.; Janzek-Hawlat, S.; Jeske, M.; Jung, M.; Woertz, K.; Dorda, W. A nationwide computerized patient medication history: Evaluation of the Austrian pilot project “e-Medikation”. Int. J. Med. Inf. 2014, 83, 655–669. [Google Scholar] [CrossRef]
- Deutsch, E.; Duftschmid, G.; Dorda, W. Critical areas of national electronic health record programs—Is our focus correct? Int. J. Med. Inf. 2010, 79, 211–222. [Google Scholar] [CrossRef]
- Gottweis, H. Die ELGA Debatte in der Öffentlichen Wahrnehmung: Zentrale Ergebnisse einer Fokusgruppenerhebung; LSG Working Paper, Research Platform Life Science Governance; University of Vienna: Vienna, Austria, 2012. [Google Scholar]
- Federal Ministry of Social Affairs, Health, Care and Consumer Protection. Elektronischer Impfpass. Available online: https://www.sozialministerium.at/Themen/Gesundheit/eHealth/Elektronischer-Impfpass.html (accessed on 16 December 2020).
- Federal Ministry of Social Affairs, Health, Care and Consumer Protection. EU Digital COVID Certificates. Available online: https://gruenerpass.gv.at (accessed on 29 September 2021).
- Schmid, D.; Holzmann, H.; Schwarz, K.; Kasper, S.; Kuo, H.-W.; Aberle, S.W.; Redlberger-Fritz, M.; Hautmann, W.; Santibanez, S.; Mankertz, A.; et al. Measles outbreak linked to a minority group in Austria, 2008. Epidemiol. Infect. 2010, 138, 415–425. [Google Scholar] [CrossRef]
- Strauss, R.; Kreidl, P.; Muscat, M.; Coulombier, D.; Mulders, M.; Gijsens, A.; König, C.; Stirling, J.; El Belazi, G.; Muchl, R.; et al. The measles situation in Austria: A rapid risk assessment by an ECDC team and the outcome of an international meeting in Vienna, Austria. Eurosurveillance 2008, 13, 18852. [Google Scholar] [CrossRef]
- ELGA GmbH ELGA. Zahlen-Daten-Fakten. Available online: https://www.elga.gv.at/elga-die-elektronische-gesundheitsakte/zahlen-daten-fakten/ (accessed on 8 June 2021).
- European Centre for Disease Prevention and Control. Immunisation Information Systems in the EU and EEA: Results of a Survey on Implementation and System Characteristics; ECDC Publications Office: Stockholm, Sweden, 2017. [Google Scholar]
- Folkhälsomyndigheten Nationella vaccinationsregistret—Folkhälsomyndigheten. Available online: http://www.folkhalsomyndigheten.se/smittskydd-beredskap/vaccinationer/nationella-vaccinationsregistret/ (accessed on 8 June 2021).
- RIVM Legal Information Rijksvaccinatieprogramma.nl. Available online: https://rijksvaccinatieprogramma.nl/over-het-programma/juridische-informatie (accessed on 8 June 2021).
- Lohninger, T. e-Impfpass-Opt-Out-Möglichkeit Hätte Vertrauen Geschaffen. 2020. Available online: https://epicenter.works/content/e-impfpass-opt-out-moeglichkeit-haette-vertrauen-geschaffen (accessed on 15 August 2021).
- Forgó, N. Über das Teilen von Gesundheitsdaten. 2021. Lecture Held at the University of Vienna. Available online: https://www.postgraduatecenter.at/offene-weiterbildung/offene-weiterbildung/unimind-university-meets-industry/rueckblick/video-lecture-ueber-das-teilen-von-gesundheitsdaten/ (accessed on 10 February 2021).
- Martani, A.; Geneviève, L.D.; Elger, B.; Wangmo, T. “It’s not something you can take in your hands”. Swiss experts’ perspectives on health data ownership: An interview-based study. BMJ Open 2021, 11, e045717. [Google Scholar] [CrossRef]
- Hoeyer, K.; Bauer, S.; Pickersgill, M. Datafication and accountability in public health: Introduction to a special issue. Soc. Stud. Sci. 2019, 49, 459–475. [Google Scholar] [CrossRef]
- Jacobson Vann, J.C.; Jacobson, R.M.; Coyne-Beasley, T.; Asafu-Adjei, J.K.; Szilagyi, P.G. Patient reminder and recall interventions to improve immunization rates. Cochrane Database Syst. Rev. 2018, 18, 1–208. [Google Scholar] [CrossRef]
- Szilagyi, P.G.; Bordley, C.; Vann, J.C.; Chelminski, A.; Kraus, R.M.; Margolis, P.A.; Rodewald, L.E. Effect of Patient Reminder/Recall Interventions on Immunization Rates: A Review. JAMA 2000, 284, 1820. [Google Scholar] [CrossRef]
- Ruppert, E.; Isin, E.; Bigo, D. Data politics. Big Data Soc. 2017, 4, 205395171771774. [Google Scholar] [CrossRef]
- Lupton, D. Digital Health: Critical and Cross-Disciplinary Perspectives, 1st ed.; Routledge: Abingdon, UK; New York, NY, USA, 2018; ISBN 978-1-315-64883-5. [Google Scholar]
- Bester, J.C. Vaccine Refusal and Trust: The Trouble with Coercion and Education and Suggestions for a Cure. J. Bioethical Inq. 2015, 12, 555–559. [Google Scholar] [CrossRef]
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2021 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Paul, K.T.; Janny, A.; Riesinger, K. Austria’s Digital Vaccination Registry: Stakeholder Views and Implications for Governance. Vaccines 2021, 9, 1495. https://doi.org/10.3390/vaccines9121495
Paul KT, Janny A, Riesinger K. Austria’s Digital Vaccination Registry: Stakeholder Views and Implications for Governance. Vaccines. 2021; 9(12):1495. https://doi.org/10.3390/vaccines9121495
Chicago/Turabian StylePaul, Katharina T., Anna Janny, and Katharina Riesinger. 2021. "Austria’s Digital Vaccination Registry: Stakeholder Views and Implications for Governance" Vaccines 9, no. 12: 1495. https://doi.org/10.3390/vaccines9121495
APA StylePaul, K. T., Janny, A., & Riesinger, K. (2021). Austria’s Digital Vaccination Registry: Stakeholder Views and Implications for Governance. Vaccines, 9(12), 1495. https://doi.org/10.3390/vaccines9121495





