Evaluating a Technology-Mediated HPV Vaccination Awareness Intervention: A Controlled, Quasi-Experimental, Mixed Methods Study
Abstract
1. Introduction
2. Materials and Methods
2.1. Study Design and Procedures
2.2. Participant Recruitment and Eligibility
2.3. HPV Vaccination Awareness Intervention
2.4. Control Intervention
2.5. Measures
2.5.1. Sociodemographic Characteristics
2.5.2. HPV Vaccination Knowledge, Attitudes, Beliefs and Behaviors
2.5.3. Intervention Engagement
2.5.4. Treatment Satisfaction
2.5.5. Weekly Reflections
2.6. Statistical Analysis
3. Results
3.1. Sample Characteristics
3.2. HPV Vaccination Knowledge, Attitudes, and Behaviors
3.3. Participants Reported Improvements in HPV Vaccination Knowledge, Attitudes, and Behaviors
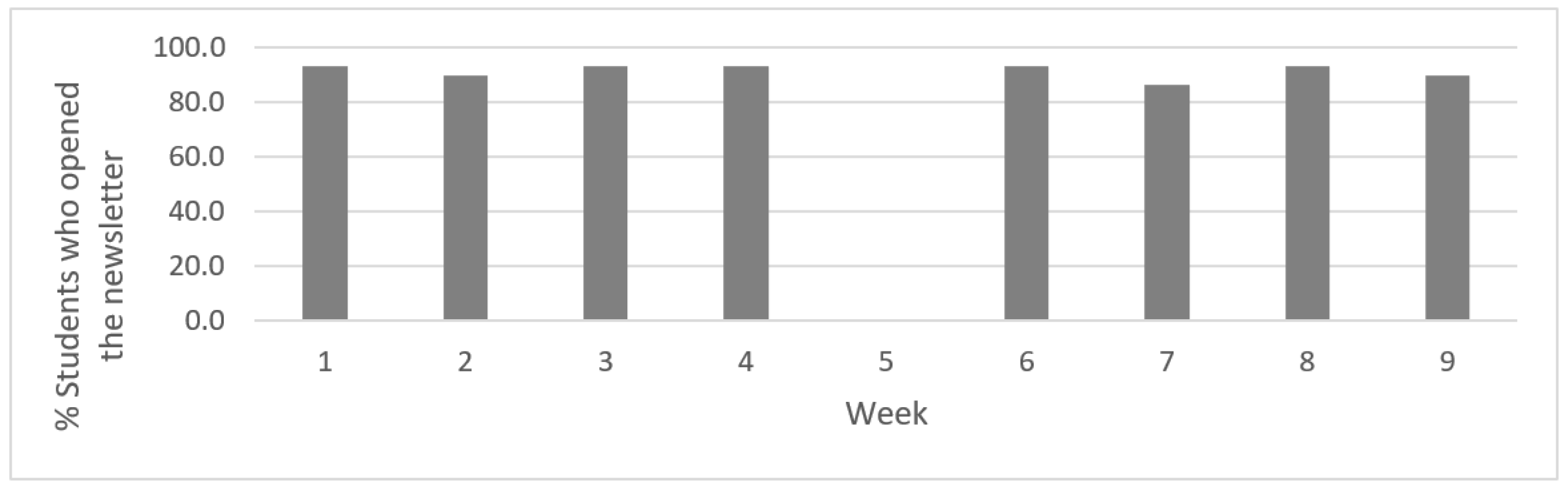
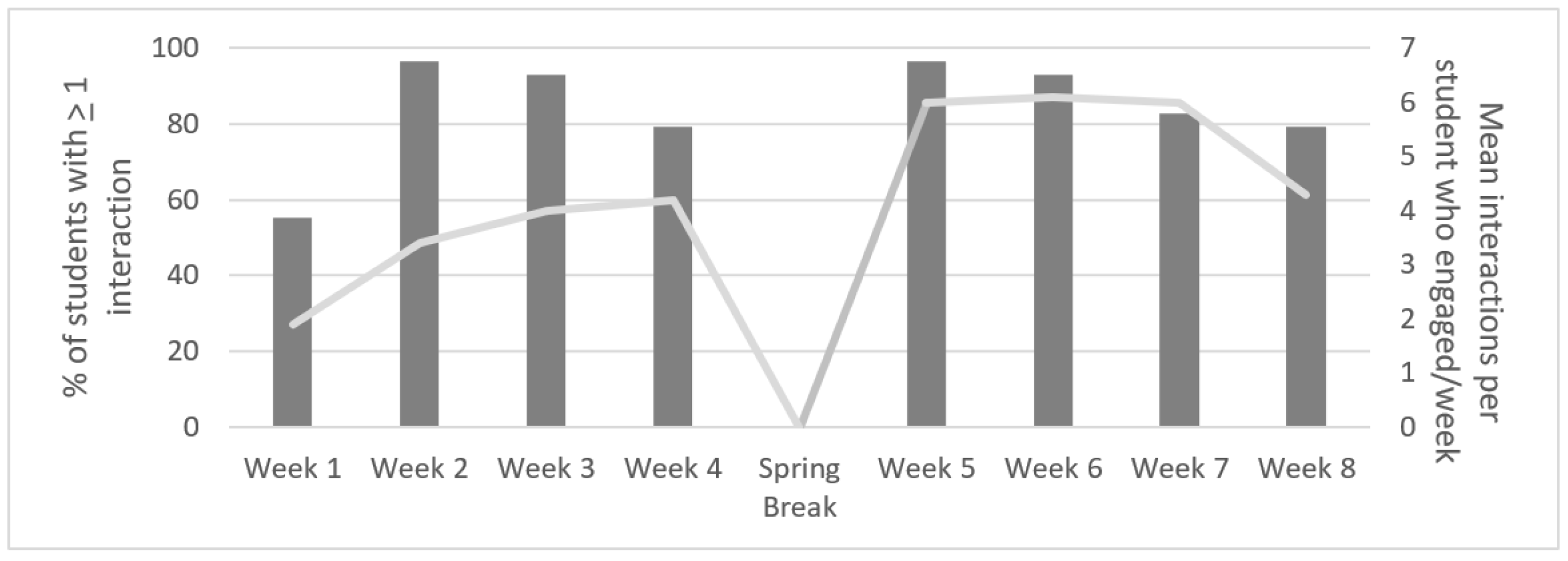
3.4. Intervention Engagement and Treatment Satisfaction
3.5. Participants Reported High Intervention Engagement and Treatment Satisfaction
4. Discussion
4.1. Implications for Practice
4.2. Study Limitations and Strengths
5. Conclusions
Author Contributions
Funding
Acknowledgments
Conflicts of Interest
References
- Markowitz, L.E.; Dunne, E.F.; Saraiya, M.; Chesson, H.W.; Curtis, C.; Robinette, C.; Gee, J.; Bocchini, J.A., Jr.; Unger, E.R.; Centers for Disease Control and Prevention (CDC). Human Papillomavirus Vaccination: Recommendations of the Advisory Committee on Immunization Practices (ACIP). Morb. Mortal. Wkly. Rep. 2014, 63, 1–30. [Google Scholar]
- Centers for Disease Control and Prevention. Young People Account for a Substantial Proportion of New STIs. Division of STD Prevention: Atlanta, GA, USA, National Center for HIV/AIDS, Viral Hepatitis, STD, and TB Prevention; 2015. Available online: https://www.cdc.gov/std/products/infographics.htm (accessed on 14 November 2020).
- Centers for Disease Control and Prevention. The Link between HPV and Cancer; National Center for Chronic Disease Prevention and Health Promotion: Atlanta, GA, USA, 2015. Available online: https://www.cdc.gov/hpv/parents/cancer.html (accessed on 14 November 2020).
- Van Dyne, E.A.; Henley, S.J.; Saraiya, M.; Thomas, C.C.; Markowitz, L.E.; Benard, V.B. Trends in Human Papillomavirus–Associated Cancers—United States, 1999–2015. Morb. Mortal. Wkly. Rep. 2018, 67, 918–924. [Google Scholar] [CrossRef]
- Food and Drug Administration (FDA). FDA Approves Gardasil 9 for Prevention of Certain Cancers Caused by Five Additional Types of HPV; U.S. Department of Health and Human Services: Silver Spring, MD, USA, 2014. Available online: http://www.fda.gov (accessed on 14 November 2020).
- Markowitz, L.E.; Drolet, M.; Perez, N.; Jit, M.; Brisson, M. Human papillomavirus vaccine effectiveness by number of doses: Systematic review of data from national immunization programs. Vaccine 2018, 36, 4806–4815. [Google Scholar] [CrossRef]
- Spinner, C.; Ding, L.; Bernstein, D.I.; Brown, D.R.; Franco, E.L.; Covert, C.; Kahn, J. Human Papillomavirus Vaccine Effectiveness and Herd Protection in Young Women. Pediatrics 2019, 143. [Google Scholar] [CrossRef] [PubMed]
- Walker, T.Y. National, Regional, State, and Selected Local Area Vaccination Coverage Among Adolescents Aged 13–17 Years—United States, 2017. Morb. Mortal. Wkly. Rep. 2018, 67. [Google Scholar] [CrossRef] [PubMed]
- Barnard, M.; George, P.; Perryman, M.L.; Wolff, L.A. Human papillomavirus (HPV) vaccine knowledge, attitudes, and uptake in college students: Implications from the Precaution Adoption Process Model. PLoS ONE 2017, 12, e0182266. [Google Scholar] [CrossRef] [PubMed]
- Brown, D.R.; Shew, M.L.; Qadadri, B.; Neptune, N.; Vargas, M.; Tu, W.; Juliar, B.E.; Breen, T.E.; Fortenberry, J.D. A longitudinal study of genital human papillomavirus infection in a cohort of closely followed adolescent women. J. Infect. Dis. 2005, 191, 182–192. [Google Scholar] [CrossRef]
- Baranowski, T.; Cullen, K.W.; Basen-Engquist, K.; Wetter, D.W.; Cummings, S.; Martineau, D.S.; Prokhorov, A.; Chorley, J.; Beech, B.; Hergenroeder, A. Transitions out of High School: Time of Increased Cancer Risk? Prev. Med. 1997, 26, 694–703. [Google Scholar] [CrossRef]
- Gerend, M.A.; Shepherd, J.E. Predicting human papillomavirus vaccine uptake in young adult women: Comparing the health belief model and theory of planned behavior. Ann. Behav. Med. Publ. Soc. Behav. Med. 2012, 44, 171–180. [Google Scholar] [CrossRef]
- Gerend, M.A.; Shepherd, M.A.; Lustria, M.L.A.; Shepherd, J.E. Predictors of provider recommendation for HPV vaccine among young adult men and women: Findings from a cross-sectional survey. Sex. Transm. Infect. 2016, 92, 104–107. [Google Scholar] [CrossRef]
- Herrera-Ortiz, A.; Conde-Glez, C.J.; Olamendi-Portugal, M.L.; García-Cisneros, S.; Plett-Torres, T.; Sánchez-Alemán, M.A. College women, HPV genotyping and sexual behavior before HPV vaccination: Results from samples stored for a long time. J. Infect. Public Health 2018, 11, 286–289. [Google Scholar] [CrossRef] [PubMed]
- Jones, S.G.; Mathis-Gamble, K.; Fenkl, E.A. Minority College Students’ HPV Knowledge, Awareness, and Vaccination History. J. Assoc. Nurses. AIDS Care 2017, 28, 675–679. [Google Scholar] [CrossRef] [PubMed]
- Kasymova, S.; Harrison, S.E.; Pascal, C. Knowledge and Awareness of Human Papillomavirus among College Students in South Carolina. Infect Dis. 2019, 12, 1178633718825077. [Google Scholar] [CrossRef] [PubMed]
- McCutcheon, T.; Schaar, G. HPV knowledge and vaccination rates in college-aged males: Implications for practice. Nurse Pract. 2017, 42, 49–53. [Google Scholar] [CrossRef] [PubMed]
- Smith, A.; Rainie, L.; Zickuhr, K. College Students and Technology. Pew Research Center. 2018. Available online: http://www.pewinternet.org/2011/07/19/college-students-and-technology/ (accessed on 14 November 2020).
- Pew Research Center. Internet/Broadband Fact Sheet. Washington, DC, USA, February 2018. Available online: https://www.pewinternet.org/fact-sheet/internet-broadband/ (accessed on 14 November 2020).
- Pew Research Center. Mobile Fact Sheet. Washington, DC, USA, February 2018. Available online: https://www.pewinternet.org/fact-sheet/mobile/ (accessed on 14 November 2020).
- Gramlich, J. 10 facts about Americans and Facebook. Pew Research Center. 2019. Available online: https://www.pewresearch.org/fact-tank/2019/02/01/facts-about-americans-and-facebook/ (accessed on 14 November 2020).
- Odone, A.; Ferrari, A.; Spagnoli, F.; Visciarelli, S.; Shefer, A.; Pasquarella, C.; Signorelli, C. Effectiveness of interventions that apply new media to improve vaccine uptake and vaccine coverage A systematic review. Hum. Vaccines Immunother. 2015, 11, 72–82. [Google Scholar] [CrossRef]
- Briones, R.; Nan, X.; Madden, K.; Waks, L. When vaccines go viral: An analysis of HPV vaccine coverage on YouTube. Health Commun. 2012, 27, 478–485. [Google Scholar] [CrossRef]
- Zhou, X.; Coiera, E.; Tsafnat, G.; Arachi, D.; Ong, M.-S.; Dunn, A.G. Using social connection information to improve opinion mining: Identifying negative sentiment about HPV vaccines on Twitter. Stud. Health Technol. Inform. 2015, 216, 761–765. [Google Scholar]
- Sundstrom, B.; Aylor, E.; Cartmell, K.B.; Brandt, H.M.; Bryant, D.C.; Hughes Halbert, C.; Young Pierce, J. Beyond the birds and the bees: A qualitative content analysis of online HPV vaccination communication. J. Commun. Healthc. 2018, 11, 205–214. [Google Scholar] [CrossRef]
- Cates, J.R.; Shafer, A.; Diehl, S.J.; Deal, A.M. Evaluating a County-Sponsored Social Marketing Campaign to Increase Mothers’ Initiation of HPV Vaccine for Their Preteen Daughters in a Primarily Rural Area. Soc. Mark. Q. 2011, 17, 4–26. [Google Scholar] [CrossRef]
- Cates, J.R.; Diehl, S.J.; Crandell, J.L.; Coyne-Beasley, T. Intervention effects from a social marketing campaign to promote HPV vaccination in preteen boys. Vaccine 2014, 32, 4171–4178. [Google Scholar] [CrossRef]
- Kennedy, A.; Sapsis, K.F.; Stokley, S.; Curtis, C.R.; Gust, D. Parental attitudes toward human papillomavirus vaccination: Evaluation of an educational intervention, 2008. J. Health Commun. 2011, 16, 300–313. [Google Scholar] [CrossRef] [PubMed]
- Cohen, E.L.; Head, K.J.; McGladrey, M.J.; Hoover, A.G.; Vanderpool, R.C.; Bridger, C.; Carman, A.; Crosby, R.A.; Darling, E.; Tucker-McLaughlin, M.; et al. Designing for Dissemination: Lessons in Message Design from “1-2-3 Pap”. Health Commun. 2015, 30, 196–207. [Google Scholar] [CrossRef] [PubMed]
- Cohen, E.L.; Head, K.J. Identifying knowledge-attitude-practice gaps to enhance HPV vaccine diffusion. J. Health Commun. 2013, 18, 1221–1234. [Google Scholar] [CrossRef] [PubMed]
- Frank, L.B.; Murphy, S.T.; Chatterjee, J.S.; Moran, M.B.; Baezconde-Garbanati, L. Telling Stories, Saving Lives: Creating Narrative Health Messages. Health Commun. 2015, 30, 154–163. [Google Scholar] [CrossRef]
- Hopfer, S. Effects of a Narrative HPV Vaccination Intervention Aimed at Reaching College Women: A Randomized Controlled Trial. Prev Sci. 2012, 13, 173–182. [Google Scholar] [CrossRef]
- Krawczyk, A.; Lau, E.; Perez, S.; Delisle, V.; Amsel, R.; Rosberger, Z. How to inform: Comparing written and video education interventions to increase human papillomavirus knowledge and vaccination intentions in young adults. J. Am. Coll. Health 2012, 60, 316–322. [Google Scholar] [CrossRef]
- Macario, E.; Matiella, A.C. A bilingual webnovela on the human papillomavirus: Will Latinas and health professionals use it? J. Commun. Healthc. 2015, 8, 55–66. [Google Scholar] [CrossRef]
- Sundstrom, B.; Carr, L.A.; DeMaria, A.L.; Korte, J.E.; Modesitt, S.C.; Pierce, J.Y. Protecting the Next Generation: Elaborating the Health Belief Model to Increase HPV Vaccination among College-Age Women. Soc. Mark. Q 2015, 21, 173–188. [Google Scholar] [CrossRef]
- Balatsoukas, P.; Kennedy, C.M.; Buchan, I.; Powell, J.; Ainsworth, J. The Role of Social Network Technologies in Online Health Promotion: A Narrative Review of Theoretical and Empirical Factors Influencing Intervention Effectiveness. J. Med. Internet Res. 2015, 17, e141. [Google Scholar] [CrossRef]
- Betsch, C. Social media targeting of health messages. Hum. Vaccines Immunother. 2014, 10, 2636–2637. [Google Scholar] [CrossRef]
- Maher, C.A.; Lewis, L.K.; Ferrar, K.; Marshall, S.; De Bourdeaudhuij, I.; Vandelanotte, C. Are health behavior change interventions that use online social networks effective? A systematic review. J. Med. Internet Res. 2014, 16, e40. [Google Scholar] [CrossRef] [PubMed]
- Raviotta, J.M.; Nowalk, M.P.; Lin, C.J.; Huang, H.-H.; Zimmerman, R.K. Using FacebookTM to Recruit College-Age Men for a Human Papillomavirus Vaccine Trial. Am. J. Mens Health 2016, 10, 110–119. [Google Scholar] [CrossRef] [PubMed]
- Zhang, N.; Tsark, J.; Campo, S.; Teti, M. Facebook for Health Promotion: Female College Students’ Perspectives on Sharing HPV Vaccine Information through Facebook. Hawaii J. Med. Public Health 2015, 74, 136–140. [Google Scholar] [PubMed]
- Lai, C.-Y.; Wu, W.-W.; Tsai, S.-Y.; Cheng, S.-F.; Lin, K.-C.; Liang, S.-Y. The Effectiveness of a Facebook-Assisted Teaching Method on Knowledge and Attitudes about Cervical Cancer Prevention and HPV Vaccination Intention among Female Adolescent Students in Taiwan. Health Educ. Behav. 2015, 42, 352–360. [Google Scholar] [CrossRef] [PubMed]
- Sundstrom, B.; Brandt, H.M.; Gray, L.; Young Pierce, J. It’s My Time: Applying the health belief model to prevent cervical cancer among college-age women. J. Commun. Manag. 2018, 22, 161–178. [Google Scholar] [CrossRef]
- West, D.S.; Monroe, C.M.; Turner-McGrievy, G.; Sundstrom, B.; Larsen, C.; Magradey, K.; Wilcox, S.; Brandt, H.M. A Technology-Mediated Behavioral Weight Gain Prevention Intervention for College Students: Controlled, Quasi-Experimental Study. J. Med. Internet Res. 2016, 18. [Google Scholar] [CrossRef] [PubMed]
- Rosenstock, I.M. The health belief model and preventive health behavior. Health Educ. Behav. 1974, 2, 354–386. [Google Scholar] [CrossRef]
- Rosenstock, I.M.; Strecher, V.J.; Becker, M.H. Social learning theory and the health belief model. Health Educ. Behav. 1988, 15, 175–183. [Google Scholar] [CrossRef]
- Prochaska, J.O.; Velicer, W.F. The Transtheoretical Model of Health Behavior Change. Am. J. Health Promot. 1997, 12, 38–48. [Google Scholar] [CrossRef]
- Mills, L.A.; Head, K.J.; Vanderpool, R.C. HPV vaccination among young adult women: A perspective from Appalachian Kentucky. Prev. Chronic Dis. 2013, 10. [Google Scholar] [CrossRef]
- Hopfer, S.; Garcia, S.; Duong, H.T.; Russo, J.A.; Tanjasiri, S.P. A Narrative Engagement Framework to Understand HPV Vaccination among Latina and Vietnamese Women in a Planned Parenthood Setting. Health Educ. Behav. 2017, 44, 738–747. [Google Scholar] [CrossRef] [PubMed]
- Bandura, A. Health promotion by social cognitive means. Health Educ. Behav. Off Publ. Soc. Public Health Educ. 2004, 31, 143–164. [Google Scholar] [CrossRef] [PubMed]
- Group TDPP (DPP) R. The Diabetes Prevention Program (DPP): Description of lifestyle intervention. Diabetes Care 2002, 25, 2165–2171. [Google Scholar]
- Patel Divya, A.; Grunzweig, K.A.; Zochowski, M.K.; Dempsey, A.F.; Carlos, R.C.; Dalton, V.K. Human Papillomavirus Vaccine Stages of Change among Male and Female University Students: Ready or Not? J. Am. Coll. Health 2013, 61, 336–346. [Google Scholar] [CrossRef] [PubMed]
- Corbin, J.; Strauss, A. Basics of Qualitative Research: Techniques and Procedures for Developing Grounded Theory, 3rd ed.; Sage Publications, Inc.: Thousand Oaks, CA, USA, 2008; 401p. [Google Scholar]
- McBride, K.R.; Singh, S. Predictors of Adults’ Knowledge and Awareness of HPV, HPV-Associated Cancers, and the HPV Vaccine: Implications for Health Education. Health Educ. Behav. 2018, 45, 68–76. [Google Scholar] [CrossRef] [PubMed]
- Kessels, S.J.M.; Marshall, H.S.; Watson, M.; Braunack-Mayer, A.J.; Reuzel, R.; Tooher, R.L. Factors associated with HPV vaccine uptake in teenage girls: A systematic review. Vaccine 2012, 30, 3546–3556. [Google Scholar] [CrossRef]
- Merchant, G.; Weibel, N.; Patrick, K.; Fowler, J.H.; Norman, G.J.; Gupta, A.; Servetas, C.; Calfas, K.; Raste, K.; Pina, L.; et al. Click “Like” to Change Your Behavior: A Mixed Methods Study of College Students’ Exposure to and Engagement With Facebook Content Designed for Weight Loss. J. Med. Internet Res. 2014, 16, e158. [Google Scholar] [CrossRef]
- Bull, S.; Ezeanochie, N. From Foucault to Freire through Facebook: Toward an Integrated Theory of mHealth. Health Educ. Behav. 2015. [Google Scholar] [CrossRef]
| Session | Topics |
|---|---|
| 1 | What is HPV? |
| 2 | Am I at risk for HPV? |
| 3 | How do I prevent HPV? |
| 4 | How do I know if I have HPV? |
| 5 | What are the risks and benefits of HPV vaccination? |
| 6 | Should I get the HPV vaccine? |
| 7 | Where do I go to get the HPV vaccine? |
| 8 | Why do I need 3 doses? |
| Measure | Total (n = 58) | HPV (n = 29) | Control (n = 29) |
|---|---|---|---|
| Age (SD), years | 21.6 (2.2) | 21.1 (0.8) | 22.1 (2.9) |
| Sex, n (%) | |||
| Female | 47 (81) | 24 (85) | 23 (79) |
| Male | 11 (19) | 5 (17) | 6 (21) |
| Hispanic, n (%) | |||
| Yes | 5 (9) | 3 (10) | 2 (7) |
| No | 53 (91) | 26 (90) | 27 (93) |
| Race, n (%) | |||
| Caucasian | 52 (90) | 28 (97) | 24 (83) * |
| African-American | 3 (5) | 1 (3) | 2 (7) |
| Asian | 2 (3) | 0 (0) | 2 (7) |
| American Indian/Native American | 1 (2) | 0 (0) | 1 (3) |
| Academic year, n (%) | |||
| 2nd year | 1 (2) | 0 (0) | 1 (3) |
| 3rd year | 17 (29) | 13 (45) | 4 (14) |
| 4th year | 33 (57) | 14 (48) | 19 (66) |
| 5th year | 7 (12) | 2 (7) | 5 (17) |
| Health Insurance Status, n (%) | |||
| Parent’s Plan | 54 (93) | 28 (97) | 26 (90) |
| None | 3 (5) | 1 (3) | 2 (7) |
| Another plan | 1 (2) | 0 (0.0) | 1 (3) |
| Age at first sexual intercourse (SD), years | 16.9 (1.6) | 17.1 (1.8) | 16.7 (1.3) |
| Number of sex partners (SD) | |||
| Past month | 0.9 (0.6) | 10 (0.6) | 0.9 (0.6) |
| Past 6 months | 1.9 (2.1) | 1.7 (1.2) | 2.1 (2.7) |
| Lifetime | 7.0 (5.7) | 6.6 (5.0) | 7.5 (6.4) |
| Current monogamous partnership | |||
| Yes | 28 (50) | 14 (48) | 14 (52) |
| No | 26 (46) | 14 (48) | 12 (44) |
| Don’t Know | 2 (4) | 1 (3) | 1 (4) |
| Retention rates | 56 (97%) | 29 (100%) | 27 (93%) |
| HPV (n = 29) | Control (n = 29) | |||
|---|---|---|---|---|
| Pre | Post | Pre | Post | |
| Received full vaccination series (%) | 19 (66) | 21 (78) | 14 (48) | 15 (52) |
| Initiated partial vaccination series (%) | 2 (7) | 0 (0) | 3 (10) | 4 (14) |
| Never vaccinated (%) | 7 (24) | 3 (11) | 9 (31) | 8 (28) |
| Intend to get vaccinated within 6 months (%) | 1 (3) | 3 (11) | 3 (10) | 2 (7) |
| HPV | Control | ||||
|---|---|---|---|---|---|
| Pre (n = 28) | Post (n = 27) | Pre (n = 29) | Post (n = 29) | Difference in Change between Groups at Posttest (p-Value) | |
| Some types of HPV can cause oral cancer. Correct answer: True | 65.5 | 100 * | 48.3 | 69.0 | 0.007 |
| Some types of HPV can cause anal cancer. Correct answer: True | 58.6 | 92.6 * | 48.3 | 65.5 | 0.04 |
| Some types of HPV can cause genital warts. Correct answer: True | 78.6 | 100 * | 69.0 | 82.8 | 0.024 |
| HPV can be spread through contact other than sexual intercourse. Correct answer: True | 69.0 | 92.6 * | 58.6 | 69.0 | 0.072 |
| Condom use fully protects against the spread of HPV. Correct answer: False | 69.0 | 92.6 | 75.9 | 82.8 | 0.42 |
| HPV can cause an abnormal Pap (cervical cancer screening) test. Correct answer: True | 82.8 | 96.3 | 82.8 | 86.2 | 0.186 |
| People who have been infected with HPV might not have symptoms. Correct answer: True | 86.2 | 100 | 96.6 | 96.6 | 0.33 |
| HPV can be spread through sexual intercourse. Correct answer: True | 100 | 100 | 93.1 | 100 | 1.00 |
| Some types of HPV can cause cervical cancer. Correct answer: True | 96.6 | 100 | 89.7 | 93.1 | 0.165 |
| An HPV infection can be cured. Correct answer: False | 27.6 | 37 | 65.5 | 41.4 | 0.049 |
| Women who get the vaccine still need regular Pap (cervical cancer screening) tests. Correct answer: True | 93.1 | 85.2 | 93.1 | 86.2 | 0.76 |
| Themes | Illustrative Quotes |
|---|---|
| HPV vaccination knowledge, attitudes, and behaviors | “After reading all of the posts and doing some other research I now believe that the vaccine is something everyone should have. I mean there is really no reason not to get vaccinated.” “My viewpoint has definitely changed for the better. At the beginning of this study, I did not know too terribly much about HPV. At this point I know quite a bit and I know the facts concerning the matter. I’ve been able to relay this information to my friends and family and help them even take steps in the right direction to protect themselves.” |
| Intervention engagement and treatment satisfaction | “I believe the material presented in this week’s Facebook post were user friendly and easy to understand and read. I am not familiar with the use of Facebook but I found it pretty easy to use and follow along with.” “Many students even got to share personal stories of people who have had issues with HPV in the past. I believe this is important to share because if you personally know someone effected by HPV or even if it is just a friend of a friend, the situation or topic of HPV automatically becomes more personal and ‘hits home’ for a lot more people. I also enjoyed reading other people’s articles that they have found from other sources. The more information or reading on this topic helps for me to get a better idea of truly how serious HPV is.” |
| Level of Engagement | Comments Number of Students | Post Likes Number of Students | Comment Likes Number of Students |
|---|---|---|---|
| High (21+) | 11 | 1 | 4 |
| Medium (11–20) | 12 | 6 | 5 |
| Low (0–10) | 6 | 22 | 20 |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2020 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Brandt, H.M.; Sundstrom, B.; Monroe, C.M.; Turner-McGrievy, G.; Larsen, C.; Stansbury, M.; Magradey, K.; Gibson, A.; West, D.S. Evaluating a Technology-Mediated HPV Vaccination Awareness Intervention: A Controlled, Quasi-Experimental, Mixed Methods Study. Vaccines 2020, 8, 749. https://doi.org/10.3390/vaccines8040749
Brandt HM, Sundstrom B, Monroe CM, Turner-McGrievy G, Larsen C, Stansbury M, Magradey K, Gibson A, West DS. Evaluating a Technology-Mediated HPV Vaccination Awareness Intervention: A Controlled, Quasi-Experimental, Mixed Methods Study. Vaccines. 2020; 8(4):749. https://doi.org/10.3390/vaccines8040749
Chicago/Turabian StyleBrandt, Heather M., Beth Sundstrom, Courtney M. Monroe, Gabrielle Turner-McGrievy, Chelsea Larsen, Melissa Stansbury, Karen Magradey, Andrea Gibson, and Delia Smith West. 2020. "Evaluating a Technology-Mediated HPV Vaccination Awareness Intervention: A Controlled, Quasi-Experimental, Mixed Methods Study" Vaccines 8, no. 4: 749. https://doi.org/10.3390/vaccines8040749
APA StyleBrandt, H. M., Sundstrom, B., Monroe, C. M., Turner-McGrievy, G., Larsen, C., Stansbury, M., Magradey, K., Gibson, A., & West, D. S. (2020). Evaluating a Technology-Mediated HPV Vaccination Awareness Intervention: A Controlled, Quasi-Experimental, Mixed Methods Study. Vaccines, 8(4), 749. https://doi.org/10.3390/vaccines8040749





