Coronavirus Disease 2019 (COVID-19) Pandemic across Africa: Current Status of Vaccinations and Implications for the Future
Abstract
1. Introduction
2. Materials and Methods
2.1. Study Design
2.2. Questionnaire Design and Analysis
- Did your country have a dedicated COVID-19 vaccine rollout programme? Was this in the public sector, private sector, or both, and were any specific age groups covered?
- Which COVID-19 vaccines were made available and how were the costs covered for each (e.g., NGOs)?
- What is the current coverage rate (different doses if known)?
- What is being done to ensure access to COVID-19 vaccines, and how would you describe the acceptance (willingness) of the population to COVID-19 vaccinations?
- What is the extent of any misinformation about the vaccine (if known), and how is misinformation being spread (e.g., social media)?
- What are the challenges with COVID-19 vaccinations in addition to the above, and what are potential ways forward or measures being undertaken by national authorities and other key stakeholders to mitigate against these challenges?
2.3. Ethical Considerations
3. Results
3.1. Vaccine Sources and Deployment
3.2. Vaccination Coverage
3.3. Access, Hesitancy, and Challenges with the COVID-19 Vaccine Roll-Out
3.4. Lessons Learnt and Ways Forward
4. Discussion
5. Conclusions
Supplementary Materials
Author Contributions
Funding
Institutional Review Board Statement
Data Availability Statement
Conflicts of Interest
References
- Bedford, J.; Enria, D.; Giesecke, J.; Heymann, D.L.; Ihekweazu, C.; Kobinger, G.; Lane, H.C.; Memish, Z.; Oh, M.-D.; Sall, A.A.; et al. COVID-19: Towards controlling of a pandemic. Lancet 2020, 395, 1015–1018. [Google Scholar] [CrossRef]
- World Health Organization. WHO COVID-19 Dashboard. 2021. Available online: https://covid19.who.int (accessed on 1 August 2022).
- Hopman, J.; Allegranzi, B.; Mehtar, S. Managing COVID-19 in Low- and Middle-Income Countries. JAMA 2020, 323, 1549. [Google Scholar] [CrossRef] [PubMed]
- Choi, A.J.; Hean, A.C.; Lee, J.K.; Tran, N.D.; Lin, T.K.; Apollonio, D.E. A Retrospective Global Assessment of Factors Associated With COVID-19 Policies and Health Outcomes. Front. Public Health 2022, 10, 843445. [Google Scholar] [CrossRef] [PubMed]
- Nussbaumer-Streit, B.; Mayr, V.; Dobrescu, A.I.; Chapman, A.; Persad, E.; Klerings, I.; Wagner, G.; Siebert, U.; Ledinger, D.; Zachariah, C.; et al. Quarantine alone or in combination with other public health measures to control COVID-19: A rapid review. Cochrane Database Syst. Rev. 2020, 9, cd013574. [Google Scholar] [PubMed]
- Tang, K.H.D. Movement control as an effective measure against COVID-19 spread in Malaysia: An overview. J. Public Health 2022, 30, 583–586. [Google Scholar] [CrossRef]
- Ng, Y.; Li, Z.; Chua, Y.X.; Chaw, W.L.; Zhao, Z.; Er, B.; Pung, R.; Chiew, C.J.; Lye, D.; Heng, D.; et al. Evaluation of the Effectiveness of Surveillance and Containment Measures for the First 100 Patients with COVID-19 in Singapore—January 2–February 29, 2020. MMWR Morb. Mortal. Wkly. Rep. 2020, 69, 307–311. [Google Scholar] [CrossRef]
- Keni, R.; Alexander, A.; Nayak, P.G.; Mudgal, J.; Nandakumar, K. COVID-19: Emergence, Spread, Possible Treatments, and Global Burden. Front. Public Health 2020, 8, 216. [Google Scholar] [CrossRef]
- Talic, S.; Shah, S.; Wild, H.; Gasevic, D.; Maharaj, A.; Ademi, Z.; Li, X.; Xu, W.; Mesa-Eguiagaray, I.; Rostron, J.; et al. Effectiveness of public health measures in reducing the incidence of COVID-19, SARS-CoV-2 transmission, and COVID-19 mortality: Systematic review and meta-analysis. BMJ 2021, 375, e068302. [Google Scholar] [CrossRef]
- Etando, A.; Amu, A.A.; Haque, M.; Schellack, N.; Kurdi, A.; Alrasheedy, A.A.; Timoney, A.; Mwita, J.C.; Rwegerera, G.M.; Patrick, O.; et al. Challenges and Innovations Brought about by the COVID-19 Pandemic Regarding Medical and Pharmacy Education Especially in Africa and Implications for the Future. Healthcare 2021, 9, 1722. [Google Scholar] [CrossRef]
- Shiraef, M.A.; Friesen, P.; Feddern, L.; Weiss, M.A. Did border closures slow SARS-CoV-2? Sci. Rep. 2022, 12, 1709. [Google Scholar] [CrossRef]
- Cheng, V.C.; Wong, S.C.; Chuang, V.W.; So, S.Y.; Chen, J.H.; Sridhar, S.; To, K.K.-W.; Chan, J.F.-W.; Hung, I.F.-N.; Ho, P.-L.; et al. The role of community-wide wearing of face mask for control of coronavirus disease 2019 (COVID-19) epidemic due to SARS-CoV-2. J. Infect. 2020, 81, 107–114. [Google Scholar] [CrossRef] [PubMed]
- Congressional Research Services. Global Economic Effects of COVID-19—Updated 10 November 2021. Available online: https://sgp.fas.org/crs/row/R46270.pdf (accessed on 2 August 2022).
- Verma, B.K.; Verma, M.; Msc, V.K.V.; Abdullah, R.B.; Nath, D.C.; Khan, H.T.A.; Verma, A.; Vishwakarma, R.K.; Verma, V. Global lockdown: An effective safeguard in responding to the threat of COVID -19. J. Eval. Clin. Pract. 2020, 26, 1592–1598. [Google Scholar] [CrossRef] [PubMed]
- Ogunleye, O.O.; Basu, D.; Mueller, D.; Sneddon, J.; Seaton, R.A.; Yinka-Ogunleye, A.F.; Wamboga, J.; Miljković, N.; Mwita, J.C.; Rwegerera, G.M.; et al. Response to the Novel Corona Virus (COVID-19) Pandemic Across Africa: Successes, Challenges, and Implications for the Future. Front. Pharmacol. 2020, 11, 1205. [Google Scholar] [CrossRef] [PubMed]
- Godman, B.; Haque, M.; Islam, S.; Iqbal, S.; Urmi, U.L.; Kamal, Z.M.; Shuvo, S.A.; Rahman, A.; Kamal, M.; Haque, M.; et al. Rapid Assessment of Price Instability and Paucity of Medicines and Protection for COVID-19 Across Asia: Findings and Public Health Implications for the Future. Front. Public Health 2020, 8, 585832. [Google Scholar] [CrossRef]
- Chan, D.K.C.; Zhang, C.-Q.; Weman-Josefsson, K. Why people failed to adhere to COVID-19 preventive behaviors? Perspectives from an integrated behavior change model. Infect. Control Hosp. Epidemiol. 2020, 42, 375–376. [Google Scholar] [CrossRef]
- Levin, A.T.; Owusu-Boaitey, N.; Pugh, S.; Fosdick, B.K.; Zwi, A.B.; Malani, A.; Soman, S.; Besançon, L.; Kashnitsky, I.; Ganesh, S.; et al. Assessing the burden of COVID-19 in developing countries: Systematic review, meta-analysis and public policy implications. BMJ Glob. Health 2022, 7, e008477. [Google Scholar] [CrossRef]
- Pan, H.; Peto, R.; Henao-Restrepo, A.M.; Preziosi, M.P.; Sathiyamoorthy, V.; Abdool Karim, Q.; Alejandria, M.M.; García, C.H.; Kieny, M.; Malekzadeh, R.; et al. Repurposed Antiviral Drugs for Covid-19—Interim WHO Solidarity Trial Results. N. Engl. J Med. 2021, 384, 497–511. [Google Scholar]
- Schellack, N.; Strydom, M.; Pepper, M.S.; Herd, C.L.; Hendricks, C.L.; Bronkhorst, E.; Meyer, J.C.; Padayachee, N.; Bangalee, V.; Truter, I.; et al. Social Media and COVID-19—Perceptions and Public Deceptions of Ivermectin, Colchicine and Hydroxychloroquine: Lessons for Future Pandemics. Antibiotics 2022, 11, 445. [Google Scholar] [CrossRef]
- Bryant, A.; Lawrie, T.A.; Dowswell, T.; Fordham, E.J.; Mitchell, S.; Hill, S.R.; Tham, T.C. Ivermectin for Prevention and Treatment of COVID-19 Infection: A Systematic Review, Meta-analysis, and Trial Sequential Analysis to Inform Clinical Guidelines. Am. J. Ther. 2021, 28, e434–e460. [Google Scholar] [CrossRef]
- Uzunova, K.; Filipova, E.; Pavlova, V.; Vekov, T. Insights into antiviral mechanisms of remdesivir, lopinavir/ritonavir and chloroquine/hydroxychloroquine affecting the new SARS-CoV-2. Biomed. Pharmacother. 2020, 131, 110668. [Google Scholar] [CrossRef]
- Abubakar, A.R.; Sani, I.H.; Godman, B.; Kumar, S.; Islam, S.; Jahan, I.; Haque, M. Systematic Review on the Therapeutic Options for COVID-19: Clinical Evidence of Drug Efficacy and Implications. Infect. Drug Resist. 2020, 13, 4673–4695. [Google Scholar] [CrossRef]
- Medhi, B.; Sarma, P.; Bhattacharyya, A.; Kaur, H.; Prajapat, M.; Prakash, A.; Kumar, S.; Bansal, S.; Kirubakaran, R.; Reddy, D.; et al. Efficacy and safety of steroid therapy in COVID-19: A rapid systematic review and Meta-analysis. Indian J. Pharmacol. 2020, 52, 535–550. [Google Scholar] [CrossRef] [PubMed]
- Sulis, G.; Batomen, B.; Kotwani, A.; Pai, M.; Gandra, S. Sales of antibiotics and hydroxychloroquine in India during the COVID-19 epidemic: An interrupted time series analysis. PLoS Med. 2021, 18, e1003682. [Google Scholar] [CrossRef] [PubMed]
- Sefah, I.A.; Ogunleye, O.O.; Essah, D.O.; Opanga, S.A.; Butt, N.; Wamaitha, A.; Guantai, A.N.; Chikowe, I.; Khuluza, F.; Kibuule, D.; et al. Rapid Assessment of the Potential Paucity and Price Increases for Suggested Medicines and Protection Equipment for COVID-19 Across Developing Countries With a Particular Focus on Africa and the Implications. Front. Pharmacol. 2021, 11, 588106. [Google Scholar] [CrossRef]
- Charan, J.; Dutta, S.; Kaur, R.; Bhardwaj, P.; Ambwani, S.; Godman, B.; Jha, P.; Sukhija, S.; Venkatesh, S.; Lugova, H.; et al. Demand of COVID-19 medicines without prescription among community pharmacies in Jodhpur, India: Findings and implications. J. Fam. Med. Prim. Care 2022, 11, 503. [Google Scholar] [CrossRef] [PubMed]
- Haque, M.; Gowere, M.; Nusrat, N.; Chowdhury, K.; Godman, B. The response to COVID 19 across countries and the implications for future pandemics. Bangladesh J. Med Sci. 2021, 20, 7–14. [Google Scholar] [CrossRef]
- Manivannan, E.; Karthikeyan, C.; Moorthy, N.S.H.N.; Chaturvedi, S.C. The Rise and Fall of Chloroquine/Hydroxychloroquine as Compassionate Therapy of COVID-19. Front. Pharmacol. 2021, 12, 584940. [Google Scholar] [CrossRef]
- Charan, J.; Kaur, R.J.; Bhardwaj, P.; Haque, M.; Sharma, P.; Misra, S.; Godman, B. Rapid review of suspected adverse drug events due to remdesivir in the WHO database; findings and implications. Expert Rev. Clin. Pharmacol. 2020, 14, 95–103. [Google Scholar] [CrossRef]
- Abena, P.M.; Decloedt, E.H.; Bottieau, E.; Suleman, F.; Adejumo, P.; Sam-Agudu, N.A.; Muyembe TamFum, J.-J.; Seydi, M.; Eholie, S.P.; Mills, E.J.; et al. Chloroquine and Hydroxychloroquine for the Prevention or Treatment of novel coronavirus disease (COVID-19) in Africa: Caution for Inappropriate Off-label Use in Healthcare Settings. Am. J. Trop. Med. Hyg. 2020, 102, 1184–1188. [Google Scholar] [CrossRef]
- RECOVERY Collaborative Group; Horby, P.; Lim, W.S.; Emberson, J.R.; Mafham, M.; Bell, J.L.; Linsell, L.; Staplin, N.; Brightling, C.; Ustianowski, A.; et al. Dexamethasone in Hospitalized Patients with Covid-19. N. Engl. J. Med. 2021, 384, 693–704. [Google Scholar] [CrossRef]
- RECOVERY Collaborative Group. Lopinavir-ritonavir in patients admitted to hospital with COVID-19 (RECOVERY): A randomised, controlled, open-label, platform trial. Lancet 2020, 396, 1345–1352. [Google Scholar] [CrossRef]
- WHO. WHO Discontinues Hydroxychloroquine and Lopinavir/Ritonavir Treatment Arms for COVID-19. 2020. Available online: https://www.who.int/news/item/04-07-2020-who-discontinues-hydroxychloroquine-and-lopinavir-ritonavir-treatment-arms-for-covid-19 (accessed on 1 August 2022).
- Dyer, O. COVID-19: Remdesivir Has Little or No Impact on Survival, WHO Trial Shows. BMJ 2020, 371, m4057. [Google Scholar] [CrossRef] [PubMed]
- Deng, J.; Zhou, F.; Ali, S.; Heybati, K.; Hou, W.; Huang, E.; Wong, C.Y. Correction to: Efficacy and safety of ivermectin for the treatment of COVID-19: A systematic review and meta-analysis. QJM Int. J. Med. 2022, 114, 721–734. [Google Scholar] [CrossRef] [PubMed]
- RECOVERY Collaborative Group; Horby, P.; Mafham, M.; Linsell, L.; Bell, J.L.; Staplin, N.; Emberson, J.R.; Wiselka, M.; Ustianowski, A.; Elmahi, E.; et al. Effect of Hydroxychloroquine in Hospitalized Patients with Covid-19. N. Engl. J. Med. 2020, 383, 2030–2040. [Google Scholar] [CrossRef] [PubMed]
- CIOMS. Medicines Assessment during Public Health Emergencies Needs Good Science, Best Practices and Proper Communication. 2020. Available online: https://cioms.ch/es-template/medicines-assessment-during-public-health-emergencies-needs-good-science-best-practices-and-proper-communication/ (accessed on 2 August 2022).
- Grimes, D.R. Medical disinformation and the unviable nature of COVID-19 conspiracy theories. PLoS ONE 2021, 16, e0245900. [Google Scholar] [CrossRef] [PubMed]
- Neil, S.J.; Campbell, E.M. Fake Science: XMRV, COVID-19, and the Toxic Legacy of Dr. Judy Mikovits. AIDS Res. Hum. Retrovir. 2020, 36, 545–549. [Google Scholar] [CrossRef]
- Carley, S.; Horner, D.; Body, R.; Mackway-Jones, K. Evidence-based medicine and COVID-19: What to believe and when to change. Emerg. Med. J. 2020, 37, 572–575. [Google Scholar] [CrossRef]
- Kluge, H.H.P.; Wickramasinghe, K.; Rippin, H.L.; Mendes, R.; Peters, D.H.; Kontsevaya, A.; Breda, J. Prevention and control of non-communicable diseases in the COVID-19 response. Lancet 2020, 395, 1678–1680. [Google Scholar] [CrossRef]
- Fatoye, F.; Gebrye, T.; Arije, O.; Fatoye, C.T.; Onigbinde, O.; Mbada, C. Economic Impact of COVID-19 Lockdown on households. Pan Afr. Med. J. 2021, 40, 225. [Google Scholar] [CrossRef]
- Glied, S.; Levy, H. The Potential Effects of Coronavirus on National Health Expenditures. JAMA 2020, 323, 2001. [Google Scholar] [CrossRef]
- Richards, F.; Kodjamanova, P.; Chen, X.; Li, N.; Atanasov, P.; Bennetts, L.; Patterson, B.J.; Yektashenas, B.; Mesa-Frias, M.; Tronczynski, K.; et al. Economic Burden of COVID-19: A Systematic Review. Clin. Outcomes Res. 2022, 14, 293–307. [Google Scholar] [CrossRef] [PubMed]
- Buheji, M.; da Costa Cunha, K.; Beka, G.; Mavric, B.; De Souza, Y.L.; da Costa Silva, S.S.; Hanafi, M.; Yein, T.C. The Extent of COVID-19 Pandemic Socio-Economic Impact on Global Poverty. A Global Integrative Multidisciplinary Review. Am. J. Econ. 2020, 10, 213–224. [Google Scholar] [CrossRef]
- Martin, A.; Markhvida, M.; Hallegatte, S.; Walsh, B. Socio-Economic Impacts of COVID-19 on Household Consumption and Poverty. Econ. Disasters Clim. Chang. 2020, 4, 453–479. [Google Scholar] [CrossRef] [PubMed]
- The Economist. What Is the Economic Cost of COVID-19? 2021. Available online: https://www.economist.com/finance-and-economics/2021/01/09/what-is-the-economic-cost-of-covid-19 (accessed on 1 August 2022).
- Suthar, S.; Das, S.; Nagpure, A.; Madhurantakam, C.; Tiwari, S.B.; Gahlot, P.; Tyagi, V.K. Epidemiology and diagnosis, environmental resources quality and socio-economic perspectives for COVID-19 pandemic. J. Environ. Manag. 2020, 280, 111700. [Google Scholar] [CrossRef]
- Riera, R.; Bagattini, M.; Pacheco, R.L.; Pachito, D.V.; Roitberg, F.; Ilbawi, A. Delays and Disruptions in Cancer Health Care Due to COVID-19 Pandemic: Systematic Review. JCO Glob. Oncol. 2021, 7, 311–323. [Google Scholar] [CrossRef]
- Moraliyage, H.; De Silva, D.; Ranasinghe, W.; Adikari, A.; Alahakoon, D.; Prasad, R.; Lawrentschuk, N.; Bolton, D. Cancer in Lockdown: Impact of the COVID -19 Pandemic on Patients with Cancer. Oncologist 2020, 26, e342–e344. [Google Scholar] [CrossRef]
- Jiang, H.; Zhou, Y.; Tang, W. Maintaining HIV care during the COVID-19 pandemic. Lancet HIV 2020, 7, e308–e309. [Google Scholar] [CrossRef]
- Ataguba, J.E. COVID-19 Pandemic, a War to be Won: Understanding its Economic Implications for Africa. Appl. Health Econ. Health Policy 2020, 18, 325–328. [Google Scholar] [CrossRef]
- Abbas, K.; Procter, S.R.; van Zandvoort, K.; Clark, A.; Funk, S.; Mengistu, T.; Hogan, D.; Dansereau, E.; Jit, M.; Flasche, S.; et al. Routine childhood immunisation during the COVID-19 pandemic in Africa: A benefit-risk analysis of health benefits versus excess risk of SARS-CoV-2 infection. Lancet Glob. Health 2020, 8, e1264–e1272. [Google Scholar] [CrossRef]
- Causey, K.; Fullman, N.; Sorensen, R.J.D.; Galles, N.C.; Zheng, P.; Aravkin, A.; Danovaro-Holliday, M.C.; Martinez-Piedra, R.; Sodha, S.V.; Velandia-González, M.P.; et al. Estimating global and regional disruptions to routine childhood vaccine coverage during the COVID-19 pandemic in 2020: A modelling study. Lancet 2021, 398, 522–534. [Google Scholar] [CrossRef]
- Shet, A.; Carr, K.; Danovaro-Holliday, M.C.; Sodha, S.V.; Prosperi, C.; Wunderlich, J.; Wonodi, C.; Reynolds, H.W.; Mirza, I.; Gacic-Dobo, M.; et al. Impact of the SARS-CoV-2 pandemic on routine immunisation services: Evidence of disruption and recovery from 170 countries and territories. Lancet Glob. Health 2022, 10, e186–e194. [Google Scholar] [CrossRef]
- Evans, B.; Jombart, T. Worldwide routine immunisation coverage regressed during the first year of the COVID-19 pandemic. Vaccine 2022, 40, 3531–3535. [Google Scholar] [CrossRef] [PubMed]
- Mohammed, I.; Nauman, A.; Paul, P.; Ganesan, S.; Chen, K.-H.; Jalil, S.M.S.; Jaouni, S.H.; Kawas, H.; Khan, W.A.; Vattoth, A.L.; et al. The efficacy and effectiveness of the COVID-19 vaccines in reducing infection, severity, hospitalization, and mortality: A systematic review. Hum. Vaccines Immunother. 2022, 18, 2027160. [Google Scholar] [CrossRef] [PubMed]
- Wang, K.; Wang, L.; Li, M.; Xie, B.; He, L.; Wang, M.; Zhang, R.; Hou, N.; Zhang, Y.; Jia, F. Real-Word Effectiveness of Global COVID-19 Vaccines Against SARS-CoV-2 Variants: A Systematic Review and Meta-Analysis. Front. Med. 2022, 9, 820544. [Google Scholar] [CrossRef]
- Feikin, D.R.; Higdon, M.M.; Abu-Raddad, L.J.; Andrews, N.; Araos, R.; Goldberg, Y.; Groome, M.J.; Huppert, A.; O’Brien, K.L.; Smith, P.G. Duration of effectiveness of vaccines against SARS-CoV-2 infection and COVID-19 disease: Results of a systematic review and meta-regression. Lancet 2022, 399, 924–944. [Google Scholar] [CrossRef]
- Korang, S.K.; von Rohden, E.; Veroniki, A.A.; Ong, G.; Ngalamika, O.; Siddiqui, F.; Juul, S.; Nielsen, E.E.; Feinberg, J.B.; Petersen, J.J.; et al. Vaccines to prevent COVID-19: A living systematic review with Trial Sequential Analysis and network meta-analysis of randomized clinical trials. PLoS ONE 2022, 17, e0260733. [Google Scholar] [CrossRef]
- Sallam, M. COVID-19 Vaccine Hesitancy Worldwide: A Concise Systematic Review of Vaccine Acceptance Rates. Vaccines 2021, 9, 160. [Google Scholar] [CrossRef]
- Zeng, B.; Gao, L.; Zhou, Q.; Yu, K.; Sun, F. Effectiveness of COVID-19 vaccines against SARS-CoV-2 variants of concern: A systematic review and meta-analysis. BMC Med. 2022, 20, 200. [Google Scholar] [CrossRef]
- Chenchula, S.; Karunakaran, P.; Sharma, S.; Chavan, M. Current evidence on efficacy of COVID-19 booster dose vaccination against the Omicron variant: A systematic review. J. Med. Virol. 2022, 94, 2969–2976. [Google Scholar] [CrossRef]
- Fajar, J.K.; Sallam, M.; Soegiarto, G.; Sugiri, Y.J.; Anshory, M.; Wulandari, L.; Kosasih, S.A.P.; Ilmawan, M.; Kusnaeni, K.; Fikri, M.; et al. Global Prevalence and Potential Influencing Factors of COVID-19 Vaccination Hesitancy: A Meta-Analysis. Vaccines 2022, 10, 1356. [Google Scholar] [CrossRef]
- Bono, S.A.; Faria de Moura Villela, E.; Siau, C.S.; Chen, W.S.; Pengpid, S.; Hasan, M.T.; Sessou, P.; Ditekemena, J.D.; Amodan, B.O.; Hosseinipour, M.C.; et al. Factors Affecting COVID-19 Vaccine Acceptance: An International Survey among Low- and Middle-Income Countries. Vaccines 2021, 9, 515. [Google Scholar] [CrossRef] [PubMed]
- Norhayati, M.N.; Yusof, R.C.; Azman, Y.M. Systematic Review and Meta-Analysis of COVID-19 Vaccination Acceptance. Front. Med. 2022, 8, 783982. [Google Scholar] [CrossRef] [PubMed]
- Kanyanda, S.; Markhof, Y.; Wollburg, P.; Zezza, A. Acceptance of COVID-19 vaccines in sub-Saharan Africa: Evidence from six national phone surveys. BMJ Open 2021, 11, e055159. [Google Scholar] [CrossRef] [PubMed]
- Adebisi, Y.A.; Alaran, A.J.; Bolarinwa, O.A.; Akande-Sholabi, W.; Lucero-Prisno, D.E. When it is available, will we take it? Social media users’ perception of hypothetical COVID-19 vaccine in Nigeria. Pan Afr. Med. J. 2021, 38, 230. [Google Scholar] [CrossRef] [PubMed]
- Adedeji-Adenola, H.; Olugbake, O.A.; Adeosun, S.A. Factors influencing COVID-19 vaccine uptake among adults in Nigeria. PLoS ONE 2022, 17, e0264371. [Google Scholar] [CrossRef]
- Oyekale, A.S. Factors Influencing Willingness to Be Vaccinated against COVID-19 in Nigeria. Int. J. Environ. Res. Public Health 2022, 19, 6816. [Google Scholar] [CrossRef]
- Tobin, E.A.; Okonofua, M.; Adeke, A.; Obi, A. Willingness to Accept a COVID-19 Vaccine in Nigeria: A Population-based Cross-sectional Study. Cent. Afr. J. Public Health 2021, 7, 53. [Google Scholar] [CrossRef]
- Al-Ali, D.; Elshafeey, A.; Mushannen, M.; Kawas, H.; Shafiq, A.; Mhaimeed, N.; Mhaimeed, O.; Mhaimeed, N.; Zeghlache, R.; Salameh, M.; et al. Cardiovascular and haematological events post COVID-19 vaccination: A systematic review. J. Cell. Mol. Med. 2021, 26, 636–653. [Google Scholar] [CrossRef]
- Hippisley-Cox, J.; Patone, M.; Mei, X.W.; Saatci, D.; Dixon, S.; Khunti, K.; Zaccardi, F.; Watkinson, P.; Shankar-Hari, M.; Doidge, J.; et al. Risk of thrombocytopenia and thromboembolism after covid-19 vaccination and SARS-CoV-2 positive testing: Self-controlled case series study. BMJ 2021, 374, n1931. [Google Scholar] [CrossRef]
- Kouhpayeh, H.; Ansari, H. Adverse events following COVID-19 vaccination: A systematic review and meta-analysis. Int. Immunopharmacol. 2022, 109, 108906. [Google Scholar] [CrossRef]
- Lau, C.L.; Galea, I. Risk-benefit analysis of COVID-19 vaccines—A neurological perspective. Nat. Rev Neurol. 2022, 18, 69–70. [Google Scholar] [CrossRef] [PubMed]
- Tabong, P.T.; Opoku Mensah, K.; Asampong, E. Preparation for COVID-19 vaccines rollout: Interventions to increase trust, acceptability, and uptake in West African countries. Int. J. Health Plan. Manag. 2022, 37, 1221–1228. [Google Scholar] [CrossRef]
- MacDonald, N.E.; Eskola, J.; Liang, X.; Chaudhuri, M.; Dube, E.; Gellin, B.; Goldstein, S.; Larson, H.; Manzo, M.L.; Reingold, A.; et al. Vaccine Hesitancy: Definition, Scope and Determinants. Vaccine 2015, 33, 4161–4164. [Google Scholar] [CrossRef] [PubMed]
- Pires, C. Global Predictors of COVID-19 Vaccine Hesitancy: A Systematic Review. Vaccines 2022, 10, 1349. [Google Scholar] [CrossRef] [PubMed]
- Sallam, M.; Al-Sanafi, M.; Sallam, M. A Global Map of COVID-19 Vaccine Acceptance Rates per Country: An Updated Concise Narrative Review. J. Multidiscip. Healthc. 2022, 15, 21–45. [Google Scholar] [CrossRef] [PubMed]
- Leach, M.; MacGregor, H.; Akello, G.; Babawo, L.; Baluku, M.; Desclaux, A.; Grant, C.; Kamara, F.; Nyakoi, M.; Parker, M.; et al. Vaccine anxieties, vaccine preparedness: Perspectives from Africa in a COVID-19 era. Soc. Sci. Med. 2022, 298, 114826. [Google Scholar] [CrossRef] [PubMed]
- Dinga, J.N.; Sinda, L.K.; Titanji, V.P.K. Assessment of Vaccine Hesitancy to a COVID-19 Vaccine in Cameroonian Adults and Its Global Implication. Vaccines 2021, 9, 175. [Google Scholar] [CrossRef] [PubMed]
- Faye, S.L.B.; Krumkamp, R.; Doumbia, S.; Tounkara, M.; Strauss, R.; Ouedraogo, H.G.; Sagna, T.; Barry, A.M.; Mbawah, A.K.; Doumbia, C.O.; et al. Factors influencing hesitancy towards adult and child COVID-19 vaccines in rural and urban West Africa: A cross-sectional study. BMJ Open 2022, 12, e059138. [Google Scholar] [CrossRef]
- Ahiakpa, J.K.; Cosmas, N.T.; Anyiam, F.E.; Enalume, K.O.; Lawan, I.; Gabriel, I.B.; Oforka, C.L.; Dahir, H.G.; Fausat, S.T.; Nwobodo, M.A.; et al. COVID-19 vaccines uptake: Public knowledge, awareness, perception and acceptance among adult Africans. PLoS ONE 2022, 17, e0268230. [Google Scholar] [CrossRef]
- Anjorin, A.A.; Odetokun, I.A.; Abioye, A.I.; Elnadi, H.; Umoren, M.V.; Damaris, B.F.; Eyedo, J.; Umar, H.I.; Nyandwi, J.B.; Abdalla, M.M.; et al. Will Africans take COVID-19 vaccination? PLoS ONE 2021, 16, e0260575. [Google Scholar] [CrossRef]
- Katoto, P.D.M.C.; Parker, S.; Coulson, N.; Pillay, N.; Cooper, S.; Jaca, A.; Mavundza, E.; Houston, G.; Groenewald, C.; Essack, Z.; et al. Predictors of COVID-19 Vaccine Hesitancy in South African Local Communities: The VaxScenes Study. Vaccines 2022, 10, 353. [Google Scholar] [CrossRef] [PubMed]
- Nindrea, R.D.; Usman, E.; Katar, Y.; Sari, N.P. Acceptance of COVID-19 vaccination and correlated variables among global populations: A systematic review and meta-analysis. Clin. Epidemiol. Glob. Health 2021, 12, 100899. [Google Scholar] [CrossRef] [PubMed]
- Shah, J.; Abeid, A.; Sharma, K.; Manji, S.; Nambafu, J.; Korom, R.; Patel, K.; Said, M.; Mohamed, M.A.; Sood, M.; et al. Perceptions and Knowledge towards COVID-19 Vaccine Hesitancy among a Subpopulation of Adults in Kenya: An English Survey at Six Healthcare Facilities. Vaccines 2022, 10, 705. [Google Scholar] [CrossRef]
- Mudenda, S.; Hikaambo, C.N.; Daka, V.; Chileshe, M.; Mfune, R.L.; Kampamba, M.; Kasanga, M.; Phiri, M.; Mufwambi, W.; Banda, M.; et al. Prevalence and factors associated with COVID-19 vaccine acceptance in Zambia: A web-based cross-sectional study. Pan Afr. Med. J. 2022, 41, 112. [Google Scholar] [CrossRef]
- Cooper, S.; van Rooyen, H.; Wiysonge, C.S. COVID-19 vaccine hesitancy in South Africa: How can we maximize uptake of COVID-19 vaccines? Expert Rev. Vaccines 2021, 20, 921–933. [Google Scholar] [CrossRef] [PubMed]
- Mundagowa, P.T.; Tozivepi, S.N.; Chiyaka, E.T.; Mukora-Mutseyekwa, F.; Makurumidze, R. Assessment of COVID-19 vaccine hesitancy among Zimbabweans: A rapid national survey. PLoS ONE 2022, 17, e0266724. [Google Scholar] [CrossRef] [PubMed]
- Acheampong, T.; Akorsikumah, E.; Osae-Kwapong, J.; Khalid, M.; Appiah, A.; Amuasi, J. Examining Vaccine Hesitancy in Sub-Saharan Africa: A Survey of the Knowledge and Attitudes among Adults to Receive COVID-19 Vaccines in Ghana. Vaccines 2021, 9, 814. [Google Scholar] [CrossRef]
- Murewanhema, G.; Musuka, G.; Mukwenha, S.; Chingombe, I.; Mapingure, M.P.; Dzinamarira, T. Hesitancy, ignorance or uncertainty? The need for effective communication strategies as Zimbabwe’s uptake of COVID-19 vaccine booster doses remains poor. Public Health Pract. 2022, 3, 100244. [Google Scholar] [CrossRef]
- Nyalile, T.; Loo, L. Situating COVID-19 Vaccine Hesitancy in Tanzania. 2021. Available online: http://somatosphere.net/2021/covid-19-vaccine-hesitancy-tanzania.html/ (accessed on 2 August 2022).
- Sippy, P. Is It Too Late to Fight Covid Skepticism and Vaccine Hesitancy in Tanzania? 2021. Available online: https://qz.com/africa/2055780/covid-skepticism-and-vaccine-hesitancy-is-widespread-in-tanzania/ (accessed on 2 August 2022).
- Ackah, M.; Ameyaw, L.; Salifu, M.G.; Asubonteng, D.P.A.; Yeboah, C.O.; Annor, E.N.; Ankapong, E.A.K.; Boakye, H. COVID-19 vaccine acceptance among health care workers in Africa: A systematic review and meta-analysis. PLoS ONE 2022, 17, e0268711. [Google Scholar] [CrossRef]
- Kanyike, A.M.; Olum, R.; Kajjimu, J.; Ojilong, D.; Akech, G.M.; Nassozi, D.R.; Agira, D.; Wamala, N.K.; Asiimwe, A.; Matovu, D.; et al. Acceptance of the coronavirus disease-2019 vaccine among medical students in Uganda. Trop. Med. Health 2021, 49, 37. [Google Scholar] [CrossRef]
- Kabamba Nzaji, M.; Kabamba Ngombe, L.; Ngoie Mwamba, G.; Banza Ndala, D.B.; Mbidi Miema, J.; Lungoyo, C.L.; Mwimba, B.L.; Bene, A.C.M.; Musenga, E.M. Acceptability of Vaccination Against COVID-19 Among Healthcare Workers in the Democratic Republic of the Congo. Pragmatic Obs. Res. 2020, 11, 103–109. [Google Scholar] [CrossRef] [PubMed]
- World Health Organization (WHO). Ten Threats to Global Health in 2019. 2019. Available online: https://www.who.int/news-room/spotlight/ten-threats-to-global-health-in-2019 (accessed on 15 February 2022).
- Anakpo, G.; Mishi, S. Hesitancy of COVID-19 vaccines: Rapid systematic review of the measurement, predictors, and preventive strategies. Hum. Vaccines Immunother. 2022, 18, 2074716. [Google Scholar] [CrossRef] [PubMed]
- Watson, O.J.; Barnsley, G.; Toor, J.; Hogan, A.B.; Winskill, P.; Ghani, A.C. Global impact of the first year of COVID-19 vaccination: A mathematical modelling study. Lancet Infect. Dis. 2022, 22, P1293–P1302. [Google Scholar] [CrossRef]
- Kricorian, K.; Civen, R.; Equils, O. COVID-19 vaccine hesitancy: Misinformation and perceptions of vaccine safety. Hum. Vaccines Immunother. 2021, 18, 1950504. [Google Scholar] [CrossRef]
- Razai, M.S.; Chaudhry, U.A.R.; Doerholt, K.; Bauld, L.; Majeed, A. Covid-19 vaccination hesitancy. BMJ 2021, 373, n1138. [Google Scholar] [CrossRef] [PubMed]
- Gerretsen, P.; Kim, J.; Caravaggio, F.; Quilty, L.; Sanches, M.; Wells, S.; Brown, E.E.; Agic, B.; Pollock, B.G.; Graff-Guerrero, A. Individual determinants of COVID-19 vaccine hesitancy. PLoS ONE 2021, 16, e0258462. [Google Scholar] [CrossRef]
- Litaker, J.R.; Tamez, N.; Bray, C.L.; Durkalski, W.; Taylor, R. Sociodemographic Factors Associated with Vaccine Hesitancy in Central Texas Immediately Prior to COVID-19 Vaccine Availability. Int. J. Environ. Res. Public Health 2021, 19, 368. [Google Scholar] [CrossRef]
- Kabakama, S.; Konje, E.T.; Dinga, J.N.; Kishamawe, C.; Morhason-Bello, I.; Hayombe, P.; Adeyemi, O.; Chimuka, E.; Lumu, I.; Amuasi, J.; et al. Commentary on COVID-19 Vaccine Hesitancy in sub-Saharan Africa. Trop. Med. Infect. Dis. 2022, 7, 130. [Google Scholar] [CrossRef]
- Chan, N.N.; Ong, K.W.; Siau, C.S.; Lee, K.W.; Peh, S.C.; Yacob, S.; Chia, Y.C.; Seow, V.K.; Ooi, P.B. The lived experiences of a COVID-19 immunization programme: Vaccine hesitancy and vaccine refusal. BMC Public Health 2022, 22, 296. [Google Scholar] [CrossRef]
- Afolabi, A.A.; Ilesanmi, O.S. Dealing with vaccine hesitancy in Africa: The prospective COVID-19 vaccine context. Pan Afr. Med. J. 2021, 38, 3. [Google Scholar] [CrossRef]
- Dzinamarira, T.; Nachipo, B.; Phiri, B.; Musuka, G. COVID-19 Vaccine Roll-Out in South Africa and Zimbabwe: Urgent Need to Address Community Preparedness, Fears and Hesitancy. Vaccines 2021, 9, 250. [Google Scholar] [CrossRef] [PubMed]
- Ekwebelem, O.C.; Yunusa, I.; Onyeaka, H.; Ekwebelem, N.C.; Nnorom-Dike, O. COVID-19 vaccine rollout: Will it affect the rates of vaccine hesitancy in Africa? Public Health 2021, 197, e18–e19. [Google Scholar] [CrossRef]
- Antimicrobial Resistance Collaborators. Global burden of bacterial antimicrobial resistance in 2019: A systematic analysis. Lancet 2022, 399, 629–655. [Google Scholar] [CrossRef]
- Alshaikh, F.S.; Godman, B.; Sindi, O.N.; Seaton, R.A.; Kurdi, A. Prevalence of bacterial coinfection and patterns of antibiotics prescribing in patients with COVID-19: A systematic review and meta-analysis. PLoS ONE 2022, 17, e0272375. [Google Scholar] [CrossRef] [PubMed]
- Founou, R.C.; Blocker, A.J.; Noubom, M.; Tsayem, C.; Choukem, S.P.; Van Dongen, M.; Founou, L.L. The COVID-19 pandemic: A threat to antimicrobial resistance containment. Futur. Sci. OA 2021, 7, FSO736. [Google Scholar] [CrossRef]
- Razai, M.S.; Oakeshott, P.; Esmail, A.; Wiysonge, C.S.; Viswanath, K.; Mills, M.C. COVID-19 vaccine hesitancy: The five Cs to tackle behavioural and sociodemographic factors. J. R. Soc. Med. 2021, 114, 295–298. [Google Scholar] [CrossRef] [PubMed]
- Roy, D.N.; Biswas, M.; Islam, E.; Azam, S. Potential factors influencing COVID-19 vaccine acceptance and hesitancy: A systematic review. PLoS ONE 2022, 17, e0265496. [Google Scholar] [CrossRef]
- Rutten, L.J.F.; Zhu, X.; Leppin, A.L.; Ridgeway, J.L.; Swift, M.D.; Griffin, J.M.; Sauver, J.L.S.; Virk, A.; Jacobson, R.M. Evidence-Based Strategies for Clinical Organizations to Address COVID-19 Vaccine Hesitancy. Mayo Clin. Proc. 2021, 96, 699–707. [Google Scholar] [CrossRef] [PubMed]
- Trogen, B.; Pirofski, L.-A. Understanding vaccine hesitancy in COVID-19. Nat. Med. 2021, 2, 498–501. [Google Scholar] [CrossRef]
- Ekowo, O.E.; Manafa, C.; Isielu, R.C.; Okoli, C.M.; Chikodi, I.; Onwuasoanya, A.F.; Echendu, S.T.; Ihedoro, I.; Nwabueze, U.D.; Nwoke, O.C. A cross sectional regional study looking at the factors responsible for the low COVID-19 vaccination rate in Nigeria. Pan Afr. Med. J. 2022, 41, 114. [Google Scholar] [CrossRef]
- Wilson, S.L.; Wiysonge, C. Social media and vaccine hesitancy. BMJ Glob. Health 2020, 5, e004206. [Google Scholar] [CrossRef] [PubMed]
- Wawrzuta, D.; Klejdysz, J.; Jaworski, M.; Gotlib, J.; Panczyk, M. Attitudes toward COVID-19 Vaccination on Social Media: A Cross-Platform Analysis. Vaccines 2022, 10, 1190. [Google Scholar] [CrossRef] [PubMed]
- Iwu, C.J.; Jordan, P.; Jaja, I.F.; Iwu, C.D.; Wiysonge, C.S. Treatment of COVID-19: Implications for antimicrobial resistance in Africa. Pan Afr. Med. J. 2020, 35 (Suppl. 2), 119. [Google Scholar] [CrossRef] [PubMed]
- Troisi, M.; Andreano, E.; Sala, C.; Kabanova, A.; Rappuoli, R. Vaccines as remedy for antimicrobial resistance and emerging infections. Curr. Opin. Immunol. 2020, 65, 102–106. [Google Scholar] [CrossRef]
- Tagoe, E.T.; Sheikh, N.; Morton, A.; Nonvignon, J.; Sarker, A.R.; Williams, L.; Megiddo, I. COVID-19 Vaccination in Lower-Middle Income Countries: National Stakeholder Views on Challenges, Barriers, and Potential Solutions. Front. Public Health 2021, 9, 709127. [Google Scholar] [CrossRef]
- Godman, B.; Egwuenu, A.; Haque, M.; Malande, O.; Schellack, N.; Kumar, S.; Saleem, Z.; Sneddon, J.; Hoxha, I.; Islam, S.; et al. Strategies to Improve Antimicrobial Utilization with a Special Focus on Developing Countries. Life 2021, 11, 528. [Google Scholar] [CrossRef]
- Godman, B.; Basu, D.; Pillay, Y.; Almeida, P.H.R.F.; Mwita, J.C.; Rwegerera, G.M.; Paramadhas, B.D.A.; Tiroyakgosi, C.; Patrick, O.; Niba, L.L.; et al. Ongoing and planned activities to improve the management of patients with Type 1 diabetes across Africa; implications for the future. Hosp. Prac. 2020, 48, 51–67. [Google Scholar] [CrossRef]
- Godman, B.; Basu, D.; Pillay, Y.; Mwita, J.C.; Rwegerera, G.M.; Paramadhas, B.D.A.; Tiroyakgosi, C.; Okwen, P.M.; Niba, L.L.; Nonvignon, J.; et al. Review of Ongoing Activities and Challenges to Improve the Care of Patients with Type 2 Diabetes Across Africa and the Implications for the Future. Front. Pharmacol. 2020, 11, 108. [Google Scholar] [CrossRef]
- Mwita, J.C.; Ogunleye, O.O.; Olalekan, A.; Kalungia, A.C.; Kurdi, A.; Saleem, Z.; Sneddon, J.; Godman, B. Key Issues Surrounding Appropriate Antibiotic Use for Prevention of Surgical Site Infections in Low- and Middle-Income Countries: A Narrative Review and the Implications. Int. J. Gen. Med. 2021, 14, 515–530. [Google Scholar] [CrossRef]
- Godman, B.; Leong, T.; Abubakar, A.R.; Kurdi, A.; Kalemeera, F.; Rwegerera, G.M.; Patrick, O.; Lum Niba, L.; Ibrahim, K.; Adefolarin, A.A.; et al. Availability and Use of Long-Acting Insulin Analogues Including Their Biosimilars across Africa: Findings and Implications. Intern. Med. 2021, 11, 343. [Google Scholar]
- Godman, B.; Grobler, C.; Van-De-Lisle, M.; Wale, J.; Barbosa, W.B.; Massele, A.; Opondo, P.; Petrova, G.; Tachkov, K.; Sefah, I.; et al. Pharmacotherapeutic interventions for bipolar disorder type II: Addressing multiple symptoms and approaches with a particular emphasis on strategies in lower and middle-income countries. Expert Opin. Pharmacother. 2019, 20, 2237–2255. [Google Scholar] [CrossRef] [PubMed]
- Godman, B.; Egwuenu, A.; Wesangula, E.; Schellack, N.; Kalungia, A.C.; Tiroyakgosi, C.; Kgatlwane, J.; Mwita, J.C.; Patrick, O.; Niba, L.L.; et al. Tackling antimicrobial resistance across sub-Saharan Africa; current challenges and implications for the future. Expert Opin. Drug Saf. 2022, 21, 1089–1111. [Google Scholar] [CrossRef]
- Mudenda, S.; Mukosha, M.; Hikaambo, C.N.; Meyer, J.C.; Fadare, J.; Kampamba, M.; Kalungia, A.C.; Munsaka, S.; Okoro, R.; Daka, V.; et al. Awareness and acceptance of COVID-19 vaccines and associated factors among pharmacy students in Zambia. Malawi Med. J. 2022, 34, 236–243. [Google Scholar]
- Godman, B.; Hill, A.; Simoens, S.; Selke, G.; Selke Krulichová, I.; Zampirolli Dias, C.; Martin, A.P.; Oortwijn, W.; Timoney, A.; Gustafsson, L.L.; et al. Potential approaches for the pricing of cancer medicines across Europe to enhance the sustainability of healthcare systems and the implications. Expert Rev. Pharmacoecon. Outcomes Res. 2021, 21, 527–540. [Google Scholar] [CrossRef] [PubMed]
- Godman, B.; Haque, M.; McKimm, J.; Abu Bakar, M.; Sneddon, J.; Wale, J.; Campbell, S.; Martin, A.P.; Hoxha, I.; Abilova, V.; et al. Ongoing strategies to improve the management of upper respiratory tract infections and reduce inappropriate antibiotic use particularly among lower and middle-income countries: Findings and implications for the future. Curr. Med. Res. Opin. 2019, 36, 301–327. [Google Scholar] [CrossRef] [PubMed]
- Gale, N.K.; Heath, G.; Cameron, E.; Rashid, S.; Redwood, S. Using the framework method for the analysis of qualitative data in multi-disciplinary health research. BMC Med. Res. Methodol. 2013, 13, 117. [Google Scholar] [CrossRef]
- Allemang, B.; Sitter, K.; Dimitropoulos, G. Pragmatism as a paradigm for patient-oriented research. Health Expect. 2021, 25, 38–47. [Google Scholar] [CrossRef]
- Kaushik, V.; Walsh, C.A. Pragmatism as a Research Paradigm and Its Implications for Social Work Research. Soc. Sci. 2019, 8, 255. [Google Scholar] [CrossRef]
- Palinkas, L.A.; Horwitz, S.M.; Green, C.A.; Wisdom, J.P.; Duan, N.; Hoagwood, K. Purposeful Sampling for Qualitative Data Collection and Analysis in Mixed Method Implementation Research. Adm. Policy Ment. Health Ment. Health Serv. Res. 2015, 42, 533–544. [Google Scholar] [CrossRef]
- World Bank. World Bank National Accounts Data—GDP Per Capita (Current US$). Available online: https://data.worldbank.org/indicator/NY.GDP.PCAP.CD (accessed on 11 September 2020).
- Worldometer. African Countries by Population. 2021. Available online: https://www.worldometers.info/population/countries-in-africa-by-population/ (accessed on 7 September 2022).
- The Economist. How We Estimated the True Death Toll of the Pandemic—Dealing with Potential Outcomes, Known Unknowns, and Uncertainty. 2021. Available online: https://www.economist.com/graphic-detail/2021/05/13/how-we-estimated-the-true-death-toll-of-the-pandemic (accessed on 7 September 2022).
- Cox, L.; Yah, C. Estimating actual COVID-19 case numbers using cumulative death count-A method of measuring effectiveness of lockdown of non-essential activities: A South African case study. Pan Afr. Med. J. 2020, 35 (Suppl. 2), 97. [Google Scholar] [CrossRef]
- Bradshaw, D.; Dorrington, R.E.; Laubscher, R.; Moultrie, T.A.; Groenewald, P. Tracking mortality in near to real time provides essential information about the impact of the COVID-19 pandemic in South Africa in 2020. S. Afr. Med J. 2021, 111, 732. [Google Scholar] [CrossRef] [PubMed]
- WHO. COVID-19 Vaccination in the WHO African Region. Monthly Bulletin June 2022. Available online: https://apps.who.int/iris/bitstream/handle/10665/359928/CV-20220714-eng.pdf (accessed on 7 September 2022).
- Ritchie, H.E.; Mathieu, L.; Rodés-Guirao, C.; Appel, C.; Giattino, E.; Ortiz-Ospina, J.; Hasell, B.; Macdonald, D.; Roser, B.A.M. Coronavirus (COVID-19) Vaccinations. 2020. Available online: https://ourworldindata.org/covid-vaccinations (accessed on 28 December 2021).
- Mathieu, E.; Ritchie, H.; Ortiz-Ospina, E.; Roser, M.; Hasell, J.; Appel, C.; Giattino, C.; Rodés-Guirao, L. A global database of COVID-19 vaccinations. Nat. Hum. Behav. 2021, 5, 947–953. [Google Scholar] [CrossRef] [PubMed]
- Rolfe, R.; Kwobah, C.; Muro, F.; Ruwanpathirana, A.; Lyamuya, F.; Bodinayake, C.; Nagahawatte, A.; Piyasiri, B.; Sheng, T.; Bollinger, J.; et al. Barriers to implementing antimicrobial stewardship programs in three low- and middle-income country tertiary care settings: Findings from a multi-site qualitative study. Antimicrob. Resist. Infect. Control 2021, 10, 60. [Google Scholar] [CrossRef] [PubMed]
- Wettermark, B.; Godman, B.; Jacobsson, B.; Haaijer-Ruskamp, F.M. Soft regulations in pharmaceutical policy making: An overview of current approaches and their consequences. Appl. Health Econ. Health Policy 2009, 7, 137–147. [Google Scholar]
- Godman, B. Health authority activities to enhance the quality and efficiency of medicine use and their impact. Adv. Hum. Biol. 2021, 11, 11. [Google Scholar] [CrossRef]
- Moon, J.; Godman, B.; Petzold, M.; Alvarez-Madrazo, S.; Bennett, K.; Bishop, I.; Bucsics, A.; Hesse, U.; Martin, A.; Simoens, S.; et al. Different initiatives across Europe to enhance losartan utilization post generics: Impact and implications. Front. Pharmacol. 2014, 5, 219. [Google Scholar] [CrossRef]
- Godman, B.; Wettermark, B.; Van Woerkom, M.; Fraeyman, J.; Alvarez-Madrazo, S.; Berg, C.; Bishop, I.; Bucsics, A.; Campbell, S.; Finlayson, A.E.; et al. Multiple policies to enhance prescribing efficiency for established medicines in Europe with a particular focus on demand-side measures: Findings and future implications. Front. Pharmacol. 2014, 5, 106. [Google Scholar] [CrossRef]
- Godman, B.; Malmström, R.E.; Diogene, E.; Gray, A.; Jayathissa, S.; Timoney, A.; Acurcio, F.; Alkan, A.; Brzezinska, A.; Bucsics, A.; et al. Are new models needed to optimize the utilization of new medicines to sustain healthcare systems? Expert Rev. Clin. Pharmacol. 2015, 8, 77–94. [Google Scholar]
- Lima-Dellamora, E.D.C.; Caetano, R.; Gustafsson, L.L.; Godman, B.B.; Patterson, K.; Osorio-De-Castro, C.G.S. An Analytical Framework for Assessing Drug and Therapeutics Committee Structure and Work Processes in Tertiary Brazilian Hospitals. Basic Clin. Pharmacol. Toxicol. 2014, 115, 268–276. [Google Scholar] [CrossRef]
- Matsitse, T.B.; Helberg, E.; Meyer, J.C.; Godman, B.; Massele, A.; Schellack, N. Compliance with the primary health care treatment guidelines and the essential medicines list in the management of sexually transmitted infections in correctional centres in South Africa: Findings and implications. Expert Rev. Anti-Infect. Ther. 2017, 15, 963–972. [Google Scholar] [CrossRef]
- Matlala, M.; Gous, A.G.; Godman, B.; Meyer, J. Structure and activities of pharmacy and therapeutics committees among public hospitals in South Africa; findings and implications. Expert Rev. Clin. Pharmacol. 2017, 10, 1273–1280. [Google Scholar] [CrossRef] [PubMed][Green Version]
- Nguyen, T.T.P.; Do, T.X.; Nguyen, H.A.; Nguyen, C.T.T.; Meyer, J.C.; Godman, B.; Skosana, P.; Nguyen, B.T. A National Survey of Dispensing Practice and Customer Knowledge on Antibiotic Use in Vietnam and the Implications. Antibiotics 2022, 11, 1091. [Google Scholar] [CrossRef] [PubMed]
- Alrasheedy, A.A.; Alsalloum, M.A.; Almuqbil, F.A.; Almuzaini, M.A.; Alkhayl, B.S.A.; Albishri, A.S.; Alharbi, F.F.; Alharbi, S.R.; Alodhayb, A.K.; Alfadl, A.A.; et al. The impact of law enforcement on dispensing antibiotics without prescription: A multi-methods study from Saudi Arabia. Expert Rev. Anti-Infect. Ther. 2019, 18, 87–97. [Google Scholar] [CrossRef] [PubMed]
- Godman, B.; Haque, M.; Abubakar, A.R.; Ogunleye, O.O.; Sani, I.H.; Sefah, I.; Kurdi, A.; Islam, S. Changes in availability, utilization, and prices of medicines and protection equipment for COVID-19 in an Urban population of Northern Nigeria. J. Res. Pharm. Prac. 2021, 10, 17–22. [Google Scholar] [CrossRef] [PubMed]
- Gad, M.; Salem, A.; Oortwijn, W.; Hill, R.; Godman, B. Mapping of Current Obstacles for Rationalizing Use of Medicines (CORUM) in Europe: Current Situation and Potential Solutions. Front. Pharmacol. 2020, 11, 144. [Google Scholar] [CrossRef] [PubMed]
- World Health Organization. COVAX. Working for Global Equitable Access to COVID-19 Vaccines. 2020. Available online: https://www.who.int/initiatives/act-accelerator/covax (accessed on 19 February 2021).
- Ritchie, H.; Mathieu, E.; Rodés-Guirao, L.; Appel, C.; Giattino, C.; Ortiz-Ospina, E.; Hasell, J.; Macdonald, B.; Beltekian, D.; Roser, M. Coronavirus Pandemic (COVID-19). 2020. Available online: https://ourworldindata.org/coronavirus (accessed on 7 September 2022).
- Xinhua. Botswana Launches Drive-through COVID-19 Caccination Campaign. 2021. Available online: http://www.news.cn/english/africa/2021-10/13/c_1310241172.htm (accessed on 1 August 2022).
- Reliefweb. Learning from Botswana’s COVID-19 Vaccine Rollout. 2021. Available online: https://reliefweb.int/report/botswana/learning-botswana-s-covid-19-vaccine-rollout (accessed on 1 August 2022).
- Daily News Egypt. Egypt Launches Campaign to Encourage Public to Register for COVID-19 Vaccination. 2021. Available online: https://www.zawya.com/en/life/egypt-launches-campaign-to-encourage-public-to-register-for-covid-19-vaccination-i6pousg2 (accessed on 2 August 2022).
- Saied, S.M.; Saied, E.M.; Kabbash, I.A.; Abdo, S.A.E. Vaccine hesitancy: Beliefs and barriers associated with COVID-19 vaccination among Egyptian medical students. J. Med. Virol. 2021, 93, 4280–4291. [Google Scholar] [CrossRef]
- Qunaibi, E.; Basheti, I.; Soudy, M.; Sultan, I. Hesitancy of Arab Healthcare Workers towards COVID-19 Vaccination: A Large-Scale Multinational Study. Vaccines 2021, 9, 446. [Google Scholar] [CrossRef]
- Nabeth, P.; Hassan, M.; Adib, K.; Abubakar, A.; Brennan, R. New COVID-19 resurgence in the WHO Eastern Mediterranean region. Lancet 2021, 397, 1348–1349. [Google Scholar] [CrossRef]
- Reliefweb. Eswatini: Vaccinating People against COVID-19 in Hard-to-Reach Communities. 2022. Available online: https://reliefweb.int/report/eswatini/eswatini-vaccinating-people-against-covid-19-hard-reach-communities (accessed on 2 August 2022).
- Reliefweb. In Eswatini, Pact Launches App to Fight COVID Misinformation, Vaccine Hesitancy. 2021. Available online: https://reliefweb.int/report/eswatini/eswatini-pact-launches-app-fight-covid-misinformation-vaccine-hesitancy (accessed on 2 August 2022).
- Head, M.; Brackstone, K.; Boateng, L. Vaccine Hesitancy Has Risen in Ghana: A Closer Look at WHO’S Worried. 2021. Available online: https://theconversation.com/vaccine-hesitancy-has-risen-in-ghana-a-closer-look-at-whos-worried-164733 (accessed on 2 August 2022).
- Brackstone, K.; Boateng, L.A.; Atengble, K.; Head, M.; Akinocho, H.; Osei, K.; Nuamah, K. Examining Drivers of COVID-19 Vaccine Hesitancy in Ghana; University of Southampton: Southampton, UK, 2021. [Google Scholar] [CrossRef]
- Alhassan, R.K.; Owusu-Agyei, S.; Ansah, E.K.; Gyapong, M. COVID-19 vaccine uptake among health care workers in Ghana: A case for targeted vaccine deployment campaigns in the global south. Hum. Resour. Health 2021, 19, 136. [Google Scholar] [CrossRef]
- Agyekum, M.W.; Afrifa-Anane, G.F.; Kyei-Arthur, F.; Addo, B. Acceptability of COVID-19 Vaccination among Health Care Workers in Ghana. Adv. Public Health 2021, 2021, 9998176. [Google Scholar] [CrossRef]
- Rufai, N. After Botched Ebola Vaccine Trial, Ghana Struggles with Vaccine Hesitancy. 2021. Available online: https://www.pbs.org/newshour/show/after-botched-ebola-vaccine-trial-ghana-struggles-with-vaccine-hesitancy (accessed on 1 August 2022).
- Afriyie, D.K.; Asare, G.A.; Amponsah, S.K.; Godman, B. COVID-19 pandemic in resource-poor countries: Challenges, experiences and opportunities in Ghana. J. Infect. Dev. Ctries 2020, 14, 838–843. [Google Scholar] [CrossRef] [PubMed]
- Fan, J.; Wang, X.; Du, S.; Mao, A.; Du, H.; Qiu, W. Discussion of the Trust in Vaccination against COVID-19. Vaccines 2022, 10, 1214. [Google Scholar] [CrossRef] [PubMed]
- Osur, J.; Muinga, E.; Carter, J.; Kuria, S.; Hussein, S.; Ireri, E.M. COVID-19 vaccine hesitancy: Vaccination intention and attitudes of community health volunteers in Kenya. PLoS Glob. Public Health 2022, 2, e0000233. [Google Scholar] [CrossRef]
- Orangi, S.; Pinchoff, J.; Mwanga, D.; Abuya, T.; Hamaluba, M.; Warimwe, G.; Austrian, K.; Barasa, E. Assessing the Level and Determinants of COVID-19 Vaccine Confidence in Kenya. Vaccines 2021, 9, 936. [Google Scholar] [CrossRef]
- Oyekale, A.S. Compliance Indicators of COVID-19 Prevention and Vaccines Hesitancy in Kenya: A Random-Effects Endogenous Probit Model. Vaccines 2021, 9, 1359. [Google Scholar] [CrossRef]
- Republic of Kenya Ministry of Health. National COVID-19 Vaccine Deployment Plan, 2021. National Vaccine & Immunization Program—Acceleration of COVID-19 Vaccination Program in Kenya. Available online: https://www.health.go.ke/wp-content/uploads/2021/09/NATIONAL-COVID-19-VACCINE-DEPLOYMENT-PLAN-2021.pdf (accessed on 2 August 2022).
- The World Bank. Rolling Out COVID-19 Vaccines in Malawi Amid Hesitancy and Supply Challenges. 2021. Available online: https://www.worldbank.org/en/news/feature/2021/10/19/rolling-out-covid-19-vaccines-in-malawi-amid-hesitancy-and-supply-challenges (accessed on 1 August 2022).
- WHO Malawi. Malawi Marks One Year of COVID-19 Vaccination, 828, 080 People Receive Full Dose. 2022. Available online: https://www.afro.who.int/countries/malawi/news/malawi-marks-one-year-covid-19-vaccination-828-080-people-receive-full-dose (accessed on 1 August 2022).
- Masina, L. Malawi Fears Its COVID Vaccines Will Expire Due to Hesitancy. 2021. Available online: https://www.voanews.com/a/africa_malawi-fears-its-covid-vaccines-will-expire-due-hesitancy/6219387.html (accessed on 1 August 2022).
- Tembo, L. Tackling COVID-19 Vaccine Misinformation Through Faith Leaders—Faith Leaders Are Key in Behaviour Change. 2022. Available online: https://www.unicef.org/malawi/stories/tackling-covid-19-vaccine-misinformation-through-faith-leaders (accessed on 1 August 2022).
- Ezigbo, O. Nigeria: Tackling Vaccine Hesitancy Fuelled by Misinformation, Propaganda. 2021. Available online: https://allafrica.com/stories/202109230882.html (accessed on 2 August 2022).
- Nomhwange, T.; Wariri, O.; Nkereuwem, E.; Olanrewaju, S.; Nwosu, N.; Adamu, U.; Danjuma, E.; Onuaguluchi, N.; Enegela, J.; Nomhwange, E.; et al. COVID-19 vaccine hesitancy amongst healthcare workers: An assessment of its magnitude and determinants during the initial phase of national vaccine deployment in Nigeria. eClinicalMedicine 2022, 50, 101499. [Google Scholar] [CrossRef]
- Njoga, E.O.; Mshelbwala, P.P.; Abah, K.O.; Awoyomi, O.J.; Wangdi, K.; Pewan, S.B.; Oyeleye, F.A.; Galadima, H.B.; Alhassan, S.A.; Okoli, C.E.; et al. COVID-19 Vaccine Hesitancy and Determinants of Acceptance among Healthcare Workers, Academics and Tertiary Students in Nigeria. Vaccines 2022, 10, 626. [Google Scholar] [CrossRef]
- Iliyasu, Z.; Umar, A.A.; Abdullahi, H.M.; Kwaku, A.A.; Amole, T.G.; Tsiga-Ahmed, F.I.; Garba, R.M.; Salihu, H.M.; Aliyu, M.H. “They have produced a vaccine, but we doubt if COVID-19 exists”: Correlates of COVID-19 vaccine acceptability among adults in Kano, Nigeria. Hum. Vaccines Immunother. 2021, 17, 4057–4064. [Google Scholar] [CrossRef]
- Chukwu, O.A.; Nnogo, C.C. Surmounting inherent challenges in healthcare service delivery for effective procurement and distribution of COVID-19 vaccines; A developing country context. Health Policy Technol. 2021, 10, 100518. [Google Scholar] [CrossRef]
- Nkanjeni, U. Over 50? The Health Department Is Offering You Free Transport to Vaccination Sites. 2021. Available online: https://www.timeslive.co.za/news/south-africa/2021-08-26-over-50-the-health-department-is-offering-you-free-transport-to-vaccination-sites/ (accessed on 2 August 2022).
- Department of Health Republic of South Africa. Vooma Voucher Communication. 2021. Available online: https://sacoronavirus.co.za/vooma-voucher-communication (accessed on 1 August 2022).
- Engelbrecht, M.; Heunis, C.; Kigozi, G. COVID-19 Vaccine Hesitancy in South Africa: Lessons for Future Pandemics. Int. J. Environ. Res. Public Health 2022, 19, 6694. [Google Scholar] [CrossRef]
- Kollamparambil, U.; Oyenubi, A.; Nwosu, C. COVID-19 vaccine intentions in South Africa: Health communication strategy to address vaccine hesitancy. BMC Public Health 2021, 21, 2113. [Google Scholar] [CrossRef] [PubMed]
- Swed, S.; Mohamed, T.; Sakkour, R.; Motawea, K.R.; Bohsas, H. COVID-19 vaccine hesitancy among indigenous people in Sudan: An incipient crisis. Ann. Med. Surg. 2022, 75, 103379. [Google Scholar] [CrossRef] [PubMed]
- Udoh, K. COVID-19 Vaccine Hesitancy in South Sudan; What Lessons Can be Learned From Angola’s Success Story? Am. J. Health Promot. 2022, 36, 579–581. [Google Scholar] [CrossRef] [PubMed]
- Raja, S.M.; Osman, M.E.; Musa, A.O.; Hussien, A.A.; Yusuf, K. COVID-19 vaccine acceptance, hesitancy, and associated factors among medical students in Sudan. PLoS ONE 2022, 17, e0266670. [Google Scholar] [CrossRef]
- Bongomin, F.; Olum, R.; Andia-Biraro, I.; Nakwagala, F.N.; Hassan, K.H.; Nassozi, D.R.; Kaddumukasa, M.; Byakika-Kibwika, P.; Kiguli, S.; Kirenga, B.J. COVID-19 vaccine acceptance among high-risk populations in Uganda. Ther. Adv. Infect. Dis. 2021, 8, 20499361211024376. [Google Scholar] [CrossRef]
- Carcelen, A.C.; Prosperi, C.; Mutembo, S.; Chongwe, G.; Mwansa, F.D.; Ndubani, P.; Simulundu, E.; Chilumba, I.; Musukwa, G.; Thuma, P.; et al. COVID-19 vaccine hesitancy in Zambia: A glimpse at the possible challenges ahead for COVID-19 vaccination rollout in sub-Saharan Africa. Hum. Vaccines Immunother. 2021, 18, 1–6. [Google Scholar] [CrossRef]
- McAbee, L.; Tapera, O.; Kanyangarara, M. Factors Associated with COVID-19 Vaccine Intentions in Eastern Zimbabwe: A Cross-Sectional Study. Vaccines 2021, 9, 1109. [Google Scholar] [CrossRef]
- Dubé, E. Addressing vaccine hesitancy: The crucial role of healthcare providers. Clin. Microbiol. Infect. 2017, 23, 279–280. [Google Scholar] [CrossRef]
- Dror, A.A.; Eisenbach, N.; Taiber, S.; Morozov, N.G.; Mizrachi, M.; Zigron, A.; Srouji, S.; Sela, E. Vaccine hesitancy: The next challenge in the fight against COVID-19. Eur. J. Epidemiol. 2020, 35, 775–779. [Google Scholar] [CrossRef]
- Freeman, D.; Waite, F.; Rosebrock, L.; Petit, A.; Causier, C.; East, A.; Jenner, L.; Teale, A.-L.; Carr, L.; Mulhall, S.; et al. Coronavirus conspiracy beliefs, mistrust, and compliance with government guidelines in England. Psychol. Med. 2020, 52, 251–263. [Google Scholar] [CrossRef]
- Huangfu, L.; Mo, Y.; Zhang, P.; Zeng, D.D.; He, S. COVID-19 Vaccine Tweets After Vaccine Rollout: Sentiment–Based Topic Modeling. J. Med. Internet Res. 2022, 24, e31726. [Google Scholar] [CrossRef] [PubMed]
- Robertson, C.T.; Bentele, K.; Meyerson, B.; Wood, A.S.A.; Salwa, J. Effects of political versus expert messaging on vaccination intentions of Trump voters. PLoS ONE 2021, 16, e0257988. [Google Scholar] [CrossRef] [PubMed]
- Ajayi, O. COVID-19: Nigeria Develops Two Vaccines, Awaits Clinical Trials, Certification. 2021. Available online: https://www.vanguardngr.com/2021/03/covid-19-nigeria-develops-two-vaccines-awaits-clinical-trials-certification-2/ (accessed on 1 August 2022).
- WHO. Pan African Clinical Trials Registry (PACTR). 2022. Available online: https://www.who.int/clinical-trials-registry-platform/network/primary-registries/pan-african-clinical-trials-registry-pactr (accessed on 2 August 2022).
- AHRI. The PAVIA Project Aims to Strengthen Pharmacovigilance (PV) in Four African Countries. 2018. Available online: https://ahri.gov.et/2021/03/04/the-pavia-project-aims-to-strengthen-pharmacovigilance-pv-in-four-african-countries/ (accessed on 2 August 2022).
- Kibuule, D.; Nambahu, L.; Sefah, I.A.; Kurdi, A.; Phuong, T.N.T.; Kwon, H.-Y.; Godman, B. Activities in Namibia to Limit the Prevalence and Mortality from COVID-19 Including Community Pharmacy Activities and the Implications. Sch. Acad. J. Pharm. 2021, 10, 82–92. [Google Scholar] [CrossRef]
- Schellack, N.; Coetzee, M.; Schellack, G.; Gijzelaar, M.; Hassim, Z.; Milne, M.; Bronkhorst, E.; Padayachee, N.; Singh, N.; Kolman, S.; et al. COVID-19: Guidelines for pharmacists in South Africa. S. Afr. J. Infect. Dis. 2020, 35, a206. [Google Scholar] [CrossRef] [PubMed]
- Cadogan, C.A.; Hughes, C.M. On the frontline against COVID-19: Community pharmacists’ contribution during a public health crisis. Res. Soc. Adm. Pharm. 2020, 17, 2032–2035. [Google Scholar] [CrossRef]
- Hedima, E.W.; Adeyemi, M.S.; Ikunaiye, N.Y. WITHDRAWN: Community pharmacists: On the frontline of health service against COVID-19 in LMICs. Res. Soc. Adm. Pharm. 2020. [Google Scholar] [CrossRef]
- Kharel, R.; Baird, J.; Vaishnav, H.; Chillara, N.; Lee, J.A.; Genisca, A.; Hayward, A.; Uzevski, V.; Elbenni, A.; Levine, A.C.; et al. Development and assessment of novel virtual COVID-19 trainer-of trainers course implemented by an academic–humanitarian partnership. Glob. Health Action 2022, 15, 2010391. [Google Scholar] [CrossRef]
- WHO. Second Training of Trainers on Infection Prevention and Control. 2021. Available online: https://www.afro.who.int/pt/node/14623 (accessed on 6 September 2022).
- Xinhua. Skepticism Still Rife Despite Rollout of COVID-19 Vaccine in Zambia. 2021. Available online: https://www.macaubusiness.com/skepticism-still-rife-despite-rollout-of-covid-19-vaccine-in-zambia/ (accessed on 1 August 2022).
- Shaaban, R.; Ghazy, R.M.; Elsherif, F.; Ali, N.; Yakoub, Y.; Aly, M.O.; ElMakhzangy, R.; Abdou, M.S.; McKinna, B.; Elzorkany, A.M.; et al. COVID-19 Vaccine Acceptance among Social Media Users: A Content Analysis, Multi-Continent Study. Int. J. Environ. Res. Public Health 2022, 19, 5737. [Google Scholar] [CrossRef]
- Muric, G.; Wu, Y.; Ferrara, E. COVID-19 Vaccine Hesitancy on Social Media: Building a Public Twitter Data Set of Antivaccine Content, Vaccine Misinformation, and Conspiracies. JMIR Public Health Surveill. 2021, 7, e30642. [Google Scholar] [CrossRef]
- IMF. Seven Finance & Trade Lessons from COVID-19 for Future Pandemics. 2022. Available online: https://www.imf.org/en/Publications/WP/Issues/2022/05/20/Seven-Finance-Trade-Lessons-from-COVID-19-for-Future-Pandemics-517755 (accessed on 2 August 2022).
- Chavula, J. COVID-19 Vaccines on Wheels. 2022. Available online: https://www.unicef.org/malawi/stories/covid-19-vaccines-wheels (accessed on 1 August 2022).
- Rahman, W. Egypt Allocates Mobile COVID-19 Vaccination Clinics for Elderly, Pensioners. 2021. Available online: https://english.aawsat.com/home/article/3008776/egypt-allocates-mobile-covid-19-vaccination-clinics-elderly-pensioners (accessed on 1 August 2022).
- WHO. New Consortium Working to Boost Vaccine Production in South Africa. 2021. Available online: https://www.who.int/news/item/30-07-2021-new-consortium-working-to-boost-vaccine-production-in-south-africa (accessed on 2 August 2022).
- DW. COVID-19: South Africa Develops Own Coronavirus Vaccine. 2021. Available online: https://www.dw.com/en/covid-19-south-africa-develops-own-coronavirus-vaccine/a-60121009 (accessed on 2 August 2022).
- Sun, T. Boosting COVID-19 Vaccine Production in Nigeria, Others. 2022. Available online: https://www.sunnewsonline.com/boosting-covid-19-vaccine-production-in-nigeria-others/ (accessed on 1 August 2022).
- Al-Monitor. Egypt Establishes Largest Coronavirus Vaccine Factory in Middle East. 2021. Available online: https://www.al-monitor.com/originals/2021/09/egypt-establishes-largest-coronavirus-vaccine-factory-middle-east (accessed on 2 August 2022).
- Bloomberg. Aspen’s Covid Flop Bodes Ill for Africa’s Vaccine Making Drive. 2022. Available online: https://www.engineeringnews.co.za/article/aspens-covid-flop-bodes-ill-for-africas-vaccine-making-drive-2022-05-18 (accessed on 6 September 2022).
- Van Nguyen, D.; Nguyen, P.-H. Social media and COVID-19 vaccination hesitancy: The mediating role of the COVID-19 vaccine perception. Heliyon 2022, e10575. [Google Scholar] [CrossRef]
- WHO. COVID-19 and Mandatory Vaccination: Ethical Considerations. 2022. Available online: https://www.who.int/publications/i/item/WHO-2019-nCoV-Policy-brief-Mandatory-vaccination-2022.1 (accessed on 2 August 2022).
- Gibelli, F.; Ricci, G.; Sirignano, A.; De Leo, D. COVID-19 Compulsory Vaccination: Legal and Bioethical Controversies. Front. Med. 2022, 9, 821522. [Google Scholar] [CrossRef] [PubMed]
- Hsu, J. How COVID-19 Is Accelerating the Threat of Antimicrobial Resistance. BMJ 2020, 369, m1983. [Google Scholar] [CrossRef] [PubMed]
- WHO. Strategy to Achieve Global Covid-19 Vaccination by Mid-2022. Available online: https://cdn.who.int/media/docs/default-source/immunization/covid-19/strategy-to-achieve-global-covid-19-vaccination-by-mid-2022.pdf (accessed on 2 August 2022).
- WHO. COVID-19 Vaccination in Africa Increases by Almost Three-Quarters in June 2022. 2022. Available online: https://www.afro.who.int/news/covid-19-vaccination-africa-increases-almost-three-quarters-june-2022 (accessed on 6 September 2022).
- Lassi, Z.; Naseem, R.; Salam, R.; Siddiqui, F.; Das, J. The Impact of the COVID-19 Pandemic on Immunization Campaigns and Programs: A Systematic Review. Int. J. Environ. Res. Public Health 2021, 18, 988. [Google Scholar] [CrossRef] [PubMed]
- Godman, B.; Sefah, I.A.; Kordorwu, H.E.; Essah, D.O.; Kurdi, A. Prevalence rate of spontaneously reported adverse events and determinants of serious adverse events amongst three outpatient care settings in Ghana: Findings and implications. Adv. Hum. Biol. 2021, 11, 97. [Google Scholar] [CrossRef]
- ECA. African Vaccine Acquisition Trust Delivers 108,000 Doses of COVID-19 Vaccine to Botswana. 2021. Available online: https://www.uneca.org/?q=stories/african-vaccine-acquisition-trust-delivers-108%2C000-doses-of-covid-19-vaccine-to-botswana (accessed on 2 August 2022).
- Ndi, N. Cameroon Receives 200,000 Doses of COVID-19 Vaccines from China. 2021. Available online: https://www.theeastafrican.co.ke/tea/rest-of-africa/cameroon-receives-covid-19-vaccines-from-china-3362950 (accessed on 1 August 2022).
- Amani, A.; Djossaya, D.; Njoh, A.A.; Fouda, A.A.B.; Ndoula, S.; Abba-Kabir, H.M.; Mossus, T.; Nguefack-Tsague, G.; Kamgno, J. The first 30 days of COVID-19 vaccination in Cameroon: Achievements, challenges, and lessons learned. Pan Afr. Med. J. 2022, 41, 201. [Google Scholar]
- Unicef Egypt. Egypt Receives 546,400 Doses of COVID-19 Vaccine Donated by France Through AVAT and COVAX Platforms. 2021. Available online: https://www.unicef.org/egypt/press-releases/egypt-receives-546400-doses-covid-19-vaccines-donated-france-through-avat-and-covax (accessed on 2 August 2022).
- Al-Monitor. Spanish Leader Promises COVID-19 Vaccines to Egypt. 2021. Available online: https://www.al-monitor.com/originals/2021/11/spanish-leader-promises-covid-19-vaccines-egypt (accessed on 2 August 2022).
- Reliefweb. Giving 110%: Eswatini’s Early Rollout of COVID-19 Vaccines. 2021. Available online: https://reliefweb.int/report/eswatini/giving-110-eswatini-s-early-rollout-covid-19-vaccines (accessed on 1 August 2022).
- MyJoyOnline. Akufo-Addo, Bawumia, Others Get Vaccinated against COVID-19. 2021. Available online: https://www.myjoyonline.com/livestream-akufo-addo-bawumia-others-get-vaccinated-against-covid-19/ (accessed on 2 August 2022).
- United Nations News. Ghana Receives First Historic Shipment of COVID-19 Vaccinations from International COVAX Facility. 2021. Available online: https://news.un.org/en/story/2021/02/1085572 (accessed on 2 August 2022).
- UNICEF. Another 410,000 COVID-19 Vaccine Doses Arrive in Kenya, Donated by the, U.K. 2021. Available online: https://www.unicef.org/kenya/press-releases/another-410000-covid-19-vaccine-doses-arrive-kenya-donated-uk (accessed on 1 August 2022).
- Njeru, B. Kenya Receives Another Vaccine Donation. 2021. Available online: https://www.standardmedia.co.ke/health/health-science/article/2001417729/kenya-receives-another-vaccine-donation (accessed on 2 August 2022).
- UNICEF. UK Donates COVID-19 Vaccines to Malawi. 2021. Available online: https://www.unicef.org/malawi/press-releases/uk-donates-covid-19-vaccines-malawi (accessed on 1 August 2022).
- UNICEF. Malawi Receives First Shipment of COVID-19 Vaccines from COVAX. 2021. Available online: https://www.unicef.org/malawi/press-releases/malawi-receives-first-shipment-covid-19-vaccines-covax (accessed on 2 August 2022).
- WHO Africa. COVID-19 Vaccines Shipped by COVAX Arrive in Nigeria. 2021. Available online: https://www.afro.who.int/news/covid-19-vaccines-shipped-covax-arrive-nigeria (accessed on 1 August 2022).
- Loembé, M.M.; Nkengasong, J.N. COVID-19 Vaccine Access in Africa: Global Distribution, Vaccine Platforms, and Challenges Ahead. Immunity 2021, 54, 1353–1362. [Google Scholar] [CrossRef]
- Ezigbo, O. Nigeria Receives 501, 600 Doses of COVID-19 Vaccine from France. 2022. Available online: https://www.thisdaylive.com/index.php/2021/10/09/nigeria-receives-501-600-doses-of-covid-19-vaccine-from-france/ (accessed on 2 August 2022).
- Adebowale-Tambe, N. COVID-19: Italian Govt Donates over Three Million Doses of Vaccine to Nigeria. 2022. Available online: https://www.premiumtimesng.com/news/top-news/523255-covid-19-italian-govt-donates-over-three-million-doses-of-vaccine-to-nigeria.html (accessed on 1 August 2022).
- Premium Times. COVID-19: Japanese Govt Donates over 800,000 Doses of AstraZeneca Vaccine to Nigeria. 2022. Available online: https://headtopics.com/ng/covid-19-japanese-govt-donates-over-800-000-doses-of-astrazeneca-vaccine-to-nigeria-24433360 (accessed on 1 August 2022).
- Chocomilo, S. Spain Donates 4.4m COVID-19 Vaccines To Nigeria. 2022. Available online: https://www.withinnigeria.com/news/2022/05/26/spain-donates-4-4m-covid-19-vaccines-to-nigeria/ (accessed on 2 August 2022).
- US Mission. U.S. Donates an Additional 2.5 Million Doses of COVID-19 Vaccines to Nigeria This Week. 2021. Available online: https://ng.usembassy.gov/u-s-donates-an-additional-2-5-million-doses-of-covid-19-vaccines-to-nigeria-this-week/ (accessed on 2 August 2022).
- Adepegba, A. India Donates 100,000 Doses of COVID-19 Vaccines to Nigeria. 2021. Available online: https://punchng.com/india-donates-100000-doses-of-covid-19-vaccines-to-nigeria/ (accessed on 1 August 2022).
- Unicef Sudan. Sudan Joins the COVAX Facility to Ensure Equitable Access to COVID-19 Vaccines—Frequently Asked Questions about COVAX and Sudan’s Participation. 2021. Available online: https://www.unicef.org/sudan/stories/sudan-joins-covax-facility-ensure-equitable-access-covid-19-vaccines (accessed on 2 August 2022).
- Ryeng, H. The First COVID-19 Vaccines Have Arrived in Tanzania—An Important Milestone in the Fight against COVID-19. 2021. Available online: https://www.unicef.org/tanzania/stories/first-covid-19-vaccines-have-arrived-tanzania (accessed on 1 August 2022).
- Africanews. Tanzania Receives 500,000 Sinopharm Vaccines from China. 2021. Available online: https://www.africanews.com/2021/11/03/tanzania-receives-500-000-sinopharm-vaccines-from-china/ (accessed on 2 August 2022).
- Kamoga, J. Uganda to Roll Out First Round of COVID-19 Vaccine on March 10. 2021. Available online: https://www.theeastafrican.co.ke/tea/science-health/uganda-to-roll-out-first-round-jabs-3315226 (accessed on 1 August 2022).
- UNICEF. Uganda to Benefit from UK COVID-19 Vaccines Donation. 2021. Available online: https://www.unicef.org/uganda/press-releases/uganda-benefit-uk-covid-19-vaccines-donation (accessed on 2 August 2022).
- The Independent. Uganda Receives COVID-19 Vaccine Donation from India. 2021. Available online: https://www.independent.co.ug/uganda-receives-covid-19-vaccine-donation-from-india/ (accessed on 1 August 2022).
- James, J. COVID-19 Vaccines Shipped by COVAX Arrive in Zambia—Donation by France; COVAX Local Press Statement on Arrival of 228,000 Vaccines in Zambia. 2021. Available online: https://www.unicef.org/zambia/press-releases/covid-19-vaccines-shipped-covax-arrive-zambia-donation-france (accessed on 2 August 2022).
- Madhi, S.A.; Baillie, V.; Cutland, C.L.; Voysey, M.; Koen, A.L.; Fairlie, L.; Padayachee, S.D.; Dheda, K.; Barnabas, S.L.; Bhorat, Q.E.; et al. Efficacy of the ChAdOx1 nCoV-19 COVID-19 Vaccine against the B.1.351 Variant. N. Engl. J. Med. 2021, 384, 1885–1898. [Google Scholar] [CrossRef]
- Sisonke Programme—Sisonke Study Protecting Healthcare Workers. 2021. Available online: https://sisonkestudy.samrc.ac.za/indexsisonke.html (accessed on 1 August 2022).
- SAMRC. Vast Majority of Breakthrough Infections in Vaccinated Health Workers Are Mild. 2021. Available online: https://www.samrc.ac.za/media-release/vast-majority-breakthrough-infections-vaccinated-health-workers-are-mild (accessed on 1 August 2022).
- APA-Mbabane. Eswatini Adds AstraZeneca to COVID-19 Booster Doses. 2022. Available online: http://apanews.net/en/news/eswatini-adds-astrazeneca-to-covid-19-booster-doses/ (accessed on 2 August 2022).
- Wikipedia. COVID-19 Vaccination in Ghana. 2021. Available online: https://en.wikipedia.org/wiki/COVID-19_vaccination_in_Ghana (accessed on 1 August 2022).
- Larbie, S. GHS Begins Administering COVID-19 Vaccine Booster Shots. 2022. Available online: https://www.gna.org.gh/1.21323473 (accessed on 2 August 2022).
- Saya, M. Kenya Starts Giving COVID-19 Vaccine Booster Shots. 2021. Available online: https://www.the-star.co.ke/news/2021-12-25-kenya-starts-giving-covid-19-vaccine-booster-shots/ (accessed on 1 August 2022).
- Kalekye, M. Kenya Administers 114,007 Covid Booster Jabs. 2022. Available online: https://www.kbc.co.ke/kenya-administers-114007-covid-booster-jabs/ (accessed on 2 August 2022).
- Silas, D. FG Govt Approves COVID-19 Vaccines Booster for Nigerians. 2021. Available online: https://dailypost.ng/2021/12/04/fg-govt-approves-covid-19-vaccines-booster-for-nigerians/ (accessed on 1 August 2022).
- The Independent. Uganda Alters COVID-19 Vaccine Roll-Out Plan to Cover More People. 2021. Available online: https://www.independent.co.ug/uganda-alters-covid-19-vaccine-roll-out-plan-to-cover-more-people/ (accessed on 2 August 2022).
- Nabatanzi, V. COVID-19: Govt to Roll Out Vaccination to Children. 2022. Available online: https://www.bukedde.co.ug/health/130937/covid-19-govt-to-roll-out-vaccination-to-chil (accessed on 1 August 2022).
- Unicef Uganda. Country Office Annual Report 2021. Available online: https://www.unicef.org/media/116466/file/Uganda-2021-COAR.pdf (accessed on 2 August 2022).
- AllAfrica. Uganda: Health Ministry Approves COVID-19 Booster Shots for Ugandans. 2021. Available online: https://allafrica.com/stories/202112280071.html (accessed on 1 August 2022).
- Jere, J. Booster Jab Available in All Public Health Centers. 2021. Available online: https://www.znbc.co.zm/news/booster-jab-available-in-all-public-health-centers/ (accessed on 2 August 2022).
- Cajnewsafrica. Zimbabwe Takes Lead in COVID-19 Rollout. 2021. Available online: https://www.cajnewsafrica.com/2021/08/05/zimbabwe-takes-lead-in-covid-19-rollout/ (accessed on 1 August 2022).
- Gonye, V. Govt Gives Guidelines on Booster Shots. 2021. Available online: https://www.newsday.co.zw/2021/12/govt-gives-guidelines-on-booster-shots/ (accessed on 2 August 2022).
| Country | Population Size (Thousands) | GDP/Capita (US$) | Accumulated Infection Rate (Thousands) | Accumulated Mortality Rate (Thousands) |
|---|---|---|---|---|
| Botswana | 2351.63 | 6711.0 | 325.5 | 2.77 |
| Cameroon | 26,545.86 | 1499.4 | 121.0 | 1.93 |
| Egypt | 102,260.0 | 4028.4 | 515.3 | 1.93 |
| Eswatini | 1160.16 | 3415.5 | 73.3 | 1.42 |
| Ghana | 31,072.94 | 2328.5 | 168.5 | 1.46 |
| Kenya | 53,771.30 | 1838.2 | 338.1 | 5.67 |
| Malawi | 19,129.95 | 625.3 | 87.7 | 2.67 |
| Nigeria | 206,139.60 | 2097.1 | 263.1 | 3.15 |
| South Africa | 59,308.69 | 5090.7 | 4010.2 | 102.1 |
| Sudan | 48,892.81 | 595 | 63.2 | 4.96 |
| Tanzania | 61,498.44 | 1136 | 38.7 | 0.84 |
| Uganda | 47,123.53 | 858 | 168.7 | 3.63 |
| Zambia | 18,383.96 | 1050.9 | 332.5 | 4.02 |
| Zimbabwe | 14,862.92 | 1128.2 | 256.6 | 5.59 |
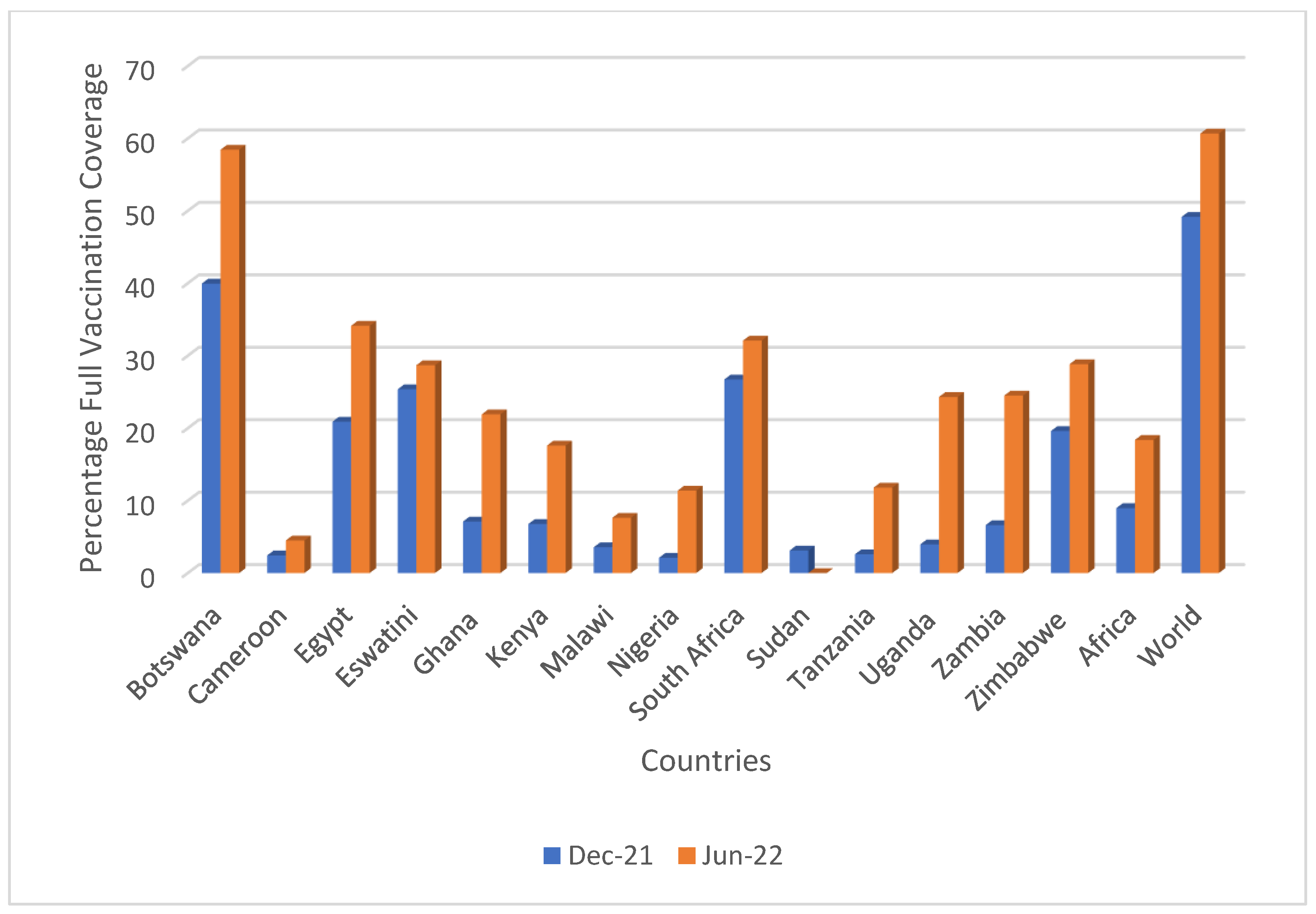
| Country | Vaccination Coverage—31 December 2021—% of the Total Population | Vaccination Coverage—30 June 2022—% of the Total Population | ||
|---|---|---|---|---|
| Full (Completed) | Partial | Full (Completed) | Partial | |
| Botswana | 39.9 | 5.2 | 58.4 | 7.1 |
| Cameroon | 2.4 | 0.6 | 4.5 | 1.3 |
| Egypt | 20.9 | 11.5 | 34.1 | 12.0 |
| Eswatini | 25.4 | 2.7 | 28.7 | 5.7 |
| Ghana | 7.1 | 10.5 | 21.9 | 9.9 |
| Kenya | 6.8 | 4.4 | 17.6 | 6.3 |
| Malawi | 3.5 | 3.96 | 7.63 | 3.05 |
| Nigeria | 2.1 | 2.7 | 11.4 | 5.6 |
| South Africa | 26.7 | 5.2 | 32.1 | 5.0 |
| Sudan | 3.1 | 3.7 | 10.4 | NA |
| Tanzania | 2.3 | 0.7 | 11.8 | 2.2 |
| Uganda | 3.9 | 18.8 | 24.3 | 11.1 |
| Zambia | 6.6 | NA | 24.5 | 35.0 |
| Zimbabwe | 19.6 | 6.2 | 28.8 | 10.6 |
| Africa | 8.9 | 4.9 | 18.4 | 5.2 |
| World | 49.2 | 8.5 | 60.7 | 5.5 |
| Countries | Doses as of 31 December 2021 | Doses as of 30 June 2022 |
|---|---|---|
| Botswana | NA | 2.73 million |
| Cameroon | 1.02 million | 1.85 million |
| Egypt | 57.49 million | 91.45 million |
| Eswatini | 404,374 | 684,176 |
| Ghana | 7.76 million | 18.24 million |
| Kenya | 10.12 million | 18.54 million |
| Malawi | 1.8 million | 3.17 million |
| Nigeria | 14.84 million | 55.47 million |
| South Africa | 27.97 million | 36.82 million |
| Sudan | 3.64 million | NA |
| Tanzania | 2.43 million | 12.07 million |
| Uganda | 12.09 million | 21.76 million |
| Zambia | 1.73 million | 7.2 million |
| Zimbabwe | 7.26 million | 11.97 million |
| Africa | 303.51 million | 550.21 million |
| World | 9.18 billion | 12.1 billion |
| Country | Access, Acceptance, Hesitancy and Challenges |
|---|---|
| Botswana [161,162] | Access:
|
| Cameroon [82,143,144] | Access:
|
| Egypt [85,163,164,165,166] | Access:
Vaccine hesitancy has been reported in many studies across Egypt due to a number of reasons. These include:
|
| Eswatini [167,168] | Access:
|
| Ghana [15,92,169,170,171,172,173,174] | Access:
|
| Kenya [120,175,176,177,178,179] | Access:
|
| Malawi [180,181,182,183] | Access:
|
| Nigeria [184,185,186,187,188] | Access:
|
| South Africa [90,189,190,191,192] | Access:
|
| Sudan [193,194,195] | Access:
|
| Tanzania | Access:
|
| Uganda [68,81,196] | Access:
|
| Zambia [89,131,197] | Access:
|
| Zimbabwe [93,106,109,175,198] | Access:
|
| Key Activities | Ways Forward |
|---|---|
| Research activities |
|
| Education | |
| Healthcare professionals (HCPs) |
|
| Medical journalists and other key influencers |
|
| General Public |
|
| Communication strategies |
|
| Engineering | |
| Access and availability [216] |
|
| Economics | |
| Patient Incentives |
|
| Local production |
|
| Financial support | |
| Enforcement | |
| Compulsory vaccination [225,226] |
|
| Health system |
|
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2022 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Ogunleye, O.O.; Godman, B.; Fadare, J.O.; Mudenda, S.; Adeoti, A.O.; Yinka-Ogunleye, A.F.; Ogundele, S.O.; Oyawole, M.R.; Schönfeldt, M.; Rashed, W.M.; et al. Coronavirus Disease 2019 (COVID-19) Pandemic across Africa: Current Status of Vaccinations and Implications for the Future. Vaccines 2022, 10, 1553. https://doi.org/10.3390/vaccines10091553
Ogunleye OO, Godman B, Fadare JO, Mudenda S, Adeoti AO, Yinka-Ogunleye AF, Ogundele SO, Oyawole MR, Schönfeldt M, Rashed WM, et al. Coronavirus Disease 2019 (COVID-19) Pandemic across Africa: Current Status of Vaccinations and Implications for the Future. Vaccines. 2022; 10(9):1553. https://doi.org/10.3390/vaccines10091553
Chicago/Turabian StyleOgunleye, Olayinka O., Brian Godman, Joseph O. Fadare, Steward Mudenda, Adekunle O. Adeoti, Adesola F. Yinka-Ogunleye, Sunday O. Ogundele, Modupe R. Oyawole, Marione Schönfeldt, Wafaa M. Rashed, and et al. 2022. "Coronavirus Disease 2019 (COVID-19) Pandemic across Africa: Current Status of Vaccinations and Implications for the Future" Vaccines 10, no. 9: 1553. https://doi.org/10.3390/vaccines10091553
APA StyleOgunleye, O. O., Godman, B., Fadare, J. O., Mudenda, S., Adeoti, A. O., Yinka-Ogunleye, A. F., Ogundele, S. O., Oyawole, M. R., Schönfeldt, M., Rashed, W. M., Galal, A. M., Masuka, N., Zaranyika, T., Kalungia, A. C., Malande, O. O., Kibuule, D., Massele, A., Chikowe, I., Khuluza, F., ... Meyer, J. C. (2022). Coronavirus Disease 2019 (COVID-19) Pandemic across Africa: Current Status of Vaccinations and Implications for the Future. Vaccines, 10(9), 1553. https://doi.org/10.3390/vaccines10091553












