Adopting a High-Polyphenolic Diet Is Associated with an Improved Glucose Profile: Prospective Analysis within the PREDIMED-Plus Trial
Abstract
1. Introduction
2. Materials and Methods
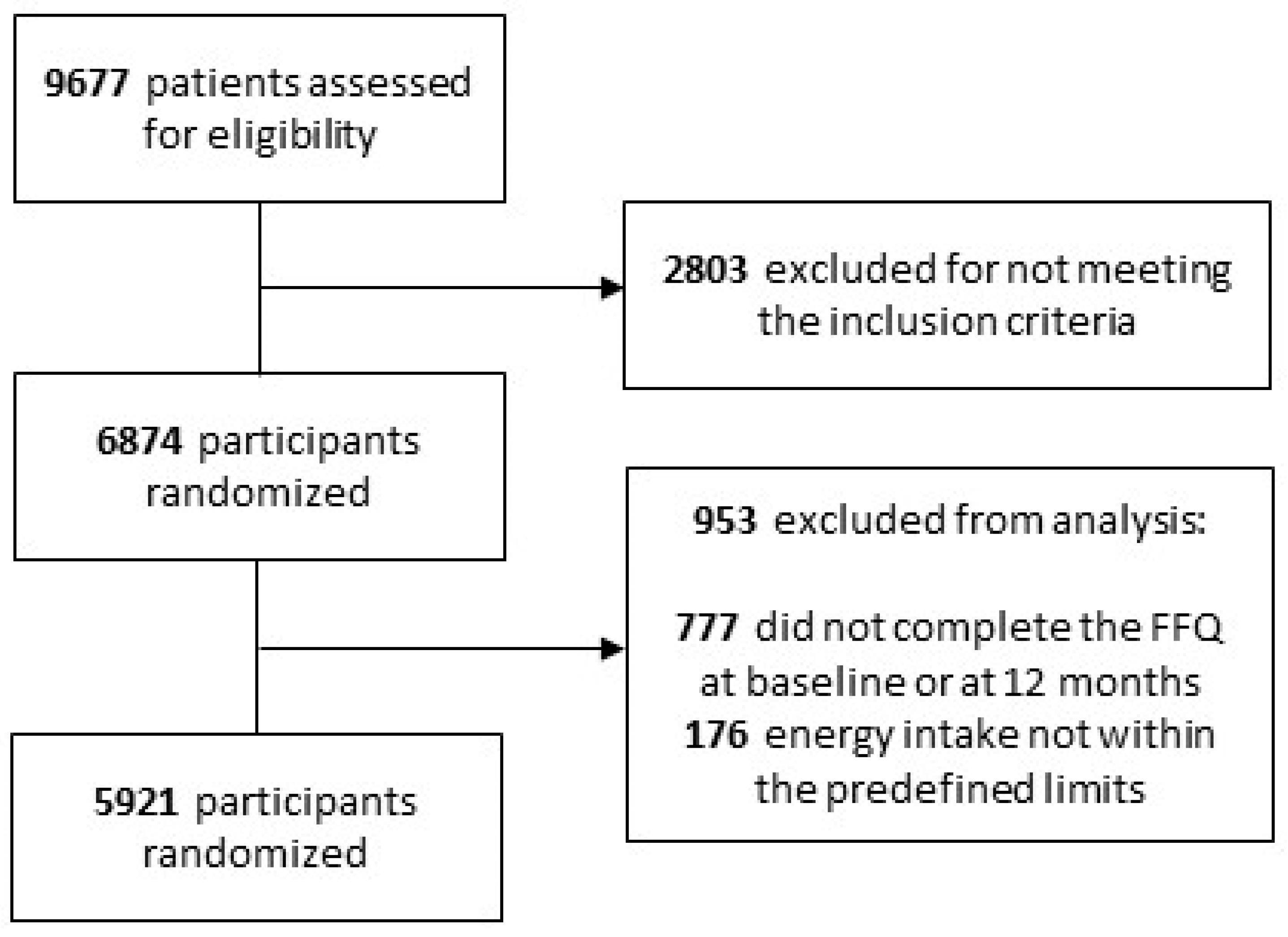
2.1. Study Design and Participants
2.2. Dietary Assessment and Polyphenol Intake
2.3. Ascertainment of the Endpoints
2.4. Assessment of Covariates
2.5. Statistical Analyses
3. Results
4. Discussion
4.1. Anthocyanidins
4.2. Proanthocyanidins
4.3. Flavones
4.4. Flavonols
4.5. Hydroxybenzoic and Hydroxycinnamic Acids
4.6. Lignans
4.7. Stilbenes
4.8. Effect Modification by Diabetes Status
4.9. Strengths and Limitations
5. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Acknowledgments
Conflicts of Interest
References
- The World Health Organization Global Report on Diabetes; WHO: Geneva, Switzerland, 2016; ISBN 9789241565257.
- Martín-Peláez, S.; Fito, M.; Castaner, O. Mediterranean Diet Effects on Type 2 Diabetes Prevention, Disease Progression, and Related Mechanisms. A Review. Nutrients 2020, 12, 2236. [Google Scholar] [CrossRef] [PubMed]
- Ley, S.; Hamdy, O.; Mohan, V.; Hu, F. Prevention and management of type 2 diabetes: Dietary components and nutritional strategies. Lancet 2014, 383, 1999–2007. [Google Scholar] [CrossRef]
- Manach, C.; Scalbert, A.; Morand, C.; Rémésy, C.; Jiménez, L. Polyphenols: Food sources and bioavailability. Am. J. Clin. Nutr. 2004, 79, 727–747. [Google Scholar] [CrossRef] [PubMed]
- Kim, Y.; Keogh, J.; Clifton, P. Polyphenols and Glycemic Control. Nutrients 2016, 8, 17. [Google Scholar] [CrossRef]
- Guasch-Ferré, M.; Merino, J.; Sun, Q.; Fitó, M.; Salas-Salvadó, J. Dietary Polyphenols, Mediterranean Diet, Prediabetes, and Type 2 Diabetes: A Narrative Review of the Evidence. Oxid. Med. Cell. Longev. 2017, 2017. [Google Scholar] [CrossRef]
- Martínez-González, M.; Buil-Cosiales, P.; Corella, D.; Bulló, M.; Fitó, M.; Vioque, J.; Romaguera, D.; Martínez, J.A.; Wärnberg, J.; López-Miranda, J.; et al. Cohort Profile: Design and methods of the PREDIMED-Plus randomized trial. Int. J. Epidemiol. 2019, 48, 387–388. [Google Scholar] [CrossRef]
- Salas-Salvadó, J.; Díaz-López, A.; Ruiz-Canela, M.; Basora, J.; Fitó, M.; Corella, D.; Serra-Majem, L.; Wärnberg, J.; Romaguera, D.; Estruch, R.; et al. Effect of a Lifestyle Intervention Program With Energy-Restricted Mediterranean Diet and Exercise on Weight Loss and Cardiovascular Risk Factors: One-Year Results of the PREDIMED-Plus Trial. Diabetes Care 2019, 42, 777–788. [Google Scholar] [CrossRef]
- Alberti, K.; Eckel, R.; Grundy, S.; Zimmet, P.; Cleeman, J.; Donato, K.A.; Fruchart, J.-C.; James, W.P.T.; Loria, C.M.; Smith, S.C., Jr.; et al. Harmonizing the Metabolic Syndrome: A Joint Interim Statement of the International Diabetes Federation Task Force on Epidemiology and Prevention; National Heart, Lung, and Blood Institute; American Heart Association; World Heart Federation; International Atherosclerosis Society; and International Association for the Study of Obesity. Circulation 2009, 120, 1640–1645. [Google Scholar] [CrossRef]
- Jenkins, D.; Kendall, C.; McKeown-Eyssen, G.; Josse, R.; Silverberg, J.; Booth, G.; Vidgen, E.; Josse, A.; Nguyen, T.H.; Corrigan, S.; et al. Effect of a low-glycemic index or a high-cereal fiber diet on type 2 diabetes: A randomized trial. JAMA 2008, 300, 2742–2753. [Google Scholar] [CrossRef]
- Fernández-Ballart, J.; Piñol, J.; Zazpe, I.; Corella, D.; Carrasco, P.; Toledo, E.; Perez-Bauer, M.; Martínez-González, M.Á.; Salas-Salvadó, J.; Martín-Moreno, J.M. Relative validity of a semi-quantitative food-frequency questionnaire in an elderly Mediterranean population of Spain. Br. J. Nutr. 2010, 103, 1808–1816. [Google Scholar] [CrossRef]
- Mataix, J. Tablas de Composición de Alimentos [Food Composition Aables], 4th ed.; Universidad de Granada: Granada, Spain, 2003. [Google Scholar]
- Schröder, H.; Zomeño, M.D.; Martínez-González, M.A.; Salas-Salvadó, J.; Corella, D.; Vioque, J.; Romaguera, D.; Martínez, J.A.; Tinahones, F.J.; Miranda, J.L.; et al. Validity of the energy-restricted Mediterranean Diet Adherence Screener. Clin. Nutr. 2021. [Google Scholar] [CrossRef] [PubMed]
- Willett, W.C.; Howe, G.R.; Kushi, L.H. Adjustment for total energy intake in epidemiologic studies. Am. J. Clin. Nutr. 1997, 65, 1220S–1228S; discussion 1229S–1231S. [Google Scholar] [CrossRef] [PubMed]
- Molina, L.; Sarmiento, M.; Peñafiel, J.; Donaire, D.; Garcia-Aymerich, J.; Gomez, M.; Ble, M.; Ruiz, S.; Frances, A.; Schröder, H.; et al. Validation of the regicor short physical activity questionnaire for the adult population. PLoS ONE 2017, 12, e0168148. [Google Scholar] [CrossRef] [PubMed]
- Gavin, J.R.; Alberti, K.G.M.M.; Davidson, M.B.; DeFronzo, R.A.; Drash, A.; Gabbe, S.G.; Genuth, S.; Harris, M.I.; Kahn, R.; Keen, H.; et al. Report of the Expert Committee on the Diagnosis and Classification of Diabetes Mellitus. Diabetes Care 2003, 26, s5–s20. [Google Scholar] [CrossRef]
- Xiao, J.; Högger, P. Dietary polyphenols and type 2 diabetes: Current insights and future perspectives. Curr. Med. Chem. 2015, 22, 23–38. [Google Scholar] [CrossRef] [PubMed]
- Yang, L.; Ling, W.; Yang, Y.; Chen, Y.; Tian, Z.; Du, Z.; Chen, J.; Xie, Y.; Liu, Z.; Yang, L. Role of Purified Anthocyanins in Improving Cardiometabolic Risk Factors in Chinese Men and Women with Prediabetes or Early Untreated Diabetes-A Randomized Controlled Trial. Nutrients 2017, 9, 1104. [Google Scholar] [CrossRef] [PubMed]
- Tresserra-Rimbau, A.; Castro-Barquero, S.; Vitelli-Storelli, F.; Becerra-Tomas, N.; Vázquez-Ruiz, Z.; Díaz-López, A.; Corella, D.; Castañer, O.; Romaguera, D.; Vioque, J.; et al. Associations between Dietary Polyphenols and Type 2 Diabetes in a Cross-Sectional Analysis of the PREDIMED-Plus Trial: Role of Body Mass Index and Sex. Antioxidants 2019, 8, 537. [Google Scholar] [CrossRef]
- Guo, X.; Yang, B.; Tan, J.; Jiang, J.; Li, D. Associations of dietary intakes of anthocyanins and berry fruits with risk of type 2 diabetes mellitus: A systematic review and meta-analysis of prospective cohort studies. Eur. J. Clin. Nutr. 2016, 70, 1360–1367. [Google Scholar] [CrossRef]
- Chambers, B.; Camire, M. Can cranberry supplementation benefit adults with type 2 diabetes? Diabetes Care 2003, 26, 2695–2696. [Google Scholar] [CrossRef]
- Hsia, D.; Zhang, D.; Beyl, R.; Greenway, F.; Khoo, C. Effect of daily consumption of cranberry beverage on insulin sensitivity and modification of cardiovascular risk factors in adults with obesity: A pilot, randomised, placebo-controlled study. Br. J. Nutr. 2020, 124, 577–585. [Google Scholar] [CrossRef]
- Novotny, J.; Baer, D.; Khoo, C.; Gebauer, S.; Charron, C. Cranberry juice consumption lowers markers of cardiometabolic risk, including blood pressure and circulating C-reactive protein, triglyceride, and glucose concentrations in adults. J. Nutr. 2015, 145, 1185–1193. [Google Scholar] [CrossRef] [PubMed]
- Tresserra-Rimbau, A.; Guasch-Ferré, M.; Salas-Salvadó, J.; Toledo, E.; Corella, D.; Castañer, O.; Guo, X.; Gómez-Gracia, E.; Lapetra, J.; Arós, F.; et al. Intake of Total Polyphenols and Some Classes of Polyphenols Is Inversely Associated with Diabetes in Elderly People at High Cardiovascular Disease Risk. J. Nutr. 2015, 146, 767–777. [Google Scholar] [CrossRef]
- Zamora-Ros, R.; Forouhi, N.G.; Sharp, S.J.; González, C.A.; Buijsse, B.; Guevara, M.; van der Schouw, Y.T.; Amiano, P.; Boeing, H.; Bredsdorff, L.; et al. The association between dietary flavonoid and lignan intakes and incident type 2 diabetes in European populations: The EPIC-InterAct study. Diabetes Care 2013, 36, 3961–3970. [Google Scholar] [CrossRef] [PubMed]
- Jacques, P.F.; Cassidy, A.; Rogers, G.; Peterson, J.J.; Meigs, J.B.; Dwyer, J.T. Higher dietary flavonol intake is associated with lower incidence of type 2 diabetes. J. Nutr. 2013, 143, 1474–1480. [Google Scholar] [CrossRef] [PubMed]
- Komorita, Y.; Iwase, M.; Fujii, H.; Ohkuma, T.; Ide, H.; Jodai-Kitamura, T.; Yoshinari, M.; Oku, Y.; Higashi, T.; Nakamura, U.; et al. Additive effects of green tea and coffee on all-cause mortality in patients with type 2 diabetes mellitus: The Fukuoka Diabetes Registry. BMJ Open Diabetes Res. Care 2020, 8. [Google Scholar] [CrossRef]
- Shahinfar, H.; Jayedi, A.; Khan, T.; Shab-Bidar, S. Coffee consumption and cardiovascular diseases and mortality in patients with type 2 diabetes: A systematic review and dose-response meta-analysis of cohort studies. Nutr. Metab. Cardiovasc. Dis. 2021, 31, 2526–2538. [Google Scholar] [CrossRef]
- Salas-Salvadó, J.; Martinez-González, M.Á.; Bulló, M.; Ros, E. The role of diet in the prevention of type 2 diabetes. Nutr. Metab. Cardiovasc. Dis. 2011, 21 (Suppl. S2). [Google Scholar] [CrossRef]
- Lane, J.; Barkauskas, C.; Surwit, R.; Feinglos, M. Caffeine impairs glucose metabolism in type 2 diabetes. Diabetes Care 2004, 27, 2047–2048. [Google Scholar] [CrossRef][Green Version]
- Hameed, A.; Galli, M.; Adamska-Patruno, E.; Krętowski, A.; Ciborowski, M. Select Polyphenol-Rich Berry Consumption to Defer or Deter Diabetes and Diabetes-Related Complications. Nutritions 2020, 12, 2538. [Google Scholar] [CrossRef]
- Sun, Q.; Wedick, N.; Pan, A.; Townsend, M.; Cassidy, A.; Franke, A.; Rimm, E.; Hu, F.; van Dam, R. Gut microbiota metabolites of dietary lignans and risk of type 2 diabetes: A prospective investigation in two cohorts of U.S. women. Diabetes Care 2014, 37, 1287–1295. [Google Scholar] [CrossRef]
- Pan, A.; Sun, J.; Chen, Y.; Ye, X.; Li, H.; Yu, Z.; Wang, Y.; Gu, W.; Zhang, X.; Chen, X.; et al. Effects of a flaxseed-derived lignan supplement in type 2 diabetic patients: A randomized, double-blind, cross-over trial. PLoS ONE 2007, 2, e1148. [Google Scholar] [CrossRef] [PubMed]
- Zhang, W.; Wang, X.; Liu, Y.; Tian, H.; Flickinger, B.; Empie, M.; Sun, S. Dietary flaxseed lignan extract lowers plasma cholesterol and glucose concentrations in hypercholesterolaemic subjects. Br. J. Nutr. 2008, 99, 1301–1309. [Google Scholar] [CrossRef] [PubMed]
- Eriksen, A.K.; Brunius, C.; Mazidi, M.; Hellström, P.M.; Risérus, U.; Iversen, K.N.; Fristedt, R.; Sun, L.; Huang, Y.; Nørskov, N.P.; et al. Effects of whole-grain wheat, rye, and lignan supplementation on cardiometabolic risk factors in men with metabolic syndrome: A randomized crossover trial. Am. J. Clin. Nutr. 2020, 111, 864–876. [Google Scholar] [CrossRef] [PubMed]
- Barre, D.; Mizier-Barre, K.; Stelmach, E.; Hobson, J.; Griscti, O.; Rudiuk, A.; Muthuthevar, D. Flaxseed lignan complex administration in older human type 2 diabetics manages central obesity and prothrombosis-an invitation to further investigation into polypharmacy reduction. J. Nutr. Metab. 2012, 2012. [Google Scholar] [CrossRef]
- Barre, D.; Mizier-Barre, K. Lignans’ Potential in Pre and Post-onset Type 2 Diabetes Management. Curr. Diabetes Rev. 2019, 16, 2–11. [Google Scholar] [CrossRef]
- Liu, K.; Zhou, R.; Wang, B.; Mi, M. Effect of resveratrol on glucose control and insulin sensitivity: A meta-analysis of 11 randomized controlled trials. Am. J. Clin. Nutr. 2014, 99, 1510–1519. [Google Scholar] [CrossRef]
- Martin, M.; Goya, L.; Ramos, S. Protective effects of tea, red wine and cocoa in diabetes. Evidences from human studies. Food Chem. Toxicol. 2017, 109, 302–314. [Google Scholar] [CrossRef]
- Salinero-Fort, M.; Carrillo-de Santa, E.; Arrieta-Blanco, F.; Abanades-Herranz, J.; Martín-Madrazo, C.; Rodés-Soldevila, B.; De Burgos-Lunar, C. Effectiveness of PRECEDE model for health education on changes and level of control of HbA1c, blood pressure, lipids, and body mass index in patients with type 2 diabetes mellitus. BMC Public Health 2011, 11, 267. [Google Scholar] [CrossRef]
- FDA Guidance for Industry Diabetes Mellitus-Evaluating Cardiovascular Risk in New Antidiabetic Therapies to Treat Type 2 Diabetes; U.S. Department of Health and Human Services Food and Drug Administration Center for Drug Evaluation and Research (CDER): Silver Spring, MD, USA, 2008.
- Koudoufio, M.; Desjardins, Y.; Feldman, F.; Spahis, S.; Delvin, E.; Levy, E. Insight into Polyphenol and Gut Microbiota Crosstalk: Are Their Metabolites the Key to Understand Protective Effects against Metabolic Disorders? Antioxidants 2020, 9, 982. [Google Scholar] [CrossRef]
- Yassour, M.; Lim, M.Y.; Yun, H.S.; Tickle, T.L.; Sung, J.; Song, Y.-M.; Lee, K.; Franzosa, E.A.; Morgan, X.C.; Gevers, D.; et al. Sub-clinical detection of gut microbial biomarkers of obesity and type 2 diabetes. Genome Med. 2016, 8, 1–14. [Google Scholar] [CrossRef]
- Bocanegra, A.; Macho-González, A.; Garcimartín, A.; Benedí, J.; Sánchez-Muniz, F.J. Whole Alga, Algal Extracts, and Compounds as Ingredients of Functional Foods: Composition and Action Mechanism Relationships in the Prevention and Treatment of Type-2 Diabetes Mellitus. Int. J. Mol. Sci. 2021, 22, 3816. [Google Scholar] [CrossRef] [PubMed]
- Wang, Y.; Alkhalidy, H.; Liu, D. The Emerging Role of Polyphenols in the Management of Type 2 Diabetes. Molecules 2021, 26, 703. [Google Scholar] [CrossRef] [PubMed]
- Tresserra-Rimbau, A.; Lamuela-Raventos, R.; Moreno, J. Polyphenols, food and pharma. Current knowledge and directions for future research. Biochem. Pharmacol. 2018, 156, 186–195. [Google Scholar] [CrossRef] [PubMed]

| Tertiles of Δ Polyphenol Intake after 1 Year | ||||
|---|---|---|---|---|
| Change of polyphenol intake (mg/day), median (min to max) | T1 −249 (−2400 to −106) | T2 1.52 (−106 to 107) | T3 256 (107 to 1400) | P |
| No. of subjects | 1974 | 1974 | 1973 | |
| Allocated in the intervention group | 901 (45.6) | 955 (48.4) | 1044 (52.9) | <0.001 |
| Age (years), mean ± SD | 65.2 ± 4.9 | 65.0 ± 4.8 | 64.9 ± 4.9 | 0.09 |
| Women, n (%) | 987 (50.0) | 971 (49.2) | 898 (45.5) | 0.01 |
| Education, n (%) | ||||
| Primary school | 981 (49.7) | 971 (49.2) | 990 (50.2) | 0.11 |
| High school | 545 (27.6) | 606 (30.7) | 550 (27.9) | |
| University | 448 (22.7) | 397 (20.1) | 433 (21.9) | |
| Current smoker, n (%) | ||||
| Baseline | 243 (12.3) | 242 (12.2) | 250 (12.7) | 0.06 |
| After 1 year | 205 (11.9) | 202 (11.9) | 214 (13.3) | 0.45 |
| Physical activity (METS.min/week), mean ± SD | ||||
| Baseline | 2543 ± 2283 | 2454 ± 2329 | 2527 ± 2353 | 0.34 |
| 1-year change | 518 ± 2480 * | 506 ± 2363 * | 567 ± 2433 * | 0.70 |
| Diabetes status | ||||
| Nondiabetic participants | 384 (19.5) | 432 (21.9) | 415 (21.0) | 0.36 |
| Pre-diabetic participants | 981 (49.7) | 950 (48.1) | 941 (47.7) | |
| Diabetic participants | 609 (30.9) | 592 (30.0) | 617 (31.3) | |
| Glucose (mg/dL), mean ± SD | ||||
| Baseline | 113.67 ± 28.70 | 112.18 ± 29.08 | 114.29 ± 28.97 | 0.06 |
| 1-year change | −2.41 ± 20.92 * | −1.59 ± 23.13 | −3.4 ± 23.04 * | 0.04 |
| HbA1c (%), mean ± SD | ||||
| Baseline | 6.12 ± 0.87 | 6.08 ± 0.87 | 6.11 ± 0.83 | 0.25 |
| 1-year change | −0.09 ± 0.53 * | −0.05 ± 0.53 | −0.09 ± 0.57 * | 0.07 |
| Tertiles of Δ Polyphenol Intake after 1 Year | |||||
|---|---|---|---|---|---|
| T1 −249 (−2400 to −106) | T2 1.52 (−106 to 107) | T3 256 (107 to 1400) | P | Adjusted P | |
| No. of subjects | 1974 | 1974 | 1973 | ||
| Total energy (Kcal/d) | |||||
| Baseline | 2382 ± 547 | 2289 ± 541 | 2430 ± 552 | <0.001 | <0.001 |
| 1-year change | −128.7 ± 524.8 | −135.1 ± 483.5 | −194.4 ± 541.7 | 0.002 | <0.001 |
| Carbohydrates (g/d) | |||||
| Baseline | 246 ± 73 | 231 ± 71 | 245 ± 73 | <0.001 | <0.001 |
| 1-year change | −34.7 ± 70.0 | −29.2 ± 66.0 | −31.6 ± 75.6 | 0.05 | <0.001 |
| Fiber (g/d) | |||||
| Baseline | 29 ± 10 | 25 ± 8 | 25 ± 8 | <0.001 | <0.001 |
| 1-year change | 0.5 ± 9.7 | 3.6 ± 8.3 | 6.8 ± 9.1 | <0.001 | <0.001 |
| Proteins (g/d) | |||||
| Baseline | 98 ± 22 | 96 ± 22 | 99 ± 22 | <0.001 | <0.001 |
| 1-year change | −1.2 ± 21.8 | −2.1 ± 20.8 | −4.0 ± 22.1 | <0.001 | <0.001 |
| MUFA (g/d) | |||||
| Baseline | 53 ± 16 | 53 ± 16 | 56 ± 16 | <0.001 | <0.001 |
| 1-year change | 7.0 ± 18.4 | 4.6 ± 16.8 | 1.9 ± 18.2 | <0.001 | <0.001 |
| PUFA (g/d) | |||||
| Baseline | 18 ± 6 | 17 ± 6 | 19 ± 7 | <0.001 | <0.001 |
| 1-year change | 1.7 ± 7.2 | 1.0 ± 6.8 | 0.1 ± 7.3 | <0.001 | <0.001 |
| SFA (Kcal/d) | |||||
| Baseline | 26 ± 9 | 25 ± 8 | 27 ± 9 | <0.001 | <0.001 |
| 1-year change | −2.5 ± 8.1 | −3.3 ± 7.3 | −4.8 ± 8.2 | <0.001 | <0.001 |
| Alcohol (g/d) | |||||
| Baseline | 11 ± 14 | 11 ± 15 | 12 ± 16 | 0.05 | 0.31 |
| 1-year change | −2.0 ± 11.3 | −1.2 ± 10 | −0.5 ± 11.8 | <0.001 | <0.001 |
| 17-points MedDiet score | |||||
| Baseline | 8.86 ± 2.7 | 8.45 ± 2.63 | 8.22 ± 2.65 | <0.001 | <0.001 |
| 1-year change | 2.6 ± 3.1 | 3.3 ± 3.2 | 3.9 ± 3.3 | <0.001 | <0.001 |
| Food items, g/day | |||||
| Vegetables | |||||
| Baseline | 348 ± 146 | 326 ± 136 | 313 ± 127 | <0.001 | <0.001 |
| 1-year change | 6.4 ± 153.5 | 32.0 ± 143.7 | 60.7 ± 146.8 | <0.001 | <0.001 |
| Fruits | |||||
| Baseline | 430 ± 240 | 341 ± 179 | 308 ± 167 | <0.001 | <0.001 |
| 1-year change | −58.5 ± 236.0 | 42.2 ± 177.9 | 146.9 ± 204.4 | <0.001 | <0.001 |
| Legumes | |||||
| Baseline | 21 ± 11 | 20 ± 11 | 20 ± 11 | 0.001 | <0.001 |
| 1-year change | 3.8 ± 13.6 | 4.6 ± 13.1 | 4.1 ± 13.3 | 0.15 | 0.04 |
| Cereals | |||||
| Baseline | 146 ± 77 | 145 ± 74 | 161 ± 82 | <0.001 | <0.001 |
| 1-year change | −15.4 ± 82.0 | −23.1 ± 76.6 | −35.2 ± 88.1 | <0.001 | <0.001 |
| Dairy | |||||
| Baseline | 348 ± 206 | 336 ± 193 | 349 ± 203 | 0.07 | 0.05 |
| 1-year change | −11.8 ± 191.7 | −19.9 ± 177.2 | −27.7 ± 193.4 | 0.03 | <0.001 |
| Meat | |||||
| Baseline | 144 ± 57 | 146 ± 57 | 153 ± 61 | <0.001 | <0.001 |
| 1-year change | −8.6 ± 57.1 | −16.1 ± 55.3 | −24.1 ± 57.0 | <0.001 | <0.001 |
| Olive oil | |||||
| Baseline | 39 ± 16 | 40 ± 17 | 42 ± 17 | <0.001 | <0.001 |
| 1-year change | 6.8 ± 18.9 | 4.7 ± 17.7 | 1.4 ± 19.1 | <0.001 | <0.001 |
| Fish | |||||
| Baseline | 105 ± 47 | 101 ± 47 | 101 ± 47 | 0.02 | 0.02 |
| 1-year change | 8.1 ± 53.0 | 10.1 ± 50.7 | 9.7 ± 50.3 | 0.43 | 0.30 |
| Nuts | |||||
| Baseline | 16 ± 17 | 14 ± 17 | 15 ± 17 | 0.04 | 0.04 |
| 1-year change | 13.8 ± 23.1 | 13.3 ± 21.0 | 14.3 ± 22.1 | 0.37 | 0.29 |
| Cookies, pastries, and sweets | |||||
| Baseline | 30 ± 31 | 23 ± 27 | 27 ± 31 | <0.001 | <0.001 |
| 1-year change | −14.7 ± 29.7 | −10.4 ± 26.4 | −11.6 ± 31.2 | <0.001 | <0.001 |
| Sugar | |||||
| Baseline | 6 ± 12 | 7 ± 12 | 7 ± 12 | 0.32 | 0.62 |
| 1-year change | −2.5 ± 9.8 | −3.1 ± 10.0 | −3.6 ± 10.8 | 0.003 | <0.001 |
| Soft drinks | |||||
| Baseline | 20 ± 59 | 21 ± 64 | 23 ± 66 | 0.16 | 0.27 |
| 1-year change | −7.0 ± 67.8 | −10.4 ± 64.1 | −12.9 ± 77.9 | 0.03 | 0.004 |
| T1 (vs. T2) | P | T2 | T3 (vs. T2) | P | T3 (vs. T1) | P | P-Trend | ||
|---|---|---|---|---|---|---|---|---|---|
| Total polyphenols | −249 (−2400, −106) a | 2 (−106, 107) | 257 (107, 1400) | ||||||
| Glucose | Model 1 | −2.56 (−3.46, −1.66) b | <0.001 | ref. | −2.34 (−3.24, −1.44) | <0.001 | 0.22 (−0.74, 1.18) | 0.66 | 0.12 |
| Model 2 | −2.78 (−3.72, −1.84) | <0.001 | ref. | −2.56 (−3.51, −1.61) | <0.001 | 0.23 (−0.78, 1.23) | 0.62 | 0.33 | |
| Model 3 | −0.94 (−2.36, 0.48) | 0.19 | ref. | −1.76 (−3.18, −0.34) | 0.015 | −0.82 (−2.24, 0.61) | 0.23 | 0.43 | |
| HbA1c | Model 1 | 0.015 (−0.008, 0.037) | 0.19 | ref. | 0.008 (−0.015, 0.031) | 0.50 | −0.007 (−0.031, 0.018) | 0.55 | 0.76 |
| Model 2 | 0.011 (−0.012, 0.034) | 0.35 | ref. | 0.001 (−0.023, 0.025) | 0.92 | −0.01 (−0.035, 0.016) | 0.44 | 0.80 | |
| Model 3 | −0.039 (−0.076, −0.002) | 0.04 | ref. | −0.032 (−0.069, 0.005) | 0.09 | 0.007 (−0.031, 0.044) | 0.36 | 0.46 | |
| Total flavonoids | −195 (−2405, −78) | 3 (−78, 84) | 193 (84, 1383) | ||||||
| Glucose | Model 1 | 0.46 (−0.45, 1.37) | 0.32 | ref. | −0.6 (−1.51, 0.31) | 0.20 | −1.06 (−2.04, −0.07) | 0.04 | 0.16 |
| Model 2 | 0.01 (−0.95, 0.96) | 0.99 | ref. | −0.79 (−1.75, 0.18) | 0.11 | −0.79 (−1.83, 0.24) | 0.14 | 0.16 | |
| Model 3 | 0.17 (−1.25, 1.59) | 0.81 | ref. | −1.39 (−2.82, 0.04) | 0.06 | −1.56 (−2.99, −0.13) | 0.03 | 0.16 | |
| HbA1c | Model 1 | −0.029 (−0.052, −0–006) | 0.014 | ref. | −0.033 (−0.057, −0.01) | 0.006 | −0.004 (−0.029, 0.021) | 0.79 | 0.42 |
| Model 2 | −0.019 (−0.043, 0.005) | 0.12 | ref. | −0.021 (−0.045, 0.004) | 0.09 | −0.002 (−0.027, 0.024) | 0.95 | 0.23 | |
| Model 3 | −0.024 (−0.061, 0.013) | 0.21 | ref. | −0.024 (−0.061, 0.013) | 0.20 | −0.001 (−0.038, 0.037) | 0.99 | 0.72 | |
| Anthocyanidins | −25 (−526, −10) | 0 (−10, 10) | 25 (10, 209) | ||||||
| Glucose | Model 1 | 1.87 (0.96, 2.78) | <0.001 | ref. | 1.72 (0.81, 2.63) | <0.001 | −0.15 (−1.1, 0.8) | 0.76 | 0.05 |
| Model 2 | 1.42 (0.46, 2.37) | 0.004 | ref. | 1.74 (0.77, 2.70) | <0.001 | 0.32 (−0.68, 1.32) | 0.56 | 0.03 | |
| Model 3 | 0.06 (−1.36, 1.48) | 0.93 | ref. | −0.43 (−1.86, 1.00) | 0.56 | −0.49 (−1.92, 0.94) | 0.50 | 0.89 | |
| HbA1c | Model 1 | 0.024 (0.001, 0.047) | 0.04 | ref. | −0.026 (−0.05, −0.003) | 0.03 | −0.05 (−0.075, −0.025) | <0.001 | 0.83 |
| Model 2 | 0.019 (−0.004, 0.043) | 0.11 | ref. | −0.019 (−0.044, 0.005) | 0.12 | −0.039 (−0.064, −0.013) | 0.003 | 0.35 | |
| Model 3 | −0.028 (−0.065, 0.009) | 0.14 | ref. | −0.037 (−0.075, 0.000) | 0.05 | −0.009 (−0.047, 0.028) | 0.66 | 0.62 | |
| Catechins | −14 (−162, −5) | 0 (−5, 6) | 14 (6, 176) | ||||||
| Glucose | Model 1 | −0.46 (−1.35, 0.42) | 0.31 | ref. | 0.25 (−0.65, 1.14) | 0.59 | 0.71 (−0.2, 1.61) | 0.12 | 0.77 |
| Model 2 | 0.00 (−0.93, 0.93) | 0.99 | ref. | 0.29 (−0.64, 1.23) | 0.54 | 0.29 (−0.66, 1.24) | 0.55 | 0.51 | |
| Model 3 | 0.76 (−0.66, 2.17) | 0.30 | ref. | −0.11 (−1.53, 1.31) | 0.90 | −0.87 (−2.29, 0.55) | 0.23 | 0.27 | |
| HbA1c | Model 1 | 0.038 (0.016, 0.06) | 0.001 | ref. | 0.029 (0.006, 0.052) | 0.01 | −0.009 (−0.032, 0.014) | 0.36 | 0.89 |
| Model 2 | 0.044 (0.021, 0.067) | <0.001 | ref. | 0.028 (0.004, 0.051) | 0.02 | −0.017 (−0.04, 0.007) | 0.15 | 0.90 | |
| Model 3 | 0.008 (−0.028, 0.045) | 0.65 | ref. | −0.019 (−0.057, 0.018) | 0.30 | −0.028 (−0.065, 0.009) | 0.14 | 0.35 | |
| Proanthocyanidins | −122 (−2169, −48) | −4 (−48, 40) | 106 (40, 1207) | ||||||
| Glucose | Model 1 | 1.97 (1.07, 2.87) | <0.001 | ref. | 0.27 (−0.63, 1.18) | 0.55 | −1.7 (−2.64, −0.75) | <0.001 | 0.10 |
| Model 2 | 1.15 (0.19, 2.11) | 0.02 | ref. | −0.35 (−1.31, 0.61) | 0.47 | −1.51 (−2.5, −0.51) | 0.003 | 0.01 | |
| Model 3 | 1.13 (−0.29, 2.55) | 0.12 | ref. | −0.15 (−1.58, 1.29) | 0.84 | −1.28 (−2.71, 0.15) | 0.08 | 0.61 | |
| HbA1c | Model 1 | 0.031 (0.008, 0.054) | 0.009 | ref. | −0.015 (−0.039, 0.008) | 0.20 | −0.046 (−0.071, −0.022) | <0.001 | 0.001 |
| Model 2 | 0.031 (0.007, 0.055) | 0.01 | ref. | −0.014 (−0.038, 0.011) | 0.28 | −0.044 (−0.07, −0.019) | 0.001 | <0.001 | |
| Model 3 | −0.012 (−0.049, 0.025) | 0.51 | ref. | −0.02 (−0.058, 0.018) | 0.30 | −0.008 (−0.045, 0.030) | 0.70 | 0.56 | |
| Flavanones | −42 (−554, −5) | 13 (−5, 36) | 77 (36, 860) | ||||||
| Glucose | Model 1 | −1.48 (−2.38, −0.58) | 0.001 | ref. | −2.27 (−3.19, −1.35) | <0.001 | −0.79 (−1.76, 0.18) | 0.11 | 0.75 |
| Model 2 | −1.37 (−2.31, −0.43) | 0.004 | ref. | −2.52 (−3.49, −1.55) | <0.001 | −1.15 (−2.16, −0.15) | 0.04 | 0.30 | |
| Model 3 | 0.53 (−0.88, 1.95) | 0.46 | ref. | −0.33 (−1.75, 1.09) | 0.65 | −0.86 (−2.28, 0.56) | 0.24 | 0.38 | |
| HbA1c | Model 1 | −0.026 (−0.048, −0.003) | 0.02 | ref. | 0.019 (−0.004, 0.043) | 0.11 | 0.045 (0.021, 0.07) | <0.001 | <0.001 |
| Model 2 | −0.013 (−0.036, 0.010) | 0.28 | ref. | 0.011 (−0.013, 0.036) | 0.36 | 0.024 (−0.001, 0.05) | 0.06 | 0.02 | |
| Model 3 | −0.015 (−0.052, 0.022) | 0.43 | ref. | 0.007 (−0.030, 0.044) | 0.71 | 0.022 (−0.015, 0.059) | 0.25 | 0.10 | |
| Flavones | −21 (−305, 1) | 13 (1, 30) | 55 (30, 344) | ||||||
| Glucose | Model 1 | 0.71 (−0.2, 1.63) | 0.12 | ref. | −0.46 (−1.44, 0.52) | 0.36 | −1.17 (−2.19, −0.16) | 0.02 | 0.007 |
| Model 2 | 1.05 (0.08, 2.02) | 0.03 | ref. | −0.09 (−1.12, 0.94) | 0.86 | −1.14 (−2.2, −0.08) | 0.03 | 0.008 | |
| Model 3 | −1.2 (−2.64, 0.23) | 0.10 | ref. | −1.56 (−3.02, −0.11) | 0.62 | −1.56 (−3.02, −0.11) | 0.04 | 0.20 | |
| HbA1c | Model 1 | −0.053 (−0.076, −0.029) | <0.001 | ref. | −0.026 (−0.051, 0.000) | 0.05 | 0.027 (0.001, 0.053) | 0.019 | <0.001 |
| Model 2 | −0.045 (−0.07, −0.021) | <0.001 | ref. | −0.024 (−0.05, 0.003) | 0.08 | 0.022 (−0.005, 0.049) | 0.06 | <0.001 | |
| Model 3 | −0.015 (−0.053, 0.022) | 0.41 | ref. | −0.049 (−0.087, −0.012) | 0.01 | −0.034 (−0.072, 0.004) | 0.08 | 0.12 | |
| Flavonols | −15 (−103, −4) | 4 (−4, 12) | 26 (12, 177) | ||||||
| Glucose | Model 1 | −1.59 (−2.5, −0.67) | 0.001 | ref. | 1.4 (0.44, 2.36) | 0.004 | 2.99 (1.96, 4.01) | <0.001 | 0.51 |
| Model 2 | −1.4 (−2.37, −0.44) | 0.004 | ref. | 1.3 (0.3, 2.3) | 0.01 | 2.7 (1.63, 3.78) | <0.001 | 0.85 | |
| Model 3 | 0.13 (−1.29, 1.55) | 0.86 | ref. | −1.36 (−2.78, 0.06) | 0.06 | −1.49 (−2.93, −0.05) | 0.04 | 0.03 | |
| HbA1c | Model 1 | 0.019 (−0.004, 0.042) | 0.11 | ref. | −0.053 (−0.077, −0.029) | <0.001 | −0.072 (−0.098, −0.045) | <0.001 | <0.001 |
| Model 2 | 0.017 (−0.007, 0.04) | 0.17 | ref. | −0.036 (−0.061, −0.011) | 0.004 | −0.053 (−0.08, −0.026) | <0.001 | 0.05 | |
| Model 3 | −0.005 (−0.042, 0.033) | 0.81 | ref. | −0.073 (−0.11, −0.036) | <0.001 | −0.069 (−0.106, −0.031) | <0.001 | 0.003 | |
| Hydroxycinnamic acids | −103 (−725, −32) | −3 (−32, 26) | 93 (26, 739) | ||||||
| Glucose | Model 1 | −3.07 (−3.96, −2.19) | <0.001 | ref. | −1.28 (−2.17, −0.38) | 0.005 | 1.8 (0.86, 2.73) | <0.001 | <0.001 |
| Model 2 | −3.24 (−4.17, −2.3) | <0.001 | ref. | −1.28 (−2.22, −0.34) | 0.007 | 1.96 (0.97, 2.94) | <0.001 | <0.001 | |
| Model 3 | −0.94 (−2.36, 0.47) | 0.19 | ref. | −0.26 (−1.68, 1.16) | 0.72 | 0.69 (−0.74, 2.11) | 0.34 | 0.47 | |
| HbA1c | Model 1 | −0.015 (−0.037, 0.007) | 0.18 | ref. | 0.02 (−0.003, 0.042) | 0.09 | 0.035 (0.011, 0.059) | 0.004 | 0.41 |
| Model 2 | −0.018 (−0.041, 0.006) | 0.14 | ref. | 0.016 (−0.007, 0.039) | 0.18 | 0.034 (0.009, 0.058) | 0.008 | 0.85 | |
| Model 3 | −0.04 (−0.077, −0.004) | 0.03 | ref. | −0.021 (−0.058, 0.016) | 0.26 | 0.019 (−0.018, 0.057) | 0.31 | 0.40 | |
| Hydroxybenzoic acids | −13 (−55, −7) | −4.4 (−7, −1) | 3.3 (−1, 64) | ||||||
| Glucose | Model 1 | 0.13 (−0.73, 0.99) | 0.77 | ref. | −0.06 (−0.94, 0.82) | 0.89 | −0.19 (−1.14, 0.76) | 0.70 | 0.79 |
| Model 2 | 0.27 (−0.63, 1.18) | 0.55 | ref. | 0.04 (−0.88, 0.96) | 0.93 | −0.23 (−1.22, 0.76) | 0.64 | 0.93 | |
| Model 3 | −0.1 (−1.53, 1.33) | 0.89 | ref. | 0.33 (−1.09, 1.76) | 0.65 | 0.44 (−1.02, 1.89) | 0.56 | 0.80 | |
| HbA1c | Model 1 | −0.038 (−0.06, −0.016) | 0.001 | ref. | −0.027 (−0.049, −0.004) | 0.02 | 0.011 (−0.013, 0.036) | 0.32 | 0.77 |
| Model 2 | −0.035 (−0.058, −0.013) | 0.002 | ref. | −0.028 (−0.051, −0.005) | 0.016 | 0.007 (−0.018, 0.032) | 0.53 | 0.70 | |
| Model 3 | 0.001 (−0.036, 0.038) | 0.96 | ref. | 0.007 (−0.03, 0.044) | 0.70 | 0.006 (−0.032, 0.044) | 0.75 | 0.77 | |
| Lignans | −0.4 (−7,2, −0.1) | 0.1 (−0.1, 0.3) | 0.5 (0.3, 5.8) | ||||||
| Glucose | Model 1 | 0.27 (−0.67, 1.2) | 0.58 | ref. | 0.63 (−0.31, 1.58) | 0.19 | 0.37 (−0.66, 1.4) | 0.50 | 0.05 |
| Model 2 | 0.33 (−0.65, 1.3) | 0.52 | ref. | 0.49 (−0.52, 1.49) | 0.34 | 0.16 (−0.91, 1.23) | 0.59 | 0.006 | |
| Model 3 | 0.54 (−0.89, 1.96) | 0.46 | ref. | −1.08 (−2.51, 0.35) | 0.14 | −1.62 (−3.07, −0.17) | 0.03 | 0.08 | |
| HbA1c | Model 1 | 0.025 (0.002, 0.049) | 0.03 | ref. | 0.001 (−0.024, 0.026) | 0.96 | −0.025 (−0.052, 0.002) | 0.06 | 0.09 |
| Model 2 | 0.03 (0.006, 0.054) | 0.01 | ref. | 0.003 (−0.023, 0.029) | 0.82 | −0.027 (−0.055, 0) | 0.04 | 0.21 | |
| Model 3 | 0.031 (−0.006, 0.068) | 0.10 | ref. | −0.041 (−0.078, −0.003) | 0.03 | −0.072 (−0.11, −0.034) | <0.001 | 0.003 | |
| Stilbenes | −1.4 (−30.3, −0.6) | 0.0 (−0.6, 0.6) | 1.7 (0.6, 27.1) | ||||||
| Glucose | Model 1 | −0.54 (−1.43, 0.35) | 0.24 | ref. | −1.17 (−2.04, −0.3) | 0.08 | −0.64 (−1.54, 0.27) | 0.15 | 0.004 |
| Model 2 | −0.28 (−1.21, 0.66) | 0.46 | ref. | −1.09 (−2, −0.18) | 0.02 | −0.81 (−1.76, 0.14) | 0.08 | 0.008 | |
| Model 3 | 1.1 (−0.35, 2.55) | 0.14 | ref. | −0.6 (−2.08, 0.87) | 0.42 | −1.7 (−3.25, −0.16) | 0.03 | 0.81 | |
| HbA1c | Model 1 | −0.057 (−0.08, −0.035) | <0.001 | ref. | −0.024 (−0.046, −0.002) | 0.03 | 0.033 (0.011, 0.056) | 0.004 | 0.60 |
| Model 2 | −0.051 (−0.074, −0.028) | <0.001 | ref. | −0.02 (−0.042, 0.003) | 0.09 | 0.032 (0.008, 0.055) | 0.009 | 0.41 | |
| Model 3 | −0.005 (−0.042, 0.033) | 0.81 | ref. | −0.038 (−0.076, 0.001) | 0.06 | −0.033 (−0.073, 0.007) | 0.11 | 0.15 |
| Non Diabetic Participants (N = 1231, 21%) | Prediabetic Participants (N = 2872, 48%) | Diabetic Participants (N = 1818, 30%) | |||||
|---|---|---|---|---|---|---|---|
| T3 vs. T1 | P | T3 vs. T1 | P | T3 vs. T1 | P | ||
| Total polyphenols (mg/d) | Glucose | −0.21 (−1.95, 1.52) a | 0.81 | −1.16 (−2.25, −0.06) | 0.04 | −0.83 (−4.95, 3.30) | 0.69 |
| HbA1c | 0.011 (−0.040, 0.062) | 0.68 | 0.011 (−0.017, 0.04) | 0.44 | −0.011 (−0.118, 0.097) | 0.85 | |
| Total flavonoids (mg/d) | Glucose | −0.99 (−2.72, 0.75) | 0.27 | −1.66 (−2.75, −0.56) | 0.001 | −2.24 (−6.39, 1.90) | 0.29 |
| HbA1c | 0.025 (−0.028, 0.077) | 0.36 | −0.009 (−0.037, 0.02) | 0.55 | −0.014 (−0.122, 0.095) | 0.81 | |
| Anthocyanidins (mg/d) | Glucose | 0.44 (−1.31, 2.19) | 0.62 | −0.4 (−1.5, 0.7) | 0.48 | −0.80 (−4.95, 3.35) | 0.71 |
| HbA1c | −0.004 (−0.057, 0.049) | 0.87 | 0.003 (−0.026, 0.031) | 0.85 | −0.025 (−0.134, 0.083) | 0.65 | |
| Catechins (mg/d) | Glucose | −0.19 (−1.91, 1.53) | 0.83 | −0.67 (−1.76, 0.42) | 0.23 | −2.08 (−6.18, 2.02) | 0.32 |
| HbA1c | 0.007 (−0.044, 0.059) | 0.79 | −0.003 (−0.031, 0.025) | 0.84 | −0.101 (−0.208, 0.006) | 0.06 | |
| Proanthocyanidins (mg/d) | Glucose | −0.58 (−2.31, 1.15) | 0.51 | −1.2 (−2.3, −0.1) | 0.03 | −2.46 (−6.59, 1.68) | 0.24 |
| HbA1c | 0.033 (−0.019, 0.085) | 0.21 | −0.008 (−0.036, 0.021) | 0.58 | −0.033 (−0.141, 0.076) | 0.56 | |
| Flavanones (mg/d) | Glucose | −0.08 (−1.81, 1.66) | 0.93 | −1.02 (−2.11, 0.08) | 0.07 | −1.22 (−5.34, 2.89) | 0.56 |
| HbA1c | 0.016 (−0.035, 0.068) | 0.54 | 0.007 (−0.022, 0.035) | 0.64 | 0.048 (−0.060, 0.155) | 0.39 | |
| Flavones (mg/d) | Glucose | −1.03 (−2.78, 0.72) | 0.25 | −1.27 (−2.39, −0.15) | 0.03 | −3.02 (−7.24, 1.20) | 0.16 |
| HbA1c | −0.000 (−0.052, 0.051) | 0.99 | −0.03 (−0.059, 0.000) | 0.05 | −0.084 (−0.194, 0.025) | 0.13 | |
| Flavonols (mg/d) | Glucose | −1.39 (−3.13, 0.34) | 0.12 | −0.95 (−2.05, 0.15) | 0.09 | −2.46 (−6.58, 1.66) | 0.24 |
| HbA1c | 0.009 (−0.042, 0.061) | 0.72 | −0.036 (−0.065, −0.007) | 0.01 | −0.148 (−0.256, −0.040) | 0.01 | |
| Total phenolics acids (mg/d) | Glucose | 0.26 (−1.46, 1.97) | 0.77 | 0.48 (−0.62, 1.57) | 0.39 | 0.01 (−4.09, 4.11) | 1.00 |
| HbA1c | 0.018 (−0.032, 0.069) | 0.48 | 0.022 (−0.007, 0.05) | 0.13 | 0.006 (−0.101, 0.113) | 0.91 | |
| Hydroxycinnamic acids (mg/d) | Glucose | 0.53 (−1.19, 2.25) | 0.54 | 0.2 (−0.89, 1.3) | 0.72 | 0.14 (−3.97, 4.24) | 0.95 |
| HbA1c | 0.02 (−0.031, 0.071) | 0.44 | 0.03 (0.001, 0.058) | 0.04 | 0.003 (−0.104, 0.110) | 0.95 | |
| Hydroxybenzoic acids (mg/d) | Glucose | −0.13 (−1.90, 1.65) | 0.89 | 0.34 (−0.77, 1.46) | 0.55 | 1.58 (−2.62, 5.78) | 0.46 |
| HbA1c | 0.009 (−0.042, 0.061) | 0.72 | −0.007 (−0.036, 0.022) | 0.63 | 0.034 (−0.077, 0.144) | 0.55 | |
| Lignans (mg/d) | Glucose | 0.1 (−1.64, 1.85) | 0.91 | −0.62 (−1.73, 0.49) | 0.27 | −4.83 (−8.99, −0.66) | 0.02 |
| HbA1c | −0.029 (−0.08, 0.023) | 0.28 | −0.039 (−0.067, −0.01) | 0.01 | −0.169 (−0.277, −0.062) | 0.002 | |
| Stilbenes (mg/d) | Glucose | 0.61 (−1.26, 2.48) | 0.52 | −0.21 (−1.39, 0.96) | 0.73 | −5.51 (−9.87, −1.14) | 0.01 |
| HbA1c | 0.022 (−0.034, 0.077) | 0.45 | −0.021 (−0.051, 0.01) | 0.18 | −0.079 (−0.192, 0.034) | 0.17 | |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2022 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Tresserra-Rimbau, A.; Castro-Barquero, S.; Becerra-Tomás, N.; Babio, N.; Martínez-González, M.Á.; Corella, D.; Fitó, M.; Romaguera, D.; Vioque, J.; Alonso-Gomez, A.M.; et al. Adopting a High-Polyphenolic Diet Is Associated with an Improved Glucose Profile: Prospective Analysis within the PREDIMED-Plus Trial. Antioxidants 2022, 11, 316. https://doi.org/10.3390/antiox11020316
Tresserra-Rimbau A, Castro-Barquero S, Becerra-Tomás N, Babio N, Martínez-González MÁ, Corella D, Fitó M, Romaguera D, Vioque J, Alonso-Gomez AM, et al. Adopting a High-Polyphenolic Diet Is Associated with an Improved Glucose Profile: Prospective Analysis within the PREDIMED-Plus Trial. Antioxidants. 2022; 11(2):316. https://doi.org/10.3390/antiox11020316
Chicago/Turabian StyleTresserra-Rimbau, Anna, Sara Castro-Barquero, Nerea Becerra-Tomás, Nancy Babio, Miguel Ángel Martínez-González, Dolores Corella, Montserrat Fitó, Dora Romaguera, Jesús Vioque, Angel M. Alonso-Gomez, and et al. 2022. "Adopting a High-Polyphenolic Diet Is Associated with an Improved Glucose Profile: Prospective Analysis within the PREDIMED-Plus Trial" Antioxidants 11, no. 2: 316. https://doi.org/10.3390/antiox11020316
APA StyleTresserra-Rimbau, A., Castro-Barquero, S., Becerra-Tomás, N., Babio, N., Martínez-González, M. Á., Corella, D., Fitó, M., Romaguera, D., Vioque, J., Alonso-Gomez, A. M., Wärnberg, J., Martínez, J. A., Serra-Majem, L., Estruch, R., Tinahones, F. J., Lapetra, J., Pintó, X., Tur, J. A., López-Miranda, J., ... Salas-Salvadó, J. (2022). Adopting a High-Polyphenolic Diet Is Associated with an Improved Glucose Profile: Prospective Analysis within the PREDIMED-Plus Trial. Antioxidants, 11(2), 316. https://doi.org/10.3390/antiox11020316

















