Olfactory Event-Related Potentials and Exhaled Organic Volatile Compounds: The Slow Link Between Olfactory Perception and Breath Metabolic Response. A Pilot Study on Phenylethyl Alcohol and Vaseline Oil
Abstract
1. Introduction
1.1. Olfactory Function and Breath
1.2. Chemosensory Event Related Potentials
1.3. The Volatile Organic Compounds (VOCs)
1.4. Connection between OERP and VOC
2. Materials and Methods
2.1. Participants
2.2. OERP Apparatus and OERP Processing
2.3. VOC Apparatus
2.4. Method
3. Statistical Analysis and Results
3.1. Statistical Analysis
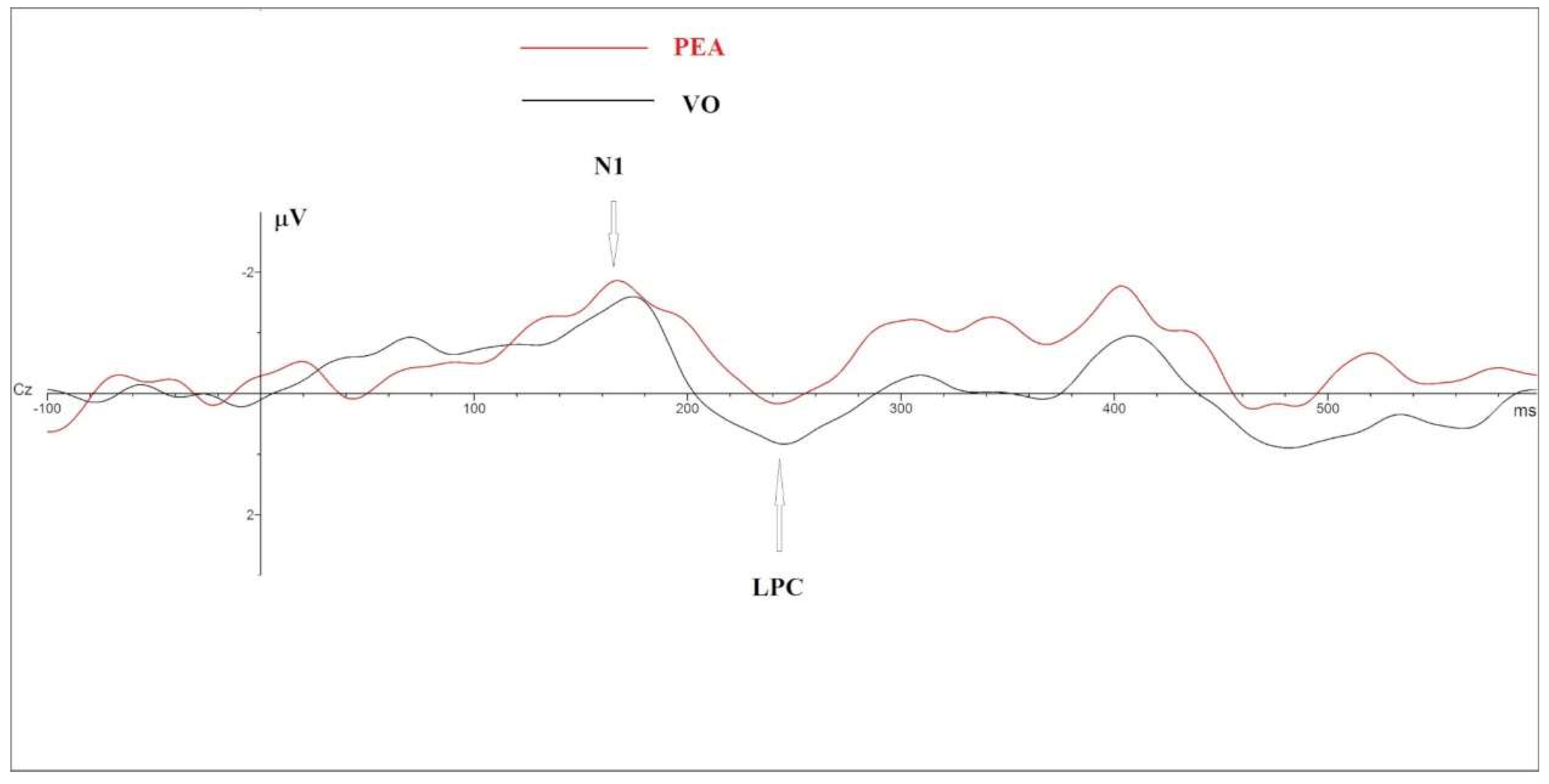
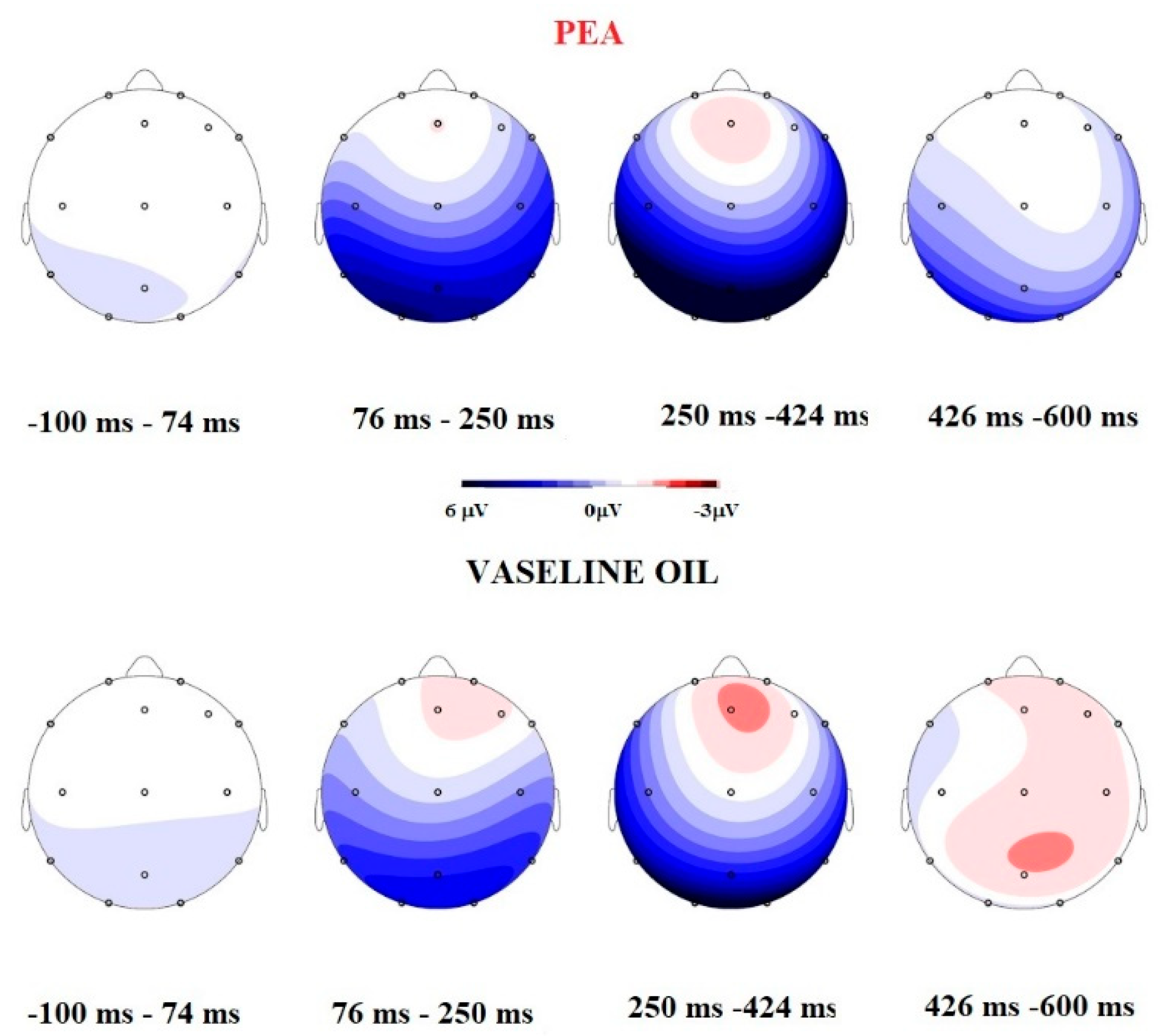
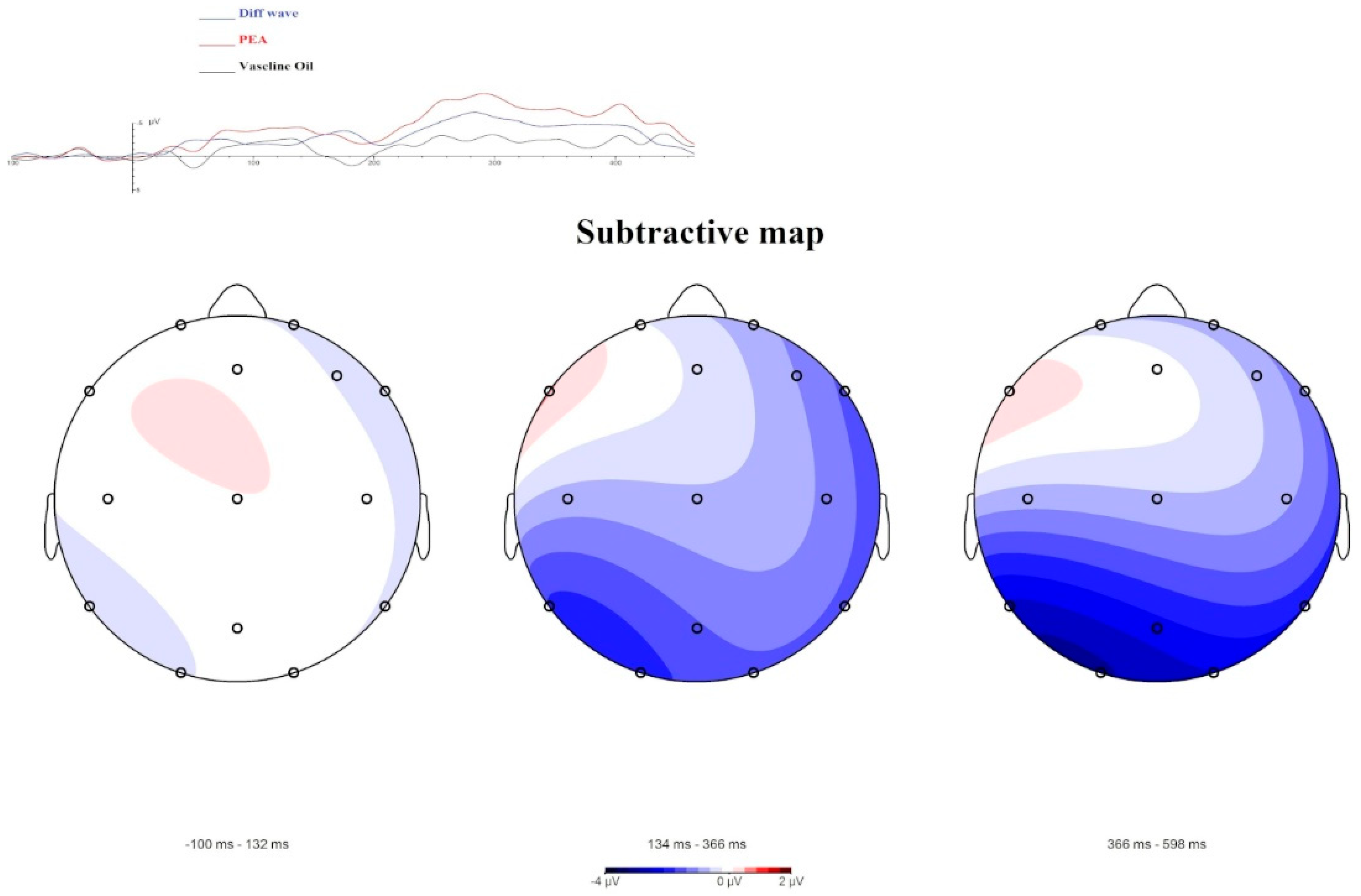
3.1.1. OERP Analysis
3.1.2. N1
3.1.3. LPC
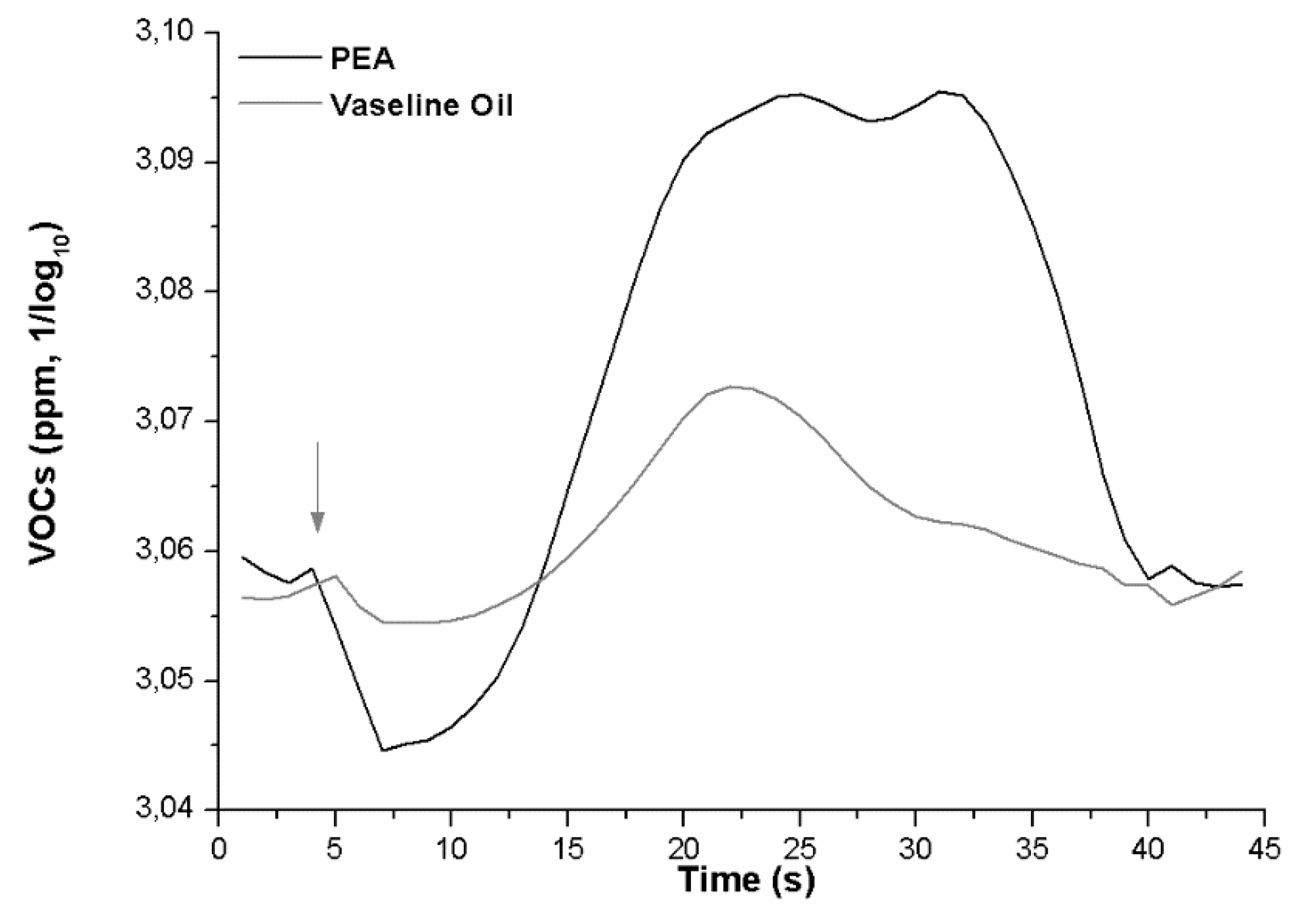
3.2. VOCs Analysis
3.3. Behavioral Results
4. Discussion and Conclusions
4.1. OERPs and VOCs can Be Comparable
4.2. The Slow Link between Olfactory Perception and VOC Metabolic Response
4.3. Limitation of the Study and Pathway for Future Research
Author Contributions
Funding
Acknowledgments
Conflicts of Interest
References
- Secundo, L.; Snitz, K.; Sobel, N. The perceptual logic of smell. Curr. Opin. Neurobiol. 2014, 25, 107–115. [Google Scholar] [CrossRef] [PubMed]
- Oelschläger, H.H. The dolphin brain—A challenge for synthetic neurobiology. Brain Res. Bull. 2008, 75, 450–459. [Google Scholar] [CrossRef]
- Palouzier-Paulignan, B.; Lacroix, M.-C.; Aimé, P.; Baly, C.; Caillol, M.; Congar, P.; Julliard, A.K.; Tucker, K.; Fadool, D.A. Olfaction Under Metabolic Influences. Chem. Senses 2012, 37, 769–797. [Google Scholar] [CrossRef] [PubMed]
- Riera, C.E.; Tsaousidou, E.; Halloran, J.; Follett, P.; Hahn, O.; Pereira, M.M.; Ruud, L.E.; Alber, J.; Tharp, K.; Anderson, C.M.; et al. The Sense of Smell Impacts Metabolic Health and Obesity. Cell Metab. 2017, 26, 198–211. [Google Scholar] [CrossRef]
- Garrison, J.L.; Knight, Z.A. Linking smell to metabolism and aging. Science 2017, 358, 718–719. [Google Scholar] [CrossRef] [PubMed]
- Franks, K.H.; Chuah, M.I.; King, A.E.; Vickers, J.C. Connectivity of Pathology: The Olfactory System as a Model for Network-Driven Mechanisms of Alzheimer’s Disease Pathogenesis. Front. Neuroinform. 2015, 7, 234. [Google Scholar] [CrossRef] [PubMed]
- Yang, M.; Crawley, J.N. Simple Behavioral Assessment of Mouse Olfaction. Curr. Protoc. Neurosci. 2009, 48, 8.24.1–8.24.12. [Google Scholar]
- Wesson, D.W.; Levy, E.; Nixon, R.A.; Wilson, D.A. Olfactory dysfunction correlates with amyloid-beta burden in an Alzheimer’s disease mouse model. J. Neurosci. 2010, 30, 505–514. [Google Scholar] [CrossRef]
- Hedner, M.; Larsson, M.; Arnold, N.; Zucco, G.M.; Hummel, T. Cognitive factors in odor detection, odor discrimination, and odor identification tasks. J. Clin. Exp. Neuropsychol. 2010, 32, 1062–1067. [Google Scholar] [CrossRef] [PubMed]
- Hummel, T.; Sekinger, B.; Wolf, S.R.; Pauli, E.; Kobal, G. ’Sniffin’ sticks’: Olfactory performance assessed by the combined testing of odor identification, odor discrimination and olfactory threshold. Chem. Senses 1997, 22, 39–52. [Google Scholar] [CrossRef]
- Khan, R.M.; Hartley, C.A.; Sobel, N.; Sullivan, E.V.; Gabrieli, J.D. Sniffing Longer rather than Stronger to Maintain Olfactory Detection Threshold. Chem. Senses 2000, 25, 1–8. [Google Scholar]
- Giessel, A.J.; Datta, S.R. Olfactory maps, circuits and computations. Curr. Opin. Neurobiol. 2014, 24, 120–132. [Google Scholar] [CrossRef] [PubMed]
- Trimmer, C.; Mainland, J.D. The Olfactory System. In Conn’s Translational Neuroscience; Academic Press: Cambridge, MA, USA, 2016; ISBN 9780128025963. [Google Scholar]
- Doty, R.L. Olfaction. Annu. Rev. Psychol. 2001, 52, 423–452. [Google Scholar] [CrossRef] [PubMed]
- Poroyko, V.A.; Carreras, A.; Khalyfa, A.; Khalyfa, A.A.; Leone, V.; Peris, E.; Almendros, I.; Gileles-Hillel, A.; Qiao, Z.; Hubert, N.; et al. Chronic Sleep Disruption Alters Gut Microbiota, Induces Systemic and Adipose Tissue Inflammation and Insulin Resistance in Mice. Sci. Rep. 2016, 6, 35405. [Google Scholar] [CrossRef]
- Invitto, S.; Calcagnì, A.; Piraino, G.; Ciccarese, V.; Balconi, M.; De Tommaso, M.; Toraldo, D.M. Obstructive sleep apnea syndrome and olfactory perception: An OERP study. Respir. Physiol. Neurobiol. 2019, 259, 37–44. [Google Scholar] [CrossRef]
- Gschwend, O.; Abraham, N.M.; Lagier, S.; Begnaud, F.; Rodríguez, I.; Carleton, A. Neuronal pattern separation in the olfactory bulb improves odor discrimination learning. Nat. Neurosci. 2015, 18, 1474–1482. [Google Scholar] [CrossRef]
- Noguchi, D.; Sugimoto, S.; Bannai, Y.; Okada, K.-I. Time characteristics of olfaction in a single breath. In Proceedings of the SIGCHI Conference on Human Factors in Computing Systems 2011, Vancouver, BC, Canada, 7–12 May 2011; p. 83. [Google Scholar]
- Lorig, T.S. The application of electroencephalographic techniques to the study of human olfaction: A review and tutorial. Int. J. Psychophysiol. 2000, 36, 91–104. [Google Scholar] [CrossRef]
- Kobal, G.; Hummel, T. Olfactory (chemosensory) event-related potentials. Toxicol. Ind. Heal. 1994, 10, 587–596. [Google Scholar]
- Gudziol, H.; Fischer, J.; Bitter, T.; Guntinas-Lichius, O. Chemosensory event-related brain potentials (CSERP) after strictly monorhinal stimulation. Int. J. Psychophysiol. 2014, 93, 305–310. [Google Scholar] [CrossRef] [PubMed]
- Andrews, G.; Howie, P.M.; Dozsa, M.; Guitar, B.E. Stuttering: Speech pattern characteristics under fluency-inducing conditions. J. Hear. Res. 1982, 25, 208–216. [Google Scholar] [CrossRef]
- Sojka, B.; Ferstl, R.; Pause, B.M. Central Processing of Odor Concentration is a Temporal Phenomenon as Revealed by Chemosensory Event-Related Potentials (CSERP). Chem. Senses 1997, 22, 9–26. [Google Scholar]
- Pause, B.M.; Krauel, K. Chemosensory event-related potentials (CSERP) as a key to the psychology of odors. Int. J. Psychophysiol. 2000, 36, 105–122. [Google Scholar] [CrossRef]
- Kobal, G.; Hummel, T. Olfactory and intranasal trigeminal event-related potentials in anosmic patients. Laryngoscope Investig. Otolaryngol. 1998, 108, 1033–1035. [Google Scholar] [CrossRef]
- Geisler, M.W.; Murphy, C. Event-related brain potentials to attended and ignored olfactory and trigeminal stimuli. Int. J. Psychophysiol. 2000, 37, 309–315. [Google Scholar] [CrossRef]
- Barz, S.; Pauli, E.; Kobal, G.; Hummel, T. Chemosensory event-related potentials change with age. Electroencephalogr. Clin. Neurophysiol. Potentials Sect. 1998, 108, 208–217. [Google Scholar]
- Invitto, S.; Piraino, G.; Ciccarese, V.; Carmillo, L.; Caggiula, M.; Trianni, G.; Nicolardi, G.; Di Nuovo, S.; Balconi, M. Potential Role of OERP as Early Marker of Mild Cognitive Impairment. Front. Neuroinform. 2018, 10, 272. [Google Scholar] [CrossRef] [PubMed]
- Brauchli, P.; Rüegg, P.B.; Etzweiler, F.; Zeier, H. Electrocortical and Autonomic Alteration by Administration of a Pleasant and an Unpleasant Odor. Chem. Senses 1995, 20, 505–515. [Google Scholar] [CrossRef] [PubMed]
- Lorig, T.S.; Schwartz, G.E. Brain and odor: I. Alteration of human EEG by odor administration. Psychobiology 1988, 16, 281–284. [Google Scholar]
- Phillips, M.; Herrera, J.; Krishnan, S.; Zain, M.; Greenberg, J.; Cataneo, R.N. Variation in volatile organic compounds in the breath of normal humans. J. Chromatogr. B Biomed. Sci. Appl. 1999, 729, 75–88. [Google Scholar] [CrossRef]
- Mazzatenta, A.; Pokorski, M.; Cozzutto, S.; Barbieri, P.; Verratti, V.; Giulio, C. Di Non-invasive assessment of exhaled breath pattern in patients with multiple chemical sensibility disorder. In Advances in Experimental Medicine and Biology; Springer: Dordrecht, The Netherlands, 2013. [Google Scholar]
- Mazzatenta, A.; Pokorski, M.; Di Giulio, C. Real-Time Breath Analysis in Type 2 Diabetes Patients During Cognitive Effort. Adv. Exp. Med. Biol. 2013, 788, 247–253. [Google Scholar]
- Mazzatenta, A.; Di Giulio, C.; Pokorski, M. Pathologies currently identified by exhaled biomarkers. Respir. Physiol. Neurobiol. 2013, 187, 128–134. [Google Scholar] [CrossRef] [PubMed]
- Mazzatenta, A.; Pokorski, M.; Di Giulio, C. Real time analysis of volatile organic compounds (VOCs) in centenarians. Respir. Physiol. Neurobiol. 2015, 209, 47–51. [Google Scholar] [CrossRef] [PubMed]
- Ionescu, R.; Broza, Y.; Shaltieli, H.; Sadeh, D.; Zilberman, Y.; Feng, X.; Glass-Marmor, L.; Lejbkowicz, I.; Müllen, K.; Miller, A.; et al. Detection of Multiple Sclerosis from Exhaled Breath Using Bilayers of Polycyclic Aromatic Hydrocarbons and Single-Wall Carbon Nanotubes. ACS Chem. Neurosci. 2011, 2, 687–693. [Google Scholar] [CrossRef] [PubMed]
- Tisch, U.; Schlesinger, I.; Ionescu, R.; Nassar, M.; Axelrod, N.; Robertman, D.; Tessler, Y.; Azar, F.; Marmur, A.; Aharon-Peretz, J.; et al. Detection of Alzheimer’s and Parkinson’s disease from exhaled breath using nanomaterial-based sensors. Nanomedicine 2013, 8, 43–56. [Google Scholar] [CrossRef]
- Mazzatenta, A.; Pokorski, M.; Sartucci, F.; Domenici, L.; Di Giulio, C. Volatile organic compounds (VOCs) fingerprint of Alzheimer’s disease. Respir. Physiol. Neurobiol. 2015, 209, 81–84. [Google Scholar] [CrossRef] [PubMed]
- Chopra, A.; Baur, A.; Hummel, T. Thresholds and chemosensory event-related potentials to malodors before, during, and after puberty: Differences related to sex and age. NeuroImage 2008, 40, 1257–1263. [Google Scholar] [CrossRef]
- Schriever, V.A.; Góis-Eanes, M.; Schuster, B.; Huart, C.; Hummel, T. Olfactory Event-Related Potentials in Infants. J. Pediatr. 2014, 165, 372–375. [Google Scholar] [CrossRef] [PubMed]
- Mazzatenta, A.; Pokorski, M.; Di Tano, A.; Cacchio, M.; Di Giulio, C. Influence of sensory stimulation on exhaled volatile organic compounds. In Advances in Experimental Medicine and Biology; Springer: Dordrecht, The Netherlands, 2016; ISBN 00652598. [Google Scholar]
- Bradley, T.D.; Floras, J.S. Obstructive sleep apnoea and its cardiovascular consequences. Lancet 2009, 373, 82–93. [Google Scholar] [CrossRef]
- Lim, D.C.; Pack, A.I. Obstructive sleep apnea and cognitive impairment: Addressing the blood–brain barrier. Sleep Med. Rev. 2014, 18, 35–48. [Google Scholar] [CrossRef]
- Masaoka, Y.; Harding, I.H.; Koiwa, N.; Yoshida, M.; Harrison, B.J.; Lorenzetti, V.; Ida, M.; Izumizaki, M.; Pantelis, C.; Homma, I. The neural cascade of olfactory processing: A combined fMRI–EEG study. Respir. Physiol. Neurobiol. 2014, 204, 71–77. [Google Scholar] [CrossRef]
- Atchley, R.; Klee, D.; Memmott, T.; Goodrich, E.; Wahbeh, H.; Oken, B. Event-related potential correlates of mindfulness meditation competence. Neuroscience 2016, 320, 83–92. [Google Scholar] [CrossRef] [PubMed]
- Menicucci, D.; Artoni, F.; Bedini, R.; Pingitore, A.; Passera, M.; Landi, A.; L’Abbate, A.; Sebastiani, L.; Gemignani, A. Brain Responses to Emotional Stimuli During Breath Holding and Hypoxia: An Approach Based on the Independent Component Analysis. Brain Topogr. 2014, 27, 771–785. [Google Scholar] [CrossRef]
- Van Houdt, P.J.; Ossenblok, P.P.W.; Van Erp, M.G.; Schreuder, K.E.; Krijn, R.J.J.; Boon, P.A.J.M.; Cluitmans, P.J.M. Automatic breath-to-breath analysis of nocturnal polysomnographic recordings. Med. Biol. Eng. Comput. 2011, 49, 819–830. [Google Scholar] [CrossRef]
- Miwa, T.; Tsukatani, T.; Furukawa, M.; Costanzo, R.M. Detection Thresholds for Phenyl Ethyl Alcohol Using Serial Dilutions in Different Solvents. Chem. Senses 2003, 28, 25–32. [Google Scholar]
- Invitto, S.; Capone, S.; Montagna, G.; Siciliano, P.A. MI2014A001344 Method and System for Measuring Physiological Parameters of a Subject Undergoing an Olfactory Stimulation. U.S. Patent No. 20170127971A1, 11 May 2017. [Google Scholar]
- Invitto, S.; Capone, S.; Montagna, G.; Siciliano, P. Virtual olfactory device in EEG and olfactory conditioning task: An OERP study. In Convegno Nazionale Sensori; Springer: Cham, Switzerland, 2018; Volume 431, ISBN 9783319550763. [Google Scholar]
- Nuwer, M.R.; Lehmann, D.; Da Silva, F.L.; Matsuoka, S.; Sutherling, W.; Vibert, J.-F. IFCN guidelines for topographic and frequency analysis of EEGs and EPs. Report of an IFCN committee. Electroencephalogr. Clin. Neurophysiol. 1994, 91, 1–5. [Google Scholar] [CrossRef]
- Luck, S.J. An Introduction to the Event-Related Potential Technique; MIT press: Cambridge, MA, USA, 2005. [Google Scholar]
- Invitto, S.; Piraino, G.; Mignozzi, A.; Capone, S.; Montagna, G.; Siciliano, P.A.; Mazzatenta, A.; Rocco, G.; De Feudis, I.; Trotta, G.F.; et al. Smell and Meaning: An OERP Study; Springer: Cham, Switzerland, 2017; Volume 69. [Google Scholar]
- Moore, A.W.; Gruber, T.; Derose, J.; Malinowski, P. Regular, brief mindfulness meditation practice improves electrophysiological markers of attentional control. Front. Hum. Neurosci. 2012, 6, 18. [Google Scholar] [CrossRef] [PubMed]
| Electrode | t Value | p | PEA | VO |
|---|---|---|---|---|
| F4 | 3.664 | 0.003 | −3.9 | −2.4 |
| C3 | 3.173 | 0.007 | −6.19 | −4.48 |
| C4 | 3.062 | 0.009 | −6.82 | −4.89 |
| P7 | 4.429 | 0.001 | −12.25 | −9.06 |
| P8 | 5.040 | 0.000 | −13.21 | −9.23 |
| O1 | 4.865 | 0.013 | −14.17 | −11.26 |
| O2 | 3.957 | 0.002 | −14.95 | −11.15 |
| F8 | 2.67 | 0.019 | −8.60 | −5.54 |
| Cz | 2.724 | 0.017 | −3.17 | −2.49 |
| Pz | 4.332 | 0.001 | −10.31 | −8.06 |
| Electrode | Latency | SEM |
|---|---|---|
| Fp1 | 389.73 | 23.7 |
| Fp2 | 358.13 | 28.36 |
| F3 | 348.67 | 26.18 |
| F4 | 367.63 | 27.55 |
| C3 | 413.6 | 26.42 |
| C4 | 386 | 31.06 |
| P7 | 416 | 28.5 |
| P8 | 404.4 | 30.74 |
| O1 | 424.53 | 25.69 |
| O2 | 424.40 | 24.5 |
| F7 | 384.93 | 25.5 |
| F8 | 348.53 | 34.05 |
| Cz | 426.53 | 23.19 |
| Pz | 447.07 | 18.95 |
| Fz | 338.27 | 20.82 |
© 2019 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Invitto, S.; Mazzatenta, A. Olfactory Event-Related Potentials and Exhaled Organic Volatile Compounds: The Slow Link Between Olfactory Perception and Breath Metabolic Response. A Pilot Study on Phenylethyl Alcohol and Vaseline Oil. Brain Sci. 2019, 9, 84. https://doi.org/10.3390/brainsci9040084
Invitto S, Mazzatenta A. Olfactory Event-Related Potentials and Exhaled Organic Volatile Compounds: The Slow Link Between Olfactory Perception and Breath Metabolic Response. A Pilot Study on Phenylethyl Alcohol and Vaseline Oil. Brain Sciences. 2019; 9(4):84. https://doi.org/10.3390/brainsci9040084
Chicago/Turabian StyleInvitto, Sara, and Andrea Mazzatenta. 2019. "Olfactory Event-Related Potentials and Exhaled Organic Volatile Compounds: The Slow Link Between Olfactory Perception and Breath Metabolic Response. A Pilot Study on Phenylethyl Alcohol and Vaseline Oil" Brain Sciences 9, no. 4: 84. https://doi.org/10.3390/brainsci9040084
APA StyleInvitto, S., & Mazzatenta, A. (2019). Olfactory Event-Related Potentials and Exhaled Organic Volatile Compounds: The Slow Link Between Olfactory Perception and Breath Metabolic Response. A Pilot Study on Phenylethyl Alcohol and Vaseline Oil. Brain Sciences, 9(4), 84. https://doi.org/10.3390/brainsci9040084






