In Vitro Biomechanical Simulation Testing of Custom Fabricated Temporomandibular Joint Parts Made of Electron Beam Melted Titanium, Zirconia, and Poly-Methyl Methacrylate
Abstract
1. Introduction
2. Materials and Methods
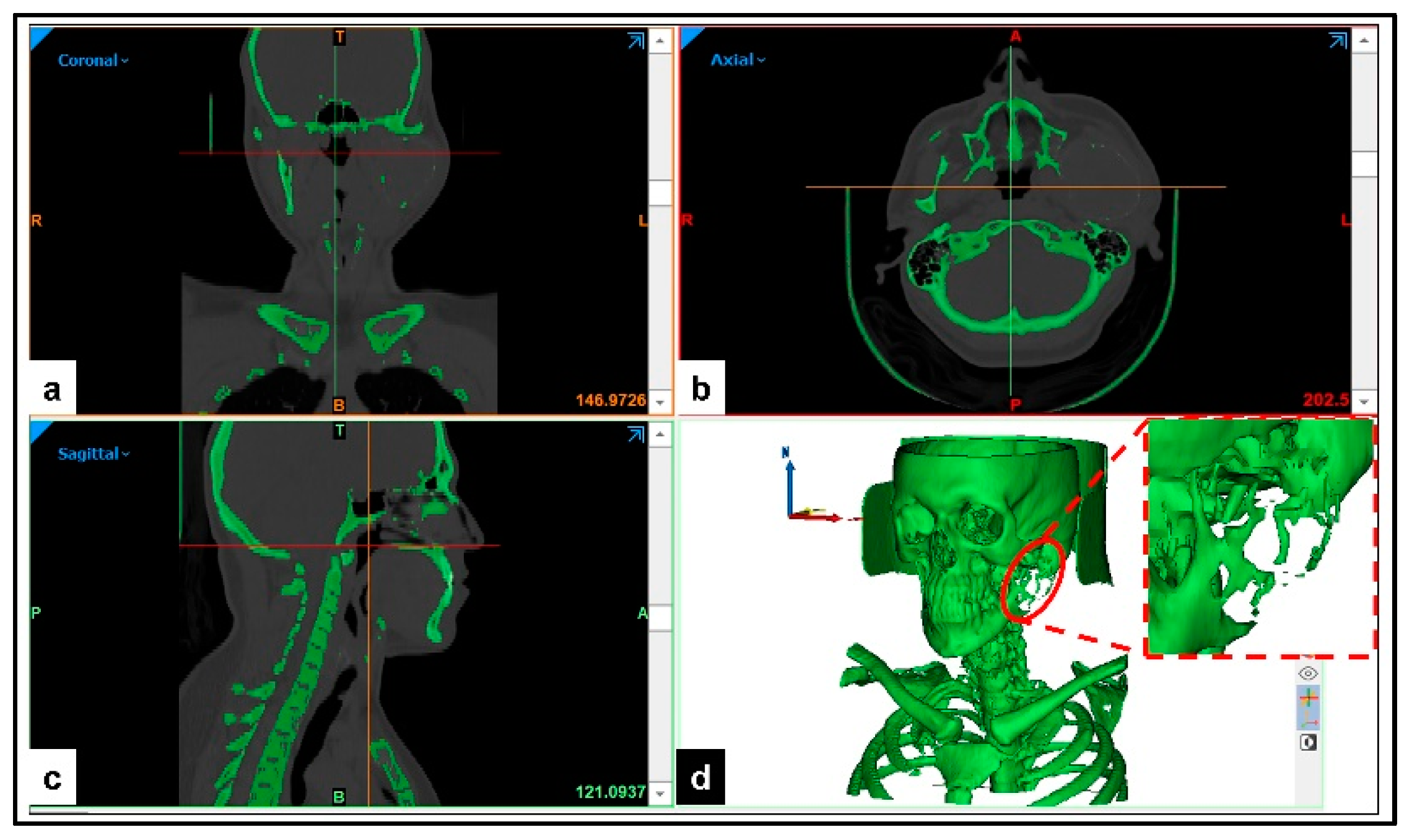
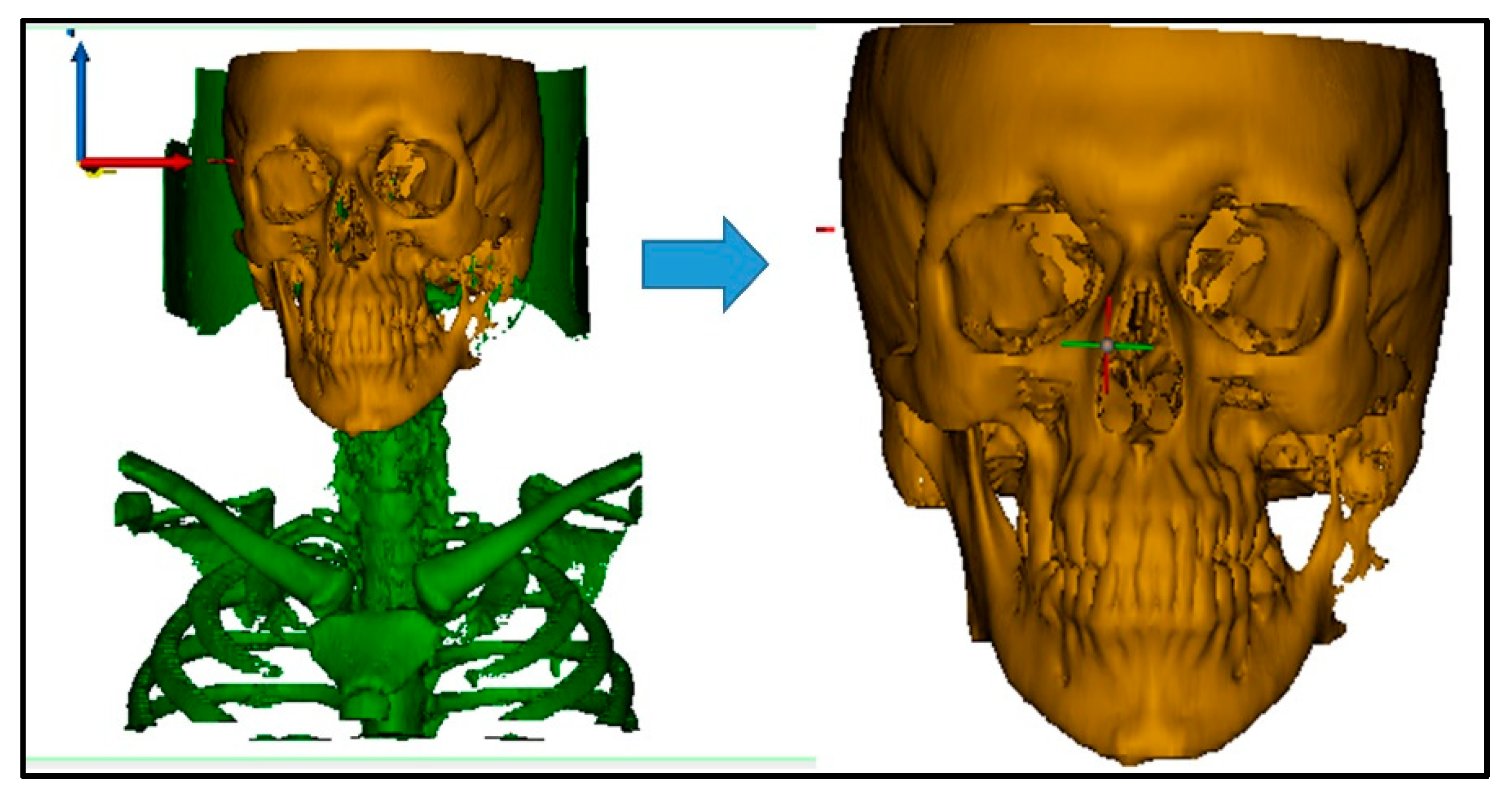
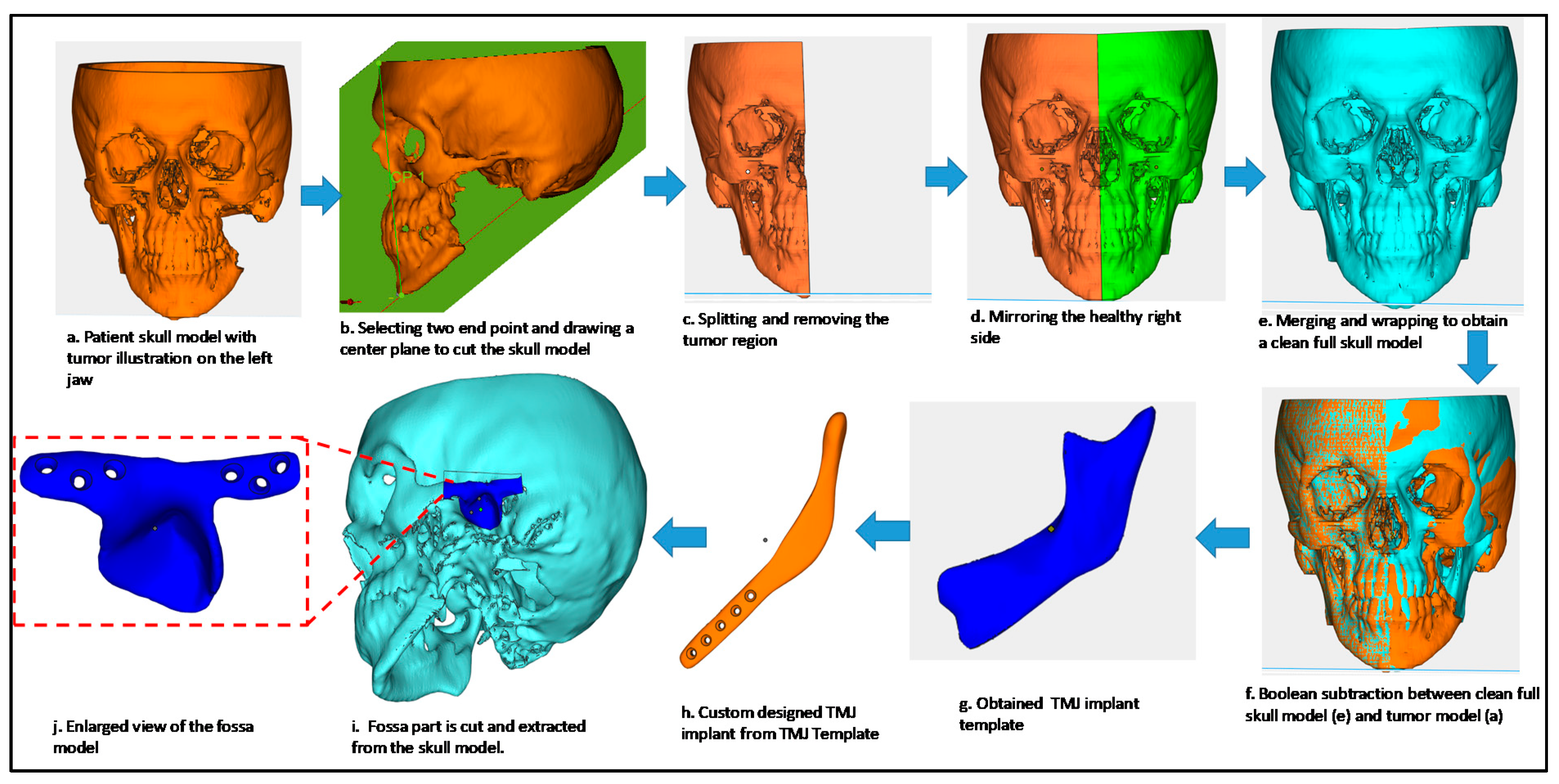
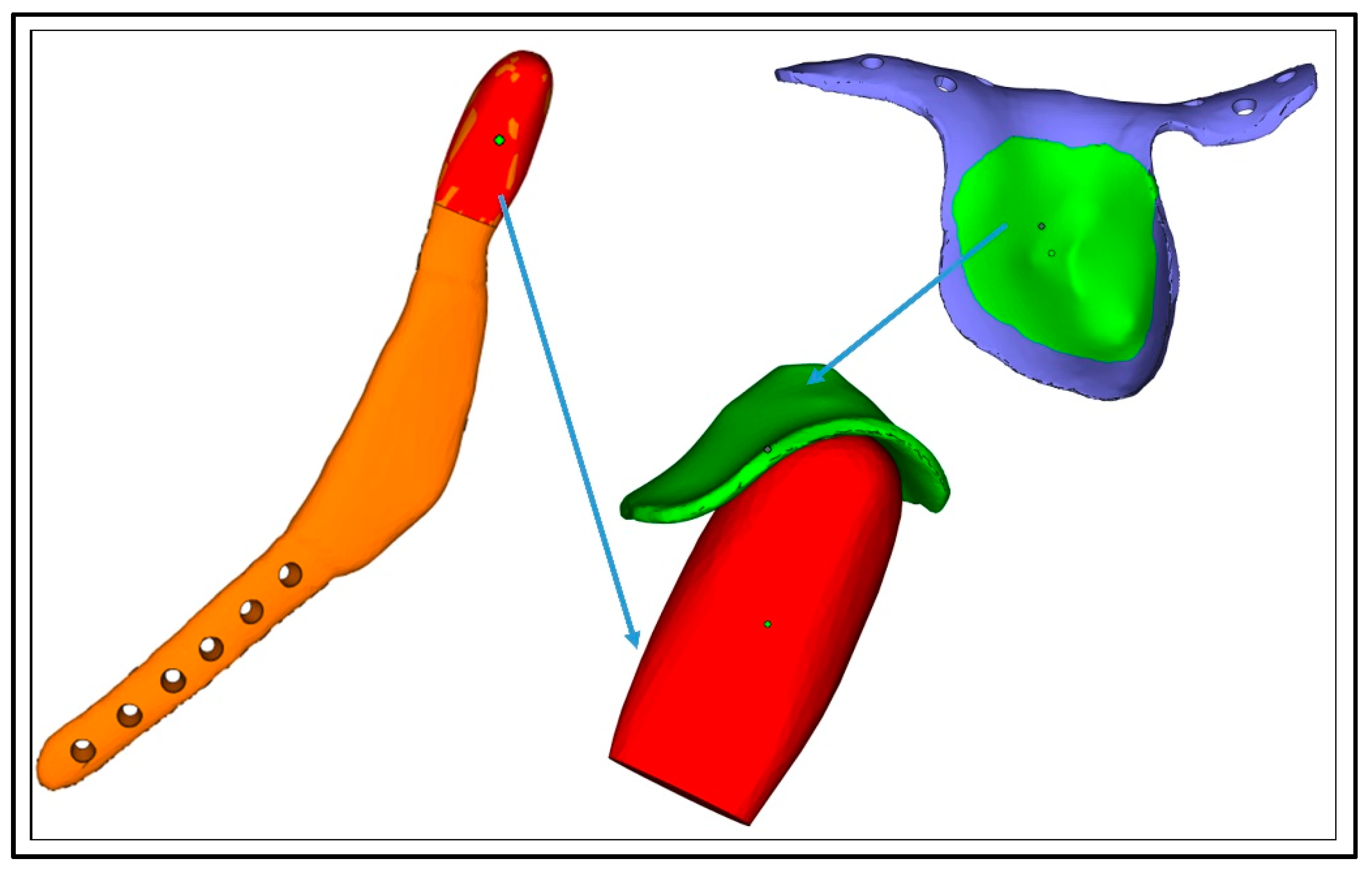
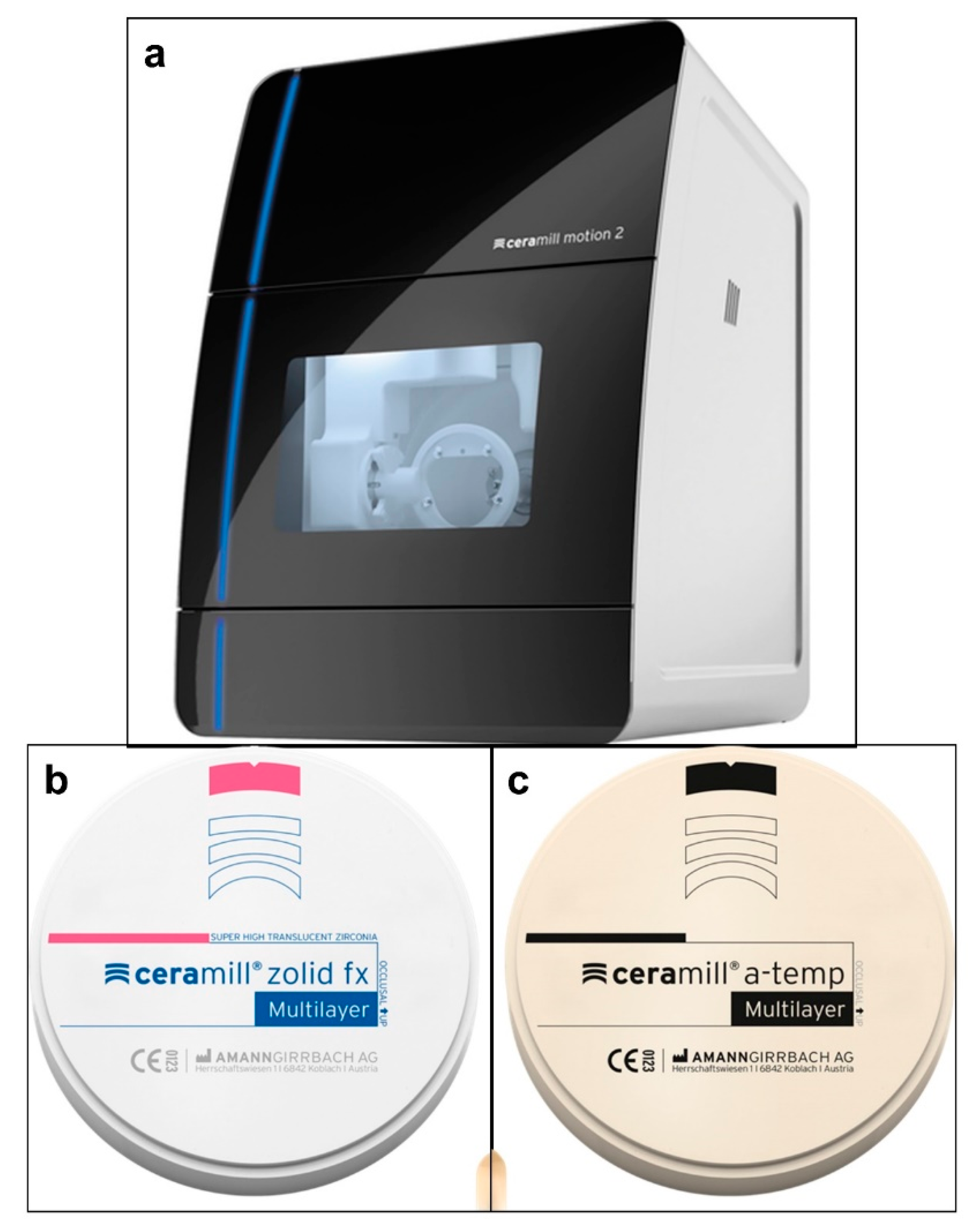
2.1. Fabrication of the Prosthetic TMJ Condyle and Glenoid Fossa Parts
2.2. Biomechanical Simulation Testing of the TMJ Condyle and Glenoid Fossa
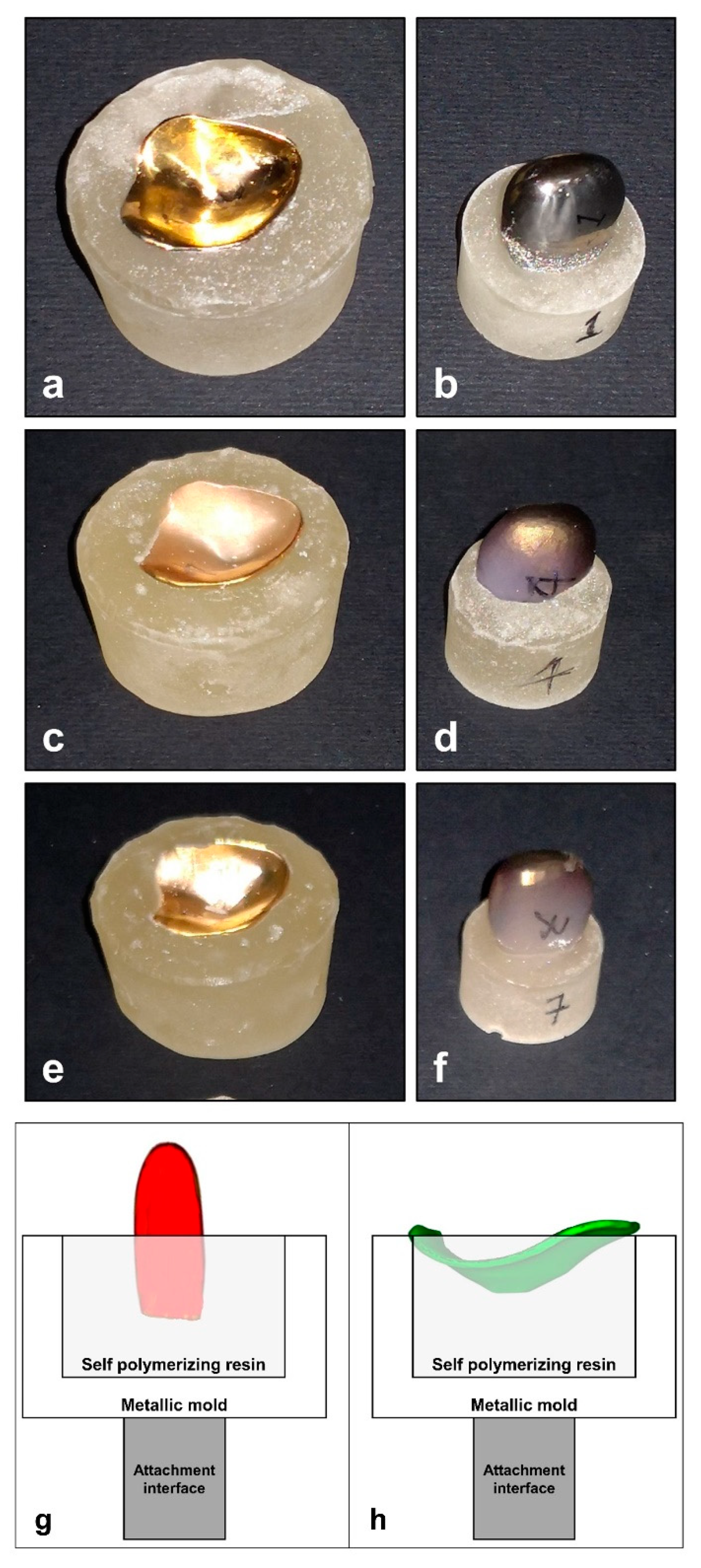
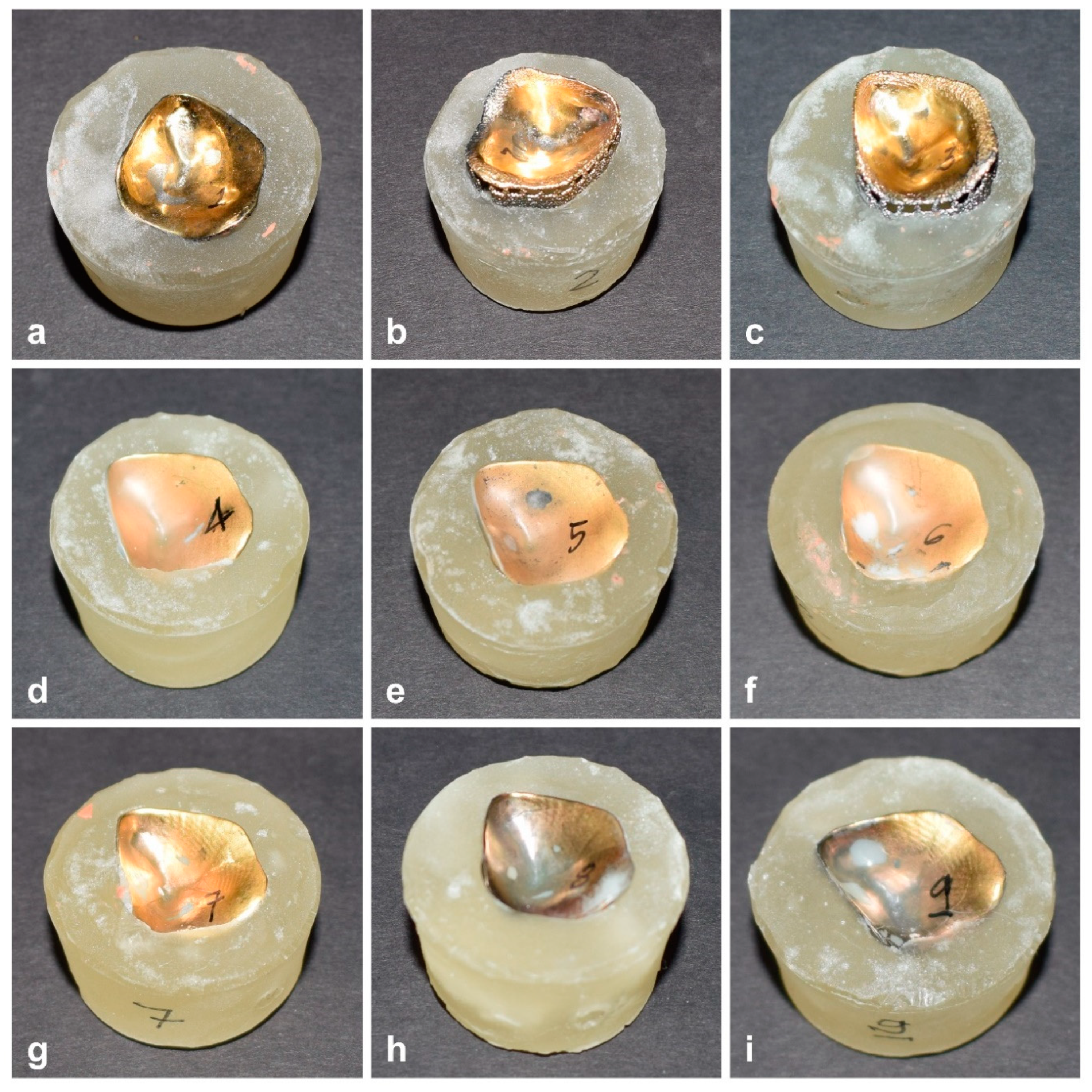
2.3. Pre-Test and Post-Test Physical Analysis of the Prosthetic TMJ Parts
3. Statistical Analysis
4. Results
5. Discussion
6. Conclusions
Author Contributions
Funding
Acknowledgments
Conflicts of Interest
Ethical Statement
References
- Sidebottom, A.J.; Gruber, E. One-year prospective outcome analysis and complications following total replacement of the temporomandibular joint with the tmj concepts system. Br. J. Oral Maxillofac. Surg. 2013, 51, 620–624. [Google Scholar] [PubMed]
- Mercuri, L.G. Total joint reconstruction—Autologous or alloplastic. Oral Maxillofac. Surg. Clin. N. Am. 2006, 18, 399–410. [Google Scholar] [CrossRef] [PubMed]
- Frayne, R.J.; Schwartz, M.; Dickey, J.P. A mastication mechanism designed for testing temporomandibular joint implants. Appl. Bionics Biomech. 2012, 9, 241–247. [Google Scholar] [CrossRef][Green Version]
- Alomar, X.; Medrano, J.; Cabratosa, J.; Clavero, J.A.; Lorente, M.; Serra, I.; Monill, J.M.; Salvador, A. Anatomy of the temporomandibular joint. Semin. Ultrasound CT MR. 2007, 28, 170–183. [Google Scholar] [CrossRef] [PubMed]
- Saeed, N.; Hensher, R.; McLeod, N.; Kent, J. Reconstruction of the temporomandibular joint autogenous compared with alloplastic. Br. J. Oral Maxillofac. Surg. 2002, 40, 296–299. [Google Scholar] [CrossRef]
- Sidebottom, A.J. Alloplastic or autogenous reconstruction of the tmj. J. Oral Biol Craniofac Res. 2013, 3, 135–139. [Google Scholar] [CrossRef]
- Burgess, M.; Bowler, M.; Jones, R.; Hase, M.; Murdoch, B. Improved outcomes after alloplastic tmj replacement: Analysis of a multicenter study from australia and new zealand. J. Oral Maxillofac. Surg. 2014, 72, 1251–1257. [Google Scholar] [CrossRef]
- Dang, R.R.; Mehra, P. Alloplastic reconstruction of the temporomandibular joint. J. Istanb. Univ. Fac. Dent. 2017, 51, S31–S40. [Google Scholar] [CrossRef]
- Park, J.-H.; Jo, E.; Cho, H.; Kim, H.J. Temporomandibular joint reconstruction with alloplastic prosthesis: The outcomes of four cases. Maxillofac. Plast. Reconstr. Surg. 2017, 39, 6. [Google Scholar] [CrossRef]
- Mercuri, L.G.; Wolford, L.M.; Sanders, B.; White, R.D.; Hurder, A.; Henderson, W. Custom cad/cam total temporomandibular joint reconstruction system: Preliminary multicenter report. J. Oral Maxillofac. Surg. 1995, 53, 106–115. [Google Scholar] [CrossRef]
- Mercuri, L.G.; Wolford, L.M.; Sanders, B.; White, R.D.; Giobbie-Hurder, A. Long-term follow-up of the cad/cam patient fitted total temporomandibular joint reconstruction system. J. Oral Maxillofac. Surg. 2002, 60, 1440–1448. [Google Scholar] [CrossRef] [PubMed]
- Gonzalez-Perez, L.M.; Gonzalez-Perez-Somarriba, B.; Centeno, G.; Vallellano, C.; Montes-Carmona, J.F. Evaluation of total alloplastic temporo-mandibular joint replacement with two different types of prostheses: A three-year prospective study. Med. Oral Patol. Oral Cir. Bucal 2016, 21, e766–e775. [Google Scholar] [CrossRef] [PubMed]
- Sidebottom, A.J.; Speculand, B.; Hensher, R. Foreign body response around total prosthetic metal-on-metal replacements of the temporomandibular joint in the UK. Br. J. Oral Maxillofac. Surg. 2008, 46, 288–292. [Google Scholar] [CrossRef]
- Alkindi, M.; Ramalingam, S.; Badwelan, M.; AlSheddi, M.A.; Alahmari, A.M.; Moiduddin, K.; Nasr, E.A. In-vivo biocompatibility and functional efficacy of customized electron beam-melted titanium mandibular reconstruction plates. J. Biomater. Tissue Eng. 2018, 8, 1642–1651. [Google Scholar] [CrossRef]
- Wolford, L.M.; Mehra, P. Custom-made total joint prostheses for temporomandibular joint reconstruction. Proc. (Bayl. Univ. Med. Cent.) 2000, 13, 135–138. [Google Scholar] [CrossRef] [PubMed]
- Parthasarathy, J. 3D modeling, custom implants and its future perspectives in craniofacial surgery. Ann. Maxillofac. Surg. 2014, 4, 9–18. [Google Scholar] [CrossRef] [PubMed]
- Maietta, S.; Gloria, A.; Improta, G.; Richetta, M.; De Santis, R.; Martorelli, M. A further analysis on ti6al4v lattice structures manufactured by selective laser melting. J. Healthc. Eng. 2019, 2019. [Google Scholar] [CrossRef]
- Vance, A.; Bari, K.; Arjunan, A. Compressive performance of an arbitrary stiffness matched anatomical ti64 implant manufactured using direct metal laser sintering. Mater. Des. 2018, 160, 1281–1294. [Google Scholar] [CrossRef]
- Moiduddin, K.; Al-Ahmari, A.; Kindi, M.A.; Nasr, E.S.A.; Mohammad, A.; Ramalingam, S. Customized porous implants by additive manufacturing for zygomatic reconstruction. Biocybern. Biomed. Eng. 2016, 36, 719–730. [Google Scholar] [CrossRef]
- Sidambe, A.T. Biocompatibility of advanced manufactured titanium implants—A review. Materials 2014, 7, 8168–8188. [Google Scholar] [CrossRef]
- Schuurhuis, J.M.; Dijkstra, P.U.; Stegenga, B.; de Bont, L.G.M.; Spijkervet, F.K.L. Groningen temporomandibular total joint prosthesis: An 8-year longitudinal follow-up on function and pain. J. Cranio Maxillofac. Surg. 2012, 40, 815–820. [Google Scholar] [CrossRef] [PubMed]
- De La Pena, A.; De La Pena-Brambila, J.; Perez-De La Torre, J.; Ochoa, M.; Gallardo, G.J. Low-cost customized cranioplasty using a 3d digital printing model: A case report. 3D Print. Med. 2018, 4, 4. [Google Scholar] [CrossRef] [PubMed]
- Lee, U.L.; Kwon, J.S.; Woo, S.H.; Choi, Y.J. Simultaneous bimaxillary surgery and mandibular reconstruction with a 3-dimensional printed titanium implant fabricated by electron beam melting: A preliminary mechanical testing of the printed mandible. J. Oral Maxillofac. Surg. 2016. [Google Scholar] [CrossRef] [PubMed]
- Fontenot, M.G.; Kent, J.N. In vitro wear performance of proplast tmj disc implants. J. Oral Maxillofac. Surg. 1992, 50, 133–139. [Google Scholar] [CrossRef]
- Alakailly, X.; Schwartz, D.; Alwanni, N.; Demko, C.; Altay, M.A.; Kilinc, Y.; Baur, D.A.; Quereshy, F. Patient-centered quality of life measures after alloplastic temporomandibular joint replacement surgery. Int. J. Oral Maxillofac. Surg. 2017, 46, 204–207. [Google Scholar] [CrossRef]
- Gerbino, G.; Zavattero, E.; Bosco, G.; Berrone, S.; Ramieri, G. Temporomandibular joint reconstruction with stock and custom-made devices: Indications and results of a 14-year experience. J. Cranio Maxillofac. Surg. 2017, 45, 1710–1715. [Google Scholar] [CrossRef]
- Westermark, A.; Heden, P.; Aagaard, E.; Cornelius, C.P. The use of tmj concepts prostheses to reconstruct patients with major temporomandibular joint and mandibular defects. Int. J. Oral Maxillofac. Surg. 2011, 40, 487–496. [Google Scholar] [CrossRef]
- Ahn, S.J.; Tsou, L.; Antonio Sanchez, C.; Fels, S.; Kwon, H.B. Analyzing center of rotation during opening and closing movements of the mandible using computer simulations. J. Biomech. 2015, 48, 666–671. [Google Scholar] [CrossRef]
- Bekcioglu, B.; Bulut, E.; Bas, B. The effects of unilateral alloplastic temporomandibular joint replacement on the opposite-side natural joint: A finite-element analysis. J. Oral Maxillofac. Surg. 2017, 75, 2316–2322. [Google Scholar] [CrossRef]
- Oshida, Y. Bioscience and Bioengineering of Titanium Materials; Elsevier: Amsterdam, The Netherlands, 2010. [Google Scholar]
- Bosshardt, D.D.; Chappuis, V.; Buser, D. Osseointegration of titanium, titanium alloy and zirconia dental implants: Current knowledge and open questions. Periodontology 2000 2017, 73, 22–40. [Google Scholar] [CrossRef]
- Cionca, N.; Hashim, D.; Mombelli, A. Zirconia dental implants: Where are we now, and where are we heading? Periodontology 2000 2017, 73, 241–258. [Google Scholar] [CrossRef] [PubMed]
- Goiato, M.C.; Freitas, E.; dos Santos, D.; de Medeiros, R.; Sonego, M. Acrylic resin cytotoxicity for denture base—Literature review. Adv. Clin. Exp. Med. 2015, 24, 679–686. [Google Scholar] [CrossRef] [PubMed]
- He, W.; Benson, R. 5—Polymeric biomaterials. In Handbook of Biopolymers and Biodegradable Plastics; Ebnesajjad, S., Ed.; William Andrew Publishing: Boston, MA, USA, 2013; pp. 87–107. [Google Scholar]
- Niinomi, M. Mechanical properties of biomedical titanium alloys. Mater. Sci. Eng. A 1998, 243, 231–236. [Google Scholar] [CrossRef]
- Albakry, M.; Guazzato, M.; Swain, M.V. Fracture toughness and hardness evaluation of three pressable all-ceramic dental materials. J. Dent. 2003, 31, 181–188. [Google Scholar] [CrossRef]
- Chen, Q.; Zhu, C.; Thouas, G.A. Progress and challenges in biomaterials used for bone tissue engineering: Bioactive glasses and elastomeric composites. Prog. Biomater. 2012, 1, 2. [Google Scholar] [CrossRef]
- Johnson, N.R.; Roberts, M.J.; Doi, S.A.; Batstone, M.D. Total temporomandibular joint replacement prostheses: A systematic review and bias-adjusted meta-analysis. Int. J. Oral Maxillofac. Surg. 2017, 46, 86–92. [Google Scholar] [CrossRef]
- George, E.; Liacouras, P.; Rybicki, F.J.; Mitsouras, D. Measuring and establishing the accuracy and reproducibility of 3d printed medical models. Radiographics 2017, 37, 1424–1450. [Google Scholar] [CrossRef]
- Zhang, K.; Yang, S.Y.; Yang, S.; Bai, L.; Li, P.; Liu, D.; Schurman, J.R., II; Wooley, P.H. Different influence of ti, pmma, uhmwpe, and co-cr particles on peripheral blood monocytes during periprosthetic inflammation. J. Biomed. Mater. Res. Part A 2015, 103, 358–364. [Google Scholar] [CrossRef]
- Rodrigues, Y.L.; Mathew, M.T.; Mercuri, L.G.; da Silva, J.S.P.; Henriques, B.; Souza, J.C.M. Biomechanical simulation of temporomandibular joint replacement (tmjr) devices: A scoping review of the finite element method. Int. J. Oral Maxillofac. Surg. 2018, 47, 1032–1042. [Google Scholar] [CrossRef]







| Nature of Prosthetic Temporomandibular Joint Parts | Prosthetic Glenoid Fossa Material | |||
|---|---|---|---|---|
| EBM-Ti | Zirconia | Acrylic | ||
| Prosthetic condyle material | EBM-Ti | Pair 1 | Pair 2 | Pair 3 |
| Zirconia | Pair 5 | Pair 4 | Pair 6 | |
| Acrylic | Pair 8 | Pair 9 | Pair 7 | |
| Sample Material (Condyle) | Opposing Material (Glenoid Fossa) | Pre-Test Weight (in Grams) | Post-Test Weight (in Grams) | Paired T-Test Values | |||||||
|---|---|---|---|---|---|---|---|---|---|---|---|
| Mean | S.D. | Mean | S.D. | Mean Diff. | S.E. | p-Value | T-Value | 95% C.I. | |||
| EBM-Ti | EBM-Ti | 9.91171 | 0.05663 | 9.90993 | 0.05726 | 0.00178 | 0.02500 | 0.94500 | 0.06990 | −0.05172 | 0.05528 |
| Zirconia | 10.17718 | 0.05815 | 10.17458 | 0.05879 | 0.00260 | 0.02600 | 0.92190 | 0.09940 | −0.05234 | 0.05753 | |
| Acrylic | 10.19273 | 0.05823 | 10.19183 | 0.05889 | 0.00090 | 0.02600 | 0.97300 | 0.03440 | −0.05412 | 0.05592 | |
| Zirconia | Zirconia | 11.84253 | 0.06861 | 11.84219 | 0.06868 | 0.00034 | 0.03100 | 0.99130 | 0.01115 | −0.06374 | 0.06442 |
| EBM-Ti | 11.70935 | 0.06783 | 11.70907 | 0.06790 | 0.00028 | 0.03000 | 0.99278 | 0.00918 | −0.06380 | 0.06436 | |
| Acrylic | 11.75028 | 0.06807 | 11.75010 | 0.06814 | 0.00018 | 0.03000 | 0.99530 | 0.00590 | −0.06381 | 0.06417 | |
| Acrylic | Acrylic | 5.29207 | 0.06205 | 5.29115 | 0.07802 | 0.00092 | 0.03200 | 0.97700 | 0.02920 | −0.06531 | 0.06715 |
| EBM-Ti | 5.30092 | 0.06215 | 5.29939 | 0.07814 | 0.00153 | 0.03200 | 0.96190 | 0.04850 | −0.06480 | 0.06786 | |
| Zirconia | 5.28628 | 0.06198 | 5.28463 | 0.07793 | 0.00165 | 0.03100 | 0.95880 | 0.05240 | −0.06450 | 0.06780 | |
| Sample Material (Glenoid Fossa) | Opposing Material (Condyle) | Pre-Test Weight (in Grams) | Post-Test Weight (in Grams) | Paired T-Test Values | |||||||
|---|---|---|---|---|---|---|---|---|---|---|---|
| Mean | S.D. | Mean | S.D. | Mean Diff. | S.E. | p-Value | T-Value | 95% C.I. | |||
| EBM-Ti | EBM-Ti | 16.62604 | 0.07611 | 16.62466 | 0.07659 | 0.00138 | 0.03400 | 0.96820 | 0.04040 | −0.07036 | 0.07312 |
| Zirconia | 17.85018 | 0.08172 | 17.84729 | 0.08222 | 0.00289 | 0.03700 | 0.93800 | 0.07880 | −0.07413 | 0.07991 | |
| Acrylic | 18.15195 | 0.08310 | 18.15093 | 0.08362 | 0.00102 | 0.03700 | 0.97850 | 0.02740 | −0.07730 | 0.07934 | |
| Zirconia | Zirconia | 16.50227 | 0.03746 | 16.50022 | 0.03753 | 0.00205 | 0.01700 | 0.90410 | 0.12230 | −0.03318 | 0.03729 |
| EBM-Ti | 17.24061 | 0.03913 | 17.23936 | 0.03922 | 0.00125 | 0.01800 | 0.94390 | 0.07130 | −0.03556 | 0.03806 | |
| Acrylic | 17.06166 | 0.03873 | 17.06126 | 0.03881 | 0.00040 | 0.01700 | 0.98180 | 0.02310 | −0.03603 | 0.03682 | |
| Acrylic | Acrylic | 15.43073 | 0.04929 | 15.42984 | 0.05218 | 0.00089 | 0.02300 | 0.96920 | 0.03920 | −0.04680 | 0.04858 |
| EBM-Ti | 15.31541 | 0.04892 | 15.31420 | 0.05179 | 0.00121 | 0.02300 | 0.95780 | 0.05370 | −0.04612 | 0.04854 | |
| Zirconia | 16.29016 | 0.05204 | 16.28533 | 0.05507 | 0.00483 | 0.02400 | 0.84250 | 0.20160 | −0.04551 | 0.05517 | |
| Sample Material (Condyle) | ||||||||||
|---|---|---|---|---|---|---|---|---|---|---|
| EBM-Ti | Zirconia | Acrylic | ||||||||
| Sample Material (Condyle) | Opposing Material (Glenoid Fossa) | EBM-Ti | Zirconia | Acrylic | Zirconia | EBM-Ti | Acrylic | Acrylic | EBM-Ti | Zirconia |
| EBM-Ti | EBM-Ti | - | 0.0008 | 0.0009 | 0.0014 | 0.0015 | 0.0016 | 0.0009 | 0.0003 | 0.0001 |
| Zirconia | - | - | 0.0017 | 0.0023 | 0.0023 | 0.0024 | 0.0017 | 0.0011 | 0.0009 | |
| Acrylic | - | - | - | 0.0006 | 0.0006 | 0.0007 | 0.0001 | 0.0006 | 0.0008 | |
| Zirconia | Zirconia | - | - | - | - | 0.0001 | 0.0002 | 0.0006 | 0.0012 | 0.0013 |
| EBM-Ti | - | - | - | - | - | 0.0001 | 0.0006 | 0.0012 | 0.0014 | |
| Acrylic | - | - | - | - | - | - | 0.0007 | 0.0013 | 0.0015 | |
| Acrylic | Acrylic | - | - | - | - | - | - | - | 0.0006 | 0.0007 |
| EBM-Ti | - | - | - | - | - | - | - | - | 0.0001 | |
| Zirconia | - | - | - | - | - | - | - | - | - | |
| Sample Material (Glenoid Fossa) | ||||||||||
|---|---|---|---|---|---|---|---|---|---|---|
| EBM-Ti | Zirconia | Acrylic | ||||||||
| Sample Material (Glenoid Fossa) | Opposing Material (Condyle) | EBM-Ti | Zirconia | Acrylic | Zirconia | EBM-Ti | Acrylic | Acrylic | EBM-Ti | Zirconia |
| EBM-Ti | EBM-Ti | - | 0.0015 | 0.0004 | 0.0007 | 0.0001 | 0.0013 | 0.0005 | 0.0002 | 0.0035 ** |
| Zirconia | - | - | 0.0019 | 0.0008 | 0.0016 | 0.0029 * | 0.0020 | 0.0017 | 0.0019 | |
| Acrylic | - | - | - | 0.0010 | 0.0002 | 0.0010 | 0.0001 | 0.0002 | 0.0038 ** | |
| Zirconia | Zirconia | - | - | - | - | 0.0008 | 0.0020 | 0.0012 | 0.0008 | 0.0028 * |
| EBM-Ti | - | - | - | - | - | 0.0012 | 0.0004 | 0.0001 | 0.0036 ** | |
| Acrylic | - | - | - | - | - | - | 0.0009 | 0.0012 | 0.0048 ** | |
| Acrylic | Acrylic | - | - | - | - | - | - | - | 0.0003 | 0.0039 ** |
| EBM-Ti | - | - | - | - | - | - | - | - | 0.0036 ** | |
| Zirconia | - | - | - | - | - | - | - | - | - | |
| Mechanical Properties | Biomaterial | Mature Cortical Bone | ||
|---|---|---|---|---|
| EBM Titanium (Ti6Al4V) | Zirconia (ZrO2) | Acrylic (PMMA) | ||
| Compressive Strength (MPa) | 940–970 | 1200–5200 | 105–117 | 100–230 |
| Tensile Strength (MPa) | 880–950 | 115–711 | 62–75 | 50–151 |
| Elastic Modulus (GPa) | 113.8–334.2 | 100–250 | 2.45–3.12 | 7–30 |
| Hardness (GPa) | 1.125–2.18 | 5.5–15.75 | 0.66–0.69 | 0.41–0.89 |
© 2019 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Alkindi, M.; Ramalingam, S.; Moiduddin, K.; Alghamdi, O.; Alkhalefah, H.; Badwelan, M. In Vitro Biomechanical Simulation Testing of Custom Fabricated Temporomandibular Joint Parts Made of Electron Beam Melted Titanium, Zirconia, and Poly-Methyl Methacrylate. Appl. Sci. 2019, 9, 5455. https://doi.org/10.3390/app9245455
Alkindi M, Ramalingam S, Moiduddin K, Alghamdi O, Alkhalefah H, Badwelan M. In Vitro Biomechanical Simulation Testing of Custom Fabricated Temporomandibular Joint Parts Made of Electron Beam Melted Titanium, Zirconia, and Poly-Methyl Methacrylate. Applied Sciences. 2019; 9(24):5455. https://doi.org/10.3390/app9245455
Chicago/Turabian StyleAlkindi, Mohammed, Sundar Ramalingam, Khaja Moiduddin, Osama Alghamdi, Hisham Alkhalefah, and Mohammed Badwelan. 2019. "In Vitro Biomechanical Simulation Testing of Custom Fabricated Temporomandibular Joint Parts Made of Electron Beam Melted Titanium, Zirconia, and Poly-Methyl Methacrylate" Applied Sciences 9, no. 24: 5455. https://doi.org/10.3390/app9245455
APA StyleAlkindi, M., Ramalingam, S., Moiduddin, K., Alghamdi, O., Alkhalefah, H., & Badwelan, M. (2019). In Vitro Biomechanical Simulation Testing of Custom Fabricated Temporomandibular Joint Parts Made of Electron Beam Melted Titanium, Zirconia, and Poly-Methyl Methacrylate. Applied Sciences, 9(24), 5455. https://doi.org/10.3390/app9245455





