Evaluation of Morphology and Prevalence of Palatoradicular Grooves on Affected Maxillary Anterior Teeth Using Cone-Beam Computed Tomography: An Institutional Retrospective Study
Abstract
1. Introduction

2. Materials and Methods
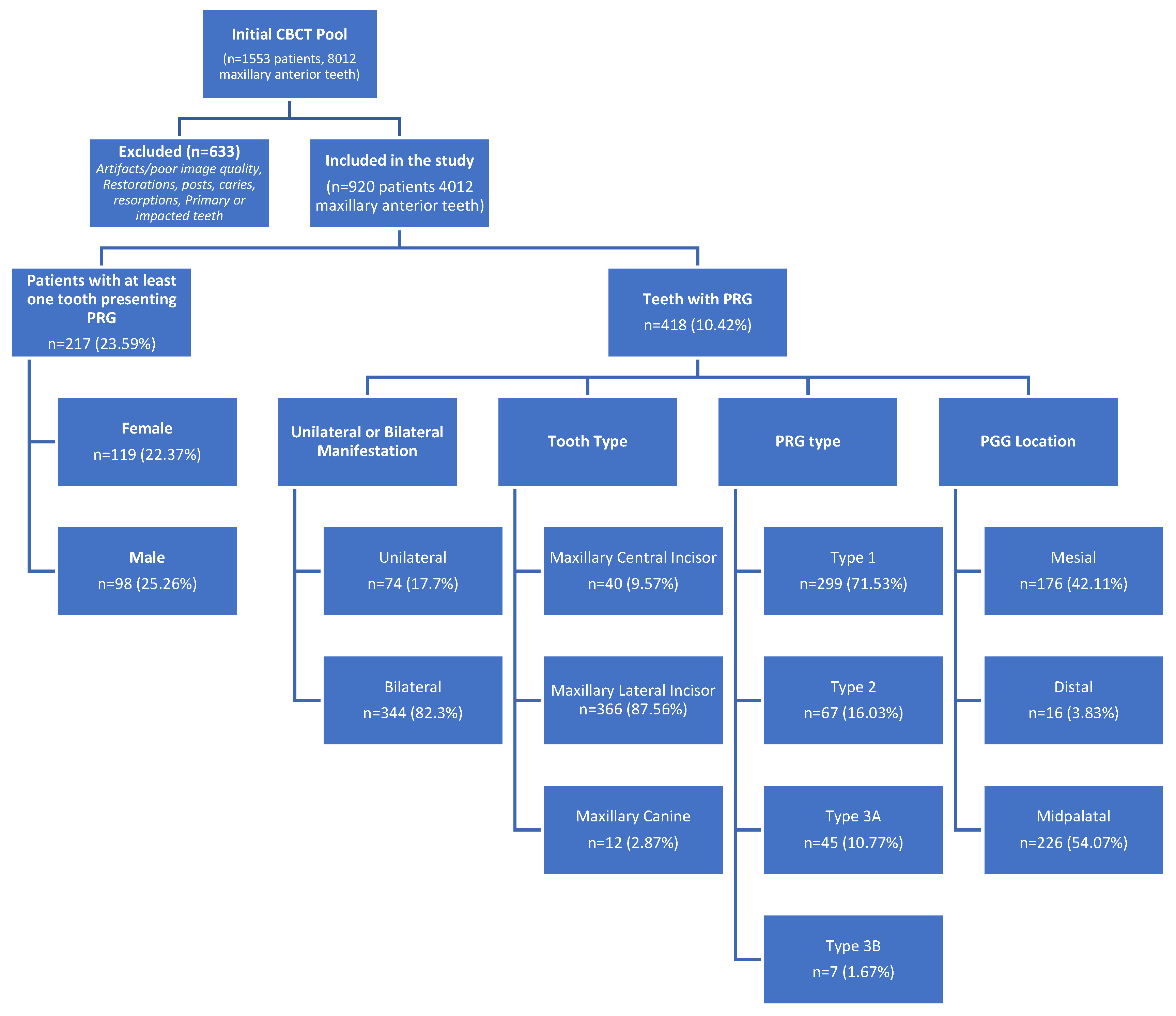
2.1. Study Sample
2.2. Sample Size Estimation
2.3. Inclusion and Exclusion Criteria
2.4. Image Assessment
2.5. Statistical Analysis
3. Results
4. Discussion
4.1. Sample Size and Basis of Calculation
- Zhang et al., (2022), in their CBCT study on 1715 Chinese patients, reported a patient-based prevalence of 8.4% and a tooth-based prevalence of 4.5% for lateral incisors [23].
- Aljuailan et al. (2023) found a patient-based prevalence of 6.3% and a tooth-based prevalence of 1.3% in a study of 509 patients [24].
- Aksoy et al. conducted a CBCT-based evaluation of 993 maxillary anterior teeth in 191 patients, reporting an overall prevalence of palatoradicular grooves (PGs) in 0.9% of teeth and 4.18% of patients [31].
4.2. Methodological Differences
4.2.1. CBCT Studies
4.2.2. In Vivo Studies Without CBCT
4.2.3. In Vitro Studies
4.3. Sample Composition
- Withers et al. (1981) also noted a prevalence of 8.5% in maxillary incisors [11].
- Arslan et al. reported an overall prevalence of radicular grooves (RGs) of 1.4% in incisors and 0.9% in all anterior teeth [25].
- In studies including all maxillary anterior teeth, the prevalence is distributed across central incisors, lateral incisors, and canines, leading to slightly lower overall rates compared to lateral, incisor-only studies. However, despite including all maxillary anterior teeth, our study reported a higher prevalence of 23.59% at the patient level and 10.42% at the tooth level. This may be due to our larger sample size (920 patients, 4012 teeth), detailed CBCT evaluations detecting subtle grooves, and inclusive criteria ensuring a representative sample.
4.4. Ethnic and Geographic Differences
- Withers et al. (1981) found no significant difference in PRG prevalence between White and Black populations [11].
- Zhang et al. (2022) and Demore et al. (2023), conducting studies in Chinese and Brazilian populations, respectively, reported prevalences of 8.4% and 21.67% [19,23]. While this may suggest potential regional differences, it is important to note that. Demore et al. (2023) found no significant racial differences within their Brazilian cohort, indicating that other factors such as sample size, methodology, or population-specific anatomical traits might account for these variations.
4.5. Limitations and Recommendations
5. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Conflicts of Interest
Abbreviations
| PRG | Palatoradicular groove |
| CBCT | Cone-beam computed tomography |
| AI | Artificial intelligence |
References
- Biswas, M.; Mazumdar, D.; Saha, B.; Agarwala, S.; Saha, K.K.; Chowdhury, K. Cone-beam Computed Tomographic Evaluation to Estimate the Prevalence of Palatogingival Groove in the Maxillary Anterior Teeth and Its Radiographic Characteristics: An Institutional Retrospective Study. J. Conserv. Dent. Endod. 2024, 27, 233–239. [Google Scholar] [CrossRef] [PubMed]
- Black, G.V. The Pathology of the Hard Tissues of the Teeth; Medico-Dental Publishing Company: Chicago, IL, USA, 1914; Volume 1. [Google Scholar]
- Everett, F.G.; Kramer, G.M. The Disto-Lingual Groove in the Maxillary Lateral Incisor; a Periodontal Hazard. J. Periodontol. 1972, 43, 352–361. [Google Scholar] [CrossRef] [PubMed]
- Simon, J.H.S.; Glick, D.H.; Frank, A.L. Predictable Endodontic and Periodontic Failures as a Result of Radicular Anomalies. Oral Surg. Oral Med. Oral Pathol. 1971, 31, 823–826. [Google Scholar] [CrossRef] [PubMed]
- Bačić, M.; Karakaš, Z.; Kaić, Z.; Šutalo, J. The Association Between Palatal Grooves in Upper Incisors and Periodontal Complications. J. Periodontol. 1990, 61, 197–199. [Google Scholar] [CrossRef] [PubMed]
- August, D.S. The Radicular Lingual Groove: An Overlooked Differential Diagnosis. J. Am. Dent. Assoc. 1978, 96, 1037–1039. [Google Scholar] [CrossRef] [PubMed]
- Meister, F.; Keating, K.; Gerstein, H.; Mayer, J.C. Successful Treatment of a Radicular Lingual Groove: Case Report. J. Endod. 1983, 9, 561–564. [Google Scholar] [CrossRef] [PubMed]
- Kogon, S.L. The Prevalence, Location and Conformation of Palato-Radicular Grooves in Maxillary Incisors. J. Periodontol. 1986, 57, 231–234. [Google Scholar] [CrossRef] [PubMed]
- Gound, T.G.; Maze, G.I. Treatment Options for the Radicular Lingual Groove: A Review and Discussion. Pract. Periodontics Aesthet. Dent. 1998, 10, 369–375; quiz 376. [Google Scholar] [PubMed]
- Lee, K.; Lee, E.C.; Poon, K. Palato-Gingival Grooves in Maxillary Incisors. A Possible Predisposing Factor to Localised Periodontal Disease. Br. Dent. J. 1968, 124, 14–18. [Google Scholar] [PubMed]
- Withers, J.A.; Brunsvold, M.A.; Killoy, W.J.; Rahe, A.J. The Relationship of Palato-Gingival Grooves to Localized Periodontal Disease. J. Periodontol. 1981, 52, 41–44. [Google Scholar] [CrossRef] [PubMed]
- Peikoff, M.D.; Perry, J.B.; Chapnick, L.A. Endodontic Failure Attributable to a Complex Radicular Lingual Groove. J. Endod. 1985, 11, 573–577. [Google Scholar] [CrossRef] [PubMed]
- Jia, J.; Cheng, M.; Shi, S.; Qiao, Y. Three-Year Follow-up Case Report: Root Canal Treatment Combined with Intentional Replantation for Treating Type III Palatogingival Groove in a Maxillary Lateral Incisor. Front. Oral Health 2024, 5, 1467327. [Google Scholar] [CrossRef] [PubMed]
- Pécora, J.D.; Sousa Neto, M.D.; Santos, T.C.; Saquy, P.C. In Vitro Study of the Incidence of Radicular Grooves in Maxillary Incisors. Braz. Dent. J. 1991, 2, 69–73. [Google Scholar] [PubMed]
- Goon, W.W.Y.; Carpenter, W.M.; Brace, N.M.; Ahlfeld, R.J. Complex Facial Radicular Groove in a Maxillary Lateral Incisor. J. Endod. 1991, 17, 244–248. [Google Scholar] [CrossRef] [PubMed]
- Smith, B.E.; Carroll, B. Maxillary Lateral Incisor with Two Developmental Grooves. Oral Surg. Oral Med. Oral Pathol. 1990, 70, 523–525. [Google Scholar] [CrossRef] [PubMed]
- Gu, Y.C. A Micro-Computed Tomographic Analysis of Maxillary Lateral Incisors with Radicular Grooves. J. Endod. 2011, 37, 789–792. [Google Scholar] [CrossRef] [PubMed]
- Tan, X.; Zhang, L.; Zhou, W.; Li, Y.; Ning, J.; Chen, X.; Song, D.; Zhou, X.; Huang, D. Palatal Radicular Groove Morphology of the Maxillary Incisors: A Case Series Report. J. Endod. 2017, 43, 827–833. [Google Scholar] [CrossRef] [PubMed]
- Demore, F.; Cecília, M.; Souza, A.; Zuza, E. Palatogingival Groove: Prevalence, Characteristics and Implications in a Cross-Sectional Study in Rio de Janeiro-Brazil. J. Int. Oral Health 2023, 15, 443–448. [Google Scholar] [CrossRef]
- Kim, H.-J.; Choi, Y.; Yu, M.-K.; Lee, K.-W.; Min, K.-S. Recognition and Management of Palatogingival Groove for Tooth Survival: A Literature Review. Restor. Dent. Endod. 2017, 42, 77. [Google Scholar] [CrossRef] [PubMed]
- Varun, K.; Arora, M.; Pubreja, L.; Juneja, R.; Middha, M. Prevalence of Dens Invaginatus and Palatogingival Groove in North India: A Cone-Beam Computed Tomography-Based Study. J. Conserv. Dent. 2022, 25, 306–310. [Google Scholar] [CrossRef] [PubMed]
- Wang, Y.; Su, S.; Chen, X.; Jia, X. CBCT Analysis of the Incidence of Maxillary Lateral Incisor Dens Invaginatus and Its Impact on Periodontal Supporting Tissues. BMC Oral Health 2024, 24, 1569. [Google Scholar] [CrossRef] [PubMed]
- Zhang, R.; Xiong, J.; Haapasalo, M.; Shen, Y.; Meng, L. Palatogingival Grooves Associated with Periodontal Bone Loss of Maxillary Incisors in a Chinese Population. Aust. Endod. J. 2022, 48, 313–321. [Google Scholar] [CrossRef] [PubMed]
- Aljuailan, A.I.; Aljuailan, R.; Gaikwad, R.N.; Kolarkodi, S.H.; Alamri, N.R. Prevalence of Palatogingival Groove Affecting Maxillary Anterior Teeth in Saudi Subpopulation: A Cone-Beam Computed Tomographic Study with Literature Review. Saudi Dent. J. 2023, 35, 1039–1047. [Google Scholar] [CrossRef] [PubMed]
- Arslan, H.; Ertas, E.T.; Topçuoǧlu, H.S.; Şekerci, A.E.; Atici, M.Y.; Ertas, H.; Demirbuǧa, S. Radicular Grooves of Maxillary Anterior Teeth in a Turkish Population: A Cone-Beam Computed Tomographic Study. Arch. Oral Biol. 2014, 59, 297–301. [Google Scholar] [CrossRef] [PubMed]
- Castelo-Baz, P.; Ramos-Barbosa, I.; Martín-Biedma, B.; Dablanca-Blanco, A.B.; Varela-Patiño, P.; Blanco-Carrión, J. Combined Endodontic-Periodontal Treatment of a Palatogingival Groove. J. Endod. 2015, 41, 1918–1922. [Google Scholar] [CrossRef] [PubMed]
- Durack, C.; Patel, S. The Use of Cone Beam Computed Tomography in the Management of Dens Invaginatus Affecting a Strategic Tooth in a Patient Affected by Hypodontia: A Case Report. Int. Endod. J. 2011, 44, 474–483. [Google Scholar] [CrossRef] [PubMed]
- Mazzi-Chaves, J.F.; Leoni, G.B.; Oliveira, J.S.; Silva-Sousa, Y.T.C.; Silva, R.G.; Pauwels, R.; Sousa-Neto, M.D. Influence of Anatomical Features in the Endodontic Treatment Planning of Maxillary Anterior Teeth. Braz. Oral Res. 2022, 36, e005. [Google Scholar] [CrossRef] [PubMed]
- Hamagharib, D.S.; Talabani, R.M.; Khursheed, D.A.; Saeed, H.M.M.; Saeed, K.M.M.; Hussein, S.A.; Noori, A.J. Prevalence of Palato Radicular Groove in Maxillary Lateral Incisors. IOSR J. Dent. Med. Sci. 2015, 14, 60–62. [Google Scholar] [CrossRef]
- Mahmood, A.; Sajid, M.; Jamil, M.; Tahir, M.W. PALATO GINGIVAL GROOVE. Prof. Med. J. 2019, 26. [Google Scholar] [CrossRef]
- Aksoy, U.; Kermeoğlu, F.; Kalender, A.; Eren, H.; Kolsuz, M.E.; Orhan, K. Cone-Beam Computed Tomography Evaluation of Palatogingival Grooves: A Retrospective Study with Literature Review. Oral Radiol. 2017, 33, 193–198. [Google Scholar] [CrossRef]
- Ghahramani, Y.; Haghighi, B.S.; Abbaszadegan, A.; Shahidi, S. Cone-Beam Computed Tomographic Evaluation of Radicular Grooves in Maxillary Anterior Teeth in a Selected Iranian Population. Iran. Endod. J. 2018, 13, 503–507. [Google Scholar] [CrossRef] [PubMed]
- Yildirim, D.P.; Goker Kamali, S. Prevalence of Palatogingival Groove and Its Association with Periapical Lesions and Periodontal Bone Loss: A Cone Beam Computed Tomography Study. BMC Oral Health 2025, 25, 313. [Google Scholar] [CrossRef] [PubMed]
- Pécora, J.D.; Miranda Da Cruz-Filho, A. Study of the Incidence of Radicular Grooves in Maxillary Incisors. Braz. Dent. J. 1992, .3, 11–16. [Google Scholar] [PubMed]
- Iqbal, N.; Tirmazi, S.M.; Majeed, H.A.; Munir, M.B. Prevalence of Palato Gingival Groove in Maxillary Lateral Incisors. Pak. Oral Dent. J. 2011, 31, 424–426. [Google Scholar]
- Shreshta, D.; Humagain, M.; Swastika, S. Prevalence of Palate-Gingival Groove in Patients of Dhulikhel Hospital. J. Coll. Med. Sci. 2014, 10, 32–36. [Google Scholar] [CrossRef]
- Lekshmi, M.S.; Sharma, S.; Gupta, S.R.; Sharma, S.; Kumar, V.; Chawla, A.; Logani, A. Prevalence and Radiological Characteristics of Palatogingival Groove: A Retrospective Cone-Beam Computed Tomography Study in an Indian Cohort. J. Conserv. Dent. 2022, 24, 359. [Google Scholar] [CrossRef]
- Albaricci, M.F.d.C.; de Toledo, B.E.C.; Zuza, E.P.; Gomes, D.A.S.; Rosetti, E.P. Prevalence and Features of Palato-Radicular Grooves: An In-Vitro Study. J. Int. Acad. Periodontol. 2008, 10, 2–5. [Google Scholar] [PubMed]
- Alkahtany, S.M.; Alrwais, F.; Altamimi, A.; Bukhary, S.M.; Mirdad, A. The Incidence of Radicular Groove on Maxillary Lateral Incisors of Saudi Population: CBCT Evaluation. BMC Oral Health 2022, 22, 583. [Google Scholar] [CrossRef] [PubMed]
- Hou, G.-L.; Tsai, C.-C. Relationship between Palato-Radicular Grooves and Localized Periodontitis. J. Clin. Periodontol. 1993, 20, 678–682. [Google Scholar] [CrossRef] [PubMed]
- Jeng, J.H.; Lu, H.-K.J.; Hou, L.T. Treatment of an Osseous Lesion Associated with a Severe Palato-Radicular Groove: A Case Report. J. Periodontol. 1992, 63, 708–712. [Google Scholar] [CrossRef] [PubMed]
- Schwartz, S.A.; Koch, M.A.; Deas, D.E.; Powell, C.A. Combined Endodontic-Periodontic Treatment of a Palatal Groove: A Case Report. J. Endod. 2006, 32, 573–578. [Google Scholar] [CrossRef] [PubMed]
- Forero-López, J.; Gamboa-Martínez, L.; Pico-Porras, L.; Niño-Barrera, J.L. Surgical Management with Intentional Replantation on a Tooth with Palato-Radicular Groove. Restor. Dent. Endod. 2014, 40, 166. [Google Scholar] [CrossRef] [PubMed]
- Attam, K.; Tiwary, R.; Talwar, S.; Lamba, A.K. Palatogingival Groove: Endodontic-Periodontal Management—Case Report. J. Endod. 2010, 36, 1717–1720. [Google Scholar] [CrossRef] [PubMed]
- Torabinejad, M.; Dinsbach, N.A.; Turman, M.; Handysides, R.; Bahjri, K.; White, S.N. Survival of Intentionally Replanted Teeth and Implant-Supported Single Crowns: A Systematic Review. J. Endod. 2015, 41, 992–998. [Google Scholar] [CrossRef] [PubMed]
- Simon, J.H.S.; Dogan, H.; Ceresa, L.M.; Silver, G.K. The Radicular Groove: Its Potential Clinical Significance. J. Endod. 2000, 26, 295–298. [Google Scholar] [CrossRef] [PubMed]
- Wei, P.; Geivelis, M.; Chan, C.; Ju, Y. Successful Treatment of Pulpal-Periodontal Combined Lesion in a Birooted Maxillary Lateral Incisor with Concomitant Palato-Radicular Groove. A Case Report. J. Periodontol. 1999, 70, 1540–1546. [Google Scholar] [CrossRef] [PubMed]

| Gender | Patients Examined | Patients with PRG | Unilateral | Bilateral |
|---|---|---|---|---|
| Female | 532 | 119 (22.37%) | 36 (6.77%) | 83 (15.6%) |
| Male | 388 | 98 (25.26%) | 23 (5.93%) | 75 (19.33%) |
| Total | 920 | 217 (23.59%) | 59 (6.41%) | 158 (17.17%) |
| p value | - | 0.347 | 0.335 | <0.001 * |
| Tooth Type | Teeth with PRG (%) | Unilateral PRGs | Bilateral PRGs |
|---|---|---|---|
| Maxillary central incisor | 40 (9.57%) | 10 (2.39%) | 30 (7.18%) |
| Maxillary lateral incisor | 366 (87.56%) | 60 (14.35%) | 306 (73.21%) |
| Maxillary canine | 12 (2.87%) | 4 (0.96%) | 8 (1.91%) |
| Total | 418 | 74 (17.7%) | 344 (82.3%) |
| p value | <0.001 1 | — | <0.001 2 |
| Tooth Type | Teeth with PRG (%) | Type 1 | Type 2 | Type 3A | Type 3B |
|---|---|---|---|---|---|
| Maxillary central incisor | 40 (9.57%) | 35 (8.37%) | 1 (0.24%) | 4 (0.96%) | - |
| Maxillary lateral incisor | 366 (87.56%) | 253 (60.53%) | 66 (15.79%) | 40 (9.57%) | 7 (1.67%) |
| Maxillary canine | 12 (2.87%) | 11 (2.63%) | - | 1 (0.24%) | - |
| Total | 418 | 299 (71.53%) | 67 (16.03%) | 45 (10.77%) | 7 (1.67%) |
| p value | <0.001 1 | <0.001 2 | <0.001 3 | <0.001 4 | — |
| Tooth Type | Teeth with PRG (%) | Mesial | Distal | Midpalatal |
|---|---|---|---|---|
| Maxillary central incisor | 40 (9.57%) | 8 (1.91%) | 1 (0.24%) | 31 (7.42%) |
| Maxillary lateral incisor | 366 (87.56%) | 164 (39.23%) | 11 (2.63%) | 191 (45.69%) |
| Maxillary canine | 12 (2.87%) | 4 (0.96%) | 4 (0.96%) | 4 (0.96%) |
| Total | 418 | 176 (42.11%) | 16 (3.83%) | 226 (54.07%) |
| p value | p < 0.001 1 | 0.037 2 | <0.001 3 | <0.001 3 |
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2025 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Baştuğ, D.; Ayrancı, L.B. Evaluation of Morphology and Prevalence of Palatoradicular Grooves on Affected Maxillary Anterior Teeth Using Cone-Beam Computed Tomography: An Institutional Retrospective Study. Appl. Sci. 2025, 15, 8031. https://doi.org/10.3390/app15148031
Baştuğ D, Ayrancı LB. Evaluation of Morphology and Prevalence of Palatoradicular Grooves on Affected Maxillary Anterior Teeth Using Cone-Beam Computed Tomography: An Institutional Retrospective Study. Applied Sciences. 2025; 15(14):8031. https://doi.org/10.3390/app15148031
Chicago/Turabian StyleBaştuğ, Dilara, and Leyla Benan Ayrancı. 2025. "Evaluation of Morphology and Prevalence of Palatoradicular Grooves on Affected Maxillary Anterior Teeth Using Cone-Beam Computed Tomography: An Institutional Retrospective Study" Applied Sciences 15, no. 14: 8031. https://doi.org/10.3390/app15148031
APA StyleBaştuğ, D., & Ayrancı, L. B. (2025). Evaluation of Morphology and Prevalence of Palatoradicular Grooves on Affected Maxillary Anterior Teeth Using Cone-Beam Computed Tomography: An Institutional Retrospective Study. Applied Sciences, 15(14), 8031. https://doi.org/10.3390/app15148031






