Tears as the Next Diagnostic Biofluid: A Comparative Study between Ocular Fluid and Blood
Abstract
:1. Introduction
2. Materials and Methods
2.1. Study Population
2.2. Plasma Sample Collection
2.3. Tear Sample Collection
2.4. Microarray Sample Preparation and Analysis
2.5. RNA Extraction for Small RNA-Seq
2.6. Library Prep with RealSeq-Dual
3. Results and Discussion
3.1. Microarray
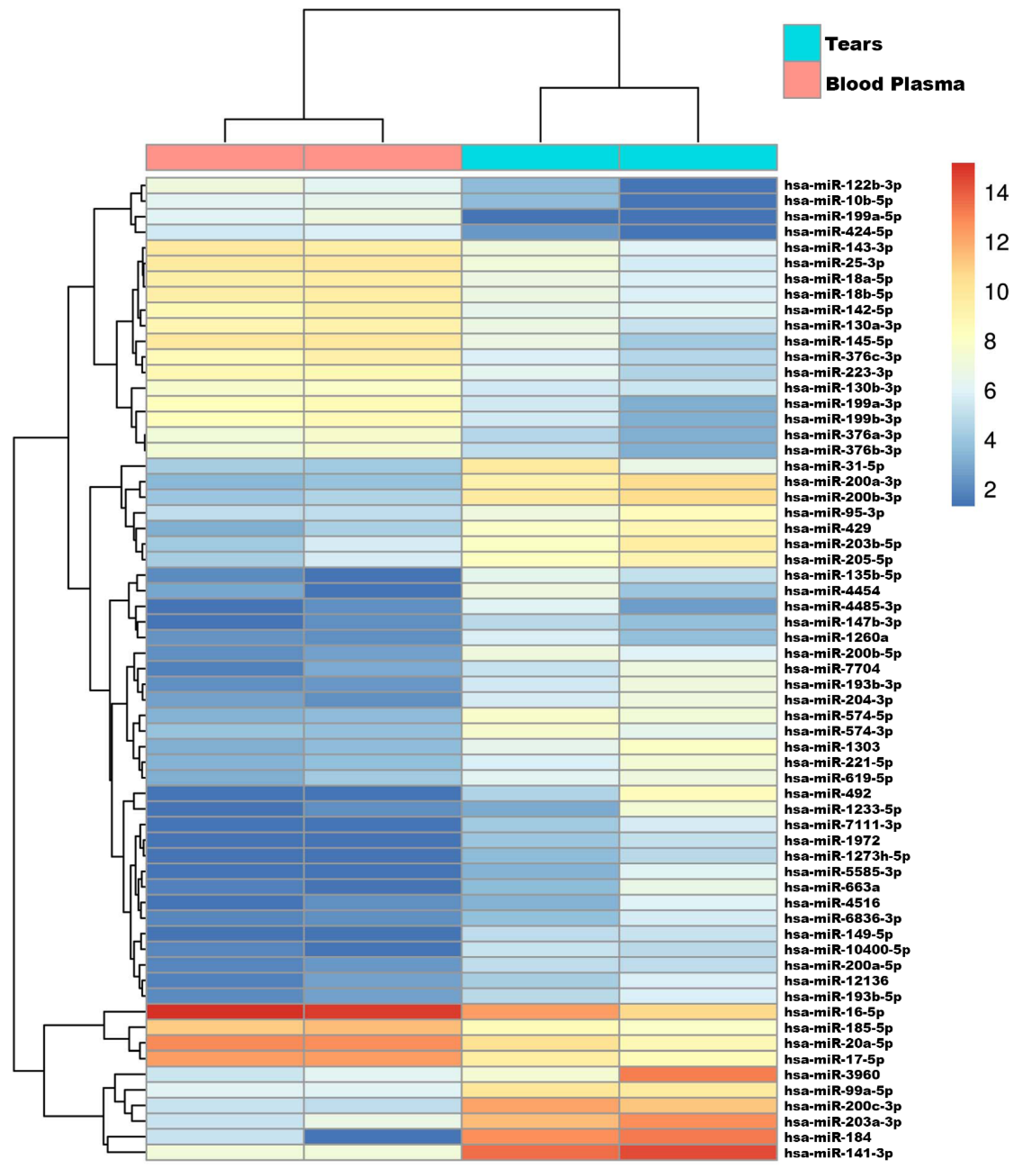
3.2. MicroRNA
4. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Acknowledgments
Conflicts of Interest
Appendix A
| Present in Tears | Present in Plasma | ||
|---|---|---|---|
| 14.3.3 gamma | Keratin 8/18 | Adiponectin | IGF-BP3 |
| 14.3.3, Pan | LewisA | Apolipoprotein E3 (Apo E3) | IL-5 |
| anti-Sm | LewisB | beta-Nerve Growth Factor (beta-NGF) | LH |
| Calponin | Metastasis-associated protein MTA1 (MAT1) | Bim (BOD) | Mucin 3 (MUC3) |
| CD25/IL-2 Receptor a | MLH1 | CD71/Transferrin Receptor | NOS-i |
| CD45RO | Mucin 5AC | Collagen II | p27Kip1 |
| CD84 | Mucin-13 (MUC13) | CREB | p63 (p53 Family Member) |
| EMA/CA15-3/MUC-1 | Myeloperoxidase | DFF40 (DNA Fragmentation Factor 40)/CAD | Parkin |
| Heat Shock Protein 70/hsp70 | Myostatin | E2F-5 | PARP (Poly ADP-Ribose Polymerase) |
| Heparan Sulfate Proteoglycan | Paxillin | Eotaxin-3 | Plasma Cell Marker |
| HER3/erbB3 | PR3 (Proteinase 3) | Factor VIII Related Antigen | Plasminogen |
| HPV 16 | S100A4 | Fibronectin | Retinol Binding Protein |
| IL-1RA | S100A6 | HRP | SV40 Large T Antigen |
| Involucrin | SHP-1 | ||
| Keratin 10 | TAG 72/CA72-4 | ||
| Keratin 16 | Thymidine Phosphorylase | ||
| Keratin 5/6/18 | Transglutaminase II | ||
References
- Magni, F.; Van Der Burgt, Y.E.; Chinello, C.; Mainini, V.; Gianazza, E.; Squeo, V.; Deelder, A.M.; Kienle, M.G. Biomarkers discovery by peptide and protein profiling in biological fluids based on functionalized magnetic beads purification and mass spectrometry. Blood Transfus. 2010, 8 (Suppl. S3), s92–s97. [Google Scholar] [CrossRef] [PubMed]
- Rafeie, M.; Zhang, J.; Asadnia, M.; Li, W.; Warkiani, M.E. Multiplexing slanted spiral microchannels for ultra-fast blood plasma separation. Lab Chip 2016, 16, 2791–2802. [Google Scholar] [CrossRef] [PubMed]
- Anjo, S.I.; Manadas, B. A translational view of cells’ secretome analysis—From untargeted proteomics to potential circulating biomarkers. Biochimie 2018, 155, 37–49. [Google Scholar] [CrossRef] [PubMed]
- Geyer, P.E.; Holdt, L.M.; Teupser, D.; Mann, M. Revisiting biomarker discovery by plasma proteomics. Mol. Syst. Biol. 2017, 13, 942. [Google Scholar] [CrossRef] [PubMed]
- Rosado, M.; Silva, R.; Bexiga, M.G.; Jones, J.G.; Manadas, B.; Anjo, S.I. Advances in biomarker detection: Alternative approaches for blood-based biomarker detection. Adv. Clin. Chem. 2019, 92, 141–199. [Google Scholar] [CrossRef] [PubMed]
- Yu, Z.T.; Aw Yong, K.M.; Fu, J. Microfluidic blood cell sorting: Now and beyond. Small 2014, 10, 1687–1703. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Pieragostino, D.; D’Alessandro, M.; di Ioia, M.; Di Ilio, C.; Sacchetta, P.; Del Boccio, P. Unraveling the molecular repertoire of tears as a source of biomarkers: Beyond ocular diseases. Proteom.-Clin. Appl. 2015, 9, 169–186. [Google Scholar] [CrossRef]
- Moshirfar, M.; Pierson, K.; Hanamaikai, K.; Santiago-Caban, L.; Muthappan, V.; Passi, S.F. Artificial tears potpourri: A literature review. Clin. Ophthalmol. 2014, 8, 1419–1433. [Google Scholar] [CrossRef] [Green Version]
- Posa, A.; Bräuer, L.; Schicht, M.; Garreis, F.; Beileke, S.; Paulsen, F. Schirmer strip vs. capillary tube method: Non-invasive methods of obtaining proteins from tear fluid. Ann. Anat.-Anat. Anz. 2013, 195, 137–142. [Google Scholar] [CrossRef]
- Akkurt Arslan, M.; Kolman, I.; Pionneau, C.; Chardonnet, S.; Magny, R.; Baudouin, C.; Brignole-Baudouin, F.; Kessal, K. Proteomic Analysis of Tears and Conjunctival Cells Collected with Schirmer Strips Using timsTOF Pro: Preanalytical Considerations. Metabolites 2022, 12, 2. [Google Scholar] [CrossRef]
- Aass, C.; Norheim, I.; Eriksen, E.F.; Thorsby, P.M.; Pepaj, M. Single unit filter-aided method for fast proteomic analysis of tear fluid. Anal. Biochem. 2015, 480, 1–5. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Azkargorta, M.; Soria, J.; Acera, A.; Iloro, I.; Elortza, F. Human tear proteomics and peptidomics in ophthalmology: Toward the translation of proteomic biomarkers into clinical practice. J. Proteom. 2017, 150, 359–367. [Google Scholar] [CrossRef] [PubMed]
- Versura, P.; Campos, E. Disease Update on Human Tear Proteome. J.-Dis. Update Hum. Tear Proteome 2013, 7, 36. [Google Scholar] [CrossRef]
- Pieczyński, J.; Szulc, U.; Harazna, J.; Szulc, A.; Kiewisz, J. Tear fluid collection methods: Review of current techniques. Eur. J. Ophthalmol. 2021, 31, 2245–2251. [Google Scholar] [CrossRef]
- Martin, M. Cutadapt removes adapter sequences from high-throughput sequencing reads. EMBnet. J. 2011, 17, 10–12. [Google Scholar] [CrossRef]
- Langmead, B.; Trapnell, C.; Pop, M.; Salzberg, S.L. Ultrafast and memory-efficient alignment of short DNA sequences to the human genome. Genome Biol. 2009, 10, R25. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Love, M.I.; Huber, W.; Anders, S. Moderated estimation of fold change and dispersion for RNA-seq data with DESeq2. Genome Biol. 2014, 15, 550. [Google Scholar] [CrossRef] [Green Version]
- Hicks, S.D.; Johnson, J.; Carney, M.C.; Bramley, H.; Olympia, R.P.; Loeffert, A.C.; Thomas, N.J. Overlapping MicroRNA Expression in Saliva and Cerebrospinal Fluid Accurately Identifies Pediatric Traumatic Brain Injury. J. Neurotrauma 2018, 35, 64–72. [Google Scholar] [CrossRef]
- LaRocca, D.; Barns, S.; Hicks, S.D.; Brindle, A.; Williams, J.; Uhlig, R.; Johnson, P.; Neville, C.; Middleton, F.A. Comparison of serum and saliva miRNAs for identification and characterization of mTBI in adult mixed martial arts fighters. PLoS ONE 2019, 14, e0207785. [Google Scholar] [CrossRef] [Green Version]
- Kim, Y.J.; Yeon, Y.; Lee, W.J.; Shin, Y.U.; Cho, H.; Sung, Y.K.; Kim, D.R.; Lim, H.W.; Kang, M.H. Comparison of MicroRNA Expression in Tears of Normal Subjects and Sjogren Syndrome Patients. Investig. Ophthalmol. Vis. Sci. 2019, 60, 4889–4895. [Google Scholar] [CrossRef] [Green Version]
- Sun, Z.; Shi, K.; Yang, S.; Liu, J.; Zhou, Q.; Wang, G.; Song, J.; Li, Z.; Zhang, Z.; Yuan, W. Effect of exosomal miRNA on cancer biology and clinical applications. Mol. Cancer 2018, 17, 147. [Google Scholar] [CrossRef]
- Li, X.; Corbett, A.L.; Taatizadeh, E.; Tasnim, N.; Little, J.P.; Garnis, C.; Daugaard, M.; Guns, E.; Hoorfar, M.; Li, I.T.S. Challenges and opportunities in exosome research-Perspectives from biology, engineering, and cancer therapy. APL Bioeng. 2019, 3, 011503. [Google Scholar] [CrossRef] [Green Version]
- Hu, G.; Drescher, K.M.; Chen, X.M. Exosomal miRNAs: Biological Properties and Therapeutic Potential. Front. Genet. 2012, 3, 56. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Inubushi, S.; Kawaguchi, H.; Mizumoto, S.; Kunihisa, T.; Baba, M.; Kitayama, Y.; Takeuchi, T.; Hoffman, R.M.; Tanino, H.; Sasaki, R. Oncogenic miRNAs Identified in Tear Exosomes from Metastatic Breast Cancer Patients. Anticancer Res. 2020, 40, 3091–3096. [Google Scholar] [CrossRef]
- Kenny, A.; Jimenez-Mateos, E.M.; Zea-Sevilla, M.A.; Rabano, A.; Gili-Manzanaro, P.; Prehn, J.H.M.; Henshall, D.C.; Avila, J.; Engel, T.; Hernandez, F. Proteins and microRNAs are differentially expressed in tear fluid from patients with Alzheimer’s disease. Sci. Rep. 2019, 9, 15437. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Weber, J.A.; Baxter, D.H.; Zhang, S.; Huang, D.Y.; Huang, K.H.; Lee, M.J.; Galas, D.J.; Wang, K. The microRNA spectrum in 12 body fluids. Clin. Chem. 2010, 56, 1733–1741. [Google Scholar] [CrossRef] [PubMed]
- Böhm, D.; Keller, K.; Pieter, J.; Boehm, N.; Wolters, D.; Siggelkow, W.; Lebrecht, A.; Schmidt, M.; Koelbl, H.; Pfeiffer, N. Comparison of tear protein levels in breast cancer patients and healthy controls using a de novo proteomic approach. Oncol. Rep. 2012, 28, 429–438. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Lebrecht, A.; Boehm, D.; Schmidt, M.; Koelbl, H.; Schwirz, R.L.; Grus, F.H. Diagnosis of breast cancer by tear proteomic pattern. Cancer Genom. Proteom. 2009, 6, 177–182. [Google Scholar]
- Ou, F.S.; Michiels, S.; Shyr, Y.; Adjei, A.A.; Oberg, A.L. Biomarker Discovery and Validation: Statistical Considerations. J. Thorac. Oncol. 2021, 16, 537–545. [Google Scholar] [CrossRef]
- Bedogni, G.; Tsybakov, A.; Berlin, S. Clinical prediction models—A practical approach to development, validation and updating. Development 2009, 18, 53. [Google Scholar] [CrossRef]
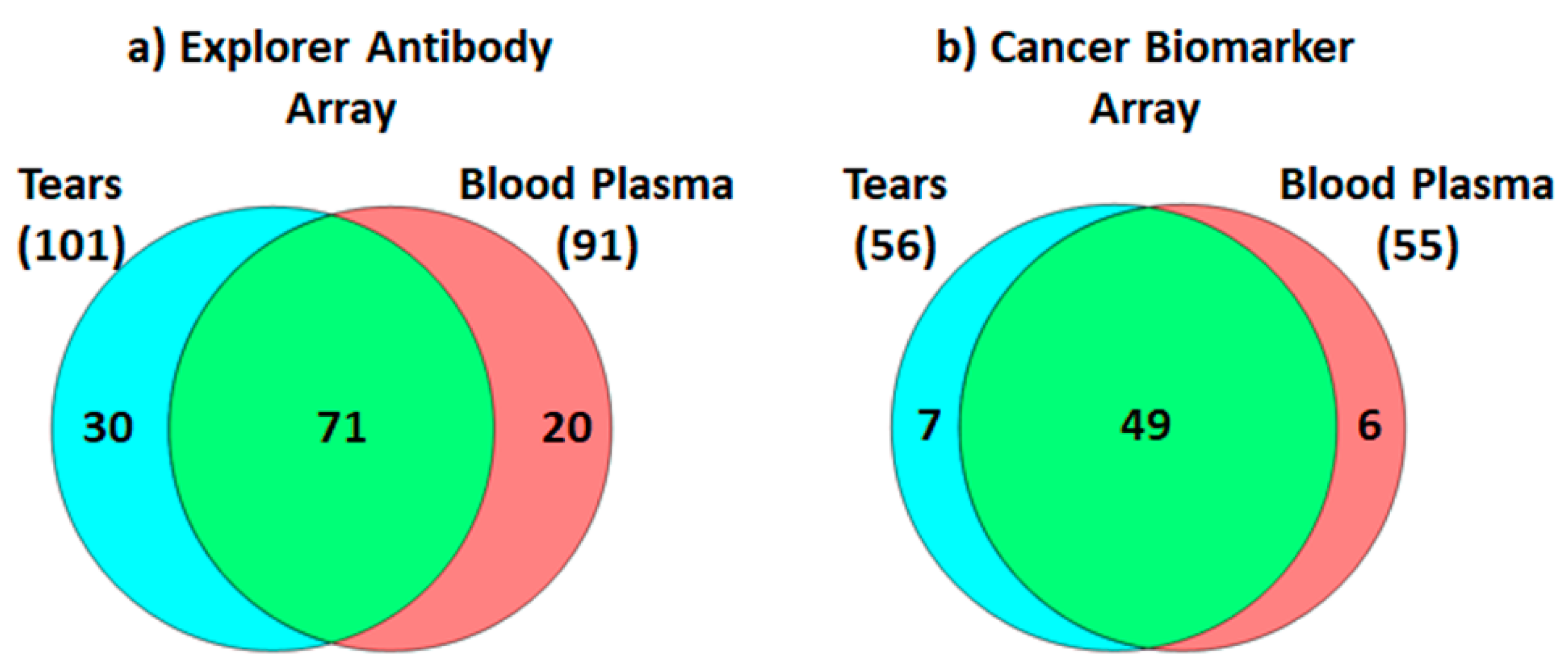
| Present in Tear and Plasma | |||
|---|---|---|---|
| ADP-ribosylation Factor (ARF-6) | CNPase | IL-12 | Parathyroid Hormone-related Protein |
| Alpha-fetoprotein (AFP) | Collagen I | IL-15 | Pax-5 |
| Apoptosis Inducing Factor (AIF) | Collagen II | Interleukin-1 receptor associated kinase (IRAK) | PDGFR alpha |
| Alpha 1 Antichymotrypsin (ACT) | Collagen III | Kappa Light Chain | PDGFR, beta |
| Alpha Lactalbumin | Collagen IV | Keratin 19 | PLC gamma 1 |
| alpha-1-antitrypsin | Cullin-3 (CUL-3) | Keratin 8 | Prohibitin |
| Bcl-2-like protein 1 (bcl-XL) | Cyclin B1 | Ku (p70/p80) | Prolactin Receptor |
| Beta actin | Desmin | Lambda Light Chain | pS2 |
| Beta-2-Microglobulin | Epithelial Specific Antigen | Laminin B1/b1 | Rad18 |
| Biotin | Ferritin | Laminin Receptor | Ras |
| Chemokine receptor type 6 (CXCR6) | Fibronectin | Laminin-s | sIL-2R alpha |
| Cancer Antigen 15-3 (CA15-3) | Follicle Stimulating Hormone (FSH) | Calprotectin | Silencer of Death Domain (SODD) |
| Cancer Antigen 19-9 (CA19-9) | Follistatin | Mammaglobin B | Streptavidin |
| Tyrosine-protein kinase ABL1 (c-Abl) | Gai1 | Mek2 | TGF beta Receptor III |
| Cadherin-pan | Glucagon | MGMT | TGF beta1 |
| Caspase 1 | Glycogen Synthase Kinase 3b (GSK3b) | MHC II (HLA-DP and DR) | Thymidylate Synthase |
| Caspase 7 (Mch 3) | Granulocyte Colony Stimulating Factor | MMP-1 | Thyroglobulin |
| CD1 | Glutathione S-transferase (GST) | MMP-10 | Thyroid Hormone Receptor alpha |
| CD10 | Haptoglobin | MMP-11 | TIMP-1 |
| CD1b | Heat Shock Protein 27/hsp27 | MMP-2 | TR2 |
| CD2 | Hepatocyte Growth Factor Receptor (MET) | MMP-2 (72 kDa Collagenase IV) | Transferrin |
| CD35/CR1 | hPL | MMP-7 | Tubulin alpha |
| CD40L Receptor | human Albumin | MSH2 | Tubulin gamma |
| CD42b | IgA | Mucin 2 | Uracil-DNA Glycosylase (UNG) |
| CD45/T200/LCA | IgA | MUTYH | VCAM-1 |
| CD57 | IgG | MyoD1 | VEGFB |
| Cdk1/p34cdc2 | IgG | Neutrophil Elastase | Vitamin D Receptor (VDR) |
| Cdk7 | IgM | Nitric Oxide Synthase, brain (bNOS) | Xanthine Oxidase |
| Cdk8 | IgM (m-Heavy Chain) | p130 | |
| CEA/CD66e | p19ARF | p130cas | |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2022 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Ravishankar, P.; Daily, A. Tears as the Next Diagnostic Biofluid: A Comparative Study between Ocular Fluid and Blood. Appl. Sci. 2022, 12, 2884. https://doi.org/10.3390/app12062884
Ravishankar P, Daily A. Tears as the Next Diagnostic Biofluid: A Comparative Study between Ocular Fluid and Blood. Applied Sciences. 2022; 12(6):2884. https://doi.org/10.3390/app12062884
Chicago/Turabian StyleRavishankar, Prashanth, and Anna Daily. 2022. "Tears as the Next Diagnostic Biofluid: A Comparative Study between Ocular Fluid and Blood" Applied Sciences 12, no. 6: 2884. https://doi.org/10.3390/app12062884
APA StyleRavishankar, P., & Daily, A. (2022). Tears as the Next Diagnostic Biofluid: A Comparative Study between Ocular Fluid and Blood. Applied Sciences, 12(6), 2884. https://doi.org/10.3390/app12062884






