Gastrocnemius Activation throughout the Competitive Season in Athletes of Different Experience Levels
Abstract
1. Introduction
2. Materials and Methods
3. Results
4. Discussion
5. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Conflicts of Interest
References
- Mickevičius, M.; Degens, H.; Kesminas, R.; Rutkauskas, S.; Satkunskiene, D.; Vadopalas, K.; Pukenas, K.; Jürimäe, J.; Skurvydas, A.; Kamandulis, S. Early anterior knee pain in male adolescent basketball players is related to body height and abnormal knee morphology. Phys. Ther. Sport 2018, 32, 273–281. [Google Scholar] [CrossRef] [PubMed]
- Haskell, W.L.; Lee, I.M.; Pate, R.R.; Powell, K.E.; Blair, S.N.; Franklin, B.A.; Macera, C.A.; Heath, G.W.; Thompson, P.D.; Bauman, A. Physical activity and public health: Updated recommendation for adults from the American College of Sports Medicine and the American Heart Association. Med. Sci. Sports Exerc. 2007, 39, 1423–1434. [Google Scholar] [CrossRef] [PubMed]
- Kong, Z.; Qi, F.; Shi, Q. The influence of basketball dribbling on repeated high-intensity intermittent runs. J. Exerc. Sci. Fit. 2015, 13, 117–122. [Google Scholar] [CrossRef] [PubMed]
- Castagna, C.; Abt, G.; Manzi, V.; Annino, G.; Padua, E.; D’Ottavio, S. Effect of recovery mode on repeated sprint ability in young basketball players. J. Strength Cond. Res. 2008, 22, 923–929. [Google Scholar] [CrossRef] [PubMed]
- Piedra, A.; Peña, J.; Ciavattini, V.; Caparrós, T. Relationship between injury risk, workload, and rate of perceived exertion in professional women’s basketball. Apunts Sports Med. 2020, 55, 71–79. [Google Scholar] [CrossRef]
- Abdelkrim, N.B.; El Fazaa, S.; El Ati, J. Time-motion analysis and physiological data of elite under-19-year-old basketball players during competition. Br. J. Sport Med. 2007, 41, 69–75. [Google Scholar] [CrossRef]
- Figueira, B.; Gonçalves, B.; Abade, E.A.; Paulauskas, R.; Masiulis, N.; Sampaio, J. Effects of a 4-week combined sloped training program in young basketball players’ physical performance. Sci. Sports 2019, 35, e1–e172. [Google Scholar] [CrossRef]
- Oliver, J.A. Basketball Fundamentals; Human Kinetics Publishers: Champaign, IL, USA, 2003; pp. 49–51. [Google Scholar]
- Borowski, L.A.; Yard, E.E.; Fields, S.K.; Comstock, R.D. The Epidemiology of US High School Basketball Injuries, 2005–2007. Epidemiol. US High Sch. Basketb. Inj. 2008, 36, 2328–2335. [Google Scholar] [CrossRef]
- Caine, D.; Maffulli, N.; Caine, C. Epidemiology of Injury in Child and Adolescent Sports: Injury Rates, Risk Factors, and Prevention. Clin. Sport Med. 2008, 27, 19–50. [Google Scholar] [CrossRef]
- Frisch, A.; Croisier, J.L.; Urhausen, A.; Seil, R.; Theisen, D. Injuries, risk factors and prevention initiatives in youth sport. Br. Med. Bull. 2009, 92, 95–121. [Google Scholar] [CrossRef][Green Version]
- Cumps, E.; Verhagen, E.; Meeusen, R. Prospective epidemiological study of basketball injuries during one competitive season: Ankle sprains and overuse knee injuries. J. Sports Sci. Med. 2007, 6, 204–211. [Google Scholar] [PubMed]
- Baker, H.; Rizzi, A.; Athiviraham, A. Injury in the Women’s National Basketball Association (WNBA) From 2015 to 2019. Arthrosc. Sport Med. Rehabil. 2020, 2, e213–e217. [Google Scholar] [CrossRef] [PubMed]
- Siu, R.; Ling, S.K.K.; Fung, N.; Pak, N.; Yung, P.S.H. Prognosis of elite basketball players after an Achilles tendon rupture. Asia-Pac. J. Sport Med. Arthrosc. Rehabil. Technol. 2020, 21, 5–10. [Google Scholar]
- Deitch, J.R.; Starkey, C.; Walters, S.L.; Moseley, J.B. Injury risk in professional basketball players: A comparison of Women’s National Basketball Association and National Basketball Association athletes. Am. J. Sports Med. 2006, 34, 1077–1083. [Google Scholar] [CrossRef]
- Agel, J.; Arendt, E.A.; Bershadsky, B. Anterior cruciate ligament injury in national collegiate athletic association basketball and soccer: A 13-year review. Am. J. Sports Med. 2005, 33, 524–530. [Google Scholar] [CrossRef]
- Klyne, D.M.; Keays, S.L.; Bullock-Saxton, J.E.; Newcombe, P.A. The effect of anterior cruciate ligament rupture on the timing and amplitude of gastrocnemius muscle activation: A study of alterations in EMG measures and their relationship to knee joint stability. J. Electromyogr. Kinesiol. 2012, 22, 446–455. [Google Scholar] [CrossRef]
- Morgan, K.D.; Donnelly, C.J.; Reinbolt, J.A. Elevated gastrocnemius forces compensate for decreased hamstrings forces during the weight-acceptance phase of single-leg jump landing: Implications for anterior cruciate ligament injury risk. J. Biomech. 2014, 47, 3295–3302. [Google Scholar] [CrossRef]
- Dewar, R.A.; Arnold, G.P.; Wang, W.; Drew, T.S.; Abboud, R.J. Comparison of 3 ankle braces in reducing ankle inversion in a basketball rebounding task. Foot (Edinb.) 2019, 39, 129–135. [Google Scholar] [CrossRef]
- McKay, G.D.; Goldie, P.A.; Payne, W.R.; Oakes, B.W. Ankle injuries in basketball: Injury rate and risk factors. Br. J. Sports Med. 2001, 35, 103–108. [Google Scholar] [CrossRef]
- Fong, D.T.; Hong, Y.; Chan, L.K.; Yung, P.S.; Chan, K.M. A systematic review on ankle injury and ankle sprain in sports. Sports Med. 2007, 37, 73–94. [Google Scholar] [CrossRef]
- Longo, U.G.; Loppini, M.; Berton, A.; Marinozzi, A.; Maffulli, N.; Denaro, V. The FIFA 11+ program is effective in preventing injuries in elite male basketball players: A cluster randomized controlled trial. Am. J. Sports Med. 2012, 40, 996–1005. [Google Scholar] [CrossRef] [PubMed]
- Klem, N.R.; Wild, C.Y.; Williams, S.A.; Ng, L. Effect of External Ankle Support on Ankle and Knee Biomechanics During the Cutting Maneuver in Basketball Players. Am. J. Sports Med. 2017, 45, 685–691. [Google Scholar] [CrossRef] [PubMed]
- Vieira, T.M.M.; Minetto, M.A.; Hodson-tole, E.F.; Botter, A. Human Movement Science How much does the human medial gastrocnemius muscle contribute to ankle torques outside the sagittal plane? Hum. Mov. Sci. 2013, 32, 753–767. [Google Scholar] [CrossRef] [PubMed]
- Sikora, M.; Paszkiel, S. Muscle activity measurement using visible light and infrared. IFAC Pap. 2019, 52, 329–334. [Google Scholar] [CrossRef]
- Massó, N.; Rey, F.; Romero, D.; Gual, G.; Costa, L.; Germán, A. Surface electromyography applications in the sport. Apunts Med. Esport 2010, 45, 127–136. [Google Scholar] [CrossRef]
- Henry, S.M.; Fung, J.; Horak, F.B. EMG responses to maintain stance during multidirectional surface translations. J. Neurophysiol. 1998, 80, 1939–1950. [Google Scholar] [CrossRef]
- Sanderson, D.J.; Martin, P.E.; Honeyman, G.; Keefer, J. Gastrocnemius and soleus muscle length, velocity, and EMG responses to changes in pedalling cadence. J. Electromyogr. Kinesiol. 2006, 16, 642–649. [Google Scholar] [CrossRef]
- Pakosz, P.; Konieczny, B.E.M. Time Analysis of Muscle Activation during Basketball Free Throws. Cent. Eur. J. Sport Sci. Med. 2016, 15, 73–79. [Google Scholar] [CrossRef][Green Version]
- Pakosz, P. EMG signal analysis of selected muscles during shots and passes in basketball. J. Health Promot. Recreat. 2011, 1, 9–14. [Google Scholar]
- Zachry, T.; Wulf, G.; Mercer, J.; Bezodis, N. Increased movement accuracy and reduced EMG activity as the result of adopting an external focus of attention. Brain Res. Bull. 2005, 30, 304–309. [Google Scholar] [CrossRef]
- Abe, S.; Nozawa, T.; Kondo, T. A Proposal of EMG-Based Training Support System for Basketball Dribbling. In Human Interface and the Management of Information. Designing Information Environments. Human Interface; Smith, M.J., Salvendy, G., Eds.; Lecture Notes in Computer Science; Springer: Berlin/Heidelberg, Germany, 2009; Volume 5617. [Google Scholar] [CrossRef]
- Hanks, M.; Oliver, G. Muscle Activation Patterns in Wheelchair Basketball Athletes with and without Physical Disability. Int. J. Physiatry 2018, 4, 013. [Google Scholar] [CrossRef][Green Version]
- Uzun, S.; Pourmoghaddam, A.; Hieronymus, M.; Thrasher, T.A. Evaluation of muscle fatigue of wheelchair basketball players with spinal cord injury using recurrence quantification analysis of surface EMG. Eur. J. Appl. Physiol. 2012, 112, 3847–3857. [Google Scholar] [CrossRef] [PubMed]
- Roman-Liu, D.; Bartuzi, P. Influence of type of MVC test on electromyography measures of biceps brachii and triceps brachii. Int. J. Occup. Saf. Ergon. 2018, 24, 200–206. [Google Scholar] [CrossRef] [PubMed]
- Mok, N.W.; Yeung, E.W.; Cho, J.C.; Hui, S.C.; Liu, K.C.; Pang, C.H. Core muscle activity during suspension exercises. J. Sci. Med. Sport 2015, 18, 189–194. [Google Scholar] [CrossRef]
- Hermens, H.J.; Freriks, B.; Merletti, R.; Stegeman, D.; Blok, J.; Rau, G.; Disselhorst-Klug, C.; Hägg, G. European Recommendations for Surface ElectroMyoGraphy. Roessingh Res. Dev. 1999, 8, 13–54. [Google Scholar]
- Arendt-Nielsen, L.; Graven-Nielsen, T.; Svarrer, H.; Svensson, P. The influence of low back pain on muscle activity and coordination during gait: A clinical and experimental study. Pain 1996, 64, 231–240. [Google Scholar] [CrossRef]
- van Hedel, H.; Tomatis, L.; Muller, R. Modulation of leg muscle activity and gait kinematics by walking speed and bodyweight unloading. Gait Posture 2006, 24, 35–45. [Google Scholar] [CrossRef]
- Ghasemi, A.; Zahediasl, S. Normality tests for statistical analysis: A guide for non-statisticians. Int. J. Endocrinol. Metab. 2012, 10, 486–489. [Google Scholar] [CrossRef]
- Guerino, M.; Vicente, R.C.; Cesário, M.D.; Guirro, R. Cold-water immersion alters muscle recruitment and balance of basketball players during vertical jump landing. J. Sports Sci. 2015, 34, 1–10. [Google Scholar] [CrossRef]
- Cibulka, M.T.; Wenthe, A.; Boyle, Z.; Callier, D.; Schwerdt, A.; Jarman, D.; Strube, M.J. Variation in medial and lateral gastrocnemius muscle activity with foot position. Int. J. Sports Phys. Ther. 2017, 12, 233–241. [Google Scholar]
- Hewit, J.; Cronin, J.; Button, C.; Hume, P. Understanding Deceleration in Sport. Strength Cond. J. 2011, 33, 47–52. [Google Scholar] [CrossRef]
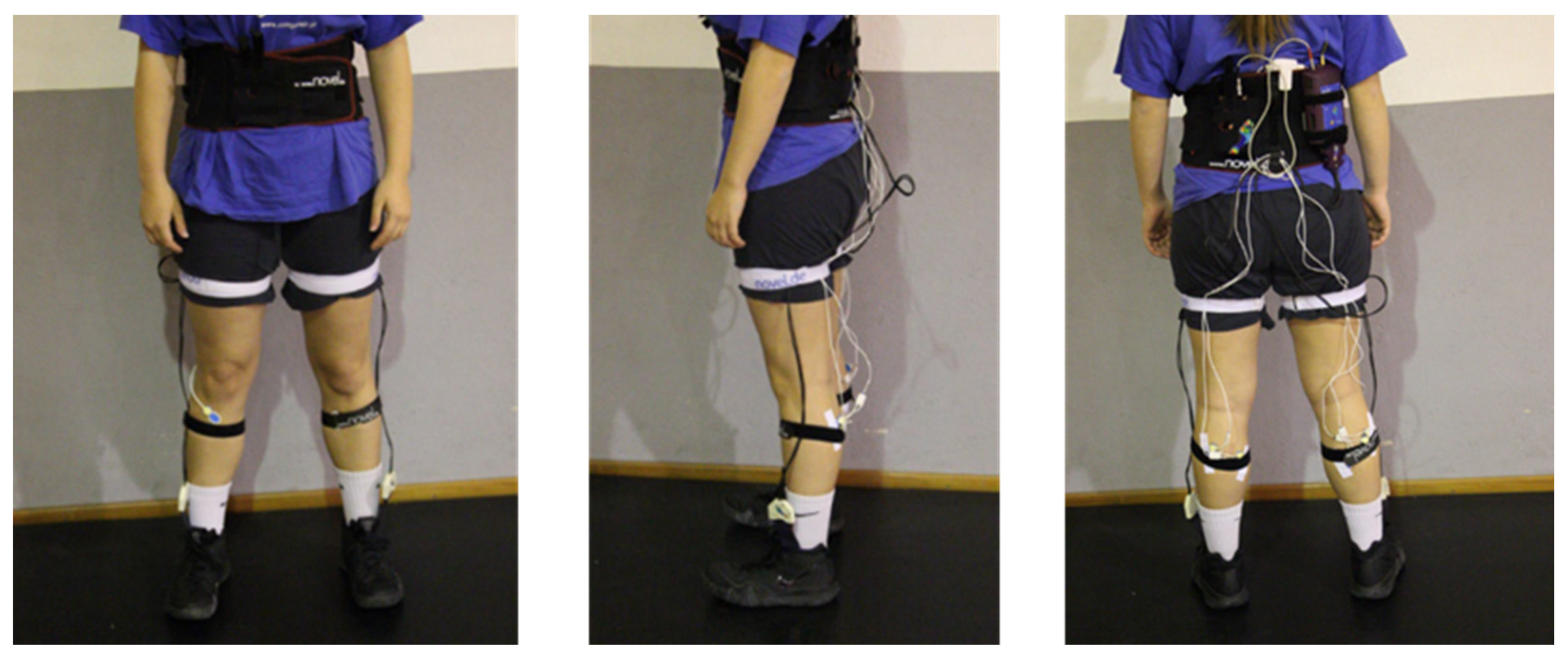
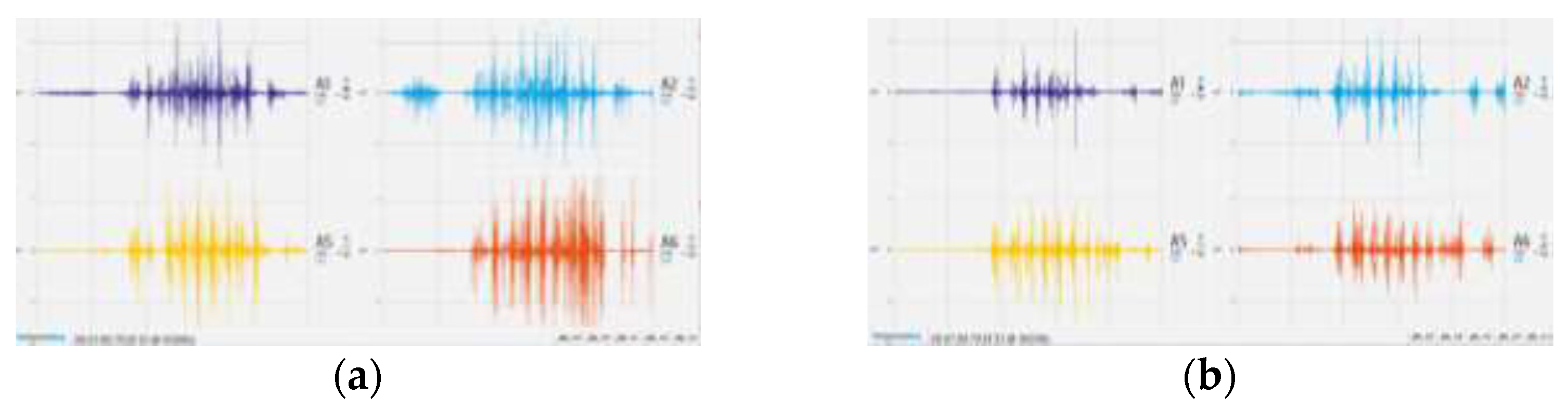
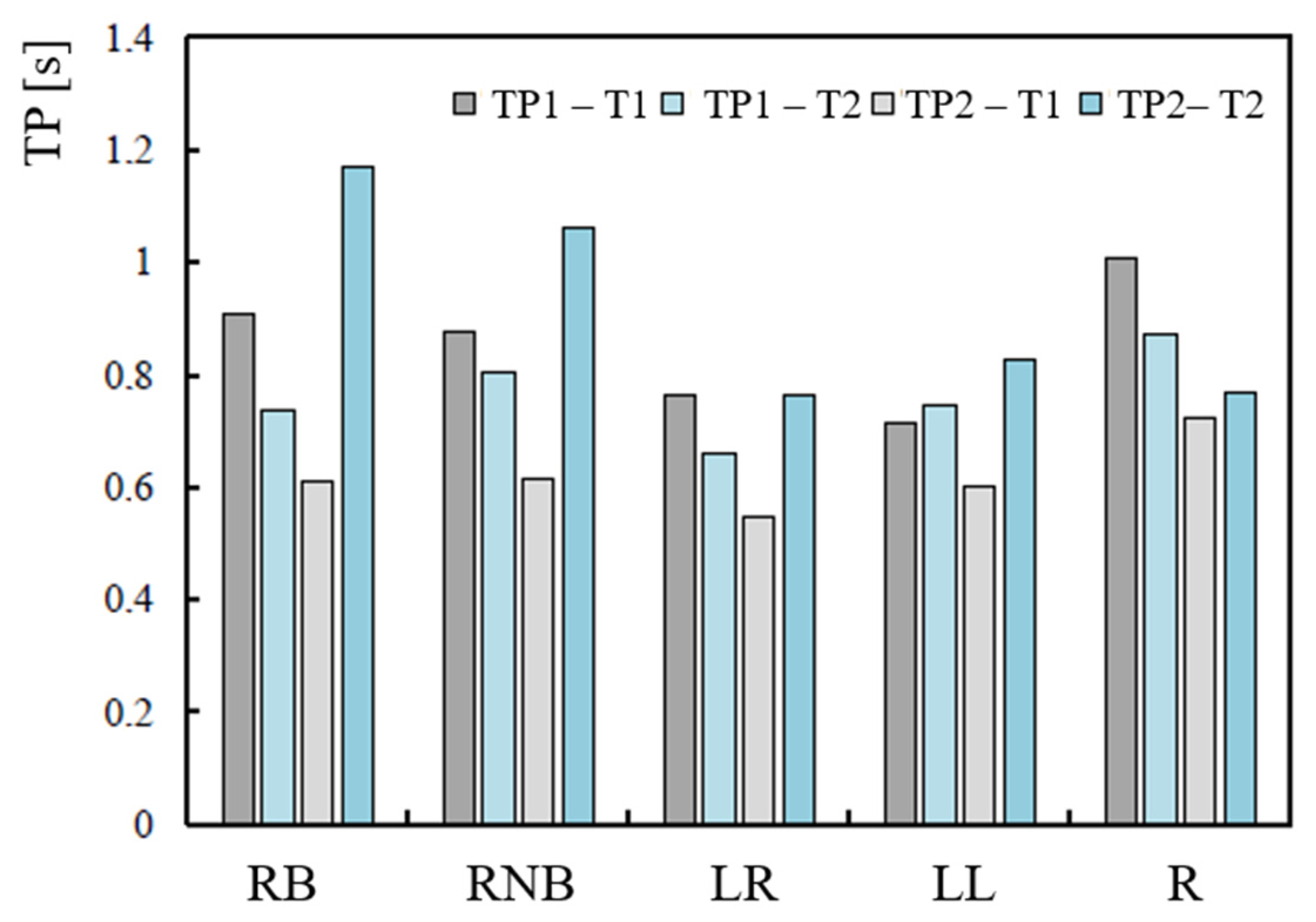
| Athletes | Age (Years) | Height (m) | Mass (kg) | BMI (kg/m2) | Dominant Hand | Years of Practice | Level of Experience |
|---|---|---|---|---|---|---|---|
| 1 | 19 | 1.79 | 73.05 | 22.8 | Right | 7 | 2 |
| 2 | 19 | 1.66 | 66.96 | 24.3 | Right | 12 | 1 |
| 3 | 19 | 1.71 | 54.97 | 18.8 | Right | 11 | 1 |
| 4 | 22 | 1.64 | 70.47 | 26.2 | Left | 17 | 1 |
| 5 | 23 | 1.69 | 72.26 | 25.3 | Right | 17 | 1 |
| 6 | 21 | 1.58 | 69.90 | 28 | Right | 7 | 2 |
| 7 | 18 | 1.62 | 51.96 | 19.8 | Right | 11 | 2 |
| 8 | 19 | 1.60 | 61.44 | 24 | Right | 6 | 2 |
| 9 | 19 | 1.66 | 52.91 | 19.2 | Left | 11 | 1 |
| Mean ± SD | 19.9 ± 1.7 | 1.66 ± 0.06 | 66.96 ± 8.60 | 23.2 ± 3.3 | - | 11.0 ± 4 | - |
| Mov. | Musc. | TP (s) | % MC | ||||
|---|---|---|---|---|---|---|---|
| T1 ± SD | T2 ± SD | p | T1 ± SD | T2 ± SD | p | ||
| RB | LGL | 0.84 ± 0.42 | 0.92 ± 0.72 | 0.953 | 83 ± 15 | 87 ± 7 | 0.441 |
| MGL | 0.71 ± 0.40 | 0.91 ± 0.71 | 0.374 | 85 ± 12 | 80 ± 22 | 0.401 | |
| LGR | 0.67 ± 0.30 | 0.88 ± 0.56 | 0.173 | 103 ± 56 | 87 ± 11 | 0.051 | |
| MGR | 0.89 ± 0.65 | 1.00 ± 0.63 | 0.594 | 78 ± 18 | 88 ± 10 | 0.214 | |
| P | 0.269 | 0.586 | 0.615 | 0.512 | |||
| RNB | LGL | 0.81 ± 0.28 | 0.96 ± 0.60 | 0.594 | 80 ± 18 | 86 ± 9 | 0.374 |
| MGL | 0.77 ± 0.23 | 0.88 ± 0.55 | 0.767 | 82 ± 11 | 88 ± 11 | 0.025 | |
| LGR | 0.67 ± 0.20 | 0.95 ± 0.50 | 0.110 | 77 ± 18 | 86 ± 10 | 0.025 | |
| MGR | 0.79 ± 0.29 | 0.88 ± 0.55 | 0.859 | 78 ± 14 | 88 ± 9 | 0.173 | |
| p | 0.506 | 0.145 | 0.865 | 0.698 | |||
| LR | LGL | 0.66 ± 0.17 | 0.73 ± 0.37 | 0.678 | 73 ± 22 | 84 ± 7 | 0.441 |
| MGL | 0.64 ± 0.17 | 0.70 ± 0.36 | 0.515 | 82 ± 9 | 88 ± 9 | 0.123 | |
| LGR | 0.62 ± 0.08 | 0.69 ± 0.18 | 0.407 | 77 ± 13 | 84 ± 5 | 0.038 | |
| MGR | 0.76 ± 0.25 | 0.80 ± 0.19 | 0.515 | 71 ± 16 | 80 ± 19 | 0.173 | |
| p | 0.053 | 0.129 | 0.137 | 0.887 | |||
| LL | LGL | 0.78 ± 0.29 | 0.75 ± 0.30 | 0.678 | 80 ± 11 | 84 ± 8 | 0.678 |
| MGL | 0.76 ± 0.24 | 0.83 ± 0.21 | 0.767 | 84 ± 9 | 85 ± 10 | 0.953 | |
| LGR | 0.66 ± 0.23 | 0.74 ± 0.22 | 0.260 | 84 ± 8 | 87 ± 5 | 0.214 | |
| MGR | 0.67 ± 0.17 | 0.81 ± 0.35 | 0.441 | 85 ± 8 | 88 ± 10 | 0.767 | |
| p | 0.068 | 0.706 | 0.959 | 0.823 | |||
| R | LGL | 0.80 ± 0.95 | 0.71 ± 0.17 | 0.314 | 81 ± 11 | 73 ± 11 | 0.26 |
| MGL | 0.91 ± 0.45 | 0.91 ± 0.36 | 0.953 | 86 ± 7 | 86 ± 08 | 0.06 | |
| LGR | 0.86 ± 0.35 | 0.84 ± 0.25 | 0.594 | 80 ± 15 | 82 ± 10 | 0.594 | |
| MGR | 0.94 ± 0.32 | 0.84 ± 0.17 | 0.953 | 81 ± 17 | 78 ± 27 | 0.594 | |
| p | 0.269 | 0.392 | 0.644 | 0.512 | |||
| Mov. | Musc. | T1 | T2 | ||||
|---|---|---|---|---|---|---|---|
| Level 1 ± SD | Level 2 ± SD | P | Level 1 ± SD | Level2 ± SD | p | ||
| RB | LGL | 0.997 ± 0.54 | 0.657 ± 0.07 | 0.465 | 0.683 ± 0.2 | 1.218 ± 1.06 | 0.465 |
| MGL | 0.855 ± 0.50 | 0.519 ± 0.06 | 0.273 | 0.737 ± 0.25 | 1.131 ± 1.06 | 0.715 | |
| LGR | 0.685 ± 0.31 | 0.645 ± 0.34 | 0.715 | 0.669 ± 0.21 | 1.134 ± 0.79 | 0.068 | |
| MGR | 1.096 ± 0.82 | 0.627 ± 0.22 | 0.068 | 0.861 ± 0.29 | 1.183 ± 0.93 | 0.715 | |
| RNB | LGL | 0.851 ± 0.36 | 0.75 ± 0.18 | 0.273 | 0.848 ± 0.33 | 1.099 ± 0.87 | 0.715 |
| MGL | 0.894 ± 0.15 | 0.621 ± 0.24 | 0.068 | 0.797 ± 0.3 | 0.975 ± 0.81 | 0.715 | |
| LGR | 0.78 ± 0.2 | 0.55 ± 0.13 | 0.144 | 0.881 ± 0.18 | 1.039 ± 0.78 | 0.06 | |
| MGR | 0.985 ± 0.24 | 0.547 ± 0.09 | 0.068 | 0.693 ± 0.15 | 1.114 ± 0.8 | 0.715 | |
| LR | LGL | 0.746 ± 0.18 | 0.55 ± 0.08 | 0.068 | 0.636 ± 0.04 | 0.837 ± 0.58 | 0.715 |
| MGL | 0.745 ± 0.16 | 0.501 ± 0.05 | 0.068 | 0.634 ± 0.09 | 0.781 ± 0.57 | 0.715 | |
| LGR | 0.671 ± 0.06 | 0.547 ± 0.05 | 0.068 | 0.652 ± 0.13 | 0.727 ± 0.24 | 0.715 | |
| MGR | 0.89 ± 0.26 | 0.587 ± 0.05 | 0.068 | 0.721 ± 0.12 | 0.713 ± 0.25 | 0.715 | |
| LL | LGL | 0.897 ± 0.36 | 0.643 ± 0.05 | 0.465 | 0.673 ± 0.06 | 0.838 ± 0.47 | 0.715 |
| MGL | 0.864 ± 0.28 | 0.634 ± 0.11 | 0.273 | 0.795 ± 0.13 | 0.863 ± 0.31 | 0.715 | |
| LGR | 0.773 ± 0.27 | 0.521 ± 0.05 | 0.273 | 0.766 ± 0.27 | 0.713 ± 0.19 | 0.273 | |
| MGR | 0.724 ± 0.18 | 0.598 ± 0.16 | 0.465 | 0.743 ± 0.31 | 0.885 ± 0.42 | 0.715 | |
| R | LGL | 0.922 ± 0.4 | 0.652 ± 0.22 | 0.715 | 0.793 ± 0.17 | 0.61 ± 0.14 | 0.068 |
| MGL | 1.093 ± 0.55 | 0.69 ± 0.1 | 0.465 | 1.025 ± 0.46 | 0.761 ± 0.11 | 0.715 | |
| LGR | 0.989 ± 0.43 | 0.706 ± 0.14 | 0.465 | 0.876 ± 0.34 | 0.796 ± 0.09 | 0.465 | |
| MGR | 1.021 ± 0.42 | 0.846 ± 0.105 | 0.715 | 0.795 ± 0.22 | 0.902 ± 0.07 | 0.465 | |
| Musc | T1 | T2 | ||
|---|---|---|---|---|
| TP | % MC | TP | % MC | |
| P | p | p | P | |
| LGL | 0.795 | 0.554 | 0.165 | 0.132 |
| MGL | 0.029 * | 0.575 | 0.004 * | 0.541 |
| LGR | 0.071 | 0.029 * | 0.281 | 0.664 |
| MGR | 0.247 | 0.144 | 0.394 | 0.897 |
| Mov. | RNB | LR | LL | R | ||||||
|---|---|---|---|---|---|---|---|---|---|---|
| P | MA | % MC | MA | % MC | MA | % MC | MA | % MC | ||
| T1 | RB | MGL | >0.05 | >0.05 | >0.05 | 0.073 | ||||
| LGR | >0.05 | 0.046 * | >0.05 | 0.171 | ||||||
| RNB | MGL | >0.05 | >0.05 | >0.05 | ||||||
| LGR | >0.05 | >0.05 | >0.05 | |||||||
| LR | MGL | >0.05 | 0.046 * | |||||||
| LGR | 0.369 | >0.05 | ||||||||
| LL | MGL | >0.05 | ||||||||
| LGR | >0.05 | |||||||||
| T2 | RB | MGL | >0.05 | 0.526 | >0.05 | 0.736 | ||||
| RNB | MGL | 0.526 | >0.05 | 0.736 | ||||||
| LR | MGL | 0.046 * | 0.002 * | |||||||
| LL | MGL | >0.05 | ||||||||
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2021 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Amaro, C.M.; Castro, M.A.; Roseiro, L.; Mendes, R.; Amaro, A.M. Gastrocnemius Activation throughout the Competitive Season in Athletes of Different Experience Levels. Appl. Sci. 2021, 11, 984. https://doi.org/10.3390/app11030984
Amaro CM, Castro MA, Roseiro L, Mendes R, Amaro AM. Gastrocnemius Activation throughout the Competitive Season in Athletes of Different Experience Levels. Applied Sciences. 2021; 11(3):984. https://doi.org/10.3390/app11030984
Chicago/Turabian StyleAmaro, Catarina M., Maria António Castro, Luis Roseiro, Rui Mendes, and Ana M. Amaro. 2021. "Gastrocnemius Activation throughout the Competitive Season in Athletes of Different Experience Levels" Applied Sciences 11, no. 3: 984. https://doi.org/10.3390/app11030984
APA StyleAmaro, C. M., Castro, M. A., Roseiro, L., Mendes, R., & Amaro, A. M. (2021). Gastrocnemius Activation throughout the Competitive Season in Athletes of Different Experience Levels. Applied Sciences, 11(3), 984. https://doi.org/10.3390/app11030984









