Workers with Active Implantable Medical Devices Exposed to EMF: In Vitro Test for the Risk Assessment
Abstract
1. Introduction
1.1. The Regulatory Framework for Workers with AIMD
1.2. General Procedure for the Risk Assessment Required for an AIMD Employee
2. Materials and Methods
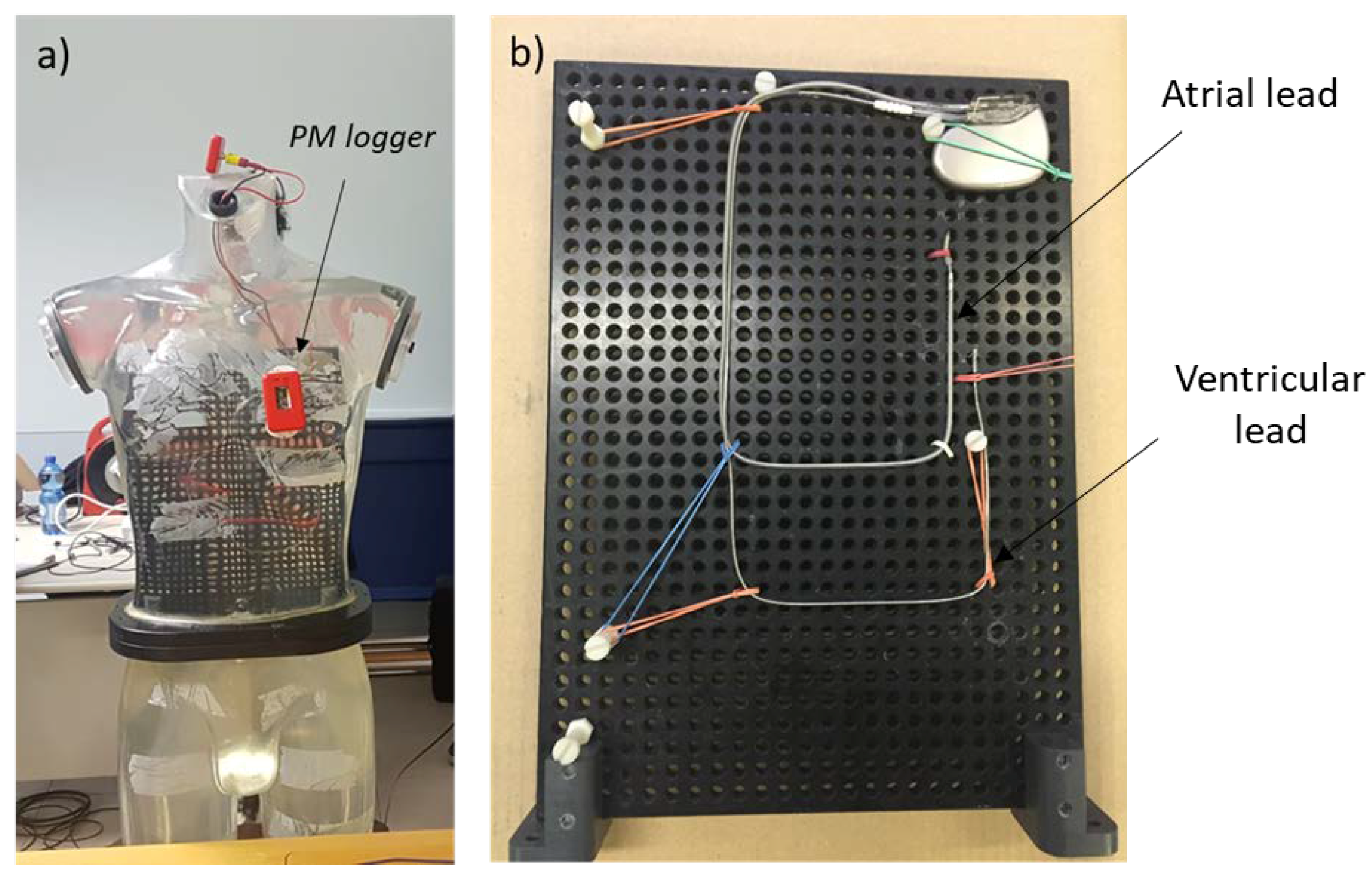
2.1. The Human Torso-Shaped Phantom
2.2. The PM Activity Logger
2.3. The Electrosurgical Unit
- Leaving the ESU electrode open, not connected to any load (worst-case condition in terms of electric field);
- Using a load of 50 Ohm at 250 W to maximize the current delivered (worst-case condition in terms of magnetic field);
- Using a load of 400 Ohm at 400 W to simulate a more realistic scenario.
2.4. The Transcranial Stimulator
- The stimulation of the parietal area, with the coil perpendicular to the trunk of the human torso-shaped phantom;
- The stimulation of the occipital area, with the coil parallel to the trunk of the human torso-shaped phantom.
2.5. The Arc Welder
- The cable raised from the floor next to the human torso-shaped phantom till reaching the worktable;
- The cable was fixed around the belt of the phantom;
- The cable was placed over both shoulders of the phantom;
- The cable was placed over one shoulder of the phantom.
3. Results
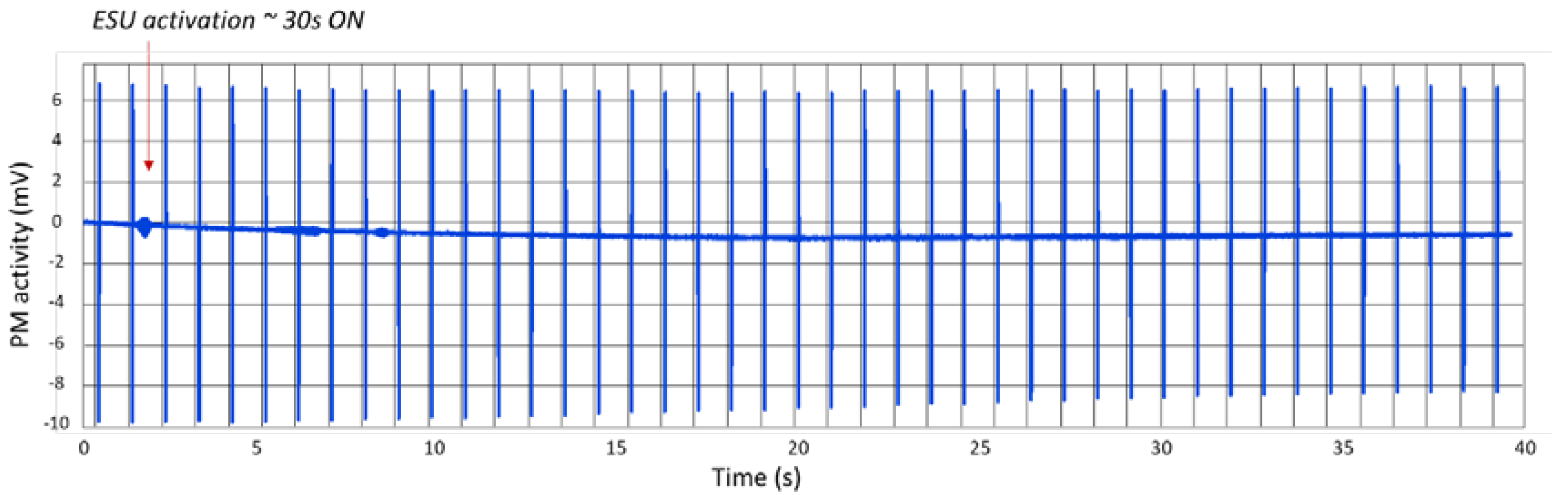
3.1. The Electrosurgical Unit
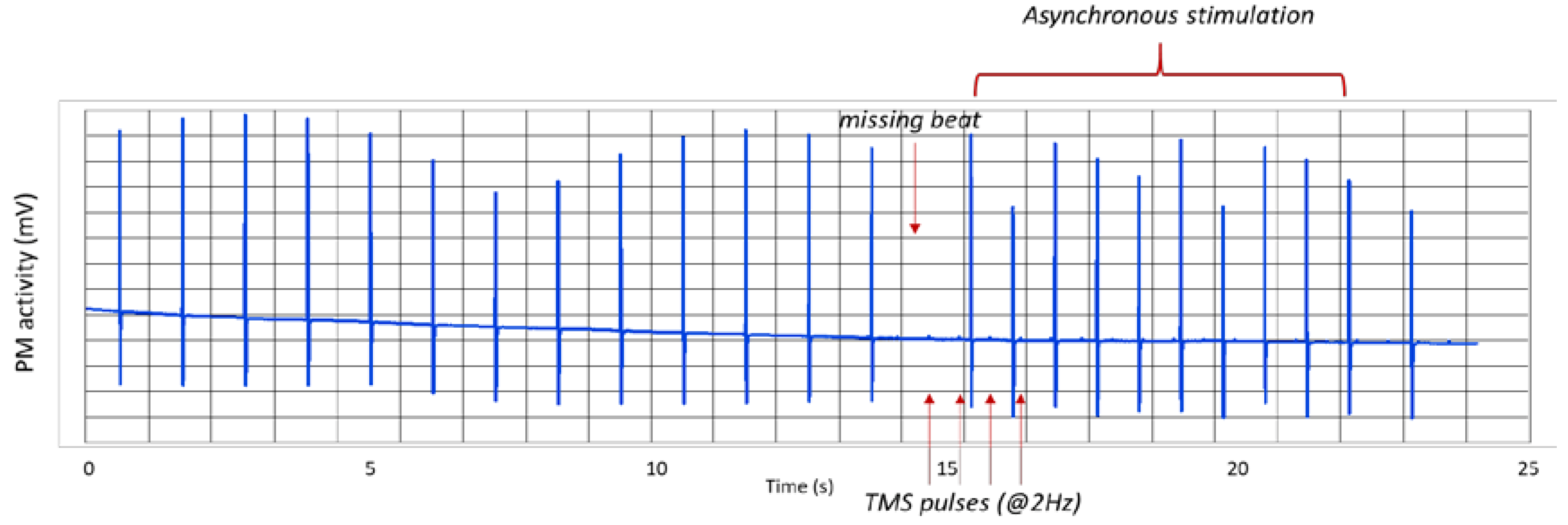
3.2. The Transcranial Stimulator
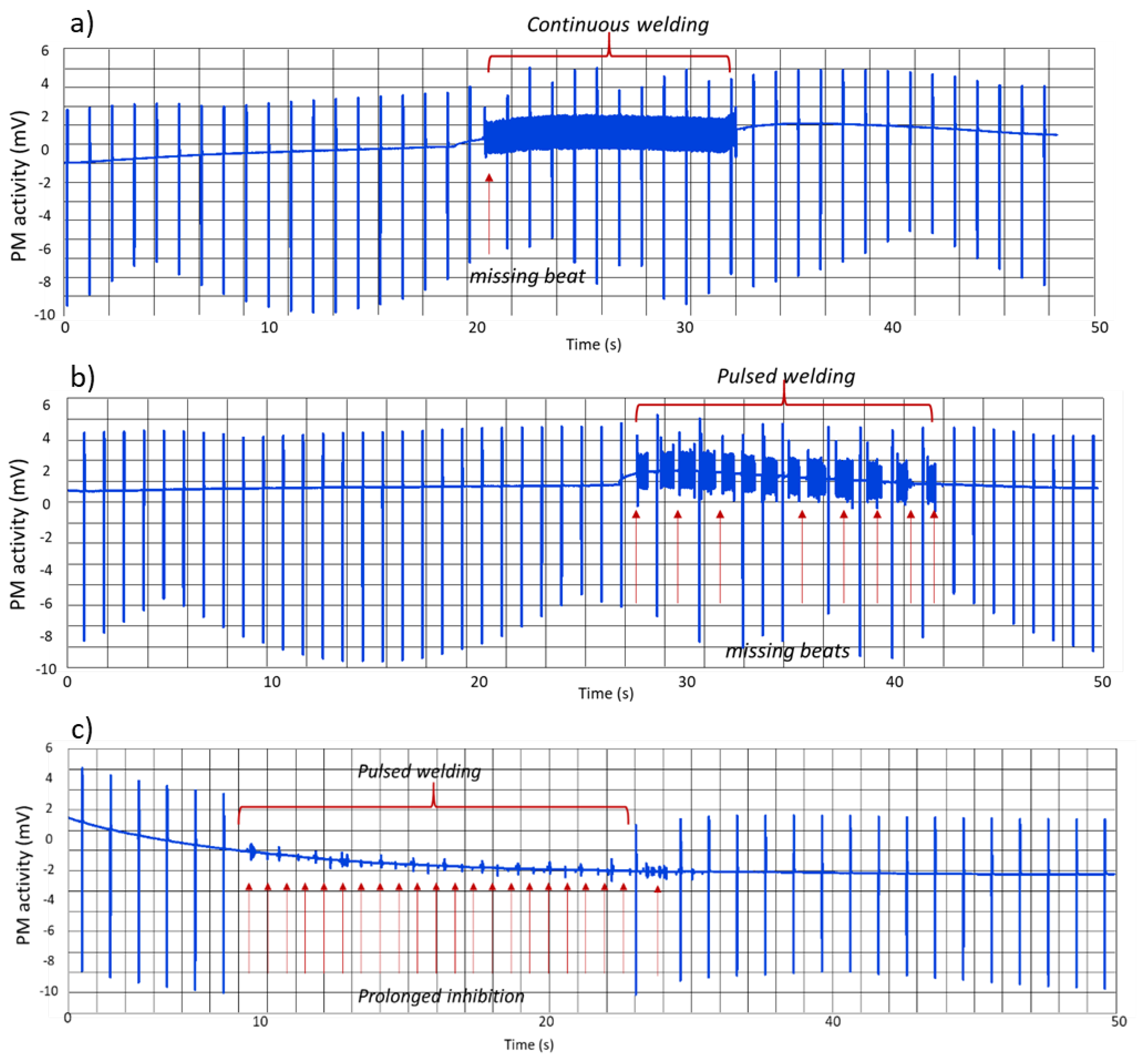
3.3. The Arc Welder
4. Discussion
- The workplace environment is such that a phantom, a monitoring device, and test personnel can be accommodated for the duration of anticipated testing;
- A fully functional pacemaker and leads of the same manufacturer and model as that implanted in the PM employee can be obtained from the manufacturer or the physician;
- A monitoring device to record and analyze the activity of the PM during the test is available.
5. Conclusions
Author Contributions
Funding
Conflicts of Interest
References
- Directive 2013/35/EU of the European Parliament and of the Council of 26 June 2013 on the Minimum Health and Safety Requirements regarding the Exposure of Workers to the Risks Arising from Physical Agents (Electromagnetic Fields) (20th Individual Directive within the Meaning of Article 16(1) of Directive 89/391/EEC) and repealing Directive 2004/40/EC. Available online: https://eur-lex.europa.eu/legal-content/EN/TXT/?uri=celex%3A32013L0035 (accessed on 14 November 2019).
- Directorate-General for Employment, Social Affairs and Inclusion (European Commission), Non-binding Guide to Good Practice for Implementing Directive 2013/35/EU Electromagnetic Fields; EU Publications: Luxembourg, 2014; Available online: https://www.portaleagentifisici.it/fo_campi_elettromagnetici_documentazione.php?lg=IT (accessed on 14 November 2019).
- EN 50527-1:2016, Procedure for the Assessment of the Exposure to Electromagnetic Fields of Workers Bearing Active Implantable Medical Devices—Part 1: General; European Committee for Electrotechnical Standardization: Brussels, Belgium, 2016.
- EN 50527-2-1:2016, Procedure for the Assessment of the Exposure to Electromagnetic Fields of Workers Bearing Active Implantable Medical Devices—Part 2-1: Specific Assessment for Workers with Cardiac Pacemakers; European Committee for Electrotechnical Standardization: Bruxelles, Belgium, 2016.
- EN 50527-2-2:2018, Procedure for the Assessment of the Exposure to Electromagnetic Fields of Workers Bearing Active Implantable Medical Devices—Part 2-2: Specific Assessment for Workers with Cardioverter Defibrillators (ICDs); European Committee for Electrotechnical Standardization: Brussels, Belgium, 2018.
- Regulation (EU) 2017/745 of the European Parliament and of the Council of 5 April 2017 on Medical Devices, Amending Directive 2001/83/EC, Regulation (EC) No 178/2002 and Regulation (EC) No 1223/2009 and Repealing Council Directives 90/385/EEC and 93/42/EEC. Available online: https://eur-lex.europa.eu/legal-content/EN/TXT/?uri=CELEX%3A32017R0745 (accessed on 14 November 2019).
- Calcagnini, G.; Censi, F.; Bartolini, P. Electromagnetic immunity of medical devices: the European regulatory framework. Ann. Ist. Super. Sanita 2007, 43, 268–276. [Google Scholar] [PubMed]
- EN 45502-1:2015, Implants for Surgery. Active Implantable Medical Devices. General Requirements for Safety, Marking and for Information to be Provided by the Manufacturer; European Committee for Electrotechnical Standardization: Brussels, Belgium, 2015.
- EN 45502-2-1:2005-Active Implantable Medical Devices—Part 2-1: Particular Requirements for Active Implantable Medical Devices Intended to Treat Bradyarrhythmia (Cardiac Pacemakers); European Committee for Electrotechnical Standardization: Brussels, Belgium, 2005.
- EN 45502-2-2:2008-Active Implantable Medical Devices. Particular Requirements for Active Implantable Medical Devices Intended to Treat Tachyarrhythmia (Includes Implantable Defibrillators); European Committee for Electrotechnical Standardization: Brussels, Belgium, 2008.
- 1999/519/EC: Council Recommendation of 12 July 1999 on the limitation of exposure of the general public to electromagnetic fields (0 Hz to 300 GHz). Off. J. Eur. Commun. 1999, 199, 59–70.
- International Commission on Non-Ionizing Radiation Protection (ICNIRP), Guidelines for limiting exposure to time-varying electric, magnetic and electromagnetic fields (up to 300 GHz). Health Phys. 1998, 99, 818–836.
- Andreuccetti, D.; Fossi, R.; Petrucci, C. An Internet Resource for the Calculation of the Dielectric Properties of Body Tissues in the Frequency Range 10 Hz–100 GHz; IFAC-CNR: Florence, Italy, 2007; Available online: http://niremf.ifac.cnr.it/tissprop/ (accessed on 14 November 2019).
- Richter, L.; Trillenberg, P.; Schweikard, A.; Schlaefer, A. Stimulus intensity for hand held and robotic transcranial magnetic stimulation. Brain Stimul. 2013, 6, 315–321. [Google Scholar] [CrossRef] [PubMed]
- Angeloni, A.; Barbaro, V.; Bartolini, P.; Calcagnini, G.; Censi, F. A novel heart/trunk simulator for the study of electromagnetic interference with active implantable devices. Med. Biol. Eng. Comput. 2003, 41, 550–555. [Google Scholar] [CrossRef] [PubMed]
- Mattei, E.; Censi, F.; Triventi, M.; Calcagnini, G. Electromagnetic immunity of implantable pacemakers exposed to wi-fi devices. Health Phys. 2014, 107, 318–325. [Google Scholar] [CrossRef] [PubMed]
- Seidman, S.J.; Brockman, R.; Lewis, B.M.; Guag, J.; Shein, M.J.; Clement, W.J.; Kippola, J.; Digby, D.; Barber, C.; Huntwork, D. In vitro tests reveal sample radiofrequency identification readers inducing clinically significant electromagnetic interference to implantable pacemakers and implantable cardioverter-defibrillators. Heart Rhythm 2010, 7, 99–107. [Google Scholar] [CrossRef] [PubMed]
- Calcagnini, G.; Triventi, M.; Censi, F.; Mattei, E.; Bartolini, P.; Kainz, W.; Bassen, H.I. In vitro investigation of pacemaker lead heating induced by magnetic resonance imaging: role of implant geometry. Off. J. Int. Soc. Magn. Reson. Med. 2008, 28, 879–886. [Google Scholar] [CrossRef] [PubMed]
- Mattei, E.; Lucano, E.; Censi, F.; Triventi, M.; Calcagnini, G. Provocative Testing for the Assessment of the Electromagnetic Interference of RFID and NFC Readers on Implantable Pacemaker. IEEE Trans. Electr. Compat. 2015, 58, 314–322. [Google Scholar] [CrossRef]
- Korpinen, L.; Kuisti, H.; Elovaara, J.; Virtanen, V. Cardiac pacemakers in electric and magnetic fields of 400-kV power lines. Pacing Clin. Electrophysiol. 2012, 35, 422–430. [Google Scholar] [CrossRef] [PubMed]
- Lin, Y.; Melby, D.P.; Krishnan, B.; Adabag, S.; Tholakanahalli, V.; Li, J.M. Frequency of pacemaker malfunction associated with monopolar electrosurgery during pulse generator replacement or upgrade surgery. J. Int. Card. Electrophysiol. 2017, 49, 205–209. [Google Scholar] [CrossRef] [PubMed]
- Roncero, C.; Mardigyan, V.; Service, E.; Singerman, J.; Whittaker, K.C.; Friedman, M.; Chertkow, H. Investigation into the effect of transcranial direct current stimulation on cardiac pacemakers. Brain Stimul. 2019. [Google Scholar] [CrossRef] [PubMed]
- Hayes, D.L.; Wang, P.J.; Reynolds, D.W.; Estes, N.M.; Griffith, J.L.; Steffens, R.A.; Carlo, G.L.; Findlay, G.K.; Johnson, C.M. Interference with cardiac pacemakers by cellular telephones. N. Engl. J. Med. 1997, 336, 1473–1479. [Google Scholar] [CrossRef] [PubMed]
- Brignole, M.; Guieu, R.; Tomaino, M.; Iori, M.; Ungar, A.; Bertolone, C.; Unterhuber, M.; Bottoni, N.; Tesi, F.; Deharo, J.C. Mechanism of syncope without prodromes with normal heart and normal electrocardiogram. Heart Rhythm 2017, 14, 234–239. [Google Scholar] [CrossRef] [PubMed]
- Tiikkaja, M.; Aro, A.L.; Alanko, T.; Lindholm, H.; Sistonen, H.; Hartikainen, J.E.; Toivonen, L.; Juutilainen, J.; Hietanen, M. Testing of common electromagnetic environments for risk of interference with cardiac pacemaker function. Saf. Health Work 2013, 4, 156–159. [Google Scholar] [CrossRef] [PubMed]
- Hikage, T.; Nojima, T.; Fujimoto, H. Active implantable medical device EMI assessment for wireless power transfer operating in LF and HF bands. Phys. Med. Biol. 2016, 61, 4522–4536. [Google Scholar] [CrossRef] [PubMed]



| Designation of Workplace | Examples of Equipment | Exceptions and Remarks |
|---|---|---|
| Medical workplaces | All medical equipment not using RF sources | If medical workplaces include static or time varying magnetic or electric fields, then operational precautions may be necessary. For equipment used at medical workplaces listed elsewhere in this table look at the appropriate sub(clause). |
| Workplaces open to the general public (as covered by Article 4.3 of EMF Directive 2004/40/EC) | Places open to the public and in compliance with the exposure limits given in Council Recommendation 1999/519/EC are deemed to comply without further assessment provided that the compliance was assessed against the reference levels. | It is possible, under certain circumstances, to exceed the reference levels and still comply with the basic restrictions of Council Recommendation 1999/519/EC. Such circumstances are usually in localised areas, close to EMF emitting equipment, so transient exposure in those areas may be permitted. In case of doubt, further guidance may be obtained from device or emitter manufacturers, medical advisors or by the use of the appropriate device specific standard. An example for such equipment could be audio frequency induction-loop systems (AFILS following EN 60118-4) for assisted hearing where the system has been assessed against the reference levels. |
© 2019 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Mattei, E.; Calcagnini, G.; Censi, F.; Pinto, I.; Bogi, A.; Falsaperla, R. Workers with Active Implantable Medical Devices Exposed to EMF: In Vitro Test for the Risk Assessment. Environments 2019, 6, 119. https://doi.org/10.3390/environments6110119
Mattei E, Calcagnini G, Censi F, Pinto I, Bogi A, Falsaperla R. Workers with Active Implantable Medical Devices Exposed to EMF: In Vitro Test for the Risk Assessment. Environments. 2019; 6(11):119. https://doi.org/10.3390/environments6110119
Chicago/Turabian StyleMattei, Eugenio, Giovanni Calcagnini, Federica Censi, Iole Pinto, Andrea Bogi, and Rosaria Falsaperla. 2019. "Workers with Active Implantable Medical Devices Exposed to EMF: In Vitro Test for the Risk Assessment" Environments 6, no. 11: 119. https://doi.org/10.3390/environments6110119
APA StyleMattei, E., Calcagnini, G., Censi, F., Pinto, I., Bogi, A., & Falsaperla, R. (2019). Workers with Active Implantable Medical Devices Exposed to EMF: In Vitro Test for the Risk Assessment. Environments, 6(11), 119. https://doi.org/10.3390/environments6110119






