Factors Associated with Sleep Problems in Children with ADHD: Focusing on Emotional Regulation, Emotional Intensity and Internalizing Symptoms
Abstract
1. Introduction
2. Materials and Methods
2.1. Participants
2.2. Procedure
2.3. Instruments
2.3.1. Sociodemographic Data Form
2.3.2. Kiddie Schedule for Affective Disorders and Schizophrenia (K-SADS-PL)
2.3.3. Children’s Sleep Habits Questionnaire (CSHQ)
2.3.4. Conners’ Parent Rating Scale-Revised: Short Form (CPRS-R-S)
2.3.5. Emotion Regulation Scale for Children-Adult Form (ERSC-A)
2.3.6. Revised Child Anxiety and Depression Scale-Parent Form: (RCADS-P)
2.4. Data Analysis
3. Results
4. Discussion
5. Conclusions
Supplementary Materials
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Acknowledgments
Conflicts of Interest
Abbreviations
| ADHD | Attention Deficit Hyperactivity Disorder |
| CPRS | Conners’ Parent Rating Scale-Revised: Short Form |
| CSHQ | Children’s Sleep Habits Questionnaire |
| DSM-5 | The Diagnostic and Statistical Manual of Mental Disorders-Fifth Edition |
| ED | Emotional Dysregulation |
| EI | Emotional Intensity |
| ER | Emotional Regulation |
| ERSC-A | Emotion Regulation Scale for Children-Adult Form |
| FMR | False Discovery Rate |
| K-SADS-PL | Kiddie Schedule for Affective Disorders and Schizophrenia |
| RCADS-P | Revised Child Anxiety and Depression Scale-Parent Form |
| SPSS | Statistical Package for Social Sciences |
| VIF | Variance Influence Factor |
References
- Accardo, J. A., Marcus, C. L., Leonard, M. B., Shults, J., Meltzer, L. J., & Elia, J. (2012). Associations between psychiatric comorbidities and sleep disturbances in children with attention-deficit/hyperactivity disorder. Journal of Developmental & Behavioral Pediatrics, 33(2), 97–105. [Google Scholar] [CrossRef]
- APA. (2013). Diagnostic and statistical manual of mental disorders (5th ed.). American Psychiatric Association. [Google Scholar]
- Becker, S. P. (2020). ADHD and sleep: Recent advances and future directions. Current Opinion in Psychology, 34, 50–56. [Google Scholar] [CrossRef] [PubMed]
- Becker, S. P., Langberg, J. M., Eadeh, H., Isaacson, P. A., & Bourchtein, E. (2019). Sleep and daytime sleepiness in adolescents with and without ADHD: Differences across ratings, daily diary, and actigraphy. Journal of Child Psychology and Psychiatry, 60(9), 1021–1031. [Google Scholar] [CrossRef] [PubMed]
- Becker, S. P., Langberg, J. M., & Evans, S. W. (2015). Sleep problems predict comorbid externalizing behaviors and depression in young adolescents with attention-deficit/hyperactivity disorder. European Child & Adolescent Psychiatry, 24(8), 897–907. [Google Scholar] [CrossRef]
- Biederman, J., Petty, C. R., Day, H., Goldin, R. L., Spencer, T., Faraone, S. V., Surman, C. B. H., & Wozniak, J. (2012). Severity of the aggression/anxiety-depression/attention child behavior checklist profile discriminates between different levels of deficits in emotional regulation in youth with attention-deficit hyperactivity disorder. Journal of Developmental & Behavioral Pediatrics, 33(3), 236–243. [Google Scholar] [CrossRef]
- Bondopandhyay, U., McGrath, J., & Coogan, A. N. (2024). Associations between sleep problems in children with ADHD and parental insomnia and ADHD symptoms. PLoS ONE, 19(5), e0298377. [Google Scholar] [CrossRef]
- Bunford, N., Evans, S. W., & Langberg, J. M. (2018). Emotion dysregulation is associated with social impairment among young adolescents with ADHD. Journal of Attention Disorders, 22(1), 66–82. [Google Scholar] [CrossRef]
- Chorpita, B. F., Yim, L., Moffitt, C., Umemoto, L. A., & Francis, S. E. (2000). Assessment of symptoms of DSM-IV anxiety and depression in children: A revised child anxiety and depression scale. Behaviour Research and Therapy, 38(8), 835–855. [Google Scholar] [CrossRef]
- Conners, C. K. (1997). Conners’ rating scales-revised. Instruments for use with children Ind adolescents. MLS. [Google Scholar]
- Corkum, P., Panton, R., Ironside, S., MacPherson, M., & Williams, T. (2007). Acute impact of immediate release methylphenidate administered three times a day on sleep in children with attention-deficit/hyperactivity disorder. Journal of Pediatric Psychology, 33(4), 368–379. [Google Scholar] [CrossRef]
- Cortese, S., Faraone, S. V., Konofal, E., & Lecendreux, M. (2009). Sleep in children with attention-deficit/hyperactivity disorder: Meta-Analysis of subjective and objective studies. Journal of the American Academy of Child & Adolescent Psychiatry, 48(9), 894–908. [Google Scholar] [CrossRef]
- Costa-López, B., Lavigne-Cerván, R., Collado-Valero, J. A., Juárez-Ruiz de Mier, R., & Navarro-Soria, I. (2023). The influence of emotional regulation and cognitive flexibility on sleep habits in Spanish children and adolescents through the lens of parents. Children, 10(8), 1390. [Google Scholar] [CrossRef] [PubMed]
- Déry, M., Lapalme, M., Jagiellowicz, J., Poirier, M., Temcheff, C., & Toupin, J. (2017). Predicting depression and anxiety from oppositional defiant disorder symptoms in elementary school-age girls and boys with conduct problems. Child Psychiatry & Human Development, 48(1), 53–62. [Google Scholar] [CrossRef]
- Dimakos, J., Gauthier-Gagné, G., Lin, L., Scholes, S., & Gruber, R. (2021). The associations between sleep and externalizing and internalizing problems in children and adolescents with attention-deficit/hyperactivity disorder. Child and Adolescent Psychiatric Clinics of North America, 30(1), 175–193. [Google Scholar] [CrossRef] [PubMed]
- Dolapoglu, N., Kirkan, T. S., & Tulaci, R. G. (2025). The relationship between attention deficit hyperactivity disorder emotion regulation difficulties and sleep quality in adults: A cross sectional study. BMC Psychiatry, 25(1), 432. [Google Scholar] [CrossRef]
- Dong, H.-Y., Miao, C.-Y., Xue, Y., Zhang, Y., Shan, L., Jia, F.-Y., & Du, L. (2024). Sleep and internalizing problems in primary school children with attention-deficit hyperactivity disorder. Pediatric Research, 96(4), 1021–1029. [Google Scholar] [CrossRef]
- Dugal, C., Godbout, N., Bélanger, C., Hébert, M., & Goulet, M. (2018). Cumulative childhood maltreatment and subsequent psychological violence in intimate relationships: The role of emotion dysregulation. Partner Abuse, 9(1), 18–40. [Google Scholar] [CrossRef]
- Ercan, E. S., Polanczyk, G., Akyol Ardıc, U., Yuce, D., Karacetın, G., Tufan, A. E., Tural, U., Aksu, H., Aktepe, E., Rodopman Arman, A., Başgül, S., Bılac, O., Coşkun, M., Celık, G. G., Karakoc Demırkaya, S., Dursun, B. O., Durukan, İ., Fidan, T., Perdahlı Fiş, N., … Yıldız, N. (2019). The prevalence of childhood psychopathology in Turkey: A cross-sectional multicenter nationwide study (EPICPAT-T). Nordic Journal of Psychiatry, 73(2), 132–140. [Google Scholar] [CrossRef]
- Esbjørn, B. H., Bender, P. K., Reinholdt-Dunne, M. L., Munck, L. A., & Ollendick, T. H. (2012). The development of anxiety disorders: Considering the contributions of attachment and emotion regulation. Clinical Child and Family Psychology Review, 15(2), 129–143. [Google Scholar] [CrossRef]
- Frick, M. A., Meyer, J., & Isaksson, J. (2023). The role of comorbid symptoms in perceived stress and sleep problems in adolescent ADHD. Child Psychiatry & Human Development, 54(4), 1141–1151. [Google Scholar] [CrossRef]
- Fulfs, T., Poulain, T., Vogel, M., Nenoff, K., & Kiess, W. (2024). Associations between sleep problems and emotional/behavioural difficulties in healthy children and adolescents. BMC Pediatrics, 24(1), 15. [Google Scholar] [CrossRef]
- Gormez, V., Kilincaslan, A., Ebesutani, C., Orengul, A. C., Kaya, I., Ceri, V., Nasiroglu, S., Filiz, M., & Chorpita, B. F. (2017). Psychometric properties of the parent version of the revised child anxiety and depression scale in a clinical sample of turkish children and adolescents. Child Psychiatry & Human Development, 48(6), 922–933. [Google Scholar] [CrossRef]
- Gratz, K. L., & Roemer, L. (2004). Multidimensional assessment of emotion regulation and dysregulation: Development, factor structure, and initial validation of the difficulties in emotion regulation scale. Journal of Psychopathology and Behavioral Assessment, 26(1), 41–54. [Google Scholar] [CrossRef]
- Hayes, A. (2013). Introduction to mediation, moderation, and conditional process analysis: A regression-based approach. Guilford Press. [Google Scholar]
- Huguet, A., Izaguirre Eguren, J., Miguel-Ruiz, D., Vall Vallés, X., & Alda, J. A. (2019). Deficient emotional self-regulation in children with attention deficit hyperactivity disorder: Mindfulness as a useful treatment modality. Journal of Developmental & Behavioral Pediatrics, 40(6), 425–431. [Google Scholar] [CrossRef] [PubMed]
- Hvolby, A. (2015). Associations of sleep disturbance with ADHD: Implications for treatment. ADHD Attention Deficit and Hyperactivity Disorders, 7(1), 1–18. [Google Scholar] [CrossRef] [PubMed]
- Kaner, S., Büyüköztürk, Ş., & İşeri, E. (2013). Conners Anababa Dereceleme Ölçeği-Yenilenmiş Kısa: Türkiye Stardardizasyon Çalışması. Nöro Psikiyatri Arşivi, 50, 100–109. [Google Scholar] [CrossRef]
- Kaufman, J., Birmaher, B., Axelson, D., Pereplitchikova, F., Brent, D., & Ryan, N. (2016). Schedule for affective disorders and schizophrenia for school-aged children: Present and lifetime version (K-SADS-PL) DSM-5, November 2016 working draft. Yale University. [Google Scholar]
- Liang, X., Qiu, H., & Li, S. X. (2023). Objectively measured sleep continuity in children and adolescents with ADHD: A systematic review and meta-analysis. Psychiatry Research, 328, 115447. [Google Scholar] [CrossRef]
- Liang, X., Zhao, M., Su, L., Haegele, J. A., Xu, R. H., Li, J., Guo, J., Tse, A. C.-Y., Li, S. X., & Shum, D. H. K. (2024). Sleep problems in children with ADHD: Associations with internalizing symptoms and physical activity. Journal of Autism and Developmental Disorders, 56(3), 1163–1172. [Google Scholar] [CrossRef]
- Loevaas, M. E. S., Sund, A. M., Patras, J., Martinsen, K., Hjemdal, O., Neumer, S.-P., Holen, S., & Reinfjell, T. (2018). Emotion regulation and its relation to symptoms of anxiety and depression in children aged 8–12 years: Does parental gender play a differentiating role? BMC Psychology, 6(1), 42. [Google Scholar] [CrossRef]
- Loram, G., Ling, M., Silk, T., & Sciberras, E. (2023). Associations between ADHD, sleep problems, and mental health symptoms in adolescents. Journal of Attention Disorders, 27(6), 635–642. [Google Scholar] [CrossRef]
- Lugo-Candelas, C., Flegenheimer, C., McDermott, J. M., & Harvey, E. (2017). Emotional understanding, reactivity, and regulation in young children with ADHD symptoms. Journal of Abnormal Child Psychology, 45(7), 1297–1310. [Google Scholar] [CrossRef]
- MacKinnon, D. P., Lockwood, C. M., & Williams, J. (2004). Confidence limits for the indirect effect: Distribution of the product and resampling methods. Multivariate Behavioral Research, 39(1), 99–128. [Google Scholar] [CrossRef] [PubMed]
- Marten, F., Keuppens, L., Baeyens, D., Boyer, B. E., Danckaerts, M., Cortese, S., & Van der Oord, S. (2023). Sleep parameters and problems in adolescents with and without ADHD: A systematic review and meta-analysis. JCPP Advances, 3(3), e12151. [Google Scholar] [CrossRef] [PubMed]
- Mick, E., Biederman, J., Jetton, J., & Faraone, S. V. (2000). Sleep disturbances associated with attention deficit hyperactivity disorder: The impact of psychiatric comorbidity and pharmacotherapy. Journal of Child and Adolescent Psychopharmacology, 10(3), 223–231. [Google Scholar] [CrossRef] [PubMed]
- Mindell, J., & Owens, J. (2010). A clinical guide to pediatric sleep: Diagnosis and management of sleep problems (2nd ed.). Lippincott Williams and Wilkins. [Google Scholar]
- Overgaard, K. R., Oerbeck, B., Aase, H., Torgersen, S., Reichborn-Kjennerud, T., & Zeiner, P. (2018). Emotional lability in preschoolers with symptoms of ADHD. Journal of Attention Disorders, 22(8), 787–795. [Google Scholar] [CrossRef]
- Owens, J. A. (2005). The ADHD and sleep conundrum. Journal of Developmental & Behavioral Pediatrics, 26(4), 312–322. [Google Scholar] [CrossRef]
- Owens, J. A., Maxim, R., Nobile, C., McGuinn, M., & Msall, M. (2000a). Parental and self-report of sleep in children with attention-deficit/hyperactivity disorder. Archives of Pediatrics & Adolescent Medicine, 154(6), 549. [Google Scholar] [CrossRef]
- Owens, J. A., Spirito, A., & McGuinn, M. (2000b). The children’s sleep habits questionnaire (CSHQ): Psychometric properties of a survey instrument for school-aged children. Sleep, 23(8), 1043–1051. [Google Scholar] [CrossRef]
- Özbaran, B., Kalyoncu, T., & Köse, S. (2018). Theory of mind and emotion regulation difficulties in children with ADHD. Psychiatry Research, 270, 117–122. [Google Scholar] [CrossRef]
- Paulus, F. W., Ohmann, S., Möhler, E., Plener, P., & Popow, C. (2021). Emotional dysregulation in children and adolescents with psychiatric disorders. A narrative review. Frontiers in Psychiatry, 12, 628252. [Google Scholar] [CrossRef]
- Perdahlı Fiş, N., Arman, A., Topuzoglu, A., Selcen GÜLER, A., Gökçe İmren, S., Ersu, R., & Berkem, M. (2010). Perdahlı Fiş ve ark. 151 Çocuk Uyku Alışkanlıkları Anketinin Türkçe geçerliliği ve güvenilirliği. Anadolu Psikiyatri Dergisi, 11(11), 151–160. [Google Scholar]
- Polanczyk, G. V., Willcutt, E. G., Salum, G. A., Kieling, C., & Rohde, L. A. (2014). ADHD prevalence estimates across three decades: An updated systematic review and meta-regression analysis. International Journal of Epidemiology, 43(2), 434–442. [Google Scholar] [CrossRef] [PubMed]
- Preacher, K. J., & Hayes, A. F. (2008). Asymptotic and resampling strategies for assessing and comparing indirect effects in multiple mediator models. Behavior Research Methods, 40(3), 879–891. [Google Scholar] [CrossRef] [PubMed]
- Rydell, A.-M., Berlin, L., & Bohlin, G. (2003). Emotionality, emotion regulation, and adaptation among 5- to 8-year-old children. Emotion, 3(1), 30–47. [Google Scholar] [CrossRef] [PubMed]
- Schatz, D. B., & Rostain, A. L. (2006). ADHD with comorbid anxiety. Journal of Attention Disorders, 10(2), 141–149. [Google Scholar] [CrossRef]
- Shanahan, L., Copeland, W. E., Angold, A., Bondy, C. L., & Costello, E. J. (2014). Sleep problems predict and are predicted by generalized anxiety/depression and oppositional defiant disorder. Journal of the American Academy of Child & Adolescent Psychiatry, 53(5), 550–558. [Google Scholar] [CrossRef]
- Soler-Gutiérrez, A.-M., Pérez-González, J.-C., & Mayas, J. (2023). Evidence of emotion dysregulation as a core symptom of adult ADHD: A systematic review. PLoS ONE, 18(1), e0280131. [Google Scholar] [CrossRef]
- Steiner, H., & Remsing, L. (2007). Practice parameter for the assessment and treatment of children and adolescents with oppositional defiant disorder. Journal of the American Academy of Child & Adolescent Psychiatry, 46(1), 126–141. [Google Scholar] [CrossRef]
- Tatlı Harmancı, S., & Güngör Aytar, F. A. (2023). Çocuklar için Duygu Düzenleme Ölçeği Çocuk Formu (ÇDDÖ) ve Yetişkin Formunun (ÇDDÖ-YF) Türkçeye Uyarlanması. Milli Eğitim, 237, 71–106. [Google Scholar] [CrossRef]
- Thompson, R. A. (1994). Emotion regulation: A theme in search of definition. Monographs of the Society for Research in Child Development, 59(2–3), 25–52. [Google Scholar] [CrossRef]
- Tomic, T., Mombelli, S., Oana, S., Ferini-Strambi, L., Raballo, A., Manconi, M., Galbiati, A., & Castelnovo, A. (2025). Psychopathology and NREM sleep parasomnias: A systematic review. Sleep Medicine Reviews, 80, 102043. [Google Scholar] [CrossRef]
- Tonacci, A., Billeci, L., Calderoni, S., Levantini, V., Masi, G., Milone, A., Pisano, S., & Muratori, P. (2019). Sympathetic arousal in children with oppositional defiant disorder and its relation to emotional dysregulation. Journal of Affective Disorders, 257, 207–213. [Google Scholar] [CrossRef]
- Tung, I., Li, J. J., Meza, J. I., Jezior, K. L., Kianmahd, J. S. V., Hentschel, P. G., O’Neil, P. M., & Lee, S. S. (2016). Patterns of comorbidity among girls with ADHD: A meta-analysis. Pediatrics, 138(4), e20160430. [Google Scholar] [CrossRef]
- Unal, F., Oktem, F., Cetin Cuhadaroglu, F., Cengel Kultur, S. E., Akdemir, D., Foto Ozdemir, D., Cak, H. T., Unal, D., Tiras, K., Aslan, C., Kalayci, B. M., Sultan Dogan, B., Kutuk, F., Yanar, E., Karaokur, R., Karabucak, B., Karakok, B., Karaer, Y., & Artik, A. (2019). Reliability and validity of the schedule for affective disorders and schizophrenia for school-age children-present and lifetime version, DSM-5 November 2016-Turkish Adaptation (K-SADS-PL-DSM-5-T). Turkish Journal of Psychiatry, 30(1), 42–50. [Google Scholar] [CrossRef]
- Wang, B., Eastwood, P. R., Becker, A., Isensee, C., Wong, J. W. Y., Huang, R.-C., Runions, K. C., Stewart, R. M., Meyer, T., Brüni, L. G., Rothenberger, A., & Zepf, F. D. (2019). Concurrent developmental course of sleep problems and emotional/behavioral problems in childhood and adolescence as reflected by the dysregulation profile. Sleep, 42(3), zsy243. [Google Scholar] [CrossRef]
- Williams, K. E., & Sciberras, E. (2016). Sleep and self-regulation from birth to 7 years. Journal of Developmental & Behavioral Pediatrics, 37(5), 385–394. [Google Scholar] [CrossRef]



| Variables | ADHD (n = 100) Mean ± SD | Control (n = 50) Mean ± SD | Statistical Analysis | ||
|---|---|---|---|---|---|
| t | p | Effect Size | |||
| Age | 9.88 ± 2.30 | 9.95 ± 2.27 | −0.164 | 0.870 | d = 0.030 |
| Mobile Phone Time | 49.22 ± 51.60 | 47.00 ± 50.44 | 0.250 | 0.803 | d = 0.043 |
| Total Screen Time | 198.30 ± 122.17 | 186.60 ± 98.71 | 0.631 | 0.529 | d = 0.105 |
| CPRS-RS | |||||
| CP/inattention | 11.42 ± 4.38 | 4.46 ± 3.81 | 9.551 | <0.001 * | d = 1.695 |
| Hyperactivity | 8.08 ± 4.69 | 2.60 ± 2.63 | 9.148 | <0.001 * | d = 1.441 |
| Oppositional defiance | 9.99 ± 4.28 | 4.48 ± 3.21 | 7.240 | <0.001 * | d = 1.456 |
| ADHD index | 22.10 ± 7.27 | 9.34 ± 6.19 | 10.630 | <0.001 * | d = 1.889 |
| CSHQ | |||||
| Bedtime resistance | 9.63 ± 3.33 | 8.76 ± 3.07 | 1.545 | 0.125 | d = 0.271 |
| Sleep onset delay | 1.56 ± 0.75 | 1.38 ± 0.63 | 1.533 | 0.128 | d = 0.259 |
| Sleep duration | 3.84 ± 1.79 | 3.86 ± 1.41 | −0.083 | 0.934 | d = 0.012 |
| Sleep anxiety | 6.46 ± 2.36 | 6.34 ± 2.31 | 0.295 | 0.768 | d = 0.051 |
| Night wakings | 4.17 ± 1.33 | 4.04 ± 1.04 | 0.602 | 0.548 | d = 0.108 |
| Parasomnias | 9.16 ± 1.95 | 8.26 ± 1.46 | 2.870 | 0.005 | d = 0.522 |
| Sleep breathing | 3.61 ± 1.15 | 3.32 ± 0.62 | 2.000 | 0.047 | d = 0.313 |
| Daytime sleepiness | 12.86 ± 3.76 | 11.82 ± 3.42 | 1.644 | 0.102 | d = 0.289 |
| Total | 47.85 ± 8.70 | 44.54 ± 7.43 | 2.301 | 0.023 | d = 0.409 |
| ERSC-A | |||||
| Emotional intensity | 51.34 ± 12.89 | 43.88 ± 10.78 | 3.520 | 0.001 * | d = 0.627 |
| Emotion regulation | 82.33 ± 17.26 | 93.36 ± 11.58 | −4.634 | <0.001 * | d = 0.750 |
| RCADS | |||||
| Internalization | 29.99 ± 18.93 | 23.34 ± 12.28 | 2.589 | 0.011 | d = 0.416 |
| n (%) | n (%) | x2 | p | ||
| Gender | 0.318 | 0.673 | |||
| Boy | 80 (80.0) | 38 (76.0) | |||
| Girl | 20 (20.0) | 12 (24.0) | |||
| Family Structure | 0.531 | 0.586 | |||
| Together | 90 (90.0) | 43 (86.0) | |||
| Separated/divorced | 10 (10.0) | 7 (14.0) | |||
| ADHD Presentation | - | - | - | ||
| Inattention | 33 (33.0) | ||||
| Hyperactivity | 4 (4.0) | ||||
| Combined | 63 (63.0) | ||||
| ADHD Medication | - | - | - | ||
| Yes | 61 (61.0) | ||||
| No | 39 (39.0) | ||||
| Variables | CSHQ-BR | CSHQ-SOD | CSHQ- SD | CSHQ- SA | CSHQ- NW | CSHQ- P | CSHQ- SDB | CSHQ- DS | CSHQ- Total |
|---|---|---|---|---|---|---|---|---|---|
| Age | −0.260 * | 0.127 | 0.089 | −0.365 * | −0.331 * | −0.089 | −0.106 | 0.115 | −0.147 |
| Mobile phone time | 0.047 | 0.180 | 0.127 | −0.018 | −0.012 | 0.003 | 0.065 | 0.144 | 0.119 |
| Total screen time | 0.009 | 0.189 | 0.206 | −0.037 | −0.098 | 0.058 | 0.131 | 0.166 | 0.136 |
| CPRS-RS Oppositional defiance | 0.314 * | 0.114 | 0.079 | 0.310 * | 0.222 | 0.372 * | 0.242 * | 0.304 * | 0.468 * |
| CPRS-RS ADHD index | 0.250 * | 0.088 | 0.037 | 0.206 | 0.230 * | 0.317 * | 0.203 * | 0.247 * | 0.377 * |
| ERSC-A Emotional intensity | 0.288 * | −0.001 | −0.008 | 0.351 * | 0.387 * | 0.302 * | 0.249 * | 0.315 * | 0.455 * |
| ERSC-A Emotion regulation | −0.252 * | −0.038 | −0.164 | −0.252 * | −0.092 | −0.214 | −0.062 | −0.178 | −0.305 * |
| RCADS-Internalization | 0.386 * | 0.140 | 0.155 | 0.404 * | 0.270 * | 0.351 * | 0.328 * | 0.316 * | 0.538 * |
| Variables | CSHQ- BR | CSHQ- SOD | CSHQ- SD | CSHQ- SA | CSHQ- NW | CSHQ- P | CSHQ- SDB | CSHQ- DS | CSHQ- Total |
|---|---|---|---|---|---|---|---|---|---|
| Age | −0.290 | −0.036 | 0.254 | −0.321 | −0.315 | −0.273 | −0.140 | 0.216 | −0.113 |
| Mobile phone time | 0.022 | 0.215 | 0.460 * | −0.053 | 0.211 | 0.250 | 0.194 | 0.293 | 0.353 |
| Total screen time | 0.121 | 0.164 | 0.235 | 0.021 | 0.122 | 0.072 | 0.135 | 0.291 | 0.305 |
| CPRS-RS Oppositional defiance | 0.119 | 0.269 | −0.088 | 0.013 | 0.073 | 0.211 | 0.095 | 0.112 | 0.183 |
| CPRS-RS ADHD index | 0.041 | 0.210 | 0.103 | −0.095 | 0.189 | 0.172 | 0.067 | 0.172 | 0.195 |
| ERSC-A Emotional intensity | 0.246 | 0.230 | −0.195 | 0.288 | 0.183 | 0.458 * | 0.103 | −0.045 | 0.256 |
| ERSC-A Emotion regulation | −0.097 | −0.108 | 0.079 | −0.027 | −0.146 | −0.037 | −0.096 | −0.208 | −0.189 |
| RCADS-Internalization | 0.221 | 0.056 | 0.118 | 0.336 | 0.336 * | 0.409 * | 0.103 | 0.283 | 0.465 * |
| Variables | β | p | Variables | β | p |
|---|---|---|---|---|---|
| DV: bedtime resistance a | DV: parasomnias f | ||||
| Age | −0.288 | 0.003 * | Age | −0.081 | 0.409 |
| ADHD index | 0.021 | 0.859 | ADHD index | 0.081 | 0.514 |
| Oppositional defiance | 0.131 | 0.391 | Oppositional defiance | 0.256 | 0.106 |
| EI | −0.137 | 0.344 | EI | −0.050 | 0.736 |
| ER | −0.031 | 0.803 | ER | 0.064 | 0.616 |
| RCADS-Internalization | 0.398 | 0.003 * | RCADS-Internalization | 0.249 | 0.064 |
| R2 = 0.242, F = 4.959 | p < 0.001 | R2 = 0.187, F = 3.576 | p = 0.003 | ||
| DV: sleep onset delay b | DV: sleep breathing g | ||||
| Age | 0.096 | 0.360 | Age | −0.121 | 0.225 |
| ADHD index | −0.010 | 0.939 | ADHD index | −0.033 | 0.793 |
| Oppositional defiance | 0.211 | 0.214 | Oppositional defiance | 0.206 | 0.199 |
| EI | −0.227 | 0.159 | EI | 0.005 | 0.976 |
| ER | 0.057 | 0.678 | ER | 0.236 | 0.071 |
| RCADS-Internalization | 0.210 | 0.145 | RCADS-Internalization | 0.354 | 0.011 * |
| R2 = 0.064, F = 1.063 | p = 0.390 | R2 = 0.159, F = 2.938 | p = 0.011 | ||
| DV: sleep duration c | DV: daytime sleepiness h | ||||
| Age | 0.049 | 0.640 | Age | 0.153 | 0.127 |
| ADHD index | −0.013 | 0.919 | ADHD index | 0.033 | 0.794 |
| Oppositional defiance | 0.042 | 0.804 | Oppositional defiance | 0.172 | 0.285 |
| EI | −0.266 | 0.099 | EI | 0.168 | 0.270 |
| ER | −0.192 | 0.162 | ER | 0.084 | 0.518 |
| RCADS-Internalization | 0.211 | 0.142 | RCADS-Internalization | 0.135 | 0.321 |
| R2 = 0.072, F = 1.197 | p = 0.315 | R2 = 0.159, F = 2.937 | p = 0.011 | ||
| DV: sleep anxiety d | DV: CSHQ-Total i | ||||
| Age | −0.393 | <0.001 * | Age | −0.147 | 0.093 |
| ADHD index | −0.073 | 0.516 | ADHD index | 0.030 | 0.784 |
| Oppositional defiance | 0.106 | 0.459 | Oppositional defiance | 0.248 | 0.076 |
| EI | −0.043 | 0.752 | EI | 0.004 | 0.977 |
| ER | 0.016 | 0.890 | ER | 0.081 | 0.470 |
| RCADS-Internalization | 0.457 | <0.001 * | RCADS-Internalization | 0.443 | <0.001 * |
| R2 = 0.333, F = 7.749 | p < 0.001 | R2 = 0.366, F = 8.956 | p < 0.001 | ||
| DV: night wakings e | |||||
| Age | −0.295 | 0.002 * | |||
| ADHD index | 0.062 | 0.603 | |||
| Oppositional defiance | −0.046 | 0.758 | |||
| EI | 0.346 | 0.017 * | |||
| ER | 0.174 | 0.156 | |||
| RCADS-Internalization | 0.137 | 0.288 | |||
| R2 = 0.256, F = 5.325 | p < 0.001 |
| Path | Standardized Coefficients | S.E. | p | 95% CI | |
|---|---|---|---|---|---|
| Lower | Upper | ||||
| Direct Effects | |||||
| X→M1 (a1) | 0.464 * | 0.158 | <0.001 | 0.508 | 1.137 |
| X→M2 (a2) | 0.202 * | 0.212 | 0.014 | 0.107 | 0.952 |
| M1→M2 (a3) | 0.603 * | 0.121 | <0.001 | 0.650 | 1.133 |
| M1→Y (b1) | 0.062 | 0.080 | 0.603 | −0.118 | 0.202 |
| M2→Y (b2) | 0.474 * | 0.054 | <0.001 | 0.108 | 0.325 |
| X→Y (c’) | 0.105 | 0.116 | 0.282 | −0.105 | 0.356 |
| Indirect Effect | |||||
| X→M1→Y | 0.028 | 0.049 | - | −0.061 | 0.137 |
| X→M2→Y | 0.095 * | 0.037 | - | 0.030 | 0.177 |
| X→M1→M2→Y | 0.132 * | 0.040 | - | 0.061 | 0.220 |
| Total Effect (c) | 0.362 * | 0.112 | <0.001 | 0.210 | 0.657 |
| Path | Standardized Coefficients | S.E. | p | 95% CI | |
|---|---|---|---|---|---|
| Lower | Upper | ||||
| Direct Effects | |||||
| X→M1 (a1) | −0.273 * | 0.234 | 0.006 | −1.115 | −0.183 |
| X→M2 (a2) | 0.376 * | 0.221 | <0.001 | 0.547 | 1.426 |
| M1→M2 (a3) | −0.386 * | 0.093 | <0.001 | −0.611 | −0.242 |
| M1→Y (b1) | −0.017 | 0.048 | 0.857 | −0.104 | 0.087 |
| M2→Y (b2) | 0.503 * | 0.048 | <0.001 | 0.134 | 0.325 |
| X→Y (c’) | 0.115 | 0.113 | 0.229 | −0.088 | 0.363 |
| Indirect Effect | |||||
| X→M1→Y | 0.004 | 0.031 | - | −0.044 | 0.082 |
| X→M2→Y | 0.189 * | 0.049 | - | 0.098 | 0.294 |
| X→M1→M2→Y | 0.053 * | 0.025 | - | 0.009 | 0.108 |
| Total Effect (c) | 0.362 * | 0.112 | <0.001 | 0.210 | 0.657 |
| Path | Standardized Coefficients | S.E. | p | 95% CI | |
|---|---|---|---|---|---|
| Lower | Upper | ||||
| Direct Effects | |||||
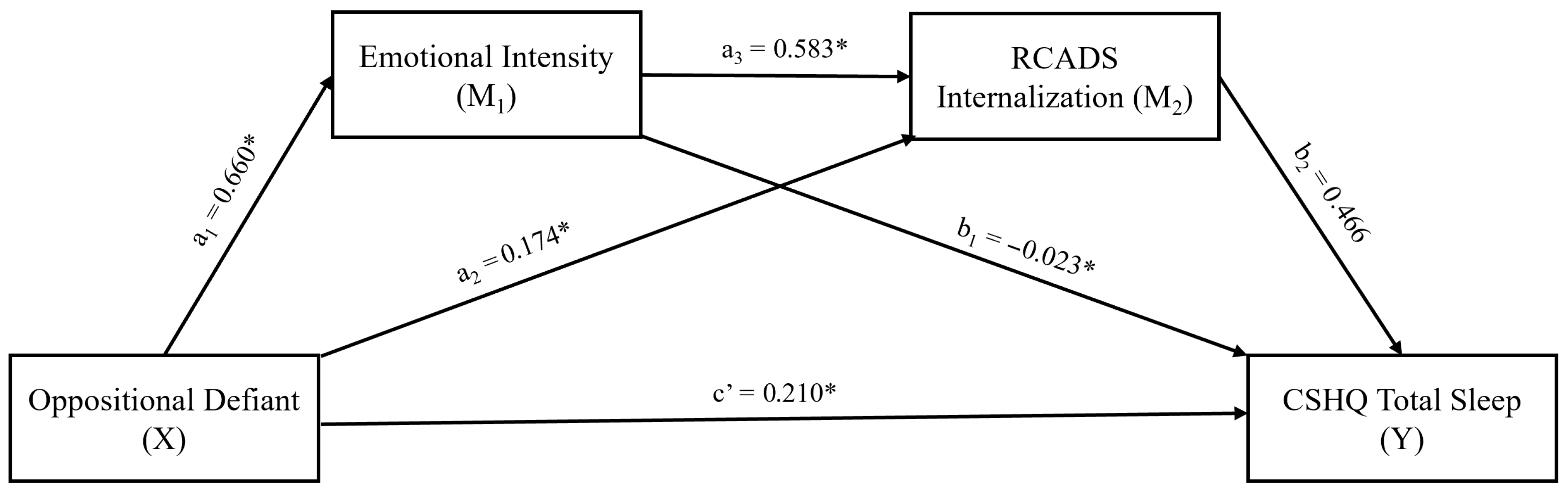
| X→M1 (a1) | 0.660 * | 0.229 | <0.001 | 1.529 | 2.442 |
| X→M2 (a2) | 0.174 | 0.435 | 0.077 | −0.087 | 1.642 |
| M1→M2 (a3) | 0.583 * | 0.145 | <0.001 | 0.573 | 1.151 |
| M1→Y (b1) | −0.023 | 0.087 | 0.860 | −0.190 | 0.159 |
| M2→Y (b2) | 0.466 * | 0.053 | <0.001 | 0.107 | 0.318 |
| X→Y (c’) | 0.210 | 0.228 | 0.063 | −0.025 | 0.881 |
| Indirect Effect | |||||
| X→M1→Y | −0.015 | 0.070 | - | −0.150 | 0.124 |
| X→M2→Y | 0.081 | 0.048 | - | −0.011 | 0.181 |
| X→M1→M2→Y | 0.179 * | 0.049 | - | 0.094 | 0.286 |
| Total Effect (c) | 0.457 * | 0.184 | <0.001 | 0.562 | 1.293 |
| Path | Standardized Coefficients | S.E. | p | 95% CI | |
|---|---|---|---|---|---|
| Lower | Upper | ||||
| Direct Effects | |||||
| X→M1 (a1) | −0.625 * | 0.327 | <0.001 | −3.167 | −1.866 |
| X→M2 (a2) | 0.412 * | 0.474 | <0.001 | 0.891 | 2.773 |
| M1→M2 (a3) | −0.236 * | 0.116 | 0.027 | −0.492 | −0.029 |
| M1→Y (b1) | 0.088 | 0.053 | 0.409 | −0.062 | 0.151 |
| M2→Y (b2) | 0.475 * | 0.046 | <0.001 | 0.124 | 0.309 |
| X→Y (c’) | 0.246 * | 0.229 | 0.031 | 0.044 | 0.955 |
| Indirect Effect | |||||
| X→M1→Y | −0.055 | 0.075 | - | −0.208 | 0.085 |
| X→M2→Y | 0.195 * | 0.064 | - | 0.074 | 0.330 |
| X→M1→M2→Y | 0.070 * | 0.038 | - | 0.005 | 0.159 |
| Total Effect (c) | 0.457 * | 0.184 | <0.001 | 0.562 | 1.293 |
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2026 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license.
Share and Cite
Sevincok, D.; Ozbay, H.C.; Ozbek, M.M.; Gul, D. Factors Associated with Sleep Problems in Children with ADHD: Focusing on Emotional Regulation, Emotional Intensity and Internalizing Symptoms. Behav. Sci. 2026, 16, 404. https://doi.org/10.3390/bs16030404
Sevincok D, Ozbay HC, Ozbek MM, Gul D. Factors Associated with Sleep Problems in Children with ADHD: Focusing on Emotional Regulation, Emotional Intensity and Internalizing Symptoms. Behavioral Sciences. 2026; 16(3):404. https://doi.org/10.3390/bs16030404
Chicago/Turabian StyleSevincok, Doga, Hasan Can Ozbay, Mutlu Muhammed Ozbek, and Doruk Gul. 2026. "Factors Associated with Sleep Problems in Children with ADHD: Focusing on Emotional Regulation, Emotional Intensity and Internalizing Symptoms" Behavioral Sciences 16, no. 3: 404. https://doi.org/10.3390/bs16030404
APA StyleSevincok, D., Ozbay, H. C., Ozbek, M. M., & Gul, D. (2026). Factors Associated with Sleep Problems in Children with ADHD: Focusing on Emotional Regulation, Emotional Intensity and Internalizing Symptoms. Behavioral Sciences, 16(3), 404. https://doi.org/10.3390/bs16030404






