Burnout and Its Associated Factors Among Long-Term Care Workers: A Mixed-Methods Study Based on the Social–Ecological Framework
Abstract
1. Introduction
2. Methods
2.1. Study Design
2.2. Samples and Sampling Methods
2.3. Data Collection Instruments
2.3.1. Quantitative: MBI Scale and Other Variables
2.3.2. Qualitative: Semi-Structured Interview Outline
2.4. Ethical Considerations and Data Protection
2.5. Data Analysis
3. Results
3.1. Quantitative Findings
3.1.1. Participant Characteristics and Descriptive Statistics for Variables
3.1.2. Factors Associated with Burnout
3.2. Qualitative Findings
3.2.1. Individual-Level Cognitive Adaptation and Comparative Advantage Enhance Career Resilience
“Honestly, we’re all from rural areas and don’t have a ton of skills. So, we work here. At first, it’s pretty tiring, but we get used to it. It’s nice to earn some money.”(A9, Female, Residential)
“I have also worked in factories, where I was told I could not keep up with the younger workers. Given my age, I felt that earning such a wage was acceptable and I should be content with my situation.”(A12, Female, Home-based)
3.2.2. Interpersonal Emotional Interaction and Caregiving Feedback Help Alleviate Burnout
“Each time I finish the home visit and say I’m about to leave, she’s still smiling—clearly happy—and I feel genuinely gratified.”(A7, Female, Home-based)
3.2.3. Intensive Caregiving Work Is a Primary Contributor to Burnout
“… It’s quite exhausting. If they need something at night…I have to get up to help them, so I don’t get enough rest.”(A4, Male, Residential)
“I’ve been doing this job for almost ten years. Honestly, I feel like my personality has been worn down over time.”(A9, Female, Residential)
3.2.4. Institution Type and Training Are Potential Protective Factors Against Burnout
“I can visit different households and talk to different people; the environment feels fresher. In the nursing home, it’s the same place every day, and sometimes it feels a bit depressing.”(A14, Female, Home-based)
“I live and work in the nursing home now. I’ve never done the kind of home-based care. I don’t like running around—it’s tiring to go back and forth, and when it rains or gets hot, it’s really inconvenient.”(A2, Female, Residential)
“I have no experience, but there is training related to caring for older adults, for example, how to turn an elderly person more quickly and easily…. I work better and faster after this, much better than when I didn’t know”(A1, Female, Residential)
3.2.5. Policy Recognition Inspires a Sense of Professional Value to Help Alleviate Burnout
“… I told myself that this really is a noble profession. Only with that belief can you do this not-so-easy job well… It’s a good policy—it has given us job opportunities and reduced the burden on older adults and their families.”(A10, Male, Residential)
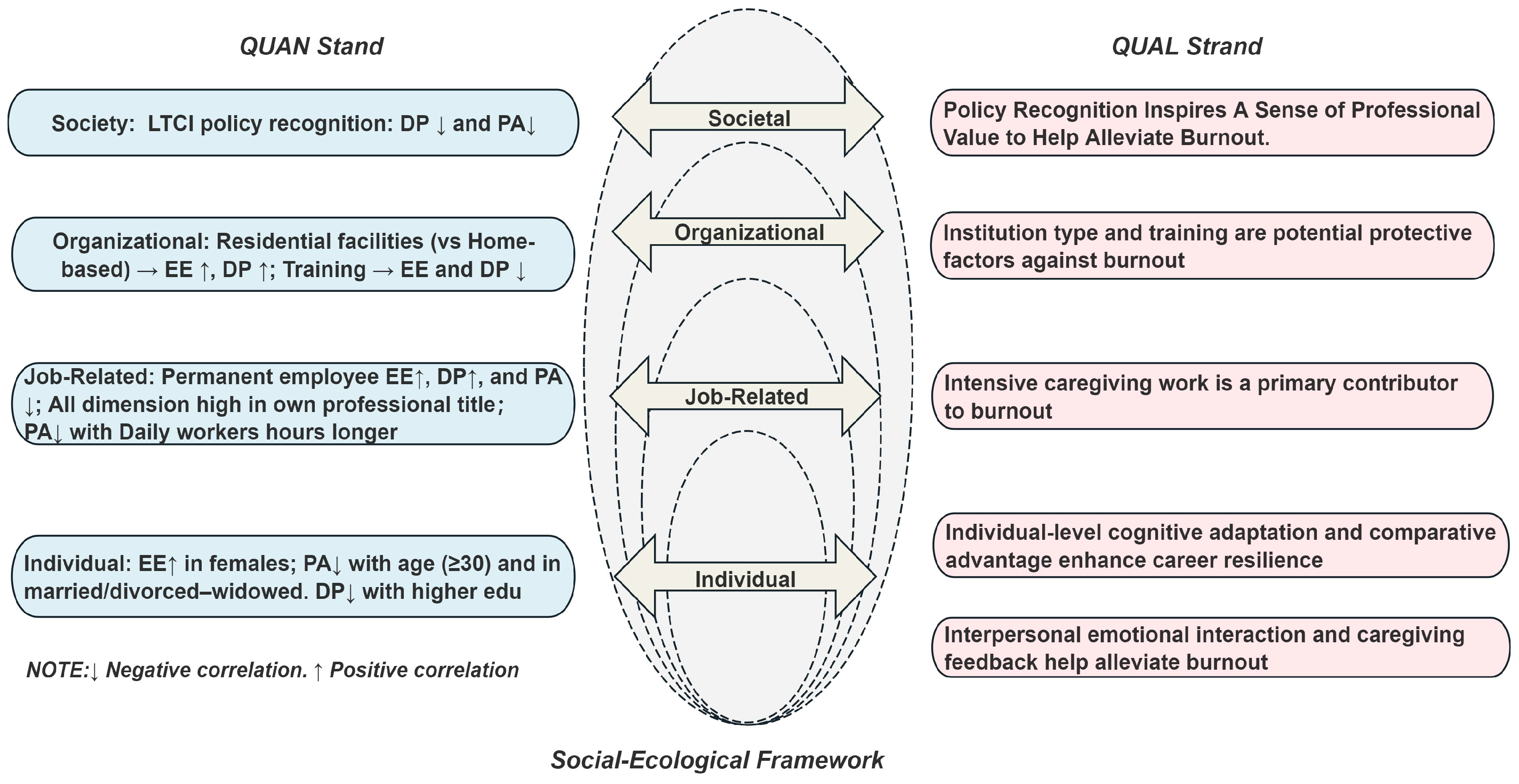
3.3. Joint Exhibition of QUAN + QUAL Findings
4. Discussion
5. Conclusions
Supplementary Materials
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Acknowledgments
Conflicts of Interest
References
- Bronfenbrenner, U. (1977). Toward an experimental ecology of human development. American Psychologist, 32(7), 513–531. [Google Scholar] [CrossRef]
- Chao, S.-F. (2019). Does geriatric nursing staff burnout predict well-being of LTC residents? Geriatric Nursing, 40(4), 360–366. [Google Scholar] [CrossRef]
- Chen, C., & Meier, S. T. (2021). Burnout and depression in nurses: A systematic review and meta-analysis. International Journal of Nursing Studies, 124, 104099. [Google Scholar] [CrossRef]
- Chen, Y., Ji, H., Shen, Y., & Liu, D. (2024). Chronic disease and multimorbidity in the Chinese older adults’ population and their impact on daily living ability: A cross-sectional study of the Chinese longitudinal healthy longevity survey (CLHLS). Archives of Public Health, 82(1), 17. [Google Scholar] [CrossRef] [PubMed]
- China News. (2024, October 28). Eight years into the LTC insurance pilot, which populations have benefited? What are the shortcomings that need to be remedied? Available online: https://news.cctv.com/2024/10/28/ARTI25QwzSWihIP46jwSixaH241028.shtml (accessed on 24 March 2025).
- Colindres, C. V., Bryce, E., Coral-Rosero, P., Ramos-Soto, R. m., Bonilla, F., & Yassi, A. (2018). Effect of effort-reward imbalance and burnout on infection control among Ecuadorian nurses. International Nursing Review, 65(2), 190–199. [Google Scholar] [CrossRef] [PubMed]
- Coomber, B., & Louise Barriball, K. (2007). Impact of job satisfaction components on intent to leave and turnover for hospital-based nurses: A review of the research literature. International Journal of Nursing Studies, 44(2), 297–314. [Google Scholar] [CrossRef]
- Dall’Ora, C., Ball, J., Reinius, M., & Griffiths, P. (2020). Burnout in nursing: A theoretical review. Human Resources for Health, 18(1), 41. [Google Scholar] [CrossRef] [PubMed]
- De Graves, B. S., Titley, H., Duan, Y., Thorne, T. E., Banerjee, S., Ginsburg, L., Salma, J., Hegadoren, K., Angel, C., Keefe, J., Lanius, R., & Estabrooks, C. A. (2024). Workforce resilience supporting staff in managing stress: A coherent breathing intervention for the long-term care workforce. Journal of the American Geriatrics Society, 72(3), 753–766. [Google Scholar] [CrossRef]
- De Lisser, R., Lauderdale, J., Dietrich, M. S., Ramanujam, R., & Stolldorf, D. P. (2024). The Social Ecology of Burnout: A framework for research on nurse practitioner burnout. Nursing Outlook, 72(4), 102188. [Google Scholar] [CrossRef]
- Fetters, M. D., Curry, L. A., & Creswell, J. W. (2013). Achieving integration in mixed methods designs-principles and practices. Health Services Research, 48(6), 2134–2156. [Google Scholar] [CrossRef] [PubMed]
- Ge, M.-W., Hu, F.-H., Jia, Y.-J., Tang, W., Zhang, W.-Q., & Chen, H.-L. (2023). Global prevalence of nursing burnout syndrome and temporal trends for the last 10 years: A meta-analysis of 94 studies covering over 30 countries. Journal of Clinical Nursing, 32(17–18), 5836–5854. [Google Scholar] [CrossRef]
- Giesbrecht, M., Stajduhar, K. I., Cloutier, D., & Dujela, C. (2021). “We are to be like machines…fill the bed before it gets cold”: Exploring the emotional geographies of healthcare providers caring for dying residents in long-term care facilities. Social Science & Medicine, 272, 113749. [Google Scholar] [CrossRef]
- Global Coalition on Aging. (2021, July). Building the caregiving workforce our aging world needs. Available online: https://globalcoalitiononaging.com/initiative/building-the-caregiving-workforce-our-aging-world-needs/ (accessed on 27 March 2025).
- Goffman, E. (2022). Asylums: Essays on the social situation of mental patients and other inmates. Penguin Books. [Google Scholar]
- Golden, S. D., & Earp, J. A. L. (2012). Social ecological approaches to individuals and their contexts: Twenty years of health education & behavior health promotion interventions. Health Education & Behavior: The Official Publication of the Society for Public Health Education, 39(3), 364–372. [Google Scholar] [CrossRef]
- Hennink, M. M., Kaiser, B. N., & Marconi, V. C. (2017). Code saturation versus meaning saturation: How many interviews are enough? Qualitative Health Research, 27(4), 591–608. [Google Scholar] [CrossRef] [PubMed]
- Heyink, J. (1993). Adaptation and well-being. Psychological Reports, 73(3), 1331–1342. [Google Scholar] [CrossRef]
- Hung, Y.-N., & Chiu, T.-Y. (2023). Examining the relationship between personality traits, work experience, burnout, and intention to stay among home care aides in Taiwan. BMC Geriatrics, 23(1), 434. [Google Scholar] [CrossRef]
- Hwalek, M., Straub, V., & Kosniewski, K. (2008). Older workers: An opportunity to expand the long-term care/direct care labor force. Gerontologist, 48, 90–103. [Google Scholar] [CrossRef][Green Version]
- Johnson, R. B., & Onwuegbuzie, A. J. (2004). Mixed Methods Research: A Research Paradigm Whose Time Has Come. Educational Researcher, 33(7), 14–26. [Google Scholar] [CrossRef]
- Khalaila, R. (2022). Does emotional empathy moderate the association between caregiver burden and burnout among arab family caregivers of older relatives? Health & Social Care in the Community, 30(5), e2478–e2488. [Google Scholar] [CrossRef]
- Kim, B. J., & Choi, C. J. W. (2023). Impact of compensation and willingness to keep same career path on burnout among long-term care workers in Japan. Human Resources for Health, 21(1), 64. [Google Scholar] [CrossRef]
- Lee-Treweek, G. (1997). Women, resistance and care: An ethnographic study of nursing auxiliary work. Work, Employment and Society, 11(1), 47–63. [Google Scholar] [CrossRef]
- Leiter, M. P., & Maslach, C. (2009). Nurse turnover: The mediating role of burnout. Journal of Nursing Management, 17(3), 331–339. [Google Scholar] [CrossRef]
- Li, C., & Shi, K. (2003). The influence of distributive justice and procedural justice on job burnout. Acta Psychologica Sinica, (5), 677–684. [Google Scholar]
- Li, Y., & Li, Y. (2006). Developing the diagnostic ctiterion of job burnout. Psychological Science, (1), 148–150, 153. [Google Scholar] [CrossRef]
- Lin, K.-H., Selvanayagam, N., Patnaik, S., & Kuo, C.-Y. (2025). Burnout among physicians and nurses working in intensive care units and emergency departments: A systematic review and meta-analysis. Journal of Emergency Nursing, 51(4), 702–720. [Google Scholar] [CrossRef]
- Liu, Y., Xu, W., Yang, Z., Wang, Y., Lu, R., Gao, Y., & Zhong, Y. (2025). Caregiving experiences of family caregivers of disabled middle-aged and older adults enrolled in long-term care insurance: A qualitative study. BMC Nursing, 24(1), 67. [Google Scholar] [CrossRef]
- Lopez, S. H. (2006). Emotional labor and organized emotional care: Conceptualizing nursing home care work. Work and Occupations, 33(2), 133–160. [Google Scholar] [CrossRef]
- Maslach, C., Schaufeli, W. B., & Leiter, M. P. (2001). Job burnout. Annual Review of Psychology, 52(1), 397–422. [Google Scholar] [CrossRef] [PubMed]
- McLeroy, K. R., Bibeau, D., Steckler, A., & Glanz, K. (1988). An ecological perspective on health promotion programs. Health Education Quarterly, 15(4), 351–377. [Google Scholar] [CrossRef]
- Miller, K. E., & Rasmussen, A. (2024). War exposure, daily stressors, and mental health 15 years on: Implications of an ecological framework for addressing the mental health of conflict-affected populations. Epidemiology and Psychiatric Sciences, 33, e78. [Google Scholar] [CrossRef] [PubMed]
- Notebaert, L., Crane, M., Carpini, J. A., Timming, A. R., & Eastham, J. (2025). Resilience to workplace incivility: How different recovery experiences influence resilience dimensions. Adversity and Resilience Science, 6(4), 431–445. [Google Scholar] [CrossRef]
- OECD. (2023). Health at a glance 2023: OECD indicators. OECD Publishing. [Google Scholar] [CrossRef]
- OECD. (2025). Health at a glance 2025: OECD indicators (Vol. 2025). OECD Publishing. [Google Scholar] [CrossRef]
- Pluut, H., & Wonders, J. (2020). Not able to lead a healthy life when you need it the most: Dual role of lifestyle behaviors in the association of blurred work-life boundaries with well-being. Frontiers in Psychology, 11, 607294. [Google Scholar] [CrossRef]
- Press Conferences of the State Council Information Office. (2026, January 26). SCIO briefing on China’s economic performance in 2025. Available online: http://english.scio.gov.cn/pressroom/2026-01/26/content_118301853.html (accessed on 26 January 2026).
- Qi, X., Dong, Z., Xie, W., Yang, L., & Li, J. (2024). Professional attractiveness among long-term care workers in nursing homes in China: A cross-sectional study. BMC Health Services Research, 24(1), 548. [Google Scholar] [CrossRef]
- Rachel, H., & Francesco, S. (2018). Factors associated with and impact of burnout in nursing and residential home care workers for the elderly. Acta Bio Medica: Atenei Parmensis, 89(7), 60–69. [Google Scholar] [CrossRef]
- Reichow, B., Kogan, C., Barbui, C., Maggin, D., Salomone, E., Smith, I. C., Yasamy, M. T., & Servili, C. (2024). Caregiver skills training for caregivers of individuals with neurodevelopmental disorders: A systematic review and meta-analysis. Developmental Medicine and Child Neurology, 66(6), 713–724. [Google Scholar] [CrossRef] [PubMed]
- Richard, L., Gauvin, L., & Raine, K. (2011). Ecological models revisited: Their uses and evolution in health promotion over two decades. Annual Review of Public Health, 32, 307–326. [Google Scholar] [CrossRef]
- Rule of Law Daily. (2024, September 12). The construction of the old-age service system with Chinese characteristics has achieved obvious results, and the “four beams and eight pillars” of the old-age service system have been basically established. Available online: http://www.npc.gov.cn/npc/c2/c30834/202409/t20240912_439389.html (accessed on 12 September 2025).
- Saunders, B., Sim, J., Kingstone, T., Baker, S., Waterfield, J., Bartlam, B., Burroughs, H., & Jinks, C. (2018). Saturation in qualitative research: Exploring its conceptualization and operationalization. Quality & Quantity, 52(4), 1893–1907. [Google Scholar] [CrossRef]
- Shaqiqi, W., & Abou El-Soud, F. A. (2024). The mediating role of social support on the relationship between secondary traumatic stress and burnout of nurses caring for COVID-19 patients: A cross-sectional study. Applied Nursing Research, 79, 151844. [Google Scholar] [CrossRef]
- Song, Y., Iaconi, A., Chamberlain, S. A., Cummings, G., Hoben, M., Norton, P., & Estabrooks, C. (2020). Characteristics and work life quality of nursing home care aides in Canada. JAMA Network Open, 3(12), e2029121. [Google Scholar] [CrossRef]
- Stokols, D. (1992). Establishing and maintaining healthy environments. Toward a social ecology of health promotion. American Psychologist, 47(1), 6–22. [Google Scholar] [CrossRef] [PubMed]
- Ugur, H. G., & Erci, B. (2019). The effect of home care for stroke patients and education of caregivers on the caregiver burden and quality of life. Acta Clinica Croatica, 58(2), 321–332. [Google Scholar] [CrossRef]
- Velando-Soriano, A., Ortega-Campos, E., Gómez-Urquiza, J. L., Ramírez-Baena, L., De La Fuente, E. I., & Cañadas-De La Fuente, G. A. (2020). Impact of social support in preventing burnout syndrome in nurses: A systematic review. Japan Journal of Nursing Science, 17(1), e12269. [Google Scholar] [CrossRef] [PubMed]
- Wang, L., Zhou, Y., Fang, X., & Qu, G. (2022). Care burden on family caregivers of patients with dementia and affecting factors in China: A systematic review. Frontiers in Psychiatry, 13, 1004552. [Google Scholar] [CrossRef]
- Wang, X. (2025). Claiming kinship through ‘filial heart’: Migrant care workers in ageing Shanghai. Journal of the Royal Anthropological Institute, 32(1), 132–149. [Google Scholar] [CrossRef]
- Wang, Y., Wang, X., Li, X., & Wen, S. (2024). Multidimensional perspectives on nurse burnout in China: A cross-sectional study of subgroups and predictors. BMC Nursing, 23(1), 941. [Google Scholar] [CrossRef] [PubMed]
- WHO. (2017, January 2). Global strategy and action plan on ageing and health. Available online: https://www.who.int/publications/i/item/9789241513500 (accessed on 28 August 2024).
- WHO. (2021, November 30). Framework for countries to achieve an integrated continuum of long-term care. Available online: https://www.who.int/publications/i/item/9789240038844 (accessed on 17 August 2024).
- WHO. (2024, December 14). Decade of healthy ageing: Plan of action. Available online: https://www.who.int/publications/m/item/decade-of-healthy-ageing-plan-of-action (accessed on 28 August 2024).
- Wu, X. (2023). Negotiating filial care in transitions: An ethnographic study of family involvement in China’s nursing homes. The Journal of Chinese Sociology, 10(1), 9. [Google Scholar] [CrossRef]
- Yan, Z. (2020). An ethical glimpse into nursing home care work in China: Mei banfa. Ethics and Social Welfare, 14(4), 417–424. [Google Scholar] [CrossRef]
- Yan, Z. (2022). “I tried to control my emotions”: Nursing home care workers’ experiences of emotional labor in China. Journal of Cross-Cultural Gerontology, 37(1), 1–22. [Google Scholar] [CrossRef]
- Yan, Z., & Luo, B. (2023). It’s your Liangxin that tells you what to do”: Interpreting workplace-induced emotions in a Chinese nursing home. Journal of Aging Studies, 64, 101111. [Google Scholar] [CrossRef]
- Yau, S. Y., Lee, Y. K. L., Li, S. Y. B., Law, S. P. S., Lai, S. K. V., & Huang, S. (2024). Health care workers’ self-perceived meaning of residential care work. BMC Health Services Research, 24(1), 766. [Google Scholar] [CrossRef]
- Yeatts, D. E., Seckin, G., Shen, Y., Thompson, M., Auden, D., & Cready, C. M. (2018). Burnout among direct-care workers in nursing homes: Influences of organisational, workplace, interpersonal and personal characteristics. Journal of Clinical Nursing, 27(19–20), 3652–3665. [Google Scholar] [CrossRef] [PubMed]
- Yin, Y., & Li, X. (2020). Survey on factors of nurses’ and caregivers’ job burnout in nursing homes. Chinese Nursing Management, 20(2), 215–221. [Google Scholar] [CrossRef]
- Zang, Z. (2022). The care types choice in filial culture: A cross-sectional study of disabled elderly in China. Frontiers in Public Health, 10, 954035. [Google Scholar] [CrossRef]
- Zeng, Y., Feng, Q., Hesketh, T., Christensen, K., & Vaupel, J. W. (2017). Survival, disabilities in activities of daily living, and physical and cognitive functioning among the oldest-old in China: A cohort study. The Lancet, 389(10079), 1619–1629. [Google Scholar] [CrossRef]
- Zhang, L., Shen, S., Zhang, W., & Fang, Y. (2024). What determines informal care need among community-dwelling older adults in China? Results from a longitudinal study. BMC Geriatrics, 24(1), 597. [Google Scholar] [CrossRef] [PubMed]

| Variables | n (%)/Median [IQR] |
|---|---|
| Gender | |
| Male | 81 (16.40) |
| Female | 413 (83.60) |
| Age (years) | 53.31 ± 9.83 |
| 20~29 | 22 (4.45) |
| 30~39 | 29 (5.87) |
| 40~49 | 70 (14.17) |
| 50~59 | 242 (48.99) |
| ≥60 | 131 (26.52) |
| Education | |
| No formal education | 15 (3.04) |
| Primary school | 118 (23.89) |
| Middle school | 204 (41.30) |
| High school/Vocational school | 110 (22.27) |
| Associate degree | 35 (7.09) |
| Bachelor’s degree | 12 (2.43) |
| Marital status | |
| Not married | 133 (26.92) |
| Married | 327 (66.19) |
| Divorced or widowed | 34 (6.88) |
| Life satisfaction | 4.14 ± 0.74 |
| Employment type | |
| Permanent | 24 (4.86) |
| Contract-based | 402 (73.89) |
| Temporary | 68 (21.26) |
| Professional title | |
| No | 232 (46.96) |
| Yes | 262 (53.04) |
| Monthly income (yuan) | |
| ≤1000 | 29 (5.87) |
| 1001–3000 | 93 (18.83) |
| 3001–5000 | 244 (49.39) |
| 5001–8000 | 103 (20.85) |
| ≥8000 | 25 (5.06) |
| Work experience (months) | |
| <3 | 15 (3.04) |
| 3~6 (include) | 31 (6.28) |
| 6~12 (include) | 78 (15.79) |
| 12~24 (include) | 123 (24.90) |
| >24 | 247 (50.00) |
| Daily working hours | |
| <4 h | 79 (15.99) |
| 4~6 (include) h | 121 (24.49) |
| 6~8 (include) h | 153 (30.97) |
| >8 h | 141 (28.54) |
| Monthly rest days | |
| no rest | 87 (17.61) |
| 1~2 | 166 (33.60) |
| 3~4 | 139 (28.14) |
| 5~6 | 45 (9.11) |
| 7~8 | 57 (11.54) |
| Type of organization | |
| Residential-based | 178 (36.03) |
| Home-based | 316 (63.97) |
| Caregiver burden | 21.00 [15.00–27.00] |
| Training Intensity Index (TII) | 12.00 [11.00–12.00] |
| LTCI policy recognition | 59.00 [52.00–65.00] |
| Burnout | 30.00 [16.00–38.00] |
| Emotional exhaustion (EE) | 10.00 [4.00–14.00] |
| Depersonalization (DP) | 8.00 [0–8.00] |
| Reduced personal accomplishment (PA) | 12.00 [4.00–13.00] |
| Level of Burnout | |
| No burnout | 95 (19.23) |
| Mild | 152 (30.77) |
| Moderate | 163 (33.00) |
| Severe | 84 (17.00) |
| Variables | EE | DP | PA | |||
|---|---|---|---|---|---|---|
| B (Robust SE) | 95% CI (LL, UL) | B (Robust SE) | 95% CI (LL, UL) | B (Robust SE) | 95% CI (LL, UL) | |
| Individual-Level Factors | ||||||
| Gender (ref: Male) | ||||||
| Female | 2.201 (0.775) *** | [0.677, 3.724] | 1.065 (0.653) | [−0.218, 2.348] | −0.813 (1.142) | [−3.057,1.431] |
| Age (years) (ref: 20~29) | ||||||
| 30~39 | −1.987 (2.030) | [−5.976, 2.001] | −0.297 (1.437) | [−3.121, 2.527] | −7.223 (3.188) ** | [−13.489, −0.957] |
| 40~49 | −1.707 (1.940) | [−5.520, 2.105] | −2.055 (1.442) | [−4.890, 0.779] | −6.956 (3.064) ** | [−12.978, −0.935] |
| 50~59 | −3.416 (1.965) | [−7.277, 0.445] | −2.232 (1.453) | [−5.088, 0.624] | −8.033 (2.989) *** | [−13.90, −2.160] |
| ≥60 | −2.678 (2.007) | [−6.622, 1.266] | −1.536 (1.485) | [−4.454, 1.383] | −7.973 (3.027) *** | [−13.922, −2.024] |
| Education (ref: No formal education) | ||||||
| Primary school | −0.930 (2.225) | [−5.302, 3.442] | −3.001 (1.947) | [−6.828, 0.825] | 2.636 (2.101) | [−1.493, 6.764] |
| Middle school | 0.663 (2.218) | [−3.696, 5.023] | −2.054 (1.911) | [−5.809, 1.702] | 3.231 (2.103) | [−0.901, 7.364] |
| High school/Vocational school | 1.027 (2.291) | [−3.476, 5.530] | −1.991 (1.969) | [−5.861, 1.879] | 3.128 (2.175) | [−1.146, 7.402] |
| Associate degree | −2.913 (2.593) | [−8.008, 2.182] | −4.920 (2.152) ** | [−9.149, −0.691] | 1.669 (3.083) | [−4.390, 7.728] |
| Bachelor’s degree | −1.299 (3.007) | [−7.208, 4.609] | −4.854 (2.435) ** | [−9.640, −0.069] | 2.962 (3.133) | [−3.195, 9.118] |
| Marital Status (ref: No Married) | ||||||
| Married | 1.175 (0.725) | [−0.250, 2.601] | 0.150 (0.559) | [−0.949, 1.249] | −4.511 *** (1.084) | [−6.641, −2.381] |
| Divorced/Widowed | 0.896 (1.220) | [−1.501, 3.293] | 0.269 (1.006) | [−1.708, 2.247] | −3.946 ** (1.674) | [−7.236, −0.656] |
| Life Satisfaction | −0.936 (0.404) ** | [−1.730, −0.142] | −0.126 (0.316) | [−0.747, 0.495] | 0.214 (0.535) | [−0.838, 1.266] |
| Job-Related Factors | ||||||
| Employment type (ref: Permanent) | ||||||
| Contract-based | −4.488 (1.515) *** | [−7.466, −1.511] | −2.647 (1.276) ** | [−5.155, −0.139] | 5.307 *** (1.630) | [2.105, 8.510] |
| Temporary | −4.200 (1.660) ** | [−7.463, −0.937] | −2.238 (1.354) | [−4.899, 0.424] | 7.747 *** (1.933) | [3.949, 11.545] |
| Professional Title (ref: No) | ||||||
| Yes | 2.343 (0.610) *** | [1.143,3.542] | 1.715 (0.467) *** | [0.796,2.634] | 3.327 *** (0.817) | [1.721,4.934] |
| Monthly Income (yuan) (ref: ≤1000) | ||||||
| 1001–3000 | 2.155 (1.208) | [−0.218, 4.529] | 0.907 (0.790) | [−0.645, 2.460] | −0.226 (1.540) | [−3.253, 2.801] |
| 3001–5000 | 2.560 (1.373) | [−0.139, 5.258] | 0.744 (0.875) | [−0.975, 2.464] | 1.651 (1.742) | [−1.772, 5.073] |
| 5001–8000 | 2.358 (1.493) | [−0.575, 5.292] | 0.329 (1.015) | [−1.665, 2.323] | 0.635 (1.963) | [−3.223, 4.492] |
| ≥8000 | −1.335 (1.655) | [−4.588, 1.918] | −0.230 (1.267) | [−2.720, 2.259] | 3.237 (2.538) | [−1.750, 8.224] |
| Years of Work Experience (ref: <3 months) | ||||||
| 3~6 (include) | −0.831 (2.320) | [−5.389, 3.728] | −0.359 (1.723) | [−3.745, 3.027] | 2.780 (3.297) | [−3.699, 9.259] |
| 6~12 (include) | −0.911 (2.085) | [−5.008, 3.185] | 1.130 (1.655) | [−2.122, 4.382] | −0.227 (3.131) | [−6.379, 5.926] |
| 12~24 (include) | −0.794 (2.045) | [−4.812, 3.225] | −0.294 (1.628) | [−3.492, 2.905] | 1.329 (3.083) | [−4.729, 7.388] |
| >24 | −0.047 (2.017) | [−4.011, 3.917] | 0.580 (1.583) | [−2.531, 3.691] | 0.824 (3.069) | [−5.208, 6.855] |
| Daily Working Hours (ref: <4 h) | ||||||
| 4~6 (include) h | −0.623 (0.975) | [−2.539, 1.293] | 0.295 (0.603) | [−0.891, 1.481] | −1.584 (1.208) | [−3.958, 0.791] |
| 6~8 (include) h | −1.294 (1.052) | [−3.361, 0.772] | −0.681 (0.681) | [−2.020, 0.658] | −3.011 ** (1.384) | [−5.731, −0.292] |
| >8 h | −0.912 (1.119) | [−3.111, 1.286] | −0.404 (0.771) | [−1.920, 1.111] | −3.408 ** (1.495) | [−6.346, −0.470] |
| Monthly Rest Days (ref: no rest) | ||||||
| 1~2 | 0.283 (0.838) | [−1.363, 1.929] | 0.039 (0.672) | [−1.281, 1.359] | −0.682 (1.120) | [−2.883, 1.518] |
| 3~4 | 1.135 (0.923) | [−0.678, 2.948] | 0.930 (0.739) | [−0.521, 2.381] | −1.038 (1.146) | [−3.291, 1.214] |
| 5~6 | −0.635 (1.113) | [−2.823, 1.553] | −1.310 (0.912) | [−3.101, 0.482] | −0.361 (1.623) | [−3.551, 2.829] |
| 7~8 | −2.399 (1.023) ** | [−4.410, −0.388] | −1.969 (0.777) ** | [−3.497, −0.441] | 1.562 (1.442) | [−1.272, 4.396] |
| Caregiver Burden | 0.331 (0.027) *** | [0.279,0.383] | 0.229 (0.023) *** | [0.184, 0.274] | −0.052 (0.033) | [−0.116, 0.012] |
| Organizational Factors | ||||||
| Type of institution (ref: Residential-based) | ||||||
| Home-based | −2.028 (0.709) *** | [−3.422, −0.634] | −2.120 (0.551) *** | [−3.204, −1.036] | 1.147 (0.862) | [−0.546, 2.841] |
| Training Intensity Index | −0.547 (0.202) *** | [−0.945, −0.149] | −0.436 (0.161) *** | [−0.752, −0.120] | −0.563 (0.319) | [−1.191, 0.065] |
| Societal Factors | ||||||
| LTCI policy recognition | −0.094 (0.048) | [−0.188, 0.001] | −0.113 (0.036) *** | [−0.183, −0.043] | −0.316 (0.059) *** | [−0.431, −0.201] |
| Constant | 22.098 (2.997) *** | [11.900, 32.296] | 19.174 (4.129) *** | [11.059, 27.288] | 37.501 (6.315) *** | [25.092, 49.910] |
| Observations | 494 | 494 | 494 | |||
| ID | Gender | Age | Years of Work Experience | Type of Organization |
|---|---|---|---|---|
| A1 | Female | 57 | 9 | Residential |
| A2 | Female | 55 | 10 | Residential |
| A3 | Female | 58 | 10 | Residential |
| A4 | Male | 53 | 1 | Residential |
| A5 | Male | 62 | 3 | Residential |
| A6 | Female | 59 | 4 | Residential |
| A7 | Female | 55 | 10 | Home-based |
| A8 | Female | 52 | 9 | Home-based |
| A9 | Female | 54 | 9 | Residential |
| A10 | Male | 57 | 3 | Residential |
| A11 | Female | 56 | 6 | Residential |
| A12 | Female | 60 | 2.5 | Home-based |
| A13 | Male | 60 | 1 | Home-based |
| A14 | Female | 46 | 2 | Home-based |
| A15 | Female | — | 2 | Residential |
| Domain | Sub-Theme | Illustrative Quotes from Participant |
|---|---|---|
| Individual | Cognitive adaptation | “Honestly, we’re all from rural areas and don’t have a ton of skills. So, we work here. At first, it’s pretty tiring, but we get used to it. It’s nice to earn some money.” (A9, Female, Residential) |
| Comparative advantage | “I have also worked in factories, where I was told I could not keep up with the younger workers. Given my age, I felt that earning such a wage was acceptable and I should be content with my situation.” (A12, Female, Home-based) | |
| Interpersonal emotional interaction | “Over time, I’ve developed feelings for the older adults. Sometimes we sit in the sun and sing together; seeing them happy lifts my spirits too.” (A6, Female, Residential) | |
| Positive feedback | “Each time I finish the home visit and say I’m about to leave, she’s still smiling—clearly happy—and I feel genuinely gratified.” (A7, Female, Home-based) | |
| Job-related | Heavy caregiving burden | “I’ve been doing this job for almost ten years. Honestly, I feel like my personality has been worn down over time.” (A9, Female, Residential) |
| “Most of the older adults are completely dependent and need to be turned regularly to prevent bedsores… I’m caring for five people now, and sometimes I also have to bathe them. By the end of the day, I’m really tired—running up and down the stairs wears me out.” (A14, Female, Residential) | ||
| Organizational | Type of organization-specific work environment trade-offs | “I can visit different households and talk to different people; the environment feels fresher. In the nursing home, it’s the same place every day, and sometimes it feels a bit depressing.” (A14, Female, Home-based) |
| “I live and work in the nursing home now. I’ve never done the kind of home-based care. I don’t like running around—it’s tiring to go back and forth, and when it rains or gets hot, it’s really inconvenient.” (A2, Female, Residential) | ||
| The training boosted confidence and efficiency | “I have no experience, but there is training related to caring for older adults, for example, how to turn an elderly person more quickly and easily…. I work better and faster after this, much better than when I didn’t know” (A1, Female, Residential) | |
| Societal | Policy recognition inspires professional value | “I feel this (LTC) has been getting better and better… it lightens the burden on older adults’ families… they can live longer, and we feel that what we do is meaningful.” (A8, Female, Home-based) |
| “… I told myself that this really is a noble profession. Only with that belief can you do this not-so-easy job well… It’s a good policy—it has given us job opportunities and reduced the burden on older adults and their families.” (A10, Male, Residential) |
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2026 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license.
Share and Cite
Tan, G.; Chao, J. Burnout and Its Associated Factors Among Long-Term Care Workers: A Mixed-Methods Study Based on the Social–Ecological Framework. Behav. Sci. 2026, 16, 419. https://doi.org/10.3390/bs16030419
Tan G, Chao J. Burnout and Its Associated Factors Among Long-Term Care Workers: A Mixed-Methods Study Based on the Social–Ecological Framework. Behavioral Sciences. 2026; 16(3):419. https://doi.org/10.3390/bs16030419
Chicago/Turabian StyleTan, Gangrui, and Jianqian Chao. 2026. "Burnout and Its Associated Factors Among Long-Term Care Workers: A Mixed-Methods Study Based on the Social–Ecological Framework" Behavioral Sciences 16, no. 3: 419. https://doi.org/10.3390/bs16030419
APA StyleTan, G., & Chao, J. (2026). Burnout and Its Associated Factors Among Long-Term Care Workers: A Mixed-Methods Study Based on the Social–Ecological Framework. Behavioral Sciences, 16(3), 419. https://doi.org/10.3390/bs16030419






