Parent-Mediated vs. Staff-Mediated Behavioral Models in Families of Autistic Children: A Comparative Study on Parental Stress, Co-Parenting, and Quality of Life
Abstract
1. Introduction
1.1. Parental Stress and Quality of Life in Families of Children with ASD
1.2. Co-Parenting in Families of Children with ASD
1.3. Scope and Hypotheses
2. Materials and Methods
2.1. Behavioral Models
2.2. Instruments
2.3. Data Analysis and Preliminary Statistics
3. Results
3.1. Correlational Analyses
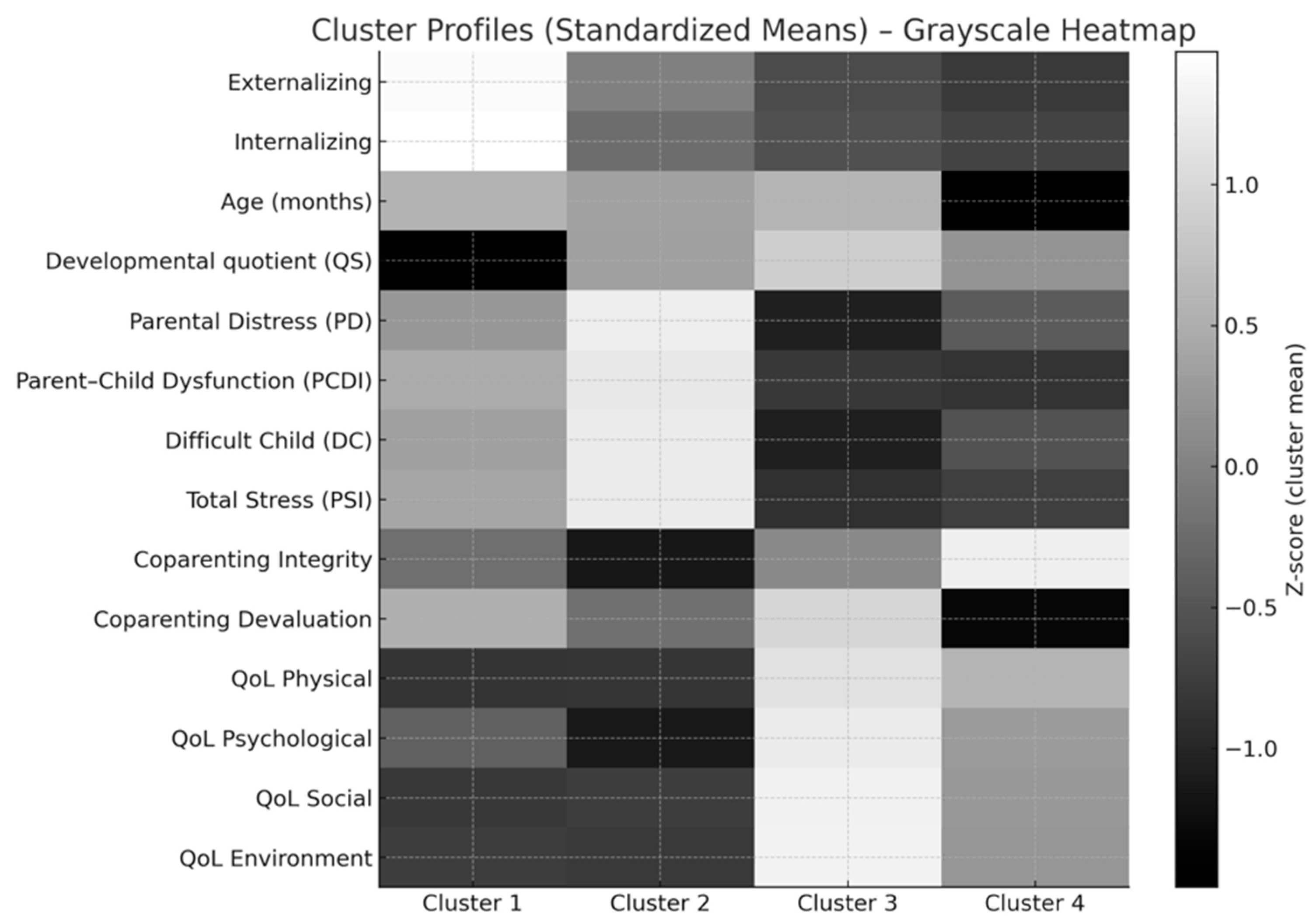
3.2. Cluster-Based Family Profiles
4. Discussion
Limitations and Future Directions
5. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Acknowledgments
Conflicts of Interest
Appendix A
| Outcome | F (Model) | p (Model) | F (Age) | p (Age) | η2p |
|---|---|---|---|---|---|
| Parent stress indexes | |||||
| Parental Distress (PD) | 0.12 | 0.731 | 1.64 | 0.204 | 0.001 |
| P-C Difficult Inter. (PCDI) | 5.08 | 0.026 | 9.76 | 0.002 | 0.052 |
| Difficult Child (DC) | 3.21 | 0.076 | 1.62 | 0.207 | 0.034 |
| Coparenting scales | |||||
| Integrity | 1.10 | 0.298 | 0.52 | 0.471 | 0.012 |
| Devaluation | 138.17 | <0.001 | 0.17 | 0.679 | 0.606 |
| Conflict | 0.62 | 0.435 | 3.44 | 0.067 | 0.007 |
| Reproach * | 0.86 | 0.357 | 0.29 | 0.590 | 0.009 |
| Quality of Life domains | |||||
| Physical | 0.12 | 0.734 | 0.84 | 0.362 | 0.001 |
| Psychological | 0.31 | 0.577 | 0.20 | 0.656 | 0.003 |
| Social * | 3.20 | 0.077 | 5.54 | 0.021 | 0.034 |
| Environment | 2.98 | 0.087 | 0.10 | 0.753 | 0.031 |
References
- Abidin, R. R. (1990). The parenting stress index-short form. Test manual. Pediatric Psychology Press. [Google Scholar]
- Abidin, R. R. (1992). The determinants of parenting behavior. Journal of Clinical Child Psychology, 21(4), 407–412. [Google Scholar] [CrossRef]
- Adams, D., Stainsby, M., & Paynter, J. (2021). Autistic mothers of autistic children: A preliminary study in an under-researched area. Autism in Adulthood, 3(4), 339–346. [Google Scholar] [CrossRef] [PubMed]
- APA. (2022). Diagnostic and statistical manual of mental disorders (5th ed.). Text Revision (DSM-5-TR). American Psychiatric Association. [Google Scholar]
- Barklı, A., & Doğan, A. (2025). Raising a child with Autism Spectrum Disorder: Examining parental factors. Current Approaches in Psychiatry, 17(2), 197–210. [Google Scholar] [CrossRef]
- Barroso, N. E., Mendez, L., Graziano, P. A., & Bagner, D. M. (2018). Parenting stress through the lens of different clinical groups: A systematic review & meta-analysis. Journal of Abnormal Child Psychology, 46(3), 449–461. [Google Scholar] [CrossRef]
- Bauminger, N., Solomon, M., & Rogers, S. J. (2010). Externalizing and internalizing behaviors in ASD. Autism Research, 3(3), 101–112. [Google Scholar] [CrossRef]
- Bitsika, V., & Sharpley, C. (2004). Stress, anxiety, and depression among parents of children with autism spectrum disorder. Journal of Psychologists and Counsellors in Schools, 14(2), 151–161. [Google Scholar] [CrossRef]
- Catalano, D., Holloway, L., & Mpofu, E. (2018). Mental health interventions for parent carers of children with autistic spectrum disorder: Practice guidelines from a critical interpretive synthesis (CIS) systematic review. International Journal of Environmental Research and Public Health, 15(2), 341. [Google Scholar] [CrossRef]
- Contreras, B. P., Hoffmann, A. N., & Slocum, T. A. (2022). Ethical behavior analysis: Evidence-based practice as a framework for ethical decision making. Behavior Analysis in Practice, 15(2), 619–634. [Google Scholar] [CrossRef]
- Crnic, K., & Low, C. (2002). Everyday stresses and parenting. In M. H. Bornstein (Ed.), Handbook of parenting, vol. 5: Practical issues in parenting (2nd ed., pp. 243–267). Lawrence Erlbaum Associates. [Google Scholar]
- Crowell, J. A., Keluskar, J., & Gorecki, A. (2019). Parenting behavior and the development of children with autism spectrum disorder. Comprehensive Psychiatry, 90, 21–29. [Google Scholar] [CrossRef]
- Davis, N. O., & Carter, A. S. (2008). Parenting stress in mothers and fathers of toddlers with autism spectrum disorders: Associations with child characteristics. Journal of Autism and Developmental Disorders, 38, 1278–1291. [Google Scholar] [CrossRef]
- Dawson-Squibb, J. J., Davids, E. L., Harrison, A. J., Molony, M. A., & de Vries, P. J. (2020). Parent education and training for autism spectrum disorders: Scoping the evidence. Autism, 24(1), 7–25. [Google Scholar] [CrossRef] [PubMed]
- Dillenburger, K. (2026). It takes a village to raise a child: Parent-mediated intervention to support profoundly autistic children. In Handbook of treatments for autism spectrum disorder (pp. 167–190). Springer Nature Switzerland. [Google Scholar]
- Doherty, M. (2025). My autistic meltdown: The impact of autistic sensory needs. The Lancet, 405(10487), 1332–1333. [Google Scholar] [CrossRef]
- Downes, N., & Cappe, E. (2021). Coparenting a child on the autism spectrum: A systematic review and call for research. Journal of Child and Family Studies, 30, 388–402. [Google Scholar] [CrossRef]
- Dunst, C. J. (2022). Systematic review and meta-analysis of family needs studies: Relationships with parent, family and child functioning. European Journal of Psychology and Educational Research, 5(1), 11–32. [Google Scholar] [CrossRef]
- Esposito, M., Sloan, J., Tancredi, A., Gerardi, G., Postiglione, P., Fotia, F., Napoli, E., Mazzone, L., Valeri, G., & Vicari, S. (2017). Using tablet applications for children with autism to increase their cognitive and social skills. Journal of Special Education Technology, 32(4), 199–209. [Google Scholar] [CrossRef]
- Falk, N. H., Norris, K., & Quinn, M. G. (2014). The factors predicting stress, anxiety and depression in the parents of children with autism. Journal of Autism and Developmental Disorders, 44, 3185–3203. [Google Scholar] [CrossRef]
- Fava, L., Strauss, K., Valeri, G., D’Elia, L., Arima, S., & Vicari, S. (2011). The effectiveness of a cross-setting complementary staff- and parent-mediated early intensive behavioral intervention for young children with ASD. Research in Autism Spectrum Disorders, 5(4), 1479–1492. [Google Scholar] [CrossRef]
- Feinberg, M. E., & Kan, M. L. (2008). Establishing family foundations: Intervention effects on coparenting, parent/infant well-being, and parent-child relations. Journal of Family Psychology, 22(2), 253–263. [Google Scholar] [CrossRef] [PubMed]
- Firth, I., & Dryer, R. (2013). The predictors of distress in parents of children with autism spectrum disorder. Journal of Intellectual and Developmental Disability, 38(2), 163–171. [Google Scholar] [CrossRef] [PubMed]
- Greenlee, J. L., Winter, M. A., & Diehl, J. J. (2018). Family level processes associated with outcomes for individuals with autism spectrum disorder: A scoping review. Research in Autism Spectrum Disorders, 53, 41–52. [Google Scholar] [CrossRef]
- Guarino, A., Di Blasio, P., D’Alessio, M., Camisasca, E., & Serantoni, G. (2008). Parenting stress index—Short form: Adattamento italiano. Organizzazioni Speciali. Available online: https://publicatt.unicatt.it/handle/10807/69068 (accessed on 1 September 2025).
- Ha, C. T. M., Nguyen, H. T., Nguyen, A. H. V., & Thien, G. P. T. (2024). Psychological stress in parents of children with autism spectrum disorder. National Journal of Community Medicine, 15(06), 451–460. [Google Scholar] [CrossRef]
- Hastings, R. P., & Brown, T. (2002). Behavior problems of children with autism, parental self-efficacy, and mental health. American Journal on Mental Retardation, 107(3), 222–232. [Google Scholar] [CrossRef]
- He, B., Wongpakaran, T., Wongpakaran, N., & Wedding, D. (2022). Marital satisfaction and perceived family support in families of children with autistic spectrum disorder: Dyadic analysis. Healthcare, 10(7), 1227. [Google Scholar] [CrossRef] [PubMed]
- Ilić, I., Šipetić-Grujičić, S., Grujičić, J., Živanović Mačužić, I., Kocić, S., & Ilić, M. (2019). Psychometric properties of the world health organization’s quality of life (WHOQOL-BREF) questionnaire in medical students. Medicina, 55(12), 772. [Google Scholar] [CrossRef]
- Jones, T. L., & Prinz, R. J. (2005). Potential roles of parental self-efficacy in parent and child adjustment: A review. Clinical Psychology Review, 25(3), 341–363. [Google Scholar] [CrossRef]
- Kanne, S. M., & Mazurek, M. O. (2011). Aggression in children and adolescents with ASD: Prevalence and risk factors. Journal of Autism and Developmental Disorders, 41, 926–937. [Google Scholar] [CrossRef] [PubMed]
- Karst, J. S., & Van Hecke, A. V. (2012). Parent and family impact of autism spectrum disorders: A review and proposed model for intervention evaluation. Clinical Child and Family Psychology Review, 15(3), 247–277. [Google Scholar] [CrossRef]
- Kiami, S. R., & Goodgold, S. (2017). Support needs and coping strategies as predictors of stress level among mothers of children with autism spectrum disorder. Autism Research and Treatment, 2017, 8685950. [Google Scholar] [CrossRef]
- Kostiukow, A., Strzelecki, W., Poniewierski, P., & Samborski, W. (2019). The estimation of the functioning of families with ASD children. AIMS Public Health, 6(4), 587–599. [Google Scholar] [CrossRef]
- Kuhn, J. C., & Carter, A. S. (2006). Maternal self-efficacy and associated parenting cognitions among mothers of children with autism. American Journal of Orthopsychiatry, 76(4), 564–575. [Google Scholar] [CrossRef]
- Lebersfeld, J. B., Swanson, M., Clesi, C. D., & O’Kelley, S. E. (2021). Systematic review and meta-analysis of the clinical utility of the ADOS-2 and the ADI-R in diagnosing autism spectrum disorders in children. Journal of Autism and Developmental Disorders, 51(11), 4101–4114. [Google Scholar] [CrossRef] [PubMed]
- Leonardi, E., Cerasa, A., Servidio, R., Costabile, A., Famà, F. I., Carrozza, C., Spadaro, L., Scifo, R., Baieli, S., Aiello, S., Marino, F., Tartarisco, G., Vagni, D., Pioggia, G., & Ruta, L. (2021). The route of stress in parents of young children with and without autism: A path-analysis study. International Journal of Environmental Research and Public Health, 18(20), 10887. [Google Scholar] [CrossRef] [PubMed]
- Mahan, S., & Matson, J. L. (2011). Convergent and discriminant validity of the Autism Spectrum Disorder-Problem Behavior for Children (ASD-PBC) against the Behavioral Assessment System for Children (BASC-2). Research in Autism Spectrum Disorders, 5(1), 222–229. [Google Scholar] [CrossRef]
- Mak, M. C. K., Yin, L., Li, M., Cheung, R. Y. H., & Oon, P. T. (2020). The relation between parenting stress and child behavior problems: Negative parenting styles as mediator. Journal of Child and Family Studies, 29(11), 2993–3003. [Google Scholar] [CrossRef]
- Mazzoni, S., Veronesi, C., Vismara, L., Laghi, F., & Philipp, D. (2018). Family coordination in families who have a child with Autism Spectrum Disorder. Journal of Child and Family Studies, 27, 3107–3116. [Google Scholar] [CrossRef]
- McHale, J., & Dickstein, S. (2019). The interpersonal context of early childhood development: A systemic approach to infant-family assessment. In A. Carter, & R. DelCarmen Wiggins (Eds.), Oxford handbook of infant, toddler, and preschool mental health assessment (2nd ed.). Oxford University Press. [Google Scholar]
- McHale, J., Tissot, H., Mazzoni, S., Hedenbro, M., Salman-Engin, S., Phillip, D., Darwiche, J., Keren, M., Coates, E., Mensi, M., Corboz-Warnery, A., & Fivaz-Depeursinge, E. (2023). Framing the work: A coparenting model for guiding infant mental health engagement with family. Infant Mental Health Journal, 44, 638–650. [Google Scholar] [CrossRef]
- McHale, J. P. (1997). Overt and covert coparenting processes in the family. Family Process, 36(2), 183–201. [Google Scholar] [CrossRef]
- McStay, R. L., Trembath, D., & Dissanayake, C. (2014). Stress and family quality of life in parents of children with autism spectrum disorder: Parent gender and the double ABCX model. Journal of Autism and Developmental Disorders, 44(12), 3101–3118. [Google Scholar] [CrossRef]
- Meirsschaut, M., Roeyers, H., & Warreyn, P. (2010). Parenting in families with a child with autism spectrum disorder and a typically developing child: Mothers’ experiences and cognitions. Research in Autism Spectrum Disorders, 4(4), 661–669. [Google Scholar] [CrossRef]
- Ni’matuzahroh, Suen, M.-W., Ningrum, V., Widayat, Yuniardi, M. S., Hasanati, N., & Wang, J.-H. (2022). The association between parenting stress, positive reappraisal coping, and quality of life in parents with Autism Spectrum Disorder (ASD) children: A systematic review. Healthcare, 10(1), 52. [Google Scholar] [CrossRef]
- Oisakede, E. O., & Cinnamond, J. (2026). A systematic review and meta-synthesis of the lived experiences of parenting a child with an autism spectrum disorder. Research in Autism, 131, 202800. [Google Scholar] [CrossRef]
- Osborne, L. A., McHugh, L., Saunders, J., & Reed, P. (2008). Parenting stress reduces the effectiveness of early teaching interventions for autistic spectrum disorders. Journal of Autism and Developmental Disorders, 38(6), 1092–1103. [Google Scholar] [CrossRef]
- Ozturk, Y., Riccadonna, S., & Venuti, P. (2014). Parenting dimensions in mothers and fathers of children with Autism Spectrum Disorders. Research in Autism Spectrum Disorders, 8(10), 1295–1306. [Google Scholar] [CrossRef]
- Partington, J. W., Bailey, A., & Partington, S. W. (2018). A pilot study examining the test–retest and internal consistency reliability of the ABLLS-R. Journal of Psychoeducational Assessment, 36(4), 405–410. [Google Scholar] [CrossRef]
- Phetrasuwan, S., & Shandor Miles, M. (2009). Parenting stress in mothers of children with autism spectrum disorders. Journal for Specialists in Pediatric Nursing, 14(3), 157–165. [Google Scholar] [CrossRef]
- Pohl, A. L., Crockford, S. K., Blakemore, M., Allison, C., & Baron-Cohen, S. (2020). A comparative study of autistic and non-autistic women’s experience of motherhood. Molecular Autism, 11(1), 3. [Google Scholar] [CrossRef]
- Rodriguez, G., Hartley, S. L., & Bolt, D. (2019). Transactional relations between parenting stress and child autism symptoms and behavior problems. Journal of Autism and Developmental Disorders, 49(5), 1887–1898. [Google Scholar] [CrossRef]
- Saccà, A., Cavallini, F., & Cavallini, M. C. (2019). Parents of children with autism spectrum disorder: A systematic review. Journal of Clinical and Developmental Psychology, 1(3), 30–44. [Google Scholar] [CrossRef]
- Sikora, D., Moran, E., Orlich, F., Hall, T. A., Kovacs, E. A., Delahaye, J., Clemons, T., & Kuhlthau, K. (2013). The relationship between family functioning and behavior problems in children with autism spectrum disorders. Research in Autism Spectrum Disorders, 7, 307–315. [Google Scholar] [CrossRef]
- Siller, M., & Morgan, L. (2018). Handbook of parent-implemented interventions for very young children with autism. Springer International Publishing AG. [Google Scholar] [CrossRef]
- Sim, A., Cordier, R., Vaz, S., & Falkmer, T. (2016). Relationship satisfaction in couples raising a child with autism spectrum disorder: A systematic review of the literature. Research in Autism Spectrum Disorders, 31, 30–52. [Google Scholar] [CrossRef]
- Skevington, S. M., Lotfy, M., & O’Connell, K. A. (2004). The World Health Organization’s WHOQOL-BREF quality of life assessment: Psychometric properties and results of the international field trial. A report from the WHOQOL group. Quality of life Research, 13(2), 299–310. [Google Scholar] [CrossRef] [PubMed]
- Slocum, T. A., Detrich, R., Wilczynski, S. M., Spencer, T. D., Lewis, T., & Wolfe, K. (2014). The evidence-based practice of applied behavior analysis. The Behavior Analyst, 37(1), 41–56. [Google Scholar] [CrossRef]
- Sofronoff, K., & Farbotko, M. (2002). The effectiveness of parent management training to increase self-efficacy in parents of children with Asperger syndrome. Autism, 6, 271–286. [Google Scholar] [CrossRef]
- Strauss, K., Servadio, M., Valeri, G., Casula, L., Vicari, S., & Fava, L. (2024). Association between child behavioural problems and parenting stress in autism spectrum disorders: The role of parenting self-efficacy. International Journal of Developmental Disabilities, 70(1), 49–58. [Google Scholar] [CrossRef]
- Suvarna, V., Farrell, L., Adams, D., Emerson, L. M., & Paynter, J. (2025). Differing relationships between parenting stress, parenting practices and externalising behaviours in autistic children. Autism, 29(3), 711–725. [Google Scholar] [CrossRef]
- Taddei, M., Bulgheroni, S., Toffalini, E., Pantaleoni, C., & Lanfranchi, S. (2023). Developmental profiles of young children with autism spectrum disorder and global developmental delay: A study with the Griffiths III scales. Autism Research, 16(7), 1344–1359. [Google Scholar] [CrossRef]
- Ten Hoopen, L. W., de Nijs, P. F., Slappendel, G., van der Ende, J., Bastiaansen, D., Greaves-Lord, K., Hakkaart-van Roijen, L., & Hillegers, M. H. (2023). Associations between autism traits and family functioning over time in autistic and non-autistic children. Autism, 27(7), 2035–2047. [Google Scholar] [CrossRef]
- Thullen, M., & Bonsall, A. (2017). Co-parenting quality, parenting stress, and feeding challenges in families with a child diagnosed with autism spectrum disorder. Journal of Autism and Developmental Disorders, 47, 878–886. [Google Scholar] [CrossRef] [PubMed]
- Vasilopoulou, E., & Nisbet, J. (2016). The quality of life of parents of children with autism spectrum disorder: A systematic review. Research in Autism Spectrum Disorders, 23, 36–49. [Google Scholar] [CrossRef]
- Walton, K. M., & Tiede, G. (2020). Brief report: Does “healthy” family functioning look different for families who have a child with autism? Research in Autism Spectrum Disorders, 72, 101527. [Google Scholar] [CrossRef]
- Wright, N., Courchesne, V., Pickles, A., Bedford, R., Duku, E., Kerns, C. M., Bennett, T., Georgiades, S., Hill, J., Richard, A., Sharp, H., Smith, I. M., Vaillancourt, T., Zaidman-Zait, A., Zwaigenbaum, L., Szatmari, P., Elsabbagh, M., & Pathways Team. (2023). A longitudinal comparison of emotional, behavioral and attention problems in autistic and typically developing children. Psychological Medicine, 53(16), 7707–7719. [Google Scholar] [CrossRef] [PubMed]
- Zaidman-Zait, A., Mirenda, P., Duku, E., Vaillancourt, T., Smith, I. M., Szatmari, P., Bryson, S., Fombonne, E., Volden, J., Waddell, C., Zwaigenbaum, L., Georgiades, S., Bennett, T., Elsabaggh, M., & Thompson, A. (2017). Impact of personal and social resources on parenting stress in mothers of children with autism spectrum disorder. Autism, 21(2), 155–166. [Google Scholar] [CrossRef] [PubMed]
- Zhang, J., Wang, L., Liu, S., Yang, Y., Fan, J., & Zhang, Y. (2025). The relationship between parenting stress and parenting burnout in parents of children with autism: The chain mediating role of social support and coping strategies. International Journal of Mental Health Promotion, 27(3), 287–302. [Google Scholar] [CrossRef]
| Variable | Model 1 | Model 2 | Test | Statistic | p |
|---|---|---|---|---|---|
| Child characteristics | |||||
| Age child (months) | 53.68 (12.26) | 75.00 (12.25) | Welch t-test | t = −8.61 | <0.001 |
| Sex child (males/females) | 44/6 | 44/4 | Chi-square | χ2 = 0.07 | 0.790 |
| Number of siblings | 0.80 (0.57) | 0.79 (0.71) | Welch t-test | t = 0.06 | 0.949 |
| Parent characteristics | |||||
| Age parent | 40.10 (5.75) | 38.88 (3.87) | Welch t-test | t = 1.24 | 0.218 |
| Sex parent (males/females) | 25/25 | 24/24 | Chi-square | χ2 = 0.00 | 1.00 |
| Education (ordinal) | 2.22 (0.68) | 2.25 (0.53) | Mann–Whitney U | U = 1195 | 0.971 |
| Marital status (married/no) | 40/10 | 40/8 | Chi-square | χ2 = 0.03 | 0.869 |
| Cognitive profile | |||||
| Developmental Q. | 60.29 (22.70) | 67.27 (16.64) | Welch t-test | t = −1.69 | 0.094 |
| Problem Behaviors | |||||
| Externalizing | 2.32 (2.39) | 2.92 (2.64) | Welch t-test | t = −1.17 | 0.244 |
| Internalizing | 5.32 (3.62) | 5.63 (3.80) | t = −0.41 | 0.686 | |
| Parent stress | |||||
| Parental Distress (PD) | 29.68 (8.64) | 30.91 (9.87) | Welch t-test | t = −0.64 | 0.521 |
| Par. Child Dif. Inter. (P-CDI) | 25.90 (6.30) | 25.60 (4.40) | t = 0.27 | 0.787 | |
| Difficult Child (DC) | 32.06 (8.56) | 29.91 (7.88) | t = 1.27 | 0.208 | |
| Co-parenting Dimensions | |||||
| Family Integrity | 5.06 (1.36) | 4.57 (0.66) | Welch t-test | t = 2.25 | 0.027 |
| Devaluation | 2.07 (0.84) | 5.25 (0.99) | t = −16.54 | <0.001 | |
| Conflict | 2.85 (1.40) | 3.04 (1.29) | t = −0.68 | 0.496 | |
| Reproach/Discipline | 3.93 (0.92) | 3.79 (0.81) | t = 0.77 | 0.441 | |
| Quality of Life (QoL) | |||||
| Physical | 3.63 (0.47) | 3.49 (0.63) | t = 1.22 | 0.224 | |
| Psychological | 3.32 (0.48) | 3.36 (0.60) | Welch t-test | t = −0.35 | 0.726 |
| Social | 3.25 (0.57) | 3.30 (0.73) | t = −0.31 | 0.752 | |
| Environment | 2.78 (0.59) | 3.03 (0.61) | t = −2.02 | 0.047 |
| Predictors | Model | PD | P-CDI | DC | T. Stress | Integrity | Devaluation | Conflict | Physical | Psychol. | Environment |
|---|---|---|---|---|---|---|---|---|---|---|---|
| Age child | M1 | −0.04 | 0.36 ** | 0.04 | 0.17 | 0.03 | 0.23 | −0.02 | −0.03 | 0.04 | −0.06 |
| Age child | M2 | 0.30 * | 0.24 | 0.26 | 0.31 * | −0.38 * | −0.16 | 0.49 *** | −0.04 | −0.15 | −0.01 |
| Dev. Quotient | M1 | 0.04 | −0.37 * | −0.11 | −0.19 | −0.05 | −0.22 | 0.06 | −0.04 | −0.14 | −0.07 |
| Dev. Quotient | M2 | −0.12 | −0.16 | −0.07 | −0.13 | −0.10 | −0.43 ** | −0.15 | 0.21 | 0.23 | 0.34 * |
| Externalizing | M1 | 0.04 | 0.54 *** | 0.34 * | 0.43 ** | −0.14 | 0.05 | −0.11 | −0.14 | −0.02 | −0.20 |
| Externalizing | M2 | 0.32 * | 0.29 | 0.39 ** | 0.29 | −0.14 | 0.04 | 0.04 | −0.54 *** | −0.36 * | −0.49 *** |
| Internalizing | M1 | 0.14 | 0.34 * | 0.32 * | 0.25 | −0.01 | 0.17 | 0.01 | −0.03 | 0.07 | −0.02 |
| Internalizing | M2 | 0.19 | 0.15 | 0.30 | 0.23 | −0.17 | 0.05 | −0.20 | −0.47 ** | −0.34 * | −0.45 ** |
| Variable | Cluster 1 (n = 16) | Cluster 2 (n = 17) | Cluster 3 (n = 22) | Cluster 4 (n = 23) |
|---|---|---|---|---|
| Externalizing Behaviors | 6.03 (3.2) | 1.41 (1.6) | 2.46 (2.6) | 1.41 (1.6) |
| Internalizing Behaviors | 10.31 (3.4) | 4.82 (2.9) | 4.82 (3.1) | 3.73 (2.4) |
| Age child | 63.0 (21.4) | 54.8 (17.1) | 79.1 (28.2) | 54.5 (16.6) |
| Developmental quotient | 50.5 (18.2) | 68.4 (21.0) | 61.8 (17.3) | 66.1 (12.7) |
| Sex child (% male) | 87% | 76% | 81% | 70% |
| PD—Parental Distress | 39.6 (8.1) | 27.0 (5.1) | 38.8 (7.0) | 33.0 (6.1) |
| PCDI—Dysfunctional Interaction | 29.1 (6.3) | 20.6 (3.4) | 30.0 (6.0) | 23.3 (4.6) |
| DC—Difficult Child | 40.0 (7.2) | 20.2 (5.8) | 36.4 (8.0) | 28.9 (6.0) |
| Total Stress (PSI) | 108.8 (13.4) | 67.4 (11.6) | 105.1 (12.7) | 85.1 (10.8) |
| Coparenting—Integrity | 3.87 (1.1) | 5.56 (0.9) | 4.57 (1.0) | 5.18 (0.8) |
| Coparenting—Devaluation | 3.98 (0.9) | 3.76 (0.8) | 4.86 (1.0) | 2.09 (0.8) |
| QoL Physical | 45.5 (11.2) | 76.0 (13.3) | 64.4 (13.0) | 63.0 (10.5) |
| QoL Psychological | 46.0 (9.3) | 69.6 (11.4) | 57.3 (14.8) | 56.2 (10.4) |
| QoL Social | 43.2 (13.8) | 70.7 (18.2) | 55.6 (18.4) | 55.4 (12.0) |
| QoL Environment | 35.1 (10.9) | 62.1 (12.4) | 48.6 (14.1) | 47.0 (8.8) |
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2026 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license.
Share and Cite
Esposito, M.; Trasolini, M.; Fadda, R.; Lucarelli, L.; Caputi, M. Parent-Mediated vs. Staff-Mediated Behavioral Models in Families of Autistic Children: A Comparative Study on Parental Stress, Co-Parenting, and Quality of Life. Behav. Sci. 2026, 16, 350. https://doi.org/10.3390/bs16030350
Esposito M, Trasolini M, Fadda R, Lucarelli L, Caputi M. Parent-Mediated vs. Staff-Mediated Behavioral Models in Families of Autistic Children: A Comparative Study on Parental Stress, Co-Parenting, and Quality of Life. Behavioral Sciences. 2026; 16(3):350. https://doi.org/10.3390/bs16030350
Chicago/Turabian StyleEsposito, Marco, Monia Trasolini, Roberta Fadda, Loredana Lucarelli, and Marcella Caputi. 2026. "Parent-Mediated vs. Staff-Mediated Behavioral Models in Families of Autistic Children: A Comparative Study on Parental Stress, Co-Parenting, and Quality of Life" Behavioral Sciences 16, no. 3: 350. https://doi.org/10.3390/bs16030350
APA StyleEsposito, M., Trasolini, M., Fadda, R., Lucarelli, L., & Caputi, M. (2026). Parent-Mediated vs. Staff-Mediated Behavioral Models in Families of Autistic Children: A Comparative Study on Parental Stress, Co-Parenting, and Quality of Life. Behavioral Sciences, 16(3), 350. https://doi.org/10.3390/bs16030350






