Preliminary Data on Behavioral Profiles of Youth with Neurodevelopmental Disorders and Trauma
Abstract
1. Introduction
Trauma and Neurodevelopmental Disorders
2. Methods
2.1. Participants
Diagnosis
2.2. Procedures
2.2.1. Review of Medical Records
2.2.2. Behavioral Assessment
2.2.3. Behavioral Treatment Details
2.2.4. Behavioral Reduction Data
2.2.5. PEARLS
2.2.6. Associations Between ACEs and Problem Behavior Reduction
2.2.7. Reliability
2.3. Power Analysis
2.4. Data Analysis
3. Results
3.1. Demographic Information
3.2. Target Behaviors Identified Through Behavioral Assessment
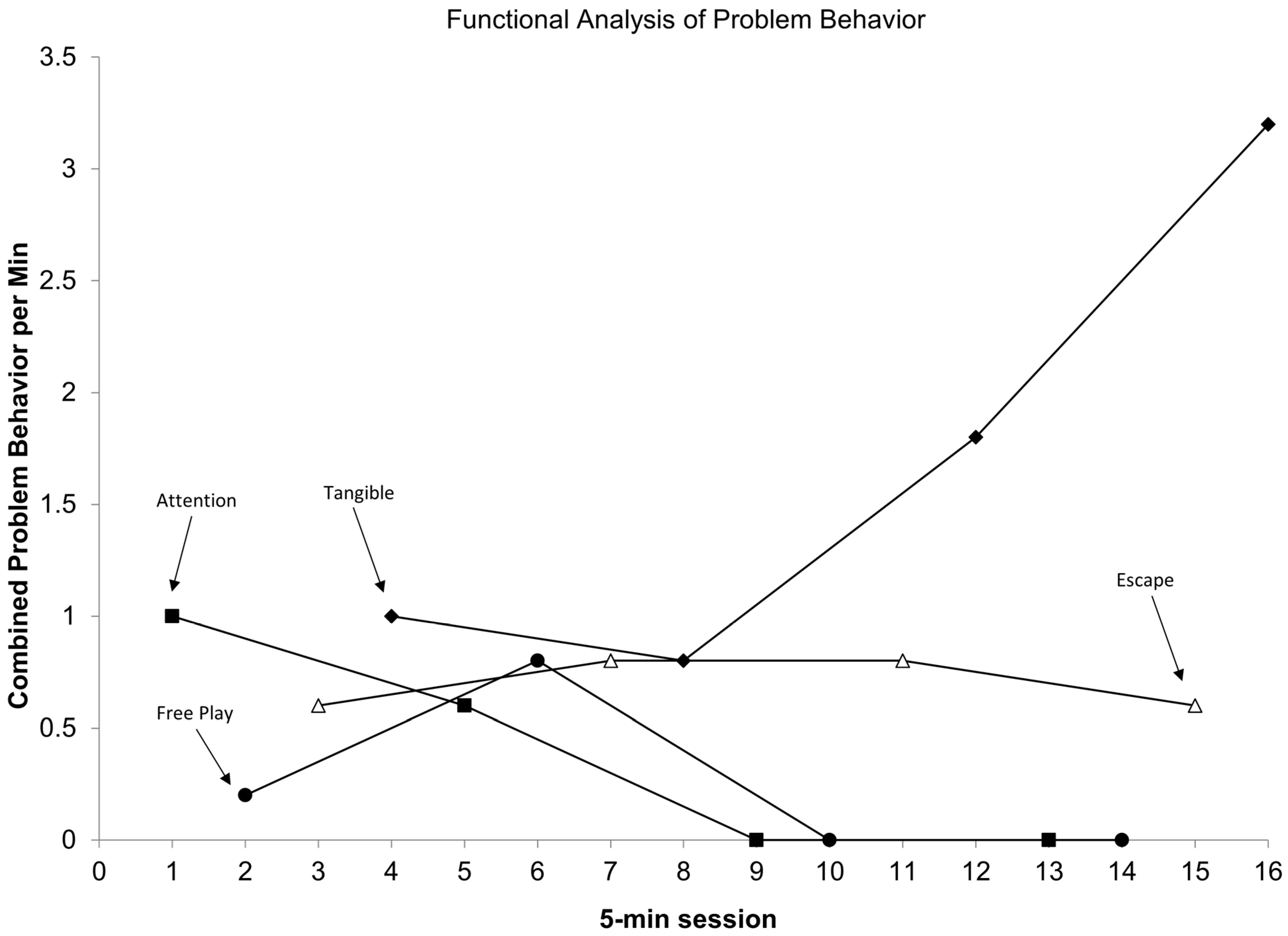
3.3. Design and Response to Individualized Intervention
3.4. PEARLS
3.5. ACEs and Reduction in Problem Behavior
4. Discussion
5. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Conflicts of Interest
| 1 | This manuscript alternates between person-first (e.g., “individuals with autism”) language and identity-first (e.g., “autistic individuals”) language to reflect the diversity of preferences within the disability community and the scholarly literature. This choice was made to respect both perspectives and acknowledge the evolving nature of inclusive language. |
References
- American Psychiatric Association. (2022). Diagnostic and statistical manual of mental disorders (5th ed., text rev.). American Psychiatric Association. [Google Scholar] [CrossRef]
- Anda, R. F., Felitti, V. J., Bremner, J. D., Walker, J. D., Whitfield, C., Perry, B. D., Dube, S. R., & Giles, W. H. (2006). The enduring effects of abuse and related adverse experiences in childhood. A convergence of evidence from neurobiology and epidemiology. European Archives of Psychiatry and Clinical Neuroscience, 256(3), 174–186. [Google Scholar] [CrossRef]
- Bader, K., Schaefer, V., Schenkel, M., Nissen, L., & Schwander, J. (2007). Adverse childhood experiences associated with sleep in primary insomnia. Journal of Sleep Research, 16(3), 285–296. [Google Scholar] [CrossRef] [PubMed]
- Baldwin, J. R., Caspi, A., Meehan, A. J., Ambler, A., Arseneault, L., Fisher, H. L., Harrington, H., Matthews, T., Odgers, C. L., Poulton, R., Ramrakha, S., Moffitt, T. E., & Danese, A. (2021). Population vs individual prediction of poor health from results of adverse childhood experiences screening. JAMA Pediatrics, 175(4), 385–393. [Google Scholar] [CrossRef]
- Beavers, G. A., Iwata, B. A., & Lerman, D. C. (2013). Thirty years of research on the functional analysis of problem behavior. Journal of Applied Behavior Analysis, 46(1), 1–21. [Google Scholar] [CrossRef] [PubMed]
- Berke, D. S., Kline, N. K., Wachen, J. S., McLean, C. P., Yarvis, J. S., Mintz, J., Young-McCaughan, S., Peterson, A. L., Foa, E., Resick, P. A., Litz, B. T., & Strong Star Consortium. (2019). Predictors of attendance and dropout in three randomized controlled trials of PTSD treatment for active duty service members. Behaviour Research and Therapy, 118, 7–17. [Google Scholar] [CrossRef] [PubMed]
- Birmaher, B., Khetarpal, S., Brent, D., Cully, M., Balach, L., Kaufman, J., & Neer, S. M. (1997). The screen for child anxiety related emotional disorders (SCARED): Scale construction and psychometric characteristics. Journal of the American Academy of Child & Adolescent Psychiatry, 36(4), 545–553. [Google Scholar] [CrossRef]
- Briere, J. N., & Scott, C. (2006). What is trauma. In Principles of trauma therapy: A guide to symptoms, evaluation, and treatment (pp. 3–11). SAGE Publications, Inc. [Google Scholar]
- Carruthers, S., Pickles, A., Slonims, V., Howlin, P., & Charman, T. (2020). Beyond intervention into daily life: A systematic review of generalisation following social communication interventions for young children with autism. Autism Research, 13(4), 506–522. [Google Scholar] [CrossRef]
- Chorpita, B. F., Yim, L., Moffitt, C., Umemoto, L. A., & Francis, S. E. (2000). Revised child anxiety and depression scale (RCADS) [Database record]. APA PsycTests. [Google Scholar] [CrossRef]
- Christoffersen, M. N., & Thorup, A. A. E. (2024). Post-traumatic stress disorder in school-age children: A nationwide prospective birth cohort study. Journal of Child & Adolescent Trauma, 17(2), 139–157. [Google Scholar] [CrossRef]
- Cook, S., & Hole, R. (2021). Trauma, intellectual and/or developmental disability, and multiple, complex needs: A scoping review of the literature. Research in Developmental Disabilities, 115, 103939. [Google Scholar] [CrossRef]
- De Bellis, M. D. (2001). Developmental traumatology: The psychobiological development of maltreated children and its implications for research, treatment, and policy. Development and Psychopathology, 13(3), 539–564. [Google Scholar] [CrossRef]
- Derby, K. M., Wacker, D. P., Peck, S., SAsso, G. A. R. Y., DeRaad, A., Berg, W., Asmus, J., & Ulrich, S. (1994). Functional analysis of separate topographies of aberrant behavior. Journal of Applied Behavior Analysis, 27(2), 267–278. [Google Scholar] [CrossRef]
- Dong, M., Anda, R. F., Felitti, V. J., Dube, S. R., Williamson, D. F., Thompson, T. J., Loo, C. M., & Giles, W. H. (2004). The interrelatedness of multiple forms of childhood abuse, neglect, and household dysfunction. Child Abuse & Neglect, 28(7), 771–784. [Google Scholar] [CrossRef] [PubMed]
- Dye, H. (2018). The impact and long-term effects of childhood trauma. Journal of Human Behavior in the Social Environment, 28(3), 381–392. [Google Scholar] [CrossRef]
- Faul, F., Erdfelder, E., Lang, A.-G., & Buchner, A. (2007). G*Power 3: A flexible statistical power analysis program for the social, behavioral, and biomedical sciences. Behavior Research Methods, 39, 175–191. [Google Scholar] [CrossRef] [PubMed]
- Greenfield, E. A., & Marks, N. F. (2010). Identifying experiences of physical and psychological violence in childhood that jeopardize mental health in adulthood. Child Abuse & Neglect, 34(3), 161–171. [Google Scholar] [CrossRef] [PubMed]
- Hagopian, L. P., Rooker, G. W., Jessel, J., & DeLeon, I. G. (2013). Initial functional analysis outcomes and modifications in pursuit of differentiation: A summary of 176 inpatient cases. Journal of Applied Behavior Analysis, 46(1), 88–100. [Google Scholar] [CrossRef]
- Hanley, G. P., Iwata, B. A., & McCord, B. E. (2003). Functional analysis of problem behavior: A review. Journal of Applied Behavior Analysis, 36(2), 147–185. [Google Scholar] [CrossRef]
- Hartley, G., Sirois, F., Purrington, J., & Rabey, Y. (2024). Adverse childhood experiences and autism: A meta-analysis. Trauma Violence Abuse, 25(3), 2297–2315. [Google Scholar] [CrossRef]
- Heath, A. K., Ganz, J. B., Parker, R., Burke, M., & Ninci, J. (2015). A meta-analytic review of functional communication training across mode of communication, age, and disability. Review Journal of Autism and Developmental Disorders, 2(2), 155–166. [Google Scholar] [CrossRef]
- Hoover, D. W. (2020). Trauma in children with neurodevelopmental disorders: Autism, intellectual disability, and attention-deficit/hyperactivity disorder. In Childhood trauma in mental disorders: A comprehensive approach (pp. 367–383). Springer International Publishing. [Google Scholar]
- Iwata, B. A., Dorsey, M. F., Slifer, K. J., Bauman, K. E., & Richman, G. S. (1994). Toward a functional analysis of self-injury. Journal of Applied Behavior Analysis, 27(2), 197–209. [Google Scholar] [CrossRef]
- Jangid, R., Seema, N., Arun, G., Barre, V. P., Walia, D., & Rana, S. (2025). Interplay between adverse childhood experiences and neurodevelopmental disorders: A systematic review of recent evidence. Annals of Neurosciences, 09727531251359413. [Google Scholar] [CrossRef]
- Jessel, J., Fruchtman, T., Raghunauth-Zaman, N., Leyman, A., Lemos, F. M., Val, H. C., Howard, M., & Hanley, G. P. (2023). A two step validation of the performance-based IISCA: A trauma-informed functional analysis model. Behavior Analysis in Practice, 17(3), 727–745. [Google Scholar] [CrossRef]
- Kuenzel, E., Al-Saoud, S., Fang, M., & Duerden, E. G. (2025). Early childhood stress and amygdala structure in children and adolescents with neurodevelopmental disorders. Brain Structure & Function, 230(1), 29. [Google Scholar]
- McLaughlin, K. A., & Sheridan, M. A. (2016). Beyond cumulative risk: A dimensional approach to childhood adversity. Current Directions in Psychological Science, 25(4), 239–245. [Google Scholar] [CrossRef] [PubMed]
- McLaughlin, K. A., Sheridan, M. A., & Lambert, H. K. (2014). Childhood adversity and neural development: Deprivation and threat as distinct dimensions of early experience. Neuroscience and Biobehavioral Reviews, 47, 578–591. [Google Scholar] [CrossRef]
- Melanson, I. J., & Fahmie, T. A. (2023). Functional analysis of problem behavior: A 40-year review. Journal of Applied Behavior Analysis, 56(2), 262–281. [Google Scholar] [CrossRef]
- Moggia, D., Lutz, W., Brakemeier, E. L., & Bickman, L. (2024). Treatment personalization and precision mental health care: Where are we and where do we want to go? Administration and Policy in Mental Health, 51(5), 611–616. [Google Scholar] [CrossRef]
- Mosavi, N. S., & Santos, M. F. (2024). Enhancing clinical decision support for precision medicine: A data-driven approach. Informatics, 11(3), 68. [Google Scholar] [CrossRef]
- Naicker, S. N., Norris, S. A., Mabaso, M., & Richter, L. M. (2017). An analysis of retrospective and repeat prospective reports of adverse childhood experiences from the South African Birth to Twenty Plus cohort. PLoS ONE, 12(7), e0181522. [Google Scholar] [CrossRef] [PubMed]
- Nelson, C. A., 3rd, & Gabard-Durnam, L. J. (2020). Early adversity and critical periods: Neurodevelopmental consequences of violating the expectable environment. Trends in Neurosciences, 43(3), 133–143. [Google Scholar] [CrossRef] [PubMed]
- Nemeroff, C. B. (2004). Neurobiological consequences of childhood trauma. Journal of Clinical Psychiatry, 65, 18–28. [Google Scholar]
- Norman, S. B., Tate, S. R., Anderson, K. G., & Brown, S. A. (2007). Do trauma history and PTSD symptoms influence addiction relapse context? Drug and Alcohol Dependence, 90(1), 89–96. [Google Scholar] [CrossRef]
- Office of the California Surgeon General. (2020). ACE screening clinical workflows, ACEs and toxic stress risk assessment algorithm, and ACE-associated health conditions: For pediatrics and adults. Available online: https://www.acesaware.org/wp-content/uploads/2019/12/ACEs-Clinical-Algorithms-Workflows-and-ACEs-Associated-Health-Conditions.pdf (accessed on 4 November 2025).
- Olusanya, B. O., Davis, A. C., Wertlieb, D., Boo, N., Nair, M., Halpern, R., Kuper, H., Breinbauer, C., de Vries, P. J., Gladstone, M., Halfon, N., Kancherla, V., Mulaudzi, M. C., Kakooza-Mwesige, A., Ogbo, F. A., Olusanya, J. O., Williams, A. N., Wright, S. M., Manguerra, H., … Kassebaum, N. J. (2018). Developmental disabilities among children younger than 5 years in 195 countries and territories, 1990–2016: A systematic analysis for the global burden of disease study 2016. Lancet Global Health, 6, e1100–e1121. [Google Scholar] [CrossRef] [PubMed]
- Patel, D. R., & Merrick, J. (2020). Neurodevelopmental and neurobehavioral disorders. Translational Pediatrics, 9, S1–S2. [Google Scholar] [CrossRef] [PubMed]
- Rajaraman, A., Austin, J. L., Gover, H. C., Cammilleri, A. P., Donnelly, D. R., & Hanley, G. P. (2022). Toward trauma-informed applications of behavior analysis. Journal of Applied Behavior Analysis, 55(1), 40–61. [Google Scholar] [CrossRef] [PubMed]
- Reuben, A., Moffitt, T. E., Caspi, A., Belsky, D. W., Harrington, H., Schroeder, F., Hogan, S., Ramrakha, S., Poulton, R., & Danese, A. (2016). Lest we forget: Comparing retrospective and prospective assessments of adverse childhood experiences in the prediction of adult health. Journal of Child Psychology and Psychiatry, and Allied Disciplines, 57(10), 1103–1112. [Google Scholar] [CrossRef]
- Roane, H. S., Fisher, W. W., Kelley, M. E., Mevers, J. L., & Bouxsein, K. (2013). Using modified visual-inspection criteria to interpret functional anlaysis outcomes. Journal of Applied Behavioral Analysis, 46(1), 130–146. [Google Scholar] [CrossRef]
- Romani, P. W., Banks, T., Barnes, J. C., Murphy, J., Sannar, E. M., & Anderson, T. (2021). Use of a short-term psychiatric inpatient model to address problem behavior exhibited by youth with intellectual or developmental disabilities. Evidence-Based Practice in Child and Adolescent Mental Health, 6(4), 447–458. [Google Scholar] [CrossRef]
- Roscoe, E. M., Schlichenmeyer, K. J., & Dube, W. V. (2015). Functional analysis of problem behavior: A systematic approach for identifying idiosyncratic variables. Journal of Applied Behavior Analysis, 48(2), 289–314. [Google Scholar] [CrossRef]
- Ross, S. L., Sharma-Patel, K., Brown, E. J., Huntt, J. S., & Chaplin, W. F. (2021). Complex trauma and trauma-focused cognitive-behavioral therapy: How do trauma chronicity and PTSD presentation affect treatment outcome? Child Abuse & Neglect, 111, 104734. [Google Scholar]
- Sheridan, M. A., & McLaughlin, K. A. (2014). Dimensions of early experience and neural development: Deprivation and threat. Trends in Cognitive Science, 18(11), 580–585. [Google Scholar] [CrossRef]
- Swedo, E. A. (2023). Prevalence of adverse childhood experiences among US adults—Behavioral risk factor surveillance system, 2011–2020. MMWR. Morbidity and Mortality Weekly Report, 72, 707–715. [Google Scholar] [CrossRef] [PubMed]
- Takeda, T., Makinodan, M., Toritsuka, M., & Iwata, N. (2024). Impacts of adverse childhood experiences on individuals with autism spectrum disorder. Current Opinion in Neurobiology, 89, 102932. [Google Scholar] [CrossRef]
- Thakur, N., Hessler, D., Koita, K., Ye, M., Benson, M., Gilgoff, R., Bucci, M., Long, D., & Harris, N. B. (2020). Pediatrics adverse childhood experiences and related life events screener (PEARLS) and health in a safety-net practice. Child Abuse & Neglect, 108, 104685. [Google Scholar] [CrossRef] [PubMed]
- Vervoort-Schel, J., Mercera, G., Wissink, I., Van der Helm, P., Lindauer, R., & Moonen, X. (2021). Prevalence of and relationship between adverse childhood experiences and family context risk factors among children with intellectual disabilities and borderline intellectual functioning. Research in Developmental Disabilities, 113, 103935. [Google Scholar] [CrossRef]
- Wacker, D. P., Harding, J. W., Berg, W. K., Lee, J. F., Schieltz, K. M., Padilla, Y. C., Nevin, J. A., & Shahan, T. A. (2011). An evaluation of persistence of treatment effects during long-term treatment of destructive behavior. Journal of the Experimental Analysis of Behavior, 96(2), 261–282. [Google Scholar] [CrossRef]
- Yamagishi, M., Satomura, Y., Sakurada, H., Kanehara, A., Sakakibara, E., Okada, N., Koike, S., Yagishita, S., Ichihashi, K., Kondo, S., Jinde, S., Fukuda, M., & Kasai, K. (2022). Retrospective chart review-based assessment scale for adverse childhood events and experiences. Psychiatry and Clinical Neurosciences Reports, 1(4), e58. [Google Scholar] [CrossRef]
- Ye, M., Hessler, D., Ford, D., Benson, M., Koita, K., Bucci, M., Long, D., Harris, N. B., & Thakur, N. (2023). Pediatric ACEs and related life event screener (PEARLS) latent domains and child health in a safety-net primary care practice. BMC Pediatrics, 23(1), 367. [Google Scholar] [CrossRef]
- Zablotsky, B., Black, L. I., Maenner, M. J., Schieve, L. A., Danielson, M. L., Bitsko, R. H., Blumberg, S. J., Kogan, M. D., & Boyle, C. A. (2019). Prevalence and trends of developmental disabilities among children in the United States: 2009–2017. Pediatrics, 144, e20190811. [Google Scholar] [CrossRef] [PubMed]

| ID# | Diagnoses | Age | Gender | Race and Ethnicity |
|---|---|---|---|---|
| 1 | DMDD, PTSD, ADHD, MiID | 12 | Male | White, nonH |
| 2 | PTSD, ADHD, ASD, DBD | 10 | Female | White, nonH |
| 3 | PTSD, ADHD, ASD | 9 | Male | White, nonH |
| 4 | GAD, PTSD, UDD, ADHD, ASD | 15 | Male | White, nonH |
| 5 | PTSD, MiID, ADHD | 9 | Male | Asian/PI, nonH |
| 6 | PTSD, ADHD, MiID | 13 | Male | White, nonH |
| 7 | DMDD, PTSD, ADHD, MiID | 10 | Male | White, nonH |
| 8 | DBD, ADHD, ASD, OSTSRD | 8 | Male | White, nonH |
| 9 | PTSD, MDD, ADHD, ASD | 9 | Male | White, nonH |
| 10 | GAD, PTSD, ADHD | 7 | Male | White, nonH |
| 11 | DBD, PTSD, DMDD, ADHD, ASD | 12 | Male | White, nonH |
| 12 | DBD, PTSD, MiID | 13 | Female | White, nonH |
| 13 | OSTSRD, DBD, MiID | 14 | Male | Black, nonH |
| 14 | PTSD, ADHD, ASD | 11 | Female | White, nonH |
| 15 | PTSD, ADHD, ASD | 12 | Transgender | White, nonH |
| 16 | DMDD, PTSD, ADHD, ASD | 12 | Transgender | White, nonH |
| 17 | PTSD, OCD, RAD, MiID, cluster B traits | 15 | Female | White, nonH |
| 18 | PTSD, ADHD, DBD | 9 | Male | Multiracial, H |
| 19 | PTSD, ADHD, ASD | 12 | Female | White, nonH |
| 20 | PTSD, ADHD, ASD, MiID | 9 | Female | White, nonH |
| 21 | MDD, OSTSRD, DMD, ASD | 13 | Female | White, nonH |
| Part ID | Topographies | FA Results | Treatment Evaluation | PB % Reduction | ACEs, Part 1 | ACEs, Part 2 |
|---|---|---|---|---|---|---|
| 1 | AGG, PD, NS, EL | AT | FCT AT | 97.1 | 6 | 1 |
| 2 | AGG, PD, NS, EL | AT | FCT ES | 100 | 7 | 1 |
| 3 | PD, NS | AT | FCT AT | 100 | 6 | 2 |
| 4 | NS | AT | FCT ES | 0 | 4 | 1 |
| 5 | PD, NS, EL | AT | FCT AT | 100 | 1 | 1 |
| FCT ES | 100 | |||||
| 6 | NS | ES, TA | FCT ES | 100 | 7 | 3 |
| 7 | NS, IV | ES | FCT AT | 0 | 2 | 2 |
| PD, NS, EL | FCT ES | 0 | ||||
| 8 | AGG, PD, NS, SIB | ES, TA | FCT ES | 60 | 7 | 1 |
| FCT TA | 100 | |||||
| 9 | NS; EL | ES | FCT ES | 52.9 | 5 | 1 |
| Ther Work | 35.3 | |||||
| 10 | NS | ES | FCT ES | 100 | 5 | 2 |
| 11 | AGG, PD, NS, SIB | ES, TA | FCT ES | 100 | 4 | 1 |
| 12 | AGG, PD, NS, SIB | Undiff | FCT ES | 100 | 3 | 1 |
| 13 | AGG, PD, NS, EL | ES, TA | FCT ES | 100 | 5 | 6 |
| 14 | NS | ES | FCT ES | 68 | 4 | 2 |
| Ther Work | 100 | |||||
| 15 | AGG, PD, NS, EL | Undiff | FCT ES | 0 | 7 | 5 |
| 16 | NS (somatic complaints) | ES | Ther Work | 40.3 | 7 | 6 |
| 17 | NS; AGG; EL | TA | FCT ES | 100 | 4 | 3 |
| FCT AT | 100 | |||||
| 18 | EL | Undiff | FCT ES | 100 | 5 | 0 |
| 19 | AGG, PD, NS, SIB | Undiff | FCT TA | 100 | 5 | 3 |
| FCT ES | 100 | |||||
| 20 | PD, NS, EL | Undiff | FCT ES | 0 | 7 | 2 |
| 21 | PD, NS, EL | Undiff | FCT AT + TA | 0 | 5 | 3 |
| Average | 72.4 | 5.0 | 2.2 | |||
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2026 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license.
Share and Cite
Luehring, M.C.; Ryland, L.; Sanchez, C.; Romani, P.W. Preliminary Data on Behavioral Profiles of Youth with Neurodevelopmental Disorders and Trauma. Behav. Sci. 2026, 16, 239. https://doi.org/10.3390/bs16020239
Luehring MC, Ryland L, Sanchez C, Romani PW. Preliminary Data on Behavioral Profiles of Youth with Neurodevelopmental Disorders and Trauma. Behavioral Sciences. 2026; 16(2):239. https://doi.org/10.3390/bs16020239
Chicago/Turabian StyleLuehring, Mathew C., Leonora Ryland, Catherine Sanchez, and Patrick W. Romani. 2026. "Preliminary Data on Behavioral Profiles of Youth with Neurodevelopmental Disorders and Trauma" Behavioral Sciences 16, no. 2: 239. https://doi.org/10.3390/bs16020239
APA StyleLuehring, M. C., Ryland, L., Sanchez, C., & Romani, P. W. (2026). Preliminary Data on Behavioral Profiles of Youth with Neurodevelopmental Disorders and Trauma. Behavioral Sciences, 16(2), 239. https://doi.org/10.3390/bs16020239







