Telehealth Pilot Study of the Effects of a Naturalistic Developmental Behavioral Intervention on Child Social Communication Outcomes in a Community Mental Health System
Abstract
1. Introduction
- To what extent does Project ImPACT improve caregiver-reported social communication outcomes for autistic children receiving the intervention from novice clinicians in the community mental health system?
- What are caregiver perspectives on the Project ImPACT strategies and their experiences with the intervention in this publicly funded service system?
2. Materials and Methods
2.1. Patient and Public Involvement
2.2. Design
2.3. Changes to the Protocol
2.4. Setting
2.5. Eligibility Criteria
2.6. Intervention
2.7. Outcomes
2.8. Sampling and Sample Size
2.9. Randomization
2.10. Statistical Methods
3. Results
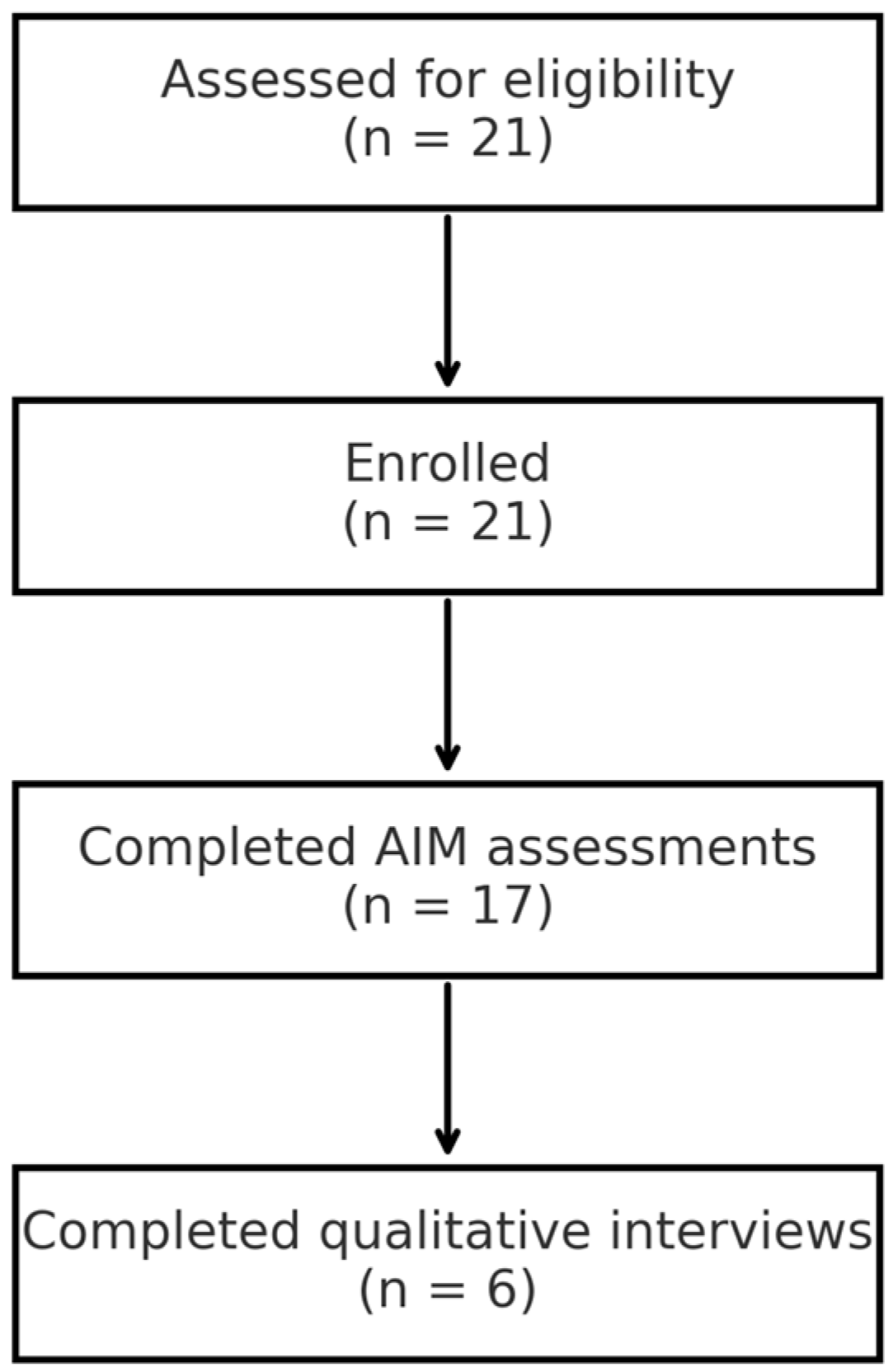
3.1. Participant Flow and Flow Diagram
3.2. Recruitment
3.3. Intervention Delivery
3.4. Baseline Data (Demographics)
3.5. Quantitative Results
3.5.1. Peer Interaction
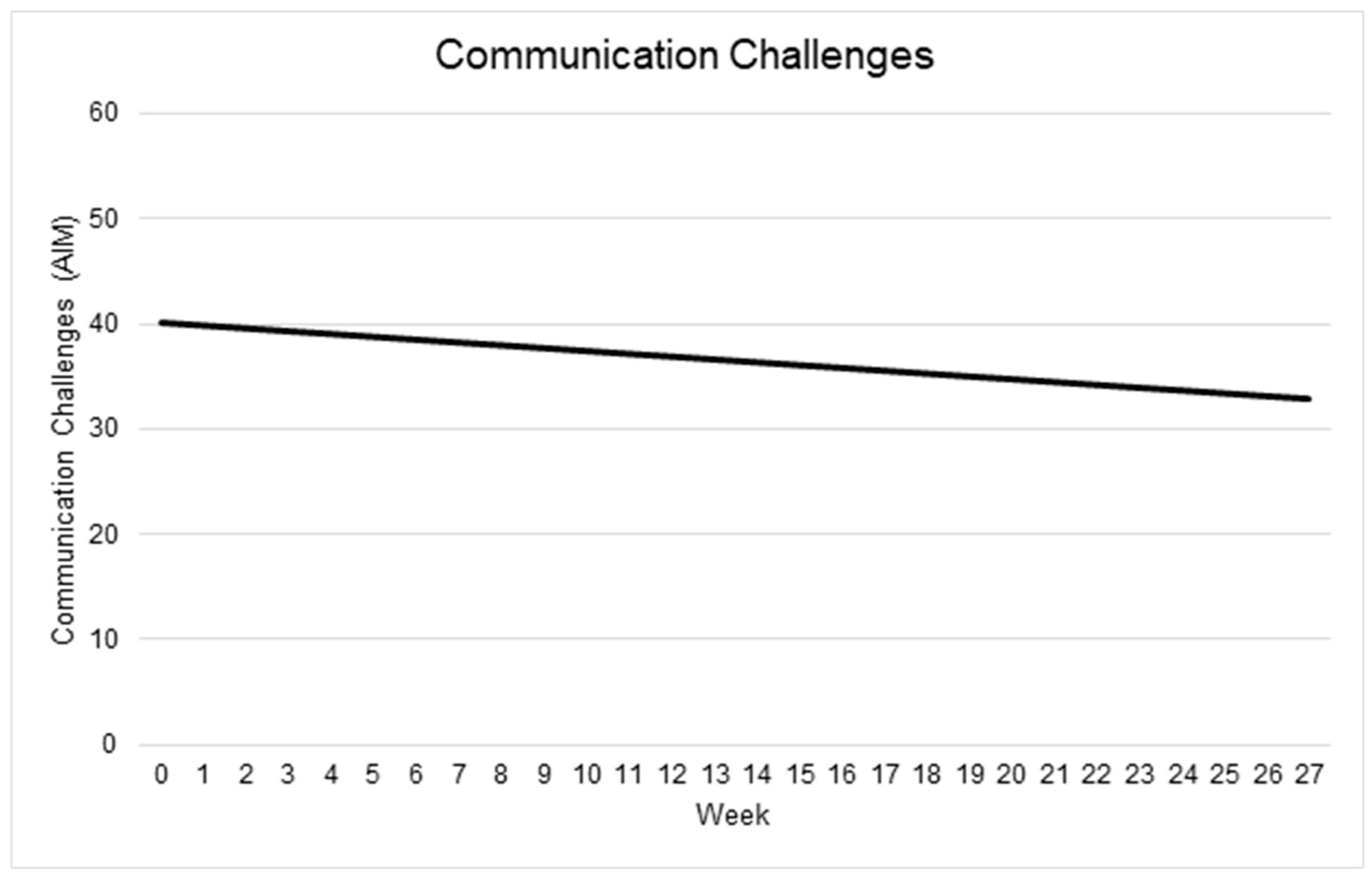
3.5.2. Communication
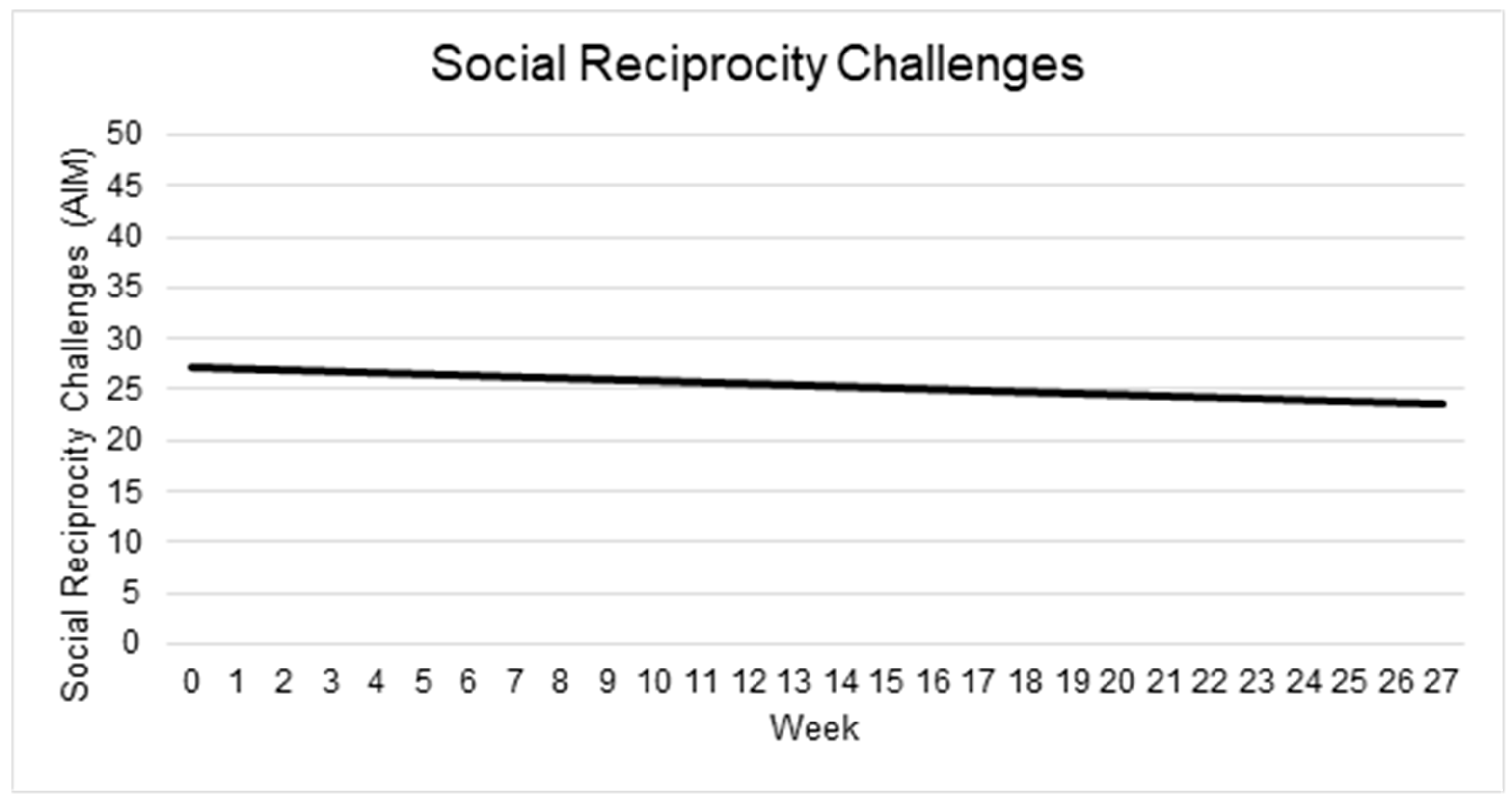
3.5.3. Social Reciprocity
3.6. Qualitative Results
3.6.1. Project ImPACT Changes How Caregivers Interact with Their Child
3.6.2. Project ImPACT Teaches Caregivers to Use NDBI Strategies That Expand the Child’s Communication
3.6.3. The NDBI Strategy of Following Your Child’s Lead Supported Child Social Engagement
3.6.4. Project ImPACT Strategies Increased Children’s Social Engagement
3.6.5. Project ImPACT Increased Peer Interaction
3.6.6. Project ImPACT Supported the Inclusion of Additional Family Members in the Child’s Intervention Services
3.6.7. Caregivers Noted Suggestions About Improving Project ImPACT Materials
4. Discussion
4.1. Child Outcomes
4.2. Caregiver and Family Outcomes
4.3. Future Research
4.4. Limitations
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Acknowledgments
Conflicts of Interest
References
- Alatar, W., Knott, F., & Loucas, T. (2023). The Effectiveness of telemedicine in coaching parents of autistic children using naturalistic developmental early interventions: A rapid review. Review Journal of Autism and Developmental Disorders, 12, 273–289. [Google Scholar] [CrossRef]
- Aranbarri, A., Stahmer, A. C., Talbott, M. R., Miller, M. E., Drahota, A., Pellecchia, M., Barber, A. B., Griffith, E. M., Morgan, E. H., & Rogers, S. J. (2021). Examining US public early intervention for toddlers with Autism: Characterizing services and readiness for evidence-based practice implementation. Frontiers in Psychiatry, 12, 786138. [Google Scholar] [CrossRef]
- Braun, V., & Clarke, V. (2013). Successful qualitative research: A practical guide for beginners. SAGE Publications Ltd. [Google Scholar]
- Carr, T., & Lord, C. (2016). A pilot study promoting participation of families with limited resources in early autism intervention. Research in Autism Spectrum Disorders, 25, 87–96. [Google Scholar] [CrossRef]
- Carr, T., Shih, W., Lawton, K., Lord, C., King, B., & Kasari, C. (2016). The relationship between treatment attendance, adherence, and outcome in a caregiver-mediated intervention for low-resourced families of young children with autism spectrum disorder. Autism, 20(6), 643–652. [Google Scholar] [CrossRef]
- Casagrande, K. A. (2021). Family training under the medicaid Autism benefit: Understanding parent perspectives on barriers to engagement. Michigan State University. [Google Scholar]
- Chapman, R., & Bovell, V. (2022). Neurodiversity, advocacy, anti-therapy. In J. L. Matson, & P. Sturmey (Eds.), Handbook of Autism and pervasive developmental disorder. Autism and child psychopathology series. Springer. [Google Scholar] [CrossRef]
- Crank, J. E., Sandbank, M., Dunham, K., Crowley, S., Bottema-Beutel, K., Feldman, J., & Woynaroski, T. G. (2021). Understanding the effects of naturalistic developmental behavioral interventions: A project AIM meta-analysis. Autism Research, 14(4), 817–834. [Google Scholar] [CrossRef]
- Cross, C. J. (2018). Extended family households among children in the United States: Differences by race/ethnicity and socio-economic status. Population Studies, 72(2), 235–251. [Google Scholar] [CrossRef]
- D’Agostino, S. R., Landon, T. J., Roylance, A., Briggs, A., & Bhana-Lopez, N. (2025). Exploring the social validity and diffusion potential of common naturalistic developmental behavioral intervention strategies implemented in community preschools. Behavioral Sciences, 15(3), 357. [Google Scholar] [CrossRef]
- Griffin, E., & Pollak, D. (2009). Student experiences of neurodiversity in higher education: Insights from the BRAINHE project. Dyslexia, 15(1), 23–41. [Google Scholar] [CrossRef] [PubMed]
- Ingersoll, B., Frost, K. M., Straiton, D., Ramos, A. P., & Casagrande, K. (2024). Telehealth coaching in project ImPACT indirectly affects children’s expressive language ability through parent intervention strategy use and child intentional communication: An RCT. Autism Research, 17(10), 2177–2187. [Google Scholar] [CrossRef] [PubMed]
- Jones, M. K., Sone, B. J., Grauzer, J., Sudec, L., Kaat, A., & Roberts, M. Y. (2023). Characterizing mechanisms of caregiver-mediated naturalistic developmental behavioral interventions for autistic toddlers: A randomized clinical trial. Autism, 28(7), 1847–1860. [Google Scholar] [CrossRef]
- Jurek, L., Leadbitter, K., Falissard, B., Colin, C., Touzet, S., & Geoffray, M.-M. (2023). Parental experience of parent-mediated intervention for children with ASD: A systematic review and qualitative evidence synthesis. Autism, 27(3), 647–666. [Google Scholar] [CrossRef]
- Kanne, S. M., Mazurek, M. O., Sikora, D., Bellando, J., Branum-Martin, L., Handen, B., Katz, T., Freedman, B., Powell, M. P., & Warren, Z. (2014). The Autism Impact Measure (AIM): Initial development of a new tool for treatment outcome measurement. Journal of Autism and Developmental Disorders, 44(1), 168–179. [Google Scholar] [CrossRef]
- Kasari, C., Lawton, K., Shih, W., Barker, T. V., Landa, R., Lord, C., Orlich, F., King, B., Wetherby, A., & Senturk, D. (2014). Caregiver-Mediated intervention for low-resourced preschoolers with Autism: An RCT. Pediatrics, 134(1), e72–e79. [Google Scholar] [CrossRef] [PubMed]
- Larson, A. L., An, Z. G., Wood, C., Uchikoshi, Y., Cycyk, L. M., Scheffner Hammer, C., Escobar, K., & Roberts, K. (2020). Social validity in early language interventions for dual language learners: A systematic review of the literature. Topics in Early Childhood Special Education, 40(1), 39–51. [Google Scholar] [CrossRef]
- Leach, D., & LaRocque, M. (2011). Increasing social reciprocity in young children with Autism. Intervention in School and Clinic, 46(3), 150–156. [Google Scholar] [CrossRef]
- Mazurek, M. O., Carlson, C., Baker-Ericzén, M., Butter, E., Norris, M., Barr, C., & Kanne, S. (2020). The Autism Impact Measure (AIM): Examination of sensitivity to change. Autism Research, 13(11), 1867–1879. [Google Scholar] [CrossRef]
- Pacia, C., Holloway, J., Gunning, C., & Lee, H. (2022). A systematic review of family-mediated social communication interventions for young children with Autism. Review Journal of Autism and Developmental Disorders, 9(2), 208–234. [Google Scholar] [CrossRef]
- Palinkas, L. A., Aarons, G. A., Horwitz, S., Chamberlain, P., Hurlburt, M., & Landsverk, J. (2011). Mixed method designs in implementation research. Administration and Policy in Mental Health and Mental Health Services Research, 38(1), 44–53. [Google Scholar] [CrossRef]
- Patterson, S. Y., Elder, L., Gulsrud, A., & Kasari, C. (2014). The association between parental interaction style and children’s joint engagement in families with toddlers with autism. Autism, 18(5), 511–518. [Google Scholar] [CrossRef] [PubMed]
- Pellecchia, M., Ingersoll, B., Marcus, S. C., Rump, K., Xie, M., Newman, J., Zeigler, L., Crabbe, S., Straiton, D., Chávez, E. C., & Mandell, D. S. (2024). Pilot randomized trial of a caregiver-mediated naturalistic developmental behavioral intervention in part C early intervention. Journal of Early Intervention, 46(2), 194–216. [Google Scholar] [CrossRef]
- Peterson, T., Dodson, J., Sherwin, R., & Frederick, S. (2024). The Effects of age and treatment intensity on behavioral target mastery with Applied Behavior Analysis (ABA) intervention using causal moderation models. Cureus, 16(8), e67179. [Google Scholar] [CrossRef] [PubMed]
- Pickard, K., Guerra, K., Hendrix, N., Khowaja, M., & Nicholson, C. (2024). Preliminary outcomes and adaptation of an NDBI for Spanish-speaking families. Journal of Early Intervention, 46(2), 217–238. [Google Scholar] [CrossRef]
- Rieder, A. D., Viljoen, M., Seris, N., Shabalala, N., Ndlovu, M., Turner, E. L., Simmons, R., de Vries, P. J., & Franz, L. (2023). Improving access to early intervention for autism: Findings from a proof-of-principle cascaded task-sharing naturalistic developmental behavioural intervention in South Africa. Child and Adolescent Psychiatry and Mental Health, 17(1), 64. [Google Scholar] [CrossRef]
- Ritchie, J., & Spencer, L. (1994). Qualitative data analysis for applied policy research. In Analyzing qualitative data. Routledge. [Google Scholar]
- Roberts, M. Y., Sone, B. J., Jones, M., Grauzer, J., Sudec, L., Stern, Y. S., Kwok, E., Losh, M., & Kaat, A. (2023). One size does not fit all for parent-mediated autism interventions: A randomized clinical trial. Autism, 27(2), 443–455. [Google Scholar] [CrossRef]
- Rocha, M. L., Schreibman, L., & Stahmer, A. C. (2007). Effectiveness of training parents to teach joint attention in children with autism. Journal of Early Intervention, 29(2), 154172. [Google Scholar] [CrossRef]
- Rogers, S. J., Stahmer, A., Talbott, M., Young, G., Fuller, E., Pellecchia, M., Barber, A., & Griffith, E. (2022). Feasibility of delivering parent-implemented NDBI interventions in low-resource regions: A pilot randomized controlled study. Journal of Neurodevelopmental Disorders, 14(1), 3. [Google Scholar] [CrossRef]
- Saldaña, J. (2015). The coding manual for qualitative researchers. SAGE. [Google Scholar]
- Sandbank, M., Bottema-Beutel, K., LaPoint, S. C., Feldman, J. I., Barrett, D. J., Caldwell, N., Dunham, K., Crank, J., Albarran, S., & Woynaroski, T. (2023). Autism intervention meta-analysis of early childhood studies (Project AIM): Updated systematic review and secondary analysis. BMJ, 383, e076733. [Google Scholar] [CrossRef]
- Schreibman, L., Dawson, G., Stahmer, A. C., Landa, R., Rogers, S. J., McGee, G. G., Kasari, C., Ingersoll, B., Kaiser, A. P., Bruinsma, Y., McNerney, E., Wetherby, A., & Halladay, A. (2015). Naturalistic developmental behavioral interventions: Empirically validated treatments for Autism spectrum disorder. Journal of Autism and Developmental Disorders, 45(8), 2411–2428. [Google Scholar] [CrossRef]
- Schuck, R. K., Dwyer, P., Baiden, K. M. P., Williams, Z. J., & Wang, M. (2024). Social validity of pivotal response treatment for young Autistic children: Perspectives of Autistic adults. Journal of Autism and Developmental Disorders, 54(2), 423–441. [Google Scholar] [CrossRef]
- Schuck, R. K., Tagavi, D. M., Baiden, K. M. P., Dwyer, P., Williams, Z. J., Osuna, A., Ferguson, E. F., Jimenez Muñoz, M., Poyser, S. K., Johnson, J. F., & Vernon, T. W. (2021). Neurodiversity and Autism intervention: Reconciling perspectives through a naturalistic developmental behavioral intervention framework. Journal of Autism and Developmental Disorders, 52(10), 4625–4645. [Google Scholar] [CrossRef]
- Simcoe, K., Stainbrook, J. A., Chazin, K. T., Schnelle, E., Wagner, L., Hooper, M., Juárez, A. P., & Warren, Z. (2025). Use of telemediated caregiver coaching to increase access to naturalistic developmental behavioral interventions within a statewide early intervention system. Autism, 29(1), 207–221. [Google Scholar] [CrossRef]
- Sivaraman, M., & Fahmie, T. A. (2020). Evaluating the efficacy and social validity of a culturally adapted training program for parents and service providers in India. Behavior Analysis in Practice, 13(4), 849–861. [Google Scholar] [CrossRef]
- Smith, K. A., Gehricke, J.-G., Iadarola, S., Wolfe, A., & Kuhlthau, K. A. (2020). Disparities in service use among children with Autism: A systematic review. Pediatrics, 145(Suppl. 1), S35–S46. [Google Scholar] [CrossRef]
- Stahmer, A. C., Rieth, S. R., Dickson, K. S., Feder, J., Burgeson, M., Searcy, K., & Brookman-Frazee, L. (2020). Project ImPACT for Toddlers: Pilot outcomes of a community adaptation of an intervention for autism risk. Autism, 24(3), 617–632. [Google Scholar] [CrossRef]
- Straiton, D., Frost, K., & Ingersoll, B. (2023). Factors that influence clinical decisions about offering parent coaching for autistic youth served within the Medicaid system. Implementation Research and Practice, 4, 26334895231153631. [Google Scholar] [CrossRef]
- Straiton, D., Groom, B., & Ingersoll, B. (2021a). A mixed methods exploration of community providers’ perceived barriers and facilitators to the use of parent training with Medicaid-enrolled clients with autism. Autism: The International Journal of Research and Practice, 25(5), 1368–1381. [Google Scholar] [CrossRef]
- Straiton, D., Groom, B., & Ingersoll, B. (2021b). Parent training for youth with Autism served in community settings: A mixed-methods investigation within a community mental health system. Journal of Autism and Developmental Disorders, 51(6), 1983–1994. [Google Scholar] [CrossRef] [PubMed]
- Straiton-Webster, D., Moeyaert, M., Greatorex, J., Ewell, A., & Ingersoll, B. (in prep). Examining the active ingredients of consultation: Effects of discrete consultation components on implementation outcomes for an autism intervention in a community mental health system.
- Tiede, G., & Walton, K. M. (2019). Meta-analysis of naturalistic developmental behavioral interventions for young children with autism spectrum disorder. Autism, 23(8), 2080–2095. [Google Scholar] [CrossRef] [PubMed]
- Tomczuk, L., Stewart, R. E., Beidas, R. S., Mandell, D. S., & Pellecchia, M. (2022). Who gets coached? A qualitative inquiry into community clinicians’ decisions to use caregiver coaching. Autism, 26(3), 575–585. [Google Scholar] [CrossRef] [PubMed]
- van Noorden, L., Gardiner, S., & Waddington, H. (2024). Parent-mediated naturalistic developmental behavioral interventions for young Autistic children: A systematic literature review of single-case research. Review Journal of Autism and Developmental Disorders. [Google Scholar] [CrossRef]
- Wolf, M. M. (1978). Social validity: The case for subjective measurement or how applied behavior analysis is finding its heart. Journal of Applied Behavior Analysis, 11(2), 203–214. [Google Scholar] [CrossRef] [PubMed]
- Zwaigenbaum, L., Bauman, M. L., Choueiri, R., Fein, D., Kasari, C., Pierce, K., Stone, W. L., Yirmiya, N., Estes, A., Hansen, R. L., McPartland, J. C., Natowicz, M. R., Buie, T., Carter, A., Davis, P. A., Granpeesheh, D., Mailloux, Z., Newschaffer, C., Robins, D., … Wetherby, A. (2015). Early identification and interventions for Autism spectrum disorder: Executive summary. Pediatrics, 136(Suppl. 1), S1–S9. [Google Scholar] [CrossRef] [PubMed]

| Demographics | Full Sample (N = 21) | Qualitative Sample (n = 6) | ||
| n | % | n | % | |
| Caregiver Gender | ||||
| Woman | 17 | 81% | 6 | 100% |
| Man | 2 | 10% | 0 | 0% |
| Unknown | 2 | 10% | 0 | 0% |
| Caregiver Age | 35.7 yrs (range: 23–54 yrs) | |||
| Caregiver Race | ||||
| White | 15 | 71% | 4 | 67% |
| American Indian or Alaska native | 1 | 5% | 0 | 0% |
| African American | 4 | 19% | 2 | 33% |
| Asian | 0 | 0% | 0 | 0% |
| Native Hawaiian or Other Pacific Islander | 0 | 0% | 0 | 0% |
| Unknown | 2 | 10% | 0 | 0% |
| Caregiver Ethnicity | ||||
| Not Hispanic or Latinx | 19 | 90% | 6 | 100% |
| Hispanic or Latinx | 0 | 0% | 0 | 0% |
| Unknown | 2 | 10% | 0 | 0% |
| Child Gender | ||||
| Girl | 7 | 33% | 2 | 33% |
| Boy | 12 | 57% | 4 | 67% |
| Unknown | 2 | 10% | 0 | 0% |
| Child Age | 55 mos (range: 24–76 mos) | |||
| Child Race | ||||
| White | 15 | 71% | 4 | 67% |
| American Indian or Alaska Native | 1 | 5% | 0 | 0% |
| Black or African American | 4 | 19% | 2 | 33% |
| Asian | 1 | 5% | 0 | 0% |
| Native Hawaiian or Other Pacific Islander | 0 | 0% | 0 | 0% |
| Unknown | 2 | 10% | 0 | 0% |
| Child Ethnicity | ||||
| Not Hispanic or Latinx | 19 | 90% | 6 | 100% |
| Hispanic or Latinx | 2 | 10% | 0 | 0% |
| Unknown | 2 | 10% | 0 | 0% |
| Caregiver’s Education | ||||
| Some High School | 0 | 0% | 0 | 0% |
| High School Graduate | 5 | 24% | 1 | 17% |
| Some college/specialized training | 8 | 38% | 4 | 67% |
| 4-year college graduate | 4 | 19% | 1 | 17% |
| Graduate degree | 2 | 10% | 0 | 0% |
| Unknown | 2 | 10% | 0 | 0% |
| Fixed Effects | b | SE | t | df | p |
|---|---|---|---|---|---|
| Intercept | 22.53 | 1.37 | 16.50 | 20.28 | <0.001 |
| Time (weeks) | −0.25 | 0.10 | −2.39 | 46.43 | 0.021 |
| Child Age (months) | −0.18 | 0.11 | −1.62 | 22.04 | 0.119 |
| Time × Child Age | 0.01 | 0.01 | 1.18 | 45.63 | 0.244 |
| Random Effects | Variance Component | SD | |||
| Intercept | 23.15 | 4.81 | |||
| Fixed Effects | b | SE | t | df | p |
|---|---|---|---|---|---|
| Intercept | 40.09 | 2.70 | 14.84 | 17.82 | <0.001 |
| Time (weeks) | −0.27 | 0.15 | −1.72 | 45.04 | 0.092 |
| Child Age (months) | −0.21 | 0.21 | −0.99 | 18.68 | 0.335 |
| Time × Child Age | −0.00 | 0.01 | −0.21 | 44.55 | 0.839 |
| Random Effects | Variance Component | SD | |||
| Intercept | 105.03 | 10.25 | |||
| Fixed Effects | b | SE | t | df | p |
|---|---|---|---|---|---|
| Intercept | 27.30 | 1.41 | 19.36 | 21.59 | <0.001 |
| Time (weeks) | −0.14 | 0.12 | −1.13 | 46.99 | 0.265 |
| Child Age (months) | −0.09 | 0.11 | −0.80 | 24.04 | 0.431 |
| Time × Child Age | 0.01 | 0.01 | 1.03 | 45.98 | 0.309 |
| Random Effects | Variance Component | SD | |||
| Intercept | 22.12 | 4.70 | |||
| Quantitative Data (n = 17) | Intercept | b (SE) | Statistics |
|---|---|---|---|
| AIM Communication Challenges | 40.09 | −0.27 (0.15) | t(45.04) = −1.72, p = 0.09 |
| AIM Peer Interaction Challenges | 22.53 | −0.25 (0.10) | t(46.43) = −2.39, p = 0.02 |
| AIM Social Reciprocity Challenges | 27.30 | −0.14 (0.12) | t(46.99) = −1.13, p = 0.27 |
| Qualitative Themes and Subthemes | Theme Count and % of Caregivers (N = 6) | Representative Quotes | Interpretation |
| Project ImPACT changes how caregivers interact with their child | 30 (100%) | “The following the lead of him made a world of difference. I was never one to really play with kids and having Project ImPACT now I’m like ‘okay we’re playing Mr. Potato Head, and this is how we do it’… You don’t have to follow the standard rules of the game.” |
|
| Project ImPACT teaches caregivers to use NDBI strategies that expand the child’s communication | 13 (83%) | “I remember one of the tasks where you just pause for a second, don’t try to help her, just let her get her own words out and she will do that or sign ‘more, please’—things like that, not just handing it to her, but making her use her actual words.” | |
| The NDBI strategy of following your child’s lead supported child social engagement | 6 (67%) | “I’m focusing on her, you know doing things she wants to do, and then the playtime can last a bit longer.” | |
| Project ImPACT strategies increased children’s social engagement | 17 (83%) | “He could always grab my hand and take me to do something. But then, once I get that item down for him, he used to just want to take off with it, but now he’ll be like, you know, ‘Do you want to do this with me?’ type of behavior, and he’ll sit down with the puzzle next to me, instead of running off with it to do his own thing.” | |
| Project ImPACT increased peer interaction | 8 (83%) | “At school, he’s been playing more with other kids.” | |
| Project ImPACT supported the inclusion of additional family members in the child’s intervention services | 5 (50%) | “And not only do I do it, but I encourage others to do it, you know, like my mom, his sister, his brother.” |
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2025 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Greatorex, J.; Straiton-Webster, D.; Ingersoll, B. Telehealth Pilot Study of the Effects of a Naturalistic Developmental Behavioral Intervention on Child Social Communication Outcomes in a Community Mental Health System. Behav. Sci. 2025, 15, 1171. https://doi.org/10.3390/bs15091171
Greatorex J, Straiton-Webster D, Ingersoll B. Telehealth Pilot Study of the Effects of a Naturalistic Developmental Behavioral Intervention on Child Social Communication Outcomes in a Community Mental Health System. Behavioral Sciences. 2025; 15(9):1171. https://doi.org/10.3390/bs15091171
Chicago/Turabian StyleGreatorex, Jessie, Diondra Straiton-Webster, and Brooke Ingersoll. 2025. "Telehealth Pilot Study of the Effects of a Naturalistic Developmental Behavioral Intervention on Child Social Communication Outcomes in a Community Mental Health System" Behavioral Sciences 15, no. 9: 1171. https://doi.org/10.3390/bs15091171
APA StyleGreatorex, J., Straiton-Webster, D., & Ingersoll, B. (2025). Telehealth Pilot Study of the Effects of a Naturalistic Developmental Behavioral Intervention on Child Social Communication Outcomes in a Community Mental Health System. Behavioral Sciences, 15(9), 1171. https://doi.org/10.3390/bs15091171






