A Review of Psychological Stress among Students and Its Assessment Using Salivary Biomarkers
Abstract
1. Introduction
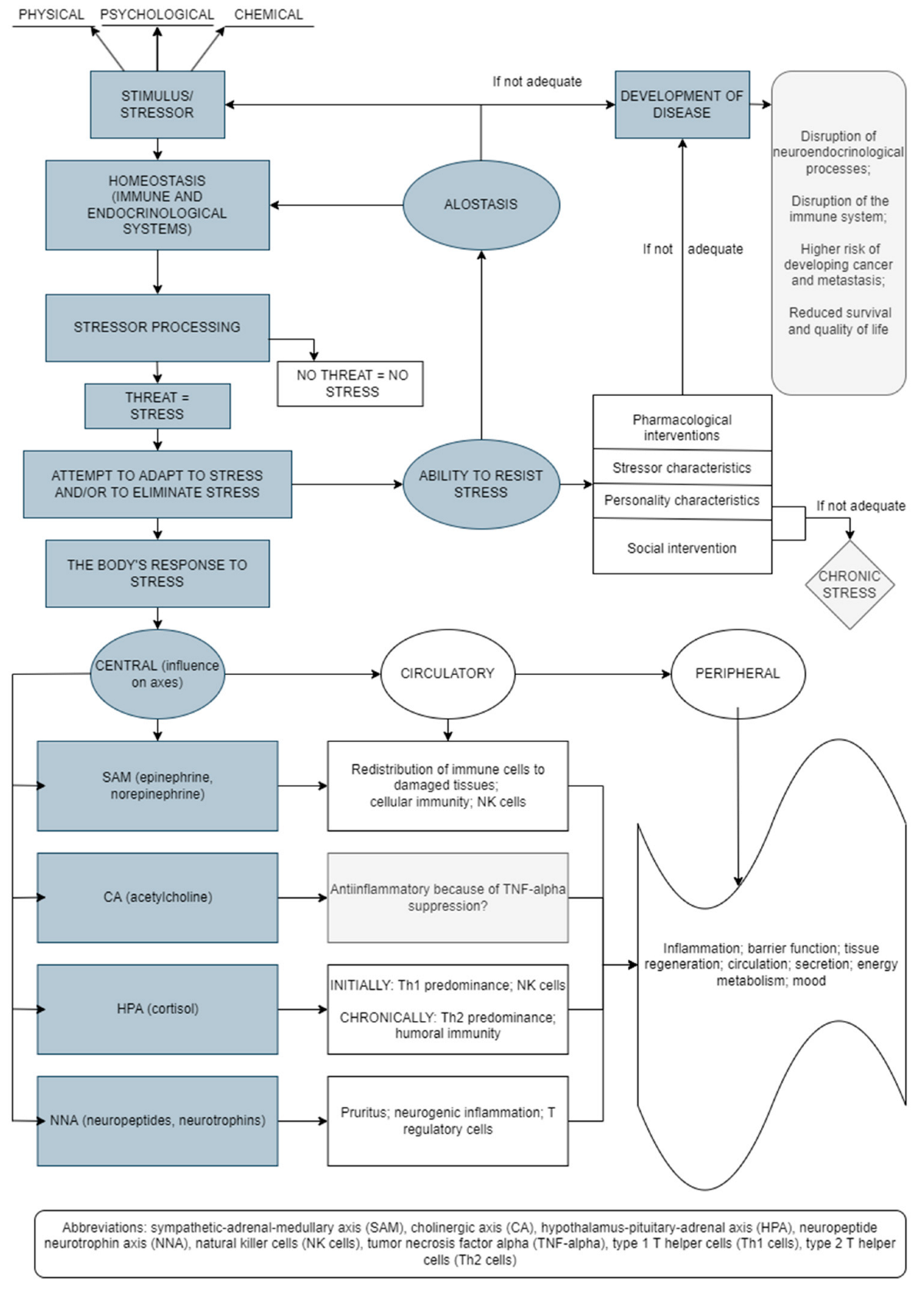
2. Physiology of Acute and Chronic Stress Reactions and the HPA Axis
3. Immunity during Stress: The Inflammatory Reaction and Stress
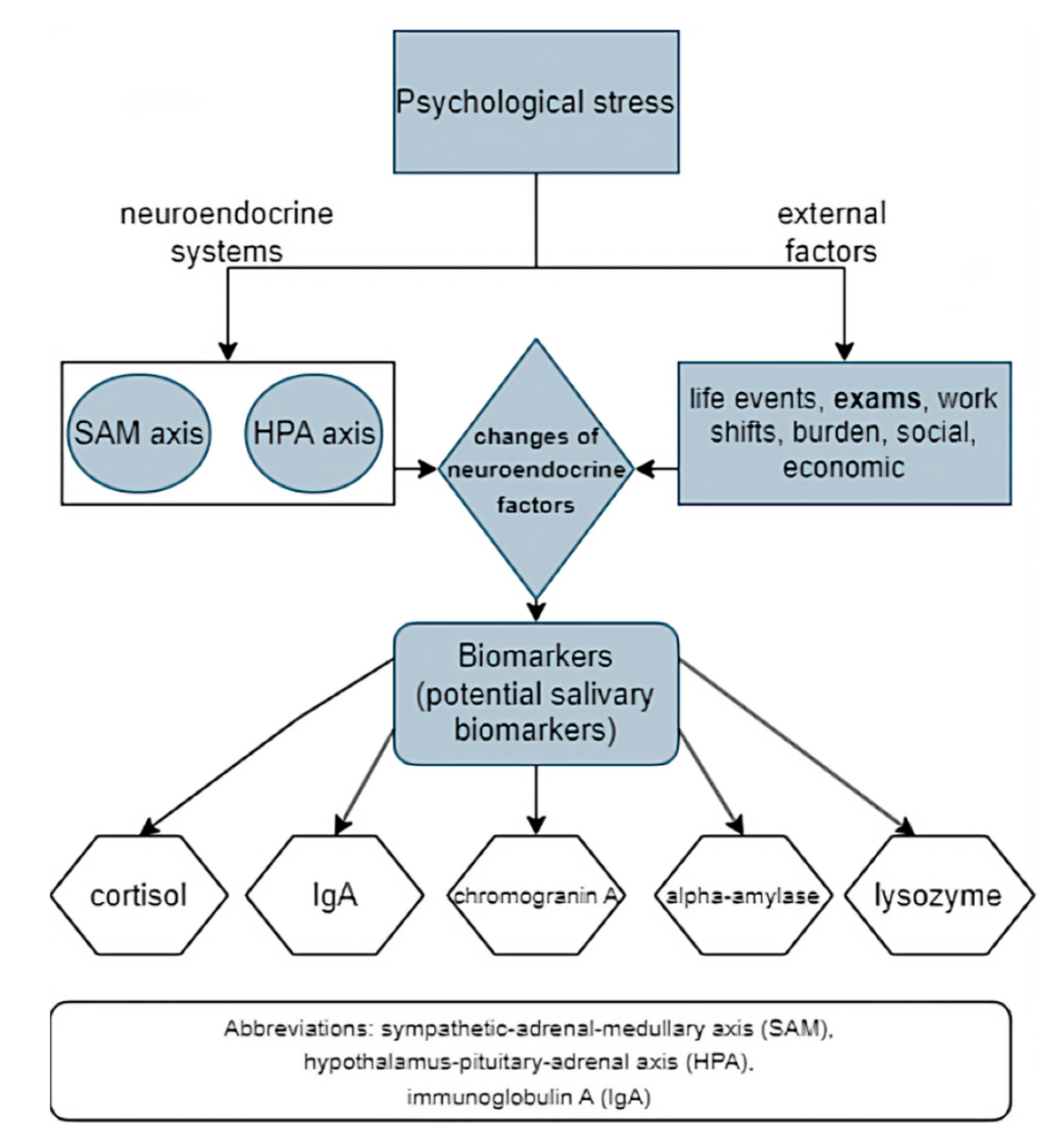
4. Salivary Biomarkers for Stress Assessment
5. Students and the Concept of Academic Stress
6. Benefits of, and Perspectives on, the Further Use of Salivary Biomarkers for Research Purposes and in Practice
7. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Conflicts of Interest
References
- Ouda, S.; Alaki, S.; Safi, M.A.; Nadhreen, A.; Johani, K.A. Salivary Stress Biomarkers–Are They predictors of Academic Assessment Exams Stress. J. Clin. Exp. Pathol. 2016, 15, 276–279. [Google Scholar]
- O’Connor, D.B.; Thayer, J.F.; Vedhara, K. Stress and Health: A Review of Psychobiological Processes. Annu. Rev. Psychol. 2020, 72, 663–688. [Google Scholar] [CrossRef] [PubMed]
- Ravishankar, T.L.; Ain, T.S.; Gowhar, O. Effect of Academic Stress on Plaque and Gingival Health among Dental Students of Moradabad, India. J. Int. Acad. Periodontol. 2014, 16, 115–120. [Google Scholar] [PubMed]
- Dhama, K.; Latheef, S.K.; Dadar, M.; Samad, H.A.; Munjal, A.; Khandia, R.; Karthik, K.; Tiwari, R.; Yatoo, M.I.; Bhatt, P.; et al. Biomarkers in Stress Related Diseases/Disorders: Diagnostic, Prognostic, and Therapeutic Values. Front. Mol. Biosci. 2019, 6, 91. [Google Scholar] [CrossRef]
- Ader, R.; Cohen, N.; Felten, D. Psychoneuroimmunology: Interactions between the Nervous System and the Immune System. Lancet 1995, 345, 99–103. [Google Scholar] [CrossRef]
- McEwen, B.S. Protective and Damaging Effects of Stress Mediators. N. Engl. J. Med. 1998, 338, 171–179. [Google Scholar] [CrossRef]
- McEwen, B.S. Physiology and Neurobiology of Stress and Adaptation: Central Role of the Brain. Physiol. Rev. 2007, 87, 873–904. [Google Scholar] [CrossRef]
- Besedovsky, H.O.; Rey, A.D. Physiology of Psychoneuroimmunology: A Personal View. Brain Behav. Immun. 2007, 21, 34–44. [Google Scholar] [CrossRef]
- Lugović-Mihić, L.; Cvitanović, H.; Djaković, I.; Kuna, M.; Šešerko, A. The Influence of Psychological Stress on HPV Infection Manifestations and Carcinogenesis. Cell Physiol. Biochem. 2021, 55, 71–88. [Google Scholar]
- Gaab, J.; Sonderegger, L.; Scherrer, S.; Ehlert, U. Psychoneuroendocrine Effects of Cognitive-Behavioral Stress Management in a Naturalistic Setting—A Randomized Controlled Trial. Psychoneuroendocrinology 2006, 31, 428–438. [Google Scholar] [CrossRef]
- Ivković, N.; Božović, Đ.; Račić, M.; Popović-Grubač, D.; Davidović, B. Biomarkers of Stress in Saliva. Acta Fac. Med. Naissensis 2015, 32, 91–99. [Google Scholar] [CrossRef]
- McGregor, B.A.; Murphy, K.M.; Albano, D.L.; Ceballos, R.M. Stress, Cortisol, and B Lymphocytes: A Novel Approach to Understanding Academic Stress and Immune Function. Stress 2016, 19, 185–191. [Google Scholar] [CrossRef] [PubMed]
- Ng, V.; Koh, D.; Mok, B.Y.Y.; Chia, S.-E.; Lim, L.-P. Salivary Biomarkers Associated with Academic Assessment Stress among Dental Undergraduates. J. Dent. Educ. 2003, 67, 1091–1094. [Google Scholar] [CrossRef] [PubMed]
- de Quervain, D.; Schwabe, L.; Roozendaal, B. Stress, Glucocorticoids and Memory: Implications for Treating Fear-Related Disorders. Nat. Rev. Neurosci. 2016, 18, 7–19. [Google Scholar] [CrossRef] [PubMed]
- Langer, K.; Wolf, O.T.; Jentsch, V.L. Delayed Effects of Acute Stress on Cognitive Emotion Regulation. Psychoneuroendocrinology 2021, 125, 105101. [Google Scholar] [CrossRef]
- Benham, G.; Nash, M.R.; Baldwin, D.R. A Comparison of Changes in Secretory Immunoglobulin a Following a Stress-Inducing and Stress-Reducing Task. Stress Health 2009, 25, 81–90. [Google Scholar] [CrossRef]
- Lenaert, B.; Barry, T.J.; Schruers, K.; Vervliet, B.; Hermans, D. Emotional Attentional Control Predicts Changes in Diurnal Cortisol Secretion Following Exposure to a Prolonged Psychosocial Stressor. Psychoneuroendocrinology 2016, 63, 291–295. [Google Scholar] [CrossRef]
- Leistner, C.; Menke, A. Hypothalamic-Pituitary-Adrenal Axis and Stress. Chapter 4: Sex Differences in Neurology and Psychiatry. In Handbook of Clinical Neurology; Lanzenberger, R.G.S., Kranz, G.S., Savic, I., Eds.; Elsevier, B.V.: Amsterdam, The Netherlands, 2020; Volume 175, pp. 55–64. [Google Scholar] [CrossRef]
- Lelou, E.; Corlu, A.; Nesseler, N.; Rauch, C.; Mallédant, Y.; Seguin, P.; Aninat, C. The Role of Catecholamines in Pathophysiological Liver Processes. Cells 2022, 11, 1021. [Google Scholar] [CrossRef]
- Jones, B.J.; Tan, T.; Bloom, S.R. Minireview: Glucagon in Stress and Energy Homeostasis. Endocrinology 2012, 153, 1049–1054. [Google Scholar] [CrossRef]
- Knowles, S.R.; Nelson, E.A.; Palombo, E.A. Investigating the Role of Perceived Stress on Bacterial Flora Activity and Salivary Cortisol Secretion: A Possible Mechanism Underlying Susceptibility to Illness. Biol. Psychol. 2008, 77, 132–137. [Google Scholar] [CrossRef]
- McKerrow, I.; Carney, P.A.; Caretta-Weyer, H.; Furnari, M.; Miller Juve, A. Trends in Medical Students’ Stress, Physical, and Emotional Health throughout Training. Med. Educ. Online 2020, 25, 1709278. [Google Scholar] [CrossRef] [PubMed]
- Lever-van Milligen, B.A.; Lamers, F.; Smit, J.H.; Penninx, B.W.J.H. Physiological Stress Markers, Mental Health and Objective Physical Function. J. Psychosom. Res. 2020, 133, 109996. [Google Scholar] [CrossRef] [PubMed]
- Deinzer, R.; Granrath, N.; Stuhl, H.; Twork, L.; Idel, H.; Waschul, B.; Herforth, A. Acute Stress Effects on Local IL-1β Responses to Pathogens in a Human in Vivo Model. Brain Behav. Immun. 2004, 18, 458–467. [Google Scholar] [CrossRef]
- Hamidovic, A.; Van Hedger, K.; Choi, S.H.; Flowers, S.; Wardle, M.; Childs, E. Quantitative Meta-Analysis of Heart Rate Variability Finds Reduced Parasympathetic Cardiac Tone in Women Compared to Men during Laboratory-Based Social Stress. Neurosci. Biobehav. Rev. 2020, 114, 194–200. [Google Scholar] [CrossRef]
- Sze, Y.; Brunton, P.J. Sex, Stress and Steroids. Eur. J. Neurosci. 2019, 52, 2487–2515. [Google Scholar] [CrossRef] [PubMed]
- Helbig, S.; Backhaus, J. Sex Differences in a Real Academic Stressor, Cognitive Appraisal and the Cortisol Response. Physiol. Behav. 2017, 179, 67–74. [Google Scholar] [CrossRef] [PubMed]
- Kamezaki, Y.; Katsuura, S.; Kuwano, Y.; Tanahashi, T.; Rokutan, K. Circulating Cytokine Signatures in Healthy Medical Students Exposed to Academic Examination Stress. Psychophysiology 2012, 49, 991–997. [Google Scholar] [CrossRef]
- Schoofs, D.; Hartmann, R.; Wolf, O.T. Neuroendocrine Stress Responses to an Oral Academic Examination: No Strong Influence of Sex, Repeated Participation and Personality Traits. Stress 2008, 11, 52–61. [Google Scholar] [CrossRef]
- Sangiorgio, J.P.M.; Seixas, G.F.; De Paula Ramos, S.; Dezan-Garbelini, C.C. Salivary Levels of SIgA and Perceived Stress among Dental Students. J. Health Biol. Sci. 2017, 6, 9. [Google Scholar] [CrossRef]
- Cvitanović, H.; Milošević, M.; Bukvić-Bešlić, I.; Lugović-Mihić, L. Determination of Psychological Stress, Serum Immune Parameters, and Cortisol Levels in Patients with Human Papilloma Virus. Clin. Ther. 2020, 42, 783–799. [Google Scholar] [CrossRef]
- Pondeljak, N.; Lugović-Mihić, L. Stress-Induced Interaction of Skin Immune Cells, Hormones, and Neurotransmitters. Clin. Ther. 2020, 42, 757–770. [Google Scholar] [CrossRef] [PubMed]
- Jemmott, J.B.; Magloire, K. Academic Stress, Social Support, and Secretory Immunoglobulin A. J. Pers. Soc. Psychol. 1988, 55, 803–810. [Google Scholar] [CrossRef] [PubMed]
- Dantzer, R.; O’Connor, J.C.; Freund, G.G.; Johnson, R.W.; Kelley, K.W. From Inflammation to Sickness and Depression: When the Immune System Subjugates the Brain. Nat. Rev. Neurosci. 2008, 9, 46–56. [Google Scholar] [CrossRef] [PubMed]
- Barrett, T.J.; Corr, E.M.; van Solingen, C.; Schlamp, F.; Brown, E.J.; Koelwyn, G.J.; Lee, A.H.; Shanley, L.C.; Spruill, T.M.; Bozal, F.; et al. Chronic Stress Primes Innate Immune Responses in Mice and Humans. Cell Rep. 2021, 36, 109595. [Google Scholar] [CrossRef]
- Mössner, R.; Mikova, O.; Koutsilieri, E.; Saoud, M.; Ehlis, A.-C.; Müller, N.; Fallgatter, A.J.; Riederer, P. Consensus Paper of the WFSBP Task Force on Biological Markers: Biological Markers in Depression. World J. Biol. Psychiatry 2007, 8, 141–174. [Google Scholar] [CrossRef] [PubMed]
- Katsuura, S.; Kamezaki, Y.; Tominaga, K.; Masuda, K.; Nishida, K.; Yamamoto, Y.; Takeo, K.; Yamagishi, N.; Tanahashi, T.; Kawai, T. High-Throughput Screening of Brief Naturalistic Stress-Responsive Cytokines in University Students Taking Examinations. Int. J. Psychophysiol. 2010, 77, 135–140. [Google Scholar] [CrossRef] [PubMed]
- Zefferino, R.; Di Gioia, S.; Conese, M. Molecular Links between Endocrine, Nervous and Immune System during Chronic Stress. Brain Behav. 2020, 11, e01960. [Google Scholar] [CrossRef]
- DiSabato, D.J.; Nemeth, D.P.; Liu, X.; Witcher, K.G.; O’Neil, S.M.; Oliver, B.; Bray, C.E.; Sheridan, J.F.; Godbout, J.P.; Quan, N. Interleukin-1 Receptor on Hippocampal Neurons Drives Social Withdrawal and Cognitive Deficits after Chronic Social Stress. Mol. Psychiatry 2020, 26, 4770–4782. [Google Scholar] [CrossRef]
- Slavish, D.C.; Graham-Engeland, J.E.; Smyth, J.M.; Engeland, C.G. Salivary Markers of Inflammation in Response to Acute Stress. Brain Behav. Immun. 2015, 44, 253–269. [Google Scholar] [CrossRef]
- Auer, B.J.; Calvi, J.L.; Jordan, N.M.; Schrader, D.; Byrd-Craven, J. Communication and Social Interaction Anxiety Enhance Interleukin-1 Beta and Cortisol Reactivity during High-Stakes Public Speaking. Psychoneuroendocrinology 2018, 94, 83–90. [Google Scholar] [CrossRef]
- Buzgoova, K.; Balagova, L.; Marko, M.; Kapsdorfer, D.; Riecansky, I.; Jezova, D. Higher Perceived Stress Is Associated with Lower Cortisol Concentrations but Higher Salivary Interleukin-1beta in Socially Evaluated Cold Pressor Test. Stress 2019, 23, 1–8. [Google Scholar] [CrossRef]
- Gassen, J.; Makhanova, A.; Maner, J.K.; Plant, E.A.; Eckel, L.A.; Nikonova, L.; Prokosch, M.L.; Boehm, G.W.; Hill, S.E. Experimentally-Induced Inflammation Predicts Present Focus. Adapt. Hum. Behav. Physiol. 2019, 5, 148–163. [Google Scholar] [CrossRef]
- Lacey, K.; Zaharia, M.D.; Griffiths, J.; Ravindran, A.V.; Merali, Z.; Anisman, H. A Prospective Study of Neuroendocrine and Immune Alterations Associated with the Stress of an Oral Academic Examination among Graduate Students. Psychoneuroendocrinology 2000, 25, 339–356. [Google Scholar] [CrossRef]
- Szabo, Y.Z.; Slavish, D.C.; Graham-Engeland, J.E. The Effect of Acute Stress on Salivary Markers of Inflammation: A Systematic Review and Meta-Analysis. Brain Behav. Immun. 2020, 88, 887–900. [Google Scholar] [CrossRef] [PubMed]
- Quinn, M.E.; Stanton, C.H.; Slavich, G.M.; Joormann, J. Executive Control, Cytokine Reactivity to Social Stress, and Depressive Symptoms: Testing the Social Signal Transduction Theory of Depression. Stress 2019, 23, 1–9. [Google Scholar] [CrossRef]
- Shields, G.S.; Dunn, T.M.; Trainor, B.C.; Yonelinas, A.P. Determining the Biological Associates of Acute Cold Pressor Post-Encoding Stress Effects on Human Memory: The Role of Salivary Interleukin-1β. Brain Behav. Immun. 2019, 81, 178–187. [Google Scholar] [CrossRef]
- Gohel, V.; Jones, J.A.; Wehler, C.J. Salivary Biomarkers and Cardiovascular Disease: A Systematic Review. Clin. Chem. Lab. Med. 2018, 56, 1432–1442. [Google Scholar] [CrossRef]
- Chauhan, A.; Yadav, S.S.; Dwivedi, P.; Lal, N.; Usman, K.; Khattri, S. Correlation of Serum and Salivary Cytokines Level with Clinical Parameters in Metabolic Syndrome with Periodontitis. J. Clin. Lab. Anal. 2016, 30, 649–655. [Google Scholar] [CrossRef]
- Silvestre-Rangil, J.; Bagan, L.; Silvestre, F.; Martinez-Herrera, M.; Bagan, J. Periodontal, Salivary and IL-6 Status in Rheumatoid Arthritis Patients. A Cross-Sectional Study. Med. Oral. Patol. Oral. Cir. Bucal. 2017, 22, 595–600. [Google Scholar] [CrossRef]
- Ebersole, J.L.; Kryscio, R.J.; Campbell, C.; Kinane, D.F.; McDevitt, J.; Christodoulides, N.; Floriano, P.N.; Miller, C.S. Salivary and Serum Adiponectin and C-Reactive Protein Levels in Acute Myocardial Infarction Related to Body Mass Index and Oral Health. J. Periodontal. Res. 2016, 52, 419–427. [Google Scholar] [CrossRef]
- Weinstock, C.; Konig, D.; Harnischmacher, R.; Keul, J.; Berg, A.; Northoff, H. Effect of Exhaustive Exercise Stress on the Cytokine Response. Med. Sci. Sports Exerc. 1997, 29, 345–354. [Google Scholar] [CrossRef] [PubMed]
- Georgiou, K.E.; Dimov, R.K.; Boyanov, N.B.; Zografos, K.G.; Larentzakis, A.V.; Marinov, B.I. Feasibility of a New Wearable Device to Estimate Acute Stress in Novices during High-Fidelity Surgical Simulation. Folia Med. (Plovdiv) 2019, 61, 49–60. [Google Scholar] [CrossRef] [PubMed]
- Chojnowska, S.; Ptaszyńska-Sarosiek, I.; Kępka, A.; Knaś, M.; Waszkiewicz, N. Salivary Biomarkers of Stress, Anxiety and Depression. J. Clin. Med. 2021, 10, 517. [Google Scholar] [CrossRef] [PubMed]
- Michopoulos, V.; Norrholm, S.D.; Jovanovic, T. Diagnostic Biomarkers for Posttraumatic Stress Disorder: Promising Horizons from Translational Neuroscience Research. Biol. Psychiatry 2015, 78, 344–353. [Google Scholar] [CrossRef]
- Takahashi, A.; Flanigan, M.E.; McEwen, B.S.; Russo, S.J. Aggression, Social Stress, and the Immune System in Humans and Animal Models. Front. Behav. Neurosci. 2018, 12, 56. [Google Scholar] [CrossRef]
- Hefnawy, A.; Helal, M.A.Y.; Sabek, A.; Shousha, S. Clinical, Behavioral and Biochemical Alterations due to Shearing Stress in Ossimi Sheep. J. Vet. Med. Sci. 2018, 80, 1281–1286. [Google Scholar] [CrossRef]
- Fiksdal, A.; Hanlin, L.; Kuras, Y.; Gianferante, D.; Chen, X.; Thoma, M.V.; Rohleder, N. Associations between Symptoms of Depression and Anxiety and Cortisol Responses to and Recovery from Acute Stress. Psychoneuroendocrinology 2019, 102, 44–52. [Google Scholar] [CrossRef]
- Montero-López, E.; Santos-Ruiz, A.; González, R.; Navarrete-Navarrete, N.; Ortego-Centeno, N.; Martínez-Augustín, O.; Rodríguez-Blázquez, M.; Peralta-Ramírez, M.I. Analyses of Hair and Salivary Cortisol for Evaluating Hypothalamic-pituitary-adrenal Axis Activation in Patients with Autoimmune Disease. Stress 2017, 20, 541–548. [Google Scholar] [CrossRef]
- Bibbey, A.; Carroll, D.; Ginty, A.T.; Phillips, A.C. Cardiovascular and Cortisol Reactions to Acute Psychological Stress under Conditions of High versus Low Social Evaluative Threat. Psychosom. Med. 2015, 77, 599–608. [Google Scholar] [CrossRef]
- Hamer, M.; O’Donnell, K.; Lahiri, A.; Steptoe, A. Salivary Cortisol Responses to Mental Stress are Associated with Coronary Artery Calcification in Healthy Men and Women. Eur. Heart J. 2010, 31, 424–429. [Google Scholar] [CrossRef]
- Shah, B.; Ashok, L.; Sujatha, G.P. Evaluation of Salivary Cortisol and Psychological Factors in Patients with Oral Lichen Planus. Indian J. Dent. Res. 2009, 20, 288–292. [Google Scholar] [CrossRef] [PubMed]
- Messina, A.; Monda, V.; Sessa, F.; Valenzano, A.; Salerno, M.; Bitetti, I.; Precenzano, F.; Marotta, R.; Lavano, F.; Lavano, S.M.; et al. Sympathetic, Metabolic Adaptations, and Oxidative Stress in Autism Spectrum Disorders: How far from Physiology? Front. Physiol. 2018, 9, 261. [Google Scholar] [CrossRef] [PubMed]
- van der Reest, J.; Lilla, S.; Zheng, L.; Zanivan, S.; Gottlieb, E. Proteome-Wide Analysis of Cysteine Oxidation Reveals Metabolic Sensitivity to Redox Stress. Nat. Commun. 2018, 9, 1581. [Google Scholar] [CrossRef] [PubMed]
- Whongsiri, P.; Phoyen, S.; Boonla, C. Oxidative Stress in Urothelial Carcinogenesis: Measurements of Protein Carbonylation and Intracellular Production of Reactive Oxygen Species. Methods Mol. Biol. 2017, 1655, 109–117. [Google Scholar]
- Egawa, M.; Haze, S.; Gozu, Y.; Hosoi, J.; Onodera, T.; Tojo, Y.; Katsuyama, M.; Hara, Y.; Katagiri, C.; Inoue, N.; et al. Evaluation of Psychological Stress in Confined Environments Using Salivary, Skin, and Facial Image Parameters. Sci. Rep. 2018, 8, 8264. [Google Scholar] [CrossRef]
- Yehuda, R.; Daskalakis, N.P.; Bierer, L.M.; Bader, H.N.; Klengel, T.; Holsboer, F.; Binder, E.B. Holocaust Exposure Induced Intergenerational Effects on FKBP5 Methylation. Biol. Psychiatry 2016, 80, 372–380. [Google Scholar] [CrossRef]
- Meštrović-Štefekov, J.; Novak-Bilić, G.; Kuna, M.; Pap, N.; Lugović-Mihić, L. Psychological Stress in Patients with Atopic Dermatitis. Acta Dermatovenerol. Croat. 2018, 26, 297–303. [Google Scholar]
- Noushad, S.; Ahmed, S.; Ansari, B.; Mustafa, U.H.; Saleem, Y.; Hazrat, H. Physiological Biomarkers of Chronic Stress: A Systematic Review. Int. J. Health Sci. 2021, 15, 46. [Google Scholar]
- Jung, J.I.; Son, J.S.; Kim, Y.O.; Chae, C.H.; Kim, C.W.; Park, H.O.; Lee, J.H.; Shin, Y.H.; Ha, J.C. Changes of Depression and Job Stress in Workers after Merger without Downsizing. Ann. Occup. Environ. Med. 2018, 30, 54. [Google Scholar] [CrossRef]
- Viena, T.D.; Banks, J.B.; Barbu, I.M.; Schulman, A.H.; Tartar, J.L. Differential Effects of Mild Chronic Stress on Cortisol and S-IgA Responses to an Acute Stressor. Biol. Psychol. 2012, 91, 307–311. [Google Scholar] [CrossRef]
- Mocci, F.; Bullitta, M.A. Perception of Stress in the Nursing Profession: Study of the Behavior of s-IgA. G. Ital. Med. Lav. Ergon. 2006, 28, 219–221. [Google Scholar] [PubMed]
- Ali, N.; Nater, U.M. Salivary Alpha-Amylase as a Biomarker of Stress in Behavioral Medicine. Int. J. Behav. Med. 2020, 27, 337–342. [Google Scholar] [CrossRef] [PubMed]
- Suh, M. Salivary Cortisol Profile under Different Stressful Situations in Female College Students. J. Neurosci. Nurs. 2018, 50, 279–285. [Google Scholar] [CrossRef] [PubMed]
- Alsulami, S.; Al Omar, Z.; Binnwejim, M.S.; Alhamdan, F.; Aldrees, A.; Al-Bawardi, A.; Alsohim, M.; Alhabeeb, M. Perception of Academic Stress Among Health Science Preparatory Program students in Two Saudi Universities. Adv. Med. Educ. Pract. 2018, 12, 159–164. [Google Scholar] [CrossRef] [PubMed]
- Anwer, S.; Manzar, M.D.; Alghadir, A.H.; Salahuddin, M.; Abdul Hameed, U. Psychometric Analysis of the Perceived Stress Scale Among Healthy University Students. Neuropsychiatr. Dis. Treat. 2020, 16, 2389–2396. [Google Scholar] [CrossRef] [PubMed]
- Meštrović-Štefekov, J.; Lugović-Mihić, L.; Hanžek, M.; Bešlić, I.; Japundžić, I.; Karlović, D. Salivary Cortisol Values and Personality Features of Atopic Dermatitis Patients: A Prospective Study. Dermatitis 2022, 33, 341–348. [Google Scholar] [CrossRef]
- Bellagambi, F.G.; Degano, I.; Ghimenti, S.; Lomonaco, T.; Dini, V.; Romanelli, M.; Mastorci, F.; Gemignani, A.; Salvo, P.; Fuoco, R.; et al. Determination of Salivary α-amylase and Cortisol in Psoriatic Subjects Undergoing the Trier Social Stress Test. Microchem. J. 2018, 136, 177–184. [Google Scholar] [CrossRef]
- Lomonaco, T.; Ghimenti, S.; Biagini, D.; Bramanti, E.; Onor, M.; Bellagambi, F.G.; Fuoco, R.; Di Francesco, F. The Effect of Sampling Procedures on the Urate and Lactate Concentration in Oral Fluid. Microchem. J. 2018, 136, 255–262. [Google Scholar] [CrossRef]
- Alzahem, A.M.; van der Molen, H.T.; de Boer, B.J. Effect of Year of Study on Stress Levels in Male Undergraduate Dental Students. Adv. Med. Educ. Pract. 2013, 4, 217–222. [Google Scholar] [CrossRef]
- Bardi, M.; Koone, T.; Mewaldt, S.; O’Connor, K. Behavioral and Physiological Correlates of Stress Related to Examination Performance in College Chemistry Students. Stress 2011, 14, 557–566. [Google Scholar] [CrossRef]
- Pani, S.C.; Al Askar, A.M.; Al Mohrij, S.I.; Al Ohali, T.A. Evaluation of Stress in Final-Year Saudi Dental Students Using Salivary Cortisol as a Biomarker. J. Dent. Educ. 2011, 75, 377–384. [Google Scholar] [CrossRef] [PubMed]
- Cipra, C.; Müller-Hilke, B. Testing Anxiety in Undergraduate Medical Students and Its Correlation with Different Learning Approaches. PLoS ONE 2019, 14, e0210130. [Google Scholar] [CrossRef] [PubMed]
- Ringeisen, T.; Lichtenfeld, S.; Becker, S.; Minkley, N. Stress Experience and Performance during an Oral Exam: The Role of Self-Efficacy, Threat Appraisals, Anxiety, and Cortisol. Anxiety Stress Coping 2018, 32, 50–66. [Google Scholar] [CrossRef] [PubMed]
- Winkel, A.F.; Honart, A.W.; Robinson, A.; Jones, A.-A.; Squires, A. Thriving in Scrubs: A Qualitative Study of Resident Resilience. Reprod. Health 2018, 15, 53. [Google Scholar] [CrossRef] [PubMed]
- Glaser, R.; Kiecolt-Glaser, J.K. Stress-Induced Immune Dysfunction: Implications for Health. Nat. Rev. Immunol. 2005, 5, 243–251. [Google Scholar] [CrossRef]
- Kiecolt-Glaser, J.K.; Speicher, C.E.; Holliday, J.E.; Glaser, R. Stress and the Transformation of Lymphocytes by Epstein-Barr Virus. J. Behav. Med. 1984, 7, 1–12. [Google Scholar] [CrossRef]
- Manolova, M.S.; Stefanova, V.P.; Manchorova-Veleva, N.A.; Panayotov, I.V.; Levallois, B.; Tramini, P.; Orti, V. A Five-Year Comparative Study of Perceived Stress among Dental Students at Two European Faculties. Folia Med. 2019, 61, 134–142. [Google Scholar] [CrossRef]
- McClelland, D.C.; Ross, G.; Patel, V. The Effect of an Academic Examination on Salivary Norepinephrine and Immunoglobulin Levels. J. Human Stress 1985, 11, 52–59. [Google Scholar] [CrossRef]
- Humphris, G.; Blinkhorn, A.; Freeman, R.; Gorter, R.; Hoad-Reddick, G.; Murtomaa, H.; O’Sullivan, R.; Splieth, C. Psychological Stress in Undergraduate Dental Students: Baseline Results from Seven European Dental Schools. Eur. J. Dent. Educ. 2002, 6, 22–29. [Google Scholar] [CrossRef]
- Muirhead, V.; Locker, D. Canadian Dental Students Perceptions of Stress and Social Support. Eur. J. Dent. Educ. 2008, 12, 144–148. [Google Scholar] [CrossRef]
- Kaczor-Urbanowicz, K.E.; Martin Carreras-Presas, C.; Aro, K.; Tu, M.; Garcia-Godoy, F.; Wong, D.T. Saliva Diagnostics—Current Views and Directions. Exp. Biol. Med. 2017, 242, 459–472. [Google Scholar] [CrossRef] [PubMed]
| Research | Participants (N) | Analyzed Factors/Methods | Results |
|---|---|---|---|
| Bardi et al. (2011) Stress. 81 | 91 college chemistry students | Stress related to examination performance in students was analyzed by salivary cortisol and dehydroepiandrosterone (DHEA) levels (before and after every major test). Students’ displacement Activities (DAs) were videorecorded during every test. Achievement was objectively recorded using grade point averages (GPA), American College Testing (ACT) scores, and final class grades. | Displacement activities under stress and salivary cortisol and DHEA levels correctly predicted whether a student would pass the semester 90% of the time. However, the method could only correctly predict who would not pass the semester 52% of the time, which is insufficient for establishing a model. |
| Cipra et al. (2019) PLoS One. 83 | 212 medical students | Studying methods, anxiety data (STAI-T and ASSIST), and acute state anxiety (measured twice during the second term) were examined. Salivary cortisol was measured four times, and STAI-T was measured prior to the oral exams. | Surface learning approach significantly correlated with trait anxiety. Students with predominantly strategic learning methods had the most academic success with the least anxiety. |
| Gaab et al. (2006) Psychoneuroendocrinology. 10 | 28 healthy economics students | Effects of cognitive-behavioral stress management (CBSM) in a naturalistic setting (four times a week for eight weeks) compared to a waiting control condition. Salivary cortisol measurements (awakening response and short circadian profile) were taken multiple times and on exam day along with a cognitive appraisal. | Pre-exam period: CBSM group had lower anxiety levels and fewer physical symptoms. On exam day: controls had much lower cortisol levels. Different associations between pre-exam period cortisol responses and the cognitive stress appraisal were noted (no dissociation in CBSM group). Concentrations of short circadian cortisol remained the same between groups. |
| Helbig et al. (2017) Physiol. Behav. 27 | 46 college students | Salivary cortisol levels were measured before and after giving an oral presentation (stress condition) or while colleagues gave a presentation (control condition). A cognitive stress appraisal questionnaire and a stress and anxiety self-assessment were conducted beforehand. | Presentations led to sharp cortisol increases (as opposed to controls). Release of cortisol was not dependent on sex, but women had higher subjective feelings of stress and displayed unfavorable cognitive appraisals; men felt their own presentations posed a greater challenge than those of their colleagues. |
| Kamezaki et al. (2012) Psychophysiology. 28 | 28 fourth-year medical students | Salivary cortisol levels and 50 circulating immune mediators were analyzed in medical students exposed to academic examination stress at seven weeks prior to, pre- and post-exam day, and one week after the exam. | Significantly increased proinflammatory and Th2 cytokines levels, as well as β-nerve growth factor linked with sharp reduction in salivary cortisol levels and feelings of anxiety when the exam ended were recorded. |
| Katsuura et al. (2010) Int J Psychophysiology. 37 | 26 medical students | The effect of exams (a short naturalistic stressor) on cortisol levels, feelings of depression and anxiety, and values of 50 serum immune mediators (analyzed seven days prior to, immediately before, and two days after the exam). | Sharp reductions in serum MIF, MCP-3, and β-NGF levels (two days after exams), related to concomitant post-exam reductions in salivary cortisol and anxiety. Only MIF deltas were significant, which culminated when exams started (much more than pre- and post-exam period). |
| Lenaert et al. (2016) Psychoneuroendocrinology. 17 | 90 undergraduate students (71 returned for follow-up testing) | Attentional control of students was assessed (Emotional Attentional Control Scale), and salivary cortisol was measured, before and after exams (six weeks of research, [three weeks of preparation and three weeks of exams]. | Lower pre-exam self-perceived emotional attentional control levels predicted increased total diurnal cortisol secretion during stress, and a less pronounced drop post-exam day. Difficulty maintaining attention throughout prolonged stressful situations may lead to chronic HPA-axis hyperactivity. |
| McGregor et al. (2016) Stress. 12 | 22 first-year graduate students and 30 control participants from the community | Perceived stress, lymphocyte phenotype and salivary cortisol measured with the start of classes in autumn and in the week preceding spring examinations. | Students expressed greater distress than controls in all measures (excluding basal stress level). There was a correlation between student stress status and a significant decrease in CD19+ B lymphocytes and decreased cortisol awakening response (CAR). |
| Ng et al. (2003) J Dent Educ. 13 | 31 dental undergraduates | Students were surveyed (one-to-five rating questionnaire) before and after an hour-long written exam; their salivary cortisol, IgA and chromogranin A (CgA) were also measured. | Pre-exam, higher self-reported stress and cortisol levels were recorded. (No significant differences in IgA and CgA samples.) Pre-exam stress scores were associated with raised salivary cortisol but not IgA or CgA. Higher perceived stress levels among students generally resulted in worse exam results. |
| Ouda et al. (2016) J Clin Exp Pathol. 1 | 90 undergraduate students | Salivary stress biomarker levels [s-cortisol, salivary alpha-amylase (sAA), and IgA] were measured in undergraduate dental students (by ELISA) by collecting two saliva samples, one before and one after the exam. | A sharp upturn of salivary stress biomarkers was noted during the assessment (stress) phase (unlike in the non-assessment [rest] phase). A strong connection was seen between salivary α-amylase and success in the academic environment, especially in males and those finishing their studies. |
| Pani et al. (2011) J Dent Educ. 82 | 40 final-year dental students | Evaluation of stress using salivary cortisol (beginning of the semester, the final week of clinical practice, and 60 min before the final exam); adapted Displacement Activities (DAs) questionnaire. | Much higher cortisol levels were seen the final week of clinical practice (even higher during the pre-examination trial). Deviations may exist between reported feelings of stress and amount of stress exposed to during studies. |
| Ringeisen et al. (2019) Anxiety Stress Coping. 84 | 92 students | Assessment of self-belief, risk evaluation, contextual anxiety and cortisol levels on a control day preceding an oral exam by a week, and again on exam day (anxiety was tested three times). | Continually reducing anxiety was seen after the exam (greater anxiety led to sharper declines). A correlation between anxiety and cortisol levels could not be established. Self-belief showed opposite trends to risk assessment and anxiety levels on the control day. Higher risk assessments were linked with more anxiety. A steep decrease in anxiety on exam day led to increased performance. |
| Schoofs et al. (2008) Stress. 29 | 40 students (20 students participated in a second examination, one to four weeks later) | Measurement of cortisol and salivary alpha-amylase (sAA) on control day, as well as pre-exam and post-exam. Personality tests were also filled out. | A big increase in cortisol and sAA levels was found as a result of examination, with noticeable increases between the two measurements. No differences between the sexes or for oral contraceptive use were found. |
| Suh M. (2018) J Neurosci Nurs. 74 | 36 female college students | Salivary cortisol measured six times a day during a phase without exams and during a stressful phase; specificities in sleep quality and anxiety were measured by actigraph and STAI (Spielberger State-Trait Anxiety Inventory). | Students with heightened feelings of anxiety enjoyed better quality of sleep; subjects experiencing poor sleep had heightened cortisol secretion during waking hours. Subjects more prone to anxiety had greater cortisol levels during exams. |
| Viena et al. (2012) Biol Psychol. 71 | 30 undergraduate students | Effects of stress on cortisol and s-IgA responses were analyzed through/by two phases of research (four weeks before exams and during final exams). Students were tested between four and six PM (when cortisol secretion is low/decreasing [not at the circadian nadir]). Students completed the Perceived Stress Scale-10 (PSS-10) and other questionnaires during both study phases. | Acute stressors strongly increase salivary cortisol levels during stress-free phases, but not when a mild chronic stress is ongoing, where s-IgA levels showed an increase on both occasions. During continuous mild stress, perceived stress is reflected in a heightened cortisol response. |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2022 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Špiljak, B.; Vilibić, M.; Glavina, A.; Crnković, M.; Šešerko, A.; Lugović-Mihić, L. A Review of Psychological Stress among Students and Its Assessment Using Salivary Biomarkers. Behav. Sci. 2022, 12, 400. https://doi.org/10.3390/bs12100400
Špiljak B, Vilibić M, Glavina A, Crnković M, Šešerko A, Lugović-Mihić L. A Review of Psychological Stress among Students and Its Assessment Using Salivary Biomarkers. Behavioral Sciences. 2022; 12(10):400. https://doi.org/10.3390/bs12100400
Chicago/Turabian StyleŠpiljak, Bruno, Maja Vilibić, Ana Glavina, Marija Crnković, Ana Šešerko, and Liborija Lugović-Mihić. 2022. "A Review of Psychological Stress among Students and Its Assessment Using Salivary Biomarkers" Behavioral Sciences 12, no. 10: 400. https://doi.org/10.3390/bs12100400
APA StyleŠpiljak, B., Vilibić, M., Glavina, A., Crnković, M., Šešerko, A., & Lugović-Mihić, L. (2022). A Review of Psychological Stress among Students and Its Assessment Using Salivary Biomarkers. Behavioral Sciences, 12(10), 400. https://doi.org/10.3390/bs12100400







