The Functional Roles of Methionine and Arginine in Intestinal and Bone Health of Poultry: Review
Abstract
Simple Summary
Abstract
1. Introduction
2. Metabolism of Methionine and Arginine
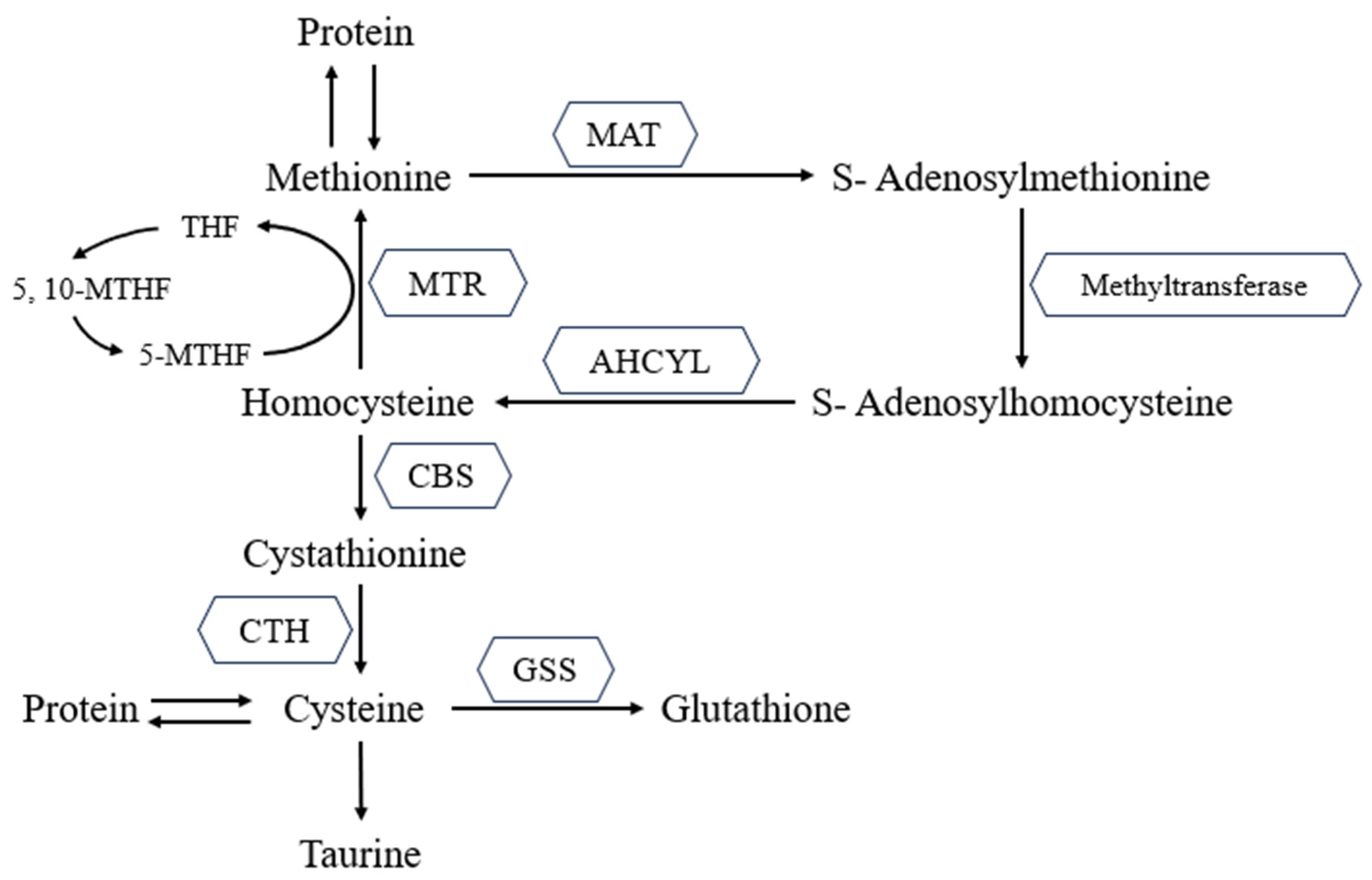
2.1. Methionine Metabolism
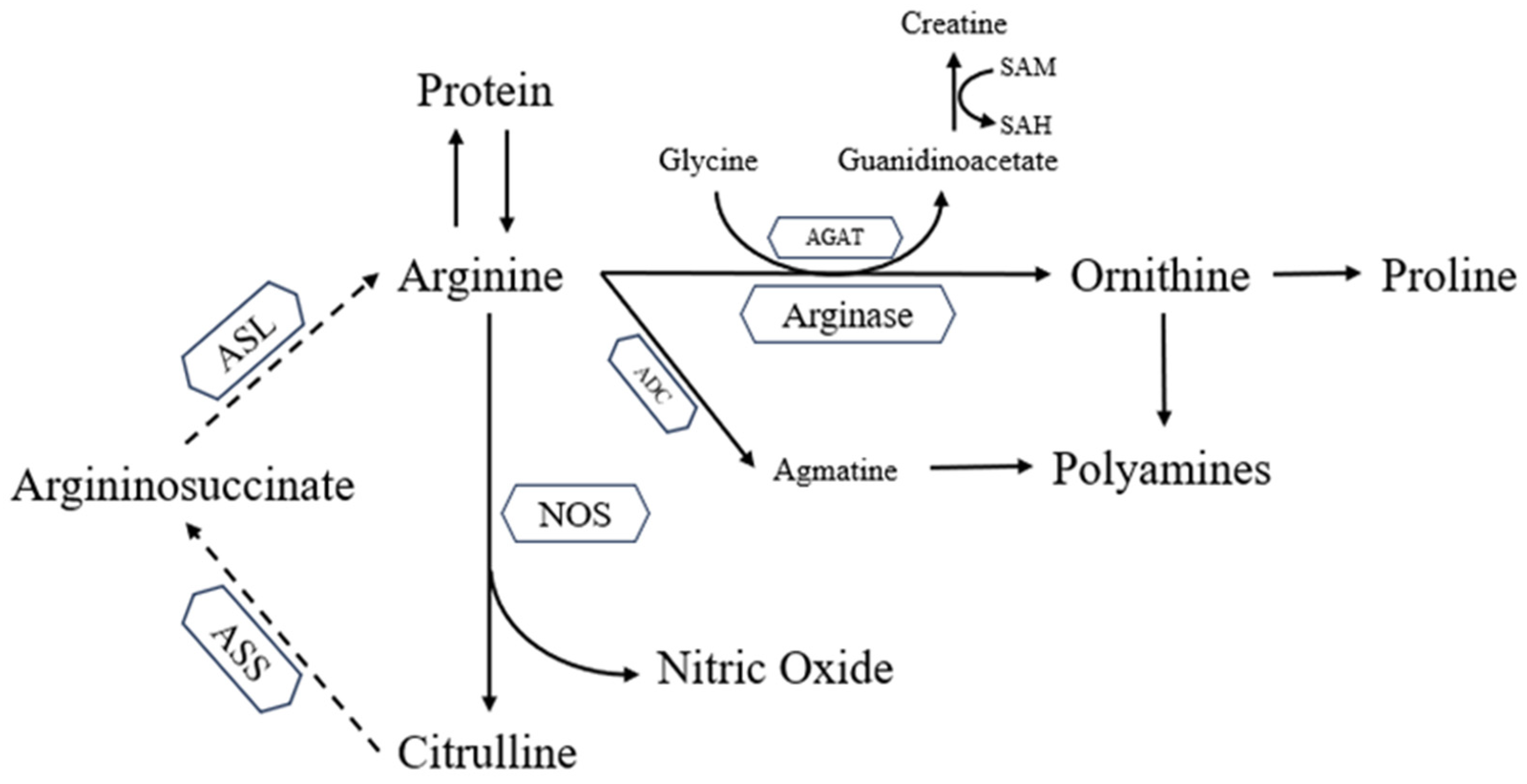
2.2. Arginine Metabolism
3. Methionine and Arginine in Intestinal Health
3.1. Methionine and Arginine in Intestinal Development and Repair
3.2. Antioxidant Effects of Methionine and Arginine on Intestinal Health
3.2.1. Oxidative Stress
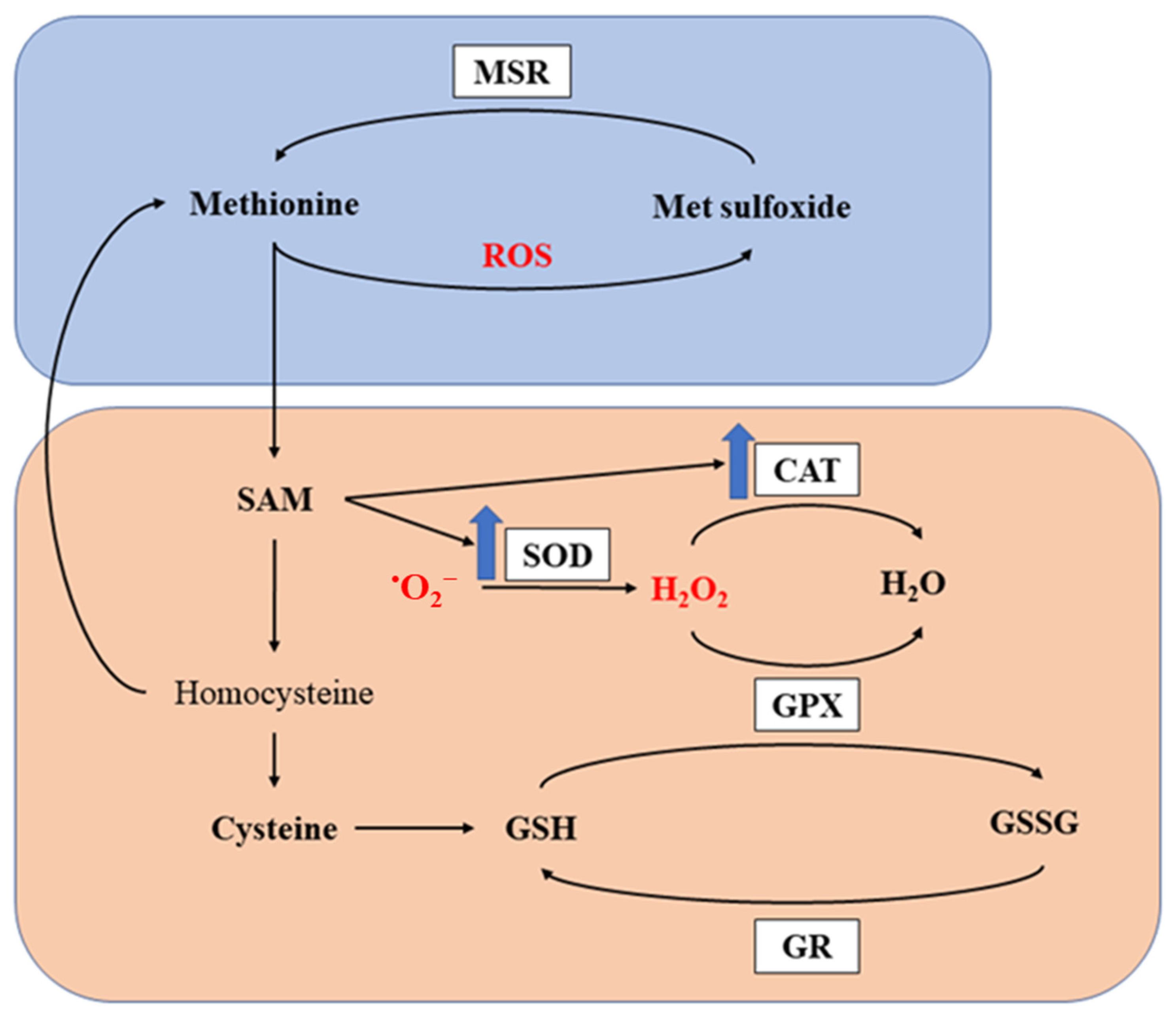
3.2.2. Antioxidant Effects of Methionine and Arginine
3.3. Methionine and Arginine in the Immune System
3.4. Methionine and Arginine in the Intestinal Microbiome
4. Methionine and Arginine in Bone Health
4.1. Bone Formation, Growth and Remodeling
4.2. Methionine and Arginine in Bone Metabolism
4.3. Oxidative Stress, Intestinal Health and Bone Health
4.4. Methionine and Arginine Effects on Bone Health in Different Growth Periods
5. Potential Risks of Excessive Methionine and Arginine
6. Conclusions
Author Contributions
Funding
Conflicts of Interest
References
- Henchion, M.; Hayes, M.; Mullen, A.M.; Fenelon, M.; Tiwari, B. Future Protein Supply and Demand: Strategies and Factors Influencing a Sustainable Equilibrium. Foods 2017, 6, 53. [Google Scholar] [CrossRef]
- Ravindran, V.; Abdollahi, M.R. Nutrition and Digestive Physiology of the Broiler Chick: State of the Art and Outlook. Animals 2021, 11, 2795. [Google Scholar] [CrossRef]
- Takiishi, T.; Fenero, C.I.M.; Câmara, N.O.S. Intestinal barrier and gut microbiota: Shaping our immune responses throughout life. Tissue Barriers 2017, 5, e1373208. [Google Scholar] [CrossRef]
- Adedokun, S.A.; Olojede, O.C. Optimizing Gastrointestinal Integrity in Poultry: The Role of Nutrients and Feed Additives. Front. Vet. Sci. 2018, 5, 348. [Google Scholar] [CrossRef]
- Ruth, M.R.; Field, C.J. The immune modifying effects of amino acids on gut-associated lymphoid tissue. J. Anim. Sci. Biotechnol. 2013, 4, 27. [Google Scholar] [CrossRef]
- Yegani, M.; Korver, D.R. Factors affecting intestinal health in poultry. Poult. Sci. 2008, 87, 2052–2063. [Google Scholar] [CrossRef]
- Alizadeh, M.; Shojadoost, B.; Boodhoo, N.; Astill, J.; Taha-Abdelaziz, K.; Hodgins, D.C.; Kulkarni, R.R.; Sharif, S. Necrotic enteritis in chickens: A review of pathogenesis, immune responses and prevention, focusing on probiotics and vaccination. Anim. Health Res. Rev. 2021, 22, 147–162. [Google Scholar] [CrossRef]
- Blake, D.P.; Knox, J.; Dehaeck, B.; Huntington, B.; Rathinam, T.; Ravipati, V.; Ayoade, S.; Gilbert, W.; Adebambo, A.O.; Jatau, I.D.; et al. Re-calculating the cost of coccidiosis in chickens. Vet. Res. 2020, 51, 115. [Google Scholar] [CrossRef]
- Cervantes, H.M. Antibiotic-free poultry production: Is it sustainable? J. Appl. Poult. Res. 2015, 24, 91–97. [Google Scholar] [CrossRef]
- Kolakshyapati, M.; Flavel, R.J.; Sibanda, T.Z.; Schneider, D.; Welch, M.C.; Ruhnke, I. Various bone parameters are positively correlated with hen body weight while range access has no beneficial effect on tibia health of free-range layers. Poult. Sci. 2019, 98, 6241–6250. [Google Scholar] [CrossRef]
- Sharma, M.K.; Regmi, P.; Applegate, T.; Chai, L.; Kim, W.K. Osteoimmunology: A Link between Gastrointestinal Diseases and Skeletal Health in Chickens. Animals 2023, 13, 1816. [Google Scholar] [CrossRef]
- Bradshaw, R.; Kirkden, R.; Broom, D. A review of the aetiology and pathology of leg weakness in broilers in relation to welfare. Avian Poult. Biol. Rev. 2002, 13, 45–104. [Google Scholar] [CrossRef]
- Kierończyk, B.; Rawski, M.; Józefiak, D.; Świątkiewicz, S. Infectious and non-infectious factors associated with leg disorders in poultry—A review. Ann. Anim. Sci. 2017, 17, 645–669. [Google Scholar]
- Wu, G. Amino acids: Metabolism, functions, and nutrition. Amino Acids 2009, 37, 1–17. [Google Scholar] [CrossRef]
- Castro, F.L.d.S.; Kim, W.K. Secondary Functions of Arginine and Sulfur Amino Acids in Poultry Health: Review. Animals 2020, 10, 2106. [Google Scholar] [CrossRef]
- Bunchasak, C. Role of dietary methionine in poultry production. J. Poult. Sci. 2009, 46, 169–179. [Google Scholar] [CrossRef]
- Sasaki, J.; Nakashima, N. Methionine-independent initiation of translation in the capsid protein of an insect RNA virus. Proc. Natl. Acad. Sci. USA 2000, 97, 1512–1515. [Google Scholar] [CrossRef]
- Brosnan, J.T.; Brosnan, M.E.; Bertolo, R.F.P.; Brunton, J.A. Methionine: A metabolically unique amino acid. Livest. Sci. 2007, 112, 2–7. [Google Scholar] [CrossRef]
- Martínez, Y.; Li, X.; Liu, G.; Bin, P.; Yan, W.; Más, D.; Valdivié, M.; Hu, C.-A.A.; Ren, W.; Yin, Y. The role of methionine on metabolism, oxidative stress, and diseases. Amino Acids 2017, 49, 2091–2098. [Google Scholar] [CrossRef]
- Levine, R.L.; Moskovitz, J.; Stadtman, E.R. Oxidation of methionine in proteins: Roles in antioxidant defense and cellular regulation. IUBMB Life 2000, 50, 301–307. [Google Scholar] [CrossRef]
- Liu, G.; Ajao, A.M.; Shanmugasundaram, R.; Taylor, J.; Ball, E.; Applegate, T.J.; Selvaraj, R.; Kyriazakis, I.; Olukosi, O.A.; Kim, W.K. The effects of arginine and branched-chain amino acid supplementation to reduced-protein diet on intestinal health, cecal short-chain fatty acid profiles, and immune response in broiler chickens challenged with Eimeria spp. Poult. Sci. 2023, 102, 102773. [Google Scholar] [CrossRef]
- Abdukalykova, S.; Zhao, X.; Ruiz-Feria, C. Arginine and vitamin E modulate the subpopulations of T lymphocytes in broiler chickens. Poult. Sci. 2008, 87, 50–55. [Google Scholar] [CrossRef]
- Lee, J.; Austic, R.; Naqi, S.; Golemboski, K.; Dietert, R. Dietary arginine intake alters avian leukocyte population distribution during infectious bronchitis challenge. Poult. Sci. 2002, 81, 793–798. [Google Scholar] [CrossRef]
- Khajali, F.; Wideman, R. Dietary arginine: Metabolic, environmental, immunological and physiological interrelationships. World’s Poult. Sci. J. 2010, 66, 751–766. [Google Scholar] [CrossRef]
- Popovic, P.J.; Zeh, H.J.; Ochoa, J.B. Arginine and Immunity123. J. Nutr. 2007, 137, 1681S–1686S. [Google Scholar] [CrossRef]
- Teng, P.-Y.; Liu, G.; Choi, J.; Yadav, S.; Wei, F.; Kim, W.K. Effects of levels of methionine supplementations in forms of L- or DL-methionine on the performance, intestinal development, immune response, and antioxidant system in broilers challenged with Eimeria spp. Poult. Sci. 2023, 102, 102586. [Google Scholar] [CrossRef]
- Lai, A.; Yuan, Z.; Wang, Z.; Chen, B.; Zhi, L.; Huang, Z.; Zhang, Y. Dietary Methionine Increased the Growth Performances and Immune Function of Partridge Shank Broilers after Challenged with Coccidia. Animals 2023, 13, 613. [Google Scholar] [CrossRef]
- Khatlab, A.d.S.; Del Vesco, A.P.; de Oliveira Neto, A.R.; Fernandes, R.P.M.; Gasparino, E. Dietary supplementation with free methionine or methionine dipeptide mitigates intestinal oxidative stress induced by Eimeria spp. challenge in broiler chickens. J. Anim. Sci. Biotechnol. 2019, 10, 58. [Google Scholar] [CrossRef]
- Miao, Z.Q.; Dong, Y.Y.; Qin, X.; Yuan, J.M.; Han, M.M.; Zhang, K.K.; Shi, S.R.; Song, X.Y.; Zhang, J.Z.; Li, J.H. Dietary supplementation of methionine mitigates oxidative stress in broilers under high stocking density. Poult. Sci. 2021, 100, 101231. [Google Scholar] [CrossRef]
- Del Vesco, A.P.; Khatlab, A.d.S.; Santana, T.P.; Pozza, P.C.; Menck Soares, M.A.; Brito, C.O.; Barbosa, L.T.; Gasparino, E. Heat stress effect on the intestinal epithelial function of broilers fed methionine supplementation. Livest. Sci. 2020, 240, 104152. [Google Scholar] [CrossRef]
- Shen, Y.B.; Ferket, P.; Park, I.; Malheiros, R.D.; Kim, S.W. Effects of feed grade L-methionine on intestinal redox status, intestinal development, and growth performance of young chickens compared with conventional DL-methionine. J. Anim. Sci. 2015, 93, 2977–2986. [Google Scholar] [CrossRef] [PubMed]
- Zhong, C.; Tong, D.Q.; Zhang, Y.R.; Wang, X.Q.; Yan, H.C.; Tan, H.Z.; Gao, C.Q. (DL)-methionine and (DL)-methionyl-(DL)-methionine increase intestinal development and activate Wnt/β-catenin signaling activity in domestic pigeons (Columba livia). Poult. Sci. 2022, 101, 101644. [Google Scholar] [CrossRef] [PubMed]
- Wu, B.; Li, L.; Ruan, T.; Peng, X. Effect of methionine deficiency on duodenal and jejunal IgA(+) B cell count and immunoglobulin level of broilers. Iran. J. Vet. Res. 2018, 19, 165–171. [Google Scholar]
- Zhang, B.; Lv, Z.; Li, Z.; Wang, W.; Li, G.; Guo, Y. Dietary l-arginine Supplementation Alleviates the Intestinal Injury and Modulates the Gut Microbiota in Broiler Chickens Challenged by Clostridium perfringens. Front. Microbiol. 2018, 9, 1716. [Google Scholar] [CrossRef]
- Ruan, D.; Fouad, A.M.; Fan, Q.L.; Huo, X.H.; Kuang, Z.X.; Wang, H.; Guo, C.Y.; Deng, Y.F.; Zhang, C.; Zhang, J.H.; et al. Dietary L-arginine supplementation enhances growth performance, intestinal antioxidative capacity, immunity and modulates gut microbiota in yellow-feathered chickens. Poult. Sci. 2020, 99, 6935–6945. [Google Scholar] [CrossRef]
- Castro, F.L.S.; Teng, P.-Y.; Yadav, S.; Gould, R.L.; Craig, S.; Pazdro, R.; Kim, W.K. The effects of L-Arginine supplementation on growth performance and intestinal health of broiler chickens challenged with Eimeria spp. Poult. Sci. 2020, 99, 5844–5857. [Google Scholar] [CrossRef] [PubMed]
- Duan, X.; Li, F.; Mou, S.; Feng, J.; Liu, P.; Xu, L. Effects of dietary L-arginine on laying performance and anti-oxidant capacity of broiler breeder hens, eggs, and offspring during the late laying period. Poult. Sci. 2015, 94, 2938–2943. [Google Scholar] [CrossRef]
- Zhang, H.; Zhang, Y.; Liu, X.; Elsabagh, M.; Yu, Y.; Peng, A.; Dai, S.; Wang, H. L-Arginine inhibits hydrogen peroxide-induced oxidative damage and inflammatory response by regulating antioxidant capacity in ovine intestinal epithelial cells. Ital. J. Anim. Sci. 2021, 20, 1620–1632. [Google Scholar] [CrossRef]
- Tan, J.; Applegate, T.J.; Liu, S.; Guo, Y.; Eicher, S.D. Supplemental dietary l-arginine attenuates intestinal mucosal disruption during a coccidial vaccine challenge in broiler chickens. Br. J. Nutr. 2014, 112, 1098–1109. [Google Scholar] [CrossRef]
- Laika, M.; Jahanian, R. Increase in dietary arginine level could ameliorate detrimental impacts of coccidial infection in broiler chickens. Livest. Sci. 2017, 195, 38–44. [Google Scholar] [CrossRef]
- Vijayan, V.; Khandelwal, M.; Manglani, K.; Gupta, S.; Surolia, A. Methionine down-regulates TLR4/MyD88/NF-κB signalling in osteoclast precursors to reduce bone loss during osteoporosis. Br. J. Pharmacol. 2014, 171, 107–121. [Google Scholar] [CrossRef]
- Ouattara, A.; Cooke, D.; Gopalakrishnan, R.; Huang, T.H.; Ables, G.P. Methionine restriction alters bone morphology and affects osteoblast differentiation. Bone Rep. 2016, 5, 33–42. [Google Scholar] [CrossRef]
- Plummer, J.; Park, M.; Perodin, F.; Horowitz, M.C.; Hens, J.R. Methionine-Restricted Diet Increases miRNAs That Can Target RUNX2 Expression and Alters Bone Structure in Young Mice. J. Cell. Biochem. 2017, 118, 31–42. [Google Scholar] [CrossRef]
- Castro, F.L.S.; Su, S.; Choi, H.; Koo, E.; Kim, W.K. L-Arginine supplementation enhances growth performance, lean muscle, and bone density but not fat in broiler chickens. Poult. Sci. 2019, 98, 1716–1722. [Google Scholar] [CrossRef]
- Huh, J.-E.; Choi, J.-Y.; Shin, Y.-O.; Park, D.-S.; Kang, J.W.; Nam, D.; Choi, D.-Y.; Lee, J.-D. Arginine Enhances Osteoblastogenesis and Inhibits Adipogenesis through the Regulation of Wnt and NFATc Signaling in Human Mesenchymal Stem Cells. Int. J. Mol. Sci. 2014, 15, 13010–13029. [Google Scholar] [CrossRef]
- Ravindran, V.; Bryden, W.L. Amino acid availability in poultry—In vitro and in vivo measurements. Aust. J. Agric. Res. 1999, 50, 889–908. [Google Scholar] [CrossRef]
- Zhang, S.; Gilbert, E.R.; Saremi, B.; Wong, E.A. Supplemental methionine sources have a neutral impact on oxidative status in broiler chickens. J. Anim. Physiol. Anim. Nutr. 2018, 102, 1274–1283. [Google Scholar] [CrossRef]
- Wu, G.; Fang, Y.-Z.; Yang, S.; Lupton, J.R.; Turner, N.D. Glutathione Metabolism and Its Implications for Health. J. Nutr. 2004, 134, 489–492. [Google Scholar] [CrossRef]
- Wang, S.-T.; Chen, H.-W.; Sheen, L.-Y.; Lii, C.-K. Methionine and Cysteine Affect Glutathione Level, Glutathione-Related Enzyme Activities and the Expression of Glutathione S-Transferase Isozymes in Rat Hepatocytes. J. Nutr. 1997, 127, 2135–2141. [Google Scholar] [CrossRef]
- Stipanuk, M.H.; Ueki, I. Dealing with methionine/homocysteine sulfur: Cysteine metabolism to taurine and inorganic sulfur. J. Inherit. Metab. Dis. 2011, 34, 17–32. [Google Scholar] [CrossRef]
- Wu, G.; Morris, S.M., Jr. Arginine metabolism: Nitric oxide and beyond. Biochem. J. 1998, 336, 1–17. [Google Scholar] [CrossRef]
- Tamir, H.; Ratner, S. Enzymes of arginine metabolism in chicks. Arch. Biochem. Biophys. 1963, 102, 249–258. [Google Scholar] [CrossRef]
- Rath, M.; Müller, I.; Kropf, P.; Closs, E.I.; Munder, M. Metabolism via Arginase or Nitric Oxide Synthase: Two Competing Arginine Pathways in Macrophages. Front. Immunol. 2014, 5, 532. [Google Scholar] [CrossRef]
- Stechmiller, J.K.; Childress, B.; Cowan, L. Arginine Supplementation and Wound Healing. Nutr. Clin. Pract. 2005, 20, 52–61. [Google Scholar] [CrossRef]
- Albaugh, V.L.; Mukherjee, K.; Barbul, A. Proline Precursors and Collagen Synthesis: Biochemical Challenges of Nutrient Supplementation and Wound Healing. J. Nutr. 2017, 147, 2011–2017. [Google Scholar] [CrossRef]
- Arike, L.; Seiman, A.; van der Post, S.; Rodriguez Piñeiro, A.M.; Ermund, A.; Schütte, A.; Bäckhed, F.; Johansson, M.E.V.; Hansson, G.C. Protein Turnover in Epithelial Cells and Mucus along the Gastrointestinal Tract Is Coordinated by the Spatial Location and Microbiota. Cell Rep. 2020, 30, 1077–1087.e73. [Google Scholar] [CrossRef] [PubMed]
- Saxton, R.A.; Sabatini, D.M. mTOR Signaling in Growth, Metabolism, and Disease. Cell 2017, 168, 960–976. [Google Scholar] [CrossRef]
- Kong, X.; Tan, B.; Yin, Y.; Gao, H.; Li, X.; Jaeger, L.A.; Bazer, F.W.; Wu, G. l-Arginine stimulates the mTOR signaling pathway and protein synthesis in porcine trophectoderm cells. J. Nutr. Biochem. 2012, 23, 1178–1183. [Google Scholar] [CrossRef]
- Kitada, M.; Xu, J.; Ogura, Y.; Monno, I.; Koya, D. Mechanism of Activation of Mechanistic Target of Rapamycin Complex 1 by Methionine. Front. Cell Dev. Biol. 2020, 8, 715. [Google Scholar] [CrossRef]
- Takahara, T.; Amemiya, Y.; Sugiyama, R.; Maki, M.; Shibata, H. Amino acid-dependent control of mTORC1 signaling: A variety of regulatory modes. J. Biomed. Sci. 2020, 27, 87. [Google Scholar] [CrossRef]
- Carroll, B.; Maetzel, D.; Maddocks, O.D.; Otten, G.; Ratcliff, M.; Smith, G.R.; Dunlop, E.A.; Passos, J.F.; Davies, O.R.; Jaenisch, R.; et al. Control of TSC2-Rheb signaling axis by arginine regulates mTORC1 activity. eLife 2016, 5, e11058. [Google Scholar] [CrossRef]
- Sampson, L.L.; Davis, A.K.; Grogg, M.W.; Zheng, Y. mTOR disruption causes intestinal epithelial cell defects and intestinal atrophy postinjury in mice. FASEB J. 2016, 30, 1263–1275. [Google Scholar] [CrossRef]
- Guan, Y.; Zhang, L.; Li, X.; Zhang, X.; Liu, S.; Gao, N.; Li, L.; Gao, G.; Wei, G.; Chen, Z. Repression of mammalian target of rapamycin complex 1 inhibits intestinal regeneration in acute inflammatory bowel disease models. J. Immunol. 2015, 195, 339–346. [Google Scholar] [CrossRef]
- Clevers, H.; Nusse, R. Wnt/β-catenin signaling and disease. Cell 2012, 149, 1192–1205. [Google Scholar] [CrossRef]
- Ootani, A.; Li, X.; Sangiorgi, E.; Ho, Q.T.; Ueno, H.; Toda, S.; Sugihara, H.; Fujimoto, K.; Weissman, I.L.; Capecchi, M.R. Sustained in vitro intestinal epithelial culture within a Wnt-dependent stem cell niche. Nat. Med. 2009, 15, 701–706. [Google Scholar] [CrossRef]
- Schuijers, J.; Junker, J.P.; Mokry, M.; Hatzis, P.; Koo, B.-K.; Sasselli, V.; Van Der Flier, L.G.; Cuppen, E.; Van Oudenaarden, A.; Clevers, H. Ascl2 acts as an R-spondin/Wnt-responsive switch to control stemness in intestinal crypts. Cell Stem Cell 2015, 16, 158–170. [Google Scholar] [CrossRef]
- Hou, Q.; Dong, Y.; Huang, J.; Liao, C.; Lei, J.; Wang, Y.; Lai, Y.; Bian, Y.; He, Y.; Sun, J.; et al. Exogenous L-arginine increases intestinal stem cell function through CD90+ stromal cells producing mTORC1-induced Wnt2b. Commun. Biol. 2020, 3, 611. [Google Scholar] [CrossRef]
- Albrecht, L.V.; Bui, M.H.; De Robertis, E.M. Canonical Wnt is inhibited by targeting one-carbon metabolism through methotrexate or methionine deprivation. Proc. Natl. Acad. Sci. USA 2019, 116, 2987–2995. [Google Scholar] [CrossRef]
- Du, Q.; Zhang, X.; Liu, Q.; Zhang, X.; Bartels, C.E.; Geller, D.A. Nitric oxide production upregulates Wnt/β-catenin signaling by inhibiting Dickkopf-1. Cancer Res. 2013, 73, 6526–6537. [Google Scholar] [CrossRef]
- Bikkavilli, R.K.; Malbon, C.C. Arginine methylation of G3BP1 in response to Wnt3a regulates β-catenin mRNA. J. Cell Sci. 2011, 124, 2310–2320. [Google Scholar] [CrossRef]
- Larqué, E.; Sabater-Molina, M.; Zamora, S. Biological significance of dietary polyamines. Nutrition 2007, 23, 87–95. [Google Scholar] [CrossRef]
- Sánchez-Jiménez, F.; Medina, M.Á.; Villalobos-Rueda, L.; Urdiales, J.L. Polyamines in mammalian pathophysiology. Cell. Mol. Life Sci. 2019, 76, 3987–4008. [Google Scholar] [CrossRef]
- McCORMACK, S.A.; Viar, M.J.; Johnson, L.R. Polyamines are necessary for cell migration by a small intestinal crypt cell line. Am. J. Physiol.-Gastrointest. Liver Physiol. 1993, 264, G367–G374. [Google Scholar] [CrossRef] [PubMed]
- Lan, A.; Blachier, F.; Benamouzig, R.; Beaumont, M.; Barrat, C.; Coelho, D.; Lancha, A., Jr.; Kong, X.; Yin, Y.; Marie, J.-C. Mucosal healing in inflammatory bowel diseases: Is there a place for nutritional supplementation? Inflamm. Bowel Dis. 2015, 21, 198–207. [Google Scholar] [CrossRef]
- Wang, J.-Y.; Johnson, L.R. Polyamines and ornithine decarboxylase during repair of duodenal mucosa after stress in rats. Gastroenterology 1991, 100, 333–343. [Google Scholar] [CrossRef]
- Wang, J.-Y.; McCormack, S.; Viar, M.; Johnson, L. Stimulation of proximal small intestinal mucosal growth by luminal polyamines. Am. J. Physiol.-Gastrointest. Liver Physiol. 1991, 261, G504–G511. [Google Scholar] [CrossRef]
- Wang, J.-Y. Polyamines and mRNA stability in regulation of intestinal mucosal growth. Amino Acids 2007, 33, 241–252. [Google Scholar] [CrossRef]
- Guo, X.; Rao, J.N.; Liu, L.; Zou, T.-T.; Turner, D.J.; Bass, B.L.; Wang, J.-Y. Regulation of adherens junctions and epithelial paracellular permeability: A novel function for polyamines. Am. J. Physiol.-Cell Physiol. 2003, 285, C1174–C1187. [Google Scholar] [CrossRef]
- Timmons, J.; Chang, E.T.; Wang, J.Y.; Rao, J.N. Polyamines and Gut Mucosal Homeostasis. J. Gastrointest. Dig. Syst. 2012, 2, 001. [Google Scholar] [CrossRef]
- Zhu, H.; Jia, Z.; Misra, H.; Li, Y.R. Oxidative stress and redox signaling mechanisms of alcoholic liver disease: Updated experimental and clinical evidence. J. Dig. Dis. 2012, 13, 133–142. [Google Scholar] [CrossRef]
- Zhang, J.; Wang, X.; Vikash, V.; Ye, Q.; Wu, D.; Liu, Y.; Dong, W. ROS and ROS-Mediated Cellular Signaling. Oxidative Med. Cell. Longev. 2016, 2016, 4350965. [Google Scholar] [CrossRef]
- Matés, J.M.; Pérez-Gómez, C.; Núñez de Castro, I. Antioxidant enzymes and human diseases. Clin. Biochem. 1999, 32, 595–603. [Google Scholar] [CrossRef]
- Liu, G.; Magnuson, A.D.; Sun, T.; Tolba, S.A.; Starkey, C.; Whelan, R.; Lei, X.G. Supplemental methionine exerted chemical form-dependent effects on antioxidant status, inflammation-related gene expression, and fatty acid profiles of broiler chicks raised at high ambient temperature1. J. Anim. Sci. 2019, 97, 4883–4894. [Google Scholar] [CrossRef]
- Magnuson, A.D.; Liu, G.; Sun, T.; Tolba, S.A.; Xi, L.; Whelan, R.; Lei, X.G. Supplemental methionine and stocking density affect antioxidant status, fatty acid profiles, and growth performance of broiler chickens. J. Anim. Sci. 2020, 98, skaa092. [Google Scholar] [CrossRef]
- Sharma, M.K.; Liu, G.; White, D.L.; Tompkins, Y.H.; Kim, W.K. Effects of mixed Eimeria challenge on performance, body composition, intestinal health, and expression of nutrient transporter genes of Hy-Line W-36 pullets (0–6 wks of age). Poult. Sci. 2022, 101, 102083. [Google Scholar] [CrossRef]
- Rao, R. Oxidative stress-induced disruption of epithelial and endothelial tight junctions. Front. Biosci. J. Virtual Libr. 2008, 13, 7210–7226. [Google Scholar] [CrossRef]
- Mishra, B.; Jha, R. Oxidative Stress in the Poultry Gut: Potential Challenges and Interventions. Front. Vet. Sci. 2019, 6, 60. [Google Scholar] [CrossRef]
- Wang, Y.; Chen, Y.; Zhang, X.; Lu, Y.; Chen, H. New insights in intestinal oxidative stress damage and the health intervention effects of nutrients: A review. J. Funct. Foods 2020, 75, 104248. [Google Scholar] [CrossRef]
- He, X.; Lu, Z.; Ma, B.; Zhang, L.; Li, J.; Jiang, Y.; Zhou, G.; Gao, F. Effects of chronic heat exposure on growth performance, intestinal epithelial histology, appetite-related hormones and genes expression in broilers. J. Sci. Food Agric. 2018, 98, 4471–4478. [Google Scholar] [CrossRef]
- Burkholder, K.; Thompson, K.; Einstein, M.; Applegate, T.; Patterson, J. Influence of stressors on normal intestinal microbiota, intestinal morphology, and susceptibility to Salmonella enteritidis colonization in broilers. Poult. Sci. 2008, 87, 1734–1741. [Google Scholar] [CrossRef]
- Lozano-Sepulveda, S.A.; Bautista-Osorio, E.; Merino-Mascorro, J.A.; Varela-Rey, M.; Muñoz-Espinosa, L.E.; Cordero-Perez, P.; Martinez-Chantar, M.L.; Rivas-Estilla, A.M. S-adenosyl-L-methionine modifies antioxidant-enzymes, glutathione-biosynthesis and methionine adenosyltransferases-1/2 in hepatitis C virus-expressing cells. World J. Gastroenterol. 2016, 22, 3746–3757. [Google Scholar] [CrossRef]
- Kachungwa Lugata, J.; Ortega, A.D.S.V.; Szabó, C. The Role of Methionine Supplementation on Oxidative Stress and Antioxidant Status of Poultry-A Review. Agriculture 2022, 12, 1701. [Google Scholar] [CrossRef]
- Del Vesco, A.P.; Gasparino, E.; Grieser, D.O.; Zancanela, V.; Gasparin, F.R.; Constantin, J.; Oliveira Neto, A.R. Effects of methionine supplementation on the redox state of acute heat stress-exposed quails. J. Anim. Sci. 2014, 92, 806–815. [Google Scholar] [CrossRef]
- Del Vesco, A.P.; Gasparino, E.; de Oliveira Grieser, D.; Zancanela, V.; Soares, M.A.M.; de Oliveira Neto, A.R. Effects of methionine supplementation on the expression of oxidative stress-related genes in acute heat stress-exposed broilers. Br. J. Nutr. 2015, 113, 549–559. [Google Scholar] [CrossRef]
- Kalvandi, O.; Sadeghi, A.; Karimi, A. Methionine supplementation improves reproductive performance, antioxidant status, immunity and maternal antibody transmission in breeder Japanese quail under heat stress conditions. Arch. Anim. Breed. 2019, 62, 275–286. [Google Scholar] [CrossRef]
- Reda, F.M.; Swelum, A.A.; Hussein, E.O.; Elnesr, S.S.; Alhimaidi, A.R.; Alagawany, M. Effects of varying dietary DL-methionine levels on productive and reproductive performance, egg quality, and blood biochemical parameters of quail breeders. Animals 2020, 10, 1839. [Google Scholar] [CrossRef]
- Chen, Y.; Chen, X.; Zhang, H.; Zhou, Y. Effects of dietary concentrations of methionine on growth performance and oxidative status of broiler chickens with different hatching weight. Br. Poult. Sci. 2013, 54, 531–537. [Google Scholar] [CrossRef]
- Ruan, T.; Li, L.; Lyu, Y.; Luo, Q.; Wu, B. Effect of methionine deficiency on oxidative stress and apoptosis in the small intestine of broilers. Acta Vet. Hung. 2018, 66, 52–65. [Google Scholar] [CrossRef]
- Chang, Y.; Tang, H.; Zhang, Z.; Yang, T.; Wu, B.; Zhao, H.; Liu, G.; Chen, X.; Tian, G.; Cai, J. Zinc methionine improves the growth performance of meat ducks by enhancing the antioxidant capacity and intestinal barrier function. Front. Vet. Sci. 2022, 9, 774160. [Google Scholar] [CrossRef]
- Shin, S.H.; Yoon, H.; Chun, Y.S.; Shin, H.W.; Lee, M.N.; Oh, G.T.; Park, J.W. Arrest defective 1 regulates the oxidative stress response in human cells and mice by acetylating methionine sulfoxide reductase A. Cell Death Dis. 2014, 5, e1490. [Google Scholar] [CrossRef]
- Moskovitz, J. Methionine sulfoxide reductases: Ubiquitous enzymes involved in antioxidant defense, protein regulation, and prevention of aging-associated diseases. Biochim. Biophys. Acta 2005, 1703, 213–219. [Google Scholar] [CrossRef] [PubMed]
- El-Sheikh, N.M.; Khalil, F.A. l-Arginine and l-glutamine as immunonutrients and modulating agents for oxidative stress and toxicity induced by sodium nitrite in rats. Food Chem. Toxicol. 2011, 49, 758–762. [Google Scholar] [CrossRef]
- Liang, M.; Wang, Z.; Li, H.; Cai, L.; Pan, J.; He, H.; Wu, Q.; Tang, Y.; Ma, J.; Yang, L. l-Arginine induces antioxidant response to prevent oxidative stress via stimulation of glutathione synthesis and activation of Nrf2 pathway. Food Chem. Toxicol. 2018, 115, 315–328. [Google Scholar] [CrossRef] [PubMed]
- Wang, Z.; Liang, M.; Li, H.; Cai, L.; He, H.; Wu, Q.; Yang, L. l-Methionine activates Nrf2-ARE pathway to induce endogenous antioxidant activity for depressing ROS-derived oxidative stress in growing rats. J. Sci. Food Agric. 2019, 99, 4849–4862. [Google Scholar] [CrossRef] [PubMed]
- Kasahara, Y. Intraepithelial lymphocytes in birds. Adv. Host Def. Mech. 1994, 37, 163–174. [Google Scholar]
- Smith, A.L.; Powers, C.; Beal, R.K. Chapter 13—The Avian Enteric Immune System in Health and Disease. In Avian Immunology, 2nd ed.; Schat, K.A., Kaspers, B., Kaiser, P., Eds.; Academic Press: Boston, MA, USA, 2014; pp. 227–250. [Google Scholar] [CrossRef]
- Ruan, T.; Li, L.; Peng, X.; Wu, B. Effects of methionine on the immune function in animals. Health 2017, 9, 857–869. [Google Scholar] [CrossRef][Green Version]
- Takahashi, K.; Konashi, S.; Akiba, Y.; Horiguchi, M. Effects of marginal excess or deficiency of dietary methionine on antibody production in growing broilers. Anim. Sci. Technol. 1993, 64, 13–19. [Google Scholar]
- Zhao, T.; Lum, J.J. Methionine cycle-dependent regulation of T cells in cancer immunity. Front. Oncol. 2022, 12, 969563. [Google Scholar] [CrossRef]
- Sinclair, L.V.; Howden, A.J.M.; Brenes, A.; Spinelli, L.; Hukelmann, J.L.; Macintyre, A.N.; Liu, X.; Thomson, S.; Taylor, P.M.; Rathmell, J.C.; et al. Antigen receptor control of methionine metabolism in T cells. eLife 2019, 8, e44210. [Google Scholar] [CrossRef] [PubMed]
- Klein Geltink, R.I.; Pearce, E.L. The importance of methionine metabolism. eLife 2019, 8, e47221. [Google Scholar] [CrossRef]
- Swain, B.K.; Johri, T.S. Effect of supplemental methionine, choline and their combinations on the performance and immune response of broilers. Br. Poult. Sci. 2000, 41, 83–88. [Google Scholar] [CrossRef]
- Mirzaaghatabar, F.; Saki, A.A.; Zamani, P.; Aliarabi, H.; Hemati Matin, H.R. Effect of different levels of diet methionine and metabolisable energy on broiler performance and immune system. Food Agric. Immunol. 2011, 22, 93–103. [Google Scholar] [CrossRef]
- Bouyeh, M. Effect of Excess Lysine and Methionine on Immune system and Performance of Broilers. Ann. Biol. Res. 2012, 3, 3218–3224. [Google Scholar]
- Wu, B.; Cui, H.; Peng, X.; Fang, J.; Cui, W.; Liu, X. Pathology of bursae of Fabricius in methionine-deficient broiler chickens. Nutrients 2013, 5, 877–886. [Google Scholar] [CrossRef] [PubMed]
- Wu, B.-y.; Cui, H.-m.; Peng, X.; Fang, J.; Cui, W.; Liu, X.-d. Effect of Methionine Deficiency on the Thymus and the Subsets and Proliferation of Peripheral Blood T-Cell, and Serum IL-2 Contents in Broilers. J. Integr. Agric. 2012, 11, 1009–1019. [Google Scholar] [CrossRef]
- Li, P.; Yin, Y.-L.; Li, D.; Woo Kim, S.; Wu, G. Amino acids and immune function. Br. J. Nutr. 2007, 98, 237–252. [Google Scholar] [CrossRef]
- Durante, W.; Johnson, F.K.; Johnson, R.A. Arginase: A critical regulator of nitric oxide synthesis and vascular function. Clin. Exp. Pharmacol. Physiol. 2007, 34, 906–911. [Google Scholar] [CrossRef]
- Bogdan, C. Nitric oxide and the immune response. Nat. Immunol. 2001, 2, 907–916. [Google Scholar] [CrossRef] [PubMed]
- Bogdan, C. Nitric oxide synthase in innate and adaptive immunity: An update. Trends Immunol. 2015, 36, 161–178. [Google Scholar] [CrossRef]
- James, S.L. Role of nitric oxide in parasitic infections. Microbiol. Rev. 1995, 59, 533–547. [Google Scholar] [CrossRef]
- Gradoni, L.; Ascenzi, P. Nitric oxide and anti-protozoan chemotherapy. Parassitologia 2004, 46, 101–103. [Google Scholar]
- Rodriguez, P.C.; Zea, A.H.; Culotta, K.S.; Zabaleta, J.; Ochoa, J.B.; Ochoa, A.C. Regulation of t cell receptor cd3ζ chain expression byl-arginine. J. Biol. Chem. 2002, 277, 21123–21129. [Google Scholar] [CrossRef]
- Oakley, B.B.; Lillehoj, H.S.; Kogut, M.H.; Kim, W.K.; Maurer, J.J.; Pedroso, A.; Lee, M.D.; Collett, S.R.; Johnson, T.J.; Cox, N.A. The chicken gastrointestinal microbiome. FEMS Microbiol. Lett. 2014, 360, 100–112. [Google Scholar] [CrossRef]
- Diaz Carrasco, J.M.; Casanova, N.A.; Fernández Miyakawa, M.E. Microbiota, gut health and chicken productivity: What is the connection? Microorganisms 2019, 7, 374. [Google Scholar] [CrossRef]
- Dunkley, K.; Dunkley, C.; Njongmeta, N.; Callaway, T.; Hume, M.; Kubena, L.; Nisbet, D.; Ricke, S. Comparison of in vitro fermentation and molecular microbial profiles of high-fiber feed substrates incubated with chicken cecal inocula. Poult. Sci. 2007, 86, 801–810. [Google Scholar] [CrossRef] [PubMed]
- Hou, K.; Wu, Z.-X.; Chen, X.-Y.; Wang, J.-Q.; Zhang, D.; Xiao, C.; Zhu, D.; Koya, J.B.; Wei, L.; Li, J.; et al. Microbiota in health and diseases. Signal Transduct. Target. Ther. 2022, 7, 135. [Google Scholar] [CrossRef]
- Pan, D.; Yu, Z. Intestinal microbiome of poultry and its interaction with host and diet. Gut Microbes 2014, 5, 108–119. [Google Scholar] [CrossRef]
- Zhang, B.; Li, G.; Shahid, M.S.; Gan, L.; Fan, H.; Lv, Z.; Yan, S.; Guo, Y. Dietary l-arginine supplementation ameliorates inflammatory response and alters gut microbiota composition in broiler chickens infected with Salmonella enterica serovar Typhimurium. Poult. Sci. 2020, 99, 1862–1874. [Google Scholar] [CrossRef]
- Brugaletta, G.; Zampiga, M.; Laghi, L.; Indio, V.; Oliveri, C.; De Cesare, A.; Sirri, F. Feeding broiler chickens with arginine above recommended levels: Effects on growth performance, metabolism, and intestinal microbiota. J. Anim. Sci. Biotechnol. 2023, 14, 33. [Google Scholar] [CrossRef]
- Kumar, S.; Adhikari, P.; Oakley, B.; Kim, W.K. Changes in cecum microbial community in response to total sulfur amino acid (TSAA: DL-methionine) in antibiotic-free and supplemented poultry birds. Poult. Sci. 2019, 98, 5809–5819. [Google Scholar] [CrossRef] [PubMed]
- Wu, X.; Han, Z.; Liu, B.; Yu, D.; Sun, J.; Ge, L.; Tang, W.; Liu, S. Gut microbiota contributes to the methionine metabolism in host. Front. Microbiol. 2022, 13, 1065668. [Google Scholar] [CrossRef]
- Whitehead, C.C. Overview of bone biology in the egg-laying hen. Poult. Sci. 2004, 83, 193–199. [Google Scholar] [CrossRef]
- Fujisawa, R.; Tamura, M. Acidic bone matrix proteins and their roles in calcification. Front. Biosci.-Landmark 2012, 17, 1891–1903. [Google Scholar] [CrossRef]
- Zhu, Y.S.; Gu, Y.; Jiang, C.; Chen, L. Osteonectin regulates the extracellular matrix mineralization of osteoblasts through P38 signaling pathway. J. Cell. Physiol. 2020, 235, 2220–2231. [Google Scholar] [CrossRef] [PubMed]
- Blair, H.C.; Larrouture, Q.C.; Li, Y.; Lin, H.; Beer-Stoltz, D.; Liu, L.; Tuan, R.S.; Robinson, L.J.; Schlesinger, P.H.; Nelson, D.J. Osteoblast Differentiation and Bone Matrix Formation In Vivo and In Vitro. Tissue Eng. Part B Rev. 2017, 23, 268–280. [Google Scholar] [CrossRef]
- Mackie, E.J.; Ahmed, Y.A.; Tatarczuch, L.; Chen, K.S.; Mirams, M. Endochondral ossification: How cartilage is converted into bone in the developing skeleton. Int. J. Biochem. Cell Biol. 2008, 40, 46–62. [Google Scholar] [CrossRef]
- Allen, M.R.; Burr, D.B. Chapter 4—Bone Modeling and Remodeling. In Basic and Applied Bone Biology; Burr, D.B., Allen, M.R., Eds.; Academic Press: San Diego, CA, USA, 2014; pp. 75–90. [Google Scholar] [CrossRef]
- Delaisse, J.M. The reversal phase of the bone-remodeling cycle: Cellular prerequisites for coupling resorption and formation. Bonekey Rep. 2014, 3, 561. [Google Scholar] [CrossRef]
- Hadjidakis, D.J.; Androulakis, I.I. Bone remodeling. Ann. N. Y. Acad. Sci. 2006, 1092, 385–396. [Google Scholar] [CrossRef]
- Mammoli, F.; Castiglioni, S.; Parenti, S.; Cappadone, C.; Farruggia, G.; Iotti, S.; Davalli, P.; Maier, J.A.M.; Grande, A.; Frassineti, C. Magnesium Is a Key Regulator of the Balance between Osteoclast and Osteoblast Differentiation in the Presence of Vitamin D3. Int. J. Mol. Sci. 2019, 20, 385. [Google Scholar] [CrossRef]
- Morris, H.A.; O’Loughlin, P.D.; Anderson, P.H. Experimental evidence for the effects of calcium and vitamin D on bone: A review. Nutrients 2010, 2, 1026–1035. [Google Scholar] [CrossRef]
- Park, J.K.; Lee, E.M.; Kim, A.Y.; Lee, E.J.; Min, C.W.; Kang, K.K.; Lee, M.M.; Jeong, K.S. Vitamin C deficiency accelerates bone loss inducing an increase in PPAR-γ expression in SMP30 knockout mice. Int. J. Exp. Pathol. 2012, 93, 332–340. [Google Scholar] [CrossRef] [PubMed]
- Devignes, C.-S.; Carmeliet, G.; Stegen, S. Amino acid metabolism in skeletal cells. Bone Rep. 2022, 17, 101620. [Google Scholar] [CrossRef]
- Lv, Z.; Shi, W.; Zhang, Q. Role of Essential Amino Acids in Age-Induced Bone Loss. Int. J. Mol. Sci. 2022, 23, 11281. [Google Scholar] [CrossRef]
- Fang, C.C.; Feng, L.; Jiang, W.D.; Wu, P.; Liu, Y.; Kuang, S.Y.; Tang, L.; Liu, X.A.; Zhou, X.Q. Effects of dietary methionine on growth performance, muscle nutritive deposition, muscle fibre growth and type I collagen synthesis of on-growing grass carp (Ctenopharyngodon idella). Br. J. Nutr. 2021, 126, 321–336. [Google Scholar] [CrossRef] [PubMed]
- Van’T Hof, R.J.; Ralston, S.H. Nitric oxide and bone. Immunology 2001, 103, 255–261. [Google Scholar] [CrossRef]
- Grassi, F.; Fan, X.; Rahnert, J.; Weitzmann, M.N.; Pacifici, R.; Nanes, M.S.; Rubin, J. Bone Re/Modeling Is More Dynamic in the Endothelial Nitric Oxide Synthase(−/−) Mouse. Endocrinology 2006, 147, 4392–4399. [Google Scholar] [CrossRef]
- Aguirre, J.; Buttery, L.; O’Shaughnessy, M.; Afzal, F.; de Marticorena, I.F.; Hukkanen, M.; Huang, P.; MacIntyre, I.; Polak, J. Endothelial nitric oxide synthase gene-deficient mice demonstrate marked retardation in postnatal bone formation, reduced bone volume, and defects in osteoblast maturation and activity. Am. J. Pathol. 2001, 158, 247–257. [Google Scholar] [CrossRef]
- Armour, K.E.; Armour, K.J.; Gallagher, M.E.; Gödecke, A.; Helfrich, M.H.; Reid, D.M.; Ralston, S.H. Defective bone formation and anabolic response to exogenous estrogen in mice with targeted disruption of endothelial nitric oxide synthase. Endocrinology 2001, 142, 760–766. [Google Scholar] [CrossRef] [PubMed]
- Hukkanen, M.; Platts, L.; Lawes, T.; Girgis, S.; Konttinen, Y.T.; Goodship, A.; MacIntyre, I.; Polak, J.M. Effect of nitric oxide donor nitroglycerin on bone mineral density in a rat model of estrogen deficiency-induced osteopenia. Bone 2003, 32, 142–149. [Google Scholar] [CrossRef]
- Pouwels, S.; Lalmohamed, A.; van Staa, T.; Cooper, C.; Souverein, P.; Leufkens, H.G.; Rejnmark, L.; de Boer, A.; Vestergaard, P.; de Vries, F. Use of organic nitrates and the risk of hip fracture: A population-based case-control study. J. Clin. Endocrinol. Metab. 2010, 95, 1924–1931. [Google Scholar] [CrossRef] [PubMed]
- Wimalawansa, S.J. Nitroglycerin therapy is as efficacious as standard estrogen replacement therapy (Premarin) in prevention of oophorectomy-induced bone loss: A human pilot clinical study. J. Bone Miner. Res. 2000, 15, 2240–2244. [Google Scholar] [CrossRef]
- Jin, Z.; Kho, J.; Dawson, B.; Jiang, M.-M.; Chen, Y.; Ali, S.; Burrage, L.C.; Grover, M.; Palmer, D.J.; Turner, D.L.; et al. Nitric oxide modulates bone anabolism through regulation of osteoblast glycolysis and differentiation. J. Clin. Investig. 2021, 131, e138935. [Google Scholar] [CrossRef]
- Dao, H.T.; Moss, A.F.; Bradbury, E.J.; Swick, R.A. Effects of L-arginine, guanidinoacetic acid and L-citrulline supplementation in reduced-protein diets on bone morphology and mineralization of laying hens. Anim. Nutr. 2023, 14, 225–234. [Google Scholar] [CrossRef]
- Pennisi, P.; D’Alcamo, M.A.; Leonetti, C.; Clementi, A.; Cutuli, V.M.; Riccobene, S.; Parisi, N.; Fiore, C.E. Supplementation of L-arginine prevents glucocorticoid-induced reduction of bone growth and bone turnover abnormalities in a growing rat model. J. Bone Miner. Metab. 2005, 23, 134–139. [Google Scholar] [CrossRef]
- Wauquier, F.; Leotoing, L.; Coxam, V.; Guicheux, J.; Wittrant, Y. Oxidative stress in bone remodelling and disease. Trends Mol. Med. 2009, 15, 468–477. [Google Scholar] [CrossRef]
- Domazetovic, V.; Marcucci, G.; Iantomasi, T.; Brandi, M.L.; Vincenzini, M.T. Oxidative stress in bone remodeling: Role of antioxidants. Clin. Cases Miner. Bone Metab. 2017, 14, 209–216. [Google Scholar] [CrossRef]
- Romagnoli, C.; Marcucci, G.; Favilli, F.; Zonefrati, R.; Mavilia, C.; Galli, G.; Tanini, A.; Iantomasi, T.; Brandi, M.L.; Vincenzini, M.T. Role of GSH/GSSG redox couple in osteogenic activity and osteoclastogenic markers of human osteoblast-like Sa OS-2 cells. FEBS J. 2013, 280, 867–879. [Google Scholar]
- Tompkins, Y.H.; Choi, J.; Teng, P.-Y.; Yamada, M.; Sugiyama, T.; Kim, W.K. Reduced bone formation and increased bone resorption drive bone loss in Eimeria infected broilers. Sci. Rep. 2023, 13, 616. [Google Scholar] [CrossRef]
- Tompkins, Y.H.; Liu, G.; Kim, W.K. Impact of exogenous hydrogen peroxide on osteogenic differentiation of broiler chicken compact bones derived mesenchymal stem cells. Front. Physiol. 2023, 14, 1124355. [Google Scholar] [CrossRef]
- Tompkins, Y.; Liu, G.; Marshall, B.; Sharma, M.K.; Kim, W.K. Effect of Hydrogen Oxide-Induced Oxidative Stress on Bone Formation in the Early Embryonic Development Stage of Chicken. Biomolecules 2023, 13, 154. [Google Scholar] [CrossRef]
- Altindag, O.; Erel, O.; Soran, N.; Celik, H.; Selek, S. Total oxidative/anti-oxidative status and relation to bone mineral density in osteoporosis. Rheumatol. Int. 2008, 28, 317–321. [Google Scholar] [CrossRef]
- Yossepowitch, O.; Pinchuk, I.; Gur, U.; Neumann, A.; Lichtenberg, D.; Baniel, J. Advanced but not localized prostate cancer is associated with increased oxidative stress. J. Urol. 2007, 178, 1238–1244. [Google Scholar] [CrossRef]
- Kabuyama, Y.; Kitamura, T.; Yamaki, J.; Homma, M.K.; Kikuchi, S.-i.; Homma, Y. Involvement of thioredoxin reductase 1 in the regulation of redox balance and viability of rheumatoid synovial cells. Biochem. Biophys. Res. Commun. 2008, 367, 491–496. [Google Scholar] [CrossRef]
- Lean, J.M.; Davies, J.T.; Fuller, K.; Jagger, C.J.; Kirstein, B.; Partington, G.A.; Urry, Z.L.; Chambers, T.J. A crucial role for thiol antioxidants in estrogen-deficiency bone loss. J. Clin. Investig. 2003, 112, 915–923. [Google Scholar] [CrossRef]
- Polat, B.; Halici, Z.; Cadirci, E.; Albayrak, A.; Karakus, E.; Bayir, Y.; Bilen, H.; Sahin, A.; Yuksel, T.N. The effect of alpha-lipoic acid in ovariectomy and inflammation-mediated osteoporosis on the skeletal status of rat bone. Eur. J. Pharmacol. 2013, 718, 469–474. [Google Scholar] [CrossRef] [PubMed]
- Jun, J.H.; Lee, S.H.; Kwak, H.B.; Lee, Z.H.; Seo, S.B.; Woo, K.M.; Ryoo, H.M.; Kim, G.S.; Baek, J.H. N-acetylcysteine stimulates osteoblastic differentiation of mouse calvarial cells. J. Cell. Biochem. 2008, 103, 1246–1255. [Google Scholar] [CrossRef]
- Zhou, A.; Wu, B.; Yu, H.; Tang, Y.; Liu, J.; Jia, Y.; Yang, X.; Xiang, L. Current Understanding of Osteoimmunology in Certain Osteoimmune Diseases. Front. Cell Dev. Biol. 2021, 9, 698068. [Google Scholar] [CrossRef]
- Hou, Q.; Huang, J.; Ayansola, H.; Masatoshi, H.; Zhang, B. Intestinal Stem Cells and Immune Cell Relationships: Potential Therapeutic Targets for Inflammatory Bowel Diseases. Front. Immunol. 2021, 11, 623691. [Google Scholar] [CrossRef]
- Shi, H.; Wang, J.; Teng, P.-Y.; Tompkins, Y.H.; Jordan, B.; Kim, W.K. Effects of phytase and coccidial vaccine on growth performance, nutrient digestibility, bone mineralization, and intestinal gene expression of broilers. Poult. Sci. 2022, 101, 102124. [Google Scholar] [CrossRef]
- Tompkins, Y.; Teng, P.; Pazdro, R.; Kim, W. Long bone mineral loss, bone microstructural changes and oxidative stress after Eimeria challenge in broilers. Front. Physiol. 2022, 13, 945740. [Google Scholar] [CrossRef]
- Oikeh, I.; Sakkas, P.; Blake, D.P.; Kyriazakis, I. Interactions between dietary calcium and phosphorus level, and vitamin D source on bone mineralization, performance, and intestinal morphology of coccidia-infected broilers1. Poult. Sci. 2019, 98, 5679–5690. [Google Scholar] [CrossRef]
- Lorenzo, J.; Horowitz, M.; Choi, Y. Osteoimmunology: Interactions of the bone and immune system. Endocr. Rev. 2008, 29, 403–440. [Google Scholar] [CrossRef] [PubMed]
- Dar, H.Y.; Azam, Z.; Anupam, R.; Mondal, R.K.; Srivastava, R.K. Osteoimmunology: The Nexus between bone and immune system. Front. Biosci.-Landmark 2018, 23, 464–492. [Google Scholar]
- Williams, B.; Waddington, D.; Murray, D.; Farquharson, C. Bone strength during growth: Influence of growth rate on cortical porosity and mineralization. Calcif. Tissue Int. 2004, 74, 236–245. [Google Scholar] [CrossRef]
- Williams, B.; Solomon, S.; Waddington, D.; Thorp, B.; Farquharson, C. Skeletal development in the meat-type chicken. Br. Poult. Sci. 2000, 41, 141–149. [Google Scholar] [CrossRef]
- Sanchez-Rodriguez, E.; Benavides-Reyes, C.; Torres, C.; Dominguez-Gasca, N.; Garcia-Ruiz, A.I.; Gonzalez-Lopez, S.; Rodriguez-Navarro, A.B. Changes with age (from 0 to 37 D) in tibiae bone mineralization, chemical composition and structural organization in broiler chickens. Poult. Sci. 2019, 98, 5215–5225. [Google Scholar] [CrossRef]
- Talaty, P.; Katanbaf, M.; Hester, P. Life cycle changes in bone mineralization and bone size traits of commercial broilers. Poult. Sci. 2009, 88, 1070–1077. [Google Scholar] [CrossRef]
- Sun, Z.W.; Fan, Q.H.; Wang, X.X.; Guo, Y.M.; Wang, H.J.; Dong, X. High stocking density alters bone-related calcium and phosphorus metabolism by changing intestinal absorption in broiler chickens. Poult. Sci. 2018, 97, 219–226. [Google Scholar] [CrossRef]
- Surai, P.F.; Kochish, I.I.; Fisinin, V.I.; Kidd, M.T. Antioxidant Defence Systems and Oxidative Stress in Poultry Biology: An Update. Antioxidants 2019, 8, 235. [Google Scholar] [CrossRef]
- Goo, D.; Kim, J.H.; Park, G.H.; Delos Reyes, J.B.; Kil, D.Y. Effect of Heat Stress and Stocking Density on Growth Performance, Breast Meat Quality, and Intestinal Barrier Function in Broiler Chickens. Animals 2019, 9, 107. [Google Scholar] [CrossRef]
- Miller, A.L. The methionine-homocysteine cycle and its effects on cognitive diseases. Altern. Med. Rev. 2003, 8, 7–19. [Google Scholar]
- Yang, Z.; Yang, Y.; Yang, J.; Wan, X.; Yang, H.; Wang, Z. Hyperhomocysteinemia Induced by Methionine Excess Is Effectively Suppressed by Betaine in Geese. Animals 2020, 10, 1642. [Google Scholar] [CrossRef]
- Xie, M.; Hou, S.S.; Huang, W.; Fan, H.P. Effect of Excess Methionine and Methionine Hydroxy Analogue on Growth Performance and Plasma Homocysteine of Growing Pekin Ducks. Poult. Sci. 2007, 86, 1995–1999. [Google Scholar] [CrossRef]
- Baszczuk, A.; Kopczyński, Z. Hyperhomocysteinemia in patients with cardiovascular disease. Adv. Hyg. Exp. Med. 2014, 68, 579–589. [Google Scholar] [CrossRef]
- Behera, J.; Bala, J.; Nuru, M.; Tyagi, S.C.; Tyagi, N. Homocysteine as a Pathological Biomarker for Bone Disease. J. Cell. Physiol. 2017, 232, 2704–2709. [Google Scholar] [CrossRef]
- Kumar, A.; Palfrey, H.A.; Pathak, R.; Kadowitz, P.J.; Gettys, T.W.; Murthy, S.N. The metabolism and significance of homocysteine in nutrition and health. Nutr. Metab. 2017, 14, 78. [Google Scholar] [CrossRef]
- Tinelli, C.; Di Pino, A.; Ficulle, E.; Marcelli, S.; Feligioni, M. Hyperhomocysteinemia as a Risk Factor and Potential Nutraceutical Target for Certain Pathologies. Front. Nutr. 2019, 6, 49. [Google Scholar] [CrossRef]
- Zaĭonts, V.; Krylov, M.; Loskot, V.; Kirillov, A. Biosynthesis of folic acid in Eimeria tenella (Coccidia). Parazitologiia 1978, 12, 3–8. [Google Scholar]
- Noack, S.; Chapman, H.D.; Selzer, P.M. Anticoccidial drugs of the livestock industry. Parasitol. Res. 2019, 118, 2009–2026. [Google Scholar] [CrossRef]
- Teng, P.-Y.; Choi, J.; Yadav, S.; Tompkins, Y.H.; Kim, W.K. Effects of low-crude protein diets supplemented with arginine, glutamine, threonine, and methionine on regulating nutrient absorption, intestinal health, and growth performance of Eimeria-infected chickens. Poult. Sci. 2021, 100, 101427. [Google Scholar] [CrossRef]
- Fernandes, J.I.M.; Murakami, A.E. Arginine metabolism in uricotelic species. Acta Sci. Anim. Sci. 2010, 32, 357–366. [Google Scholar] [CrossRef]
- Balnave, D.; Barke, J. Re-evaluation of the classical dietary arginine:lysine interaction for modern poultry diets: A review. World’s Poult. Sci. J. 2002, 58, 275–289. [Google Scholar] [CrossRef]
| Methionine/Arginine Levels and Experiment Settings | Type of Birds/Models | Effects of Supplementation 1 | Reference |
|---|---|---|---|
| Intestinal health: | |||
| Methionine: DL-Met or L-Met at 60%, 80%, 100% of breeder recommendations. Settings: Mixed Eimeria spp. challenge | Male Cobb 500 broilers | Increased growth performance; reduced intestinal permeability; improved activities of antioxidant enzymes; and affected tight junction protein expression. | [26] |
| Methionine: 0.33%, 0.39%, 0.45%, 0.51%, or 0.57% of diet. Settings: Mixed Eimeria spp. challenge | Partridge Shank Broilers | Improved growth performance; increased relative weight of bursa of Fabricius; increased GPX activity, increased serum TAC; increased sIgA concentration; decreased lesion score. | [27] |
| Methionine: 0.24 or 0.45% of diet, supplemented with free Met or Met dipeptide. Setting: Mixed Eimeria spp. challenge. | Male Cobb 500 broilers | Increased TAC and decreased SOD activity in the jejunum; increased expression of B0AT1 and TLR5 in the jejunum. | [28] |
| Methionine: 0.35%, 0.4%, 0.45%, or 0.5% of diet. Setting: High stocking density | Male Arbor Acres broilers | Improved the GSH: GSSG ratio and GPX activity; increased the VH and VH:CD ratio. | [29] |
| Methionine: No Met supplementation or Met supplemented at recommended level. Setting: Heat stress. | Male Cobb 500 broilers | Improved growth performance; decreased the expressions of proinflammatory cytokines in jejunum and ileum; improved the tight junction protein expressions in the ileum. | [30] |
| Methionine: DL-Met or L-Met at 60%, 70%, 80%, 90% of breeder recommendations. | Mixed sex Ross 308 broilers | Increased the concentration of GSH and reduced MDA contents in duodenum mucosa; increased the VH and VH:CD ratio. | [31] |
| Methionine: 0.3% higher than the control diet supplemented with DL-Met or DL-methionyl-DL-Met. | White king breeding pigeons | Increased relative intestinal weight; increased VH and VH:CD ratio; increased expressions of cell proliferation markers, tight junction proteins, and PEPT1 in the jejunum; upregulated the Wnt/β-catenin signaling pathway. | [32] |
| Methionine: No Met supplementation or Met supplemented at recommended level. | Cobb broilers | Met deficiency decreased IgA+ B cell count; reduced contents of sIgA, IgA, IgG and IgM in duodenum and jejunum. | [33] |
| Arginine: 50% above recommendation in reduced protein diet. Setting: Mixed Eimeria spp. challenge. | Male Cobb 500 broilers | Improved growth performance; decreased intestinal permeability; increased macrophage NO production; increased bile IgA content; improved T cell functions. | [21] |
| Arginine: 0.3% higher than the recommendation. Setting: Clostridium perfringens challenge. | Male Arbor Acres broilers | Increased jejunal VH; balanced the ileal microbiota; increased relative abundance of KEGG pathways related to membrane transport, replication and repair, translation and nucleotide metabolism. | [34] |
| Arginine: 8.5, 9.7, 10.9, 12.1, and 13.3 g/kg of diet. | Female Qingyuan partridge chickens | Increased growth performance; increased activities of antioxidant enzymes; increased TAC in jejunum and ileum; decreased expression of proinflammatory cytokines in the ileum; increased sIgA production; improved ileal microbiota profile. | [35] |
| Arginine: 1.04, 1.14, 1.24, 1.34, 1.44% of diet. Setting: Mixed Eimeria spp. challenge. | Male Cobb 500 broilers | Improved growth performance; reduced intestinal permeability; increased expression of tight junction proteins. | [36] |
| Arginine: 0.96%, 1.16%, 1.36%, 1.56%, and 1.76% digestible arginine. | Female Arbor Acres broiler breeders | Increased TAC; increased activity of GPX, and decreased MDA in the breeder and the offspring. | [37] |
| Arginine: 350 μM in DMEM culture medium. Setting: Oxidative stress induced by hydrogen peroxide. | Ovine intestinal epithelial cells | Reduced hydrogen peroxide-induced ROS production; increased protein levels of GPX, tight junction protein 1, and nitric oxide synthase, whereas decreased the TNFα level. | [38] |
| Arginine: 11.1, 13.3 and 20.2 g/kg of diet. Setting: Mixed Eimeria spp. challenge. | Male Ross 708 broilers | Increased VH and decreased CD; increased goblet cell density; decreased expression of proinflammatory cytokine; increased mucosal maltase activity; 13.3 g/kg of Arg supplementation showed highest expression of anti-apoptosis gene and mTOR. | [39] |
| Arginine: 100, 105, and 110% of the recommendation. Setting: Mixed Eimeria spp. challenge. | Male Ross 308 broilers | Improved growth performance; increased VH and VH:CD ratio; decreased oocyst count. | [40] |
| Bone health: | |||
| Methionine: 250 mg/kg body weight in drinking water. | Ovariectomized rats | Increased bone density; decreased development of osteoclasts by inhibiting the TLR-4/MyD88/NF-κB pathway. | [41] |
| Methionine: Study 1: 0.12% and 0.84% of mice diet. Study 2: α-MEM culture media with restricted sulfur amino acids. | Study 1: Male and female mice. Study 2: Mouse preosteoblast cell line. | Study 1: Met deficiency decreased bone mineral density, bone mineral content, and microarchitecture parameters; increased collagen degradation. Study 2: Met restriction delayed osteoblast differentiation and decreased expressions of genes regulating bone formation. | [42] |
| Methionine: 0.12% and 0.86% of diet. | Young male C57BL/6J mice | Decreased cortical bone density; decreased trabecular bone density, bone surface, trabecula and bone volume, and trabecular thickness; increased fragility; reduced expression of RUNX2 in bone marrow. | [43] |
| Arginine: 70, 80, 90, 100, and 110% of the recommendation. | Male Ross 308 broilers. | Improved growth performance, lean deposition, and bone mineral density. | [44] |
| Arginine: 0, 0.1, 1, and 10 µM in DMEM culture medium. | Human mesenchymal stem cells. | Increased osteogenic differentiation; increased expression of RUNX2, Dlx5, osterix, and wnt5a; decreased expression of adaptogenic transcription factors. | [45] |
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2023 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Liu, G.; Kim, W.K. The Functional Roles of Methionine and Arginine in Intestinal and Bone Health of Poultry: Review. Animals 2023, 13, 2949. https://doi.org/10.3390/ani13182949
Liu G, Kim WK. The Functional Roles of Methionine and Arginine in Intestinal and Bone Health of Poultry: Review. Animals. 2023; 13(18):2949. https://doi.org/10.3390/ani13182949
Chicago/Turabian StyleLiu, Guanchen, and Woo Kyun Kim. 2023. "The Functional Roles of Methionine and Arginine in Intestinal and Bone Health of Poultry: Review" Animals 13, no. 18: 2949. https://doi.org/10.3390/ani13182949
APA StyleLiu, G., & Kim, W. K. (2023). The Functional Roles of Methionine and Arginine in Intestinal and Bone Health of Poultry: Review. Animals, 13(18), 2949. https://doi.org/10.3390/ani13182949





