One Health Approach: An Overview of Q Fever in Livestock, Wildlife and Humans in Asturias (Northwestern Spain)
Abstract
Simple Summary
Abstract
1. Introduction
2. Materials and Methods
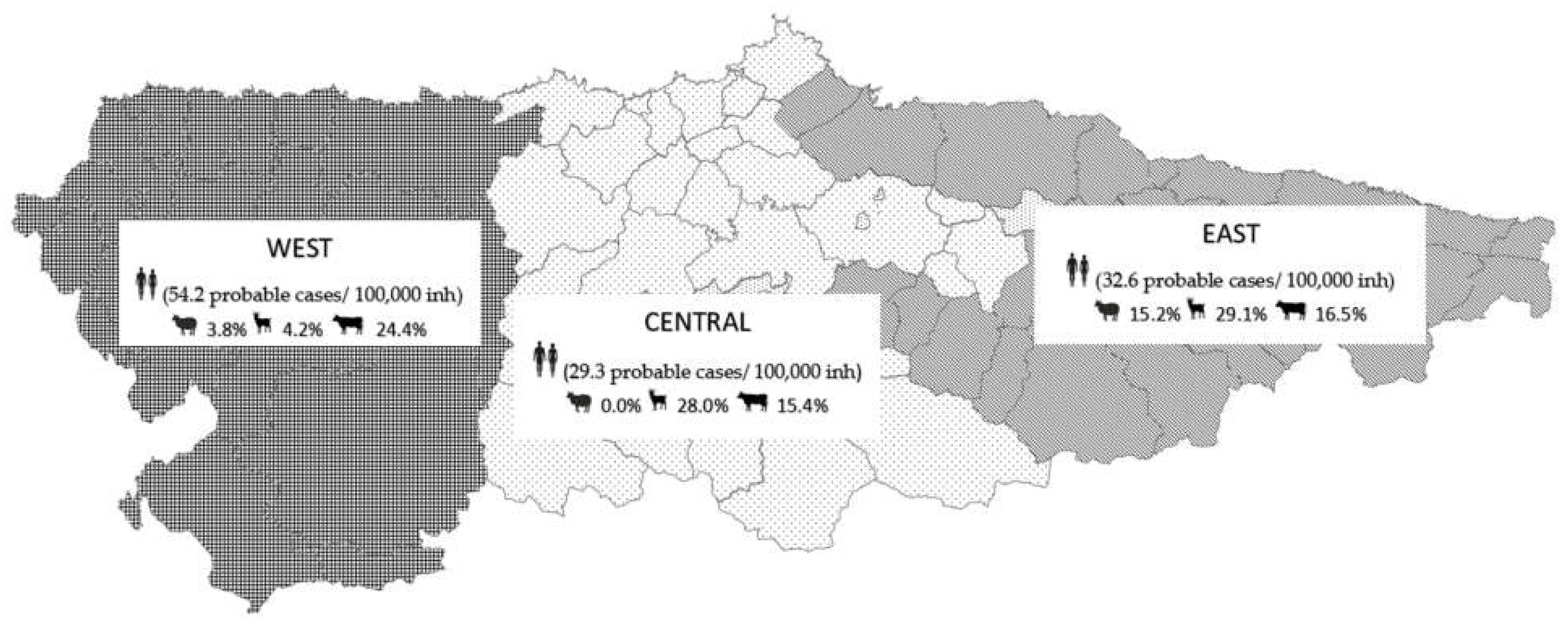
2.1. Study Area
2.2. Animal and Human Population Investigated and Sample Collection
2.2.1. Livestock
2.2.2. Wildlife
2.2.3. Human Population Investigated
2.3. Serological Analyses
2.3.1. Animal Sera
2.3.2. Human Sera
2.3.3. Molecular Analyses
2.3.4. Statistical Analysis
2.3.5. Ethics Statement
3. Results
3.1. Seroprevalence in Livestock
3.2. Investigation of C. burnetii DNA in Animal Premises
3.3. Seroprevalence in Wildlife
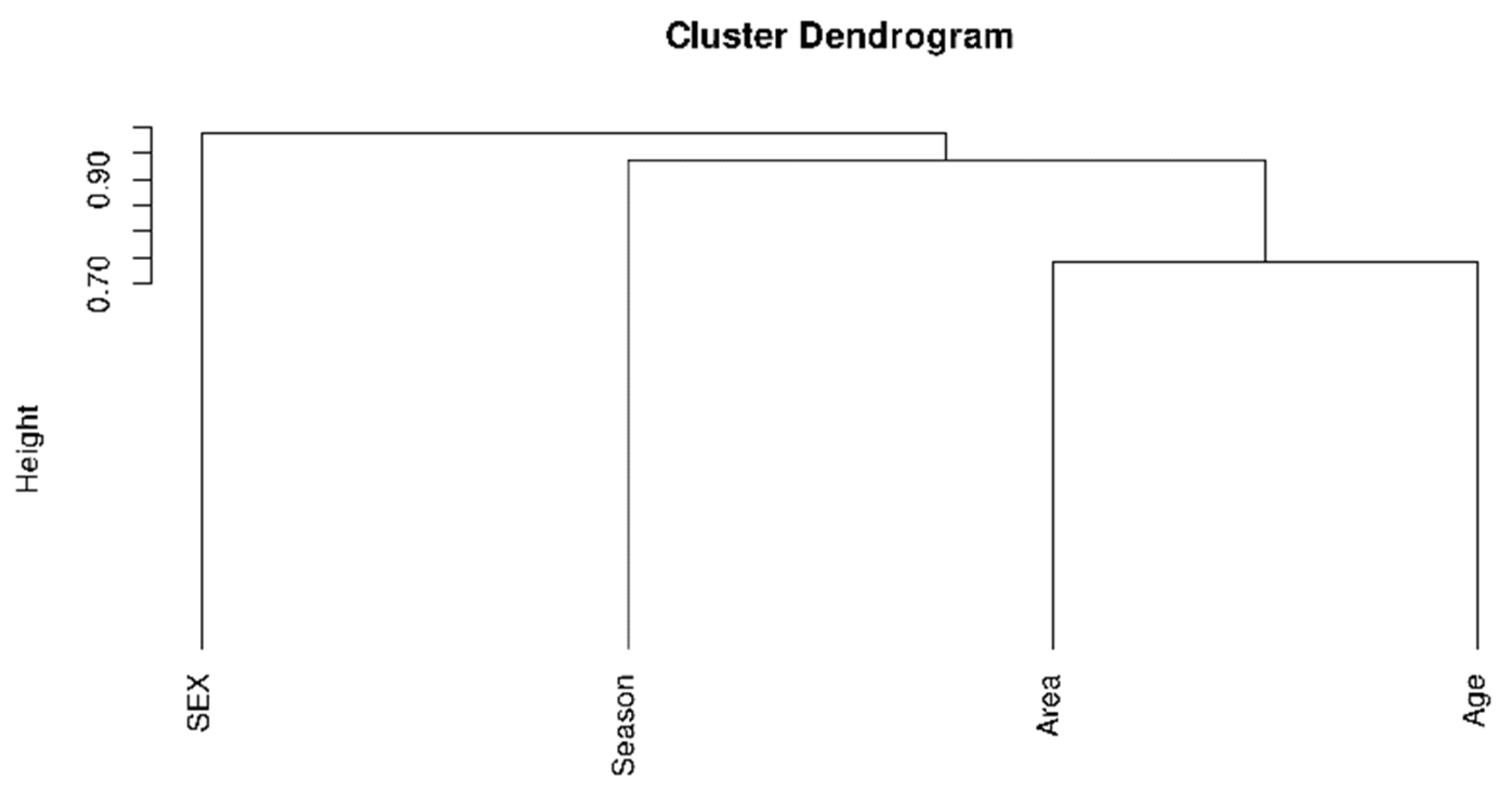
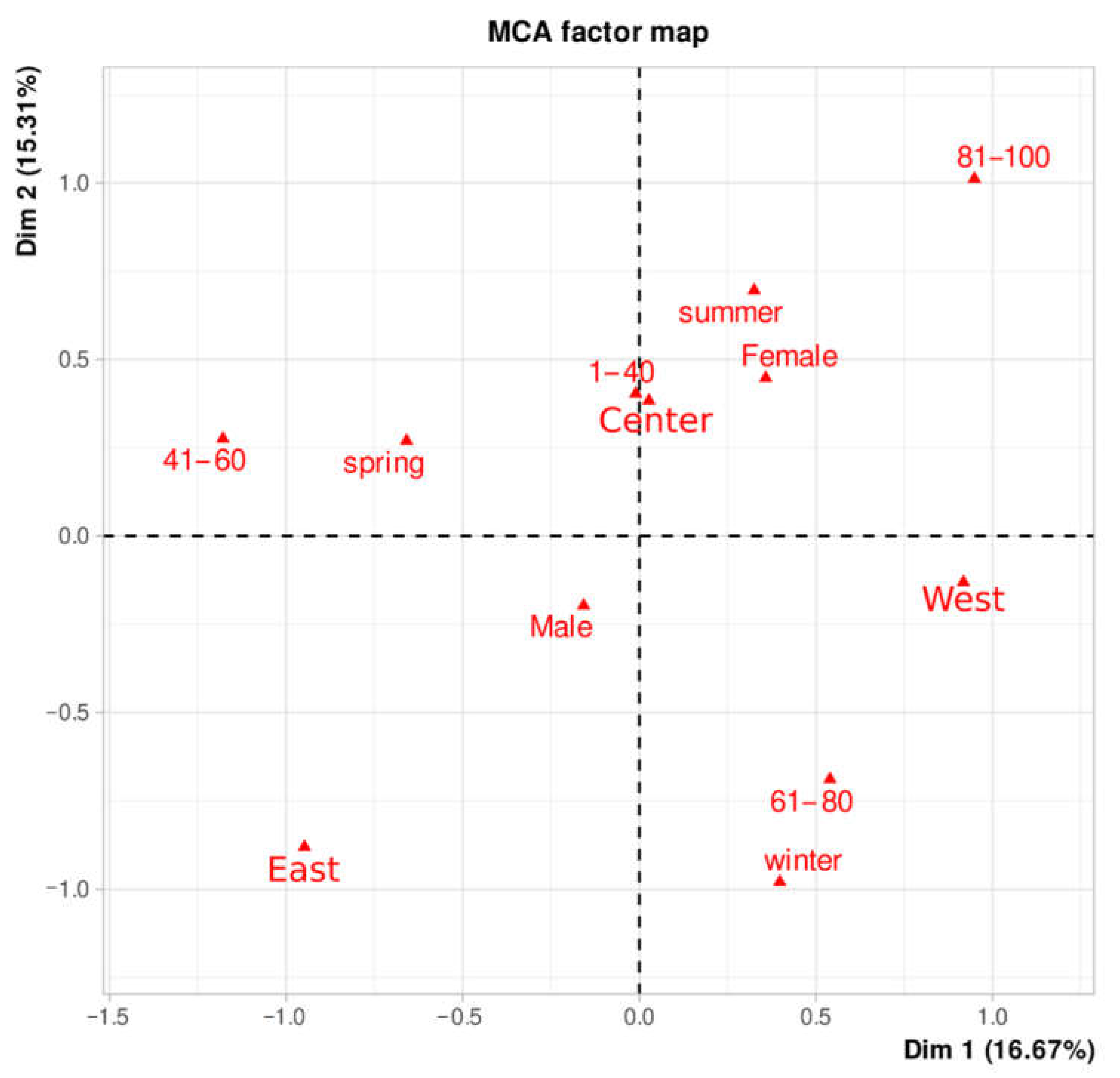
3.4. Estimation of Q Fever Incidence in Humans
4. Discussion
5. Conclusions
Supplementary Materials
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Acknowledgments
Conflicts of Interest
References
- Eldin, C.; Mélenotte, C.; Mediannikov, O.; Ghigo, E.; Million, M.; Edouard, S.; Mege, J.-L.; Maurin, M.; Raoult, D. From Q Fever to Coxiella burnetii Infection: A Paradigm Change. Clin. Microbiol. Rev. 2017, 30, 115–190. [Google Scholar] [CrossRef] [PubMed]
- Roest, H.I.; Bossers, A.; Van Zijderveld, F.G.; Rebel, J.M. Clinical microbiology ofCoxiella burnetiiand relevant aspects for the diagnosis and control of the zoonotic disease Q fever. Vet. Q. 2013, 33, 148–160. [Google Scholar] [CrossRef] [PubMed]
- EFSA Panel on Animal Health and Welfare (AHAW). Scientific Opinion on Q fever. EFSA J. 2010, 8, 1595. [Google Scholar] [CrossRef]
- Brom, R.D.; Engelen, E.; Roest, H.; der Hoek, W.; Vellema, P. Coxiella burnetii infections in sheep or goats: An opinionated review. Vet. Microbiol. 2015, 181, 119–129. [Google Scholar] [CrossRef] [PubMed]
- González-Barrio, D.; Ruiz-Fons, F. Coxiella burnetiiin wild mammals: A systematic review. Transbound. Emerg. Dis. 2019, 66, 662–671. [Google Scholar] [CrossRef]
- Gortazar, C.; Reperant, L.A.; Kuiken, T.; De La Fuente, J.; Boadella, M.; Martínez-Lopez, B.; Ruiz-Fons, F.; Estrada-Peña, A.; Drosten, C.; Medley, G.; et al. Crossing the Interspecies Barrier: Opening the Door to Zoonotic Pathogens. PLoS Pathog. 2014, 10, e1004129. [Google Scholar] [CrossRef]
- Rodríguez-Alonso, B.; Almeida, H.; Alonso-Sardón, M.; López-Bernus, A.; Pardo-Lledias, J.; Velasco-Tirado, V.; Carranza-Rodríguez, C.; Pérez-Arellano, J.L.; Belhassen-García, M. Epidemiological scenario of Q fever hospitalized patients in the Spanish Health System: What’s new. Int. J. Infect. Dis. 2020, 90, 226–233. [Google Scholar] [CrossRef]
- Instituto de Salud Carlos III.Red Nacional de Vigilancia Epidemiológica. Informe anual del Sistema de Información Microbiológica 2016. Available online: https://repisalud.isciii.es/bitstream/20.500.12105/6975/7/InformeAnualDelSistema_2017.pdf (accessed on 15 September 2020).
- Alende-Castro, V.; Macía-Rodríguez, C.; Novo-Veleiro, I.; García-Fernández, X.; Treviño-Castellano, M.; Rodríguez-Fernández, S.; González-Quintela, A. Q fever in Spain: Description of a new series, and systematic review. PLoS Negl. Trop. Dis. 2018, 12, e0006338. [Google Scholar] [CrossRef] [PubMed]
- Clemente, M.M.G.; Seco-García, A.J.; Gutiérrez-Rodríguez, M.; Romero-Álvarez, P.; Fernández-Bustamante, J.; Rodríguez-Pérez, M. Brote epidémico de neumonía por Coxiella burnetii. Enferm. Infecc. Microbiol. Clínica 2007, 25, 184–186. [Google Scholar] [CrossRef]
- Margolles, M.; Herrojo, A.; Ávarez, B.S.O.; González, M.; Redondo, M.A. La Brucelosis y la Fiebre Q: Actuaciones Clínicas y EpiDemiológicas. Situación en un Colectivo de Alto Riesgo. Asturias 1993; Direccion Regional de Salud Pública. Consejería de Sanidad. Principado de Asturias: Oviedo, Spain, 1994; pp. 1–33. [Google Scholar]
- Nuño, F.J.; Noval, J.; Campoamor, M.T.; del Valle, A. Fiebre Q aguda en Asturias. Rev. Clin. Esp. 2002, 202, 569–573. [Google Scholar]
- González-Barrio, D.; Ávila, A.L.V.; Boadella, M.; Beltrán-Beck, B.; Barasona, J.Á.; Santos, J.P.V.; Queirós, J.; García-Pérez, A.L.; Barral, M.; Ruiz-Fons, F. Host and Environmental Factors Modulate the Exposure of Free-Ranging and Farmed Red Deer (Cervus elaphus) to Coxiella burnetii. Appl. Environ. Microbiol. 2015, 81, 6223–6231. [Google Scholar] [CrossRef]
- Ruiz-Fons, F.; Rodríguez, Ó.; Torina, A.; Naranjo, V.; Gortázar, C.; De La Fuente, J. Prevalence of Coxiella burnetti infection in wild and farmed ungulates. Vet. Microbiol. 2008, 126, 282–286. [Google Scholar] [CrossRef]
- Instituto de Desarrollo Económico del Principado de Asturias. Demografía y población a fecha (2019). Available online: https://www.idepa.es/conocimiento/asturias-en-cifras/demografia (accessed on 15 September 2020).
- Peel, M.C.; Finlayson, B.L.; McMahon, T.A. Updated world map of the Köppen-Geiger climate classification. Hydrol. Earth Syst. Sci. 2007, 11, 1633–1644. [Google Scholar] [CrossRef]
- Consejería de Desarrollo Rural y Recursos Naturales: Sección de Prospectiva y Estadística. Declaración Anual Obligatoria—PACA—Estadísticas a fecha 15 de noviembre de 2017. Available online: https://www.asturias.es/portal/site/webasturias/template.PAGE/BuscadorOpenDataTransparencia (accessed on 15 September 2020).
- Stöbel, K.; Schönberg, A.; Staak, C. A new non-species dependent ELISA for detection of antibodies to Borrelia burgdorferi s. l. in zoo animals. Int. J. Med. Microbiol. 2002, 291, 88–99. [Google Scholar] [CrossRef]
- CDC. Q Fever (Coxiella burnetii) 2009 Case Definition. Available online: https://wwwn.cdc.gov/nndss/conditions/q-fever/case-definition/2009 (accessed on 15 September 2020).
- Schets, F.; De Heer, L.; Husman, A.D.R. Coxiella burnetii in sewage water at sewage water treatment plants in a Q fever epidemic area. Int. J. Hyg. Environ. Health 2013, 216, 698–702. [Google Scholar] [CrossRef] [PubMed]
- Chavent, M.; Kuentz, V.; Liquet, B.; Saracco, J. ClustOfVar: Clustering of variables. R package version 1.1.2017. Available online: https://CRAN.R-project.org/package=ClustOfVar (accessed on 15 September 2020).
- Lê, S.; Josse, J.; Husson, F. FactoMineR: AnRPackage for Multivariate Analysis. J. Stat. Softw. 2008, 25, 1–18. [Google Scholar] [CrossRef]
- R Core Team. R: A Language and Environment for Statistical Computing. R Foundation for Statistical Computing, Vienna, Austria. Available online: http://www.R-project.org/ (accessed on 11 March 2021).
- Rahaman, R.; Milazzo, A.; Marshall, H.; Bi, P. Is a One Health Approach Utilized for Q Fever Control? A Comprehensive Literature Review. Int. J. Environ. Res. Public Health 2019, 16, 730. [Google Scholar] [CrossRef]
- Espi, A.; Prieto, M.; Álvarez, M. Situación sanitaria del ovino en Asturias: Seroprevalencia de la Enfermedad de la Frontera, Maedi-Visna, Aborto Enzoótico, Agalaxia Contagiosa, Fiebre Q y Leptospirosis; Consejería de Agricultura y Pesca. Viceconsejería. Servicio de Publicaciones y Divulgación: Sevilla, Spain, 2001; pp. 708–713. [Google Scholar]
- WHO (World Organization for Animal Health). Manual of diagnostic Tests and vaccines for terrestrial animals (mammals, birds and bees). Chapter 2.7.11 “Q fever”. Available online: https://www.oie.int/doc/ged/D7709.PDF (accessed on 15 September 2020).
- Alonso, E.; Eizaguirre, D.; Lopez-Etxaniz, I.; Olaizola, J.I.; Ocabo, B.; Barandika, J.F.; Jado, I.; Álvarez-Alonso, R.; Hurtado, A.; García-Pérez, A.L. A Q fever outbreak associated to courier transport of pets. PLoS ONE 2019, 14, e0225605. [Google Scholar] [CrossRef] [PubMed]
- Álvarez-Alonso, R.; Basterretxea, M.; Barandika, J.F.; Hurtado, A.; Idiazabal, J.; Jado, I.; Beraza, X.; Montes, M.; Liendo, P.; García-Pérez, A.L. A Q Fever Outbreak with a High Rate of Abortions at a Dairy Goat Farm:Coxiella burnetiiShedding, Environmental Contamination, and Viability. Appl. Environ. Microbiol. 2018, 84, 01650–18. [Google Scholar] [CrossRef]
- Hurtado, A.; Alonso, E.; Aspiritxaga, I.; Etxaniz, I.L.; Ocabo, B.; Barandika, J.F.; De Murúa, J.I.F.-O.; Urbaneja, F.; Álvarez-Alonso, R.; Jado, I.; et al. Environmental sampling coupled with real-time PCR and genotyping to investigate the source of a Q fever outbreak in a work setting. Epidemiol. Infect. 2017, 145, 1834–1842. [Google Scholar] [CrossRef]
- Cruz, R.; Esteves, F.; Vasconcelos-Nóbrega, C.; Santos, C.; Ferreira, A.S.; Mega, C.; Coelho, A.C.; Vala, H.; Mesquita, J.R. A Nationwide Seroepidemiologic Study on Q Fever Antibodies in Sheep of Portugal. Vector Borne Zoonotic Dis. 2018, 18, 601–604. [Google Scholar] [CrossRef]
- Ruiz-Fons, F.; Astobiza, I.; Barandika, J.F.; Hurtado, A.; Atxaerandio, R.; Juste, R.A.; Garcia-Perez, A.L. Seroepidemiological study of Q fever in domestic ruminants in semi-extensive grazing systems. BMC Vet. Res. 2010, 6, 3. [Google Scholar] [CrossRef] [PubMed]
- Rodríguez, N.F.; Carranza, C.; Bolaños, M.; Pérez-Arellano, J.L.; Gutierrez, C. Seroprevalence of Coxiella burnetii in domestic ruminants in Gran Canaria island, Spain. Transbound. Emerg. Dis. 2010, 57, 66–67. [Google Scholar] [CrossRef]
- Astobiza, I.; Barral, M.; Ruiz-Fons, F.; Barandika, J.; Gerrikagoitia, X.; Hurtado, A.; García-Pérez, A. Molecular investigation of the occurrence of Coxiella burnetii in wildlife and ticks in an endemic area. Vet. Microbiol. 2011, 147, 190–194. [Google Scholar] [CrossRef] [PubMed]
- Álvarez-Alonso, R.; Zendoia, I.I.; Barandika, J.F.; Jado, I.; Hurtado, A.; López, C.M.; García-Pérez, A.L. Monitoring Coxiella burnetii Infection in Naturally Infected Dairy Sheep Flocks Throughout Four Lambing Seasons and Investigation of Viable Bacteria. Front. Vet. Sci. 2020, 7, 352. [Google Scholar] [CrossRef] [PubMed]
- Roest, H.J.; van Gelderen, B.; Dinkla, A.; Frangoulidis, D.; van Zijderveld, F.G.; Rebel, J.; van Keulen, L. Q fever in pregnant goats: Pathogenesis and excretion of Coxiella burnetii. PLoS ONE 2012, 7, e48949. [Google Scholar] [CrossRef] [PubMed]
- Mori, M.; Roest, H.-J. Farming Q fever and public health: Agricultural practices and beyond. Arch. Public Health 2018, 76, 2. [Google Scholar] [CrossRef]
- Anderson, A.D.; Bijlmer, H.; Fournier, P.E.; Graves, S.; Hartzell, J.; Kersh, G.J.; Limonard, G.J.; Marrie, T.J.; Massung, R.F.; McQuiston, J.H.; et al. Diagnosis and management of Q fever—United States, 2013: Recommendations from CDC and the Q Fever Working Group. MMWR 2013, 62, 1–30. [Google Scholar]
- Cilla, G.; Montes, M.; Pérez-Trallero, E. Q fever in the Netherlands—What matters is seriousness of disease rather than quantity. Eurosurveillance 2008, 13, 18975. [Google Scholar] [CrossRef][Green Version]
- Agger, J.F.; Paul, S. Increasing prevalence of Coxiella burnetii seropositive Danish dairy cattle herds. Acta Vet. Scand. 2014, 56, 46. [Google Scholar] [CrossRef]
- Carrié, P.; Barry, S.; Rousset, E.; De Crémoux, R.; Sala, C.; Calavas, D.; Perrin, J.-B.; Bronner, A.; Gasqui, P.; Gilot-Fromont, E.; et al. Swab cloths as a tool for revealing environmental contamination by Q fever in ruminant farms. Transbound. Emerg. Dis. 2019, 66, 1202–1209. [Google Scholar] [CrossRef] [PubMed]
- Tissot-Dupont, H.; Amadei, M.-A.; Nezri, M.; Raoult, D. Wind in November, Q Fever in December. Emerg. Infect. Dis. 2004, 10, 1264–1269. [Google Scholar] [CrossRef] [PubMed]
- Maurin, M.; Raoult, D. Q Fever. Clin. Microbiol. Rev. 1999, 12, 518–553. [Google Scholar] [CrossRef] [PubMed]
| AREA | Sheep | Goats | Cattle | |||||||||
|---|---|---|---|---|---|---|---|---|---|---|---|---|
| Census | Analyzed | ELISA + | Seropre- | Census | Analyzed | ELISA + | Seropre- | Census | Analyzed | ELISA + | Seropre- | |
| (n) | (n) | (n) | valence | (n) | (n) | (n) | valence | (n) | (n) | (n) | valence | |
| West | 7493 | 26 | 1 | 3.8 | 6609 | 24 | 1 | 4.2 | 150,250 | 45 | 11 | 24.4 |
| Central | 14,557 | 49 | 0 | 0.0 | 5676 | 25 | 7 | 28.0 | 132,841 | 39 | 6 | 15.4 |
| East | 23,954 | 79 | 12 | 15.2 | 18,738 | 86 | 25 | 29.1 | 109,698 | 79 | 13 | 16.5 |
| Asturias | 46,004 | 154 | 13 | 8.4 | 31,023 | 135 | 33 | 24.4 | 392,789 | 163 | 30 | 18.4 |
| A—Sheep | Estimate | Z-value | Pr (>│t│) | OR | CI 95% |
| Intercept | −3.9802 | −4.978 | 0.0001 | 0.02 | 0.01–0.07 |
| Sampling 2016 (ref.) | |||||
| Sampling 2017 | 1.0638 | 1.260 | 0.2060 | 2.90 | 0.64–20.60 |
| Sampling 2018 | 2.0249 | 2.121 | 0.0339 | 7.58 | 1.25–62.66 |
| Census 1–49 animals (ref.) | |||||
| Census 50–120 | 1.9716 | 3.139 | 0.0017 | 7.18 | 2.10–25.78 |
| B—Goats | Estimate | Z-value | Pr (>│t│) | OR | CI 95% |
| Intercept | −3.0910 | −3.0236 | 0.0025 | 0.05 | 0.01–0.22 |
| Western Asturias (ref.) | |||||
| Central Asturias | 1.9014 | 1.7135 | 0.0866 | 6.70 | 1.07–130.56 |
| Eastern Asturias | 2.2669 | 2.1587 | 0.0309 | 9.65 | 1.86–177.50 |
| Wildlife Species | Analyzed (n) | ELISA Positive (n) | Seropre- Valence |
|---|---|---|---|
| Iberian red deer (Cervus elaphus hispanicus) | 83 | 7 | 8.43 |
| Roe deer (Capreolus capreolus) | 57 | 2 | 3.51 |
| Cantabrian chamois (Rupicapra rupicapra) | 41 | 3 | 7.32 |
| Fallow deer (Dama dama) | 73 | 5 | 6.85 |
| European wild boar (Sus scrofa) | 73 | 4 | 5.48 |
| Total | 327 | 21 | 6.42 |
| AGE | Men | Women | n | SEASON | n | IFAT Titer | n |
|---|---|---|---|---|---|---|---|
| 1–40 | 17 | 13 | 30 | Spring (Mar–May) | 74 | 1:128 | 76 |
| 41–60 | 46 | 17 | 63 | Summer (Jun–Oct) | 68 | 1:256 | 56 |
| 61–80 | 62 | 23 | 85 | Autumn–Winter | 66 | 1:512 | 44 |
| 81–100 | 19 | 11 | 30 | (Nov–Feb) | 1:1024 | 31 | |
| 1:4096 | 1 | ||||||
| Total | 144 | 64 | 208 | Total | 208 | Total | 208 |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2021 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Espí, A.; del Cerro, A.; Oleaga, Á.; Rodríguez-Pérez, M.; López, C.M.; Hurtado, A.; Rodríguez-Martínez, L.D.; Barandika, J.F.; García-Pérez, A.L. One Health Approach: An Overview of Q Fever in Livestock, Wildlife and Humans in Asturias (Northwestern Spain). Animals 2021, 11, 1395. https://doi.org/10.3390/ani11051395
Espí A, del Cerro A, Oleaga Á, Rodríguez-Pérez M, López CM, Hurtado A, Rodríguez-Martínez LD, Barandika JF, García-Pérez AL. One Health Approach: An Overview of Q Fever in Livestock, Wildlife and Humans in Asturias (Northwestern Spain). Animals. 2021; 11(5):1395. https://doi.org/10.3390/ani11051395
Chicago/Turabian StyleEspí, Alberto, Ana del Cerro, Álvaro Oleaga, Mercedes Rodríguez-Pérez, Ceferino M. López, Ana Hurtado, Luís D. Rodríguez-Martínez, Jesús F. Barandika, and Ana L. García-Pérez. 2021. "One Health Approach: An Overview of Q Fever in Livestock, Wildlife and Humans in Asturias (Northwestern Spain)" Animals 11, no. 5: 1395. https://doi.org/10.3390/ani11051395
APA StyleEspí, A., del Cerro, A., Oleaga, Á., Rodríguez-Pérez, M., López, C. M., Hurtado, A., Rodríguez-Martínez, L. D., Barandika, J. F., & García-Pérez, A. L. (2021). One Health Approach: An Overview of Q Fever in Livestock, Wildlife and Humans in Asturias (Northwestern Spain). Animals, 11(5), 1395. https://doi.org/10.3390/ani11051395








