Effects of High Intensity Laser Therapy in the Treatment of Tendon and Ligament Injuries in Performance Horses
Simple Summary
Abstract
1. Introduction
2. Materials and Methods
2.1. Animals
- Physical evidence of tendon or ligament injury (SDFT, superficial digital flexor tendon; DDFT, deep digital flexor tendon; SL, suspensory ligament), where at least two of the following symptoms were present: pain on palpation, limb swelling, lameness;
- Presence of tendon or ligament injury with damage of collagen fibres visible in ultrasound scanning;
- No previous treatment of the present injury.
2.2. Study Design
2.3. Clinical Assessment
- No reaction to palpation—no pain (0);
- Avoidance characterized by muscle contraction with slight limb movement—mild pain (1);
- Resistance to palpation, where the horse is reluctant to lift the limb or pulls the limb away—moderate pain (2);
- Violent avoidance characterized by nervous reaction—severe pain (3).
2.4. Imaging
- Isoechoic (0);
- Mildly hypoechoic (1);
- Moderate hypoechoic (2);
- Anechoic (3).
2.5. High Intensity Laser Therapy
2.6. Data Analysis
3. Results
3.1. Animals
3.2. Clinical Assessment
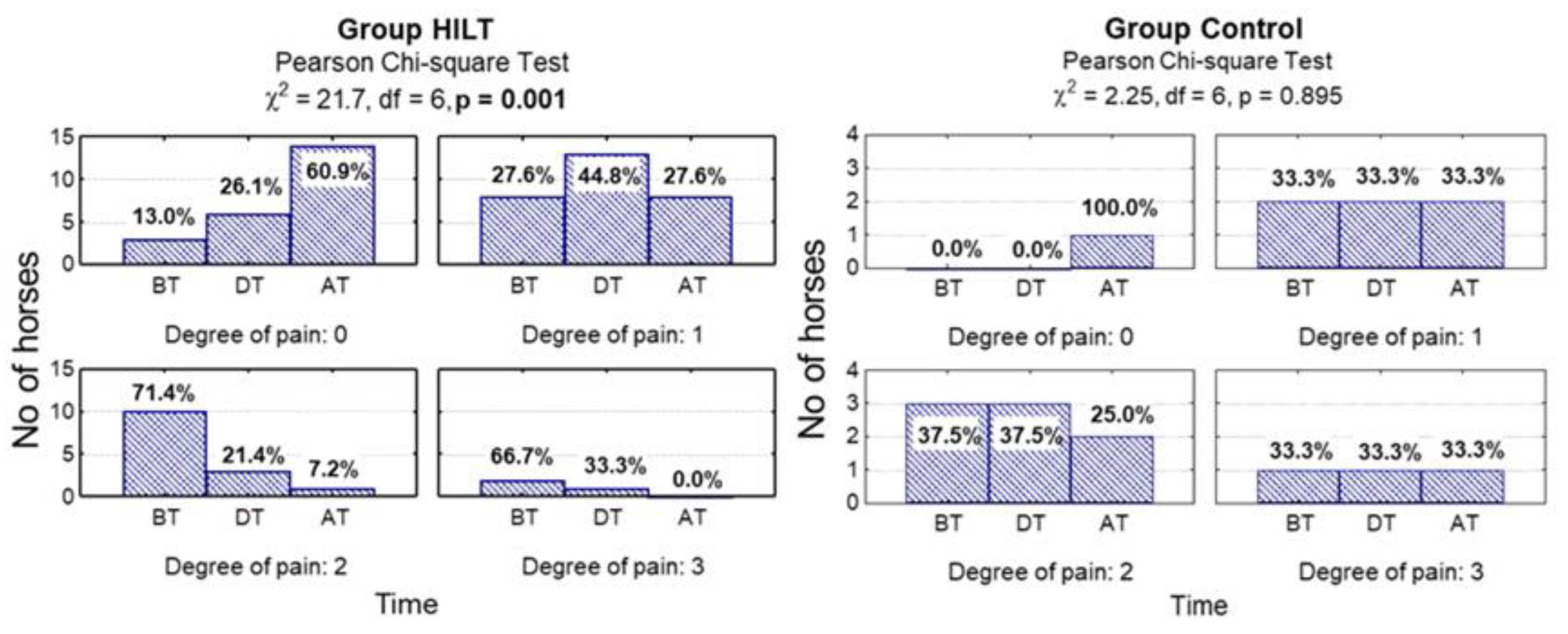
3.2.1. Pain
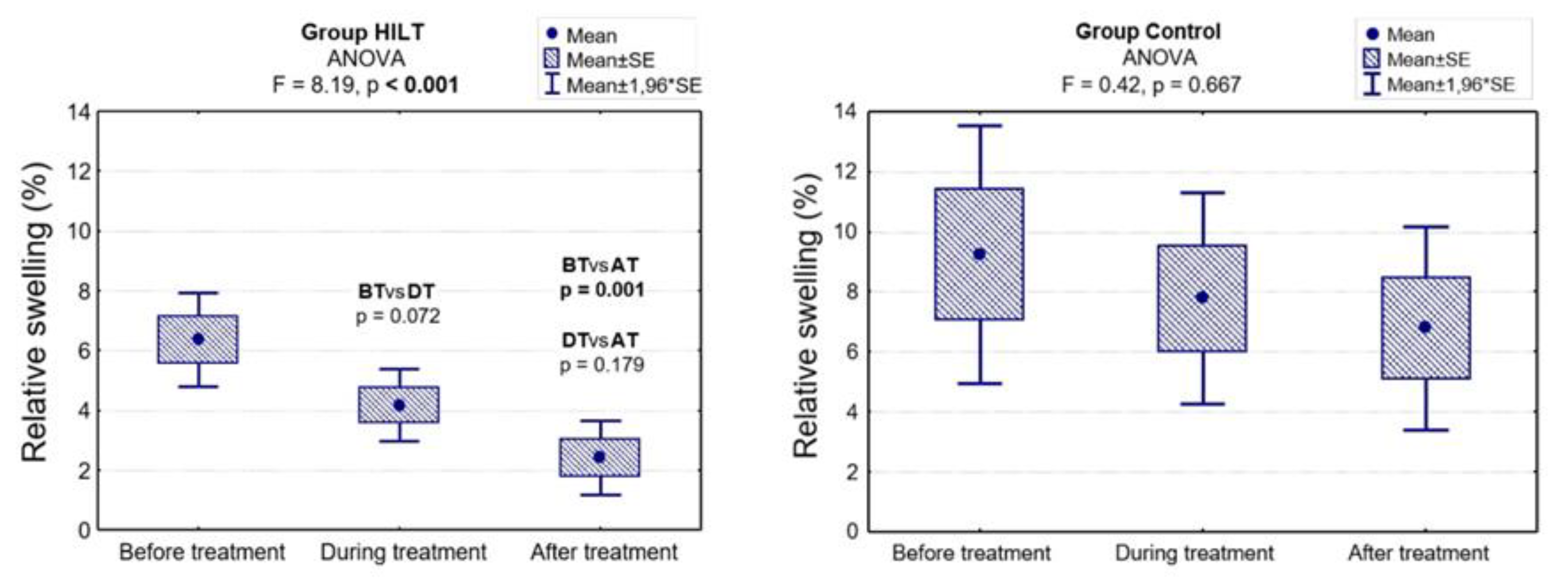
3.2.2. Swelling
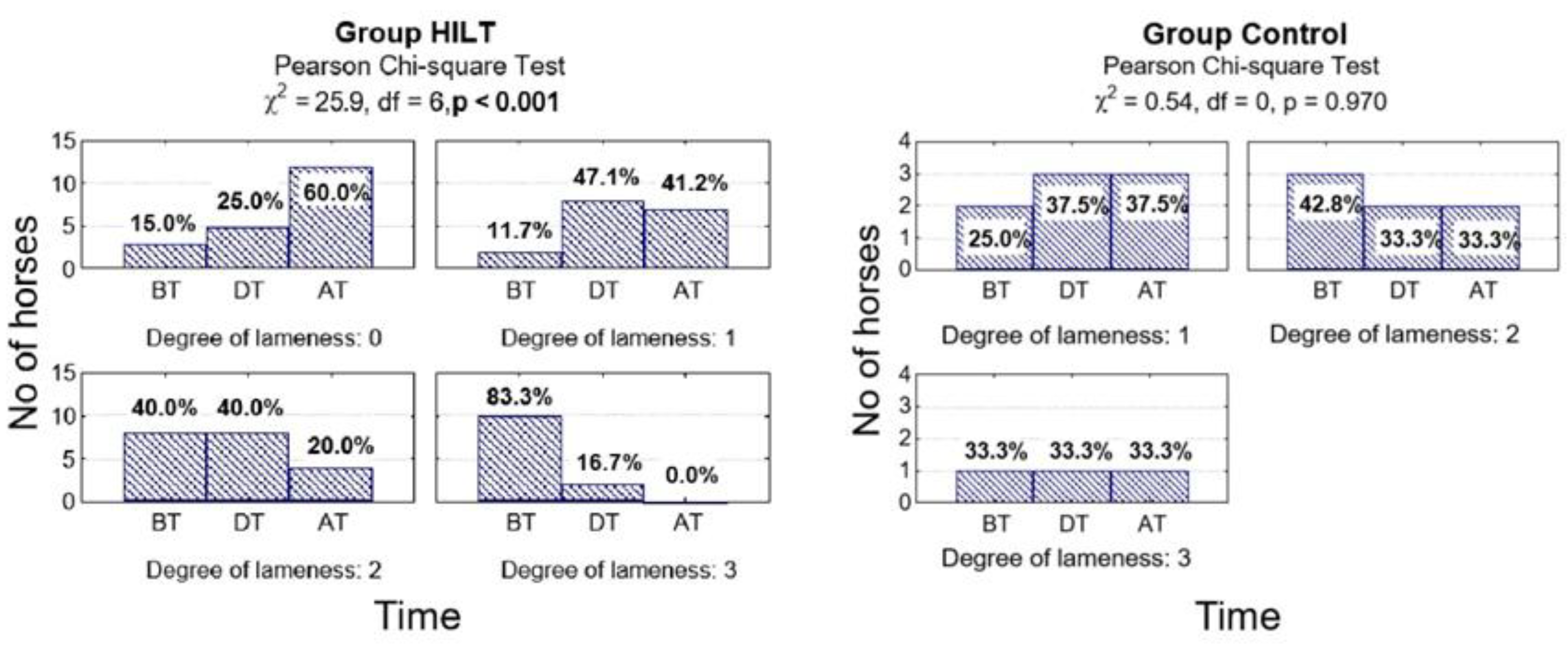
3.2.3. Lameness
3.3. Ultrasound Examination
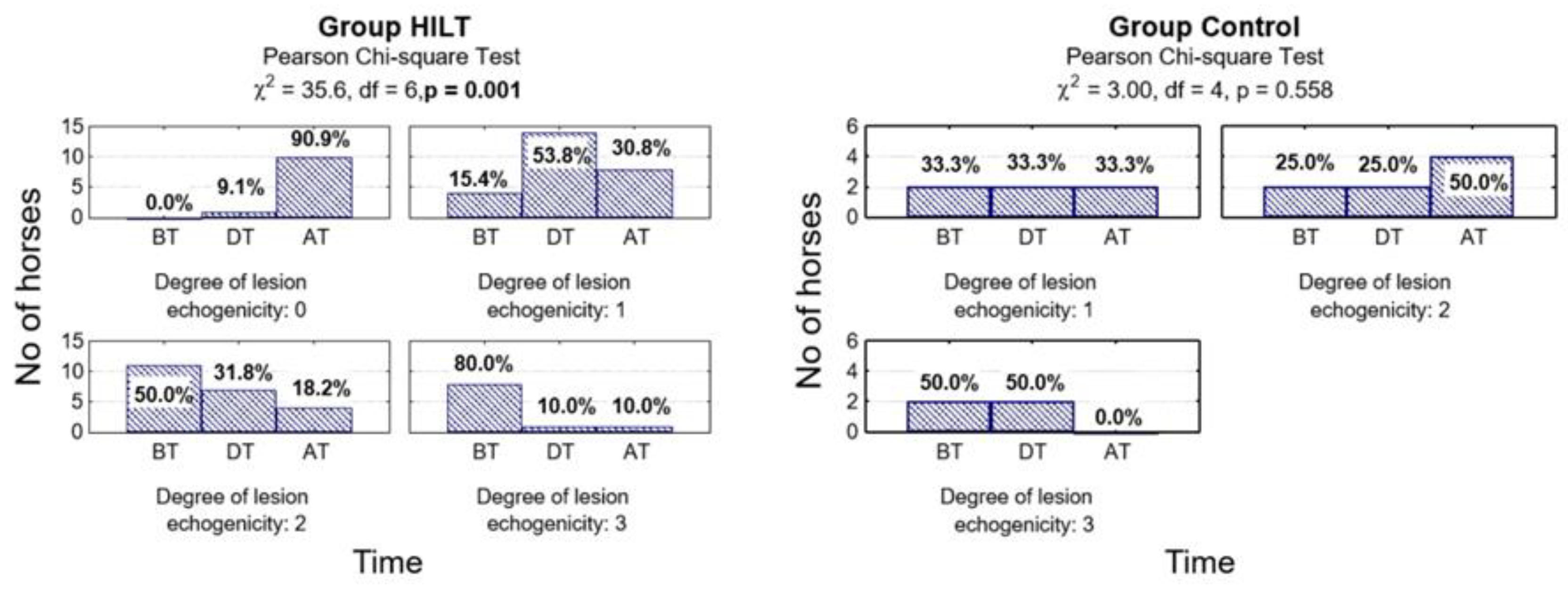
3.3.1. Lesion Echogenicity
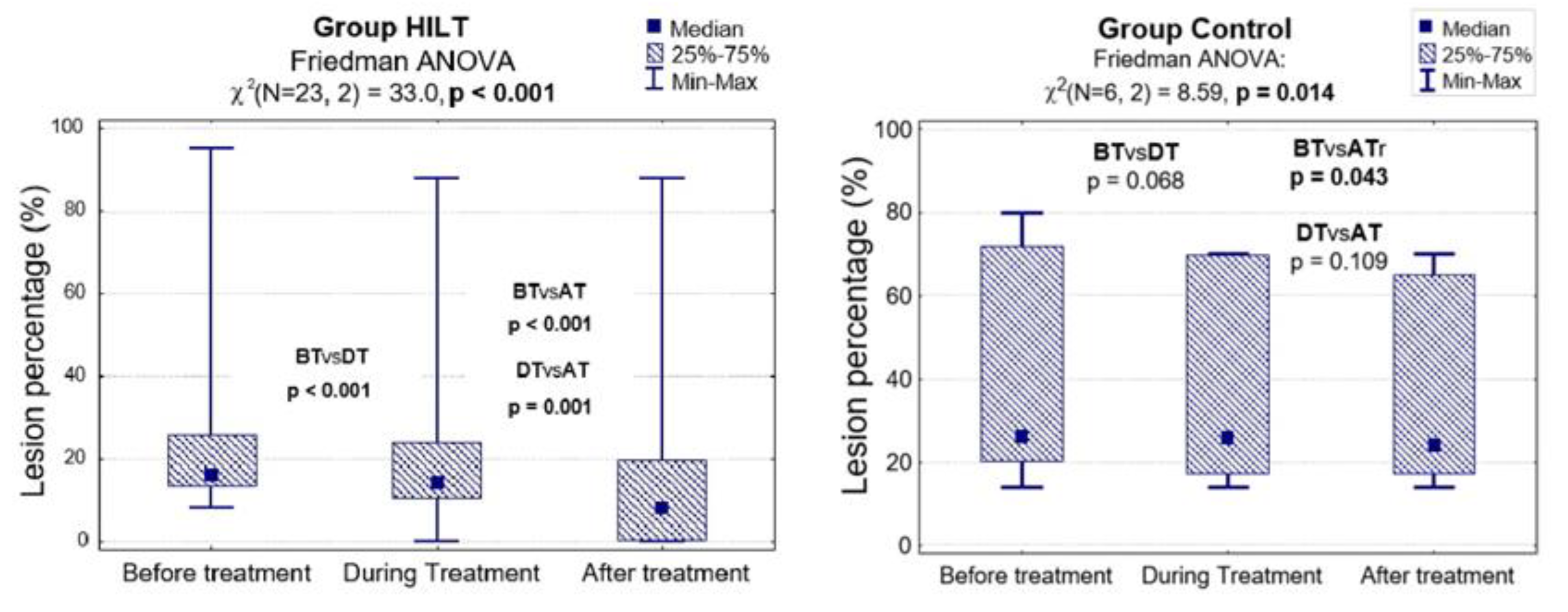
3.3.2. Lesion Percentage
4. Discussion
5. Conclusions
Author Contributions
Funding
Acknowledgments
Conflicts of Interest
References
- Södersten, F. Cartilage oligomeric matrix protein (COMP), thrombospondin-4 (TSP-4) and type I and III collagens in tendon. Acta Univ. Agric. Suec. 2006, 94, 11–12. [Google Scholar]
- Dyson, S.J. Medical management of superficial digital flexor tendonitis: A comparative study in 219 horses (1992–2000). Equine Veter. J. 2004, 36, 415–419. [Google Scholar] [CrossRef] [PubMed]
- Dahlgren, L.A. Pathobiology of tendon and ligament injuries. Clin. Tech. Equine Pr. 2007, 6, 168–173. [Google Scholar] [CrossRef]
- Lin, T.W.; Cardenas, L.; Soslowsky, L.J. Biomechanics of tendon injury and repair. J. Biomech. 2004, 37, 865–877. [Google Scholar] [CrossRef]
- Van Schie, H.T.M.; Bakker, E.M.; Cherdchutham, W.; Jonker, A.M.; Van De Lest, C.H.; Van Weeren, R. Monitoring of the repair process of surgically created lesions in equine superficial digital flexor tendons by use of computerized ultrasonography. Am. J. Vet. Res. 2009, 70, 37–48. [Google Scholar] [CrossRef]
- Bosch, G.; Moleman, M.; Barneveld, A.; Van Weeren, P.R.; Van Schie, H.T.M. The effect of platelet-rich plasma on the neovascularization of surgically created equine superficial digital flexor tendon lesions. Scand. J. Med. Sci. Sports 2010, 21, 554–561. [Google Scholar] [CrossRef]
- Davis, C.S.; Smith, R.K. Diagnosis and management of tendon and ligament disorders. In Equine Surgery, 3rd ed.; Auer, J.A., Stick, J.A., Eds.; Saunders Elsevier: St. Louis, MO, USA, 2006; pp. 1086–1111. [Google Scholar]
- Zielińska, P.; Soroko, M.; Zwyrzykowska, A.; Kiełbowicz, Z. The use of laser biostimulation in human and animal physiotherapy—A review. Acta Vet. Brno 2017, 86, 91–96. [Google Scholar] [CrossRef]
- Fortuna, D.; Rossi, G.; Paolini, C.; Magi, A.; Losani, F.; Fallaci, S.; Pacini, F.; Porciani, C.; Sandler, A.; Torre, R.D.; et al. Nd:YAG pulsed-wave laser as support therapy in the treatment of teno-desmopathies of athlete horses: A clinical and experimental trial. In Proceedings of the SPIE 4903, Laser Florence 2001: A Window on the Laser Medicine World, Florence, Italy, 7–11 November 2001; pp. 105–118. [Google Scholar] [CrossRef]
- Pluim, M.; Martens, A.; Vanderperren, K.; Sarrazin, S.; Koene, M.; Luciani, A.; Van Weeren, P.; Delesalle, C. Short- and long term follow-up of 150 sports horses diagnosed with tendinopathy or desmopathy by ultrasonographic examination and treated with high-power laser therapy. Res. Vet. Sci. 2018, 119, 232–238. [Google Scholar] [CrossRef]
- Santamato, A.; Solfrizzi, V.; Panza, F.; Tondi, G.; Frisardi, V.; Leggin, B.G.; Ranieri, M.; Fiore, P. Short-term effects of high-intensity laser therapy versus ultrasound therapy in the treatment of people with subacromial impingement syndrome: A randomized clinical trial. Phys. Ther. 2009, 89, 643–652. [Google Scholar] [CrossRef]
- Voronkov, M.G.; Motorina, I.G.; Iushkov, G.G.; Benemanski, V.V.; Rasulov, M.M.; Snisarenko, T.A.; Abzaeva, K.A.; Shukina, O.G.; Malishkina, N.A. Effect of laser radiation of infrared and red range on healing of burn wounds. Dokl. Biochem. Biophys. 2014, 456, 85–87. [Google Scholar] [CrossRef]
- Albertini, R.; Villaverde, A.; Aimbire, F.; Salgado, M.; Bjordal, J.; Alves, L.P.; Munin, E.; Costa, M. Anti-inflammatory effects of low-level laser therapy (LLLT) with two different red wavelengths (660nm and 684nm) in carrageenan-induced rat paw edema. J. Photochem. Photobiol. B: Boil. 2007, 89, 50–55. [Google Scholar] [CrossRef]
- Alayat, M.S.M.; Atya, A.; Ali, M.M.E.; Shosha, T.M. Long-term effect of high-intensity laser therapy in the treatment of patients with chronic low back pain: A randomized blinded placebo-controlled trial. Lasers Med. Sci. 2013, 29, 1065–1073. [Google Scholar] [CrossRef] [PubMed]
- Kheshie, A.R.; Alayat, M.S.M.; Ali, M.M.E. High-intensity versus low-level laser therapy in the treatment of patients with knee osteoarthritis: A randomized controlled trial. Lasers Med. Sci. 2014, 29, 1371–1376. [Google Scholar] [CrossRef] [PubMed]
- Moore, P.; Ridgway, T.D.; Higbee, R.G.; Howard, E.W.; Lucroy, M.D. Effect of wavelength on low-intensity laser irradiation-stimulated cell proliferation in vitro. Lasers Surg. Med. 2005, 36, 8–12. [Google Scholar] [CrossRef]
- Young, S.; Bolton, P.; Dyson, M.; Harvey, W.; Diamantopoulos, C. Macrophage responsiveness to light therapy. Lasers Surg. Med. 1989, 9, 497–505. [Google Scholar] [CrossRef] [PubMed]
- Passarella, S.; Casamassima, E.; Molinari, S.; Pastore, D.; Quagliariello, E.; Catalano, I.; Cingolani, A. Increase of proton electrochemical potential and ATP synthesis in rat liver mitochondria irradiated in vitro by helium-neon laser. FEBS Lett. 1984, 175, 95–99. [Google Scholar] [CrossRef]
- Fiore, P.; Panza, F.; Cassatella, G.; Russo, A.; Frisardi, V.; Solfrizzi, V.; Ranieri, M.; Di Teo, L.; Santamato, A. Short-term effects of high-intensity laser therapy versus ultrasound therapy in the treatment of low back pain: A randomized controlled trial. Eur. J. Phys. Rehabil. Med. 2011, 47, 367–373. [Google Scholar]
- Quiney, L.; Murray, R.; Dyson, S. Management of primary injuries of the medial collateral ligament of the carpus in two horses. J. Equine Vet. Sci. 2020, 86, 102878. [Google Scholar] [CrossRef]
- Zielińska, P.; Kiełbowicz, Z.; Paczuska, J. High Intensity Laser Therapy (HILT) in treatment of orthopedic diseases in horses. Med. Weter. 2015, 7, 373–376. [Google Scholar]
- Ashley, F.H.; E Waterman-Pearson, A.; Whay, H.R. Behavioural assessment of pain in horses and donkeys: Application to clinical practice and future studies. Equine Vet. J. 2005, 37, 565–575. [Google Scholar] [CrossRef]
- Bussières, G.; Jacques, C.; Lainay, O.; Beauchamp, G.; Leblond, A.; Cadoré, J.-L.; Desmaizières, L.-M.; Cuvelliez, S.; Troncy, E. Development of a composite orthopaedic pain scale in horses. Res. Vet. Sci. 2008, 85, 294–306. [Google Scholar] [CrossRef] [PubMed]
- AAEP. Guide to Veterinary Services for Horse Shows, 7th ed.; AAEP: Lexington, KY, USA, 1999. [Google Scholar]
- Genovese, R.L.; Rantanen, N.W.; Hauser, M.L.; Simpson, B.S. Clinical application of diagnostic ultrasound to the equine limb. Proc. Annu. Conv. AAEP 1985, 31, 701–721. [Google Scholar]
- Genovese, J.W. Laser de Baixa Intensidade: Aplicações Terapêuticas em Odontologia; Lovise Ltda: São Paulo, Brasil, 2000; pp. 170–175. (In Portuguese) [Google Scholar]
- Brown, A.W.; Weber, D.C. Physical agent modalities. In Physical Medicine and Rehabilitation; Braddom, R.L., Ed.; WB Saunders, Harcourt Health Sciences Company: London, UK, 2000; pp. 440–458. [Google Scholar]
- Frigo, L.; Fávero, G.M.; Lima, H.J.C.; Maria, D.A.; Bjordal, J.M.; Joensen, J.; Iversen, V.V.; Marcos, R.L.; Parizzoto, N.A.; Lopes-Martins, R.A. Low-level laser irradiation (InGaAlP-660 nm) increases fibroblast cell proliferation and reduces cell death in a dose-dependent manner. Photomed. Laser Surg. 2010, 28, 151–156. [Google Scholar] [CrossRef] [PubMed]
- Nicolau, R.A.; Martinez, M.S.; Rigau, J.; Tomàs, J. Neurotransmitter release changes induced by low power 830 nm diode laser irradiation on the neuromuscular junctions of the mouse. Lasers Surg. Med. 2004, 35, 236–241. [Google Scholar] [CrossRef] [PubMed]
- Wakabayashi, H.; Hamba, M.; Matsumoto, K.; Tachibana, H. Effect of irradiation by semiconductor laser on responses evoked intrigeminal caudal neurons by tooth pulp stimulation. Lasers Surg. Med. 1993, 13, 605–610. [Google Scholar] [CrossRef] [PubMed]
- Lievens, P.C. The effect of a combined HeNe and i.r. laser treatment on the regeneration of the lymphatic system during the process of wound healing. Lasers Med. Sci. 1991, 6, 193–199. [Google Scholar] [CrossRef]
- Stiglić-Rogoznica, N.; Stamenković, D.; Frlan-Vrgoc, L.; Avancini-Dobrović, V.; Vrbanić, T.S.-L. Analgesic effect of high intensity laser therapy in knee osteoarthritis. Coll. Antropol. 2011, 35, 183–185. [Google Scholar]
- Tsuchiya, K.; Kawatani, M.; Takeshige, C.; Matsumoto, I. Laser irradiation abates neuronal responses to nociceptive stimulation of rat-paw skin. Brain Res. Bull. 1994, 34, 369–374. [Google Scholar] [CrossRef]
- Gelberman, R.H.; Manske, P.R.; Berg, J.S.V.; Lesker, P.A.; Akeson, W.H. Flexor tendon repairin vitro: A comparative histologic study of the rabbit, chicken, dog, and monkey. J. Orthop. Res. 1984, 2, 39–48. [Google Scholar] [CrossRef] [PubMed]
- Potenza, A.D. Tendon healing within the flexor digital sheath in the dog: An experimental study. Am. J. Orthop. 1962, 44, 49–64. [Google Scholar] [CrossRef]
- Lundborg, G.; Rank, F. Experimental studies on cellular mechanisms involved in healing of animal and human flexor tendon in synovial environment. Hand 1980, 1, 3–11. [Google Scholar] [CrossRef]
- Voleti, P.; Buckley, M.R.; Soslowsky, L.J. Tendon healing: Repair and regeneration. Annu. Rev. Biomed. Eng. 2012, 14, 47–71. [Google Scholar] [CrossRef] [PubMed]
- Manske, P.R.; Gelberman, R.H.; A Lesker, P. Flexor tendon healing. Hand Clin. 1985, 1, 25–34. [Google Scholar] [CrossRef]
- Marcos, R.L.; Junior, E.C.L.; Arnold, G.; Magnenet, V.; Rahouadj, R.; Wang, X.; Demeurie, F.; Magdalou, J.; De Carvalho, M.H.C.; Lopes-Martins, R.A. Low-level laser therapy in collagenase-induced Achilles tendinitis in rats: Analyses of biochemical and biomechanical aspects. J. Orthop. Res. 2012, 30, 1945–1951. [Google Scholar] [CrossRef]
- Notarnicola, A.; Maccagnano, G.; Silvio, T.; Forcignanò, M.I.; Panella, A.; Moretti, B. CHELT therapy in the treatment of chronic insertional Achilles tendinopathy. Lasers Med. Sci. 2013, 29, 1217–1225. [Google Scholar] [CrossRef]
- Evangelos, N.P.T.; Anorthosis, P.T.; Dimitrios, S. Treatment of chronic patellar tendinopathy using an exercise program consisting of eccentric training and static stretching exercises combined with high intensity light therapy. A pilot study. MOJ Orthop. Rheumatol. 2018, 10, 157–161. [Google Scholar]
| Clinical Assessment and Ultrasound Examination | Degree of Pain | Degree of Lameness | Degree of Lesion Echogenicity | ||||||
|---|---|---|---|---|---|---|---|---|---|
| Group HILT N = 23 | Group C N = 6 | HILT vs. C p-Value | Group HILT N = 23 | Group C N = 6 | HILT vs. C p-Value | Group HILT N = 23 | Group C N = 6 | HILT vs. C p-Value | |
| Degree | n (%) | n (%) | n (%) | n (%) | n (%) | n (%) | n (%) | n (%) | n (%) |
| Before treatment | 0.772 | 0.254 | 0.667 | ||||||
| 0 | 3 (13.0) | 0 (0.0) | 3 (13.0) | 0 (0.0) | 0 (0.0) | 0 (0.0) | |||
| 1 | 8 (34.8) | 2 (33.3) | 2 (8.7) | 2 (33.3) | 4 (17.4) | 2 (33.3) | |||
| 2 | 10 (43.5) | 3 (50.0) | 8 (34.8) | 3 (50.0) | 11 (47.8) | 2 (33.3) | |||
| 3 | 2 (8.7) | 1 (16.7) | 10 (43.5) | 1 (16.7) | 8 (34.8) | 2 (33.3) | |||
| During treatment | 0.100 | 0.596 | 0.188 | ||||||
| 0 | 6 (26.1) | 0 (0.0) | 5 (21.7) | 0 (0.0) | 1 (4.3) | 0 (0.0) | |||
| 1 | 13 (56.6) | 2 (33.3) | 8 (34.8) | 3 (50.0) | 14 (60.9) | 2 (33.3) | |||
| 2 | 3 (13.0) | 3 (50.0) | 8 (34.8) | 2 (33.3) | 7 (30.5) | 2 (33.3) | |||
| 3 | 1 (4.3) | 1 (16.7) | 2 (8.7) | 1 (16.7) | 1 (4.3) | 2 (33.3) | |||
| After treatment | 0.023 | 0.044 | 0.070 | ||||||
| 0 | 14 (60.9) | 1 (16.7) | 12 (52.2) | 0 (0.0) | 10 (43.5) | 0 (0.0) | |||
| 1 | 8 (34.8) | 2 (33.3) | 7 (30.4) | 3 (50.0) | 8 (34.8) | 0 (50.0) | |||
| 2 | 1 (4.3) | 2 (33.3) | 4 (17.4) | 2 (33.3) | 4 (17.4) | 2 (33.3) | |||
| 3 | 0 (0.0) | 1 (16.7) | 0 (0.0) | 1 (16.7) | 1 (4.3) | 4 (66.7) | |||
| Degree of reduction p-value | <0.001 | 0.895 | - | <0.001 | 0.970 | - | <0.001 | 0.558 | - |
| Relative Swelling | Group HILT N = 23 | Group C N = 6 | HILT vs. C p-Value |
|---|---|---|---|
| Before treatment (%): | 0.144 | ||
| Me [Q1; Q3] | 6 [4; 11] | 8 [6; 15] | |
| Min–Max | 0–15 | 2–16 | |
| During treatment (%) | 0.024 | ||
| Me [Q1; Q3] | 3 [2; 5] | 7 [5; 11] | |
| Min–Max | 0–12 | 2–14 | |
| After treatment (%) | 0.008 | ||
| Me [Q1; Q3] | 2 [0; 3] | 6 [4; 8] | |
| Min–Max | 0–12 | 2–14 | |
| ANOVA: p-value | <0.001 | 0.667 | - |
| Lesion Percentage (%) | Group HILT N = 23 | Group C N = 6 | HILT vs. C p-Value |
|---|---|---|---|
| Before treatment (%) | 0.085 | ||
| Me [Q1; Q3] | 16 [13; 26] | 26 [20; 72] | |
| Min–Max | 8–95 | 14–80 | |
| During treatment (%) | 0.038 | ||
| Me [Q1; Q3] | 14 [10; 24] | 26 [17; 70] | |
| Min–Max | 0–88 | 14–70 | |
| After treatment (%) | 0.019 | ||
| Me [Q1; Q3] | 8 [0; 20] | 24 [17; 65] | |
| Min–Max | 0–88 | 14–70 | |
| ANOVA: p-value | <0.001 | 0.014 | - |
© 2020 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Zielińska, P.; Nicpoń, J.; Kiełbowicz, Z.; Soroko, M.; Dudek, K.; Zaborski, D. Effects of High Intensity Laser Therapy in the Treatment of Tendon and Ligament Injuries in Performance Horses. Animals 2020, 10, 1327. https://doi.org/10.3390/ani10081327
Zielińska P, Nicpoń J, Kiełbowicz Z, Soroko M, Dudek K, Zaborski D. Effects of High Intensity Laser Therapy in the Treatment of Tendon and Ligament Injuries in Performance Horses. Animals. 2020; 10(8):1327. https://doi.org/10.3390/ani10081327
Chicago/Turabian StyleZielińska, Paulina, Jakub Nicpoń, Zdzisław Kiełbowicz, Maria Soroko, Krzysztof Dudek, and Daniel Zaborski. 2020. "Effects of High Intensity Laser Therapy in the Treatment of Tendon and Ligament Injuries in Performance Horses" Animals 10, no. 8: 1327. https://doi.org/10.3390/ani10081327
APA StyleZielińska, P., Nicpoń, J., Kiełbowicz, Z., Soroko, M., Dudek, K., & Zaborski, D. (2020). Effects of High Intensity Laser Therapy in the Treatment of Tendon and Ligament Injuries in Performance Horses. Animals, 10(8), 1327. https://doi.org/10.3390/ani10081327





