A Systematic Review Comparing Experimental Design of Animal and Human Methotrexate Efficacy Studies for Rheumatoid Arthritis: Lessons for the Translational Value of Animal Studies
Simple Summary
Abstract
1. Introduction
2. Methods
2.1. Paper Search and Selection
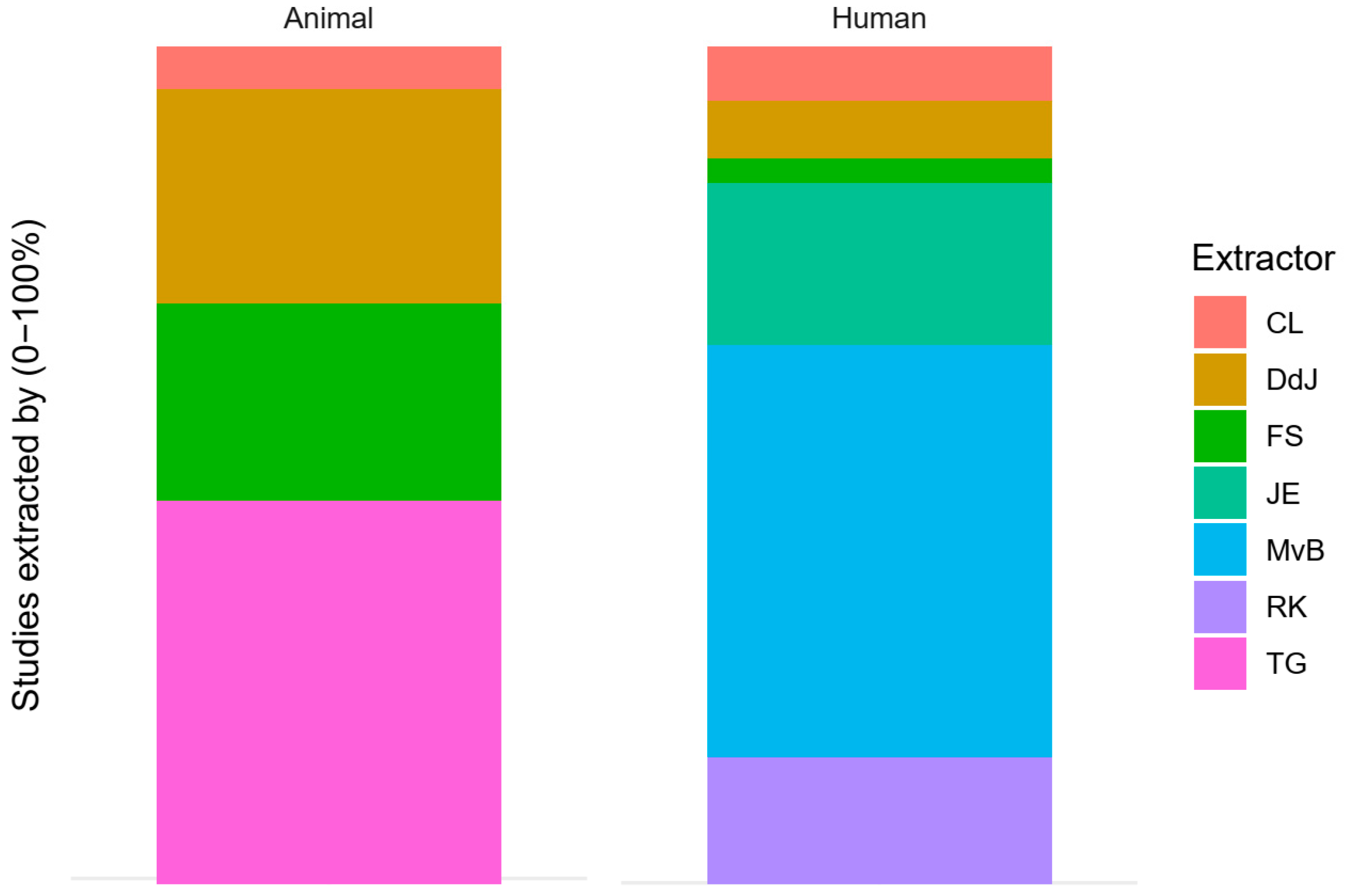
2.2. Data Extraction and Cleaning
2.3. Data Analysis
2.4. Protocol Deviations
3. Results
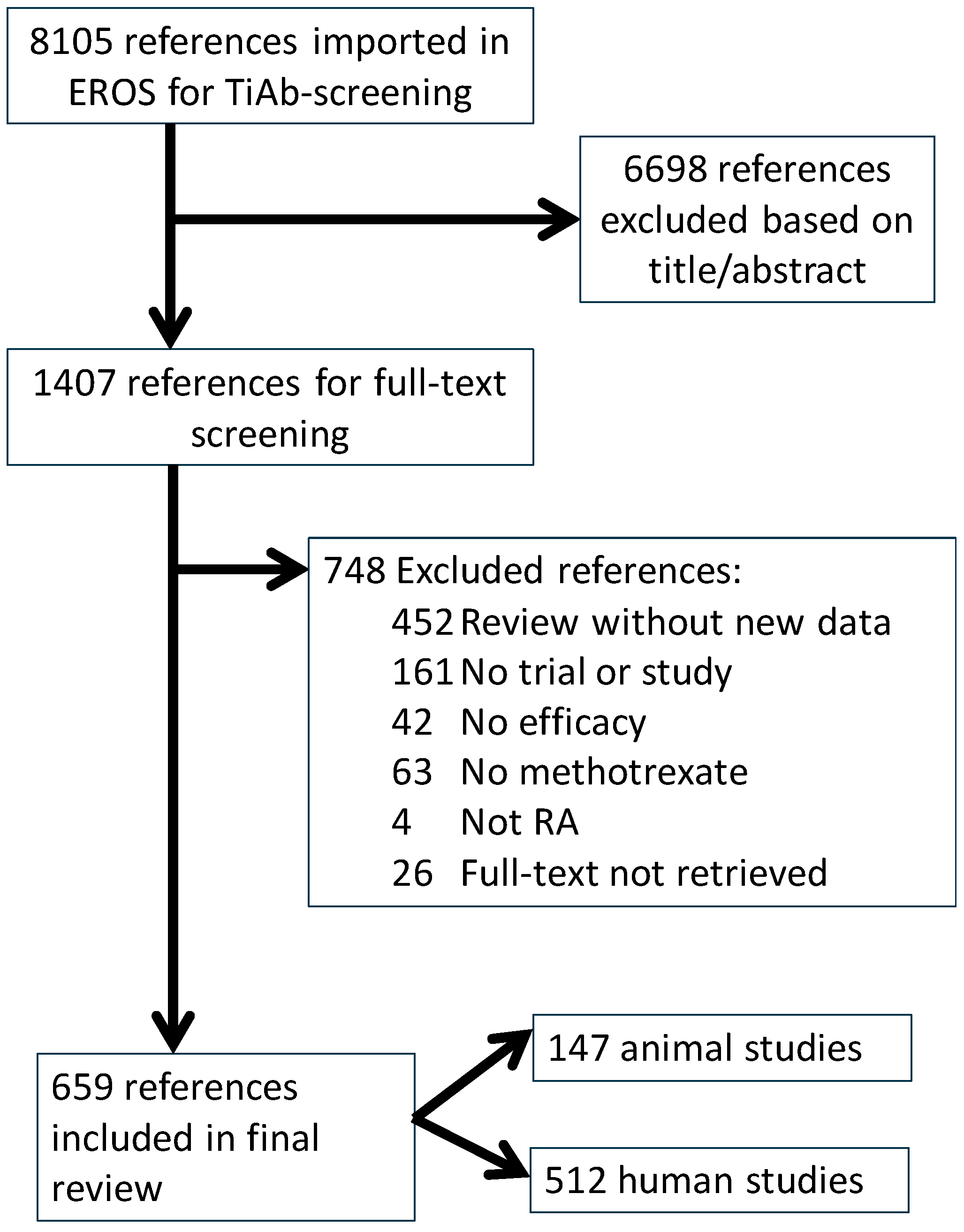
3.1. Paper Flow
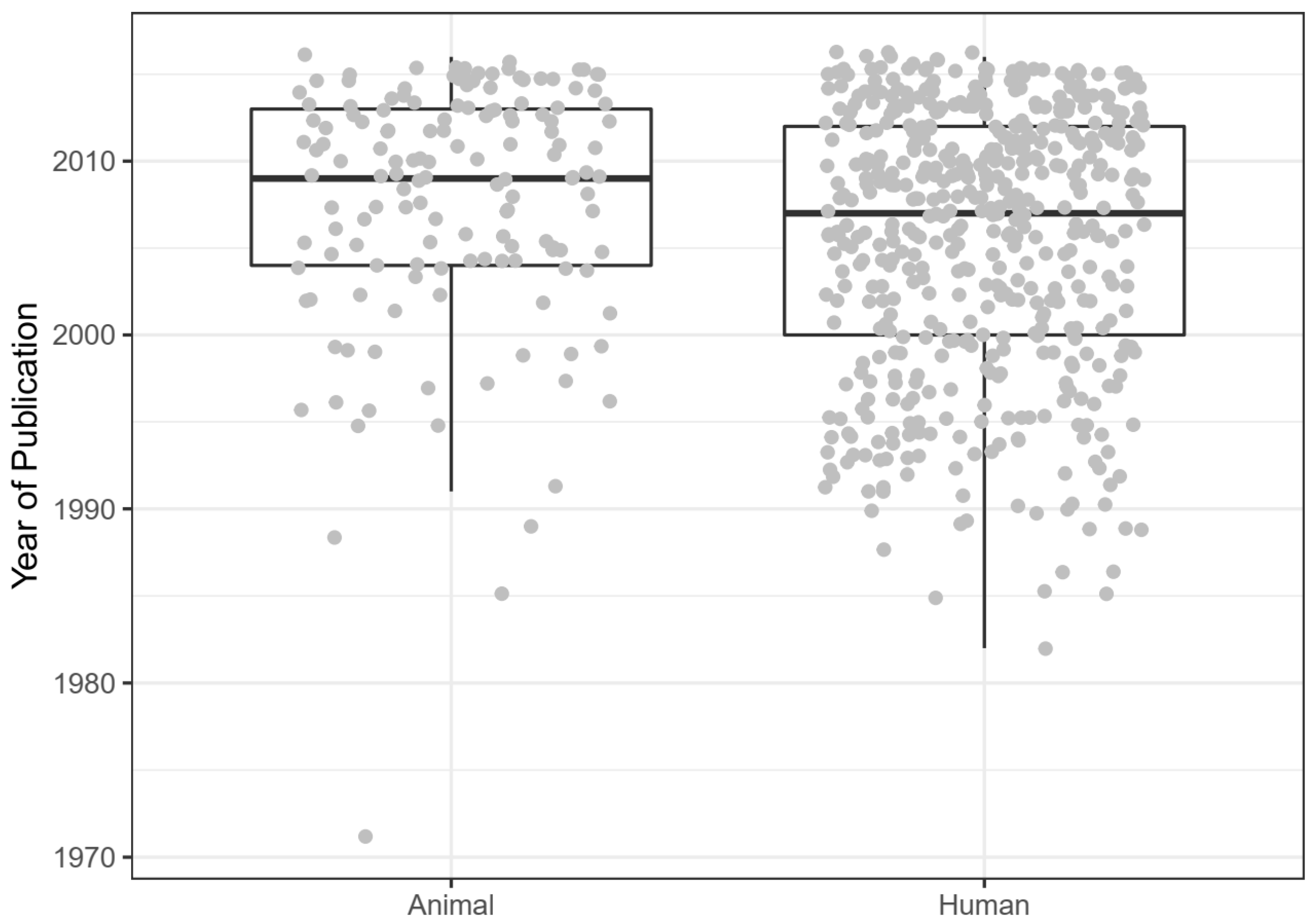
3.2. Bibliographic Details
3.3. Experimental Design in Animal and Human Trials
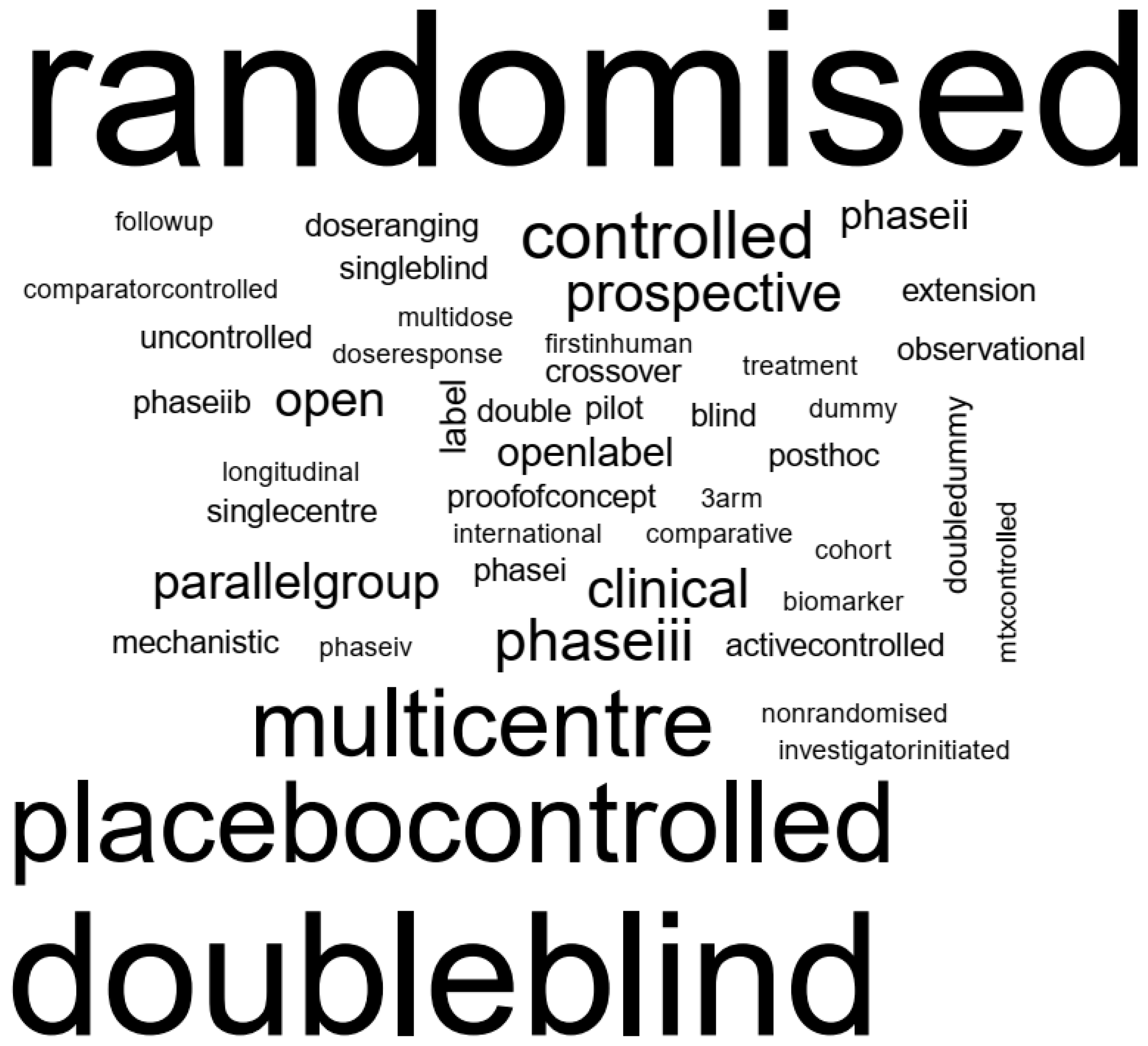
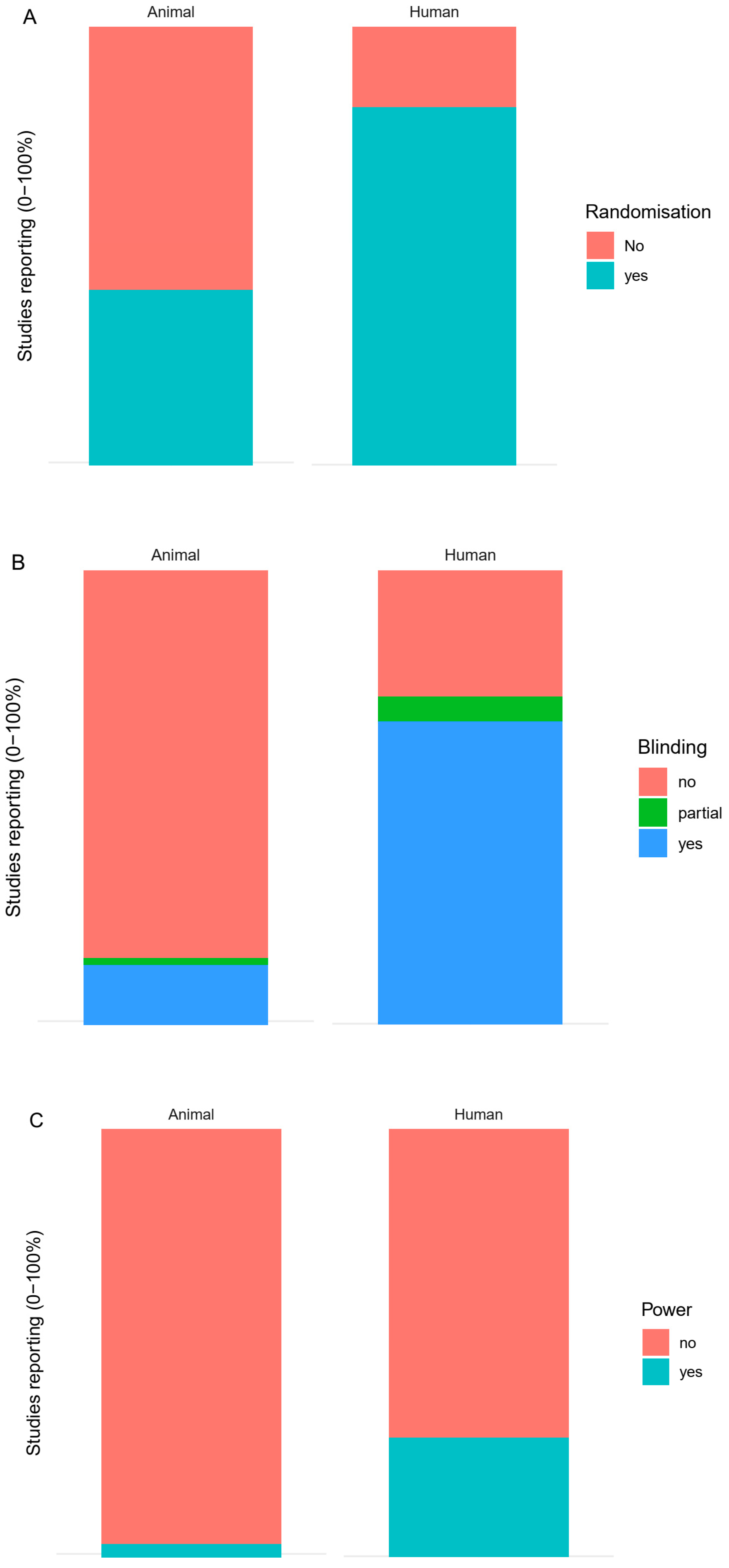
3.3.1. General Experimental Design
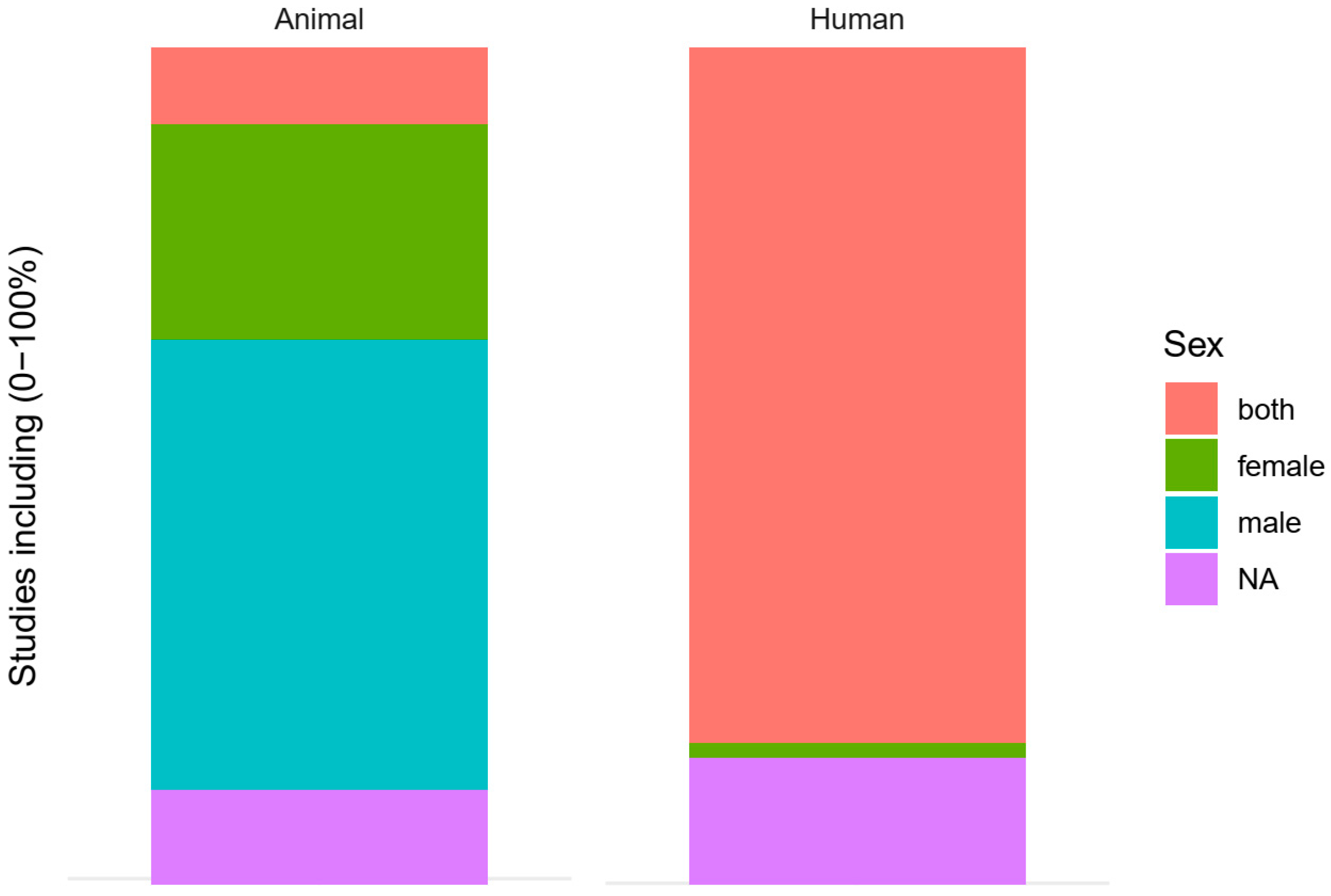
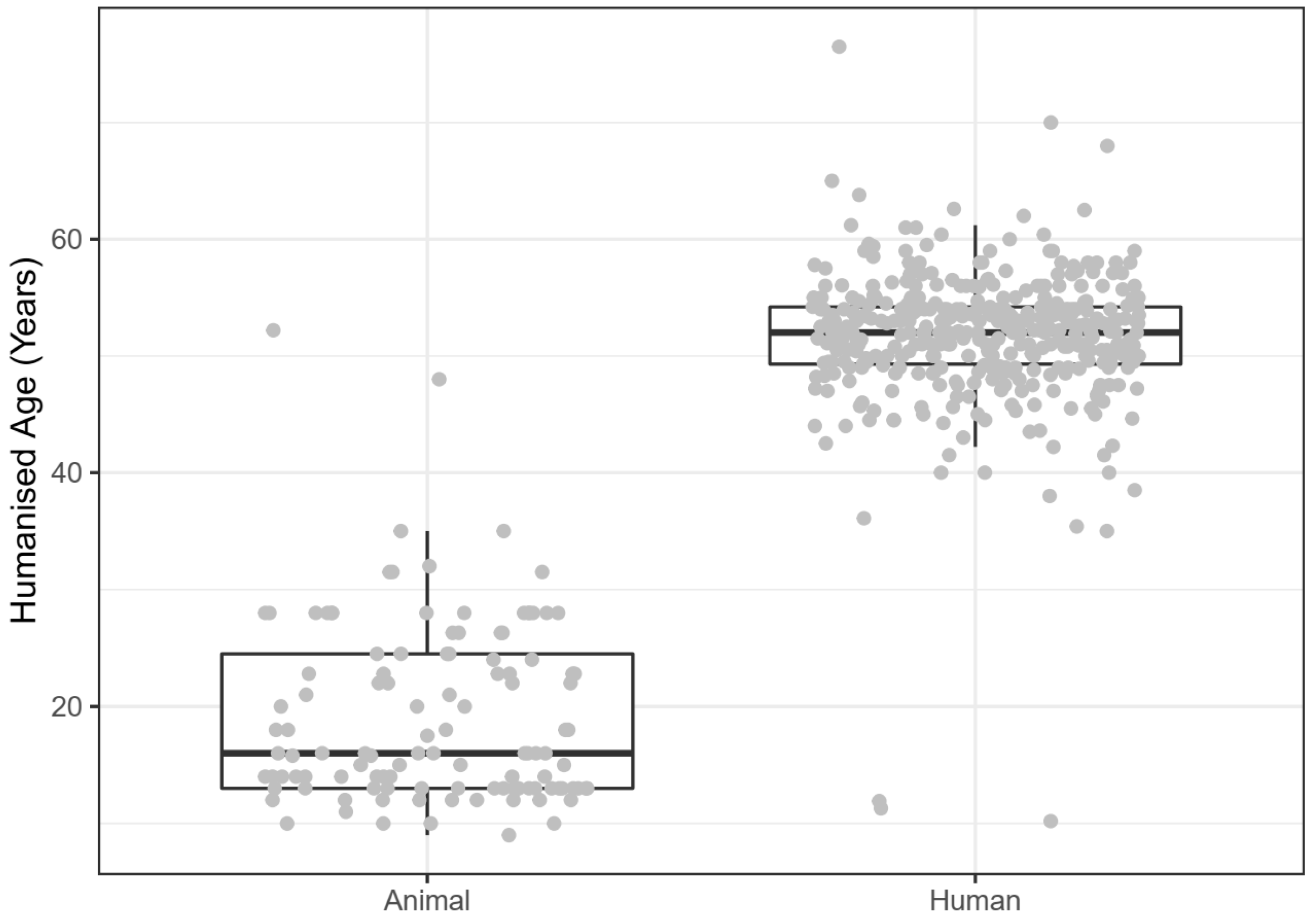
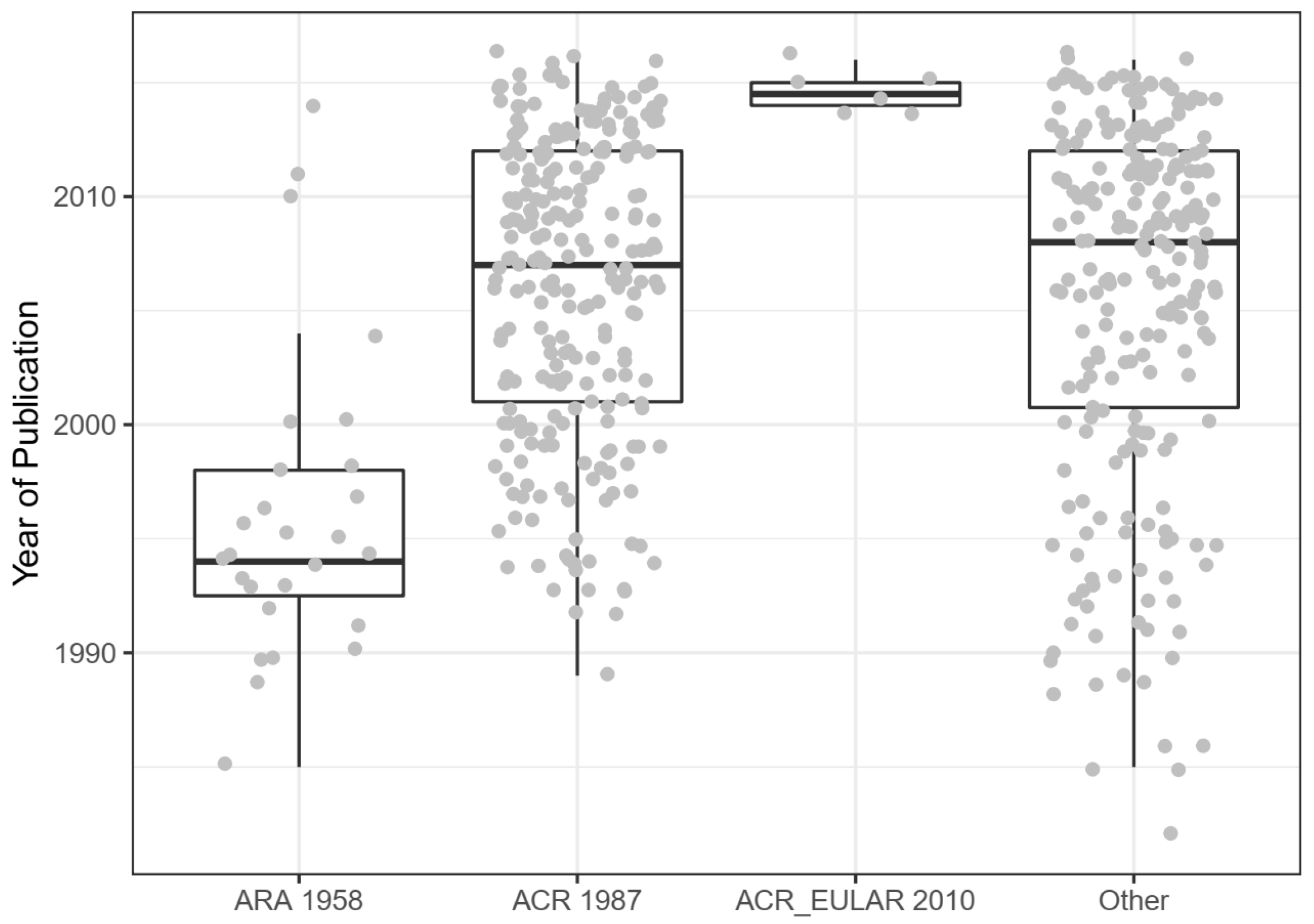
3.3.2. Tested Populations
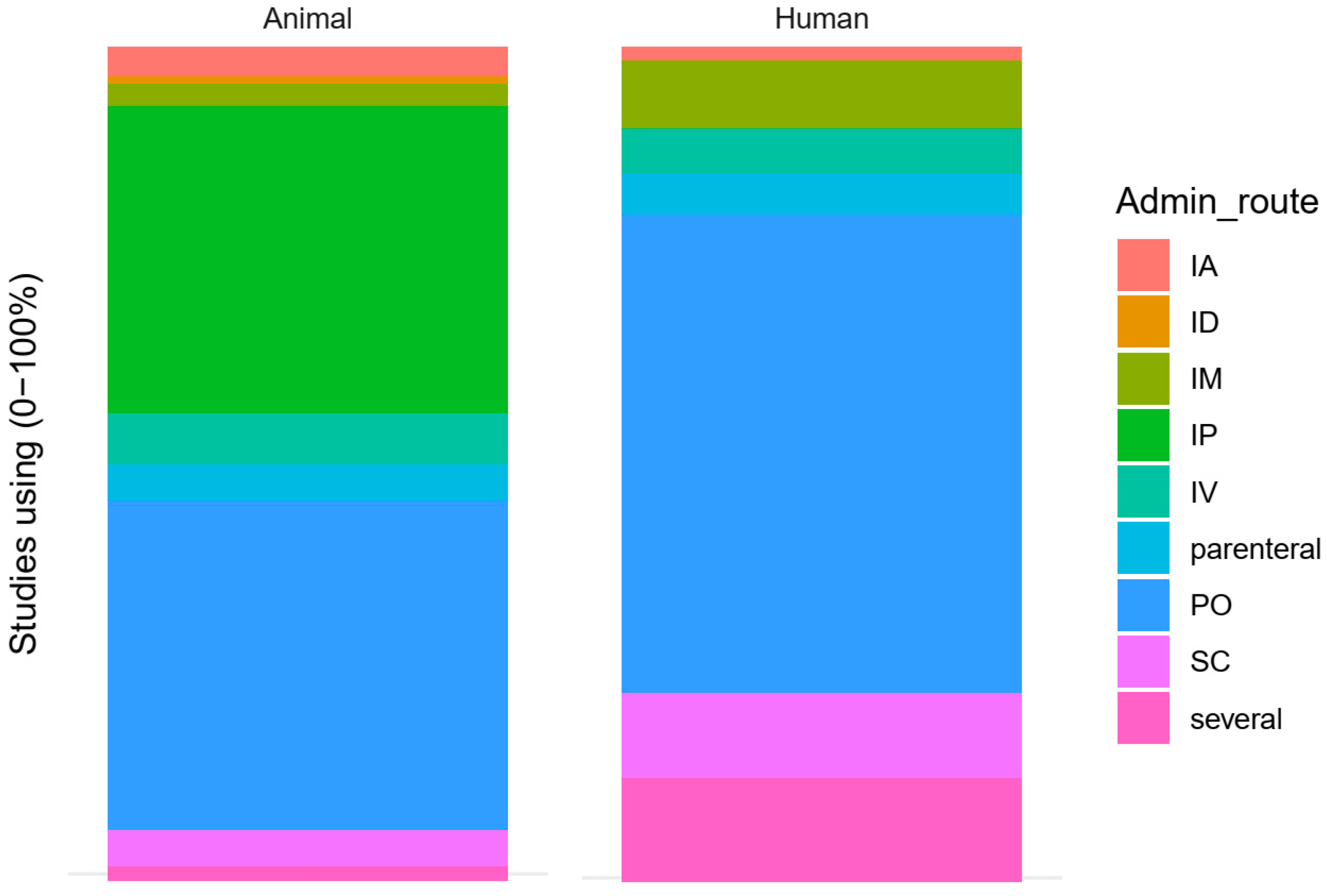
3.3.3. MTX Interventions
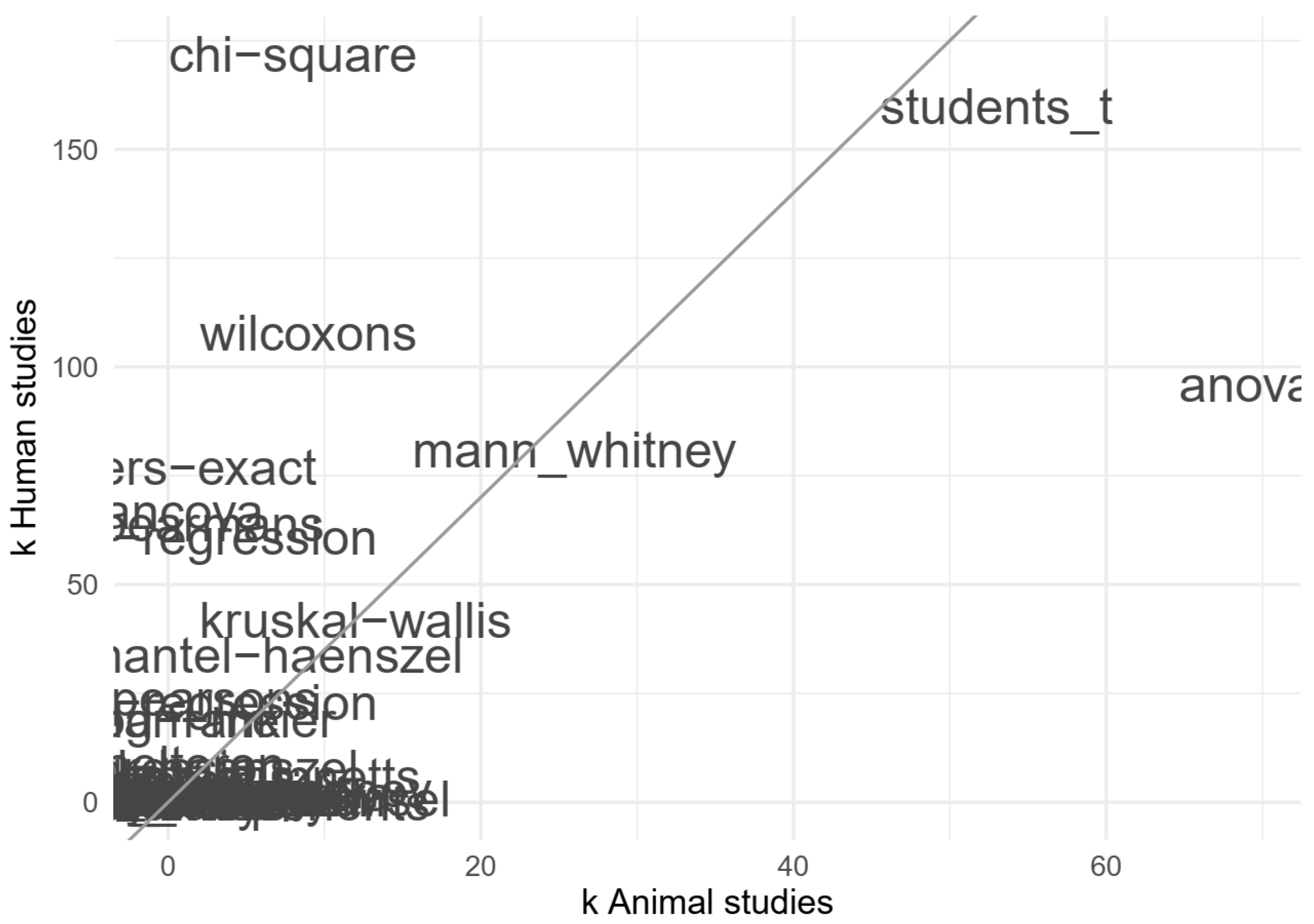
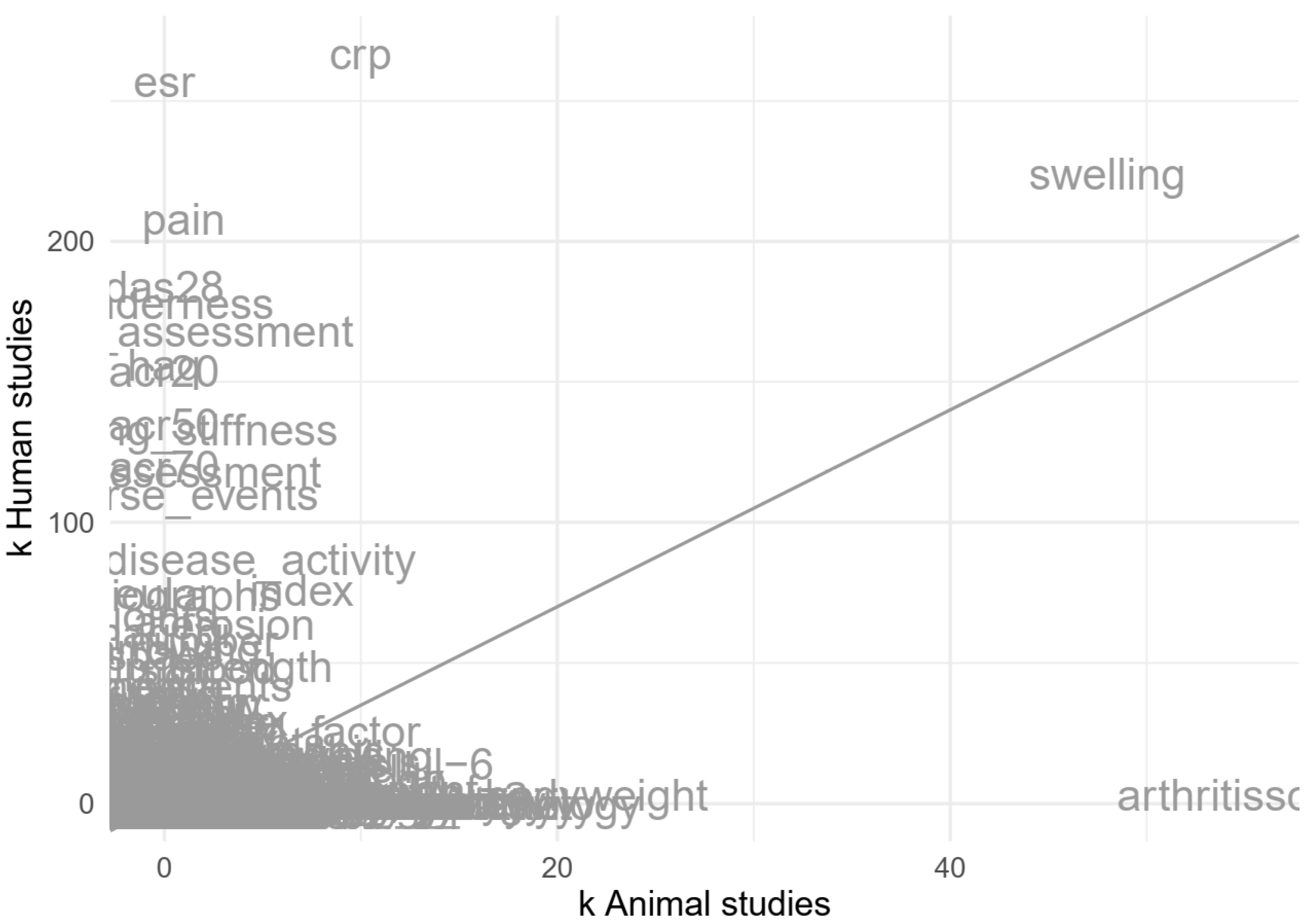
3.3.4. Analysed Outcome Measures
4. Discussion
5. Conclusions
Supplementary Materials
Author Contributions
Funding
Acknowledgments
Conflicts of Interest
References
- Leenaars, C.H.C.; Kouwenaar, C.; Stafleu, F.R.; Bleich, A.; Ritskes-Hoitinga, M.; De Vries, R.B.M.; Meijboom, F.L.B. Animal to human translation: A systematic scoping review of reported concordance rates. J. Transl. Med. 2019, 17, 223. [Google Scholar] [CrossRef]
- Sena, E.; van der Worp, H.B.; Howells, D.; Macleod, M. How can we improve the pre-clinical development of drugs for stroke? Trends Neurosci. 2007, 30, 433–439. [Google Scholar] [CrossRef]
- Hooijmans, C.R.; de Vries, R.B.; Rovers, M.M.; Gooszen, H.G.; Ritskes-Hoitinga, M. The effects of probiotic supplementation on experimental acute pancreatitis: A systematic review and meta-analysis. PLoS ONE 2012, 7, e48811. [Google Scholar] [CrossRef]
- Brossi, P.M.; Moreira, J.J.; Machado, T.S.; Baccarin, R.Y. Platelet-rich plasma in orthopedic therapy: A comparative systematic review of clinical and experimental data in equine and human musculoskeletal lesions. BMC Vet. Res. 2015, 11, 98. [Google Scholar] [CrossRef]
- Lee, D.S.; Nguyen, Q.T.; Lapointe, N.; Austin, P.C.; Ohlsson, A.; Tu, J.V.; Stewart, D.J.; Rouleau, J.L. Meta-analysis of the effects of endothelin receptor blockade on survival in experimental heart failure. J. Card. Fail. 2003, 9, 368–374. [Google Scholar] [CrossRef]
- Macleod, M.R.; Lawson McLean, A.; Kyriakopoulou, A.; Serghiou, S.; de Wilde, A.; Sherratt, N.; Hirst, T.; Hemblade, R.; Bahor, Z.; Nunes-Fonseca, C.; et al. Risk of Bias in Reports of In Vivo Research: A Focus for Improvement. PLoS Biol. 2015, 13, e1002273. [Google Scholar] [CrossRef] [PubMed]
- Cassotta, M.; Pistollato, F.; Battino, M. Rheumatoid arthritis research in the 21st century: Limitations of traditional models, new technologies, and opportunities for a human biology-based approach. ALTEX 2020, 37, 223–242. [Google Scholar] [CrossRef] [PubMed]
- Lopez-Olivo, M.A.; Siddhanamatha, H.R.; Shea, B.; Tugwell, P.; Wells, G.A.; Suarez-Almazor, M.E. Methotrexate for treating rheumatoid arthritis. Cochrane Database Syst. Rev. 2014. [Google Scholar] [CrossRef]
- Leenaars, C.H.; De Jong, D.H.; Coenen, T.; Stafleu, F.R.; De Vries, R.B.; Ritskes-Hoitinga, M. Experimental Design in Methotrexate Efficacy Studies for Rheumatoid Arthritis; SYRCLE: Nijmegen, The Netherlands, 2016. [Google Scholar]
- R_Core_Team. R: A Language and Environment for Statistical Computing; R_Core_Team: Vienna, Austria, 2020. [Google Scholar]
- Wickham, H.; Bryan, J. Readxl: Read Excel Files. R Package Version 1.3.1. Available online: https://CRAN.R-project.org/package=readxl (accessed on 6 May 2020).
- Wickham, H.; François, R.; Henry, L.; Müller, K. dplyr: A Grammar of Data Manipulation. R Package Version 0.8.5. Available online: https://CRAN.R-project.org/package=dplyr (accessed on 6 May 2020).
- Feinerer, I.; Hornik, K.; Meyer, D. Text Mining Infrastructure in R. J. Stat. Softw. 2008, 25, 1–54. [Google Scholar] [CrossRef]
- Wickham, H. ggplot2: Elegant Graphics for Data Analysis.; Springer: New York, NY, USA, 2016. [Google Scholar]
- Fellows, I. Wordcloud: Word Clouds. R Package Version 2.6. Available online: https://CRAN.R-project.org/package=wordcloud (accessed on 6 May 2020).
- South, A. rworldmap: A new r package for mapping global data. R J. 2011, 3, 35–43. [Google Scholar] [CrossRef]
- Faggion, C.M., Jr.; Chambrone, L.; Gondim, V.; Schmitter, M.; Tu, Y.K. Comparison of the effects of treatment of peri-implant infection in animal and human studies: Systematic review and meta-analysis. Clin. Oral. Implant. Res. 2010, 21, 137–147. [Google Scholar] [CrossRef]
- Sultan, S.R.; Millar, S.A.; England, T.J.; O’Sullivan, S.E. A systematic review and meta-analysis of the haemodynamic effects of cannabidiol. Front. Pharmacol. 2017, 8, 81. [Google Scholar] [CrossRef] [PubMed]
- Valles, C.; Rodriguez-Ciurana, X.; Clementini, M.; Baglivo, M.; Paniagua, B.; Nart, J. Influence of subcrestal implant placement compared with equicrestal position on the peri-implant hard and soft tissues around platform-switched implants: A systematic review and meta-analysis. Clin. Oral. Investig. 2018, 22, 555–570. [Google Scholar] [CrossRef] [PubMed]
- Yen, C.C.; Tu, Y.K.; Chen, T.H.; Lu, H.K. Comparison of treatment effects of guided tissue regeneration on infrabony lesions between animal and human studies: A systematic review and meta-analysis. J. Periodontal Res. 2014, 49, 415–424. [Google Scholar] [CrossRef] [PubMed]
- Leenaars, C.H.; Geurts, T.; Van der Mierden, S.; Den Broeder, A.; Staffleu, F.R.; Keubler, L.; De Vries, R.; Meijboom, F.L.B.; Ritskes-Hoitinga, M.; Tolba, R.; et al. Severity Assessment in Animal Models for Rheumatoid Arthritis—A Systematic Review. Available online: http://syrf.org.uk/protocols/ (accessed on 5 April 2020).
- Grotsch, B.; Bozec, A.; Schett, G. In Vivo Models of Rheumatoid Arthritis. Methods Mol. Biol. 2019, 1914, 269–280. [Google Scholar] [CrossRef] [PubMed]
- Aletaha, D.; Neogi, T.; Silman, A.J.; Funovits, J.; Felson, D.T.; Bingham, C.O., 3rd; Birnbaum, N.S.; Burmester, G.R.; Bykerk, V.P.; Cohen, M.D.; et al. 2010 Rheumatoid arthritis classification criteria: An American College of Rheumatology/European League Against Rheumatism collaborative initiative. Arthritis Rheum. 2010, 62, 2569–2581. [Google Scholar] [CrossRef] [PubMed]
- Matsuno, H.; Yoshida, K.; Ochiai, A.; Okamoto, M. Requirement of methotrexate in combination with anti-tumor necrosis factor-alpha therapy for adequate suppression of osteoclastogenesis in rheumatoid arthritis. J. Rheumatol. 2007, 34, 2326–2333. [Google Scholar]
- Delano, D.L.; Montesinos, M.C.; Desai, A.; Wilder, T.; Fernandez, P.; Eustachio, P.; Wiltshire, T.; Cronstein, B.N. Genetically based resistance to the antiinflammatory effects of methotrexate in the air-pouch model of acute inflammation. Arthritis Rheum. 2005, 52, 2567–2575. [Google Scholar] [CrossRef]
- Liang, Q.H.; Li, C.Y.; He, J.H.; Chen, J.; Li, X.L.; Wang, A.Y.; Tang, T.F. Effect of bizhongxiao decoction on the expression of vascular endothelial growth factor in the synovial membrane and symptom of rheumatoid arthritis in rats. Chin. J. Clin. Rehabil. 2004, 27, 2391–2393. [Google Scholar]
- Pigott, E.; Duhadaway, J.B.; Muller, A.J.; Gilmour, S.; Prendergast, G.C.; Mandik-Nayak, L. 1-Methyl-tryptophan synergizes with methotrexate to alleviate arthritis in a mouse model of arthritis. Autoimmunity 2014, 47, 409–418. [Google Scholar] [CrossRef]
- Feketeova, L.; Jancova, P.; Moravcova, P.; Janegova, A.; Bauerova, K.; Ponist, S.; Mihalova, D.; Janega, P.; Babal, P. Effect of methotrexate on inflammatory cells redistribution in experimental adjuvant arthritis. Rheumatol. Int. 2012, 32, 3517–3523. [Google Scholar] [CrossRef] [PubMed]
- Xi, L.; Shao, F.L.; Liu, A.J. Effect of thalidomide on inflammatory factor expression in rats with collagen induced arthritis. J. Clin. Rehabil. Tissue Eng. Res. 2010, 14, 3666–3668. [Google Scholar]
- Zhang, L.; Li, P.; Song, S.; Liu, Y.; Wang, Q.; Chang, Y.; Wu, Y.; Chen, J.; Zhao, W.; Zhang, Y.; et al. Comparative efficacy of TACI-Ig with TNF-alpha inhibitor and methotrexate in DBA/1 mice with collagen-induced arthritis. Eur. J. Pharmacol. 2013, 708, 113–123. [Google Scholar] [CrossRef] [PubMed]
- Zhang, W.D.; Wang, P.M.; Han, R.X.; Zhang, T.S. Efficacy and safety evaluation of fire needling for rats with rheumatoid arthritis. Zhongguo Zhen Jiu Chin. Acupunct. Moxibustion 2013, 33, 334–338. [Google Scholar]
- Barsig, J.; Yam, G.; Lehner, M.D.; Beume, R. Methotrexate treatment suppresses local cytokine and chemokine production in rat adjuvant arthritis. Drugs Exp. Clin. Res. 2005, 31, 7–11. [Google Scholar]
- Chen, Z.; Tu, S.; Hu, Y.; Wang, Y.; Xia, Y.; Jiang, Y. Prediction of response of collagen-induced arthritis rats to methotrexate: An 1H-NMR-based urine metabolomic analysis. J. Huazhong Univ. Sci. Technol. Med Sci. 2012, 32, 438–443. [Google Scholar] [CrossRef]
- Abe, C.; Kikukawa, T.; Komatsu, Y. Combination therapy on murine arthritis - Salazosulfapyridine, bucillamine, and methotrexate. Int. J. Immunother. 1995, 11, 129–132. [Google Scholar]
- Shahin, D.; el Toraby, E.; Abdel-Malek, H.; Boshra, V.; Elsamanoudy, A.Z.; Shaheen, D. Effect of peroxisome proliferator-activated receptor gamma agonist (pioglitazone) and methotrexate on disease activity in rheumatoid arthritis (experimental and clinical study). Clin. Med. Insights Arthritis Musculoskelet. Disord. 2011, 4, 1–10. [Google Scholar] [CrossRef]
- Currey, H.L. A comparison of immunosuppressive and anti-inflammatory agents in the rat. Clin. Exp. Immunol. 1971, 9, 879–887. [Google Scholar]
- Willkens, R.F.; Watson, M.A. Methotrexate: A perspective of its use in the treatment of rheumatic diseases. J. Lab. Clin. Med. 1982, 100, 314–321. [Google Scholar]
- Malaviya, A.N. Landmark papers on the discovery of methotrexate for the treatment of rheumatoid arthritis and other systemic inflammatory rheumatic diseases: A fascinating story. Int. J. Rheum. Dis. 2016, 19, 844–851. [Google Scholar] [CrossRef] [PubMed]
- Pullar, T. Disease modifying drugs for rheumatoid arthritis: Yesterday’s treatment today or today’s treatment tomorrow? Br. J. Clin. Pharmacol. 1990, 30, 501–510. [Google Scholar] [CrossRef] [PubMed]
- Weinblatt, M.E. Methotrexate in rheumatoid arthritis: A quarter century of development. Trans Am. Clin. Climatol. Assoc. 2013, 124, 16–25. [Google Scholar] [PubMed]
- Ting, K.H.; Hill, C.L.; Whittle, S.L. Quality of reporting of interventional animal studies in rheumatology: A systematic review using the ARRIVE guidelines. Int. J. Rheum. Dis. 2015, 18, 488–494. [Google Scholar] [CrossRef]
- Singh, S.; Fumery, M.; Singh, A.G.; Singh, N.; Prokop, L.J.; Dulai, P.S.; Sandborn, W.J.; Curtis, J.R. Comparative Risk of Cardiovascular Events With Biologic and Synthetic Disease-Modifying Antirheumatic Drugs in Patients With Rheumatoid Arthritis: A Systematic Review and Meta-Analysis. Arthritis Care Res. 2020, 72, 561–576. [Google Scholar] [CrossRef]
- Wang, Y.; Zhao, R.; Gu, Z.; Dong, C.; Guo, G.; Li, L. Effects of glucocorticoids on osteoporosis in rheumatoid arthritis: A systematic review and meta-analysis. Osteoporos. Int. 2020. [Google Scholar] [CrossRef]
- Bebarta, V.; Luyten, D.; Heard, K. Emergency medicine animal research: Does use of randomization and blinding affect the results? Acad. Emerg. Med. 2003, 10, 684–687. [Google Scholar] [CrossRef]
- Schulz, K.F.; Grimes, D.A. Blinding in randomised trials: Hiding who got what. Lancet 2002, 359, 696–700. [Google Scholar] [CrossRef]
- Hooijmans, C.R.; Rovers, M.M.; de Vries, R.B.; Leenaars, M.; Ritskes-Hoitinga, M.; Langendam, M.W. SYRCLE’s risk of bias tool for animal studies. BMC Med. Res. Methodol. 2014, 14, 43. [Google Scholar] [CrossRef]
- Hirst, J.A.; Howick, J.; Aronson, J.K.; Roberts, N.; Perera, R.; Koshiaris, C.; Heneghan, C. The need for randomization in animal trials: An overview of systematic reviews. PLoS ONE 2014, 9, e98856. [Google Scholar] [CrossRef] [PubMed]
- Paludan-Muller, A.; Teindl Laursen, D.R.; Hrobjartsson, A. Mechanisms and direction of allocation bias in randomised clinical trials. BMC Med. Res. Methodol. 2016, 16, 133. [Google Scholar] [CrossRef] [PubMed]
- Probst, P.; Zaschke, S.; Heger, P.; Harnoss, J.C.; Huttner, F.J.; Mihaljevic, A.L.; Knebel, P.; Diener, M.K. Evidence-based recommendations for blinding in surgical trials. Langenbecks Arch. Surg. 2019, 404, 273–284. [Google Scholar] [CrossRef] [PubMed]
- Higginson, A.D.; Munafo, M.R. Current Incentives for Scientists Lead to Underpowered Studies with Erroneous Conclusions. PLoS Biol. 2016, 14, e2000995. [Google Scholar] [CrossRef] [PubMed]
- Mitchell, S.J.; Scheibye-Knudsen, M.; Longo, D.L.; de Cabo, R. Animal models of aging research: Implications for human aging and age-related diseases. Annu. Rev. Anim. Biosci. 2015, 3, 283–303. [Google Scholar] [CrossRef] [PubMed]
- Starr, M.E.; Saito, H. Sepsis in old age: Review of human and animal studies. Aging Dis. 2014, 5, 126–136. [Google Scholar] [CrossRef]
- Hegen, M.; Keith, J.C., Jr.; Collins, M.; Nickerson-Nutter, C.L. Utility of animal models for identification of potential therapeutics for rheumatoid arthritis. Ann. Rheum. Dis. 2008, 67, 1505–1515. [Google Scholar] [CrossRef]
- Dekkers, J.S.; Schoones, J.W.; Huizinga, T.W.; Toes, R.E.; van der Helm-van Mil, A.H. Possibilities for preventive treatment in rheumatoid arthritis? Lessons from experimental animal models of arthritis: A systematic literature review and meta-analysis. Ann. Rheum. Dis. 2017, 76, 458–467. [Google Scholar] [CrossRef]
- Voelkl, B.; Vogt, L.; Sena, E.S.; Wurbel, H. Reproducibility of preclinical animal research improves with heterogeneity of study samples. PLoS Biol. 2018, 16, e2003693. [Google Scholar] [CrossRef]
- de Vries, R.B.; Buma, P.; Leenaars, M.; Ritskes-Hoitinga, M.; Gordijn, B. Reducing the number of laboratory animals used in tissue engineering research by restricting the variety of animal models. Articular cartilage tissue engineering as a case study. Tissue Eng. Part B Rev. 2012, 18, 427–435. [Google Scholar] [CrossRef]
- Elsheemy, M.S.; Hasanin, A.H.; Mansour, A.; Mehrez, S.I.; Abdel-Bary, M. Etanercept improved anemia and decreased hepcidin gene expression in a rat model of rheumatoid arthritis. Biomed. Pharmacother. 2019, 112, 108740. [Google Scholar] [CrossRef]
- Huang, Q.Q.; Birkett, R.; Doyle, R.; Shi, B.; Roberts, E.L.; Mao, Q.; Pope, R.M. The Role of Macrophages in the Response to TNF Inhibition in Experimental Arthritis. J. Immunol. 2018, 200, 130–138. [Google Scholar] [CrossRef] [PubMed]
- Karagianni, N.; Kranidioti, K.; Fikas, N.; Tsochatzidou, M.; Chouvardas, P.; Denis, M.C.; Kollias, G.; Nikolaou, C. An integrative transcriptome analysis framework for drug efficacy and similarity reveals drug-specific signatures of anti-TNF treatment in a mouse model of inflammatory polyarthritis. PLoS Comput. Biol. 2019, 15, e1006933. [Google Scholar] [CrossRef] [PubMed]


© 2020 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Leenaars, C.; Stafleu, F.; de Jong, D.; van Berlo, M.; Geurts, T.; Coenen-de Roo, T.; Prins, J.-B.; Kempkes, R.; Elzinga, J.; Bleich, A.; et al. A Systematic Review Comparing Experimental Design of Animal and Human Methotrexate Efficacy Studies for Rheumatoid Arthritis: Lessons for the Translational Value of Animal Studies. Animals 2020, 10, 1047. https://doi.org/10.3390/ani10061047
Leenaars C, Stafleu F, de Jong D, van Berlo M, Geurts T, Coenen-de Roo T, Prins J-B, Kempkes R, Elzinga J, Bleich A, et al. A Systematic Review Comparing Experimental Design of Animal and Human Methotrexate Efficacy Studies for Rheumatoid Arthritis: Lessons for the Translational Value of Animal Studies. Animals. 2020; 10(6):1047. https://doi.org/10.3390/ani10061047
Chicago/Turabian StyleLeenaars, Cathalijn, Frans Stafleu, David de Jong, Maikel van Berlo, Tijmen Geurts, Tineke Coenen-de Roo, Jan-Bas Prins, Rosalie Kempkes, Janneke Elzinga, André Bleich, and et al. 2020. "A Systematic Review Comparing Experimental Design of Animal and Human Methotrexate Efficacy Studies for Rheumatoid Arthritis: Lessons for the Translational Value of Animal Studies" Animals 10, no. 6: 1047. https://doi.org/10.3390/ani10061047
APA StyleLeenaars, C., Stafleu, F., de Jong, D., van Berlo, M., Geurts, T., Coenen-de Roo, T., Prins, J.-B., Kempkes, R., Elzinga, J., Bleich, A., de Vries, R., Meijboom, F., & Ritskes-Hoitinga, M. (2020). A Systematic Review Comparing Experimental Design of Animal and Human Methotrexate Efficacy Studies for Rheumatoid Arthritis: Lessons for the Translational Value of Animal Studies. Animals, 10(6), 1047. https://doi.org/10.3390/ani10061047





