Antimicrobial Resistance and Virulence Properties of Campylobacter Spp. Originating from Domestic Geese in Poland
Simple summary
Abstract
1. Introduction
2. Material and Methods
2.1. Isolation of Bacterial Strains
2.2. Species Identification
2.3. Virulence Factor Genes
2.4. Antimicrobial Resistance
2.5. Statistical Analysis
3. Results
3.1. Isolation and Identification of Bacterial Strains
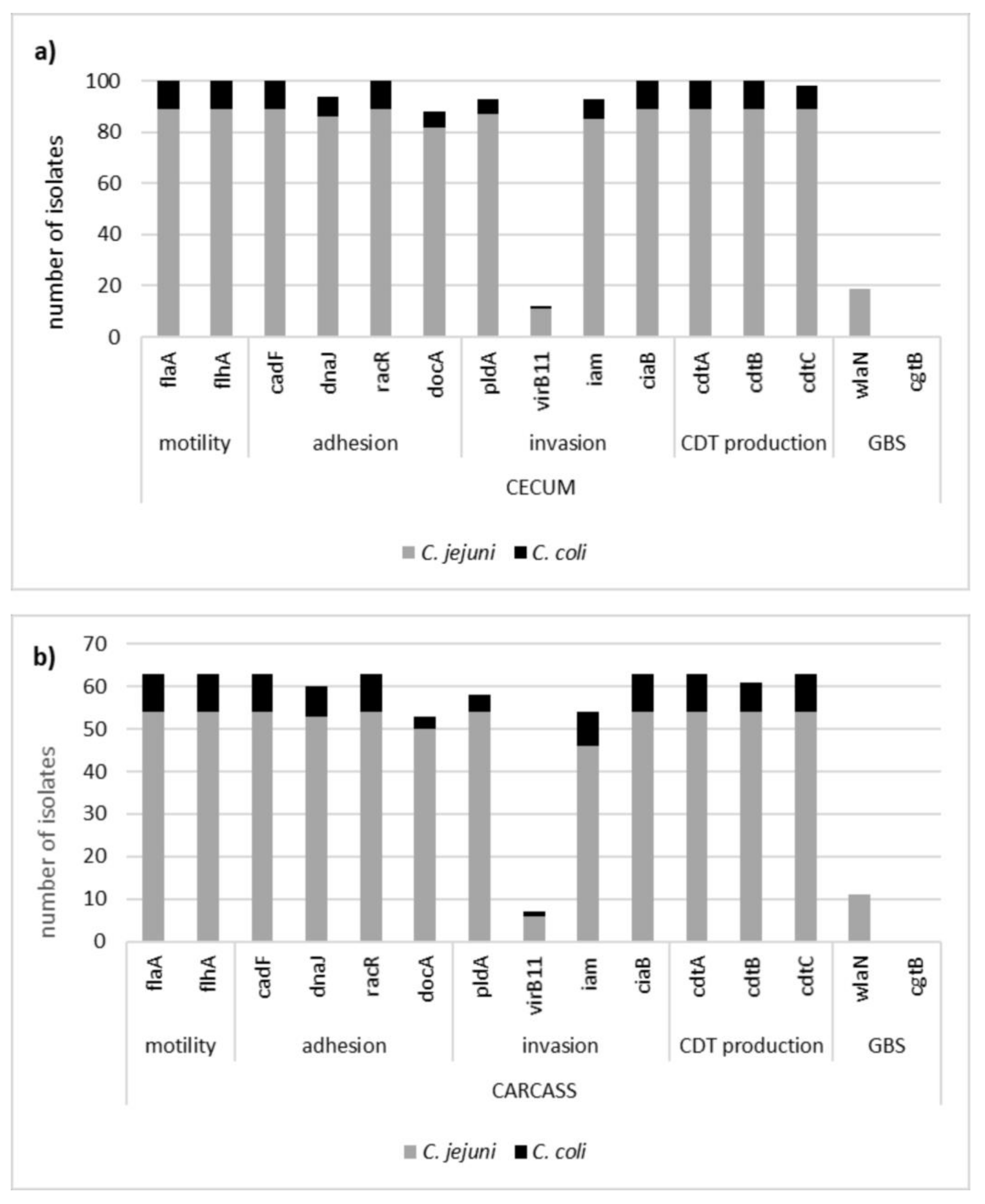
3.2. Virulence Factor Genes
3.3. Antimicrobial Resistance
4. Discussion
5. Conclusions
Author Contributions
Funding
Conflicts of Interest
References
- Gutić, S. Importance of foodborne diseases. Meso 2015, 4, 378–384. [Google Scholar]
- Roberts, J. Economic aspects of food-borne outbreaks and their control. Br. Med. 2000, 56, 133–141. [Google Scholar] [CrossRef] [PubMed][Green Version]
- Black, A.P.; Kirk, M.D.; Millard, G. Campylobacter outbreak due to chicken consumption at an Australian Capital Territory restaurant. Commun. Dis. Intell. 2006, 30, 373–377. [Google Scholar]
- Skarp, C.P.; Hanninen, M.L.; Rautelin, H.I. Campylobacteriosis: The role of poultry meat. Clin. Microbiol. Infect. 2016, 22, 103–109. [Google Scholar] [CrossRef]
- Chai, S.J.; Cole, D.; Nisler, A.; Mahon, B.E. Poultry: The most common food in outbreaks with known pathogens, United States, 1998–2012. Epidemiol. Infect. 2017, 145, 316–325. [Google Scholar] [CrossRef] [PubMed]
- Althaus, D.; Zweifel, C.; Stephan, R. Analysis of a poultry slaughter process: Influence of process stages on the microbiological contamination of broiler carcasses. Ital. J. Food Saf. 2017, 6, 7097. [Google Scholar] [CrossRef]
- Franchin, P.R.; Aidoo, K.E.; Batista, C.R.V. Sources of poultry meat contamination with thermophilic with thermophilic Campylobacter before slaughter. Brazilian, J. Microbiol. 2005, 36, 157–162. [Google Scholar] [CrossRef]
- Kaakoush, N.O.; Castano-Rodriguez, N.; Mitchell, H.M.; Man, S.M. Global epidemiology of Campylobacter infection. Clin. Microbiol. Rev. 2015, 38, 687–720. [Google Scholar] [CrossRef] [PubMed]
- Black, R.E.; Levine, M.M.; Clements, M.L.; Hughes, T.P.; Blaser, M.J. Experimental Campylobacter jejuni infection in humans. J. Infect. Dis. 1988, 157, 472–479. [Google Scholar] [CrossRef]
- Hara-Kudo, Y.; Takatori, K. Contamination level and ingestion dose of foodborne pathogens associated with infections. Epidemiol. Infect. 2011, 139, 1505–1510. [Google Scholar] [CrossRef] [PubMed]
- Man, S.M. The clinical importance of emerging Campylobacter species. Nat. Rev. Gastroenterol. Hepatol. 2011, 8, 669–685. [Google Scholar] [CrossRef] [PubMed]
- Nachamkin, I.; Allos, B.M.; Ho, T.W. Campylobacter jejuni infection and the association with Guillain-Barré syndrome. In Campylobacter, 2nd ed.; Nachamkin, I., Blaser, M.J., Eds.; ASM Press: Washington, DC, USA, 2000; pp. 155–178. [Google Scholar]
- Wieczorek, K.; Wołkowicz, T.; Osek, J. flaA-SVR Based genetic diversity of multiresistant Campylobacter jejuni isolated from chickens and humans. Front. Microbiol. 2019, 10, 1176. [Google Scholar] [CrossRef] [PubMed]
- Linton, D.; Gilbert, M.; Hitchen, P.G.; Dell, A.; Morris, H.R.; Wakarchuk, W.W.; Gregson, N.A.; Wren, B.W. Phase variation of a beta-1,3 galactosyltransferase involved in generation of the ganglioside GM1-like lipo-oligosaccharide of Campylobacter jejuni. Mol. Microbiol. 2000, 37, 501–514. [Google Scholar] [CrossRef]
- Datta, S.; Niwa, H.; Itoh, K. Prevalence of 11 pathogenic genes of Campylobacter jejuni by PCR in strains isolated from humans, poultry meat and broiler and bovine faeces. J. Med. Microbiol. 2003, 52, 345–348. [Google Scholar] [CrossRef] [PubMed]
- Casabonne, C.; Gonzalez, A.; Aquili, V.; Subils, T.; Balague, C. Prevalence of seven virulence genes of Campylobacter jejuni isolated from patients with diarrhea in Rosario, Argentina. Int. J. Infect. 2016, 3, 1–6. [Google Scholar] [CrossRef]
- Redondo, N.; Carroll, A.; McNamara, E. Molecular characterization of Campylobacter causing human clinical infection using whole-genome sequencing: Virulence, antimicrobial resistance and phylogeny in Ireland. PLoS ONE 2019, 14, e0219088. [Google Scholar] [CrossRef]
- Guirado, P.; Paytubi, S.; Miró, E.; Iglesias-Torrens, Y.; Navarro, F.; Cerdà-Cuéllar, M.; Stephan-Otto Attolini, C.; Balsalobre, C.; Madrid, C. Differential distribution of the wlaN and cgtB genes, associated with Guillain-Barré Syndrome, in Campylobacter jejuni isolates from humans, broiler chickens, and wild birds. Microorganisms 2020, 8, E325. [Google Scholar] [CrossRef]
- Luangtongkum, T.; Jeon, B.; Han, J.; Plummer, P.; Logue, C.M.; Zhang, Q. Antibiotic resistance in Campylobacter emergence, transmission and persistence. Future Microbiol. 2009, 4, 189–200. [Google Scholar] [CrossRef]
- Blaser, B.; Engberg, J. Clinical aspects of Campylobacter jejuni and Campylobacter coli infections. In Campylobacter; Nachamkin, I., Szymanski, C.M., Blaser, M.J., Eds.; American Society for Microbiology: Washington, DC, USA, 2008; pp. 99–121. [Google Scholar]
- ISO 10272-1:2017. Microbiology of the Food Chain—Horizontal Method for Detection and Enumeration of Campylobacter spp.—Part 1: Detection Method; ISO: Geneva, Switzerland, 2017. [Google Scholar]
- Wieczorek, K.; Osek, J. Multiplex PCR assays for simultaneous identification of Campylobacter jejuni and Campylobacter coli. Med. Weter. 2005, 61, 797–799. [Google Scholar]
- Müller, J.; Schulze, F.; Müller, W.; Hänel, I. PCR detection of virulence-associated genes in Campylobacter jejuni strains with differential ability to invade Caco-2 cells and to colonize the chick gut. Vet. Microbiol. 2006, 13, 123–129. [Google Scholar] [CrossRef]
- Chansiripornchai, N.; Sasipreeyajan, J. PCR detection of four virulence-associated genes of Campylobacter jejuni isolates from Thai broilers and their abilities of adhesion to and invasion of INT-407 cells. J. Vet. Med. Sci. 2009, 71, 839–844. [Google Scholar] [CrossRef] [PubMed]
- Konkel, M.E.; Kim, B.J.; Rivera-Amill, V.; Garvis, S.G. Identification of proteins required for the internalization of Campylobacter jejuni into cultured mammalian cells. Adv. Exp. Med. Biol. 1999, 473, 215–224. [Google Scholar] [PubMed]
- Carvalho, A.C.; Ruiz Palacios, G.M.; Ramos Cervantes, P.; Cervantes, L.E.; Jiang, X.; Pickering, L.K. Molecular characterization of invasive and noninvasive Campylobacter jejuni and Campylobacter coli isolates. J. Clin. Microbiol. 2001, 39, 1353–1359. [Google Scholar] [CrossRef] [PubMed]
- Wysok, B.; Wojtacka, J. Detection of virulence genes determining the ability to adhere and invade in Campylobacter spp. from cattle and swine in Poland. Microb. Pathog. 2018, 115, 257–263. [Google Scholar] [CrossRef]
- Clinical and Laboratory Standards Institute. Methods for Antimicrobial Dilution and Disk Susceptibility Testing of Infrequently Isolated or Fastidious Bacteria; CLSI: Wayne, PA, USA, 2016. [Google Scholar]
- European Food Safety Authority (EFSA). Analysis of the baseline survey on the prevalence of Campylobacter in broiler batches and of Campylobacter and Salmonella on broiler carcasses in the EU, 2008—Part A: Campylobacter and Salmonella prevalence estimates. EFSA J. 2010, 8, 1522. [Google Scholar] [CrossRef]
- Korsak, D.; Maćkiw, E.; Rożynek, E.; Żyłowska, M. Prevalence of Campylobacter species in retail chicken, turkey, pork, and beef meat in Poland between 2009 and 2013. J. Food Prot. 2015, 78, 1024–1028. [Google Scholar] [CrossRef]
- Rahimi, E.; Ameri, M.; Kazemeini, H.R. Prevalence and antimicrobial resistance of Campylobacter species isolated from raw camel, beef, lamb, and goat meat in Iran. Foodb. Pathog. Dis. 2010, 7, 443–447. [Google Scholar] [CrossRef]
- Whyte, P.; McGill, K.; Cowley, D.; Madden, R.H.; Moran, L.; Scates, P.; Carroll, C.; O’Leary, A.; Fanning, S.; Collins, J.D.; et al. Occurrence of Campylobacter in retail foods in Ireland. Int. J. Food Microbiol. 2004, 95, 111–118. [Google Scholar] [CrossRef]
- Kim, J.; Park, H.; Kim, J.; Kim, J.H.; Jung, J.I.; Cho, S.; Ryu, S.; Jeon, B. Comparative analysis of aerotolerance, antibiotic resistance, and virulence gene prevalence in Campylobacter jejuni isolates from retail raw chicken and duck meat in South Korea. Microorganisms 2019, 7, 433. [Google Scholar] [CrossRef]
- Little, C.L.; Richardson, J.F.; Owen, R.J.; De Pinna, E.; Threlfall, E.J. Prevalence, characterization and antimicrobial resistance of Campylobacter and Salmonella in raw poultry meat in the UK, 20032–005. Int. J. Environ. Health Res. 2008, 18, 403–414. [Google Scholar] [CrossRef]
- Fosse, J.; Seegers, H.; Magras, C. Prevalence and risk factors for bacterial food-borne zoonotic hazards in slaughter pigs: A review. Zoonoses Public Health 2009, 56, 429–454. [Google Scholar] [CrossRef] [PubMed]
- Horrocks, S.M.; Anderson, R.C.; Nisbet, D.J.; Ricke, S.C. Incidence and ecology of Campylobacter jejuni and coli in animals. Anaerobe 2009, 15, 18–25. [Google Scholar] [CrossRef]
- Inglis, G.D.; Boras, V.F.; Houde, A. Enteric campylobacteria and RNA viruses associated with healthy and diarrheic humans in the Chinook Heath Region of Southwestern Alberta, Canada. J. Clin. Microbiol. 2011, 49, 209–219. [Google Scholar] [CrossRef] [PubMed]
- Hiett, K.L.; Cox, N.A.; Stern, N.J. Direct polymerase chain reaction detection of Campylobacter spp. in poultry hatchery samples. Avian Dis. 2002, 46, 219–223. [Google Scholar] [CrossRef]
- Golden, N.J.; Acheson, D.W. Identification of motility and autoagglutination Campylobacter jejuni mutants by random transposon mutagenesis. Infect. Immun. 2002, 70, 1761–1771. [Google Scholar] [CrossRef]
- Nguyen, T.N.; Hotzel, H.; El-Adawy, H.; Tran, H.T.; Le, M.T.; Tomaso, H.; Neubauer, H.; Hafez, H.M. Genotyping and antibiotic resistance of thermophilic Campylobacter isolated from chicken and pig meat in Vietnam. Gut Pathog. 2016, 8, 19. [Google Scholar] [CrossRef]
- Frazao, M.R.; Medeiros, M.I.C.; Da Silva Duque, S.; Falcão, J.P. Pathogenic potential and genotypic diversity of Campylobacter jejuni: A neglected food-borne pathogen in Brazil. J. Med. Microbiol. 2017, 66, 350–359. [Google Scholar] [CrossRef]
- Bang, D.D.; Borck, B.; Nielsen, E.; Scheutz, M.F.; Pedersen, K.; Madsen, M. Detection of seven virulence and toxin genes of Campylobacter jejuni isolates from Danish turkeys by PCR and cytolethal distending toxin production of the isolates. J. Food Prot. 2004, 67, 2171–2177. [Google Scholar] [CrossRef]
- Guerry, P. Campylobacter flagella: Not just for motility. Trends Microbiol. 2007, 15, 456–461. [Google Scholar] [CrossRef]
- Scanlan, E.; Ardill, L.; Whelan, M.V.; Shortt, C.; Nally, J.E.; Bourke, B.Ó.; Cróinin, T. Relaxation of DNA supercoiling leads to increased invasion of epithelial cells and protein secretion by Campylobacter jejuni. Mol. Microbiol. 2017, 104, 92–104. [Google Scholar] [CrossRef]
- Konkel, M.E.; Christensen, J.E.; Keech, A.M.; Monteville, M.R.; Klena, J.D.; Garvis, S.G. Identification of a fibronectin binding domain within the Campylobacter jejuni CadF protein. Mol. Microbiol. 2005, 57, 1022–1035. [Google Scholar] [CrossRef] [PubMed]
- Krause-Gruszczynska, M.; Van Alphen, L.B.; Oyarzabal, O.A.; Alter, T.; Hanel, I.; Schliephake, A.; Konig, W.; Van Putten, J.P.M.; Konkel, M.E.; Backert, S. Expression patterns and role of the CadF protein in Campylobacter jejuni and Campylobacter coli. FEMS Microbiol. Lett. 2007, 274, 9–16. [Google Scholar] [CrossRef] [PubMed]
- Jin, S.; Joe, A.; Lynett, J.; Hani, E.K.; Sherman, P.; Chan, V.L. JlpA, a novel surface exposed lipoprotein specific to Campylobacter jejuni, mediates adherence to host epithelial cells. Mol. Microbiol. 2001, 39, 1225–1236. [Google Scholar] [CrossRef] [PubMed]
- Biswas, D.; Hannon, S.J.; Townsend, H.G.G.; Potter, A.; Allan, B.J. Genes coding for virulence determinants of Campylobacter jejuni in human clinical and cattle isolates from Alberta, Canada, and their potential role in colonization of poultry. Int. Microbiol. 2011, 14, 25–32. [Google Scholar]
- Wieczorek, K.; Wolkowicz, T.; Osek, J. Antimicrobial resistance and virulence-associated traits of Campylobacter jejuni isolated from poultry food chain and humans with diarrhea. Front. Microbiol. 2018, 9, 1508. [Google Scholar] [CrossRef]
- Bacon, D.J.; Alm, R.A.; Burr, D.H.; Hu, L.; Kopecko, D.J.; Ewing, C.P.; Trust, T.J.; Guerry, P. Involvement of a plasmid in virulence of Campylobacter jejuni 81–176. Infect. Immun. 2000, 68, 4384–4390. [Google Scholar] [CrossRef]
- Melo, R.T.; Nalevaiko, P.C.; Mendonca, E.P.; Borges, L.W.; Fonseca, B.B.; Beletti, M.E.; Rossi, D.A. Campylobacter jejuni strains isolated from chicken meat harbour several virulence factors and represent a potential risk to humans. Food Control. 2013, 33, 227–231. [Google Scholar] [CrossRef]
- Lara-Tejero, M.; Galán, J.E. CdtA, CdtB, and CdtC form a tripartite complex that is required for cytolethal distending toxin activity. Infect. Immun. 2001, 69, 4358–4365. [Google Scholar] [CrossRef]
- Rozynek, E.; Dzierżanowska-Fangrat, K.; Jozwiak, P.; Popowski, J.; Korsak, D.; Dzierżanowska, D. Prevalence of potential virulence markers in Polish Campylobacter jejuni and Campylobacter coli isolates obtained from hospitalized children and from chicken carcasses. J. Med. Microbiol. 2005, 54, 615–619. [Google Scholar] [CrossRef]
- Islam, Z.; Islam, M.B.; Jacobs, B.C.; Jahan, I.; Mohammad, Q.D.; Endtz, H.P. Campylobacter jejuni infection and Guillain-Barré syndrome: An emerging cause of acute flaccid paralysis after the eradication of poliomyelitis in Bangladesh. Int. J. Infect. Dis. 2016, 45, 176. [Google Scholar] [CrossRef][Green Version]
- Wegener, H. Antibitiotic Resistance—Linking Humans and Animal Health. In Improving Food Safety Through a One Health Approach: Workshop Summary; National Academies Press: Washington, DC, USA, 2012. [Google Scholar]
- Gibreel, A.; Taylor, D.E. Macrolide resistance in Campylobacter jejuni and Campylobacter coli. J. Antimicrob. Chemother. 2006, 58, 243–255. [Google Scholar] [CrossRef]
- Wieczorek, K.; Osek, J. A five-year study on prevalence and antimicrobial resistance of Campylobacter from poultry carcasses in Poland. Food Microbiol. 2015, 49, 161–165. [Google Scholar] [CrossRef]
- Andrzejewska, M.; Szczepańska, B.; Śpica, D.; Klawe, J.J. Trends in the occurrence and characteristics of Campylobacter jejuni and Campylobacter coli isolates from poultry meat in Northern Poland. Food Microbiol. 2015, 51, 190–194. [Google Scholar] [CrossRef]
- Bywater, R.; Deluyker, H.; Deroover, E.; De Jong, A.; Marion, H.; McConville, M.; Rowan, T.; Shryock, T.; Shuster, D.; Thomas, V.; et al. A European survey of antimicrobial susceptibility among zoonotic and commensal bacteria isolated from food-producing animals. J. Antimicrob. Chemother. 2004, 54, 744–754. [Google Scholar] [CrossRef] [PubMed]
- Unicomb, L.E.; Ferguson, J.; Stafford, R.J.; Ashbolt, R.; Kirk, M.D.; Becker, N.G.; Patel, M.S.; Gilbert, G.L.; Valcanis, M.; Mickan, L. Low-level fluoroquinolone resistance among Campylobacter jejuni isolates in Australia. Clin. Infect. Dis. 2006, 42, 1368–1374. [Google Scholar] [CrossRef] [PubMed]
- Obeng, A.S.; Rickard, H.; Sexton, M.; Pang, Y.; Peng, H.; Barton, M. Antimicrobial susceptibilities and resistance genes in Campylobacter strains isolated from poultry and pigs in Australia. J. Appl. Microbiol. 2012, 113, 294–307. [Google Scholar] [CrossRef] [PubMed]
- Sierra-Arguello, Y.M.; Morgan, R.B.; Perdoncini, G.; Lima, L.M.; Gomes, M.J.P.; Do Nascimento, V.P. Resistance to β-lactam and tetracycline in Campylobacter spp. isolated from broiler slaughterhouses in southern Brazil. Pesq. Vet. Bras. 2015, 35, 637–642. [Google Scholar] [CrossRef]
- Aydin, F.; Atabay, H.I.; Akan, M. The isolation and characterization of Campylobacter jejuni subsp. jejuni from domestic geese (Anser anser). J. Appl. Microbiol. 2001, 90, 637–642. [Google Scholar]
- Fallon, R.; O’Sullivan, N.; Maher, M.; Carroll, C. Antimicrobial resistance of Campylobacter jejuni and Campylobacter coli isolates from broiler chickens isolated at an Irish poultry processing plant. Lett. Appl. Microbiol. 2003, 36, 277–281. [Google Scholar] [CrossRef]
- Jamali, H.; Ghaderpour, A.; Radmehr, B.; Chuan, S.; Wei, K.; Chai, L.C.; Ismail, S. Prevalence and antimicrobial resistance of Campylobacter species isolates in ducks and geese. Food Control. 2015, 50, 328–330. [Google Scholar] [CrossRef]
- Kos, V.N.; Keelan, M.; Taylor, D.E. Antimicrobial susceptibilities of Campylobacter jejuni isolates from poultry from Alberta, Canada. Antimicrob. Agents Chemother. 2006, 50, 778–780. [Google Scholar] [CrossRef] [PubMed]
- El-Adawy, H.; Hotzel, H.; Düpre, S.; Tomaso, H.; Neubauer, H.; Hafez, H.M. Determination of antimicrobial sensitivities of Campylobacter jejuni isolated from commercial turkey farms in Germany. Avian Dis. 2012, 56, 685–692. [Google Scholar] [CrossRef] [PubMed]
- Wieczorek, K.; Bocian, Ł.; Osek, J. Prevalence and antimicrobial resistance of Campylobacter isolated from carcasses of chickens slaughtered in Poland—a retrospective study. Food Control. 2020, 12, 107159. [Google Scholar] [CrossRef]
- Karikari, A.B.; Obiri-Danso, K.; Frimpong, E.H.; Krogfelt, K.A. Multidrug resistant Campylobacter in faecal and carcasses of commercially produced poultry. Afr. J. Microbiol. Res. 2017, 11, 271–277. [Google Scholar]
| Target Gene | Sequences (5’–3’) | Product Size (bp) | Annealing Temperature °C | References |
|---|---|---|---|---|
| 16S rRNA for Campylobacter spp. | F-ATCTAATGGCTTAACCATTAAAC R-GGACGGTAACTAGTTTAGTATT | 857 | 58 | [22] |
| mapA for C. jejuni | F-CTATTTTATTTTTGAGTGCTTGTG R-GCTTTATTTGCCATTTGTTTTATTA | 589 | 58 | [22] |
| ceuE for C. coli | F-AATTGAAAATTGCTCCAACTATG R-TGATTTTATTATTTGTAGCAGCG | 462 | 58 | [22] |
| flaA | F-AATAAAAATGCTGATAAAACAGGTG R-TACCGAACCAATGTCTGCTCTGATT | 855 | 53 | [15] |
| flhA | F-GGAAGCGGCACTTGGTTTGC R-GCTGTGAGTGAGATTATAGCAG | 735 | 53 | [23] |
| dnaJ | F-ATTGATTTTGCTGCGGGTAG R-ATCCGCAAAAGCTTCAAAAA | 177 | 50 | [24] |
| cadF | F-TTGAAGGTAATTTAGATATG R-CTAATACCTAAAGTTGAAAC | 400 | 45 | [25] |
| virB11 | F-TCTTGTGAGTTGCCTTACCCCTTTT R-CCTGCGTGTCCTGTGTTATTTACCC | 494 | 53 | [15] |
| docA | F-ATAAGGTGCGGTTTTGGC R-GTCTTTGCAGTAGATATG | 725 | 50 | [23] |
| Iam | F-GCGCAAAATATTATCACCC R-TTCACGACTACTATGCGG | 518 | 52 | [26] |
| ciaB | F-TGCGAGATTTTTCGAGAATG R-TGCCCGCCTTAGAACTTACA | 527 | 54 | [24] |
| racR | F-GATGATCCTGACTTTG R-TCTCCTATTTTTACCC | 584 | 45 | [15] |
| pldA | F-AAGCTTATGCGTTTTT R-TATAAGGCTTTCTCCA | 913 | 45 | [15] |
| cdtA | F-CCTTGTGATGCAAGCAATC R-ACACTCCATTTGCTTTCTG | 370 | 49 | [15] |
| cdtB | F-CAGAAAGCAAATGGAGTGTT R-AGCTAAAAGCGGTGGAGTAT | 620 | 51 | [15] |
| cdtC | F-CGATGAGTTAAAACAAAAAGATA R-TTGGCATTATAGAAAATACAGTT | 182 | 47 | [15] |
| wlaN | F-TGCTGGGTATACAAAGGTTGTG R-ATTTTGGATATGGGTGGGG | 330 | 55 | [23] |
| cgtB | F-TAAGAGCAAGATATGAAGGTG R-GCACATAGAGAACGCTACAA | 561 | 52 | [14] |
| Flocks | Sampling | No. of Slaughtered Geese | No. of Positive Samples/No. of Tested Samples | |||
|---|---|---|---|---|---|---|
| Ceca | Carcasses | |||||
| n | % | n | % | |||
| A | X 2016 | 1470 | 5/5 | 100 | 5/5 | 100 |
| B | X 2016 | 5100 | 5/5 | 100 | 2/5 | 40.0 |
| C | X 2016 | 3500 | 5/5 | 100 | 5/5 | 100 |
| D | X 2016 | 6170 | - | - | - | - |
| E | X 2016 | 750 | 5/5 | 100 | 5/5 | 100 |
| F | XI 2016 | 1500 | 5/5 | 100 | 5/5 | 100 |
| G | XI 2016 | 2300 | 5/5 | 100 | 2/5 | 40.0 |
| H | XI 2016 | 1760 | - | - | - | - |
| I | XI 2016 | 800 | 5/5 | 100 | 5/5 | 100 |
| J | XI 2016 | 1230 | 5/5 | 100 | 2/5 | 40.0 |
| K | XII 2016 | 2100 | 5/5 | 100 | 2/5 | 40.0 |
| L | XII 2016 | 2270 | 5/5 | 100 | - | - |
| M | X 2017 | 4900 | 5/5 | 100 | 2/5 | 40.0 |
| N | X 2017 | 540 | 5/5 | 100 | 5/5 | 100 |
| O | X 2017 | 2200 | 5/5 | 100 | 2/5 | 40.0 |
| P | X 2017 | 7900 | - | - | - | - |
| Q | XI 2017 | 3080 | - | - | 1/5 | 20.0 |
| R | XI 2017 | 1890 | 5/5 | 100 | - | - |
| S | XI 2017 | 1550 | 5/5 | 100 | 5/5 | 100 |
| T | XI 2017 | 4300 | 5/5 | 100 | 2/5 | 40.0 |
| U | XI 2017 | 2250 | 5/5 | 100 | 5/5 | 100 |
| V | XII 2017 | 1800 | 5/5 | 100 | - | - |
| W | XII 2017 | 11000 | 5/5 | 100 | 2/5 | 40.0 |
| Z | XII 2017 | 2200 | 5/5 | 100 | 5/5 | 100 |
| Antimicrobials | No. of Resistant Isolates (%) | ||||||||
|---|---|---|---|---|---|---|---|---|---|
| Cecum | Carcass | Together | |||||||
| C. jejuni n = 89 | C. coli n = 11 | Total n = 100 | C. jejuni n = 54 | C. coli n = 9 | Total n = 63 | C. jejuni n = 143 | C. coli n = 20 | Total n = 163 | |
| Ciprofloxacin (CIP) | 82 (92.1) | 10 (90.9) | 92 (92.0) | 50 (92.6) | 9 (100) | 59 (93.6) | 132 (92.3) | 19 (95.0) | 151 (92.6) |
| Nalidixic acid (NAL) | 79 (88.7) | 9 (81.8) | 88 (88.0) | 49 (90.7) | 8 (88.9) | 57 (90.5) | 128 (89.5) | 17 (85.0) | 145 (88.9) |
| Gentamicin (G) | 0 (0.0) | 0 (0.0) | 0 (0.0) | 0 (0.0) | 0 (0.0) | 0 (0.0) | 0 (0.0) | 0 (0.0) | 0 (0.0) |
| Erythromycin (ERY) | 0 (0.0) | 1 (9.0) | 1 (1.0) | 0 (0.0) | 0 (0.0) | 0 (0.0) | 0 (0.0) | 1 (5.0) | 1 (0.6) |
| Tetracycline (TET) | 72 (80.9) | 9 (81.8) | 81 (81.0) | 42 (77.8) | 7 (77.8) | 49 (77.8) | 114 (79.7) | 16 (80.0) | 130 (79.8) |
| Ampicillin (AMP) | 23 (32.6) | 3 (27.3) | 32 (32.0) | 19 (35.2) | 4 (44.4) | 23 (36.5) | 48 (33.6) | 7 (35.0) | 55 (33.7) |
| Chloramphenicol (CHL) | 0 (0.0) | 0 (0.0) | 0 (0.0) | 0 (0.0) | 0 (0.0) | 0 (0.0) | 0 (0.0) | 0 (0.0) | 0 (0.0) |
| Source and Species of Isolates | Gene Pattern | No. of Isolates (%) |
|---|---|---|
| Isolates from Cecum | ||
| C. coli | CIP_NAL | 1/11 (9.1) |
| CIP_NAL_TET | 5/11 (45.5) | |
| CIP_NAL_TET_AMP * | 3/11 (2.3) | |
| CIP_NAL_ERY_TET * | 1/11 (9.1) | |
| C. jejuni | TET | 3/89 (3.4) |
| TET_AMP | 2/89 (2.2) | |
| CIP_NAL | 11/89 (12.4) | |
| CIP_AMP | 1/89 (1.1) | |
| CIP_NAL_TET | 43/89 (48.3) | |
| CIP_NAL_AMP | 3/89 (3.4) | |
| CIP_TET_AMP * | 2/89 (2.2) | |
| CIP_NAL_TET_AMP * | 22/89 (24.7) | |
| Isolates from Carcasses | ||
| C. coli | CIP_NAL | 1/9 (11.1) |
| CIP_NAL_TET | 4/9 (44.4) | |
| CIP_NAL_AMP | 1/9 (11.1) | |
| CIP_TET_AMP * | 1/9 (11.1) | |
| CIP_NAL_TET_AMP * | 2/9 (22.2) | |
| C. jejuni | CIP | 1/54 (1.8) |
| TET | 1/54 (1.8) | |
| TET_AMP | 1/54 (1.8) | |
| CIP_NAL | 7/54 (12.9) | |
| CIP_NAL_AMP | 2/54 (3.7) | |
| CIP_NAL_TET | 24/54 (44.4) | |
| CIP_NAL_TET_AMP * | 16/54 (29.6) |
© 2020 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Wysok, B.; Wojtacka, J.; Wiszniewska-Łaszczych, A.; Szteyn, J. Antimicrobial Resistance and Virulence Properties of Campylobacter Spp. Originating from Domestic Geese in Poland. Animals 2020, 10, 742. https://doi.org/10.3390/ani10040742
Wysok B, Wojtacka J, Wiszniewska-Łaszczych A, Szteyn J. Antimicrobial Resistance and Virulence Properties of Campylobacter Spp. Originating from Domestic Geese in Poland. Animals. 2020; 10(4):742. https://doi.org/10.3390/ani10040742
Chicago/Turabian StyleWysok, Beata, Joanna Wojtacka, Agnieszka Wiszniewska-Łaszczych, and Joanna Szteyn. 2020. "Antimicrobial Resistance and Virulence Properties of Campylobacter Spp. Originating from Domestic Geese in Poland" Animals 10, no. 4: 742. https://doi.org/10.3390/ani10040742
APA StyleWysok, B., Wojtacka, J., Wiszniewska-Łaszczych, A., & Szteyn, J. (2020). Antimicrobial Resistance and Virulence Properties of Campylobacter Spp. Originating from Domestic Geese in Poland. Animals, 10(4), 742. https://doi.org/10.3390/ani10040742





