Thiosemicarbazone Copper Chelator BLT-1 Blocks Apicomplexan Parasite Replication by Selective Inhibition of Scavenger Receptor B Type 1 (SR-BI)
Abstract
1. Introduction
2. Materials and Methods
2.1. Host Cell Culture
2.2. Parasites
2.3. BLT-1 Treatments of Host Cells and Parasite Infections
2.4. Live Cell 3D Holotomographic Microscopy and Lipid Droplet (LD) Visualization
2.5. Ca++ Flux Measurements
2.6. Flow Cytometric Analysis (FACS) of Neutral Lipids in BUVEC
2.7. RT-qPCR for Relative Quantification of SR-BI Gene Transcripts
2.8. Cell Viability Assessment
2.9. Statistical Analysis
3. Results
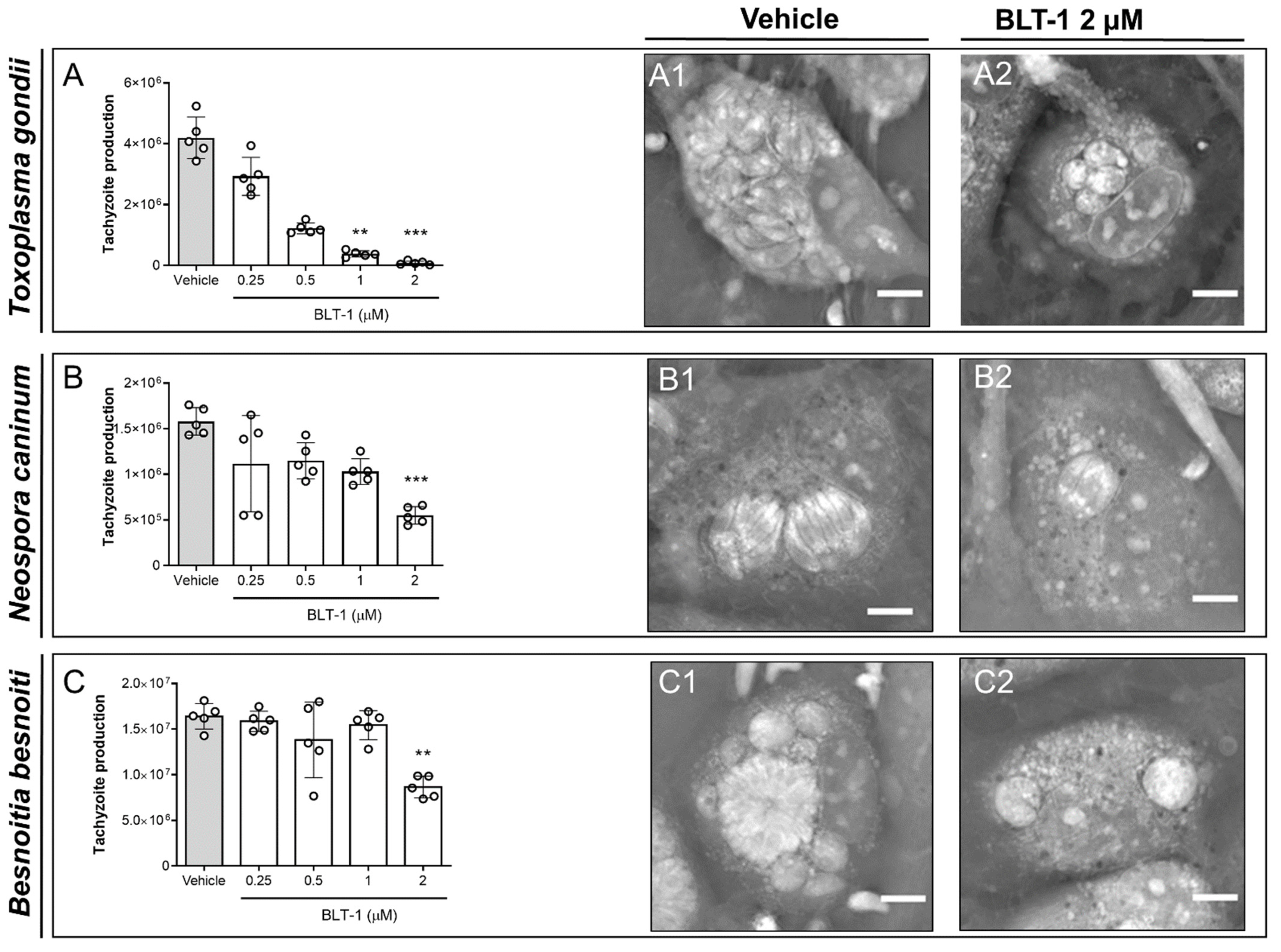
3.1. BLT-1 Treatments Induce Dose-Dependent Blockage of Tachyzoite Replication
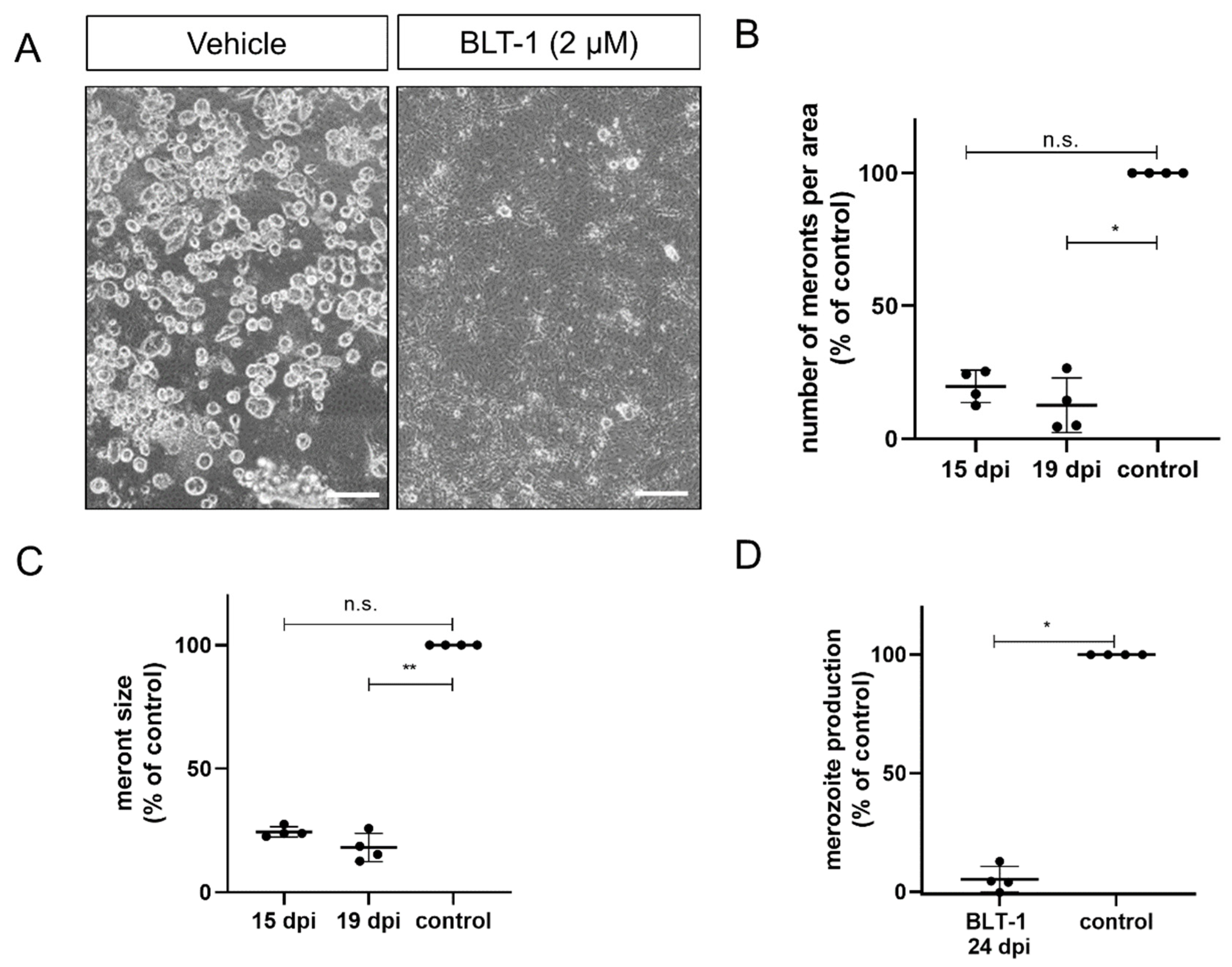
3.2. BLT-1 Treatments Interfere with E. bovis and E. arloingi Macromeront Formation and Block Merozoite I Production
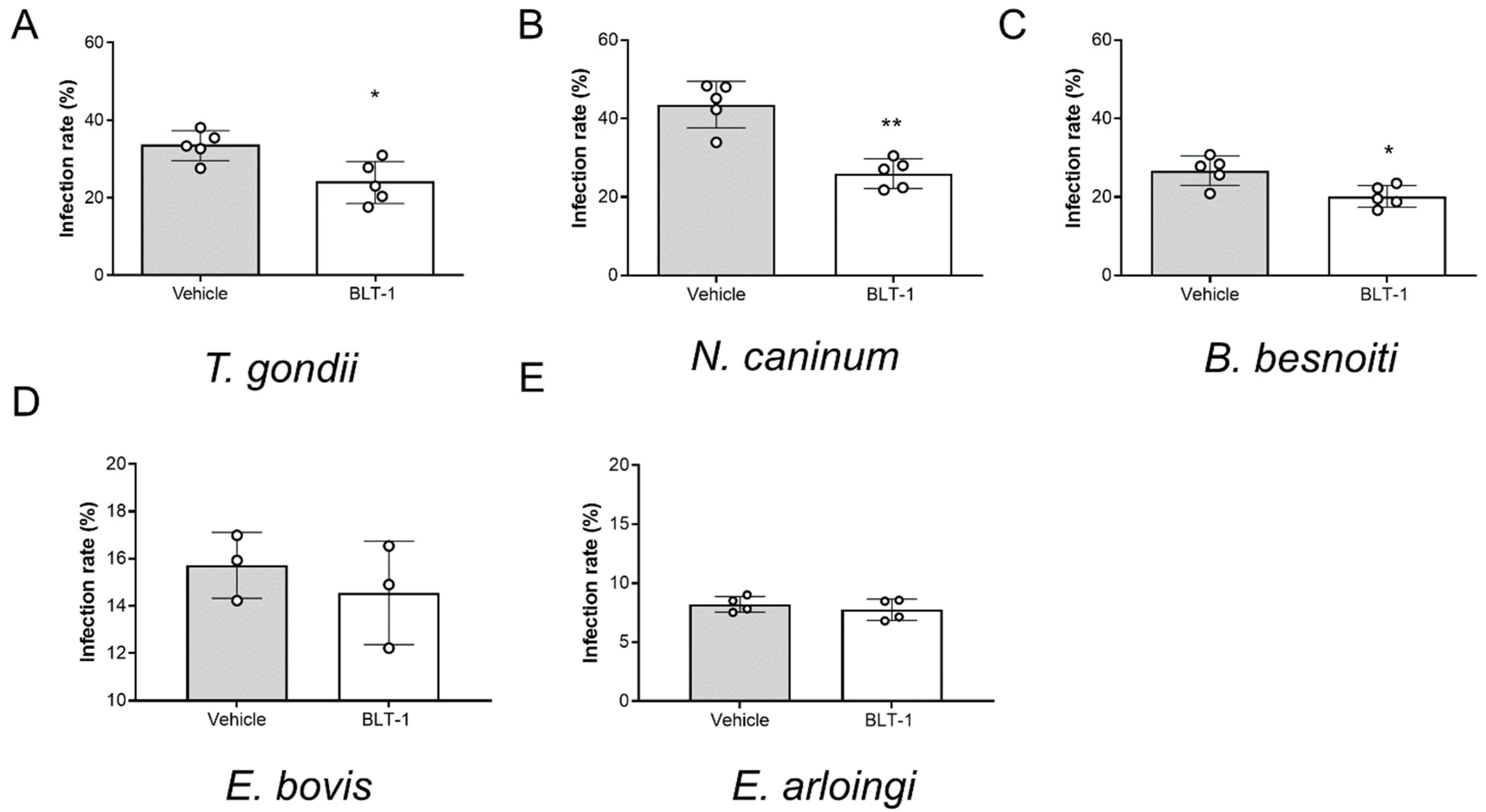
3.3. BLT-1 Treatment Impairs Infectivity of Fast Replicating Tachyzoites but Has No Effect on Slow Replicating Sporozoites
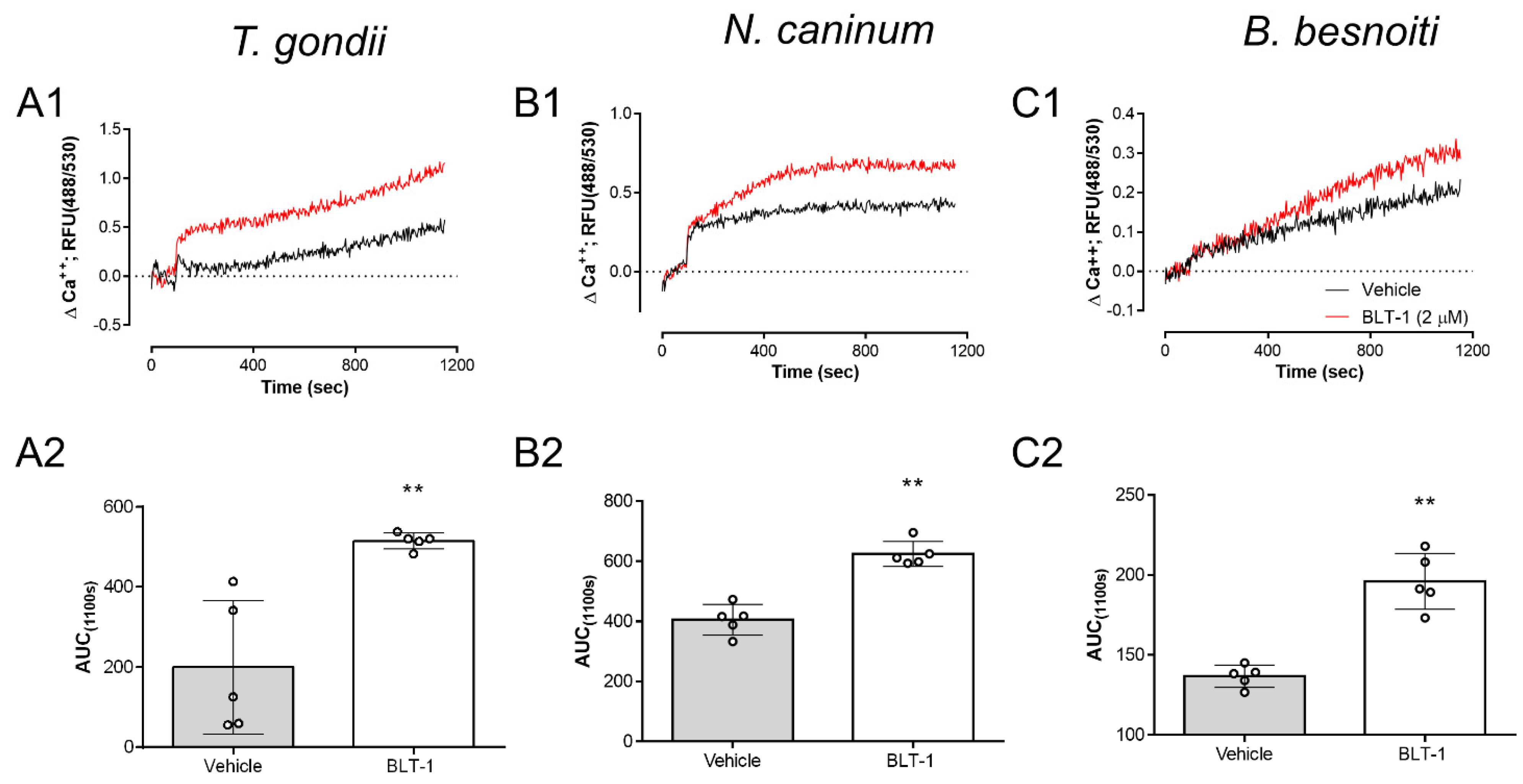
3.4. BLT-1 Treatments Trigger Ca++ Fluxes in Free Tachyzoites
3.5. BLT-1 Treatments Alter Neutral Lipid Contents and Cholesterol Distribution in BUVEC
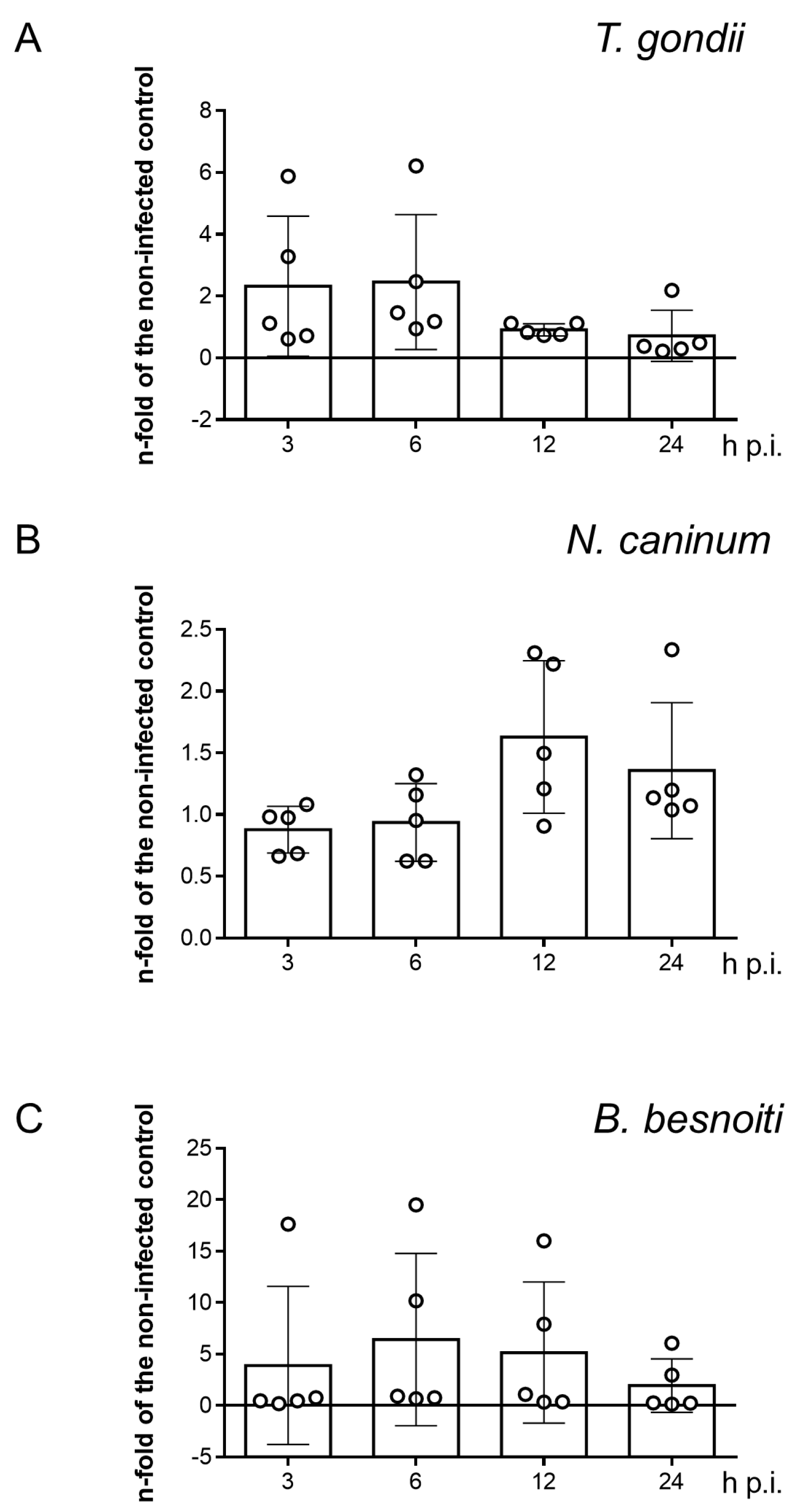
3.6. SR-BI Gene Transcription Is Not Affected by T. gondii, N. caninum and B. besnoiti Tachyzoite Infections
4. Discussion
Supplementary Materials
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Acknowledgments
Conflicts of Interest
References
- Votýpka, J.; Modrý, D.; Oborník, M.; Šlapeta, J.; Lukeš, J. Apicomplexa. In Handbook of the Protists; Archibald, J.M., Simpson, A.G.B., Slamovits, C.H., Eds.; Springer International Publishing: Cham, Switzerland, 2017; pp. 567–624. ISBN 978-3-319-28149-0. [Google Scholar]
- Benavides, J.; Fernández, M.; Castaño, P.; Ferreras, M.C.; Ortega-Mora, L.; Pérez, V. Ovine Toxoplasmosis: A New Look at Its Pathogenesis. J. Comp. Pathol. 2017, 157, 34–38. [Google Scholar] [CrossRef] [PubMed]
- Innes, E.A. A Brief History and Overview of Toxoplasma gondii. Zoonoses Public Health 2010, 57, 1–7. [Google Scholar] [CrossRef] [PubMed]
- Dubey, J.P. Review of Neospora caninum and Neosporosis in Animals. Korean J. Parasitol. 2003, 41, 1–16. [Google Scholar] [CrossRef] [PubMed]
- Reichel, M.P.; Alejandra Ayanegui-Alcérreca, M.; Gondim, L.F.P.; Ellis, J.T. What Is the Global Economic Impact of Neospora caninum in Cattle—The Billion Dollar Question. Int. J. Parasitol. 2013, 43, 133–142. [Google Scholar] [CrossRef] [PubMed]
- Alvarez-García, G.; García-Lunar, P.; Gutiérrez-Expósito, D.; Shkap, V.; Ortega-Mora, L.M. Dynamics of Besnoitia besnoiti Infection in Cattle. Parasitology 2014, 141, 1419–1435. [Google Scholar] [CrossRef]
- Cortes, H.; Leitão, A.; Gottstein, B.; Hemphill, A. A Review on Bovine Besnoitiosis: A Disease with Economic Impact in Herd Health Management, Caused by Besnoitia besnoiti (Franco and Borges, 1916). Parasitology 2014, 141, 1406–1417. [Google Scholar] [CrossRef]
- Daugschies, A.; Najdrowski, M. Eimeriosis in Cattle: Current Understanding. J. Vet. Med. B Infect. Dis. Vet. Public Health 2005, 52, 417–427. [Google Scholar] [CrossRef]
- Black, M.W.; Boothroyd, J.C. Lytic Cycle of Toxoplasma gondii. Microbiol. Mol. Biol. Rev. 2000, 64, 607–623. [Google Scholar] [CrossRef]
- Lindsay, D.S.; Dubey, J.P. Neosporosis, Toxoplasmosis, and Sarcocystosis in Ruminants: An Update. Vet. Clin. N. Am. Food Anim. Pract. 2020, 36, 205–222. [Google Scholar] [CrossRef]
- Pellérdy, L.P. Coccidia and Coccidiosis, 2nd ed.; Parey: Berlin/Hamburg, Germany, 1974; ISBN 978-3-489-73317-1. [Google Scholar]
- López-Osorio, S.; Silva, L.M.R.; Taubert, A.; Chaparro-Gutiérrez, J.J.; Hermosilla, C.R. Concomitant In Vitro Development of Eimeria zuernii- and Eimeria bovis-Macromeronts in Primary Host Endothelial Cells. Parasitol. Int. 2018, 67, 742–750. [Google Scholar] [CrossRef]
- Silva, L.M.R.; Vila-Viçosa, M.J.M.; Cortes, H.C.E.; Taubert, A.; Hermosilla, C. Suitable In Vitro Eimeria arloingi Macromeront Formation in Host Endothelial Cells and Modulation of Adhesion Molecule, Cytokine and Chemokine Gene Transcription. Parasitol. Res. 2015, 114, 113–124. [Google Scholar] [CrossRef]
- Hamid, P.H.; Hirzmann, J.; Kerner, K.; Gimpl, G.; Lochnit, G.; Hermosilla, C.R.; Taubert, A. Eimeria bovis Infection Modulates Endothelial Host Cell Cholesterol Metabolism for Successful Replication. Vet. Res. 2015, 46, 100. [Google Scholar] [CrossRef]
- Larrazabal, C.; Silva, L.M.R.; Pervizaj-Oruqaj, L.; Herold, S.; Hermosilla, C.; Taubert, A. P-Glycoprotein Inhibitors Differently Affect Toxoplasma gondii, Neospora caninum and Besnoitia besnoiti Proliferation in Bovine Primary Endothelial Cells. Pathogens 2021, 10, 395. [Google Scholar] [CrossRef]
- Larrazabal, C.; Silva, L.M.R.; Hermosilla, C.; Taubert, A. Ezetimibe Blocks Toxoplasma gondii-, Neospora caninum- and Besnoitia besnoiti-Tachyzoite Infectivity and Replication in Primary Bovine Endothelial Host Cells. Parasitology 2021, 148, 1107–1115. [Google Scholar] [CrossRef] [PubMed]
- Coppens, I. Targeting Lipid Biosynthesis and Salvage in Apicomplexan Parasites for Improved Chemotherapies. Nat. Rev. Microbiol. 2013, 11, 823–835. [Google Scholar] [CrossRef] [PubMed]
- Ikonen, E. Cellular Cholesterol Trafficking and Compartmentalization. Nat. Rev. Mol. Cell. Biol. 2008, 9, 125–138. [Google Scholar] [CrossRef] [PubMed]
- Luo, J.; Yang, H.; Song, B.-L. Mechanisms and Regulation of Cholesterol Homeostasis. Nat. Rev. Mol. Cell. Biol. 2020, 21, 225–245. [Google Scholar] [CrossRef]
- Coppens, I.; Sinai, A.P.; Joiner, K.A. Toxoplasma gondii Exploits Host Low-Density Lipoprotein Receptor-Mediated Endocytosis for Cholesterol Acquisition. J. Cell Biol. 2000, 149, 167–180. [Google Scholar] [CrossRef]
- Nolan, S.J.; Romano, J.D.; Luechtefeld, T.; Coppens, I. Neospora caninum Recruits Host Cell Structures to Its Parasitophorous Vacuole and Salvages Lipids from Organelles. Eukaryot. Cell 2015, 14, 454–473. [Google Scholar] [CrossRef]
- Silva, L.M.R.; Lütjohann, D.; Hamid, P.; Velasquez, Z.D.; Kerner, K.; Larrazabal, C.; Failing, K.; Hermosilla, C.; Taubert, A. Besnoitia besnoiti Infection Alters Both Endogenous Cholesterol de Novo Synthesis and Exogenous LDL Uptake in Host Endothelial Cells. Sci. Rep. 2019, 9, 6650. [Google Scholar] [CrossRef]
- Meng, Y.; Heybrock, S.; Neculai, D.; Saftig, P. Cholesterol Handling in Lysosomes and Beyond. Trends Cell Biol. 2020, 30, 452–466. [Google Scholar] [CrossRef] [PubMed]
- Simons, K.; Ikonen, E. How Cells Handle Cholesterol. Science 2000, 290, 1721–1726. [Google Scholar] [CrossRef] [PubMed]
- Nolan, S.J.; Romano, J.D.; Coppens, I. Host Lipid Droplets: An Important Source of Lipids Salvaged by the Intracellular Parasite Toxoplasma gondii. PLoS Pathog. 2017, 13, e1006362. [Google Scholar] [CrossRef]
- Dean, M.; Rzhetsky, A.; Allikmets, R. The Human ATP-Binding Cassette (ABC) Transporter Superfamily. Genome Res. 2001, 11, 1156–1166. [Google Scholar] [CrossRef] [PubMed]
- Adachi, H.; Tsujimoto, M. Endothelial Scavenger Receptors. Prog. Lipid Res. 2006, 45, 379–404. [Google Scholar] [CrossRef] [PubMed]
- Hoekstra, M.; Van Berkel, T.-J.; Van Eck, M. Scavenger Receptor BI: A Multi-Purpose Player in Cholesterol and Steroid Metabolism. World J. Gastroenterol. 2010, 16, 5916–5924. [Google Scholar] [CrossRef]
- Van Eck, M.; Twisk, J.; Hoekstra, M.; Van Rij, B.T.; Van der Lans, C.A.C.; Bos, I.S.T.; Kruijt, J.K.; Kuipers, F.; Van Berkel, T.J.C. Differential Effects of Scavenger Receptor BI Deficiency on Lipid Metabolism in Cells of the Arterial Wall and in the Liver. J. Biol. Chem. 2003, 278, 23699–23705. [Google Scholar] [CrossRef]
- Linton, M.F.; Tao, H.; Linton, E.F.; Yancey, P.G. SR-BI: A Multifunctional Receptor in Cholesterol Homeostasis and Atherosclerosis. Trends Endocrinol. Metab. 2017, 28, 461–472. [Google Scholar] [CrossRef]
- Vishnyakova, T.G.; Bocharov, A.V.; Baranova, I.N.; Kurlander, R.; Drake, S.K.; Chen, Z.; Amar, M.; Sviridov, D.; Vaisman, B.; Poliakov, E.; et al. SR-BI Mediates Neutral Lipid Sorting from LDL to Lipid Droplets and Facilitates Their Formation. PLoS ONE 2020, 15, e0240659. [Google Scholar] [CrossRef]
- Gutierrez-Pajares, J.L.; Ben Hassen, C.; Chevalier, S.; Frank, P.G. SR-BI: Linking Cholesterol and Lipoprotein Metabolism with Breast and Prostate Cancer. Front. Pharmacol. 2016, 7, 338. [Google Scholar] [CrossRef]
- Rodrigues, C.D.; Hannus, M.; Prudêncio, M.; Martin, C.; Gonçalves, L.A.; Portugal, S.; Epiphanio, S.; Akinc, A.; Hadwiger, P.; Jahn-Hofmann, K.; et al. Host Scavenger Receptor SR-BI Plays a Dual Role in the Establishment of Malaria Parasite Liver Infection. Cell Host Microbe 2008, 4, 271–282. [Google Scholar] [CrossRef]
- Yalaoui, S.; Huby, T.; Franetich, J.-F.; Gego, A.; Rametti, A.; Moreau, M.; Collet, X.; Siau, A.; van Gemert, G.-J.; Sauerwein, R.W.; et al. Scavenger Receptor BI Boosts Hepatocyte Permissiveness to Plasmodium Infection. Cell Host Microbe 2008, 4, 283–292. [Google Scholar] [CrossRef]
- Taubert, A.; Zahner, H.; Hermosilla, C. Dynamics of Transcription of Immunomodulatory Genes in Endothelial Cells Infected with Different Coccidian Parasites. Vet. Parasitol. 2006, 142, 214–222. [Google Scholar] [CrossRef] [PubMed]
- Maksimov, P.; Hermosilla, C.; Kleinertz, S.; Hirzmann, J.; Taubert, A. Besnoitia besnoiti Infections Activate Primary Bovine Endothelial Cells and Promote PMN Adhesion and NET Formation under Physiological Flow Condition. Parasitol. Res. 2016, 115, 1991–2001. [Google Scholar] [CrossRef] [PubMed]
- López-Osorio, S.; Silva, L.M.R.; Chaparro-Gutierréz, J.J.; Velásquez, Z.D.; Taubert, A.; Hermosilla, C. Optimized Excystation Protocol for Ruminant Eimeria bovis- and Eimeria arloingi-Sporulated Oocysts and First 3D Holotomographic Microscopy Analysis of Differing Sporozoite Egress. Parasitol. Int. 2020, 76, 102068. [Google Scholar] [CrossRef] [PubMed]
- Taubert, A.; Silva, L.M.R.; Velásquez, Z.D.; Larrazabal, C.; Lütjohann, D.; Hermosilla, C. Modulation of Cholesterol-Related Sterols during Eimeria bovis Macromeront Formation and Impact of Selected Oxysterols on Parasite Development. Mol. Biochem. Parasitol. 2018, 223, 1–12. [Google Scholar] [CrossRef]
- Astanina, K.; Koch, M.; Jüngst, C.; Zumbusch, A.; Kiemer, A.K. Lipid Droplets as a Novel Cargo of Tunnelling Nanotubes in Endothelial Cells. Sci. Rep. 2015, 5, 11453. [Google Scholar] [CrossRef]
- Cervantes-Valencia, M.E.; Hermosilla, C.; Alcalá-Canto, Y.; Tapia, G.; Taubert, A.; Silva, L.M.R. Antiparasitic Efficacy of Curcumin Against Besnoitia besnoiti Tachyzoites In Vitro. Front. Vet. Sci. 2018, 5, 333. [Google Scholar] [CrossRef]
- Horcajo, P.; Xia, D.; Randle, N.; Collantes-Fernández, E.; Wastling, J.; Ortega-Mora, L.M.; Regidor-Cerrillo, J. Integrative Transcriptome and Proteome Analyses Define Marked Differences between Neospora caninum Isolates throughout the Tachyzoite Lytic Cycle. J. Proteom. 2018, 180, 108–119. [Google Scholar] [CrossRef]
- Jiménez-Meléndez, A.; Ramakrishnan, C.; Hehl, A.B.; Russo, G.; Álvarez-García, G. RNA-Seq Analyses Reveal That Endothelial Activation and Fibrosis Are Induced Early and Progressively by Besnoitia besnoiti Host Cell Invasion and Proliferation. Front. Cell. Infect. Microbiol. 2020, 10, 218. [Google Scholar] [CrossRef]
- Taubert, A.; Wimmers, K.; Ponsuksili, S.; Jimenez, C.A.; Zahner, H.; Hermosilla, C. Microarray-Based Transcriptional Profiling of Eimeria bovis-Infected Bovine Endothelial Host Cells. Vet. Res. 2010, 41, 70. [Google Scholar] [CrossRef]
- Ehrenman, K.; Wanyiri, J.W.; Bhat, N.; Ward, H.D.; Coppens, I. Cryptosporidium parvum Scavenges LDL-Derived Cholesterol and Micellar Cholesterol Internalized into Enterocytes. Cell. Microbiol. 2013, 15, 1182–1197. [Google Scholar] [CrossRef] [PubMed]
- Dockendorff, C.; Faloon, P.W.; Germain, A.; Yu, M.; Youngsaye, W.; Nag, P.P.; Bennion, M.; Penman, M.; Nieland, T.J.F.; Dandapani, S.; et al. Discovery of Bisamide-Heterocycles as Inhibitors of Scavenger Receptor BI (SR-BI)-Mediated Lipid Uptake. Bioorg. Med. Chem. Lett. 2015, 25, 2594–2598. [Google Scholar] [CrossRef] [PubMed][Green Version]
- Yu, M.; Romer, K.A.; Nieland, T.J.F.; Xu, S.; Saenz-Vash, V.; Penman, M.; Yesilaltay, A.; Carr, S.A.; Krieger, M. Exoplasmic Cysteine Cys384 of the HDL Receptor SR-BI Is Critical for Its Sensitivity to a Small-Molecule Inhibitor and Normal Lipid Transport Activity. Proc. Natl. Acad. Sci. USA 2011, 108, 12243–12248. [Google Scholar] [CrossRef] [PubMed]
- Francia, M.E.; Striepen, B. Cell Division in Apicomplexan Parasites. Nat. Rev. Microbiol. 2014, 12, 125–136. [Google Scholar] [CrossRef]
- Hermosilla, C.; Barbisch, B.; Heise, A.; Kowalik, S.; Zahner, H. Development of Eimeria bovis In Vitro: Suitability of Several Bovine, Human and Porcine Endothelial Cell Lines, Bovine Fetal Gastrointestinal, Madin-Darby Bovine Kidney (MDBK) and African Green Monkey Kidney (VERO) Cells. Parasitol. Res. 2002, 88, 301–307. [Google Scholar] [CrossRef] [PubMed]
- Hamid, P.H.; Hirzmann, J.; Hermosilla, C.; Taubert, A. Differential Inhibition of Host Cell Cholesterol de Novo Biosynthesis and Processing Abrogates Eimeria bovis Intracellular Development. Parasitol. Res. 2014, 113, 4165–4176. [Google Scholar] [CrossRef] [PubMed]
- Lourido, S.; Moreno, S.N.J. The Calcium Signaling Toolkit of the Apicomplexan Parasites Toxoplasma gondii and Plasmodium spp. Cell Calcium 2015, 57, 186–193. [Google Scholar] [CrossRef]
- Raldúa, D.; Babin, P.J. BLT-1, a Specific Inhibitor of the HDL Receptor SR-BI, Induces a Copper-Dependent Phenotype during Zebrafish Development. Toxicol. Lett. 2007, 175, 1–7. [Google Scholar] [CrossRef]
- Pagler, T.A.; Rhode, S.; Neuhofer, A.; Laggner, H.; Strobl, W.; Hinterndorfer, C.; Volf, I.; Pavelka, M.; Eckhardt, E.R.M.; van der Westhuyzen, D.R.; et al. SR-BI-Mediated High Density Lipoprotein (HDL) Endocytosis Leads to HDL Resecretion Facilitating Cholesterol Efflux. J. Biol. Chem. 2006, 281, 11193–11204. [Google Scholar] [CrossRef]
- Fukata, Y.; Yu, X.; Imachi, H.; Nishiuchi, T.; Lyu, J.; Seo, K.; Takeuchi, A.; Iwama, H.; Masugata, H.; Hoshikawa, H.; et al. 17β-Estradiol Regulates Scavenger Receptor Class BI Gene Expression via Protein Kinase C in Vascular Endothelial Cells. Endocrine 2014, 46, 644–650. [Google Scholar] [CrossRef] [PubMed]
- Norata, G.D.; Ongari, M.; Uboldi, P.; Pellegatta, F.; Catapano, A.L. Liver X Receptor and Retinoic X Receptor Agonists Modulate the Expression of Genes Involved in Lipid Metabolism in Human Endothelial Cells. Int. J. Mol. Med. 2005, 16, 717–722. [Google Scholar] [PubMed]


Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2021 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Larrazabal, C.; López-Osorio, S.; Velásquez, Z.D.; Hermosilla, C.; Taubert, A.; Silva, L.M.R. Thiosemicarbazone Copper Chelator BLT-1 Blocks Apicomplexan Parasite Replication by Selective Inhibition of Scavenger Receptor B Type 1 (SR-BI). Microorganisms 2021, 9, 2372. https://doi.org/10.3390/microorganisms9112372
Larrazabal C, López-Osorio S, Velásquez ZD, Hermosilla C, Taubert A, Silva LMR. Thiosemicarbazone Copper Chelator BLT-1 Blocks Apicomplexan Parasite Replication by Selective Inhibition of Scavenger Receptor B Type 1 (SR-BI). Microorganisms. 2021; 9(11):2372. https://doi.org/10.3390/microorganisms9112372
Chicago/Turabian StyleLarrazabal, Camilo, Sara López-Osorio, Zahady D. Velásquez, Carlos Hermosilla, Anja Taubert, and Liliana M. R. Silva. 2021. "Thiosemicarbazone Copper Chelator BLT-1 Blocks Apicomplexan Parasite Replication by Selective Inhibition of Scavenger Receptor B Type 1 (SR-BI)" Microorganisms 9, no. 11: 2372. https://doi.org/10.3390/microorganisms9112372
APA StyleLarrazabal, C., López-Osorio, S., Velásquez, Z. D., Hermosilla, C., Taubert, A., & Silva, L. M. R. (2021). Thiosemicarbazone Copper Chelator BLT-1 Blocks Apicomplexan Parasite Replication by Selective Inhibition of Scavenger Receptor B Type 1 (SR-BI). Microorganisms, 9(11), 2372. https://doi.org/10.3390/microorganisms9112372






