Towards Advances in Medicinal Plant Antimicrobial Activity: A Review Study on Challenges and Future Perspectives
Abstract
1. Introduction
2. Antimicrobial Activity of Medicinal Plant Extracts
3. Mechanisms of Action of Antimicrobial Agents
3.1. Bacterial Protein Biosynthesis
3.2. Inhibition of Nucleic Acid Synthesis
3.3. Cell-Wall Biosynthesis
3.4. Destruction of Bacterial Cell Wall
4. Mechanisms of Resistance to Antimicrobial Agents
4.1. Efflux Pump
4.2. Structural Modification of Porins
4.3. Enzymatic Inactivation
4.4. Destruction of Antibacterial Agent
4.5. Alteration of Target Sites
5. Antimicrobial Activity Mechanisms of Medicinal Plant-Derived Chemical Compounds
5.1. Alkaloids
5.2. Phenolic Compounds/Polyphenols
5.3. Sulfur-Containing Compounds
5.4. Coumarins
5.5. Terpenes
6. Interaction between Medicinal Plant Extracts and Conventional Antibiotics
7. Challenges Surrounding Medicinal Plant Antimicrobial Activity
7.1. Use of Antimicrobials from Medicinal Plant Extracts
- The use of medicinal plants has been associated with the adulteration of valuable compounds, poor cultivation and collection procedures, lack of standardization during preparation, poor storage conditions, ultimately affecting the process of development of new antimicrobials [191]. Factors such as the season of harvest, region of cultivation, plant parts used, and type of processing can affect the levels and mechanisms of various compounds in extracts. Therefore, the comparison of the different literature data for the plant extracts antimicrobial activity may be problematic due to the composition of plant extracts varying according to local climate and environmental conditions [82]. In particular, rainfall and humidity are versatile in different geographical locations, which could change the composition and production of the compounds when the same species medicinal plant is growing in different geographical locations. Moreover, global changing of climate is another challenge modulating the weather condition and therefore jeopardizing the compounds composition and production, even in the same geographical locations.
- It is difficult for scientists to map all the complex interactions that might be taken place between all the various compounds found in a medicinal plant. The detailed knowledge of the plant extracts composition is another inherent difficulty since these extracts contain many components and hence are difficult to interpret. The isolation of single compounds with the desired antimicrobial activity can be time- consuming and possibly requires a large amount of plant material. Rediscovery of the same compounds from different sources also presents problems. Thus, standardization, stability, and quality control are feasible, but not easy. However, the prospect to study a high quantity of unexplored compounds may contribute to the renovated attention on medicinal plants [192].
- Synergism among compounds in a complex mixture presents unique difficulties as the technology to study multiple compounds acting on potentially multiple biological targets has not yet been fully developed.
- Making arrangements for access to medicinal plant species can sometimes be difficult, especially in an international setting. Regulations concerning plant collation and plant export/import differ depending on where the research is being conducted [193].
7.2. Innovative Methods for the Preparation of Medicinal Plant Extracts Chemical Compounds
7.3. Determination of Antimicrobial Efficacy of Medicinal Plant Extracts
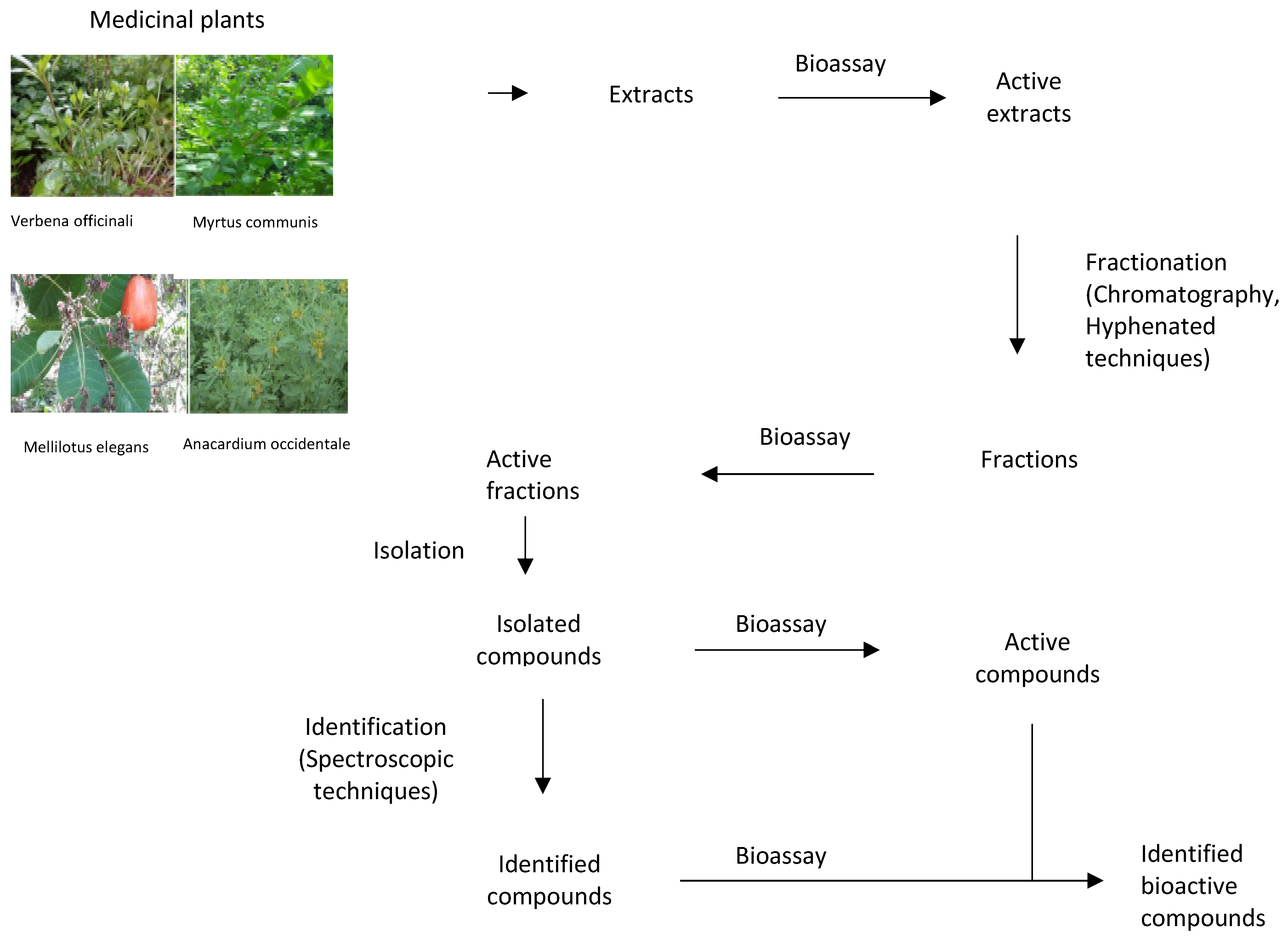
7.4. The Challenges of Development New Antimicrobials from Medicinal Plant Extracts
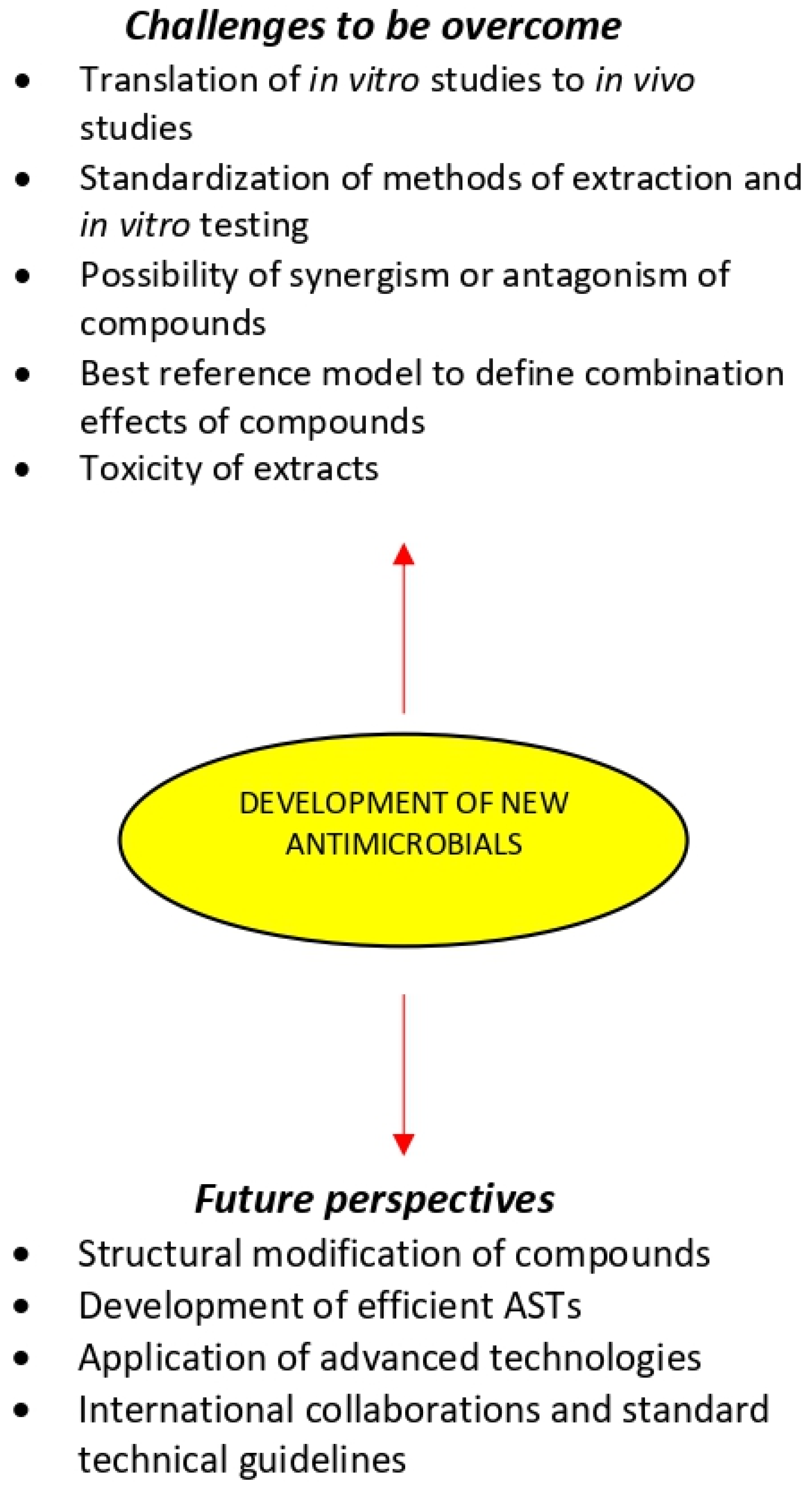
- The translation of in vitro studies to in vivo experiments and finally to human clinical trials has been the major challenge in the development of new antimicrobials. In vivo research should be carried out for a better understanding of the exact mechanisms of the medicinal plant chemical compounds and whether they can be considered an alternative or supplement to the existing strategies for the treatments of microbial diseases.
- Only medicinal plant extracts that inhibit the growth of microorganisms in low or moderated MIC values should deserve the utmost attention and additional research may be done [24].
- Extracts should also be tested for their MBC, because the bactericidal potential hinders the possibility of antimicrobial resistance.
- The utilization of unique traditional knowledge of medicinal plants medicine has great potential to generate biocompatible solutions and will hasten the discovery of new antimicrobials. This knowledge is important to design efficient and environmentally friendly technologies of fractionation and contribute to the effective exploitation of bioactive plant extracts.
- The method of extraction and in vitro testing should be standardized so that the search for new antimicrobial drugs from medicinal plants could be more systematic, and it will facilitate proper interpretation of results [34].
- Despite the increasing number of compounds isolated from antimicrobial medicinal plants, there are still only relatively few plant-derived drugs in clinical use. This may be because plant compounds often require complex combination effects between components to synergize the activity of the bioactive compound. A number of studies have shown that the overall activity of plant extracts can result from mixtures of compounds with synergistic, additive, and antagonistic activity [33,222,223,224,225]. Therefore, a major concern in the development of antimicrobials from medicinal plants is related to the possibility of synergism or antagonism effects due to the complexity in extracts composition [80,226]. Synergism within and between plant extracts have been extensively reviewed, providing compelling evidence that at least in some cases, the combined effect of plant mixtures is not simply the summation of their individual compounds [33,220,224,227,228,229]. However, it is likely that such combinations could produce antagonism, leading to the cancelation of the therapeutic effect [189]. The classification of combination effects within complex mixtures and the identification of contributing compounds remains a challenging task, particularly when most established tools have been designed to reduce complexity and identify single active compounds of natural products mixtures. Therefore, the use of bioassay-guided or synergy-guided fractionation to predict which compounds/mixtures are responsible for a specific activity is of extreme importance [225].
- Recent developments in metabolomics may play a key role in the identification and effective application of new occurring natural antimicrobials. Statistical modeling used to predict and correlate the metabolomic profile of extracts and their bioactivity has gained much attention [227]. However, there is a lack of consensus in the field about which reference models are best for defining combination effects, making the interpretation of studies challenging. Recent models using the specific mean equation [230] and the zero-interaction potency model [231] represent newly developed and robust reference models that may permit improved identification combination effects. There are also several emerging technologies, such as nanotechnology and bio-adhesive technology and materials, namely hydrogel formulations and active packaging materials which can enhance the effectiveness of plant antimicrobial compounds.
- The development of antimicrobials for oral therapy requires the application of methodologies that consider the effect of digestion on the bioactivity of the extracts [232]. However, even using sophisticated in vitro digestion models, it is still impossible to fully mimic the overall digestive parameters in vivo.
- Studies concerning the toxicity of the most promising medicinal plant extracts are major challenge for their use as antimicrobials [233,234]. Most extracts have not been evaluated by the U.S. Food and Drug Administration [235]. Therefore, the lack of official information regarding the actual toxicity of many extracts is concerning, since the adverse effects caused by the misuse of medicinal plants are characterized as a public health problem [236]. Reasons for plant extracts toxicity are improper identification/authentication and improper labeling on standardization. Thus, the extracts should be regulated through official controls and rigorous manufacturing standards.
- Another challenge in the development of antimicrobials from the medicinal plants is related to poor financial support for research and therefore lack of high- quality studies on the comprehension of structure-activity relationship with individual compounds [76].
7.5. Enhancement of the Antimicrobial Activity of Medicinal Plant Extracts
7.6. A Potential ‘ESCAPE’ from Antimicrobial Resistance of ‘ESKAPE’ Pathogens by Exploiting Medicinal Plants
8. Study Limitations
9. Future Perspectives
10. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Conflicts of Interest
References
- Mishra, A.; Sharma, A.; Kumar, S.; Saxena, A.; Pandey, A. Bauhinia. Variegataleaf Extracts Exhibit Considerable Antibacterial, Antioxidant, And Anticancer Activities. BioMed Res. Int. 2013, 2013, 1–10. [Google Scholar] [CrossRef]
- Duraipandiyan, V.; Ayyanar, M.; Ignacimuthu, S. Antimicrobial Activity of some Ethnomedicinal Plants Used by Paliyar Tribe from Tamil Nadu, India. BMC Complement. Altern. Med. 2006, 6. [Google Scholar] [CrossRef]
- Chin, Y.; Balunas, M.; Chai, H.; Kinghorn, A. Drug Discovery from Natural Sources. AAPS J. 2006, 8, e239–e253. [Google Scholar] [CrossRef]
- Christenhusz, M.; Byng, J. The Number of Known Plants Species in the World Aand its Annual Increase. Phytotaxa 2016, 261, 21–217. [Google Scholar] [CrossRef]
- MNPS. Medicinal Plant Names Services (MNPS). Available online: https://www.kew.org/science/our-science/science-services/medicinal-plant-names-services (accessed on 14 August 2021).
- Srinivasan, D.; Nathan, S.; Suresh, T.; Lakshmana Perumalsamy, P. Antimicrobial Activity of Certain Indian Medicinal Plants used In Folkloric Medicine. J. Ethnopharmacol. 2001, 74, 217–220. [Google Scholar] [CrossRef]
- Yadav, R.; Agarwala, M. Phytochemical Analysis of some Medicinal Plants. J. Phytol. 2011, 3, 10–14. [Google Scholar]
- Tajkarimi, M.; Ibrahim, S.; Cliver, D. Antimicrobial Herb and Spice Compounds in Food. Food Control 2010, 21, 1199–1218. [Google Scholar] [CrossRef]
- Pandey, A.; Kumar, S. Perspective on Plant Products as Antimicrobials Agents: A Review. Pharmacologia 2013, 4, 469–480. [Google Scholar] [CrossRef]
- WHO. Antimicrobial Resistance; World Health Organization: Geneva, Switzerland, 2014. [Google Scholar]
- Baym, M.; Stone, L.; Kishony, R. Multidrug Evolutionary Strategies to Reverse Antibiotic Resistance. Science 2015, 351, aad3292. [Google Scholar] [CrossRef]
- Davies, J.; Davies, D. Origins and Evolution of Antibiotic Resistance. Microbiol. Mol. Biol. Rev. 2010, 74, 417–433. [Google Scholar] [CrossRef]
- WHO. Antimicrobial Resistance. Available online: https://www.who.int/health-topics/antimicrobial-resistance (accessed on 14 August 2021).
- Khameneh, B.; Diab, R.; Ghazvini, K.; Fazly Bazzaz, B. Breakthroughs in Bacterial Resistance Mechanisms and the Potential Ways to Combat them. Microb. Pathogen. 2016, 95, 32–42. [Google Scholar] [CrossRef]
- Tortorella, E.; Tedesco, P.; Palma Esposito, F.; January, G.; Fani, R.; Jaspars, M.; de Pascale, D. Antibiotics from Deep-Sea Microorganisms: Current Discoveries and Perspectives. Mar. Drugs 2018, 16, 355. [Google Scholar] [CrossRef]
- Penesyan, A.; Kjelleberg, S.; Egan, S. Development of Novel Drugs from Marine Surface Associated Microorganisms. Mar. Drugs 2010, 8, 438–459. [Google Scholar] [CrossRef]
- Talib, W.H. Anticancer and Antimicrobial Potential of Plant-Derived Natural Products. In Phytochemicals—Bioactivities and Impact on Health; Rasooli, I., Ed.; IntechOpen: London, UK, 2011; pp. 141–158. [Google Scholar] [CrossRef]
- Chavan, S.S.; Damale, M.G.; Shinde, D.B.; Sangshetti, J.N. Antibacterial and Antifungal Drugs from Natural Source: A Review of Clinical Development. In Natural Products in Clinical Trials; Benthan Science Books: Sharjah, United Arab Emirates, 2018; Volume 1, pp. 114–164. [Google Scholar] [CrossRef]
- Hostett, K. Strategy for the Biological and Chemical Evaluation of Plant Extracts. Pure Appl. Chem. 1998, 70, 1–9. [Google Scholar]
- Lampinen, J. Continuous Antimicrobial Susceptibility Testing in Drug Discovery. Drug Plus Int. 2005, 7, 1–3. Available online: http://www.thermoreadingroom.com/files/application_pdfs/File_30585.pdf (accessed on 14 August 2021).
- Emma, N.Q.; Antonio, R.S.; Marta, A.V. Screening Antifungal Activities of Selected Medicinal Plants. J. Ethnopharmacol. 2001, 74, 89–96. [Google Scholar] [CrossRef]
- Fazly Bazzaz, B.; Sarabandi, S.; Khameneh, B.; Hosseinzadeh, H. Effect of Catechins, Green Tea Extract and Methylxanthines in Combination with Gentamicin against Staphylococcus aureus and Pseudomonas aeruginosa—Combination Therapy Against Resistant Bacteria. J. Pharmacopunct. 2016, 19, 312–318. [Google Scholar] [CrossRef]
- Fazly Bazzaz, B.S.; Khameneh, B.; ZahedianOstad, M.R.; Hosseinzadeh, H. In vitro evaluation of antibacterial activity of verbascoside, lemon verbena extract and caffeine in combination with gentamicin against drug-resistant Staphylococcus aureus and Escherichia coli clinical isolates. Avicenna J. Phytomed. 2018, 8, 246–253. [Google Scholar]
- Ríos, J.; Recio, M. Medicinal Plants and Antimicrobial Activity. J. Ethnopharmacol. 2005, 100, 80–84. [Google Scholar] [CrossRef] [PubMed]
- Savoia, D. Plant-Derived Antimicrobial Compounds: Alternatives to Antibiotics. Future Microbiol. 2012, 7, 979–990. [Google Scholar] [CrossRef]
- Mehta, S.R.; Yusuf, S.; Peters, R.J.G.; Bertrand, M.E.; Lewis, B.S.; Natarajan, M.K.; Malmberg, K.; Rupprecht, H.-J.; Zhao, F.; Chrolavicius, S.; et al. Effects of pretreatment with clopidogrel and aspirin followed by long-term therapy in patients undergoing percutaneous coronary intervention: The PCI-CURE study. Lancet 2001, 358, 527–533. [Google Scholar] [CrossRef]
- Shankar, S.R.; Rangarajan, R.; Sarada, D.V.L.; Kumar, C.S. Evaluation of Antibacterial Activity and Phytochemical Screening of Wrightia Tinctoria L. Pharmacogn. J. 2010, 2, 19–22. [Google Scholar] [CrossRef]
- Lewis, K.; Ausubel, F.M. Prospects for Plant-Derived Antibacterials. Nat. Biotechnol. 2006, 24, 1504–1507. [Google Scholar] [CrossRef]
- Ody, P. The Complete Medicinal Herbal: A Practical Guide to the Healing Properties of Herbs; Skyhorse Publishing Inc.: New York, NY, USA, 2017; pp. 1–271. [Google Scholar]
- Ruddaraju, L.K.; Pammi, S.V.N.; Guntuku, G.S.; Padavala, V.S.; Kolapalli, V.R.M. A Review on Anti-Bacterials to Combat Resistance: From Ancient Era of Plants and Metals to Present and Future Perspectives of Green Nano Technological Combinations. Asian J. Pharm. Sci. 2020, 15, 42–59. [Google Scholar] [CrossRef]
- Reker, D.; Perna, A.M.; Rodrigues, T.; Schneider, P.; Reutlinger, M.; Mönch, B.; Koeberle, A.; Lamers, C.; Gabler, M.; Steinmetz, H.; et al. Revealing the Macromolecular Targets of Complex Natural Products. Nat. Chem. 2014, 6, 1072–1078. [Google Scholar] [CrossRef]
- Almabruk, K.H.; Dinh, L.K.; Philmus, B. Self-Resistance of Natural Product Producers: Past, Present, and Future Focusing on Self-Resistant Protein Variants. ACS Chem. Biol. 2018, 13, 1426–1437. [Google Scholar] [CrossRef]
- Wagner, H.; Ulrich-Merzenich, G. Synergy Research: Approaching a New Generation of Phytopharmaceuticals. Phytomedicine 2009, 16, 97–110. [Google Scholar] [CrossRef]
- Cowan, M.M. Plant Products as Antimicrobial Agents. Clin. Microbiol. Rev. 1999, 12, 564–582. [Google Scholar] [CrossRef]
- Tlili, N.; Elfalleh, W.; Saadaoui, E.; Khaldi, A.; Triki, S.; Nasri, N. The Caper (Capparis L.): Ethnopharmacology, Phytochemical and Pharmacological Properties. Fitoterapia 2011, 82, 93–101. [Google Scholar] [CrossRef]
- Joshi, R.K. A Perspective on the Phytopharmaceuticals Responsible for the Therapeutic Applications. In Recent Advances in Drug Delivery Technology; Keservani, R.K., Sharma, A.K., Keservani, R.K., Eds.; IGI Global: Hershey, PA, USA, 2017; pp. 208–228. [Google Scholar] [CrossRef]
- Kuete, V. Potential of Cameroonian Plants and Derived Products against Microbial Infections: A Review. Planta Med. 2010, 76, 1479–1491. [Google Scholar] [CrossRef]
- Dzotam, J.K.; Kuete, V. Antibacterial and Antibiotic-Modifying Activity of Methanol Extracts from Six Cameroonian Food Plants against Multidrug-Resistant Enteric Bacteria. BioMed Res. Int. 2017, 2017, 1583510. [Google Scholar] [CrossRef] [PubMed]
- Orozco-Topete, R.; Sierra-Madero, J.; Cano-Dominguez, C.; Kershenovich, J.; Ortiz-Pedroza, G.; Vazquez-Valls, E.; Garcia-Cosio, C.; Soria-Cordoba, A.; Armendariz, A.M.; Teran-Toledo, X.; et al. Safety and Efficacy of Virend for Topical Treatment of Genital and Anal Herpes Simplex Lesions in Patients with AIDS. Antivir. Res. 1997, 35, 91–103. [Google Scholar] [CrossRef]
- Wangchuk, P.; Keller, P.A.; Pyne, S.G.; Taweechotipatr, M.; Tonsomboon, A.; Rattanajak, R.; Kamchonwongpaisan, S. Evaluation of an Ethnopharmacologically Selected Bhutanese Medicinal Plants for Their Major Classes of Phytochemicals and Biological Activities. J. Ethnopharmacol. 2011, 137, 730–742. [Google Scholar] [CrossRef] [PubMed]
- Manandhar, S.; Luitel, S.; Dahal, R. In Vitro Antimicrobial Activity of Some Medicinal Plants against Human Pathogenic Bacteria. J. Trop. Med. 2019, 2019, 1–5. [Google Scholar] [CrossRef]
- Bereksi, M.; Hassaine, H.; Bekhechi, C.; Abdelouahid, D. Evaluation of Antibacterial Activity of Some Medicinal Plants Extracts Commonly Used in Algerian Traditional Medicine against Some Pathogenic Bacteria. Pharmacogn. J. 2018, 10, 507–512. [Google Scholar] [CrossRef]
- Osman, K.; Evangelopoulos, D.; Basavannacharya, C.; Gupta, A.; McHugh, T.D.; Bhakta, S.; Gibbons, S. An Antibacterial from Hypericum Acmosepalum Inhibits ATP-Dependent MurE Ligase from Mycobacterium Tuberculosis. Int. J. Antimicrob. Agents 2012, 39, 124–129. [Google Scholar] [CrossRef]
- Shiu, W.K.P.; Rahman, M.M.; Curry, J.; Stapleton, P.; Zloh, M.; Malkinson, J.P.; Gibbons, S. Antibacterial Acylphloroglucinols from Hypericum Olympicum. J. Nat. Prod. 2012, 75, 336–343. [Google Scholar] [CrossRef]
- Termentzi, A.; Fokialakis, N.; Skaltsounis, A.L. Natural Resins and Bioactive Natural Products Thereof as Potential Antimicrobial Agents. Curr. Pharm. Des. 2011, 17, 1267–1290. [Google Scholar] [CrossRef]
- Paraschos, S.; Mitakou, S.; Skaltsounis, A.-L. Chios Gum Mastic: A Review of its Biological Activities. Curr. Med. Chem. 2012, 19, 2292–2302. [Google Scholar] [CrossRef] [PubMed]
- Bosio, K.; Avanzini, C.; D’avolio, A.; Ozino, O.; Savoia, D. In Vitro Activity of Propolis against Streptococcus Pyogenes. Lett. Appl. Microbiol. 2000, 31, 174–177. [Google Scholar] [CrossRef] [PubMed]
- Kim, M.J.; Kim, C.S.; Kim, B.-H.; Ro, S.-B.; Lim, Y.K.; Park, S.-N.; Cho, E.; Cho, E.; Ko, J.-H.; Kwon, S.-S.; et al. Antimicrobial Effect of Korean Propolis against the Mutans Streptococci Isolated from Korean. J. Microb. 2011, 49, 161–164. [Google Scholar] [CrossRef]
- Jin, L.; Quan, C.; Hou, X.; Fan, S. Potential Pharmacological Resources: Natural Bioactive Compounds from Marine-Derived Fungi. Mar. Drugs 2016, 14, 76. [Google Scholar] [CrossRef] [PubMed]
- Reichling, J.; Schnitzler, P.; Suschke, U.; Saller, R. Essential Oils of Aromatic Plants with Antibacterial, Antifungal, Antiviral, and Cytotoxic Properties-An Overview. Forsch Komplementmed 2009, 16, 79–90. [Google Scholar] [CrossRef] [PubMed]
- Sienkiewicz, M.; Łysakowska, M.; Ciećwierz, J.; Denys, P.; Kowalczyk, E. Antibacterial Activity of Thyme and Lavender Essential Oils. Med. Chem. 2011, 7, 674–689. [Google Scholar] [CrossRef]
- Magiorakos, A.-P.; Srinivasan, A.; Carey, R.B.; Carmeli, Y.; Falagas, M.E.; Giske, C.G.; Harbarth, S.; Hindler, J.F.; Kahlmeter, G.; Olsson-Liljequist, B.; et al. Multidrug-Resistant, Extensively Drug-Resistant and Pandrug-Resistant Bacteria: An International Expert Proposal for Interim Standard Definitions for Acquired Resistance. Clin. Microbiol. Infect. 2012, 18, 268–281. [Google Scholar] [CrossRef]
- Velayati, A.A.; Masjedi, M.R.; Farnia, P.; Tabarsi, P.; Ghanavi, J.; ZiaZarifi, A.H.; Hoffner, S.E. Emergence of New Forms of Totally Drug-Resistant Tuberculosis Bacilli: Super Extensively Drug-Resistant Tuberculosis or Totally Drug-Resistant Strains in Iran. Chest 2009, 136, 420–425. [Google Scholar] [CrossRef] [PubMed]
- Walsh, C. Where Will New Antibiotics Come From? Nat. Rev. Microbiol. 2003, 1, 65–70. [Google Scholar] [CrossRef]
- Maxwell, A. DNA Gyrase as a Drug Target. Trends Microbiol. 1997, 5, 102–109. [Google Scholar] [CrossRef]
- Schneider, T.; Sahl, H.-G. An Oldie but a Goodie—Cell Wall Biosynthesis as Antibiotic Target Pathway. Int. J. Med. Microbiol. 2010, 300, 161–169. [Google Scholar] [CrossRef]
- Poyrel, L.; Jayol, A.; Norrdmann, P. Polymyxins: Antibacterial Activity, Susceptibility Testing, and Resistance Mechanisms Encoded by Plasmids or Chromosomes. Clin. Microb. Rev. 2017, 30, 557–596. [Google Scholar] [CrossRef]
- Bezirtzoglou, E.; Alexopoulos, A.; Voidarou, C. Apparent antibiotic misuse in environmental ecosystems and food. Microb. Ecol. Health Dis. 2008, 20, 197–198. [Google Scholar] [CrossRef]
- Zilberberg, M.D.; Shorr, A.F.; Micek, S.T.; Vazquez-Guillamet, C.; Kollef, M.H. Multi-Drug Resistance, Inappropriate Initial Antibiotic Therapy and Mortality in Gram-Negative Severe Sepsis and Septic Shock: A Retrospective Cohort Study. Crit. Care 2014, 18, 596. [Google Scholar] [CrossRef]
- Morar, M.; Wright, G.D. The Genomic Enzymology of Antibiotic Resistance. Annu. Rev. Genet. 2010, 44, 25–51. [Google Scholar] [CrossRef] [PubMed]
- Ficker, C.E.; Arnason, J.T.; Vindas, P.S.; Alvarez, L.P.; Akpagana, K.; Gbéassor, M.; De Souza, C.; Smith, M.L. Inhibition of Human Pathogenic Fungi by Ethnobotanically Selected Plant Extracts. Mycoses 2003, 4, 29–37. [Google Scholar] [CrossRef]
- Pandey, A.K. Anti-Staphylococcal Activity of a Pan-Tropical Aggressive and Obnoxious Weed Parthenium Histerophorus: An in Vitro Study. Natl. Acad. Sci. Lett. 2007, 30, 383–386. [Google Scholar]
- Levy, S.B. Active Efflux Mechanisms for Antimicrobial Resistance. Antimicrob. Agents Chemother. 1992, 36, 695–703. [Google Scholar] [CrossRef]
- Tegos, G.P.; Haynes, M.; Strouse, J.J.; Khan, M.M.T.; Bologa, C.G.; Oprea, T.I.; Sklar, L.A. Microbial Efflux Pump Inhibition: Tactics and Strategies. Curr. Pharm. Des. 2011, 17, 1291–1302. [Google Scholar] [CrossRef] [PubMed]
- Lomovskaya, O.; Bostian, K.A. Practical Applications and Feasibility of Efflux Pump Inhibitors in the Clinic—A Vision for Applied Use. Biochem. Pharmacol. 2006, 71, 910–918. [Google Scholar] [CrossRef]
- Pagès, J.-M.; James, C.E.; Winterhalter, M. The Porin and the Permeating Antibiotic: A Selective Diffusion Barrier in Gram-Negative Bacteria. Nat. Rev. Microbiol. 2008, 6, 893–903. [Google Scholar] [CrossRef] [PubMed]
- Dé, E.; Baslé, A.; Jaquinod, M.; Saint, N.; Malléa, M.; Molle, G.; Pagès, J.M. A New Mechanism of Antibiotic Resistance in Enterobacteriaceae Induced by a Structural Modification of the Major Porin. Mol. Microbiol. 2001, 41, 189–198. [Google Scholar] [CrossRef]
- Shaw, K.J.; Rather, P.N.; Hare, R.S.; Miller, G.H. Molecular Genetics of Aminoglycoside Resistance Genes and Familial Relationships of the Aminoglycoside-Modifying Enzymes. Microbiol. Rev. 1993, 57, 138–163. [Google Scholar] [CrossRef]
- Over, U.; Gür, D.; Unal, S.; Miller, G.H.; Aminoglycoside Resistance Study Group. The Changing Nature of Aminoglycoside Resistance Mechanisms and Prevalence of Newly Recognized Resistance Mechanisms in Turkey. Clin. Microbiol. Infect. 2001, 7, 470–478. [Google Scholar] [CrossRef]
- Blair, J.M.A.; Webber, M.A.; Baylay, A.J.; Ogbolu, D.O.; Piddock, L.J.V. Molecular Mechanisms of Antibiotic Resistance. Nat. Rev. Microbiol. 2015, 13, 42–51. [Google Scholar] [CrossRef]
- Dever, L.A.; Dermody, T.S. Mechanisms of Bacterial Resistance to Antibiotics. Arch. Intern. Med. 1991, 151, 886–895. [Google Scholar] [CrossRef]
- Spratt, B.G. Resistance to Antibiotics Mediated by Target Alterations. Science 1994, 264, 388–393. [Google Scholar] [CrossRef] [PubMed]
- Bugg, T.D.; Wright, G.D.; Dutka-Malen, S.; Arthur, M.; Courvalin, P.; Walsh, C.T. Molecular Basis for Vancomycin Resistance in Enterococcus Faecium BM4147: Biosynthesis of a Depsipeptide Peptidoglycan Precursor by Vancomycin Resistance Proteins VanH and VanA. Biochemistry 1991, 30, 10408–10415. [Google Scholar] [CrossRef] [PubMed]
- Moloney, M.G. Natural Products as a Source for Novel Antibiotics. Trends Pharmacol. Sci. 2016, 37, 689–701. [Google Scholar] [CrossRef]
- Verpoorte, R. Exploration of Nature’s Chemodiversity: The Role of Secondary Metabolites as Leads in Drug Development. Drug Discov. Today 1998, 3, 232–238. [Google Scholar] [CrossRef]
- Mahmood, Z.A.; Mahmood, S.B.Z. Antibiotic Natural Products: Opportunities and Challenges. In Microbial Pathogens and Strategies for Combating Them: Science, Technology and Education; Méndez-Vilas, A., Ed.; Colorcon Limited: Dartford Kent, UK, 2013; pp. 823–833. [Google Scholar]
- Barbieri, R.; Coppo, E.; Marchese, A.; Daglia, M.; Sobarzo-Sánchez, E.; Nabavi, S.F.; Nabavi, S.M. Phytochemicals for Human Disease: An Update on Plant-Derived Compounds Antibacterial Activity. Microbiol. Res. 2017, 196, 44–68. [Google Scholar] [CrossRef]
- Stefanovic, O. Synergistic Antibacterial Interaction between Melissa Officinalis Extracts and Antibiotics. J. Appl. Pharm. Sci. 2012, 2, 1–5. [Google Scholar]
- Merkl, R.; Hrádková, I.; Filip, V.; Šmidrkal, J. Antimicrobial and Antioxidant Properties of Phenolic Acids Alkyl Esters. Czech J. Food Sci. 2010, 28, 275–279. [Google Scholar] [CrossRef]
- Arima, H.; Ashida, H.; Danno, G. Rutin-Enhanced Antibacterial Activities of Flavonoids against Bacillus cereus and Salmonella enteritidis. Biosci. Biotechnol. Biochem. 2002, 66, 1009–1014. [Google Scholar] [CrossRef]
- Assob, J.C.N.; Kamga, H.L.F.; Nsagha, D.S.; Njunda, A.L.; Nde, P.F.; Asongalem, E.A.; Njouendou, A.J.; Sandjon, B.; Penlap, V.B. Antimicrobial and Toxicological Activities of Five Medicinal Plant Species from Cameroon Traditional Medicine. BMC Complement. Altern. Med. 2011, 11, 70. [Google Scholar] [CrossRef]
- Radulović, N.S.; Blagojević, P.D.; Stojanović-Radić, Z.Z.; Stojanović, N.M. Antimicrobial Plant Metabolites: Structural Diversity and Mechanism of Action. Curr. Med. Chem. 2013, 20, 932–952. [Google Scholar] [PubMed]
- Saleem, M.; Nazir, M.; Ali, M.S.; Hussain, H.; Lee, Y.S.; Riaz, N.; Jabbar, A. Antimicrobial Natural Products: An Update on Future Antibiotic Drug Candidates. Nat. Prod. Rep. 2010, 27, 238–254. [Google Scholar] [CrossRef] [PubMed]
- Vadhana, P.; Singh, B.; Bharadwaj, M.; Singh, S. Emergence of Herbal Antimicrobial Drug Resistance in Clinical Bacterial Isolates. Pharm. Anal. Acta 2015, 6, 1–7. [Google Scholar] [CrossRef]
- Anandhi, D.; Srinivasan, P.T.; Kumar, G.P.; Jagatheesh, S. DNA Fragmentation Induced by the Glycosides and Flavonoids from C. coriaria. Int. J. Curr. Microbiol. Appl. Sci. 2014, 3, 666–673. [Google Scholar]
- Mogosanu, G.D.; Grumezescu, A.M.; Huang, K.-S.; Bejenaru, L.E.; Bejenaru, C. Prevention of Microbial Communities: Novel Approaches Based Natural Products. Curr. Pharm. Biotechnol. 2015, 16, 94–111. [Google Scholar] [CrossRef]
- Quave, C.L.; Estévez-Carmona, M.; Compadre, C.M.; Hobby, G.; Hendrickson, H.; Beenken, K.E.; Smeltzer, M.S. Ellagic Acid Derivatives from Rubus Ulmifolius Inhibit Staphylococcus aureus Biofilm Formation and Improve Response to Antibiotics. PLoS ONE 2012, 7, e28737. [Google Scholar] [CrossRef]
- Talekar, S.J.; Chochua, S.; Nelson, K.; Klugman, K.P.; Quave, C.L.; Vidal, J.E. 220D-F2 from Rubus Ulmifolius Kills Streptococcus Pneumoniae Planktonic Cells and Pneumococcal Biofilms. PLoS ONE 2014, 9, e97314. [Google Scholar] [CrossRef]
- Rajasekaran, D.; Palombo, E.A.; Yeo, T.C.; Ley, D.L.S.; Tu, C.L.; Malherbe, F.; Grollo, L. Evidence of Synergistic Activity of Medicinal Plant Extracts against Neuraminidase Inhibitor Resistant Strains of Influenza Viruses. Adv. Microbiol. 2014, 4, 1260. [Google Scholar] [CrossRef][Green Version]
- Kabera, J.N.; Semana, E.; Mussa, A.R.; He, X. Plant Secondary Metabolites: Biosynthesis, Classification, Function and Pharmacological Properties. J. Pharm. Pharmacol. 2014, 2, 377–392. [Google Scholar]
- Alamgir, A.N.M. Pharmacognostical Botany: Classification of Medicinal and Aromatic Plants (MAPs), Botanical Taxonomy, Morphology, and Anatomy of Drug Plants. In Therapeutic Use of Medicinal Plants and Their Extracts: Volume 1: Pharmacognosy; Progress in Drug Research; Alamgir, A.N.M., Ed.; Springer International Publishing: Berlin/Heidelberg, Germany, 2017; pp. 177–293. [Google Scholar] [CrossRef]
- Sridevi, D.; Shankar, C.; Prakash, P.; Park, J.H.; Thamaraiselvi, K. Inhibitory Effects of Reserpine against Efflux Pump Activity of Antibiotic Resistance Bacteria. Chem. Biol. Lett. 2017, 4, 69–72. [Google Scholar]
- Khameneh, B.; Iranshahy, M.; Ghandadi, M.; Atashbeyk, D.G.; Fazly Bazzaz, B.S.; Iranshahi, M. Investigation of the Antibacterial Activity and Efflux Pump Inhibitory Effect of Co-Loaded Piperine and Gentamicin Nanoliposomes in Methicillin-Resistant Staphylococcus aureus. Drug Dev. Ind. Pharm. 2015, 41, 989–994. [Google Scholar] [CrossRef] [PubMed]
- Siriyong, T.; Srimanote, P.; Chusri, S.; Yingyongnarongkul, B.-E.; Suaisom, C.; Tipmanee, V.; Voravuthikunchai, S.P. Conessine as a Novel Inhibitor of Multidrug Efflux Pump Systems in Pseudomonas Aeruginosa. BMC Complement. Altern. Med. 2017, 17, 1–7. [Google Scholar] [CrossRef] [PubMed]
- Boberek, J.; Stach, J.; Good, L. Genetic Evidence for Inhibition of Bacterial Division Protein FtsZ by Berberine. PLoS ONE 2010, 5, e13745. [Google Scholar] [CrossRef] [PubMed]
- Guay, I.; Boulanger, S.; Isabelle, C.; Brouillette, E.; Chagnon, F.; Bouarab, K.; Marsault, E.; Malouin, F. Tomatidine and Analog FC04–100 Possess Bactericidal Activities against Listeria, Bacillus and Staphylococcus spp. BMC Pharmacol. Toxicol. 2018, 19, 1–12. [Google Scholar] [CrossRef] [PubMed]
- Brown, A.R.; Ettefagh, K.A.; Todd, D.; Cole, P.S.; Egan, J.M.; Foil, D.H.; Graf, T.N.; Schindler, B.D.; Kaatz, G.W.; Cech, N.B. A Mass Spectrometry-Based Assay for Improved Quantitative Measurements of Efflux Pump Inhibition. PLoS ONE 2015, 10, e0124814. [Google Scholar] [CrossRef]
- Li, B.-H.; Zhang, R.; Du, Y.-T.; Sun, Y.-H.; Tian, W.-X. Inactivation Mechanism of the Beta-Ketoacyl-[Acyl Carrier Protein] Reductase of Bacterial Type-II Fatty Acid Synthase by Epigallocatechin Gallate. Biochem. Cell Biol. 2006, 84, 755–762. [Google Scholar] [CrossRef]
- Patel, K.; Tyagi, C.; Goyal, S.; Jamal, S.; Wahi, D.; Jain, R.; Bharadvaja, N.; Grover, A. Identification of Chebulinic Acid as Potent Natural Inhibitor of M. Tuberculosis DNA Gyrase and Molecular Insights into Its Binding Mode of Action. Comput. Biol. Chem. 2015, 59, 37–47. [Google Scholar] [CrossRef]
- Wu, Y.; Bai, J.; Zhong, K.; Huang, Y.; Qi, H.; Jiang, Y.; Gao, H. Antibacterial Activity and Membrane-Disruptive Mechanism of 3-p-Trans- Coumaroyl-2-Hydroxyquinic Acid, a Novel Phenolic Compound from Pine Needles of Cedrus Deodara, against Staphylococcus aureus. Molecules 2016, 21, 1084. [Google Scholar] [CrossRef] [PubMed]
- Wu, D.; Kong, Y.; Han, C.; Chen, J.; Hu, L.; Jiang, H.; Shen, X. D-Alanine: D-Alanine Ligase as a New Target for the Flavonoids Quercetin and Apigenin. Int. J. Antimicrob. Agents 2008, 32, 421–426. [Google Scholar] [CrossRef] [PubMed]
- Reiter, J.; Levina, N.; Van der Linden, M.; Gruhlke, M.; Martin, C.; Slusarenko, A.J. Diallylthiosulfinate (Allicin), a Volatile Antimicrobial from Garlic (Allium sativum), Kills Human Lung Pathogenic Bacteria, Including MDR Strains, as a Vapor. Molecules 2017, 22, 1711. [Google Scholar] [CrossRef]
- Wu, H.-Z.; Fei, H.-J.; Zhao, Y.; Liu, X.; Huang, Y.; Wu, S. Antibacterial mechanism of sulforaphane on Escherichia coli. Sichuan Da Xue Xue Bao Yi Xue Ban 2012, 43, 386–390. [Google Scholar] [PubMed]
- Beevi, S.S.; Mangamoori, L.N.; Dhand, V.; Ramakrishna, D.S. Isothiocyanate Profile and Selective Antibacterial Activity of Root, Stem, and Leaf Extracts Derived from Raphanus sativus L. Foodborne Pathog. Dis. 2009, 6, 129–136. [Google Scholar] [CrossRef] [PubMed]
- Basile, A.; Sorbo, S.; Spadaro, V.; Bruno, M.; Maggio, A.; Faraone, N.; Rosselli, S. Antimicrobial and Antioxidant Activities of Coumarins from the Roots of Ferulago Campestris (Apiaceae). Molecules 2009, 14, 939–952. [Google Scholar] [CrossRef] [PubMed]
- Tan, N.; Yazıcı-Tütüniş, S.; Bilgin, M.; Tan, E.; Miski, M. Antibacterial Activities of Pyrenylated Coumarins from the Roots of PrangosHulusii. Molecules 2017, 22, 1098. [Google Scholar] [CrossRef]
- Maxwell, A. The Interaction between Coumarin Drugs and DNA Gyrase. Mol. Microbiol. 1993, 9, 681–686. [Google Scholar] [CrossRef]
- Roy, S.K.; Kumari, N.; Pahwa, S.; Agrahari, U.C.; Bhutani, K.K.; Jachak, S.M.; Nandanwar, H. NorA Efflux Pump Inhibitory Activity of Coumarins from Mesua Ferrea. Fitoterapia 2013, 90, 140–150. [Google Scholar] [CrossRef]
- Togashi, N.; Hamashima, H.; Shiraishi, A.; Inoue, Y.; Takano, A. Antibacterial Activities Against Staphylococcus aureus of Terpene Alcohols With Aliphatic Carbon Chains. J. Essent. Oil Res. 2010, 22, 263–269. [Google Scholar] [CrossRef]
- De Carvalho, C.C.C.R.; da Fonseca, M.M.R. Carvone: Why and How Should One Bother to Produce This Terpene. Food Chem. 2006, 95, 413–422. [Google Scholar] [CrossRef]
- Sharifzadeh, A.; Khosravi, A.R.; Shokri, H.; Shirzadi, H. Potential Effect of 2-Isopropyl-5-Methylphenol (Thymol) Alone and in Combination with Fluconazole against Clinical Isolates of Candida albicans, C. glabrata and C. krusei. J. Mycol. Med. 2018, 28, 294–299. [Google Scholar] [CrossRef] [PubMed]
- Marinelli, L.; Di Stefano, A.; Cacciatore, I. Carvacrol and Its Derivatives as Antibacterial Agents. Phytochem. Rev. 2018, 17, 903–921. [Google Scholar] [CrossRef]
- Ali, S.M.; Khan, A.A.; Ahmed, I.; Musaddiq, M.; Ahmed, K.S.; Polasa, H.; Rao, L.V.; Habibullah, C.M.; Sechi, L.A.; Ahmed, N. Antimicrobial Activities of Eugenol and Cinnamaldehyde against the Human Gastric Pathogen Helicobacter pylori. Ann. Clin. Microbiol. Antimicrob. 2005, 4, 20. [Google Scholar] [CrossRef] [PubMed]
- Stary, F. The Natural Guide to Medicinal Herbs and Plants; Barnes & Noble Books: New York, NY, USA, 1996. [Google Scholar]
- Kim, S.H.; Lee, S.J.; Lee, J.H.; Sun, W.S.; Kim, J.H. Antimicrobial Activity of 9-O-Acyl- and 9-O-Alkylberberrubine Derivatives. Planta Med. 2002, 68, 277–281. [Google Scholar] [CrossRef] [PubMed]
- Cushnie, T.P.T.; Cushnie, B.; Lamb, A.J. Alkaloids: An Overview of Their Antibacterial, Antibiotic-Enhancing and Antivirulence Activities. Int. J. Antimicrob. Agents 2014, 44, 377–386. [Google Scholar] [CrossRef]
- Silva, O.; Duarte, A.; Cabrita, J.; Pimentel, M.; Diniz, A.; Gomes, E. Antimicrobial Activity of Guinea-Bissau Traditional Remedies. J. Ethnopharmacol. 1996, 50, 55–59. [Google Scholar] [CrossRef]
- Iwu, M.M.; Duncan, A.R.; Okunji, C.O. New Antimicrobials of Plant Origin. In Perspectives on New Crops and New Uses; Janick, J., Ed.; ASHS Press: Alexandria, VA, USA, 1999; pp. 457–462. [Google Scholar]
- Iwasa, K.; Moriyasu, M.; Yamori, T.; Turuo, T.; Lee, D.-U.; Wiegrebe, W. In Vitro Cytotoxicity of the Protoberberine-Type Alkaloids. J. Nat. Prod. 2001, 64, 896–898. [Google Scholar] [CrossRef]
- Yi, Z.B.; Yan, Y.; Liang, Y.Z.; Zeng, B. Evaluation of the Antimicrobial Mode of Berberine by LC/ESI-MS Combined with Principal Component Analysis. J. Pharm. Biomed. Anal. 2007, 44, 301–304. [Google Scholar] [CrossRef]
- Peng, L.; Kang, S.; Yin, Z.; Jia, R.; Song, X.; Li, L.; Li, Z.; Zou, Y.; Liang, X.; Li, L.; et al. Antibacterial Activity and Mechanism of Berberine against Streptococcus agalactiae. Int. J. Clin. Exp. Pathol. 2015, 8, 5217–5223. [Google Scholar]
- Ram, N.; Urs, R.; Dunleavy, J. Enhancement of the Bactericidal Activity of a Peroxidase System by Phenolic Compounds. Phytopathology 1975, 65, 686. [Google Scholar] [CrossRef]
- Kurek, A.; Grudniak, A.M.; Kraczkiewicz-Dowjat, A.; Wolska, K.I. New Antibacterial Therapeutics and Strategies. Pol. J. Microbiol. 2011, 60, 3–12. [Google Scholar] [CrossRef]
- Srivastava, J.; Chandra, H.; Nautiyal, A.R.; Kalra, S.J.S. Antimicrobial Resistance (AMR) and Plant-Derived Antimicrobials (PDAms) as an Alternative Drug Line to Control Infections. 3 Biotech 2014, 4, 451–460. [Google Scholar] [CrossRef] [PubMed]
- Friedman, M.; Henika, P.R.; Levin, C.E.; Mandrell, R.E.; Kozukue, N. Antimicrobial Activities of Tea Catechins and Theaflavins and Tea Extracts against Bacillus cereus. J. Food Prot. 2006, 69, 354–361. [Google Scholar] [CrossRef]
- Betts, J.W.; Kelly, S.M.; Haswell, S.J. Antibacterial Effects of Theaflavin and Synergy with Epicatechin against Clinical Isolates of Acinetobacter baumannii and Stenotrophomonas maltophilia. Int. J. Antimicrob. Agents 2011, 38, 421–425. [Google Scholar] [CrossRef] [PubMed]
- Cisowska, A.; Wojnicz, D.; Hendrich, A.B. Anthocyanins as Antimicrobial Agents of Natural Plant Origin. Nat. Prod. Commun. 2011, 6, 149–156. [Google Scholar] [CrossRef] [PubMed]
- Bouarab-Chibane, L.; Forquet, V.; Lantéri, P.; Clément, Y.; Léonard-Akkari, L.; Oulahal, N.; Degraeve, P.; Bordes, C. Antibacterial Properties of Polyphenols: Characterization and QSAR (Quantitative Structure–Activity Relationship) Models. Front. Microbiol. 2019, 10, 829. [Google Scholar] [CrossRef]
- Farhadi, F.; Khameneh, B.; Iranshahi, M.; Iranshahy, M. Antibacterial Activity of Flavonoids and Their Structure–Activity Relationship: An Update Review. Phytother. Res. 2019, 33, 13–40. [Google Scholar] [CrossRef]
- Górniak, I.; Bartoszewski, R.; Króliczewski, J. Comprehensive Review of Antimicrobial Activities of Plant Flavonoids. Phytochem. Rev. 2019, 18, 241–272. [Google Scholar] [CrossRef]
- Cazarolli, L.H.; Zanatta, L.; Alberton, E.H.; Figueiredo, M.S.R.B.; Folador, P.; Damazio, R.G.; Pizzolatti, M.G.; Silva, F.R.M.B. Flavonoids: Prospective Drug Candidates. Mini Rev. Med. Chem. 2008, 8, 1429–1440. [Google Scholar] [CrossRef]
- Ciocan, L.; Bara, B. Plant Products as Antimicrobial Agents. Genet. Biol. Mol. 2007, 8, 151–156. [Google Scholar] [CrossRef]
- Chandra, H.; Bishnoi, P.; Yadav, A.; Patni, B.; Mishra, A.P.; Nautiyal, A.R. Antimicrobial Resistance and the Alternative Resources with Special Emphasis on Plant-Based Antimicrobials—A Review. Plants 2017, 6, 16. [Google Scholar] [CrossRef]
- de Freitas Araújo, M.G.; Hilário, F.; Nogueira, L.G.; Vilegas, W.; dos Santos, L.C.; Bauab, T.M. Chemical Constituents of the Methanolic Extract of Leaves of Leiothrix Spiralis Ruhland and Their Antimicrobial Activity. Molecules 2011, 16, 10479–10490. [Google Scholar] [CrossRef]
- García, A.; Bocanegra-García, V.; Palma-Nicolás, J.P.; Rivera, G. Recent Advances in Antitubercular Natural Products. Eur. J. Med. Chem. 2012, 49, 1–23. [Google Scholar] [CrossRef]
- Cushnie, T.P.T.; Lamb, A.J. Antimicrobial Activity of Flavonoids. Int. J. Antimicrob. Agents 2005, 26, 343–356. [Google Scholar] [CrossRef] [PubMed]
- Engels, C.; Schieber, A.; Gänzle, M.G. Inhibitory Spectra and Modes of Antimicrobial Action of Gallotannins from Mango Kernels (Mangifera indica L.). Appl. Environ. Microbiol. 2011, 77, 2215–2223. [Google Scholar] [CrossRef] [PubMed]
- Drobnica, L.; Zemanová, M.; Nemec, P.; Antos, K.; Kristián, P.; Martvon, A.; Závodská, E. Antifungal Activity of Isothiocyanates and Related Compounds. 3. Derivatives of Biphenyl, Stilbene, Azobenzene, and Several Polycondensed Aromatic Hydrocarbons. Appl. Microbiol. 1968, 16, 582–587. [Google Scholar] [CrossRef] [PubMed]
- Kim, S.; Kubec, R.; Musah, R.A. Antibacterial and Antifungal Activity of Sulfur-Containing Compounds from Petiveria alliacea L. J. Ethnopharmacol. 2006, 104, 188–192. [Google Scholar] [CrossRef]
- Iranshahi, M.; Hassanzadeh-Khayat, M.; Bazzaz, B.S.F.; Sabeti, Z.; Enayati, F. High Content of Polysulphides in the Volatile Oil of FerulaLatisecta Rech. F. et Aell. Fruits and Antimicrobial Activity of the Oil. J. Essent. Oil Res. 2008, 20, 183–185. [Google Scholar] [CrossRef]
- Rehman, F.; Mairaj, S. Antimicrobial Studies of Allicin and Ajoene | Request PDF. Int. J. Pharm. Bio Sci. 2013, 4, 1095–1105. [Google Scholar]
- Haristoy, X.; Fahey, J.W.; Scholtus, I.; Lozniewski, A. Evaluation of the Antimicrobial Effects of Several Isothiocyanates on Helicobacter pylori. Planta Med. 2005, 71, 326–330. [Google Scholar] [CrossRef] [PubMed]
- Moon, J.-K.; Kim, J.-R.; Ahn, Y.-J.; Shibamoto, T. Analysis and Anti-Helicobacter Activity of Sulforaphane and Related Compounds Present in Broccoli (Brassica oleracea L.) Sprouts. J. Agric. Food Chem. 2010, 58, 6672–6677. [Google Scholar] [CrossRef] [PubMed]
- Fahey, J.W.; Stephenson, K.K.; Wade, K.L.; Talalay, P. Urease from Helicobacter pylori Is Inactivated by Sulforaphane and Other Isothiocyanates. Biochem. Biophys. Res. Commun. 2013, 435, 1–7. [Google Scholar] [CrossRef]
- Sobolewska, D.; Podolak, I.; Makowska-Wąs, J. Allium Ursinum: Botanical, Phytochemical and Pharmacological Overview. Phytochem. Rev. 2015, 14, 81–97. [Google Scholar] [CrossRef] [PubMed]
- Boghrati, Z.; Iranshahi, M. Ferula Species: A Rich Source of Antimicrobial Compounds. J. Herb. Med. 2019, 16, 100244. [Google Scholar] [CrossRef]
- Feldberg, R.S.; Chang, S.C.; Kotik, A.N.; Nadler, M.; Neuwirth, Z.; Sundstrom, D.C.; Thompson, N.H. In Vitro Mechanism of Inhibition of Bacterial Cell Growth by Allicin. Antimicrob. Agents Chemother. 1988, 32, 1763–1768. [Google Scholar] [CrossRef] [PubMed]
- Lanzotti, V.; Scala, F.; Bonanomi, G. Compounds from Allium Species with Cytotoxic and Antimicrobial Activity. Phytochem. Rev. 2014, 13, 769–791. [Google Scholar] [CrossRef]
- Lin, C.-M.; Preston, J.F.; Wei, C.-I. Antibacterial Mechanism of Allyl Isothiocyanate. J. Food Prot. 2000, 63, 727–734. [Google Scholar] [CrossRef]
- Sofrata, A.; Santangelo, E.M.; Azeem, M.; Borg-Karlson, A.-K.; Gustafsson, A.; Pütsep, K. Benzyl Isothiocyanate, a Major Component from the Roots of Salvadora Persica Is Highly Active against Gram-Negative Bacteria. PLoS ONE 2011, 6, e23045. [Google Scholar] [CrossRef]
- Calmes, B.; N’Guyen, G.; Dumur, J.; Brisach, C.A.; Campion, C.; Iacomi, B.; Pigné, S.; Dias, E.; Macherel, D.; Guillemette, T.; et al. Glucosinolate-Derived Isothiocyanates Impact Mitochondrial Function in Fungal Cells and Elicit an Oxidative Stress Response Necessary for Growth Recovery. Front. Plant Sci. 2015, 6, 414. [Google Scholar] [CrossRef]
- O’Kennedy, R.; Thornes, R.D.; Wiley. Coumarins: Biology, Applications and Mode of Action. Available online: https://www.wiley.com/en-us/Coumarins%3A+Biology%2C+Applications+and+Mode+of+Action-p-9780471969976 (accessed on 18 August 2021).
- Smyth, T.; Ramachandran, V.N.; Smyth, W.F. A Study of the Antimicrobial Activity of Selected Naturally Occurring and Synthetic Coumarins. Int. J. Antimicrob. Agents 2009, 33, 421–426. [Google Scholar] [CrossRef]
- Zhang, Y.; Sass, A.; Van Acker, H.; Wille, J.; Verhasselt, B.; Van Nieuwerburgh, F.; Kaever, V.; Crabbé, A.; Coenye, T. Coumarin Reduces Virulence and Biofilm Formation in Pseudomonas aeruginosa by Affecting Quorum Sensing, Type III Secretion and C-Di-GMP Levels. Front. Microbiol. 2018, 9, 1952. [Google Scholar] [CrossRef]
- Reen, F.J.; Gutiérrez-Barranquero, J.A.; Parages, M.L.; O Gara, F. Coumarin: A Novel Player in Microbial Quorum Sensing and Biofilm Formation Inhibition. Appl. Microbiol. Biotechnol. 2018, 102, 2063–2073. [Google Scholar] [CrossRef]
- Paduch, R.; Kandefer-Szerszeń, M.; Trytek, M.; Fiedurek, J. Terpenes: Substances Useful in Human Healthcare. ArchImmunol. Ther. Exp. 2007, 55, 315–327. [Google Scholar] [CrossRef]
- Oldfield, E.; Lin, F.-Y. Terpene Biosynthesis: Modularity Rules. Angew. Chem. Int. Ed. 2012, 51, 1124–1137. [Google Scholar] [CrossRef]
- Chang, S.-T.; Chen, P.-F.; Chang, S.-C. Antibacterial Activity of Leaf Essential Oils and Their Constituents from Cinnamomum Osmophloeum. J. Ethnopharmacol. 2001, 77, 123–127. [Google Scholar] [CrossRef]
- Imai, H.; Osawa, K.; Yasuda, H.; Hamashima, H.; Arai, T.; Sasatsu, M. Inhibition by the Essential Oils of Peppermint and Spearmint of the Growth of Pathogenic Bacteria. Microbios 2001, 106, 31–39. [Google Scholar]
- Zuzarte, M.; Gonçalves, M.J.; Cavaleiro, C.; Canhoto, J.; Vale-Silva, L.; Silva, M.J.; Pinto, E.; Salgueiro, L. Chemical Composition and Antifungal Activity of the Essential Oils of Lavandula viridis L’Her. J. Med. Microbiol. 2011, 60 Pt 5, 612–618. [Google Scholar] [CrossRef]
- Kamazeri, T.S.A.T.; Samah, O.A.; Taher, M.; Susanti, D.; Qaralleh, H. Antimicrobial Activity and Essential Oils of Curcuma aeruginosa, Curcuma mangga, and Zingiber cassumunar from Malaysia. Asian Pac. J. Trop Med. 2012, 5, 202–209. [Google Scholar] [CrossRef]
- Wan, J.; Wilcock, A.; Coventry, M.J. The Effect of Essential Oils of Basil on the Growth of Aeromonas Hydrophila and Pseudomonas Fluorescens. J. Appl. Microbiol. 1998, 84, 152–158. [Google Scholar] [CrossRef]
- Kaltschmidt, B.P.; Ennen, I.; Greiner, J.F.W.; Dietsch, R.; Patel, A.; Kaltschmidt, B.; Kaltschmidt, C.; Hütten, A. Preparation of Terpenoid-Invasomes with Selective Activity against S. Aureus and Characterization by Cryo Transmission Electron Microscopy. Biomedicines 2020, 8, 105. [Google Scholar] [CrossRef] [PubMed]
- Banso, A. Phytochemical and Antibacterial Investigation of Bark Extracts of Acacia Nilotica. JMPR 2009, 3, 082–085. [Google Scholar] [CrossRef]
- Copp, B.R. Antimycobacterial Natural Products. Nat. Prod. Rep. 2003, 20, 535–557. [Google Scholar] [CrossRef] [PubMed]
- Chouhan, S.; Sharma, K.; Guleria, S. Antimicrobial Activity of Some Essential Oils-Present Status and Future Perspectives. Medicines 2017, 4, 58. [Google Scholar] [CrossRef]
- Phitaktim, S.; Chomnawang, M.; Sirichaiwetchakoon, K.; Dunkhunthod, B.; Hobbs, G.; Eumkeb, G. Synergism and the Mechanism of Action of the Combination of α-Mangostin Isolated from Garcinia Mangostana L. and Oxacillin against an Oxacillin-Resistant Staphylococcus Saprophyticus. BMC Microbiol. 2016, 16, 195. [Google Scholar] [CrossRef]
- Gibbons, S.; Oluwatuyi, M.; Veitch, N.C.; Gray, A.I. Bacterial Resistance Modifying Agents from Lycopus Europaeus. Phytochemistry 2003, 62, 83–87. [Google Scholar] [CrossRef]
- Al-hebshi, N.; Al-haroni, M.; Skaug, N. In Vitro Antimicrobial and Resistance-Modifying Activities of Aqueous Crude Khat Extracts against Oral Microorganisms. Arch. Oral Biol. 2006, 51, 183–188. [Google Scholar] [CrossRef]
- Szalek, E.; Grzeskowiak, E.; Kozielczyk, J. Interactions between Herbal and Synthetic Drugs. Advantages and Risks. Herba Pol. 2006, 52, 153–157. [Google Scholar]
- Aiyegoro, O.A.; Afolayan, A.J.; Okoh, A.I. In Vitro Antibacterial Activities of Crude Extracts of the Leaves of Helichrysum Longifolium in Combination with Selected Antibiotics. Afr. J. Pharm. Pharmacol. 2009, 3, 293–300. [Google Scholar]
- Farooqui, A.; Khan, A.; Borghetto, I.; Kazmi, S.U.; Rubino, S.; Paglietti, B. Synergistic Antimicrobial Activity of Camellia Sinensis and Juglans Regia against Multidrug-Resistant Bacteria. PLoS ONE 2015, 10, e0118431. [Google Scholar] [CrossRef]
- Marquez, B.; Neuville, L.; Moreau, N.J.; Genet, J.-P.; dos Santos, A.F.; Caño de Andrade, M.C.; Goulart Sant’Ana, A.E. Multidrug Resistance Reversal Agent from Jatropha Elliptica. Phytochemistry 2005, 66, 1804–1811. [Google Scholar] [CrossRef] [PubMed]
- Morel, C.; Stermitz, F.R.; Tegos, G.; Lewis, K. Isoflavones as Potentiators of Antibacterial Activity. J. Agric. Food. Chem. 2003, 51, 5677–5679. [Google Scholar] [CrossRef] [PubMed]
- Abreu, A.C.; McBain, A.J.; Simões, M. Plants as Sources of New Antimicrobials and Resistance-Modifying Agents. Nat. Prod. Rep. 2012, 29, 1007–1021. [Google Scholar] [CrossRef] [PubMed]
- Stavri, M.; Piddock, L.J.V.; Gibbons, S. Bacterial Efflux Pump Inhibitors from Natural Sources. J. Antimicrob. Chemother. 2007, 59, 1247–1260. [Google Scholar] [CrossRef]
- Shin, S. Anti-Aspergillus Activities of Plant Essential Oils and Their Combination Effects with Ketoconazole or Amphotericin B. Arch. Pharm. Res. 2003, 26, 389–393. [Google Scholar] [CrossRef]
- Shin, S.; Kang, C.-A. Antifungal Activity of the Essential Oil of Agastache Rugosa Kuntze and Its Synergism with Ketoconazole. Lett. Appl. Microbiol. 2003, 36, 111–115. [Google Scholar] [CrossRef]
- Dos Santos, K.K.A.; Matias, E.F.F.; Tintino, S.R.; Souza, C.E.S.; Braga, M.F.B.M.; Guedes, G.M.M.; Rolón, M.; Vega, C.; de Arias, A.R.; Costa, J.G.M.; et al. Cytotoxic, Trypanocidal, and Antifungal Activities of Eugenia Jambolana L. J. Med. Food 2012, 15, 66–70. [Google Scholar] [CrossRef]
- Chovanová, R.; Mikulášová, M.; Vaverková, S. In Vitro Antibacterial and Antibiotic Resistance Modifying Effect of Bioactive Plant Extracts on Methicillin-Resistant Staphylococcus Epidermidis. Int. J. Microbiol. 2013, 2013, 760969. [Google Scholar] [CrossRef]
- Chusri, S.; Villanueva, I.; Voravuthikunchai, S.P.; Davies, J. Enhancing Antibiotic Activity: A Strategy to Control Acinetobacter Infections. J. Antimicrob. Chemother. 2009, 64, 1203–1211. [Google Scholar] [CrossRef]
- Gallucci, N.; Casero, C.; Oliva, M.; Zygadlo, J.; Demo, M.; Córdoba, P. Interaction between Terpenes and Penicillin on Bacterial Strains Resistant to Beta- Lactam Antibiotics. Mol. Med. Chem. 2006, 10, 30–32. [Google Scholar]
- Oliveira, R.A.G.; Lima, E.O.; Vieira, W.L.; Freire, K.R.L.; Trajano, V.N.; Lima, I.O. Study of the Interference of Essential Oils on the Activity of Some Antiniotics Used Clinically. Rev. Bras. Pharmacogn. 2006, 16, 77–82. [Google Scholar] [CrossRef]
- van Vuuren, S.F.; Suliman, S.; Viljoen, A.M. The Antimicrobial Activity of Four Commercial Essential Oils in Combination with Conventional Antimicrobials. Lett. Appl. Microbiol. 2009, 48, 440–446. [Google Scholar] [CrossRef] [PubMed]
- Ghosh, A.; Das, B.K.; Roy, A.; Mandal, B.; Chandra, G. Antibacterial Activity of Some Medicinal Plant Extracts. J. Nat. Med. 2008, 62, 259–262. [Google Scholar] [CrossRef]
- Pandey, A.; Kumar, S. Antioxidant, Lipo-Protective and Antibacterial Activities of Phytoconstituents Present in Solanum Xanthocarpum Root. Int. Rev. Biophys. Chem. 2012, 3, 42–47. [Google Scholar] [CrossRef]
- Pandey, A.; Tripathi, S. Concept of Standardization, Extraction and Pre Phytochemical Screening Strategies for Herbal Drug. J. Pharmacogn. Phytochem. 2014, 2, 115–119. [Google Scholar]
- Ingle, K.; Deshmukh, A.G.; Padole, D.A.; Dudhare, M.; Moharil, M.; Vc, K. Phytochemicals: Extraction Methods, Identification and Detection of Bioactive Compounds from Plant Extracts. J. Pharmacogn. Phytochem. 2017, 6, 32–36. [Google Scholar]
- Deutch, C.E. Limited Effectiveness of Over-the-Counter Plant Preparations Used for the Treatment of Urinary Tract Infections as Inhibitors of the Urease Activity from Staphylococcus saprophyticus. J. Appl. Microbiol. 2017, 122, 1380–1388. [Google Scholar] [CrossRef] [PubMed]
- Calixto, J.B. Efficacy, Safety, Quality Control, Marketing and Regulatory Guidelines for Herbal Medicines (Phytotherapeutic Agents). Braz. J. Med. Biol. Res. 2000, 33, 179–189. [Google Scholar] [CrossRef]
- Njume, C.; Goduka, N.I. Treatment of Diarrhoea in Rural African Communities: An Overview of Measures to Maximise the Medicinal Potentials of Indigenous Plants. Int. J. Environ. Res. Public Health 2012, 9, 3911–3933. [Google Scholar] [CrossRef]
- Rodrigues, E.; Barnes, J. Pharmacovigilance of Herbal Medicines: The Potential Contributions of Ethnobotanical and Ethnopharmacological Studies. Drug Saf. 2013, 36, 1–12. [Google Scholar] [CrossRef]
- Bhardwaj, S.; Verma, R.; Gupta, J. Challenges and Future Prospects of Herbal Medicine. Int. Res. Med. Health Sci. 2018. [Google Scholar] [CrossRef]
- Eloff, J.N. Which Extractant Should Be Used for the Screening and Isolation of Antimicrobial Components from Plants? J. Ethnopharmacol. 1998, 60, 1–8. [Google Scholar] [CrossRef]
- Parekh, J.; Jadeja, D.; Chanda, S. Efficacy of Aqueous and Methanol Extracts of Some Medicinal Plants for Potential Antibacterial Activity. Turk. J. Biol. 2005, 29, 203–210. [Google Scholar]
- Serkedjieva, J.; Manolova, N.; Bankova, V. Anti-Influenza Virus Effect of Some Propolis Constituents and Their Analogues (Esters of Substituted Cinnamic Acids). J. Nat. Prod. 1992, 55, 294–302. [Google Scholar] [CrossRef]
- Masoko, P.; Eloff, J.N. Bioautography Indicates the Multiplicity of Antifungal Compounds from Twenty-Four Southern African Combretum Species (Combretaceae). Afr. J. Biotechnol. 2006, 5, 1625–1647. [Google Scholar] [CrossRef]
- Eloff, J.N. A Sensitive and Quick Microplate Method to Determine the Minimal Inhibitory Concentration of Plant Extracts for Bacteria. Planta Med. 1998, 64, 711–713. [Google Scholar] [CrossRef] [PubMed]
- Nostro, A.; Germanò, M.P.; D’Angelo, V.; Marino, A.; Cannatelli, M.A. Extraction Methods and Bioautography for Evaluation of Medicinal Plant Antimicrobial Activity. Lett. Appl. Microbiol. 2000, 30, 379–384. [Google Scholar] [CrossRef] [PubMed]
- Green, R.J. Antioxidant Activity of Peanut Plant Tissues; NC State: Raleigh, NC, USA, 2004. [Google Scholar]
- Majekodunmi, S.O. Review of extraction of medicinal plants for pharmaceutical research. Merit. Res. J. Med. Med. Sci. 2015, 11, 521–527. [Google Scholar]
- Sasidharan, S.; Chen, Y.; Saravanan, D.; Sundram, K.M.; Yoga Latha, L. Extraction, Isolation and Characterization of Bioactive Compounds from Plants’ Extracts. Afr. J. Tradit. Complement. Altern. Med. 2011, 8, 1–10. [Google Scholar] [CrossRef] [PubMed]
- Handa, S.S.; Khanuja, S.P.S.; Longo, G.; Rakesh, D.D.; United Nations Industrial Development Organization; International Centre for Science and High Technology. Extraction Technologies for Medicinal and Aromatic Plants; Earth, Environmental and Marine Sciences and Technologies: Trieste, Italy, 2008. [Google Scholar]
- Banu, K.S.; Cathrine, L. General Techniques Involved in Phytochemical Analysis. Int. J. Adv. Res. Chem. Sci. 2015, 2, 25–32. [Google Scholar]
- Altemimi, A.; Lakhssassi, N.; Baharlouei, A.; Watson, D.G.; Lightfoot, D.A. Phytochemicals: Extraction, Isolation, and Identification of Bioactive Compounds from Plant Extracts. Plants 2017, 6, 42. [Google Scholar] [CrossRef] [PubMed]
- Tan, J.B.L.; Lim, Y.Y. Critical Analysis of Current Methods for Assessing the in Vitro Antioxidant and Antibacterial Activity of Plant Extracts. Food Chem. 2015, 172, 814–822. [Google Scholar] [CrossRef] [PubMed]
- Huie, C.W. A Review of Modern Sample-Preparation Techniques for the Extraction and Analysis of Medicinal Plants. Anal. Bioanal. Chem. 2002, 373, 23–30. [Google Scholar] [CrossRef] [PubMed]
- Vilegas, J.H.Y.; de Marchi, E.; Lancas, F.M. Extraction of Low-Polarity Compounds (with Emphasis on Coumarin and Kaurenoic Acid) from Mikania glomerata (‘Guaco’) Leaves. Phytochem. Anal. 1997, 8, 266–270. [Google Scholar] [CrossRef]
- EUCAST. Determination of Minimum Inhibitory Concentrations (MICs) of Antibacterial Agents by Broth Dilution. Clin. Microbiol. Infect. 2003, 9, ix–xv. [Google Scholar] [CrossRef]
- Rios, J.L.; Recio, M.C.; Villar, A. Screening Methods for Natural Products with Antimicrobial Activity: A Review of the Literature. J. Ethnopharmacol. 1988, 23, 127–149. [Google Scholar] [CrossRef]
- Ross, Z.M.; O’Gara, E.A.; Hill, D.J.; Sleightholme, H.V.; Maslin, D.J. Antimicrobial Properties of Garlic Oil against Human Enteric Bacteria: Evaluation of Methodologies and Comparisons with Garlic Oil Sulfides and Garlic Powder. Appl. Environ. Microbiol. 2001, 67, 475–480. [Google Scholar] [CrossRef]
- Hammer, K.A.; Carson, C.F.; Riley, T.V. Antimicrobial Activity of Essential Oils and Other Plant Extracts. J. Appl. Microbiol. 1999, 86, 985–990. [Google Scholar] [CrossRef]
- Balouiri, M.; Sadiki, M.; Ibnsouda, S.K. Methods for in Vitro Evaluating Antimicrobial Activity: A Review. J. Pharm. Anal. 2016, 6, 71–79. [Google Scholar] [CrossRef]
- Ncube, N.S.; Afolayan, A.J.; Okoh, A.I. Assessment Techniques of Antimicrobial Properties of Natural Compounds of Plant Origin: Current Methods and Future Trends. Afr. J. Biotechnol. 2008, 7, 1797–1806. [Google Scholar] [CrossRef]
- Valgas, C.; de Souza, S.M.; Smânia, E.F.A.; Smânia, A., Jr. Screening Methods to Determine Antibacterial Activity of Natural Products. Braz. J. Microbiol. 2007, 38, 369–380. [Google Scholar] [CrossRef]
- Wiegand, I.; Hilpert, K.; Hancock, R.E.W. Agar and Broth Dilution Methods to Determine the Minimal Inhibitory Concentration (MIC) of Antimicrobial Substances. Nat. Protoc. 2008, 3, 163–175. [Google Scholar] [CrossRef] [PubMed]
- Langfield, R.D.; Scarano, F.J.; Heitzman, M.E.; Kondo, M.; Hammond, G.B.; Neto, C.C. Use of a Modified Microplate Bioassay Method to Investigate Antibacterial Activity in the Peruvian Medicinal Plant Peperomia Galioides. J. Ethnopharmacol. 2004, 94, 279–281. [Google Scholar] [CrossRef] [PubMed]
- Schwalbe, R.; Steele-Moore, L.; Goodwin, A.C. Antimicrobial Susceptibility Testing Protocols; CRC Press: Boca Raton, FL, USA, 2007. [Google Scholar] [CrossRef]
- Efferth, T.; Koch, E. Complex Interactions between Phytochemicals. The Multi-Target Therapeutic Concept of Phytotherapy. Curr. Drug Targets 2011, 12, 122–132. [Google Scholar] [CrossRef] [PubMed]
- van Vuuren, S.; Viljoen, A. Plant-Based Antimicrobial Studies--Methods and Approaches to Study the Interaction between Natural Products. Planta Med. 2011, 77, 1168–1182. [Google Scholar] [CrossRef] [PubMed]
- Enke, C.G.; Nagels, L.J. Undetected Components in Natural Mixtures: How Many? What Concentrations? Do They Account for Chemical Noise? What Is Needed to Detect Them? Anal. Chem. 2011, 83, 2539–2546. [Google Scholar] [CrossRef]
- Stermitz, F.R.; Lorenz, P.; Tawara, J.N.; Zenewicz, L.A.; Lewis, K. Synergy in a Medicinal Plant: Antimicrobial Action of Berberine Potentiated by 5′-Methoxyhydnocarpin, a Multidrug Pump Inhibitor. Proc. Natl. Acad. Sci. USA 2000, 97, 1433–1437. [Google Scholar] [CrossRef]
- Stermitz, F.R.; Scriven, L.N.; Tegos, G.; Lewis, K. Two Flavonols from Artemisa Annua Which Potentiate the Activity of Berberine and Norfloxacin against a Resistant Strain of Staphylococcus aureus. Planta Med. 2002, 68, 1140–1141. [Google Scholar] [CrossRef]
- Ulrich-Merzenich, G.; Panek, D.; Zeitler, H.; Vetter, H.; Wagner, H. Drug Development from Natural Products: Exploiting Synergistic Effects. Indian J. Exp. Biol. 2010, 48, 208–219. [Google Scholar]
- Junio, H.A.; Sy-Cordero, A.A.; Ettefagh, K.A.; Burns, J.T.; Micko, K.T.; Graf, T.N.; Richter, S.J.; Cannon, R.E.; Oberlies, N.H.; Cech, N.B. Synergy-Directed Fractionation of Botanical Medicines: A Case Study with Goldenseal (Hydrastis canadensis). J. Nat. Prod. 2011, 74, 1621–1629. [Google Scholar] [CrossRef]
- Tian, F.; Li, B.; Ji, B.; Zhang, G.; Luo, Y. Identification and Structure-Activity Relationship of Gallotannins Separated from Galla Chinensis. LWT Food Sci. Technol. 2009, 42, 1289–1295. [Google Scholar] [CrossRef]
- Ma, X.H.; Zheng, C.J.; Han, L.Y.; Xie, B.; Jia, J.; Cao, Z.W.; Li, Y.X.; Chen, Y.Z. Synergistic Therapeutic Actions of Herbal Ingredients and Their Mechanisms from Molecular Interaction and Network Perspectives. Drug Discov. Today 2009, 14, 579–588. [Google Scholar] [CrossRef]
- Rather, M.A.; Bhat, B.A.; Qurishi, M.A. Multicomponent Phytotherapeutic Approach Gaining Momentum: Is the “One Drug to Fit All” Model Breaking Down? Phytomedicine 2013, 21, 1–14. [Google Scholar] [CrossRef]
- Kellogg, J.J.; Todd, D.A.; Egan, J.M.; Raja, H.A.; Oberlies, N.H.; Kvalheim, O.M.; Cech, N.B. Biochemometrics for Natural Products Research: Comparison of Data Analysis Approaches and Application to Identification of Bioactive Compounds. J. Nat. Prod. 2016, 79, 376–386. [Google Scholar] [CrossRef] [PubMed]
- Lederer, S.; Dijkstra, T.M.H.; Heskes, T. Additive Dose Response Models: Explicit Formulation and the Loewe Additivity Consistency Condition. Front. Pharmacol. 2018, 9, 31. [Google Scholar] [CrossRef] [PubMed]
- Yadav, B.; Wennerberg, K.; Aittokallio, T.; Tang, J. Searching for Drug Synergy in Complex Dose–Response Landscapes Using an Interaction Potency Model. Comp. Struct. Biotechnol. J. 2015, 13, 504–513. [Google Scholar] [CrossRef]
- Alminger, M.; Aura, A.-M.; Bohn, T.; Dufour, C.; El, S.N.; Gomes, A.; Karakaya, S.; Martínez-Cuesta, M.C.; McDougall, G.J.; Requena, T.; et al. In Vitro Models for Studying Secondary Plant Metabolite Digestion and Bioaccessibility. Compr. Rev. Food Sci. Food Saf. 2014, 13, 413–436. [Google Scholar] [CrossRef]
- Owais, M.; Sharad, K.S.; Shehbaz, A.; Saleemuddin, M. Antibacterial Efficacy of Withania somnifera (Ashwagandha) an Indigenous Medicinal Plant against Experimental Murine Salmonellosis. Phytomedicine 2005, 12, 229–235. [Google Scholar] [CrossRef]
- Kengni, F.; Fodouop, S.P.C.; Tala, D.S.; Djimeli, M.N.; Fokunang, C.; Gatsing, D. Antityphoid Properties and Toxicity Evaluation of Harungana madagascariensis Lam (Hypericaceae) Aqueous Leaf Extract. J. Ethnopharmacol. 2016, 179, 137–145. [Google Scholar] [CrossRef] [PubMed]
- Holst, L.; Havnen, G.C.; Nordeng, H. Echinacea and Elderberryâ should They Be Used against Upper Respiratory Tract Infections during Pregnancy? Front. Pharmacol. 2014, 5, 1–12. [Google Scholar] [CrossRef]
- Boullata, J.I.; Nace, A.M. Safety Issues with Herbal Medicine. Pharmacotherapy 2000, 20, 257–269. [Google Scholar] [CrossRef] [PubMed]
- Canter, P.H.; Thomas, H.; Ernst, E. Bringing Medicinal Plants into Cultivation: Opportunities and Challenges for Biotechnology. Trends Biotechnol. 2005, 23, 180–185. [Google Scholar] [CrossRef] [PubMed]
- Charlwood, B.V.; Pletsch, M. Manipulation of Natural Product Accumulation in Plants Through Genetic Engineering. J. Herbs Spices Med. Plants 2002, 9, 139–151. [Google Scholar] [CrossRef]
- Tsigalou, C.; Konstantinidis, T.; Stavropoulou, E.; Bezirtzoglou, E.; Tsakris, A. Potential Elimination of Human Gut Resistome by Exploiting the Benefits of Functional Foods. Front. Microbiol. 2020, 11, 50. [Google Scholar] [CrossRef] [PubMed]
- Bhatia, P.; Sharma, A.; George, A.J.; Anvitha, D.; Kumar, P.; Dwivedi, V.P.; Chandra, N.S. Antibacterial activity of medicinal plants against ESKAPE: An update. Heliyon 2021, 7, e06310. [Google Scholar] [CrossRef] [PubMed]
- Boucher, H.W.; Talbot, G.H.; Bradley, J.S.; Edwards, J.E.; Gilbert, D.; Rice, L.B.; Scheld, M.; Spellberg, B.; Bartlett, J. Bad bugs, no drugs: No ESKAPE! An update from the Infectious Diseases Society of America. Clin. Infect. Dis. 2009, 48, 1–12. [Google Scholar] [CrossRef] [PubMed]
- WHO. Traditional Medicine Strategy 2002–2005; WHO: Geneva, Switzerland, 2002. [Google Scholar]
- Khan, M.F.; Tang, H.; Lyles, J.T.; Pineau, R.; Mashwani, Z.U.; Quave, C.L. Antibacterial Properties of Medicinal Plants from Pakistan Against Multidrug-Resistant ESKAPE Pathogens. Front. Pharmacol. 2018, 9, 815. [Google Scholar] [CrossRef] [PubMed]
- Chandrasekharan, D.; Ballal, R.; Ballal, B.B.; Khetmalas, M.B. Evaluation of Selected Medicinal Plants for Their Potential Antimicrobial Activities Against ESKAPE Pathogens and The Study of P-Glycoprotein Related Antibiosis; An Indirect Approach To Assess Efflux Mechanism. Int. J. Recent Sci. Res. 2018, 9, 29461–29466. [Google Scholar]
- Dong, Y.; Wang, B.; Zhang, Y. Clinical and Experimental Study on Treatment of Infantile Mycotic Enteritis by Jiechang Mixture. Chin. J. Integr. Trad. West. Med. 2001, 21, 419–421. [Google Scholar]
- Yang, X.; Chen, D.; Chai, L.; Duan, H.; Guo, H.; Li, S.; Xiao, M.; Chen, H. A Case Report of Poisoning Caused by Incorrect Use of Salvia. Am. J. Case Rep. 2016, 17, 580–583. [Google Scholar] [CrossRef]
- Mann, C.M.; Markham, J.L. A New Method for Determining the Minimum Inhibitory Concentration of Essential Oils. J Appl. Microbiol. 1998, 84, 538–544. [Google Scholar] [CrossRef] [PubMed]
- McGrady, B.; Ho, C.S. Identifying Gaps in International Food Safety Regulation. Food Drug Law J. 2011, 66, 183–202. [Google Scholar] [PubMed]
- Raclariu, A.C.; Heinrich, M.; Ichim, M.C.; de Boer, H. Benefits and Limitations of DNA Barcoding and Metabarcoding in Herbal Product Authentication: DNA Barcoding and Metabarcoding in Herbal Product Authentication. Phytochem. Anal. 2018, 29, 123–128. [Google Scholar] [CrossRef]
- Adaszyńska, M.; Swarcewicz, M.; Dzięcioł, M.; Dobrowolska, A. Comparison of Chemical Composition and Antibacterial Activity of Lavender Varieties from Poland. Nat. Prod. Res. 2013, 27, 1497–1501. [Google Scholar] [CrossRef]
- Quave, C.L. Antibiotics from Nature: Traditional Medicine as a Source of New Solutions for Combating Antimicrobial Resistance. In AMR Control 2016: Overcoming Global Antimicrobial Resistance; World Alliance Against Antibiotic Resistance; Emory University: Atlanta, GA, USA, 2016. [Google Scholar]
- UN. Nagoya Protocol on Access to Genetic Resources and the Fair and Equitable Sharing of Benefits Arising from Their Utilization to the Convention on Biological Diversity. Text and Annex; Nagoya Protocol; UN: Nagoya, Japan, 2011.

| Plant Sources | Class of Compound | Compound | Mechanisms | Susceptible Microorganism | References |
|---|---|---|---|---|---|
| Rauwolfia serpentine | Alkaloid | Reserpine | EP inhibitor | Staphylococcus sp., Streptococcus sp., Micrococcus sp., | [92] |
| Piper nigrum | Piperine | EP inhibitor | MRSA, Staphylococcus aureus | [93] | |
| Conessine | EP inhibitor | Pseudomonas aeruginosa | [94] | ||
| Berberine | Protein and DNA synthesis inhibitor | Escherichia coli, Candida albicans | [95] | ||
| Berberis vulgaris | Tomatidine | ATP synthetase inhibitor | Listeria, Bacillus Staphylococcus spp. | [96] | |
| Phenolic compound/polyphenols | Rhamentin | EP inhibitor | Staphylococcus aureus | [97] | |
| Camellia sinensis | Epigallocatechin gallate | Beta-ketoacyl-reductase | Escherichia coli | [98] | |
| Chebulinic acid | DNA gyrase | Mycobactrium tuberculosis | [99] | ||
| 3-p-Trans-coumaroyl-2-hydroxyquinic acid | Cell membrane damage | Staphylococcus aureus | [100] | ||
| Cedrus deodara | Apigenin | d-Alanine:d-alanine ligase | Helicobacter pylori, Escherichia coli | [101] | |
| Allium sativum | Sulfur-containing compounds | Allicin | Protein and DNA synthesis inhibitor | Staphylococcus epidermidis, Pseudomonas aeruginosa, Streptococcus agalactiae | [102] |
| Rubus ulmifolius | Ajoene | Sulphydryl-depe endent enzyme inhibitor | Cambylobacter jejuni, Streptococcus, Staphylococcus Escherichia coli | [88] | |
| Sulforaphane | Destruction of bacterial membrane, Protein and DNA synthesis inhbitor, ATP synthase inhibitor | Escherichia coli | [103] | ||
| Alyssin | Helicobacter pylori | [83] | |||
| Raphanus sativus | Allyl isothiocyanate Benzyl isothiocyanate Phenethyl isothiocyanate | Bacillus subtilis,
Staphylococcus aureus, Staphylococcus epidermidis, Enterococcus faecalis, Salmonella typhimurium, Enterobacter cloacae, Escherichia coli | [104] | ||
| Ferulago campestris | Coumarin | Aegelinol | DNA gyrase inhibitor | Salmonella enterica serovar Typhi,
Enterobacter aerogenes, Enterobacter cloacae, Staphylococcus aureus | [105] |
| Agasyllin | DNA gyrase inhibitor | Salmonella enterica serovar Typhi,
Enterobacter aerogenes, Enterobacter cloacae, Staphylococcus aureus, Helicobacter pylori | [105] | ||
| Prangos hulusii | 4′-senecioiloxyosthol | DNA gyrase inhibitor | Bacillus subtilis | [106] | |
| Osthole | DNA gyrase inhibitor | Bacillus subtilis, Staphylococcus aureus, Klebsiella pneumoniae, MRSA | [106,107] | ||
| Mesua ferrea | Bergamottin epoxide | EB inhibitor | MRSA | [108] | |
| Thymus vulgaris | Terpene | Furnesol | Cell membrane disturbance | Staphylococcus aureus | [109] |
| (4R)-carbone | Cell membrane disturbance | Cambylobacter jejuni, Enterococcus faecalis, Escherichia coli | [110] | ||
| Thymol | Cell membrane (H+)-ATPase inhibition, Cell membrane disturbance, EP inhibitor | Candida albicans,
Candida glabrata, Candida crusei, Escherichia coli, Staphylococcus aureus, Pseudomonas aeruginosa, Aspergillus niger, Aspergillus flavus, Fusarium oxysporum | [111] | ||
| Carvacrol | Cell membrane disturbance, EP inhibitor | Escherichia coli,
Enterobacter aerogenes, Staphylococcus aureus, Pseudomonas aeruginosa, Salmonella typhimarium. Aspergillus niger, Aspergillus fumigatus, Epadosporium spp., Rhizopus oryzae | [112] | ||
| Cinnamaldehyde | Cell membrane disturbance | Helicobacter pylori | [113] |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2021 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Vaou, N.; Stavropoulou, E.; Voidarou, C.; Tsigalou, C.; Bezirtzoglou, E. Towards Advances in Medicinal Plant Antimicrobial Activity: A Review Study on Challenges and Future Perspectives. Microorganisms 2021, 9, 2041. https://doi.org/10.3390/microorganisms9102041
Vaou N, Stavropoulou E, Voidarou C, Tsigalou C, Bezirtzoglou E. Towards Advances in Medicinal Plant Antimicrobial Activity: A Review Study on Challenges and Future Perspectives. Microorganisms. 2021; 9(10):2041. https://doi.org/10.3390/microorganisms9102041
Chicago/Turabian StyleVaou, Natalia, Elisavet Stavropoulou, Chrysa Voidarou, Christina Tsigalou, and Eugenia Bezirtzoglou. 2021. "Towards Advances in Medicinal Plant Antimicrobial Activity: A Review Study on Challenges and Future Perspectives" Microorganisms 9, no. 10: 2041. https://doi.org/10.3390/microorganisms9102041
APA StyleVaou, N., Stavropoulou, E., Voidarou, C., Tsigalou, C., & Bezirtzoglou, E. (2021). Towards Advances in Medicinal Plant Antimicrobial Activity: A Review Study on Challenges and Future Perspectives. Microorganisms, 9(10), 2041. https://doi.org/10.3390/microorganisms9102041








