Toxoplasma gondii Antibodies in Raw Milk and Sera of Cows in China
Abstract
1. Introduction
2. Results
3. Discussion
4. Materials and Methods
4.1. Ethical Certificate
4.2. Sampling
4.3. Serologic Examination
4.4. Statistical Analysis
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Conflicts of Interest
References
- Dubey, J.P. Toxoplasmosis of Animals and Humans; CRC Press: Boca Raton, FL, USA, 2010. [Google Scholar]
- Huang, J.F.; Wu, Y.L.; Wang, M.F.; Zhu, Y.Y.; Lin, S. Lower vitamin D levels are associated with higher seroprevalence of Toxoplasma gondii—A US national survey study. Zoonoses 2022, 2, 25. [Google Scholar] [CrossRef]
- Li, M.Y.; Gao, X.N.; Ma, J.Y.; Elsheikha, H.M.; Cong, W. A systematic review, meta-analysis and meta-regression of the global prevalence of Toxoplasma gondii infection in wild marine mammals and associations with epidemiological variables. Transbound. Emerg. Dis. 2022, 1–18. [Google Scholar] [CrossRef]
- Khamsian, E.M.; Hajimohammadi, B.; Eslami, G.; Fallahzadeh, M.H.; Hosseini, S.S. Toxoplasma gondii in milk of human and goat from the Desert Area in central Iran. Iran. J. Parasitol. 2021, 16, 601–609. [Google Scholar]
- Liu, Y.M.; Wang, L.; Wang, H.Y.; Li, C.H.; Jiang, Y.H.; Sun, W.W. First detection of anti-Toxoplasma gondii antibodies in domestic goat’s serum and milk during lactation in China. Microb. Pathog. 2021, 161 Pt B, 105268. [Google Scholar] [CrossRef]
- Luptakova, L.; Benova, K.; Rencko, A.; Petrovova, E. DNA detection of Toxoplasma gondii in sheep milk and blood samples in relation to phase of infection. Vet. Parasitol. 2015, 208, 250–253. [Google Scholar] [CrossRef]
- Chen, L.; Zhao, Z.J.; Meng, Q.F. Detection of specific IgG-antibodies against Toxoplasma gondii in the serum and milk of domestic donkeys during lactation in China: A potential public health concern. Front. Cell. Infect. Microbiol. 2021, 11, 760400. [Google Scholar] [CrossRef]
- Koethe, M.; Schade, C.; Fehlhaber, K.; Ludewig, M. Survival of Toxoplasma gondii tachyzoites in simulated gastric fluid and cow’s milk. Vet. Parasitol. 2017, 233, 111–114. [Google Scholar] [CrossRef]
- Dehkordi, F.S.; Borujeni, M.R.; Rahimi, E.; Abdizadeh, R. Detection of Toxoplasma gondii in raw caprine, ovine, buffalo, bovine, and camel milk using cell cultivation, cat bioassay, capture ELISA, and PCR methods in Iran. Foodborne Pathog. Dis. 2013, 10, 120–125. [Google Scholar] [CrossRef]
- Iacobucci, E.; Taus, N.S.; Ueti, M.W.; Sukhbaatar, L.; Bastsukh, Z.; Papageorgiou, S.; Fritz, H. Detection and genotypic characterization of Toxoplasma gondii DNA within the milk of Mongolian livestock. Parasitol. Res. 2019, 118, 2005–2008. [Google Scholar] [CrossRef]
- Powell, C.C.; Brewer, M.; Lappin, M.R. Detection of Toxoplasma gondii in the milk of experimentally infected lactating cats. Vet. Parasitol. 2001, 102, 29–33. [Google Scholar] [CrossRef]
- EFSA. Surveillance and monitoring of Toxoplasma in humans, food and animals: Scientific opinion of the Panel on Biological Hazards. EFSA J. 2007, 583, 1–64. [Google Scholar]
- Sacks, J.J.; Roberto, R.R.; Brooks, N.F. Toxoplasmosis infection associated with raw goat’s milk. JAMA 1982, 248, 1728–1732. [Google Scholar] [CrossRef]
- Alvarado-Esquivel, C.; Liesenfeld, O.; Torres-Castorena, A.; Estrada-Martinez, S.; Urbina-Alvarez, J.D.; Ramos-de la Rocha, M.; Marquez-Conde, J.A.; Dubey, J.P. Seroepidemiology of Toxoplasma gondii infection in patients with vision and hearing impairments, cancer, HIV, or undergoing hemodialysis in Durango, Mexico. J. Parasitol. 2010, 96, 505–508. [Google Scholar] [CrossRef]
- da Silva, M.G.; Vinaud, M.C.; de Castro, A.M. Epidemiological factors associated with seropositivity for toxoplasmosis in pregnant women from Gurupi, State of Tocantins, Brazil. Rev. Soc. Bras. Med. Trop. 2014, 47, 469–475. [Google Scholar] [CrossRef]
- Bai, Z.; Lee, M.R.F.; Ma, L.; Ledgard, S.; Oenema, O.; Velthof, G.L.; Ma, W.; Guo, M.; Zhao, Z.; Wei, S.; et al. Global environmental costs of China’s thirst for milk. Glob. Chang. Biol. 2018, 24, 2198–2211. [Google Scholar] [CrossRef]
- Moura, F.L.; Amendoeira, M.R.; Bastos, O.M.; Mattos, D.P.; Fonseca, A.B.; Nicolau, J.L.; Neves, L.B.; Millar, P.R. Prevalence and risk factors for Toxoplasma gondii infection among pregnant and postpartum women attended at public healthcare facilities in the city of Niteroi, state of Rio de Janeiro, Brazil. Rev. Soc. Bras. Med. Trop. 2013, 46, 200–207. [Google Scholar] [CrossRef]
- Elsheikha, H.M.; Azab, M.S.; Abousamra, N.K.; Rahbar, M.H.; Elghannam, D.M.; Raafat, D. Seroprevalence of and risk factors for Toxoplasma gondii antibodies among asymptomatic blood donors in Egypt. Parasitol. Res. 2009, 104, 1471–1476. [Google Scholar] [CrossRef]
- Heukelbach, J.; Meyer-Cirkel, V.; Moura, R.C.; Gomide, M.; Queiroz, J.A.; Saweljew, P.; Liesenfeld, O. Waterborne toxoplasmosis, northeastern Brazil. Emerg. Infect. Dis. 2007, 13, 287–289. [Google Scholar] [CrossRef]
- Cisak, E.; Zając, V.; Sroka, J.; Sawczyn, A.; Kloc, A.; Dutkiewicz, J.; Wójcik-Fatla, A. Presence of pathogenic Rickettsiae and protozoan in samples of raw milk from cows, goats, and sheep. Foodborne Pathog. Dis. 2017, 14, 189–194. [Google Scholar] [CrossRef]
- Razmi, G.; Barati, M. Prevalence of Neospora caninum and Toxoplasma gondii antibodies in bulk milk of dairy cattle, Mashhad, Iran. Arch. Razi Inst. 2017, 72, 265–269. [Google Scholar]
- Gharekhani, J.; Yakhchali, M.; Afshari, A.; Adabi, M. Herd-level contamination of Neospora caninum, Toxoplasma gondii and Brucella in milk of Iranian dairy farms. Food Microbiol. 2021, 100, 103873. [Google Scholar] [CrossRef]
- Gong, Q.L.; Li, J.; Li, D.; Tian, T.; Leng, X.; Li, J.M.; Shi, K.; Zhang, N.Z.; Du, R.; Zhao, Q. Seroprevalence of Toxoplasma gondii in cattle in China from 2010 to 2019: A systematic review and meta-analysis. Acta Trop. 2020, 211, 105439. [Google Scholar] [CrossRef]
- Nayeri, T.; Sarvi, S.; Moosazadeh, M.; Daryani, A. Global prevalence of Toxoplasma gondii infection in the aborted fetuses and ruminants that had an abortion: A systematic review and meta-analysis. Vet. Parasitol. 2021, 290, 109370. [Google Scholar] [CrossRef]
- Sah, R.P.; Dey, A.R.; Rahman, A.K.M.A.; Alam, M.Z.; Talukder, M.H. Molecular detection of Toxoplasma gondii from aborted fetuses of sheep, goats and cattle in Bangladesh. Vet. Parasitol. Reg. Stud. Rep. 2019, 18, 100347. [Google Scholar] [CrossRef]
- Almeria, S.; Dubey, J.P. Foodborne transmission of Toxoplasma gondii infection in the last decade. An overview. Res. Vet. Sci. 2021, 135, 371–385. [Google Scholar] [CrossRef]
- Stelzer, S.; Basso, W.; Silv’an, J.B.; Ortega-Mora, L.; Maksimov, P.; Gethmann, J.; Conrathsa, F.J.; Schares, G. Toxoplasma gondii infection and toxoplasmosis in farm animals: Risk factors and economic impact. Food Waterborne Parasitol. 2019, 15, e00037. [Google Scholar] [CrossRef]
- Dubey, J.P. Advances in the life cycle of Toxoplasma gondii. Int. J. Parasitol. 1998, 28, 1019–1024. [Google Scholar] [CrossRef]
- Wiengcharoen, J.; Thompson, R.C.; Nakthong, C.; Rattanakorn, P.; Sukthana, Y. Transplacental transmission in cattle: Is Toxoplasma gondii less potent than Neospora caninum? Parasitol. Res. 2011, 108, 1235–1241. [Google Scholar] [CrossRef]
- Esteban-Redondo, I.; Innes, E.A. Toxoplasma gondii infection in sheep and cattle. Comp. Immunol. Microbiol. Infect. Dis. 1997, 20, 191–196. [Google Scholar] [CrossRef]
- Wei, X.Y.; An, Q.; Xue, N.Y.; Chen, Y.; Chen, Y.Y.; Zhang, Y.; Zhao, Q.; Wang, C.R. Seroprevalence and risk factors of Neospora caninum infection in cattle in China from 2011 to 2020: A systematic review and meta-analysis. Prev. Vet. Med. 2022, 203, 105620. [Google Scholar] [CrossRef]
- Radon, K.; Windstetter, D.; Eckart, J.; Dressel, H.; Leitritz, L.; Reichert, J.; Schmid, M.; Praml, G.; Schosser, M.; von Mutius, E.; et al. Farming exposure in childhood, exposure to markers of infections and the development of atopy in rural subjects. Clin. Exp. Allergy 2004, 34, 1178–1183. [Google Scholar] [CrossRef] [PubMed]
- Ishag, M.Y.; Magzoub, E.; Majid, M. Detection of Toxoplasma gondii tachyzoites in the milk of experimentally infected lacting She-Camels. J. Anim. Vet. Adv. 2006, 5, 456–458. [Google Scholar]
- Hiramoto, R.M.; Mayrbaurl-Borges, M.; Galisteo, A.J., Jr.; Meireles, L.R.; Macre, M.S.; Andrade, H.F., Jr. Infectivity of cysts of the ME-49 Toxoplasma gondii strain in bovine milk and homemade cheese. Rev. Saude Publica 2001, 35, 113–118. [Google Scholar] [CrossRef] [PubMed][Green Version]
- Dubey, J.P.; Murata, F.H.A.; Cerqueira-Cézar, C.K.; Kwok, O.C.H.; Yang, Y.R. Public Health Significance of Toxoplasma gondii Infections in Cattle: 2009–2020. J. Parasitol. 2020, 106, 772–788. [Google Scholar] [CrossRef]
- Petruzzelli, A.; Amagliani, G.; Micci, E.; Foglini, M.; Di Renzo, E.; Brandi, G.; Tonucci, F. Prevalence assessment of Coxiella burnetii and verocytotoxin-producing Escherichia coli in bovine raw milk through molecular identification. Food Control 2013, 32, 532–536. [Google Scholar] [CrossRef]
- Gazzonis, A.L.; Zanzani, S.A.; Villa, L.; Manfredi, M.T. Toxoplasma gondii in naturally infected goats: Monitoring of specific IgG levels in serum and milk during lactation and parasitic DNA detection in milk. Prev. Vet. Med. 2019, 170, 104738. [Google Scholar] [CrossRef]
- Gazzonis, A.L.; Zanzani, S.A.; Stradiotto, K.; Olivieri, E.; Villa, L.; Manfredi, M.T. Toxoplasma gondii antibodies in bulk tank milk samples of caprine dairy herds. J. Parasitol. 2018, 104, 560–565. [Google Scholar] [CrossRef]
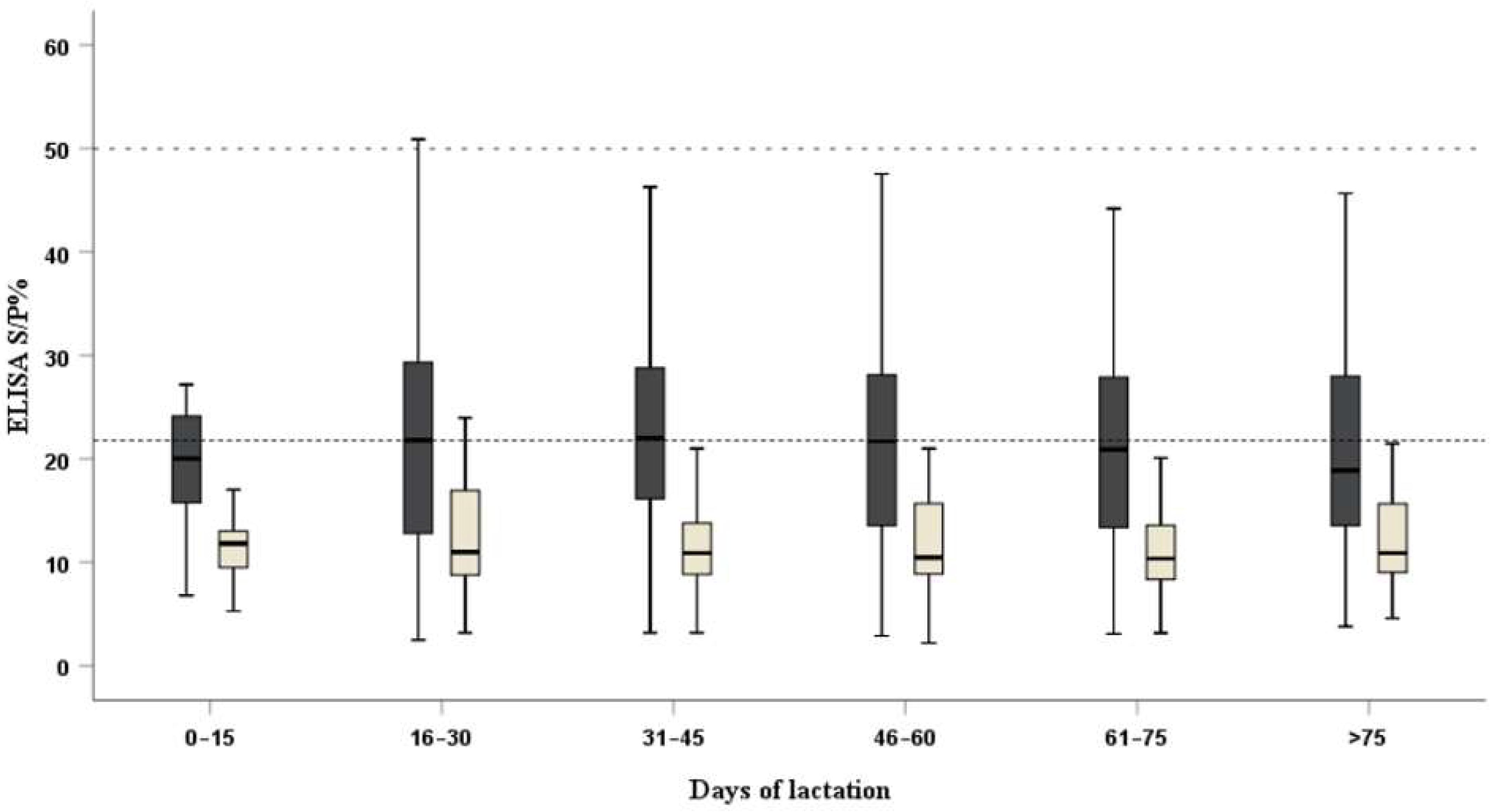

| Statistical Analysis | Days Postpartum | |||||
|---|---|---|---|---|---|---|
| 0–15 | 16–30 | 31–45 | 46–60 | 61–75 | >75 | |
| Kendall’s Tau (p-value) | 0.644 (0.000) | 0.687 (0.000) | 0.605 (0.000) | 0.598 (0.000) | 0.593 (0.000) | 0.583 (0.000) |
| Spearman’s coefficient (p-value) | 0.796 (0.000) | 0.867 (0.000) | 0.792 (0.000) | 0.772 (0.000) | 0.780 (0.000) | 0.751 (0.000) |
| Variable | Classification | Number | Serum | Milk | ||||
|---|---|---|---|---|---|---|---|---|
| Positive | Prevalence | p-Value | Positive | Prevalence | p-Value | |||
| Age (month) | ≤24 | 38 | 3 | 7.89 | 0.898 | 3 | 7.89 | 0.873 |
| 25–36 | 281 | 18 | 6.41 | 16 | 5.69 | |||
| 37–48 | 193 | 12 | 6.22 | 12 | 6.22 | |||
| 49–60 | 263 | 21 | 7.98 | 16 | 6.08 | |||
| >60 | 119 | 10 | 8.40 | 10 | 8.40 | |||
| Region | Changchun | 188 | 7 | 3.72 | 0.164 | 7 | 3.72 | 0.192 |
| Jilin | 153 | 10 | 6.54 | 9 | 5.88 | |||
| Baicheng | 142 | 9 | 6.34 | 7 | 4.93 | |||
| Shuangyashan | 93 | 6 | 6.45 | 5 | 5.38 | |||
| Daqing | 159 | 17 | 10.69 | 16 | 10.06 | |||
| Suihua | 159 | 15 | 9.43 | 13 | 8.18 | |||
| History of abortion | Yes | 144 | 16 | 11.11 | 0.045 | 15 | 10.42 | 0.030 |
| No | 750 | 48 | 6.40 | 42 | 5.60 | |||
| Days postpartum | 0–15 | 21 | 1 | 4.76 | 0.374 | 1 | 4.76 | 0.709 |
| 16–30 | 228 | 15 | 6.58 | 15 | 6.58 | |||
| 31–45 | 164 | 6 | 3.66 | 6 | 3.66 | |||
| 46–60 | 259 | 24 | 9.27 | 19 | 7.34 | |||
| 61–75 | 148 | 12 | 8.11 | 10 | 6.76 | |||
| >75 | 74 | 6 | 8.11 | 6 | 8.11 | |||
| Cat in house | Yes | 262 | 24 | 9.16 | 0.135 | 21 | 8.02 | 0.196 |
| No | 632 | 40 | 6.33 | 36 | 5.70 | |||
| Type of drinking water | Well water | 276 | 22 | 7.97 | 0.529 | 21 | 7.61 | 0.313 |
| Tap water | 618 | 42 | 6.80 | 36 | 5.83 | |||
| Type of fodder | Forage | 581 | 45 | 7.75 | 0.354 | 39 | 6.71 | 0.575 |
| Forage/commercial feed | 313 | 19 | 6.07 | 18 | 5.75 | |||
| Total | 894 | 64 | 7.16 | 57 | 6.38 | |||
| Variable | Odds Ratio (95% Confidence Internal) | p-Value |
|---|---|---|
| Age (month) (≤24 vs. >60) | 1.37 (0.35–5.32) | 0.647 |
| Age (month) (25–36 vs. >60) | 0.90 (0.40–2.02) | 0.800 |
| Age (month) (37–48 vs. >60) | 0.87 (0.36–2.12) | 0.761 |
| Age (month) (49–60 vs. >60) | 0.98 (0.44–2.17) | 0.964 |
| Region (Changchun vs. Suihua) | 0.40 (0.16–1.01) | 0.053 |
| Region (Jilin vs. Suihua) | 0.72 (0.31–1.66) | 0.442 |
| Region (Baicheng vs. Suihua) | 0.67 (0.29–1.58) | 0.360 |
| Region (Shuangyashan vs. Suihua) | 0.72 (0.27–1.93) | 0.517 |
| Region (Daqing vs. Suihua) | 1.16 (0.56–2.41) | 0.687 |
| History of abortion | 2.03 (1.11–3.72) | 0.022 |
| Days postpartum (0–15 vs. >75) | 0.58 (0.07–5.13) | 0.625 |
| Days postpartum (16–30 vs. >75) | 0.76 (0.28–2.03) | 0.577 |
| Days postpartum (30–45 vs. >75) | 0.41 (0.13–1.32) | 0.133 |
| Days postpartum (41–60 vs. >75) | 1.17 (0.43–3.00) | 0.738 |
| Days postpartum (61–75 vs. >75) | 1.06 (0.38–2.93) | 0.913 |
| Cat in house | 1.42 (0.84–2.42) | 0.193 |
| Type of drinking water | 1.16 (0.68–1.99) | 0.591 |
| Type of fodder | 1.30 (0.75–2.26) | 0.358 |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2022 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Liu, Y.-M.; Zhang, Y.-Y.; Wang, L.; Wang, H.-Y.; Li, C.-H.; Jiang, Y.-H.; Sun, W.-W. Toxoplasma gondii Antibodies in Raw Milk and Sera of Cows in China. Pathogens 2022, 11, 1079. https://doi.org/10.3390/pathogens11101079
Liu Y-M, Zhang Y-Y, Wang L, Wang H-Y, Li C-H, Jiang Y-H, Sun W-W. Toxoplasma gondii Antibodies in Raw Milk and Sera of Cows in China. Pathogens. 2022; 11(10):1079. https://doi.org/10.3390/pathogens11101079
Chicago/Turabian StyleLiu, Yu-Min, Yang-Yang Zhang, Lu Wang, Hai-Yang Wang, Chun-Hua Li, Yu-Hang Jiang, and Wu-Wen Sun. 2022. "Toxoplasma gondii Antibodies in Raw Milk and Sera of Cows in China" Pathogens 11, no. 10: 1079. https://doi.org/10.3390/pathogens11101079
APA StyleLiu, Y.-M., Zhang, Y.-Y., Wang, L., Wang, H.-Y., Li, C.-H., Jiang, Y.-H., & Sun, W.-W. (2022). Toxoplasma gondii Antibodies in Raw Milk and Sera of Cows in China. Pathogens, 11(10), 1079. https://doi.org/10.3390/pathogens11101079








