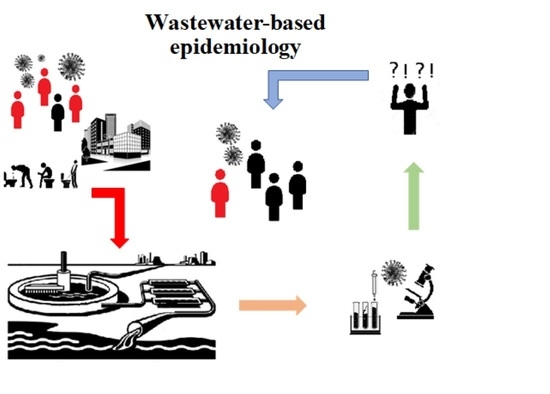
Wastewater Based Epidemiology Perspective as a Faster Protocol for Detecting Coronavirus RNA in Human Populations: A Review with Specific Reference to SARS-CoV-2 Virus
Abstract
:1. Background of Application of Wastewater Based Epidemiology
2. Cutting-Edge of Wastewater Based Epidemiology Concept
3. Actual Status of Wastewater Contamination with SARS-CoV-2
4. Molecular Detection of SARS-CoV-2 in Wastewater and Treatment Plant Sludge
4.1. Sampling
4.2. Storage
4.3. Inactivation of SARS-CoV-2
4.4. Preconditioning
4.5. Concentration
4.6. Extraction
4.7. Detection and Quantification
5. Conclusions
- Recent data proved that SARS-CoV-2 RNA can be detected in human feces from a few days to a week before the onset of symptoms. Therefore, the monitoring of SARS-CoV-2 genetic signals in wastewater samples seems to be a useful methodology for prediction of COVID-19 outbreaks. However, at the early stage of COVID-19 prevalence, its surveillance in sewage network may not be quite accurate due to the extremely low concentration of virus in wastewater.
- One liter of wastewater is like an ocean of information that can provide valuable data about the timing and prevalence of COVID-19 outbreaks in communities, especially in low-income countries with low clinical COVID-19 testing rates.
- Periodically collecting wastewater samples from sewer networks for the trace of the SARS-CoV-2 virus can be effective as a primary non-clinical warning tool for early detection.
- Considering that SARS-CoV-2 RNA has already been detected in the activated sludge, the dissociation of SARS-CoV-2 genetic material from solids/semisolids in wastewater arises urgent issue to be sought for accurate quantification. In this sense, a protocol tailored to SARS-CoV-2 is another crucial need.
- Although the sampling method is one of the most important steps of WBE SARS-CoV-2 surveillance, there is no real consensus on adequate and representative wastewater sampling technique. Then, further studies are required to find out a properly designed and well-defined sampling procedure.
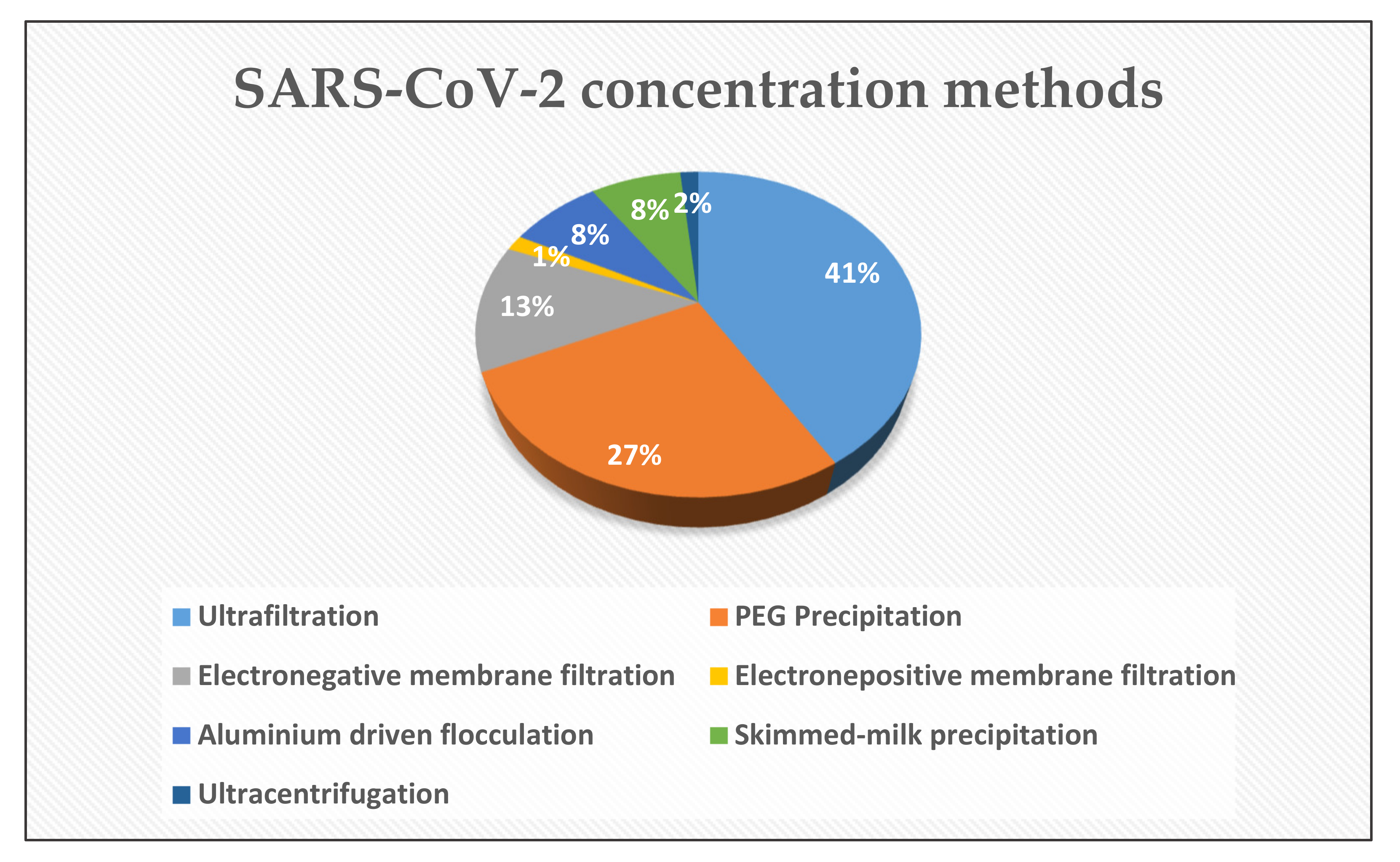
- Among the concentration techniques, CeUF, double UF, and PEG precipitation seem to be promising concentration techniques for SARS-CoV-2 RNA enrichment from wastewater/sludge after re-partitioning.
- Findings prevailed that more standardization and quality control studies covering (i) selection of appropriate sample volume, (ii) improvement of preconditioning step including the significant contribution of the solid fraction of raw wastewater, (iii) spike controls, (iv) PCR inhibitor removal, and (v) selection of suitable extraction approach must be performed to maximize the SARS-CoV-2 recovery efficiency.
- An urgent issue to be faced is the development of molecular techniques providing information on the viability of the virus in the sewage system for worker safety.
- Recent data have revealed a correlation between genetic material in wastewater and the number of clinically reported positive cases confirming that WBE surveillance could be utilized as a sensitive tool to trace the circulation of SARS-CoV-2 virus in the population. Nevertheless, an accurate mathematical model considering several factors such as wastewater characteristics, climate, and sewage system structure, among others, should be developed.
- WBE for SARS-CoV-2 is a fast and effective surveillance system with the clearest potential to avoid and control the infectious disease outbreak.
Author Contributions
Funding
Data Availability Statement
Acknowledgments
Conflicts of Interest
References
- Sims, N.; Kasprzyk-Hordern, B. Future perspectives of wastewater-based epidemiology: Monitoring infectious disease spread and resistance to the community level. Environ. Int. 2020, 139, 105689. [Google Scholar] [CrossRef] [PubMed]
- Daughton, C. The international imperative to rapidly and inexpensively monitor community-wide Covid-19 infection status and trends. Sci. Total. Environ. 2020, 726, 138149. [Google Scholar] [CrossRef] [PubMed]
- Daughton, C.G. Wastewater surveillance for population-wide Covid-19: The present and future. Sci. Total. Environ. 2020, 139631. [Google Scholar] [CrossRef] [PubMed]
- Andrés-Costa, M.J.; Andreu, V.; Pico, Y. Liquid chromatography–mass spectrometry as a tool for wastewater-based epidemiology: Assessing new psychoactive substances and other human biomarkers. TrAC Trends Anal. Chem. 2017, 94, 21–38. [Google Scholar] [CrossRef]
- Hellmér, M.; Paxéus, N.; Magnius, L.; Enache, L.; Arnholm, B.; Johansson, A.; Bergström, T.; Norder, H. Detection of pathogenic viruses in sewage provided early warnings of hepatitis A virus and norovirus outbreaks. Appl. Environ. Microbiol. 2014, 80, 6771–6781. [Google Scholar] [CrossRef] [Green Version]
- Sinclair, R.G.; Choi, C.Y.; Riley, M.R.; Gerba, C.P. Pathogen surveillance through monitoring of sewer systems. Adv. Appl. Microbiol. 2008, 65, 249. [Google Scholar]
- Weidhaas, J.; Aanderud, Z.T.; Roper, D.K.; VanDerslice, J.; Gaddis, E.B.; Ostermiller, J.; Hoffman, K.; Jamal, R.; Heck, P.; Zhang, Y. Correlation of SARS-CoV-2 RNA in wastewater with COVID-19 disease burden in sewersheds. Sci. Total. Environ. 2021, 775, 145790. [Google Scholar] [CrossRef]
- Hamouda, M.; Mustafa, F.; Maraqa, M.; Rizvi, T.; Hassan, A.A. Wastewater surveillance for SARS-CoV-2: Lessons learnt from recent studies to define future applications. Sci. Total. Environ. 2020, 143493. [Google Scholar] [CrossRef]
- Mao, K.; Zhang, H.; Yang, Z. Can a paper-based device trace COVID-19 sources with wastewater-based epidemiology? Environ. Sci. Technol. 2020, 54, 3733–3735. [Google Scholar] [CrossRef]
- Barcelo, D. An environmental and health perspective for COVID-19 outbreak: Meteorology and air quality influence, sewage epidemiology indicator, hospitals disinfection, drug therapies and recommendations. J. Environ. Chem. Eng. 2020, 8, 104006. [Google Scholar] [CrossRef]
- Miura, F.; Kitajima, M.; Omori, R. Duration of SARS-CoV-2 viral shedding in faeces as a parameter for wastewater-based epidemiology: Re-analysis of patient data using a shedding dynamics model. Sci. Total. Environ. 2021, 769, 144549. [Google Scholar] [CrossRef]
- Aguiar-Oliveira, M.d.L.; Campos, A.; Matos, A.R.; Rigotto, C.; Sotero-Martins, A.; Teixeira, P.F.; Siqueira, M.M. Wastewater-Based Epidemiology (WBE) and Viral Detection in Polluted Surface Water: A Valuable Tool for COVID-19 Surveillance—A Brief Review. Int. J. Environ. Res. Public Health 2020, 17, 9251. [Google Scholar] [CrossRef]
- Ahmed, F.; Islam, M.A.; Kumar, M.; Hossain, M.; Bhattacharya, P.; Islam, M.T.; Hossen, F.; Hossain, M.S.; Islam, M.S.; Uddin, M.M. First detection of SARS-CoV-2 genetic material in the vicinity of COVID-19 isolation Centre in Bangladesh: Variation along the sewer network. Sci. Total. Environ. 2021, 776, 145724. [Google Scholar] [CrossRef]
- Randazzo, W.; Truchado, P.; Cuevas-Ferrando, E.; Simón, P.; Allende, A.; Sánchez, G. SARS-CoV-2 RNA in wastewater anticipated COVID-19 occurrence in a low prevalence area. Water Res. 2020, 181, 115942. [Google Scholar] [CrossRef] [PubMed]
- Wang, J.; Feng, H.; Zhang, S.; Ni, Z.; Ni, L.; Chen, Y.; Zhuo, L.; Zhong, Z.; Qu, T. SARS-CoV-2 RNA detection of hospital isolation wards hygiene monitoring during the Coronavirus Disease 2019 outbreak in a Chinese hospital. Int. J. Infect. Dis. 2020, 94, 103–106. [Google Scholar] [CrossRef] [PubMed]
- World Health Organization. Water, Sanitation, Hygiene, and Waste Management for the COVID-19 Virus: Interim Guidance; World Health Organization: Geneva, Switzerland, 2020. [Google Scholar]
- Medema, G.; Heijnen, L.; Elsinga, G.; Italiaander, R.; Brouwer, A. Presence of SARS-Coronavirus-2 RNA in sewage and correlation with reported COVID-19 prevalence in the early stage of the epidemic in the Netherlands. Environ. Sci. Technol. Lett. 2020, 7, 511–516. [Google Scholar] [CrossRef]
- Annalaura, C.; Ileana, F.; Dasheng, L.; Marco, V. Making waves: Coronavirus detection, presence and persistence in the water environment: State of the art and knowledge needs for public health. Water Res. 2020, 115907. [Google Scholar]
- Ihsanullah, I.; Bilal, M.; Naushad, M. Coronavirus 2 (SARS-CoV-2) in water environments: Current status, challenges and research opportunities. J. Water Process. Eng. 2021, 39, 101735. [Google Scholar] [CrossRef]
- Kitajima, M.; Ahmed, W.; Bibby, K.; Carducci, A.; Gerba, C.P.; Hamilton, K.A.; Haramoto, E.; Rose, J.B. SARS-CoV-2 in wastewater: State of the knowledge and research needs. Sci. Total. Environ. 2020, 739, 139076. [Google Scholar] [CrossRef] [PubMed]
- La Rosa, G.; Bonadonna, L.; Lucentini, L.; Kenmoe, S.; Suffredini, E. Coronavirus in water environments: Occurrence, persistence and concentration methods-A scoping review. Water Res. 2020, 179, 115899. [Google Scholar] [CrossRef]
- Saawarn, B.; Hait, S. Occurrence, fate and removal of SARS-CoV-2 in wastewater: Current knowledge and future perspectives. J. Environ. Chem. Eng. 2020, 104870. [Google Scholar]
- Chen, C.; Kostakis, C.; Gerber, J.P.; Tscharke, B.J.; Irvine, R.J.; White, J.M. Towards finding a population biomarker for wastewater epidemiology studies. Sci. Total. Environ. 2014, 487, 621–628. [Google Scholar] [CrossRef] [PubMed]
- Lorenzo, M.; Picó, Y. Wastewater-based epidemiology: Current status and future prospects. Curr. Opin. Environ. Sci. Health 2019, 9, 77–84. [Google Scholar] [CrossRef]
- Kumar, M.; Patel, A.K.; Shah, A.V.; Raval, J.; Rajpara, N.; Joshi, M.; Joshi, C.G. First proof of the capability of wastewater surveillance for COVID-19 in India through detection of genetic material of SARS-CoV-2. Sci. Total. Environ. 2020, 746, 141326. [Google Scholar] [CrossRef]
- Barceló, D. Wastewater-Based Epidemiology to monitor COVID-19 outbreak: Present and future diagnostic methods to be in your radar. Case Stud. Chem. Environ. Eng. 2020, 2, 100042. [Google Scholar] [CrossRef]
- Collivignarelli, M.C.; Collivignarelli, C.; Miino, M.C.; Abbà, A.; Pedrazzani, R.; Bertanza, G. SARS-CoV-2 in sewer systems and connected facilities. Process. Saf. Environ. Prot. 2020, 143, 196–203. [Google Scholar] [CrossRef]
- Foladori, P.; Cutrupi, F.; Segata, N.; Manara, S.; Pinto, F.; Malpei, F.; Bruni, L.; La Rosa, G. SARS-CoV-2 from faeces to wastewater treatment: What do we know? A review. Sci. Total. Environ. 2020, 743, 140444. [Google Scholar] [CrossRef] [PubMed]
- Mao, K.; Zhang, H.; Pan, Y.; Yang, Z. Biosensors for wastewater-based epidemiology for monitoring public health. Water Res. 2020, 116787. [Google Scholar] [CrossRef]
- Wang, W.; Xu, Y.; Gao, R.; Lu, R.; Han, K.; Wu, G.; Tan, W. Detection of SARS-CoV-2 in different types of clinical specimens. JAMA 2020, 323, 1843–1844. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Wu, Y.; Guo, C.; Tang, L.; Hong, Z.; Zhou, J.; Dong, X.; Yin, H.; Xiao, Q.; Tang, Y.; Qu, X. Prolonged presence of SARS-CoV-2 viral RNA in faecal samples. Lancet Gastroenterol. Hepatol. 2020, 5, 434–435. [Google Scholar] [CrossRef]
- Zhang, T.; Cui, X.; Zhao, X.; Wang, J.; Zheng, J.; Zheng, G.; Guo, W.; Cai, C.; He, S.; Xu, Y. Detectable SARS-CoV-2 viral RNA in feces of three children during recovery period of COVID-19 pneumonia. J. Med Virol. 2020, 92, 909–914. [Google Scholar] [CrossRef] [PubMed]
- Li, X.; Zhang, S.; Shi, J.; Luby, S.P.; Jiang, G. Uncertainties in estimating SARS-CoV-2 prevalence by wastewater-based epidemiology. Chem. Eng. J. 2021, 415, 129039. [Google Scholar] [CrossRef]
- Carrillo-Reyes, J.; Barragán-Trinidad, M.; Buitrón, G. Surveillance of SARS-CoV-2 in sewage and wastewater treatment plants in Mexico. J. Water Process. Eng. 2021, 40, 101815. [Google Scholar] [CrossRef]
- Zhang, D.; Ling, H.; Huang, X.; Li, J.; Li, W.; Yi, C.; Zhang, T.; Jiang, Y.; He, Y.; Deng, S. Potential spreading risks and disinfection challenges of medical wastewater by the presence of Severe Acute Respiratory Syndrome Coronavirus 2 (SARS-CoV-2) viral RNA in septic tanks of Fangcang Hospital. Sci. Total. Environ. 2020, 741, 140445. [Google Scholar] [CrossRef] [PubMed]
- EU. Commission Recommendation (EU) 2021/472, Official Journal of the European Union. 17 March 2021. Available online: https://eur-lex.europa.eu/legal-content/EN/TXT/PDF/?uri=CELEX:32021H0472&from=EN (accessed on 1 July 2021).
- Lotfi, M.; Hamblin, M.R.; Rezaei, N. COVID-19: Transmission, prevention, and potential therapeutic opportunities. Clin. Chim. Acta 2020, 508, 254–266. [Google Scholar] [CrossRef]
- Paital, B. Nurture to nature via COVID-19, a self-regenerating environmental strategy of environment in global context. Sci. Total. Environ. 2020, 729, 139088. [Google Scholar] [CrossRef] [PubMed]
- Paital, B.; Agrawal, P.K. Air pollution by NO2 and PM2.5 explains COVID-19 infection severity by overexpression of angiotensin-converting enzyme 2 in respiratory cells: A review. Environ. Chem. Lett. 2020, 18, 1–18. [Google Scholar] [CrossRef]
- Paital, B.; Das, K.; Parida, S.K. Inter nation social lockdown versus medical care against COVID-19, a mild environmental insight with special reference to India. Sci. Total. Environ. 2020, 728, 138914. [Google Scholar] [CrossRef]
- Zhang, N.; Gong, Y.; Meng, F.; Bi, Y.; Yang, P.; Wang, F. Virus shedding patterns in nasopharyngeal and fecal specimens of COVID-19 patients. MedRxiv 2020. [Google Scholar] [CrossRef]
- Hart, O.E.; Halden, R.U. Computational analysis of SARS-CoV-2/COVID-19 surveillance by wastewater-based epidemiology locally and globally: Feasibility, economy, opportunities and challenges. Sci. Total. Environ. 2020, 730, 138875. [Google Scholar] [CrossRef]
- Ahn, D.-G.; Shin, H.-J.; Kim, M.-H.; Lee, S.; Kim, H.-S.; Myoung, J.; Kim, B.-T.; Kim, S.-J. Current status of epidemiology, diagnosis, therapeutics, and vaccines for novel coronavirus disease 2019 (COVID-19). J. Microbiol. Biotechnol. 2020, 30, 313–324. [Google Scholar] [CrossRef]
- Das, K.; Paital, B. First week of social lockdown versus medical care against COVID-19-with special reference to India. Curr. Trend Biotechnol. Pharm. 2020, 14, 190–210. [Google Scholar] [CrossRef]
- Van Doremalen, N.; Bushmaker, T.; Morris, D.H.; Holbrook, M.G.; Gamble, A.; Williamson, B.N.; Tamin, A.; Harcourt, J.L.; Thornburg, N.J.; Gerber, S.I. Aerosol and surface stability of SARS-CoV-2 as compared with SARS-CoV-1. N. Engl. J. Med. 2020, 382, 1564–1567. [Google Scholar] [CrossRef]
- Rooney, C.M.; Moura, I.B.; Wilcox, M.H. Tracking COVID-19 via sewage. Curr. Opin. Gastroenterol. 2021, 37, 4–8. [Google Scholar] [CrossRef] [PubMed]
- Saguti, F.; Magnil, E.; Enache, L.; Churqui, M.P.; Johansson, A.; Lumley, D.; Davidsson, F.; Dotevall, L.; Mattsson, A.; Trybala, E. Surveillance of wastewater revealed peaks of SARS-CoV-2 preceding those of hospitalized patients with COVID-19. Water Res. 2021, 189, 116620. [Google Scholar] [CrossRef] [PubMed]
- Urban, R.C.; Nakada, L.Y.K. COVID-19 pandemic: Solid waste and environmental impacts in Brazil. Sci. Total. Environ. 2021, 755, 142471. [Google Scholar] [CrossRef]
- Westhaus, S.; Weber, F.-A.; Schiwy, S.; Linnemann, V.; Brinkmann, M.; Widera, M.; Greve, C.; Janke, A.; Hollert, H.; Wintgens, T. Detection of SARS-CoV-2 in raw and treated wastewater in Germany–suitability for COVID-19 surveillance and potential transmission risks. Sci. Total. Environ. 2021, 751, 141750. [Google Scholar] [CrossRef]
- Das, K.; Behera, T.R.; Paital, B. Heat Shock Protein, Corona Virus COVID-19. In Outbreak Challenges in Indian Migrant Pregnant and Lactating Mothers: Learnt Lesson Demands Hierarchical Strategy for Such Future Situation; Kaur, P., Asea, A., Eds.; Springer: New York, NY, USA, 2021. [Google Scholar]
- Paital, B.; Das, K.; Behera, T.R. Social lockdown and ecological intervention for the prevention of the community spread of COVID-19. Cancer Res. Stat. Treat. 2020, 3, 667. [Google Scholar]
- Al Huraimel, K.; Alhosani, M.; Kunhabdulla, S.; Stietiya, M.H. SARS-CoV-2 in the environment: Modes of transmission, early detection and potential role of pollutions. Sci. Total. Environ. 2020, 140946. [Google Scholar] [CrossRef]
- Nicastri, E.; D’Abramo, A.; Faggioni, G.; De Santis, R.; Mariano, A.; Lepore, L.; Molinari, F.; Petralito, G.; Fillo, S.; Munzi, D. Coronavirus disease (COVID-19) in a paucisymptomatic patient: Epidemiological and clinical challenge in settings with limited community transmission, Italy, February 2020. Eurosurveillance 2020, 25, 2000230. [Google Scholar] [CrossRef] [Green Version]
- Urban, R.C.; Nakada, L.Y.K. GIS-based spatial modelling of COVID-19 death incidence in São Paulo, Brazil. Environ. Urban. 2020, 33, 229–238. [Google Scholar] [CrossRef]
- Fuschi, C.; Pu, H.; Negri, M.; Colwell, R.; Chen, J. Wastewater-Based Epidemiology for Managing the COVID-19 Pandemic. ACS Est. Water 2021. [Google Scholar] [CrossRef]
- Rimoldi, S.G.; Stefani, F.; Gigantiello, A.; Polesello, S.; Comandatore, F.; Mileto, D.; Maresca, M.; Longobardi, C.; Mancon, A.; Romeri, F. Presence and infectivity of SARS-CoV-2 virus in wastewaters and rivers. Sci. Total. Environ. 2020, 744, 140911. [Google Scholar] [CrossRef]
- Döhla, M.; Wilbring, G.; Schulte, B.; Kümmerer, B.M.; Diegmann, C.; Sib, E.; Richter, E.; Haag, A.; Engelhart, S.; Eis-Hübinger, A.M. SARS-CoV-2 in environmental samples of quarantined households. medRxiv 2020. [Google Scholar] [CrossRef]
- La Rosa, G.; Mancini, P.; Ferraro, G.B.; Veneri, C.; Iaconelli, M.; Bonadonna, L.; Lucentini, L.; Suffredini, E. SARS-CoV-2 has been circulating in northern Italy since December 2019: Evidence from environmental monitoring. Sci. Total. Environ. 2021, 750, 141711. [Google Scholar] [CrossRef] [PubMed]
- Chavarria-Miró, G.; Anfruns-Estrada, E.; Guix, S.; Paraira, M.; Galofré, B.; Sáanchez, G.; Pintó, R.; Bosch, A. Sentinel surveillance of SARS-CoV-2 in wastewater anticipates the occurrence of COVID-19 cases. MedRxiv 2020. [Google Scholar] [CrossRef]
- Or, I.B.; Yaniv, K.; Shagan, M.; Ozer, E.; Erster, O.; Mendelson, E.; Mannasse, B.; Shirazi, R.; Kramarsky-Winter, E.; Nir, O. Regressing SARS-CoV-2 sewage measurements onto COVID-19 burden in the population: A proof-of-concept for quantitative environmental surveillance. MedRxiv 2020. [Google Scholar] [CrossRef]
- Wurtzer, S.; Marechal, V.; Mouchel, J.; Maday, Y.; Teyssou, R.; Richard, E.; Almayrac, J.; Moulin, L. Evaluation of lockdown effect on SARS-CoV-2 dynamics through viral genome quantification in waste water, Greater Paris, France, 5 March to 23 April 2020. Eurosurveillance 2020, 25, 2000776. [Google Scholar] [CrossRef]
- Wu, F.; Zhang, J.; Xiao, A.; Gu, X.; Lee, W.L.; Armas, F.; Kauffman, K.; Hanage, W.; Matus, M.; Ghaeli, N. SARS-CoV-2 titers in wastewater are higher than expected from clinically confirmed cases. Msystems 2020, 5, 9. [Google Scholar] [CrossRef] [PubMed]
- Sherchan, S.P.; Shahin, S.; Ward, L.M.; Tandukar, S.; Aw, T.G.; Schmitz, B.; Ahmed, W.; Kitajima, M. First detection of SARS-CoV-2 RNA in wastewater in North America: A study in Louisiana, USA. Sci. Total. Environ. 2020, 743, 140621. [Google Scholar] [CrossRef] [PubMed]
- D’Aoust, P.M.; Mercier, E.; Montpetit, D.; Jia, J.-J.; Alexandrov, I.; Neault, N.; Baig, A.T.; Mayne, J.; Zhang, X.; Alain, T. Quantitative analysis of SARS-CoV-2 RNA from wastewater solids in communities with low COVID-19 incidence and prevalence. Water Res. 2021, 188, 116560. [Google Scholar] [CrossRef] [PubMed]
- La Rosa, G.; Iaconelli, M.; Mancini, P.; Ferraro, G.B.; Veneri, C.; Bonadonna, L.; Lucentini, L.; Suffredini, E. First detection of SARS-CoV-2 in untreated wastewaters in Italy. Sci. Total. Environ. 2020, 736, 139652. [Google Scholar] [CrossRef]
- Kocamemi, B.A.; Kurt, H.; Hacioglu, S.; Yarali, C.; Saatci, A.M.; Pakdemirli, B. First data-set on SARS-CoV-2 detection for Istanbul wastewaters in Turkey. MedRxiv 2020. [Google Scholar] [CrossRef]
- Mlejnkova, H.; Sovova, K.; Vasickova, P.; Ocenaskova, V.; Jasikova, L.; Juranova, E. Preliminary study of Sars-Cov-2 occurrence in wastewater in the Czech Republic. Int. J. Environ. Res. Public Health 2020, 17, 5508. [Google Scholar] [CrossRef]
- Gonçalves, J.; Koritnik, T.; Mioč, V.; Trkov, M.; Bolješič, M.; Berginc, N.; Prosenc, K.; Kotar, T.; Paragi, M. Detection of SARS-CoV-2 RNA in hospital wastewater from a low COVID-19 disease prevalence area. Sci. Total. 2021, 755, 143226. [Google Scholar] [CrossRef] [PubMed]
- O’Brien, E.; Xagoraraki, I. A water-focused one-health approach for early detection and prevention of viral outbreaks. One Heal. 2019, 7, 100094. [Google Scholar] [CrossRef] [PubMed]
- Prado, T.; Fumian, T.M.; Mannarino, C.F.; Maranhão, A.G.; Siqueira, M.M.; Miagostovich, M.P. Preliminary results of SARS-CoV-2 detection in sewerage system in Niterói municipality, Rio de Janeiro, Brazil. Memórias Do Inst. Oswaldo Cruz 2020, 115. [Google Scholar] [CrossRef]
- Haramoto, E.; Malla, B.; Thakali, O.; Kitajima, M. First environmental surveillance for the presence of SARS-CoV-2 RNA in wastewater and river water in Japan. Sci. Total. Environ. 2020, 737, 140405. [Google Scholar] [CrossRef]
- Guerrero-Latorre, L.; Ballesteros, I.; Villacrés-Granda, I.; Granda, M.G.; Freire-Paspuel, B.; Ríos-Touma, B. SARS-CoV-2 in river water: Implications in low sanitation countries. Sci. Total. Environ. 2020, 743, 140832. [Google Scholar] [CrossRef]
- Iglesias, N.G.; Gebhard, L.G.; Carballeda, J.M.; Aiello, I.; Recalde, E.; Terny, G.; Ambrosolio, S.; L’Arco, G.; Konfino, J.; Brardinelli, J.I. SARS-CoV-2 surveillance in untreated wastewater: First detection in a low-resource community in Buenos Aires, Argentina. medRxiv 2020. [Google Scholar] [CrossRef]
- Ampuero, M.; Valenzuela, S.; Valiente-Echeverria, F.; Soto-Rifo, R.; Barriga, G.P.; Chnaiderman, J.; Rojas, C.; Guajardo-Leiva, S.; Diez, B.; Gaggero, A. SARS-CoV-2 Detection in Sewage in Santiago, Chile-Preliminary results. MedRxiv 2020. [Google Scholar] [CrossRef]
- Khan, R.; Saxena, A.; Shukla, S.; Sekar, S.; Goel, P. Effect of COVID-19 lockdown on the water quality index of River Gomti, India, with potential hazard of faecal-oral transmission. Environ. Sci. Pollut. Res. 2021, 28, 33021–33029. [Google Scholar] [CrossRef]
- Baldovin, T.; Amoruso, I.; Fonzo, M.; Buja, A.; Baldo, V.; Cocchio, S.; Bertoncello, C. SARS-CoV-2 RNA detection and persistence in wastewater samples: An experimental network for COVID-19 environmental surveillance in Padua, Veneto Region (NE Italy). Sci. Total. Environ. 2021, 760, 143329. [Google Scholar] [CrossRef] [PubMed]
- Hokajärvi, A.-M.; Rytkönen, A.; Tiwari, A.; Kauppinen, A.; Oikarinen, S.; Lehto, K.-M.; Kankaanpää, A.; Gunnar, T.; Al-Hello, H.; Blomqvist, S. The detection and stability of the SARS-CoV-2 RNA biomarkers in wastewater influent in Helsinki, Finland. Sci. Total. Environ. 2021, 770, 145274. [Google Scholar] [CrossRef] [PubMed]
- Sharif, S.; Ikram, A.; Khurshid, A.; Salman, M.; Mehmood, N.; Arshad, Y.; Ahmad, J.; Angez, M.; Alam, M.M.; Rehman, L. Detection of SARS-Coronavirus-2 in wastewater, using the existing environmental surveillance network: An epidemiological gateway to an early warning for COVID-19 in communities. MedRxiv 2020. [Google Scholar] [CrossRef]
- Ahmed, W.; Tscharke, B.; Bertsch, P.M.; Bibby, K.; Bivins, A.; Choi, P.; Clarke, L.; Dwyer, J.; Edson, J.; Nguyen, T.M.H. SARS-CoV-2 RNA monitoring in wastewater as a potential early warning system for COVID-19 transmission in the community: A temporal case study. Sci. Total. Environ. 2021, 761, 144216. [Google Scholar] [CrossRef]
- Johnson, R.; Muller, C.; Ghoor, S.; Louw, J.; Archer, E.; Surujlal-Naicker, S.; Berkowitz, N.; Volschenk, M.; Bröcker, L.; Wolfaardt, G. Qualitative and quantitative detection of SARS-CoV-2 RNA in untreated wastewater in Western Cape Province, South Africa. South Afr. Med. J. 2021. [Google Scholar] [CrossRef]
- Mousazadeh, M.; Paital, B.; Naghdali, Z.; Mortezania, Z.; Hashemi, M.; Niaragh, E.K.; Aghababaei, M.; Ghorbankhani, M.; Lichtfouse, E.; Sillanpää, M. Positive environmental effects of the coronavirus 2020 episode: A review. Environ. Dev. Sustain. 2021, 23, 12738–12760. [Google Scholar] [CrossRef]
- Ahmed, W.; Angel, N.; Edson, J.; Bibby, K.; Bivins, A.; O’Brien, J.W.; Choi, P.M.; Kitajima, M.; Simpson, S.L.; Li, J. First confirmed detection of SARS-CoV-2 in untreated wastewater in Australia: A proof of concept for the wastewater surveillance of COVID-19 in the community. Sci. Total. Environ. 2020, 728, 138764. [Google Scholar] [CrossRef]
- Ahmed, W.; Bertsch, P.M.; Bivins, A.; Bibby, K.; Farkas, K.; Gathercole, A.; Haramoto, E.; Gyawali, P.; Korajkic, A.; McMinn, B.R. Comparison of virus concentration methods for the RT-qPCR-based recovery of murine hepatitis virus, a surrogate for SARS-CoV-2 from untreated wastewater. Sci. Total. Environ. 2020, 739, 139960. [Google Scholar] [CrossRef]
- Jafferali, M.H.; Khatami, K.; Atasoy, M.; Birgersson, M.; Williams, C.; Cetecioglu, Z. Benchmarking virus concentration methods for quantification of SARS-CoV-2 in raw wastewater. Sci. Total. Environ. 2021, 755, 142939. [Google Scholar] [CrossRef]
- Kitamura, K.; Sadamasu, K.; Muramatsu, M.; Yoshida, H. Efficient detection of SARS-CoV-2 RNA in the solid fraction of wastewater. Sci. Total. Environ. 2021, 763, 144587. [Google Scholar] [CrossRef]
- Hasan, S.W.; Ibrahim, Y.; Daou, M.; Kannout, H.; Jan, N.; Lopes, A.; Alsafar, H.; Yousef, A.F. Detection and quantification of SARS-CoV-2 RNA in wastewater and treated effluents: Surveillance of COVID-19 epidemic in the United Arab Emirates. Sci. Total. Environ. 2021, 764, 142929. [Google Scholar] [CrossRef] [PubMed]
- Bertrand, I.; Challant, J.; Jeulin, H.; Hartard, C.; Mathieu, L.; Lopez, S.; Obépine, S.I.G.; Schvoerer, E.; Courtois, S.; Gantzer, C. Epidemiological surveillance of SARS-CoV-2 by genome quantification in wastewater applied to a city in the northeast of France: Comparison of ultrafiltration-and protein precipitation-based methods. Int. J. Hyg. Environ. Health 2021, 233, 113692. [Google Scholar] [CrossRef] [PubMed]
- Torii, S.; Furumai, H.; Katayama, H. Applicability of polyethylene glycol precipitation followed by acid guanidinium thiocyanate-phenol-chloroform extraction for the detection of SARS-CoV-2 RNA from municipal wastewater. Sci. Total. Environ. 2021, 756, 143067. [Google Scholar] [CrossRef]
- Kumar, M.; Kuroda, K.; Patel, A.K.; Patel, N.; Bhattacharya, P.; Joshi, M.; Joshi, C.G. Decay of SARS-CoV-2 RNA along the wastewater treatment outfitted with Upflow Anaerobic Sludge Blanket (UASB) system evaluated through two sample concentration techniques. Sci. Total. Environ. 2021, 754, 142329. [Google Scholar] [CrossRef] [PubMed]
- Balboa, S.; Mauricio-Iglesias, M.; Rodríguez, S.; Martínez-Lamas, L.; Vasallo, F.J.; Regueiro, B.; Lema, J.M. The fate of SARS-CoV-2 in wastewater treatment plants points out the sludge line as a suitable spot for incidence monitoring. medRxiv 2020. [Google Scholar] [CrossRef]
- Martin, J.; Klapsa, D.; Wilton, T.; Zambon, M.; Bentley, E.; Bujaki, E.; Fritzsche, M.; Mate, R.; Majumdar, M. Tracking SARS-CoV-2 in sewage: Evidence of changes in virus variant predominance during COVID-19 pandemic. Viruses 2020, 12, 1144. [Google Scholar] [CrossRef] [PubMed]
- Jahn, K.; Dreifuss, D.; Topolsky, I.; Kull, A.; Ganesanandamoorthy, P.; Fernandez-Cassi, X.; Bänziger, C.; Stachler, E.; Fuhrmann, L.; Jablonski, K.P. Detection of SARS-CoV-2 variants in Switzerland by genomic analysis of wastewater samples. medRxiv 2021. [Google Scholar] [CrossRef]
- Forés, E.; Bofill-Mas, S.; Itarte, M.; Martínez-Puchol, S.; Hundesa, A.; Calvo, M.; Borrego, C.M.; Corominas, L.; Girones, R.; Rusiñol, M. Evaluation of two rapid ultrafiltration-based methods for SARS-CoV-2 concentration from wastewater. Sci. Total. Environ. 2021, 768, 144786. [Google Scholar] [CrossRef]
- Thurston-Enriquez, J.A.; Haas, C.N.; Jacangelo, J.; Riley, K.; Gerba, C.P. Inactivation of feline calicivirus and adenovirus type 40 by UV radiation. Appl. Environ. Microbiol. 2003, 69, 577–582. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Gerrity, D.; Papp, K.; Stoker, M.; Sims, A.; Frehner, W. Early-pandemic wastewater surveillance of SARS-CoV-2 in Southern Nevada: Methodology, occurrence, and incidence/prevalence considerations. Water Res. 2021, 10, 100086. [Google Scholar]
- Barril, P.A.; Pianciola, L.A.; Mazzeo, M.; Ousset, M.J.; Jaureguiberry, M.V.; Alessandrello, M.; Sánchez, G.; Oteiza, J.M. Evaluation of viral concentration methods for SARS-CoV-2 recovery from wastewaters. Sci. Total. Environ. 2021, 756, 144105. [Google Scholar] [CrossRef] [PubMed]
- Ozawa, H.; Yoshida, H.; Usuku, S. Environmental surveillance can dynamically track ecological changes in enteroviruses. Appl. Environ. Microbiol. 2019, 85, e01604–e01619. [Google Scholar] [CrossRef]
- Chomczynski, P.; Sacchi, N. Single-step method of rna isolation by acid guanidinium thiocyanate phenol chloroform extraction. Anal. Biochem. 1987, 162, 156–159. [Google Scholar] [CrossRef]
- Kocamemi, B.; Kurt, H.; Sait, A.; Sarac, F.; Saatci, A.; Pakdemirli, B. SARS-CoV-2 Detection in Istanbul Wastewater Treatment Plant Sludges. medRxiv 2020. [Google Scholar] [CrossRef]
- Hata, A.; Hara-Yamamura, H.; Meuchi, Y.; Imai, S.; Honda, R. Detection of SARS-CoV-2 in wastewater in Japan during a COVID-19 outbreak. Sci. Total. Environ. 2021, 758, 143578. [Google Scholar] [CrossRef]
- Calgua, B.; Rodriguez-Manzano, J.; Hundesa, A.; Sunen, E.; Calvo, M.; Bofill-Mas, S.; Girones, R. New methods for the concentration of viruses from urban sewage using quantitative PCR. J. Virol. Methods 2013, 187, 215–221. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Zhou, N.A.; Tharpe, C.; Meschke, J.S.; Ferguson, C.M. Survey of rapid development of environmental surveillance methods for SARS-CoV-2 detection in wastewater. Sci. Total. Environ. 2021, 769, 144852. [Google Scholar] [CrossRef] [PubMed]
- Pastorino, B.; Touret, F.; Gilles, M.; de Lamballerie, X.; Charrel, R.N. Prolonged infectivity of SARS-CoV-2 in fomites. Emerg. Infect. Dis. 2020, 26, 2256. [Google Scholar] [CrossRef]
- Graham, K.E.; Loeb, S.K.; Wolfe, M.K.; Catoe, D.; Sinnott-Armstrong, N.; Kim, S.; Yamahara, K.M.; Sassoubre, L.M.; Mendoza Grijalva, L.M.; Roldan-Hernandez, L. SARS-CoV-2 RNA in Wastewater Settled Solids Is Associated with COVID-19 Cases in a Large Urban Sewershed. Environ. Sci. Technol. 2020, 55, 488–498. [Google Scholar] [CrossRef] [PubMed]
- Ikner, L.A.; Gerba, C.P.; Bright, K.R. Concentration and recovery of viruses from water: A comprehensive review. Food Environ. Virol. 2012, 4, 41–67. [Google Scholar] [CrossRef]
- Farkas, K.; Hillary, L.S.; Malham, S.K.; McDonald, J.E.; Jones, D.L. Wastewater and public health: The potential of wastewater surveillance for monitoring COVID-19. Curr. Opin. Environ. Sci. Health 2020, 17, 14–20. [Google Scholar] [CrossRef]
- Katayama, H.; Shimasaki, A.; Ohgaki, S. Development of a virus concentration method and its application to detection of enterovirus and Norwalk virus from coastal seawater. Appl. Environ. Microbiol. 2002, 68, 1033–1039. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Petala, M.; Dafou, D.; Kostoglou, M.; Karapantsios, T.; Kanata, E.; Chatziefstathiou, A.; Sakaveli, F.; Kotoulas, K.; Arsenakis, M.; Roilides, E. A physicochemical model for rationalizing SARS-CoV-2 concentration in sewage. Case study: The city of Thessaloniki in Greece. Sci. Total. Environ. 2021, 755, 142855. [Google Scholar] [CrossRef]
- Trottier, J.; Darques, R.; Mouheb, N.A.; Partiot, E.; Bakhache, W.; Deffieu, M.S.; Gaudin, R. Post-lockdown detection of SARS-CoV-2 RNA in the wastewater of Montpellier, France. One Health 2020, 10, 100157. [Google Scholar] [CrossRef] [PubMed]
- Albertsson, P.-å.; Frick, G. Partition of virus particles in a liquid two-phase system. Biochim. Et Biophys. Acta 1960, 37, 230–237. [Google Scholar] [CrossRef]
- Lu, D.; Huang, Z.; Luo, J.; Zhang, X.; Sha, S. Primary concentration–The critical step in implementing the wastewater based epidemiology for the COVID-19 pandemic: A mini-review. Sci. Total. Environ. 2020, 747, 141245. [Google Scholar] [CrossRef]
- Shuval, H.I.; Cymbalista, B.F.S.; Goldblum, N. The phase-separation method for the concentration and detection of viruses in water. Water Res. 1969, 3, 225–240. [Google Scholar] [CrossRef]
- Wallis, C.; Grinstein, S.; Melnick, J.L.; Fields, J.E. Concentration of viruses from sewage and excreta on insoluble polyelectrolytes. Appl. Microbiol. 1969, 18, 1007–1014. [Google Scholar] [CrossRef]
- Word Health Organization. Guidelines for Environmental Surveillance of Poliovirus Circulation; WHO: Geneva, Swithzerland, 2003. [Google Scholar]
- Rothman, J.A.; Loveless, T.B.; Griffith, M.L.; Steele, J.A.; Griffith, J.F.; Whiteson, K.L. Metagenomics of Wastewater Influent from Southern California Wastewater Treatment Facilities in the Era of COVID-19. Microbiol. Resour. Announc. 2020, 9. [Google Scholar] [CrossRef] [PubMed]
- Corman, V.M.; Landt, O.; Kaiser, M.; Molenkamp, R.; Meijer, A.; Chu, D.K.; Bleicker, T.; Brünink, S.; Schneider, J.; Schmidt, M.L. Detection of 2019 novel coronavirus (2019-nCoV) by real-time RT-PCR. Eurosurveillance 2020, 25, 2000045. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Jones, T.H.; Johns, M.W. Improved detection of F-specific RNA coliphages in fecal material by extraction and polyethylene glycol precipitation. Appl. Environ. Microbiol. 2009, 75, 6142–6146. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- United States Environmental Protection Agency. Method 1623: Cryptosporidium and Giardia in Water by Filtration/IMS/FAEPA 821-R-01–025; EPA US Environmental Protection Agency: Washington, DC, USA, 2005.
- Miyani, B.; Fonoll, X.; Norton, J.; Mehrotra, A.; Xagoraraki, I. SARS-CoV-2 in Detroit wastewater. J. Environ. Eng. 2020, 146, 06020004. [Google Scholar] [CrossRef]
- Philo, S.E.; Keim, E.K.; Swanstrom, R.; Ong, A.Q.; Burnor, E.A.; Kossik, A.L.; Harrison, J.C.; Demeke, B.A.; Zhou, N.A.; Beck, N.K. A comparison of SARS-CoV-2 wastewater concentration methods for environmental surveillance. Sci. Total. Environ. 2021, 760, 144215. [Google Scholar] [CrossRef]
- Michael-Kordatou, I.; Karaolia, P.; Fatta-Kassinos, D. Sewage analysis as a tool for the COVID-19 pandemic response and management: The urgent need for optimised protocols for SARS-CoV-2 detection and quantification. J. Environ. Chem. Eng. 2020, 8, 104306. [Google Scholar] [CrossRef]
- Tavares, L.; Alves, P.M.; Ferreira, R.B.; Santos, C.N. Comparison of different methods for DNA-free RNA isolation from SK-N-MC neuroblastoma. BMC Res. Notes 2011, 4, 1–5. [Google Scholar] [CrossRef]
- CDC. 2019-nCoV Real-Time RT-PCR Diagnostic Panel. Instructions for Use; (Effective 4 February 2020); CDC: Atlanta, GA, USA, 2020. [Google Scholar]
- Bhatt, A.; Arora, P.; Prajapati, S.K. Occurrence, fates and potential treatment approaches for removal of viruses from wastewater: A review with emphasis on SARS-CoV-2. J. Environ. Chem. Eng. 2020, 104429. [Google Scholar] [CrossRef]
- Lodder, W.; de Roda Husman, A.M. SARS-CoV-2 in wastewater: Potential health risk, but also data source. Lancet Gastroenterol. Hepatol. 2020, 5, 533–534. [Google Scholar] [CrossRef]
- Mallapaty, S. How sewage could reveal true scale of coronavirus outbreak. Nature 2020, 580, 176–177. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Gonzalez, R.; Curtis, K.; Bivins, A.; Bibby, K.; Weir, M.H.; Yetka, K.; Thompson, H.; Keeling, D.; Mitchell, J.; Gonzalez, D. COVID-19 surveillance in Southeastern Virginia using wastewater-based epidemiology. Water Res. 2020, 186, 116296. [Google Scholar] [CrossRef] [PubMed]
- Langone, M.; Petta, L.; Cellamare, C.; Ferraris, M.; Guzzinati, R.; Mattioli, D.; Sabia, G. SARS-CoV-2 in water services: Presence and impacts. Environ. Pollut. 2020, 268, 115806. [Google Scholar] [CrossRef] [PubMed]
- Nemudryi, A.; Nemudraia, A.; Wiegand, T.; Surya, K.; Buyukyoruk, M.; Cicha, C.; Vanderwood, K.K.; Wilkinson, R.; Wiedenheft, B. Temporal detection and phylogenetic assessment of SARS-CoV-2 in municipal wastewater. Cell Rep. Med. 2020, 1, 100098. [Google Scholar] [CrossRef]
- Jung, Y.; Park, G.-S.; Moon, J.H.; Ku, K.; Beak, S.-H.; Lee, C.-S.; Kim, S.; Park, E.C.; Park, D.; Lee, J.-H. Comparative analysis of primer–probe sets for RT-qPCR of COVID-19 causative virus (SARS-CoV-2). ACS Infect. Dis. 2020, 6, 2513–2523. [Google Scholar] [CrossRef]
- Nalla, A.K.; Casto, A.M.; Huang, M.-L.W.; Perchetti, G.A.; Sampoleo, R.; Shrestha, L.; Wei, Y.; Zhu, H.; Jerome, K.R.; Greninger, A.L. Comparative performance of SARS-CoV-2 detection assays using seven different primer-probe sets and one assay kit. J. Clin. Microbiol. 2020, 58, e00557-20. [Google Scholar] [CrossRef] [Green Version]
- Vogels, C.B.; Brito, A.F.; Wyllie, A.L.; Fauver, J.R.; Ott, I.M.; Kalinich, C.C.; Petrone, M.E.; Casanovas-Massana, A.; Muenker, M.C.; Moore, A.J. Analytical sensitivity and efficiency comparisons of SARS-CoV-2 RT–qPCR primer–probe sets. Nat. Microbiol. 2020, 5, 1299–1305. [Google Scholar] [CrossRef] [PubMed]
- Chu, D.K.; Pan, Y.; Cheng, S.M.; Hui, K.P.; Krishnan, P.; Liu, Y.; Ng, D.Y.; Wan, C.K.; Yang, P.; Wang, Q. Molecular diagnosis of a novel coronavirus (2019-nCoV) causing an outbreak of pneumonia. Clin. Chem. 2020, 66, 549–555. [Google Scholar] [CrossRef] [Green Version]
- Shirato, K.; Nao, N.; Katano, H.; Takayama, I.; Saito, S.; Kato, F.; Katoh, H.; Sakata, M.; Nakatsu, Y.; Mori, Y. Development of genetic diagnostic methods for novel coronavirus 2019 (nCoV-2019) in Japan. Jpn. J. Infect. Dis. 2020, 73. [Google Scholar] [CrossRef] [Green Version]

| Sample | Volume | Preconditioning Step | Concentration/Extraction/Detection | Reference |
|---|---|---|---|---|
| Single sample from WWTP influent in Brisbane, Australia | 100–200 mL | UF1 Centrifuge the sample at 4500× g for 10 min at 4 °C Ultracentrifugation Centrifuge at 100,000× g for 1 h at 4 °C. PEG precipitation Centrifuge at 10,000× g for 20 min at 4 °C to remove larger particles and debris. Transfer the supernatant to a new centrifuge tube Store the supernatant at 4° (S1) | UF1: Centrifuge at 4750× g for 10 min through centrifugal filter (30 kDa) UF2: Centrifuge at 3500× g for 30 min through centrifugal filter (10 kDa) ENMF 1: Filtrate through 0.45 μm of ENM ENMF 2: After addition MgCl2 (final concentration of 25 mM), filtrate 0.45 μm of ENM ENMF 3: After adjusting pH 4.0 (2 N HCl) pass through membrane filter (0.45 μm) Ultracentrifugation (UFC): Re-suspend the pellet in 3.5 mL of 0.25 N glycine buffer (pH 9.5), incubate it on ice (30 min), add 3 mL of 2 × PBS (pH 7.2), centrifuge eat 12,000× g for 15 min at 4 °C, UFC at 100,000× g for 1 h at 4 °C to recover the virus, re-suspend the pellet in PBS (pH 7.2) PEG Precipitation: Re-suspend the pellet in beef extract (3% w/v) in 0.05 M glycine (pH 9.0) at a ratio of 1:5; agitate at 200 rpm for 30 min at room temp., centrifuge at 10,000× g for 10 min at 4 °C, transfer the pellet suspension into S1; neutralize pH (2 M HCl), add PEG 8000 (10%) and NaCl (2% w v−1), incubate at 120 rpm at 4 °C for 2 h, centrifuge it at 10,000× g at 4 °C for 30 min; discard the supernatant; re-suspend the pellet in 800 μL Trizol, further steps: as described in Ahmed et al. [82]. | [83] |
| Composite samples from a PS and two WWTPs in Southeast Queensland, Canada | 100–200 mL | UF Centrifuge the sample at 4750× g for 30 min at 4 °C | UF: Centrifuge at 3500× g for 15 min through centrifugal filter (10 kDa); invert and place the concentrate cup on top of the sample filter cup, centrifuge at 1000× g for 2 min. RNA Extraction—PCR assay: RNeasy PowerMicrobiome Kit® via QIAcube Connect platform RT-qPCR: Bio-Rad CFX96 thermal cycler, targeting gene: N protein | [82] |
| Untreated municipal samples from three different regions in Stockholm, Sweden, and one region from the North of Italy | N.A. | As described in the next column | UF: Centrifuge at 4600× g at 4 °C for 30 min; filter centrifugal ultrafilter (10 kDa) at 1500× g for 15 min Double UF: Application of UF twice Adsorption-extraction-ENMF: Add MgCl2 (25 mM), filtrate (0.45 μm-ENMF) Centrifugation-adsorption-extraction-ENMF: Centrifuge at 4600× g at 4 °C for 30 min, add MgCl2 (25 mM) to the sample, filtrate (0.45 μm-ENMF) Extract RNA obtained UF and double UF by TRIzol-chloroform using miRNeasy™ Mini Kit Extract RNA obtain from ENMFs using RNeasy™ Power Microbiome Kit RTqPCR analysis (Primers targeting the nucleocapsid (N) gene) | [84] |
| Grab WW samples, WWTPs in Italy | 100 mL | Filter on 0.22 μm polyether sulfone (PES) | UF: Filtrate through centrifugal 10 kDa filter units in a swinging bucket rotor at 4000 × g for 10 min, RNA extraction: QIAamp™ viral RNA mini kit; StepOnePlus™ Real-Time PCR System | [17] |
| 24 h composite and grab wastewater samples; WWTPs in Louisiana, USA | 250 mL | Centrifuge the sample at 3000× g for 30 min | UF: Centrifuge at 1500× g for 15 min through centrifugal filter (100 kDa); invert and centrifuge the filtrate unit at 1000× g for 2 RNA extraction using ZR™ Viral RNA Kit (RT-qPCR) assays (CDC N1 and N2) | [63] |
| Grab; 2 WWTPs; MH in Japan | 400 mL | Centrifuge at 3000 rpm (1840× g) for 30 min | UF: Following instructions of Ahmed et al. [82] using centrifugal filter (30 kDa), further steps as described in Table 2 | [85] |
| 24 h composite, 11 WWTPs, MH, PS | Pasteurize in a 60 °C water bath for 90 min Filter through 0.22 μm polyethersulfone filter | UF: Centrifuge polypropylene (PP) concentration/spin column (30 kDa) Further steps as described in Table 2 | [86] | |
| Grab samples (after the decantation before the activated sludge process) in French Grand Est | 2 volumes of 50 mL | Not applied | UF: Centrifuge at 1500× g for 15 min a centrifugal ultrafilter (100 kDa), inverting the system and applying centrifugation (1000× g for 2 min), wash the ultrafilter with 3.5 mL deionised water, combine washing water (3.5 mL) with the concentrate (1.5 mL), apply further two washing steps using 5 mL NucliSENS® lysis buffer (bioM’erieux) for an incubation time of 5 min, use the entire for nucleic acid extraction | [87] |
| Grab and composite samples in Japan | 40 mL | Centrifuge at 3500× g for 5 min | UF: Centrifuge at 3500× g for 20 min a centrifugal ultrafilter (30 kDa) Further steps as described in Table 2 | [88] |
| 24 h composite samples; WWTP in Montpellier, France | 50 mL (COS) | Centrifuge at 4500× g for 30 min at 4 °C Pass the supernatant through a 40 μm cell strainer Froze at −20 °C for further analyses | UF: Centrifuge through centrifugal ultrafilter (50 kDa) RNA extraction: the NucleoSpin™ RNA Virus kit TaqPath One-Step RT-qPCR, CG master mix | [85] |
| A Mixture comprised of 3 grab samples | 50 mL | Centrifuge at 4500× g for 30 min Filtrate through 0.22 μm membrane filters | UF: Concentrate (30 times) the filtrate using the 96 well filter plate (10 kDa) Further steps as described in Table 2 | [89] |
| B 24 h composite WW samples | Centrifuge at 4500× g for 30min | UF: Centrifuge through centrifugal ultrafilter (10 kDa), buffer pH to 7.4 with PBS Further steps as described in Table 2 | [90] | |
| C Samples from in İstanbul, Turkey | 250 mL | Centrifuge at 3200× g for 45 min | UF: Centrifugation at 3200× g for 25–40 min, through centrifugal ultrafilter (10 kDa), Further steps as described in Table 2 | [66] |
| 24 h composite WWTP in Southeast England | 120–240 mL | Centrifugation at 3200× g Filter through 0.45 μm filter | UF: Centrifuge through centrifugal filter (10 kDa) Real-time RT-qPCR using a qScript XLT qPCR Toughmix system | [91] |
| Samples from 3 WWTPs in Zurich (A), Lausanne (B), in a resort Switzerland | 50 mL | On the sample taken from a WWTP Filtrate through 2 µm and 0.22 µm filters On the sample taken from WWTPs B Centrifuge at 4863× g for 30 min | UF: Concentrate the supernatant using centrifugal filter units (Centricon® Plus-70 Ultrafilter, 10 kDa) by centrifugation at 3000× g for 30 min RNA extraction by the QiaAmp™ Viral RNA MiniKit, store the extracted sample at −80 °C cDNA transcripts using NGS; Sequencing using the Illumina NovaSeq 6000 platform | [92] |
| 24 h-composite raw wastewater samples from 6 WWTPs, in Catalonia, Spain | 200 mL | Seed an aliquot of 200 mL of the sample with 107 GC mL−1 of MS2 and MHV (1:100, v v−1) Centrifuge at 4750× g for 30 min | UF1: Concentration Pipette CP-Select™ using Hollow Fiber Polysulfone PVP high-flow pipette (150 kDa), elute viral particles with 0.075% Tween-20/Tris using Wet Foam Elution™ cans UF2: Centrifuge through centrifugal ultrafilter (30 kDa) at 3000× g for 30 min Elute the virus by inverting the CeUF device, centrifuge at 1000× g for 3 min RNA extraction: the QIAmp Viral RNA Mini kit | [93] |
| D Water/wastewater composite and grabs samples | 150 mL | Filter only samples from one facility with 100-mm filter paper and others as is | HFUF: Hollow fiber ultrafiltration (30 kDa) UF: Centrifugal ultrafiltration (30 kDa or 100 kDa) Centrifuge at 3500× g for 15–30 min at 10 °C, analyse as-is or further processed with 2nd concentration via Centricon ultrafilters or PEG precipitation according to [94] Extract RNA and DNA using Purelink Viral™ RNA/DNA Mini Kit CFX96 or CFX384 Touch™ Real-Time PCR Detection Systems | [95] |
| 24 h composite WWTP, in Helsinki, Finland | 60 mL | Centrifuge at 4654× g for 30 min | UF: Centrifuge through centrifugal filters (10 K) at 3000× g for 25 min, followed by concentrate collection with 1000× g for 2 min (~400 μL of concentrate) | [77] |
| 24 h flow-dependent composite influent and effluent samples, 6 WWTPs in Germany | Liquid phase: Centrifuge at 4700× g for 30 min Solid phase: Centrifuge at 4700× g for 30 min Wash the separated pellets with deionized water Centrifuge at 4700× g for 5 min before being re-suspended in 150 μL deionized water Re-centrifuge at 4700× g for 5 min | UF: Concentrate the supernatant by centrifugal ultrafiltration units Amicon® Ultra-15 Centrifugal Filter Unit by centrifugation for 15 min at 3500× g Repeat twice centrifugation (~450 μL of the concentrated) RNA extraction: the NucleoSpin ™RNA Virus kit RNA analyses: by OneStep RT-qPCR using Luna Universal Probe One-Step RT-qPCR Kit or LightCycler®Multiplex RNA Virus Master and the CFX96 Real-Time System, with a C1000 Touch Thermal Cycler | [49] |
| Sample | Concentration Method | RNA Extraction | PCR Assays | Ref |
|---|---|---|---|---|
| 24 h composite samples of raw sewage from urban WWTP in Massachusetts, USA | PEG precipitation Pasteurize in a 60 °C water bath for 90 min Filter through a 0.2 μm membrane Mix the filtrate with PEG 6000 (a final concentration of 8% (w v−1) and NaCl to 0.3 M Dissolve the chemical by about 15 min Centrifuge at 12,000× g for 2 h Discard the PEG-containing supernatant Re-suspend the pellet 1.5 mL TRIzol reagent | TRIzol-chloroform method Mix the re-suspended samples with 300 μL chloroform for 1 min Incubate for 5 min at room temperature Centrifuge at 16,000× g at 4 °C for 15 min Transfer aqueous phase to a new 1.5 mL tube Mix with an equal volume of isopropanol Centrifuge at 16,000× g for 10 min Discard the supernatant, wash twice the pellet with 75% ethanol, Recover RNA using 30 μL of diethyl pyrocarbonate (DEPC) water | A Bio-Rad CFX96 real-time (RT) PCR detection system PCR: TaqMan Fast Advanced master mix, CDC N1, N2, and N3 primer-probes (IDT); and cDNA as a template | [62] |
| 24 h composite wastewater samples from 7 WWTPs in California, USA | According to the protocol of Wu et al. [62] | According to the protocol of Wu et al. [62] | N.A. | [62] |
| Grab samples from influent of WWTP in Neuquen city, Argentina | PEG precipitation Adjust pH to 6.5–7.2, Add PEG 6000 (10% w v−1) and NaCl (0.3 M) Stir for 2 h at 4 °C Centrifuge at 10,000× g for 25 min at 4 °C Discard the suspension, suspend the pellet in 1 mL PBS (pH 7.2), adjust pH to 8.0, incubate at room temp. for 1 h with occasional agitation, centrifuge the suspension at 10,000× g for 20 min, store at −70 °C | The commercial kit Direct-zol RNA Miniprep™ | One-step real time RT-PCR assay Target regions of the SARS-CoV-2 nucleocapsid gene (N1 and N2) by TaqMan probe | [96] |
| Grab samples from influent of WWTP in Neuquen city, Argentina | Aluminum-driven flocculation [14] Method Add 1:100 v v−1 of 9% PAC Adjust pH to 6.0, gently agitate for 30 min at room temp. Centrifuge at 1700× g for 20 min Re-suspended pellets into 10 mL of 3% beef extract (pH 7.4), shack for 20 min at 80 rpm Centrifuge at 1900× g for 30 min Re-suspended the pellet in 1mL of PBS, store at−70 °C | The commercial kit Direct-zol RNA Miniprep™ | One-step real time RT-PCR assay Target regions of the SARS-CoV-2 nucleocapsid gene (N1 and N2) by TaqMan probe | [96] |
| Influent, secondary and tertiary treated effluent water samples in the Region of Murcia, Spain | Aluminum-driven flocculation As explained in [96] | The Nucleo-Spin RNA virus kit | TaqMan real-time RT-PCR (RT-qPCR) on LightCycler 480 instrument | [14] |
| Grab samples from influent of 2 WWTPs and a manhole in a metropolitan region in Japan. | Centrifuge the sample (400) 3000 rpm (1840× g) for 30 min PEG precipitation According to the protocol of Wu et al. [62] ENMA [62,97] Filter with a pore size of 1.0 μm and 0.45 μM membrane, adjust pH to 3.5 using 0.5 N HCl, elute the adsorbed viruses with 3% beef extract solution UF: As explained in Table 1 | A RNeasy Microbiome kit® For sediment extraction: The RNeasy PowerSoil kit® | The One Step PrimeScript III RT-qPCR Mix™ for the NIID_N2 assay The SARS-CoV-2 Direct Detection RT-qPCR Kit™ for the CDC_N1N2 assay. | [85] |
| Grab samples (after the decantation before the activated sludge process) from WWTP and from suspected COVID-19 patients hospitalized in the local university hospital (60%) and from retirement home residents (40%) | PEG precipitation Dissolve 3 g beef extract powder, 3 g NaCl, and 0.37 g glycine in 100 mL of sample, Add 20 g of PEG 6000 to the mixture Stir gently at 4 °C for 2 h, store at 4 °C overnight Centrifuge at 4500× g, 4 °C for 45 min. re-suspended the pellet in deionised water, add 10 mL NucliSENS® lysis buffer, incubate for 10 min at room temperature UF Centrifuge 2 volumes of 50 mL at 1500× g for 15 min using MWCO of 100 kD | Transfer the sample in lysis buffer in a 50 mL conical tube, containing 4 g of a mixture of high-vacuum silicon grease (Dow Corning®) and silicon dioxide (Sigma) (90:10 w/w) Add 15 mL phenol-chloroform-isoamyl alcohol Stir 15 s by hand, centrifuge at 3500× g for 5 min Recover the hydrophile supernatant (15 mL) Use 70 μL of magnetic silica beads and the NucliSENS® easyMAG™ platform to extract RNA Elute the extracted in 100 μL of elution buffer Remove residual environmental inhibitors using OneStep PCR Inhibitor Removal kit™,store at −80 °C | Real-time RT-PCR and RT-digital droplet PCR (RT-ddPCR) For the RdRp_IP4, E, and VTB4-Fph GGII sets, quantification using an RNA UltraSens™ One-Step Quantitative RT-PCR system (Applied Biosystems™) StepOnePlus Real-Time PCR System (Applied Biosystems™) | [87] |
| A grab sample from WWTP in Niigata Prefecture, composite samples WWTPs in Kanagawa Prefecture and Tokyo in Japan | Pretreatment: Centrifuge at 3500× g for 5 min PEG precipitation: using PEG8000 and NaCl (to final concentrations of 10% and 1 M), overnight mixing at 4 °C UF: Centrifuge at 3500× g for 20min to filter (30 kDa) Electronegative membrane vortex (EMV): Filter of raw sewage (50 mL) inoculated with 500 μL of 2.5 M MgCl2 through 0.45 μm membrane by vacuum aspiration. | Spin column-based nucleic acid purification using QIAamp Viral RNA Mini Kit™ Acid guanidinium thiocyanate–phenol– chloroform extraction according to the protocol of Chomczynski and Sacchi [98] using TRIzol LS reagent | qPCR:TaqMan™ Gene Expression Master Mix Specific forward primers/reverse primers, and TaqMan Probe | [88] |
| 24 h composite samples Influent and effluent of 11 WWTPs, MH, PSs | Pasteurize in a 60 °C water bath for 90 min Filter through 0.22 μm polyethersulfone filter PEG precipitation: According to Wu et al. [99] Ultrafiltration: using MWCO of 30 kDa | ABIOpure Viral DNA/RNA Extraction kit Ultrafiltration columns/RNA extraction kit PEG/TRIzol extraction | RT-qPCR using GENESIG COVID-19 kit | [86] |
| 24 h composite WWTPs in Spain | PEG precipitation: with 20% PEG 6000; re-suspend the pellet in 3 mL of PBS, pH 7.4 | NucliSENS® miniMAG® extraction system | One-step RT-qPCR assays; UltraSense One-step Quantitative RT-PCR System™ | [59] |
| Grab sample seeding with gamma irradiated (5 × 106 RADs) SARS-CoV-2, PEDV and MgV | Add 25 mL of TGEB pH 9.5 to the seeded sample Incubated at 300 rpm for 2 h at 4 °C. Centrifuge at 2500× g for 10 min at 4 °C PEG Precipitation: with PEG 8000 and NaCl (20% + 0.3 M) in agitation overnight at 4 °C, centrifuge at 3500× g for 30 min at 4 °C, re-suspend the pellet in PBS, store at −80 °C Aluminum-driven flocculation According to the protocol of Randazzo et al. [14] | Manual column-based commercial kit Nucleospin RNA virus Kit™ according to the manufacturer’s protocol together with an initial pre-treatment step with Plant RNA Isolation Aid [14] An automated instrument relying on magnetic beads for nucleic acid purification, Maxwell® RSC Instrument used for automated nucleic acid isolation using the Maxwell RSC Pure Food GMO and authentication kit | RT-qPCR using One Step Prime Script™ RT-PCR Kit | [14] |
| Grab samples influent and UASB effluent of Old Pirana WWTP in Ahmedabad, in India | Centrifuge at 4500× g for 30min Filtrate through 0.22 μm membrane filters PEG precipitation: with PEG 9000 (80 g L−1) and NaCl (17.5 g L−1), incubating overnight at 17 °C, at 100 rpm; centrifuge the mixture at 13,000× g for 90 min | Mix 10 μL MS2 phage, 20 μL Proteinase K (20 mg mL−1) solution and 600 μL of RAV1 buffer containing carrier RNA with the concentrated viral particles (200 μL) and follow steps instructed in the product manual of NucleoSpin® RNA Virus kit | The detection of ORF1ab, N gene and S gene of SARS-CoV-2 and MS2 (internal process control) by RT-PCR using TaqPath™ Covid-19 RT-PCR Kit Real Time PCR system | [25] |
| A Mixture comprised of 3 grab samples (Table 1) | Centrifuge/PEG precipitation as described by [25] Centrifuge at 4500× g for 30 min and filtrate (0.22 μm) UF: (30 times) using the filtrate using the 96 well filter plate with a capacity to filter less than 10 kDa molecules | Mix 10 μL MS2 phage, 20 μL Proteinase K (20 mg/mL) solution and 600 μL of RAV1 buffer containing carrier RNA with the concentrated viral particles (200 μL) and follow steps instructed in the product manual of NucleoSpin® RNA Virus kit | The detection of ORF1ab, N gene and S gene of SARS-CoV-2 and MS2 (internal process control) by RT-PCR using TaqPath™ Covid-19 RT-PCR Kit | [82] |
| Samples from 7 WWTPs and samples from 2 MHs nearby pandemic hospitals in İstanbul, Turkey | Centrifugation at 3000× g for 45 min PEG precipitation: with PEG 8000 (10% w v−1) and NaCl (0.3 M), incubating overnight at 4 °C, at 60 rpm; centrifuge the mixture at 5700× g for 2 h at 4 °C, store at −80 °C | QIAmp cador Pathogen Mini Kit | RT-qPCR QuantiNova Pathogen + IC kit Bio-Rad CFX96 thermal cycler™ | [66] |
| Primary sludge and the waste activated sludge samples from 7 WWTPs in İstanbul, Turkey | Shake at 100 rpm, at 4 °C for 30 min to transfer viruses into liquid phase Centrifugation at 7471× g for 30 min, sequentially filter supernatant through a 0.45 and 0.2 μm membranes PEG precipitation: as described [66] | Extract of 1 mL virus concentrate with Roche MagNA pure LC total nucleic acid isolation kit™ using Roche MagNA pure LC system™ in accordance with the manufacturer’s protocols Quantify the RNA with Thermo NanoDrop 2000c™ | Real time ready RNA virus Master™ contained 0.8 nM of forward primer and reverse primer, 0.25 nM probe and 5 μL of template RNA. | [99] |
| Grab samples from WWTP in Ishikawa prefecture and WWTPs in Toyama prefecture, in Japan | Centrifuge the sample at 5000× g for 5 min PEG precipitation: with PEG 8000 and NaCl (10% and 1 M) incubating the mixture overnight on a shaker at 4 °C, centrifuge at 10,000× g for 30 min, re-suspend the pellet in phosphate buffer | A 60 μL of RNA extract, in accordance with the manufacturer’s instructions using a QIAamp Viral RNA Mini Kit® | TaqMan-based qRT-PCR assays One Step PrimeScript™ RT-PCR Kit™ RT-nested PCR assays | [100] |
| 24 h composites, wastewater samples: influent and effluent of primary settling tank, effluents of secondary settling tanks; sludge samples; primary and secondary settling tanks, thickener, thermal hydrolysis (Spain) | Centrifuge at 4500× g for 30min UF: with a capacity to filter less than 10 kDa molecules by filtration using Amicon 15 mL 10 K centrifugal device, buffer pH to7.4 with PBS PEG precipitation for the sludge samples: Add glycine buffer (1:8 (v v)) to the sludge, incubate the mixture at 4°C for 2 h, centrifuge at 8000× g for 30 min, filter through a 0.45 μm polyethersulfone, precipitate by adding 1:5 (v v−1) of PEG 8000 (80g/L) and NaCl (17.5 g/L), shack at 150 rpm overnight at 4 °C, centrifuge at 13,000× g for 90 min, re-suspended in PBS buffer pH 7.4, store at −80 °C | MicrolabStarlet IVD™ using the STARMag 96 × 4 Universal Cartridge Kit™ according to manufacturer specifications | One-step multiplex RT-qPCR Allplex system™ 2019-nCoV For the RT-PCR, the CFX96 system™ | [90] |
| 24 h composite samples from 5 WWTPs in Milan, Turin, and Bologna, Italy | Pasteurize in a 60 °C water bath for 90 min Centrifuge at 1200× g for 30 min Two-phase (PEG-dextran) separation method Pool the supernatants in a 1 L Erlenmeyer flask and keep the pellets (P1) at 4 °C, adjust the pH of the supernatant to pH 7 –7.5, add 19.8 mL of 22% dextran, 143.5 mL 29% PEG 6000, and 17.5 mL 5N NaCl to 250 mL of supernatant, agitate for 30 min at 4 °C, pour the mixture a sterile conical separation funnel, leave overnight at 4 °C, collect the entire lower layer (S1), re-suspend the pellet (P1) into S1, extract with 20% volume of chloroform by shaking vigorously for 10 min, centrifuge 1200× g for 10 min | The NucliSENS miniMAG™ Semi-automated extraction system with magnetic silica | Real-time RT-qPCR assays targeting the E gene of the SARS Betacoronavirus and the RdRp gene of SARS-CoV-2 A newly developed real-time RT-(q)PCR designed using the Primer3 Software targeting the ORF1ab region (nsp14; 3′-to-5′ exonuclease) of the SARS-CoV-2 genome | [58] |
| 24 h composite post-grit chamber influent solids and primary clarified sludge samples from the City of Ottawa’s Robert O. Pickard Environmental Centre, Ontario, and the City of Gatineau, Quebec, WRRFs in Canada | After settling at 4 °C for an hour, decant the supernatant Filter through 1.5 μm glass fiber filter and 0.45 μm GF6 mixed cellulose ester (MCE) filter, collect eluate fraction by passing 32 mL of elution buffer (0.05 M KH2PO4, 1.0 M NaCl, 0.1% (v v−1) Triton X-100, pH 9.2) through the spent filters. PEG Precipitation: with PEG 8000 (80 g/L and 0.3M NaCl (pH 7.3), agitating at 4 °C and 160 rpm for 12–17 h hours, centrifuge at 10,000× g for 45 min at 4 °C, decant the supernatant samples, centrifuge at 10,000× g for 10 min, decant the remaining supernatant, transfer a new RNase-free centrifuge tube, store at −80 °C until RNA extraction | Lysis buffer/TRIzol LS extraction Analysis with The RNeasy Power Microbiome® Add 200 mg of sample pellet in place of 200 μL of liquid sample; add lysis buffer/TRIzol LS reagent to maximize lysis of cells/virion encapsulated fragments and protect RNA prior to vortexing and centrifugation; retain the resulting aqueous phase of the lysis procedure, processed as per the recommended protocol including the on-column enzymatic DNA removal step | Singleplex, probe-based, one-step RT-qPCR Singleplex, probe-based, one-step RT-ddPCR | [64] |
| Grab samples from Quito’s river receiving untreated sewage | Skim milk flocculation Prepare the pre-flocculated skimmed-milk solution (PRSMS) (1% w v−1) [101] Adjust pH to 3.5, add PRSMS of 10 mL L−1 to the supernatant Stir slowly at room temp for 8 h Precipitate by centrifugation at 8000× g for 40 min Carefully remove the supernatants Re-suspend the pellet in 10 mL of PBS (pH 7.2) Store at −70 °C. | AccuPrep® Universal RNA Extraction Kit | CFX96 Real-Time detection system using TaqMan™ Fast Virus 1-Step Master Mix and the RTqPCR diagnostic panel assays for N1 and N2 regions of N gene | [72] |
| Composite samples, PS station and 2 WWTPs in Canada | Adjust pH to ~3.5 to 4 (2.0 N HCl) ENMF: Pass the sample (100–200 mL) through 0.45-μm-pore-size, 90-mm-diameter electronegative membrane | Use a 5 mL bead tube from RNeasy PowerWater Kit to accommodate the electronegative homogenize the samples ranging from 3 × 20 s at 8000 rpm at a 10 s interval membrane | RT-qPCR assays using a Bio-Rad CFX96 thermal cycler | [82] |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2021 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Mousazadeh, M.; Ashoori, R.; Paital, B.; Kabdaşlı, I.; Frontistis, Z.; Hashemi, M.; Sandoval, M.A.; Sherchan, S.; Das, K.; Emamjomeh, M.M. Wastewater Based Epidemiology Perspective as a Faster Protocol for Detecting Coronavirus RNA in Human Populations: A Review with Specific Reference to SARS-CoV-2 Virus. Pathogens 2021, 10, 1008. https://doi.org/10.3390/pathogens10081008
Mousazadeh M, Ashoori R, Paital B, Kabdaşlı I, Frontistis Z, Hashemi M, Sandoval MA, Sherchan S, Das K, Emamjomeh MM. Wastewater Based Epidemiology Perspective as a Faster Protocol for Detecting Coronavirus RNA in Human Populations: A Review with Specific Reference to SARS-CoV-2 Virus. Pathogens. 2021; 10(8):1008. https://doi.org/10.3390/pathogens10081008
Chicago/Turabian StyleMousazadeh, Milad, Razieh Ashoori, Biswaranjan Paital, Işık Kabdaşlı, Zacharias Frontistis, Marjan Hashemi, Miguel A. Sandoval, Samendra Sherchan, Kabita Das, and Mohammad Mahdi Emamjomeh. 2021. "Wastewater Based Epidemiology Perspective as a Faster Protocol for Detecting Coronavirus RNA in Human Populations: A Review with Specific Reference to SARS-CoV-2 Virus" Pathogens 10, no. 8: 1008. https://doi.org/10.3390/pathogens10081008
APA StyleMousazadeh, M., Ashoori, R., Paital, B., Kabdaşlı, I., Frontistis, Z., Hashemi, M., Sandoval, M. A., Sherchan, S., Das, K., & Emamjomeh, M. M. (2021). Wastewater Based Epidemiology Perspective as a Faster Protocol for Detecting Coronavirus RNA in Human Populations: A Review with Specific Reference to SARS-CoV-2 Virus. Pathogens, 10(8), 1008. https://doi.org/10.3390/pathogens10081008