Social Support Networks and the Mental Health of Runaway and Homeless Youth
Abstract
:1. Introduction
1.1. The Health and Mental Health of RHY
1.2. The Support Networks of RHY
2. Methods
2.1. Data and Sample
2.2. Measures
2.2.1. Mental Health Status
2.2.2. Social Network Support
2.2.3. Demographic Variables
2.3. Analytic Procedures
3. Results
4. Discussion
5. Conclusions
Acknowledgments
Author Contributions
Conflicts of Interest
References
- Auerswald, Colette L., Eiko Sugano, Jonathan M. Ellen, and Jeffrey D. Klausner. 2006. Street-based STD testing and treatment of homeless youth are feasible, acceptable and effective. Journal of Adolescent Health 38: 208–12. [Google Scholar] [CrossRef] [PubMed]
- Bannon, William M., Jr., Nisha Beharie, Orly Olshtain-Mann, Mary McKay, Leah Goldstein, Mary Acri, Marni L. LoIacono-Merves, Laura J. Elwyn, Kosta Kalogerogiannis, Ervin Torres, and et al. 2012. Youth Substance Use in a Context of Family Homelessness. Children and Youth Services Review 34: 1–7. [Google Scholar] [CrossRef] [PubMed]
- Barman-Adhikari, Anamika, and Eric Rice. 2014. Social networks as the context for understanding employment services utilization among homeless youth. Evaluation and Program Planning 45: 90–101. [Google Scholar] [CrossRef] [PubMed]
- Barman-Adhikari, Anamika, Stephanie Begun, Eric Rice, Amanda Yoshioka-Maxwell, and Andrea Perez-Portillo. 2016. Sociometric network structure and its association with methamphetamine use norms among homeless youth. Social Science Research 58: 292–308. [Google Scholar] [CrossRef] [PubMed]
- Bender, Kimberly, Sanna Thompson, Kristin Ferguson, and Lisa Langenderfer. 2014. Substance use predictors of victimization profiles among homeless youth: A latent class analysis. Journal of Adolescence 37: 155–64. [Google Scholar] [CrossRef] [PubMed]
- Blakeslee, Jennifer. 2012. Expanding the scope of research with transition-age foster youth: Applications of the social network perspective. Child & Family Social Work 17: 326–36. [Google Scholar] [CrossRef]
- Castellanos, H. Daniel. 2016. The Role of Institutional Placement, Family Conflict, and Homosexuality in Homelessness Pathways among Latino LGBT Youth in New York City. Journal of Homosexuality 63: 601–32. [Google Scholar] [CrossRef] [PubMed]
- Castro, Anne L., Erika L. Gustafson, Ashley E. Ford, Jennifer P. Edidin, Dale L. Smith, Scott J. Hunter, and Narijan S. Karnik. 2014. Psychiatric disorders, high-risk behaviors, and chronicity of episodes among predominantly African American homeless Chicago youth. Journal of Health Care for the Poor and Underserved 25: 1201–16. [Google Scholar] [CrossRef] [PubMed]
- Cotterell, John. 2013. Social Networks in Youth and Adolescence. New York: Routledge. [Google Scholar]
- Dank, Meredith, Jennifer Yahner, Kuniko Madden, Isela Bañuelos, Lilly Yu, Andrea Ritchie, Mitchyll Mora, and Brendan Conner. 2015. Surviving the Streets of New York. New York: Urban Institute, Available online: https://www.urban.org/sites/default/files/publication/42186/2000119-Surviving-the-Streets-of-New-York.pdf (accessed on 2 February 2017).
- Davies, Benjamin R., and Nicholas B. Allen. 2017. Review: Trauma and homelessness in youth: Psychopathology and intervention. Clinical Psychology Review 54: 17–28. [Google Scholar] [CrossRef] [PubMed]
- De la Haye, Kayla, Harold D. Green, David P. Kennedy, Annie Zhou, Daniella Golinelli, Suzanne L. Wenzel, and Joan S. Tucker. 2012. Who is supporting homeless youth? Predictors of support in personal networks. Journal of Research on Adolescence 22: 604–16. [Google Scholar] [CrossRef] [PubMed]
- Dworsky, Amy, Keri-Nichole Dillman, M. Robin Dion, Brandon Coffee-Borden, and Miriam Rosenau. 2012. Housing for Youth Aging out of Foster Care: A Review of the Literature and Program Typology. Washington: Mathematica Policy Research, Inc. [Google Scholar]
- Edidin, Jennifer P., Zoe Ganim, Scott J. Hunter, and Niranjan S. Karnik. 2012. The mental and physical health of homeless youth: A literature review. Child Psychiatry & Human Development 43: 354–75. [Google Scholar] [CrossRef]
- Ennett, Susan T., Susan L. Bailey, and E. Belle Federman. 1999. Social network characteristics associated with risky behaviors among runaway and homeless youth. Journal of Health and Social Behavior 40: 63–78. [Google Scholar] [CrossRef] [PubMed]
- Falci, Christina D., Les B. Whitbeck, Dan R. Hoyt, and Trina Rose. 2011. Predictors of change in self-reported social networks among homeless young people. Journal of Research on Adolescence 21: 827–41. [Google Scholar] [CrossRef] [PubMed]
- Fernandes-Alcantara, A. L. 2013. Runaway and Homeless Youth: Demographics and Programs (No. RL33785). Washington: Congressional Research Service. [Google Scholar]
- Flowers, Claudia P., Takako Chris Oshima, and Nambury S. Raju. 1999. A description and demonstration of the polytomous-DFIT framework. Applied Psychological Measurement 23: 309–26. [Google Scholar] [CrossRef]
- Fulginiti, Anthony, Eric Rice, Hsun-Ta Hsu, Harmony Rhoades, and Hailey Winetrobe. 2016. Risky integration: A social network analysis of network position, exposure, and suicidal ideation among homeless youth. Crisis: The Journal of Crisis Intervention and Suicide Prevention 37: 184–93. [Google Scholar] [CrossRef] [PubMed]
- Gwadz, Marya, Charles M. Cleland, Robert Quiles, David Nish, John Welsh, Lucky S. Michaels, Jose L. Gonzales, Amanda S. Ritchie, and Noelle R. Leonard. 2010. CDC HIV testing guidelines and the rapid and convention testing practices of homeless youth. AIDS Education and Prevention 22: 312–27. [Google Scholar] [CrossRef] [PubMed]
- Hartwell, Stephanie W., and Paul R. Benson. 2007. Social Integration: A Conceptual overview and two case studies. In Mental Health, Social Mirror. Boston: Springer, pp. 329–53. [Google Scholar]
- Henry, Meghan, Rian Watt, Lily Rosenthal, Azim Shivji, Jill Khadduri, and Dennis P. Culhane. 2016. The 2016 Annual Homeless Assessment Report (AHAR) to Congress: Part 1, Point in Time Estimates. Washington: US Department of Housing and Urban Development, Available online: https://www.hudexchange.info/resources/documents/2016-AHAR-Part-1.pdf (accessed on 26 June 2017).
- Holtschneider, Casey. 2016. A part of something: The importance of transitional living programs within a Housing First framework for youth experiencing homelessness. Children and Youth Services Review 65: 204–15. [Google Scholar] [CrossRef]
- Irwin, Jay, Mark LaGory, Ferris Ritchey, and Kevin Fitzpatrick. 2008. Social assets and mental distress among the homeless: Exploring the roles of social support and other forms of social capital on depression. Social Science and Medicine 67: 1935–43. [Google Scholar] [CrossRef] [PubMed]
- Jacobson, Isabel G., Margaret A. K. Ryan, Tomoko I. Hooper, Tyler C. Smith, Paul J. Amoroso, Edward J. Boyko, Gary D. Gackstetter, Timothy S. Wells, and Nicole S. Bell. 2008. Alcohol use and alcohol-related problems before and after military combat deployment. JAMA Journal of the American Medical Association 300: 663–75. [Google Scholar] [CrossRef] [PubMed]
- Kamieniecki, Gregory W. 2001. Prevalence of psychological distress and psychiatric disorders among homeless youth in Australia: A comparative review. Australian and New Zealand Journal of Psychiatry 35: 352–58. [Google Scholar] [CrossRef] [PubMed]
- Kessler, Ronald C., Gavin Andrews, Lisa J. Colpe, Eva Hiripi, Daniel K. Mroczek, S. -L. T. Normand, Ellen E. Walters, and Alan M. Zaslavsky. 2002. Short screening scales to monitor population prevalences and trends in non-specific psychological distress. Psychological Medicine 32: 959–76. [Google Scholar] [CrossRef] [PubMed]
- Kessler, Ronald C., Peggy R. Barker, Lisa J. Colpe, Joan F. Epstein, Joseph C. Gfroerer, Eva V. Hiripi, Mary V. Howes, Sharon-Lise T. Normand, Ronald W. Manderscheid, Ellen E. Walters, and et al. 2003. Screening for serious mental illness in the general population. Archives of General Psychiatry 60: 184–89. [Google Scholar] [CrossRef] [PubMed]
- Kessler, Ronald C., Jennifer Green, Michael J. Gruber, Nancy Sampson, Evelyn Bromet, Marius Cuitan, Toshi A. Furukawa, Oye Gureje, Hristo Hinov, Chi-Yi Hu, and et al. 2010. Screening for serious mental illness in the general population with the K6 screening scale: Results from the WHO World Mental Health (WMH) survey initiative. International Journal of Methods in Psychiatric Research 19: 4–22. [Google Scholar] [CrossRef] [PubMed]
- Kidd, Sean, and Golan Shahar. 2008. Resilience in homeless youth: The key role of self-esteem. American Journal of Orthopsychiatry 78: 163–72. [Google Scholar] [CrossRef] [PubMed]
- Kipke, Michelle D., Susanne B. Montgomery, Thomas R. Simon, and Ellen F. Iverson. 1997. “Substance Abuse” disorders among runaway and homeless youth. Substance Use and Misuse 32: 969–86. [Google Scholar] [CrossRef] [PubMed]
- Marsden, P. V. 1987. Core discussion networks of Americans. American Sociological Review 53: 122–31. [Google Scholar] [CrossRef]
- McCarthy, Bill, and John Hagan. 1992. Surviving on the street: The experiences of homeless youth. Journal of Adolescent Research 7: 412–30. [Google Scholar] [CrossRef]
- Mewton, Louise, Ronald C. Kessler, Tim Slade, Megan Hobbs, Louise Brownhill, Louise Birrell, Zoe Tonks, Maree Teesson, Nicola Newton, Cath Chapman, and et al. 2016. The psychometric properties of the Kessler Psychological Distress Scale (K6) in a general population sample of adolescents. Psychological Assessment 28: 1232–42. [Google Scholar] [CrossRef] [PubMed]
- Moskowitz, Amanda, Judith A. Stein, and Marguerita Lightfoot. 2013. The mediating roles of stress and maladaptive behaviors on self-harm and suicide attempts among runaway and homeless youth. Journal of Youth and Adolescence 42: 1015–27. [Google Scholar] [CrossRef] [PubMed]
- National Coalition for the Homeless. 2017. Youth Homelessness [WWW Document]. Natl. Coalit. Homeless. Available online: http://nationalhomeless.org/issues/youth/ (accessed on 26 June 2017).
- National Health Care for the Homeless Council. 2015. Behavioral Health among Youth Experiencing Homelessness. A Quarterly Research Review of the National HCH Council. Washington: National Health Care for the Homeless Council. [Google Scholar]
- Nyamathi, Adeline M., Ashley Christiani, Folasade Windokun, Tonia Jones, Aaron Strehlow, and Steve Shoptaw. 2005. Hepatitis C virus infection, substance use, and mental illness among homeless youth: A review. AIDS 19: S34–S40. [Google Scholar] [CrossRef] [PubMed]
- Perry, Brea L., and Bernice A. Pescosolido. 2015. Social network activation: The role of health discussion partners in recovery from mental illness. Social Science and Medicine 125: 116–28. [Google Scholar] [CrossRef] [PubMed]
- Perry, Brea L., Erin Pullen, and Bernice A. Pescosolido. 2017. Interactions between patients’ experiences in mental health treatment and lay social network attitudes toward doctors in recovery from mental illness. Network Science, 1–26. [Google Scholar] [CrossRef]
- Pinkerton, John, and Pat Dolan. 2007. Family support, social capital, resilience and adolescent coping. Child & Family Social Work 12: 219–28. [Google Scholar] [CrossRef]
- R Core Team. 2017. R: A Language and Environment for Statistical Computing. Vienna: R Foundation for Statistical Computing, Available online: https://www.R-project.org/ (accessed on 5 February 2017).
- Rew, Lynn, Margaret Taylor-Seehafer, Nancy Y. Thomas, and Ronald D. Yockey. 2001. Correlates of resilience in homeless adolescents. Journal of Nursing Scholarship 33: 33–40. [Google Scholar] [CrossRef] [PubMed]
- Rice, Eric, Norweeta Milburn, Mary Jane Rotheram-Borus, Shelley Mallett, and Doreen Rosenthal. 2005. The effects of peer group network properties on drug use among homeless youth. American Behavioral Scientist 48: 1102–23. [Google Scholar] [CrossRef] [PubMed]
- Rice, Eric, Norweeta G. Milburn, and Mary Jane Rotheram-Borus. 2007. Pro-social and problematic social network influences on HIV/AIDS risk behaviours among newly homeless youth in Los Angeles. AIDS Care 19: 697–704. [Google Scholar] [CrossRef] [PubMed]
- Rice, Eric, Judith A. Stein, and Norweeta Milburn. 2008. Countervailing social network influences on problem behaviors among homeless youth. Journal of Adolescence 31: 625–39. [Google Scholar] [CrossRef] [PubMed]
- Rizopoulos, Dimitris. 2006. ltm: An R package for latent variable modelling and item response theory analyses. Journal of Statistical Software 17: 1–25. [Google Scholar] [CrossRef]
- Samejima, Fumiko. 1969. Estimation of latent ability using a response pattern of graded responses. Psychometrika Monograph Supplement 1: 17. [Google Scholar] [CrossRef]
- Scott, John. 2017. Social Network Analysis. Thousand Oaks: SAGE. [Google Scholar]
- Smith, Kristen P., and Nicholas A. Christakis. 2008. Social networks and health. Annual Review of Sociology 34: 405–29. [Google Scholar] [CrossRef]
- Snyder, Susan M., Robin Hartinger-Saunders, Timothy Brezina, Elizabeth Beck, Eric R. Wright, Nicholas Forge, and Brian E. Bride. 2016. Homeless youth, strain, and justice system involvement: An application of general strain theory. Children and Youth Services Review 62: 90–96. [Google Scholar] [CrossRef]
- Thoits, Peggu A. 2011. Mechanisms linking social ties and support to physical and mental health. Journal of Health and Social Behavior 52: 145–61. [Google Scholar] [CrossRef] [PubMed]
- Toolis, Erin E., and Phillip L. Hammack. 2015. The lived experience of homeless youth: A narrative approach. Qualitative Psychology 2: 50–68. [Google Scholar] [CrossRef]
- Toro, Paul A., Tegan M. Lesperance, and Jordan M. Braciszewski. 2011. The Heterogeneity of Homeless Youth in America: Examining Typologies. Washington: Homelessness Research Institute, Available online: http://www.youthmovingforward.org/wp-content/uploads/2010/07/file_The_Heterogeneity_of_Homeless_Youth_in_America1.pdf (accessed on 26 June 2017).
- Tucker, Joan S., Jianhui Hu, Daniela Golinelli, David P. Kennedy, Harold D. Green, and Suzanne L. Wenzel. 2012. Social network and individual correlates of sexual risk behavior among homeless young men who have sex with men. Journal of Adolescent Health 51: 386–92. [Google Scholar] [CrossRef] [PubMed]
- Tyler, Kimberly A. 2008. Social network characteristics and risky sexual and drug related behaviors among homeless young adults. Social Science Research 37: 673–85. [Google Scholar] [CrossRef] [PubMed]
- Tyler, Kimberly A. 2013. Homeless youths’ HIV risk behaviors with strangers: Investigating the importance of social networks. Archives of Sexual Behavior 42: 1583–91. [Google Scholar] [CrossRef] [PubMed]
- Tyler, Kimberly A., and Lisa A. Melander. 2011. A qualitative study of the formation and composition of social networks among homeless youth. Journal of Research on Adolescence 21: 802–17. [Google Scholar] [CrossRef] [PubMed]
- Tyler, Kimberly A., Sarah L. Akinyemi, and Lisa A. Kort-Butler. 2012. Correlates of service utilization among homeless youth. Children and Youth Services Review 34: 1344–50. [Google Scholar] [CrossRef] [PubMed]
- U.S. Department of Health and Human Services, Family and Youth Services Bureau. 2013. Report to Congress on the Runaway and Homeless Youth Programs Fiscal Years 2010 and 2011; Washington: U.S. Department of Health and Human Services, Family and Youth Services Bureau.
- Unger, Jennifer B., Michelle D. Kipke, Thomas R. Simon, Christine J. Johnson, Susanne B. Montgomery, and Ellen Iverson. 1998. Stress, coping, and social support among homeless youth. Journal of Adolescent Research 13: 134–57. [Google Scholar] [CrossRef]
- Wellman, Barry. 2007. Challenges in collecting personal network data: The nature of personal network analysis. Field Methods 19: 111–15. [Google Scholar] [CrossRef]
- Wenzel, Suzanne, Ian Holloway, Daniela Golinelli, Brett Ewing, Richard Bowman, and Joan Tucker. 2012. Social networks of homeless youth in emerging adulthood. Journal of Youth and Adolescence 41: 561–71. [Google Scholar] [CrossRef] [PubMed]
- Wickham, Hadley. 2009. ggplot2: Elegant Graphics for Data Analysis. New York: Springer. [Google Scholar]
- Wright, E. R., and R. E. Connoley. 2002. Empowering forces: Professional careworkers in the support networks of gay, lesbian, and bisexual youth. In Childcare & Inequality: Rethinking Carework for Children and Youth. Edited by Francesca M. Cancian, Demie Kurz, Andrew S. London, Rebecca Reviere and Mary C. Tuominen. Boston: Routledge-Kegan Paul, pp. 159–73. [Google Scholar]
- Wright, Eric R., Erin Ruel, Morgan Justice Fuoco, Alex Trouteaud, Travis Sanchez, Ana LaBoy, Halley Myers, Kara Tsukerman, Christopher Vidmar, Matthew Gayman, and et al. 2016. Atlanta Youth Count! Homeless Youth Count and Needs Assessment Final Report. Available online: http://atlantayouthcount.weebly.com/uploads/7/9/0/5/79053356/aycna_final_report_may_2016_final.pdf (accessed on 18 June 2016).
| Mean or Proportion | Standard Deviation | |
|---|---|---|
| Mental Health Status | ||
| Probable Severe Mental Illness | 0.28 | - |
| Non-probable Severe Mental Illness | 0.72 | - |
| IRT-Scored Kessler 6 | 9.02 | 4.95 |
| Social Support | ||
| Adults | 0.60 | - |
| Family | 0.60 | - |
| Friends | 0.65 | - |
| Professionals | 0.40 | - |
| Continuous Social Support Measure | 2.99 | 2.05 |
| Demographic Variables | ||
| Age, scaled | 6.50 | 2.56 |
| Black | 0.71 | - |
| Cisgender Woman | 0.33 | - |
| Homeless 2 Months To 6 Months | 0.25 | - |
| Homeless 6 Months To 1 Year | 0.15 | - |
| Homeless More than 1 Year | 0.24 | - |
| Lesbian or Gay | 0.14 | - |
| Transgender | 0.06 | - |
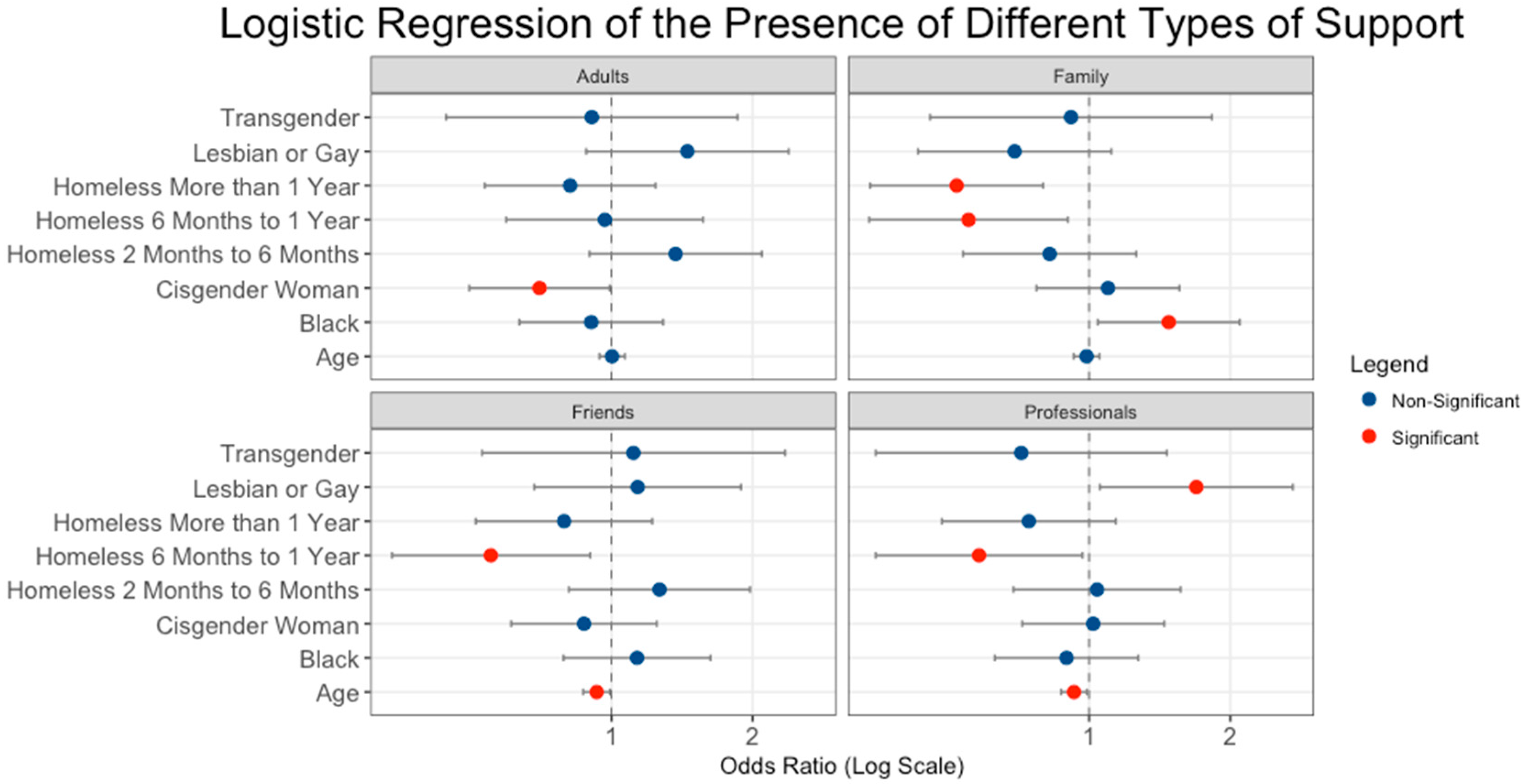
| Adults | Family | Friends | Professionals | |
|---|---|---|---|---|
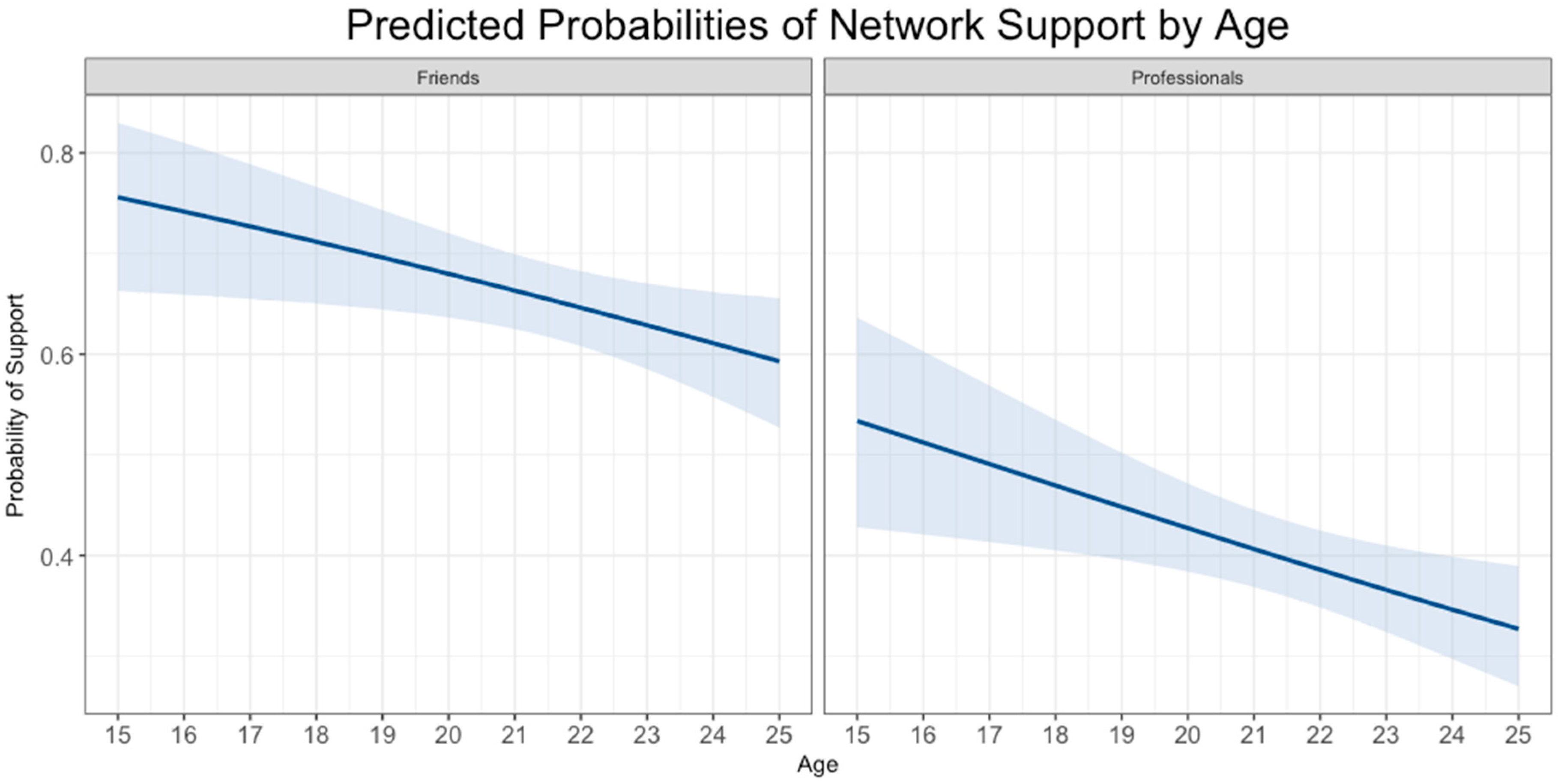
| Age | 1.00 | 0.99 | 0.93 * | 0.93 * |
| (0.94–1.07) | (0.93–1.05) | (0.87–0.99) | (0.87–0.99) | |
| Black | 0.91 | 1.48 * | 1.13 | 0.89 |
| (0.64–1.29) | (1.04–2.09) | (0.79–1.63) | (0.63–1.27) | |
| Cisgender Woman | 0.70 * | 1.10 | 0.87 | 1.02 |
| (0.50–0.99) | (0.77–1.56) | (0.61–1.25) | (0.72–1.45) | |
| Homeless 2 Months To 6 Months | 1.37 | 0.82 | 1.27 | 1.04 |
| (0.90–2.09) | (0.54–1.26) | (0.81–1.98) | (0.69–1.57) | |
| Homeless 6 Months To 1 Year | 0.97 | 0.55 * | 0.55 * | 0.58 * |
| (0.60–1.57) | (0.34–0.90) | (0.34–0.90) | (0.35–0.97) | |
| Homeless More than 1 Year | 0.82 | 0.52 ** | 0.79 | 0.74 |
| (0.54–1.24) | (0.34–0.80) | (0.51–1.22) | (0.49–1.14) | |
| Lesbian or Gay | 1.45 | 0.69 | 1.14 | 1.69 * |
| (0.88–2.39) | (0.43–1.12) | (0.68–1.89) | (1.05–2.72) | |
| Transgender | 0.91 | 0.91 | 1.11 | 0.72 |
| (0.44–1.86) | (0.46–1.83) | (0.53–2.35) | (0.35–1.46) | |
| Pseudo R2 | 0.01 | 0.02 | 0.02 | 0.02 |
| Coefficient | 95% Confidence Interval | |
|---|---|---|
| Intercept | 3.53 *** | (2.98–4.07) |
| Age | −0.05 | (−0.11–0.01) |
| Black | 0.10 | (−0.25–0.44) |
| Cisgender Woman | −0.46 ** | (−0.80–−0.11) |
| Homeless 2 Months To 6 Months | 0.14 | (−0.26–0.55) |
| Homeless 6 Months To 1 Year | −0.58 * | (−1.06–−0.10) |
| Homeless More than 1 Year | −0.40 | (−0.81–0.02) |
| Lesbian or Gay | 0.23 | (−0.24–0.70) |
| Transgender | −0.22 | (−0.91–0.47) |
| R2 | 0.03 |
| Model 1 | Model 2 | |||
|---|---|---|---|---|
| Odds Ratio | 95% Confidence Interval | Odds Ratio | 95% Confidence Interval | |
| Age | 0.99 | (0.92–1.06) | 0.97 | (0.91–1.05) |
| Black | 0.86 | (0.59–1.25) | 0.87 | (0.59–1.27) |
| Cisgender Woman | 1.29 | (0.89–1.87) | 1.21 | (0.83–1.77) |
| Homeless 2 Months To 6 Months | 1.23 | (0.78–1.95) | 1.27 | (0.80–2.01) |
| Homeless 6 Months To 1 Year | 1.80 | (1.08–3.01) | 1.65 | (0.98–2.78) |
| Homeless More than 1 Year | 1.21 | (0.75–1.93) | 1.13 | (0.70–1.82) |
| Lesbian or Gay | 0.86 | (0.51–1.47) | 0.89 | (0.52–1.52) |
| Transgender | 1.99 | (0.98–4.05) | 1.96 | (0.95–4.02) |
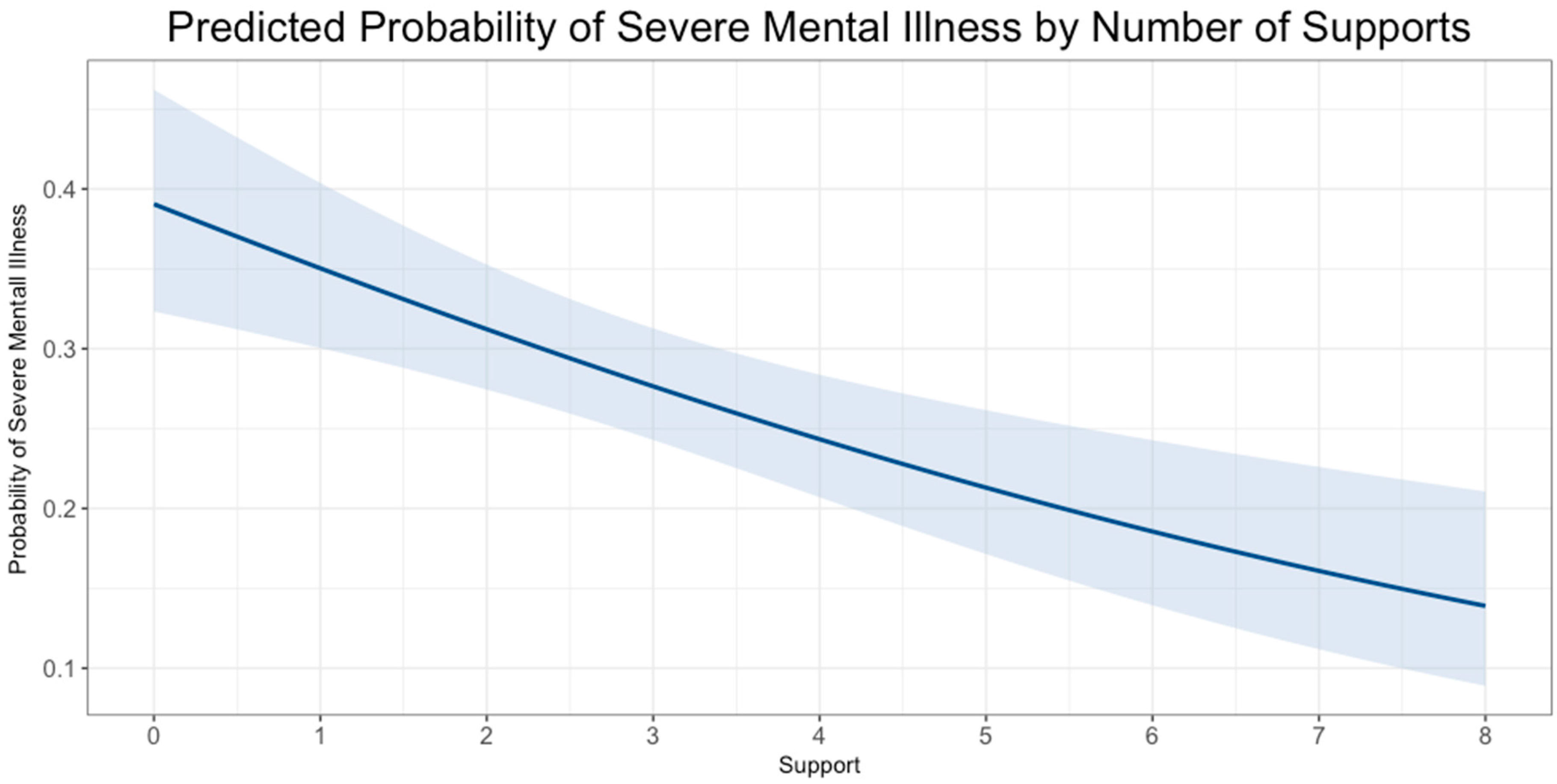
| Social Support Network | 0.85 *** | (0.77–0.93) | ||
| Pseduo R2 | 0.01 | 0.03 | ||
| Model 1 | Model 2 | |||
|---|---|---|---|---|
| Coefficient | 95% Confidence Interval | Coefficient | 95% Confidence Interval | |
| Intercept | 7.92 *** | (6.60–9.23) | 9.08 *** | (7.62–10.53) |
| Age | 0.05 | (−0.09–0.20) | 0.04 | (−0.11–0.19) |
| Black | −0.32 | (−1.16–0.52) | −0.29 | (−1.12–0.54) |
| Cisgender Woman | 1.05 * | (0.25–1.88) | 0.90* | (0.08–1.73) |
| Homeless 2 Months To 6 Months | 0.50 | (−0.49–1.49) | 0.55 | (−0.43–1.53) |
| Homeless 6 Months To 1 Year | 1.31 * | (0.14–2.47) | 1.12 | (−0.04–2.27) |
| Homeless More than 1 Year | 0.84 | (−0.17–1.85) | 0.71 | (−0.29–1.71) |
| Lesbian or Gay | −0.37 | (−1.51–0.77) | −0.29 | (−1.43–0.84) |
| Transgender | 2.39 ** | (0.72–4.06) | 2.32 ** | (0.66–3.97) |
| Social Network Support | −0.33 *** | (−0.51–−0.14) | ||
| R2 | 0.03 | 0.05 | ||
© 2017 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Wright, E.R.; Attell, B.K.; Ruel, E. Social Support Networks and the Mental Health of Runaway and Homeless Youth. Soc. Sci. 2017, 6, 117. https://doi.org/10.3390/socsci6040117
Wright ER, Attell BK, Ruel E. Social Support Networks and the Mental Health of Runaway and Homeless Youth. Social Sciences. 2017; 6(4):117. https://doi.org/10.3390/socsci6040117
Chicago/Turabian StyleWright, Eric R., Brandon K. Attell, and Erin Ruel. 2017. "Social Support Networks and the Mental Health of Runaway and Homeless Youth" Social Sciences 6, no. 4: 117. https://doi.org/10.3390/socsci6040117
APA StyleWright, E. R., Attell, B. K., & Ruel, E. (2017). Social Support Networks and the Mental Health of Runaway and Homeless Youth. Social Sciences, 6(4), 117. https://doi.org/10.3390/socsci6040117






