Abstract
Since at least 2012, UK housing providers (and policy makers) have introduced policies aimed at developing autonomy and independence among service users, through an agenda sometimes referred to as ‘responsibilisation’. This paper considers the role that technologies play in this agenda, through an analysis of how wellbeing and independence are facilitated amongst older social housing tenants. Based on case studies of four supported housing schemes in England, the research considers the capacity to exercise agency amongst older persons, through their willingness and ability to accept technological interventions, and the role of support networks to facilitate independent living. Using the concept of modalities of agency, the research examines the impact of implementing ‘low-level’ assistive technologies in the home, based on the perspectives of residents and staff. The interventions studied were designed to improve social relationships, promote self-sufficiency and support self-managed care (based on the principle that the most effective projects facilitate individual agency). The research findings identified that residents responded differentially to technology, based on their levels of capability, motivation, reluctance and resistance. Whilst the study demonstrated that small technological innovations could have disproportionately positive impacts in improving wellbeing, the research demonstrates the complex nature of agency and limits of responsibility. The paper argues that responsibilisation is part of a wider neoliberal project, where choice and agency are manufactured to create an idealised notion of the autonomous actor (in this case through technology-enabled care). The article argues that a collaborative approach to service provision in which responsibility is shared, via co-managed care, is a more effective means of enhancing agency, than one which advocates a withdrawal of support (in the guise of autonomy).
1. Introduction
The UK government’s introduction of extensive welfare reforms (from at least 2012) has seen social housing providers increasingly engaged in ‘housing plus’ activities, such as income maximisation and other interventions to enhance wellbeing, addressing the social welfare needs of tenants (Blank et al. 2019). A prime objective of these reforms was to extend personal choice and autonomy, encouraging individuals to be accountable for their own behaviours and welfare, with social service providers being co-opted to facilitate behaviour change. There is also a noted tension in the negotiation of planning for ageing between personal responsibility and public intervention (McCall 2022). With respect to responsibilisation in health and social care contexts, technology plays a key role in helping individuals to be self-managers of their own care, thereby (in theory) easing demands on health and social care infrastructure (NHS 2020). There is a sizeable body of work focusing specifically on the impact of ‘digital health technologies’ to improve the support, information and health outcomes of clinically vulnerable populations, and to empower older patients to self-manage their healthcare, improving self-efficacy and ‘self-control’ (Gaikwad and Warren 2009; Chiarini et al. 2013; García-Lizana and Sarría-Santamera 2007). In responding to the needs of older and more vulnerable tenants, supported housing providers have incorporated a range of assistive technologies, including ‘lowlevel’ aids to help with day-to-day living as well as higher-level technology such as remote care services via ‘telecare’ and various forms of mobile digital technology, in the provision of housing services (Varey et al. 2021).
The aim of this article is to examine the role that technology plays in promoting ‘responsibilisation’ in contemporary housing provision and the consequences for older individuals. In exploring the intersections between housing and social care, the study examines how technology can (or should) facilitate agency and independence for older people in residential settings. The article pays specific attention to the importance of social relationships and the role technology-enabled care can play in facilitating wellbeing. The study considers the following questions:
- How can assistive technology support the agency and independence of older residents?
- What role does agency play in accepting technology-enabled care and how is this facilitated through social support networks?
- How effective is responsibilisation in improving wellbeing and independence amongst older residents?
Based on a study of supported housing schemes in England, the paper considers the background to the responsibilisation agenda in health and social care, and its impacts in relation to the introduction of ‘assistive technologies’ within supported housing settings. Section 1 considers how the responsibilisation agenda is practiced in ‘wider-role’ housing functions, focusing on the impact of austerity, an ageing population, and a recent public health crisis during the COVID-19 pandemic. Crucially, this research considers how these wider processes play out at the individual level to consider the extent to which older persons can become empowered to become ‘self-managers’ of care. The empirical material considers the importance of agency in later life and the role of actors who facilitate the use of ‘low-level’ assistive technology in supportive housing. The article demonstrates the limitations of the responsibilisation agenda (at the individual level) and argues that a collaborative approach, based on shared responsibilities and the co-management of care, is more effective than one based purely on autonomy.
2. Background: Responsibilisation, Technology and Co-Management of Care in Supported Housing
The concept of responsibilisation is often situated within a wider agenda of neoliberalism, which as an economic project that calls for the deregulation of markets and the privatisation of services provided by the public sector, such as housing and social welfare. As a political agenda, neoliberalism advocates limiting the role of government in welfare whilst extending its intervention in policing and supporting markets. Civil society under neoliberalism comprises ‘consumer’ citizens, a collection of individuals who compete to pursue their own self-interest (Adams et al. 2019). Individualism is therefore a key tenet of neoliberalist ideology, with the consumer citizen being autonomous, individualised, self-responsible, self-acting, and self-directing (Bondi 2005; Cradock 2007). At a systemic level, the ideal neoliberal individual takes responsibility for their own behaviours (Brown and Baker 2012), and within a health and social care context, does not rely on the state to provide health care and social welfare (O’Malley 2009). Responsibility is imparted on individuals through personal choice and autonomy—it is the means by which citizens participate in their own self-discipline (Trnka and Trundle 2014; White 2002). Service retrenchment is therefore justified as citizens assume greater responsibility for their own welfare.
In the UK context of a shrinking welfare state and a national health system increasingly incapable of meeting the social care needs of an ageing population, some social landlords have widened their service, offering to include a range of social support, focusing on more holistic interventions for social tenants (Power et al. 2014). Housing support, for older renters especially, lies at the interface between health and social care (Blank et al. 2019). In addition to delivering support to older people in mainstream social housing, many social landlords are engaged in the provision of ‘sheltered’ or ‘extra care housing’ for older people (Housing LIN 2015). The scale of supported housing has grown markedly over the past two decades, as national government, local authorities and social housing providers have attempted to respond to increasing demand from an expanding older population (Darton 2022). In the process of growth, the range of models has also become substantially more diverse. However, there are several common features which can be identified, which aim to address age-related issues, including self-contained properties within buildings which are purpose-built or adapted for age/disability-friendly design; those with communal facilities which enable group activities; those with a back-up alarm system and other assistive technologies; those with a restaurant or dining room; and those with some level of staffing on-site or covering multiple sites (Housing LIN 2016). All of these elements are intended to enable people to remain living in this relatively independent setting as they age, thereby avoiding the need to move into residential care. The growth of supported housing is therefore driven by the individual desire to retain independence in later life, but also by budgetary pressures on local authorities, who are responsible for the care costs of low-income households (Darton 2022).
Whilst the above discussion is useful in illustrating the challenges placed on institutions and organisations to promote responsibilisation, analyses at a systemic level often neglect focusing on implications for individuals and communities. Critics of neoliberalism argue that the concept of responsibility ignores the role of social relationships, with individuals being viewed as autonomous rather than socially situated actors (Freeman and Napier 2009). At a conceptual level, a major criticism of ‘responsibilisation’ within the literature on advanced liberalism and governmentality (in which the concept originates) is the over-rationalisation of power and its exercise, which downplays the complex nature of agency and social relationships (Flint 2002). For example, few studies concerning the role of technology in health responsibilisation have acknowledged how older adults use technologies in collaboration with other people, such as family carers (Lindberg et al. 2013; Magnusson et al. 2004; Reeder et al. 2013) and health care professionals (Oudshoorn 2008; Segrelles-Calvo et al. 2016). These studies demonstrate the importance of social context (created by relationships with other people) in relation to health (Wiltshire et al. 2018; Frohlich et al. 2001; Robertson et al. 2022) and illustrate how a co-managed approach to technology-enabled care can be effective. Such studies emphasise the role of collaboration and partnership between individuals, family members, professional carers and others in their support network.
Co-managed approaches call for greater recognition of the mutually constituting impacts that technologies and care services have on each other (including how care is defined within policy discourses). In terms of delivery, co-managed approaches involve designing and implementing services which emphasise a shared understanding of technology-enabled, or perhaps more accurately, technology-mediated care. The research undertaken for this article therefore focusses on such co-managed approaches by paying attention to the ‘hidden work’ of housing support staff, as well as of family and other residents, to support technology-enabled care in residential settings, thereby demonstrating the limited extent to which older and more vulnerable tech users can be expected to be self-managers of care.
3. Research Methods
Using a longitudinal case study approach, data were obtained during a twelve-month period (2021–2022) within four supported housing schemes in England, covering 212 properties with variations in the size of the schemes, the proportion of residents with diagnosed/suspected dementia, and the size/rurality of the place in which the schemes are based. Respondents demonstrated a range of health conditions, including arthritis, mobility and memory problems. The study adopted qualitative research methods to examine the impact of assistive technologies in the home from the perspectives of residents and staff across the four sites. A total of 82 residents and 9 staff participated in person-centred in-depth qualitative interviews over two waves of on-site fieldwork. Interviews lasted between 15 and 60 min. All interviews were audio-recorded and transcribed verbatim, and the analysis was underpinned by a thematic approach. The analysis involved the development of a coding schedule; the data was coded for the factors facilitating or inhibiting the use of technology, focusing on the perceptions of, motivations of and support available to older tech users, as well as support staff, participating in the research. The NVivo software was used to organise the data and structure the analysis. Written consent was obtained from all participants at both stages. The anonymity of participants was ensured by the use of pseudonyms for people and places.
The first wave of interviews took place immediately following the lifting of COVID-19 restrictions from June to October 2021, involving 41 residents (22 females and 19 males, in the age range 40–98, of a mean age of 73.37) and 6 staff. Data were collected in semi-structured interviews around residents’ interest in, and potential need for, new technologies, using the ‘Talking Mats’ visual communication tool. Talking Mats is an interactive, symbol-based tool designed to help residents explore their needs, priorities and what they found challenging day-to-day. Following these interviews, the research team adopted a collaborative, co-production approach, including on-site staff, residents and wider family members, which produced a list of assistive technologies that supported the needs expressed during the wave 1 interviews. Technologies included in this list consisted of higher-tech general digital devices, such as smartphones, tablets and smart speakers, as well as ‘low’-tech aids and adaptations including grab rails or chair risers, and household gadgets such as tin or jar openers and hot water dispensers—often used in combination with each other. Residents were then assisted by the project research team and onsite staff to engage with and try out these technologies before deciding which items they wanted to take to use in their own flats. The aim of this co-production approach was to develop interventions to improve wellbeing and independence that are meaningful, and thus, more effective at supporting communities and individuals to improve their self-managed care. From January to May 2022, we conducted a second wave of data collection to explore the experiences of residents who adopted the provided technologies over time and the impact of the technologies on their lives. Following the wave 1 interviews and prior to wave 2, an additional 41 residents opted to join the study and were assessed for and supplied with assistive technologies by the onsite staff. These new participants also took part in ‘check-in’ interviews with the research team, for a total of 82 residents in this study. In wave 2, 73 residents (45 females and 28 males in the age range 40–98, with a mean age of 71.63) were successfully reinterviewed, representing a level of attrition of approximately 11%, and 7 staff (of which 4 had been interviewed in wave 1). The reasons for residents opting out in wave 2 included the fact that they became deceased (1), were sent to the hospital (1), lacked the capacity (1), became unavailable (3) and were given no tech (3).
4. Theory: Structure and the Modalities of Agency
In order to understand the operation of responsibility and the role that technology can play in wellbeing, it is important to situate agency within a wider structural context. At the macro level, the role of the state, the operation of housing policies and the practices of social landlords will determine the degree to which housing associations adopt technologies, self-management and responsibilisation as a core policy within their services. At a meso level, support staff will determine the success in introducing technologies and support tenants in their ongoing use, particularly when these conflict with the functional abilities and the wants and needs of residents. It is the micro level that is the main focus of the empirical material, demonstrating that the successful adoption of technology in the housing sector is dependent on the skills, capabilities, motivation and willingness of residents to engage with devices.
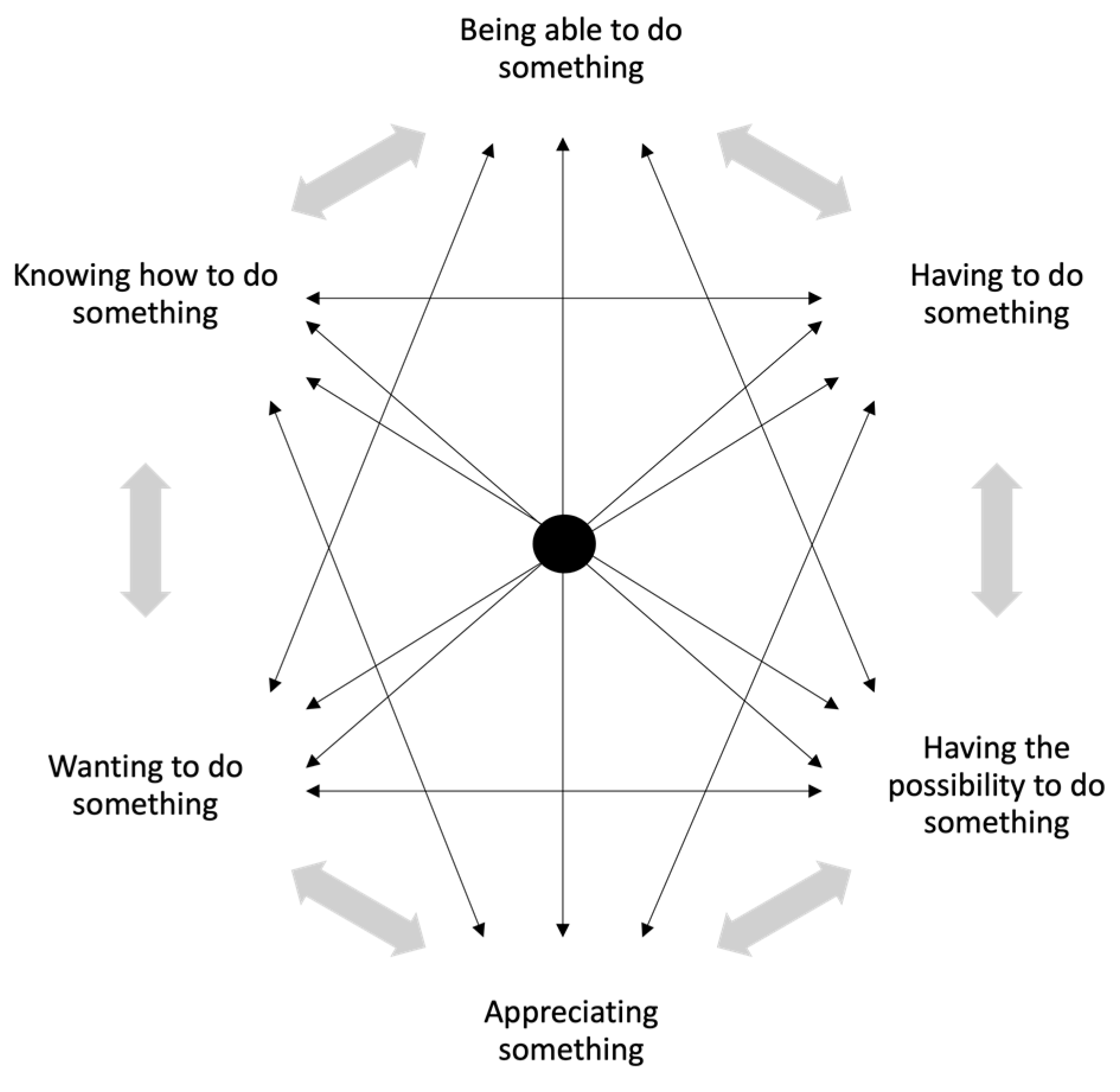
Within this context, the study applies Jyrkämä’s (2007) modalities of agency model, to consider six specific modalities of agency that are in ‘dynamic interaction’ and are ‘context-bound’ (see Figure 1 below). By identifying four key categories that broadly describe the different types of attitudes and approaches participants had towards assistive technology, we argue that the extent to which one is a capable user is determined by their ‘being able to do something’, ‘knowing how to do something’ and ‘appreciating something’, whereas the modalities of agency activated within a motivated user are primarily their ‘wanting to do something’ and ‘having the possibility to do something’. In contrast, one becomes a more reluctant user when one’s agency is constrained or limited to ‘having to do something’. Finally, resistant users are conceived as those who do not express any of these six modalities, instead deploying agency in the choice not to accept or use the assistive technology.
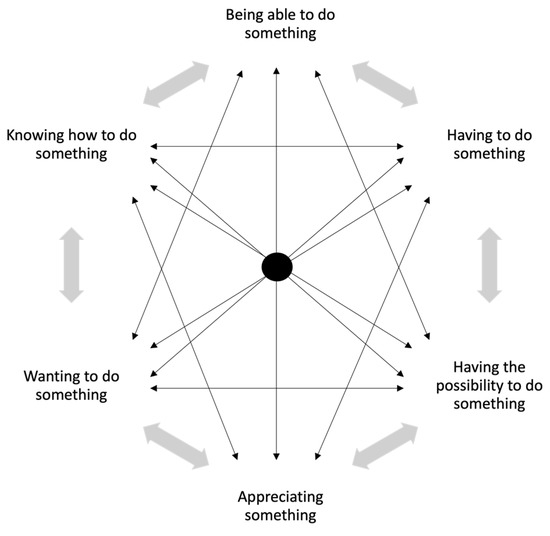
Figure 1.
Modalities of Agency Model (Adapted from Jyrkämä 2007 cited in Sallinen et al. 2015).
5. Results: Understanding Capability, Motivation, Reluctance and Resistance
The limits of responsibilisation lie within the agency of individuals, or the extent to which individuals are capable—or willing—to take responsibility for their own behaviour (Juhila et al. 2017). In this study, when supported housing residents were introduced to technologies enabling self-managed care, responses to the intervention underscored the importance of agency; many were enthusiastic and motivated around technology and embraced the aids in their day-to-day lives—aligning to the ideal ‘responsible self’. Other residents did not embrace technology and did not connect to it as a mechanism to support health or wellbeing self-management.
As the results below demonstrate, this study found that in order to support the independence, autonomy and active agency of older adults, technological solutions must be based on the perceived needs of the individual and the design should be adaptable to one’s functional limitations. The successful implementation of technology-enabled care and support (as defined in terms of acceptance, use and positive impact) is in part attributed to one’s physical, mental and social skills and competencies, but crucially also to one’s choice to use that functioning.
The following discussion therefore focusses on the perceptions, motivations and capabilities of older tech users in supported housing by identifying four key categories that broadly describe the different types of attitudes and approaches that participants had towards ‘technology’: capabilities, motivation, reluctance and resistance.
5.1. The Capable User
The first group of users involved respondents who were comfortable with technological change, who were confident in using technology and who made effective use of their capabilities to enhance their knowledge and skills. These respondents described a high level of motivation, enthusiasm and confidence in both the opportunities offered and their ability to take advantage of available possibilities. It should be noted that these users often understated their own abilities, but were characterised by a willingness to learn new skills, including learning how to use newly introduced technologies. The most confident residents were those who had been able to learn for themselves. Instead of focusing on functional limitations, these respondents highlighted how ‘being able to do something’, physically or mentally, underscored their enthusiasm for adopting the technology.
For those who emphasized ‘knowing how to do something’ as primarily motivating the adoption of tech, the skills and knowledge concerning technology were addressed from two different points of view. On the one hand, some respondents reflected upon their earlier experiences and skills on technological devices. They were also interested in new systems and were eager to have guidance in, for example, computer skills, the use of Skype or new cell phones. For example, Fay emphasised that her knowledge and skills were basic, but that she was helped by a long familiarity with certain kinds of technology: ‘I mean, I’m not brilliant, but I have worked on the computer since I was 17′ (Fay, Site C). On the other hand, some respondents were reserved about their abilities to learn to use new devices. In the beginning, lack of knowledge and unfamiliarity with the devices had caused confusion but with guidance—be it from staff, family or other residents—their use of the devices had become more confident. For example, one respondent commented ‘I always ask [the support worker] or my granddaughter—she’s only six, but she’ll know more than me’ (Julia, Site A). A key theme with more capable users was overcoming an initial fear about their own ability to make effective use of technology in the management of health conditions and day-to-day living:
I think that’s the attitude of a lot of people, that they’re frightened of breaking [digital technology]. You can’t break it, you just switch it off and switch it back on, if you do something wrong, don’t you, you know? But yeah, I think a lot of people are missing out, and interacting with family and stuff like that, you know? I mean, I’ve not seen my family for ages, apart from my daughter, but yes, as I say, just to be able to send them a message.(Julia, Site A)
This group of users sometimes emphasised how their use of technology had become automatic, to the extent that some were no longer able to imagine functioning without assistance. As familiarity and confidence in using the technology increased, so did the expression of ‘appreciation for something’ as the reason for adopting the tech into their everyday lives. Danielle, for instance, felt empowered by her new smartphone in managing her health care and the day-to-day, such as internet banking and shopping: I don’t know how I managed without it [smartphone] to be honest (Danielle, Site A). Other residents made use of technology to assist in their own hobbies and activities, which was important for wellbeing particularly in the context of COVID-19:
I do the basics, like I say, Facebook, YouTube, emailing, messaging on Facebook. But although my wife will tell you that I do spend a lot of time on the iPad, because I’m a saxophonist I listen to saxophone on YouTube, and then because I like art I’m looking into watercolour styles, one thing or another... So there’s lots of things going on in my life which keep me occupied. I find it difficult to get bored.(Ed, Site C)
This evidence illustrates that the perception of technology and its usage is subjective, and that people interpret accessibility and ease of technology differently. Those in this group tended to experience fewer barriers to technology use, including having less need for support and few or no long-term health conditions. More capable users seemed to connect their ‘being able to do something’ or ‘knowing how to do something’ with their choice to incorporate the assistive technology into their day-to-day lives. The most confident in this group included those who had prior experience with digital technology, but also those who received the ‘lower’ forms of tech interventions, such as tin openers, which were perceived as intuitive or self-explanatory in their use. This group generally embraced and expressed great appreciation for the possibilities technology afforded them to live more independently and manage the day-to-day. Often, these more capable users became a locus of support within the home for the other types of users in their peer groups; hence, co-management becomes constituted and embedded through peer networks.
5.2. The Motivated User
The second group included respondents who were motivated to learn new skills. This group included those who were hesitant and sometimes fearful about how to use resources, but who were nevertheless enthusiastic to utilise the support available to increase their facility with new technology. The role of others—family, friends, staff, other residents—are therefore the key points of success or of the unsuccessful take-up of technology for this group in the study. It is not the ‘gadget’ that is key in many ways, but rather the people around the person to facilitate, help and motivate them. As the largest group of respondents, these tech users involved residents who were often fearful of their capability to use technology, but who expressed a willingness to make use of available resources and to improve their skills. Many of these respondents explained they had initially been fearful of using technology but (partly due to the pandemic) had mastered new skills out of necessity (for example, to stay connected with family and friends during lockdown). Their ‘wanting to do something’ was a key motivator for overcoming difficulties in using technology. For example, contact with family members and friends was seen as an essential part of life and some respondents saw that this could and should be enhanced by technology, especially if the family lived far away, as Sean illustrated:
I think that we would like to keep in touch with relatives abroad and so on. They talk about Skype and…Zoom and this face and that face and what have you and we just literally don’t have a clue. I think we have managed once by luck or chance than anything else to actually talk to someone on a video call. But I didn’t even know I was doing it until they popped up and said, ‘oh hi dad, I didn’t know you knew about this stuff’…But, I am looking forward to it, yes. You are never too old to learn are you?.(Sean, Site B)
Many residents were keen to learn technology, but cautious about potential difficulties. Staff, friends and family were particularly important in supporting and motivating, as well as influencing whether or not they ‘wanted to do something’. For example, there was a high degree of fear (particularly with older residents) in using new technologies. As one staff member commented: ‘I completely understand where a lot of our customers are and a lot of it is they’re scared of it anyway, they’re scared’ (Staff member, Site D). Part of this fear was due to the perceived high degree of risk in using services (such as online banking). However, residents who wanted to learn new skills were able to overcome these concerns: I am very interested, and I’d love to be able to get into it yeah, properly and be confident with it…It does make you worry yes, because I know I don’t know what I’m really doing...and that’s really put me off (Whitney, Site C).
‘Wanting to do something’ is linked to motivation and individual objectives in life, whereas ‘having a possibility to do something’ frames the options one may have. A number of initially reluctant users described how they had been persuaded by specific forms of technology (such as physical fitness apps and wearable technology—such as the Fitbit), and consequently became more open to the possibility of using other forms of tech. Technology that was perceived as being easy to operate, or immediately recognised as offering personal benefits, had the impact of making some older tech users more receptive to the idea of assistive technology:
Before I had my gadget, I was very ‘anti’ this because…I wasn’t really prepared to embrace any of this technology. I thought it was for older, weaker people but it’s [fitbit] made me less reluctant to accept the technology that’s available. It’s not a black mark against me. It’s something to improve the quality of my life…. It’s getting over the hurdle of it’s there for my benefit. It’s not there because I’m old and decrepit and can’t get by without it. It’s not that. It just makes my life better (Phillipe, Site C). This comment referred to the way that assistive technology was able to address feelings of inadequacy; for example, one mechanism (a can opener) was described in the following way: ‘it’s not saying you’re rubbish mate, but it’s there to help me. It’s not saying you can’t do it. It just makes it easier’ (Phillipe, Cite C).
Staff described the intensive level of support they initially had to provide to older residents to overcome learning curves with technology, and consequently adopted various strategies in order to more effectively support less capable but nonetheless motivated tech users. The approaches used by staff included pairing similar platforms together (for example, providing an iPhone to a participant who also had an iPad), as well as paying attention to the sequencing of tech intervention (for example, helping to familiarise one with a tablet first and then graduating to something with more complicated functionality, such as a smartphone).
5.3. The Reluctant User
The third group were classified as reluctant users. This group was sceptical about the benefits of technology, were often fearful of change and sometimes displayed resentment about the extent to which they were expected to embrace various aspects of technology. This group comprised those who were initially resistant to using technology, but who had come to accept the necessity of becoming proficient at it, due to the scale of change in contemporary life. Such residents would often describe themselves as having been forced to adapt due to the demands of the pandemic, when they had no other option to ensure they remained in contact with loved ones and friends. This group felt that the consequences of not participating in digital life (for example, being disconnected from loved ones or being unable to manage personal finances) were too great and were no longer a viable choice. Much of this reluctance was attributed to fear, both of their own lack of ability and also of being a victim of online crime. A lack of awareness of how technology works, combined with a fear of making mistakes (which might be catastrophic) contributed to a reluctance in using technology. Having a lack of choice was a common theme amongst interviews with more reluctant users:
You’re not getting a choice anymore. It’s assumed that everybody can do these things with technology, and it’s not right. I mean, I’m 72, and I think I’m fairly computer literate for a 72-year-old. There’s a hell of a lot of people my age and above that who are not. We were brought up in a generation whereby you interacted with people and you spoke to people. But these days, you’re just getting to the stage where you’ve got to embrace the fact that you need technology to progress with anything in life these days.(Bonnie, Site A)
A further cause of trepidation was associated with anxiety about the cognitive demands of learning and using technology (a strong factor amongst older residents). In the ‘having to do something’ modality, the constraints, musts and limitations were clearly articulated. A key theme for this group was the ability to cope with a bewildering—and often overwhelming—level of change. Many residents had experience of using technology, but this experience was often restricted to outdated systems and processes. Such learning curves were often compounded by personal impairments relating to learning difficulties and/or long-term health conditions. Earl, for example, felt limited in the extent to which he can be expected to learn new technology as a result of his advanced age:
I’m not very good at all with technology. I’ve had basic training on computers but that was a long time ago with the old computers …my concentration is not very good…I do find computers difficult to handle. Some of the buttons and the mouse and stuff, I find it difficult to use. But soon as I get help I do it quite a few times, I do find it a bit of a difficulty.(Earl, Site A)
Despite perceptual and physical limitations, these users were seen as amenable to change and could be persuaded if support was offered, as one resident who supports her neighbours with various technical issues explained: ‘My personal opinion is sometimes it’s easier just to say, oh no, I’m not interested, rather than looking into the options and realising how helpful being on the internet can be’ (Julia, Site A). Therefore, the reasons for reluctance towards using technology can range from fears around safety, security, the risk of fraud and the overwhelming pace of change. This evidence supports the need to focus on support for introducing technology and also then support for after technology is introduced. The examples above show clearly that the provision of a computer in itself, for example, will not be sufficient to ensure its effective use.
5.4. The Resistant User
The final group were described as displaying an attitude of hostility and explicit resistance to the use of technology. These respondents were notable for their active choice to refuse tech and exercise agency perhaps in the converse of the modalities discussed (for example not ‘wanting to do something’ or not ‘appreciating something’—although, it is debatable how much one decides to not ‘know how to do something’ or not ‘be able to do something’). They were suspicious of change and were not interested in being given devices (even if for free). This group described themselves as ‘technophobes’ and resented how technology could be used to control and monitor behaviour. This group included residents who expressed a strong antipathy to the demands and expectations of using technology to manage one’s own health and wellbeing. This group included residents who felt that technology was over-intrusive and used at times as an instrument of control (rather than support). For example, some suggested:
‘It’s getting very difficult to have any kind of privacy or life away from technology’.(Paula, Site A)
‘In all honesty, sometimes, because it is so intrusive, you see them and they see you, but you might not have wanted to talk to them’.(Nigel, Site A)
There appeared to be considerable resistance to the lack of choice and an element of perceived compulsion surrounding technology: respondents described being ‘pressured’. Like some more reluctant users, this group also described how they were given no alternative but to use technology, but instead of capitulating, such demands to contemporise further reinforced feelings of resistance:
I feel a bit negative towards it because it’s a big driver in the modern world and I think people spend far too much time and…They could be something less boring instead… I’ve not really been a technology person…I’ve got two computers sitting in a box doing nothing…I’ve got mobile phones but, again, I’m limited as to what I use them on.(Alex, Site A)
Some staff members described residents who were strongly resistant to technology, who resented the element of what they saw as compulsion and who would refuse to be engaged in the process: ‘They were saying that they didn’t want to learn it, they were too old to learn it, they don’t want…another box that needs charging, you know, stuff they just didn’t want to do or were that interested in. A few people said, ‘we know it’s the way of the world, I’m not doing it’ (Staff member, Site D).
The group included residents who were not concerned at their own ability to use technology but wanted to protect their autonomy and choice in whether or not to use online services or digital technologies, expressing a strong preference for face-to-face contact. ‘I’m perfectly capable of using a computer, but I still prefer to speak to somebody. And this seems to be a dying thing at the moment’ (Paula, Site A).
Older residents simply stated that their age was an inherent barrier for to challenges presented by learning technology as they lacked the experience, knowledge, awareness and skills required to master new technology. This attitude that technology was not designed for the needs of an older age profile was commonly expressed. Phrases such as ‘too old’ and ‘too old-fashioned’ were expressed to explain why it was just not possible to be open to the possibility of incorporating technology in their day-to-day life. One resident commented on her own attitude towards technology that she felt was shared by other residents:
I’m too old for stuff like that…I think unfortunately, you’ll find that that is probably the attitude to a lot of people…a lot of them round here, they won’t get involved in anything that involves technology. I haven’t got the answer to why some people will just resist every effort to get them online and other people are open to it.(Julia, Site A)
Some residents were strongly opposed to what they saw as unreasonable demands to use technology, frustrated with a lack of choice and anxious that face-to-face contact would become redundant. For older and more vulnerable residents, the limits of responsibilisation become clearer, as this quote illustrates when a participant reflected on the reasonableness of expecting her elderly neighbour to use technology to self-manage her care:
If you are looking at a ninety-year-old woman, with slight memory problems and mobility issues, and who has never even tried driving a mouse, she probably thinks, a mouse—what is that and I do not want any pets—you know. Trying to get them to remember the specific name of the unit and then the password to get into the account to set it up and how to pair it, these are all words that they do not understand.(Bonnie, Site A)
6. Conclusions: Agency and the Limits of ‘Responsibilisation’
Assistive technology has become well established within the health and social care systems within the UK over the last 20 years, driven by government policies to provide more care with fewer resources. The same is true for the housing sector, which is an often under-recognised but a key partner in supporting the health, wellbeing and independence of older people and the wider aged care sector. Our research challenges discourses which centre on responsibilisation via self-management as a key goal and outcome in the adoption of technology-enabled care in housing.
The research demonstrates that the concept of agency is complex and multifaceted. Seen from the perspective of a neoliberal understanding or agency, the idea of responsibilisation is part of a wider project to marketise public social welfare services (Varey et al. 2021). An idealised notion of the responsible self often underpins an attempt to define independence by policy makers and housing providers as self-management through technological interventions. What is clear in our findings is that co-management and the networks built around a technology which support co-management are the key to its success, rather than the intervention—or gadget—itself. Therefore, independence per se is a misconception. A more sophisticated understanding of agency is needed to understand the limits of responsibility and how technology interventions can support interdependence.
The benefit of Jyrkämä’s (2007) modalities of agency model is to help understand that the acceptance and use of tech is a complex and nuanced matter combining a person’s functionality and associated needs with personal choice, including interests in technology and in the specific things technologies can do for them. The concept of interdependence supports the co-management approach, and centralises wider ageing and/or disability-related person-led support needs. Interdependence as a practice also highlights the idea of technology as a process—not a thing or gadget—in which individuals need support in the set-up, introduction, use, maintenance, and repair of technological interventions. Therefore, technological intervention sits within a wider picture of co-management in which the people, the networks and the wider investment and support make it work in a cycle of interdependence. Initiatives to enable tenants to become responsible self-managers of care need to take into account the interdependence of social networks and social embeddedness of residents—no one is a purely autonomous actor, and as this research demonstrates, there are limitations to the extent to which older and more vulnerable social tenants can be empowered to exercise their individual choice and responsibility. Instead, it should be understood that individuals are bound by social ties, which can (in certain circumstances) be enhanced by technology. The limits of individual autonomy and the responsibilisation agenda should be seen within a setting of societal (including state and public policy) obligations.
There is also clear reluctance and resistance to managing wellbeing and independence via technology support, giving rise to a population who will potentially be left behind as the deployment of technology-based support grows. For these reasons, the question of whether or not housing associations should provide intervention is nuanced. For some reluctant or resistant users, confidence was gained by the availability of support and training in tech, through support with tech from housing staff or from other residents. For these more reluctant users, non-digital interventions such as kitchen implements had significant impacts. However, the resistant group of residents raises further moral and ethical questions and highlights that provision of any type of support cannot be universal, and that tenants should not be compelled to engage. The findings also raise important practical challenges around tech provision at the ground-level—e.g., if providing the tech, organisations also then adopt the risk (e.g., scams or a leakage of sensitive data) created by people being online. Co-managed approaches therefore should have the option to not introduce technology, providing alternative solutions to those unable or unwilling to engage. Ongoing co-management of care therefore provides the interface between housing, health and technology-enabled care needed to bridge health inequalities in older and more vulnerable populations.
Dependence on skills and capabilities in using technology extends beyond the capabilities of residents to include other tenants and front-line housing staff. Even among the motivated and capable user groups, technology adoption and use were shaped by housing staff. Front-line housing staff were crucial and central to the co-management of technology-enabled solutions. Within our successful examples of technology adoption, front-line staff played a central role in identifying solutions appropriate to the needs of each resident. This involved a close attunement to resident wants and needs, working out what solutions and arrangements would work for that specific individual, and then having access to the resources needed to put that solution in place. Much of this work was ‘hidden’ in that it did not feature in job descriptions, role profiles or workload allocations, but was fundamental to the successful deployment of many technologies. Importantly, learning from these experiences was also shared between residents, staff and the housing organisation, developing organisational knowledge about what worked for residents in relation to technology. To support this approach to co-management, developing digital support skills among front-line housing staff, especially with assistive devices that need ongoing maintenance, is required. The presence of skilled staff at the front-line further ensures the building of trust in the technology, establishes a technology support mechanism and, in this project, widened the number of service users willing to try technological interventions. Retaining and developing this organisational knowledge is therefore crucial.
This paper highlights the challenges posed by the ideology of neoliberalism. Although there are key policies supporting ‘digitisation’, technological intervention, and wider infrastructural investment (e.g., the plan for digital health and social care, such provisions are very much under-represented for the housing sector. There is high-level policy encouragement, but investment is minimal and the partnership working context between the housing sector and health and social care is under-resourced and very complex (McCall 2022). Housing associations can effectively provide technology-enabled care; however, this provision needs to supplement social (co-managed) care rather than substitute autonomy and self-management with state support. The responsibilisation agenda is only effective at achieving the empowerment of individuals if it is based on co-management, resource provision and interdependence.
Author Contributions
R.C.S., S.R., G.G., J.L. and V.M. contributed equally to this research. All authors have read and agreed to the published version of the manuscript.
Funding
This research was conducted in partnership with the Stonewater Housing Association and funded by the Longleigh Foundation. The Longleigh Foundation is the independent charitable foundation for the social housing sector, founded by Stonewater. Company number: 9923402/Charity number: 1169016.
Institutional Review Board Statement
The study was conducted in accordance with the Declaration of Helsinki, and approved by the Ethics Committee General University Ethics Panel (GUEP) at the University of Stirling (GUEP (19 20) 955 19/08/20 and GUEP (2021) 1030 01/12/20).
Informed Consent Statement
Informed consent was obtained from all subjects involved in the study.
Data Availability Statement
The data are not publicly available due to confidentiality and anonymity reasons. However, further qualitative data can be found in the full research report and other research outputs on the public website: https://www.stonewater.org/about-us/thought-leadership/invite-project/ accessed on 13 April 2023.
Conflicts of Interest
The authors declare no conflict of interest.
References
- Adams, Glenn, Sara Estrada-Villalta, Daniel Sullivan, and Hazel Rose Markus. 2019. The psychology of neoliberalism and the neoliberalism of psychology. Journal of Social Issues 75: 189–216. [Google Scholar] [CrossRef]
- Blank, Lindsay, Eleanor Holding, Mary Crowder, Sally Butterworth, Ed Ferrari, and Elizabeth Goyder. 2019. Taking preventative health messages into the wider caring professions: The views of housing staff and tenants. Journal of Public Health 41: 674–80. [Google Scholar] [CrossRef] [PubMed]
- Bondi, Liz. 2005. Working the spaces of neoliberal subjectivity: Psychotherapeutic technologies, professionalisation and counselling. Antipode 37: 497–514. [Google Scholar] [CrossRef]
- Brown, Brian, and Sally Baker. 2012. Responsible Citizens: Individuals, Health and Policy under Neoliberalism. London: Anthem Press. [Google Scholar]
- Chiarini, Giovanni, Pradeep Ray, Shahriar Akter, Cristina Masella, and Aura Ganz. 2013. mHealth technologies for chronic diseases and elders: A systematic review. IEEE Journal on Selected Areas in Communications 31: 6–18. [Google Scholar] [CrossRef]
- Cradock, Gerald. 2007. The responsibility dance: Creating neoliberal children. Childhood 14: 153–72. [Google Scholar] [CrossRef]
- Darton, Robin. 2022. Extra care housing: The current state of research and prospects for the future. Social Policy and Society 21: 292–303. [Google Scholar] [CrossRef]
- Flint, John. 2002. Social housing agencies and the governance of anti-social behaviour. Housing Studies 17: 619–37. [Google Scholar] [CrossRef]
- Freeman, Michael, and David Napier. 2009. Law and Anthropology. Oxford: Oxford University Press. [Google Scholar]
- Frohlich, Katherine, Ellen Corin, and Louise Potvin. 2001. A theoretical proposal for the relationship between context and disease. Sociology of Health & Illness 23: 776–97. [Google Scholar]
- Gaikwad, Rekha, and Jim Warren. 2009. The role of home-based information and communications technology interventions in chronic disease management: A systematic literature review. Health Informatics Journal 15: 122–46. [Google Scholar] [CrossRef]
- García-Lizana, Francisca, and Antonio Sarría-Santamera. 2007. New technologies for chronic disease management and control: A systematic review. Journal of Telemedicine and Telecare 13: 62–68. [Google Scholar] [CrossRef]
- Housing LIN. 2015. Extra Care Housing—What Is It in 2015? London: Housing Learning and Improvement Network. [Google Scholar]
- Housing LIN. 2016. Care and Support in Housing with Care for Older People: Policy Technical Brief. London: Housing Learning and Improvement Network. [Google Scholar]
- Juhila, Kirsi, Suvi Raitakari, and Christopher Hall. 2017. Responsibilisation at the Margins of Welfare Services. London: Routledge. [Google Scholar]
- Jyrkämä, Jyrki. 2007. Toimijuus ja toimijatilanteet–aineksia ikääntymisen arjen tutkimiseen. In Vanhuus ja sosiaalityö. Sosiaalityö avuttomuuden ja toimijuuden välissä. Edited by M. Seppänen, A. Kariswto and T. Kröger. Jyväskylä: PS-kustannus, pp. 195–217. [Google Scholar]
- Lindberg, Birgitta, Carina Nilsson, Daniel Zotterman, Siv Söderberg, and Lisa Skär. 2013. Using information and communication technology in home care for communication between patients, family members, and healthcare professionals: A systematic review. International Journal of Telemedicine and Applications 2013: 2. [Google Scholar] [CrossRef] [PubMed]
- Magnusson, Lennart, Elizabeth Hanson, and Martin Borg. 2004. A literature review study of information and communication technology as a support for frail older people living at home and their family carers. Technology and Disability 16: 223–35. [Google Scholar] [CrossRef]
- McCall, Vikki. 2022. Inclusive Living: Ageing, adaptations and future-proofing homes. Buildings and Cities 3: 250–64. [Google Scholar] [CrossRef]
- NHS. 2020. Empower the Person. Available online: https://digital.nhs.uk/about-nhs-digital/our-work/transforming-health-and-care-through-technology/empower-the-person-formerly-domain-a (accessed on 29 November 2022).
- O’Malley, Peter. 2009. Governmentality and Risk: Legal Studies Research Paper No. 09/98. Sydney: Sydney Law School. Available online: https://papers.ssrn.com/sol3/papers.cfm?abstract_id=1478289 (accessed on 26 October 2022).
- Oudshoorn, Nelly. 2008. Diagnosis at a distance: The invisible work of patients and healthcare professionals in cardiac telemonitoring technology. Sociology of Health & Illness 30: 272–88. [Google Scholar]
- Power, Anne, Bert Provan, and Eileen Herdern. 2014. The Impact of Welfare Reform on Social Landlords and Tenants. Joseph Rowntree Foundation. Available online: https://www.jrf.org.uk/report/impact-elfarereform-social-landlords-and-tenants (accessed on 3 November 2022).
- Reeder, Blaine, Ellen Meyer, Amanda Lazar, Shomir Chaudhuri, Hilaire Thompson, and George Demiris. 2013. Framing the evidence for health smart homes and home-based consumer health technologies as a public health intervention for independent aging: A systematic review. International Journal of Medical Informatics 82: 565–79. [Google Scholar] [CrossRef] [PubMed]
- Robertson, Jane, Grant Gibson, Corrine Greasley-Adams, Vikki McCall, Joan Gibson, Janice Mason-Duff, and Ro Pengally. 2022. ‘It gives you a reason to be in this world’: The interdependency of communities, environments and social justice for quality of life in older people. Ageing and Society 42: 539–56. [Google Scholar] [CrossRef]
- Sallinen, Merja, Outi Hentonen, and Anne Kärki. 2015. Technology and active agency of older adults living in service house environment. Disability and Rehabilitation: Assistive Technology 10: 27–31. [Google Scholar] [CrossRef]
- Segrelles-Calvo, Gonzalo, Daniel López-Padilla, and Jose Ignacio de Granda-Orive. 2016. Pros and cons of telemedicine in the management of patients with chronic respiratory diseases. Arch Bronconeumol 52: 575–76. [Google Scholar] [CrossRef]
- Trnka, Susanna, and Catherine Trundle. 2014. Competing responsibilities: Moving beyond neoliberal responsibilisation. Anthropological Forum 24: 136–53. [Google Scholar] [CrossRef]
- Varey, Sandra, Mandy Dixon, Alejandra Hernández, Ceu Mateus, Tom Palmer, and Christine Milligan. 2021. The role of Combinatorial Health Technologies in supporting older people with long-term conditions: Responsibilisation or co-management of healthcare. Social Science & Medicine 269: E113545. [Google Scholar]
- White, Melanie. 2002. Neoliberalism and the rise of the citizen as consumer. In Citizens or Consumers? Social Policy in a Market Society. Edited by Dave Broad and Wayne Antony. Winnipeg: Fernwood Publications, pp. 56–64. [Google Scholar]
- Wiltshire, Gareth, Simone Fullagar, and Clare Stevinson. 2018. Exploring parkrun as a social context for collective health practices: Running with and against the moral imperatives of health responsibilisation. Sociology of Health & Illness 40: 3–17. [Google Scholar]
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2023 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).