A Systematic Review of the Protective and Risk Factors Influencing the Mental Health of Forced Migrants: Implications for Sustainable Intercultural Mental Health Practice
Abstract
:1. Introduction
1.1. Literature Review
1.2. Applying an Ecological Perspective
2. Rational for the Study
3. Materials and Methods
3.1. Design
3.2. Search Strategy
3.3. Eligibility Criteria
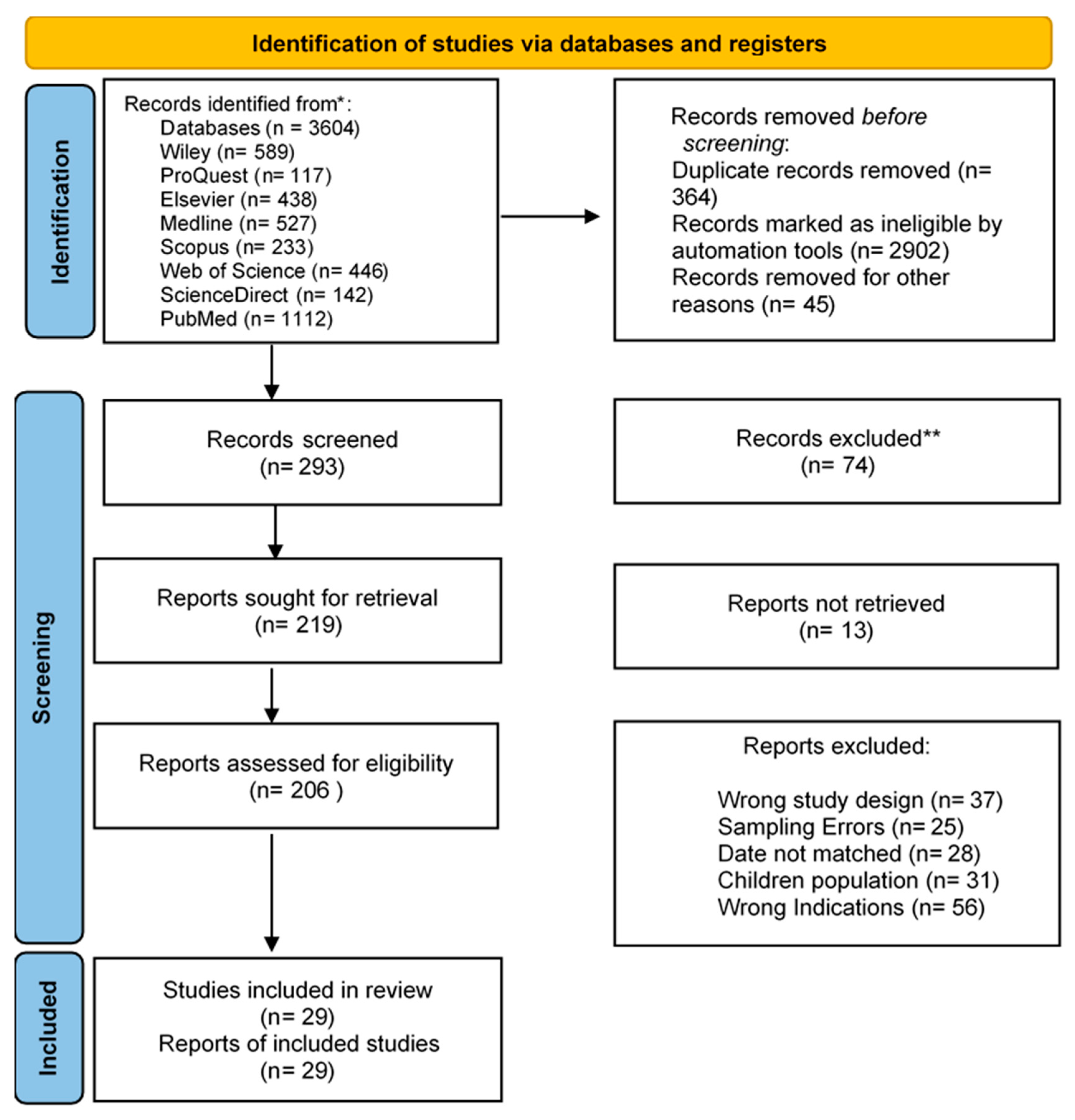
3.4. Selection of the Studies
3.5. Data Extraction
3.6. Quality Assessment
3.7. Data Analysis
4. Findings
4.1. Comparing Risk and Protective Factors across Mental Health Diagnosis
4.2. Risk Factors
4.3. Protective Factors
5. Discussion
5.1. Promoting Mental Health Care—Implications for Sustainable Social Work Practice
5.2. Limitations
6. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Conflicts of Interest
References
- Acarturk, Caren, Mustafa Cetinkaya, Ibrahim Senay, Birgul Gulen, Tamer Aker, and Devon Hinton. 2018. Prevalence and Predictors of Posttraumatic Stress and Depression Symptoms among Syrian Refugees in a Refugee Camp. The Journal of Nervous and Mental Disease 206: 40–45. [Google Scholar] [CrossRef]
- Affleck, William, Umaharan Thamotharampillai, Judy Jeyakumar, and Rob Whitley. 2018. “If One does Not Fulfil His Duties, He must Not be a Man”: Masculinity, Mental Health and Resilience Amongst Sri Lankan Tamil Refugee Men in Canada. Culture, Medicine and Psychiatry 42: 840–61. [Google Scholar] [CrossRef]
- Agrawal, Pooja, and Arjun Krishna Venkatesh. 2016. Refugee Resettlement Patterns and State-Level Health Care Insurance Access in the United States. American Journal of Public Health (1971) 106: 662–63. [Google Scholar] [CrossRef] [PubMed]
- Alemi, Qais, Sigrid James, and Susanne Montgomery. 2016. Contextualizing Afghan Refugee Views of Depression through Narratives of Trauma, Resettlement Stress, and Coping. Transcultural Psychiatry 53: 630–53. [Google Scholar] [CrossRef] [PubMed]
- Alemi, Qais, Susan C. Weller, Susanne Montgomery, and Sigrid James. 2017. Afghan Refugee Explanatory Models of Depression: Exploring Core Cultural Beliefs and Gender Variations. Medical Anthropology Quarterly 31: 177–97. [Google Scholar] [CrossRef] [PubMed]
- Balshem, Howard, Mark Helfand, Holger J. Schünemann, Andrew D. Oxman, Regina Kunz, Jan Brozek, Gunn E. Vist, Yngve Falck-Ytter, Joerg Meerpohl, Susan Norris, and et al. 2011. GRADE Guidelines: 3. Rating the Quality of Evidence. Journal of Clinical Epidemiology 64: 401–6. [Google Scholar] [CrossRef] [PubMed]
- Beiser, Morton, and Feng Hou. 2001. Language Acquisition, Unemployment and Depressive Disorder among Southeast Asian Refugees: A 10-Year Study. Social Science & Medicine (1982) 53: 1321–34. [Google Scholar]
- Bogic, Marija, Anthony Njoku, and Stefan Priebe. 2015. Long-Term Mental Health of War-Refugees: A Systematic Literature Review. BMC International Health and Human Rights 15: 29. [Google Scholar] [CrossRef] [Green Version]
- Bronfenbrenner, Urie. 1979. Contexts of Child Rearing: Problems and Prospects. The American Psychologist 34: 844–50. [Google Scholar] [CrossRef]
- Brown, Menna, Alexander Glendenning, Alice E. Hoon, and Ann John. 2016. Effectiveness of Web-Delivered Acceptance and Commitment Therapy in Relation to Mental Health and Well-being: A Systematic Review and Meta-Analysis. Journal of Medical Internet Research 18: e221. [Google Scholar] [CrossRef] [Green Version]
- Campbell, Mark R., Kay D. Mann, Suzanne Moffatt, Mona Dave, and Mark S. Pearce. 2018. Social Determinants of Emotional Well-being in New Refugees in the UK. Public Health 164: 72–81. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Cantor-Graae, Elizabeth, and Jean-Paul Selten. 2005. Schizophrenia and Migration: A Meta-Analysis and Review. The American Journal of Psychiatry 162: 12–24. [Google Scholar] [CrossRef] [Green Version]
- Carswell, Kenneth, Pennie Blackburn, and Chris Barker. 2011. The Relationship between Trauma, Post-Migration Problems and the Psychological Well-being of Refugees and Asylum Seekers. International Journal of Social Psychiatry 57: 107–19. [Google Scholar] [CrossRef]
- Ceri, Veysi, Zeliha Özlü-Erkilic, Ürün Özer, Tayyib Kadak, Dietmar Winkler, Burak Dogangün, and Türkan Akkaya-Kalayci. 2017. Mental Health Problems of Second Generation Children and Adolescents with Migration Background. International Journal of Psychiatry in Clinical Practice 21: 142–47. [Google Scholar] [CrossRef]
- Chen, Wen, Brian J. Hall, Ling Li, and Andre MN Renzaho. 2017. Pre-Migration and Post-Migration Factors Associated with Mental Health in Humanitarian Migrants in Australia and the Moderation Effect of Post-Migration Stressors: Findings from the First Wave Data of the BNLA Cohort Study. The Lancet. Psychiatry 4: 218–29. [Google Scholar] [CrossRef]
- Chung, Man, Nowf AlQarni, Mariam AlMazrouei, Shamsa Al Muhairi, Mudar Shakra, Britt Mitchell, Sara Al Mazrouei, and Shurooq Al Hashimi. 2018. Posttraumatic Stress Disorder and Psychiatric Co-Morbidity among Syrian Refugees of Different Ages: The Role of Trauma Centrality. Psychiatric Quarterly 89: 909–21. [Google Scholar] [CrossRef] [Green Version]
- Colucci, Erminia, Harry Minas, Josef Szwarc, Carmel Guerra, and Georgia Paxton. 2015. In or out? barriers and facilitators to refugee-background young people accessing mental health services. Transcultural Psychiatry 52: 766–90. [Google Scholar] [CrossRef] [PubMed]
- de Anstiss, Helena, Tahereh Ziaian, Nicholas Procter, Jane Warland, and Peter Baghurst. 2009. Help-Seeking for Mental Health Problems in Young Refugees: A Review of the Literature with Implications for Policy, Practice, and Research. Transcultural Psychiatry 46: 584–607. [Google Scholar] [CrossRef]
- Dietrich, Hans, Radwan Al Ali, Sefik Tagay, Johannes Hebebrand, and Volker Reissner. 2019. Screening for Posttraumatic Stress Disorder in Young Adult Refugees from Syria and Iraq. Comprehensive Psychiatry 90: 73–81. [Google Scholar] [CrossRef] [PubMed]
- Georgiadou, Ekaterini, Ali Zbidat, Gregor M. Schmitt, and Yesim Erim. 2018. Prevalence of Mental Distress among Syrian Refugees with Residence Permission in Germany: A Registry-Based Study. Frontiers in Psychiatry 9: 393. [Google Scholar] [CrossRef] [Green Version]
- Grupp, Freyja, Marie Rose Moro, Urs M. Nater, Sara M. Skandrani, and Ricarda Mewes. 2018. “It’s that Route that Makes Us Sick”: Exploring Lay Beliefs about Causes of Post-Traumatic Stress Disorder among Sub-Saharan African Asylum Seekers in Germany. Frontiers in Psychiatry 9: 628. [Google Scholar] [CrossRef] [PubMed]
- Guyatt, Gordon H., Andrew D. Oxman, Victor Montori, Gunn Vist, Regina Kunz, Jan Brozek, Pablo Alonso-Coello, Ben Djulbegovic, David Atkins, Yngve Falck-Ytter, and et al. 2011. GRADE Guidelines: 5. Rating the Quality of Evidence—publication Bias. Journal of Clinical Epidemiology 64: 1277–82. [Google Scholar] [CrossRef] [PubMed]
- Hagelund, Anniken. 2020. After the Refugee Crisis: Public Discourse and Policy Change in Denmark, Norway and Sweden. Comparative Migration Studies 8: 1–17. [Google Scholar] [CrossRef] [Green Version]
- Hall, Brian J., and Miranda Olff. 2016. Global Mental Health: Trauma and Adversity among Populations in Transition. European Journal of Psychotraumatology 7: 31140–3. [Google Scholar] [CrossRef] [PubMed]
- Henderson, Dawn, and Tiffany Baffour. 2015. Applying a Socio-Ecological Framework to Thematic Analysis using a Statewide Assessment of Disproportionate Minority Contact in the United States. Qualitative Report 20: 1960. [Google Scholar]
- Hocking, Debbie, and Suresh Sundram. 2015. Demoralisation Syndrome does Not Explain the Psychological Profile of Community-Based Asylum-Seekers. Comprehensive Psychiatry 63: 55–64. [Google Scholar] [CrossRef]
- Hollander, Anna-Clara, Henrik Dal, Glyn Lewis, Cecilia Magnusson, James B. Kirkbride, and Christina Dalman. 2016. Refugee Migration and Risk of Schizophrenia and Other Non-Affective Psychoses: Cohort Study of 1.3 Million People in Sweden. BMJ 352: i1030. [Google Scholar] [CrossRef] [Green Version]
- Howie, Hunter, Chuda M. Rijal, and Kerry J. Ressler. 2019. A Review of Epigenetic Contributions to Post-Traumatic Stress Disorder. Dialogues in Clinical Neuroscience 21: 417–28. [Google Scholar]
- Hutchinson, Mary, and Pat Dorsett. 2012. What does the Literature Say about Resilience in Refugee People? Implications for Practice. Journal of Social Inclusion 3: 55–78. [Google Scholar] [CrossRef] [Green Version]
- Hynie, Michaela. 2018. The Social Determinants of Refugee Mental Health in the Post-Migration Context: A Critical Review. Los Angeles: SAGE Publications. [Google Scholar]
- Im, Hyojin, Aidan Ferguson, and Margaret Hunter. 2017. Cultural Translation of Refugee Trauma: Cultural Idioms of Distress among Somali Refugees in Displacement. Transcultural Psychiatry 54: 626–52. [Google Scholar] [CrossRef]
- International Organization for Migration. 2019. IOM Glossary on Migration. Grand-Saconnex: International Organization for Migration, pp. 1–248. [Google Scholar]
- Kandemir, Hasan, Hülya Karataş, Veysi Çeri, Filiz Solmaz, Sultan Kandemir, and Abdullah Solmaz. 2018. Prevalence of War-Related Adverse Events, Depression and Anxiety among Syrian Refugee Children Settled in Turkey. European Child & Adolescent Psychiatry 27: 1513–17. [Google Scholar]
- Kilanowski, Jill F. 2017. Breadth of the Socio-Ecological Model. Journal of Agromedicine 22: 295–97. [Google Scholar] [CrossRef] [PubMed]
- Kim, Robinson. 2014. Voices from the Front Line: Social Work with Refugees and Asylum Seekers in Australia and the UK. The British Journal of Social Work 44: 1602–20. [Google Scholar]
- Kira, Ibrahim Aref, and Pratyusha Tummala-Narra. 2015. Psychotherapy with Refugees: Emerging Paradigm. Journal of Loss & Trauma 20: 449–67. [Google Scholar]
- Lamkaddem, Majda, Karien Stronks, Walter D. Devillé, Miranda Olff, Annette A. M. Gerritsen, and Marie-Louise Essink-Bot. 2014. Course of Post-Traumatic Stress Disorder and Health Care Utilisation among Resettled Refugees in the Netherlands. BMC Psychiatry 14: 90. [Google Scholar] [CrossRef] [Green Version]
- Leiler, Anna, Anna Bjärtå, Johanna Ekdahl, and Elisabet Wasteson. 2019. Mental Health and Quality of Life among Asylum Seekers and Refugees Living in Refugee Housing Facilities in Sweden. Social Psychiatry and Psychiatric Epidemiology 54: 543–51. [Google Scholar] [CrossRef] [Green Version]
- Li, Susan, Belinda Liddell, and Angela Nickerson. 2016. The Relationship between Post-Migration Stress and Psychological Disorders in Refugees and Asylum Seekers. Current Psychiatry Reports 18: 1–9. [Google Scholar] [CrossRef]
- Liberati, Alessandro, Douglas G. Altman, Jennifer Tetzlaff, Cynthia Mulrow, Peter C. Gøtzsche, John P. A. Ioannidis, Mike Clarke, P. J. Devereaux, Jos Kleijnen, and David Moher. 2009. The PRISMA Statement for Reporting Systematic Reviews and Meta-Analyses of Studies that Evaluate Healthcare Interventions: Explanation and Elaboration. BMJ 339: b2700. [Google Scholar] [CrossRef] [Green Version]
- Lillee, Alyssa, Aesen Thambiran, and Jonathan Laugharne. 2015. Evaluating the Mental Health of Recently Arrived Refugee Adults in Western Australia. Journal of Public Mental Health 14: 56–68. [Google Scholar] [CrossRef]
- Lindert, Jutta, and Schinina Guglielmo. 2011. Mental Health of Refugees and Asylum Seekers. In Migration and Health in the European Union. Edited by Rechel Bernd, Mladovsky Philipa, Deville Walter, Rijks Barbara, Petrova-Benedict Raumyana and Mckee Martin. Berkshire: Open University Press, pp. 169–81. [Google Scholar]
- Mallett, Richard, Jessica Hagen-Zanker, Rachel Slater, and Maren Duvendack. 2012. The Benefits and Challenges of using Systematic Reviews in International Development Research. Journal of Development Effectiveness 4: 445–55. [Google Scholar] [CrossRef]
- Marmot, Michael. 2020. Health Equity in England: The Marmot Review 10 Years On. BMJ 368: m693. [Google Scholar] [CrossRef]
- McLeroy, Kenneth R., Daniel Bibeau, Allan Steckler, and Karen Glanz. 1988. An Ecological Perspective on Health Promotion Programs. Health Education Quarterly 15: 351–77. [Google Scholar] [CrossRef] [PubMed]
- Mölsä, Mulki, Marja Tiilikainen, and Raija-Leena Punamäki. 2019. Usage of Healthcare Services and Preference for Mental Healthcare among Older Somali Immigrants in Finland. Ethnicity & Health 24: 607–22. [Google Scholar]
- Moreno, Alejandro, Linda Piwowarczyk, Wayne LaMorte, and Michael Grodin. 2006. Characteristics and Utilization of Primary Care Services in a Torture Rehabilitation Center. Journal of Immigrant and Minority Health 8: 163–71. [Google Scholar] [CrossRef] [PubMed]
- Murray, Kate E., Graham R. Davidson, and Robert D. Schweitzer. 2010. Review of Refugee Mental Health Interventions Following Resettlement: Best Practices and Recommendations. American Journal of Orthopsychiatry 80: 576–85. [Google Scholar] [CrossRef] [Green Version]
- Nickerson, Angela, Richard A. Bryant, Derrick Silove, and Zachary Steel. 2011. A Critical Review of Psychological Treatments of Posttraumatic Stress Disorder in Refugees. Clinical Psychology Review 31: 399–417. [Google Scholar] [CrossRef]
- Omar, Yusuf Sheikh, Justin Kuay, and Can Tuncer. 2017. ‘Putting Your Feet in Gloves Designed for Hands’: Horn of Africa Muslim Men Perspectives in Emotional Wellbeing and Access to Mental Health Services in Australia. International Journal of Culture and Mental Health 10: 376–88. [Google Scholar] [CrossRef]
- Ottisova, Livia, Patrick Smith, Hitesh Shetty, Daniel Stahl, Johnny Downs, and Sian Oram. 2018. Psychological Consequences of Child Trafficking: An Historical Cohort Study of Trafficked Children in Contact with Secondary Mental Health Services. PLoS ONE 13: e0192321. [Google Scholar] [CrossRef] [Green Version]
- Page, Matthew J., Joanne E. McKenzie, Patrick M. Bossuyt, Isabelle Boutron, Tammy C. Hoffmann, Cynthia D. Mulrow, Larissa Shamseer, Jennifer M. Tetzlaff, Elie A. Akl, Sue E. Brennan, and et al. 2021. The PRISMA 2020 Statement: An Updated Guideline for Reporting Systematic Reviews. Systematic Reviews 10: 89. [Google Scholar] [CrossRef]
- Pandya, Samta. 2018. Spirituality for Mental Health and Well-being of Adult Refugees in Europe. Journal of Immigrant and Minority Health 20: 1396–403. [Google Scholar] [CrossRef]
- Perrin, Benjamin. 2010. Just Passing through? International Legal Obligations and Policies of Transit Countries in Combating Trafficking in Persons. European Journal of Criminology 7: 11–27. [Google Scholar] [CrossRef]
- Phillimore, Jenny, and Lisa Goodson. 2006. Problem Or Opportunity? Asylum Seekers, Refugees, Employment and Social Exclusion in Deprived Urban Areas. Urban Studies (Edinburgh, Scotland) 43: 1715–36. [Google Scholar] [CrossRef]
- Poole, Danielle N., Bethany Hedt-Gauthier, Shirley Liao, Nathaniel A. Raymond, and Till Bärnighausen. 2018. Major Depressive Disorder Prevalence and Risk Factors among Syrian Asylum Seekers in Greece. BMC Public Health 18: 908. [Google Scholar] [CrossRef] [Green Version]
- Poudel-Tandukar, Kalpana, Cynthia S. Jacelon, Genevieve E. Chandler, Bhuwan Gautam, and Paula H. Palmer. 2019. Sociocultural Perceptions and Enablers to Seeking Mental Health Support among Bhutanese Refugees in Western Massachusetts. International Quarterly of Community Health Education 39: 135–45. [Google Scholar] [CrossRef] [PubMed]
- Rankopo, Morena J., and Kwaku Osei-Hwedie. 2011. Globalization and Culturally Relevant Social Work: African Perspectives on Indigenization. International Social Work 54: 137–47. [Google Scholar] [CrossRef]
- Rizkalla, Niveen, and Steven P. Segal. 2018. Well-Being and Posttraumatic Growth among Syrian Refugees in Jordan. Journal of Traumatic Stress 31: 213–22. [Google Scholar] [CrossRef]
- Savic, Michael, Anna Chur-Hansen, Mohammad Afzal Mahmood, and Vivienne M. Moore. 2016. ‘We Don’t have to Go and See a Special Person to Solve this Problem’: Trauma, Mental Health Beliefs and Processes for Addressing ‘mental Health Issues’ among Sudanese Refugees in Australia. International Journal of Social Psychiatry 62: 76–83. [Google Scholar] [CrossRef]
- Schünemann, Holger, Andrew Oxman, Jan Brozek, Paul Glasziou, Patrick Bossuyt, Stephanie Chang, Paola Muti, Roman Jaeschke, and Gordon Guyatt. 2009. GRADE: Assessing the Quality of Evidence for Diagnostic Recommendations. ACP Journal Club 149: 2. [Google Scholar] [CrossRef]
- Schweitzer, Robert D., Lyn Vromans, Mark Brough, Mary Asic-Kobe, Ignacio Correa-Velez, Kate Murray, and Caroline Lenette. 2018. Recently Resettled Refugee Women-at-Risk in Australia Evidence High Levels of Psychiatric Symptoms: Individual, Trauma and Post-Migration Factors Predict Outcomes. BMC Medicine 16: 149. [Google Scholar] [CrossRef] [PubMed]
- Segal, Steven, Vicky Khoury, Ramy Salah, and Jess Ghannam. 2018. Contributors to Screening Positive for Mental Illness in Lebanon’s Shatila Palestinian Refugee Camp. The Journal of Nervous and Mental Disease 206: 46–51. [Google Scholar] [CrossRef] [PubMed]
- Shawyer, Frances, Joanne C. Enticott, Andrew A. Block, I-Hao Cheng, and Graham N. Meadows. 2017. The Mental Health Status of Refugees and Asylum Seekers Attending a Refugee Health Clinic Including Comparisons with a Matched Sample of Australian-Born Residents. BMC Psychiatry 17: 76. [Google Scholar] [CrossRef] [Green Version]
- Şimşek, Zeynep, Nebiye Yentur Doni, Nese Gül Hilali, and Gokhan Yildirimkaya. 2018. A Community-Based Survey on Syrian Refugee Women’s Health and its Predictors in Şanliurfa, Turkey. Women & Health 58: 617–31. [Google Scholar] [CrossRef]
- Siriwardhana, Chesmal, Shirwa Sheik Ali, Bayard Roberts, and Robert Stewart. 2014. A Systematic Review of Resilience and Mental Health Outcomes of Conflict-Driven Adult Forced Migrants. Conflict and Health 8: 13. [Google Scholar] [CrossRef] [Green Version]
- Slewa-Younan, Shameran, Anisa Yaser, Maria Gabriela Uribe Guajardo, Haider Mannan, Caroline A. Smith, and Jonathan M. Mond. 2017. The Mental Health and Help-Seeking Behavior of Resettled Afghan Refugees in Australia. International Journal of Mental Health Systems 11: 56. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Szaflarski, Magdalena, and Shawn Bauldry. 2019. The Effects of Perceived Discrimination on Immigrant and Refugee Physical and Mental Health. In Immigration and Health. Bingley: Emerald Publishing Limited, pp. 173–204. [Google Scholar]
- Tinghög, Petter, Andreas Malm, Charlotta Arwidson, Erika Sigvardsdotter, Andreas Lundin, and Fredrik Saboonchi. 2017. Prevalence of Mental Ill Health, Traumas and Post Migration Stress among Refugees from Syria Resettled in Sweden After 2011: A Population-Based Survey. BMJ Open 7: e018899. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Turrini, Giulia, Marianna Purgato, Francesca Ballette, Michela Nosè, Giovanni Ostuzzi, and Corrado Barbui. 2017. Common Mental Disorders in Asylum Seekers and Refugees: Umbrella Review of Prevalence and Intervention Studies. International Journal of Mental Health Systems 11: 51. [Google Scholar] [CrossRef] [PubMed]
- United Nations High Commissioner for Refugees. 2019. Global Trends: Forced Displacement in 2018. Geneva: United Nations High Commissioner for Refugees. [Google Scholar]
- United Nations High Commissioner for Refugees. 2021. Global Trends: Forced Displacement in 2020. Copenhagen: Knowledge Bylanes. [Google Scholar]
- Valtonen, Kathleen. 2008. Social Work and Migration. Abingdon: Routledge. [Google Scholar]
- van Wyk, Sierra, Sierra van Wyk, Robert Schweitzer, and Robert Schweitzer. 2014. A Systematic Review of Naturalistic Interventions in Refugee Populations. Journal of Immigrant and Minority Health 16: 968–77. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Vitale, Agata, and Judy Ryde. 2016. Promoting Male Refugees’ Mental Health After they have been Granted Leave to Remain (Refugee Status). The International Journal of Mental Health Promotion 18: 106–25. [Google Scholar] [CrossRef]
- Watters, Charles. 2001. Emerging Paradigms in the Mental Health Care of Refugees. Social Science & Medicine (1982) 52: 1709–18. [Google Scholar]
- Wong, William Chi Wai, Sealing Cheung, Heidi Yin Hai Miu, Julie Chen, Kelley Ann Loper, and Eleanor Holroyd. 2017. Mental Health of African Asylum-Seekers and Refugees in Hong Kong: Using the Social Determinants of Health Framework. BMC Public Health 17: 153. [Google Scholar] [CrossRef] [Green Version]
- Wood, Tamara. 2019. Who is a Refugee in Africa? A Principled Framework for Interpreting and Applying Africa’s Expanded Refugee Definition. International Journal of Refugee Law 31: 290–320. [Google Scholar] [CrossRef]
- Yaser, Anisa, Shameran Slewa-Younan, Caroline A. Smith, Rebecca E. Olson, Maria Gabriela Uribe Guajardo, and Jonathan Mond. 2016. Beliefs and Knowledge about Post-Traumatic Stress Disorder Amongst Resettled Afghan Refugees in Australia. International Journal of Mental Health Systems 10: 31. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Yassin, Nasser, Nasser Yassin, Asma Taha, Asma Taha, Zeina Ghantous, Zeina Ghantous, Mia Atoui, Mia Atoui, Fabio Forgione, and Fabio Forgione. 2018. Evaluating a Mental Health Program for Palestinian Refugees in Lebanon. Journal of Immigrant and Minority Health 20: 388–98. [Google Scholar] [CrossRef]
- Yu, Shieun, Jungeun Jang, Jin-Won Noh, Young Dae Kwon, Hyunchun Park, and Jong-Min Woo. 2018. What is it to be Mentally Healthy from the North Korean Refugees’ Perspective?: Qualitative Research on the Changes in Mental Health Awareness among the North Korean Refugees. Psychiatry Investigation 15: 1019–29. [Google Scholar] [CrossRef]
| N | Author (s) Country | Time Period | Sampling Method | Interview Method | Study Population | Sample Size | Age Range | Theoretical Framework | Protective Factors | Risk Factors |
|---|---|---|---|---|---|---|---|---|---|---|
| 1 | (Page et al. 2021; Affleck et al. 2018) Canada | 2012–2016 | Convenience Snowball | Semi-structured | Sri Lankan Tamil refugee men | 33 | 20–60 | Grounded Theory | Participating in religious rituals, meditation, adherence to familial and community duties | Inability to protect family members, inability to fulfill cultural duties, inability to perform social roles, Un/Uder-employment, inner-family conflicts |
| 2 | (Alemi et al. 2017) USA | July–October 2012 | Snowball | Semi-structure | Afghan refugees & asylum seekers | 18 = (11) males, (7) females | 36–71 | Cutural Consensus Analysis | Family reunification, community support, prayers, successfulness of the children | Imprisonment of family members, arbitrary home invasions, constant fears of being killed or maltreated, harsh fleeing path, abrupt separation from family-cultural adjustment issues, fear of deportation, language learning barriers, intergenerational challenges with children, unemployment, cultural insensitiveness of social services, losing culture and identity |
| 3 | (Im et al. 2017) Kenya | Unknown | Purposive | Semi-structure and focus groups | Somali refugees | 15 key informants, 31 focus group participants | 18–56 | Kleinman’s (1991) Explanatory Approach | Counseling, job opportunities, mindfulness exercises, socializing, prayers, personal reflections, | lack of educational opportunities, work and decent life, isolation, daily physical health issues, distressing events, unfulfilled desires. insufficient means of support, losing loved ones, community violence |
| 4 | (Omar et al. 2017) Astralia | 2013–2014 | Purposive | Semi-structure and focus groups | Muslim refugees from Somalia, Eritrea, Ethiopia, and Djibouti | 36 | 18–60 | None (Inductive Ethnographic Analysis) | Prayer, confidence in Allah, family and community support, cultural rehabilitation methods (visiting African environment) | Unemployment, underemployment, intercultural conflicts in the host country, religious boundaries, inability to support families overseas, lack of mental health literacy, doubt in identifies treatment strategies (faith-based) treatments, |
| 5 | (Savic et al. 2016) Australia | Unknown | Unknown | Semi-structure | Refugees, health service providers | 45 | +18 | None (Inductive Framework Approach) | Community counselling, community supports | Pre-migration experiences e.g., exposure to violence, rape, loss of loved ones, distrust of western mental health services, medicalized nature of western mental health services, stigmatization of mental health issues, incompatibility of needs and offered mental health services |
| 6 | (Poudel-Tandukar et al. 2019) USA | Unknown | Convenience Snowball | Focus groups | Bhutanese refugees | 67 | +18 | PEN-3 Cultural Model | Community supports, sharing problems with peers, cultural empowerments and raising awareness | language learning issues, decreased support systems, increased responsibilities in the host countries, socio-economic disadvantages, lack of access to services, change in family dynamics, discrimination, stigmatization |
| 7 | (Yaser et al. 2016) Australia | 2015–2016 | Convenience Snowball | Semi-structure | Afghan Refugees | 150 = (74) males, (76) females | 20–45 | The Mental Health Literacy | Improving diet or exercise, raising self-awareness, psychotherapy focusing on the past events, finding new hobbies, physical activity, socializing, meditation, herbal medication, | None |
| 8 | (Yassin et al. 2018) Lebanon | August–November 2015 | Convnience | Semi-structure | Palestinian refugees | 49 = (28) refugees, (11) service providers, (10) local community representatives | 24–58 | Inductive Thematic Content Analysis | Easy access to services, home visits of social workers, individual based treatments, raising awareness of refugees about mental health, access to the history of mental health issues of refugees, sustainability of the mental health services, prompt access to mental health services upon entry to the country | None |
| 9 | (Yu et al. 2018) South Korea | July–August 2013 | Purposive | Semi-structure | North Korean refugees | 10 = (8) females (2) males | 20–69 | None (Inductive Qualitative Analysis) | Prompt treatment upon arrival, raised self-awareness, counselling | Absence of mental health awareness, issues of survival, stigmatization, lack of access to mental health services, trauma experienced during the escape, cultural encounter shocks, isolation and lose identity |
| 10 | (Vitale and Ryde 2016) U.K. | 2015 | Purposive | Semi-structure | Refugees (Iraq-Sudan-Iran-Eritrea-Morocco-Somalia) | 9 | 29–62 | None (Exploratory and inductive) | Voluntary works, target oriented work trainings | Stress of deportation, asylum seeking process, sense of powerlessness, confinement in the detention centers, inadequate supports, feelings of re-traumatization, un/underemployment, high expectations upon arrival, inadequate means of living, lack of practical information, lack of integration in the host community, inability to establish new networks, cultural barriers, inadequate mental health services, no opportunities to be an active citizen |
| N | Author (s) Country | Time Period | Methodology | Study Population | Sample Size | Age Range | Theoretical Framework | Protective Factors | Risk Factors |
|---|---|---|---|---|---|---|---|---|---|
| 11 | (Poole et al. 2018) Greece | January 2017 | Survey | Syrian Refugees | 135 | 18–61 | Patient Health Questionnaire-8 (PHQ-8) | Not mentioned | Gender (being women), having children, increased time in the asylum process |
| 12 | (Chung et al. 2018) Turkey, Sweden | 2017 | Survey | Syrian Refugees | 1197 (482 females, 715 males) | +18 | Centrality of Event Scale, Harvard Trauma Questionnaire, General Health Questionnaire-28 | Age (younger refugees are more resilient), stable relationship with community, employment, social networks | Location of resettlement, came alone of with family, having less community networks |
| 13 | (Hocking and Sundram 2015) Australia | Not metioned | Survey | Refugees (n = 33) and asylum seekers (n = 98) form Zimbabwe, Afghanistan, Iran, Iraq, Lebanon, Pakistan, Sri Lanka | 131 | +18 | The Harvard Trauma Questionnaire-Revised (HTQ) and the Hopkins Symptom Checklist-25 (HSCL), Post-Migration Living Difficulties Checklist (PMLDC) | Social networks, employment | Gender, age, social isolation, low socio-economic status, family separation, unclear residence status, detention experience, mode of arrival |
| 14 | (Campbell et al. 2018) U.K. | 2005–2007 | Longitudinal survey | Refugees | 5678 | +18 | Health Survey Questionnaire | Involvement in community networks, easy access to healthcare services | unemployment, language barriers, unsatisfactory accommodation, being victims of discrimination, infrequent contact with relatives |
| 15 | (Şimşek et al. 2018) Turkey | 2015 | Cross-sectional, interview | Refugees | 458 = females, 15–49 years old | 15–49 | Reproductive Health Assessment Toolkit for Conflict-Affected Women, General Health Questionnaire 12 | social support, community-based and culturally sensitive health education programs, inclusion of mental health care within basic primary care services | Household size, difficulty to get health services |
| 16 | (Dietrich et al. 2019) Germany | Not mentioned | Interview, survey | Refugees from Syria and Iraq | 2057 | 18–24.9 | Essen Trauma Inventory, Short Screening Scale for Posttraumatic Stress Disorder | social support and networks, higher education | Experience of violence, poor housing and sense of insecurity |
| 17 | (Georgiadou et al. 2018) Germany | Not metioned | Survey | Syrian refugees | 518 | 18–63 | Essen Trauma Inventory, Patient Health Questionnaire—Depression Module (PHQ-9), Generalized Anxiety Disorder (GAD-7) | Inclusive welfare system | Death of a loved one, age, shorter validity of residence permit, longer duration of asylum procedure, poor economic conditions |
| 18 | (Schweitzer et al. 2018) Australia | 2013–2015 | Cross-sectional survey | Refugees | 104 | 18–70 | Harvard Trauma Questionnaire (HTQ), Hopkins Symptom Checklist (HSCL-37), Post-migration Living Difficulties Checklist (PMLD) | Access to health and welfare services, improved pre-arrival information about the host societies | Traumatic experiences, racial discrimination |
| 19 | (Segal et al. 2018) Lebanon | 2012–2013 | Survey, interview | Palestinian refugees | 254 | 18–89 | Primary Care Posttraumatic Stress Disorder (PTSD), Kessler-6 | Housing stability, economically gainful employment, social networks, immediate access to mental health clinics | Traumatic experiences, human right violations |
| 20 | (Grupp et al. 2018) Germany | Not mentioned | Survey, focus groups | African refugees, German population | 239 | 18–54 | Revised Illness Perception Questionnaire (IPQ-R) | Praying, ability to fulfill religious rituals | Isolation, Intergenerational conflicts |
| 21 | (Kandemir et al. 2018) Turkey | Not mentioned | Survey | Syrian refugees | 355 | Mean: 11 (SD: 3.67) | Children’s Depression Inventory, Screen for Child Anxiety Related Disorders | Social and welfare supports, education, social networks | Traumatic experiences, gender, proper housing, enough food, experiences of discrimination and racism |
| 22 | (Shawyer et al. 2017) Australia | Not mentioned | Survey | Refugees, and asylum-seekers | 135 | 18–66 | Kessler-10 (K10), PTSD-8 | Culturally responsive mental health services, early mental health assessments and treatments | Human right violations, stressful migration experiences, cultural and language barriers to get access to mental health services, country of origin |
| 23 | (Slewa-Younan et al. 2017) Australia | 2013 | Interview, survey | Afghan refugees | 150 | Mean: 32.8 (SD: 12.2) | Hopkins Symptoms Check List (HSCL-25), Afghan War Experience Scale (AWES) | Early intervention programs | Past traumatic experiences |
| 24 | (Tinghög et al. 2017) Sweden | 2011–2013 | Cross-sectional survey | Syrian refugees | 1215 | 18–64 | Hopkins Symptom Checklist (HSCL-25), Harvard Trauma Questionnaire (HTQ), WHO-5 Well-being Index | Reunion with family members | Gender, traumatic experiences, lower education, Isolation in host society, ethnic discrimination |
| 25 | (Lillee et al. 2015) Australia | Not mentioned | Survey | Refugees | 300 | 18–70 | The Kessler Psychological Distress Scale (K10), General Health Questionnaire (GHQ-12) | Routine use of mental health services, culturally sensitive mental health care | Marital status, having more children, past traumatic events, stigmatization, |
| 26 | (Leiler et al. 2019) Sweden | Not mentioned | Survey, interview | refugees and asylum seekers | 510 | +18 | Patient Health Questionnaire-9, General Anxiety Disorder 7, Primary Care PTSD Screen, WHOQOL-BREF | Safety, access to health care upon arrival, shortening asylum process | unclear residence permit status, poor neighborhoods |
| 27 | (Rizkalla and Segal 2018) Jordan | 2014–2016 | Survey | Syrian refugees | 250 | 16–75 | Harvard Trauma Questionnaire, War Events Questionnaire, K6, The PTGI, The HTQ | Active NGOs, refugee-friendly mental health services | Traumatic events, un/ underemployment, poor neighborhood disadvantages |
| 28 | (Acarturk et al. 2018) Turkey | March–May 2013 | Survey, interview | Syrian refugees | 781 | Mean: 35.2 (SD: 11) | Impact of Event Scale–Revised, Beck Depression Inventory | Inclusive public health policies | Traumatic events, losing sources of income, gender, living in camps |
| 29 | (Pandya 2018) Europe | Not mentioned | Survey | Refugees | 4504 | +30 | Trauma Screening Questionnaire (TSQ), Life Orientation Test-revised (LOT-R), Mental Health Inventory-38 (MHI-38) | Voluntary participation in mental health programs, self-practice willingness, spirituality, group-based interventions | Country of origin, refugee status duration, gender, past traumatic experiences |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2021 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Farahani, H.; Joubert, N.; Anand, J.C.; Toikko, T.; Tavakol, M. A Systematic Review of the Protective and Risk Factors Influencing the Mental Health of Forced Migrants: Implications for Sustainable Intercultural Mental Health Practice. Soc. Sci. 2021, 10, 334. https://doi.org/10.3390/socsci10090334
Farahani H, Joubert N, Anand JC, Toikko T, Tavakol M. A Systematic Review of the Protective and Risk Factors Influencing the Mental Health of Forced Migrants: Implications for Sustainable Intercultural Mental Health Practice. Social Sciences. 2021; 10(9):334. https://doi.org/10.3390/socsci10090334
Chicago/Turabian StyleFarahani, Hadi, Natalie Joubert, Janet Carter Anand, Timo Toikko, and Mohamad Tavakol. 2021. "A Systematic Review of the Protective and Risk Factors Influencing the Mental Health of Forced Migrants: Implications for Sustainable Intercultural Mental Health Practice" Social Sciences 10, no. 9: 334. https://doi.org/10.3390/socsci10090334
APA StyleFarahani, H., Joubert, N., Anand, J. C., Toikko, T., & Tavakol, M. (2021). A Systematic Review of the Protective and Risk Factors Influencing the Mental Health of Forced Migrants: Implications for Sustainable Intercultural Mental Health Practice. Social Sciences, 10(9), 334. https://doi.org/10.3390/socsci10090334






