The Prospects of Zinc as a Structural Material for Biodegradable Implants—A Review Paper
Abstract
:1. Introduction
- Similar to magnesium and iron, zinc is an essential trace element in the human body. It is a component of more than 300 enzymes and an even greater number of other proteins, highlighting its indispensable role in human health. Optimal nucleic acid and protein metabolism, as well as cell growth, division, and function, require sufficient availability of zinc [30,35]. From this perspective, zinc ions released from the implant during the degradation phase could integrate into the normal metabolic activity of the host without producing systemic toxic side effects [36].
- Zinc exhibits high chemical activity, with an electrode potential (−0.762 V) falling between that of magnesium (−2.372 V) and iron (−0.444 V) [36,37,38]. Pure zinc metal, therefore, exhibits moderate degradation rates (faster than the slowly degrading Fe and its alloys, but slower than the rapidly degrading Mg and its alloys) due to passive layers of moderate stability, formed by corrosion products [19,39,40,41].
2. Zinc in the Human Body
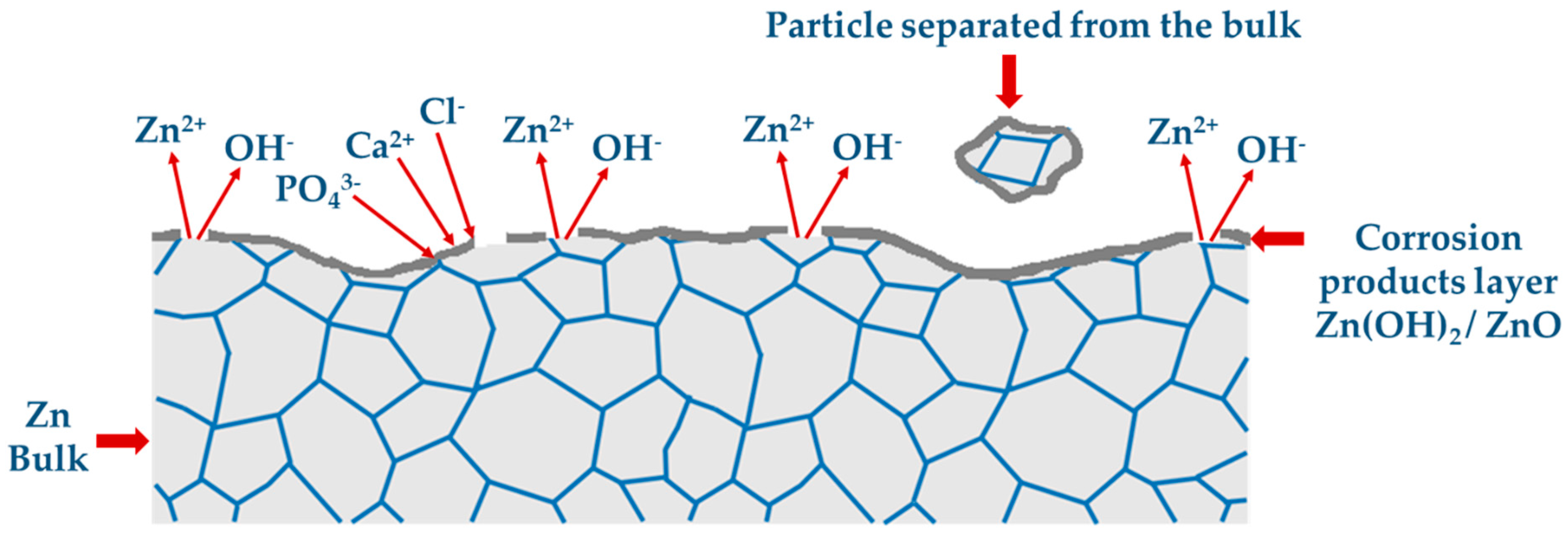
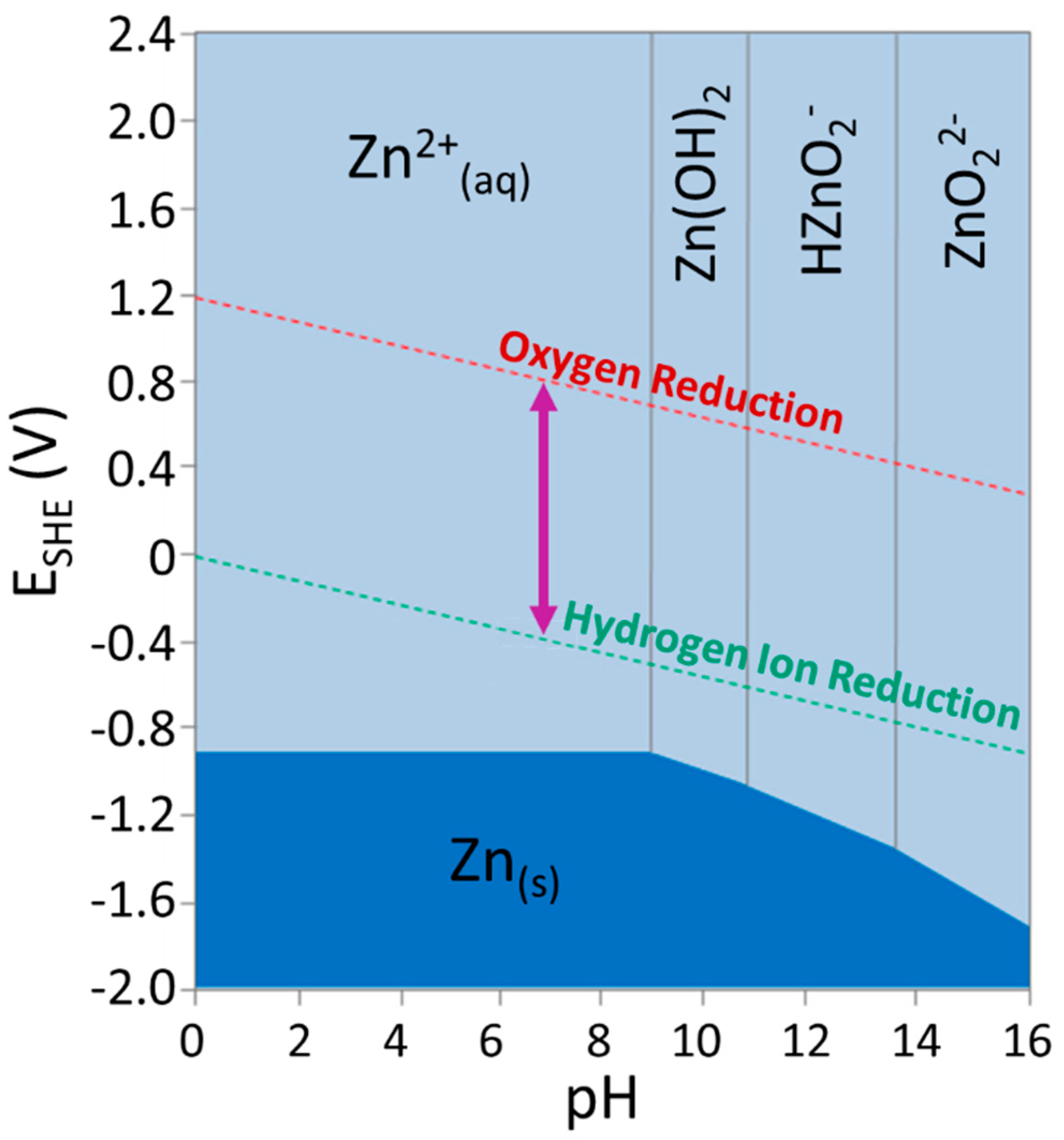
3. Corrosion Behavior of Zinc in the Physiological Environment
4. Biocompatibility and Biological Performances of Zinc and Evaluated Zinc Alloys
4.1. Pure Zinc
4.1.1. In Vitro Examination
4.1.2. In Vivo Examination
4.2. Zinc Alloys
5. Mechanical Properties of Zinc Alloys
6. Concluding Remarks and Perspectives
Author Contributions
Conflicts of Interest
References
- Katarivas Levy, G.; Aghion, E. Influence of heat treatment temperature on corrosion characteristics of biodegradable EW10X04 Mg alloy coated with Nd. Adv. Eng. Mater. 2016, 18, 269–276. [Google Scholar] [CrossRef]
- Holzapfel, B.M.; Reichert, J.C.; Schantz, J.-T.; Gbureck, U.; Rackwitz, L.; Nöth, U.; Jakob, F.; Rudert, M.; Groll, J.; Hutmacher, D.W. How smart do biomaterials need to be? A translational science and clinical point of view. Adv. Drug Deliv. Rev. 2013, 65, 581–603. [Google Scholar] [CrossRef] [PubMed]
- Shen, C.; Liu, X.; Fan, B.; Lan, P.; Zhou, F.; Li, X.; Wang, H.; Xiao, X.; Li, L.; Zhao, S. Mechanical properties, in vitro degradation behavior, hemocompatibility and cytotoxicity evaluation of Zn–1.2 Mg alloy for biodegradable implants. RSC Adv. 2016, 6, 86410–86419. [Google Scholar] [CrossRef]
- Niinomi, M. Metallic biomaterials. J. Artif. Organs 2008, 11, 105–110. [Google Scholar] [CrossRef] [PubMed]
- Katarivas Levy, G.; Ventura, Y.; Goldman, J.; Vago, R.; Aghion, E. Cytotoxic characteristics of biodegradable EW10X04 Mg alloy after nd coating and subsequent heat treatment. Mater. Sci. Eng. C 2016, 62, 752–761. [Google Scholar] [CrossRef] [PubMed]
- Pospíšilová, I.; Soukupová, V.; Vojtěch, D. Influence of calcium on the structure and mechanical properties of biodegradable zinc alloys. In Materials Science Forum; Trans Tech Publication Ltd.: Stafa-Zurich, Switzerland, 2017; pp. 400–403. [Google Scholar]
- Aghion, E.; Levy, G.; Ovadia, S. In Vivo behavior of biodegradable Mg–Nd–Y–Zr–Ca alloy. J. Mater. Sci. 2012, 23, 805–812. [Google Scholar] [CrossRef] [PubMed]
- Zheng, Y.; Gu, X.; Witte, F. Biodegradable metals. Mater. Sci. Eng. C 2014, 77, 1–34. [Google Scholar] [CrossRef]
- Mostaed, E.; Sikora-Jasinska, M.; Mostaed, A.; Loffredo, S.; Demir, A.; Previtali, B.; Mantovani, D.; Beanland, R.; Vedani, M. Novel zn-based alloys for biodegradable stent applications: Design, development and in vitro degradation. J. Mech. Behav. Biomed. Mater. 2016, 60, 581–602. [Google Scholar] [CrossRef] [PubMed]
- Gu, X.-N.; Zheng, Y.-F. A review on magnesium alloys as biodegradable materials. Front. Mater. Sci. China 2010, 4, 111–115. [Google Scholar] [CrossRef]
- Witte, F.; Hort, N.; Vogt, C.; Cohen, S.; Kainer, K.U.; Willumeit, R.; Feyerabend, F. Degradable biomaterials based on magnesium corrosion. Curr. Opin. Solid State Mater. Sci. 2008, 12, 63–72. [Google Scholar] [CrossRef]
- Jablonská, E.; Vojtěch, D.; Fousová, M.; Kubásek, J.; Lipov, J.; Fojt, J.; Ruml, T. Influence of surface pre-treatment on the cytocompatibility of a novel biodegradable ZnMg alloy. Mater. Sci. Eng. C 2016, 68, 198–204. [Google Scholar] [CrossRef] [PubMed]
- Demir, A.G.; Monguzzi, L.; Previtali, B. Selective laser melting of pure Zn with high density for biodegradable implant manufacturing. Addit. Manuf. 2017, 15, 20–28. [Google Scholar] [CrossRef]
- Wang, C.; Yu, Z.; Cui, Y.; Zhang, Y.; Yu, S.; Qu, G.; Gong, H. Processing of a novel Zn alloy micro-tube for biodegradable vascular stent application. J. Mater. Sci. Technol. 2016, 32, 925–929. [Google Scholar] [CrossRef]
- Luo, M.; Shen, W.; Wang, Y.; Allen, M. In Vitro Degradation of Biodegradable Metal Zn And Zn/Fe-Couples and Their Application as Conductors in Biodegradable Sensors. In Proceedings of the 2015 Transducers-2015 18th International Conference on Solid-State Sensors, Actuators and Microsystems (TRANSDUCERS), Anchorage, AK, USA, 21–25 June 2015; pp. 1370–1373. [Google Scholar]
- Ma, J.; Zhao, N.; Zhu, D. Endothelial cellular responses to biodegradable metal zinc. ACS Biomater. Sci. Eng. 2015, 1, 1174–1182. [Google Scholar] [CrossRef] [PubMed]
- Aghion, E.; Levy, G. The effect of Ca on the in vitro corrosion performance of biodegradable Mg-Nd-Y-Zr alloy. J. Mater. Sci. 2010, 45, 3096–3101. [Google Scholar] [CrossRef]
- Levy, G.; Aghion, E. Effect of diffusion coating of Nd on the corrosion resistance of biodegradable Mg implants in simulated physiological electrolyte. Acta Biomater. 2013, 9, 8624–8630. [Google Scholar] [CrossRef] [PubMed]
- Murni, N.; Dambatta, M.; Yeap, S.; Froemming, G.; Hermawan, H. Cytotoxicity evaluation of biodegradable Zn–3Mg alloy toward normal human osteoblast cells. Mater. Sci. Eng. C 2015, 49, 560–566. [Google Scholar] [CrossRef] [PubMed]
- Guillory, R.J.; Bowen, P.K.; Hopkins, S.P.; Shearier, E.R.; Earley, E.J.; Gillette, A.A.; Aghion, E.; Bocks, M.; Drelich, J.W.; Goldman, J. Corrosion characteristics dictate the long-term inflammatory profile of degradable zinc arterial implants. ACS Biomater. Sci. Eng. 2016, 2, 2355–2364. [Google Scholar] [CrossRef]
- Hakimi, O.; Ventura, Y.; Goldman, J.; Vago, R.; Aghion, E. Porous biodegradable EW62 medical implants resist tumor cell growth. Mater. Sci. Eng. C 2016, 61, 516–525. [Google Scholar] [CrossRef] [PubMed]
- Li, H.; Xie, X.; Zheng, Y.; Cong, Y.; Zhou, F.; Qiu, K.; Wang, X.; Chen, S.; Huang, L.; Tian, L. Development of biodegradable Zn-1X binary alloys with nutrient alloying elements Mg, Ca and Sr. Sci. Rep. 2015, 5, 10719. [Google Scholar] [CrossRef] [PubMed]
- Liu, X.; Sun, J.; Yang, Y.; Pu, Z.; Zheng, Y. In vitro investigation of ultra-pure Zn and its mini-tube as potential bioabsorbable stent material. Mater. Lett. 2015, 161, 53–56. [Google Scholar] [CrossRef]
- Kubásek, J.; Vojtěch, D.; Jablonská, E.; Pospíšilová, I.; Lipov, J.; Ruml, T. Structure, mechanical characteristics and in vitro degradation, cytotoxicity, genotoxicity and mutagenicity of novel biodegradable Zn–Mg alloys. Mater. Sci. Eng. C 2016, 58, 24–35. [Google Scholar] [CrossRef] [PubMed]
- Zhao, S.; McNamara, C.T.; Bowen, P.K.; Verhun, N.; Braykovich, J.P.; Goldman, J.; Drelich, J.W. Structural characteristics and in vitro biodegradation of a novel Zn-Li alloy prepared by induction melting and hot rolling. Metall. Mater. Trans. A 2017, 3, 1204–1215. [Google Scholar] [CrossRef]
- Ma, J.; Zhao, N.; Zhu, D. Bioabsorbable zinc ion induced biphasic cellular responses in vascular smooth muscle cells. Sci. Rep. 2016, 6, 26661. [Google Scholar] [CrossRef] [PubMed]
- Kubasek, J.; Vojtěch, D. Zn-based alloys as an alternative biodegradable materials. Proc Met. 2012, 5, 23–25. [Google Scholar]
- Kubasek, J.; Pospisilova, I.; Vojtech, D.; Jablonska, E.; Ruml, T. Structural, mechanical and cytotoxicity characterization of as-cast biodegradable Zn–xMg (x = 0.8%–8.3%) alloys. Mater. Tehnol. 2014, 48, 623–629. [Google Scholar]
- Dunne, C.F.; Katarivas Levy, G.; Hakimi, O.; Aghion, E.; Twomey, B.; Stanton, K.T. Corrosion behaviour of biodegradable magnesium alloys with hydroxyapatite coatings. Surf. Coat. Technol. 2016, 289, 37–44. [Google Scholar] [CrossRef]
- Seitz, J.M.; Durisin, M.; Goldman, J.; Drelich, J.W. Recent advances in biodegradable metals for medical sutures: A critical review. Adv. Healthc. Mater. 2015, 4, 1915–1936. [Google Scholar] [CrossRef] [PubMed]
- Wang, C.; Yang, H.; Li, X.; Zheng, Y. In vitro evaluation of the feasibility of commercial Zn alloys as biodegradable metals. J. Mater. Sci. Technol. 2016, 32, 909–918. [Google Scholar] [CrossRef]
- Törne, K.; Larsson, M.; Norlin, A.; Weissenrieder, J. Degradation of zinc in saline solutions, plasma, and whole blood. J. Biomed. Mater. Res. Part B 2016, 104, 1141–1151. [Google Scholar] [CrossRef] [PubMed]
- Bolz, A.; Popp, T. Implantable, Bioresorbable Vessel Wall Support, in Particular Coronary Stent. U.S. Patent 6,287,332 B1, 11 September 2001. [Google Scholar]
- Zhou, G.; Gongqi, Q.; Gong, H. Kind of Absorbable High Strength and Toughness Corrosion-Resistant Zinc Alloy Implant Material for Human Body. U.S. Patent 20170028107 A1, 2 February 2017. [Google Scholar]
- Plum, L.M.; Rink, L.; Haase, H. The essential toxin: Impact of zinc on human health. Int. J. Environ. Res. Public Health 2010, 7, 1342–1365. [Google Scholar] [CrossRef] [PubMed]
- Liu, X.; Sun, J.; Qiu, K.; Yang, Y.; Pu, Z.; Li, L.; Zheng, Y. Effects of alloying elements (Ca and Sr) on microstructure, mechanical property and in vitro corrosion behavior of biodegradable Zn–1.5Mg alloy. J. Alloys Compd. 2016, 664, 444–452. [Google Scholar] [CrossRef]
- Niu, J.; Tang, Z.; Huang, H.; Pei, J.; Zhang, H.; Yuan, G.; Ding, W. Research on a Zn-Cu alloy as a biodegradable material for potential vascular stents application. Mater. Sci. Eng. C 2016, 69, 407–413. [Google Scholar] [CrossRef] [PubMed]
- Huang, T.; Zheng, Y.; Han, Y. Accelerating degradation rate of pure iron by zinc ion implantation. Regen. Biomater. 2016, 3, 205–215. [Google Scholar] [CrossRef] [PubMed]
- Vojtech, D.; Pospisilova, I.; Michalcova, A.; Maixner, J. Microstructure and mechanical properties of the micrograined hypoeutectic zn-mg alloy. Int. J. Miner. Metall. Mater. 2016, 23, 1167–1176. [Google Scholar]
- Pospíšilová, I.; Vojtěch, D. Zinc alloys for biodegradable medical implants. In Materials Science Forum; Trans Tech Publlication: Stafa-Zurich, Switzerland, 2014; pp. 457–460. [Google Scholar]
- Zhao, L.; Zhang, Z.; Song, Y.; Liu, S.; Qi, Y.; Wang, X.; Wang, Q.; Cui, C. Mechanical properties and in vitro biodegradation of newly developed porous Zn scaffolds for biomedical applications. Mater. Des. 2016, 108, 136–144. [Google Scholar] [CrossRef]
- Vojtěch, D.; Kubásek, J.; Šerák, J.; Novák, P. Mechanical and corrosion properties of newly developed biodegradable Zn-based alloys for bone fixation. Acta Biomater. 2011, 7, 3515–3522. [Google Scholar] [CrossRef] [PubMed]
- Guleryuz, L.; Ipek, R.; Arıtman, I.; Karaoglu, S. Microstructure and Mechanical Properties of Zn-Mg Alloys as Implant Materials Manufactured by Powder Metallurgy Method. In AIP Conference Proceedings; AIP Publishing: Melville, NY, USA, 2017. [Google Scholar]
- Li, H.; Yang, H.; Zheng, Y.; Zhou, F.; Qiu, K.; Wang, X. Design and characterizations of novel biodegradable ternary Zn-based alloys with iia nutrient alloying elements mg, ca and sr. Mater. Des. 2015, 83, 95–102. [Google Scholar] [CrossRef]
- Sikora-Jasinska, M.; Mostaed, E.; Mostaed, A.; Beanland, R.; Mantovani, D.; Vedani, M. Fabrication, mechanical properties and in vitro degradation behavior of newly developed ZnAg alloys for degradable implant applications. Mater. Sci. Eng. C 2017, 77, 1170–1181. [Google Scholar] [CrossRef] [PubMed]
- Gong, H.; Wang, K.; Strich, R.; Zhou, J.G. In vitro biodegradation behavior, mechanical properties, and cytotoxicity of biodegradable Zn–Mg alloy. J. Biomed. Mater. Res. Part B 2015, 103, 1632–1640. [Google Scholar] [CrossRef] [PubMed]
- Katarivas Levy, G.L.; Leon, A.; Kafri, A.; Ventura, Y.; Drelich, J.W.; Goldman, J.; Vago, R.; Aghion, E. Evaluation of biodegradable Zn–1%Mg and Zn–1%Mg–0.5%Ca alloys for biomedical applications. J. Mater. Sci. Mater. Med. 2017. accepted. [Google Scholar] [CrossRef]
- Dambatta, M.; Izman, S.; Kurniawan, D.; Farahany, S.; Yahaya, B.; Hermawan, H. Influence of thermal treatment on microstructure, mechanical and degradation properties of Zn–3Mg alloy as potential biodegradable implant material. Mater. Des. 2015, 85, 431–437. [Google Scholar] [CrossRef]
- Liu, X.; Sun, J.; Yang, Y.; Zhou, F.; Pu, Z.; Li, L.; Zheng, Y. Microstructure, mechanical properties, in vitro degradation behavior and hemocompatibility of novel Zn–Mg–Sr alloys as biodegradable metals. Mater. Lett. 2016, 162, 242–245. [Google Scholar] [CrossRef]
- Liu, X.; Sun, J.; Zhou, F.; Yang, Y.; Chang, R.; Qiu, K.; Pu, Z.; Li, L.; Zheng, Y. Micro-alloying with Mn in Zn–Mg alloy for future biodegradable metals application. Mater. Des. 2016, 94, 95–104. [Google Scholar] [CrossRef]
- Bakhsheshi-Rad, H.; Hamzah, E.; Low, H.; Kasiri-Asgarani, M.; Farahany, S.; Akbari, E.; Cho, M. Fabrication of biodegradable Zn-Al-Mg alloy: Mechanical properties, corrosion behavior, cytotoxicity and antibacterial activities. Mater. Sci. Eng. C 2017, 73, 215–219. [Google Scholar] [CrossRef] [PubMed]
- Bowen, P.; Seitz, J.; Guillory, R.; Braykovich, J.; Zhao, F.; Goldman, J.; Drelich, J. Evaluation of wrought Zn-Al alloys (1, 3, and 5 wt % al) through mechanical and in vivo corrosion testing for stent applications. J. Biomed. Mater. Res. Part B 2016. [Google Scholar] [CrossRef]
- Bakhsheshi-Rad, H.; Hamzah, E.; Low, H.; Cho, M.; Kasiri-Asgarani, M.; Farahany, S.; Mostafa, A.; Medraj, M. Thermal characteristics, mechanical properties, in vitro degradation and cytotoxicity of novel biodegradable Zn–Al–Mg and Zn–Al–Mg–xBi alloys. Acta Metall. Sin. (Engl. Lett.) 2017, 30, 201–211. [Google Scholar] [CrossRef]
- Tang, Z.; Niu, J.; Huang, H.; Zhang, H.; Pei, J.; Ou, J.; Yuan, G. Potential biodegradable Zn-Cu binary alloys developed for cardiovascular implant applications. J. Mech. Behav. Biomed. Mater. 2017, 72, 182–191. [Google Scholar] [CrossRef] [PubMed]
- Tang, Z.; Huang, H.; Niu, J.; Zhang, L.; Zhang, H.; Pei, J.; Tan, J.; Yuan, G. Design and characterizations of novel biodegradable Zn-Cu-Mg alloys for potential biodegradable implants. Mater. Des. 2017, 117, 84–94. [Google Scholar] [CrossRef]
- Zhao, S.; Seitz, J.-M.; Eifler, R.; Maier, H.J.; Guillory, R.J.; Earley, E.J.; Drelich, A.; Goldman, J.; Drelich, J.W. Zn-Li alloy after extrusion and drawing: Structural, mechanical characterization, and biodegradation in abdominal aorta of rat. Mater. Sci. Eng. C 2017, 76, 301–312. [Google Scholar] [CrossRef] [PubMed]
- Roohani, N.; Hurrell, R.; Kelishadi, R.; Schulin, R. Zinc and its importance for human health: An integrative review. J. Res. Med. Sci. 2013, 18, 144. [Google Scholar] [PubMed]
- Jackson, M. Physiology of zinc: General aspects. In Zinc in Human Biology; Springer: Berlin, Germany, 1989; pp. 1–14. [Google Scholar]
- Bowen, P.K.; Drelich, J.; Goldman, J. Zinc exhibits ideal physiological corrosion behavior for bioabsorbable stents. Adv. Mater. 2013, 25, 2577–2582. [Google Scholar] [CrossRef] [PubMed]
- Moonga, B.S.; Dempster, D.W. Zinc is a potent inhibitor of osteoclastic bone resorption in vitro. J. Bone Miner. Res. 1995, 10, 453–457. [Google Scholar] [CrossRef] [PubMed]
- Yamaguchi, M. Role of zinc in bone formation and bone resorption. J. Trace Elem. Exp. Med. 1998, 11, 119–135. [Google Scholar] [CrossRef]
- Bowen, P.K.; Shearier, E.R.; Zhao, S.; Guillory, R.J.; Zhao, F.; Goldman, J.; Drelich, J.W. Biodegradable metals for cardiovascular stents: From clinical concerns to recent Zn-alloys. Adv. Healthc. Mater. 2016, 5, 1121–1140. [Google Scholar] [CrossRef] [PubMed]
- Kaltenberg, J.; Plum, L.M.; Ober-Blobaum, J.L.; Honscheid, A.; Rink, L.; Haase, H. Zinc signals promote IL-2-dependent proliferation of T cells. Eur. J. Immunol. 2010, 40, 1496–1503. [Google Scholar] [CrossRef] [PubMed]
- Shankar, A.H.; Prasad, A.S. Zinc and immune function: The biological basis of altered resistance to infection. Am. J. Clin. Nutr. 1998, 68, 447s–463s. [Google Scholar] [PubMed]
- Kaur, G. Biodegradable metals as bioactive materials. In Bioactive Glasses: Potential Biomaterials for Future Therapy; Springer International Publishing: Cham, Switzerland, 2017. [Google Scholar]
- Krezel, A.; Maret, W. The biological inorganic chemistry of zinc ions. Arch. Biochem. Biophys. 2016, 611, 3–19. [Google Scholar] [CrossRef] [PubMed]
- Thomas, S.; Birbilis, N.; Venkatraman, M.S.; Cole, I.S. Corrosion of zinc as a function of pH. J. Sci. Eng. 2012, 68. [Google Scholar] [CrossRef]
- Drelich, A.; Zhao, S.; Guillory, R.J.; Drelich, J.W.; Goldman, J. Long-term surveillance of zinc implant in murine artery: Surprisingly steady biocorrosion rate. Acta Biomater. 2017, 58, 539–549. [Google Scholar] [CrossRef] [PubMed]
- Shearier, E.R.; Bowen, P.K.; He, W.; Drelich, A.; Drelich, J.; Goldman, J.; Zhao, F. In vitro cytotoxicity, adhesion, and proliferation of human vascular cells exposed to zinc. ACS Biomater. Sci. Eng. 2016, 2, 634–642. [Google Scholar] [CrossRef] [PubMed]
- Zhu, D.H.; Su, Y.C.; Young, M.L.; Ma, J.; Zheng, Y.F.; Tang, L.P. Biological responses and mechanisms of human bone marrow mesenchymal stem cells to Zn and Mg biomaterials. ACS Appl. Mater. Interfaces 2017, 9, 27453–27461. [Google Scholar] [CrossRef] [PubMed]
- Qiao, Y.Q.; Zhang, W.J.; Tian, P.; Meng, F.H.; Zhu, H.Q.; Jiang, X.Q.; Liu, X.Y.; Chu, P.K. Stimulation of bone growth following zinc incorporation into biomaterials. Biomaterials 2014, 35, 6882–6897. [Google Scholar] [CrossRef] [PubMed]
- Al Qaysi, M.; Petrie, A.; Shah, R.; Knowles, J.C. Degradation of zinc containing phosphate-based glass as a material for orthopedic tissue engineering. J. Mater. Sci. 2016. [Google Scholar] [CrossRef]
- Zhong, Z.; Ma, J. Fabrication, characterization, and in vitro study of zinc substituted hydroxyapatite/silk fibroin composite coatings on titanium for biomedical applications. J. Biomater. Appl. 2017, 32, 399–409. [Google Scholar] [CrossRef] [PubMed]
- Yu, J.M.; Xu, L.Z.; Li, K.; Xie, N.; Xi, Y.H.; Wang, Y.; Zheng, X.B.; Chen, X.S.; Wang, M.Y.; Ye, X.J. Zinc-modified calcium silicate coatings promote osteogenic differentiation through TGF-β/Smad pathway and osseointegration in osteopenic rabbits. Sci. Rep. 2017, 7, 3440. [Google Scholar] [CrossRef] [PubMed]
- Cama, G.; Nkhwa, S.; Gharibi, B.; Lagazzo, A.; Cabella, R.; Carbone, C.; Dubruel, P.; Haugen, H.; Di Silvio, L.; Deb, S. The role of new zinc incorporated monetite cements on osteogenic differentiation of human mesenchymal stem cells. Mater. Sci. Eng. C 2017, 78, 485–494. [Google Scholar] [CrossRef] [PubMed]
- Ferreira, E.C.S.; Bortolin, R.H.; Freire-Neto, F.P.; Souza, K.S.C.; Bezerra, J.F.; Ururahy, M.A.G.; Ramos, A.M.O.; Himelfarb, S.T.; Abreu, B.J.; Didone, T.V.N.; et al. Zinc supplementation reduces RANKL/OPG ratio and prevents bone architecture alterations in ovariectomized and type 1 diabetic rats. Nutr. Res. 2017, 40, 48–56. [Google Scholar] [CrossRef] [PubMed]
- Yu, W.L.; Sun, T.W.; Qi, C.; Ding, Z.Y.; Zhao, H.K.; Zhao, S.C.; Shi, Z.M.; Zhu, Y.J.; Chen, D.Y.; He, Y.H. Evaluation of zinc-doped mesoporous hydroxyapatite microspheres for the construction of a novel biomimetic scaffold optimized for bone augmentation. Int. J. Nanomed. 2017, 12, 2293–2306. [Google Scholar] [CrossRef] [PubMed]
- Yusa, K.; Yamamoto, O.; Takano, H.; Fukuda, M.; Iino, M. Zinc-modified titanium surface enhances osteoblast differentiation of dental pulp stem cells in vitro. Sci. Rep. 2016, 6. [Google Scholar] [CrossRef] [PubMed]
- An, S.F.; Gong, Q.M.; Huang, Y.H. Promotive effect of zinc ions on the vitality, migration, and osteogenic differentiation of human dental pulp cells. Biol. Trace Elem. Res. 2017, 175, 112–121. [Google Scholar] [CrossRef] [PubMed]
- Bowen, P.K.; Guillory, R.J.; Shearier, E.R.; Seitz, J.-M.; Drelich, J.; Bocks, M.; Zhao, F.; Goldman, J. Metallic zinc exhibits optimal biocompatibility for bioabsorbable endovascular stents. Mater. Sci. Eng.C 2015, 56, 467–472. [Google Scholar] [CrossRef] [PubMed]
- Yang, H.; Wang, C.; Liu, C.; Chen, H.; Wu, Y.; Han, J.; Jia, Z.; Lin, W.; Zhang, D.; Li, W.; et al. Evolution of the degradation mechanism of pure zinc stent in the one-year study of rabbit abdominal aorta model. Biomaterials 2017, 145, 92–105. [Google Scholar] [CrossRef] [PubMed]
- Lansdown, A.B. Silver in health care: Antimicrobial effects and safety in use. In Biofunctional Textiles and the Skin; Karger: Basel, Switzerland, 2006. [Google Scholar]
- Mertz, W. Trace Elements in Human and Animal Nutrition; Academic Press, INC.: Orlando, FL, USA, 1986. [Google Scholar]
| Family | Representive Alloys and Alloying Elements (wt %) | Main Phases | References |
|---|---|---|---|
| Zn–Mg | Zn–0.15Mg | α-Zn, Mg2Zn11 | [9] |
| Zn–0.5Mg | α-Zn, Mg2Zn11 | [9] | |
| Zn–1Mg, ZnMg1 | α-Zn, Mg2Zn11 | [9,22,42,46,47] | |
| Zn–1.2Mg | α-Zn, Mg2Zn11 | [3] | |
| Zn–1.5Mg, ZnMg1.5 | α-Zn, Mg2Zn11 | [36,42] | |
| Zn–3Mg, ZnMg3 | α-Zn, Mg2Zn11 | [9,42,48] | |
| Zn–1.5Mg–0.1Ca | α-Zn, Mg2Zn11, CaZn13 | [36] | |
| Zn–1Mg–0.5Ca | α-Zn, Mg2Zn11, CaZn13 | [47] | |
| Zn–1Mg–1Ca | α-Zn, Mg2Zn11, CaZn13 | [44] | |
| Zn–1Mg–0.1Sr | Zn, MgZn2, SrZn13 | [49] | |
| Zn–1Mg–0.5Sr | Zn, MgZn2, SrZn13 | [49] | |
| Zn–1.5Mg–0.1Sr | α-Zn, Mg2Zn11, SrZn13 | [36] | |
| Zn–1Mg–1Sr | α-Zn, Mg2Zn11, SrZn13 | [44] | |
| Zn–1Mg–0.1Mn | Zn, MgZn2 | [50] | |
| Zn–1.5Mg–0.1Mn | Zn, MgZn2 | [50] | |
| Zn–Ca | Zn–1Ca | α-Zn, CaZn13 | [22] |
| Zn–1Ca–1Sr | α-Zn, CaZn13, SrZn13 | [44] | |
| Zn–Sr | Zn–1Sr | α-Zn, SrZn13 | [22] |
| Zn–Al | Zn–0.5Al | Zn, Al | [9,51] |
| Zn–1Al | Zn, Al | [9,52] | |
| Zn–3Al | Zn, Al | [52] | |
| Zn–5Al | Zn, Al | [52] | |
| ZnAl4Cu1 | Zn, Al | [42] | |
| ZA0.1Mg | α-Zn, Mg2(Zn,Al)11 | [51] | |
| ZA0.3Mg | α-Zn, Mg2(Zn,Al)11 | [51] | |
| ZA0.5Mg/Zn-0.5Al-0.5Mg | α-Zn, Mg2(Zn,Al)11 | [51,53] | |
| Zn–0.5Al–0.5Mg–0.1Bi | Zn, Mg2(Zn,Al)11, Mg3Bi2 | [53] | |
| Zn–0.5Al–0.5Mg–0.3Bi | Zn, Mg2(Zn,Al)11, Mg3Bi2 | [53] | |
| Zn–0.5Al–0.5Mg–0.5Bi | Zn, Mg2(Zn,Al)11, Mg3Bi2 | [53] | |
| 3.5–.5Al, 0.75–1.25Cu, 0.03–0.08Mg | Zn, Al | [31] | |
| 3.5–4.3Al, 2.5–3.2Cu, 0.03–0.06Mg | Zn, Al | [31] | |
| 5.6–6Al, 1.2–1.6Cu | Zn, Al | [31] | |
| Zn–Cu | Zn–1Cu | η-Zn, ε-CuZn5 | [54] |
| Zn–2Cu | η-Zn, ε-CuZn5 | [54] | |
| Zn–3Cu | η-Zn, ε-CuZn5 | [54,55] | |
| Zn–4Cu | η-Zn, ε-CuZn5 | [37,54] | |
| Zn–3Cu–0.1Mg | Zn, CuZn5, Mg2Zn11 | [55] | |
| Zn–3Cu–0.5Mg | Zn, CuZn5, Mg2Zn11 | [55] | |
| Zn–3Cu–1Mg | Zn, CuZn5, Mg2Zn11 | [55] | |
| Zn–Li | Zn–2Li | Zn, α-LiZn4 | [25] |
| Zn–4Li | Zn, α-LiZn4 | [25] | |
| Zn–6Li | Zn, α-LiZn4 | [25] | |
| Zn–Li | Zn, α-LiZn4 | [56] | |
| Zn–Ag | Zn–2.5Ag | η-Zn, ε-AgZn3 | [45] |
| Zn–5Ag | η-Zn, ε-AgZn3 | [45] | |
| Zn–7Ag | η-Zn, ε-AgZn3 | [45] |
| Organ or System | Zinc Deficiency | Zinc Excess |
|---|---|---|
| Brain | Decreased nerve conduction, neuropsychiatric and neurosensory disorders, mental lethargy | Lethargy, focal neuronal deficits. |
| Respiratory tract | - | Respiratory disorder after inhalation of zinc smoke, metal fume fever. |
| Immune system | Impaired immune system function, increased susceptibility to pathogens | Altered lymphocyte function. |
| Thymus | Thymic atrophy | - |
| Skin | Skin lesions, decreased wound healing, acrodermatitis | - |
| Gastrointestinal tract | - | Nausea/vomiting, epigastric pain, diarrhea. |
| Reproductive system | Infertility, retarded genital development, hypogonadism | - |
| Prostate | - | Elevated risk of prostate cancer. |
| Element | Blood Serum Level | Daily Allowance | Pathophysiology | Toxicology | Effect on Zinc Alloys |
|---|---|---|---|---|---|
| Essential Elements | |||||
| Mg | 17.7–25.8 mg/L | 700 mg | Activator of many enzymes; co-regulator of protein synthesis and muscle contraction; stabilizer of DNA and RNA | Excessive Mg leads to nausea | Mg: ↑mechanical properties & ↑corrosion rates [22] |
| Ca | 36.8–39.8 mg/L | 800 mg | More than 99% have structural functions in the skeleton; the solution Ca has signaling functions, including muscle contraction, blood clotting, cell function, etc. | Inhibit the intestinal absorption of other essential minerals | Ca: ↑mechanical properties & ↑corrosion rates [22] |
| Fe | 5000–17,600 mg/L | 10–20 mg | Component of several metalloproteins; crucial in vital biochemical activities, i.e., oxygen sensing and transport | Iron toxicity gives rise to lesions in the gastrointestinal tract, shock and liver damage | Fe: ↑corrosion rates by galvanic corrosion mechanism [15] |
| Essential Trace Elements | |||||
| Zn | 0.8–1.14 mg/L | 15 mg | Trace element; appears in all enzyme classes; most Zn appears in muscle | Neurotoxic and hinders bone development at higher concentrations | - |
| Cu | 4.51–8.32 mg/L | 1–3 mg | Cu plays a vital role in the immune system; has beneficial effects on endothelial cell proliferation and has been reported to enhance antibacterial properties [55] | Excessive Cu (>1 mg/day) can cause neurodegenerative diseases, including Alzheimer’s, Menkes and Wilson’s diseases [55] | ↑Cu (1–4%): ↑mechanical properties & ↑corrosion rates [37,54] |
| Mn | <0.0008 mg/L | 4 mg | Activator of enzymes; Mn deficiency is related to osteoporosis, diabetes mellitus, and atherosclerosis | Excessive Mn results in neurotoxicity | Mn improves the casting process. Mn ↑ susceptibility of galvanic micro-cell corrosion [50] |
| Other Elements | |||||
| Sr | 0.17 mg a | 2 mg | 99% is located in bone; shows dose dependent metabolic effects on bone; low doses stimulate new bone formation | High doses induce skeletal abnormalities | Sr: ↑mechanical properties & ↑corrosion rates [22] |
| Li | 0.002–0.004 mg/L | 0.2–0.6 mg | Used in the treatment of manic depressive psychoses | Plasma concentrations of 2 mM are associated with reduced kidney function and neurotoxicity, 4 mM may be fatal | Li: ↑ultimate tensile strength, ↓ductility & ↓corrosion rate [56] |
| Al | 0.0021–0.0048 mg/L | - | - | Primarily accumulates in the bone and nervous systems; implicated in the pathogenesis of Alzheimer’s disease; can cause muscle fiber damage; decreases osteoblast viability | Al: ↑mechanical properties & ↑corrosion rates |
| Alloy | In Vitro Corrosion Rate | In Vivo Corrosion Rate (mm/year) | References | |
|---|---|---|---|---|
| Electrochemical (μA/cm2) | Immersion (mm/year) | |||
| Zn | 1.8–9.2 (Hank’s) 0.05 (plasma) 0.04 (whole blood) 0.035 (PBS) | 0.027–0.13 (Hank’s) | 0.02–0.05 (1.5–6 months) | [9,20,22,23,31,32,45,53,59] |
| Zn * | 8.98 | - | - | [9] |
| Zn–Mg | ||||
| Zn–0.15Mg c | 11.52 (Hank’s) | 0.17 (Hank’s) | - | [9] |
| Zn–0.15Mg *,c | 10.98 (Hank’s) | - | - | [9] |
| Zn–0.5Mg c | 11.73 (Hank’s) | 0.175 (Hank’s) | - | [9] |
| Zn–0.5Mg *,c | 11.01 (Hank’s) | - | - | [9] |
| Zn–1Mg f/ZnMg1 b | 9.9–11.9 (Hank’s) 0.28–1.2 (SBF) 0.74 (PBS) | 0.085–0.18 (Hank’s) 0.06–0.28 (SBF) 0.027 (PBS) | 0.17 | [9,22,42,46,47] |
| Zn–1Mg * | 11.32 (Hank’s) | 0.12 (SBF) | - | [9,46] |
| Zn–1.2Mg | 7.7 (Hank’s) | 0.08 (Hank’s) | - | [3] |
| Zn–1.2Mg * | 12.4 (Hank’s) | 0.11 (Hank’s) | - | [3] |
| Zn–1.5Mg d/ZnMg1.5 b | 8.8 (SBF) | 0.063 (Hank’s) 0.05 (SBF) | - | [4,36] |
| Zn–3Mg/ZnMg3 b | 9.01 (Hank’s) 7.4 (SBF) | 0.13 (Hank’s) 0.06–0.21 (SBF) | - | [9,42,48] |
| Zn–3Mg * | 8.6 (Hank’s) | - | - | [9] |
| Zn–3Mg *** | - | 0.13 (SBF) | - | [48] |
| Zn–1.5Mg–0.1Ca d | - | 0.12 (Hank’s) | - | [36] |
| Zn–1Mg–0.5Ca | 4.3 (PBS) | 0.37 (PBS) | [47] | |
| Zn–-1Mg–1Ca e | 0.17 (Hank’s) | 0.09 (Hank’s) | - | [44] |
| Zn–-1Mg–0.1Sr | 7.85 (Hank’s) | - | - | [49] |
| Zn–1Mg–0.5Sr | 7.83 (Hank’s) | - | - | [49] |
| Zn–1.5Mg–0.1Sr d | - | 0.1 (Hank’s) | - | [36] |
| Zn–1Mg–1Sr e | 0.175 (Hank’s) | 0.095 (Hank’s) | - | [44] |
| Zn–1Mg–0.1Mn | 17.21 (Hank’s) | 0.12 (Hank’s) | - | [50] |
| Zn–1.5Mg–0.1Mn | 9.34 (Hank’s) | 0.09 (Hank’s) | - | [50] |
| Zn–Ca | ||||
| Zn–1Ca f | 10.75 (Hank’s) | 0.09 (Hank’s) | 0.19 | [22] |
| Zn–1Ca–1Sr e | 0.185 (Hank’s) | 0.11 (Hank’s) | - | [44] |
| Zn–Sr | ||||
| Zn–1Sr f | 11.76 (Hank’s) | 0.095 (Hank’s) | 0.22 | [22] |
| Zn–Al | ||||
| Zn–0.5Al | 11.08 (Hank’s) 20 (SBF) | 0.14 (Hank’s) 15 (SBF) | - | [9,51] |
| Zn–0.5Al *,c | 9.6 (Hank’s) | - | - | [9] |
| Zn–1Al | 11.11 (Hank’s) | 0.16 (Hank’s) | - | [9] |
| Zn–1Al * | 9.7 (Hank’s) | - | - | [9] |
| ZnAl4Cu1 b | 5.2 (SBF) | 0.07 (SBF) | - | [42] |
| ZA0.1Mg | 17 (SBF) | 0.13 (SBF) | - | [51] |
| ZA0.3Mg | 11.2 (SBF) | 0.11 (SBF) | - | [51] |
| ZA0.5Mg/Zn–0.5Al–0.5Mg | 9.5 (SBF) | 0.11–0.15 (SBF) | - | [51,53] |
| Zn–0.5Al–0.5Mg–0.1Bi | 12 (SBF) | 0.17 (SBF) | - | [53] |
| Zn–0.5Al–0.5Mg–0.3Bi | 16 (SBF) | 0.2 (SBF) | - | [53] |
| Zn–0.5Al–0.5Mg–0.5Bi | 23 (SBF) | 0.28 (SBF) | - | [53] |
| ZA4–1 | 2.986 (Hank’s) | - | - | [31] |
| ZA4–3 | 7.209 (Hank’s) | - | - | [31] |
| ZA6–1 | 5.331 (Hank’s) | - | - | [31] |
| Zn–Cu | ||||
| Zn–1Cu *,a | - | 0.033 (c-SBF) | - | [54] |
| Zn–2Cu *,a | - | 0.027 (c-SBF) | - | [54] |
| Zn–3Cu *,a | 0.372 (Hank’s) | 0.012 (Hank’s) 0.03 (c-SBF) | - | [54,55] |
| Zn–4Cu *,a | 4.1 (Hank’s) | 0.009 (Hank’s) 0.025 (c-SBF) | - | [37,54] |
| Zn–3Cu–0.1Mg * | 1.18 (Hank’s) | 0.023 (Hank’s) | - | [55] |
| Zn–3Cu–0.5Mg * | 1.56 (Hank’s) | 0.03 (Hank’s) | - | [55] |
| Zn–3Cu–1Mg * | 12.4 (Hank’s) | 0.0432 (Hank’s) | - | [55] |
| Zn–Ag | ||||
| Zn–2.5Ag | 9.2 (Hank’s) | 0.079 (Hank’s) | - | [45] |
| Zn–5Ag | 9.7 (Hank’s) | 0.081 (Hank’s) | - | [45] |
| Zn–7Ag | 9.9 (Hank’s) | 0.084 (Hank’s) | - | [45] |
| Zn–Li | ||||
| Zn–2Li | 0.011 (SBF) | - | - | [25] |
| Zn–4Li | 0.004 (SBF) | - | - | [25] |
| Zn–6Li | 0.0038 (SBF) | - | - | [25] |
| Zn–1Li | - | - | 0.02–0.05 | [56] |
| Tissue/Alloy | Mechanical Properties | References | |||
|---|---|---|---|---|---|
| Yield Strength (YS) (MPa) | Ultimate Tensile Strength (UTS) (MPa) | Elongation (%) | Hardness (HV) | ||
| Cortical bone | 104.9–114.3 | 35–283 | 5–23 | - | [10,11] |
| Cancellous bone | - | 1.5–38 | - | - | [10,11] |
| Arterial wall | - | 0.5–1.72 | - | - | [10,11] |
| Zn c | 10 | 18 | 0.32 | 38 | [44] |
| Zn *,c | 35 | 60 | 3.5 | - | [44] |
| Zn **,c,d | 30–110 | 50–140 | 5.8–36 | 39 | [44,52] |
| Zn–Mg | |||||
| Zn–-0.15Mg * | 114 | 250 | 22 | 52 | [9] |
| Zn–0.5Mg * | 159 | 297 | 13 | 65 | [9] |
| Zn–1Mg/ZnMg1 | 180 | 340 | 6 | 75–86 | [9,22,42,47] |
| Zn–1Mg *,f | 175 | 250 | 12 | - | [46] |
| Zn–1.2Mg | 116 | 130 | 1.4 | 93 | [3] |
| Zn–1.2Mg * | 220 | 362 | 21 | 96 | [3] |
| Zn-1.5Mg | 112 | 150 | 1.3 | 155 | [36] |
| Zn–3Mg/ZnMg3 | - | 104 | 2.3 | 201 | [48] |
| Zn–3Mg * | 291 | 399 | 1 | 117 | [9] |
| Zn–3Mg *** | - | 88 | 8.8 | 175 | [48] |
| Zn–1.5Mg–0.1Ca | 173 | 241 | 1.72 | 150 | [36] |
| Zn–1Mg–0.5Ca | - | 150 | 1.34 | 116 | [47] |
| Zn–1Mg–1Ca c | 80 | 130 | 1 | 90 | [44] |
| Zn–1Mg–1Ca *,c | 205 | 250 | 5.2 | - | [44] |
| Zn–1Mg–1Ca **,c | 138 | 197 | 8.5 | 105 | [44] |
| Zn–1Mg–0.1Sr | 109 | 133 | 1.4 | 94 | [49] |
| Zn–1Mg–0.5Sr | 129 | 144 | 1.1 | 109 | [49] |
| Zn–1.5Mg–0.1Sr | 130 | 209 | 2.0 | 145 | [36] |
| Zn–1Mg–1Sr c | 85 | 135 | 1.2 | 85 | [44] |
| Zn–1Mg–1Sr *,c | 200 | 250 | 7.3 | - | [44] |
| Zn–1Mg–1Sr **,c | 140 | 200 | 9.7 | 90 | [44] |
| Zn–1Mg–0.1Mn | 114 | 132 | 98 | 1.11 | [50] |
| Zn–1.5Mg–0.1Mn | 115 | 122 | 149 | 0.77 | [50] |
| Zn–Ca | |||||
| Zn–1Ca | 119 | 165 | 2 | 73 | [22] |
| Zn–1Ca–1Sr c | 83 | 140 | 1.1 | 90 | [44] |
| Zn–1Ca–1Sr *,c | 210 | 260 | 6.8 | - | [44] |
| Zn–1Ca–1Sr **,c | 145 | 203 | 8.6 | 85 | [44] |
| Zn–Sr | |||||
| Zn–1Sr | 120 | 171 | 2 | 61 | [22] |
| Zn–Al | |||||
| Zn–0.5Al * | 119 | 203 | 33 | 59 | [9] |
| Zn–1Al * | 134 | 223 | 24 | 73 | [9] |
| Zn–1Al **,d | 190 | 220 | 24 | - | [52] |
| Zn–3Al **,d | 200 | 240 | 30 | - | [52] |
| Zn–5Al **,d | 240 | 300 | 16 | - | [52] |
| ZnAl4Cu1 | 171 | 210 | 1 | 80 | [42] |
| ZA0.1Mg | - | 87 | 1.6 | 79 | [51] |
| ZA0.3Mg | - | 93 | 1.7 | 89 | [51] |
| ZA0.5Mg/Zn–0.5Al–0.5Mg | - | 92–102 | 1.73–2.1 | 94 | [51,53] |
| Zn–0.5Al–0.5Mg–0.1Bi | - | 102 | 2.4 | 102 | [53] |
| Zn–0.5Al–0.5Mg–0.3Bi | - | 108 | 2.7 | 109 | [53] |
| Zn–0.5Al–0.5Mg–0.5Bi | - | 98 | 1.97 | 99 | [53] |
| ZA4–1 | 75 | 180 | ~112 | 50 | [31] |
| ZA4–3 | 110 | 200 | ~130 | 55 | [31] |
| ZA6–1 | 175 | 275 | ~170 | 65 | [31] |
| Zn–Cu | |||||
| Zn–1Cu * | 149 | 186 | 21 | - | [54] |
| Zn–2Cu * | 199 | 240 | 46 | - | [54] |
| Zn–3Cu * | 213 | 257 | 47 | - | [54,55] |
| Zn–4Cu * | 227–250 | 270 | 51 | - | [37,54] |
| Zn–3Cu–0.1Mg *,b | 340 | 355 | 5 | - | [55] |
| Zn–3Cu–0.5Mg *,b | 390 | 400 | 2 | - | [55] |
| Zn–3Cu–1Mg *,b | 427 | 441 | 0.9 | - | [55] |
| Zn–Ag | |||||
| Zn–2.5Ag *,a | 174 | 200 | 35 | - | [45] |
| Zn–5Ag *,a | 236 | 250 | 36 | - | [45] |
| Zn–7Ag *,a | 258 | 287 | 32 | - | [45] |
| Zn–Li | |||||
| Zn–2Li **,e | 240 | 360 | 14.2 | 98 | [25] |
| Zn–4Li **,e | 420 | 440 | 13.7 | 115 | [25] |
| Zn–6Li **,e | 470 | 560 | 2.2 | 136 | [25] |
| Zn–1Li | 238 | 274 | 17 | 97 | [56] |
© 2017 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Katarivas Levy, G.; Goldman, J.; Aghion, E. The Prospects of Zinc as a Structural Material for Biodegradable Implants—A Review Paper. Metals 2017, 7, 402. https://doi.org/10.3390/met7100402
Katarivas Levy G, Goldman J, Aghion E. The Prospects of Zinc as a Structural Material for Biodegradable Implants—A Review Paper. Metals. 2017; 7(10):402. https://doi.org/10.3390/met7100402
Chicago/Turabian StyleKatarivas Levy, Galit, Jeremy Goldman, and Eli Aghion. 2017. "The Prospects of Zinc as a Structural Material for Biodegradable Implants—A Review Paper" Metals 7, no. 10: 402. https://doi.org/10.3390/met7100402
APA StyleKatarivas Levy, G., Goldman, J., & Aghion, E. (2017). The Prospects of Zinc as a Structural Material for Biodegradable Implants—A Review Paper. Metals, 7(10), 402. https://doi.org/10.3390/met7100402






