Upper Extremity Muscle Activation during Bodyblade Exercises Following Six Weeks of Intervention Focusing on the Lumbopelvic-Hip Complex
Abstract
:1. Introduction
2. Methods
2.1. Study Design
2.2. Participants
2.3. Procedure
Manual Muscle Testing

2.4. Intervention Program
Intervention Exercises
- Side Plank: The participant supported their body on side with weight on their forearm and lateral aspect of foot. Body remained in a straight line, pelvis was held in neutral. Position was held for 30 s (Figure 2).
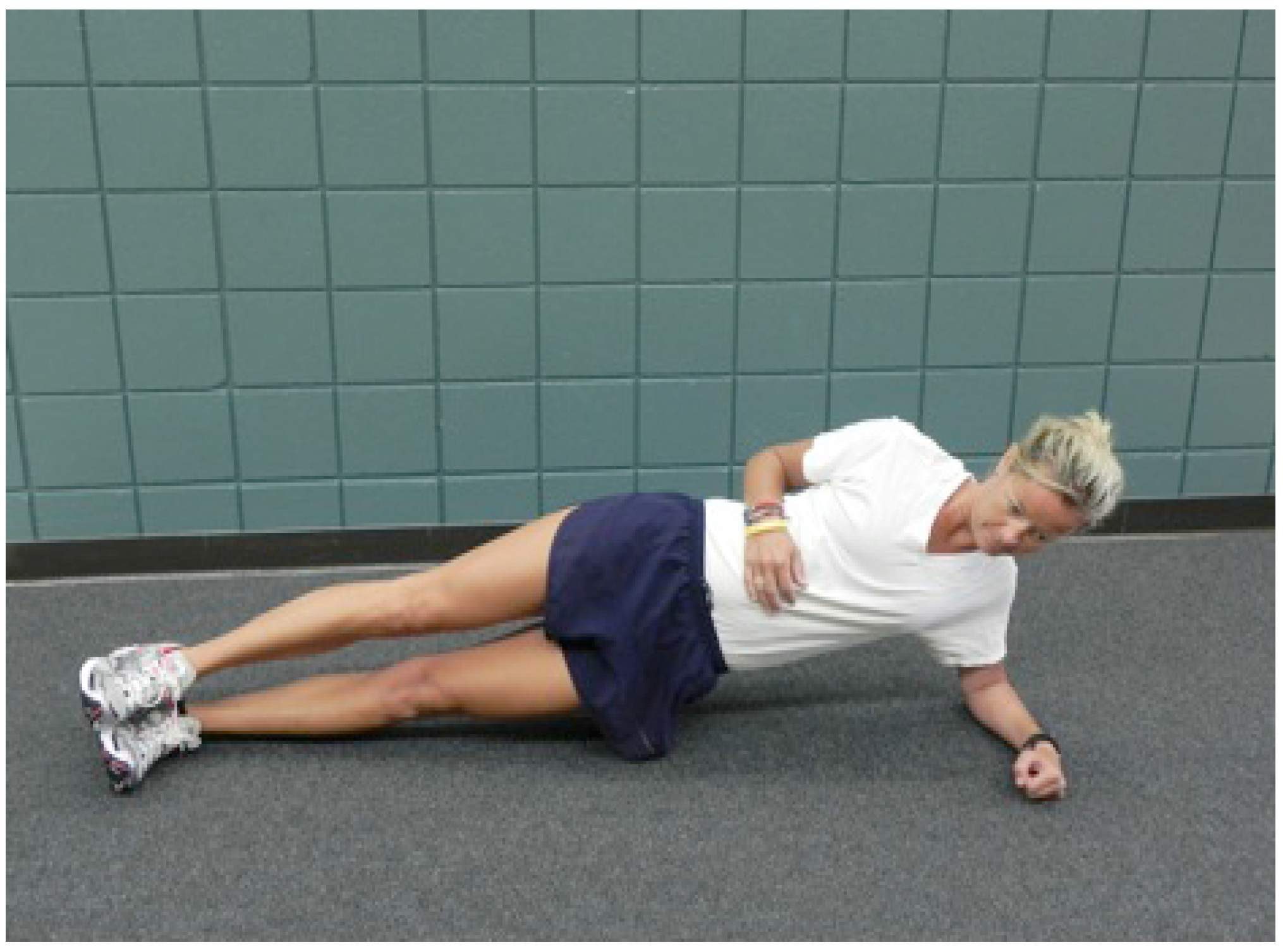
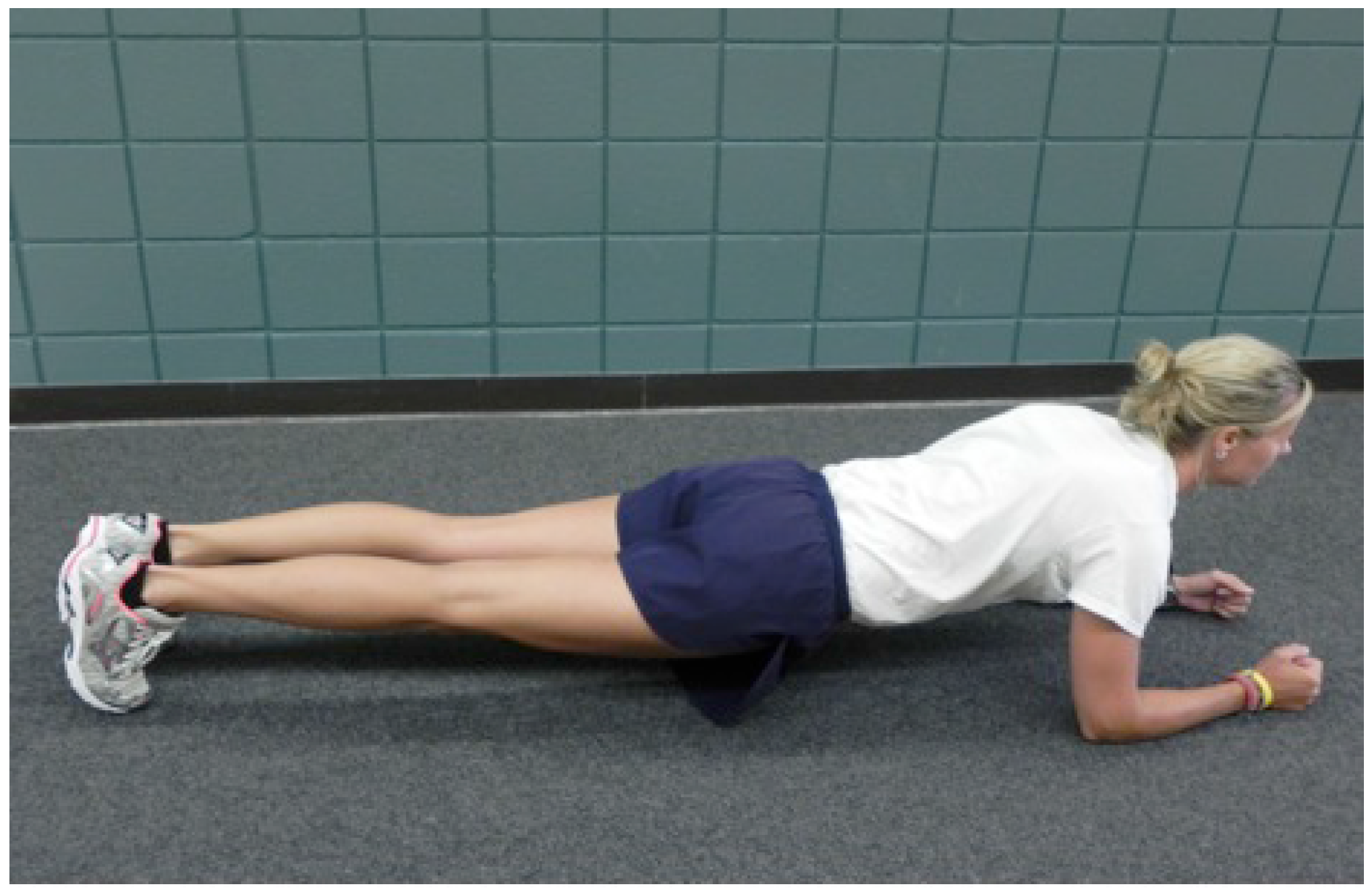
- Front Plank: The participant supported their body on bilateral forearms and balls of feet. The body remained in a straight line and pelvis was held in neutral. This position was held for 30 s (Figure 3).
- Flying Squirrel: Participant was prone with knees flexed, hips internally rotated and extended (legs off the floor), pelvis held in neutral. The shoulders were externally rotated and elbows flexed. This position was held for 30 s (Figure 4).
- Bird Dog: The participant was on all fours and then extended contralateral arm and leg and maintained their pelvis in neutral. This position was held for 30 s (Figure 5).


- Advanced Front Plank: Participant was in front plank position and extended contralateral arm and leg. The pelvis was held in neutral and the position was held for 30 s (Figure 6).
- Single Leg Pelvic Tilt: The participant was supine. Participant’s contralateral hip was in maximal flexion and held by participant with their hands. Ipsilateral foot was on ground. Ipsilateral foot pushed into floor to raise LPHC off floor. The participant’s body remain in straight line and this position was held for 30 s (Figure 7).


- Advanced Bird Dog: The participant positioned to perform the Bird Dog and then dropped into hip flexion while remaining in hip extension on the contralateral side. Position was held for 30 s (Figure 8).
- Push-Up Hold: Participant was prone with weight supported on bilateral balls of feet and palms of hands. The participant’s pelvis was in neutral and body was in a straight line, this position was held for 30 s (Figure 9).

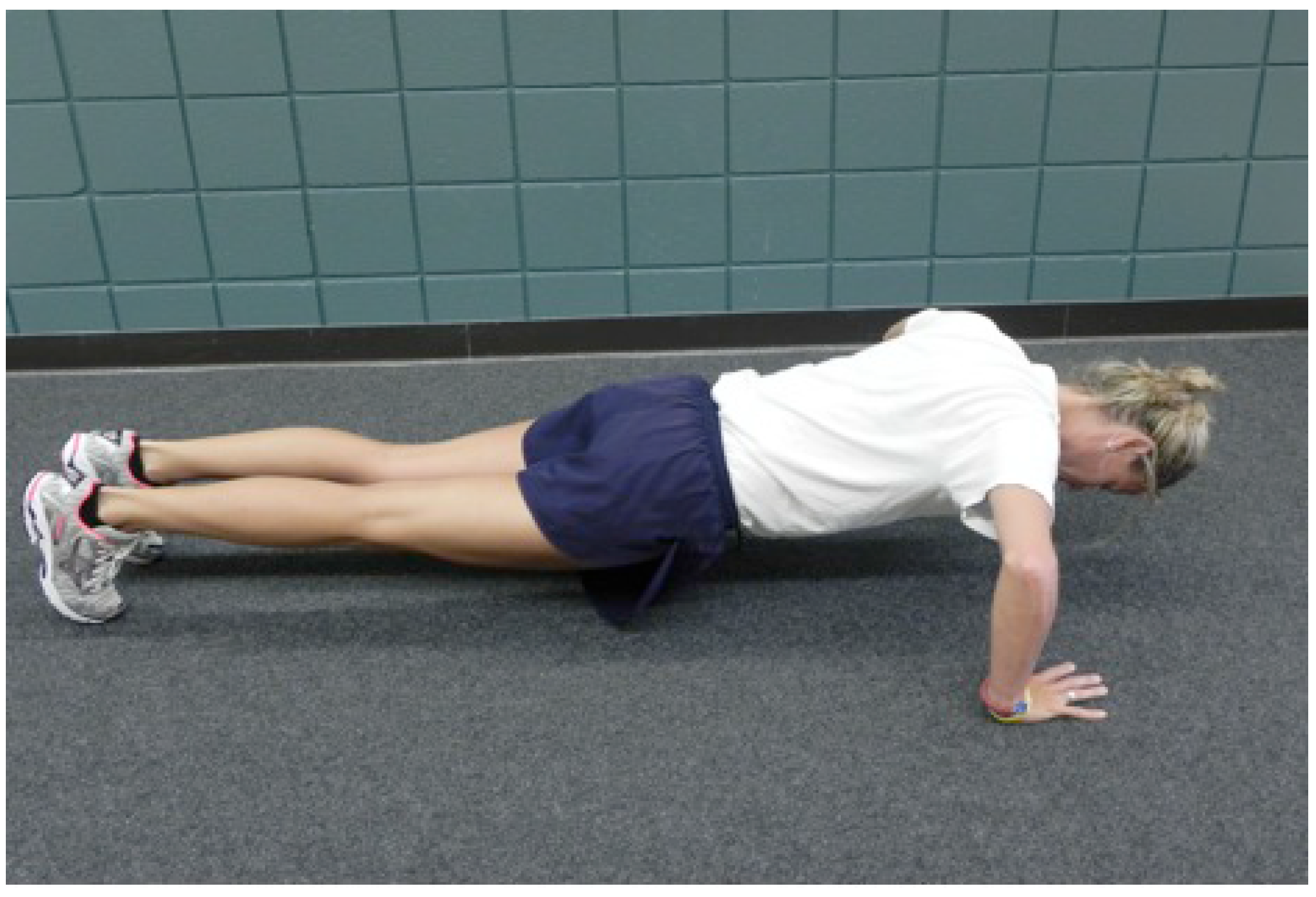
2.5. Statistical Analysis
3. Results
| Control | Intervention | |||
|---|---|---|---|---|
| Muscle | Power | N | Power | N |
| Lower trapezius | 0.45 | 14 | 0.28 | 15 |
| Middle trapezius | 0.77 | 14 | 0.09 | 15 |
| Infraspinatus | 0.14 | 14 | 0.05 | 15 |
| Mutifidus | 0.84 | 14 | 0.21 | 15 |
| Latissimus dorsi | 0.98 | 14 | 0.33 | 15 |
| Serratus Anterior | 0.15 | 14 | 0.98 | 15 |
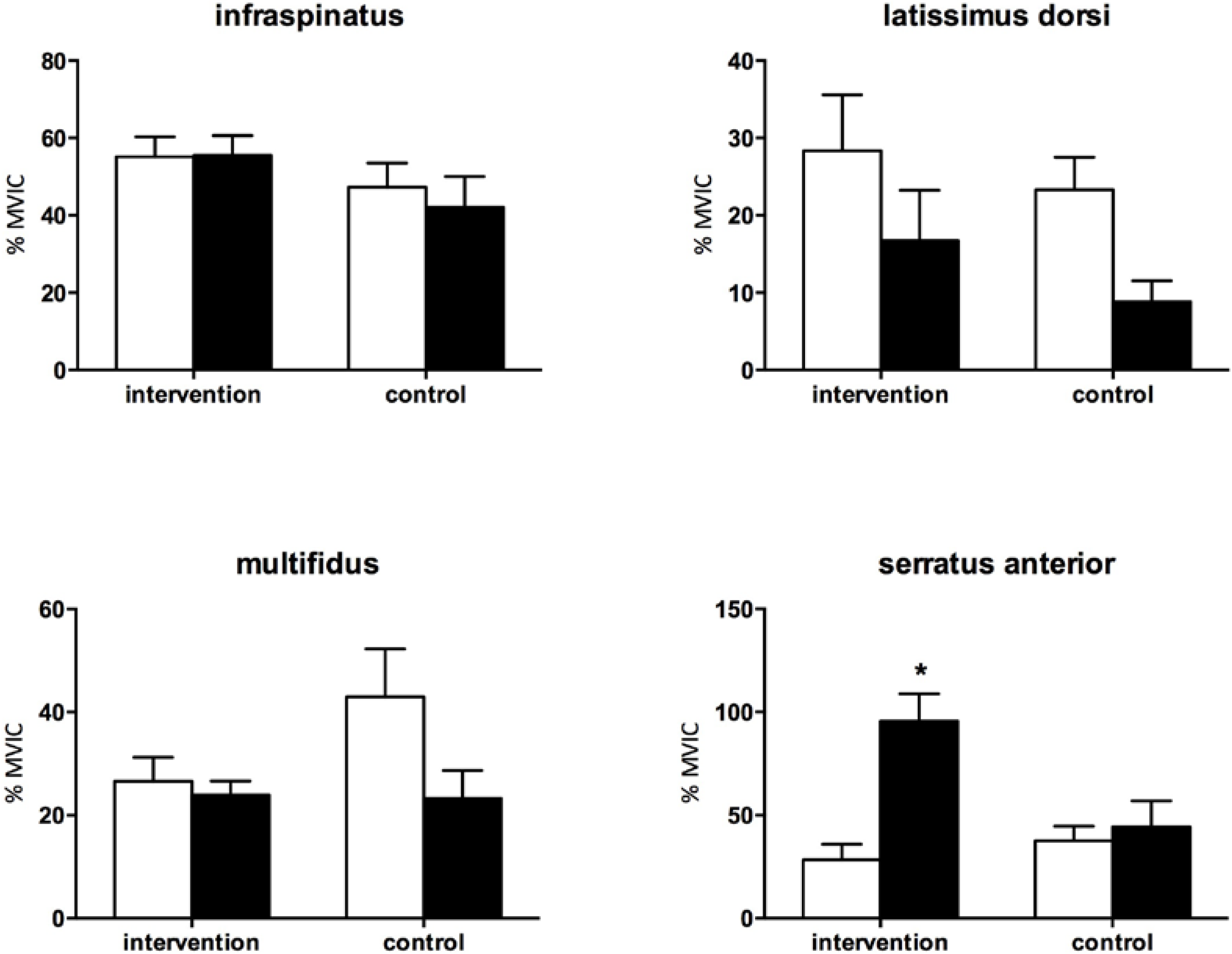
4. Discussion
Author Contributions
Conflicts of Interest
References
- McMullen, J.; Uhl, T.L. A kinetic chain approach for shoulder rehabilitation. J Athl. Train. 2000, 35, 329–337. [Google Scholar] [PubMed]
- Kibler, W.B.; Press, J.; Sciascia, A. The role of core stability in athletic function. Sports Med. 2006, 36, 189–198. [Google Scholar] [CrossRef] [PubMed]
- Kibler, W.B.; Sciascia, A.D.; Uhl, T.L.; Tambay, N.; Cunningham, T. Electromyographic analysis of specific exercises for scapular control in early phases of shoulder rehabilitation. Am. J. Sports Med. 2008, 36, 1789–1798. [Google Scholar] [CrossRef] [PubMed]
- Kibler, W.B.; McMullen, J.; Uhl, T. Shoulder rehabilitation strategies, guidance and practice. Oper. Tech. Sports Med. 2012, 20, 103–112. [Google Scholar] [CrossRef]
- Kibler, W.B. The role of the scapula in athletic shoulder function. Am. J. Sports Med. 1998, 26, 325–337. [Google Scholar] [PubMed]
- Kibler, W.B.; Kuhn, J.E.; Wilk, K.; Sciascia, A.; Moore, S.; Laudner, K.; Ellenbecker, T.; Thigpen, C.; Uhl, T. The disabled throwing shoulder: Spectrum of pathology-10year update. Arthroscopy 2013, 29, 141–161. [Google Scholar] [CrossRef] [PubMed]
- Elliott, B.C.; Marshall, R.; Noffal, G. Contributions of upper limb segment rotation during the power serve in tennis. J. Appl. Biomech. 1995, 11, 443–447. [Google Scholar]
- Linter, D.; Noonan, T.J.; Kibler, W.B. Injury patterns and biomechanics of the athlete’s shoulder. Clin. Sports Med. 2008, 27, 527–552. [Google Scholar] [CrossRef] [PubMed]
- Toyoshima, S.; Miyashita, M. Force-velocity relation in throwing. Res. Quart. 1973, 44, 86–95. [Google Scholar]
- Putnam, C.A. Sequential motions of body segments in striking and throwing skills: Description and explanations. J. Biomech. 1993, 26, 125–135. [Google Scholar] [CrossRef]
- Fleisig, G.S.; Andrews, J.R.; Dillman, C.J.; Escamilla, R.F. Kinetics of baseball pitching with implications about injury mechanisms. Am. J. Sports Med. 1995, 23, 233–239. [Google Scholar] [CrossRef] [PubMed]
- Fleisig, G.S.; Barrentine, S.W.; Escamilla, R.F.; Andrews, J.R. Biomechanics of overhead throwing implications for injury. Sports Med. 1996, 21, 421–437. [Google Scholar] [CrossRef] [PubMed]
- Cordo, P.J.; Nashner, L.M. Properties of postural adjustments associated with rapid arm movements. J. Neurophysiol. 1982, 47, 287–308. [Google Scholar] [PubMed]
- Sciascia, A.; Thigpen, C.; Namdair, S.; Baldwin, K. Kinetic chain abnormalities in the athletic shoulder. Sports Med. Arthrosc. Rev. 2012, 20, 16–21. [Google Scholar] [CrossRef] [PubMed]
- Sewick, A.; Kelly, J.D.; Rubin, B. Physical examination of the overhead athlete’s shoulder. Sports Med. Arthrosc. Rev. 2012, 20, 11–15. [Google Scholar] [CrossRef] [PubMed]
- Hodges, P.W.; Richardson, C.A. Relationship between limb movement speed and associated contraction of the trunk. Ergonomics 1997, 40, 1220–1230. [Google Scholar] [CrossRef] [PubMed]
- Hodges, P.W.; Richardson, C.A. Feedforward contraction of transversus abdominis is not influenced by the direction of arm movement. Exp. Brain Res. 1997, 114, 362–370. [Google Scholar] [CrossRef] [PubMed]
- Oliver, G.D.; Sola, M.; Dougherty, C.P.; Huddleston, S. Quantitative examination of upper and lower extremity muscle activation during common shoulder rehabilitation exercises using the Bodyblade. J. Strength Cond. Res. 2013, 27, 2509–2517. [Google Scholar] [CrossRef] [PubMed]
- Moreside, J.M.; Vera-Garacia, F.J.; McGill, S.M. Trunk muscle activation patterns, lumbar compressive force, and spine stability when using the Bodyblade. Phys. Ther. 2007, 87, 153–521. [Google Scholar] [CrossRef] [PubMed]
- Brumitt, J.; Dale, R.B. Integrating shoulder and core exercises when rehabilitating athletes performing overhead activities. N. Am. J. Sports Phys. Ther. 2009, 4, 132–138. [Google Scholar] [PubMed]
- Oliver, G.D.; Stone, A.J.; Plummer, H. Electromyographic examination of selected muscle activation during isometric exercises. Clin. J. Sports Med. 2010, 20, 452–457. [Google Scholar] [CrossRef] [PubMed]
- Basmajian, J.V.; Deluca, C.J. Apparatus, detection, and recording techniques. In Muscles Alive, Their Functions Revealed by Electromyography, 5th ed.; Butler, J.P., Ed.; Williams and Wilkins: Baltimore, MD, USA, 1985; pp. 19–64. [Google Scholar]
- Cram, J.R.; Kasman, G.S.; Holtz, J. (Eds.) Electrode placement. In Introduction to Surface Electromyography; Aspen Publishers: Gaithersburg, MD, USA, 1998; pp. 237–383.
- Zipp, P. Recommendations for the standardization of lead positions in surface electromyography. Eur. J. Appl. Physiol. 1982, 50, 41–54. [Google Scholar] [CrossRef]
- Hintermeister, R.A.; Lange, G.A.; Schultheis, J.M.; Bey, M.J.; Hawkins, R.J. Electromyographic activity and applied load during shoulder rehabilitation exercises using elastic resistance. Am. J. Sports Med. 1982, 26, 210–220. [Google Scholar]
- Oliver, G.D.; Plummer, H.A. Ground reaction forces, kinematics, and muscle activation during the windmill softball pitch. J. Sport Sci. 2011, 29, 1071–1077. [Google Scholar] [CrossRef] [PubMed]
- Kendall, F.P.; McCreary, E.K.; Provance, P.G. Muscles: Testing and Function, 4th ed.; Williams and Wilkins: Baltimore, MD, USA, 1993. [Google Scholar]
- Oliver, G.D.; Adams-Blair, H.R.; Dougherty, C.P. Implementation of a core stability program for elementary school children. Athl. Train. Sports Health Care 2010, 2, 261–266. [Google Scholar] [CrossRef]
- Roling, K.; Oliver, G.D.; Dittmore, S.; Moiseichik, M. The effects of a lumpopelvic-hip strengthening intervention program on functional testing in collegiate female tennis players. Clin. Kinesiol. 2012, 66, 13–18. [Google Scholar]
- Campbell, B.M.; Stodden, D.F.; Nixon, M.K. Lower extremity muscle activation during baseball pitching. J. Strength Cond. Res. 2010, 24, 964–971. [Google Scholar] [CrossRef] [PubMed]
- Tucker, S.; Armstrong, C.W.; Swartz, E.E.; Campbell, B.; Rankin, J.M. An electromyographic analysis of the cuff link rehabilitation device. J Sport Rehabil. 2005, 14, 124–136. [Google Scholar]
- Cools, A.M.; Lanszweert, F.; Notebaert, D.; Roets, A.; Soetens, B.; Cagnie, B.; Witvrouw, E.E. Rehabilitation of scapular muscle balance. Which exercise to prescribe. Am. J. Sports Med. 2007, 35, 1744–1751. [Google Scholar] [CrossRef] [PubMed]
- Cools, A.M.; Witurouw, E.E.; Declercq, G.; Danneels, L.A.; Cambier, D.C. Scapular muscle recruitment patterns: Trapezius muscle latency with and without impingement symptoms. Am. J. Sports Med. 2003, 31, 542–549. [Google Scholar] [PubMed]
- Cools, A.M.; Witurouw, E.E.; Declercq, G.; Vanderstraeten, G.G.; Cambier, D.C. Evaluation of isokinetic force production and associated muscle activity in the scapular rotators during a protraction-retraction movement in overhead athletes with impingement syndrome. Br. J. Sports Med. 2004, 38, 64–68. [Google Scholar] [CrossRef] [PubMed]
- Cools, A.M.; Witurouw, E.E.; Mahieu, N.N.; Danneels, L.A. Isokinetic scapular muscle performance in overhead athletes with and without impingement symptoms. J. Athl. Train. 2005, 40, 104–110. [Google Scholar] [PubMed]
- Ludewig, P.; Cook, T. Alterations in shoulder kinematics and associated muscle activity in people with symptoms of shoulder impingement. Phys. Ther. 2000, 80, 276–291. [Google Scholar] [PubMed]
- Wadsworth, D.J.S.; Bullock-Saxton, J.E. Recruitment patterns of the scapular rotator muscles in freestyle swimmers with subacromial impingement. Int. J. Sports Med. 1997, 18, 618–624. [Google Scholar] [CrossRef] [PubMed]
© 2015 by the authors; licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Oliver, G.D.; Stone, A.J.; Weimar, W.H.; Lemak, L.; Washington, J.K.; Dougherty, C.P. Upper Extremity Muscle Activation during Bodyblade Exercises Following Six Weeks of Intervention Focusing on the Lumbopelvic-Hip Complex. Sports 2015, 3, 188-201. https://doi.org/10.3390/sports3030188
Oliver GD, Stone AJ, Weimar WH, Lemak L, Washington JK, Dougherty CP. Upper Extremity Muscle Activation during Bodyblade Exercises Following Six Weeks of Intervention Focusing on the Lumbopelvic-Hip Complex. Sports. 2015; 3(3):188-201. https://doi.org/10.3390/sports3030188
Chicago/Turabian StyleOliver, Gretchen D., Audrey J. Stone, Wendi H. Weimar, Lawrence Lemak, Jessica K. Washington, and Christopher P. Dougherty. 2015. "Upper Extremity Muscle Activation during Bodyblade Exercises Following Six Weeks of Intervention Focusing on the Lumbopelvic-Hip Complex" Sports 3, no. 3: 188-201. https://doi.org/10.3390/sports3030188
APA StyleOliver, G. D., Stone, A. J., Weimar, W. H., Lemak, L., Washington, J. K., & Dougherty, C. P. (2015). Upper Extremity Muscle Activation during Bodyblade Exercises Following Six Weeks of Intervention Focusing on the Lumbopelvic-Hip Complex. Sports, 3(3), 188-201. https://doi.org/10.3390/sports3030188





